Abstract
Objectives
In this clinical study, the 8-year clinical performances of a flowable resin composite was compared with that of a conventional resin composite.
Materials and methods
Ninety non-carious cervical lesions (NCCLs) in 19 participants were involved in this trial. NCCLs were restored with a flowable composite (Clearfil Flow FX: FX, Kuraray Noritake, Japan) or a conventional resin composite (Clearfil AP-X: AP) in conjunction with a one-step self-etch adhesive (Clearfil S3 Bond). Each participant had both types of resin composite restorations that were randomly allocated. The restorations were evaluated at baseline and annually up to 8 years using modified USPHS criteria. The data were statistically analyzed using the Fisher’s exact test, Kaplan–Meier method, and a multivariate Cox-regression with frailty models (p < 0.05).
Results
The 8-year participant recall rate was 95%. One hundred percent retention was recorded for AP, whereas four out of 46 restorations were lost for FX during the 8 years. The incidence of marginal staining increased over time regardless of the type of resin composite, showing 48% for AP and 57% for FX after 8 years. Wear of the resin composite occurred only for the flowable material and there was a significant difference between the types of resin composite (p = 0.024). Overall survival rates at 8 years for AP and FX were 98% and 82% respectively (p = 0.110).
Conclusions
The flowable resin composite presented lower wear resistance and showed a lower survival rate compared with the conventional composite after eight years of clinical service.
Clinical relevance
Flowable resin composites may show greater wear after long-term clinical service.
Trial registration number: UMIN000028745, Date of registration: August 19, 2017.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A non-carious cervical lesion (NCCL) is a non-carious hard tissue defect at the cementoenamel junction of teeth [1]. Many studies have shown that the prevalence and incidence of NCCLs increase with age [1, 2]. Elderly populations with many retained teeth are increasing; therefore, the opportunity for management or treatment of NCCLs will likely increase. The restoration of a NCCL is often considered a challenging procedure since its major part is composed of dentin, no retention form is present and the cervical dentin or cementum margin is usually located subgingivally [3, 4]. Although no definitive conclusion can be found in the literature, it has been stated that NCCLs suspected of being caused primarily by abfraction should be restored with a microfilled resin composite or a flowable resin that has a low modulus of elasticity because these will flex with the tooth and not compromise retention [4,5,6].
Early flowable resin composites in the late 1990s were created by retaining the same filler particle sizes of conventional resin composites but just reducing the filler content by 20 to 25 wt% [7]. Therefore, there have been concerns about poor mechanical properties and wear resistance of flowable composites due to their lower filler contents [8,9,10]. Mechanical properties depend not only on the size and amount of filler but also on the composition of the resin matrix and on the silane coupling agent [11, 12]. Continuous efforts have continued to develop a new product and to improve mechanical and handling properties of resin composites [12,13,14,15]. Several laboratory studies have reported that recent flowable resin composites have shown wear resistance comparable to conventional resin composites [16,17,18].
Our laboratory study revealed that flowable resin composites in NCCLs bonded with self-etch adhesive systems did not show any deterioration of marginal sealing under flexural load cycling, whereas they showed more microleakage than a conventional hybrid resin composite under thermocycling [19]. These overall findings may raise a concern about the marginal sealing ability of relatively large NCCLs if they are restored with flowable resin composites in conjunction with self-etch systems. Only a well-controlled clinical trial can provide the ultimate proof of clinical effectiveness. Therefore, a randomized controlled clinical trial (RCT) was conducted to evaluate the effectiveness of a flowable resin composite as a filling restorative material [20]. Both types of resin composite demonstrated an acceptable clinical performance after 3 years of clinical service, and there were no significant differences in the clinical performances between them. These findings have been supported by other clinical trials [21,22,23,24,25]. Three years is a relatively short time period to determine the durability and clinical effectiveness of a flowable resin composite in cervical restorations [20, 23, 25]. Unfortunately, however, more long-term clinical trials on flowable resin composites are very limited.
The aim of this study was to compare the 8-year clinical performance of two types of resin composite in NCCLs. The null hypothesis tested was that there is no significant difference in eight-year clinical performance between the two types of resin composite.
