Abstract
The aim of this study is to assess the influence of various Er:YAG laser energies on dentin surface micromorphology and dentine-resin shear bond strength (SBS). Eighty dentin specimens were prepared and divided randomly into ten groups: control group (CG), phosphoric acid-etched group (AG), four laser-conditioned groups treated with various pulse energies of 40, 60, 80, and 100 mJ (L40, L60, L80, L100), and four laser-conditioned acid-etched groups (LA40, LA60, LA80, LA100). Two specimens from each group underwent scanning electron microscopy examination, while the remaining six were subjected to the dentin-resin SBS test. Statistical analyses included Welch’s analysis of variance (ANOVA), followed by post hoc Tamhane's T2 multiple comparisons test, Pearson's correlation, and Fisher's exact test. Pulse energies of 60, 80, and 100 mJ fully exposed the dentin tubule orifices, although 100 mJ lead to microcracks. Laser-conditioned surfaces exhibited smaller tubule diameters compared to acid-etched surfaces, and tubule diameters positively correlated with dentin-resin SBS. Laser-conditioned groups showed lower SBS values, while laser-conditioned acid-etched groups demonstrated higher SBS values. No significant relationship was observed between dentin surface roughness and SBS. The range of laser energies used for dentin conditioning had limited effects on SBS or failure modes. Laser conditioning with energies ranging from 40 to 100 mJ effectively removes the smear layer from the dentin surface. However, to enhance dentin-resin bond strength, further acid etching of the laser-conditioned surface is necessary.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Since their initial implementation in dentistry, lasers have demonstrated unique advantages when used in conjunction with or as an alternative to conventional techniques [1]. The two most commonly used erbium lasers in dentistry are erbium: yttrium aluminum garnet (Er:YAG) and erbium, chromium: yttrium-scandium-gallium-garnet (Er,Cr:YSGG), which exhibit a slight yet significant difference in their respective laser wavelengths. The wavelengths of the Er:YAG (2.94 μm) and Er,Cr:YSGG (2.78 μm) lasers closely match the absorption peaks of water (3.0 μm) and hydroxyapatite (2.8 μm) in dental hard tissues. It has been established that the Er:YAG laser provides a superior and more efficient solution for dental hard tissue ablation [2]. In addition to wavelength absorption, the efficiency of laser ablation also depends on energy density, pulse duration (pulse width), pulse energy, irradiation time, and the number of pulses per second. Different settings of these variable parameters can ultimately determine the success or failure of dental bonding.
One of the key factors contributing to the success of dental restorations is dental bonding. Acid etching plays a critical role in the conventional dental bonding process. By demineralizing the surface dentin and exposing the collagen fibrils, acid etching removes the smear layer and increases the surface free energy [3]. Unlike acid etching, Er:YAG laser conditioning produces a tooth cavity surface devoid of debris and demineralization, resulting in a microscopically rough surface and open dentinal tubules [4,5,6,7,8,9]. However, the values of laser parameters used by different research organizations vary significantly, as indicated in previous literature. Currently, there is no standardized protocol that must be followed.
Challenges exist regarding resin adhesion to dentin and the use of lasers to modify the dentinal surface. Although this topic has been previously studied, further analysis is still needed due to variations in study setups and contradictory results [10, 11]. Some studies have demonstrated that laser-treated dentin provides a suitable bonding surface for composites [12, 13]. According to certain researchers, combining laser conditioning with acid etching can result in stronger bond strength compared to either procedure applied independently [7, 14]. However, other studies have reported that laser conditioning alone or in conjunction with acid etching did not enhance bonding [15,16,17].
The objectives of this study were to evaluate the effect of different Er:YAG laser pulse energy settings on the dentin surface, shear bond strength (SBS), and dentin micromorphology using scanning electron microscopy (SEM). The null hypothesis was that the SBS of dentin-resin would be positively correlated with the surface roughness of dentin, indicating that laser conditioning could increase the roughness of the dentin surface and enhance bond strength, while acid etching would have the opposite effect.
