Abstract
Objective
To verify the photobiomodulation effect on angiogenic proteins produced and released by dental human pulpal fibroblasts (HPFs).
Material and methods
HPFs were irradiated with 660-nm low-level laser at fluences of 2.5 J/cm2 and 3.7 J/cm2. The control group was not irradiated. MTT, crystal violet, and ELISA assays respectively verified viability, proliferation, and angiogenic protein (supernatant/lysate) at 6 h, 12 h, and 24 h after photobiomodulation. Capillary-like structure formation assay verified functional role. Two-way ANOVA/Tukey’s test and ANOVA/Bonferroni’s multiple comparisons test respectively verified cell viability/proliferation and intragroup and intergroup comparisons of protein synthesis (p < 0.05).
Results
Irradiated and non-irradiated HPFs showed statistically similar cell viability and proliferation pattern. Intragroup comparisons showed similar patterns of protein synthesis for all groups: VEGF-A, VEGF-C, and vascular endothelial growth factor receptor 1 (VEGFR1) increased significantly in the supernatant, while FGF-2 and VEGF-A increased significantly in the lysate. The lower fluence significantly increased BMP-9 (6 h) in the supernatant and VEGFR1 (6 h and 12 h) and VEGF-D (24 h) in the lysate, while the higher fluence significantly increased BMP-9 (6 h) in the supernatant and VEGFR1 (12 h) in the lysate. Regardless of the time, both fluences statistically downregulated placental growth factor (PLGF) and PDGF secretion. Both fluences statistically decreased VEGF-A secretion (24 h) and PLGF production (6 h).
Conclusion
Photobiomodulation produced stimulatory effects on angiogenic protein secretion by pulp fibroblasts. In terms of photobiomodulation, over time, both fluences significantly increased the secretion of VEGF-A, VEGF-C, and VEGFR1 and significantly upregulated BMP-9 (6 h) in the supernatant; for capillary-like structure formation, the fluence of 2.5 J/cm2 was better than the fluence of 3.7 J/cm2.
Clinical relevance
This study results addressed effective photobiomodulation parameters tailored for pulp angiogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Angiogenesis is the main process to form blood vessels in wound repair mediated by angiogenic molecules [1]. VEGF family proteins (vascular endothelial growth factor A (VEGF-A), vascular endothelial growth factor C (VEGF-C), vascular endothelial growth factor D (VEGF-D), and placenta growth factor (PLGF)) and receptors (vascular endothelial growth factor receptor 1 (VEGFR1) and vascular endothelial growth factor receptor 2 (VEGFR2)) regulate the biological activity response of the endothelial cells through proliferation, migration, vascular permeability, and angiogenesis [2]. Other angiogenic growth factors are fibroblast growth factor 2 (FGF-2), growth/differentiation factor 2 (BMP-9), platelet-derived growth factor (PDGF), and platelet endothelial cell adhesion molecule 1 (PECAM-1). FGF-2 and BMP-9 regulate angiogenesis [3]. PDGF has an indirect angiogenic effect by maintaining and stabilizing newly formed blood vessels [4]. The literature reports the PECAM-1 regulation of angiogenesis [5].
One of the pulp healing keystones is angiogenesis [6]. Pulp fibroblasts produce these angiogenic molecules and receptors for physiological angiogenesis in a paracrine manner, promoting endothelial cell chemotaxis, proliferation, and differentiation [7, 8]. Different stress conditions, such as caries or trauma, result in different compositions and concentrations of the secretome from pulp cells [9].
Photobiomodulation is the application of light to inhibit or stimulate biological cellular processes [10]. Aiming at pulp healing, photobiomodulation has been advocated as an alternative for vital pulp therapy of primary teeth [11,12,13,14]. However, the literature lacks a protocol regarding the most effective photobiomodulation parameters [13, 14]. Photobiomodulation biological effects depend on wavelength, dose, and application time [15], so that different fluences may result in different biological responses [16].
Therapies that keep pulp vitality after caries or trauma relies on the pulp tissue capable of regenerating [17]. From a biological point of view, pulp healing depends on extracellular matrix formation, neurogenesis, and angiogenesis, so these biological events should be assessed to determine effective photobiomodulation parameters tailored for maintaining pulp vitality. In this context, studies revealed effective photobiomodulation of pulp cell viability, proliferation, and gene expression of type 1 collagen by human pulpal fibroblasts (HPFs) [18,19,20].
Works from other fields show the photobiomodulation of angiogenic growth factor synthesis by mesenchymal stem cells from adipose tissue [21] and gingival fibroblasts [22]. Recently, the literature reports that photobiomodulation at 660 nm increases VEGF gene expression in fibroblasts [23], but little is known whether higher gene expression results in higher protein production and secretion. Thus, this study aimed to verify the effect on angiogenic growth factors produced and released by dental pulp fibroblasts after photobiomodulation. The null hypothesis was that photobiomodulation would increase the angiogenic growth factors accounting for pulp healing.
