Abstract
Purpose
To retrospectively compare the clinical outcomes of closed treatment (closed reduction and intermaxillary fixation) with open treatment (open reduction and internal fixation with miniplates and screws) of unilateral mandibular condylar process fractures.
Methods
Adult patients with unilateral condylar fractures treated from January 2011 to July 2013 in the Oral and Maxillofacial Surgery Service at the Base Hospital of the Federal District, Brazil, were invited to participate. Those who agreed to participate were scheduled for clinical evaluation, which consisted of a subjective questionnaire (completed by the examiner) and an objective physical examination of the temporomandibular joints and mandibular range of motion. The following variables were analyzed: mouth opening; lateral excursions of the mandible; presence of clicking; mandibular function impairment (speech, chewing); and occlusion.
Results
Seventeen patients (15 men and 2 women) attended the scheduled appointment: 9 had received open treatment (surgical) and 8 had received closed treatment (nonsurgical). Patients were evaluated at 6–30 months postoperatively. Only maximum mouth opening (p = 0.044) and maximum lateral excursion to the unaffected side (p = 0.030) showed a significant difference between the closed and open treatment groups.
Conclusions
Our findings are consistent with those reported in the literature as both methods (closed and open treatment) produced satisfactory outcomes. The only between-group difference was the amount of maximum mouth opening and lateral excursion to the unaffected side. Further randomized studies with a larger number of patients with condylar process fractures are needed to verify the results obtained with each treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mandibular fractures are commonly seen in the emergency departments of oral and maxillofacial surgery services worldwide, accounting for approximately 35% of all facial injuries treated by the oral and maxillofacial surgeon [1]. Of these, about one-third involve the condylar process [2].
Condylar fractures deserve special attention not only because of the risk of facial asymmetry and malocclusion but also because their treatment remains controversial. Condylar fractures have been treated either conservatively or surgically [3,4,5]. Nonsurgical treatment consists of closed reduction and maxillomandibular fixation (MMF) for 2–4 weeks [4, 5] or 4–6 weeks [6], followed by intensive postoperative physical therapy for restoration of masticatory function [6]. Surgical treatment consists of open reduction and internal fixation (ORIF) of the condylar fracture with titanium plates and screws [7].
In view of the advantages and disadvantages of each type of treatment and the fact that complications can arise from both open and closed approaches [8, 9], we conducted a non-randomized, uncontrolled study to retrospectively compare the clinical outcomes of closed treatment (nonsurgical) with open treatment (surgical) of unilateral mandibular condylar process fractures.
Materials and methods
The electronic medical records of all patients treated from January 2011 to July 2013 in the Oral and Maxillofacial Surgery Service at the Base Hospital of the Federal District, located in Brasília, the capital of Brazil, were retrospectively reviewed for patient selection. Eligible participants were all patients who had received either open treatment or closed treatment for unilateral mandibular condylar process fractures during the study period. Patients aged < 18 years and patients who had bilateral condylar fractures were excluded. This study was approved by the research ethics committee of the institution, via Plataforma Brasil (www.saude.gov.br/plataformabrasil), under Ethics Approval Certificate number 380 663. Written informed consent was obtained from all individual participants included in the study.
Eligible patients were contacted by telephone and invited to participate in the study. Those who agreed to participate were scheduled for clinical evaluation, which consisted of a subjective questionnaire (completed by the examiner) and an objective physical examination of the temporomandibular joints (TMJs) bilaterally and of mandibular range of motion. All participants were evaluated clinically and radiographically by a single examiner in a single appointment.
During questionnaire administration, patients were asked to subjectively evaluate mouth opening, presence of clicking, mandibular function impairment (speech, chewing), and self-perception of occlusion. Physical examination followed a specific sequence consisting of measurement of maximum mouth opening and maximum lateral excursions of the mandible (to the unaffected side and to the affected side, measured from the maxillary midline and the incisal edges of the lower and upper incisors), (digital caliper, KingTools 150 mm, vernier—0.01 mm, 502,550), presence of clicking during mouth opening and during lateral excursion (auscultation with a stethoscope), and occlusion. At the same appointment, integrity of the condylar process (resorption), integrity of synthesis materials, and type of fixation used were assessed on panoramic radiographs of the mandible (posteroanterior view and reverse Towne view).