Materials and methods
Study design and setting
The protocol of this clinical trial was designed referring to the ADA guidelines and initiated as a randomized controlled trial in 2005 [26]. The clinical trial protocol was approved by the Ethics Committee of Nagasaki University School of Dentistry (No. 20). Three-year results were reported in 2010 [20]. After that, the participants continued to be seen regularly (at least twice a year), and the restorations were also followed up annually. In order to report a more long-term clinical performance, a clinical trial protocol was further submitted to the Ethics Committee of Nagasaki University Hospital and approved as an observational study (17041717) and registered with the University Hospital Medical Information Network (UMIN000028745).
Participant and lesion selection
Participants were recruited from patients who had been regularly attending the Department of Conservative Dentistry, Nagasaki University Hospital. Inclusion criteria were patients with at least one pair of similarly sized NCCLs that were in need for restoration were selected. The depth of NCCLs was less than 2 mm. Reasons for restoration were cervical hypersensitivity, prevention of further tooth loss, and/or esthetic concerns. Exclusion criteria were patients with suffering from severe periodontitis or bruxism. Three patients had to be excluded due to severe periodontitis or bruxism. One patient declined to participate in this trial. As a result, nineteen participants, 10 males and 9 females (mean age: 60.4 years, range: 29–74 years) and a total of 90 NCCLs were included. The purpose and the research protocol, as well as the expected benefits and possible discomfort, were explained to the participants, and written informed consent was obtained from all participants.
Allocation concealment
Each participant received both the test composite (improved flowable resin composite: Clearfil Flow FX, Kuraray Noritake Dental, Tokyo, Japan) and a control resin composite (a conventional resin composite: Clearfil AP-X, Kuraray Noritake Dental). Composition and mechanical properties of these materials are listed in Table 1. All but two participants had three restorations or less for each of the resin composites. Computer-generated random tables created by an independent researcher were used to allocate the resin composites. Just before the restorative procedure began, an assistant who was not involved in this study directly opened the sealed envelope to reveal the allocation corresponding to the lowest quadrant number. The first randomly selected type of resin composite was placed into all NCCLs requiring restorations in the lowest quadrant number (according to the FDI system), and the alternative resin composite was used for the second lowest quadrant number. This method was used for every other quadrant if there was at least one NCCL requiring a restoration. In case of one participant with two lesions which were located in a quadrant, one lesion was restored with Clearfil AP-X (AP), and the other was restored with Clearfil Flow FX (FX). Participants were blinded to group assignment.
Restorative procedures
All restorative procedures were performed by SK. A 1-mm bevel was prepared at the enamel margin using a high-speed, water-cooled, diamond bur. In order to remove the contaminated layer, dentin walls were lightly ground with a slow-speed steel round bur without local anesthesia. No retention grooves were placed. In order to secure contamination-free access to the cavity, the adjacent gingiva was retracted with an unmedicated gingival retraction cord, and the operating field was isolated with cotton rolls and a saliva ejector. The cavities were treated with a one-step self-etch adhesive (Clearfil S3 Bond, Kuraray Noritake Dental) according to the manufacturer’s instructions. S3 Bond was applied to the cavity and left for 20 s. The solvent was evaporated with high pressure air for 10 s which also thinned the adhesive layer. The adhesive was irradiated for 10 s with a conventional halogen light-curing unit (New Light VL-II, GC Corp., Tokyo, Japan). The light intensity output of the curing unit was checked periodically with a radiometer (Curing Radiometer Model 100, Demetron Research Corp., Danbury, CT, USA) to ensure that it exceeded 400 mW/cm2. For AP, the resin composite was placed in a single increment, contoured with a hand instrument, and light-cured for 40 s except for three very large and/or deep lesions which were restored in two increments. For FX, the resin composite was placed in two or three increments except for small and shallow cavities. Each increment was cured for 20 s. The excess composite was trimmed and contoured with an ultrafine diamond bur with water coolant. The restorations were finished with ultrafine diamond points, and polished with slow speed silicone points at a next visit that was usually scheduled within 2 weeks.