Materials and methods
Preparation of dentin specimens
A total of 80 third molars without caries, defects, cracks, or fillings were obtained from the Department of Stomatology at Shanxi Bethune Hospital. The periodontal tissue and calculus were removed, and the molars were stored in normal saline at 4 °C. The enamel was then removed from the molars using a high-speed turbine handpiece with a TF-11 bur (MTI Dental, Coatesville, PA, USA) and water cooling, revealing the occlusal dentin. The root was cut 2 mm below the enamel-cement junction. The occlusal dentin surface was polished for 30 s using 600-grit silicon carbide paper (QMAXIS LLC, Wynnewood, PA, USA), followed by a 30 s rinse with distilled water. This process resulted in the preparation of 80 dentin specimens with a cross-section measuring 4.0 mm × 4.0 mm and a length of 4 mm.
Dentin conditioning treatment
The 80 dentin specimens were randomly divided into ten groups, each containing eight specimens: the control group (CG), the phosphoric acid-etched group (AG), four laser-conditioned groups treated with different pulse energies (L40, L60, L80, and L100), and four laser-conditioned acid-etched groups treated with different pulse energies and then etched with phosphoric acid (LA40, LA60, LA80, LA100). The CG did not undergo any laser conditioning or acid etching. In the AG, 37% phosphoric acid gel (3 M ESPE, St. Paul, MN, USA) was applied to the dentin surface for 15 s, followed by a 30 s rinse and drying. The dentin surfaces in the laser-conditioned groups (L40, L60, L80, and L100) were subjected to laser irradiation with different pulse energies. In the laser-conditioned acid-etched groups (LA1, LA2, LA3, and LA4), the dentin surfaces were first treated with various pulse energies, followed by etching with 37% phosphoric acid for 15 s, rinsing for 30 s, and drying. The output energy of the laser in each group is presented in Table 1.
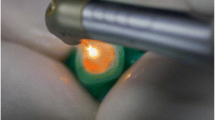
For this study, the Er:YAG laser (2.94 μm, Fidelis AT, Fotona, Ljubljana, Slovenia) was selected. The laser non-contact mode was used with the R14 handpiece, which had a 1.3-mm-diameter, 8-mm-length sapphire tip. In all laser groups, the laser duration was adjusted to micro short pulse (MSP) with a pulse duration of 100 μs, a pulse frequency of 20 Hz, and a water/air ratio of 7:3. The distance between the tip and the dentin surface was maintained at 1 mm, and the laser beam was applied perpendicularly to the entire surface, with manual movement at a speed of 1–2 mm/s.
SEM analysis
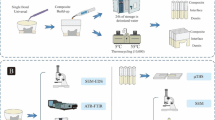
Two specimens were randomly selected from each group for SEM inspection. After completing the dentin conditioning treatment, the dentin surfaces were observed using a SEM (GEMINI SEM 300, Zeiss, Oberkochen, Germany). The samples were fixed in a refrigerator at 4 °C for 24 h with 2% glutaraldehyde and allowed to dehydrate naturally. Subsequently, conductive adhesive was used to attach the samples to a sample table, and the surfaces were coated with gold. Images of the dentin surface morphology for each group were captured after adjusting the magnifying lens and focus length.
The SEM pictures were used to measure the dentin tubule diameter using ImageJ software (1.53t, NIH, Bethesda, MD, USA). ImageJ software, using gray values (GV), was employed to evaluate the surface roughness characteristics. Although this method is not as effective as an atomic force microscope (AFM), it is increasingly accepted among researchers [18,19,20]. The SurfCharJ plugin in ImageJ was used to investigate surface characteristics and measure roughness parameters, including arithmetical mean roughness (Ra) and root mean square roughness (Rq) [21].
