Abstract
Parkinson’s disease (PD) is the second most common neurodegenerative disorder caused by the selective and progressive loss of dopaminergic neurons in the substantia nigra pars compacta. Although PD has been heavily researched, the precise etiology and pathogenesis for PD are still inconclusive. Consequently, current pharmacological treatments for PD are largely symptomatic rather than preventive and there is still no cure for this disease nowadays. Moreover, nonmotor symptoms caused by intrinsic PD pathology or side effects induced by currently used pharmacological interventions are gaining increasing attention and urgently need to be treated due to their influence on quality of life. As ancient traditional healing systems, Tai Chi, Yoga, acupuncture and natural products have long been considered as complementary or alternative therapeutic options for PD. Recently, several newly developed non-pharmacological therapeutic strategies, including deep brain stimulation, repetitive transcranial magnetic stimulation, near-infrared light, gene therapy and cell replacement therapy, have also been suggested to give benefits to relieve parkinsonian symptoms. This review will summarize and update the therapeutic potential and the most recent research progresses of these traditional and modern therapeutic options and highlight their clinical meaning for the therapy of not only PD but also other neurodegenerative diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is the second most common neurodegenerative disease worldwide after Alzheimer’s disease, affecting 1–2 % of population older than 60 years (Healy et al. 2008; Tarsy 2012). The classic clinical manifestations of PD include bradykinesia, resting tremor, rigidity and postural instability, which are largely caused by the deficiency of dopamine (DA) in the striatum due to the selective and progressive loss of dopaminergic (DAergic) neurons in the substantia nigra pars compacta (Fahn 2003). PD is believed to be caused by both genetic and environmental risk factors (Warner and Schapira 2003; Verstraeten et al., 2015; Polito et al. 2016). Pathologically, neuroinflammation, mitochondrial dysfunction, protein degradation failure, endoplasmic reticulum stress, and reactive oxygen species overproduction, have been implicated to be involved in PD pathogenesis (Hirsch et al. 2013; Kansara et al. 2013; Shen et al. 2013; Zuo and Motherwell 2013; Tang et al. 2014; Ciechanover and Kwon 2015; Michel et al. 2016). Unfortunately, until now, the precise mechanisms for PD are still largely inconclusive and most PD therapies are symptoms-based rather than preventive or disease-modifying.
Clinically, motor symptoms are the main features of PD onset and progression, but nonmotor symptoms, including depression, fatigue, hyposmia, sleep disorders, automatic dysfunction, cognitive impairment and dementia, also could be evident in some PD patients. Since 1960s, treatment for PD has been focused on the replacement or supplement of DA. Various DAergic drugs or novel mechanism-based therapeutic candidates have been developed and are subjected into clinical usage or clinical trials for PD treatment (Dong et al. 2016a, b). As the most effective pharmacological medications for PD, levodopa and other DAergic drugs benefit almost all PD patients (Poewe 2009). However, long-term use of levodopa is often accompanied by motor complications, including levodopa-induced dyskinesia (LID) and motor fluctuations, which range in severity from mild and non-disabling to incapacitating. Once motor complications emerge, it means that PD patients have entered the advanced stage, in which the dosage of levodopa should be modified and the formulation of levodopa should be changed to combine with DA agonists or other drugs to control the adverse symptoms. In addition, although some motor dysfunctions of PD, such as tremor and dyskinesia, may be alleviated with drug therapy, characteristics such as postural instability and nonmotor symptoms, especially neuropsychiatric disorders, are less responsive to current medications and require alternative approaches (Nirenberg and Fahn 2005; Schapira and Olanow 2005).
All these above-mentioned limitations of pharmacological treatments generate a notion that non-pharmacological or complementary and alternative management may offer both symptomatic relief and disease-modifications that are beneficial for PD patients. Here, we outline recent studies and summarize evidence on the effectiveness of both traditional and modern therapeutic modalities for PD (Results of clinical trials or meta-analysis of alternative therapies for PD are sumarized in Table1). Moreover, the methodological challenges and possible directions of these therapeutic options for future research are also discussed separately.
Traditional complementary and alternative therapy of PD
Complementary and alternative management of PD is normally defined as a diverse group of therapies, practices or products that share in common their exclusion from conventional and well-accepted medicinal or pharmacological therapies of PD. The variety of traditional complementary and alternative management is increasing yearly, mainly including physio-exercise therapy, Tai chi, Qi gong, relaxation training, acupuncture, traditional herbal medicines, and daily beverage and neutraceuticals.
Physio-exercises therapy
Exercise is an integral part of PD management because physical activity has been shown to retard the deterioration of motor functions, to prolong functional independence and to improve the cognitive disabilities (Lugassy and Gracies 2005; Goodwin et al. 2008; Dibble et al. 2009; Tomlinson et al. 2013, 2014; van der Kolk and King 2013). As for the underlying mechanisms, it has been shown that physio-exercise has a protective effect on the dopaminergic function of PD animals by enhancing neurotrophic factors expression, increasing mitochondrial function and stimulating neuroplasticity (Zigmond and Smeyne 2014; Vivar et al. 2016). More precisely, recent studies further reveal that physio-exercise reduces the alteration of the DAergic neurons in the substantia nigra and contributes toward reconstituting the function of the basal ganglia involved in the motor command through increasing brain-derived neurotrophic factor (BDNF) expression and recovering DA and glutamate neurotransmission (Speelman et al. 2011; Wu et al. 2011), restore mitochondrial function, and attenuate neuroinflammation (Lau et al. 2011), thereafter play neuroprotective roles and restore motor deficits (Frazzitta et al. 2013; Zigmond and Smeyne 2014; Sconce et al. 2015; Svensson et al. 2015; Tuon et al. 2015).
Recent clinical trials have further suggested that aerobic exercise including aerobic walking and stretching could ameliorate motor functions such as gait, balance, physical performance, and nonmotor functions such as fatigue, depression and cognition, but not for fall prevention in PD patients (Uc et al. 2014; Canning et al. 2015). Moreover, it has been reported that intensive training modalities could improve muscle strength and mobility (Cruickshank et al. 2015; Uhrbrand et al. 2015), and low-intensity exercise caused a better performance on gait speed than high-intensity (Shulman et al. 2013). Additionally, resistance-based exercises that address deficits in balance and strength have shown positive effects (Scandalis et al. 2001; Hirsch et al. 2003; Dibble et al. 2006). However, the efficiencies of physio-exercises therapy for PD are not compliant to all clinical symptoms and need more long-term and follow-up studies. In addition, the safety and dose–response relationships (i.e., frequency, intensity, and duration) of physio-exercise therapy for PD are still requires monitoring.
Tai chi and Qi gong
Compared with conventional physio-exercises, Tai chi, an ancient traditional Chinese exercise combining with conscious breath control, relaxation, and slow movements, has been proved effective in reducing balance impairment and falls, with additional functional improvement (Li et al. 2012; Tsang 2013). According to the recent meta-analysis, Tai chi showed positive effects in motor function and balance, but not in gait velocity, step length and gait endurance improvements (Yang et al. 2014). Except for improving motor function, Tai chi could also relieve stress and is beneficial for improving quality of life and mood (Esch et al. 2007; Nocera et al. 2013). It is likely that the benefits of Tai chi are a combination of physical training of strength, balance, stretching, and breathing, and additional improvements in mood and stress. Although the exact mechanisms underlying its therapeutic potential is still barely investigated, Tai chi has been proved to be a safe and feasible exercise that improves quality of life, and it could be a good exercise strategy for PD patients with mild to moderate severity.
Qi gong is another traditional Chinese exercise like Tai chi focusing on the movement of internal energy (chi) through the practice of meditation-like practice and focused movements. One randomized controlled trial (RCT) has suggested that Qi gong could improve Unified Parkinson’s Disease Rating Scale (UPDRS)-III score, together with several nonmotor symptoms amelioration (Schmitz-Hübsch et al. 2006). In contrast, another small-scale RCT demonstrated that there was no significant motor benefit after Qi gong practice when compared with aerobic training (Burini et al. 2006). Therefore, it still needs more studies to confirm the exact efficacies and explore the best training pattern for anti-Parkinsonism potential of Qi gong.
Mindfulness meditation, Yoga, and other relaxation training
Mindfulness is an ancient spiritual practice as well as a form of stress-reductive meditation training, in which participants are guided towards greater awareness and acceptance of the current moment (Kabat-Zinn 2009). Fitzpatrick et al. (2010) have found that mindfulness has a qualitatively beneficial effect on the PD patients’ ability to cope. Subsequently, a quantitative controlled study by Pickut et al. (2015) has suggested an improvement in the observing subscale of the Five Facet Mindfulness Questionnaire (FFMQ) and a reduction in motor disability, but no change in depression measured using the Beck Depression Inventory. In line with previous studies, one recent study found that modified Mindfulness-Based Stress Reduction training improve both motor and nonmotor symptoms of PD, as evidenced by a significant increase in the FFMQ-Observing subscale, a reduction in anxiety and depression scores, an improvement in cognition, a decrease in postural instability and gait difficulty symptomatology, and a reduction in symptom distress observed from the Outcome Questionnaire-45 (Dissanayaka et al. 2016). As for the underlying mechanism for the ameliorating effects of mindfulness against PD, Pickut et al. (2013) have found that, versus non-treated control patients, PD patients subjected to 8 weeks of a mindfulness-based training showed significant increases in gray matter density in the cuneus and lingual gyrus of the left occipital lobe, the left thalamus, the left parahippocampus, and bilaterally in the temporoparietal junction. Most of these brain regions are responsible for emotion, anxiety, and cognitive and motor functioning relevant to PD (Pickut et al. 2013). To date, however, formal evaluations of potential benefits have not been reported. Given the low cost and risk, mindfulness is a reasonable complementary practice to PD patients pending the results of further research testing.
Yoga is a traditional mindfulness-based exercise and is another form of exercise which combines multiple physical elements with relaxation and breathing. It has been shown to significantly improve measures of gait, flexibility, muscle force, fatigue, and quality of life in healthy elderly and people with medical disorders including back pain, arthritis, hypertension, anxiety, and depression. One pilot study has shown that, after 6–12 weeks training, Yoga participants report a significant UPDRS scores improvement and positive trends of ameliorations in tremor, depression scores, body weight and forced expiratory volume (Sharma et al. 2015). Another pilot study has demonstrated that after an 8-week Yoga program, some texts such as sit-and-reach text, single-leg balance text improved significantly, and depression was alleviated to some extent (Boulgarides et al. 2014). Except for these small studies, until now, there is still no big-scale RCT about Yoga in PD treatment. It still requires larger size of individuals and further investigation to ascertain the therapeutic efficiency of Yoga for PD patients.
Besides mindfulness and Yoga, various forms of massage have been indicated to be one of the most common forms of relaxation and alternative therapy for PD (Rajendran et al. 2001). Massage is a broad category that includes different forms of soft tissue manipulation, often incorporated with relaxation. Two months of Japanese massage shows a positive effect in various PD symptoms including shoulder stiffness, muscle pain and fatigue (Donoyama and Ohkoshi 2012). Another before–after study has also suggested that after 40-min Anma massage, the movement difficulties of PD patients were generally improved (Donoyama et al. 2014). A small pilot study of whole body therapeutic massage in PD patients has found an improvement in quality of life and self-reported function (Paterson et al. 2005). Alexander technique uses hand contact to assess and manipulate changes in muscle activity by addressing the relationship between thought and the resultant muscle activity. One RCT of 3-month massage and Alexander technique in 93 PD patients by Stallibrass et al. (2002) has found that, compared with no intervention control group, the Alexander technique participants show improved on self-assessment disability scores and depression ratings. Reflexology is another form of relax and stress-reductive therapeutic massage and is reported to induce improvements of nonmotor symptoms of PD (Johns et al. 2010). Another study compared massage therapy with simple muscle relaxation techniques and found that massage therapy resulted in significantly lower urinary stress hormone levels, and also self-reported improvements in sleep quality (Hernandez-Reif et al. 2002). In addition, Craig et al. (2006) have demonstrated that neuromuscular therapy, a technique similar to massage but which relies on direct compression of trigger points, was more effective than relaxation at improving motor UPDRS scores in 36 PD patients over a 4-week intervention period. However, these studies did not see a significant increase of urinary DA in PD patients. Moreover, a small RCT recently found that massage significantly reduced salivary cortisol levels in PD patients directly after the treatment, but had no long-lasting effect on diurnal cortisol levels (Törnhage et al. 2013). Although these forms of massage have been shown to be safe and beneficial, larger clinical trials are needed to more fully document their therapeutic efficacy in PD.