Clinical evaluation
Restorations were visually and physically examined with a dental mirror and an explorer, and were evaluated at baseline, 6 months and annually until 8 years by SK using criteria for direct clinical evaluation (Table 2) which were prepared referring to previously published modified USPHS criteria [27, 28]. Recurrence of NCCL was added as a new category. In addition, at each recall visit, participants were asked if they had any complaints such as esthetic dissatisfaction and/or hypersensitivity. These evaluated results and the extent of the observed event: marginal discoloration, crevice, wear and development of NCCL, were recorded by SK on an evaluation sheet (Fig. 1). In view of the need to observe the restorations at future recalls, no attempt was made to remove any visible excess by refurbishing. NCCLs that continued to develop were also followed up to investigate the progression of NCCLs if the participants did not have any complaints. To facilitate the investigation and confirm the clinical evaluation outcomes, color photographs (1:1) were taken at baseline, 6 months, and the annual recall visits (Nikon F3, Medical-Nikkor 120 mm F4, Nikon, Tokyo, Japan and/or Sonictechno ring flash system in conjunction with Canon EOS 60D, Tokyo, Japan) to allow for a later review and reconfirmation. The photographic records also allowed for a time-based comparative evaluation for each restoration across all recall periods.
Before checking SK’s evaluations, three evaluators who were blinded to the group assignment were trained for both intra-evaluator and inter-evaluator reliability, using representative photographs of each score for each criterion. An agreement between the evaluators was necessary to be at least 85%. The first (ET) and second (KK) evaluators rated the restorations by observing the clinical photographs in terms of retention, second caries, marginal discoloration, marginal adaptation, anatomic form, and recurrence of NCCL. The third evaluator (YT) checked the evaluation sheets recorded by SK, against the scores of the two evaluators to determine the final rating.
Statistical analysis
The Fisher's exact test was used at first to avoid multicollinearity. Data were statistically analyzed using JMP 15 software package (SAS Institute Japan, Tokyo, Japan) and R Studio (Foundation for Statistical Computing, Vienna, Austria). Survival time was defined as the age when the restoration was replaced, repaired or tooth extracted. If the restorations still survived at the end of the study, they were treated as censored cases. Likewise, in case of marginal discoloration, survival time was defined as the age when marginal discoloration was first observed. Survival analysis was performed using the Kaplan–Meier method to obtain the survival curves. Variables associated with failure were assessed by multivariate Cox regression analysis with shared frailty, considering restorations clustered in participants. The age variable was converted into three ordinal scales. The hazard ratios (HRs) and the respective 95% confidence intervals (CIs) were determined. Only those variables presenting p values < 0.25 in univariate analyses were selected for the multivariate analysis except for the type of resin composite. A significance level of 5% was considered for all analyses.
Results
A CONSORT flow diagram with the number of participants, restorations analyzed, and dropouts at 3- and 8-year recalls is shown in Fig. 2. The 8-year participant recall rate was 95%. Out of 19 participants, one participant with 7 restorations, four for AP and three for FX, did not attend the recalls due to death after 5 years. Furthermore, one restoration for AP (deep marginal discoloration) and seven restorations for FX (3 lost, 2 secondary caries, 1 severe wear and 1 replacement by crown) were lost to follow-up.
Recall rates, number of restorations examined, and the results of evaluation according to the criteria per group at each recall interval are summarized in Table 3. One hundred percent retention was recorded for AP, whereas four out of 46 restorations were lost over the 8 years of the study for FX (91%). Three retention failures occurred within 6 months, one restoration loss was found at the 8-year recalls. The incidence of marginal discoloration increased over time regardless of the type of resin composite (Fig. 3). During 8 years of clinical service, marginal discoloration occurred around 21 restorations for AP (48%) and 28 restorations for FX (57%). The extent of marginal discoloration still appeared to be superficial except for the marginal discoloration of three restorations. Marginal discolorations of these three restorations progressed to deep marginal discoloration, two FX restorations of which was also diagnosed as second caries. Cox regression with shared frailty models revealed that none of the variables had any significant effect on the incidence of marginal discoloration (Table 4). Three and five clinically acceptable crevices were found for AP and FX, respectively. Wear of the resin composite occurred on five restorations only in the FX group and there was a significant difference between the types of resin composite (p = 0.024). Wear of the flowable composite was initially observed after 4 years of clinical service, and then the extent of wear as well as the number of restorations showing wear gradually increased. One restoration showed clinically unacceptable wear after 5 years.
