Abstract
A meta-analysis was performed to identify the pooled prevalence of mental health disorders (MHDs) among runaway and homeless youth (RHY). Relevant studies published between December 1, 1985, and October 1, 2023, were identified in the PubMed, Scopus, Web of Science, and Cochrane Library databases. A preliminary screening of 11,266 papers resulted in the inclusion of 101 studies. The pooled-prevalence estimates were obtained using a random-effects model. The findings showed varying lifetime prevalence rates of MHDs: 47% (conduct disorders and psychological distress), 43% (depression), 34% (major depressive disorders), 33% (post-traumatic stress disorder), 27% (personality disorders), 25% (attention-deficit/hyperactivity disorder), 23% (bipolar disorders), 22% (anxiety), 21% (oppositional defiant disorders), 15% (anorexia), 15% (adjustment disorders), 14% (dysthymia), 11% (schizophrenia), 9% (obsessive–compulsive disorders), and 8% (gambling disorder). The current prevalence rates were: 31% (depression), 23% (major depressive disorder), 23% (anxiety), 21% (post-traumatic stress disorder), 16% (attention-deficit/hyperactivity disorder), 15% (bipolar disorder), 13% (personality disorders), 13% (oppositional defiant disorders), 8% (schizophrenia), and 6% (obsessive–compulsive disorders). Regular screening and the implementation of evidence-based treatments and the promotion of integration and coordination between mental health services for adolescent minors and young adults with other service systems are recommended.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mental health disorders (MHDs) among runaway and homeless youth (RHY) have become a major public health issue worldwide [1]. RHY refers to individuals aged 12–24 years who either leave their homes without parental or legal guardian consent [2], lack a permanent dwelling, and reside in public spaces, shelters, with unfamiliar individuals, on the streets, with friends, in transitional housing, or other non-domicile settings [3].
The prevalence of RHY has increased in recent years [4]. Moreover, RHY are more likely to report co-occurring disorders, such as MHDs [5,6,7], suicidal behaviors [8] and/or substance abuse [9, 10]. They also are more likely to report risky sexual behaviors [11] and experience trauma disorders [1]. While these findings highlight RHY as one of the most vulnerable populations globally, RHY culture can serve as a substitute for absent parental support, creating significant challenges for healthcare and human services professionals working with this group [1]. Indeed, RHY often exhibit resistance to traditional methods of assistance, including substance use counseling, HIV prevention programs, and psychotherapy [1].
Youth experience homelessness or run away for various reasons. Some are compelled to leave their homes or voluntarily choose to depart due to family conflicts or dysfunction [12]. Homelessness can also result from inadequate discharge planning and a deficiency of support services for youth transitioning from child welfare or juvenile justice systems [13, 14]. Moreover, familial residential instability, familial poverty, and financial hardships significantly impact the lives of many RHY [15, 16].
Two previous meta-analyses have reported the prevalence of MHDs among homeless children (10–26%) [17], or children and adolescents in the child welfare system (4–27%) [18], but neither focused on RHY. As well as being almost a decade old, these studies: (i) only included homeless children (< 18 years) [17] or children and adolescents in the child welfare system (7–17 years) [18]; (ii) only reported the pooled prevalence rate of some specific MHDs (i.e., they did not report the pooled prevalence rate of psychological distress, major depressive disorders, bipolar disorders, personality disorders, adjustment disorders, or schizophrenia); (iii) did not report the lifetime and current pooled prevalence rate of MHDs; (iv) did not compare two groups of RHY (adolescent minors vs. young adults); and (v) did not conduct any subgroup analyses and sensitivity analyses, or meta-regression to detect sources of heterogeneity [17].
To the best of the present authors’ knowledge, there are no previous meta-analyses examining the lifetime and current pooled prevalence rates of a wide range of MHDs among RHY. Consequently, the present study is novel in its aim of estimating the pooled prevalence of MHDs among youth, encompassing both adolescents and young adults. The findings could enhance researchers’ understanding of the pooled prevalence rates of various MHDs, assisting practitioners and policymakers in targeting RHY with suitable interventions, developing adapted psychiatric services, providing professional training, and planning further research.
Methods
Registration and protocol
The present systematic review and meta-analysis was conducted based on Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [19]. The review protocol was registered on PROSPERO (Ref: CRD42023476261).
Search strategy
A thorough search of English-language published papers and abstracts from December 1, 1985, to October 1, 2023, was systematically conducted using the Scopus, PubMed, Web of Science, and Cochrane Library databases. Additionally, a search on Google Scholar was performed to locate any additional relevant studies. The search strategy, employing crucial Boolean operators (AND/OR), was developed and adjusted for diverse databases, utilizing the following initial keywords: “(mental disorders), (psychotic disorders), (mentally ill persons), (homeless youth), (homeless persons), (runaway youth), (adolescent), (young adult), (adult children)”. Furthermore, the bibliographies of the published studies included in the meta-analysis were examined to locate the presence of any additional relevant studies. If multiple studies presented findings on the same sample of RHY, the data providing the most comprehensive details regarding the prevalence of MHDs were used in the analysis. The specifics of the search strategy, encompassing the amalgamation of keywords employed across various electronic databases, are outlined in Table 1.
Study eligibility and exclusion criteria
The eligibility criteria used for inclusion were: (a) RHY aged 12–24 years [2, 3]; (b) reporting original prevalence data on RHYs’ MHDs, and life-time MHDs including ever having a MHD (at least one time) and current MHDs (defined as having MHDs within the past 30 days); and (c) any type of quantitative empirical study (e.g., cross-sectional, cohort, case–control, mixed-methods, and interventions with baseline data). The study excluded qualitative papers, secondary analyses without primary data, systematic reviews, meta-analyses, and unpublished theses (i.e., those not peer-reviewed, such as PhD theses and Master’s theses).
Data extraction process
EndNote X7 software was utilized to eliminate duplicate papers. Subsequently, two authors (BA and JH) independently assessed the titles and abstracts in accordance with the study’s inclusion and exclusion criteria. In instances of disagreement between the two reviewers, resolution was sought from a third author (RM). In the subsequent step, the full texts of the studies were examined based on the criteria for eligibility in the study. Two authors (BA and JH) independently conducted the extraction of data for the studies selected for inclusion in the meta-analysis. The extracted information encompassed details such as the study authors, participants’ age, publication year, country where the data were collected, study design, sample size, population specifics, quality assessment of studies, and criteria for assessing MHDs. Where necessary, the authors of the selected studies were contacted to obtain additional information. The agreement between the two authors was assessed using Cohen’s Kappa statistic. The degree of agreement was categorized into levels such as poor, slight, fair, moderate, substantial, and almost perfect. Corresponding numerical values were assigned as follows: 0, 0.01–0.02, 0.021–0.04, 0.041–0.06, 0.061–0.08, and 0.081–1.00, respectively [20]. Discrepancies between the two authors (comprising less than 10% of the total) were addressed through the intervention of a third author.
Risk of bias of studies
The Newcastle–Ottawa Scale (NOS) [21] was used to evaluate the quality of studies, encompassing three criteria: (i) the selection domain, which includes the representativeness of the exposed group, selection of the non-exposed group, and ascertainment of exposure (three items for cross-sectional studies and four items for cohort studies); (ii) the comparability domain, involving group comparability based on the study design or analysis (one item each for both cross-sectional and cohort studies); and (iii) the exposure/outcome domain, incorporating the assessment of outcome (one item for cross-sectional studies and three items for cohort studies) (Table 2). The studies were classified into four categories: unsatisfactory, satisfactory, good, or very good, with a potential maximum score of 8 for cohort and case–control studies. In assigning scores, studies with a total score of 0–2 were deemed “unsatisfactory,” those with scores of 3–4 were labeled “satisfactory,” 5–6 were considered “good,” and 7–8 were categorized as “very good.” In total, 23 studies received a high-quality rating, 41 were rated as good quality, and 37 were rated as satisfactory quality.
Study selection process
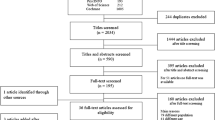
Initially, 11,266 papers were found through the four database searches (Fig. 1). After paper duplicates were excluded (n = 6358), the titles and abstracts of 4,908 papers were screened. Of these, 845 were found to be related to the study’s aim. After a full text review, 744 studies were excluded. The main reasons for exclusion were as follows: 39 studies did not meet the quality appraisal score (5%), and 705 studies utilized a non-quantitative methodology or did not report parametric measurements such as lifetime prevalence of suicidal behaviors, coefficients or odd ratios of relative risks of determinants of study outcomes (95%). Following these exclusions, 101 studies remained for meta-analysis [6, 22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120].
