Abstract
Purpose
Cardiac autonomic dysfunction has been reported in patients with long-standing multiple sclerosis (MS); however, data in early disease are limited. The present study was aimed at evaluating cardiac autonomic function in patients with early MS in the context of white matter metabolic status, which could potentially affect functions of the autonomic brain centers.
Methods
Cardiac sympathetic and baroreflex cardiovagal responses to the Valsalva maneuver, orthostatic test, and the Stroop test were evaluated in 16 early, treatment-naïve patients with relapsing–remitting MS, and in 14 healthy participants. Proton magnetic resonance spectroscopic imaging (MRSI) of the brain was performed in eight of these MS patients and in eight controls.
Results
Valsalva maneuver outcomes were comparable between patients and controls. At baseline, norepinephrine levels were lower (p = 0.027) in MS patients compared to controls. The patients had higher heart rate (p = 0.034) and lower stroke volume (p = 0.008), but similar blood pressure, cardiac output and norepinephrine increments from baseline to 2 min of the orthostatic test compared to controls. MS patients and controls did not differ in responses to the Stroop test. MRSI showed lower total N-acetylaspartate/total creatine (p = 0.038) and higher myo-inositol/total creatine (p = 0.013) in MS lesions compared to non-lesional white matter.
Conclusion
Our results show normal cardiac sympathetic and baroreflex cardiovagal function in MS patients with relapsing–remitting MS with lesions at the post-acute/early resolving stage.
Trial registration
The study was registered at ClinicalTrials.gov under the Identifier: NCT 03052595 and complies with the STROBE checklist for cohort, case–control, and cross-sectional studies.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Multiple sclerosis (MS) is a chronic neuroinflammatory disease of the central nervous system (CNS), leading to demyelination and neurodegeneration. The most frequent symptoms include motor impairment, visual disturbances, sensory problems, pain, fatigue, and cognitive impairment, resulting in severe physical disability [3]. Abnormalities in several domains of the autonomic nervous system (ANS), including sympathetic noradrenergic, parasympathetic cholinergic, and enteric subsystems, have been reported in 45–84% of MS patients [33, 34]. The spectrum of autonomic symptoms appears to depend upon disease-related factors such as clinical form, rate of progression, disability status, lesion localization, or clinical activity at the time of investigation [22, 34]. Furthermore, the severity of dysautonomia ranges from discrete alterations in autonomic functions to clinically apparent symptoms such as bowel and bladder control problems or orthostatic hypotension [13, 26].
In a recent review, Findling and coauthors highlighted the importance of cardiac autonomic dysfunction assessment in MS patients due to its correlation with underlying inflammation and neurodegeneration and association with fatigue, rare serious cardiovascular complications, and implications for treatment [5]. Among the subclinical signs of cardiac autonomic dysfunction, heart rate variability (HRV) in time and frequency domains, abnormal heart rate (HR), and blood pressure have been reported most frequently [2, 8, 25, 27, 30, 37, 40]. Parasympathetic dysfunction seems to correlate with disease progression and disability; thus, it could be the consequence of MS [6]. On the other hand, signs of cardiac sympathetic dysfunction, such as HRV alterations and orthostatic intolerance in MS, appear to correlate more with underlying inflammation and clinical activity at the time of investigation [35]. Recently, Habek and coworkers showed worsening of ANS abnormalities in approximately one third of patients with clinically isolated syndrome during a 2-year follow-up [11]. Overall, cardiac autonomic dysfunction may contribute to disability and cardiovascular complications during disease progression [19].
The neuroendocrine-immune interactions, in particular the immunoregulatory role of the ANS, have generated interest in the role of autonomic dysfunction in the pathogenesis of MS [33]. However, it remains unclear whether the autonomic dysfunction represents a primary factor in MS pathogenesis, or is a mere consequence of the structural damage in the centers regulating ANS activity. Nevertheless, the presence of postural orthostatic tachycardia syndrome in patients with clinical isolated syndrome was found to be a prognostic factor indicating a more active disease course [14]. Investigations of autonomic function in the early stages of the disease before initiation of treatment could help to elucidate the role of dysautonomia in MS pathophysiology [12]. Therefore, the first aim of our study was to evaluate cardiac sympathetic and cardiovagal baroreflex function in treatment-naïve patients with suspected MS at the time of their first referral to a specialized MS center.
Recent advances in proton magnetic resonance spectroscopic imaging (MRSI) of the brain, in particular an increase in spatial resolution, have enabled metabolic activity assessment of the MS lesions without partial volume contamination from normal-appearing tissue [16]. It has also been shown that the pattern of metabolites in the MRSI signal may reflect the evolution of the MS lesions, potentially serving as a marker of disease progression [20]. Furthermore, a limited association between focal lesion burden and physical and cognitive function, known as the clinico-radiological paradox, suggests that MS pathology extends beyond lesions affecting normal-appearing white matter (NAWM) [29]. The latter could theoretically contribute to autonomic dysfunction. Therefore, the second aim of our study was to investigate cardiac autonomic function in the context of lesional white matter (LWM) and non-lesional white matter (NLWM) metabolic status.