Further development of the NCCLs, which were not directly related to the restorations, were found in 10 out of 19 participants. A total of 17 recurrent NCCLs adjacent to the restorations, 7 for AP and 10 for FX, occurred from the 2-year recall to 8-year recall. Five newly developed NCCLs, 2 for AP and 3 for FX, progressed to be clinically unacceptable within a few years after detection (Fig. 4), and the remaining 12 NCCLs continued to slowly progress or were nearly arrested.
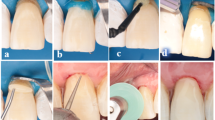
Development and progression of a recurrent NCCL. The restoration that belonged to the AP group was evaluated clinically unacceptable due to a clear NCCL after 5 years of clinical service. a Immediately after restoration with AP. b Development of NCCL adjacent to the gingival margin at 2-year recall. c Progressed (clinically unacceptable) recurrent NCCL at 5-year recall. d Eight-year recall
Figure 5 shows the survival curves of the two types of resin composites, excluding the above 5 restorations with clear NCCL. Eight-year survival rates of AP and FX were 98% and 82%, respectively. Although univariate analyses demonstrated that location (left and right: p = 0.012) and materials (AP and FX: p = 0.021) had significant effects on the survival rates at the 8-year recall, the Cox regression analysis with shared frailty revealed that none of the variables had any significant effects on clinical performance (Table 5).
Discussion
In RCTs or prospective cohort studies, more than 80% of the follow-up rate is considered to be necessary to obtain a high level of evidence [29]. Fortunately, the 8-year participant recall rate was 95% and fulfilled this requirement. In addition, even the 8-year restoration recall rate was 83%, but 8 out of 15 restorations that were not followed-up until the 8-year recall had already been rated B (clinically acceptable) or C (clinically unacceptable).
The overall retention rate after 8 years of clinical functioning was 95% (78/82). A systematic review of adhesives for the restoration of NCCLs reported a somewhat higher annual failure rate of 2.6 for Clearfil S3 Bond compared to our result [30]. Brackett et al. [31] reported that S3 Bond used by inexperienced clinicians in adhesive technology showed relatively high retention failures after 2 years. Several long-term clinical studies indicated that early loss of restorations was no longer a clinical problem when reliable adhesives are used [5, 28, 32,33,34], but retention rates decreased over time probably due to fatigue of the adhesive [33]. The slight tendency towards poorer bonding durability observed for S3 Bond compared to HEMA-free G Bond (GC Corp, Japan) may be due to the presence of HEMA in its formulation, which negatively influences hydrolytic stability and durability of the adhesive interface complex [30, 35]. However, this study demonstrated good bonding durability of S3 Bond and suggests that early retention failures within a year were most likely caused by technical error. It has been speculated that resin composites with a lower elastic modulus relieve the stresses at the adhesive interface generated by polymerization contraction, thermal and occlusal stresses [36]. This stress-breaking effect was not found over the 8 years of clinical service in this study which has also been reported in another long-term clinical trial [5].
Slight detectable discrepancies were frequently observed at the restoration margins, regardless of the type of resin composite. These A-rated marginal defects appeared to be caused by chipping of excess resin composite at the edge of the restoration where is it typically very thin. FX was released only to the Japanese market in 2004, whereas AP was introduced into the global market in 1994. Although FX is a newer product compared with AP, the fracture toughness of FX is likely to be inferior to that of AP due to its lower filler content [37]. Even with AP, excess restorative material may fracture easily since self-etch adhesives show lower bond strength to uncut enamel compared to cut enamel [38]. The crevices appeared to have been caused by marginal fracture of the composite, regardless of their size.
The incidence of marginal discoloration increased over time which confirmed earlier reported findings [5, 28, 34]. Marginal discoloration was found in about half of the restorations after 8 years of clinical functioning. However, all but three cases of marginal discoloration appeared to be superficial and should be able to be easily removed by polishing and/or refurbishing of the stained margin area. Superficial marginal discoloration is likely to be caused by the accumulation of stains at the marginal defect. Deeper marginal discoloration may be due to microleakage around the region where there is excess restorative material and uncut enamel which leaves a thin fin of material in the marginal region. This speculation is supported by the fact that the deep discoloration was occasionally reduced when the excess restorative material chipped off as shown in Fig. 6. With respect to the types of resin composite, there was no significant difference in incidence of marginal discoloration between AP and FX. This may be supported by the findings of a previous long-term clinical trial that compared the clinical performance of a hybrid resin composite and a micro-filled composite with a greater flexibility similar to that of flowable resin composites [5]. Marginal discoloration was observed around more than half of the restorations in 13 participants in the current study, whereas no discoloration was observed in 3 participants. Participant-related factors such as diet, chewing, oral hygiene and smoking habits as well as oral flora may have had some effects on the marginal discoloration [39, 40].