Material and methods
This study was submitted and approved by the institutional review board (protocol CAAE 54859816.1.0000.5417). Pulp fibroblasts were obtained from six teeth donated by six children regulated according to the ethical aspects as reported by the previous literature [18, 19, 24]. To overcome possible variation, all donors met the following inclusion criteria: children of both genders, age from 5 to 9 years, and with good general health and sound teeth indicated for extraction due to orthodontic reasons [19]. Children taking any type of medicines or with teeth with caries lesions were excluded [19].
Primary culture and characterization
Pulp fibroblasts from human primary teeth (HPFs) were obtained through primary culture. The establishment of the HPF primary culture was based on the previous literature [19, 24]. Following extraction, the tooth was stored in Dulbecco’s modified Eagle’s medium (DMEM) (Gibco; Thermo Fisher Scientific in Waltham, MA, USA) supplemented with 20% fetal bovine serum (FBS) (Gibco; Thermo Fisher Scientific in Waltham, MA, USA). Inside the laminar flow cabinet, in a Petri dish, the pulp tissue was removed; cut in small pieces; immersed in DMEM + 20% FBS supplemented with 600 μl of penicillin (Gibco; Thermo Fisher Scientific in Waltham, MA, USA), 300 μl of gentamicin (Gibco; Thermo Fisher Scientific in Waltham, MA, USA), and 100 μl of amphotericin B (Gibco; Thermo Fisher Scientific in Waltham, MA, USA); and incubated at 37 °C and 5% CO2 for 40 min [24]. Next, all tissue cuts were collected in a falcon tube and centrifuged at 1200 rpm for 5 min. The supernatant was discarded, and the pellet resuspended in new culture medium (DMEM + 20% FBS), placed in 25-cm2 culture flasks, and incubated at 37 °C and 5% CO2 [24]. The culture medium was changed at every 2 days.
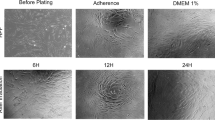
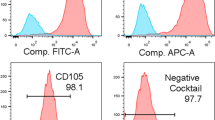
The dental pulp cells were characterized as fibroblasts by immunofluorescence staining [19]. A density of 1 × 104 cells/well was plated on 8-well chamber slides, led to adhere, fixed with 4% paraformaldehyde for 15 min, incubated in ammonium chloride solution for another 15 min, and washed with phosphate-buffered saline (PBS) + 3% bovine serum albumin (BSA) for 5 min at room temperature. The primary monoclonal antibody and anti-human fibroblast surface protein (anti-FSP) (Abcam, Cambridge, UK) at a final concentration of 2 μg/ml were used to mark the cells. The slides were analyzed through laser confocal microscopy (Leica TCS SPE, Mannheim, Germany) and demonstrated positive staining for fibroblasts.
Photobiomodulation irradiation
The study groups were divided according to different fluences (2.5 J/cm2–10 mW/10 s; 3.7 J/cm2–15 mW/10 s). In this study, we used a marketable aluminum-gallium-indium-phosphide (InGaAlP) diode laser (Twin Flex Evolution MM Optics®, São Carlos, Brazil), at 660 nm wavelength, collimated by the manufacturer, and a 0.04-cm2 laser tip output area, 0.225 cm laser tip diameter, and continuous mode were applied according to the study groups [18,19,20, 25]. The manufacturer assured the full utilization of the emitted power, without losses at the target. Fluence directed at a spot during the therapy was calculated by the following formula: F (J/cm2) = Energy (J) / Output area (cm2) [26]. Energy was calculated by Energy (J) = P (W) × t (s), where P is the power and t is the time during which the laser was used.
Based on previous studies [18, 19], a black mask covers the culture plate, and the distance between the laser beam and the cell culture was standardized at 1 mm from the bottom of the plate with the aid of a customized device to assure perpendicularity. The output power was checked by a radiometer (Laser Check MM Optics®, São Carlos/São Paulo, Brazil), prior to and after laser application, considering a low-level laser transmission loss of about 12% [27]. To avoid laser overexposure, we maintained the emptiness of the wells adjacent to each test well [18, 19].
Considering that the optically clear 96-well plate (cell and proliferation assay) has an area of 0.32 cm2/well, each well was irradiated in a single point [19]; for 24-well plates (protein immunoassay), each well (1.9 cm2/well) was irradiated in five equidistant points [25]. All irradiation procedures were accomplished in controlled temperature (± 24 °C) in a dark room. The control group (not irradiated) was exposed to the same conditions of the irradiation groups [18, 19].
