Abstract
The spread of multi-drug resistant (MDR) Klebsiella pneumoniae strains producing carbapenemases points to a pressing need for new antibacterial agents. To this end, the in-vitro antibacterial activity of a synthetic N-terminal peptide of human lactoferrin, further referred to as hLF1–11, was evaluated against K. pneumoniae strains harboring different carbapenemase genes (i.e. OXA-48, KPC-2, KPC-3, VIM-1), with different susceptibility to colistin and other antibiotics, alone or in combination with conventional antibiotics (gentamicin, tigecycline, rifampicin, clindamycin, and clarithromycin). An antimicrobial peptide susceptibility assay was used to assess the bactericidal activity of hLF1–11 against the different K. pneumoniae strains tested. The synergistic activity was evaluated by a checkerboard titration method, and the fractional inhibitory concentration (FIC) index was calculated for the various combinations. hLF1–11 was more efficient in killing a K. pneumoniae strain susceptible to most antimicrobials (including colistin) than a colistin-susceptible strain and a colistin-resistant MDR K. pneumoniae strain. In addition, hLF1–11 exhibited a synergistic effect with the tested antibiotics against MDR K. pneumoniae strains. The results of this study indicate that resistance to hLF1–11 and colistin are not strictly associated, and suggest an hLF1–11-induced sensitizing effect of K. pneumoniae to antibiotics, especially to hydrophobic antibiotics, which are normally not effective on Gram-negative bacteria. Altogether, these data indicate that hLF1–11 in combination with antibiotics is a promising candidate to treat infections caused by MDR-K. pneumoniae strains.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The worldwide spread of carbapenem-resistant Klebsiella pneumoniae strains represents a major concern for public health [1]. Carbapenem resistance is mostly due to the production of carbapenemases that hydrolyze all β-lactam antibiotics including carbapenems, which are considered one of the last resorts for treating infections caused by Enterobacteriaceae [2,3,4]. Carbapenemases have been classified into three different molecular classes: Amber class A (such as KPC type), class B (such as VIM type), and class D (such as OXA-48 type). All of these are widely distributed among Enterobacteriaceae, particularly in K. pneumoniae strains associated with systemic infections [5, 6]. Moreover, strains harboring KPC-type genes of class A are often resistant to several other classes of drugs, including fluoroquinolones and aminoglycosides [6, 7]. Therefore, the therapeutic options to treat infections caused by such MDR strains are very limited, and high rates of mortality are recorded [8,9,10]. Among the few drugs that are still effective, colistin, tigecycline, gentamicin, and fosfomycin are often used in combination therapy [11, 12], yet K. pneumoniae strains resistant to these drugs have been recently isolated [13, 14]. It should be noted that development of novel antimicrobial agents against Gram-negative bacteria is also very limited [8, 15].
In this context, cationic antimicrobial peptides (AMP) have gained attention as possible new therapeutic candidates. A generally accepted mechanism of action of antimicrobial peptides involves electrostatic binding between the positively charged peptides and negatively charged structural elements of bacteria, e.g., lipopolysaccharide [16, 17]. Lactoferrin (LF) is a 77 kDa iron-binding multifunctional glycoprotein. It is present in the milk of humans and other mammals, in the blood plasma and neutrophil-specific granules, and is one of the major components of virtually all exocrine secretions of mammals, such as saliva, bile, tears, and pancreatic juice. Its functions include the regulation of innate immunity, iron transfer to cells, control of the level of free iron in blood, interaction with nucleic acids, heparin, and polysaccharides, and pronounced antimicrobial and antiviral activities [18, 19]. Importantly, lactoferrin is a source of peptides with antimicrobial activity. Human LF generates, by acid-pepsinolysis, the antimicrobial peptide lactoferricin H (residues 1 to 47), which contains two cationic domains (residues 2 to 5 and 28 to 31). A synthetic peptide comprising the first cationic domain of lactoferricin H, further referred to as hLF1–11, exerts effective antibacterial and antifungal activities, as demonstrated by in-vitro and in-vivo studies in systemic infections caused by fluconazole-resistant Candida albicans, multidrug-resistant Staphylococcus aureus, and Acinetobacter baumannii strains [20,21,22,23,24,25,26]. Moreover, hLF1–11 exerts modulatory effects on cells of the human immune system [27, 28], which is increasingly recognized as an important contribution to the clearance of infections [29,30,31].
Several AMP have shown synergistic activity with conventional antibacterial and antifungal agents, and combination therapies have also been proposed as a mean to reduce the frequency of emergence of resistant strains [32,33,34,35]. In the present study, we aimed at evaluating the antibacterial activity of hLF1–11 alone or in combination with various antibiotics against carbapenemase-producing K. pneumoniae strains harboring different resistance genes.