Subjects and methods
People with suspected MS were referred to the MS center at the 1st Department of Neurology, Faculty of Medicine, Comenius University by general practitioner offices or outpatient neurology practices in Bratislava, Slovakia. After admission to the MS center, ANS testing was performed before diagnostic lumbar puncture, magnetic resonance imaging (MRI), and initiation of therapy in order to minimize the possible effects of these procedures on autonomic functions. Subsequently, preliminary diagnosis of clinically isolated syndrome (13 patients), relapsing–remitting MS (two patients), suspected demyelinating disorder (two patients), and other neurological disease (nine patients) was established based on the 2010 McDonald criteria [32]. The preliminary diagnosis of all patients enrolled in the study was revised after approximately 2 years of clinical monitoring, and the most recent available diagnosis was used for the present study. From the initial 26 people with suspected MS, the relapsing–remitting form was confirmed in 16 subjects (MS group) after the initial investigations, and this form of MS was ruled out in ten subjects (data not shown). Fourteen healthy subjects served as controls (Table 1). Inclusion criteria for all subjects were as follows: (a) no history of cardiovascular, metabolic, endocrine, renal or hepatic disease, malignancy, or acute or chronic infection; (b) non-smokers; (c) women not pregnant or breastfeeding; (d) and not currently on any medication. Healthy controls were recruited from among the employees of the Biomedical Research Center and 1st Department of Neurology.
All patients and controls gave their written informed consent to participate in the study. The study was approved by the Ethics Committee of the Faculty of Medicine, Comenius University and University Hospital in Bratislava, Slovakia (reference number 110/2016) and by the Ethics Committee of the Bratislava Self-Governing Region, Bratislava, Slovakia (reference number 00581/2017/HF). After a detailed explanation, all subjects participating in the study signed informed consent. For each subject, a complete medical and medication history and physical examination were taken, with emphasis on symptoms and signs of MS. Of all the study participants, eight people with MS and eight healthy subjects, agreed to participate in the MRSI investigation.
All subjects were asked to fast overnight and to abstain from intense physical activity, smoking, caffeine, alcohol, and any medication for 12 h before each test. The testing started between 8:00 and 9:00 am and was performed in a quiet room to prevent possible distractions. Body height was measured manually, and body weight, body mass index, and percentage body fat were determined with quadrupedal bioimpedance (BF-511, Omron, Kyoto, Japan). An intravenous catheter was inserted into the cubital vein and subjects were asked to rest in the supine position for at least 15 min. The baseline blood sample was taken, and blood pressure was measured after this stabilization period in the supine position.
For assessment of cardiovagal baroreflex function, noninvasive measurement of beat-to-beat blood pressure was obtained using a Nexfin (BMEYE, Amsterdam, The Netherlands) device. After at least a 15-min baseline period after catheter insertion, while supine with head on the pillow, each subject performed at least two Valsalva maneuvers approximately 5 min apart, as described elsewhere [10, 18]. Briefly, the patient blew into a plastic tube connected to a sphygmomanometer, maintaining pressure of 30 mmHg for 12 s. The cardiovagal baroreflex gain (BRG) was calculated as the slope of the relationship between the cardiac inter-beat interval and the beat-to-beat systolic blood pressure (SBP) (with a 1-beat delay) during the descent of pressure in Phase II of the maneuver. A slope of 3 ms/mmHg or less, about one half of normal, defined cardiovagal baroreflex failure [9]. A Valsalva ratio (VR) was calculated to provide information pertaining to cardiovagal function. The VR was calculated by obtaining the maximum HR (HRmax) generated during the maneuver divided by the minimum HR (HRmin) attained within 30 s of the peak HR (VR = HRmax/HRmin). The HR change in Phase IV was calculated as HRmax − HRmin. In addition to the HR analysis, the blood pressure-related outcomes of the Valsalva maneuver were analyzed as described elsewhere [36]. Briefly, baseline blood pressure was calculated as an average of the SBP approximately 1 min preceding each Valsalva maneuver, with the exclusion of the 15 s immediately prior to the test. Phase II Early drop was measured as the difference between the baseline blood pressure and Phase II Early; Phase II Late rise was calculated as the rise in SBP from Phase II Early to Phase II Late; Phase IV overshoot was calculated as the difference between the baseline blood pressure and the maximal SBP value after termination of expiration: pressure recovery time was calculated as the duration from the lowest SBP in Phase III until the blood pressure reached baseline. Flat-top responses were classified as Phase II Early, not descending below baseline blood pressure. Observations with no rise in blood pressure following Phase II Early during the Valsalva maneuver were classified as responses with no Phase II Late.