Data synthesis and statistical analysis
The analysis considered the lifetime or current prevalence of conduct disorders, psychological distress, depression, major depressive disorders, post-traumatic stress disorder (PTSD), personality disorders, attention-deficit/hyperactivity disorder (ADHD), bipolar disorders, anxiety, oppositional defiant disorders, anorexia, adjustment disorders, dysthymia, schizophrenia, obsessive–compulsive disorders, and gambling disorder as MHDs. Any reports of overall prevalence without mentioning the specific time period in the studies were considered as lifetime use for the purposes of the meta-analysis. The pooled-prevalence estimates were obtained using a robust random-effects model [121], which considered the various sampling methods employed in the studies. Additionally, the sources of heterogeneity among studies were evaluated through the application of Cochran’s Q and I2 tests. Subgroup analyses were performed to pinpoint the sources of heterogeneity, considering factors such as participants’ age, year of publication, geographical location, quality assessment of studies, diagnosis criteria for MHDs, and sample size. For each subgroup analysis, a minimum of two studies reporting data on the variable of interest was necessary. A sensitivity analysis was performed using Baujat plots to assess the impact of the most significant study on overall heterogeneity and to exclude it during the evaluation of each specific study’s effect on the overall estimate. Ultimately, a multivariate meta-regression analysis was undertaken to investigate the primary source of heterogeneity. Statistical significance was defined as a p-value < 0.05, and the meta-analysis was performed using R 3.5.1 with the “meta” package.
Results
Study characteristics
Of 101 studies selected, 90 were from the America region (n = 123,197 participants), one from the African region (n = 227 participants), five from the European region (n = 541 participants), one from the Western pacific region (n = 187 participants) and four from the South-East Asia region (n = 326 participants). The country with the highest number of included studies was the USA, with 82 studies (n = 122,037) (Table 3). Considering country income level, 96 studies were conducted in high-income countries (n = 123,925), four studies were conducted in a lower-middle-income country (n = 532), and one was conducted in an upper-middle income country (n = 21). The study sample size had a mean of 1232 participants, with 21 being the lowest sample size [56] and 76,596 being the largest sample size [71]. Response rates between the studies varied from 35% to 100%. Participants had a mean age of 18.43 years and were more likely to be male (mean 56%), varying from 0% to 100%. Moreover, 47% had adolescent minors as participants (12–17 years old) and 53% had young adults as participants (18–25 years). Almost all studies were cross-sectional (93%). Finally, 57 studies were published between 2010 and 2023 (56%), 73 studies used a standard scale/questionnaire to determine MHDs (72%), with the Diagnostic and Statistical Manual of Mental Disorders (DSM) being the most prevalent (22%), followed by the Mini International Neuropsychiatry Interview MINI and the Center for Epidemiological Studies-Depression Scale (CES-D) (both 19%).
Pooled prevalence of life-time and current MHDs among RHY
The findings showed that lifetime MHDs most frequently reported by RHY were conduct disorders (47%), psychological distress (47%), depression (43%), major depressive disorders (34%), post-traumatic stress disorder (PTSD) (33%), personality disorders (27%), ADHD (25%), bipolar disorders (23%), anxiety (22%), oppositional defiant disorders (21%), anorexia (15%), adjustment disorders (15%), dysthymia (14%), schizophrenia (11%), obsessive–compulsive disorders (9%), and gambling disorder (8%) (Table 4 and Supplementary Files 1–26). In addition, the data showed that the current MHDs most frequently reported by RHY were depression (31%), major depressive disorder (23%), anxiety (23%), PTSD (21%), ADHD (16%), bipolar disorder (15%), personality disorders (13%), oppositional defiant disorders (13%), schizophrenia (8%), and obsessive–compulsive disorders (6%).
Subgroup analysis
Several subgroup analyses were conducted to determine the primary factor causing heterogeneity in the pooled odds of MHDs (Supplementary Files 27–105). The factors considered included participants’ age, year of study publication, geographical location, quality assessment of studies, diagnostic criteria for MHDs, and sample size. Subgroup analyses detected some source of heterogeneity in some specific MHDs (see next two sections).
Subgroup analyses of pooled prevalence of life-time and current MHDs based on age of participants among RHY
The participants were divided into two groups based on their age, and a subgroup analysis was conducted with those aged: (i) 12–17 years (adolescent minors) and (ii) 18–24 years (young adults) (Table 4 and Supplementary Files 27–41). Results showed that as age increased, the (i) lifetime and current prevalence of depression, bipolar disorder, anxiety and PTSD increased, (ii) lifetime prevalence of schizophrenia and major depressive disorders increased, (iii) lifetime and current prevalence of personality disorders decreased, (iv) lifetime prevalence of ADHD, conduct disorders, and obsessive–compulsive disorders decreased, and (v) current major depressive disorders decreased. The lifetime prevalence of adjustment disorders at these specific ages was stable. The findings also show that externalizing disorders were predominantly prevalent among adolescent minors (except for current major depressive disorders), while internalizing disorders were more prevalent among young adults.
Subgroup analyses of pooled prevalence of life-time and current MHDs based on time of study publication among RHY
The studies were divided into two groups based on the year of publication for each study and a subgroup analysis was conducted by classifying the studies into two different time periods: (i) ≤ 2010 and (ii) > 2010 (Table 4 and Supplementary Files 42–58). This analysis showed several trends: (i) an increase in the lifetime and current prevalence of depression, major depressive disorders, PTSD, and schizophrenia; (ii) an increase in the lifetime prevalence of anxiety, ADHD, personality disorders, conduct disorders, and psychological distress; (iii) an increase in the lifetime prevalence of bipolar disorders; (iv) a decrease in the lifetime prevalence of bipolar disorders, oppositional defiant disorders, and obsessive–compulsive disorders; and (v) no difference in the lifetime prevalence of adjustment disorders over time.
Sensitivity analysis
Sensitivity analysis utilizing Baujat plots was conducted to evaluate influential effects. Effects on the right-hand side of the plots indicate studies with higher levels of heterogeneity (Supplementary Files 106–147). The sensitivity analysis was able to decrease the heterogeneity between studies for lifetime prevalence of anorexia (Cutuli (2018) [83] made the most significant contribution to heterogeneity), dysthymia (Feitel et al. (1992) [88] made the most significant contribution to heterogeneity), gambling disorders (Taylor et al. (2006) [117] made the most significant contribution to heterogeneity), and psychological distress (Narendorf et al. (2020 and 2023) [41, 113] made the most significant contributions to heterogeneity). The test did not detect heterogeneity between studies for other lifetime prevalence of MHDs. The sensitivity analysis reduced the heterogeneity between studies for current prevalence of anxiety and schizophrenia (Middleton et al. (2018] [103] made the most significant contributions to heterogeneity), but was unable to decrease the heterogeneity between studies for other current prevalence of MHDs.
Meta-regression
Multivariate meta-regression analysis was conducted to further investigate the sources of heterogeneity (Table 5). The meta-regression results indicated that the age of participants may contribute to the heterogeneity between the included studies in terms of the lifetime prevalence of depression, conduct disorders, and obsessive–compulsive disorders. Additionally, it was found that the year of study publication may contribute to the heterogeneity between the included studies for (i) the current prevalence of depression and (ii) the lifetime prevalence of anxiety and ADHD. Moreover, diagnostic criteria for MHDs may contribute to the heterogeneity among the included studies on lifetime bipolar and obsessive–compulsive disorders. Finally, the quality assessment of studies may contribute to the heterogeneity among the included studies on the lifetime prevalence of conduct disorders.
Moderator analysis
Subgroup analyses confirmed that (i) age was a statistically significant moderator for current depression, current major depressive disorders, lifetime adjustment disorders, and lifetime obsessive–compulsive disorders; (ii) year of study publication was a statistically significant moderator for current depression, lifetime adjustment disorders, and current schizophrenia; (iii) geographical location was a statistically significant moderator for current anxiety, current bipolar, lifetime bipolar, and lifetime obsessive–compulsive disorders; (iv) the quality assessment of studies was a statistically significant moderator for current major depressive disorders, lifetime obsessive–compulsive disorders, lifetime personality disorders, current PTSD, and lifetime psychological distress; (v) diagnostic criteria for MHDs were statistically significant moderators for lifetime depression, lifetime adjustment disorders, lifetime schizophrenia, lifetime obsessive–compulsive disorders, and lifetime personality disorders; and (vi) sample size was as a statistically significant moderator for current depression and lifetime obsessive–compulsive disorders.