Materials and methods
Bacteria
Three K. pneumoniae strains were isolated from positive blood cultures of patients admitted to the Azienda Ospedaliero–Universitaria Pisana (Pisa, Italy) and selected on the basis of their antimicrobial susceptibility profile: a susceptible K. pneumoniae strain, a colistin-sensitive MDR strain, and a colistin-resistant (MIC 16 μg/ml) MDR K. pneumoniae strain. Their antimicrobial susceptibility profile was determined by the Vitek 2 system (bioMeriéux, l’Etoile, France) and confirmed by E-test (bioMeriéux) and Sensititre Aris System (Trek Diagnostic Systems, Thermo Fisher Scientific, OH, USA). The antimicrobials tested were the following: amoxicillin/clavulanic acid, ampicillin, carbapenems (imipenem, meropenem, ertapenem), piperacillin/tazobactam, cephalosporins (cefepime, cefotaxime, ceftazidime), aminoglycosides (amikacin, gentamicin, and tobramycin), fluoroquinolones (levofloxacin and ciprofloxacin), colistin, tigecycline, and trimethoprim/sulfamethoxazole. For both MDR K. pneumoniae strains, phenotypic and genotypic tests were performed to determine the type of carbapenemase. A combination disk test was used for the phenotypic characterization (Neosensitabs®, Rosco, Taastrup, Denmark). For genotypic characterization, after DNA extraction [36], the presence of bla KPC gene was determined using Hy-KPC real-time PCR, kindly provided by Hy-Labs (Hy-Labs, Israel), with the ABI Prism® 7500 instrument (Applied Biosystems, Foster City, CA, USA). Next, the bla KPC gene fragment (1010 bp) was amplified using KPC-fw/KPC-rv primers [37], purified after 1% agarose gel electrophoresis by 5Prime-Agarose GelExtract mini kit (5 Prime GmbH, Hilden, Germany), and sequenced using cycle sequencing technology (dideoxy chain termination/cycle sequencing) on ABI 3730XL sequencing apparatus (Eurofins Genomics Ebersberg, Germany). Sequencing results were analyzed by the sequence alignment Geneious software platform [38], and compared with the reference sequence from NC-021660 (Klebsiella pneumoniae FCF3SP plasmid, bla KPC type 2).
In addition, four multidrug resistant K. pneumoniae strains producing different carbapenemases (OXA-48, KPC-2, KPC-3, and VIM-1) and previously described [39] were used, and a K. pneumoniae ATCC® BAA-1705™ was included as a positive control for KPC production. Bacteria were cultured in Luria Bertani (LB) broth (Sigma–Aldrich, St. Louis, MO, USA) to mid-log phase; aliquots of this culture, containing 108 colony-forming unit (CFU)/ml, were supplemented with 20% (vol/vol) glycerol and stored at −80 °C. For antimicrobial susceptibility tests and synergy studies, each strain was cultured overnight in LB at 37 °C, and sub-cultured for 2 h on a rotary wheel at 37 °C.
Synthetic peptide and antibiotics
The synthetic peptide corresponding to residues 1–11 (GRRRRSVQWCA) of hLF, further referred to as hLF1–11, was purchased from Peptisyntha (Brussels, Belgium). The purity of this peptide exceeded 99%, as determined by reverse-phase high performance liquid chromatography (RP-HPLC). Peptide stocks at a concentration of 10 mM in 0.01% acetic acid (pH 3.7) were stored at −20 °C, and diluted to the desired concentration before use. The following antibiotics were tested in synergy studies: rifampicin, clarithromycin, clindamycin, gentamicin, and tigecycline, all purchased from Sigma–Aldrich (St. Louis, MO, USA). Rifampicin and tigecycline were dissolved in dimethyl sulfoxide (Fluka Chemie GmbH, Sigma–Aldrich Chemie BV, Zwijndrecht, The Netherlands) and stored at −80 °C. The final concentration of DMSO was <0.1%. The other antibiotics were dissolved in sterile distilled water and stored at −20 °C until use. Mueller Hinton (1:16 diluted) and NaPB (10 mM Na-phosphate buffer, pH 7.4) were freshly prepared for each experiment.
Antimicrobial peptide susceptibility assay
To assess the bactericidal activity of hLF1–11, K. pneumoniae cells were harvested in mid-log phase by centrifugation at 4,500 × g for 10 min, washed twice to completely remove traces amounts of culture medium (LB broth), and resuspended at a concentration of 107 CFU/ml in NaPB. Aliquots of this suspension were mixed with equal volumes of various concentrations of hLF1–11, prepared in NaPB, and incubated for 1 h at 37 °C. Thereafter, the number of viable bacterial cells was determined by plating serial dilutions of each sample on blood agar plates (Becton Dickinson & Co, BD; Milan, Italy).
Synergy studies
Synergy analyses of hLF1–11 and antimicrobial agents were carried out by a checkerboard titration method using 96-well round bottom polystyrene microtiter plates. This assay was performed in MH broth (MHB; Oxoid, Milan, Italy) diluted 1/16 in NaPB, since in preliminary experiments hLF1–11 showed no antibacterial activity in full strength medium (data not shown). In fact, similarly to what was observed with other antimicrobial peptides [40,41,42], the high ionic strength of MHB could possibly inhibit the interaction between the positive charges of hLF1–11 and the negatively charged bacterial surface. MIC values of each antibiotic were also assessed for comparison in undiluted MHB (Online supplementary materials, Table S1).
The ranges of concentration of the six antimicrobials tested were as follows: 0.125–32 μg/ml for rifampicin, 0.25–256 μg/ml for clarithromycin, 0.125–64 μg/ml for clindamycin, 0.015–16 μg/ml for gentamicin, and 0.06–16 μg/ml for tigecycline. The range of concentrations of hLF1–11 peptide was 2.7–88 μg/ml.
Briefly, the two-fold dilutions of each agent were set up in 100 μl of 1/8 strength Mueller–Hinton broth, and then an equal volume of the mid-log phase bacterial suspension in NaPB was inoculated into each well of the plate at a final concentration of approximately 5 × 105 CFU/ml. Sterility control wells, containing the medium alone, were included in each plate.
