Abstract
Objectives
This retrospective study analyzed restoration survival of composite fillings in children with at high caries risk in relation to age, sex, operator, tooth type, filling extension, and material used.
Materials and methods
Among 667 children treated in 2004–2012 in a university setting without sedation or general anesthesia, 2388 composite fillings were included. Relevant data from regular recall intervals were retrieved from patients’ records. Either total-etch or a self-etch adhesive combined with flowable and/or (nano)hybrid composite was used. The Kaplan-Meier estimator and Cox proportional hazard analysis with backward elimination model were applied for survival analysis.
Results
For the observation period of 8 years (mean 1.7 years), the cumulative failure rate was 17.2 % with annual failure rates of 10.0 %. In 8.8 % of the cases, fillings failed due to secondary caries. In 8.3 % technical failure due to total filling loss, loosening, marginal gaps, or tooth fracture occurred. Tooth type, filling extension, age, operator, dental dam, and type of adhesive were significant for survival (p < 0.05).
Conclusions
Filling survival was comparably lower to composite restorations observed in prospective clinical studies on permanent teeth and other tooth-colored restoratives used in primary teeth. Due to the very high caries risk and young age of the population, frequent loss due to secondary caries was observed. With respect to the high caries risk, composite restorations can be used to treat carious primary teeth, though a strict caries prevention regimen should be followed to minimize restoration failure.
Clinical relevance
Filling loss of composites in the primary dentition is associated with secondary caries on the long term.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Children suffering from caries are at continuing risk of developing caries in the future [1–3]. In addition to the implementation of sufficient preventive dental care, it is necessary to provide the patient with high-quality, long-lasting treatment options that will reduce the need for repeated treatment, pain, or swelling [1, 4]. Different filling materials, such as amalgam, glass ionomer cement, compomer, and composite for smaller lesions or stainless steel crowns for full coverage of teeth with extended or multi-surface lesions, are the treatment options of choice for carious lesions in the primary dentition [5–7]. Concerns about the use of amalgam in the pediatric population have been raised over the last few decades. This concern has led to the prohibition of amalgam in some European countries, and in others, the use of non-amalgam options to treat children and other vulnerable patient groups has been strongly recommended [8–10]. In general, tooth-colored fillings like glass-ionomer, compomere, or composite have been gaining increasing popularity over the last few decades as an alternative to amalgam in restorative dentistry, and they have become part of the dental teaching curricula in many countries [11–17]. Currently, high-quality composites are available on the market that provides good handling and functional performance in addition to meeting patients’ demands regarding esthetics, especially for the anterior teeth. Additionally, composites are frequently used in pediatric dentistry to restore carious lesions in primary teeth [18]. Numerous in vivo and in vitro studies have shown that composite fillings are a durable, long-lasting restoration option for cavities in the permanent dentition [19]. A large, retrospective study under clinical conditions showed that composite restorations were suitable for use as an effective long-term treatment option for large and multi-surface cavities [20]. Kopperud et al. showed in a prospective practice-based study that the longevity of composite fillings in permanent teeth was less than that of amalgam, but they had a survival probability of nearly 90 % after 3 years and approximately 70 % after 6 years [21]. For permanent teeth situated in mixed and young permanent dentition, a cumulative survival rate of 84 % for composite fillings that had been followed prospectively for 8 years was recently reported [22]. However, long-term data on the performance and longevity of composites as restoration materials in the primary dentition remain sparse [5, 7, 23].
Therefore, this study aimed to acquire information in a pediatric population regarding the longevity of composite fillings with regard to (1) patients’ sex and age; (2) operator; and (3) tooth type, filling extension, and restoration technique.
Materials and methods
The approval of the ethics committee of the medical faculty of the university was obtained (project no. 030-13) for this retrospective study, and the study was conducted in accordance with the Declaration of Helsinki.
Study population
The records of all patients treated for dental caries in primary teeth between January 1, 2004, and December 31, 2012, in the Pediatric Division of the Department of Conservative Dentistry were screened for composite restorations. Patients undergoing treatment for caries in the primary or mixed dentition were exclusively recruited as the study population. A total of 2388 fillings placed by eight different operators in 667 patients met the following inclusion and exclusion criteria.
Inclusion criteria
All composite restorations exclusively placed due to primary caries were selected. Fillings had to be placed by dentists of the pediatric division of the department, with either a total etch or self-etching system and a flowable and/or universal micro- or nano-hybrid composite. In addition, all patients had to be part of a postoperative follow-up system for at least six months.
Exclusion criteria
Fillings that were placed due to other reasons, such as filling loss, secondary caries, or hypomineralization or hypoplasia of the tooth, were excluded from the study. Any restorations that were performed under general anesthesia or sedation were not considered. On molars that showed extensive destruction, either stainless steel crowns were placed or extraction was performed. These teeth were not part of this study. No other exclusion criteria were applied.
