Abstract
We have previously found that ex vivo expanded human CD4+CD25+Treg cells suppress proliferation of lymphoma B-cell lines. Here we demonstrate that the immunomodulatory drug lenalidomide potentiates suppression of lymphoma B-cell proliferation by freshly isolated CD4+CD25+Tregs, as well as suppression by Tregs expanded polyclonally in the presence of rapamycin from CD4+CD25+T cells or CD4+CD25+CD127loT cells. The regulation of lymphoma cell proliferation by Tregs pre-expanded with “third-party” allogeneic MoDCs in the presence of rapamycin was also potentiated by lenalidomide. Lenalidomide contributed to the suppression exerted by Tregs despite concomitant downregulation of Treg proliferation. Lenalidomide did not reduce the suppression of conventional T cells by expanded Tregs. The exposure of polyclonally expanded Tregs to lenalidomide did not significantly alter their phenotype. There was no uniform pattern of lenalidomide effect on Treg-mediated regulation of lymphoma B cells freshly isolated from patients. Freshly isolated lymphoma cells activated with multimeric CD40L and IL-4 to support their survival in vitro varied in their sensitivity to lenalidomide, and the regulatory effect of Tregs on such lymphoma cells ranged from suppression to help in individual patients. Lenalidomide potentiated or attenuated Treg effects on the survival of freshly isolated lymphoma cells. A combination of lenalidomide treatment with adoptive transfer of CD4+CD25+Tregs or CD4+CD25+CD127loTregs expanded ex vivo could be used to suppress proliferation of residual lymphoma in select patients with lymphoma responsive to the regulation by Tregs and sensitive to lenalidomide.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lenalidomide (Revlimid®), a synthetic derivate of thalidomide, is a drug with anti-angiogenic, anticancer, and pleiotropic immunomodulatory activities [1]. Lenalidomide has been approved by the US Food and Drug Administration for the treatment of patients (pts) with transfusion-dependent anemia due to low- or intermediate-1-risk deletion 5q myelodysplastic syndromes, with mantle cell lymphoma (MCL) relapsed or progressed after two prior therapies, and in combination with dexamethasone for the treatment of pts with plasma cell myeloma (PCM) [2]. Lenalidomide has undergone clinical trials as a treatment of pts with newly diagnosed PCM, chronic lymphocytic leukemia (CLL) and relapsed/refractory non-Hodgkin lymphoma (NHL) [3–5].
Lenalidomide has been classified as an immunomodulatory drug because of its pleiotropic modulatory effects on the immune system. Lenalidomide enhances antigen-specific CD8+ T-cell effector functions [6] and costimulates both CD4+ and CD8+ T cells which results in the increased production of IL-2 and IFN-γ [7–9]. This effect is mediated by degradation of Ikaros and Aiolos which are repressors of IL-2 promoter [10, 11]. Lenalidomide enhances binding of transcription factors Ikaros (IKZF1, IKAROS family zinc finger 1) and Aiolos (IKZF3) to CRBN and leads to their proteasomal degradation in both malignant B cells and normal T cells [10–12]. Lenalidomide modulates interactions of immune cells and malignant cells, i.e., repairs T-cell immunologic synapse dysfunction induced by CLL cells [13] and follicular lymphoma (FL) cells [14] by restoring appropriate F-actin formation and T-cell signaling [13, 15]. Normal LFA-1-mediated adhesion and migration in T cells from CLL pts is also restored by lenalidomide [16].
Lenalidomide was reported to inhibit Treg expansion, FOXP3 expression, and the suppressive function of Tregs toward autologous CD4+CD25− T cells in vitro [17]. Lenalidomide reduced suppressive effect of Tregs isolated from PCM pts on the proliferation and cytokine production of autologous CD8+ T cells [18]. Reports on Treg frequency in pts treated with lenalidomide are ambiguous. In CLL pts, one study showed that lenalidomide treatment reduced proportion of Tregs in peripheral blood [19], and another one that the percentage of peripheral blood Tregs increased after 3 cycles of treatment, but decreased after 15 cycles [20]. Treg frequency increased in peripheral blood of PCM pts after maintenance or salvage treatment with lenalidomide following allo-HCT [21–23], and also after lenalidomide treatment not preceded by allo-HCT [24, 25].
Reports on the role of Tregs in hematological neoplasms are conflicting. High numbers of intratumoral or peripheral Tregs have been shown to correlate with improved survival in germinal center B-cell-like DLBCL [26, 27], FL [27–29], and classical Hodgkin lymphoma (HL) [27, 30, 31]. Other studies showed association of follicular localization of Tregs with poor survival and high risk of transformation in FL [32]. The low number of circulating Tregs was associated with poor prognosis in pts with DLBCL [33], but in CLL pts and PCM pts unfavorable prognosis was associated with high number of Tregs [34, 35]. It was shown that in vitro CD4+FOXP3+ and CD4+FOXP3− T cells kill autologous leukemic B cells [36].
We have shown recently that polyclonal Tregs expanded in the presence of rapamycin and a low dose of IL-2 in vitro from CD4+CD25+ T cells as well as from CD4+CD25+CD127lo T cells suppressed proliferation of lymphoma B cells [37]. Here we investigated whether lenalidomide affects interaction of steady-state Tregs or Tregs activated and expanded in vitro with lymphoma B cells.
Materials and methods
Human cell samples
Established cell lines: mantle cell lymphoma (MCL)—MINO, JEKO-1, REC-1; follicular lymphoma (FL)—DOHH-2, diffuse large B-cell lymphoma (DLBCL)—U-2940; Hodgkin lymphoma (HL)—KM-H2, L-1236, L-428; and Burkitt lymphoma (BL)—Ramos were purchased from DSMZ (Germany).
Buffy coats processed from the peripheral blood of healthy donors were obtained from the Regional Blood Centre (Warszawa, Poland).
Patient characteristics
The study was approved by the institutional Bioethical Committee. Between April 2013 and October 2014, 18 pts were included. All pts signed informed consent for obtaining samples by fine needle aspiration biopsy of lymph nodes or extranodal tumors and/or donation of up to 4 mL peripheral blood from samples drawn for routine tests.
Patients of age 33–72 years, including 7 females and 11 males, were diagnosed with follicular lymphoma (FL) (n = 3), chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) (n = 6/3), diffuse large B-cell lymphoma, not otherwise specified (DLBCL NOS) (n = 3), mantle cell lymphoma (MCL) (n = 3). Six pts had recurrent disease (CLL/SLL–4, FL–1, DLBCL–1), 16 pts required treatment, and 2 were eligible for observation only.
Treg and Tcon isolation
Peripheral blood mononuclear cells (PBMC) were isolated by centrifugation on Ficoll-Paque Plus (Amersham Biosciences) density gradient and incubated for 35 min in plastic flasks to separate adherent and non-adherent cells. CD4+CD25+Tregs were isolated by magnetic separation with the use of Dynabeads® Regulatory CD4+CD25+ T-cell Kit (Invitrogen, Life Technologies). CD4+CD25− conventional T cells (Tcons) were obtained during Treg isolation procedure.
Cell population enriched in Tregs contained 94.5 ± 2.46 % CD4+ cells, 4.45 ± 2.77 % CD4−CD8− cells, and 0.91 ± 0.39 % CD4−CD8+ cells. CD127hi and CD127lo subpopulations of CD4+CD25+T cells were sorted on FACSAriaIII (BD Biosciences) cell sorter. The median purity of CD127hi subpopulation was 96.80 % (range 89.60–98.60), and that of CD127lo subpopulation was 99.20 % (range 91.80–99.80).