Dance and music therapy
Dance is a multi-dimensional activity offering auditory, visual and sensory stimulation, musical experience, social interaction, memory, motor learning and emotional perception, expression and interaction (Kattenstroth et al. 2010). As an intervention for PD patients, dance could improve both motor and nonmotor symptoms. The recent meta-analysis suggests that short-term dance significantly improves UPDRS scores, balance and gait as compared with no intervention controls (Sharp and Hewitt 2014). Dance, especially Tango, has been reported to alleviate motor function and balance, as compared with conventional exercise (Hackney et al. 2007). Additionally, Tango is also thought to offer cognitive benefits such as improving cuing strategies, as it incorporates aerobic activity and movements that challenge gait and balance with progressive motor skill learning in the presence of external cues provided by the partner and the music. Other forms of dance such as waltz/foxtrot, may show similar benefits to Tango in PD (Hackney and Earhart 2009). However, each dance form has different qualities and researchers have hypothesized that certain qualities will target specific PD symptoms. For example, Tango requires frequent movement initiation and cessation, spontaneous directional changes and movement speeds, which may target movement initiation, turning and bradykinesia. In contrast, ballet challenges strength and flexibility to emphasize posture, body alignment, projection of eye focus and limb extension, as well as whole body coordination (Houston and McGill 2013). Although there is sufficient evidence that dance therapy is enjoyable and effective for improving gait and balance in PD patients, long-term outcome data are still lacking. In addition, the safety of dance programs also needs to be adequately reported to ensure the safe and appropriate implementation of dance interventions.
Music therapy uses music or any of its elements (sound, rhythm, melody, or harmony) to facilitate and promote mobilization and expression in order to meet physical, emotional, mental, social, or cognitive requirements. Previous studies have suggested that music may have an ability to impact both motor (including gait and dexterity) and nonmotor (including cognition, anxiety, apathy and depression) functions of PD patients. Pacchetti et al. (2000) have found that the PD patients in the music therapy group show significant improvement in certain motor and quality-of-life measures. de Bruin et al. (2010) also demonstrated improvements in stride length, gait velocity, and cadence among PD patients walking to an individualized playlist compared to controls. Music has been associated with the release of some specific neurochemicals and hormones in both animal and human studies (Möckel et al. 1994; Knight and Rickard 2001; Chanda and Levitin 2013). Additionally, functional magnetic resonance imaging studies have demonstrated an association between music therapy and increased mesolimbic dopamine release (Menon and Levitin 2005).
Acupuncture
Acupuncture, as a vital part of traditional Chinese medicine, has been applies for over 3000 years. In general, acupuncture needle inserted at the specific acupoint stimulates nerve receptors both directly or indirectly, through mechanical coupling via the connective tissues surrounding the needle, then through the local reflex and the central nervous system, induces endocrine, neuroendocrine, autonomic, and systemic behavioral responses. Clinical trials or practices have demonstrated that acupuncture either manual or electro relieves some motor symptoms in PD patients (Yang et al. 2006; Ren 2008; Cho et al. 2012; Toosizadeh et al. 2015) and markedly improves many nonmotor symptoms such as psychiatric disorders, sleep problems, and gastrointestinal symptoms (Cho et al. 2012; Zeng and Zhao 2016). Additionally, previous studies have demonstrated that acupuncture could improved therapeutic efficacy and reduced dosage of levodopa and also ameliorate drugs-induced side effects or complications (Zou 2006; Kim et al. 2014). Acupuncture studies in PD animal models have reported multiple mechanisms for its neuroprotective effects and therapeutic potential. Acupuncture elicited significant recovery and reduced degeneration of substantia nigra dopaminergic neurons in 6-hydroxydopamine (6-OHDA) lesion rat model (Park et al. 2003). Electroacupuncture may modulate apoptosis and neuroinflammation in the 1-methyl 4-phenyl 1,2,3,6-tetrahydropyridine (MPTP) mouse model, suggesting neuroprotective effects (Jeon et al. 2008), possibly via p53-related signaling (Park et al. 2015). Acupuncture or electroacupuncture has also been reported to modulate the expressions of dopamine transporter (DAT) and DA receptors, increase postsynaptic dopamine neurotransmission, and inhibit microglial activation and inflammatory events (Kang et al. 2007; Kim et al. 2011; Rui et al. 2013). Using functional magnetic resonance imaging technique, another randomized trial revealed that acupuncture brought significant improvement of motor function with putamen and primary motor cortex activation, as compared with placebo control groups (Chae et al. 2009). All these findings suggested that acupuncture may serve as a promising complementary and alternative therapy for PD, although more studies, either comparative effectiveness research or high-quality placebo-controlled clinical studies are still warranted.
Traditional herbal medicines
Traditional herbal medicines have been used for centuries. Recent preclinical studies have suggested that some of herbal medicines, either as single agent or in various combinations, may have neuroprotective effects in PD animal models. Ginseng is a plant substance which has been used in Eastern Asian countries for centuries and is proposed to have anti-inflammatory properties, improve fatigue and cognition. Multiple components of Ginseng, such as Rb1, Rg1, Rd, Re, Notoginsenoside R2, and Pseudoginsenoside-F11 have attracted remarkable interest as promising agents due to their beneficial effects in various PD animal models (González-Burgos et al. 2015). These compounds exert their neuroprotective activity through different mechanisms including inhibition of oxidative stress and neuroinflammation, decreases in apoptosis and nigral iron levels, and regulation of N-methyl-d-aspartate receptor activity (Wang et al. 2009; González-Burgos et al. 2015; Zhou et al. 2016). Ginkgo biloba, as another one widely used herbal medicine with potential antioxidant and neuroprotective properties, has beneficial effects in MPTP animal models (Rojas et al. 2012a, b). The Ginkgo biloba extract EGb 761 and its main constituent flavonoids and ginkgolides increase extracellular dopamine levels in the rat prefrontal cortex (Yoshitake et al. 2010). Clinically, a case report has demonstrated that PD patients showed a dramatic improvement after supplementation with ginkgo and a multivitamin–multimineral supplement (Conrad 2014). Interestingly, herbs containing high concentrations of levodopa, such as Mucuna pruriens and Vicia faba, have been reported to have neuroprotective effects, including recovering endogenous DA production and reducing oxidative stress in the substantia nigra (Manyam et al. 2004; Yadav et al. 2013), and have also been shown to potentially result in less dyskinesia (Rabey et al. 1992; Kasture et al. 2009; Lieu et al. 2010, 2012). Traditional Chinese decoction, San-Huang-Xie-Xin-Tang, composed of Coptidis rhizoma, Scutellariae radix, and Rhei rhizoma, possesses beneficial protection against MPTP model of PD via antioxidative and antiapoptotic effects (Lo et al. 2012). One pilot study reported that dietary extract rikkunshi-to could reduce gastroparesis in terms of shortening gastric emptying time in PD (Doi et al. 2014). Yokukansan is another kind of herbal extract, which is efficient in ameliorating neuropsychiatric symptoms of PD, such as hallucinations, anxiety and apathy, according to a small-scale exploratory trial (Hatano et al. 2014). Through evaluating some neurotransmitters in the brain, Bushen huoxue formulas are considered to enhance the levels of serotonin and norepinephrine, and to improve the depression of PD (Wang et al. 2014). Although previous studies have provided evidence supporting the positive therapeutic potential of herbal medicines for PD, there is still a long way to go for the clinical usage of herbal medicines in PD therapy due to the deficiency of exact bioactive components spectrum data and the lack of sufficient clinical data and safety profile.
Life habits and nutrition supplements
Previous studies have reported an inverse association between cigarette smoking and PD (Morens et al. 1995; Kyrozis et al. 2013). Additionally, numerous case–control studies or cohort studies provide evidence for the protective effect of smoking (Sasco and Paffenbarger 1990; Grandinetti et al. 1994; Gorell et al. 1999; Benedetti et al. 2000; Li et al. 2015). As for the possible mechanisms, previous studies have demonstrated that the anti-PD and neuroprotective effect of cigarette smoking might be due to the reducing enzymatic activity of type B monoamine oxidase (MAO-B) (Fowler et al. 1996), which catabolizes DA and may activate neurotoxicants. Moreover, 2,3,6-trimethyl-1,4-naphthoquinone, one major naphthoquinone component isolated from tobacco, has also been found to exert MAO-B-inhibiting activity and attenuate the DAergic system toxicity in MPTP mouse model (Castagnoli et al. 2001). An animal model further suggests that nicotine, another one major component of cigarette, may act as an antioxidant or prevent excitotoxicity (Halliwell 2006). However, there is no available clinical evidence to indicate that smoking or the use of nicotine and other components of tobacco is beneficial once PD has appeared. Moreover, the healthy concern of tobacco also limits its clinical usage as an alternative therapy for PD.
Similar with smoking, results from epidemiological studies reveal a consistent inverse association between coffee consumption and the risk of PD. A meta-analysis of eight case–control and five cohort studies conducted in four countries between 1968 and 2001 found a 31 % lower risk of PD in coffee drinkers than non-coffee drinkers (Hernán et al. 2002). In addition, this protective potential of coffee against PD shows significant gender preference and hormone sensitivity, as evidenced by the lower PD risk in man and the impacts of postmenopausal hormones on PD risk in women (Ascherio et al. 2003). The protective effect of coffee on PD could be ascribed to caffeine, which is the most important component of coffee and is recently considered as potent Adenosine A2A receptor antagonist. Caffeine and other A2 adenosine receptor antagonists have been shown to stimulate DA release and protect against DAergic neurotoxicity in animal models (Chen et al. 2001; Trevitt et al. 2009; Petzer and Petzer 2015). Although these clinical or preclinical studies have suggested a protective potential of coffee consumption against PD, however, the mechanisms involved are not fully understood and it is premature to recommend increasing coffee consumption to prevent PD, especially in women taking postmenopausal hormones.
In contrast to smoking and coffee, the previously reported relationship between alcohol consumption and PD risk is contradictory. While Palacios et al. (2012) demonstrated that the consumption of beer, wine, or liquor was not associated with PD risk, a more recent meta-analysis of observational studies has revealed an inverse association between alcohol consumption and risk of PD (Zhang et al. 2014). Moreover, multiple lines of evidence have suggested that resveratrol, one natural product present in grape and red wine, could ameliorate neuroinflammation, restor mitochondrial function, reverse oxidative stress over-production, and thereafter provide benefits to various PD animal models (Anandhan et al. 2010; Zhang et al. 2010; Ferretta et al. 2014).
Among the various lifestyle factors, tea consumption has attracted increasing interest, as one of the traditional and most consumed beverages in the world. Previous case–control studies and a cohort study have reported an inverse association between tea drinking and PD risk (Chan et al. 1998; Checkoway et al. 2002; Tan et al. 2003, 2008). Polyphenols components in tea may play important roles in delaying the onset or halting the progression of PD. Green tea and black tea are rich sources of polyphenols, including the most abundant and well-known epigallocatechin-3-gallate (EGCG) and theaflavins. There is now consistent mechanistic data on the neuroprotective and neuroregenerative effects of tea and its major bioactive components (Xu et al. 2006), indicating that they do not just possess anti-oxidant, anti-neuroinflammation or anti-chelating properties (as reviewed by Caruana and Vassallo 2015) but may directly inhibit α-synuclein aggregation and modulate intracellular signaling pathways, both in vitro and in vivo (Bieschke et al. 2010; Camilleri et al. 2013; Chen et al. 2014). However, despite significant data on the potential neuroprotective effects of tea and its bioactive components, clinical studies are still very limited and to date only EGCG has reached phase II trials.
Modern medicine practices that integrate traditional beliefs often focus on nutrition or nutraceuticals, as part of a healthy lifestyle, with the expectation that lowering inflammation and free radical damage may protect against further neuronal death and thus delay or halt disease progression. Evidence from epidemiological studies have been presented that various nutritional supplements, especially vitamins, decrease the risk for PD. For example, vitamin B6 intake has been associated with a significantly decreased risk of PD in smokers (de Lau et al. 2006), vitamin D is also inversely associated with PD (Knekt et al. 2010; Wang et al. 2015). Despite vitamins, other nutraceuticals, such as coenzyme Q10, fish oil and selenium, have shown therapeutic potential for PD. Coenzyme Q10, as the electron acceptor for mitochondrial complexes I and II, can improve complex I activity and reduced levels of coenzyme Q10 have been identified in the mitochondria of PD patients (Shults et al. 1997). However, a phase III trial demonstrates that high-dosage of coenzyme Q10 shows no benefits in early PD (Beal et al. 2014). Similar as coenzyme Q10, although fish oil, glutathione and seletium have been reported to exert antioxidant and anti-neuroinflammation properties, there is still no sufficient evidence to support their clinical usage for PD and the toxicological profiles and side effects of these nutraceuticals should be concerned.