Treatment protocol
The treatment procedures were chosen according to the recommendations of the current guidelines and policies of the American Association of Pediatric Dentistry [24]. All of the patients underwent a desensitization process prior to operative care and were considered to be sufficiently cooperative to be eligible for a chair-side composite restoration performed without sedation. Bitewing or apical X-rays were obtained preoperatively for treatment-related caries diagnosis and/or exclusion of interradicular or periapical infections, if necessary. All of the radiographs were obtained in accordance with the ethics committee and national radiological regulations and the Guidelines of the European Academy of Pediatric Dentistry [25–27]. Depending on the location and depth of the filling, local anesthesia was applied to provide appropriate analgesia of the operating field if considered necessary. Composite fillings were chosen for single- or multi-surface primary incisors or canine lesions. If multi-surface lesions were small on molars, they were also filled with composite.
Prior to restorative treatment, all of the teeth were cleaned using a polishing brush and prophylaxis paste (Zircate® Prophy Paste, Dentsply DeTrey, York, PA, USA). The standardized treatment protocol consisted of adequate isolation of the affected and adjacent teeth with either a dental dam or cotton rolls and the preparation of a defect-oriented, small, and unbeveled access cavity using a high-speed diamond-coated bur with water cooling.
Caries excavation was performed using a low-speed tungsten carbide bur (Gebr. Brassler, Lemgo, Germany) or hand excavation (Hu-Friedy, Rotterdam, Netherlands). Cavity margins were accepted for filling only if they were caries free. Caries removal near the pulp was considered to be sufficient if the remaining dentin was discolored but hard. In addition, in cases with deep caries near the pulp, a calcium hydroxide paste (UltraCal® XS, Ultradent, South Jordan, UT, USA) and a calcium hydroxide liner (Life®, Kerr, Orange, CA, USA) were placed prior to etching and filling. In cases of pulp exposure, a pulpotomy was performed using a medical Portland cement (ProRoot® MTA, Dentsply De Trey, York, PA, USA) or reinforced zinc oxide-eugenol material (IRM® Dentsply De Trey, York, PA, USA) after hemostasis had been achieved by the application of 15.5 % ferric sulfate solution (Astringident®, Ultradent, South Jordan, UT, USA) for 20 s. For lesions comprising the approximal surfaces, a matrix (AutoMatrix®, Dentsply De Trey, York, PA, USA) was placed and adapted using a wooden wedge. Enamel and dentin bonding was achieved either via a total-etch technique with 37.5 % phosphoric acid (Total Etch®, Ivoclar Vivadent, Shaan, Liechtenstein) combined with a dentin adhesive (Syntac Classic®, Ivoclar Vivadent, Shaan, Liechtenstein) or with a self-etching adhesive (Clearfil™ SE Bond, Kuraray Noritake Dental Inc., Tokyo, Japan). The majority of cavities were filled with a flowable (Tetric Flow® or Tetric EvoFlow®, A1, Ivoclar Vivadent, Shaan, Liechtenstein) or universal micro- or nano-hybrid (Tetric Ceram®, Tetric EvoCeram®, A1, Ivoclar Vivadent, Shaan, Liechtenstein) composite or a combination of both materials. Increments of a maximum height of 2 mm were cured separately for 40 s. A rubber polisher and paste (Enhance®, Dentsply Caulk, Milford, DE, USA) were used to finish and polish the filling surfaces. Occlusion and articulation were assessed.
Follow-up
Follow-up visits for caries-preventive purposes consisted of visual inspection according to WHO standards, oral hygiene instruction for the child and parents, professional cleaning, nutritional advice, radiographs if indicated, and fluoride varnish application. Depending on the individual caries risk, follow-ups were scheduled three to four times a year.
Failure assessment
The overall observation time was 8 years with a mean observation time of 1.71 years. The overall annual failure rate was calculated by dividing the total number of failures by the total number of restorations divided by the average observation time in years.
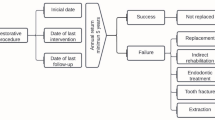
Other dentists than the operators in this study performed the filling assessment. Two graduated dentists collected the data independently and discussed questionable results with an experienced pediatric dentist. All operators were solely active in the pediatric division of the department. Operators 1 and 5 were holding a certificate for a 3-year university-based training in pediatric dentistry within the observation period, whereas the other operators were gaining experience and training in this field. FDI criteria 2–6, 9, and 11–14 were applied for the determination of clinical failure of the fillings. Data on fillings were classified according to the FDI criteria and were judged as “success” when rated as clinically very good, good, or sufficient/satisfactory and as “failure” when rated as clinically unsatisfactory or poor [28]. The restorations were recorded as having lost if they had to be repaired or replaced with 395 failures remaining (395/2388; 16.5 %) for analysis. If the tooth was extracted with an intact filling for endodontic or orthodontic reasons or if the filling was present when the tooth exfoliated physiologically, the filling was recorded as censored. For censored patients, the observation period was defined as the time point when the restored tooth was last examined with an intact filling.
