Abstract
Objective
To evaluate the effect of adjustment and finishing procedures and thermal aging of monolithic zirconia on the surface roughness, phase transformation, and flexural strength.
Material and methods
One hundred disk-shaped monolithic zirconia specimens were randomly divided into 5 groups: control, received only glazing; group Gr, was grinded; group GrP, was grinded and polished; group GrG, was grinded and re-glazed; group GrPG, was re-glazed after grinding and polishing. Half of the each group were stored in distilled water for 24 h and the remaining were thermocycled for 5000 cycles. Topographic evaluations were done with profilometer and scanning electron microscope. Phase changes were assessed through X-ray diffractometer. The biaxial flexural strength test was calculated by universal test machine. Statistical analysis was performed by using two-way ANOVA and Tukey multiple comparison test (p < 0.05).
Results
Group Gr showed statistically higher surface roughness and flexural strength values than the other groups (p < 0.001). However, no significant differences were observed between finishing groups (p >0.05). Phase transformation was occurred in all groups but the differences were not statically significant (p >0.05). Artificial aging had no effect on surface roughness, flexural strength, and phase transformation (p >0.05).
Conclusion
Surface roughness significantly increased after grinding, but finishing procedure approximated it to the control group. Glazing after grinding decreased the flexural strength, but polishing did not. Zirconia polishing system may be an alternative to re-glazing for monolithic zirconia.
Clinical relevance
Polishing is one of the most effective finishing procedures that can improve the physical properties of the material without damaging its mechanical properties.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The popularity of zirconia restorations has increased for dental applications because of their superior mechanical and chemical properties, biocompatibility, and esthetical advantage compared to conventional metal-ceramic restorations [1,2,3,4]. Currently, zirconia restorations can be used in two different methods; these are zirconia-based porcelain restorations and monolithic zirconia [5]. Two layer restorations commonly cause bonding issues which are concluded with fracture and chipping of porcelain. However, monolithic zirconia is an anatomic-contoured restoration without esthetic material fabricated by the computer-aided design and computer-aided manufacturing systems (CAD/CAM) which often eliminate the clinical complications of zirconia-based porcelain restorations [5, 6]. Although CAD/CAM technology works precisely, the intraoral adjustments are necessary to optimize occlusal, axial, and proximal contacts [7, 8]. But intraoral adjustments cause loss of glaze layer and increase surface roughness of restorations. Roughness can lead to the plaque accumulations, dental caries, gingival inflammations, or wear of the opposite tooth surface [9, 10]. Re-glaze process or intraoral polishing has to be used for smoothing the irregular and rough structure on the surface. As is known, irregularities and surface flaws are filled by glazing and zirconia is strengthened by compressive stress that occurs during cooling process. However, re-glaze means multiple office visits and extra firing process which may cause catastrophic effect on zirconia surface and reverse phase transformation [5, 6, 10, 11]. Also, some studies stated that heat treatment triggers the phase transformation of zirconia and damage the flexural strength of restoration [11,12,13]. Besides these, intraoral zirconia polishing systems may reduce the surface flaws without extra firing requirement and office visits and studies asserted that polishing improves the flexural strength and longevity of restorations [5, 14, 15].
Zirconium, a polymorph material, can be found in 3 different phases (monoclinic, cubic, tetragonal) with transformation toughening ability. External stimulations induce compressive stress on the surface which is attended by volume expansion that prevent the crack the propagation [2, 16,17,18]. Microcracks can improve the strength of zirconia by phase transformation, but the depth of the crack should not exceed the compressive stress layer. From this point of view, clinical adjustment and finishing procedure conditions may affect the phase transformation in parallel to strength of the zirconia restorations [12,13,14,15,16,17,18,19,20].
The purpose of the present study was to evaluate and compare the effect of adjustment and finishing procedure and thermal aging of monolithic zirconia on the surface roughness, topographic properties, phase transformation, and flexural strength. The null hypothesis was that adjustment and finishing procedures and thermal aging do not affect the surface roughness, phase transformations, and flexural strength of monolithic zirconia.