After a stabilization period of approximately 15 min, the orthostatic test was performed on a motorized tilt table for 10 min, as described elsewhere [17]. In the case of orthostatic intolerance symptoms, e.g. lightheadedness or presyncope, the patient was tilted back to the supine position before the end of the test at 10 min. An electrocardiogram was recorded continuously using a PowerLab device and LabChart software (ADInstruments Pty Ltd, Australia) connected to a personal computer during the Valsalva maneuver and the orthostatic test. Data extraction for SBP, diastolic blood pressure (DBP), HR, stroke volume (SV), and systemic vascular resistance (SVR) was performed on the approximately 1-min artifact-free recording from the noninvasive continuous blood pressure monitor (Nexfin, BMEYE, Amsterdam, Netherlands) before and 1, 2, 3, and 5 min after tilt. Cardiac output (CO) was calculated from the extracted SV and HR values in the respective time intervals. The blood pressure module for LabChart software (ADInstruments Pty Ltd, Australia) was used to extract SBP data from Valsalva maneuver recordings. For assessment of HRV, approximately 5-min-long artifact-free electrocardiogram segments corresponding to the time of blood sampling were analyzed using the HRV module for LabChart software (ADInstruments Pty Ltd, Australia). The following HRV parameters were calculated: mean length of the NN (normal-to-normal) interval, total power (TP) in the range of 0.00–0.40 Hz, low-frequency power (LF) in the range of 0.04–0.15 Hz, high-frequency power (HF) in the range of 0.15–0.40 Hz, LF/HF ratio, and LF and HF in normalized units (LFnu, HFnu). The LFnu was calculated using the equations LFnu = 100.0 × LF Power/(Total Power − VLF Power) and HFnu = 100.0 × HF Power/(Total Power − VLF Power) by the HRV module. If respiratory rhythm at the time of measurement was less than nine per min (0.15 Hz), the electrocardiogram sample was excluded from HRV analysis.
In the present study, the Stroop color and word test was used as a mental challenge, as described elsewhere [7]. Briefly, the test is based on the interference between the words and the colors. Sample color words are printed in colored fonts, which are incongruent with respect to the color word itself. The total duration of the mental stress procedure was 10 min. Before the Stroop test started, the subjects were asked to change from supine to sitting position, the ECG leads and blood pressure finger cuff used in the previous testing (the orthostatic test) were disconnected, and the testing procedure was explained in detail by the investigator. After at least 15 min in sitting position, baseline blood samples were collected (0 min); the second blood sample was taken at the end of the Stroop test (10 min). Blood pressure was measured using a digital sphygmomanometer (Omron M2, Omron Corporation, Kyoto, Japan) by manually triggering measurement before and after the Stroop test at 10 min. HRV was not analyzed due to speech interference with breathing patterns during the Stroop test.
For the orthostatic and Stroop tests, blood was drawn into polyethylene tubes with EDTA as anticoagulant and immediately cooled in ice. After centrifugation at 4 °C, all plasma aliquots were stored at −70 °C until assay. Plasma epinephrine (EPI) and norepinephrine (NE) concentrations were measured with commercially available enzyme-linked immunosorbent assay kits (Demeditec Diagnostics GmbH, Kiel, Germany) according to the manufacturer’s instructions.
Proton magnetic resonance spectroscopic imaging (1H MRSI) was performed on a 7 T whole-body MR scanner (Magnetom; Siemens Healthcare, Erlangen, Germany) using a 32-channel head coil (Nova Medical, Wilmington, MA, USA). Anatomical images (three-dimensional T2-weighted fluid-attenuated inversion recovery and three-dimensional T1-weighted magnetization-prepared 2 rapid acquisition gradient echoes) were acquired to visualize MS lesions and position MRSI volume of interest. MR spectra were obtained with two-dimensional MRSI based on free induction decay acquisition and with fourfold parallel imaging acceleration implemented [1, 15, 41]. The sequence parameters were as follows: acquisition delay/repetition time, 1.3/200 ms; field of view, 200 × 200 mm2; slice thickness, 8 mm; matrix size, 100 × 100; nominal voxel volume, 2.2 × 2.2 × 8 mm3; flip angle, 29°; acquisition time, 6:06 min. In-house-developed software was used for automatic data processing, including LCModel (version 6.3-1; http://s-provencher.com/lcmodel.shtml) spectral fitting. Three regions of interest were analyzed: lesional white matter (LWM) and non-lesional white matter (NLWM) in people with MS, and normal-appearing white matter (NAWM) in healthy participants. The regions were drawn manually on corresponding T2-weighted fluid-attenuated inversion recovery images using ITK-SNAP software (version 3.6; http://www.itksnap.org/pmwiki/pmwiki.php). In NLWM, one region of interest was placed close to the LWM (< 1 cm) and another, if possible, far from the LWM (> 3 cm). For each location, i.e. LWM, NLWM close to lesion, NLWM far from a lesion, and NAWM, two regions were drawn per subject.