Statistics
Data were collected and sorted using Microsoft Excel software (Microsoft Office®, Excel 2010®, Unterschleißheim, Germany) and were subsequently exported into R statistical software (version 3.0.2, R Development Core Team, Vienna, Austria) for descriptive statistics and further testing in addition to the “survival” package for R (version 2.37-4, Therneau T, 2013).
Kaplan-Meier survival analysis was performed to describe the survival of the composite fillings with regard to sex, age, operator, type of tooth, number of filled surfaces, Black classification, dental dam, type of adhesive, and type of composite. (Figs. 2a–d and 3a–f). The curves were terminated if the number of surviving fillings fell below n = 20. Therefore, observation years 7 and 8 were not included in the graphs of the survival analysis.
Cox proportional hazard model with backward elimination was used to perform multivariate analysis on the variables sex, patients’ age, operator, tooth type, number of filled surfaces, Black classification, dental dam, and type of etching/bonding material and filling material on survival probability. The factors with statistical significance were presented in the Tables 1 and 2 leaving out the insignificant variables.
Results
In total, 2388 fillings in 1031 teeth belonging to 667 patients (314 girls and 353 boys), with a mean dmft of 5.66 (±3.9), were included in this retrospective study. The patients were 1–13 years of age with a mean age of 6.6 years (±2.2 years). The distribution between the sexes was almost equal regarding both patient (m/f = 1.1:1) and filling distribution (1296[m]/1092[f] = 1.2:1). While 798 of all the fillings were placed in patients <6 years of age (n = 227), a total of 1590 fillings were placed in the age group ≥6 years (n = 533).
A total of 331 (331/2388; 13.9 %) fillings were placed under dental dams. For the majority (1968/2388; 82.4 %) of fillings, a total etch system was used. Mostly, this system was combined with a flowable composite (1337/2388; 56.0 %), followed by the combination of universal micro- or nano-hybrid and flowable composite (510/2388; 21.4 %), and universal micro- or nano- hybrid composite alone (121/2388; 5.1 %). In 17.6 % of restorations (420/2388), a self-etching adhesive was used. It was followed by a flowable composite (344/2388; 14.4 %), a universal micro or nano-hybrid composite (65/2388; 2.7 %), or a combination of both (21/2388; 0.9 %). The distribution of fillings with regard to type of tooth, number of filled surfaces, and Black classification is presented in Table 1.
The maximum observation period included 8 years with an annual failure rate of 10.0 % (Fig. 1). Due to the overall low number of fillings (<20), years 7 and 8 were excluded in the graphs. In 8.9 % of the cases, the fillings failed due to secondary caries (212/2388), and in 8.2 % (196/2388), failure occurred due to other reasons, such as technical failure comprising total filling loss, loosening, marginal gaps, tooth fracture, and other reasons, which mostly occurred within the first year (Fig. 1).
Kaplan-Meier estimator
The overall survival was about 75 % after 2 years dropping to 50 % after about five and a half years (Fig. 2a). After 2 years, canines showed the highest survival probability (>85 %), followed by molars (>75 %) and incisors (<70 %) (Fig. 2b). Single- and two-surface composite fillings showed an almost equally high survival probability of >85 % for the first year, and the survival probability of two-surface fillings decreased to <70 % in the third year, while single-surface fillings showed >70 % survival. Three-surface fillings showed a lower longevity of ≈60 % after 3 years. The lowest survival probability of <50 % after 3 years was observed when more than four surfaces were filled. Regarding the Black classification, class IV fillings had the lowest survival probability of ≈60 % after 2 years, decreasing to ≈50 % after 3 years, compared to ≥80 % for classes I and V and ≥70 % for classes II and III, which decreased to ≥75 and ≥60 %, respectively (Fig. 2c). For the parameter sex, survival curves were very similar to that of the overall survival curve (Fig. 2a). Regarding age, patients younger than 6 years showed a 75 % survival of less than 2 years, while patients above six years had a 75 % survival of over 2 years (Fig. 3a). Operators performed very differently, while operators 1 and 2 performed almost equal with a 75 % survival of about 2 years, the experienced operator 5 performed best, while the less experienced operator 6 performed less favorable (Fig. 3b). The use of dental dam resulted in a more than 1-year higher survival of 75 % of fillings (Fig. 3c). Also, the use of self etching adhesive showed a more than 1-year higher survival for 75 % of the fillings (Fig. 3d). Flowable composite or the use of a combination of flowable and hybrid composite performed almost equally over the years with a 75 % survival of about 2 years.