Lymphoma, MoDC, and T-cell expansion cultures
Normal lymphocytes, monocyte-derived dendritic cells (MoDCs), and lymphoma cells were cultured in serum-free AIM-V medium (Life Technologies). Culture medium used for MCL and HL cell lines was supplemented with 2.5 % of fetal calf serum (Gibco). To generate MoDCs, adherent monocytes were cultured for 7 days with GM-CSF (Leukine, Berlex, 100 ng/mL) and rhIL-4 (CellGenix, 250 IU/mL). Treg expansion was initiated in 96-well flat bottom plates at 1 × 105–1 × 106 cells per well with anti-CD3, anti-CD28, anti-CD2 moAb-coated beads (T-cell Activation/Expansion Kit, Miltenyi Biotech) at a bead-to-cell ratio 1:2 in the presence of rhIL-2 (R&D Systems, 50 IU/mL) or at 1 × 106 cells per well with allogeneic MoDCs irradiated 30 Gy from 137Cs source added to Tregs at a proportion 1:10, in the presence of rhIL-2 (10 IU/mL). Rapamycin (Sigma-Aldrich, 100 ng/mL) was added to the cultures on day 4. The cultures were continued in 24-well plates at a cell density of 5 × 105–2 × 106/mL, and restimulated polyclonally with moAb-coated beads or with MoDCs in 2-week intervals. Cells were split depending on cell growth, and fresh medium with IL-2 and rapamycin, was added in 2–3 day intervals.
Reagents
Lenalidomide (CC-5013, IMiD3) provided by Celgene Corp (Summit, New Jersey, USA) was dissolved in DMSO (Sigma-Aldrich) at concentration of 10 mM and stored in aliquots at −20 °C. For all experiments, lenalidomide was used at a concentration of 1 μM, a dose within the range of the concentrations of this drug found either in serum or plasma or in the whole blood determined by pharmacokinetic analysis following oral administration of this drug to pts [38]. DMSO was used as a vehicle control in all experiments.
Antibodies and flow cytometry
FITC-, PE-, PerCP-, APC-, APC-Cy7-anti-CD3; FITC-, PE-, APC-anti-CD4; FITC-, PE-, PerCP-anti-CD8; PE-Cy7- anti-CD19; FITC-anti-CD20; PE-Cy7-anti-CD25; PE-anti-CD73; PE-anti-CD127; APC-anti-CD152; FITC-anti-granzyme B were purchased from BD Biosciences. APC-anti-CD4; PE-Cy7-anti-CD19; PE-anti-CD20; FITC-anti-CD39; FITC-anti-CD62L; PE-anti-GITR (CD357); PE-anti-granzyme A; AlexaFluor647-anti-FOXP3 (Clone 259D); AlexaFluor647-anti-IgG1; PacificBlue-anti-FOXP3 (Clone 206D) were purchased from Biolegend. PE-anti-TIGIT; AlexaFluor647-anti-GARP were purchased from eBioscience. Intracellular staining was performed using Foxp3 Staining Buffer Set (eBioscience). Cells were incubated for 5 h with BD GolgiStop (BD Biosciences) before staining for granzyme A and granzyme B.
Flow cytometry was performed using FACSCantoII or FACSAriaIII (both from BD Biosciences). Data were analyzed using the FACSDiva software (BD Biosciences) and the FlowJo software (TreeStar).
Treg functional analysis
Mixed leukocyte cultures (MLC) of Tregs with lymphoma cell lines or Tcons were carried in triplicates in 48-well plates or in 24-well transwell plates (BD Biosciences) in the absence of rapamycin, with rhIL-2 (10 IU/mL), and with lenalidomide (1 μM) or with vehicle (DMSO) at a corresponding concentration (0.1 %). Freshly isolated Tregs or Tregs collected 7 days after the last restimulation step were mixed with responders at ratios ranging from 1:1 to 1:4. Established lymphoma B-cell lines or non-adherent peripheral blood mononuclear cells (NAC) or Tcons used as responders were plated at 105 cells/well after labeling with carboxyfluorescein succinimidyl ester (CFSE) using Cell Trace™ CFSE Cell Proliferation Kit (Invitrogen, Life Technologies), according to manufacturer’s instructions. Prior to CFSE labeling, NAC or Tcons used as responders were stimulated with anti-CD3/CD28/CD2-moAbs-coated beads in the presence of IL-2 (10 IU/mL) for 3 h. Expanded Tregs were labeled using Cell Proliferation Dye eFluor670® (eBioscience) or Cell Tracker™ Orange CMTMR (Molecular Probes), according to manufacturer’s protocols. If freshly isolated Tregs were plated in MLC, Tregs were identified by staining with anti-CD3 moAb on day of cell harvest. To determine cell viability, harvested cells were stained with 7-amino-actinomycin D (7-AAD, BD Biosciences). The proliferation pattern of CFSE-labeled cells and eFluor670-labeled cells was evaluated by flow cytometry. To compare cell yield in the cultures, equivalent cell samples were collected at a constant time and flow rate. A total cell yield in cultures was calculated basing on a proportion of direct cell count in a hemocytometer under a microscope to cell count in flow cytometry samples. The expansion indices were calculated as the proportion of the mean final yield of viable cells to the initial cell number in the cultures.
Lymphoma cells from suspensions collected by fine needle aspiration or leukemic cells from peripheral blood obtained from pts were usually isolated by centrifugation on Ficoll-Paque. Freshly isolated lymphoma/leukemia cells were cocultured with expanded Tregs at a cell ratio 4:1 in 96-well plates in the presence of soluble MultimericCD40L™ (AdipoGen, 25 ng/mL), rhIL-2 (10 IU/mL), and rhIL-4 (250 IU/mL). Staining with moAbs to B-cell markers (CD19, CD20) depending on individual lymphoma phenotype was performed on day of MLC harvest to distinguish lymphoma cells from allogeneic Tregs and autologous T cells. If possible, lymphoma cells were stained with CFSE prior to MLC plating. Tregs were stained with eFluor670 prior to MLC and/or with anti-CD3 moAb on a day of cell harvest.
Statistics
Statistical significance between groups was evaluated with 2-tailed t test for unpaired samples or with Wilcoxon nonparametric test using SPSS 14.0 (SPSS Inc). Data were considered statistical significant at p < 0.05.