Statistical analyses were performed using IBM SPSS Statistics version 19 (SPSS Inc., Chicago, IL, USA). Changes associated with the tilt table test were analyzed using the general linear model for repeated measures. Group differences in mean values were analyzed by Student’s t test or the Mann–Whitney U test, depending on the normality of the data distributions. The paired-sample t test was used to analyze the mean ratios of MRSI brain metabolites in LWM compared to NLWM in people with MS. Autonomic testing outcomes were correlated with MRSI data using the nonparametric Spearman’s rank test. All values are expressed as mean ± standard error of the mean unless stated otherwise. Fisher’s exact test was used to calculate proportions of subjects with orthostatic intolerance during the tilt table test. A p value of less than 0.05 was considered statistically significant.
Results
After the definitive diagnosis of relapsing–remitting MS was confirmed or ruled out, non-MS subjects were excluded from further analyses. The basic characteristics of the people with MS and healthy participants are shown in Table 1. BRG measured during late phase II of the Valsalva maneuver did not differ between people with MS and healthy participants. All the subjects had BRG higher than 3 ms/mmHg. HRmax, HRmin, and VR and HR change in Phase IV of the test were comparable between the MS and control groups (Table 2). SBP responses to the Valsalva maneuver during the Phase II Early, Phase II Late, Phase IV, and pressure recovery time were comparable between the groups. Two people with MS (12.5%) and one healthy participant (7.1%) had flat-top response to the Valsalva maneuver.
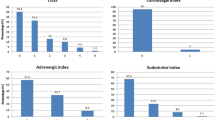
Orthostatic intolerance occurred in one MS subject and in one healthy participant during the orthostatic test. These subjects were immediately placed in the supine position, and blood samples were taken prematurely. Head-up tilt caused a significant increase in DBP (Fig. 1), CO, SVR, EPI, and NE (p < 0.001 for all parameters) compared to the supine position. LFnu and LF/HF ratio significantly increased (p < 0.001), and HFnu significantly decreased (p < 0.001) during the orthostatic test compared to the supine position. During the orthostatic test, the changes in HR (p = 0.034) and SV (p = 0.008) between 2 min and baseline were significantly larger in the MS group than in the control group (Fig. 1). Although the baseline plasma NE was lower (p = 0.018) in MS patients than in controls, the groups did not differ in NE response to orthostasis (Fig. 1). Responses of SBP, DBP, CO, SVR, EPI, LFnu, HFnu, and LF/HF ratio to head-up tilt were comparable between the MS and control groups.
Systolic (circles) and diastolic (squares) blood pressure (a), heart rate (b), stroke volume (c), and norepinephrine (d) responses to orthostasis in 16 relapsing–remitting multiple sclerosis patients (MS, filled symbols) and 14 healthy controls (empty symbols). NS nonsignificant, *p = 0.034 (general linear model for repeated measures), ##p = 0.008 (general linear model for repeated measures), +p = 0.018 (t test)
SBP and EPI were significantly (p < 0.05 for all measures) higher at 10 min of the Stroop color and word test compared to baseline. However, the increases were comparable between the groups, with only a tendency toward lower EPI (p = 0.076) in people with MS compared to healthy participants. DBP, NE, and HR did not change significantly in response to the Stroop test.
MRSI data are shown in Table 3 and in Fig. 2. The NLWM of MS patients localized close to suspected lesions and far from them (data not shown) did not differ in any of the analyzed MRSI parameters; therefore, only NLWM close to lesions was used for further analysis. LWM had lower total N-acetylaspartate (tNAA)/total creatine (tCr) (p = 0.038) and higher myo-inositol (mIns)/tCr (p = 0.013), higher mIns/tNAA (p = 0.01), and higher choline-containing metabolites (tCho)/tNAA (p = 0.028) in the MS group. LWM had also lower tNAA/tCr (p = 0.001) and higher (p < 0.001) mIns/tCr, higher mIns/tNAA (p = 0.001), and higher tCho/tNAA (p = 0.01) compared to the control group. In addition, the similar trend in lower tNAA and higher mIns was also observed in the NLWM of MS patients versus healthy participants (Table 3). Glutamate-glutamine (Glx)/tNAA and Glx/tCr ratios did not differ between MS and controls. There was a positive correlation between Glx/tNAA and VR in the NLWM of MS patients (r = 0.79, p = 0.021, n = 8) but not in the NAWM of controls during the Valsalva maneuver (Table 4). Similarly, a positive correlation was found between Glx/tCr and HR variability in the low-frequency spectrum (r = 0.79, p = 0.021, n = 8) as well as a negative correlation between Glx/tCr and HR variability in the high-frequency band (r = −0.74, r = 0.037, n = 8) at 2 min of the orthostatic test. On the other hand, a positive correlation was found between these Glx ratios and NE increments during the orthostatic test in healthy participants but not in patients with MS (Table 4).