Cox proportional hazard model
The model revealed overall significance for the parameters tooth type, Black classification, age, operator, dental dam, and type of adhesive used. Not significant were the parameters number of surfaces filled, sex, and type of composite. Longevity of fillings differed significantly from different tooth types (p = 0.02). While fillings in molars and canines showed a lower risk for failure than restorations in incisors, only canines showed significance (p < 0.01). Though numbers of filled surfaces did not influence survival significantly, Black classification did (p = 0.005) with filled class II cavities performing significantly lower than class I cavity restorations (p = 0.01). Patients aged ≥6 years showed a statistically significant lower risk for filling failure over the whole observation period compared to children aged <6 years (p < 0.001). The operator was a significant factor influencing survival with hazard ratios ranging from 0.62 to 2.74. While the less experienced operators 6 (p = 0.004) and 7 (p = 0.04) performed significantly weaker than operator 1, operator 5 performed better and was also holding a certificate for a university-based training in pediatric dentistry (p = 0.03). Also, the use of dental dam (p = 0.02) and use of self-etching adhesives (SE) (p = 0.02) resulted in a lower risk, while the type of composite used did not (p = 0.33).
Discussion
In this study, retrospective clinical data were provided about the survival probability of composite fillings placed in primary dentition that had been part of frequent recall monitoring. The Kaplan-Meier estimator has been frequently applied in retrospective, long-term studies to evaluate the longevity characteristics of direct restorations placed in permanent teeth under clinical conditions. In the primary dentition, it has been applied for glasionomer cement and compomere fillings, but has been used only rarely for composites [8, 14–17, 20, 23, 29–33]. For the primary dentition, Kählilehto et al. recently used the Kaplan-Meier estimator in a larger population, evaluating the longevity of a comparably high number of 2755 glass ionomer cement and compomer restorations in primary molars, but no composite was used as a filling material [8]. To our knowledge, this was the first study to provide such information for composite fillings including all primary tooth types, filling classifications and materials used in a comparably large population with such a high caries risk. The dmft of the study population was about 2.5 times as high as that for the average child population of the area [34]. Treatment of patients always included recommendations towards adherence to a frequent preventive recall regimen, which was accessible to all patients exempt of additional costs. Naturally, though we do not have any reliable information about the background of the children, high caries risk populations are often related with a low socioeconomic background will have an ongoing high caries risk in the future [35]. Compliance with regard to a tooth-friendly behavior pattern including proper oral hygiene, non-cariogenic nutrition, and beverages as well as adherence to recall appointments are often observed.
Two studies using the Kaplan-Meier estimator in smaller populations treated with composite fillings found survival rates of 85.5 % for chair-side-treated primary molars after 3 years and 81.5 % for children treated under general anesthesia with an observation period of 6 years [23, 33]. A systematic review, including all types of studies on filling materials in primary molars, described a 3-year survival rate of 85.1 %, which is also within the same approximate survival range [5]. The survival rate in this study of a high caries risk population treated without general anesthesia and sedation was lower. It can be speculated that this is related to the very high caries risk of the described population as well as to the retrospective design of the study.
Annual failure rates for composite restorations in the permanent dentition in long-term, practice-based clinical and retrospective studies have ranged from 1.7 to 3.4 % and had been lower compared to the annual failure rates of 10 % in this study and 4.2 % in a previous study conducted on fillings placed in primary teeth under general anesthesia [20, 30, 32, 36]. Chair side treatment without sedation or general anesthesia in children does not offer the same optimal conditions as in treatments on the fully anesthetized patient. It has generally been assumed that fillings in primary teeth will be lost more frequently due to technical failure. Mostly, it has been argued that this failure rate is due to specific psychological or anatomical issues associated with the child and the less favorable microstructural properties of the primary teeth for adhesive techniques [37–39]. Although technical failures in this study occurred mainly within the first year, which has been described as quite typical, they were outnumbered by losses due to secondary caries over the whole observation period [8, 40, 41]. In high caries risk populations, the development of secondary caries has frequently been described as the main reason for replacing fillings in the primary, as well as the permanent, dentition, especially with longer observation periods because secondary caries will develop over time [20, 30, 40–46]. This might also explain the enhanced failure rate in relation to results of Qvist et al. found for amalgam as well as resin reinforced and conventional glasionomer cement [15–17]. In addition, the censoring process and definition of the observation period was different in this study leading to shorter survival times.