Modern non-pharmacological therapy of PD
Despite those above-mentioned traditional complementary and alternative modalities for PD, recent progress of modern technologies greatly promote the progression of the development of novel strategies for PD therapy. These minimally surgical or non-surgical therapeutic strategies attract attentions and greatly enrich the scope of PD alternative therapy and their clinical benefits for future PD management.
Deep brain stimulation (DBS)
Deep brain stimulation has generally been accepted as an alternative therapy for the amelioration of parkinsonian motor symptoms. Subthalamic nucleus (STN) and globus pallidus internus (GPi), two most hyperactive brain regions during PD progression, are usually used as targets for DBS. In addition, STN-DBS could be preferred to manage patients with advanced PD who have predominantly posture and gait disorders due to its larger improvements in off time (Odekerken et al. 2013). The beneficial effects of DBS on appendicular symptoms such as tremor, rigidity, limb bradykinesia and dyskinesia are well established (Roper et al. 2016), although the exact underlying mechanisms for DBS still remain poorly understood. After long-term observation, both STN- and GPi-targeted DBS therapy showed significant improvement in “on–off” conditions, dyskinesias and motor fluctuations (Weaver et al. 2012; Rizzone et al. 2014). Recently, DBS treatment at 60 Hz frequency shows a promising application potential to improve swallowing, gait freezing, and axial motor signs, almost overall motor signs of PD (Khoo et al. 2014; Xie et al. 2015). Despite the STN and Gpis, DBS therapy with pedunculopontine tegmental nucleus (PPNs) as stimulation targets has recently been found to be an alternative to STN-DBS (Follett et al. 2012; Katz et al. 2015). Moreover, a novel 32-contact electrode of DBS, brings more potential benefits via widened therapeutic window and increased effectiveness (Contarino et al. 2014). As for the mechanisms for therapeutic potential of DBS against PD, preclinical trials, by using either non-human primates or other mammalian species, have shown that there is an improvement of DAergic neurons survival and an increase of BDNF level in the substantia nigra and primary motor cortex after STN-DBS exposure, suggesting the neuroprotective effect of DBS (Wallace et al. 2007; Spieles-Engemann et al. 2011). The local effects of DBS tend to result in the inhibition of neuronal-cell bodies and the excitation of neighboring axons. In addition, astrocytes are stimulated to release calcium, which may lead to a release of glutamate and adenosine, improved microvascular integrity, as well as local increases in cerebral blood flow. Finally, there is evidence that deep brain stimulation can induce local and possibly distal proliferation of neural precursor cells (Okun 2012; Pienaar et al. 2015). From a neurophysiological view, the “disruption hypothesis” seems to be more and more accepted, in which DBS dissociates input and output signals, resulting in the disruption of abnormal information flow through the stimulation site (Chiken and Nambu 2016). Although gross motor improvement is frequently observed following DBS therapy in PD, lack of uniformity in methodology and measured outcomes has clouded the interpretation of DBS benefits across the motor domain. In addition, despite these therapeutic benefits to motor performance of PD, the effects of DBS on nonmotor cognitive and psychiatric symptoms of PD have been controversial. A progressive worsening of neuropsychological performance and movement disorder are even observed (Merola et al. 2011; Baizabal-Carvallo and Jankovic J 2016), although some scholars consider the impairment of neurocognition might be due to the disease progress and medication reduction, not the DBS itself (Sáez-Zea et al. 2012; Weaver et al. 2012; Albuquerque et al. 2014). Finally, further large sample size trials for brain target site analyses should be performed for clarify the different therapeutic outcomes of various DBS stimulation targets, including STN, GPi and PPNs (Diamond and Jankovic 2005; Baizabal-Carvallo and Jankovic 2014).
Repetitive transcranial magnetic stimulation (rTMS)
Surgical therapies, including DBS, improve advanced symptoms above the best medical therapy, however, only limited (less than 5 %) PD population is suitable candidates for this surgical procedure (Morgante et al. 2007). During the past two decades, rTMS has been closely examined as a possible therapeutic option for PD (Pascual-Leone et al. 1994a, b; Fregni et al. 2005; Elahi et al. 2009). As a noninvasive therapeutic procedure, rTMS delivers repeated magnetic pulses to a specific brain area within a short time through a stimulation coil placed over the scalp without surgery or anesthesia. The repeated magnetic pulses not only alter excitability at local site of stimulation but also influence distant brain regions via the cortico-basal ganglia-thalamo-cortical motor circuit (Strafella et al. 2001; Kim et al. 2008; González-García et al. 2011). Additionally, different types of rTMS may cause different response of cortical excitability. For examples, while high-frequency rTMS induces cortical excitability (Pascual-Leone et al. 1994a, b), low-frequency rTMS causes a depressed cortical activity (Chen et al. 1997). Continuous high-frequency rTMS decreases cortical excitability, whereas intermittent high-frequency rTMS increases cortical excitability (Huang et al. 2005). Because rTMS can produce changes in neural activity and motor signs last well after stimulation, this technique has generated much interest as a potential therapeutic intervention for patients with PD and many rTMS trials have been uptaken to investigate its clinical benefits (Chou et al. 2015; Zanjani et al. 2015). Moreover, several types of rTMS were reported to be effective for drugs-induced dyskinesia and also been tried for non-pharmacological treatment of nonmotor symptoms of PD including depression (Shirota et al. 2016). One most recent meta-analysis further advocates the beneficial effect of rTMS on upper limb function in the short term and on walking performance and motor signs measured by UPDRS III in both the short- and long terms (Chung and Mak 2016). The use of rTMS has a minimal risk of adverse events in the PD patient population and should be encouraged as an alternative treatment for PD so long as it is thought to produce clinically relevant improvements in motor functions. However, the potential risk for seizure as well as a small risk of transient headache and scalp pain should be concerned (Vonloh et al. 2013).
Near-infrared light (NIr) therapy
NIr has been applied in clinical practice mainly for treating tissue contusion for many years. There have also been many in vivo studies of NIr-induced neuroprotection in various PD animal models. Previous preclinical studies have demonstrated that NIr could improve behavior deficits and DAergic neurons survival in parkinsonian mice (Shaw et al. 2010; Johnstone et al. 2014; Moro et al. 2014; Reinhart et al. 2015a, b; El Massri et al. 2016). Remarkably, a recent primate trial has further supported the notion that NIr was neuroprotective but not toxic to brain, which brought a step closer to clinical translation (Darlot et al. 2016). Although substantial evidence supports the therapeutic efficacy of NIr in PD animal models, there have been only limited research reports to date on the efficacy of NIr treatment in PD patients. There is a recent non-controlled and non-randomized clinical report indicating improved speech, cognition, freezing episodes and gait after extracranial NIr therapy in PD patients (Maloney et al. 2010); there are also some clinical reports suggesting improvements in parkinsonian signs in PD patients after intranasal NIr therapy (Zhao et al. 2003). We should note that extracranially delivered NIr may not reach the zones of pathology in the brainstem of PD patients and would only provide symptomatic effects. Hence, an intracranial system might be developed and suggested for PD patients to play neuroprotective and disease-modifying roles to maximize its therapeutic effects.
Neurotrophic factors (NTFs) therapy
Most of the current pharmacological therapies for PD focus on managing symptoms, rather than the molecular pathogenic causes. Therefore, the greatest unmet demand in PD therapy is to discover and develop disease-modifying strategies, which can halt or reverse the ongoing progression of dopaminergic neurons degeneration. One of the promising candidates for disease-modifying therapies is NTFs. NTFs are secreted growth factors that regulate survival, growth, differentiation and maintenance of neurons in both the central nervous system and the peripheral nervous system. Although many animal research suggesting the therapeutic potential of neurotrophic factors for treating neurodegenerative diseases, the clinical trials have not produced conclusive evidence to supporting their utilities as therapies (for reviews see Sullivan and Toulouse 2011; Hegarty et al. 2014; Bartus and Johnson 2016a, b). Following the series of disappointing outcomes from systemic administration of NTFs, including GDNF, CNTF, BDNF and IGF-1, to improve their therapeutic efficiency, NTFs was later tested using intrathecal, Intraventricular or intraparenchymal delivery. However, these types of delivery are associated with several practical problems, such as the poor targeting and rapid biometabolism of NTFs by endogenous enzymes in vivo. Gene therapy can overcome these limitations by incorporating the gene for the therapeutic protein into brain cells, achieving long-term and targeted delivery. Recombinant adeno-associated viral (AAV) or lentiviral vectors (LV) have been used to induce over-expression of NTFs in animal models of PD (for recent review see Kelly et al. 2015) and led to considerable advancements in the ongoing development of clinical neuroprotective therapies for PD. However, in contrast to the successful studies which used GDNF in the 6-OHDA lesion rat models, GDNF delivery by either AAV or LV vectors was not effective in preventing neurodegeneration in the AAV-α-synuclein model (Decressac et al. 2011). Further investigation demonstrated that α-synuclein overexpression downregulates the expression of Nurr1 and its downstream target, the GDNF receptor Ret, in DA neurons of the SN (Decressac et al. 2012). These findings suggest that the development of DAergic NTFs might be Ret-dependent and Ret/NTFs combined gene delivery approach or other Ret-independent NTFs should be explored (Sullivan and O’Keeffe 2016).
Gene therapy
In general, gene therapy methodology is achieved by counteracting or replacing a malfunctioning gene within the cells adversely affected by the condition. For the most part, viruses-based vectors are used to deliver therapeutic molecules including glutamic acid decarboxylase (GAD), aromatic l-amino acid decarboxylase (AADC), neurturin, and neurotrophic factors by now. A phase 1/2 trial with one-year follow-up has shown that ProSavin, a LV vector-based gene therapy to deliver tyrosine hydroxylase, GAD and AADC, significantly improves UPDES-III scores of PD patients without serious side effects (Palfi et al. 2014). Transfer of GAD with AAV2 can modulate γ-aminobutyric acid production with a great improvement of UPDRS scores over 6 months as well (LeWitt et al. 2011). Others like AAV2-hAADC and AAV2-neurturin (CERE-120) have also shown the similar therapeutic benefits and safety profiles (Marks et al. 2010; Mittermeyer et al. 2012; Bartus et al. 2013). Moreover, modified virus-based vectors and non-virus vectors are developed constantly. For examples, tropism-modified Ad5 vectors exert neuron-selective targeting property to enhance gene delivery efficiency (Lewis et al. 2014). Angiopep-conjugated nanoparticles for cellular uptake and gene expression can carry specific genes (Huang et al. 2013). A recently developed non-viral vector has been found to deliver short interfering RNA (siRNA) against the α-synuclein gene specific for neuronal cells, and prevent PD-like symptoms both in vitro and in vivo. Interestingly, this non-viral vector not only helps siRNA duplexes cross the blood–brain barrier in mice, but also stabilize these siRNAs leading to a sustainable knockdown of α-synuclein protein (Javed et al. 2016). Although recent clinical trials of gene therapy have shown remarkable therapeutic benefits and an excellent safety record, however, at this time, no study has demonstrated robust clinical benefits using rigorous double-blind assessments. In addition, as currently practiced, gene therapy for PD only addressed the cardinal motor symptoms, and the possible impacts of gene therapy on other clinical signs of PD should be further investigated.