Examples of metabolic images acquired with proton magnetic resonance spectroscopic imaging at 7 T in a person with multiple sclerosis (MS) and healthy control (CON) (a) together with representative MR spectra from lesional (MS lesion) and non-lesional white matter of MS patient (NLWM) and normal-appearing white matter (NAWM) of healthy control (b). tNAA Total N-acetylaspartate, tCr total creatine, mIns myo-inositol, tCho choline-containing metabolites, Glx glutamate and glutamine, FLAIR fluid-attenuated inversion recovery, T1w T1-weighted
Discussion
In the present study, we evaluated sympathetic noradrenergic and cardiovagal baroreflex functions in people with relapsing–remitting MS. Our results show normal catecholamine and cardiac autonomic responses to non-postural and postural hemodynamic blood pressure changes as well as to mental stress. These results indicate preserved autonomic control of the cardiovascular system at around the first episode of neurological symptoms of MS and before the initiation of therapy.
As reviewed recently, sympathetic activity may be significantly increased during the early stages of MS, while later disease stages may lead to progressive noradrenergic failure and adrenergic receptor dysfunction [5, 23, 33]. Our present results are in line with the former, showing higher HR response to an orthostatic challenge in people with MS at the early stages of the disease compared to healthy participants. The findings of higher HR response to a significantly larger SV decrease in the MS group compared to controls during the tilting confirms that sympathetic noradrenergic activation was able to maintain adequate blood pressure in subjects with suspected MS. Moreover, normal baroreflex gain and SBP responses during the Valsalva maneuver indicate well-preserved sympathetic-mediated baroreflex function in our group of relapsing–remitting MS subjects. Comparable plasma NE and EPI responses to orthostasis and mental challenge between patients and controls support the interpretation of our findings.
An assessment of the baroreflex provides important information on the function of the sympathetic noradrenergic and parasympathetic cholinergic (vagal) branches of the ANS. In addition to high-frequency power of HRV as a generally accepted respiration-related measure of parasympathetic cardiovagal outflow, low-frequency power has been shown to reflect baroreflex-mediated phasic changes in cardiovagal and sympathetic noradrenergic outflows [28]. In our study, comparable VR and HRV in the high-frequency spectrum between patients with MS and healthy participants indicate normal cardiovagal function in the early stages of MS. Overall our findings are consistent with the notion that cardiac autonomic failure develops with MS progression, reflecting structural damage of centers involved in cardiovascular control and cardiovascular responses [5, 23, 33, 42]. In line with the results of other studies [4], the observed changes in cardiac autonomic function in our study may reflect cardiovascular deconditioning during the extremely stressful period of life for suspected MS subjects, as commonly seen in cancer patients [24].
In recent years, MRSI has been used to measure metabolite concentrations in lesions as well as in the NAWM of MS patients in order to identify a stage of disease. Characteristic metabolic markers tNAA reflects neuroaxonal integrity; tCr represents a putative marker for cell proliferation; tCho involved in membrane turnover represents the course of inflammation, demyelination, and remyelination; Ins indicates glial (astrocytic) proliferation; and Glx are markers of glia-neuron metabolism based on non-oxidative glucose consumption [31]. As expected, our results of in vivo MRSI showed lower tNAA/tCr and higher mIns/tCr ratios in the LWM of MS patients, reflecting a decline in neuronal health, mitochondrial function, astroglial activation, and gliosis [38]. In contrast to previous studies with conventional MRSI or single-voxel spectroscopy methods, the present results were acquired at much higher spatial resolution (i.e. ~ 2 × 2 mm2 in-plane), which allowed us to assess relatively small MS lesions without the partial volume bias typical for low-resolution MRSI [16]. Recently, Kirov et al. described a sequence of changes in MRSI metabolites in pre-lesional tissue and acute and resolving MS lesions [20]. Based on the specific temporal pattern of tNAA and mIns, i.e., the decline in acute lesions followed by a gradual return to pre-lesion levels in tNAA and higher mIns in resolving lesions [20], the lesions analyzed in our patients with MS were likely in the post-acute/early resolving stage. On the other hand, only a modest difference in the tCho signal was detected in lesions of our MS group compared to the control group, consistent with the early stages of the disease characterized more by neuroinflammation than de- and remyelination.
A longitudinal MRSI observation by Kirov et al. showed that diffuse white matter glial abnormalities were present in MS, suggesting that brain functions other than those affected by actual lesions can contribute to the disease pathophysiology [21]. In our study, the similar pattern of lower tNAA/tCr and higher mIns/tCr ratios, as detected in lesions, was also found in the NLWM of MS subjects compared to healthy controls, suggesting that neuronal health, mitochondrial function, and glial activation might not be exclusive to areas affected by inflammatory reactions, but also present nonspecifically in other brain areas. Theoretically, these nonspecific changes could affect brain regions involved in autonomic control in MS. Our study explored this possibility by correlating MRSI signal with clinical and neurochemical outcomes of cardiac autonomic testing, i.e., Valsalva maneuver and the orthostatic test. Interestingly, we found an association between Glx signal and markers of sympathetic/parasympathetic balance during the latter two tests in people with MS but not in healthy participants. These correlations suggest a possible link between the NLWM metabolic activity in MS and sympathetic/parasympathetic balance; however, this interpretation is limited by the low number of subjects in the MRSI part of our study. Further large-scale MRSI studies are necessary to analyze the metabolic activity of brain regions involved in autonomic control in MS.