Multivariate meta-regression analysis found that the year of study publication was a statistically significant moderator for the current pooled prevalence of depression. Additionally, the (i) age of participants was a statistically significant moderator for the lifetime pooled prevalence of depression, conduct disorders, and obsessive–compulsive disorders; (ii) year of study publication was a statistically significant moderator for the lifetime prevalence of anxiety and ADHD; (iii) diagnostic criteria for MHDs were statistically significant moderators for the lifetime prevalence of bipolar and obsessive–compulsive disorders; and (iv) quality assessment of studies was a statistically significant moderator for the lifetime prevalence of conduct disorders. Older age (younger adults) was associated with a higher prevalence of depression, while younger age (adolescent minors) was associated with a higher prevalence of conduct and obsessive–compulsive disorders (p < 0.05). Publishing a study after 2010 was associated with a higher prevalence of current depression and lifetime prevalence of anxiety and ADHD (p < 0.05). Diagnostic criteria for MHDs other than DSM and MINI were associated with a higher prevalence of lifetime bipolar and obsessive–compulsive disorders (p < 0.05). Studies of lower quality were associated with a higher prevalence of conduct disorders (p < 0.05).
Discussion
The present meta-analysis estimated the pooled prevalence rates of MHDs among RHY. As far as the present authors are aware, no previous meta-analyses have ever been conducted estimating the pooled prevalence of MHDs among RHY. Findings from the present study indicated that the lifetime pooled prevalence of MHDs among RHY ranged from 8% to 47%, while the current pooled prevalence ranged from 6% to 31%. It was expected that the lifetime pooled prevalence of MHDs among RHY would be higher than the current pooled prevalence rate and this was the case. The prevalence in the present study was higher than the pooled prevalence rate of MHDs in previous meta-analyses among the general population of children and adolescents (13%) [122], homeless children (10–26%) [17], and children and adolescents in the child welfare system (4–27%) [18]. A possible reason for this may be that RHY face several challenges and have multiple health issues [123, 124], leading to a higher rate of MHDs. Additionally, adverse experiences such as maltreatment and serious neglect among RHY [125,126,127] may contribute to an increased prevalence of MHDs among RHY.
Regarding the most common MHDs among RHY, psychological distress and conduct disorders had the highest lifetime pooled prevalence rates (both 47%), while depression had the highest current pooled prevalence rate (31%). These rates are higher than those reported in previous meta-analyses among children and adolescents in the child welfare system or general population of children and adolescents for conduct disorders (6%-20%) [18, 122] and depression (3%–18%) [18, 122]. To the best of the present authors’ knowledge, no previous study has reported the pooled prevalence rate of psychological distress among RHY.
The elevated prevalence of psychological distress among RHY can be attributed to various factors. Firstly, as indicated by prior studies, psychological distress is associated with several adverse behaviors, including substance abuse, conduct problems, and engaging in sexual risk behavior [6, 7, 9,10,11], behaviors that may all be present among RHY. Secondly, this heightened psychological distress might stem from a lack of self-determination within the RHY population [128]. Lastly, the intricate dynamics of loneliness and social support may contribute to this phenomenon [129]. While ‘close’ relationships can offer some degree of support, they simultaneously expose individuals to potential victimization and challenging interactions with other distressed RHY [130].
According to previous studies, RHY are more likely to have conduct disorders than peers who reside in stable housing [25, 77]. Research also indicates that conduct disorder diagnoses are typically feasible until the age of 18 years, with a noticeable decline in prevalence among young adults aged 18 to 25 years [131, 132]. This could be due to the fact that aggression and impulsivity can have negative effects on RHYs’ abilities to reside in housing and shelter systems, reducing access to mental health support and potentially increasing the odds that they will experience homelessness [133]. Another explanation could be the fact that the presence of conduct disorder heightens the likelihood of initiating substance use by the age of 15 years, particularly illicit substances, with this risk persisting until 18 years of age [132]. Moreover, the probability of initiating cocaine, amphetamines, inhalants, and club drugs remains notably elevated up to the age of 21 years [134].
Also, RHY may experience a high level of neighborhood violence, have violent and criminal peers, and be involved with gangs [4]. For everyone, whether housed or not, adolescence may be a challenging period characterized by self-doubt and low self-esteem [123]. RHY may experience various forms of physical and sexual abuse, leading to diminished self-worth [135]. Additionally, facing abuse in the streets, from passers-by or the police, contributes to a reduction in their self-image, potentially leading to increased depression [135].
Examining other MHDs as reported in previous meta-analyses, the prevalence rates were notably higher among RHY. More specifically, 22% had anxiety, 25% had ADHD, 21% exhibited oppositional defiant disorders, and 33% had PTSD, each of these much higher the rates observed among the general population of children and adolescents (6.5% for anxiety, 3.4% for ADHD) [122]. Additionally, the rates in the present study were higher than those found among children and adolescents within the child welfare system (18% for anxiety, 12% for oppositional defiant disorders, 11% for ADHD, and 4% for PTSD) [18].
Another important finding was the increasing prevalence of MHDs over time. However, there is no previous study reporting the prevalence of MHDs among RHY over time. According to a previous meta-analysis, there had been a minor increase of MHDs between the 1980s and the 2000s among the general adolescent population [136]. There have been noticeable indications of parallel trends among the general adolescent population, including a rise in symptoms related to MHDs [137]. Furthermore, there has been an increase in the utilization of health services for the diagnosis and treatment of both psychosomatic health complaints and MHDs in high-income countries [138]. These trends broadly align with the findings from the present review. However, it is important to note that not all findings were equally consistent.
Another novel finding of the present study was that internalizing disorders (e.g., anxiety disorders, depression, PTSD) were more prevalent among young adults, while externalizing disorders (e.g., conduct disorders, ADHD) were more prevalent among adolescent minors. This finding is in line with previous studies with US and Swedish adolescents [139, 140] which reported that there is a trend of increasing internalizing symptoms and decreasing externalizing symptoms among general adolescents. One possible explanation for this finding could be that young adults with MHDs may engage in substance use concurrently [141], experience family conflicts [142] and increased violence [143] and/or have limited access to therapeutic and supportive care in the community [144], leading to an increase in internalizing symptoms among this cohort. Moreover, internalizing symptoms, linked to adverse social and health outcomes in young adults [145], hold clinical significance. Given that these symptoms can progress to psychiatric disorders among a subset of young adults [146], clinicians should be vigilant about the rising prevalence of internalizing symptoms among young adults. Finally, the trend of the rise in internalizing symptoms and the decline in externalizing symptoms suggests a shift more closely associated with the natural evolution of psychiatric disorders rather than homelessness.
Finally, the current meta-analysis identified several sources of heterogeneity between studies through meta-regression and moderator analysis. Similar levels of heterogeneity have been observed in previous meta-analyses conducted within the general adolescent population [122]. Heightened heterogeneity can be influenced by several factors, including country variations, mean age, sample size, year of publication, diagnostic criteria, and the quality assessment of studies. These aspects may contribute to methodological challenges and should be considered in future studies. In the present study, there was a lower estimate of the lifetime pooled prevalence of major depressive disorders and obsessive–compulsive disorders with increasing age. This finding is unexpected, as an inverse relationship was anticipated. This should be examined in future studies. It was also found that studies published after 2010 were associated with a higher prevalence of current depression, as well as lifetime prevalence of anxiety and ADHD. This association could be due to increased numbers of studies carried out post-2010, leading to more comprehensive assessments of MHDs among RHY. There were also variations in the diagnostic criteria which could have led to discrepancies in the prevalence rates, aligning with findings from prior meta-analyses [18, 122]. In an older study examining two prominent nosological systems, the DSM-IV-TR consistently categorized a higher number of children and adolescents as having an anxiety disorder compared to the ICD-10 [147]. Moreover, it was observed that studies of lower quality exhibited a higher prevalence of conduct disorders. This highlights the importance of acknowledging that studies with lower quality may yield elevated prevalence rates compared to those with higher quality data. This consideration should be taken into account in future epidemiological studies.