SBS test
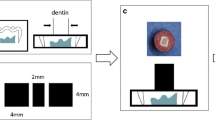
For the remaining six specimens in each group, dentin-resin bonding was performed using wet bonding technique. Adper Single Bond 2 (3 M ESPE, St. Paul, MN, USA) adhesive was applied with a small brush following the manufacturer's instructions. The adhesive was gently blown for 5 s and then light-cured for 10 s using a VALO light-curing lamp (Ultradent Products Inc., South Jordan, UT, USA). A layer of X-tra fill composite resin (VOCO GmbH, Cuxhaven, Germany) was applied and light-cured for 20 s. A total of 60 rectangular dentin-resin specimens with dimensions of 8 mm in length and 4.0 mm × 4.0 mm in cross-sectional area were prepared. Prior to the SBS tests, the specimens were incubated in an incubator at 37 °C for 24 h.
The rectangular specimens were securely clamped to an electronic universal testing machine (ETM-102A, Wance, Shenzhen, China) with a loading speed of 0.05 mm/min. The force was applied until the specimen fractured (Fig. 1). The load–displacement curve was continuously recorded by the computer during the failure process. The failure value was determined as the peak load when the sample reached its maximum load. SBS was calculated in megapascals (MPa) using the formula: SBS (MPa) = instantaneous shear force (N) / cross-sectional area (mm2).
Failure modes analysis
After the SBS test, all failure modes were examined and recorded to identify the type of failure. The failure modes included cohesive failure in dentin (DC), cohesive failure in resin (RC), adhesive failure (AF), and mixed failure (MF). DC (or RC) refers to failures that occur entirely within the dentin (or resin) without involving the adhesive interface. AF occurs when the adhesive interface does not contain any residual composite resin and neither the dentin nor the resin have failed. MF indicates simultaneous involvement of the dentin, resin, and adhesive interfaces in the failure.
Statistical analysis
The dentin tubule diameter, surface characteristics (Ra, Rq), and SBS of dentin-resin were analyzed using SPSS Statistics software (version 26.0, IBM Corp., Armonk, NY, USA) to calculate the mean and standard deviation. Welch's analysis of variance (ANOVA) was conducted, followed by post hoc Tamhane's T2 multiple comparisons test, to compare the differences in dentin tubule diameter, surface features, and SBS values among the specimens. Pearson's correlation was used to assess the relationship between SBS and dentin tubule diameter, Ra, and Rq. The Fisher exact test was employed to analyze the types of dentin-resin failure modes. A bilateral α = 0.05 was set as the significance level, with P < 0.05 indicating statistical significance.
Results
Morphological observation of the dentin interface
The dentin surface in the CG group was fully covered by a thick smear layer, obscuring tubule orifices and preventing the visualization of peritubular and intertubular dentin. In contrast, the AG group exhibited a normal, clean, and smooth dentin surface after the elimination of the smear layer by acid treatment. However, distinguishing between intertubular and peritubular dentin was challenging (Fig. 2).
In the laser-conditioned groups (L40-L100), the dentin surfaces appeared uneven, clean, and free of debris and smear layers (Fig. 3). In the L40 group, partial opening of tubules was observed due to incomplete ablation of dentin. The boundary between intertubular and peritubular dentin was not clearly discernible. In the L60, L80, and L100 groups, the dentin surfaces exhibited a fish-scale and lamellar appearance, with all tubule orifices open and visible. The dentin surface was highly distinct and the boundary between intertubular and peritubular dentin was easily identifiable in the L60 group. In the L80 group, the peritubular and intertubular dentin boundaries were ablated, but the dentin around the tubules remained intact. In the L100 group, excessive peritubular dentin ablation compromised the integrity of the peritubular dentin, resulting in a protrusion on the irregular surface. Additionally, a few microcracks were observed on the dentin surface (highlighted in a black rectangle), although there were no signs of coking or carbonization. The dentin surfaces in the laser-conditioned acid-etched groups (LA40-LA100) appeared similar, with clean and smooth surfaces. Notably, the influence of phosphoric acid etching eliminated peritubular dentin damage and dentin "microcracks" caused by laser energy at 100 mJ.