The major limitation of the present study is the relatively small number of studied subjects due to strict inclusion criteria and relatively short time period between MS diagnosis and treatment initiation at our center. Another important limitation of our study is that the disease activity could not be measured using the annualized relapse rate or relapse-free proportions due to the relatively short follow-up period after the initial investigation. The most appropriate way to perform the Valsalva maneuver is to maintain 40 mmHg expiratory pressure for 15 s; however, in our study the 30 mmHg target pressure with 12 s duration was chosen to minimize difficulties in maintaining the target pressure by people with MS, especially those in the relapse phase of the disease. The lower target expiratory pressure and shorter duration of the forceful exhalation phase of the test might have affected the outcomes of the Valsalva maneuver. The height of the mercury column should be maintained at 40 mm (not 30 mm). A high degree of variability in clinical MRI findings, i.e., supra- and infratentorial localization of lesions, did not allow us to infer a possible association between potential damage to autonomic centers and autonomic functions, and the MRSI was not a priori targeted to the autonomic centers of the brain. In our study, the Nexfin device was used to monitor beat-to-beat blood pressure, HR, SV, CO, and SVR during the orthostatic test. Although noninvasive photoplethysmography has been shown to reliably estimate blood pressure and HR changes, the use of this method for hemodynamic parameters, i.e. SV, CO, and SVR, remains controversial [39].
In conclusion, our results show normal cardiac sympathetic and baroreflex cardiovagal function in people with relapsing–remitting MS. Rather than being the primary factor in the MS pathogenesis, these results suggest that autonomic dysfunction develops as a secondary epiphenomenon with disease progression. Our MRSI findings reflect a decline in neuronal health, mitochondrial function, astroglial activation, and gliosis in the LWM, consistent with the post-acute/early resolving stage of the lesions in our group of people with MS. In addition to LWM, our data show that metabolic changes are also present in the NLWM of MS subjects.
Availability of data and materials
The data sets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Bogner W, Gruber S, Trattnig S, Chmelik M (2012) High-resolution mapping of human brain metabolites by free induction decay (1)H MRSI at 7 T. NMR Biomed 25:873–882
Damla O, Altug C, Pinar KK, Alper K, Dilek IG, Kadriye A (2018) Heart rate variability analysis in patients with multiple sclerosis. MultSclerRelatDisord 24:64–68
Dendrou CA, Fugger L, Friese MA (2015) Immunopathology of multiple sclerosis. Nat Rev Immunol 15:545–558
Feltham MG, Collett J, Izadi H, Wade DT, Morris MG, Meaney AJ, Howells K, Sackley C, Dawes H (2013) Cardiovascular adaptation in people with multiple sclerosis following a twelve week exercise programme suggest deconditioning rather than autonomic dysfunction caused by the disease. Results from a randomized controlled trial. Eur J Phys Rehabil Med 49:765–774
Findling O, Hauer L, Pezawas T, Rommer PS, Struhal W, Sellner J (2020) Cardiac autonomic dysfunction in multiple sclerosis: a systematic review of current knowledge and impact of immunotherapies. J Clin Med 9:335
Flachenecker P, Reiners K, Krauser M, Wolf A, Toyka KV (2001) Autonomic dysfunction in multiple sclerosis is related to disease activity and progression of disability. MultScler 7:327–334
Garafova A, Penesova A, Cizmarova E, Marko A, Vlcek M, Jezova D (2014) Cardiovascular and sympathetic responses to a mental stress task in young patients with hypertension and/or obesity. Physiol Res 63(Suppl 4):S459-467
Gervasoni E, Bove M, Sinatra M, Grosso C, Rovaris M, Cattaneo D, Merati G (2018) Cardiac autonomic function during postural changes and exercise in people with multiple sclerosis: a cross-sectional study. MultSclerRelatDisord 24:85–90
Goldstein DS, Cheshire WP Jr (2017) Beat-to-beat blood pressure and heart rate responses to the Valsalva maneuver. ClinAuton Res 27:361–367
Goldstein DS, Imrich R, Peckham E, Holmes C, Lopez G, Crews C, Hardy J, Singleton A, Hallett M (2007) Neurocirculatory and nigrostriatal abnormalities in Parkinson disease from LRRK2 mutation. Neurology 69:1580–1584