Open treatment (surgical)
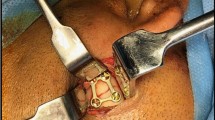
Open reduction was performed using a retromandibular approach by dissecting the skin and subcutaneous tissue vertically to the mandibular angle using the 3-cm incision line to 5 mm inferior to the auricular lobe. After intermaxillary fixation (IMF), condylar fracture reduction and fixation was achieved with two straight five-hole miniplates (trapezoidal arrangement) secured with four 8-mm screws.
Closed treatment (nonsurgical)
For closed reduction, IMF was performed using arch bars and wires and maintained for 2–3 weeks. After achieving stable union of the fractured site, the fixation wires were removed and normal occlusion was induced using guiding elastics. Soft diet was maintained for 2 weeks.
Data derived from yes-or-no answers were treated as categorical variables (patient-reported clicking and occlusal changes and auscultated clicking during mouth opening and during lateral excursion), and those derived from measurable quantities were treated as quantitative variables (maximum mouth opening and maximum lateral excursions of the mandible to the unaffected and affected sides measured in mm). Fisher’s exact test was used for quantitative variables, with 95% confidence interval, while Student’s t test was used to compare the means of categorical variables. For quantitative variables, the Shapiro-Wilk test was used to determine the normality of data distribution. When the data were normally distributed, but population variance was unknown, sampling variance was calculated for application of Student’s t test. Statistical analysis was performed using SPSS, version 23.0. A p value < 0.05 was considered statistically significant.
Results
The initial screening resulted in the selection of 77 patients to be contacted for the study. Of these, we were unable to contact 45 patients because they had no telephone numbers available, or they had an out-of-date or a wrong number. Of the 32 patients who were successfully contacted by telephone, 17 agreed to participate and were scheduled for clinical evaluation. All 17 patients (15 men and 2 women) attended the scheduled appointment. Of these, 9 had received open treatment (surgical) and 8 had received closed treatment (nonsurgical).
Patients were evaluated at 6–30 months postoperatively. There was a significant difference between the closed treatment and open treatment groups in maximum mouth opening and maximum lateral excursion to the unaffected side, favoring patients who were treated surgically (Table 1).
As shown in Fig. 1, maximum mouth opening ranged from 42 to 55 mm in the open treatment group and from 33 to 55 mm in the closed treatment group, with a significant difference between the groups (p = 0.044).
As shown in Fig. 2, maximum lateral excursion to the unaffected side ranged from 2 to 15 mm in the closed treatment group and from 3 to 14 mm in the open treatment group, with a significant difference between the groups (p = 0.030). After outlier removal (a patient with maximum lateral excursion of 15 mm in the closed treatment group), the values of maximum lateral excursion to the unaffected side in the open treatment group were significantly different from those of the affected side, suggesting that the anatomical reduction rehabilitated the affected side, thus allowing functional displacement with adequate translation of the condyle (unaffected side mean of 8.62 mm for open treatment and of 6.11 mm for closed treatment).
Maximum lateral excursion to the affected side ranged from 3 to 13 mm in the closed treatment group and from 3 to 10 mm in the open treatment group, with no significant difference between the groups (p = 0.960) (Fig. 3).
Regarding the subjective evaluation of clicking, 5 (55.6%) patients in the open treatment group and 3 (37.5%) in the closed treatment group reported clicking of the TMJ, with no significant difference between the groups (p = 0.637). Only 2 patients (one in each group) reported having TMJ pain associated with clicking; however, both cases were considered occasional and of low intensity (both were rated 4 on a 1–10 pain scale, where 1 = no pain). As for self-perception of occlusion, 4 (44.4%) patients in the open treatment group and 4 (50.0%) in the closed treatment group reported occlusal changes after treatment, with no significant difference between the groups (p = 1.0).