Dentin tubule diameters were measured using ImageJ software. The results showed that the tubule diameters in the acid-etched groups were significantly wider compared to the laser-conditioned surfaces without acid etching (Table 2, Fig. 4A).
Evaluation of FEM surface roughness
Normal distribution was observed in the data, but variance homogeneity was not confirmed in this study. Data analysis was conducted using Welch's ANOVA, followed by post hoc Tamhane's T2 multiple comparisons test. The surface roughness values (Ra, Rq) are presented in Table 2 and Fig. 4B–C. The control group was excluded from the surface roughness analysis due to the presence of a smear layer, which obscured the dentinal tubules and true surface structure. Dentin roughness was influenced by both acid etching and laser conditioning, but statistical significance was only observed when it reached a specific threshold. Figure 5 provides an illustration of how ImageJ software calculated surface roughness using the L60 and LA40 specimens.
SBS test
The SBS results for each group are displayed in Table 2 and Fig. 4D. Welch's ANOVA revealed statistically significant differences (P < 0.001) in dentin-resin SBS. Dentin treated with laser conditioning, acid etching, or both procedures exhibited increased SBS compared to the control group (P < 0.001). Insufficient laser output energy (40 mJ) resulted in incomplete exposure of dentinal tubule orifices, leading to decreased resin bonding strength (P < 0.001). The SBS of dentin surfaces treated with laser conditioning was lower than that of dentin surfaces treated solely with acid etching (P < 0.01). However, the SBS of acid-etched dentin that had firstly undergone laser conditioning was higher compared to dentin treated only with acid etching (P < 0.05). The SBS of dentin-resin after surface treatment showed a correlation with the diameter of exposed dentin tubules (R2 = 0.7853, P < 0.01) (Fig. 4E), but this correlation was not statistically significant (P > 0.05) with respect to dentin surface roughness (Ra, Rq).
Failure type
Following the SBS test, Fig. 4F illustrates the failure modes observed in each group. The most common type of failure in this study was mixed, and there was no significant difference between the groups (P = 0.7323), indicating that neither phosphoric acid etching nor laser conditioning had a significant effect on the type of dentin-resin failures.
Discussion
Numerous researchers have conducted laser conditioning and acid etching on dentin to analyze the dentin-resin bonding interface's SBS. They have concluded that laser conditioning creates an irregular dentin surface with exposed dentin tubules and no smear layers [3, 4, 7, 8, 14, 22,23,24,25,26]. This study referred to these previous experimental methods and further analyzed the obtained SEM images using ImageJ image processing software. In addition to removing the smear layer, the Er:YAG laser can effectively remove composite fillings or restorations from the dentin surface [27, 28].
Insufficient output energy settings make the Er:YAG laser less effective on peritubular dentin due to its lower water content. In addition to these established theories, our main interest is to determine how different treatment modalities influence the bonding strength of dentin-resin by affecting the diameter of dentin tubules and the roughness of the dentin surface. The diameter of dentin tubules is larger in the dentin layer close to the pulp chamber and becomes thinner towards the surface [29]. For sample preparation and measurement, preference was given to occlusal dentin. When dentin tubules were subjected only to laser conditioning, their diameters were noticeably smaller compared to when they underwent acid etching, where they were comparable to previously reported values [5, 6, 25, 30]. This phenomenon was caused by the dissolution of peritubular dentin and the increase in tubule orifices. The mean surface roughness values of the laser-conditioned acid-etched groups were lower than those of the laser-conditioned groups, yet their dentin-resin SBS mean values were higher.