Habek M, Crnosija L, Gabelic T, Barun B, Adamec I, Junakovic A, Ruska B, Pavicic T, KrbotSkoric M (2019) Longitudinal assessment of autonomic nervous system in patients with first demyelinating event suggestive of multiple sclerosis. Eur J Neurol 26:1377–1383
Habek M, Crnosija L, Lovric M, Junakovic A, KrbotSkoric M, Adamec I (2016) Sympathetic cardiovascular and sudomotor functions are frequently affected in early multiple sclerosis. ClinAuton Res 26:385–393
Habek M, KrbotSkoric M, Crnosija L, Adamec I (2015) Brainstem dysfunction protects against syncope in multiple sclerosis. J NeurolSci 357:69–74
Habek M, KrbotSkoric M, Crnosija L, Gabelic T, Barun B, Adamec I (2017) Postural orthostatic tachycardia predicts early conversion to multiple sclerosis after clinically isolated syndrome. EurNeurol 77:253–257
Hangel G, Strasser B, Povazan M, Heckova E, Hingerl L, Boubela R, Gruber S, Trattnig S, Bogner W (2018) Ultra-high resolution brain metabolite mapping at 7 T by short-TR Hadamard-encoded FID-MRSI. Neuroimage 168:199–210
Heckova E, Strasser B, Hangel GJ, Povazan M, Dal-Bianco A, Rommer PS, Bednarik P, Gruber S, Leutmezer F, Lassmann H, Trattnig S, Bogner W (2019) 7 T magnetic resonance spectroscopic imaging in multiple sclerosis: how does spatial resolution affect the detectability of metabolic changes in brain lesions? Invest Radiol 54:247–254
Imrich R, Alevizos I, Bebris L, Goldstein DS, Holmes CS, Illei GG, Nikolov NP (2015) Predominant glandular cholinergic dysautonomia in patients with primary Sjogren’s syndrome. Arthritis Rheumatol 67:1345–1352
Imrich R, Vernino S, Eldadah BA, Holmes C, Goldstein DS (2009) Autoimmune autonomic ganglionopathy: treatment by plasma exchanges and rituximab. ClinAuton Res 19:259–262
Kaplan TB, Berkowitz AL, Samuels MA (2015) Cardiovascular dysfunction in multiple sclerosis. Neurologist 20:108–114
Kirov II, Liu S, Tal A, Wu WE, Davitz MS, Babb JS, Rusinek H, Herbert J, Gonen O (2017) Proton MR spectroscopy of lesion evolution in multiple sclerosis: steady-state metabolism and its relationship to conventional imaging. Hum Brain Mapp 38:4047–4063
Kirov II, Tal A, Babb JS, Herbert J, Gonen O (2013) Serial proton MR spectroscopy of gray and white matter in relapsing-remitting MS. Neurology 80:39–46
KrbotSkoric M, Crnosija L, Adamec I, Barun B, Gabelic T, Smoljo T, Stanic I, Pavicic T, Pavlovic I, Drulovic J, Pekmezovic T, Habek M (2019) Autonomic symptom burden is an independent contributor to multiple sclerosis related fatigue. ClinAuton Res 29:321–328
KrbotSkoric M, Crnosija L, Gabelic T, Barun B, Adamec I, Junakovic A, Pavicic T, Ruska B, Habek M (2019) Autonomic symptom burden can predict disease activity in early multiple sclerosis. MultSclerRelatDisord 28:250–255
Lakoski SG, Eves ND, Douglas PS, Jones LW (2012) Exercise rehabilitation in patients with cancer. Nat Rev ClinOncol 9:288–296
Limmroth V, Ziemssen T, Kleiter I, Wagner B, Schmidt S, Lassek C, Baier-Ebert M, Wendt G, Dechend R, Haverkamp W (2020) A Comprehensive monitoring study on electrocardiographic assessments and cardiac events after fingolimod first dose-possible predictors of cardiac outcomes. Front Neurol 11:818
Lin SD, Butler JE, Boswell-Ruys CL, Hoang P, Jarvis T, Gandevia SC, McCaughey EJ (2019) The frequency of bowel and bladder problems in multiple sclerosis and its relation to fatigue: a single centre experience. PLoS ONE 14:e0222731
Mahovic D, Lakusic N (2007) Progressive impairment of autonomic control of heart rate in patients with multiple sclerosis. Arch Med Res 38:322–325
Moak JP, Goldstein DS, Eldadah BA, Saleem A, Holmes C, Pechnik S, Sharabi Y (2007) Supine low-frequency power of heart rate variability reflects baroreflex function, not cardiac sympathetic innervation. Heart Rhythm 4:1523–1529
Mollison D, Sellar R, Bastin M, Chandran S, Wardlaw J, Connick P (2017) The clinico-radiological paradox of cognitive function and MRI burden of white matter lesions in people with multiple sclerosis: a systematic review and meta-analysis. PLoS ONE 12:e0177727
Monge-Argiles JA, Palacios-Ortega F, Vila-Sobrino JA, Matias-Guiu J (1998) Heart rate variability in multiple sclerosis during a stable phase. ActaNeurolScand 97:86–92
Obert D, Helms G, Sattler MB, Jung K, Kretzschmar B, Bahr M, Dechent P, Diem R, Hein K (2016) Brain metabolite changes in patients with relapsing-remitting and secondary progressive multiple sclerosis: a two-year follow-up study. PLoS ONE 11:e0162583