Cell replacement therapy
Cell transplantation is available nowadays and numerous preclinical studies and several clinical trials have shown therapeutic effects of various types of stem cell transplantation, such as motor signs improvement or medication dosage reduction (O’Keeffe et al. 2008; Venkataramana et al. 2010; Gonzalez et al. 2015a, b; Han et al. 2015). Although transplantation of stem cells-derived DAergic neuron can alleviate motor deficiencies of PD, previous studies also found that tumor formation was an unacceptable complication associated with stem cells, especially embryonic stem cells (ESCs) transplantation (Bjorklund et al. 2002; Kim et al. 2002). To minimize the risk of tumor formation, a number of techniques have been developed, including prolonged pre-differentiation of ESCs, selection of differentiated cells for transplantation and genetic engineering to block tumourigenic pathways (Ambasudhan et al. 2014). In addition, Acquarone et al. (2015) pretreated undifferentiated mouse ESCs with mitomycin, then injected into striatum in nude mice. After 15-month follow-up, mitomycin-treated ESCs alleviated motor functions dramatically without unlimited cell proliferation that would be a novel replacement therapy for PD. Besides, reprogrammed neurons, such as combination of new transcriptional therapy may decrease the tumorigenic potential (Yamashita and Abe 2014). Using human unfertilized cell or induced pluripotent stem cells (iPSCs) also offers an unlimited supply for transplantation. The animal experiments confirm its safety and efficiency on motor symptoms (Gonzalez et al. 2015a, b; Han et al. 2015). In a long-term 14-year observation after DAergic neuron transplantation, the majority of transplanted neurons maintain healthy and functional, as shown by the persistent expression of DA transporters and normal mitochondrial morphologies, which proves the rationality and feasibility of cell transplantation as alternative therapy in PD (Hallett et al. 2014). Although many types of stem cells, such as ESCs, iPSCs and NSCs, have been induced into DAergic neurons for PD treatment in various animal models, so far few has been clinically proved functional for patients with PD. Besides the tumorigenic potential, the cell sources, optimal transplantation protocols, including reliable delivery system, transplantation locations and timing, also need to be further explored before clinical use of stem cells-derived DAergic neurons for the transplantation into PD patients.
Environmental enrichment (EE)
Enriched environments are normally defined as a combination of complex inanimate and social stimulation. For rodent studies, EE is generally constituted by bigger cages, with a running wheel and a few toys that are periodically changed to stimulate animal curiosity and exploration. Previous studies have suggested that EE could protect brain damage and promote neuroplasticity in various neurodegenerative animal models including PD. Faherty et al. (2005) have demonstrated that exposure to an EE procedure (a combination of exercise, social interactions and learning) during adulthood totally protects against MPTP-induced Parkinsonism. Furthermore, this neuroprotection of dopamine neurons in the nigrostriatal system might be due to the increased GDNF and decreased DAT and vesicular monoamine transporter (VMAT2) levels (Faherty et al. 2005; Zhu et al. 2005). Similar neuroprotective effects of enriched environment in PD have also been confirmed in 6-OHDA animal model (Steiner et al. 2006; Anastasía et al. 2009). Although all these preclinical findings predict significant implications of this non-pharmacological approach for the prevention and/or treatment of PD, the exact molecular mechanisms are far from being clearly understood. Much more importantly, till now the clinical efficacy of EE therapy in PD patients is rarely reported. Moreover, the containing elements and the training procedure in EE therapy for PD should be further explored before the translation of this non-pharmacological modality from benchside to bedside.
Conclusion
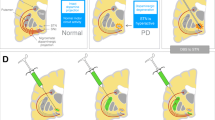
PD patients exhibit various degrees of motor impairment as well as nonmotor symptoms which include depression, apathy, cognitive impairment, sleep disturbances, and autonomic dysfunctions. In the absence of any disease-modifying therapy, the mainstay of PD treatment is pharmacologic therapy aimed at replacement of DAergic function. While this is generally effective for motor symptoms, long-term medication may fail to treat, or even worsen, troublesome nonmotor symptoms and may lead to motor complications. It is not surprising then that nearly 40 % of PD patients in US were using complementary and alternative practices in addition to or instead of conventional treatment options (Rajendran et al. 2001). Centuries of experience using conventional medical modalities (such as herbal medicines and acupuncture) and traditional physical training (includes Tai chi, Qi gong and Yoga) in Eastern countries have been proved to be effective to relieve some of PD symptoms via various mechanisms. In addition, the rapid development of modern science and technology has add new meaning into this traditional remedies and greatly promote the discovery of novel non-pharmacological therapies of PD, including DBS, NIr, gene therapy and cell replacement therapies, as well as some other complementary management (Fig. 1). All these newly developed therapeutic options have been demonstrated to be able to provide potential clinical benefits to patients with PD to relieve either motor or nonmotor deficiencies or drugs-induced side effects. Much more importantly, following the clinical usage of these alternative therapeutic options, we could learn more about the precise pathogenic mechanisms of PD and found more therapeutic targets by which to discover more disease-modifying drugs. In addition, it is proposed that these new therapies may bring promise to give new cures to not only PD, but also other neurodegenerative diseases (Nithianantharajah and Hannan 2006; Perlmutter and Mink 2006; Ljubisavljevic et al. 2013; Soligo et al. 2013).
References
Acquarone M, de Melo TM, Meireles F, Brito-Moreira J, Oliveira G, Ferreira ST, Castro NG, Tovar-Moll F, Houzel JC, Rehen SK (2015) Mitomycin-treated undifferentiated embryonic stem cells as a safe and effective therapeutic strategy in a mouse model of Parkinson’s disease. Front Cell Neurosci 9:97
Albuquerque L, Coelho M, Martins M, Guedes LC, Rosa MM, Ferreira JJ, Cattoni MB, Carvalho H, Ferreira AG, Martins IP (2014) STN-DBS does not change emotion recognition in advanced Parkinson’s disease. Parkinsonism Relat Disord 20:166–169
Ambasudhan R, Dolatabadi N, Nutter A, Masliah E, Mckercher SR, Lipton SA (2014) Potential for cell therapy in Parkinson’s disease using genetically programmed human embryonic stem cell-derived neural progenitor cells. J Comp Neurol 522:2845–2856
Anandhan A, Tamilselvam K, Vijayraja D, Ashokkumar N, Rajasankar S, Manivasagam T (2010) Resveratrol attenuates oxidative stress and improves behaviour in 1 -methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) challenged mice. Ann Neurosci 17:113–119
Anastasía A, Torre L, de Erausquin GA, Mascó DH (2009) Enriched environment protects the nigrostriatal dopaminergic system and induces astroglial reaction in the 6-OHDA rat model of Parkinson’s disease. J Neurochem 109:755–765
Ascherio A, Chen H, Schwarzschild MA, Zhang SM, Colditz GA, Speizer FE (2003) Caffeine, postmenopausal estrogen, and risk of Parkinson’s disease. Neurology 60:790–795
Baizabal-Carvallo JF, Jankovic J (2014) Deep brain stimulation of the subthalamic nucleus for peripherally induced parkinsonism. Neuromodulation 17(1):104–106
Baizabal-Carvallo JF, Jankovic J (2016) Movement disorders induced by deep brain stimulation. Parkinsonism Relat Disord 25:1–9
Bartus RT, Johnson EM Jr (2016a) Clinical tests of neurotrophic factors for human neurodegenerative diseases, part 1: where have we been and what have we learned? Neurobiol Dis. doi:10.1016/j.nbd.2016.03.027
Bartus RT, Johnson EM Jr (2016b) Clinical tests of neurotrophic factors for human neurodegenerative diseases, part 2: where do we stand and where must we go next? Neurobiol Dis. doi:10.1016/j.nbd.2016.03.026
Bartus RT, Baumann TL, Siffert J, Herzog CD, Alterman R, Boulis N, Turner DA, Stacy M, Lang AE, Lozano AM, Olanow CW (2013) Safety/feasibility of targeting the substantia nigra with AAV2-neurturin in Parkinson patients. Neurology 80:1698–1701
Beal MF, Oakes D, Shoulson I, Henchcliffe C, Galpern WR, Haas R, Juncos JL, Nutt JG, Voss TS, Ravina B, Shults CM, Helles K, Snively V, Lew MF, Griebner B, Watts A, Gao S, Pourcher E, Bond L, Kompoliti K, Agarwal P, Sia C, Jog M, Cole L, Sultana M, Kurlan R, Richard I, Deeley C, Waters CH, Figueroa A, Arkun A, Brodsky M, Ondo WG, Hunter CB, Jimenez-Shahed J, Palao A, Miyasaki JM, So J, Tetrud J, Reys L, Smith K, Singer C, Blenke A, Russell DS, Cotto C, Friedman JH, Lannon M, Zhang L, Drasby E, Kumar R, Subramanian T, Ford DS, Grimes DA, Cote D, Conway J, Siderowf AD, Evatt ML, Sommerfeld B, Lieberman AN, Okun MS, Rodriguez RL, Merritt S, Swartz CL, Martin WR, King P, Stover N, Guthrie S, Watts RL, Ahmed A, Fernandez HH, Winters A, Mari Z, Dawson TM, Dunlop B, Feigin AS, Shannon B, Nirenberg MJ, Ogg M, Ellias SA, Thomas CA, Frei K, Bodis-Wollner I, Glazman S, Mayer T, Hauser RA, Pahwa R, Langhammer A, Ranawaya R, Derwent L, Sethi KD, Farrow B, Prakash R, Litvan I, Robinson A, Sahay A, Gartner M, Hinson VK, Markind S, Pelikan M, Perlmutter JS, Hartlein J, Molho E, Evans S, Adler CH, Duffy A, Lind M, Elmer L, Davis K, Spears J, Wilson S, Leehey MA, Hermanowicz N, Niswonger S, Shill HA, Obradov S, Rajput A, Cowper M, Lessig S, Song D, Fontaine D, Zadikoff C, Williams K, Blindauer KA, Bergholte J, Propsom CS, Stacy MA, Field J, Mihaila D, Chilton M, Uc EY, Sieren J, Simon DK, Kraics L, Silver A, Boyd JT, Hamill RW, Ingvoldstad C, Young J, Thomas K, Kostyk SK, Wojcieszek J, Pfeiffer RF, Panisset M, Beland M, Reich SG, Cines M, Zappala N, Rivest J, Zweig R, Lumina LP, Hilliard CL, Grill S, Kellermann M, Tuite P, Rolandelli S, Kang UJ, Young J, Rao J, Cook MM, Severt L, Boyar K (2014) A randomized clinical trial of high-dosage coenzyme Q10 in early Parkinson disease: no evidence of benefit. JAMA Neurol 71:543–552
Benedetti MD, Bower JH, Maraganore DM, McDonnell SK, Peterson BJ, Ahlskog JE, Schaid DJ, Rocca WA (2000) Smoking, alcohol, and coffee consumption preceding Parkinson’s disease: a case-control study. Neurology 55:1350–1358
Bieschke J, Russ J, Friedrich RP, Ehrnhoefer DE, Wobst H, Neugebauer K, Wanker EE (2010) EGCG remodels mature alpha-synuclein and amyloid-beta fibrils and reduces cellular toxicity. Proc Natl Acad Sci USA 107:7710–7715