The null hypothesis, which posited that lasers could enhance the bond strength between dentin and resin by increasing the roughness of the dentin surface, was rejected. Although Er:YAG laser application alters the dentin surface and consequently the bonding mechanism of adhesives to dentin, its contribution to bond strength is still weaker than that of acid etching. The findings of this study align more with acid etching, which increases the diameter of exposed dentin tubule orifices by dissolving peritubular dentin, thereby enhancing the dentin-resin bond strength. Our findings are consistent with those of Saikaew et al., who reported that SBS was unaffected by surface roughness resulting from various surface preparations [31]. Some researchers have also reported that a smooth dentin surface can improve the bond strength of dentin-resin [32, 33]. It appears that smooth dentin surfaces are achieved through acid etching, which widens the dentin tubule diameters. Vermelho et al. attributed lower bond strength values in adhesive-applied laser-treated dentin to the lack of a hybrid layer [16]. Therefore, in addition to the hybrid layer, the diameter of exposed dentin tubule orifices on the surface is another important factor influencing bond strength. Given the small sample size of the current study, future research may require a controlled study with larger samples.
A recent systematic review identified the main parameters for laser irradiation of dentin, including a pulse duration ranging from 100 to 400 μs, an output energy ranging from 50 to 600 mJ per pulse, and a frequency ranging from 2 to 30 Hz [11]. In this study, we chose a pulse duration of 100 μs, a minimum output energy of 40 mJ per pulse, and a frequency of 20 Hz to minimize thermal damage. In the MSP mode with a pulse duration of 100 μs, a pulse energy of 40 mJ could not fully expose the dentin tubule orifices. However, pulses of 60 and 80 mJ completely exposed the dentin tubule orifices without causing any microcracks. When the pulse energy reached 100 mJ or more, cracks formed on the laser-conditioned dentin surface. As a result, laser energy in the range of 40–100 mJ clearly affected the microstructure of the dentin surface but only slightly affected the final bond strength of the dentin resin. Moreover, the laser energy had little effect on the subsequent acid etching and the final bond strength.
The failure mode is a crucial indicator for assessing bond strength. In this study, the most common failure mode observed was mixed failure, and no statistically significant difference or correlation between failure modes and SBS was found. It is worth noting that the laser settings and bonding materials used in this investigation differ greatly from those in previous publications, resulting in varied failure modes [33,34,35,36,37]. It is important to consider that the type of failure, such as the presence of micro-cracks or cavities on or beneath the dentin bonding surface, may be influenced by specimen preparation. Therefore, when preparing specimens, it is crucial to avoid introducing these flawed structures, as they are more likely to fail under stress.
Conclusion
Laser conditioning of dentin surfaces results in smaller tubule diameters compared to acid etching, and the diameter of tubules has an impact on the bond strength between dentin and resin. While laser conditioning effectively removes the smear layer, further etching is necessary to enhance the bond strength. Furthermore, the laser energy used in this study, ranging from 40 to 100 mJ with a pulse duration of 100 μs and a pulse frequency of 20 Hz, using a fiber tip with a diameter of 1.3 mm, did not have a statistically significant effect on dentin-resin SBS.
Data availability
The data applied in this study are reasonably available from the corresponding authors.