Results
The suppression of lymphoma B-cell proliferation by ex vivo expanded Tregs is augmented by lenalidomide despite the concurrently downmodulated proliferation of Tregs
We evaluated the effect of lenalidomide on the interaction of in vitro expanded Tregs with established lymphoma B-cell lines. CD4+CD25+Tregs obtained from peripheral blood of healthy donors were activated with anti-CD3/CD28/CD2 antibody-coated beads and expanded in vitro in the presence of IL-2 (50 U/mL) and rapamycin (100 ng/mL) for 3–5 weeks. The expanded Tregs were cocultured with lymphoma cells in mixed leukocyte cultures (MLC) in the presence of IL-2 (10 U/mL), but without rapamycin. All but one of the studied lymphoma B-cell lines were responsive to the regulation by expanded polyclonal Tregs. Lenalidomide at a concentration of 1 μM did not inhibit proliferation of BL line Ramos, but potentiated suppression of this line exerted by expanded polyclonal CD4+CD25+Tregs (Fig. 1a, b). Lenalidomide alone partially inhibited proliferation of MCL line MINO (Fig. 1c), DLBCL line U-2940 (Fig. 1d), HL line L-1236 (Fig. 1e), and FL line DOHH-2 (not shown), and augmented suppression of these lymphoma cell lines exerted by expanded Tregs. The cumulative effect of lenalidomide and Tregs was observed at different Treg/lymphoma cell ratios (Fig. 1e). L-428 (HL), JEKO-1 (MCL), and KM-H2 (HL) cell lines were weakly or not sensitive to inhibitory effect of lenalidomide, and lenalidomide did not augment suppression of these lines by expanded Tregs (a representative experiment in Fig. 1f). REC-1 (MCL) cell line was not susceptible to suppression exerted by Tregs, but was inhibited by lenalidomide (Fig. 1g). Lymphoma B-cell lines mostly stimulated pre-expanded polyclonal CD4+CD25+Tregs to proliferate in MLC. Lenalidomide partially inhibited CD4+CD25+Treg proliferation induced by lymphoma cells in 5-day MLC in the presence of IL-2 (10 U/mL) (Fig. 1h), but did not significantly affect viability of Tregs cultured alone with IL-2 (10 U/mL). In one-day cultures, lenalidomide did not evoke any excessive apoptosis in expanded Tregs cultured alone or cocultured with lymphoma cells in MLC (data not shown).
Lenalidomide contributes to suppression of lymphoma B cells by ex vivo expanded CD4+CD25+Tregs but downmodulates Treg proliferation in MLC. a Flow cytometry plots and histograms show CFSE dilution pattern in viable CFSE-labeled Ramos lymphoma cells (L) and eFluor670 dilution pattern in viable eFluor670-labeled Tregs (Treg) cultured alone or cocultured (L + Treg) for 5 days at L/Treg ratio 2:1, with vehicle (DMSO) only or with 1 μM lenalidomide (LENA). Except from the CFSE histogram of Ramos cells stained on day 0 prior to MLC plating (L d.0), a scale of cell count axis in the histograms was normalized, and a proportion of areas under curve in histograms depicts the proportion of cell yields in the respective cultures. Plots and histograms are representative of triplicate cultures of the experiment shown in Fig. 1b. b Mean fold expansion ± standard deviation (SD) of Ramos cells plated alone or in MLC with expanded Tregs in the representative experiment (n = 4). c Mean fold expansion indices of MINO cells plated alone or in MLC. Each symbol represents one out of 7 experiments. d Mean fold expansion ±SD of U-2940 cells plated alone or in MLC in the representative experiment (n = 4). e Mean fold expansion ±SD of L-1236 cells plated alone or in MLC at L-1236/Treg ratio 1:1, 2:1, and 4:1. f Mean fold expansion ±SD of KM-H2 cells plated alone or in MLC in the representative experiment (n = 4). g Mean fold expansion ±SD of REC-1 cells plated alone and in MLC in the representative experiment (n = 2). h Mean fold expansion indices of Tregs plated alone or in MLC with B lymphoma cell lines. Each symbol represents one out of 17 experiments performed with Tregs from 8 different donors. Tregs were expanded polyclonally for 3 or 5 weeks prior to MLC plating. Each cell line was tested only once with Tregs obtained from a particular donor. L/Treg ratio in 5-day MLC was 2:1, if not otherwise indicated. Statistical differences between groups were determined by independent 2-tailed t test, (b, d–g) or by nonparametric Wilcoxon test (c, h), *p < 0.05, ns no statistically significant difference
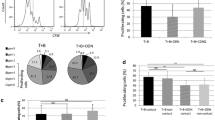
We have previously found that Tregs, expanded with rapamycin from CD4+CD25+ T cells and from sorted CD4+CD25+CD127hi T cells or from CD4+CD25+CD127lo T cells, mediate equally potent suppression of proliferation in established lymphoma B-cell lines [37]. Here we found that the suppression of lymphoma B cells exerted by Tregs expanded from magnetically separated CD4+CD25+ T cells and from their sorted CD127hi or CD127lo subsets increased in the presence of lenalidomide (Fig. 2a), although lenalidomide partially inhibited the proliferation of all these Treg populations in MLC (Fig. 2b). Lenalidomide did not inhibit the regulatory function of the expanded CD4+CD25+Tregs or CD4+CD25+CD127hiTregs or CD4+CD25+CD127loTregs exerted toward allogeneic conventional T cells or autologous conventional T cells (Fig. 3a–c).
Lenalidomide contributes to suppression of lymphoma B cells exerted by polyclonally expanded CD4+CD25+Tregs as well as by polyclonally expanded CD4+CD25+CD127hiTregs and CD4+CD25+CD127loTregs. a Viable cell yield ±SD of MINO cells plated alone or in MLC and b viable cell yield ±SD of Tregs plated in MLC. Black arrow indicates initial lymphoma (a) or Treg (b) cell number in well. Lymphoma cells and ex vivo expanded Tregs were cultured alone or cocultured at L/Treg ratio 2:1 in 5-day MLC, without or with 1 μM lenalidomide (LENA). Prior to MLC plating, Tregs were expanded polyclonally for 5 weeks from total CD4+CD25+ T cells (Treg), sorted CD4+CD25+CD127hi T cells (Treg CD127hi) and sorted CD4+CD25+CD127lo T cells (Treg CD127lo). The experiment is representative out of four experiments performed with different lymphoma lines. Statistical differences between groups were determined by independent 2-tailed t test, *p < 0.05
Lenalidomide does not inhibit regulatory function of polyclonally expanded Tregs toward allogeneic and autologous conventional T cells. a Proliferation profiles of CFSE-labeled and polyclonally activated CD4+CD8− Tcons plated alone (Tcon only) or cocultured with allo-Tregs (Tcon + Treg) at a ratio 1:1 and 4:1 in 4-day MLC, with vehicle (DMSO) only or with 1 μM lenalidomide (LENA). Histograms show representative profiles of triplicate cultures of the experiment shown in Fig. 3b. b Mean fold expansion ±SD of polyclonally activated CD4+CD8− Tcons plated alone or cocultured with allo-Tregs. The graph shows one representative out of 3 experiments. Tregs were expanded for 5 weeks prior to MLC. c Proliferation profiles of CFSE-labeled and polyclonally activated non-adherent peripheral blood mononuclear cells (NAC) plated alone or plated in 4-day MLC with expanded autologous total CD4+CD25+ Tregs (NAC + Treg), CD4+CD25+CD127hi Tregs (NAC + Treg CD127hi) or CD4+CD25+CD127lo Tregs (NAC + Treg CD127lo) at a ratio 2:1, with vehicle (DMSO) or with 1 μM lenalidomide (LENA). Tregs were expanded polyclonally for 5 weeks prior to MLC. Histograms show representative profiles of triplicate cultures in one experiment representative out of 4. Statistical differences between groups were determined by independent 2-tailed t test, *p < 0.05
It was reported that Tregs kill normal B cells and lymphoma B cells at Treg/B-cell ratio as high as 20:1 [36]. We have previously found that at a low Treg/lymphoma cell ratio, i.e., 1:2 or 1:4, apoptosis did not play an essential role in suppressive effect of Tregs toward lymphoma cell lines [37]. In this study, we did not observe a substantial effect of lenalidomide on the early and late apoptosis level of MINO and Ramos lymphoma cell lines cultured alone or in MLC with Tregs for 1 day (data not shown).