Bjorklund LM, Sánchez-Pernaute R, Chung S, Andersson T, Chen IY, McNaught KS, Brownell AL, Jenkins BG, Wahlestedt C, Kim KS, Isacson O (2002) Embryonic stem cells develop into functional dopaminergic neurons after transplantation in a Parkinson rat model. Proc Natl Acad Sci USA 99:2344–2349
Boulgarides LK, Barakatt E, Coleman-Salgado B (2014) Measuring the effect of an eight-week adaptive yoga program on the physical and psychological status of individuals with Parkinson’s disease. A pilot study. Int J Yoga Therapy 24:31–41
Burini D, Farabollini B, Iacucci S, Rimatori C, Riccardi G, Capecci M, Provinciali L, Ceravolo MG (2006) A randomised controlled cross-over trial of aerobic training versus qigong in advanced Parkinson’s disease. Eur Medicophys 42:231–238
Camilleri A, Zarb C, Caruana M, Ostermeier U, Ghio S, Hogen T, Schmidt F, Giese A, Vassallo N (2013) Mitochondrial membrane permeabilisation by amyloid aggregates and protection by polyphenols. Biochim Biophys Acta 1828:2532–2543
Canning CG, Sherrington C, Lord SR, Close JC, Heritier S, Heller GZ, Howard K, Allen NE, Latt MD, Murray SM, O’Rourke SD, Paul SS, Song J, Fung VS (2015) Exercise for falls prevention in Parkinson disease: a randomized controlled trial. Neurology 84:304–312
Caruana M, Vassallo N (2015) Tea polyphenols in Parkinson’s disease. Adv Exp Med Biol 863:117–137
Castagnoli KP, Steyn SJ, Petzer JP, Van der Schyf CJ, Castagnoli N Jr (2001) Neuroprotection in the MPTP parkinsonian C57BL/6 mouse model by a compound isolated from tobacco. Chem Res Toxicol 14:523–527
Chae Y, Lee H, Kim H, Kim CH, Chang DI, Kim KM, Park HJ (2009) Parsing brain activity associated with acupuncture treatment in Parkinson’s diseases. Mov Disord 24:1794–1802
Chan DK, Woo J, Ho SC, Pang CP, Law LK, Ng PW, Hung WT, Kwok T, Hui E, Orr K, Leung MF, Kay R (1998) Genetic and environmental risk factors for Parkinson’s disease in a Chinese population. J Neurol Neurosurg Psychiatry 65:781–784
Chanda ML, Levitin DJ (2013) The neurochemistry of music. Trends Cogn Sci 17:179–193
Checkoway H, Powers K, Smith-Weller T, Franklin GM, Longstreth WT, Swanson PD (2002) Parkinson’s disease risks associated with cigarette smoking, alcohol consumption, and caffeine intake. Am J Epidemiol 155:732–738
Chen R, Classen J, Gerloff C, Celnik P, Wassermann EM, Hallett M, Cohen LG (1997) Depression of motor cortex excitability by low-frequency transcranial magnetic stimulation. Neurology 48:1398–1403
Chen JF, Xu K, Petzer JP, Staal R, Xu YH, Beilstein M, Sonsalla PK, Castagnoli K, Castagnoli N Jr, Schwarzschild MA (2001) Neuroprotection by caffeine and A(2A) adenosine receptor inactivation in a model of Parkinson’s disease. J Neurosci 21:RC 143
Chen M, Wang T, Yue F, Li X, Wang P, Li Y, Chan P, Yu S (2014) Tea polyphenols alleviate motor impairments, dopaminergic neuronal injury, and cerebral α-synuclein aggregation in MPTP-intoxicated parkinsonian monkeys. Neuroscience 286:383–392
Chiken S, Nambu A (2016) Mechanism of deep brain stimulation: inhibition, excitation, or disruption? Neuroscientist 22:313–322
Cho SY, Shim SR, Rhee HY, Park HJ, Jung WS, Moon SK, Park JM, Ko CN, Cho KH, Park SU (2012) Effectiveness of acupuncture and bee venom acupuncture in idiopathic Parkinson’s disease. Parkinsonism Relat Disord 18:948–952
Chou YH, Hickey PT, Sundman M, Song AW, Chen NK (2015) Effects of repetitive transcranial magnetic stimulation on motor symptoms in Parkinson disease: a systematic review and meta-analysis. JAMA Neurol 72:432–440
Chung CL, Mak MK (2016) Effect of repetitive transcranial magnetic stimulation on physical function and motor signs in Parkinson’s disease: a systematic review and meta-analysis. Brain Stimul 9:475–487
Ciechanover A, Kwon YT (2015) Degradation of misfolded proteins in neurodegenerative diseases: therapeutic targets and strategies. Exp Mol Med 47:e147
Conrad GD (2014) Is Ginkgo biloba and/or a multivitamin-multimineral supplement a therapeutic option for Parkinson’s disease? A case report. Glob Adv Health Med 3:43–44
Contarino MF, Bour LJ, Verhagen R, Lourens MA, de Bie RM, van den Munckhof P, Schuurman PR (2014) Directional steering: a novel approach to deep brain stimulation. Neurology 83:1163–1169
Craig LH, Svircev A, Haber M, Juncos JL (2006) Controlled pilot study of the effects of neuromuscular therapy in patients with Parkinson’s disease. Mov Disord 21:2127–2133
Cruickshank TM, Reyes AR, Ziman MR (2015) A systematic review and meta-analysis of strength training in individuals with multiple sclerosis or Parkinson disease. Medicine (Baltimore) 94:e411
Darlot F, Moro C, El Massri N, Chabrol C, Johnstone DM, Reinhart F, Agay D, Torres N, Bekha D, Auboiroux V, Costecalde T, Peoples CL, Anastascio HD, Shaw VE, Stone J, Mitrofanis J, Benabid AL (2016) Near-infrared light is neuroprotective in a monkey model of Parkinson disease. Ann Neurol 79:59–75
de Bruin N, Doan JB, Turnbull G, Suchowersky O, Bonfield S, Hu B, Brown LA (2010) Walking with music is a safe and viable tool for gait training in Parkinson’s disease: the effect of a 13-week feasibility study on single and dual task walking. Parkinsons Dis 2010:483530
de Lau LM, Koudstaal PJ, Witteman JC, Hofman A, Breteler MM (2006) Dietary folate, vitamin B12, and vitamin B6 and the risk of Parkinson disease. Neurology 67:315–318
Decressac M, Ulusoy A, Mattsson B, Georgievska B, Romero-Ramos M, Kirik D, Bjorklund A (2011) GDNF fails to exert neuroprotection in a rat alpha-synuclein model of Parkinson’s disease. Brain 134:2302–2311
Decressac M, Kadkhodaei B, Mattsson B, Laguna A, Perlmann T, Bjorklund A (2012) alpha-Synuclein-induced down-regulation of Nurr1 disrupts GDNF signaling in nigral dopamine neurons. Sci Transl Med 4:163ra156
Diamond A, Jankovic J (2005) The effect of deep brain stimulation on quality of life in movement disorders. J Neurol Neurosurg Psychiatry 76(9):1188–1193
Dibble LE, Hale T, Marcus RL, Gerber JP, Lastayo PC (2006) The safety and feasibility of high-force eccentric resistance exercise in persons with Parkinson’s disease. Arch Phys Med Rehabil 87:1280–1282
Dibble LE, Addison O, Papa E (2009) The effects of exercise on balance in persons with Parkinson’s disease: a systematic review across the disability spectrum. J Neurol Phys Ther 33:14–26
Dissanayaka NN, Idu Jion F, Pachana NA, O’Sullivan JD, Marsh R, Byrne GJ, Harnett P (2016) Mindfulness for motor and nonmotor dysfunctions in Parkinson’s disease. Parkinsons Dis 2016:7109052
Doi H, Sakakibara R, Sato M, Hirai S, Masaka T, Kishi M, Tsuyusaki Y, Tateno A, Tateno F, Takahashi O, Ogata T (2014) Dietary herb extract rikkunshi-to ameliorates gastroparesis in Parkinson’s disease: a pilot study. Eur Neurol 71:193–195
Dong J, Cui Y, Li S, Le W (2016a) Current pharmaceutical treatments and alternative therapies of Parkinson’s disease. Curr Neuropharmacol 14:339–355
Dong J, Li S, Mo JL, Cai HB, Le WD (2016b) Nurr1-based therapies for Parkinson’s disease. CNS Neurosci Ther 22:351–359
Donoyama N, Ohkoshi N (2012) Effects of traditional Japanese massage therapy on various symptoms in patients with Parkinson’s disease: a case-series study. J Altern Complement Med 18:294–299
Donoyama N, Suoh S, Ohkoshi N (2014) Effectiveness of anma massage therapy in alleviating physical symptoms in outpatients with Parkinson’s disease: a before–after study. Complement Ther Clin Pract 20:251–261
El Massri N, Johnstone DM, Peoples CL, Moro C, Reinhart F, Torres N, Stone J, Benabid AL, Mitrofanis J (2016) The effect of different doses of near infrared light on dopaminergic cell survival and gliosis in MPTP-treated mice. Int J Neurosci 126:76–87
Elahi B, Elahi B, Chen R (2009) Effect of transcranial magnetic stimulation on Parkinson motor function—systematic review of controlled clinical trials. Mov Disord 24:357–363
Esch T, Duckstein J, Welke J, Braun V (2007) Mind/body techniques for physiological and psychological stress reduction: stress management via Tai Chi training—a pilot study. Med Sci Monit 1:CR488–CR497
Faherty CJ, Raviie Shepherd K, Herasimtschuk A, Smeyne RJ (2005) Environmental enrichment in adulthood eliminates neuronal death in experimental Parkinsonism. Brain Res Mol Brain Res 134:170–179
Fahn S (2003) Description of Parkinson’s disease as a clinical syndrome. Ann N Y Acad Sci 991:1–14
Ferretta A, Gaballo A, Tanzarella P, Piccoli C, Capitanio N, Nico B, Annese T, Di Paola M, Dell’aquila C, De Mari M, Ferranini E, Bonifati V, Pacelli C, Cocco T (2014) Effect of resveratrol on mitochondrial function: implications in parkin-associated familiar Parkinson’s disease. Biochim Biophys Acta 1842:902–915
Fitzpatrick L, Simpson J, Smith A (2010) A qualitative analysis of mindfulness-based cognitive therapy (MBCT) in Parkinson’s disease. Psychol Psychother 83:179–192
Follett KA, Torres-Russotto D (2012) Deep brain stimulation of globus pallidus interna, subthalamic nucleus, and pedunculopontine nucleus for Parkinson’s disease: which target? Parkinsonism Relat Disord 18:S165–S167
Fowler JS, Volkow ND, Wang GJ, Pappas N, Logan J, MacGregor R, Alexoff D, Shea C, Schlyer D, Wolf AP, Warner D, Zezulkova I, Cilento R (1996) Inhibition of monoamine oxidase B in the brains of smokers. Nature 379:733–736
Frazzitta G, Balbi P, Maestri R, Bertotti G, Boveri N, Pezzoli G (2013) The beneficial role of intensive exercise on Parkinson disease progression. Am J Phys Med Rehabil 92:523–532
Fregni F, Simon DK, Wu A, Pascual-Leone A (2005) Non-invasive brain stimulation for Parkinson’s disease: a systematic review and meta-analysis of the literature. J Neurol Neurosurg Psychiatry 76:1614–1623
Gonzalez C, Bonilla S, Flores AI, Cano E, Liste I (2015a) An update on human stem cell-based therapy in Parkinson’s disease. Curr Stem Cell Res Ther. doi:10.2174/1574888X10666150531172612
Gonzalez R, Garitaonandia I, Crain A, Poustovoitov M, Abramihina T, Noskov A, Jiang C, Morey R, Laurent LC, Elsworth JD, Snyder EY, Redmond DE Jr, Semechkin R (2015b) Proof of concept studies exploring the safety and functional activity of human parthenogenetic-derived neural stem cells for the treatment of Parkinson’s disease. Cell Transplant 24:681–690
González-Burgos E, Fernandez-Moriano C, Gómez-Serranillos MP (2015) Potential neuroprotective activity of Ginseng in Parkinson’s disease: a review. J Neuroimmune Pharmacol 10:14–29
González-García N, Armony JL, Soto J, Trejo D, Alegría MA, Drucker-Colín R (2011) Effects of rTMS on Parkinson’s disease: a longitudinal fMRI study. J Neurol 258:1268–1280
Goodwin VA, Richards SH, Taylor RS, Taylor AH, Campbell JL (2008) The effectiveness of exercise interventions for people with Parkinson’s disease: a systematic review and meta-analysis. Mov Disord 23:631–640
Gorell JM, Rybicki BA, Johnson CC, Peterson EL (1999) Smoking and Parkinson’s disease: a dose–response relationship. Neurology 52:115–119
Grandinetti A, Morens DM, Reed D, MacEachern D (1994) Prospective study of cigarette smoking and the risk of developing idiopathic Parkinson’s disease. Am J Epidemiol 139:1129–1138