Limitations
The present meta-analysis has several limitations that should be noted. First, nine-tenths of the studies were carried out in the US and Canada (89%), and the distribution of MHDs was unequally dispersed across the 101 included studies. Therefore, the authors were unable to create a distribution map for each MHD in each country or continent. Second, almost all studies (95%) were conducted in high-income countries, and the findings may not be generalizable to other countries. Third, there was inconsistency in defining MHDs across various studies. For instance, some studies relied on self-reporting rather than adhering to standardized criteria. Fourth, some studies did not specify the duration (whether it was lifetime or current) of MHDs. Fifth, in some studies, the type of MHD was not specified (i.e., they reported MHDs without specifying the particular type of MHD. Therefore, these studies were excluded from the analysis. Sixth, several important pieces of data were not available from studies (e.g., age at the first episode of homelessness or runaway, co-occurring disorders such as substance use, and receiving treatment). Therefore, these trends could not be investigated with these crucial covariates. For example, according to a study from 2005 to 2018, only one-fifth of adolescents received MHD treatment [148], and receiving treatment might affect MHD trends. Finally, excluded from consideration were gray literature sources such as dissertations, research and committee reports, government reports, conference papers, ongoing research, manuscripts, and unpublished studies. The decision to exclude these sources was based on the research team’s inability to adequately assess their quality and the fact that they had not been peer-reviewed.
Conclusion
The present study is the first meta-analysis to estimate the lifetime and current pooled prevalence rate of MHDs among RHY. Several innovative subgroup analyses, such as trends of MHDs over time and comparisons of MHDs among adolescent minors vs. young adults, were conducted. Additionally, to the best of the authors’ knowledge, the present study is the first to perform meta-regression and moderator analysis to detect potential contributing factors to the heterogeneity of studies on the lifetime and current pooled prevalence rate of MHDs among RHY. The findings suggest that RHY had significantly higher prevalence of MHDs compared to other high-risk populations reviewed. Regular screening and the implementation of evidence-based treatments, and the promotion of integration and coordination between mental health services for adolescent minors and young adults with other service systems are recommended.
Based on the present results, externalizing symptoms were observed among adolescent minors, while internalizing symptoms were evident among young adults. Tailoring mental health services based on the type of symptoms and age is crucial, because adolescent minors and young adults may require distinct interventions for internalizing and/or externalizing symptoms. Future research should investigate the causal factors driving the observed difference between internalizing and externalizing symptom trends among adolescent minors and young adults. Moreover, it is imperative to formulate and implement effective brief and low-intensity psychological interventions [149, 150], including cognitive-behavioral therapy [151], for mitigating internalizing disorders among young adults. Additionally, it is recommended to incorporate selective parent training, family support, and school-based programs [152] for addressing and reducing externalizing disorders among adolescent minors.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- ADHD:
-
Attention-deficit/hyperactivity disorder
- MHDs:
-
Mental health disorders
- NOS:
-
Newcastle–Ottawa Scale
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PTSD:
-
Post-traumatic stress disorder
- RHY:
-
Runaway and homeless youth
References
Davies BR, Allen NB (2017) Trauma and homelessness in youth: Psychopathology and intervention. Clin Psychol Rev 54:17–28. https://doi.org/10.1016/j.cpr.2017.03.005
Ennett ST, Bailey SL, Federman EB (1999) Social network characteristics associated with risky behaviors among runaway and homeless youth. J Health Soc Behav 40(1):63–78. https://doi.org/10.2307/2676379
Tyler KA, Schmitz RM (2020) Childhood disadvantage, social and psychological stress, and substance use among homeless youth: a life stress framework. Youth Soc 52(2):272–287. https://doi.org/10.1177/0044118x18767032
Morewitz SJ (2016) Runaway youth at the time of their disappearance. In: Runaway and homeless youth: New research and clinical perspectives. edn. Edited by Morewitz SJ. Cham: Springer International Publishing 1–16
Havlicek J, Garcia A, Smith DC (2013) Mental health and substance use disorders among foster youth transitioning to adulthood: Past research and future directions. Child Youth Serv Rev 35(1):194–203. https://doi.org/10.1016/j.childyouth.2012.10.003
Burke CW, Firmin ES, Lanni S, Ducharme P, DiSalvo M, Wilens TE (2023) Substance use disorders and psychiatric illness among transitional age youth experiencing homelessness. JAACAP Open 1(1):3–11. https://doi.org/10.1016/j.jaacop.2023.01.001
Smith-Grant J, Kilmer G, Brener N, Robin L, Underwood JM (2022) Risk behaviors and experiences among youth experiencing homelessness—youth risk behavior survey, 23 U.S. States and 11 local school districts, 2019. J Commun Health. 47(2):324–333. https://doi.org/10.1007/s10900-021-01056-2
Armoon B, Mohammadi R, Griffiths MD (2024) The global prevalence of non-suicidal self-injury, suicide behaviors, and associated risk factors among runaway and homeless youth: a meta-analysis. Commun Ment Health J 60(5):919–944. https://doi.org/10.1007/s10597-024-01245-y
Armoon B, Griffiths MD, Mohammadi R (2023) The global distribution and epidemiology of psychoactive substance use and injection drug use among street-involved children and youth: a meta-analysis. Subst Use Misuse 58(6):746–764. https://doi.org/10.1080/10826084.2023.2181036
Armoon B, Griffiths MD, Mohammadi R, Ahounbar E (2023) The global distribution and epidemiology of alcohol and drug use among street-involved children and youth: a meta-analysis. Am J Drug Alcohol Abuse 49(4):381–398. https://doi.org/10.1080/00952990.2023.2201872
Heerde JA, Hemphill SA (2016) Sexual risk behaviors, sexual offenses, and sexual victimization among homeless youth: a systematic review of associations with substance use. Trauma Violence Abuse 17(5):468–489. https://doi.org/10.1177/1524838015584371
Morrow QJ, McGuire JK (2023) A qualitative inquiry of associations between family environment and suicidality for transgender youth experiencing homelessness. J Adolesc Res 39(1):196–233. https://doi.org/10.1177/07435584231163191
Castellanos HD (2016) The role of institutional placement, family conflict, and homosexuality in homelessness pathways among Latino LGBT youth in New York City. J Homosex 63(5):601–632. https://doi.org/10.1080/00918369.2015.1111108
Verstraete J, Pannecoucke I, Meeus B, De Decker P (2018) Leaving an Institution in Flanders (Belgium): a road to homelessness? J Soc Serv Res 44(5):665–683. https://doi.org/10.1080/01488376.2018.1479330
Giano Z, Williams A, Hankey C, Merrill R, Lisnic R, Herring A (2020) Forty years of research on predictors of homelessness. Community Ment Health J 56(4):692–709. https://doi.org/10.1007/s10597-019-00530-5
Kamieniecki GW (2001) Prevalence of psychological distress and psychiatric disorders among homeless youth in Australia: a comparative review. Aust N Z J Psychiatry 35(3):352–358. https://doi.org/10.1046/j.1440-1614.2001.00910.x
Bassuk EL, Richard MK, Tsertsvadze A (2015) The prevalence of mental illness in homeless children: a systematic review and meta-analysis. J Am Acad Child Adolesc Psychiatry 54(2):86-96.e82. https://doi.org/10.1016/j.jaac.2014.11.008