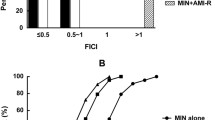
After 18–24 h incubation at 37 °C, the MIC of both the peptide and antibiotics were defined on the basis of the turbidity of the wells as the lowest concentration of the agent that produced the complete inhibition of visible growth. A variability of one dilution was considered acceptable to determine the MIC of hLF1–11 and antibiotics for each strain. The fractional inhibitory concentration (FIC) index for the combinations was calculated using the following formula: FIC index = (MIC drug A in combination)/(MIC drug A alone) + (MIC drug B in combination)/(MIC drug B alone). The FIC indices were interpreted as follows: ≤0.5, synergy, >0.5 to ≤4, indifference, and >4, antagonism [43]. FIC index was reported in this study as the mean of the lowest FIC indices of at least three independent experiments.
In addition, for antimicrobial combinations resulting in indifference by the checkerboard method, bactericidal kinetics synergy studies were performed at sub-inhibitory concentrations of each antimicrobial agent (1/2 MIC of hLF1–11, and 1/4 MIC of tigecycline), diluted in 1:16 MHB immediately before use. At 0, 1, 2, 3, 6, and 24 h, serial dilutions of cultures were plated onto solid media to determine the number of CFU per milliliter. Synergy was defined as a decrease in CFU/ml of ≥2 Log of the combination of hLF1–11 and drug, in comparison with its most active constituent [44]. All tests were performed in triplicate.
Hemolysis assay
A hemolysis assay was used to evaluate the cytotoxicity of the peptide and antibiotics alone and in combination. Briefly, blood from three healthy individuals was collected in vacuum tubes containing citrate (Becton Dickinson & Co, BD; Milan, Italy) as anticoagulant. Red blood cells (RBCs) were harvested by centrifugation at 1,600 × g for 5 min at room temperature, washed three times with phosphate-buffered saline (PBS, pH 7.4) and resuspended in PBS to a concentration of 8% (v/v). An aliquot (100 μl) of this suspension was transferred into each well of a 96-well microtiter plate and mixed with 100 μl of peptide or antibiotic solution at twice the desired concentration or 50 μl of 4× the peptide and antibiotic for synergy combinations.
After incubation for 1 h at 37 °C, the microtiter plate was centrifuged (1,600 × g, 5 min) and 100 μl of the supernatants were transferred to a flat-bottom 96-well plate for measurement of the hemoglobin release by reading the absorbance at 450 nm. Data were normalized between the 0% hemolysis of RBCs in PBS and 100% hemolysis of RBCs in 1% Triton X-100. The percentage of hemolysis was calculated by the following formula: (A peptide/antibiotic─ A PBS)/(A Triton X-100─A PBS) × 100%.
Statistical analysis
Data were expressed as means ± standard deviation of the mean (SD). Results obtained by the antimicrobial peptide susceptibility test and bactericidal kinetics synergy studies were analyzed by one-way ANOVA test after logarithmic transformation, using GraphPad Instat software (version 6.05 for Windows, La Jolla, CA, USA). Comparisons between the means of the untreated control and treated groups were made applying the Bonferroni post-hoc test. Comparisons between three strains for each peptide concentration were made applying the Tukey post-hoc test. The level of significance was set at a P value of <0.05.
Results
Antimicrobial peptide susceptibility assay
The antimicrobial activity of hLF1–11 was evaluated against three K. pneumoniae strains isolated from positive blood cultures. One strain was susceptible to all the tested antimicrobials with the exception of levofloxacin and ciprofloxacin, in addition to ampicillin to which K. pneumoniae is naturally resistant. Another strain, further referred to as 1R, showed a multidrug-resistant profile (including colistin resistance), and a third strain had a multidrug-resistant profile but was susceptible to colistin. The complete antimicrobial susceptibility profile of these K. pneumoniae strains is reported in Table S2 (Online supplementary materials). The characterization of the MDR strains by the combined disk method revealed that both K. pneumoniae strains were KPC-producing. Genotypic characterization by Hy-KPC real-time PCR indicated the presence of bla KPC gene in both the MDR K. pneumoniae strains. For the colistin-resistant 1R strain, which was further investigated in synergy studies, the variant of bla KPC gene was evaluated by sequencing, and the results revealed the presence of the variant type 3 of the bla KPC gene (Table 1).
In-vitro killing assays revealed that the hLF1–11-induced bactericidal activity was significantly (P < 0.05) higher against the non-carbapenemase-producing than both carbapenemase-producing K. pneumoniae strains (colistin-sensitive and colistin-resistant) at all the concentrations tested of hLF1–11 ≥ 88 μΜ, as shown in Fig. 1.
Antibacterial activity of hLF1–11 at different concentrations against three K. pneumoniae strains: a clinical susceptible K. pneumoniae strain (S, square), a colistin-resistant KPC K. pneumoniae strain (KPC R, circle, a), and a colistin-sensitive KPC K. pneumoniae strain (KPC S, triangle, b). Data are means ± SD of at least three independent experiments. K. pneumoniae cells (106 CFU/ml) were incubated with hLF1–11 for 1 h at 37 °C. The number of viable bacterial cells was determined by plating serial dilutions of each sample onto blood agar plates. * Significantly different (P < 0.05, ANOVA, Bonferroni test) as compared to untreated K. pneumoniae cells; # Significantly different (P < 0.05, ANOVA, Tukey test) from values obtained with the susceptible K. pneumoniae strain
Synergistic effect of hLF1–11 with antibiotics
Synergy studies combining various concentrations of hLF1–11 with antibiotics were performed by the checkerboard method against the 1R K. pneumoniae strain and other strains harboring different bla KPC genes and producing different types of carbapenemases. The MIC values of hLF1–11 and the various antibiotics tested are reported in Table 1. All K. pneumoniae strains were inhibited by hLF1–11, with MIC values ranging from 22 to 88 μg/ml.