Material and methods
A hundred disks (15 mm diameter × 1.2 mm thickness) were prepared from monolithic zirconia blocks (Ceramill Zolid fx White; Amann Girrbach GmbH, Pforzheim, Germany) by milling machine (Yenadent DC40, Yenadent Ltd., Istanbul, Turkey). The specimens were finished by silicon carbide paper (600, 800, 1200 grit, Struers A/S, Cleveland, USA) for 15 s in one direction before sintering in a furnace (Everest Therm; KaVo Dental GmbH, Biberach, Germany). Each specimen’s size was controlled by digital caliper (TorQ 150 × 0.001 mm Digital Caliper, China). The untreated surface of the specimens was marked and the unmarked surface of each specimen was glazed (Ceramill Stain and Glaze, Amann Girrbach GmbH, Pforzheim, Germany) in a furnace (Ivoclar Vivadent AG, Liechtenstein, Germany) for 1 min at 850 °C (Table 1).
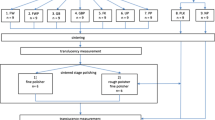
The specimens were randomly separated into 5 groups (n = 20):
-
Group C, control. No process was applied to the specimens in this group after glazing.
-
Group Gr, grinding. Grinding process was performed with 100 μm diamond particle blue band bur (881Z4, Meisinger, Neuss, Germany). Grinding was applied with sweeping motion continuously in forward–backward for 20 s at 20,000 rpm under water coolant. Bur was changed after every 5 specimens.
-
Group GrP, grinding + polishing. Specimens were grinded as previously described for group Gr. An intraoral zirconia polishing kit (EVE Diacera RA 322, EVA Ernst Vetter GmbH, Pforzheim, Germany) was used by the same examiner in a 3-step procedure: gray blue rubber (removing), green rubber (smoothing), and orange rubber (high-luster polishing). Polishing was carried out in one direction for 30 s by using low-speed handpiece (Ti-Max X600L; NSK, Tochigi Ken, Japan) and then was continued at an angle of 90° for 30 s by the same examiner. Polishing was performed for a total 3 min in the same specimen, and 1 min for each polisher of the polishing kit. After polishing, specimens were ultrasonically cleaned (Bandelin Sonorex, Bandelin Electronic GmbH & Co., Berlin, Germany) in distilled water for 1 min and then air dried.
-
Group GrG, grinding + glaze. Specimens were grinded as previously described for group Gr and then re-glazed.
-
Group GrPG, grinding + polishing + glaze. Specimens were grinded and polished as previously described for group GrP and then re-glazed.
Thermal aging process
Each group (n = 20) was divided in two subgroups according to thermal aging process. Half of the specimens of the groups (n = 10) underwent 5000 thermocycles (between 5 and 55 °C) with a 30-s dwell time in each water bath by using an thermocycling machine (Gökçeler Machines, Sivas, Turkey) after adjustment and finishing process. And the other specimens (n = 10) were stored in distilled water at 37 °C for 24 h after adjustment and finishing process.
Surface roughness measurements and SEM evaluations
Surface roughness of the monolithic zirconia specimens was evaluated with a stylus profilometer (Perthometer M2, Mahr GmbH, Göttingen, Germany). Three individual measurements at different locations were recorded from each specimen. The Ra value of each specimen was calculated by the arithmetic mean of the measurements. An additional specimen was prepared for each group to evaluate the topographical surface with scanning electron microscopy (JSM-6610, Jeol Ltd., Peabody, USA) at × 2000 magnification.
X-ray diffraction analysis
X-ray diffractometer (XRD, Smartlab-201307, Rigaku Corporation, Tokyo, Japan) was used to examine the crystallographic phase change of the specimens. Irradiation was performed at 0.02°/step between the intervals of 20–40° (2Ɵ). Garvie-Nicholson [21] method was used to calculate the relative amount of the monoclinic phase (XM) of zirconia specimens:
- I :
-
intensity detected by the detector at angular position
- M(111):
-
major monoclinic peak
- M(111 −):
-
major monoclinic peak
- T(111):
-
tetragonal peak
Biaxial flexural strength text
Specimens were subjected to a biaxial flexural strength test (piston on three ball) according to the Internal Organization for Standardization (ISO) 6872–74 [22] standards using a universal test machine (Instron 3340, Wycombe, UK). Biaxial flexural strength test was performed on a 10 mm diameter metallic platform that contains three 3.2 mm diameter spherical stainless steel balls at equal distance supporting the specimens. The load was applied to the center of the specimen with a flat piston (1.4 mm diameter). The crosshead speed was set at a 0.15 mm/min and the failure stress was calculated using the following equation.
where S is the maximum center tensile stress (MPa) and P is the total load causing fracture.