Bronsard G, Alessandrini M, Fond G, Loundou A, Auquier P, Tordjman S et al (2016) The prevalence of mental disorders among children and adolescents in the child welfare system: a systematic review and meta-analysis. Medicine 95(7):e2622. https://doi.org/10.1097/md.0000000000002622
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33(1):159–174. https://doi.org/10.2307/2529310
Peterson J, Welch V, Losos M, Tugwell P (2011) The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. In: Ottawa: Ottawa Hospital Research Institute 2:1–12
Cohen E, Mackenzie RG, Yates GL (1991) HEADSS, a psychosocial risk assessment instrument: implications for designing effective intervention programs for runaway youth. J Adolesc Health 12(7):539–544. https://doi.org/10.1016/0197-0070(91)90084-y
Yates GL, MacKenzie R, Pennbridge J, Cohen E (1988) A risk profile comparison of runaway and non-runaway youth. Am J Public Health 78(7):820–821. https://doi.org/10.2105/ajph.78.7.820
Powers JL, Eckenrode J, Jaklitsch B (1990) Maltreatment among runaway and homeless youth. Child Abuse Negl 14(1):87–98. https://doi.org/10.1016/0145-2134(90)90084-7
Whitbeck LB, Chen X, Hoyt DR, Tyler KA, Johnson KD (2004) Mental disorder, subsistence strategies, and victimization among gay, lesbian, and bisexual homeless and runaway adolescents. J Sex Res 41(4):329–342. https://doi.org/10.1080/00224490409552240
Solorio MR, Rosenthal D, Milburn NG, Weiss RE, Batterham PJ, Gandara M et al (2008) Predictors of sexual risk behaviors among newly homeless youth: a longitudinal study. J Adolesc Health 42(4):401–409. https://doi.org/10.1016/j.jadohealth.2007.09.023
Tucker JS, D’Amico EJ, Pedersen ER, Garvey R, Rodriguez A, Klein DJ (2020) Behavioral health and service usage during the COVID-19 pandemic among emerging adults currently or recently experiencing homelessness. J Adolesc Health 67(4):603–605. https://doi.org/10.1016/j.jadohealth.2020.07.013
Doré-Gauthier V, Côté H, Jutras-Aswad D, Ouellet-Plamondon C, Abdel-Baki A (2019) How to help homeless youth suffering from first episode psychosis and substance use disorders? The creation of a new intensive outreach intervention team. Psychiatry Res 273:603–612. https://doi.org/10.1016/j.psychres.2019.01.076
Robert M, Pauzé R, Fournier L (2005) Factors associated with homelessness of adolescents under supervision of the youth protection system. J Adolesc 28(2):215–230. https://doi.org/10.1016/j.adolescence.2005.02.004
Gwadz MV, Nish D, Leonard NR, Strauss SM (2007) Gender differences in traumatic events and rates of post-traumatic stress disorder among homeless youth. J Adolesc 30(1):117–129. https://doi.org/10.1016/j.adolescence.2006.01.004
Gwadz MV, Gostnell K, Smolenski C, Willis B, Nish D, Nolan TC et al (2009) The initiation of homeless youth into the street economy. J Adolesc 32(2):357–377. https://doi.org/10.1016/j.adolescence.2008.01.004
Petering R (2016) Sexual risk, substance use, mental health, and trauma experiences of gang-involved homeless youth. J Adolesc 48:73–81. https://doi.org/10.1016/j.adolescence.2016.01.009
Bender K, Ferguson K, Thompson S, Langenderfer L (2014) Mental health correlates of victimization classes among homeless youth. Child Abuse Negl 38(10):1628–1635. https://doi.org/10.1016/j.chiabu.2014.03.001
Bounds DT, Edinburgh LD, Fogg LF, Saeywc EM (2019) A nurse practitioner-led intervention for runaway adolescents who have been sexually assaulted or sexually exploited: effects on trauma symptoms, suicidality, and self-injury. Child Abuse Negl 90:99–107. https://doi.org/10.1016/j.chiabu.2019.01.023
Ryan KD, Kilmer RP, Cauce AM, Watanabe H, Hoyt DR (2000) Psychological consequences of child maltreatment in homeless adolescents: untangling the unique effects of maltreatment and family environment. Child Abuse Negl 24(3):333–352. https://doi.org/10.1016/s0145-2134(99)00156-8
Thompson S, Jun J, Bender K, Ferguson KM, Pollio DE (2010) Estrangement factors associated with addiction to alcohol and drugs among homeless youth in three U.S. cities. Eval Prog Plann 33(4):418–427. https://doi.org/10.1016/j.evalprogplan.2010.02.002
Courtney ME, Zinn A (2009) Predictors of running away from out-of-home care. Child Youth Serv Rev 31(12):1298–1306. https://doi.org/10.1016/j.childyouth.2009.06.003
Keller TE, Salazar AM, Courtney ME (2010) Prevalence and timing of diagnosable mental health, alcohol, and substance use problems among older adolescents in the child welfare system. Child Youth Serv Rev 32(4):626–634. https://doi.org/10.1016/j.childyouth.2009.12.010
Narendorf SC, Bowen E, Santa Maria D, Thibaudeau E (2018) Risk and resilience among young adults experiencing homelessness: a typology for service planning. Child Youth Serv Rev 86:157–165. https://doi.org/10.1016/j.childyouth.2018.01.034
Crosby SD, Hsu H-T, Jones K, Rice E (2018) Factors that contribute to help-seeking among homeless, trauma-exposed youth: a social-ecological perspective. Child Youth Serv Rev 93:126–134. https://doi.org/10.1016/j.childyouth.2018.07.015
Narendorf SC, Brydon DM, Santa Maria D, Bender K, Ferguson KM, Hsu H-T et al (2020) System involvement among young adults experiencing homelessness: characteristics of four system-involved subgroups and relationship to risk outcomes. Child Youth Serv Rev 108:104609. https://doi.org/10.1016/j.childyouth.2019.104609
Ferguson KM, Bender K, Thompson SJ (2015) Gender, coping strategies, homelessness stressors, and income generation among homeless young adults in three cities. Soc Sci Med 135:47–55. https://doi.org/10.1016/j.socscimed.2015.04.028
Rhoades H, Winetrobe H, Rice E (2014) Prescription drug misuse among homeless youth. Drug Alcohol Depend 138:229–233. https://doi.org/10.1016/j.drugalcdep.2014.02.011
Narendorf SC, Cross MB, Santa Maria D, Swank PR, Bordnick PS (2017) Relations between mental health diagnoses, mental health treatment, and substance use in homeless youth. Drug Alcohol Depend 175:1–8. https://doi.org/10.1016/j.drugalcdep.2017.01.028
DiGuiseppi GT, Davis JP, Christie NC, Rice E (2020) Polysubstance use among youth experiencing homelessness: the role of trauma, mental health, and social network composition. Drug Alcohol Depend 216:108228. https://doi.org/10.1016/j.drugalcdep.2020.108228
Booth RE, Zhang Y (1997) Conduct disorder and HIV risk behaviors among runaway and homeless adolescents. Drug Alcohol Depend 48(2):69–76. https://doi.org/10.1016/s0376-8716(97)00113-0
Bagley SM, Hadland SE, Schoenberger SF, Gai MJ, Topp D, Hallett E et al (2021) Integrating substance use care into primary care for adolescents and young adults: Lessons learned. J Subst Abuse Treat 129:108376. https://doi.org/10.1016/j.jsat.2021.108376
Stewart AJ, Steiman M, Cauce AM, Cochran BN, Whitbeck LB, Hoyt DR (2004) Victimization and posttraumatic stress disorder among homeless adolescents. J Am Acad Child Adolesc Psychiatry 43(3):325–331. https://doi.org/10.1097/00004583-200403000-00015
Embry LE, Vander Stoep AV, Evens C, Ryan KD, Pollock A (2000) Risk factors for homelessness in adolescents released from psychiatric residential treatment. J Am Acad Child Adolesc Psychiatry 39(10):1293–1299. https://doi.org/10.1097/00004583-200010000-00017
Yoder KA (1999) Comparing suicide attempters, suicide ideators, and nonsuicidal homeless and runaway adolescents. Suicide Life Threat Behav 29(1):25–36. https://doi.org/10.1111/j.1943-278X.1999.tb00760.x
Hodgson KJ, Shelton KH, van den Bree MB (2014) Mental health problems in young people with experiences of homelessness and the relationship with health service use: a follow-up study. Evid Based Ment Health 17(3):76–80. https://doi.org/10.1136/eb-2014-101810
Ferguson KM, Bender K, Thompson SJ, Maccio EM, Xie B, Pollio D (2011) Social control correlates of arrest behavior among homeless youth in five U.S. cities. Violence Vict. 26(5):648–668. https://doi.org/10.1891/0886-6708.26.5.648
Fulginiti A, Rice E, Hsu H-T, Rhoades H, Winetrobe H (2016) Risky integration: a social network analysis of network position, exposure, and suicidal ideation among homeless youth. Crisis 37(3):184–193. https://doi.org/10.1027/0227-5910/a000374