Clicking during mouth opening and during lateral excursion was auscultated by the examiner, respectively, in 7 (77.8%) and 5 (55.6%) patients in the open treatment group and in 5 (62.5%) and 4 (50.0%) patients in the closed treatment group, with no significant difference between the groups in either parameter (p = 0.619 and p = 1.0, respectively).
Discussion
The results of the present study are consistent with those reported in the literature indicating that there are no statistically significant differences between open (surgical) and closed (nonsurgical) treatment of unilateral mandibular condylar process fractures [10, 11]. It is worth noting that, in the present study, of 17 patients, only 2 (11.8%) failed to achieve a mouth opening > 40 mm, and both of them were in the open treatment group.
Early active mobilization of the mandible has been associated with better outcomes regarding mandibular movement [12, 13]. Palmieri et al. [12] suggested that elimination of the MMF period, allowing immediate mobilization of the jaw, benefits patients receiving closed treatment. In the present study, patients in the closed treatment group had an average 6 mm greater maximum mouth opening than those in the open treatment group. It should be noted that 2 patients treated closed remained with the IMF wires for 2 weeks, while the other 6 patients remained with the IMF wires for up to 6 weeks. Only after this period could they regain mandibular mobility and undergo physical therapy for mouth opening with wooden tongue depressors, and such period did not seem to affect the long-term results with respect to mouth opening.
Sforza et al. [14] stated that the amount of maximum mouth opening cannot be used as an endpoint for TMJ function, and the use of measures such as the reciprocal amount of translation and rotation between the intact and fractured condyles could provide more useful information. The interincisal distance during mouth opening results from a combination of rotation and translation of the condylar heads, and a similar degree of mouth opening may be obtained with a variety of combinations of different degrees of condylar translational and rotational movements [12, 15]. However, no correlation has been found between maximum mouth opening and condylar translation [16]. A greater than normal translational movement of a non-fractured joint may compensate for the limited translation of the fractured joint. Therefore, using interincisal distance, i.e., maximum mouth opening, to clinically evaluate condylar movements may mistakenly suggest normal function when, in fact, condylar movements are abnormal [12].
The mean duration of treatment with IMF in the present study was similar to that reported by Vesnaver et al. [6], in which closed treatment consisted of IMF for 3–4 weeks, followed by the use of guiding elastics for 2 weeks. In their study, no significant difference was found between groups in mouth opening, but there was a difference in the symmetry of lateral movements, thus partially supporting the present results.
Throckmorton and Ellis [15] showed that patients treated closed had significantly smaller than normal excursion toward the non-fractured side even after 3 years of follow-up. According to Stiesch-Scholz et al. [17], a possible reason for the decreased joint range of motion after closed treatment is that immobilization of the injured joint leads to degeneration of the articular surface and development of fibrous adhesion, resulting in limited mobility. Gupta et al. [11], however, obtained better results with closed treatment, with an average 2 mm greater protrusive movement in the nonsurgical group than in the surgical group after 12 months of follow-up. The authors suggested that patients with less trismus at initial assessment are potentially favorable for closed treatment [11]. Silvennoinen et al. [18], investigating adult patients with unilateral condylar fractures, found that mandibular ramus height is significantly reduced in patients with persistent malocclusion, regardless of the degree of fragments or direction of displacement. They concluded that condylar fractures potentially causing future occlusal problems can be identified preoperatively by simply measuring the ramus height, and those with reduced height should be elected for surgical treatment [18].
In the present study, occlusal changes were evaluated subjectively by asking patients if they considered their occlusion altered compared with before the fracture. Because patients’ occlusal examinations from before the trauma were not available, comparative objective tests could not be performed. However, in general, patients reported no significant occlusal changes in addition to pre-existing dental defects, such as multiple missing teeth in the posterior region. Also, all patients who reported a painful condition were classified as “early stage” according to the Wilkes classification, i.e., clinically there were no significant mechanical symptoms other than clicking and radiographically there was good anatomical contour and mild anterior displacement of the condyle [19]. In a study of surgical complications associated with ORIF using a retromandibular approach in 10 patients with displaced unilateral/bilateral condylar fractures, 2 patients had clicking in the operated joint 1 week postoperatively, which resolved gradually [20]. In a retrospective study of 144 patients with 163 condylar fractures treated conservatively, the most common self-reported and observed post-treatment complications were clicking, crepitation, and occlusal changes [21]. In a healthy population, a 2-year longitudinal study reported a prevalence of clicking and/or crepitation ranging from 13 to 35% according to age group [22].