Cell viability and proliferation assays
HPFs were used at 4th passage and a density of 1 × 104 cells/well and seeded in a 96-well plate (well area 0.32 cm2) with DMEM + 10% FBS. After 24 h, at 37 °C/5% CO2, the culture medium was replaced by DMEM + 1% FBS to synchronize the cell cycle prior to irradiation [18, 19]. After more 24 h, at 37 °C/5% CO2, prior to irradiation, the culture medium was replaced by DMEM without phenol red (Sigma Chemical Co., St. Louis, MO, USA) + 10% FBS [19]. The negative and positive controls had the same cell density and were maintained in DMEM without phenol red + 1% or + 10% FBS, respectively [18,19,20]. Groups were plated in triplicate, and the assays were repeated three times as in previous studies [18, 19].
Cell viability was analyzed by 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) (Sigma-Aldrich Co., St. Louis, MO, USA), at 6 h, 12 h, and 24 h after irradiation. After the removal of the culture medium, HPFs were washed with PBS 1×. Next, 110 μl of MTT solution (0.5 mg/ml in DMEM) was added to each well. Plates were covered with aluminum foil and incubated at 37 °C and 5% CO2 for 4 h. Elapsed that period, MTT solution was removed and 200 μl of dimethyl sulfoxide (DMSO; Fisher Scientific, Hampton, VA, USA) was added per well. The absorbance was determined in a spectrophotometer (Synergy H1 MultiMode Reader; BioTek, Winooski, Vermont, USA) at 570 nm wavelength [19].
Cell proliferation was analyzed by crystal violet assay, at 6 h, 12 h, and 24 h after irradiation. The culture medium was removed, and HPFs were washed with PBS 1×. Methanol (methyl alcohol 99.8%, Vetec; Sigma-Aldrich, Duque de Caxias, RJ, Brazil) was added to each well for 10 min. After that, crystal violet solution was added to each well for 3 min. Then, HPFs were washed twice with PBS 1×. The HPFs received sodium citrate (0.05 mol/l) for 10 min. The absorbance was determined in a spectrophotometer (Synergy H1 MultiMode Reader; BioTek, Winooski, Vermont, USA) at 540 nm wavelength [19]. Cell proliferation assay was repeated three times with a washout period of 1 week [19].
Protein immunoassay
There were 2 × 104 cells/well seeded in a 24-well plate (code 3524, polystyrene; Corning, NY, USA; well area 1.9 cm2) with DMEM + 10% FBS and incubated at 37 °C and 5% CO2, for 24 h to adhere. The culture medium was replaced by DMEM + 1% FBS to synchronize the cell cycle prior to irradiation and achieve proliferative deficit [18, 19]. After 24 h, prior to irradiation, the culture medium was replaced by DMEM without phenol red + 10% FBS for all groups [18, 19]. Groups were plated in triplicate, and the assays were repeated three times as previous studies [18, 19].
After 6 h, 12 h, and 24 h, the supernatant of all groups was collected and stored for the analysis. After the collection of the supernatant, 300 μl/well of lysis solution (CelLytic M, Sigma-Aldrich, C2978-50ML) was dispensed to obtain the chemical lysis. Also, the mechanical lysis was performed by scratching the pipette tip. The lysate of all groups was collected and stored for analysis.
The following panels were used to verify the protein synthesis and secretion of VEGF-A, VEGF-C, VEGF-D, VEGFR1, VEGFR2, FGF2, PLGF, PDGF, PECAM-1, and BMP-9 at 6 h, 12 h, and 24 h after irradiation, in the lysate and supernatant: HAGP1MAG-12K (MILLIPLEX® MAP Human Angiogenesis Panel 1) and HANG2MAG-12K (MILLIPLEX® MAP Human Angiogenesis Panel 2) (Merck Millipore, Darmstadt, Germany). All samples, quality control samples, and standards were prepared as recommended in the MILLIPLEX® map assay kit protocols with supplied diluents, following the manufacturer’s instructions. The assay plate was then analyzed with the Luminex® instrument equipped with xPONENT® and Multiplex Analyst 5.1 software (Merck Millipore, Darmstadt, Germany). The results were obtained in pg/ml.
Capillary-like structure formation assay
Human umbilical vein endothelial cells (HUVECs) were plated on 24-well plates at 1 × 104 cells/well [28,29,30]. After 24 h for adhesion, HUVEC were treated with 1 ml/well of conditioned medium with aliquots of the supernatants secreted by HPFs after the irradiation with both fluences at 6 h. The conditioned medium was obtained with equal proportions of Dulbecco’s modified Eagle’s medium/Nutrient Mixture F-12 (Gibco; Thermo Fisher Scientific in Waltham, MA, USA) (DMEM/F-12) + 10% FBS and supernatant aliquots. The control group was maintained in DMEM/F-12 + 10% FBS. The cells were observed at every 24 h in optical microscopic. After 96 h, the cells were fixed and stained by hematoxylin-eosin for descriptive analysis.