Regarding wear of flowable resin composite, there have been concerns about reduced wear resistance, since flowable resin composites were created by reducing the filler content to reduce the viscosity of the uncured material [7,8,9]. Although many laboratory studies have investigated wear of flowable resin composites [7,8,9, 15,16,17,18], Heintze et al. [41] reported that laboratory wear methods do not reflect clinical wear results. Unfortunately, clinical studies on wear of flowable resin composites are scarce, besides, they have typically been evaluated as short-term occlusal wear of nanocomposites [42]. A systematic review reported that the clinical wear resistance of flowable composites has yet to be determined [37]. In this study, visible wear began to be observed only on FX following about 4 years of clinical service, and then gradually increased thereafter. Not only the composition of fillers, such as filler content, filler particle size, filler mixing method, but also the composition of resin matrix, and silane coupling agents may play an important role in wear resistance of resin composites [16, 17]. Filler content of FX is 65 W% and 40 Vol%, whereas that of AP is 85 W% and 70 Vol%. In addition, FX is not a nanocomposite which is likely to show better wear resistance [16,17,18]. It should be noted that even if the restoration shows wear, it will inhibit the progression of an NCCL toward the dental pulp.
In this clinical trial, NCCLs were merely restored, and there was no intention to investigate the causes of the NCCLs and try to eliminate any causative factors. Consequently, the NCCLs continued to progress around the restorations in half of the participants. This result indicates the importance of attempting to identify then remove any etiological factors causing the NCCL. It has been generally accepted that the initiation and progression of NCCLs have a multifactorial etiology, such as incorrect tooth brushing, erosive agents and occlusal forces [2]. Unfortunately, the relative contributions of the various etiological factors still remain unclear. It was observed that the recurrence of NCCLs gradually increased over time. Three recurrent NCCLs progressed rapidly in the early years following restoration, after which the progression slowed (Fig. 4). Two recurrent NCCLs progressed rapidly after being detected, and progression of remaining 12 recurrent NCCLs appeared to be slow or arrested. These findings suggest that NCCLs may progress through active and inactive stages [43].
Although univariate analyses demonstrated that location and materials had significant effects on the survival rates at the 8-year recall, the Cox regression analysis with shared frailty revealed that none of the variables had any significant effects on clinical performance. For AP, one restoration with sever marginal discoloration required repair or replacement. By contrast, for FX, a total of 8 restorations that were evaluated as clinically unacceptable: 4 lost restorations, 2 with severe marginal discoloration and/or secondary caries, 1 severe wear, 1 hypersensitivity associated with recurrent NCCLs. Among these parameters, only wear resistance is likely to be directly related to properties of the type of resin composite. A patient’s esthetic demands and complaints may also have a great effect on scoring. Throughout the whole study, none of the participants had any complaints with regard to the esthetics even when the restorations showed deep marginal discoloration.
One aspect of this study is that the restorative procedures and main clinical evaluations were performed by the same investigator, and which may have led to an unconscious bias. In order to reduce this bias as much as possible, three independent blinded examiners evaluated the restorations by observing clinical photographs. Although most of clinical parameters were likely to be underestimated because of the limitations of this type of evaluation, retention failures and problems that progressed over time that would normally be repaired or replaced can be determined with sufficient precision. This clinical trial protocol was developed referring to the ADA guidelines, which states that no more than three restorations per product per patient shall be counted and there should be at least 25 patients at baseline [26]. Four out of 19 participants had more than three restorations for either AP or FX. To address this cluster effect, the factors associated with failure were assessed by multivariate Cox regression analysis with shared frailty, which considered that observations within the participant were correlated and shared the same frailty [44]. The number of participants was less than requirement because the planned recruitment and restoration placement period was only 6 months.