The results obtained by the combination of hLF1–11 with the various antibiotics, expressed as FIC index, are shown in Table 2. The results revealed that hLF1–11 showed synergism with all antibiotics against at least some K. pneumoniae strains. A synergistic effect was observed with rifampicin, clarithromycin, and clindamycin (hydrophobic antibiotics) against all tested strains. The FIC index ranged from 0.22 to 0.47 in the combination of hLF1–11 with rifampicin, from 0.15 to 0.5 and from 0.19 to 0.5 in the combinations with clarithromycin and clindamycin respectively. In the presence of hLF1–11, the MIC of rifampicin was reduced by 64-fold (from 8 μg/ml to 0.125 μg/ml) for OXA-48 and VIM-1 K. pneumoniae strains, by 32-fold (from 16 μg/ml to 0.5 μg/ml and from 8 μg/ml to 0.25 μg/ml, respectively) for K. pneumoniae ATCC® BAA-1705™ and KPC-3 (colistin-sensitive), and by 8- to 16-fold for KPC 1R and KPC-2 strains.
In the peptide–clarithromycin combination, the MIC of the antibiotic was decreased from 4- to 64-fold, with the highest reductions observed against KPC-2 (from 32- to 64-fold), ATCC® BAA-1705™, and VIM-1 (both from 16- to 32-fold) strains. Among all strains, KPC 1R and KPC-3 showed the highest values of FIC indices.
In the peptide–clindamycin combination, the MIC of the antibiotic was decreased from 4- to 32-fold, with the highest reductions observed against VIM-1 (from 8- to 32-fold), and ATCC® BAA-1705™ (from 8- to 16-fold) strains. Among all strains, KPC 1R and KPC-3 showed the highest values of FIC indices.
Synergy was also obtained when hLF1–11 was tested in combination with gentamicin, as evidenced by FIC indices ranging from 0.21 to 0.5, and with tigecycline with FIC indices of 0.38–0.5. In contrast, no synergistic effect was observed with the hLF1–11 peptide-tigecycline combination against the KPC 1R strain and K. pneumoniae harboring the bla KPC-3 gene, with FIC indices of 0.84 and 0.75 respectively. Antibacterial kinetics experiments also showed no synergism in the peptide–tigecycline combination against the 1R strain at 24 h (Fig. 2), but revealed a synergistic effect at earlier time points. In fact, as shown in Fig. 2, the results of antibacterial kinetics experiments revealed a 3 Log CFU reduction at 6 h by the peptide–antibiotic combination in comparison to its most active constituent [44].
Kinetics of the antibacterial activity of hLF1–11 and tigecycline against KPC 1R K. pneumoniae strain. K. pneumoniae cells (106 CFU/ml) were incubated with 22 μg/ml hLF1–11 (diamond), 0.25 μg/ml tigecycline (circle), the combination of the same concentrations of hLF1–11 and tigecycline (square), or no treatment (triangle). The number of viable bacterial cells was determined at 0, 1, 2, 3, 6, and 24 h by plating serial dilutions of each sample onto blood agar plates. Data are means ± SD of at least three independent experiments. * Synergistic effect of the combination of hLF1–11 and tigecycline in comparison to its most active constituent (P < 0.05, ANOVA, Bonferroni test)
Hemolysis assay
A hemolysis assay was performed to evaluate possible toxic effects of the hLF1–11 peptide and antibiotics on human red blood cells (Fig. 3). The results revealed that hLF1–11 alone had no hemolytic activity (<1%) even at 10× the highest MIC value (880 μg/ml). In addition, all the tested antibiotics alone showed no hemolysis (≤1%), with the exception of rifampicin, which exhibited 1–5% hemolysis at 8–32 μg/ml and 37% hemolysis at 10× the highest MIC value (320 μg/ml). All combinations of the peptide with antibiotics showed no hemolysis (<1%) even at 10× MIC for both constituents (Fig. 4), with the exception of the combination of hLF1–11 with rifampicin, which exhibited no hemolysis at MIC (<1%) but 3% hemolysis at 10× MIC.
Hemolytic activity of peptide and antibiotics alone at various MICs. The values above the bars indicate the tested concentrations (μg/ml). The antibiotic or the peptide was incubated with 8% RBC suspension. The results are expressed as mean of percentage of hemolysis. RBCs incubated with 1% Triton X-100 and PBS (untreated) were considered as 100% and 0% hemolysis respectively. The percentage of hemolysis was calculated as follows: (A peptide/antibiotic─ A PBS)/(A Triton X-100─A PBS) × 100% ± SD from three independent experiments. RIF, rifampicin; CLR, clarithromycin; CLI, clindamycin; GEN, gentamicin; TGC, tigecycline
Hemolytic activity of the combination of the hLF1–11 peptide and antibiotics at MICs (open bars) and 10× MICs (gray bars). The values above the open bars indicate the tested concentrations (μg/ml). The tested concentrations are reported as x/y, where x and y represent the concentrations of the antibiotic and peptide respectively. The antibiotic and peptide were incubated with 8% RBC suspension. The results are expressed as mean of percentage of hemolysis. RBCs incubated with 1% Triton X-100 and PBS (untreated) were considered as 100% and 0% hemolysis respectively. The percentage of hemolysis was calculated as follows: (A peptide/antibiotic─ A PBS)/(A Triton X-100─A PBS) × 100% ± SD from three independent experiments. RIF, rifampicin; CLR, clarithromycin; CLI, clindamycin; GEN, gentamicin; TGC, tigecycline
Discussion
Carbapenem-resistant K. pneumoniae strains are often resistant to multiple classes of antibiotics, including fluoroquinolones, aminoglycosides, and β-lactams [45] and, therefore, treatment of infections caused by such strains often meets with failure, and is associated with high mortality rates. Combination therapies have been shown to significantly improve the therapeutic efficacy in the treatment of bacterial infections [46], and there is evidence suggesting that emergence of antimicrobial resistance may be reduced by using combination therapy regimens [47, 48]. However, this is a controversial issue and some studies indicate that, unless highly inhibitory antibiotic doses are maintained until the pathogen is eradicated, combination therapy can have the opposite effect, i.e., to accelerate the emergence and spread of MDR bacterial strains [49, 50]. Another, recently proposed approach to combat infections caused by MDR bacterial strains consists in combining antibiotics and antimicrobial peptides [51]. These latter show broad-spectrum antimicrobial activity, frequently show strong synergism with conventional antibiotics [52], and have been suggested to help in preventing or delaying the emergence of antibiotic resistance [51, 52].