References
Najeeb S, Khurshid Z, Zafar MS, Ajlal S (2016) Applications of light amplification by stimulated emission of radiation (lasers) for restorative dentistry. Med Princ Pract 25(3):201–211. https://doi.org/10.1159/000443144
Diaci J, Gašpirc B (2012) Comparison of Er:YAG and Er,Cr:YSGG lasers used in dentistry. J laser health Acad 1(1):1–13. Retrieved December 5, 2022, from https://www.laserandhealthacademy.com/en/journal/?id=1218
Susin AH, Alves LS, Melo GP, Lenzi TL (2008) Comparative scanning electron microscopic study of the effect of different dental conditioners on dentin micromorphology. J Appl Oral Sci 16(2):100–105. https://doi.org/10.1590/s1678-77572008000200004
Kohara EK, Hossain M, Kimura Y, Matsumoto K, Inoue M, Sasa R (2002) Morphological and microleakage studies of the cavities prepared by Er:YAG laser irradiation in primary teeth. J Clin Laser Med Surg 20(3):141–147. https://doi.org/10.1089/104454702760090227
Bertrand MF, Hessleyer D, Muller-Bolla M, Nammour S, Rocca JP (2004) Scanning electron microscopic evaluation of resin-dentin interface after Er:YAG laser preparation. Lasers Surg Med 35(1):51–57. https://doi.org/10.1002/lsm.20063
Ismatullaev A, Tasin S, Usumez A (2021) Evaluation of bond strength of resin cement to Er:YAG laser-etched enamel and dentin after cementation of ceramic discs. Lasers Med Sci 36(2):447–454. https://doi.org/10.1007/s10103-020-03103-1
Nahas P, Nammour S, Gerges E, Zeinoun T (2020) Comparison between shear bond strength of Er:YAG and Er,Cr:YSGG lasers-assisted dentinal adhesion of self-adhering resin composite: an ex vivo study. Dent J (Basel) 8(3). https://doi.org/10.3390/dj8030066
Wang JH, Yang K, Zhang BZ, Zhou ZF, Wang ZR, Ge X, Wang LL, Chen YJ, Wang XJ (2020) Effects of Er:YAG laser pre-treatment on dentin structure and bonding strength of primary teeth: an in vitro study. BMC Oral Health 20(1):316. https://doi.org/10.1186/s12903-020-01315-z
Kucukyilmaz E, Botsali MS, Korkut E, Sener Y, Sari T (2017) Effect of different modes of erbium:yttrium aluminum garnet laser on shear bond strength to dentin. Niger J Clin Pract 20(10):1277–1282. https://doi.org/10.4103/1119-3077.181402
Lopes RM, Trevelin LT, da Cunha SR, de Oliveira RF, de Andrade Salgado DM, de Freitas PM, de Paula EC, Aranha AC (2015) Dental adhesion to erbium-lased tooth structure: a review of the literature. Photomed Laser Surg 33(8):393–403. https://doi.org/10.1089/pho.2015.3892
Dua D, Dua A, Anagnostaki E, Poli R, Parker S (2022) Effect of different types of adhesive systems on the bond strength and marginal integrity of composite restorations in cavities prepared with the erbium laser-a systematic review. Lasers Med Sci 37(1):19–45. https://doi.org/10.1007/s10103-021-03294-1
Visuri SR, Gilbert JL, Wright DD, Wigdor HA, Walsh JT Jr (1996) Shear strength of composite bonded to Er:YAG laser-prepared dentin. J Dent Res 75(1):599–605. https://doi.org/10.1177/00220345960750011401
de Carvalho RC, de Freitas PM, Otsuki M, de Eduardo CP, Tagami J (2008) Micro-shear bond strength of Er:YAG-laser-treated dentin. Lasers Med Sci 23(2):117–124. https://doi.org/10.1007/s10103-006-0434-6
Verma M, Kumari P, Gupta R, Gill S, Gupta A (2015) Comparative evaluation of surface topography of tooth prepared using erbium, chromium: Yttrium, scandium, gallium, garnet laser and bur and its clinical implications. J Indian Prosthodont Soc 15(1):23–28. https://doi.org/10.4103/0972-4052.155042