Although it was found by Qvist et al. that the operator plays an important role in the longevity of a dental restoration with amalgam, glass ionomer cement, and compomere in the primary dentition, evidence from clinical studies has not always supported this presumption and has shown that in clinical filling procedures on posterior permanent teeth, the number of operators does not have any significant influence on filling survival if the operators are experienced [15–17, 30, 47]. As was observed in this study, more experienced and efficiently working dentists produced fillings with significance to a higher survival probability than less-skilled dentists [48]. No significantly lower survival probability of composite fillings in the primary dentition was found for male patients, as has been reported by others [33].
Other observed parameters significantly influencing the longevity of restorations were the age of the patient, the type of tooth, the use of dental dam, and the extent of filling with regard to the Black classification. In addition, the use of the bonding technique showed a significant influence on the survival probability.
A high caries risk as well as a reduced ability to cooperate properly during treatment procedures might have contributed to a significantly higher risk of filling loss in patients <6 years of age [23, 37]. In this study, incisors showed a significantly lower survival probability compared to molars. Data regarding this difference have been sparse because studies have mainly focused on the molar region when describing the longevity of composite fillings in the primary and permanent dentition. In the molar region, Black class II restorations have been reported to have an almost threefold greater risk of failure than class I restorations as was confirmed by this study [19, 29]. In primary and permanent teeth, a significantly lower survival rate has been reported by several authors for an increasing extent of the filling, expressed as a high number of filled surfaces compared to single-surface lesions in the primary and permanent dentition [29, 30, 32, 41, 43, 45, 46, 49].
As described by other investigators, the type and system of etching and bonding can have a large impact on the survival probability of fillings [29, 49]. Self-etching bonding systems have been reported to be the most successful in the primary dentition, most likely due to their less aggressive etching properties than classical conditioning with phosphoric acid for the less-mineralized dentin as well as the reduced time of recontamination of the cavity [50, 51]. Additionally, different components of the bonding agent itself have recently been reported to enhance bonding to primary dentin and could also provide a certain resistance against hydrolytic degradation at the resin-dentin interface [52, 53].
During the observation period, the composite materials that were used changed from a highly filled, microhybrid resin composite to a nano-hybrid resin composite with altered composition, especially regarding filler size and loading. It was shown in vitro that nano-hybrid composites have good mechanical properties, such as reduced wear and improved surface characteristics; however, they also showed lower flexural strength and elastic-modulus. Van Dijken and Pallesen demonstrated in a prospective clinical trial on permanent teeth that the survival rates of the two materials did not differ significantly over an observation period of 6 years for class II restorations [54]. Another group, comparing the same micro-hybrid versus a different nano-hybrid composite, confirmed these findings over an 8-year period [55, 56]. Because esthetic aspects and wear were not focuses of this study, micro-hybrid and nano-hybrid filling materials were divided into three groups: universal viscosity, flowable, and the combined use of both materials. While in general, a combined technique does not seem to enhance the longevity of fillings, it is not recommended to use a flowable composite for larger cavities in the posterior region because of reduced wear resistance but rather to utilize universal micro- or nano-hybrid composites [41, 55, 57, 58]. In the literature, it is generally concluded that the use of a flowable material might have a negative impact on the survival probability in larger cavities, but the influence of other factors, such as the onset of caries and caries risk, as well as the size of the cavity, may play a more important role.
There is only little information on retrospective evaluation of other tooth colored filling materials for the primary dentition. In addition, study populations in prospective studies will be included in a setup that will make cooperation with regard to recall appointments and prevention a prerequisite. Most probably, survival rates found in prospective studies would experience a drop-down when they would be approached by a retrospective design investigating a real-life situation of a high-risk population. In addition, it was stressed by Käkilehto et al. that for the younger patients and patients high at risk for caries, survival rates are lower. In that large retrospective cohort study, high-risk patients were at a threefold higher risk for failure of glasionomer fillings than low-risk patients [8].
Therefore, no conclusive interpretation regarding the preference of other materials over the use of composite could be drawn within the results of this study. From the clinical perspective, with regard to practicability, the operator would prefer not to use two different materials in one treatment session when restoring primary and permanent teeth at the same time. Second, the use of time saving self-etching adhesive has been supported to be the more favorable treatment option over total etch systems. In addition, retrospective data that focus on the filling survial in such high-risk children are sparse and mainly not so well comparable due to differences in setting and design of studies.