The present study aimed at evaluating the antibacterial activity of hLF1–11, alone or in combination with various antimicrobial drugs, against different strains of K. pneumoniae. The mechanism of action of cationic AMP is commonly related to their ability to interact with negatively charged components of cell membranes, and a correlation between colistin resistance and cross-resistance to host antimicrobial peptides has been reported, thus suggesting the existence of shared mechanisms of action for these compounds [53]. Therefore, the hLF1–11-induced bactericidal activity was evaluated against two MDR K. pneumoniae strains differing for colistin susceptibility and a K. pneumoniae strain susceptible to most of the antibiotics tested. The results revealed that the hLF1–11-induced bactericidal activity was significantly (P < 0.05) higher against a non-carbapenemase-producing K. pneumoniae than a colistin-sensitive and a colistin-resistant carbapenemase-producing K. pneumoniae strain in an in-vitro killing assay. This evidence indicates that resistance to colistin and to the hLF1–11 peptide are not strictly associated. Therefore, other distinct mechanisms of resistance to the hLF1–11 peptide and to colistin should also be considered [54].
The main conclusion from the present data is that hLF1–11 is a promising candidate for combination therapies with various antibiotics in the treatment of infections caused by MDR K. pneumoniae strains. This conclusion is based on the following findings. First, the hLF1–11 peptide exerted synergistic effects in combination with most of the antibiotics tested by the checkerboard assay. Rifampicin, clarithromycin, or clindamycin, which are hydrophobic antimicrobial drugs, are normally not able to permeate through the outer membrane of Gram-negative bacteria, thereby being ineffective against these microorganisms [55]. Indeed, hLF1–11 induced up to a 64-fold reduction in the MIC of these hydrophobic antibiotics and a 4- to 16-fold reduction in the MIC of gentamicin or tigecycline against the tested K. pneumoniae strains. These results suggest a hLF1–11-induced sensitizing effect on KPC K. pneumoniae strains to antibiotics. The mechanism underlying the synergistic effect between hLF1–11 and otherwise impermeable hydrophobic antibiotics might be the result of a transient loss of membrane potential induced by hLF1–11 and subsequent increase in cell membrane permeabilization. Further studies will help to elucidate the mechanism of action underlying these synergistic effects. Second, the highest FIC indices by the checkerboard assay, indicating indifference, were observed in the combinations of hLF1–11 and tigecycline against the two K. pneumoniae strains harboring the bla KPC-3 gene. However, antibacterial kinetics studies, performed against K. pneumoniae 1R showed a synergistic effect exerted by the combination of hLF1–11 and tigecycline at 6 h. In agreement with the results obtained by the checkerboard assay, no synergistic effect was observed at 24 h. Due to the chemical nature of the peptide, it is possible that hLF1–11 was progressively inactivated by bacterial cell components, such as proteases, released by dead cells after incubation with the antimicrobial peptide. A multiple daily administration regimen for the combination hLF1–11/tigecycline as well as for other antimicrobial peptide/antibiotic combinations might be considered in order to achieve complete eradication of bacteria. Chemical modification of the peptide enhancing its stability in biological fluids might also be attempted [56]. Alternatively, resumption of bacterial growth might be due to rapid evolutionary adaptation of K. pneumoniae persistence, though this phenomenon is usually associated with repeated antibiotic application rather than with a single-dose exposure [57]. Further studies will be needed to shed light on this issue. Third, all combinations of the peptide with antibiotics showed no hemolytic activity (<1%) even at 10× MIC, with the only exception of rifampicin, which exhibited 3% hemolysis at 10× MIC in combination with hLF1–11. The latter observation is not surprising, since the rifampicin-induced hemolytic activity by eryptosis has already been described [58]. These results indicate that hLF1–11 might be safe to be used in combination with antibiotics in the treatment of infections caused by KPC K. pneumoniae strains.
Overall, the results of the present study indicate that a combination therapy consisting of hLF1–11 and conventional antibiotics may be considered, and might be helpful as a last resort to treat infections sustained by antibiotic resistant bacterial strains. Such combination therapies represent a promising approach to treat infections caused by MDR K. pneumoniae strains for which conventional antibiotics are no longer effective and hydrophobic antibiotics are not indicated. Since the ionic strength in biological fluids may affect the antibacterial activity of hLF1–11, further studies will be needed to assess the in-vivo efficacy of hLF1–11, alone or in combination with antibiotics, against MDR K. pneumoniae strains, and to elucidate the mechanisms of action underlying the sensitizing effect of hLF1–11 to antibiotics.