Jaberi Ansari Z, Fekrazad R, Feizi S, Younessian F, Kalhori KA, Gutknecht N (2012) The effect of an Er, Cr:YSGG laser on the micro-shear bond strength of composite to the enamel and dentin of human permanent teeth. Lasers Med Sci 27(4):761–765. https://doi.org/10.1007/s10103-011-0961-7
Vermelho PM, Freitas PM, Reis AF, Giannini M (2022) Influence of Er:YAG laser irradiation settings on dentin-adhesive interfacial ultramorphology and dentin bond strength. Microsc Res Tech 85(8):2943–2952. https://doi.org/10.1002/jemt.24144
Sharafeddin F, Maroufi S (2022) Effect of Er:YAG, Co2 lasers, papain, and bromelain enzymes dentin treatment on shear bond strength of composite resin. Clin Exp Dent Res. https://doi.org/10.1002/cre2.651
Almohareb RA, Barakat R, Albohairy F (2022) New heat-treated vs electropolished nickel-titanium instruments used in root canal treatment: Influence of autoclave sterilization on surface roughness. PLoS One 17(3):e0265226. https://doi.org/10.1371/journal.pone.0265226
Balderrama IF, Stuani VT, Cardoso MV, Oliveira RC, Lopes MMR, Greghi SLA, Adriana Campos Passanezi S (2021) The influence of implant surface roughness on decontamination by antimicrobial photodynamic therapy and chemical agents: A preliminary study in vitro. Photodiagnosis Photodyn Ther 33:102105. https://doi.org/10.1016/j.pdpdt.2020.102105
Van Pham K, Vo CQ (2020) A new method for assessment of nickel-titanium endodontic instrument surface roughness using field emission scanning electronic microscope. BMC Oral Health 20(1):240. https://doi.org/10.1186/s12903-020-01233-0
Chinga G, Johnsen PO, Dougherty R, Berli EL, Walter J (2007) Quantification of the 3D microstructure of SC surfaces. J Microsc 227(Pt 3):254–265. https://doi.org/10.1111/j.1365-2818.2007.01809.x
Issar R, Mazumdar D, Ranjan S, Krishna NK, Kole R, Singh P, Lakiang D, Jayam C (2016) Comparative evaluation of the etching pattern of Er, Cr:YSGG & acid etching on extracted human teeth-an ESEM analysis. J Clin Diagn Res 10(5):ZC01-05. https://doi.org/10.7860/JCDR/2016/19739.7705
Flury S, Koch T, Peutzfeldt A, Lussi A (2012) Micromorphology and adhesive performance of Er:YAG laser-treated dentin of primary teeth. Lasers Med Sci 27(3):529–535. https://doi.org/10.1007/s10103-011-0882-5
Brulat N, Rocca JP, Leforestier E, Fiorucci G, Nammour S, Bertrand MF (2009) Shear bond strength of self-etching adhesive systems to Er:YAG-laser-prepared dentin. Lasers Med Sci 24(1):53–57. https://doi.org/10.1007/s10103-007-0519-x
Chou JC, Chen CC, Ding SJ (2009) Effect of Er, Cr:YSGG laser parameters on shear bond strength and microstructure of dentine. Photomed Laser Surg 27(3):481–486. https://doi.org/10.1089/pho.2008.2282
Esteves-Oliveira M, Zezell DM, Apel C, Turbino ML, Aranha AC, Eduardo Cde P, Gutknecht N (2007) Bond strength of self-etching primer to bur cut, Er, Cr:YSGG, and Er:YAG lased dental surfaces. Photomed Laser Surg 25(5):373–380. https://doi.org/10.1089/pho.2007.2044
Zakrzewski W, Dobrzynski M, Kuropka P, Matys J, Malecka M, Kiryk J, Rybak Z, Dominiak M, Grzech-Lesniak K, Wiglusz K, Wiglusz RJ (2020) Removal of composite restoration from the root surface in the cervical region using Er: YAG laser and drill-in vitro study. Materials (Basel) 13(13). https://doi.org/10.3390/ma13133027
Kiryk J, Matys J, Grzech-Leśniak K, Dominiak M, Małecka M, Kuropka P, Wiglusz RJ, Dobrzyński M (2021) SEM evaluation of tooth surface after a composite filling removal using Er:YAG Laser, drills with and without curettes, and optional EDTA or NaOCl conditioning. materials (Basel) 14(16). https://doi.org/10.3390/ma14164469