- Ɣ:
-
Poison ratio (0.25)
where r1 is the radius of support circle, r2 is the radius of the loaded area, r3 is the radius of the specimen, and d is thickness of the specimen.
Statistical analysis
Statistical analysis was performed with Statistical Package for Social Sciences statistical software Graduate Package 20.0. (SPSS Inc., Chicago, IL, USA). The power analysis was calculated according to the previous article [23] by considering the effect size = 2, beta error = 0.80, and alpha error = 0.95. Finally, it was decided to use 20 specimens for each group that could be adequate for statistical evaluation. Two-way ANOVA and Tukey’s post hoc were used for pairwise comparisons at a significance level of p < 0.05.
Results
Surface roughness and SEM evaluations
Table 2 presents the mean and standard deviation (SD) values of surface roughness. While the highest surface roughness values were found for group Gr, the lowest surface roughness values were found in group C for both aged and non-aged groups. All finishing procedure (groups GrP, GrG, and GrPG) exhibited a smoother surface than group Gr (p < 0.001). No statistically significant differences were found in surface roughness after thermal aging (p > 0.05).
SEM evaluations verified the results of the surface roughness test. SEM results showed that control group (group C) showed smooth surface without grooves or scratches (Fig. 1A). The images of the grinding group (group Gr) showed that the homogeneous structure in the control groups was destroyed by grinding. Scratches parallel to the grinding direction was clearly observed (Fig. 2A). The images of group GrP showed that the image formed by grinding is partially smoothed but deep grooves and scratches could not entirely removed, and striations were observed (Fig. 3A). The images of group GrG and group GrPG showed similar surface properties with control group (Figs. 4A and 5A). The aging process did not affect the SEM images (Figs. 1B and 5B).
XRD analysis
Means and standard deviations of relative amount of monoclinic phase for all groups are presented in Table 3. The finishing and grinding procedure increased the relative amount of monoclinic zirconia but the differences were not statistically significant (p > 0.05). The higher XM values were found in group Gr and the lowest values were found in the control group.
Aging process caused degradation of XM values but the differences were not statistically significant (p > 0.05).
Flexural strength test
Means and standard deviations of biaxial flexural strength for all groups are presented in Table 4. Among the non-aged groups, group C showed the lowest flexural strength values while group Gr showed the highest mean value. Among the aged group, group GrG showed the lowest flexural strength values while group Gr showed the highest mean value.
Both aged and non-aged grinding groups showed statistically significant higher values than the other groups (p < 0.001). Finishing groups (groups GrP, GrG, and GrGP) showed similar values to the control group. It was shown that aging process had a negative effect on flexural strength but it was not statistically significant.
Discussion
The present study investigated the effect of adjustment and finishing procedures and thermal aging on surface roughness, phase transformation, and flexural strength of monolithic zirconia. The null hypothesis that adjustment and polishing procedures and thermal aging do not affect the surface roughness, phase transformation, and flexural strength of monolithic zirconia was partially rejected because only intraoral adjustment significantly affected the flexural strength and surface roughness of monolithic zirconia.
Precise preparation of CAD/CAM for monolithic zirconia restorations does not eliminate the requirement of chairside adjustment procedure. Grinding which is done for establishing optimal occlusal contacts leads to remove the glaze layer and creates a very rough surface with deep surface flaws. Resultant rough surface causes bacteria accumulation and antagonistic tooth wear. Bollen et al. [24] emphasized that surface roughness of hard tissues in oral environment had a significant effect on the formation of subgingival and supragingival plaques and they claimed that the Ra value of 0.2 μm was the threshold value. In the present study while grinding increased the surface roughness, all finishing procedures (groups GrG, GrP, and GrGP) revealed surface roughness values below the threshold values of Bollen et al. [24] which means that the surface roughness values are clinically acceptable.
Studies have investigated the surface roughness and wear behavior of polished and glazed monolithic zirconia and they stated that the glaze process eliminates the surface irregularities ideally but durability of glaze layer is suspicious under function [5, 25]. The duration of this smoothness is as important as the surface roughness value. For this reason, the studies have concluded that polished zirconia is more wear-friendly for the opposing teeth [25, 26]. In the present study, the aging process showed the longevity of glaze layer. The aged re-glaze groups (groups GrG and GrPG) showed higher surface roughness values than the non-aged re-glaze groups. It may be due to damaged glazing layer on the surface. However, the non-aged polishing group (group GrP) showed similar surface roughness values to the aged polishing group.