References
Lee CR, Lee JH, Park KS, Kim YB, Jeong BC, Lee SH (2016) Global dissemination of carbapenemase-producing Klebsiella pneumoniae: epidemiology, genetic context, treatment options, and detection methods. Front Microbiol 7:895. doi:10.3389/fmicb.2016.00895
Tsakris A, Poulou A, Pournaras S, Voulgari E, Vrioni G, Themeli-Digalaki K et al (2010) A simple phenotypic method for the differentiation of metallo-beta-lactamases and class a KPC carbapenemases in Enterobacteriaceae clinical isolates. J Antimicrob Chemother 65(8):1664–1671. doi:10.1093/jac/dkq210
Walsh TR (2010) Emerging carbapenemases: a global perspective. Int J Antimicrob Agents 36(3):S8–S14. doi:10.1016/S0924-8579(10)70004-2
Nordmann P, Naas T, Poirel L (2011) Global spread of carbapenemase-producing Enterobacteriaceae. Emerg Infect Dis 17(10):1791–1798. doi:10.3201/eid1710.110655
Cantòn R, Akòva M, Carmeli Y, Giske CG, Glupczynski Y, Gniadkowski M et al (2012) The European network on Carbapenemases. Rapid evolution and spread of carbapenemases among Enterobacteriaceae in Europe. Clin Microbiol Infect 18(5):413–431. doi:10.1111/j.1469-0691.2012.03821.x
Nordmann P, Cuzon G, Naas T (2009) The real threat of Klebsiella pneumoniae carbapenemase-producing bacteria. Lancet Infect Dis 9(4):228–236. doi:10.1016/S1473-3099(09)70054-4
Elemam A, Rahimian J, Doymaz M (2010) In vitro evaluation of antibiotic synergy for polymyxin B-resistant carbapenemase-producing Klebsiella pneumoniae. J Clin Microbiol 48(10):3558–3562. doi:10.1128/JCM.01106-10
Livermore D (2009) Has the era of untreatable infections arrived? J Antimicrob Chemother 64(Suppl 1):i29–i36. doi:10.1093/jac/dkp255
Borer A, Saidel-Odes L, Riesenberg K, Eskira S, Peled N, Nativ R et al (2009) Attributable mortality rate for carbapenem resistant Klebsiella pneumoniae bacteremia. Infect Control Hosp Epidemiol 30(10):972–976. doi:10.1086/605922
Souli M, Galani I, Antoniadou A, Papadomichelakis E, Poulakou G, Panagea T et al (2010) An outbreak of infection due to β-lactamase Klebsiella pneumoniae carbapenemase 2-producing K. pneumoniae in a Greek University hospital: molecular characterization, epidemiology, and outcomes. Clin Infect Dis 50(3):364–373. doi:10.1086/649865
Kelesidis T, Karageorgopoulos DE, Kelesidis I, Falagas ME (2008) Tigecycline for the treatment of multidrug-resistant Enterobacteriaceae: a systematic review of the evidence from microbiological and clinical studies. J Antimicrob Chemoter 62(5):895–904. doi:10.1093/jac/dkn311
Chen LF, Anderson DJ, Paterson DL (2012) Overview of the epidemiology and the threat of K. pneumoniae carbapenemases (KPC) resistance. Infect Drug Resist 5:133–141. doi:10.2147/IDR.S26613
Giani T, Arena F, Vaggelli G, Conte V, Chiarelli A, Henrici De Angelis L et al (2015) Large nosocomial outbreak of colistin-resistant, carbapenemase-producing Klebsiella pneumoniae traced to clonal expansion of an mgrB deletion mutant. J Clin Microbiol 53(10):3341–3344. doi:10.1128/JCM.01017-15
Spanu T, De Angelis G, Cipriani M, Pedruzzi B, D’Inzeo T, Cataldo MA et al (2012) In vivo emergence of tigecycline resistance in multidrug-resistant Klebsiella pneumoniae and Escherichia coli. Antimicrob Agents Chemother 56(8):4516–4518. doi:10.1128/AAC.00234-12
Boucher HW, Talbot GH, Bradley JS, Edwards JE, Gilbert D, Rice LB et al (2009) Bad bugs, no drugs: no eskape! An update from the Infectious Diseases Society of America. Clin Infect Dis 48(1):1–12. doi:10.1086/595011
Baltzer SA, Brown MH (2011) Antimicrobial peptides—promising alternatives to conventional antibiotics. J Mol Microbiol Biotechnol 20(4):228–235. doi:10.1159/000331009
Appelt C, Schrey AK, Soderhall JA, Schmieder P (2007) Design of antimicrobial compounds based on peptide structures. Bioorg Med Chem Lett 17(8):2334–2337
González-Chávez SA, Arévalo-Gallegos S, Rascón-Cruz Q (2009) Lactoferrin: structure, function and applications. Int J Antimicrob Agents 33(4):301.e1–301.e8. doi:10.1016/j.ijantimicag.2008.07.020
Deriy LV, Chor J, Thomas LL (2000) Surface expression of lactoferrin by resting neutrophils. Biochem Biophys Res Commun 275(1):241–246
Lupetti A, Paulusma-Annema A, Welling MM, Senesi S, van Dissel JT, Nibbering PH (2000) Candidacidal activities of human lactoferrin peptides derived from the N terminus. Antimicrob Agents Chemother 44(12):3257–3263
Nibbering PH, Ravensbergen WMM, van Berkel LA, van Berkel PH, Pauwels EK et al (2001) Human lactoferrin and peptides derived from its N terminus are highly effective against infection with antibiotic-resistant bacteria. Infect Immun 69(3):1469–1476
Lupetti A, Paulusma-Annema A, Welling MM, Dogterom-Ballering H, Brouwer CP, Senesi S et al (2003) Synergistic activity of the N-terminal peptide of human lactoferrin and fluconazole against Candida species. Antimicrob Agents Chemother 47(1):262–267