According to the results of this study, the null hypothesis that there is no significant difference in eight-year clinical performance between the two types of resin composite was rejected. Continued long-term follow-up of this study is necessary to clearly determine bonding durability, wear resistance of flowable composites, and the progression of marginal discoloration. Furthermore, a long-term clinical trial using recent so-called nanofilled or highly filled flowable composites is also required to better understand their performance over the long term.
Conclusion
Under the protocol used in this study, the following conclusions were drawn:
-
1.
Eight-year clinical study revealed lower wear resistance of the flowable resin composite compared with the conventional composite.
-
2.
The flowable resin composite showed a lower survival rate than the conventional composite after eight years of clinical service.
Change history
12 July 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00784-022-04621-8
References
Borcic J, Anic I, Urek MM, Ferreri S (2004) The prevalence of noncarious cervical lesions in permanent dentition. J Oral Rehabil 31:117–123. https://doi.org/10.1046/j.0305-182x.2003.01223.x
Wood I, Jawad Z, Paisley C, Brunton P (2008) Non-carious cervical tooth surface loss: A literature review. J Dent 36:759–766. https://doi.org/10.1016/j.jdent.2008.06.004
Santos MJMC, Ari N, Steele S, Costella J, Banting D (2014) Retention of tooth-colored restorations in non-carious cervical lesions—a systematic review. Clin Oral Investig 18:1369–1381. https://doi.org/10.1007/s00784-014-1220-7
Peumans M, Politano G, Van Meerbeek B (2020) Treatment of noncarious cervical lesions: when, why, and how. Int J Esthet Dent 15:16–42
Peumans M, De Munck J, Van Landuyt KL, Kanumilli P, Yoshida Y, Inoue S, Lambrechts P, Van Meerbeek B (2007) Restoring cervical lesions with flexible composites. Dent Mater 23:749–754. https://doi.org/10.1016/j.dental.2006.06.013
Szesz A, Parreiras S, Martini E, Reis A, Loguercio A (2017) Effect of flowable composites on the clinical performance of non-carious cervical lesions: a systematic review and meta-analysis. J Dent 65:11–21. https://doi.org/10.1016/j.jdent.2017.07.007
Bayne SC, Thompson JY, Swift EJ Jr, Stamatiades P, Wilkerson M (1998) A characterization of first-generation flowable composites. J Am Dent Assoc 129: 567–577 https://doi.org/10.14219/jada.archive.1998.0274
Garcia FCP, Wang L, D’Alpino PHP, de Souza JB, de Araújo PA, de Lia Mondelli RF (2004) Evaluation of the roughness and mass loss of the flowable composites after simulated tooth brushing abrasion. Braz Oral Res 18:156–161. https://doi.org/10.1590/s1806-83242004000200012
Clelland NL, Pagnotto MP, Kerby RE, Seghi RR (2005) Relative wear of flowable and highly filled composite. J Prosthet Dent 93:153–157
Han L, Okamoto A, Fukushima M, Okiji T (2008) evaluation of flowable resin composite surfaces eroded by acid and alcoholic drinks. Dent Mater J 27:455–465
Peutzfeldt A (1997) Resin composites in dentistry: the monomer systems. Eur J Oral Sci 105:97–116. https://doi.org/10.1111/j.1600-0722.1997.tb00188.x
Ferracane JL (2011) Resin composite—state of the art. Dent Mater 27:29–38. https://doi.org/10.1016/j.dental.2010.10.020
Mitra SB, Wu D, Holmes BN (2003) An application of nanotechnology in advanced dental materials. J Am Dent Assoc 134:1382–1390
Ilie N, Hickel, (2011) Investigations on a methacrylate-based flowable composite based on the SDR ™ technology. Dent Mater 27:348–355. https://doi.org/10.1016/j.dental.2010.11.014
Shinkai K, Taira Y, Suzuki S, Kawashima S, Suzuki M (2018) Effect of filler size and filler loading on wear of experimental flowable resin composites. J Appl Oral Sci 26:e20160652. https://doi.org/10.1590/1678-7757-2016-0652