Hackney ME, Earhart GM (2009) Effects of dance on movement control in Parkinson’s disease: a comparison of Argentine tango and American ballroom. J Rehabil Med 41:475–481
Hackney ME, Kantorovich S, Levin R, Earhart GM (2007) Effects of tango on functional mobility in Parkinson’s disease: a preliminary study. J Neurol Phys Ther 31:173–179
Hallett PJ, Cooper O, Sadi D, Robertson H, Mendez I, Isacson O (2014) Long-term health of dopaminergic neuron transplants in Parkinson’s disease patients. Cell Rep 7:1755–1761
Halliwell B (2006) Oxidative stress and neurodegeneration: where are we now? J Neurochem 97:1634–1658
Han F, Wang W, Chen B, Chen C, Li S, Lu X, Duan J, Zhang Y, Zhang YA, Guo W, Li G (2015) Human induced pluripotent stem cell-derived neurons improve motor asymmetry in a 6-hydroxydopamine-induced rat model of Parkinson’s disease. Cytotherapy 17:665–679
Hatano T, Hattori N, Kawanabe T, Terayama Y, Suzuki N, Iwasaki Y, Fujioka T, Yokukansan Parkinson’s Disease Study Group (2014) An exploratory study of the efficacy and safety of yokukansan for neuropsychiatric symptoms in patients with Parkinson’s disease. J Neural Transm 121:275–281
Healy DG, Falchi M, O’Sullivan SS, Bonifati V, Durr A, Bressman S, Brice A, Aasly J, Zabetian CP, Goldwurm S, Ferreira JJ, Tolosa E, Kay DM, Klein C, Williams DR, Marras C, Lang AE, Wszolek ZK, Berciano J, Schapira AH, Lynch T, Bhatia KP, Gasser T, Lees AJ, Wood NW, International LRRK2 Consortium (2008) Phenotype, genotype, and worldwide genetic penetrance of LRRK2-associated Parkinson’s disease: a case-control study. Lancet Neurol 7:583–590
Hegarty SV, O’Keeffe GW, Sullivan AM (2014) Neurotrophic factors: from neurodevelopmental regulators to novel therapies for Parkinson’s disease. Neural Regen Res 9:1708–1711
Hernán MA, Takkouche B, Caamaño-Isorna F, Gestal-Otero JJ (2002) A meta-analysis of coffee drinking, cigarette smoking, and the risk of Parkinson’s disease. Ann Neurol 52:276–284
Hernandez-Reif MFT, Largie S, Cullan C, Beutler J, Sanders C, Weiner W, Rodriguez-Bateman D, Zelaya L, Schanber S, Kuhn C (2002) Parkinson’s disease symptoms are differently affected by massage therapy vs. progressive muscle relaxation: a pilot study. J Bodyw Mov Ther 6:177–182
Hirsch MA, Toole T, Maitland CG, Rider RA (2003) The effects of balance training and high-intensity resistance training on persons with idiopathic Parkinson’s disease. Arch Phys Med Rehabil 84:1109–1117
Hirsch EC, Jenner P, Przedborski S (2013) Pathogenesis of Parkinson’s disease. Mov Disord 28:24–30
Houston S, McGill A (2013) A mixed-methods study into ballet for people living with Parkinson’s. Arts Health 5:103–119
Huang YZ, Edwards MJ, Rounis E, Bhatia KP, Rothwell JC (2005) Theta burst stimulation of the human motor cortex. Neuron 45:201–206
Huang R, Ma H, Guo Y, Liu S, Kuang Y, Shao K, Li J, Liu Y, Han L, Huang S, An S, Ye L, Lou J, Jiang C (2013) Angiopep-conjugated nanoparticles for targeted long-term gene therapy of Parkinson’s disease. Pharm Res 30:2549–2559
Javed H, Menon SA, Al-Mansoori KM, Al-Wandi A, Majbour NK, Ardah MT, Varghese S, Vaikath NN, Haque ME, Azzouz M, El-Agnaf OM (2016) Development of nonviral vectors targeting the brain as a therapeutic approach for Parkinson’s disease and other brain disorders. Mol Ther 24:746–758
Jeon S, Kim YJ, Kim ST, Moon W, Chae Y, Kang M, Chung MY, Lee H, Hong MS, Chung JH, Joh TH, Lee H, Park HJ (2008) Proteomic analysis of the neuroprotective mechanisms of acupuncture treatment in a Parkinson’s disease mouse model. Proteomics 8:4822–4832
Johns C, Blake D, Sinclair A (2010) Can reflexology maintain or improve the well-being of people with Parkinson’s disease? Complement Ther Clin Pract 16:96–100
Johnstone DM, el Massri N, Moro C, Spana S, Wang XS, Torres N, Chabrol C, De Jaeger X, Reinhart F, Purushothuman S, Benabid AL, Stone J, Mitrofanis J (2014) Indirect application of near infrared light induces neuroprotection in a mouse model of parkinsonism—an abscopal neuroprotective effect. Neuroscience 274:93–101
Kabat-Zinn J (2009) Full catastrophe living: using the wisdom of your body and mind to face stress, pain, and illness. Delta, New York
Kang JM, Park HJ, Choi YG, Choe IH, Park JH, Kim YS, Lim S (2007) Acupuncture inhibits microglial activation and inflammatory events in the MPTP-induced mouse model. Brain Res 1131:211–219
Kansara S, Trivedi A, Chen S, Jankovic J, Le W (2013) Early diagnosis and therapy of Parkinson’s disease: can disease progression be curbed? J Neural Transm 120:197–210
Kasture S, Pontis S, Pinna A, Schintu N, Spina L, Longoni R, Simola N, Ballero M, Morelli M (2009) Assessment of symptomatic and neuroprotective efficacy of Mucuna pruriens seed extract in rodent model of Parkinson’s disease. Neurotox Res 15:111–122
Kattenstroth JC, Kolankowska I, Kalisch T, Dinse HR (2010) Superior sensory, motor, and cognitive performance in elderly individuals with multi-year dancing activities. Front Aging Neurosci 2:31
Katz M, Luciano MS, Carlson K, Luo P, Marks WJ Jr, Larson PS, Starr PA, Follett KA, Weaver FM, Stern MB, Reda DJ, Ostrem JL, CSP 468 Study Group (2015) Differential effects of deep brain stimulation target on motor subtypes in Parkinson’s disease. Ann Neurol 77:710–719
Kelly MJ, O’Keeffe GW, Sullivan AM (2015) Viral vector delivery of neurotrophic factors for Parkinson’s disease therapy. Exp Rev Mol Med 17(e8):1–14
Khoo HM, Kishima H, Hosomi K, Maruo T, Tani N, Oshino S, Shimokawa T, Yokoe M, Mochizuki H, Saitoh Y, Yoshimine T (2014) Low-frequency subthalamic nucleus stimulation in Parkinson’s disease: a randomized clinical trial. Mov Disord 29:270–274
Kim JH, Auerbach JM, Rodríguez-Gómez JA, Velasco I, Gavin D, Lumelsky N, Lee SH, Nguyen J, Sánchez-Pernaute R, Bankiewicz K, McKay R (2002) Dopamine neurons derived from embryonic stem cells function in an animal model of Parkinson’s disease. Nature 418:50–56
Kim JY, Chung EJ, Lee WY, Shin HY, Lee GH, Choe YS, Choi Y, Kim BJ (2008) Therapeutic effect of repetitive transcranial magnetic stimulation in Parkinson’s disease: analysis of [11C] raclopride PET study. Mov Disord 23:207–211
Kim SN, Doo AR, Park JY, Bae H, Chae Y, Shim I, Lee H, Moon W, Lee H, Park HJ (2011) Acupuncture enhances the synaptic dopamine availability to improve motor function in a mouse model of Parkinson’s disease. PLoS One 6:e27566
Kim SN, Doo AR, Park JY, Choo HJ, Shim I, Park JJ, Chae Y, Lee B, Lee H, Park HJ (2014) Combined treatment with acupuncture reduces effective dose and alleviates adverse effect of l-dopa by normalizing Parkinson’s disease-induced neurochemical imbalance. Brain Res 1544:33–44
Knekt P, Kilkkinen A, Rissanen H, Marniemi J, Sääksjärvi K, Heliövaara M (2010) Serum vitamin D and the risk of Parkinson disease. Arch Neurol 67:808–811
Knight WE, Rickard NS (2001) Relaxing music prevents stressinduced increases in subjective anxiety, systolic blood pressure, and heart rate in healthy males and females. J Music Ther 38:254–272
Kyrozis A, Ghika A, Stathopoulos P, Vassilopoulos D, Trichopoulos D, Trichopoulou A (2013) Dietary and lifestyle variables in relation to incidence of Parkinson’s disease in Greece. Eur J Epidemiol 28:67–77
Lau YS, Patki G, Das-Panja K, Le WD, Ahmad SO (2011) Neuroprotective effects and mechanisms of exercise in a chronic mouse model of Parkinson’s disease with moderate neurodegeneration. Eur J Neurosci 33:1264–1274
Lewis TB, Glasgow JN, Harms AS, Standaert DG, Curiel DT (2014) Fiber-modified adenovirus for central nervous system Parkinson’s disease gene therapy. Viruses 6:3293–3310
LeWitt PA, Rezai AR, Leehey MA, Ojemann SG, Flaherty AW, Eskandar EN, Kostyk SK, Thomas K, Sarkar A, Siddiqui MS, Tatter SB, Schwalb JM, Poston KL, Henderson JM, Kurlan RM, Richard IH, Van Meter L, Sapan CV, During MJ, Kaplitt MG, Feigin A (2011) AAV2-GAD gene therapy for advanced Parkinson’s disease: a double-blind, sham-surgery controlled, randomised trial. Lancet Neurol 10:309–319
Li F, Harmer P, Fitzgerald K, Eckstrom E, Stock R, Galver J, Maddalozzo G, Batya SS (2012) Tai Chi and postural stability in patients with Parkinson’s disease. N Engl J Med 366:511–519
Li X, Li W, Liu G, Shen X, Tang Y (2015) Association between cigarette smoking and Parkinson’s disease: a meta-analysis. Arch Gerontol Geriatr 61:510–516
Lieu CA, Kunselman AR, Manyam BV, Venkiteswaran K, Subramanian T (2010) A water extract of Mucuna pruriens provides long-term amelioration of parkinsonism with reduced risk for dyskinesias. Parkinsonism Relat Disord 16:458–465
Lieu CA, Venkiteswaran K, Gilmour TP, Rao AN, Petticoffer AC, Gilbert EV, Deogaonkar M, Manyam BV, Subramanian T (2012) The antiparkinsonian and antidyskinetic mechanisms of Mucuna pruriens in the MPTP-treated nonhuman primate. Evid Based Complement Alternat Med 2012:840247
Ljubisavljevic MR, Ismail FY, Filipovic S (2013) Transcranial magnetic stimulation of degenerating brain: a comparison of normal aging, Alzheimer’s, Parkinson’s and Huntington’s disease. Curr Alzheimer Res 10:578–596
Lo YC, Shih YT, Tseng YT, Hsu HT (2012) Neuroprotective effects of san-huang-xie-xin-tang in the MPP(+)/MPTP models of Parkinson’s disease in vitro and in vivo. Evid Based Complement Alternat Med 2012:501032
Lugassy M, Gracies JM (2005) Physical therapy in Parkinson’s disease. In: Schapira AHV, Olanow CW (eds) Principles of treatment in Parkinson’s disease. Butterworth-Heinemann Elsevier, Philadelphia, pp 313–330
Maloney R, Shanks S, Maloney J (2010) The application of low-level laser therapy for the symptomatic care of late stage Parkinson’s disease: a non-controlled, non-randomized study. Am Soc Laser Med Surg Abs 2010:185
Manyam BV, Dhanasekaran M, Hare TA (2004) Neuroprotective effects of the antiparkinson drug Mucuna pruriens. Phytother Res 18:706–712
Marks WJ Jr, Bartus RT, Siffert J, Davis CS, Lozano A, Boulis N, Vitek J, Stacy M, Turner D, Verhagen L, Bakay R, Watts R, Guthrie B, Jankovic J, Simpson R, Tagliati M, Alterman R, Stern M, Baltuch G, Starr PA, Larson PS, Ostrem JL, Nutt J, Kieburtz K, Kordower JH, Olanow CW (2010) Gene delivery of AAV2-neurturin for Parkinson’s disease: a double-blind, randomised, controlled trial. Lancet Neurol 9:1164–1172
Menon V, Levitin DJ (2005) The rewards of music listening: response and physiological connectivity of the mesolimbic system. Neuroimage 28:175–184
Merola A, Zibetti M, Angrisano S, Rizzi L, Ricchi V, Artusi CA, Lanotte M, Rizzone MG, Lopiano L (2011) Parkinson’s disease progression at 30 years: a study of subthalamic deep brain-stimulated patients. Brain 134:2074–2084
Michel PP, Hirsch EC, Hunot S (2016) Understanding dopaminergic cell death pathways in Parkinson disease. Neuron 90:675–691
Mittermeyer G, Christine CW, Rosenbluth KH, Baker SL, Starr P, Larson P, Kaplan PL, Forsayeth J, Aminoff MJ, Bankiewicz KS (2012) Long-term evaluation of a phase 1 study of AADC gene therapy for Parkinson’s disease. Hum Gene Ther 23:377–381