Dijkshoorn L, Brouwer CP, Bogaards SJ, Nemec A, van den Broek PJ, Nibbering PH (2004) The synthetic N-terminal peptide of human lactoferrin, hLF(1-11), is highly effective against experimental infection caused by multidrug-resistant Acinetobacter baumannii. Antimicrob Agents Chemother 48(12):4919–4921
Lupetti A, Brouwer PJM, Bogaards SJP, Welling MM, de Heer E, Campa M et al (2007) Human lactoferrin-derived peptide’s antifungal activities against disseminated Candida albicans infection. J Infect Dis 196(9):1416–1424
Lupetti A, van Dissel JT, Brouwer CPJM, Nibbering PH (2008) Human antimicrobial peptides’ antifungal activity against Aspergillus fumigatus. Eur J Clin Microbiol Infect Dis 27(11):1125–1129. doi:10.1007/s10096-008-0553-z
Lupetti A, Welling MM, Pauwels EK, Nibbering PH (2003) Radiolabelled antimicrobial peptides for infection detection. Lancet Infect Dis 3(4):223–229
Easton DM, Nijnik A, Mayer ML, Hancock RE (2009) Potential of immunomodulatory host defense peptides as novel anti-infectives. Trends Biotechnol 27(10):582–590. doi:10.1016/j.tibtech.2009.07.004
Niyonsaba F, Nagaoka I, Ogawa H, Okumura K (2009) Multifunctional antimicrobial proteins and peptides: natural activators of immune systems. Curr Pharm Des 15(21):2393–2413
van der Does AM, Joosten SA, Vroomans E, Bogaards SJ, van Meijgaarden KE, Ottenhoff TH et al (2012) The antimicrobial peptide hLF1-11 drives monocyte-dendritic cell differentiation toward dendritic cells that promote antifungal responses and enhance Th17 polarization. J Innate Immun 4(3):284–292. doi:10.1159/000332941
van der Does AM, Bogaards SJ, Jonk L, Wulferink M, Velders MP, Nibbering PH (2010) The human lactoferrin-derived peptide hLF1-11 primes monocytes for an enhanced TLR-mediated immune response. Biometals 23(3):493–505. doi:10.1007/s10534-010-9322-4
van der Does AM, Hensbergen PJ, Bogaards SJ, Cansoy M, Deelder AM, van Leeuwen HC et al (2012) The human lactoferrin-derived peptide hLF1-11 exerts immunomodulatory effects by specific inhibition of myeloperoxidase activity. J Immunol 188(10):5012–5019. doi:10.4049/jimmunol.1102777
Barriere SL (1992) Bacterial resistance to beta-lactams, and its prevention with combination antimicrobial therapy. Pharmacotherapy 12:397–402
Wu YL, Scott EM, Po AL, Tariq VN (1999) Development of resistance and cross-resistance in Pseudomonas aeruginosa exposed to subinhibitory antibiotic concentrations. APMIS 107(6):585–592
Cassone M, Otvos L Jr (2010) Synergy among antibacterial peptides and between peptides and small-molecule antibiotics. Expert Rev Anti-Infect Ther 8(6):703–716. doi:10.1586/eri.10.38
Zhang Y, Liu Y, Sun Y, Liu Q, Wang X, Li Z et al (2014) In vitro synergistic activities of antimicrobial peptide Brevinin-2CE with five kinds of antibiotics against multidrug resistant clinical isolates. Curr Microbiol 68(6):685–692. doi:10.1007/s00284-014-0529-4
Chen L, Mediavilla JR, Oliveira DC, Willey BM, de Lencastre H, Kreiswirth BN (2009) Multiplex real-time PCR for rapid staphylococcal cassette chromosome mec typing. J Clin Microbiol 47(11):3692–3706. doi:10.1128/JCM.00766-09
Yigit H, Queenan AM, Anderson GJ, Domenech-Sanchez A, Biddle JW, Steward CD et al (2001) Novel carbapenem-hydrolyzing beta-lactamase, KPC-1, from a carbapenem-resistant strain of Klebsiella pneumoniae. Antimicrob Agents Chemother 45(4):1151–1161
Kearse M, Moir R, Wilson A, Stones-Havas S, Cheung M, Sturrock S et al (2012) Geneious basic: an integrated and extendable desktop software platform for the organization and analysis of sequence data. Bioinformatics 28(12):1647–1649. doi:10.1093/bioinformatics/bts199
Giani T, Pini B, Arena F, Conte V, Bracco S, Migliavacca R, Pantosti A, Pagani L, Luzzaro F, Rossolini GM; AMCLI-CRE Survey Participants (2013) Epidemic diffusion of KPC carbapenemase-producing Klebsiella pneumoniae in Italy: results of the first countrywide survey, 15 May to 30 June 2011. Euro Surveill 18(22):pii 20489
Cudic M, Condie BA, Weiner DJ, Lysenko ES, Xiang ZQ, Insug O, Bulet P, Otvos L Jr (2002) Development of novel antibacterial peptides that kill resistant isolates. Peptides 23:2071–2083
Yan H, Hancock REW (2001) Synergistic interactions between mammalian antimicrobial defence peptides. Antimicrob Agents Chemother 45(5):1558–1560
Cassone M, Vogiatzi P, La Montagna R, De Olivier IV, Cudic P, Wade JD, Otvos L Jr (2008) Scope and limitations of the designer proline-rich antibacterial peptide dimer, A3-APO, alone or in synergy with conventional antibiotics. Peptides 29(11):1878–1886. doi:10.1016/j.peptides.2008.07.016