In the present study, phase transformation was observed in all test groups, especially group Gr and group GrP showed higher XM values than the other groups. However, no statistically significant differences were found among the groups. Similar to the present study, Huh et al. [23] and Al-Haj Husain et al. [27] stated that neither grinding nor polishing cause statistically significant differences in phase transformation. However, Lee et al. [28] stated that phase transformation was occurred after grinding with different diamond burs. The reason of discrepancy of the studies is about grinding parameters. Lee et al. [28] used 150 μm particle coarse bur for grinding but other studies [23, 27] prevented the phase transformation by using 100 μm particle bur. Also studies [5, 7, 9, 13] stated that phase transformation may occur to a larger extent when zirconia polishing or grinding treatments are carried out without water. In the present study, grinding was applied with 100 μm particle diamond bur under water cooling for preventing the reverse phase transformation. However, Park et al. [7] indicated the increase of monolithic phase of monolithic zirconia when polishing procedure was applied for 8 min under water cooling. They also stated that the time range of polishing should be limited within 2 to 8 min for clinical polishing. In light of these results, polishing application time was restricted for a total of 3 min to prevent the reverse phase transformation in the present study. Lee et al. [29] also studied about polishing and grinding of zirconia and remarked that polishing ground monolithic zirconia caused reduction of XM values similar to the present study. It is because polishing removed the monoclinic phase transformed from tetragonal phase by coarse bur grinding on the zirconia surface [28, 29].
Grinding process create a compressive stress layer on monolithic zirconia surface that is assumed to increase flexural strength by transformation toughening mechanism. Kosmac et al. [30] advocated that fine grinding process improved the flexural strength and reliability of zirconia. However, Xu et al. [31] emphasized that coarser grinding resulted in strength diminution. In the present study, the highest flexural strength value was found in grinding groups. It is because grinding causes residual surface compressive stress, which can increase the mean flexural strength of monolithic zirconia. Finishing groups also showed higher flexural strength values than the control group but differences were not statistically significant. Among the finishing groups, it stood out the reduction of flexural strength values after glazing. The reason for this reduction can be explained as the exposure of monolithic zirconia to heat during the glaze process. Local temperature increase during glazing may be the reason of reverse transformation. Although it is suggested that glazing improves the flexural strength by decreasing the depth of cracks on zirconia layer, Mohammadi-Bassir et al. [13] reported that zirconia was exposed to heat and moisture during the glazing which made zirconia susceptible to degradation. Guazzato et al. [32] also remarked that grinding without heat treatment may have improved the flexural strength of zirconia but heat treatment after grinding or polishing decreased the flexural strength by impairing the compressive stress layer and triggering the reverse phase transformation. It means that smoothness of the material surface should not always be the only feature to be considered for finishing processes. Even though the lowest surface roughness was obtained in the over-glazed groups (groups GrG and GrPG), it was observed that the polishing group was better in mechanical properties in the present study.
There are some limitations in the present study. The study is based on the use of a single zirconia block and cannot be generalized to other zirconia brands. Different brands may include different grain sizes which affect the mechanical properties. Also, different zirconia polishing kit may have different polishing stages that can affect the mechanical and physical properties of the zirconia. The study was evaluated under in vitro conditions which exclude most variants occurring in the mouth such as parafunctional habits or dynamic occlusal load. Further studies should be structured by different brands of monolithic zirconia and polishing kit under clinical conditions.
Conclusion
Within the limitations of the study, the following conclusions were drawn:
-
1.
Intraoral adjustment increased the surface roughness but all finishing groups diminished it to the control group.
-
2.
Grinding increased the flexural strength of monolithic zirconia and finishing groups had no unfavorable effect on flexural strength of ground monolithic zirconia.
-
3.
Polishing may be an alternative finishing technique of monolithic zirconia instead of over-glazing after intraoral adjustments.
-
4.
Aging had no significant effect on surface roughness, flexural strength, and phase transformation.