The strength of this study lies in the reported short recall periods and the large number of observed fillings that were performed over a long period of time following the same protocol and with a consistent use of the same materials, reflecting filling application under real clinical conditions for a high-caries pediatric population. Long-term data for pediatric cohorts, especially for restorations on primary teeth, have been rare and were added to this study [8]. Although a practice-based, retrospective study design will not be able to answer specific detailed questions reliably, e.g., the influence of bruxism, behavioral problems, or the social background of individual patients, it could provide true information about the longevity of restorations in daily practice. The use of a randomized, prospective study design (RCT) would have been more precise to answer detailed questions regarding the influence of certain factors on failure, but it might also have resulted in selection bias with regard to patient acquisition if mostly patients who appeared to be reliable and motivated regarding regular attendance and oral hygiene were chosen. Nevertheless, due to the retrospective design of this study, the results should be interpreted cautiously, and conclusions should be drawn within its limitations.
Conclusions
This study on a pediatric high caries risk population revealed secondary caries as the main reason for an elevated filling loss in the long term. It supports the use of self-etching systems when using composite fillings for the restoration of primary teeth and underlines the accompanying intensified preventive care.
References
Skeie MS, Raadal M, Strand GV, Esplid I (2006) The relationship between caries in the primary dentition at 5 years of age and permanent dentition at 10 years of age—a longitudinal study. Int J Paediatr Dent 16:152–160
Alm A, Wendt LK, Koch G, Birkhed D, Nilsson M (2012) Caries in adolescence-influence from early childhood. Community Dent Oral Epidemiol 40:125–133. doi:10.1111/j.1600-0528.2011.00647.x
Finucane D (2012) Rationale for restoration of carious primary teeth: a review. Eur Arch Paediatr Dent 13:281–292
Drummond BK, Meldrum AM, Boyd D (2013) Influence of dental care on children’s oral health and wellbeing. Br Dent J 214:E27. doi:10.1038/sj.bdj.2013.533
Hickel R, Kaaden C, Paschos E, Buerkle V, García-Godoy F, Manhart J (2005) Longevity of occlusally-stressed restorations in posterior primary teeth. Am J Dent 18:198–211
Kandiah T, Johnson J, Fayle SA (2010) British Society of Paediatric Dentistry: a policy document on management of caries in the primary dentition. Int J Paediatr Dent 20:5. doi:10.1111/j.1365-263X.2010.01087.x
Yengopal V, Harneker SY, Patel N, Siegfried N (2009) Dental fillings for the treatment of caries in the primary dentition. Cochrane Database Syst Rev (2):CD004483. doi:10.1002/14651858.CD004483.pub2
Käkilehto T, Välimäki S, Tjäderhane L, Vähänikkilä H, Salo S, Anttonen V (2013) Survival of primary molar restorations in four birth cohorts—a retrospective, practice-based study. Acta Odontol Scand 71:1418–1422. doi:10.3109/00016357.2013.766359
Burke FJT (2004) Amalgam to tooth-coloured materials—implications for clinical practice and dental education: governmental restrictions and amalgam-usage survey results. J Dent 32:343–345
BIO Intelligence Service (2012) Study on the potential for reducing mercury pollution from dental amalgam and batteries, final report prepared for the European Commission –DG ENV. http://ec.europa.eu/environment/chemicals/mercury/pdf/Final_report_11.07.12.pdf. Accessed 29 Nov 2013
Vidnes-Kopperud S, Tveit AB, Esplid I (2011) Changes in the treatment concept for approximal caries from 1983 to 2009 in Norway. Caries Res 45:113–120. doi:10.1159/000324810
Lynch CD, Guillem SE, Nagrani B, Gilmour AS, Ericson D (2010) Attitudes of some European dental undergraduate students to the placement of direct restorative materials in posterior teeth. J Oral Rehabil 37:916–926. doi:10.1111/j.1365-2842.2010.02119.x
Lynch CD, Frazier KB, Blum IR, Wilson NHF (2011) Minimally invasive management of dental caries: contemporary teaching of posterior resin-based composite placement in U.S. and Canadian dental schools. J Am Dent Assoc 142:612–620
Qvist V, Poulsen A, Teglers PT, Mjör IA (2010) The longevity of different restorations in primary teeth. Int J Paediatr Dent 20:1–7. doi:10.1111/j.1365-263X.2009.01017.x