As an alternative method to initiate Treg expansion, Tregs were activated with allogeneic monocyte-derived dendritic cells (MoDCs) in the presence of IL-2 (10 U/mL) and rapamycin (100 ng/mL). The effect of Tregs pre-expanded with “third-party” allogeneic MoDCs on the proliferation of lymphoma B cells in MLC was evaluated in the absence of rapamycin. Lenalidomide potentiated suppression of lymphoma B-cell proliferation by Tregs pre-expanded with allogeneic MoDCs (Fig. 4).
Lenalidomide augments suppression of lymphoma B cells by Tregs expanded following activation with allogeneic MoDC. Mean fold expansion indices of lymphoma cells (L) plated alone or plated in 5-day MLC with Tregs at L/Treg ratio 2:1 or 4:1(#), with vehicle only or with 1 μM lenalidomide (LENA). Each symbol represents one out of five experiments. Prior to MLC plating, Tregs were expanded for 3 or 4 weeks in the presence of allogeneic MoDCs. U-2940 lymphoma cell line was tested with Tregs obtained from two different donors. Statistical differences between groups were determined by nonparametric Wilcoxon test, *p < 0.05
Tregs expanded polyclonally or with MoDCs suppressed lymphoma B-cell proliferation both in cell-to-cell contact and if Tregs and lymphoma cells were separated by a semipermeable membrane. Lenalidomide potentiated suppression exerted by Tregs in cell-to-cell contact and mediated by soluble factors (representative experiments in Fig. 5a, b). In our previous study, we have detected IFN-γ, IL-10, CD40L, and TNF-α in the supernatants collected from the cultures of Tregs alone and from MLC of Tregs with lymphoma B-cell lines MINO and U-2940 and PCM line U-266 [37]. In this study, we did not observe alteration of cytokine secretion pattern if lenalidomide was added to Tregs cultured alone or to MLC (data not shown).
Lenalidomide augments suppression of lymphoma B cells exerted by Tregs in cell-to-cell contact and by soluble factors. a, b Histograms show CFSE dilution pattern in viable CFSE-labeled lymphoma cells cultured alone (L), cultured in MLC with expanded Tregs (L + Treg), cultured alone under the insert (L[]) or separated from Tregs by a semipermeable membrane (L + [Treg]). Tregs were expanded polyclonally for 4 weeks (a) or in the presence of allogeneic MoDCs for 4 weeks (b), and subsequently cocultured with lymphoma cells at lymphoma cell/Treg ratio 1:1, either with vehicle (DMSO) only or with 1 μM lenalidomide (LENA). Except from the CFSE histogram of lymphoma cells stained on day 0 prior to MLC plating (day 0), a scale of cell count axis in the histograms was normalized, and a proportion of areas under curves in histograms depicts the proportion of cell yield in the respective 5-day cultures. The experiment shown in Fig. 5a is representative out of 3 experiments. The experiment shown in Fig. 5b is representative out of 3 experiments
We investigated whether lenalidomide affects the capacity of the polyclonally expanded Tregs to respond to the restimulation with anti-CD3/CD28/CD2 antibody-coated beads. On day 7, after the first or the second restimulation step, the expanded Tregs were once again activated with stimulatory beads and IL-2 (10 U/mL), with or without lenalidomide or continuously cultured with IL-2 without restimulation, with or without lenalidomide. Lenalidomide inhibited the proliferation of Tregs restimulated with freshly added stimulatory beads, but did not affect the proliferation of Tregs maintained in the presence of IL-2 (Fig. 6a, b).
Lenalidomide inhibits the expansion of Tregs if present during the activation step, but does not affect the proliferation and phenotype of Tregs activated in the absence of lenalidomide and thereafter exposed to lenalidomide. a Histograms display eFluor670 dilution pattern in Tregs cultured with IL-2 (10 U/mL) only (Treg) or Tregs restimulated with stimulatory beads in the presence of IL-2 (Treg + αCD3/2/28), with vehicle (DMSO) only or with 1 μM lenalidomide (LENA) for 5 days, beginning on day 7 after the previous restimulation step. The scale of cell count axis in the histograms was normalized, and the proportion of areas under the curve in the histograms depicts the proportion of cell yields in the respective cultures. The representative histograms of triplicate cultures are shown. b Mean fold expansion ±SD of triplicate Treg cultures in the experiment shown in Fig. 6a. Statistical difference between means was determined by independent 2-tailed t test *p < 0.05, ns–no statistically significant difference. Similar results were obtained in 6 experiments. c FOXP3 expression in CD4+CD25+ Tregs (Treg) polyclonally expanded for 3 weeks prior to incubation for 3 days with vehicle (DMSO) only or with lenalidomide (LENA). Histograms are representative out of 5 experiments. d Flow cytometry analysis of CD4+CD25+Tregs (Treg), CD4+CD25+CD127hiTregs (CD127hiTreg) and CD4+CD25+CD127loTregs (CD127loTreg) expanded for 5 weeks prior to incubation for 3 days with vehicle (DMSO) only or with lenalidomide (LENA). Shaded histograms depict control, solid lines depict indicated markers. CTLA-4 (CD152) expression was analyzed following intracellular labeling. Histograms are representative out of 4 experiments
The expression of markers associated with function is not modulated by lenalidomide in polyclonal Tregs pre-expanded in vitro
Tregs collected after 3- or 5-week polyclonal expansion in vitro were subsequently incubated in the presence of IL-2 (10 U/mL) with or without lenalidomide for 3 days. Lenalidomide did not alter FOXP3 expression in Tregs pre-expanded in vitro for 3–5 weeks (Fig. 6c, d). We found quantitative but not qualitative differences in the expression of several common markers of Treg phenotype and function in expanded CD4+CD25+Tregs and in CD127lo and CD127hi Treg subsets. The expression of markers such as GARP, TIGIT, CD62L, CD73, CD39, intracellular CTLA-4 (CD152), and granzyme A in CD4+CD25+Tregs and in CD127lo and CD127hi Treg subsets pre-expanded in vitro was not modified if these Treg populations were exposed to lenalidomide (Fig. 6d). The proportion of GITR(CD357)-expressing cells increased in all expanded Treg populations exposed to lenalidomide, but the observed differences did not reach statistical significance.
Lenalidomide augments suppression of B-lymphoma cell proliferation exerted by freshly isolated Tregs
Freshly isolated allogeneic CD4+CD25+Tregs mostly moderately suppressed proliferation of established lymphoma B-cell lines, and in some cases Tregs helped lymphoma cells to proliferate. A stimulation with anti-CD3/CD28/CD2 moAb-coated beads potentiated the suppressive effect of CD4+CD25+Tregs in MLC, and induced CD4+CD25+Tregs to suppress when lymphoma cells on their own did not do it. The suppression exerted by freshly isolated Tregs activated solely by lymphoma cells was augmented by lenalidomide. However, lenalidomide did not augment the suppressive effect of Tregs in MLC if Tregs were concomitantly activated with stimulatory anti-CD3/CD28/CD2 -moAbs-coated beads (Fig. 7a, b). Lymphoma cells supported survival and expansion of freshly isolated Tregs in MLC. Freshly isolated Tregs did not survive for 4–5 days if cultured alone in the presence of IL-2 (10 U/mL) at a cell density of 0.125 × 106/mL. Treg expansion induced in MLC by lymphoma cells was partially inhibited by lenalidomide (Fig. 7a, right graph). Despite the inhibitory effect of lenalidomide on Treg expansion, the suppression of lymphoma cells in MLC in the presence of lenalidomide was at least equally potent as in the absence of lenalidomide. However, it cannot be excluded that the inhibition of Treg proliferation by lenalidomide could somehow counterbalance Treg functional efficiency.