Statistical analysis
All statistical analyses were obtained with the level of significance of 5%. Intragroup and intergroup comparisons of cell viability and proliferation were analyzed by two-way ANOVA followed by Tukey’s test (Statistica 10.0 software for Windows). Intragroup (time) and intergroup (fluences) comparisons of the protein immunoassay were analyzed by two-way ANOVA followed by Bonferroni’s multiple comparisons test for each protein separately (Prism GraphPad 7 for Windows).
Results
Cell viability and proliferation assays
The intragroup comparison showed that cell viability statistically decreased over time for all groups (p < 0.001). The intergroup comparison revealed that the negative control statistically showed the smallest viability mean (p < 0.001; Fig. 1a). Cell proliferation did not show statistically significant differences over time (p = 0.2046). The negative control group showed statistically significant lower proliferation than the positive control group (p = 0.0276; Fig. 1b).
Protein immunoassay
Intragroup comparison
In the control group, HPFs produced and secreted all the tested proteins before photobiomodulation, except for PDGF in the lysate. Non-irradiated HPFs secreted higher levels of VEGF-A, VEGF-C, and VEGFR2, but low levels of FGF-2, PDGF, VEGFR1, PECAM-1, VEGF-D, PLGF, and BMP-9 in the supernatant (Table 1). In the lysate, non-irradiated HPFs produced higher levels of FGF-2, VEGF-C, and VEGFR2, but lower levels of VEGFR1, VEGF-A, PECAM-1, VEGF-D, PLGF, and BMP-9 (Table 1). Over time, VEGF-A, VEGF-C, VEGFR1, and BMP-9 by non-irradiated HPFs increased significantly in the supernatant, while FGF-2 and VEGF-A increased significantly in the lysate (p < 0.05). In the supernatant of non-irradiated HPF, VEGFR2 and PLGF decreased the secretion over time, while FGF-2 had a peak of maximum secretion at 12 h and PDGF, PECAM-1, VEGF-D, and BMP-9 had different secretion patterns, but without statistically significant differences (p > 0.05). In the lysate of non-irradiated HPFs, VEGFR2, VEGF-C, and VEGFR1 decreased the synthesis over time, while PECAM1, VEGF-D, PLGF, and BMP-9 were constant, but without statistically significant differences (p > 0.05).
HPFs irradiated with 2.5 J/cm2 produced and secreted all tested proteins, except for PDGF in the lysate. The quantification of the proteins in both the supernatant and lysate after irradiation with 2.5 J/cm2 showed a pattern similar to that of the control group. Over time, VEGF-A, VEGF-C, and VEGFR1 increased significantly in the supernatant (p < 0.05), while FGF-2, VEGF-A, and VEGF-D increased significantly in the lysate (p < 0.05) (Table 2). The other angiogenic proteins had different patterns of synthesis and secretion over time, but without statistically significant differences (p > 0.05) (Table 2).
HPFs irradiated with 3.7 J/cm2 produced and secreted all tested proteins, except for PDGF in the lysate. The quantification of the proteins in both the supernatant and lysate after irradiation with 3.7 J/cm2 showed a pattern similar to that of the control group (Table 3). Over time, VEGF-A, VEGF-C, and VEGFR1 increased significantly in the supernatant (p < 0.05), while FGF-2 and VEGF-A increased significantly in the lysate after irradiation with 3.7 J/cm2 (p < 0.05) (Table 3). The other proteins had different patterns of synthesis and secretion over time, but without statistically significant differences (p > 0.05) (Table 3).
Intergroup comparison
The results were normalized and expressed as percentage of controls. In the supernatant, at 6 h, the both fluences significantly increased BMP-9 secretion (Fig. 2). A significant decrease of PLGF occurred in the supernatant with both fluences, at 6 h (Fig. 2). At 12 h, both fluences significantly downregulated the secretion of PLGF (Fig. 3). At 24 h, VEGF-A, VEGF-C, PDGF, and PLGF secretion significantly decreased after photobiomodulation application with 2.5 J/cm2, while the fluence of 3.7 J/cm2 significantly downregulated VEGF-A, PDGF, and PLGF secretion (Fig. 4).
In the lysate, at 6 h, the fluence of 3.7 J/cm2 significantly decreased VEGFR1 production compared with 2.5 J/cm2 and the control group (Fig. 2). Statistically significantly lower values of PLGF production occurred at 6 h in the lysate for both fluences (Fig. 2). Both fluences significantly decreased BMP-9 production in the lysate, 12 h after photobiomodulation (Fig. 3). At 24 h, VEGF-D production in the lysate significantly increased after photobiomodulation with 2.5 J/cm2 (Fig. 4).
Capillary-like structure formation assay
HUVECs treated with the conditioned medium with the supernatant released by HPFs irradiated with both fluences showed capillary-like structure formation (Fig. 5) compared with those maintained in the culture medium + 10% FBS. The supernatant obtained after the irradiation with the fluence of 2.5 J/cm2 (Fig. 5a) showed more frequent capillary-like structure formation than with the fluence of 3.7 J/cm2 (Fig. 5b).