Qvist V, Laurberg L, Poulsen A, Teglers PT (2004) Eight-year study on conventional glass ionomer and amalgam restorations in primary teeth. Acta Odontol Scand 62:37–45
Qvist V, Manscher E, Teglers PT (2004) Resin-modified and conventional glass ionomer restorations in primary teeth: 8-year results. J Dent 32:285–294
Qvist V, Laurberg L, Poulsen A, Teglers PT (2004) Class II restorations in primary teeth: 7-year study on three resin-modified glass ionomer cements and a compomer. Eur J Oral Sci 112:188–196
Buerkle V, Kuehnisch J, Guelmann M, Hickel R (2005) Restoration materials for primary molars—results from a European survey. J Dent 33:275–281
Manhart J, Chen H, Hamm G, Hickel R (2004) Buonocore Memorial Lecture. Review of the clinical survival of direct and indirect restorations in posterior teeth of the permanent dentition. Oper Dent 29:481–508
Opdam NJ, Bronkhorst EM, Loomans BA, Huysmans MC (2010) 12-year survival of composite vs. amalgam restorations. J Dent Res 89:1063–1067. doi:10.1177/0022034510376071
Kopperud SE, Tveit AB, Gaarden T, Sandvik L, Esplid I (2012) Longevity of posterior dental restorations and reason for failure. Eur J Oral Sci 120:539–548
Pallesen U, Van Kijken JWV, Halken J, Hallonsten AL, Höigaard R (2014) A prospective 8-year follow-up of posterior resin composite restorations in permanent teeth of children and adolescents in Public Dental Health Service: reasons for replacement. Clin Oral Investig 18:819–827. doi:10.1007/s00784-013-1052-x
Bücher K, Tautz A, Hickel R, Kühnisch J (2014) Longevity of composite restorations in patients with early childhood caries (ECC). Clin Oral Investig 18:775–782. doi:10.1007/s00784-013-1043-y
American Academy of Pediatric Dentistry (2012) Guideline on pediatric restorative dentistry. Pediatr Dent 34:173–180
Bundesministerium der Justiz Deutschland (1987) Verordnung über den Schutz vor Schäden durch Röntgenstrahlen (Röntgenverordnung - RöV). http://www.gesetze-im-internet.de/r_v_1987/BJNR001140987.html. Accessed 29 Nov 2013
Espelid I, Mejàre I, Weerheijm K, EAPD (2003) EAPD guidelines for use of radiographs in children. Eur J Paediatr Dent 4:40–48
European Commission (2004) Radiation protection No. 136. European guidelines on radiation protection in dental radiology. The safe use of radiographs in dental practice. http://ec.europa.eu/energy/nuclear/radioprotection/publication/doc/136_en.pdf. Accessed 29 Nov 2013
Hickel R, Peschke A, Tyas M, Mjör I, Bayne S, Peters M, Hiller KA, Randall R, Vanherle G, Heintze SD (2010) FDI World Dental Federation—clinical criteria for the evaluation of direct and indirect restorations. Update and clinical examples. J Adhes Dent 12:259–272. doi:10.3290/j.jad.a19262
Da Rosa Rodolpho PA, Cenci MS, Donassollo TA, Loguércio AD, Demarco FF (2006) A clinical evaluation of posterior composite restorations: 17-year findings. J Dent 34:427–435
Opdam NJ, Bronkhorst EM, Roeters JM, Loomans BA (2007) Longevity and reasons for failure of sandwich and total-etch posterior composite resin restorations. J Adhes Dent 9:469–475
Opdam NJ, Bronkhorst EM, Cenci MS, Huysmans MC, Wilson NH (2011) Age of failed restorations: a deceptive longevity parameter. J Dent 39:225–230. doi:10.1016/j.dent.2010.12.008
Van de Sande FH, Opdam NJ, da Rosa Rodolpho PA, Correa MB, Demarco FF, Cenci MS (2013) Patient risk factors’ influence on survival of posterior composites. J Dent Res 92(7 Suppl):78S–83S. doi:10.1177/0022034513484337
Attin T, Opatowski A, Meyer C, Zingg-Meyer B, Buchalla W, Mönting JS (2001) Three-year follow up assessment of class II restorations in primary molars with a polyacid-modified composite resin and a hybrid composite. Am J Dent 14:148–152
DAJ (Deutsche Arbeitsgemeinschaft für Jugendzahnpflege) (2010) Epidemiologische Begleituntersuchung zur Gruppenprophylaxe 2009. DAJ, Bonn
Thomson WM, Poulton R, Milne BJ, Caspi A, Broughton JR, Ayers KM (2004) Socioeconomic inequalities in oral health in childhood and adulthood in a birth cohort. Community Dent Oral Epidemiol 32:345–353
Van Dijken JWV, Pallesen U (2011) Clinical performance of a hybrid resin composite with and without an intermediate layer of flowable resin composite: a 7-year evaluation. Dent Mater 27:150–156. doi:10.1016/j.dental.2010.09.010
Eidelman E, Faibis S, Peretz B (2000) A comparison of restorations for children with early childhood caries treated under general anesthesia or conscious sedation. Pediatr Dent 22:33–37