Polman CH, Reingold SC, Banwell B, Clanet M, Cohen JA, Filippi M, Fujihara K, Havrdova E, Hutchinson M, Kappos L, Lublin FD, Montalban X, O’Connor P, Sandberg-Wollheim M, Thompson AJ, Waubant E, Weinshenker B, Wolinsky JS (2011) Diagnostic criteria for multiple sclerosis: 2010 revisions to the McDonald criteria. Ann Neurol 69:292–302
Racosta JM, Kimpinski K (2016) Autonomic dysfunction, immune regulation, and multiple sclerosis. ClinAuton Res 26:23–31
Racosta JM, Kimpinski K, Morrow SA, Kremenchutzky M (2015) Autonomic dysfunction in multiple sclerosis. AutonNeurosci 193:1–6
Racosta JM, Sposato LA, Morrow SA, Cipriano L, Kimpinski K, Kremenchutzky M (2015) Cardiovascular autonomic dysfunction in multiple sclerosis: a meta-analysis. MultSclerRelatDisord 4:104–111
Rasmussen TK, Hansen J, Low PA, Sandroni P, Singer W, Jensen TS, Terkelsen AJ (2017) Autonomic function testing: compliance and consequences. AutonNeurosci 208:150–155
Reynders T, Gidron Y, De Ville J, Bjerke M, Weets I, Van Remoortel A, Devolder L, D’Haeseleer M, De Keyser J, Nagels G, D’Hooghe MB (2019) Relation between heart rate variability and disease course in multiple sclerosis. J Clin Med 9:3
Rovira A, Alonso J (2013) 1H magnetic resonance spectroscopy in multiple sclerosis and related disorders. Neuroimaging Clin N Am 23:459–474
Sauder KA, Pokorney PE, McCrea CE, Ulbrecht JS, Kris-Etherton PM, West SG (2015) Noninvasive assessment of hemodynamics: a comparative analysis of fingertip pulse contour analysis and impedance cardiography. Blood Press Monit 20:209–214
Shirbani F, Barin E, Lee YC, Ng K, Parratt JDE, Butlin M, Avolio AP (2018) Characterisation of cardiac autonomic function in multiple sclerosis based on spontaneous changes of heart rate and blood pressure. MultSclerRelatDisord 22:120–127
Strasser B, Povazan M, Hangel G, Hingerl L, Chmelik M, Gruber S, Trattnig S, Bogner W (2017) (2 + 1)D-CAIPIRINHA accelerated MR spectroscopic imaging of the brain at 7T. MagnReson Med 78:429–440
Vlcek M, Penesova A, Imrich R, Meskova M, Mravcova M, Grunnerova L, Garafova A, Sivakova M, Turcani P, Kollar B, Jezova D (2018) Autonomic nervous system response to stressors in newly diagnosed patients with multiple sclerosis. Cell MolNeurobiol 38:363–370
Funding
This study was supported by the following grants: Slovak Research and Development Agency (APVV-15-0228), Ministry of Health of the Slovak Republic (MZ- 2018/37-LFUK-11), and the Austrian Science Fund (KLI 718).
Author information
Authors and Affiliations
Contributions
RI and PT made substantial contributions to the study preparation, design of the examinations, and obtaining the approvals. MS, PS, and BK were responsible for the neurological examination of the patients, diagnosis, treatment, and obtaining informed consent from the participants. AH was responsible for blood processing, analysis of measures, analysis of inflammatory parameters, and interpretation of data. AP, MV, RI, and ŽR performed autonomic testing; TS performed data extraction and analyses. EH, GH, BS, and WB were responsible for the MR spectroscopic imaging sequence development and data acquisition, processing, and evaluation. All authors read the manuscript, added valuable comments to its improvement, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors of the manuscript declare that they have no competing interests.
Ethics approval and consent to participate
The Ethics Committee of the Faculty of Medicine, Comenius University, and University Hospital in Bratislava, Slovakia, approved the study design on December 12, 2016, under reference number 110/2016. The Ethics Committee of the Bratislava Self-Governing Region, Bratislava, Slovakia, approved the study on March 7, 2017, under reference number 00581/2017/HF.
Consent to participate
After detailed explanation, all subjects participating in the study signed informed consent.
Consent for publication
The manuscript does not contain any individual personal data in any form. All authors reviewed the final version of the manuscript and agree with the submission.
Rights and permissions
About this article
Cite this article
Imrich, R., Vlcek, M., Penesova, A. et al. Cardiac autonomic function in patients with early multiple sclerosis. Clin Auton Res 31, 553–562 (2021). https://doi.org/10.1007/s10286-021-00790-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10286-021-00790-w