Discussion
This study showed the inhibitory and stimulatory photobiomodulation of the main angiogenic factors in the supernatant and lysate by pulp fibroblasts. Despite some differences in the results, both fluences resulted in capillary-like structure formation. To the best of our knowledge, this is the first study addressing the synthesis and secretion of angiogenic proteins by pulp fibroblasts after photobiomodulation, which makes comparisons difficult.
In terms of photobiomodulation, the lower fluence significantly upregulated BMP-9 in the supernatant at 6 h and VEGF-D in the lysate at 24 h. The higher fluence significantly upregulated BMP-9 in the supernatant at 6 h. In general, stimulatory photobiomodulation of angiogenic factors occurs due to nitric oxide modulation [23] through nitric oxide production synthase via activation of PLCϒ-Ca-dependent influx [31, 32]. At 6 h, the statistically increased secretion of BMP-9 may have led to the inhibition of other angiogenic factors as VEGF-A and its isoforms because BMP-9 suppresses VEGF expression by activating VEGFR1 [33]. VEGF isoforms have negative and positive feedback mechanisms with their related receptors, and VEGFR1 is the main mediator, so VEGF upregulation increases VEGFR1 availability [3, 8]. VEGFR1 controls vascular biology acting as “VEGF trap” by sequestering VEGF isoforms away from VEGFR2 and forming non-signaling VEGFR1-VEGFR2 heterodimer through dimerization, transphosphorylation, and regulation of expression levels, in a negative feedback cycle [3, 8, 34, 35].
In the supernatant, at 24 h after photobiomodulation, the secretion of VEGF-A was statistically lower than that of the control group for the fluence of 2.5 J/cm2 and 3.7 J/cm2. The regulation of VEGF family proteins and receptors is a complex interplay. Many factors regulated VEGF synthesis: VEGFR1 and BMP-9 (as mentioned above) [3, 8, 33,34,35], VEGF bioavailability through either plasmin cleavage or extracellular proteolysis [3], splicing of VEGF proteins affecting temporal and spatial distribution [35], FGF controlling of VEGF upstream [3], and VEGFR2 binding to integrin [3, 29, 35]. Integrin is a transmembrane heterodimer that mediates cell-matrix adhesion through binding to extracellular proteins, such as collagen, fibronectin, and laminin [35]. Integrin recruitment qualitatively modulates the signaling of VEGF receptors [35], and the VEGFR2 binding to integrin prevents aberrant angiogenesis stimulation [3]. Photobiomodulation increases COL1 gene expression by HPFs [18]. Collagen 1 downregulates the VEGF-A-mediated activation of VEGFR2 through phosphatase SHP2 recruitment [35]. As demonstrated by Table 2, the irradiated and non-irradiated groups showed the same cell viability and proliferation pattern, excluding the probability that the fluctuation of the protein quantity, in this study, would have been caused by HPF death in later periods. Taken together, this information suggests the crosstalk between proteins and receptors of the VEGF signaling cascade.
Both fluences downregulated PDGF and PLGF in the supernatant and lysate. The literature lacks studies on the protein synthesis and secretion of PLGF by pulp fibroblasts. Studies on angiogenesis show that PLGF plays a crucial role in inflammation-associated angiogenesis by recruiting inflammatory cells, mediated by binding VEGFR1 [3, 34]. The literature reported an increase in PDGF levels after photobiomodulation, but with different wavelengths (1064 nm) and fluences (1.6 J/cm2) on different cells (palatal tissue) [36, 37]. Works from other fields highlighted the inhibitory effect of photobiomodulation in PDGF-stimulated cells [38]. Although Rombouts et al. [9] report the increase of PDGF transcription by pulp cells, we did not find the same protein transduction in this study.
The methodology of this study was based on previous research using 660-nm wavelength [18,19,20, 23]. Before photobiomodulation, HPFs secreted and produced all the tested angiogenic factors, except for PDGF in the lysate, which agrees with the literature [39, 40]. Other studies show that to simulate pulp stress conditions, either hypoxia or serum deprivation leads to different angiogenic secretions by pulp cells [9, 41,42,43]. This would explain the synthesis of angiogenic proteins by non-irradiated HPFs in this present study.
Although this study used HPFs, the results have the inherent limitations of an in vitro study. At this point, this study provided two fluences tailored for pulp angiogenesis. However, further studies are necessary to verify the photobiomodulation effect of these doses on different pulp cells and on the control of pulp inflammation and to elucidate other molecular mechanisms of the angiogenesis of pulp healing to help in developing photobiomodulation-mediated strategies.
To sum up, photobiomodulation with either 2.5 J/cm2 or 3.7 J/cm2 produced stimulatory and inhibitory effects on angiogenic protein production and secretion by pulp fibroblasts, resulting in capillary-like structure formation.