Lenzi TL, Guglielmi Cde A, Arana-Chavez VE, Raggio DP (2013) Tubule density and diameter in coronal dentin from primary and permanent human teeth. Microsc Microanal 19(6):1445–1449. https://doi.org/10.1017/S1431927613012725
de Los Angeles Moyaho-Bernal M, Contreras-Bulnes R, Rodriguez-Vilchis LE, Rubio-Rosas E (2018) Changes in deciduous and permanent dentinal tubules diameter after several conditioning protocols: In vitro study. Microsc Res Tech 81(8):865–871. https://doi.org/10.1002/jemt.23048
Saikaew P, Senawongse P, Chowdhury AA, Sano H, Harnirattisai C (2018) Effect of smear layer and surface roughness on resin-dentin bond strength of self-etching adhesives. Dent Mater J 37(6):973–980. https://doi.org/10.4012/dmj.2017-349
Aker Sagen M, Vos L, Dahl JE, Ronold HJ (2022) Shear bond strength of resin bonded zirconia and lithium disilicate - effect of surface treatment of ceramics and dentin. Biomater Investig Dent 9(1):10–19. https://doi.org/10.1080/26415275.2022.2038177
Son SA, Kim BN, Kim JH, Seo DG, Park JK (2022) Influence of dentin surface roughness, drying time, and primer application on self-adhesive composite-cement bond strength. J Adhes Dent 24(1):137–146. https://doi.org/10.3290/j.jad.b2916387
Al Habdan AH, Al Rabiah R, Al Busayes R (2021) Shear bond strength of acid and laser conditioned enamel and dentine to composite resin restorations: an in vitro study. Clin Exp Dent Res 7(3):331–337. https://doi.org/10.1002/cre2.409
Alkhudhairy F, Vohra F, Naseem M (2020) Influence of Er, Cr:YSGG laser dentin conditioning on the bond strength of bioactive and conventional bulk-fill dental restorative material. Photobiomodul Photomed Laser Surg 38(1):30–35. https://doi.org/10.1089/photob.2019.4661
Koliniotou-Koumpia E, Kouros P, Zafiriadis L, Koumpia E, Dionysopoulos P, Karagiannis V (2012) Bonding of adhesives to Er:YAG laser-treated dentin. Eur J Dent 6(1):16–23. Retrieved December 5, 2022, from https://www.ncbi.nlm.nih.gov/pubmed/22229003
Armstrong SR, Keller JC, Boyer DB (2001) Mode of failure in the dentin-adhesive resin-resin composite bonded joint as determined by strength-based (muTBS) and fracture-based (CNSB) mechanical testing. Dent Mater 17(3):201–210. https://doi.org/10.1016/s0109-5641(00)00070-1
Acknowledgements
We thank all our colleagues who helped us during the current study.
Funding
This study was supported by the National Natural Science Foundation of China (No:62175135), Fundamental Research Program of Shanxi Province (202203021221240), Program of State Key Laboratory of Quantum Optics and Quantum Optics Devices, Shanxi University (KF202105), and Fund for Shanxi Bethune Hospital "Beacon Project" Talent Training (2022FH18).
Author information
Authors and Affiliations
Contributions
Conceptualization: [Min Liu], [Qingmei Liu]; Methodology: [Min Liu], [Xin Xu]; Formal analysis and investigation: [Pengfei Xin]; Writing—original draft preparation: [Min Liu]; Writing—review and editing: [Pengfei Xin]; Funding acquisition: [Kuanshou Zhang], [Pengfei Xin]; Resources: [Min Liu], [Qingmei Liu]; Supervision: [Qingmei Liu], [Kuanshou Zhang].
Corresponding author
Ethics declarations
Ethics approval
Ethics approval was approved and supervised by the Science Ethical Review Committee of Shanxi University (SXULL2021043).
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, M., Xu, X., Liu, Q. et al. Effect of various Er:YAG laser conditioning energies on dentin surface: micromorphological investigation and dentin-resin shear bond strength test. Lasers Med Sci 38, 242 (2023). https://doi.org/10.1007/s10103-023-03915-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-023-03915-x