Winiarski DA, Rufa AK, Bounds DT, Glover AC, Hill KA, Karnik NS (2020) Assessing and treating complex mental health needs among homeless youth in a shelter-based clinic. BMC Health Serv Res 20(1):109. https://doi.org/10.1186/s12913-020-4953-9
Oppong Asante K, Meyer-Weitz A, Petersen I (2015) Correlates of psychological functioning of homeless youth in Accra, Ghana: A cross-sectional study. Int J Ment Health Syst 9(1):1. https://doi.org/10.1186/1752-4458-9-1
Techakasem P, Kolkijkovin V (2006) Runaway youths and correlating factors, study in Thailand. J Med Assoc Thai. 89(2):212–216
Kurtz PD, Jarvis SV, Kurtz GL (1991) Problems of homeless youths: empirical findings and human services issues. Soc Work 36(4):309–314. https://doi.org/10.1093/sw/36.4.309
Barman-Adhikari A, Craddock J, Bowen E, Das R, Rice E (2017) The relative influence of injunctive and descriptive social norms on methamphetamine, heroin, and injection drug use among homeless youths: The impact of different referent groups. J Drug Issues 48(1):17–35. https://doi.org/10.1177/0022042617726080
Johnson KD, Whitbeck LB, Hoyt DR (2005) Substance abuse disorders among homeless and runaway adolescents. J Drug Issues 35(4):799–816. https://doi.org/10.1177/002204260503500407
Auslander WF, McMillen JC, Elze D, Thompson R, Jonson-Reid M, Stiffman A (2002) Mental health problems and sexual abuse among adolescents in foster care: relationship to HIV risk behaviors and intentions. AIDS Behav 6(4):351–359. https://doi.org/10.1023/A:1021152813774
Sleegers J, Spijker J, van Limbeek J, van Engeland H (1998) Mental health problems among homeless adolescents. Acta Psychiatr Scand 97(4):253–259. https://doi.org/10.1111/j.1600-0447.1998.tb09996.x
Adlaf EM, Zdanowicz YM, Smart RG (1996) Alcohol and other drug use among street-involved youth in Toronto. Addict Res 4(1):11–24. https://doi.org/10.3109/16066359609005559
Nyamathi A, Hudson A, Greengold B, Leake B (2012) Characteristics of homeless youth who use cocaine and methamphetamine. Am J Addict 21(3):243–249. https://doi.org/10.1111/j.1521-0391.2012.00233.x
Unger JB, Kipke MD, Simon TR, Montgomery SB, Johnson CJ (1997) Homeless youths and young adults in Los Angeles: prevalence of mental health problems and the relationship between mental health and substance abuse disorders. Am J Commun Psychol 25(3):371–394. https://doi.org/10.1023/a:1024680727864
Slesnick N, Tonigan JS (2004) Assessment of alcohol and other drug use by runaway youths: a test-retest study of the form 90. Alcohol Treat Q 22(2):21–34. https://doi.org/10.1300/J020v22n02_03
Baer JS, Ginzler JA, Peterson PL (2003) DSM-IV alcohol and substance abuse and dependence in homeless youth. J Stud Alcohol 64(1):5–14. https://doi.org/10.15288/jsa.2003.64.5
Begun S, Bender KA, Brown SM, Barman-Adhikari A, Ferguson K (2016) Social connectedness, self-efficacy, and mental health outcomes among homeless youth: prioritizing approaches to service provision in a time of limited agency resources. Youth Soc 50(7):989–1014. https://doi.org/10.1177/0044118X16650459
Quimby EG, Edidin JP, Ganim Z, Gustafson E, Hunter SJ, Karnik NS (2012) Psychiatric disorders and substance use in homeless youth: A preliminary comparison of San Francisco and Chicago. Behav Sci (Basel) 2(3):186–194. https://doi.org/10.3390/bs2030186
Bender K, Ferguson K, Thompson S, Komlo C, Pollio D (2010) Factors associated with trauma and posttraumatic stress disorder among homeless youth in three U.S. cities: the importance of transience. J Trauma Stress. 23(1):161–168. https://doi.org/10.1002/jts.20501
Dadds MR, Braddock D, Cuers S, Elliott A, Kelly A (1993) Personal and family distress in homeless adolescents. Commun Ment Health J 29(5):413–422. https://doi.org/10.1007/bf00754409
Pottick KJ, Warner LA, Yoder KA (2005) Youths living away from families in the US mental health system: opportunities for targeted intervention. J Behav Health Serv Res 32(3):264–281. https://doi.org/10.1007/bf02291827
Khurana S, Sharma N, Jena S, Saha R, Ingle GK (2004) Mental health status of runaway adolescents. Indian J Pediatr 71(5):405–409. https://doi.org/10.1007/bf02725627
Warheit GJ, Biafora F (1991) Mental health and substance abuse patterns among a sample of homeless post-adolescents. Int J Adolesc Youth 3(1–2):9–27. https://doi.org/10.1080/02673843.1991.9747692
Rohde P, Noell J, Ochs L, Seeley JR (2001) Depression, suicidal ideation and STD-related risk in homeless older adolescents. J Adolesc 24(4):447–460. https://doi.org/10.1006/jado.2001.0382
McCaskill PA, Toro PA, Wolfe SM (1998) Homeless and matched housed adolescents: a comparative study of psychopathology. J Clin Child Psychol 27(3):306–319. https://doi.org/10.1207/s15374424jccp2703_7
Bhat DP, Singh M, Meena GS (2012) Screening for abuse and mental health problems among illiterate runaway adolescents in an Indian metropolis. Arch Dis Child 97(11):947–951. https://doi.org/10.1136/archdischild-2011-301603
Busen NH, Engebretson JC (2008) Facilitating risk reduction among homeless and street-involved youth. J Am Acad Nurse Pract 20(11):567–575. https://doi.org/10.1111/j.1745-7599.2008.00358.x
Cauce AM, Paradise M, Ginzler JA, Embry L, Morgan CJ, Lohr Y et al (2000) The characteristics and mental health of homeless adolescents: age and gender differences. J Emot Behav Disord 8(4):230–239. https://doi.org/10.1177/106342660000800403
Saddichha S, Linden I, Krausz MR (2014) Physical and mental health issues among homeless youth in British Columbia, Canada: are they different from older homeless adults? J Can Acad Child Adolesc Psychiatry. 23(3):200–206
Chen X, Thrane L, Whitbeck LB, Johnson K (2006) Mental disorders, comorbidity, and postrunaway arrests among homeless and runaway adolescents. J Res Adolesc 16(3):379–402. https://doi.org/10.1111/j.1532-7795.2006.00499.x
Labelle R, Berthiaume C, Daigle M, Breton J-J, Houle J (2020) Mental health, suicidal behaviour, and primary healthcare among homeless youth. Can J Commun Ment Health 39(4):25–38. https://doi.org/10.7870/cjcmh-2020-029
Crawford DM, Trotter EC, Hartshorn KJ, Whitbeck LB (2011) Pregnancy and mental health of young homeless women. Am J Orthopsychiatry 81(2):173–183. https://doi.org/10.1111/j.1939-0025.2011.01086.x
Cutuli JJ (2018) Homelessness in high school: Population-representative rates of self-reported homelessness, resilience, and risk in philadelphia. Soc Work Res 42(3):159–168. https://doi.org/10.1093/swr/svy013
Ko M, Hong M, Kim Y-E, Ha J, Lee SM, Kim H-S (2016) Depression, attachment and addiction problems in runaway youths. J Korean Acad Child Adolesc Psychiatry 27(3):181–187. https://doi.org/10.5765/jkacap.2016.27.3.181
Gupta R, Nehra DK, Kumar V, Sharma P, Kumar P (2013) Psychiatric illnesses in homeless (runaway or throwaway) girl inmates: a preliminary study. Dysphrenia. 4(1):31–35
Slesnick N, Prestopnik J (2005) Dual and multiple diagnosis among substance using runaway youth. Am J Drug Alcohol Abuse 31(1):179–201. https://doi.org/10.1081/ada-200047916
Winetrobe H, Rice E, Rhoades H, Milburn N (2016) Health insurance coverage and healthcare utilization among homeless young adults in Venice. CA J Public Health (Oxf) 38(1):147–155. https://doi.org/10.1093/pubmed/fdv001
Feitel B, Margetson N, Chamas J, Lipman C (1992) Psychosocial background and behavioral and emotional disorders of homeless and runaway youth. Hosp Commun Psychiatry 43(2):155–159. https://doi.org/10.1176/ps.43.2.155
Santa Maria D, Daundasekara SS, Hernandez DC, Zhang W, Narendorf SC (2020) Sexual risk classes among youth experiencing homelessness: relation to childhood adversities, current mental symptoms, substance use, and HIV testing. PLoS One 15(1):e0227331. https://doi.org/10.1371/journal.pone.0227331
Whitbeck LB, Hoyt DR, Johnson KD, Chen X (2007) Victimization and posttraumatic stress disorder among runaway and homeless adolescents. Violence Vict 22(6):721–734. https://doi.org/10.1891/088667007782793165