Conclusion
Photobiomodulation produced stimulatory effects on angiogenic protein secretion by pulp fibroblasts. In terms of photobiomodulation,
-
Over time, both fluences significantly increased the secretion of VEGF-A, VEGF-C, and VEGFR1;
-
Both fluences significantly upregulated BMP-9 (6 h) in the supernatant;
-
For capillary-like structure formation, the fluence of 2.5 J/cm2 was better than the fluence of 3.7 J/cm2.
References
Folkman J, Shing Y (1992) Angiogenesis. J Biol Chem 267(16):10931–10934
Smith GA, Fearnley GW, Harrison MA, Tomlinson DC, Wheatcroft SB, Ponnambalam S (2015) Vascular endothelial growth factors: multitasking functionality in metabolism, health and disease. J Inherit Metab Dis 38(4):753–763. https://doi.org/10.1007/s10545-015-9838-4
Simons M, Gordon E, Claesson-Welsh L (2016) Mechanisms and regulation of endothelial VEGF receptor signalling. Nat Rev Mol Cell Biol 17(10):611–625. https://doi.org/10.1038/nrm.2016.87
Zhang M, Jiang F, Zhang X, Wang S, Jin Y, Zhang W, Jiang X (2017) The effects of platelet-derived growth factor-BB on human dental pulp stem cells mediated dentin-pulp complex regeneration. Stem Cells Transl Med 6(12):2126–2134. https://doi.org/10.1002/sctm.17-0033
Marques NCT, Neto NL, Prado MTO, Vitor LLR, Rodini CO, Sakai VT, Machado MAAM, Santos CF, Oliveira TM (2018) CD31 expression in human primary teeth treated with photobiomodulation therapy. Laser Dent Sci 2(2):103–108
Cooper PR, Holder MJ, Smith AJ (2014) Inflammation and regeneration in the dentin-pulp complex: a double-edged sword. J Endod 40(4 Suppl):S46–S51. https://doi.org/10.1016/j.joen.2014.01.021
Chmilewsky F, Jeanneau C, Laurent P, About I (2014) Pulp fibroblasts synthesize functional complement proteins involved in initiating dentin-pulp regeneration. Am J Pathol 184(7):1991–2000. https://doi.org/10.1016/j.ajpath.2014.04.003
Smith Gina A, Fearnley Gareth W, Tomlinson Darren C, Harrison Michael A, Ponnambalam S (2015) The cellular response to vascular endothelial growth factors requires co-ordinated signal transduction, trafficking and proteolysis. Biosci Rep 35(5):e00253. https://doi.org/10.1042/BSR20150171
Rombouts C, Giraud T, Jeanneau C, About I (2017) Pulp vascularization during tooth development, regeneration, and therapy. J Dent Res 96(2):137–144. https://doi.org/10.1177/0022034516671688
Hadis MA, Zainal SA, Holder MJ, Carroll JD, Cooper PR, Milward MR, Palin WM (2016) The dark art of light measurement: accurate radiometry for low-level light therapy. Lasers Med Sci 31(4):789–809. https://doi.org/10.1007/s10103-016-1914-y
Marques NC, Neto NL, Rodini Cde O, Fernandes AP, Sakai VT, Machado MA, Oliveira TM (2015) Low-level laser therapy as an alternative for pulpotomy in human primary teeth. Lasers Med Sci 30(7):1815–1822. https://doi.org/10.1007/s10103-014-1656-7
Smail-Faugeron V, Glenny AM, Courson F, Durieux P, Muller-Bolla M, Fron Chabouis H (2018) Pulp treatment for extensive decay in primary teeth. Cochrane Database Syst Rev 5:Cd003220. https://doi.org/10.1002/14651858.CD003220.pub3
Nematollahi H, Shirazi AS, Mehrabkhani M, Sabbagh S (2018) Clinical and radiographic outcomes of laser pulpotomy in vital primary teeth: a systematic review and meta-analysis. Eur Arch Paediatr Dent 19(4):205–220. https://doi.org/10.1007/s40368-018-0358-4
Ansari G, Safi Aghdam H, Taheri P, Ahsaie MG (2018) Laser pulpotomy-an effective alternative to conventional techniques-a systematic review of literature and meta-analysis. Lasers Med Sci 33(8):1621–1629. https://doi.org/10.1007/s10103-018-2588-4
Karu T (1989) Photobiology of low-power laser effects. Health Phys 56(5):691–704
Huang YY, Chen AC, Carroll JD, Hamblin MR (2009) Biphasic dose response in low level light therapy. Dose-Response 7(4):358–383. https://doi.org/10.2203/dose-response.09-027.Hamblin
Coll JA, Seale NS, Vargas K, Marghalani AA, Al Shamali S, Graham L (2017) Primary tooth vital pulp therapy: a systematic review and meta-analysis. Pediatr Dent 39(1):16–123
Vitor LLR, Prado MTO, Lourenço-Neto N, Oliveira RC, Santos CF, Machado MAAM, Oliveira TM (2018) Photobiomodulation changes type 1 collagen gene expression by pulp fibroblasts. Laser Phys 28(6):065603