Limitations
We acknowledge the limitations of the retrospective, non-randomized nature of our study. In the literature, most non-randomized studies comparing open versus closed treatment have methodological biases, since most unilateral condylar fractures with severe displacement or dislocation and bilateral fractures, which have a worse prognosis, tend to be treated surgically, while the groups receiving closed treatment often involve unilateral and uncomplicated fractures [23]. Also, the lack of random patient selection prevented us from evaluating clinical variables that have the potential to influence functional outcomes, such as age, degree of dislocation, fracture level, unilateral/bilateral fractures, and other associated facial injuries [10]. However, Landes and Lipphardt [5], after analyzing the results of a literature review, highlighted that a complete randomization—for example, performing closed treatment in severely displaced condylar fractures—would not be considered ethically acceptable. Although there are numerous publications on the issue of condyle fracture, the therapeutic behavior of surgeons is often based on personal beliefs rather than on evidence from the literature [5]. Prospective studies are therefore needed to avoid the inherent limitations in retrospective studies. However, we recognize that evidence-based protocols are difficult to develop [24]. It should be noted that each fracture is unique, and the decision about which treatment is most appropriate for each case must be based on the literature as well as on clinical and radiological findings, the surgeon’s experience, and the patient’s willingness to periodically attend follow-up appointments [6, 25].
Conclusions
The present results are consistent with those reported in the literature as both methods (closed and open treatment) produced satisfactory outcomes. The only between-group differences were an average 6 mm greater maximum mouth opening in the closed treatment group and an average 2.5 mm greater maximum lateral excursion to the unaffected side in the open treatment group. Further randomized studies with a larger number of patients with condylar process fractures are needed to verify the results obtained with each treatment in order to achieve reliable results that can lend confidence to the choice of treatment.
References
Montovani JC, Campos LMP, Gomes MA, Moraes VRC, Ferreira FD, Nogueira EA (2006) Etiology and incidence facial fractures in adults and children: experience in 513 cases. Rev Bras Otorrinolaringol 72:235–241
Biglioli F, Colletti G (2008) Mini-retromandibular approach to condylar fractures. J Cranio-Maxillofac Surg 38(7):378–383
Andrade Filho EF, Martins DMFS, Neto MS, Toledo Junior CS, Pereira MD, Ferreira LM (2003) Fractures of the mandibular condyle: retrospective analysis of clinical indications and treatment. Rev Assoc Med Bras 49(1):54–59
Choi K-Y, Yang J-D, Chung H-Y, Cho B-C (2012) Current concepts in the mandibular condyle fracture management part II: open reduction versus closed reduction. Arch Plast Surg 39:301–308
Landes CA, Lipphardt R (2005) Prospective evaluation of a pragmatic treatment rationale: open reduction and internal fixation of displaced and dislocated condyle and condylar head fractures and closed reduction of non-displaced, non-dislocated fractures Part I: condyle and subcondylar fractures. Int J Oral Maxillofac Surg 34(8):859–870
Vesnaver A, Ahcan U, Rozman J (2012) Evaluation of surgical treatment in mandibular condyle fractures. J Craniomaxillofac Surg 40:647–653
Ellis E III, Throckmorton GS, Palmieri C (2000) Open treatment of condylar process fractures: assessment of adequacy of repositioning and maintenance of stability. J Oral Maxillofac Surg 58(1):27–34
Worsaae N, Thorn JJ (1994) Surgical versus nonsurgical treatment of unilateral dislocated low subcondylar fractures: a clinical study of 52 cases. J Oral Maxillofac Surg 52:353–360