Sumino N, Tsubota K, Takamizawa T, Shiratsuchi K, Miyazaki M, Latta MA (2013) Comparison of the wear and flexural characteristics of flowable resin composites for posterior lesions. Act Odontol Scand 71:820–827. https://doi.org/10.3109/00016357.2012.734405
Lazaridou D, Belli R, Petschelt A, Lohbauer U (2015) Are resin composites suitable replacements for amalgam? A study of two-body wear. Clin Oral Investig 19:1485–1492. https://doi.org/10.1007/s00784-014-1373-4
Imai A, Takamizawa T, Sugimura R, Tsujimoto A, Ishii R, Kawazu M, Saito T, Miyazaki M (2019) Interrelation among the handling, mechanical, and wear properties of the newly developed flowable resin composites. J Mech Behav Biomed Mater 89:72–80. https://doi.org/10.1016/j.jmbbm.2018.09.019
Kubo S, Yokota H, Yokota H, Hayashi Y (2004) Microleakage of cervical cavities restored with flowable composites. Am J Dent 17:33–37
Kubo S, Yokota H, Yokota Y, Hayashi Y (2010) Three-year clinical evaluation of a flowable and a hybrid resin composite in non-carious cervical lesions. J Dent 38:191–200. https://doi.org/10.1016/j.jdent.2009.10.003
Çelik Ç, Özgünaltay G, Attar N (2007) Clinical evaluation of flowable resins in non-carious cervical lesions: two-year results. Oper Dent 32:313–321. https://doi.org/10.2341/06-93
Karaman E, Yazici AR, Ozgunaltay G, Dayangac B (2012) Clinical evaluation of a nanohybrid and a flowable resin composite in noncarious cervical lesions: 24-month results. J Adhes Dent 14:485–492. https://doi.org/10.3290/j.jad.a27794
May S, Cieplik F, Hiller K-A, Buchalla W, Federlin M, Schmalz G (2017) Flowable composites for restoration of non-carious cervical lesions: three-year results. Dent Mater 33:e136–e145. https://doi.org/10.1016/j.dental.2016.12.009
Canali GD, Ignácio SA, Rached RN, Souza EM (2019) One-year clinical evaluation of bulk-fill flowable vs. regular nanofilled composite in non-carious cervical lesions. Clin Oral Investig 23:889–897. https://doi.org/10.1007/s00784-018-2509-8
Zhang H, Wang L, Hua L, Guan R, Hou B (2021) Randomized controlled clinical trial of a highly filled flowable composite in non-carious cervical lesions: 3-year results. Clin Oral Investig 25:5955–5965. https://doi.org/10.1007/s00784-021-03901-z
ADA Council on Scientific Affairs (2001) ADA acceptance program guidelines: dentin and enamel adhesive materials. Chicago, IL: ADA Council on Scientific Affairs.
van Dijken JWV (1986) A clinical evaluation of anterior conventional, microfiller and hybrid composite resin fillings. A six year follow up study. Acta Odontol Scand 44:357–367
Ritter AV, Swift Jr EJ, Heymann HO, Sturdevant JR, Wilder Jr AD (2009) An eight-year clinical evaluation of filled and unfilled one-bottle dental adhesives. J Am Dent Assoc 140:28–37 https://doi.org/10.14219/jada.archive.2009.0015
Oxford Centre for Evidence-Based Medicine: Levels of Evidence (March 2009) https://www.cebm.ox.ac.uk/resources/levels-of-evidence/oxford-centre-for-evidence-based-medicine-levels-of-evidence-march-2009. Accessed November 16 2021
Peumans M, De Munck J, Mine A, Van Meerbeek B (2014) Clinical effectiveness of contemporary adhesives for the restoration of non-carious cervical lesions. A systematic review. Dent Mater 30:1089–1103. https://doi.org/10.1016/j.dental.2014.07.007
Brackett MG, Dib A, Franco G, Estrada BE, Brackett WW (2010) Two-year clinical performance of Clearfil SE and Clearfil S3 in restoration of unabraded non-carious Class V lesions. Oper Dent 35:273–278. https://doi.org/10.2341/09-266-C
Kubo S, Kawasaki K, Yokota H, Hayashi Y (2006) Five-year clinical evaluation of two adhesive systems in non-carious cervical lesions. J Dent 34:97–105. https://doi.org/10.1016/j.jdent.2005.04.003
Van Dijken JWV (2010) A prospective 8-year evaluation of a mild two-step self-etching adhesive and a heavily filled two-step etch-and-rinse system in non-carious cervical lesions. Dent Mater 26:940–946. https://doi.org/10.1016/j.dental.2010.05.009