Lenalidomide augments suppression of lymphoma B cells by freshly isolated CD4+CD25+Tregs activated by lymphoma cells, but concurrently downmodulates Treg proliferation in MLC. a Left graph shows mean fold expansion indices of lymphoma cells plated alone or cocultured with freshly isolated Tregs at L/Treg ratio 1:1 or 4:1(#) for 5 days, without or with 1 μM lenalidomide (LENA), without or with stimulatory beads (+αCD3/2/28). Right graph shows mean fold expansion indices of Treg cells plated in MLC with lymphoma cell lines (L). Each symbol represents one out of 18 experiments performed with Tregs obtained from 12 different donors. Each lymphoma line was tested only once with Tregs obtained from a particular donor. Statistical differences between groups were determined by nonparametric Wilcoxon test *p < 0.05, ns no statistically significant difference. b Flow cytometry plots and histograms show CFSE dilution pattern in viable CFSE-labeled MINO cells (L) cultured alone or with freshly isolated Tregs (L + Treg) at 2:1 ratio in 4-day MLC, with vehicle (DMSO) or with 1 μM lenalidomide (LENA) and without or with anti-CD3/2/28-moAbs-coated beads (+αCD3/2/28). At the day of cell harvest, Tregs were identified by staining with anti-CD3 moAb. Except from the CFSE histogram of MINO cells stained on day 0 prior to MLC plating (L d.0), a scale of cell count axis in the histograms was normalized, and a proportion of areas under curve in histograms depicts the proportion of cell yields in the respective cultures
Diverse effects of lenalidomide and Tregs on the survival of freshly isolated lymphoma cells activated in vitro with CD40L and IL-4 are variably combined in individual patients
We found previously that the regulatory effect of Tregs expanded with rapamycin on survival of freshly isolated lymphoma cells activated with soluble multimeric CD40L and IL-4 was variable across lymphoma entities [37]. Lymphoma cells were activated with soluble multimeric CD40L and IL-4 to promote their survival in vitro [39, 40]. Here we examined the influence of lenalidomide on the regulatory effect of in vitro expanded allogeneic Tregs on lymphoma cells freshly isolated from pts (n = 18). Quantitative and qualitative immunophenotype of neoplastic cells analyzed according to the previously described procedure [41] is shown in Online Resource 1 (Table 1). Freshly isolated lymphoma cells were activated with soluble multimeric CD40L and IL-4 in 5–6 day MLC with Tregs at Treg/lymphoma ratio 1:4, with IL-2 (10 U/mL), without or with lenalidomide. The effects of Tregs and lenalidomide on the lymphoma cell survival were convergent or opposite, and consequently there was no uniform pattern of effects of combined lenalidomide and Tregs on freshly isolated lymphoma cells. In some cases, lenalidomide potentiated suppression of lymphoma B-cell survival by Tregs or enhanced helper effect of Tregs, but in others lenalidomide attenuated or did not affect regulation of lymphoma cells by Tregs (Fig. 8a, b). Lenalidomide did not modify Treg effect on the level of early and late apoptosis in lymphoma cells during one-day MLC at Treg/lymphoma cell ratio 1:4 (data not shown).
Combination of lenalidomide and Tregs variably affects the survival of freshly isolated lymphoma cells activated in vitro with CD40L and IL-4. a The graphs show mean ratio ±SD of viable lymphoma cell count in cultures without or with Tregs, without or with 1 μM lenalidomide (LENA) to the mean lymphoma cell count in the control with vehicle (DMSO) evaluated in individual pts. Lymphoma cells were cocultured at a ratio 4:1 with Tregs for 5–6 days, except for lymphoma cells obtained from Pt 10 cocultured for 3 days. Cultures were set at least in quadruplicates. Statistical difference between means was determined by independent 2-tailed t test *p < 0.05. b Lenalidomide and Tregs affected both survival and proliferation of lymphoma B cells. Flow cytometry plots show viable lymphoma cells (L) obtained from Pt 4, cultured alone or cocultured with expanded Tregs (L + Treg), with vehicle (DMSO) only or with lenalidomide (LENA). Lymphoma cells were identified by staining with anti-CD19 moAb and Tregs were labeled with eFluor670. Histograms show CFSE dilution pattern in lymphoma cells collected in a gate set both on lymphoma cells alone and on double-stained events (doublets)
Discussion
Here we demonstrated that lenalidomide exerts diverse immunomodulatory effects on lymphoma B cells and CD4+CD25+Tregs and in addition modulates their mutual interactions. Lenalidomide interfered with polyclonal activation of Tregs as well as with activation induced by lymphoma cells resulting in decreased Treg proliferation. However, lenalidomide did not affect viability and expansion of Tregs induced to proliferate in the absence of lenalidomide. These data imply that lenalidomide interferes with signals inducing Treg proliferation, but does not directly inhibit proliferation of Tregs that have been previously activated in the absence of lenalidomide. Galustian et al. [17] reported that the expansion of CD4+CD25highCTLA-4+FOXP3+ Tregs among PBMC cultured for 7 days with IL-2 (150 U/mL) was inhibited in the presence of lenalidomide. Their data also indicate that lenalidomide may inhibit the conversion of conventional T cells to FOXP3+ T cells as well as the proliferation of peripheral Tregs among PBMCs incubated for 7 days with IL-2 at concentration of 500 U/mL. Luptakova et al. [42] showed that following anti-CD3/CD28 stimulation in the presence of lenalidomide, the percentage of CD4+CD25+ FOXP3+ T cells decreased among T cells obtained from healthy donors or PCM pts. Galustian et al. [17] observed decreased FOXP3 expression in Tregs pretreated with lenalidomide. We found that Tregs expanded polyclonally with rapamycin and then exposed to lenalidomide expressed FOXP3 at the same level as Tregs not exposed to lenalidomide.
A mechanism of lenalidomide interference with Treg activation process requires further studies. Lenalidomide affects the expression level of transcription factors, such as Ikaros, Aiolos and IRF4, in malignant and non-malignant cells [10–12, 43, 44]. Human memory Helios−FOXP3+ Tregs express transcriptional regulator Aiolos [45]. The functional activation of Tregs induced by transforming growth factor β1 requires action of Aiolos. It was suggested that Aiolos interacts with Foxp3 to silence the transcriptional program of effector T cells and promote the differentiation of functional Tregs [46]. Then, the degradation of Aiolos induced by lenalidomide could interfere with activation of induced Tregs. Lenalidomide downregulates the expression of transcription factor IRF4 [43]. Since IRF4 is essential for the differentiation of effector Tregs [47], downmodulation of IRF4 may be considered as a possible mechanism of lenalidomide inhibitory effect on Treg activation. Luptakova et al. [42] observed a decreased proportion of CD4+CD25+ FOXP3+ T cells in T-cell population stimulated in vitro with dendritic cell/PCM fusions in the presence of lenalidomide that was accompanied by 50 % decrease in the amount of phosphorylated STAT5 in this T-cell population. Since STAT5 activation promotes Treg expansion [48, 49], it suggests that the inhibition of STAT5 phosphorylation is one of the mechanisms responsible for inhibition of Treg expansion by lenalidomide.