Harris T, Rice E, Rhoades H, Winetrobe H, Wenzel S (2017) Gender differences in the path from sexual victimization to HIV risk behavior among homeless youth. J Child Sex Abus 26(3):334–351. https://doi.org/10.1080/10538712.2017.1287146
Pedersen ER, Tucker JS, Klein DJ, Parast L (2018) Perceived need and receipt of behavioral health services at drop-in centers among homeless youth. Health Serv Res 53(6):4609–4628. https://doi.org/10.1111/1475-6773.12990
Hodgson KJ, Shelton KH, van den Bree MB (2015) Psychopathology among young homeless people: longitudinal mental health outcomes for different subgroups. Br J Clin Psychol 54(3):307–325. https://doi.org/10.1111/bjc.12075
Hogan KA, Roe-Sepowitz D (2023) LGBTQ+ homeless young adults and sex trafficking vulnerability. J Hum Traffick 9(1):63–78. https://doi.org/10.1080/23322705.2020.1841985
Craig TK, Hodson S (1998) Homeless youth in London: I. Childhood antecedents and psychiatric disorder. Psychol Med. 28(6):1379–1388. https://doi.org/10.1017/s0033291798007351
Toro PA, Tulloch E, Ouellette N (2008) Stress, social support, and outcomes in two probability samples of homeless adults. J Commun Psychol 36(4):483–498. https://doi.org/10.1002/jcop.20190
Hao J, Beld M, Khoddam-Khorasani L, Flentje A, Kersey E, Mousseau H et al (2021) Comparing substance use and mental health among sexual and gender minority and heterosexual cisgender youth experiencing homelessness. PLoS One 16(3):e0248077. https://doi.org/10.1371/journal.pone.0248077
Jain JP, Santos G-M, Hao J, Leonard A, Miller AM, Cuca YP et al (2022) The syndemic effects of adverse mental health conditions and polysubstance use on being at risk of clinical depression among marginally housed and homeless transitional age youth living in San Francisco, California. PLoS One 17(3):e0265397. https://doi.org/10.1371/journal.pone.0265397
Kirst M, Frederick T, Erickson PG (2011) Concurrent mental health and substance use problems among street-involved youth. Int J Ment Health Addict 9(5):543–553. https://doi.org/10.1007/s11469-011-9328-3
Kozloff N, Adair CE, Palma Lazgare LI, Poremski D, Cheung AH, Sandu R et al (2016) “Housing First” for homeless youth with mental illness. Pediatrics. https://doi.org/10.1542/peds.2016-1514
Merscham C, Van Leeuwen JM, McGuire M (2009) Mental health and substance abuse indicators among homeless youth in Denver, Colorado. Child Welfare 88(2):93–110
Dunn SB, Orchard TS, Andridge R, Rymut SM, Slesnick N, Hatsu IE (2023) Mental health in society’s margins: Poor n-3 PUFA intake and psychological well-being of homeless youth. Br J Nutr. https://doi.org/10.1017/s000711452300212x
Middleton JS, Gattis MN, Frey LM, Roe-Sepowitz D (2018) Youth experiences survey (YES): exploring the scope and complexity of sex trafficking in a sample of youth experiencing homelessness. J Soc Serv Res 44(2):141–157. https://doi.org/10.1080/01488376.2018.1428924
Moore H, Benbenishty R, Astor RA, Rice E (2018) The positive role of school climate on school victimization, depression, and suicidal ideation among school-attending homeless youth. J Sch Violence 17(3):298–310. https://doi.org/10.1080/15388220.2017.1322518
Castro AL, Gustafson EL, Ford AE, Edidin JP, Smith DL, Hunter SJ et al (2014) Psychiatric disorders, high-risk behaviors, and chronicity of episodes among predominantly African American homeless Chicago youth. J Health Care Poor Underserved 25(3):1201–1216. https://doi.org/10.1353/hpu.2014.0124
Gewirtz O’Brien JR, Edinburgh LD, Barnes AJ, McRee AL (2020) Mental health outcomes among homeless, runaway, and stably housed youth. Pediatrics. https://doi.org/10.1542/peds.2019-2674
Kushel MB, Yen IH, Gee L, Courtney ME (2007) Homelessness and health care access after emancipation: results from the Midwest evaluation of adult functioning of former foster youth. Arch Pediatr Adolesc Med 161(10):986–993. https://doi.org/10.1001/archpedi.161.10.986
Prock KA, Kennedy AC (2020) Characteristics, experiences, and service utilization patterns of homeless youth in a transitional living program: differences by LGBQ identity. Child Youth Serv Rev 116:105176. https://doi.org/10.1016/j.childyouth.2020.105176
Ferguson KM, Xie B, Glynn S (2012) Adapting the individual placement and support model with homeless young adults. Child Youth Care Forum 41(3):277–294. https://doi.org/10.1007/s10566-011-9163-5
Rhoades H, Winetrobe H, Rice E (2015) Pet ownership among homeless youth: associations with mental health, service utilization and housing status. Child Psychiatry Hum Dev 46(2):237–244. https://doi.org/10.1007/s10578-014-0463-5
Petering R, Rhoades H, Winetrobe H, Dent D, Rice E (2017) Violence, trauma, mental health, and substance use among homeless youth Juggalos. Child Psychiatry Hum Dev 48(4):642–650. https://doi.org/10.1007/s10578-016-0689-5
Brown SM, Begun S, Bender K, Ferguson KM, Thompson SJ (2015) An exploratory factor analysis of coping styles and relationship to depression among a sample of homeless youth. Community Ment Health J 51(7):818–827. https://doi.org/10.1007/s10597-015-9870-8
Narendorf SC, Arora A, Santa Maria D, Bender K, Shelton J, Hsu HT et al (2023) Self-identification of mental health problems among young adults experiencing homelessness. Community Ment Health J 59(5):844–854. https://doi.org/10.1007/s10597-022-01068-9
Solorio MR, Milburn NG, Andersen RM, Trifskin S, Rodríguez MA (2006) Emotional distress and mental health service use among urban homeless adolescents. J Behav Health Serv Res 33(4):381–393. https://doi.org/10.1007/s11414-006-9037-z
Saperstein AM, Lee S, Ronan EJ, Seeman RS, Medalia A (2014) Cognitive deficit and mental health in homeless transition-age youth. Pediatrics 134(1):e138-145. https://doi.org/10.1542/peds.2013-4302
Siconolfi D, Tucker JS, Shadel WG, Seelam R, Golinelli D (2020) Health, homelessness severity, and substance use among sexual minority youth experiencing homelessness: a comparison of bisexual versus gay and lesbian youth. J Sex Res 57(7):933–942. https://doi.org/10.1080/00224499.2019.1695723
Taylor H, Stuttaford M, Broad B, Vostanis P (2006) Why a “roof” is not enough: the characteristics of young homeless people referred to a designated mental health service. J Ment Health 15(4):491–501. https://doi.org/10.1080/09638230600801504
Thornton T, Goldstein A, Tonmyr L, Werkele C, Erickson P (2012) Homelessness and child welfare involvement: risks for co-occurring mental health symptoms and substance use? Int J Ment Health Promot 14(4):237–250. https://doi.org/10.1080/14623730.2013.771460
Tyler KA, Olson K, Ray CM (2019) Understanding daily depression, drinking, and marijuana use among homeless youth using short message service surveying. J Child Adolesc Subst Abuse 28(3):170–179. https://doi.org/10.1080/1067828x.2019.1667286
Yates GL, Mackenzie RG, Pennbridge J, Swofford A (1991) A risk profile comparison of homeless youth involved in prostitution and homeless youth not involved. J Adolesc Health 12(7):545–548. https://doi.org/10.1016/0197-0070(91)90085-z
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188. https://doi.org/10.1016/0197-2456(86)90046-2
Polanczyk GV, Salum GA, Sugaya LS, Caye A, Rohde LA (2015) Annual research review: a meta-analysis of the worldwide prevalence of mental disorders in children and adolescents. J Child Psychol Psychiatry 56(3):345–365. https://doi.org/10.1111/jcpp.12381
Kulik DM, Gaetz S, Crowe C, Ford-Jones EL (2011) Homeless youth’s overwhelming health burden: a review of the literature. Paediatr Child Health 16(6):e43-47. https://doi.org/10.1093/pch/16.6.e43
Lim C, Rice E, Rhoades H (2016) Depressive symptoms and their association with adverse environmental factors and substance use in runaway and homeless youths. J Res Adolesc 26(3):403–417. https://doi.org/10.1111/jora.12200
Yoshioka-Maxwell A (2023) Experiences of abuse: Homeless former foster youth and their experiences of abuse in out-of-home care. Child Adolesc Social Work J 40(6):787–796. https://doi.org/10.1007/s10560-021-00810-8