Angker L, Swain MV, Kilpatrick N (2003) Micro-mechanical characterization of the porperties of primary tooth dentine. J Dent 31:261–267
Papathanasiou AG, Curzon ME, Fairpo CG (1994) The influence of restorative material on the survival rate of restorations in primary molars. Pediatr Dent 16:282–288
Brunthaler A, Konig F, Lucas T, Sperr W, Schedle A (2003) Longevity of direct resin composite restorations in posterior teeth. Clin Oral Investig 7:63–70
Demarco FF, Corrêa MB, Cenci MS, Moraes RR, Opdam NJ (2012) Longevity of posterior composite restorations: not only a matter of materials. Dent Mater 28:87–101. doi:10.1016/j.dental.2011.09.003
Andersson-Wenckert I, Sunnegårdh-Grönberg K (2006) Flowable resin composite as a class II restorative in primary molars: a two-year clinical evaluation. Acta Odontol Scand 64:334–340
Bernardo M, Luis H, Martin MD, Leroux BG, Rue T, Leitão J, DeRouen TA (2007) Survival and reasons for failure of amalgam versus composite posterior restorations placed in a randomized clinical trial. J Am Dent Assoc 138:775–783
Köhler B, Rasmusson CG, Odman P (2000) A five-year clinical evaluation of class II composite resin restorations. J Dent 28:111–116
Soncini JA, Maserejian NN, Trachtenberg F, Tavares M, Hayes C (2007) The longevity of amalgam versus compomer/composite restorations in posterior primary and permanent teeth: findings from the New England Children’s Amalgam Trial. J Am Dent Assoc 138:763–772
Alves dos Santos MP, Luiz RR, Maia LC (2010) Randomised trial of resin-based restorations in class I and class II beveled preparations in primary molars: 48-Month results. J Dent 38:451–459. doi:10.1016/j.jdent.2010.02.004
Loomans BA, Opdam NJ, Roeters FJ, Bronkhorst EM, Burgersdijk RC, Dorfer CE (2006) A randomized clinical trial on proximal contacts of posterior composites. J Dent 34:292–297
Coppola MN, Ozcan YA, Bogacki R (2003) Evaluation of performance of dental providers on posterior restorations: does experience matter? A data envelopment analysis (DEA) approach. J Med Syst 27:445–456
Friedl KH, Hiller KA, Schmalz G (1995) Placement and replacement of composite restorations in Germany. Oper Dent 20:34–37
Osorio R, Aguilera F, Otero P, Romero M, Osorio E, García-Godoy F, Toledano M (2010) Primary dentin etching time, bond strength and ultra-structure characterization of dentin surfaces. J Dent 38:222–231. doi:10.1016/j.jdent.2009.11.001
Kaaden C, Schmalz G, Powers JM (2003) Morphological characterization of the resin-dentin interface in primary teeth. Clin Oral Investig 7:235–240
Krämer N, Tilch D, Lücker S, Frankenberger R (2014) Status of ten self-etch adhesives for bonding to dentin of primary teeth. Int J Paediatr Dent 24:192–199. doi:10.1111/ipd.12059
Van Landuyt KL, Snauwaert J, De Munck J, Peumans M, Yoshida Y, Poitevin A, Coutinho E, Suzuki K, Lambrechts P, Van Meerbeek B (2007) Systematic review of the chemical composition of contemporary dental adhesives. Biomaterials 28:3757–3785
Van Dijken JWV, Pallesen U (2013) A six-year prospective randomized study of a nano-hybrid and a conventional hybrid resin composite in class II restorations. Dent Mater 29:191–198. doi:10.1016/j.dental.2012.08.013
Krämer N, García-Godoy F, Reinelt C, Feilzer AJ, Frankenberger R (2011) Nanohybrid vs. fine hybrid composite in extended class II cavities after six years. Dent Mater 27:455–464. doi:10.1016/j.dental2011.01.004
Frankenberger N, Reinelt C, Krämer N (2014) Nanohybrid vs. fine hybrid composite in extended class II cavities: 8-year-results. Clin Oral Investig 18:125–137. doi:10.1007/s00784-013-0957-8
Clelland NL, Pagnotto MP, Kerby RE, Seghi RR (2005) Relative wear of flowable and highly filled composite. J Prosthet Dent 93:153–157
Boeckler A, Schaller HG, Gernhardt CR (2012) A prospective, double-blind, randomized clinical trial of a one-step, self-etch adhesive with and without an intermediary layer of a flowable composite: a 2-year evaluation. Quintessence Int 43:279–286
Conflict of interest
The authors certify that they have no proprietary, financial, or other personal interests in any products and/or companies that are presented in this article and that they are free of conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bücher, K., Metz, I., Pitchika, V. et al. Survival characteristics of composite restorations in primary teeth. Clin Oral Invest 19, 1653–1662 (2015). https://doi.org/10.1007/s00784-014-1389-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-014-1389-9