Galustian et al. [17] showed that the regulatory capacity of CD4+CD25+Tregs diminished after treatment with lenalidomide. These authors exposed Tregs to lenalidomide and subsequently evaluated their suppressive function toward autologous conventional T cells in the absence of lenalidomide. In our study, lenalidomide was added directly to MLC of freshly isolated or in vitro expanded CD4+CD25+Tregs with conventional T cells or with lymphoma cells, so it could affect each of mixed cell populations during their interaction. We did not observe an inhibition of Treg suppressive effects directed against established lymphoma B-cell lines and against conventional T cells by lenalidomide. Lenalidomide enhances suppression of lymphoma B-cell proliferation exerted by freshly isolated or ex vivo expanded CD4+CD25+Tregs.
CD127 expression is inversely correlated with FOXP3 expression in CD4+CD25+ T-cell compartment [50, 51]. The isolation of CD4+CD25+CD127lo T cells is as a way of obtaining purified Tregs with high FOXP3 expression and with demethylated FOXP3 intronic Treg-specific demethylation region (TSDR). We have previously found that Tregs expanded in the presence of rapamycin from total CD4+CD25+ T cells and from their sorted CD127lo and CD127hi subsets expressed the same molecules delivering coinhibitory signals, molecules involved in cytotoxicity, and ectonucleases mediating metabolic suppression, although there were some quantitative differences at the expression level of some of these molecules. Nevertheless, CD4+CD25+Tregs, CD4+CD25+CD127loTregs, and CD4+CD25+CD127hiTregs were equally potent suppressors [37]. Here we observed that lenalidomide similarly augmented suppression exerted by expanded CD4+CD25+ Tregs, CD4+CD25+CD127hi Tregs and CD4+CD25+CD127lo Tregs toward lymphoma B cells and conventional T cells.
We found previously that the effect of expanded CD4+CD25+Tregs on the survival of freshly isolated lymphoma cells activated in vitro with soluble multimeric CD40L and IL-4 was variable across lymphoma entities, and ranged from suppression to help in individual pts [37]. Polyclonal Tregs expanded with rapamycin displayed a wide spectrum of coinhibitory and cytotoxic molecules, but also secreted pleiotropic inflammatory cytokines that could suppress or stimulate B cells. Possibly, the contrasting outcomes of Treg interaction with lymphoma cells could result of the various sensitivities of lymphoma cells obtained from different pts to particular mechanisms of the regulation by Tregs. Here we demonstrated highly variable effects of lenalidomide alone or combined with CD4+CD25+Tregs on survival of freshly isolated lymphoma B cells activated with soluble multimeric CD40L and IL-4.
It was reported that lenalidomide downregulated the expression of coinhibitory surface molecules in tumor cells and in this manner prevented tumor-induced T-cell immunologic synapse impairment [15]. The profound molecular and functional synapse defects observed in T cells after CLL or FL tumor-cell coculture were global. Nevertheless, Ramsay et al. [15] reported that they could not demonstrate any involvement of regulatory T cells in the observed immune synapse defect. Here we demonstrated that lenalidomide variably affected Treg response to stimulatory signals delivered by lymphoma B cells to Tregs in MLC. Lenalidomide decreased the proliferative response of Tregs to stimulation by lymphoma cells, but concomitantly enhanced Treg suppressive activity induced by lymphoma cells in MLC. Since Tregs expanded with rapamycin do not express PD-1(CD279) [37], the downregulation of PD-L1 expression in lymphoma cells by lenalidomide does not seem to be a part of the mechanism of enhancement of Treg functional activity in MLC. The inhibitory signal delivered via PD-L1(CD274)-PD-1(CD279) axis induces profound suppression of effector cytokine signaling in conventional CD4+ T cells [52], and therefore lenalidomide can be used to block lymphoma-mediated suppression of conventional T cells [15]. We have not found any substantial lenalidomide effects on the expression of markers associated with Treg function or the secretion of cytokines by Tregs, as it was observed in conventional T cells [7]. The direct inhibitory effect of lenalidomide on lymphoma cell proliferation and suppressive effect of Tregs were usually additive. However, we also observed a modulation of lymphoma cell–Treg interaction by lenalidomide leading to the enhanced Treg-mediated suppression in the absence of detectable direct inhibitory effect of lenalidomide on lymphoma cell proliferation.
The inhibitory effect of lenalidomide is restricted to malignant cells expressing transcription factors Ikaros, Aiolos [10, 12] and IRF4 [43, 44]. Zhang et al. [43] observed that 4 of 16 established DLBCL lines were inhibited by lenalidomide, but the proliferation of two lines was enhanced in the presence of lenalidomide. We found that lenalidomide, used at a clinically relevant concentration, inhibited proliferation of 5 of 9 evaluated lymphoma B-cell lines, but did not eliminate these lines from the cultures. Since the lenalidomide effect on the proliferation of various B-cell lymphoma lines is different, it may differently combine with Treg-mediated regulation of lymphoma cells.
Our data suggest that in select pts with lymphoma sensitive to lenalidomide and responsive to regulation by Tregs, lenalidomide treatment could be applied to induce or enhance the suppressive activity of Tregs directed against malignant B cells in the tumor microenvironment, optionally if lenalidomide could be combined with other factors activating Tregs to the suppressive function. So far, administration of low dose of IL-2 has been shown to specifically activate and expand Treg populations in vivo [53]. Recently, a humanized anti-CD4 monoclonal antibody tregalizumab was reported to selectively activate Tregs [54]. A combination of lenalidomide treatment with adoptive transfer of CD4+CD25+Tregs or CD4+CD25+CD127loTregs expanded ex vivo could be used to suppress proliferation of residual lymphoma following autologous HCT.
Adoptive transfer of donor Tregs freshly isolated or expanded ex vivo is explored as an option to surmount GVHD following allogeneic HCT [55, 56]. Possibly, benefits of adoptive Treg transfer accompanying allogeneic HCT could increase if Tregs were pre-activated ex vivo to suppress lymphoma cells. However, it does not seem reasonable to combine adoptive Treg transfer accompanying allogeneic HCT with lenalidomide therapy. The HOVON 76 clinical trial revealed that lenalidomide maintenance therapy after non-myeloablative allo-HCT was not feasible in PCM pts, mainly because of the induced rapid development of GVHD [22].
In conclusion, we showed that lenalidomide treatment could be used to enhance suppression of lymphoma B-cell proliferation by Tregs in the lymphoma microenvironment. Hypothetically, lenalidomide may be combined with adoptive transfer of Treg expanded ex vivo and/or with treatment aimed to activate anti-lymphoma suppressive activity of Tregs in pts with hematological malignancies following auto-HCT. A prerequisite for such therapies is the sensitivity of lymphoma to lenalidomide and to the regulation by Tregs. It is worth considering the adoptive transfer of Tregs committed to regulate both effector T cells and lymphoma cells in pts after allogeneic HCT, but not in a combination with lenalidomide treatment which is associated with increased risk of GVHD.
References
Lentzsch S, LeBlanc R, Podar K, et al. Immunomodulatory analogs of thalidomide inhibit growth of Hs Sultan cells and angiogenesis in vivo. Leukemia. 2003;17(1):41–4.
Desai M, Newberry K, Ou Z, Wang M, Zhang L. Lenalidomide in relapsed or refractory mantle cell lymphoma: overview and perspective. Ther Adv Hematol. 2014;5(3):91–101.