Marques NCT, Lourenço-Neto N, Prado MTO, Vitor LLR, Oliveira RC, Sakai VT, Santos CF, Machado M, Oliveira TM (2017) Effects of photobiomodulation in different energy densities and irradiance on maintaining cell viability and proliferation of pulp fibroblasts from human primary teeth. Lasers Med Sci 32(7):1621–1628. https://doi.org/10.1007/s10103-017-2301-z
Fernandes A, Lourenço-Neto N, Marques NCT, Vitor LLR, Prado MTO, Oliveira RC, Machado MAAM, Oliveira TM (2018) Cellular response of pulp fibroblast to single or multiple photobiomodulation applications. Laser Phys 28(6):065604
Oliveira TS, Serra AJ, Manchini MT, Bassaneze V, Krieger JE, de Tarso Camillo de Carvalho P, Antunes DE, Bocalini DS, Ferreira Tucci PJ, Silva JA Jr (2015) Effects of low level laser therapy on attachment, proliferation, and gene expression of VEGF and VEGF receptor 2 of adipocyte-derived mesenchymal stem cells cultivated under nutritional deficiency. Lasers Med Sci 30(1):217–223. https://doi.org/10.1007/s10103-014-1646-9
Damante CA, De Micheli G, Miyagi SP, Feist IS, Marques MM (2009) Effect of laser phototherapy on the release of fibroblast growth factors by human gingival fibroblasts. Lasers Med Sci 24(6):885–891. https://doi.org/10.1007/s10103-008-0582-y
Szezerbaty SKF, de Oliveira RF, Pires-Oliveira DAA, Soares CP, Sartori D, Poli-Frederico RC (2018) The effect of low-level laser therapy (660 nm) on the gene expression involved in tissue repair. Lasers Med Sci 33(2):315–321. https://doi.org/10.1007/s10103-017-2375-7
Lourenço-Neto N, Pereira LF, Marques NCT, Prado M, Vitor LLR, Tokuhara CK, Oliveira RC, Machado MAAM, Oliveira TM (2017) Storage protocol of dental pulp cells from human exfoliated deciduous teeth. Braz Dent Sci 20(3):126–131
Ferreira LS, Diniz IMA, Maranduba CMS, Miyagi SPH, Rodrigues M, Moura-Netto C, Marques MM (2019) Short-term evaluation of photobiomodulation therapy on the proliferation and undifferentiated status of dental pulp stem cells. Lasers Med Sci 34(4):659–666. https://doi.org/10.1007/s10103-018-2637-z
Laakso L, Richardson C, Cramond T (1993) Factors affecting low level laser therapy. Aust J Physiother 39(2):95–99. https://doi.org/10.1016/s0004-9514(14)60473-6
Damante CA, Marques MM (2014) Laser power loss through polystyrene plates for cell culture. Lasers Med Sci 29(1):373. https://doi.org/10.1007/s10103-013-1271-z
Zhao M, Bai H, Wang E, Forrester JV, McCaig CD (2004) Electrical stimulation directly induces preangiogenic responses in vascular endothelial cells by signaling through VEGF receptors. J Cell Sci 117(Pt 3):397–405
Liu J, Deng YH, Yang L, Chen Y, Lawali M, Sun LP, Liu Y (2015) CPU-12, a novel synthesized oxazolo[5,4-d]pyrimidine derivative, showed superior anti-angiogenic activity. J Pharmacol Sci 129(1):9–17
Simara P, Tesarova L, Rehakova D, Farkas S, Salingova B, Kutalkova K, Vavreckova E, Matula P, Matula P, Veverkova L, Koutna I (2018) Reprogramming of adult peripheral blood cells into human induced pluripotent stem cells as a safe and accessible source of endothelial cells. Stem Cells Dev 27(1):10–22
Fraisl P (2013) Crosstalk between oxygen- and nitric oxide-dependent signaling pathways in angiogenesis. Exp Cell Res 319(9):1331–1339. https://doi.org/10.1016/j.yexcr.2013.02.010
Koch S, Tugues S, Li X, Gualandi L, Claesson-Welsh L (2011) Signal transduction by vascular endothelial growth factor receptors. Biochem J 437(2):169–183. https://doi.org/10.1042/bj20110301
Shao ES, Lin L, Yao Y, Bostrom KI (2009) Expression of vascular endothelial growth factor is coordinately regulated by the activin-like kinase receptors 1 and 5 in endothelial cells. Blood 114(10):2197–2206. https://doi.org/10.1182/blood-2009-01-199166
Claesson-Welsh L (2016) VEGF receptor signal transduction – a brief update. Vasc Pharmacol 86:14–17. https://doi.org/10.1016/j.vph.2016.05.011
Koch S, Claesson-Welsh L (2012) Signal transduction by vascular endothelial growth factor receptors. Cold Spring Harb Perspect Med 2(7):a006502. https://doi.org/10.1101/cshperspect.a006502