Möckel M, Röcker L, Störk T, Vollert J, Danne O, Eichstädt H, Müller R, Hochrein H (1994) Immediate physiological responses of healthy volunteers to different types of music: cardiovascular, hormonal and mental changes. Eur J Appl Physiol Occup Physiol 68:451–459
Morens DM, Grandinetti A, Reed D, White LR, Ross GW (1995) Cigarette smoking and protection from Parkinson’s disease: false association or etiologic clue? Neurology 45:1041–1051
Morgante L, Morgante F, Moro E, Epifanio A, Girlanda P, Ragonese P, Antonini A, Barone P, Bonuccelli U, Contarino MF, Capus L, Ceravolo MG, Marconi R, Ceravolo R, D’Amelio M, Savettieri G (2007) How many parkinsonian patients are suitable candidates for deep brain stimulation of subthalamic nucleus? results of a questionnaire. Parkinsonism Relat Disord 13:528–531
Moro C, Massri NE, Torres N, Ratel D, De Jaeger X, Chabrol C, Perraut F, Bourgerette A, Berger M, Purushothuman S, Johnstone D, Stone J, Mitrofanis J, Benabid AL (2014) Photobiomodulation inside the brain: a novel method of applying near-infrared light intracranially and its impact on dopaminergic cell survival in MPTP-treated mice. J Neurosurg 120:670–683
Nirenberg MJ, Fahn S (2005) The role of levodopa and catechol-O-methyltransferase inhibitors. In: Schapira AHV, Olanow CW (eds) Principles of treatment in Parkinson’s disease. Butterworth-Heinemann Elsevier, Philadelphia, pp 3–24
Nithianantharajah J, Hannan AJ (2006) Enriched environments, experience-dependent plasticity and disorders of the nervous system. Nat Rev Neurosci 7:697–709
Nocera JR, Amano S, Vallabhajosula S, Hass CJ (2013) Tai Chi exercise to improve non-motor symptoms of Parkinson’s disease. J Yoga Phys Ther 3:137
Odekerken VJ, van Laar T, Staal MJ, Mosch A, Hoffmann CF, Nijssen PC, Beute GN, van Vugt JP, Lenders MW, Contarino MF, Mink MS, Bour LJ, van den Munckhof P, Schmand BA, de Haan RJ, Schuurman PR, de Bie RM (2013) Subthalamic nucleus versus globus pallidus bilateral deep brain stimulation for advanced Parkinson’s disease (NSTAPS study): a randomised controlled trial. Lancet Neurol 12:37–44
O’Keeffe FE, Scott SA, Tyers P, O’Keeffe GW, Dalley JW, Zufferey R, Caldwell MA (2008) Induction of A9 dopaminergic neurons from neural stem cells improves motor function in an animal model of Parkinson’s disease. Brain 131:630–641
Okun MS (2012) Deep-brain stimulation for Parkinson’s disease. N Engl J Med 367:1529–1538
Pacchetti C, Mancini F, Aglieri R, Fundarò C, Martignoni E, Nappi G (2000) Active music therapy in Parkinson’s disease: an integrative method for motor and emotional rehabilitation. Psychosom Med 62:386–393
Palacios N, Gao X, O’Reilly E, Schwarzschild M, McCullough ML, Mayo T, Gapstur SM, Ascherio AA (2012) Alcohol and risk of Parkinson’s disease in a large, prospective cohort of men and women. Mov Disord 27:980–987
Palfi S, Gurruchaga JM, Ralph GS, Lepetit H, Lavisse S, Buttery PC, Watts C, Miskin J, Kelleher M, Deeley S, Iwamuro H, Lefaucheur JP, Thiriez C, Fenelon G, Lucas C, Brugières P, Gabriel I, Abhay K, Drouot X, Tani N, Kas A, Ghaleh B, Le Corvoisier P, Dolphin P, Breen DP, Mason S, Guzman NV, Mazarakis ND, Radcliffe PA, Harrop R, Kingsman SM, Rascol O, Naylor S, Barker RA, Hantraye P, Remy P, Cesaro P, Mitrophanous KA (2014) Long-term safety and tolerability of ProSavin, a lentiviral vector-based gene therapy for Parkinson’s disease: a dose escalation, open-label, phase 1/2 trial. Lancet 383:1138–1146
Park HJ, Lim S, Joo WS, Yin CS, Lee HS, Lee HJ, Seo JC, Leem K, Son YS, Kim YJ, Kim CJ, Kim YS, Chung JH (2003) Acupuncture prevents 6-hydroxydopamine-induced neuronal death in the nigrostriatal dopaminergic system in the rat Parkinson’s disease model. Exp Neurol 180:93–98
Park JY, Choi H, Baek S, Jang J, Lee A, Jeon S, Kim J, Park HJ (2015) p53 signalling mediates acupuncture-induced neuroprotection in Parkinson’s disease. Biochem Biophys Res Commun 460:772–779
Pascual-Leone A, Valls-Solé J, Wassermann EM, Hallett M (1994a) Responses to rapid-rate transcranial magnetic stimulation of the human motor cortex. Brain 117:847–858
Pascual-Leone A, Valls-Solé J, Brasil-Neto JP, Cammarota A, Grafman J, Hallett M (1994b) Akinesia in Parkinson’s disease, II: effects of subthreshold repetitive transcranial motor cortex stimulation. Neurology 4:892–898
Paterson C, Allen JA, Browning M, Barlow G, Ewings P (2005) A pilot study of therapeutic massage for people with Parkinson’s disease: the added value of user involvement. Complement Ther Clin Pract 11:161–171
Perlmutter JS, Mink JW (2006) Deep brain stimulation. Annu Rev Neurosci 29:229–257
Petzer JP, Petzer A (2015) Caffeine as a lead compound for the design of therapeutic agents for the treatment of Parkinson’s disease. Curr Med Chem 22:975–988
Pickut B, Van Hecke W, Kerckhofs E, Mariën P, Vanneste S, Cras P, Parizel PM (2013) Mindfulness based intervention in Parkinson’s disease leads to structural brain changes on MRI: a randomized controlled longitudinal trial. Clin Neurol Neurosurg 115:2419–2425
Pickut B, Vanneste S, Hirsch MA, Van Hecke W, Kerckhofs E, Mariën P, Parizel PM, Crosiers D, Cras P (2015) Mindfulness training among individuals with Parkinson’s disease: neurobehavioral effects. Parkinsons Dis 2015:816404
Pienaar IS, Lee CH, Elson JL, McGuinness L, Gentleman SM, Kalaria RN, Dexter DT (2015) Deep-brain stimulation associates with improved microvascular integrity in the subthalamic nucleus in Parkinson’s disease. Neurobiol Dis 74:392–405
Poewe W (2009) Treatments for Parkinson disease—past achievements and current clinical needs. Neurology 72:S65–S73
Polito L, Greco A, Seripa D (2016) Genetic profile, environmental exposure, and their Interaction in Parkinson’s disease. Parkinsons Dis 2016:6465793
Rabey JM, Vered Y, Shabtai H, Graff E, Korczyn AD (1992) Improvement of parkinsonian features correlate with high plasma levodopa values after broad bean (Vicia faba) consumption. J Neurol Neurosurg Psychiatry 55:725–727
Rajendran PR, Thompson RE, Reich SG (2001) The use of alternative therapies by patients with Parkinson’s disease. Neurology 57:790–794
Reinhart F, Massri NE, Chabrol C, Cretallaz C, Johnstone DM, Torres N, Darlot F, Costecalde T, Stone J, Mitrofanis J, Benabid AL, Moro C (2015a) Intracranial application of near-infrared light in a hemi-parkinsonian rat model: the impact on behavior and cell survival. J Neurosurg 2015:1–13
Reinhart F, Massri NE, Darlot F, Torres N, Johnstone DM, Chabrol C, Costecalde T, Stone J, Mitrofanis J, Benabid AL, Moro C (2015b) 810 nm near-infrared light offers neuroprotection and improves locomotor activity in MPTP-treated mice. Neurosci Res 92:86–90
Ren XM (2008) Fifty cases of Parkinson’s disease treated by acupuncture combined with madopar. J Tradit Chin Med 28:255–257
Rizzone MG, Fasano A, Daniele A, Zibetti M, Merola A, Rizzi L, Piano C, Piccininni C, Romito LM, Lopiano L, Albanese A (2014) Long-term outcome of subthalamic nucleus DBS in Parkinson’s disease: from the advanced phase towards the late stage of the disease? Parkinsonism Relat Disord 20:376–381
Rojas P, Montes P, Rojas C, Serrano-García N, Rojas-Castañeda JC (2012a) Effect of a phytopharmaceutical medicine, Ginko biloba extract 761, in an animal model of Parkinson’s disease: therapeutic perspectives. Nutrition 28:1081–1088
Rojas P, Ruiz-Sánchez E, Rojas C, Ogren SO (2012b) Ginkgo biloba extract (EGb 761) modulates the expression of dopamine-related genes in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced Parkinsonism in mice. Neuroscience 223:246–257
Roper JA, Kang N, Ben J, Cauraugh JH, Okun MS, Hass CJ (2016) Deep brain stimulation improves gait velocity in Parkinson’s disease: a systematic review and meta-analysis. J Neurol 263:1195–1203
Rui G, Guangjian Z, Yong W, Jie F, Yanchao C, Xi J, Fen L (2013) High frequency electro-acupuncture enhances striatum DAT and D1 receptor expression, but decreases D2 receptor level in 6-OHDA lesioned rats. Behav Brain Res 237:263–269
Sáez-Zea C, Escamilla-Sevilla F, Katati MJ, Mínguez-Castellanos A (2012) Cognitive effects of subthalamic nucleus stimulation in Parkinson’s disease: a controlled study. Eur Neurol 68:361–366
Sasco AJ, Paffenbarger RS (1990) Smoking and Parkinson’s disease. Epidemiology 1:460–465
Scandalis TA, Bosak A, Berliner JC, Helman LL, Wells MR (2001) Resistance training and gait function in patients with Parkinson’s disease. Am J Phys Med Rehabil 80:38–43
Schapira AHV, Olanow CW (2005) The medical management of Parkinson’s disease. In: Schapira AHV, Olanow CW (eds) Principles of treatment in Parkinson’s disease. Butterworth-Heinemann Elsevier, Philadelphia, pp 119–143
Schmitz-Hübsch T, Pyfer D, Kielwein K, Fimmers R, Klockgether T, Wüllner U (2006) Qigong exercise for the symptoms of Parkinson’s disease: a randomized, controlled pilot study. Mov Disord 21:543–548
Sconce MD, Churchill MJ, Greene RE, Meshul CK (2015) Intervention with exercise restores motor deficits but not nigrostriatal loss in a progressive MPTP mouse model of Parkinson’s disease. Neuroscience 299:156–174
Sharma NK, Robbins K, Wagner K, Colgrove YM (2015) A randomized controlled pilot study of the therapeutic effects of yoga in people with Parkinson’s disease. Int J Yoga 8:74–79
Sharp K, Hewitt J (2014) Dance as an intervention for people with Parkinson’s disease: a systematic review and meta-analysis. Neurosci Biobehav Rev 47:445–456
Shaw VE, Keay KA, Ashkan K, Benabid AL, Mitrofanis J (2010) Dopaminergic cells in the periaqueductal grey matter of MPTP-treated monkeys and mice; patterns of survival and effect of deep brain stimulation and lesion of the subthalamic nucleus. Parkinsonism Relat Disord 16:338–344
Shen YF, Tang Y, Zhang XJ, Huang KX, Le WD (2013) Adaptive changes in autophagy after UPS impairment in Parkinson’s disease. Acta Pharmacol Sin 34:667–673
Shirota Y, Hamada M, Ugawa Y (2016) Clinical applications of rTMS in Parkinson’s disease. In: Platz T (ed) Therapeutic rTMS in neurology: principles, evidence, and practice recommendations. Springer, Berlin, pp 129–145
Shulman LM, Katzel LI, Ivey FM, Sorkin JD, Favors K, Anderson KE, Smith BA, Reich SG, Weiner WJ, Macko RF (2013) Randomized clinical trial of 3 types of physical exercise for patients with Parkinson disease. JAMA Neurol 70:183–190
Shults CW, Haas RH, Passov D, Beal MF (1997) Coenzyme Q10 levels correlate with the activities of complexes I and II/III in mitochondria from parkinsonian and nonparkinsonian subjects. Ann Neurol 42:261–264
Soligo M, Nori SL, Protto V, Florenzano F, Manni L (2013) Acupuncture and neurotrophin modulation. Int Rev Neurobiol 111:91–124
Speelman AD, van de Warrenburg BP, van Nimwegen M, Petzinger GM, Munneke M, Bloem BR (2011) How might physical activity benefit patients with Parkinson disease? Nat Rev Neurol 7:528–534