Chanan-Khan AA, Cheson BD. Lenalidomide for the treatment of B-cell malignancies. J Clin Oncol. 2008;26(9):1544–52.
Carballido E, Veliz M, Komrokji R, Pinilla-Ibarz J. Immunomodulatory drugs and active immunotherapy for chronic lymphocytic leukemia. Cancer Control. 2012;19(1):54–67.
Saloura V, Grivas PD. Lenalidomide: a synthetic compound with an evolving role in cancer management. Hematology. 2010;15(5):318–31.
Haslett PA, Hanekom WA, Muller G, Kaplan G. Thalidomide and a thalidomide analogue drug costimulate virus-specific CD8+T cells in vitro. J Infect Dis. 2003;187(6):946–55.
Gorgun G, Calabrese E, Soydan E, et al. Immunomodulatory effects of lenalidomide and pomalidomide on interaction of tumor and bone marrow accessory cells in multiple myeloma. Blood. 2010;116(17):3227–37.
Marriott JB, Clarke IA, Dredge K, Muller G, Stirling D, Dalgleish AG. Thalidomide and its analogues have distinct and opposing effects on TNF-alpha and TNFR2 during co-stimulation of both CD4(+) and CD8(+) T cells. Clin Exp Immunol. 2002;130(1):75–84.
Schafer PH, Gandhi AK, Loveland MA, et al. Enhancement of cytokine production and AP-1 transcriptional activity in T cells by thalidomide-related immunomodulatory drugs. J Pharmacol Exp Ther. 2003;305(3):1222–32.
Kronke J, Udeshi ND, Narla A, et al. Lenalidomide causes selective degradation of IKZF1 and IKZF3 in multiple myeloma cells. Science. 2014;343(6168):301–5.
Gandhi AK, Kang J, Havens CG, et al. Immunomodulatory agents lenalidomide and pomalidomide co-stimulate T cells by inducing degradation of T cell repressors Ikaros and Aiolos via modulation of the E3 ubiquitin ligase complex CRL4(CRBN.). Br J Haematol. 2014;164(6):811–21.
Lu G, Middleton RE, Sun H, et al. The myeloma drug lenalidomide promotes the cereblon-dependent destruction of Ikaros proteins. Science. 2014;343(6168):305–9.
Ramsay AG, Johnson AJ, Lee AM, et al. Chronic lymphocytic leukemia T cells show impaired immunological synapse formation that can be reversed with an immunomodulating drug. J Clin Invest. 2008;118(7):2427–37.
Ramsay AG, Clear AJ, Kelly G, et al. Follicular lymphoma cells induce T-cell immunologic synapse dysfunction that can be repaired with lenalidomide: implications for the tumor microenvironment and immunotherapy. Blood. 2009;114(21):4713–20.
Ramsay AG, Clear AJ, Fatah R, Gribben JG. Multiple inhibitory ligands induce impaired T-cell immunologic synapse function in chronic lymphocytic leukemia that can be blocked with lenalidomide: establishing a reversible immune evasion mechanism in human cancer. Blood. 2012;120(7):1412–21.
Ramsay AG, Evans R, Kiaii S, Svensson L, Hogg N, Gribben JG. Chronic lymphocytic leukemia cells induce defective LFA-1-directed T-cell motility by altering Rho GTPase signaling that is reversible with lenalidomide. Blood. 2013;121(14):2704–14.
Galustian C, Meyer B, Labarthe MC, et al. The anti-cancer agents lenalidomide and pomalidomide inhibit the proliferation and function of T regulatory cells. Cancer Immunol Immunother. 2009;58(7):1033–45.
De Keersmaecker B, Fostier K, Corthals J, et al. Immunomodulatory drugs improve the immune environment for dendritic cell-based immunotherapy in multiple myeloma patients after autologous stem cell transplantation. Cancer Immunol Immunother. 2014;63(10):1023–36.
Idler I, Giannopoulos K, Zenz T, et al. Lenalidomide treatment of chronic lymphocytic leukaemia patients reduces regulatory T cells and induces Th17 T helper cells. Br J Haematol. 2010;148(6):948–50.
Lee BN, Gao H, Cohen EN, et al. Treatment with lenalidomide modulates T-cell immunophenotype and cytokine production in patients with chronic lymphocytic leukemia. Cancer. 2011;117(17):3999–4008.
Minnema MC, van der Veer MS, Aarts T, Emmelot M, Mutis T, Lokhorst HM. Lenalidomide alone or in combination with dexamethasone is highly effective in patients with relapsed multiple myeloma following allogeneic stem cell transplantation and increases the frequency of CD4+Foxp3+T cells. Leukemia. 2009;23(3):605–7.
Kneppers E, van der Holt B, Kersten MJ, et al. Lenalidomide maintenance after nonmyeloablative allogeneic stem cell transplantation in multiple myeloma is not feasible: results of the HOVON 76 Trial. Blood. 2011;118(9):2413–9.
Lioznov M, El-Cheikh J Jr, Hoffmann F, et al. Lenalidomide as salvage therapy after allo-SCT for multiple myeloma is effective and leads to an increase of activated NK (NKp44(+)) and T (HLA-DR(+)) cells. Bone Marrow Transplant. 2010;45(2):349–53.
Busch A, Zeh D, Janzen V, et al. Treatment with lenalidomide induces immunoactivating and counter-regulatory immunosuppressive changes in myeloma patients. Clin Exp Immunol. 2014;177(2):439–53.
Muthu-Raja KR, Kovarova L, Hajek R. Induction by lenalidomide and dexamethasone combination increases regulatory cells of patients with previously untreated multiple myeloma. Leuk Lymphoma. 2012;53(7):1406–8.
Lee NR, Song EK, Jang KY, et al. Prognostic impact of tumor infiltrating FOXP3 positive regulatory T cells in diffuse large B-cell lymphoma at diagnosis. Leuk Lymphoma. 2008;49(2):247–56.
Tzankov A, Meier C, Hirschmann P, Went P, Pileri SA, Dirnhofer S. Correlation of high numbers of intratumoral FOXP3+ regulatory T cells with improved survival in germinal center-like diffuse large B-cell lymphoma, follicular lymphoma and classical Hodgkin’s lymphoma. Haematologica. 2008;93(2):193–200.
Wahlin BE, Aggarwal M, Montes-Moreno S, et al. A unifying microenvironment model in follicular lymphoma: outcome is predicted by programmed death-1–positive, regulatory, cytotoxic, and helper T cells and macrophages. Clin Cancer Res. 2010;16(2):637–50.
Carreras J, Lopez-Guillermo A, Fox BC, et al. High numbers of tumor-infiltrating FOXP3-positive regulatory T cells are associated with improved overall survival in follicular lymphoma. Blood. 2006;108(9):2957–64.
Alvaro T, Lejeune M, Salvado MT, et al. Outcome in Hodgkin’s lymphoma can be predicted from the presence of accompanying cytotoxic and regulatory T cells. Clin Cancer Res. 2005;11(4):1467–73.
Kelley TW, Pohlman B, Elson P, Hsi ED. The ratio of FOXP3+ regulatory T cells to granzyme B+ cytotoxic T/NK cells predicts prognosis in classical Hodgkin lymphoma and is independent of bcl-2 and MAL expression. Am J Clin Pathol. 2007;128(6):958–65.