References
Pereira GKR, Silvestri T, Camargo R, Rippe MP, Amaral M, Kleverlaan CJ, Valandro LF (2016) Mechanical behaviour of a Y-TZP ceramic for monolithic restorations: effect of grinding and low-temperature aging. Mater Sci Eng C Mater Biol Appl 63:70–77. https://doi.org/10.1016/j.msec.2016.02.049
Piconi C, Maccauro G (1999) Zirconia as a ceramic biomaterial. Biomaterials 20:1–25. https://doi.org/10.1016/s0142-9612(98)00010-6
Zhang Y (2014) Making yttria-stabilized tetragonal zirconia translucent. Dent Mater 30:1195–1203. https://doi.org/10.1016/j.dental.2014.08.375
Lazar DR, Bottino MC, Ozcan M, Valandro LF, Amaral R, Ussui V, Bressiani AH (2008) Y-TZP ceramic processing from coprecipitated powders: a comparative study with three commercial dental ceramics. Dent Mater 24:1676–1685. https://doi.org/10.1016/j.dental.2008.04.002
Caglar I, Ates SM, Yesil DZ (2018) The effect of various polishing systems on surface roughness and phase transformation of monolithic zirconia. J Adv Prosthodont 10:132–137. https://doi.org/10.4047/jap.2018.10.2.132
Rosentritt M, Preis V, Behr M, Hahnel S, Handel G, Kolbeck C (2012) Two-body wear of dental porcelain and substructure oxide ceramics. Clin Oral Investig 16:935–943. https://doi.org/10.1007/s00784-011-0589-9
Park C, Vang MS, Park SW, Lim HP (2017) Effect of various polishing systems on the surface roughness and phase transformation of zirconia and the durability of the polishing systems. J Prosthet Dent 117:430–437. https://doi.org/10.1016/j.prosdent.2016.10.005
Hmaidouch R, Müller WD, Lauer HC, Weigl P (2014) Surface roughness of zirconia for full-contour crowns after clinically simulated grinding and polishing. Int J Oral Sci 6:241–246. https://doi.org/10.1038/ijos.2014.34
Khayat W, Chebib N, Finkelman M, Khayat S, Ali A (2018) Effect of grinding and polishing on roughness and strength of zirconia. J Prosthet Dent 119:626–631. https://doi.org/10.1016/j.prosdent.2017.04.003
Aravind P, Razak PA, Francis PG, Issac JK, Shanoj RP, Sasikumar TP (2013) Comparative evaluation of the efficiency of four ceramic finishing systems. J Int Oral Health 5:59–64
Fairhurst CW, Lockwood PE, Ringle RD, Thompson WO (1992) The effect of glaze on porcelain strength. Dent Mater 8:203–207. https://doi.org/10.1016/0109-5641(92)90084-P
Caglar İ, Yanıkoğlu N (2016) The effect of sandblasting, Er:YAG laser and heat treatment on the mechanical properties of different zirconia cores. Photomed Laser Surg 34:17–26. https://doi.org/10.1089/pho.2015.3980
Mohammadi-Bassir M, Babasafari M, Rezvani MB, Jamshidian M (2017) Effect of coarse grinding, overglazing, and 2 polishing systems on the flexural strength, surface roughness, and phase transformation of yttrium-stabilized tetragonal zirconia. J Prosthet Dent 118:658–665. https://doi.org/10.1016/j.prosdent.2016.12.019
Preis V, Behr M, Handel G, Schneider-Feyrer S, Hahnel S, Rosentritt M (2012) Wear performance of dental ceramics after grinding and polishing treatments. J Mech Behav Biomed Mater 10:13–22. https://doi.org/10.1016/j.jmbbm.2012.03.002
Preis V, Behr M, Kolbeck C, Hahnel S, Handel G, Rosentritt M (2011) Wear performance of substructure ceramics and veneering porcelains. Dent Mater 27:796–804. https://doi.org/10.1016/j.dental.2011.04.001
Mitov G, Heintze SD, Walz S, Woll K, Muecklich F, Pospiech P (2012) Wear behavior of dental Y-TZP ceramic against natural enamel after different finishing procedures. Dent Mater 28:909–918. https://doi.org/10.1016/j.dental.2012.04.010
Luthardt RG, Holzhüter M, Sandkuhl O, Herold V, Schnapp JD, Kuhlisch E (2002) Reliability and properties of ground Y-TZP-Zirconia ceramics. J Dent Res 81:487–491. https://doi.org/10.1177/154405910208100711
Mohammadi-Bassir M, Rezvani MB, Golzari H, Moravej Salehi E, Fahimi MA, Kharazi Fard MJ (2019) Effect of two polishing systems on surface roughness, topography, and flexural strength of a monolithic lithium disilicate ceramic. J Prosthodont 28:e172–e180. https://doi.org/10.1111/jopr.12586