Moody JA (1992) Synergism testing: broth microdilution checkerboard and broth macrodilution methods. In: Isenberg HD (ed) Clinical procedures handbook. ASM Press, Washington, pp 5.18.1–5.18.28
Odds FC (2003) Synergy, antagonism, and what the chequerboard puts between them. J Antimicrob Chemother 52(1):1. doi:10.1093/jac/dkg301
Schultsz C, Geerlings S (2012) Plasmid-mediated resistance in Enterobacteriaceae: changing landscape and implications for therapy. Drugs 72(1):1–16. doi:10.2165/11597960-000000000-00000
Toledo PV, Aranha AA Jr, Arend LN, Ribeiro V, Zavascki AP, Tuon FF (2015) Activity of antimicrobial combinations against KPC-2-producing Klebsiella pneumoniae in a rat model and time-kill assay. Antimicrob Agents Chemother 59(7):4301–4304. doi:10.1128/AAC.00323-15
Drusano GL, Sgambati N, Eichas A (2010) The combination of rifampin plus moxifloxacin is synergistic for suppression of resistance but antagonistic for cell kill of Mycobacterium tuberculosis as determined in a hollow-fiber infection model. MBio 1(3):1–8. doi:10.1128/mBio.00139-10
Rodriguez De Evgrafov M, Gumpert H, Munck C et al (2015) Collateral resistance and sensitivity modulate evolution of high-level resistance to drug combination treatment in Staphylococcus aureus. Mol Biol Evol 32:1175–1185
Hegreness MJ, Shoresh N, Damian D et al (2008) Accelerated evolution of resistance in multidrug environments. Proc Natl Acad Sci 105:13977–13981
Pena-Miller R, Laehnemann D, Jansen G et al (2013) When the most potent combination of antibiotics selects for the greatest bacterial load: the smile–frown transition. PLoS Biol 11:e1001540
Feng Q, Huang Y, Chen M, Li G, Chen Y (2015) Functional synergy of α-helical antimicrobial peptides and traditional antibiotics against Gram-negative and Gram-positive bacteria in vitro and in vivo. Eur J Clin Microbiol Infect Dis 34(1):197–204. doi:10.1007/s10096-014-2219-3
Mataraci E, Dosler S (2012) In vitro activities of antibiotics and antimicrobial cationic peptides alone and in combination against methicillin-resistant Staphylococcus aureus biofilms. Antimicrob Agents Chemother 56(12):6366–6371
Napier BA, Burd EM, Satola SW, Cagle SM, Ray SM, McGann P et al (2013) Clinical use of colistin induces cross-resistance to host antimicrobials in Acinetobacter baumannii. MBio 4(3):e00021–e00013. doi:10.1128/mBio.00021-13
Formosa C, Herold M, Vidaillac C, Duval RE, Dague E (2015) Unravelling of a mechanism of resistance to colistin in Klebsiella pneumoniae using atomic force microscopy. J Antimicrob Chemother 70(8):2261–2270. doi:10.1093/jac/dkv118
Vaara M (1990) Antimicrobial susceptibility of Salmonella typhimurium carrying the outer membrane permeability mutation SS-B. Antimicrob Agents Chemother 34(5):853–857
Kim H, Jang JH, Kim SC, Cho JH (2014) De novo generation of short antimicrobial peptides with enhanced stability and cell specificità. J Antimicrob Chemother 69:121–132
Van den Bergh B, Michiels JE, Wenseleers T, Windels EM, Boer PV, Kestemont D, De Meester L, Verstrepen KJ, Verstraeten N, Fauvart M, Michiels J (2016) Frequency of antibiotic application drives rapid evolutionary adaptation of Escherichia coli persistence. Nat Microbiol 1:16020. doi:10.1038/nmicrobiol.2016.20
Abed M, Towhid ST, Shaik N, Lang F (2012) Stimulation of suicidal death of erythrocytes by rifampicin. Toxicology 302:123–128. doi:10.1016/j.tox.2012.10.006
Acknowledgements
The authors pay tribute to the late Prof. Mario Campa for his longstanding inspiration and support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Italian Ministero dell’Istruzione, dell’Università e della Ricerca (MIUR), research grant number 2012WJSX8K_005.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was notified to the local ethical committee, Comitato Etico di Area Vasta Nord-Ovest, University of Pisa, and conducted in full accordance with the principles of the Declaration of Helsinki. Samples were taken as part of the standard patient care. These samples were anonymized by the clinical personnel. Research personnel received and used these samples anonymously. For this type of study, no written informed consent was necessary.
Furthermore, three blood samples were withdrawn from healthy volunteers, casually chosen among the authors of this manuscript, to perform the hemolysis assay. The local ethical committee ruled that no notification was necessary in this case.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Morici, P., Florio, W., Rizzato, C. et al. Synergistic activity of synthetic N-terminal peptide of human lactoferrin in combination with various antibiotics against carbapenem-resistant Klebsiella pneumoniae strains. Eur J Clin Microbiol Infect Dis 36, 1739–1748 (2017). https://doi.org/10.1007/s10096-017-2987-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-017-2987-7