Peumans M, Wouters L, De Munck J, Van Meerbeek B, van Landuyt K (2018) Nine-year clinical performance of a HEMA-free one-step self-etch adhesive in non-carious cervical lesions. J Adhes Dent 20:195–203. https://doi.org/10.3290/j.jad.a40630
Hosaka K, Nakajima M, Takahashi M, Itoh S, Ikeda M, Tagami J, Pashley DH (2010) Relationship between mechanical properties of one-step self-etch adhesives and water sorption. Dent Mater 26:360–367. https://doi.org/10.1016/j.dental.2009.12.007
Van Meerbeek B, Braem M, Lambrechts P, Vanherle G (1993) Evaluation of two dentin adhesives in cervical lesions. J Prosthet Dent 70:308–314. https://doi.org/10.1016/0022-3913(93)90213-8
Baroudi K, Rodrigues JC (2015) Flowable Resin Composites: A Systematic Review and Clinical Considerations. J Clin Diagn Res 9:ZE18–ZE24 https://doi.org/10.7860/JCDR/2015/12294.6129
Perdigão J, Gomes G, Duarte S Jr, Lopes MM (2005) Enamel bond strengths of pairs of adhesives from the same manufacturer. Oper Dent 30:492–499
Burrow MF, Tyas MJ (2012) Clinical investigation of G-Bond resin-based adhesive to non-carious cervical lesions over five years. Aust Dent J 57:458–463. https://doi.org/10.1111/j.1834-7819.2012.01729.x
Moretto SG, Russo EMA, Carvalho RCR, De Munck J, Van Landuyt K, Peumans M, Van Meerbeek B, Cardoso MV (2013) 3-year clinical effectiveness of one-step adhesives in non-carious cervical lesions. J Dent 41:675–682. https://doi.org/10.1016/j.jdent.2013.05.016
Heintze SD, Faouzi M, Rousson V, Özcan M (2012) Correlation of wear in vivo and six laboratory wear methods. Dent Mater 28:961–973. https://doi.org/10.1016/j.dent.2012.04.006
Lawson NC, Radhakrishnan R, Givan DA, Ramp LC, Burgess JO (2015) Two-year randomized, controlled clinical trial of a flowable and conventional composite in class I restorations. Oper Dent 40:594–602. https://doi.org/10.2341/15-038-C
Hayashi M, Kubo S, Pereira P, Ikeda M, Takagaki T, Nikaido T, Tagami J (2022) Progression of non-carious cervical lesions: 3D morphological analysis. Clin Oral Invest 26:575–583. https://doi.org/10.1007/s00784-021-04036-x
Hougaard P (1995) Frailty models for survival data. Lifetime Data Anal 1:255–273. https://doi.org/10.1007/BF00985760
Acknowledgements
The authors would like to express their gratitude to Prof. Michael F Burrow, University of Hong Kong, for assistance in preparation of the manuscript. The authors also wish to thank Dr. Nobuaki Magata for his invaluable help with the statistical analysis using the frailty models. Furthermore, the authors would like to thank all individual participants who took part in this study.
Funding
This work was supported by Japan Society for the Promotion of Science (JSPS) KAKENHI Grant Number 18K09602.
Author information
Authors and Affiliations
Contributions
Evaluations were performed by all authors. SK analyzed data. KK and SK wrote the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study protocol was approved by the Ethics Committee of Nagasaki University Hospital (No. 17041717).
Consent to participate
Written informed consent was obtained from all individual participants included in the study.
Consent to publish
Participants signed informed consent regarding publishing their data and photographs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised: This article was originally published with an omitted data for table 3.
Rights and permissions
About this article
Cite this article
Kaida, K., Kubo, S., Egoshi, T. et al. Eight-year clinical evaluation of two types of resin composite in non-carious cervical lesions. Clin Oral Invest 26, 6327–6337 (2022). https://doi.org/10.1007/s00784-022-04587-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04587-7