Farinha P, Al-Tourah A, Gill K, Klasa R, Connors JM, Gascoyne RD. The architectural pattern of FOXP3-positive T cells in follicular lymphoma is an independent predictor of survival and histologic transformation. Blood. 2010;115(2):289–95.
Glowala-Kosinska M, Chwieduk A, Nieckula J, et al. Association of circulating regulatory T cell number with the incidence and prognosis of diffuse large B-cell lymphoma. Eur J Haematol. 2013;91(2):122–8.
Giannopoulos K, Schmitt M, Kowal M, et al. Characterization of regulatory T cells in patients with B-cell chronic lymphocytic leukemia. Oncol Rep. 2008;20(3):677–82.
Giannopoulos K, Kaminska W, Hus I, Dmoszynska A. The frequency of T regulatory cells modulates the survival of multiple myeloma patients: detailed characterisation of immune status in multiple myeloma. Br J Cancer. 2012;106(3):546–52.
Lindqvist CA, Christiansson LH, Thorn I, et al. Both CD4+ FoxP3+ and CD4+ FoxP3- T cells from patients with B-cell malignancy express cytolytic markers and kill autologous leukaemic B cells in vitro. Immunology. 2011;133(3):296–306.
Grygorowicz MA, Biernacka M, Bujko M, et al. Human regulatory T cells suppress proliferation of B lymphoma cells. Leuk Lymphoma. 2016;. doi:10.3109/10428194.2015.1121260.
Blum W, Klisovic RB, Becker H, et al. Dose escalation of lenalidomide in relapsed or refractory acute leukemias. J Clin Oncol. 2010;28(33):4919–25.
Andersen NS, Larsen JK, Christiansen J, et al. Soluble CD40 ligand induces selective proliferation of lymphoma cells in primary mantle cell lymphoma cell cultures. Blood. 2000;96(6):2219–25.
Neelapu SS, Baskar S, Gause BL, et al. Human autologous tumor-specific T-cell responses induced by liposomal delivery of a lymphoma antigen. Clin Cancer Res. 2004;10(24):8309–17.
Woroniecka R, Rymkiewicz G, Grygalewicz B, et al. Cytogenetic and flow cytometry evaluation of Richter syndrome reveals MYC, CDKN2A, IGH alterations with loss of CD52, CD62L and increase of CD71 antigen expression as the most frequent recurrent abnormalities. Am J Clin Pathol. 2015;143(1):25–35.
Luptakova K, Rosenblatt J, Glotzbecker B, et al. Lenalidomide enhances anti-myeloma cellular immunity. Cancer Immunol Immunother. 2013;62(1):39–49.
Zhang LH, Kosek J, Wang M, Heise C, Schafer PH, Chopra R. Lenalidomide efficacy in activated B-cell-like subtype diffuse large B-cell lymphoma is dependent upon IRF4 and cereblon expression. Br J Haematol. 2013;160(4):487–502.
Lopez-Girona A, Heintel D, Zhang LH, et al. Lenalidomide downregulates the cell survival factor, interferon regulatory factor-4, providing a potential mechanistic link for predicting response. Br J Haematol. 2011;154(3):325–36.
Raffin C, Pignon P, Celse C, Debien E, Valmori D, Ayyoub M. Human memory Helios- FOXP3+ regulatory T cells (Tregs) encompass induced Tregs that express Aiolos and respond to IL-1beta by downregulating their suppressor functions. J Immunol. 2013;191(9):4619–27.
Gandhi R, Kumar D, Burns EJ, et al. Activation of the aryl hydrocarbon receptor induces human type 1 regulatory T cell-like and Foxp3(+) regulatory T cells. Nat Immunol. 2010;11(9):846–53.
Cretney E, Xin A, Shi W, et al. The transcription factors Blimp-1 and IRF4 jointly control the differentiation and function of effector regulatory T cells. Nat Immunol. 2011;12(4):304–11.
Yao Z, Kanno Y, Kerenyi M, et al. Nonredundant roles for Stat5a/b in directly regulating Foxp3. Blood. 2007;109(10):4368–75.
Cohen AC, Nadeau KC, Tu W, et al. Cutting edge: decreased accumulation and regulatory function of CD4+ CD25(high) T cells in human STAT5b deficiency. J Immunol. 2006;177(5):2770–4.
Liu W, Putnam AL, Xu-Yu Z, et al. CD127 expression inversely correlates with FoxP3 and suppressive function of human CD4+ T reg cells. J Exp Med. 2006;203(7):1701–11.
Seddiki N, Santner-Nanan B, Martinson J, et al. Expression of interleukin (IL)-2 and IL-7 receptors discriminates between human regulatory and activated T cells. J Exp Med. 2006;203(7):1693–700.
Myklebust JH, Irish JM, Brody J, et al. High PD-1 expression and suppressed cytokine signaling distinguish T cells infiltrating follicular lymphoma tumors from peripheral T cells. Blood. 2013;121(8):1367–76.
Klatzmann D, Abbas AK. The promise of low-dose interleukin-2 therapy for autoimmune and inflammatory diseases. Nat Rev Immunol. 2015;15(5):283–94.
Helling B, Konig M, Dalken B, et al. A specific CD4 epitope bound by tregalizumab mediates activation of regulatory T cells by a unique signaling pathway. Immunol Cell Biol. 2015;93(4):396–405.
Di Ianni M, Falzetti F, Carotti A, et al. Tregs prevent GVHD and promote immune reconstitution in HLA-haploidentical transplantation. Blood. 2011;117(14):3921–8.
Trzonkowski P, Bieniaszewska M, Juscinska J, et al. First-in-man clinical results of the treatment of patients with graft versus host disease with human ex vivo expanded CD4+ CD25+ CD127- T regulatory cells. Clin Immunol. 2009;133(1):22–6.
Acknowledgments
Contribution: M.A.G. designed and performed experiments, analyzed data, made the figures, and cowrote the manuscript; I.S.B. and E.N. performed experiments, analyzed data, and made the figures; G.R. and E.P.-K. provided patient samples, analyzed data, and cowrote the manuscript; K.B. analyzed patient samples; M. Biernacka designed and performed experiments; M. Bujko performed experiments, analyzed data, and cowrote the manuscript, J.W. designed and supervised the study, and cowrote the manuscript; S.M designed and supervised the study, analyzed data, and cowrote the manuscript. This work was supported by a grant from National Science Centre, Poland (N N402 454739), for S.M.
Funding
This work was supported by a grant from National Science Centre, Poland (N N402 454739), for S.M.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
JW.: Roche, Takeda, Mundipharma, Celgene, Teva, Gilead, Sanofi—lecture honoraria, Roche, Takeda, Janssen-Cilag, Teva, Boehringer Ingelheim, Celgene, Mundipharma, Karyopharm, Ariad—consulting/advisory role, Roche, Mundipharma, Celgene, GSK/Novartis—research funding, Roche, Celgene, Takeda, Seattle Genetics, Sanofi—travel/accommodation expenses; E.P.-K: Roche—lecture honoraria, advisory role, travel/accommodation expenses, Sandoz—lecture honoraria; M.A.G., M.Biernacka, M.Bujko, E.N., G.R., I.S.B., Z.B. and S.M. declared no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional review board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Grygorowicz, M.A., Borycka, I.S., Nowak, E. et al. Lenalidomide potentiates CD4+CD25+Treg-related suppression of lymphoma B-cell proliferation. Clin Exp Med 17, 193–207 (2017). https://doi.org/10.1007/s10238-016-0411-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10238-016-0411-8