Tyler KA, Schmitz RM (2018) Child abuse, mental health and sleeping arrangements among homeless youth: links to physical and sexual street victimization. Child Youth Serv Rev 95:327–333. https://doi.org/10.1016/j.childyouth.2018.11.018
Tyler KA, Ray CM (2019) A latent class analysis of lifetime victimization among homeless youth. J Interpers Violence 36(15–16):7202–7222. https://doi.org/10.1177/0886260519834090
Julien EG, Senécal C, Poitras S (2009) Subjective psychological distress among young adults: the role of global and contextual levels of selfdetermined behavior. Hellenic J Psychol 6:145–168
Cleverley K, Kidd SA (2011) Resilience and suicidality among homeless youth. J Adolesc 34(5):1049–1054. https://doi.org/10.1016/j.adolescence.2010.11.003
Perron JL, Cleverley K, Kidd SA (2014) Resilience, loneliness, and psychological distress among homeless youth. Arch Psychiatr Nurs 28(4):226–229. https://doi.org/10.1016/j.apnu.2014.05.004
Bachmann CJ, Scholle O, Bliddal M, dosReis S, Odsbu I, Skurtveit S et al (2024) Recognition and management of children and adolescents with conduct disorder: a real-world data study from four western countries. Child Adolesc Psychiatry Ment Health 18(1):18. https://doi.org/10.1186/s13034-024-00710-6
Masroor A, Patel RS, Bhimanadham NN, Raveendran S, Ahmad N, Queeneth U et al (2019) Conduct disorder-related hospitalization and substance use disorders in American teens. Behav Sci 9(7):73. https://doi.org/10.3390/bs9070073
Winiarski DA, Glover AC, Bounds DT, Karnik NS (2021) Addressing intersecting social and mental health needs among transition-age homeless youths: a review of the literature. Psychiatr Serv 72(3):317–324. https://doi.org/10.1176/appi.ps.201900498
Hopfer C, Salomonsen-Sautel S, Mikulich-Gilbertson S, Min S-J, McQueen M, Crowley T et al (2013) Conduct disorder and initiation of substance use: a prospective longitudinal study. J Am Acad Child Adolesc Psychiatry 52(5):511-518.e514. https://doi.org/10.1016/j.jaac.2013.02.014
Boivin JF, Roy E, Haley N, Galbaud du Fort G (2005) The health of street youth: a Canadian perspective. Can J Public Health 96(6):432–437. https://doi.org/10.1007/bf03405183
Potrebny T, Wiium N, Lundegård MM-I (2017) Temporal trends in adolescents’ self-reported psychosomatic health complaints from 1980–2016: a systematic review and meta-analysis. PLoS One. 12(11):e0188374. https://doi.org/10.1371/journal.pone.0188374
Bor W, Dean AJ, Najman J, Hayatbakhsh R (2014) Are child and adolescent mental health problems increasing in the 21st century? A systematic review. Aust N Z J Psychiatry 48(7):606–616. https://doi.org/10.1177/0004867414533834
Collishaw S (2015) Annual research review: secular trends in child and adolescent mental health. J Child Psychol Psychiatry 56(3):370–393. https://doi.org/10.1111/jcpp.12372
Askari MS, Rutherford CG, Mauro PM, Kreski NT, Keyes KM (2022) Structure and trends of externalizing and internalizing psychiatric symptoms and gender differences among adolescents in the US from 1991 to 2018. Soc Psychiatry Psychiatr Epidemiol 57(4):737–748. https://doi.org/10.1007/s00127-021-02189-4
Blomqvist I, Henje Blom E, Hägglöf B, Hammarström A (2019) Increase of internalized mental health symptoms among adolescents during the last three decades. Eur J Public Health 29(5):925–931. https://doi.org/10.1093/eurpub/ckz028
Winstanley EL, Steinwachs DM, Stitzer ML, Fishman MJ (2012) Adolescent substance abuse and mental health: Problem co-occurrence and access to services. J Child Adolesc Subst Abuse 21(4):310–322. https://doi.org/10.1080/1067828x.2012.709453
Herrenkohl TI, Kosterman R, Hawkins JD, Mason WA (2009) Effects of growth in family conflict in adolescence on adult depressive symptoms: mediating and moderating effects of stress and school bonding. J Adolesc Health 44(2):146–152. https://doi.org/10.1016/j.jadohealth.2008.07.005
Copeland-Linder N, Lambert SF, Ialongo NS (2010) Community violence, protective factors, and adolescent mental health: a profile analysis. J Clin Child Adolesc Psychol 39(2):176–186. https://doi.org/10.1080/15374410903532601
Gulliver A, Griffiths KM, Christensen H (2010) Perceived barriers and facilitators to mental health help-seeking in young people: a systematic review. BMC Psychiatry 10:113. https://doi.org/10.1186/1471-244x-10-113
Rapee RM, Oar EL, Johnco CJ, Forbes MK, Fardouly J, Magson NR et al (2019) Adolescent development and risk for the onset of social-emotional disorders: a review and conceptual model. Behav Res Ther 123:103501. https://doi.org/10.1016/j.brat.2019.103501
Nivard MG, Lubke GH, Dolan CV, Evans DM, St Pourcain B, Munafò MR et al (2017) Joint developmental trajectories of internalizing and externalizing disorders between childhood and adolescence. Dev Psychopathol 29(3):919–928. https://doi.org/10.1017/s0954579416000572
Adornetto C, Suppiger A, In-Albon T, Neuschwander M, Schneider S (2012) Concordances and discrepancies between ICD-10 and DSM-IV criteria for anxiety disorders in childhood and adolescence. Child Adolesc Psychiatry Ment Health 6(1):40. https://doi.org/10.1186/1753-2000-6-40
Mojtabai R, Olfson M (2020) National trends in mental health care for US adolescents. JAMA Psychiat 77(7):703–714. https://doi.org/10.1001/jamapsychiatry.2020.0279
McDanal R, Parisi D, Opara I, Schleider JL (2022) Effects of brief interventions on internalizing symptoms and substance use in youth: a systematic review. Clin Child Fam Psychol Rev 25(2):339–355. https://doi.org/10.1007/s10567-021-00372-2
Roach A, Cullinan S, Shafran R, Heyman I, Bennett S (2023) Implementing brief and low-intensity psychological interventions for children and young people with internalizing disorders: a rapid realist review. Br Med Bull 145(1):120–131. https://doi.org/10.1093/bmb/ldad001
Wergeland GJH, Riise EN, Öst LG (2021) Cognitive behavior therapy for internalizing disorders in children and adolescents in routine clinical care: a systematic review and meta-analysis. Clin Psychol Rev 83:101918. https://doi.org/10.1016/j.cpr.2020.101918
Smedler AC, Hjern A, Wiklund S, Anttila S, Pettersson A (2015) Programs for prevention of externalizing problems in children: limited evidence for effect beyond 6 months post intervention. Child Youth Care Forum 44:251–276. https://doi.org/10.1007/s10566-014-9281-y
Acknowledgements
None.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or non-for-profit sectors.
Author information
Authors and Affiliations
Contributions
BA. Conceived the study BA. Collected all data. RM, and BA analyzed and interpreted the data. BA, JH and AGHP drafted the manuscript. BA, AL and MDG revised the first draft, and MDG was responsible for all final editing. All authors commented on the drafts of the manuscript and approved the final copy of the paper for submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests. MDG has received research funding fromNorsk Tipping(the gambling operator owned by the Norwegian government). MDG has received funding for a number of research projects in the area of gambling education for young people, social responsibility in gambling and gambling treatment fromGambleAware (formerly the Responsibility in Gambling Trust), a charitable body which funds its research program based on donations from the gambling industry. MDG undertakes consultancy for various gambling companies in the area of player protection and social responsibility in gambling.
Ethics approval and consent to participate
The present study was an analysis of preexisting literature and did not use human participants.
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Armoon, B., Ghadipasha, A., Mohammadi, R. et al. The global prevalence of mental health disorders among runaway and homeless youth: A meta-analysis. Eur Child Adolesc Psychiatry (2024). https://doi.org/10.1007/s00787-024-02519-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00787-024-02519-2