Keskiner I, Lutfioglu M, Aydogdu A, Saygun NI, Serdar MA (2016) Effect of photobiomodulation on transforming growth factor-beta1, platelet-derived growth factor-BB, and interleukin-8 release in palatal wounds after free gingival graft harvesting: a randomized clinical study. Photomed Laser Surg 34(6):263–271. https://doi.org/10.1089/pho.2016.4094
Tim CR, Pinto KN, Rossi BR, Fernandes K, Matsumoto MA, Parizotto NA, Renno AC (2014) Low-level laser therapy enhances the expression of osteogenic factors during bone repair in rats. Lasers Med Sci 29(1):147–156. https://doi.org/10.1007/s10103-013-1302-9
Baek S, Lee KP, Cui L, Ryu Y, Hong JM, Kim J, Jung SH, Bae YM, Won KJ, Kim B (2017) Low-power laser irradiation inhibits PDGF-BB-induced migration and proliferation via apoptotic cell death in vascular smooth muscle cells. Lasers Med Sci 32(9):2121–2127. https://doi.org/10.1007/s10103-017-2338-z
Caviedes-Bucheli J, Gomez-Sosa JF, Azuero-Holguin MM, Ormeno-Gomez M, Pinto-Pascual V, Munoz HR (2017) Angiogenic mechanisms of human dental pulp and their relationship with substance P expression in response to occlusal trauma. Int Endod J 50(4):339–351. https://doi.org/10.1111/iej.12627
Chang Y-C, Chang M-C, Chen Y-J, Liou J-U, Chang H-H, Huang W-L, Liao W-C, Chan C-P, Jeng P-Y, Jeng J-H (2017) Basic fibroblast growth factor regulates gene and protein expression related to proliferation, differentiation, and matrix production of human dental pulp cells. J Endod 43(6):936–942. https://doi.org/10.1016/j.joen.2017.01.024
Aranha AM, Zhang Z, Neiva KG, Costa CA, Hebling J, Nor JE (2010) Hypoxia enhances the angiogenic potential of human dental pulp cells. J Endod 36(10):1633–1637. https://doi.org/10.1016/j.joen.2010.05.013
Bakopoulou A, Kritis A, Andreadis D, Papachristou E, Leyhausen G, Koidis P, Geurtsen W, Tsiftsoglou A (2015) Angiogenic potential and secretome of human apical papilla mesenchymal stem cells in various stress microenvironments. Stem Cells Dev 24(21):2496–2512. https://doi.org/10.1089/scd.2015.0197
Mignon C, Uzunbajakava NE, Raafs B, Botchkareva NV, Tobin DJ (2017) Photobiomodulation of human dermal fibroblasts in vitro: decisive role of cell culture conditions and treatment protocols on experimental outcome. Sci Rep 7(1):2797. https://doi.org/10.1038/s41598-017-02802-0
Acknowledgments
The authors thank Evandro José Dionisio (in memoriam), Thiago Dionisio, and Cintia Kazuko Tokuhara for their laboratorial assistance.
Funding
This study was funded by Sao Paulo Research Foundation (FAPESP) (grant nos. 2018/20316-6 and 2017/11396-3).
Author information
Authors and Affiliations
Contributions
Luciana Lourenço Ribeiro Vitor participated in the study design, performed the analyses, and drafted the manuscript.
Mariel Tavares Oliveira Prado Bergamo performed the analyses and drafted the manuscript.
Natalino Lourenço-Neto participated in the study design, helped in analyzing the results, and drafted the manuscript.
Vivien Thiemy Sakai participated in the study design, helped in analyzing the results, and drafted the manuscript.
Rodrigo Cardoso Oliveira participated in the study design, helped in analyzing the results, and drafted the manuscript.
Thiago Cruvinel helped in the analyses and drafted the manuscript.
Daniela Rios helped in the analyses and drafted the manuscript.
Gustavo Pompermaier Garlet participated in the study design, helped in analyzing the results, and drafted the manuscript.
Carlos Ferreira Santos helped in analyzing the results and drafted the manuscript.
Maria Aparecida Andrade Moreira Machado participated in the study design and drafted the manuscript.
Thais Marchini Oliveira conceived the study, participated in the study design, and drafted the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards (protocol CAAE 54859816.1.0000.5417).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vitor, L.L.R., Bergamo, M.T.O.P., Lourenço-Neto, N. et al. Photobiomodulation effect on angiogenic proteins produced and released by dental pulp cells. Clin Oral Invest 24, 4343–4354 (2020). https://doi.org/10.1007/s00784-020-03298-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03298-1