Ellis E III, McFadden D, Simon P, Throckmorton G (2000) Surgical complications with open treatment of mandibular condylar process fractures. J Oral Maxillofac Surg 58:950–958
Yang W-G, Chen C-T, Tsay P-K, Chen Y-R (2002) Functional results of unilateral mandibular condylar process fractures after open and closed treatment. J Trauma 52:498–503
Gupta M, Iyer N, Das D, Nagaraj J (2012) Analysis of different treatment protocols for fractures of condylar process of mandible. J Oral Maxillofac Surg 70:83–91
Palmieri C, Ellis E III, Throckmorton G (1999) Mandibular motion after closed and open treatment of unilateral mandibular condylar process fractures. J Oral Maxiliofac Surg 57:764–775
Ellis E III, Throckmorton GS (2005) Treatment of mandibular condylar process fractures: biological considerations. J Oral Maxillofac Surg 63:115–134
Sforza C, Ugolini A, Sozzi D, Galante D, Mapelli A, Bozzetti A (2011) Three-dimensional mandibular motion after closed and open reduction of unilateral mandibular condylar process fractures. J Craniomaxillofac Surg 39:249–255
Throckmorton G, Ellis E III (2000) Recovery of mandibular motion after closed and open treatment of unilateral mandibular condylar process fractures. Int J Oral Maxillofac Surg 29:421–427
Mapelli A, Galante D, Lovecchio N, Sforza C, Ferrario VF (2009) Translation and rotation movements of the mandible during mouth opening and closing. Clin Anat 22(3):311–318
Stiesch-Scholz M, Schmidt S, Eckardt A (2005) Condylar motion after open and closed treatment of mandibular condylar fractures. J Oral Maxillofac Surg 63(9):1304–1309
Silvennoinen U, Iizuka T, Oikarinen K, Lindqvist C (1994) Analysis of possible factors leading to problems after nonsurgical treatment of condylar fractures. J Oral Maxillofac Surg 53:793–799
Wilkes C (1989) Internal derangements of the temporomandibular joint. Pathological variations. Arch Otolaryngol Head Neck Surg 115:469–477
Bindra S, Choudhary K, Sharma P, Sheorain A, Sharma CB (2010) Management of mandibular sub condylar and condylar fractures using retromandibular approach and assessment of associated surgical complications. J Maxillofac Oral Surg 9(4):355–362
Jinghede A (2013) A retrospective follow-up study on condylar mandibular fractures and post treatment complications in conservatively treated patients during a 12 years period. 44p Dissertation, Karolinska Institut Odontologi https://slidex.tips/download/anna-jinghede-stockholm-2013-nr-160-institutionen-fr-odontologi. Accessed 10 Feb 2018
Wänman A, Agerberg G (1990) Temporomandibular joint sounds in adolescents: a longitudinal study. Oral Surg Oral Med Oral Pathol 69:2–9
Eckelt U, Schneider M, Erasmus F, Gerlach KL, Kuhlisch E, Loukota R, Rasse M, Schubert J, Terheyden H (2006) Open versus closed treatment of fractures of the mandibular condylar process – a prospective randomized multi-centre study. J Cranio-Maxillofac Surg 34:306–314
Sim I (1997) Trial banks: an informatics foundation for evidence-based medicine Stanford University. 246 p Dissertation, Stanford University http://infolab.stanford.edu/pub/cstr/reports/cs/tr/97/1599/CS-TR-97-1599.pdf. Accessed 10 Feb 2018
Ellis E III (2009) Method to determine when open treatment of condylar process fractures is not necessary. J Oral Maxillofac Surg 67:1685–1690
Acknowledgments
The authors are grateful to Dr. Caio Cezar Rebouças e Cerqueira, Oral and Maxillofacial Surgeon from Feira de Santana, Bahia, Brazil, for his valuable advice on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Research Ethics Committee of the Base Hospital of the Federal District, via Plataforma Brasil (www.saude.gov.br/plataformabrasil), under Ethics Approval Certificate number 380 663. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stypulkowski, R.P., Santos, A.G., de Paula e Silva, E. et al. Unilateral mandibular condylar process fractures: a retrospective clinical comparison of open versus closed treatment. Oral Maxillofac Surg 23, 209–214 (2019). https://doi.org/10.1007/s10006-019-00760-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-019-00760-7