Spieles-Engemann AL, Steece-Collier K, Behbehani MM, Collier TJ, Wohlgenant SL, Kemp CJ, Cole-Strauss A, Levine ND, Gombash SE, Thompson VB, Lipton JW, Sortwell CE (2011) Subthalamic nucleus stimulation increases brain derived neurotrophic factor in the nigrostriatal system and primary motor cortex. J Parkinsons Dis 1:123–136
Stallibrass C, Sissons P, Chalmers C (2002) Randomized controlled trial of the Alexander technique for idiopathic Parkinson’s disease. Clin Rehabil 16:695–708
Steiner B, Winter C, Hosman K, Siebert E, Kempermann G, Petrus DS, Kupsch A (2006) Enriched environment induces cellular plasticity in the adult substantia nigra and improves motor behavior function in the 6-OHDA rat model of Parkinson’s disease. Exp Neurol 199:291–300
Strafella AP, Paus T, Barrett J, Dagher A (2001) Repetitive transcranial magnetic stimulation of the human prefrontal cortex induces dopamine release in the caudate nucleus. J Neurosci 21:RC 157
Sullivan AM, O’Keeffe GW (2016) Neurotrophic factor therapy for Parkinson’s disease: past, present and future. Neural Regen Res 11:205–207
Sullivan AM, Toulouse A (2011) Neurotrophic factors for the treatment of Parkinson’s disease. Cytokine Growth Factor Rev 22:157–165
Svensson M, Lexell J, Deierborg T (2015) Effects of physical exercise on neuroinflammation, neuroplasticity, neurodegeneration, and behavior: what we can learn from animal models in clinical settings. Neurorehabil Neural Repair 29:577–589
Tan EK, Tan C, Fook-Chong SMC, Lum SY, Chai A, Chung H, Shen H, Zhao Y, Teoh ML, Yih Y, Pavanni R, Chandran VR, Wong MC (2003) Dose-dependent protective effect of coffee, tea, and smoking in Parkinson’s disease: a study in ethnic Chinese. J Neurol Sci 216:163–167
Tan LC, Koh W-P, Yuan J-M, Wang R, Au W-L, Tan JH, Tan E-K, Yu MC (2008) Differential effects of black versus green tea on risk of Parkinson’s disease in the Singapore Chinese Health Study. Am J Epidemiol 167:553–560
Tang Y, Li T, Li J, Yang J, Liu H, Zhang XJ, Le W (2014) Jmjd3 is essential for the epigenetic modulation of microglia phenotypes in the immune pathogenesis of Parkinson’s disease. Cell Death Differ 21:369–380
Tarsy D (2012) Treatment of Parkinson disease: a 64-year-old man with motor complications of advanced Parkinson disease. JAMA 307:2305–2314
Tomlinson CL, Patel S, Meek C, Herd CP, Clarke CE, Stowe R, Shah L, Sackley CM, Deane KH, Wheatley K, Ives N (2013) Physiotherapy versus placebo or no intervention in Parkinson’s disease. Cochrane Database Syst Rev 9:CD002817
Tomlinson CL, Herd CP, Clarke CE, Meek C, Patel S, Stowe R, Deane KH, Shah L, Sackley CM, Wheatley K, Ives N (2014) Physiotherapy for Parkinson’s disease: a comparison of techniques. Cochrane Database Syst Rev 6:CD002815
Toosizadeh N, Lei H, Schwenk M, Sherman SJ, Sternberg E, Mohler J, Najafi B (2015) Does integrative medicine enhance balance in aging adults? Proof of concept for the benefit of electroacupuncture therapy in Parkinson’s disease. Gerontology 61:3–14
Törnhage CJ, Skogar Ö, Borg A, Larsson B, Robertsson L, Andersson L, Andersson L, Backström P, Fall PA, Hallgren G, Bringer B, Carlsson M, Lennartsson UB, Sandbjörk H, Lökk J (2013) Short- and long-term effects of tactile massage on salivary cortisol concentrations in Parkinson’s disease: a randomised controlled pilot study. BMC Complement Alternat Med 13:357
Trevitt J, Kawa K, Jalali A, Larsen C (2009) Differential effects of adenosine antagonists in two models of parkinsonian tremor. Pharmacol Biochem Behav 94:24–29
Tsang WW (2013) Tai Chi training is effective in reducing balance impairments and falls in patients with Parkinson’s disease. J Physiother 59:55
Tuon T, Souza PS, Santos MF, Pereira FT, Pedroso GS, Luciano TF, De Souza CT, Dutra RC, Silveira PC, Pinho RA (2015) Physical training regulates mitochondrial parameters and neuroinflammatory mechanisms in an experimental model of Parkinson’s disease. Oxid Med Cell Longev 2015:261809
Uc EY, Doerschug KC, Magnotta V, Dawson JD, Thomsen TR, Kline JN, Rizzo M, Newman SR, Mehta S, Grabowski TJ, Bruss J, Blanchette DR, Anderson SW, Voss MW, Kramer AF, Darling WG (2014) Phase I/II randomized trial of aerobic exercise in Parkinson disease in a community setting. Neurology 83:413–425
Uhrbrand A, Stenager E, Pedersen MS, Dalgas U (2015) Parkinson’s disease and intensive exercise therapy—a systematic review and meta-analysis of randomized controlled trials. J Neurol Sci 353:9–19
van der Kolk NM, King LA (2013) Effects of exercise on mobility in people with Parkinson’s disease. Mov Disord 28:1587–1596
Venkataramana NK, Kumar SK, Balaraju S, Radhakrishnan RC, Bansal A, Dixit A, Rao DK, Das M, Jan M, Gupta PK, Totey SM (2010) Open-labeled study of unilateral autologous bone-marrow-derived mesenchymal stem cell transplantation in Parkinson’s disease. Transl Res 155:62–70
Verstraeten A, Theuns J, Van Broeckhoven C (2015) Progress in unraveling the genetic etiology of Parkinson disease in a genomic era. Trends Genet 31:140–149
Vivar C, Peterson BD, van Praag H (2016) Running rewires the neuronal network of adult-born dentate granule cells. Neuroimage 131:29–41
Vonloh M, Chen R, Kluger B (2013) Safety of transcranial magnetic stimulation in Parkinson’s disease: a review of the literature. Parkinsonism Relat Disord 19:573–585
Wallace BA, Ashkan K, Heise CE, Foote KD, Torres N, Mitrofanis J, Benabid AL (2007) Survival of midbrain dopaminergic cells after lesion or deep brain stimulation of the subthalamic nucleus in MPTP-treated monkeys. Brain 130:2129–2145
Wang J, Xu HM, Yang HD, Du XX, Jiang H, Xie JX (2009) Rg1 reduces nigral iron levels of MPTP-treated C57BL6 mice by regulating certain iron transport proteins. Neurochem Int 54:43–48
Wang HM, Yang MH, Liu Y, Li SD, Li M (2014) Effectiveness of Bushen Huoxue Granule on 5-serotonin and norepinephrine in the brain of Parkinson’s disease patients with depressive state. Chin J Integr Med 20:944–948
Wang L, Evatt ML, Maldonado LG, Perry WR, Ritchie JC, Beecham GW, Martin ER, Haines JL, Pericak-Vance MA, Vance JM, Scott WK (2015) Vitamin D from different sources is inversely associated with Parkinson disease. Mov Disord 30:560–566
Warner TT, Schapira AH (2003) Genetic and environmental factors in the cause of Parkinson’s disease. Ann Neurol 53(Suppl 3):S16–S25
Weaver FM, Follett KA, Stern M, Luo P, Harris CL, Hur K, Marks WJ Jr, Rothlind J, Sagher O, Moy C, Pahwa R, Burchiel K, Hogarth P, Lai EC, Duda JE, Holloway K, Samii A, Horn S, Bronstein JM, Stoner G, Starr PA, Simpson R, Baltuch G, De Salles A, Huang GD, Reda DJ, CSP 468 Study Group (2012) Randomized trial of deep brain stimulation for Parkinson disease: thirty-six-month outcomes. Neurology 79:55–65
Wu SY, Wang TF, Yu L, Jen CJ, Chuang JI, Wu FS, Wu CW, Kuo YM (2011) Running exercise protects the substantia nigra dopaminergic neurons against inflammation-induced degeneration via the activation of BDNF signaling pathway. Brain Behav Immun 25:135–146
Xie T, Vigil J, MacCracken E, Gasparaitis A, Young J, Kang W, Bernard J, Warnke P, Kang UJ (2015) Low-frequency stimulation of STN-DBS reduces aspiration and freezing of gait in patients with PD. Neurology 84:415–420
Xu Z, Chen S, Li X, Luo G, Li L, Le W (2006) Neuroprotective effects of (–)-epigallocatechin-3-gallate in a transgenic mouse model of amyotrophic lateral sclerosis. Neurochem Res 31:1263–1269
Yadav SK, Prakash J, Chouhan S, Singh SP (2013) Mucuna pruriens seed extract reduces oxidative stress in nigrostriatal tissue and improves neurobehavioral activity in paraquat-induced Parkinsonian mouse model. Neurochem Int 62:1039–1047
Yamashita T, Abe K (2014) Direct reprogrammed neuronal cells as a novel resource for cell transplantation therapy. Cell Transplant 23:435–439
Yang DH, Shi Y, Jia YM (2006) Influence of acupuncture plus drug in the amelioration of symptoms and blood antioxidant system of patients with Parkinson’s disease. Chin J Chin Rehabil 10:14–16
Yang Y, Li XY, Gong L, Zhu YL, Hao YL (2014) Tai Chi for improvement of motor function, balance and gait in Parkinson’s disease: a systematic review and meta-analysis. PLoS One 9:e102942
Yoshitake T, Yoshitake S, Kehr J (2010) The Ginkgo biloba extract EGb 761(R) and its main constituent flavonoids and ginkgolides increase extracellular dopamine levels in the rat prefrontal cortex. Br J Pharmacol 159:659–668
Zanjani A, Zakzanis KK, Daskalakis ZJ, Chen R (2015) Repetitive transcranial magnetic stimulation of the primary motor cortex in the treatment of motor signs in Parkinson’s disease: a quantitative review of the literature. Mov Disord 30:750–758
Zeng BY, Zhao K (2016) Effect of acupuncture on the motor and nonmotor symptoms in Parkinson’s disease—a review of clinical studies. CNS Neurosci Ther 22:333–341
Zhang F, Shi JS, Zhou H, Wilson B, Hong JS, Gao HM (2010) Resveratrol protects dopamine neurons against lipopolysaccharide-induced neurotoxicity through its anti-inflammatory actions. Mol Pharmacol 78:466–477
Zhang D, Jiang H, Xie J (2014) Alcohol intake and risk of Parkinson’s disease: a meta-analysis of observational studies. Mov Disord 29:819–822
Zhao G, Guo K, Dan J (2003) 36 case analysis of Parkinson’s disease treated by endonasal low energy He-Ne laser. Acta Acad Med Qingdao Univ 39:398
Zhou T, Zu G, Zhang X, Wang X, Li S, Gong X, Liang Z, Zhao J (2016) Neuroprotective effects of ginsenoside Rg1 through the Wnt/β-catenin signaling pathway in both in vivo and in vitro models of Parkinson’s disease. Neuropharmacology 101:480–489
Zhu J, Apparsundaram S, Bardo MT, Dwoskin LP (2005) Environmental enrichment decreases cell surface expression of the dopamine transporter in rat medial prefrontal cortex. J Neurochem 93:1434–1443
Zigmond MJ, Smeyne RJ (2014) Exercise: is it a neuroprotective and if so, how does it work? Parkinsonism Relat Disord 20(Suppl 1):S123–S127
Zou Y (2006) Clinical observation on acupuncture treatment of Parkinson’s syndrome. J Acupunct Tuina Sci 4:211–212
Zuo L, Motherwell MS (2013) The impact of reactive oxygen species and genetic mitochondrial mutations in Parkinson’s disease. Gene 532:18–23
Acknowledgments
This review was supported by grants from the National Natural Science Foundation of China (81370470 and 81430021), the Program for Liaoning Innovative Research Team in University (LT2015009), the Scientific Research Fund of Liaoning Provincial Education Department (L2015145) and Liaoning Science and Technology Project (2015225008).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) confirm that this article content has no conflict of interest.
Additional information
S. Li and J. Dong contributed equally to this work.
Rights and permissions
About this article
Cite this article
Li, S., Dong, J., Cheng, C. et al. Therapies for Parkinson’s diseases: alternatives to current pharmacological interventions. J Neural Transm 123, 1279–1299 (2016). https://doi.org/10.1007/s00702-016-1603-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-016-1603-9