Karakoca S, Yilmaz H (2009) Influence of surface treatments on surface roughness, phase transformation, and biaxial flexural strength of Y-TZP ceramics. J Biomed Mater Res B Appl Biomater 91:930–937. https://doi.org/10.1002/jbm.b.31477
Kasmac T, Oblak C, Jevnikar P, Funduk N, Marion L (1999) The effect of surface grinding and sandblasting on flexural strength and reliability of Y-TZP zirconia ceramic. Dent Mater 15:426–33. https://doi.org/10.1016/s0109-5641(99)00070-6
Garvie RC, Nicholson PS (1972) Phase analysis in zirconia systems. J Am Ceram Soc 55:303–305. https://doi.org/10.1111/j.1151-2916.1972.tb11290.x
Wendler M, Belli R, Petschelt A, Mevec D, Harrer W, Lube T, Danzer R, Lohbauer U (2017) Chairside CAD/CAM materials. Part 2: flexural strength testing. Dent Mater 33:99–109. https://doi.org/10.1016/j.dental.2016.10.008
Huh YH, Park CJ, Cho LR (2016) Evaluation of various polishing systems and the phase transformation of monolithic zirconia. J Prosthet Dent 116:440–449. https://doi.org/10.1016/j.prosdent.2016.01.021
Bollen CM, Lambrechts P, Quirynen M (1997) Comparison of surface roughness of oral hard materials to the threshold surface roughness for bacterial plaque retention: a review of the literature. Dent Mater 13:258–269. https://doi.org/10.1016/s0109-5641(97)80038-3
Sabrah AH, Cook NB, Luangruangrong P, Hara AT, Bottino MC (2013) Full-contour Y-TZP ceramic surface roughness effect on synthetic hydroxyapatite wear. Dent Mater 29:666–673. https://doi.org/10.1016/j.dental.2013.03.008
Janyavula S, Lawson N, Cakir D, Beck P, Ramp LC, Burgess JO (2013) The wear of polished and glazed zirconia against enamel. J Prosthet Dent 109:22–29. https://doi.org/10.1016/S0022-3913(13)60005-0
Al-Haj Husain N, Camilleri J, Özcan M (2016) Effect of polishing instruments and polishing regimens on surface topography and phase transformation of monolithic zirconia: an evaluation with XPS and XRD analysis. J Mech Behav Biomed Mater 64:104–112. https://doi.org/10.1016/j.jmbbm.2016.07.025
Lee KR, Choe HC, Heo YR, Lee JJ, Son MK (2016) Effect of different grinding burs on the physical properties of zirconia. J Adv Prosthodont 8:137–143. https://doi.org/10.4047/jap.2016.8.2.137
Lee JY, Jang GW, Park II, Heo YR, Son MK (2019) The effects of surface grinding and polishing on the phase transformation and flexural strength of zirconia. J Adv Prosthodont 11:1–6. https://doi.org/10.4047/jap.2019.11.1.1
Kosmac T, Oblak C, Jevnikar P, Fandak N, Marion L (2000) Strength and reliability of surface treated Y-TZP dental ceramics. J Biomed Mater Res 53:304–13. https://doi.org/10.1002/1097-4636(2000)53:4%3c304::aid-jbm4%3e3.0.co;2-s
Xu HHK, Jahanmir S, Ives LK (1997) Effect of grinding on strength of tetragonal zirconia and zirconia toughened alumina. Mach Sci Technol 1:49–66. https://doi.org/10.1080/10940349708945637
Guazzato M, Quach L, Albakry M, Swain MV (2005) Influence of surface and heat treatments on the flexural strength of Y-TZP dental ceramic. J Dent 33:9–18. https://doi.org/10.1016/j.jdent.2004.07.001
Funding
This study was supported by the Research Projects Fund of Recep Tayyip Erdogan University (Grant no: TDH-2018–933).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Consent to participate
For this type of study, formal consent is not required.
Conflict of interest
Isıl Ozturk declares that she has no conflict of interest. Ipek Caglar declares that she has no conflict of interest. Zeynep Yesil Duymus declares that she has no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ozturk, I., Caglar, I. & Duymus, Z.Y. The effect of adjustment and finishing procedure on roughness, strength, and phase transformation of monolithic zirconia. Clin Oral Invest 26, 4761–4768 (2022). https://doi.org/10.1007/s00784-022-04440-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04440-x