Abstract
Background
While pure mesenchymal stem cell (MSC) treatment for spinal cord injury (SCI) is known to be safe, its efficacy is insufficient. Therefore, gene-modified stem cells are being developed to enhance the effect of pure MSCs. We investigated the effect of stem cell therapy through the transfection of a Wnt3a-producing gene that stimulates axonal regeneration.
Method
MSCs obtained from the human umbilical cord blood (hMSCs) were multiplied, cultivated, and transfected with the pLenti-Wnt3a-GFP viral vector to produce Wnt3a-secreting hMSCs. A total of 50 rats were injured with an Infinite Horizon impactor at the level of the T7-8 vertebrae. Rats were divided into five groups according to the transplanted material: (1) phosphate-buffered saline injection group (sham group, n = 10); (Pertz et al. Proc Natl Acad Sci USA 105:1931–1936, 39) Wnt3a protein injection group (Wnt3a protein group, n = 10); (3) hMSC transplantation group (MSC group, n = 10); (4) hMSCs transfected with the pLenti vector transplantation group (pLenti-MSC group, n = 10); (5) hMSCs transfected with the pLenti+Wnt3a vector transplantation group (Wnt3a-MSC group, n = 10). Behavioral tests were performed daily for the first 3 days after injury and then weekly for 8 weeks. The injured spinal cords were extracted, and axonal regeneration markers including choline acetyltransferase (ChAT), growth-associated protein 43 (GAP43), and microtubule-associated protein 2 (MAP2) were investigated by immunofluorescence, RT-PCR, and western blotting.
Results
Seven weeks after the transplantation (8 weeks after SCI), rats in the Wnt3a-MSC group achieved significantly higher average scores in the motor behavior tests than those in the other groups (p < 0.05). Immunofluorescent stains showed greater immunoreactivity of ChAT, GAP43, and MAP2 in the Wnt3a-MSC group than in the other groups. RT-PCR and western blots revealed greater expression of these proteins in the Wnt3a-MSC group than in the other groups (p < 0.05).
Conclusions
Wnt3a-secreting hMSC transplantation considerably improved neurological recovery and axonal regeneration in a rat SCI model.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Spinal cord injury (SCI) in humans is generally known to produce irreversible neurological deficits due to the lack of regeneration of injured axons and reorganization of the remaining circuitry in the adult central nervous system (CNS) [7]. Therefore, promoting axonal regeneration is an important prerequisite for effective recovery from SCI [12, 24, 27].
Trophic factors such as the nerve growth factor, vascular endothelial growth factor, and brain-derived neurotrophic factor are thought to play a role in promoting axonal regeneration after SCI in rats [9, 44]. In addition, Wnt proteins inhibit glycogen synthase kinase 3 (GSK-3), which suppresses axonal elongation through a canonical signaling transduction pathway, and facilitates axonal regeneration and activation of neurotrophins [3, 40]. Wnt proteins are known as significant regulators of cell proliferation, self-renewal, specification, and neural precursor differentiation in the CNS [22]. They also play important roles in axon development during the formation of the nervous system, by acting as bi-functional axon-guidance molecules [22]. Particularly, several Wnt proteins mediate guidance of corticospinal tract axons along the spinal cord.
Of these, Wnt-1 and Wnt-3a control spinal cord dorsal interneuron differentiation [21]. In addition, we have demonstrated the axonal regenerative effects of Wnt3a-secreting fibroblasts in SCI rat models [37, 45].
Mesenchymal stem cells (MSCs) are multipotent cells that can differentiate along several mesenchymal pathways into multiple cell types, including chondrocytes, osteoblasts, and adipocytes [5]. In addition, transplanted MSCs have therapeutic effects in a rat SCI model through increased tissue preservation, decreased cyst and injury size, and increased axonal regeneration [1, 13, 20, 25, 34, 35, 41, 43]. Among the MSCs, human bone marrow-derived MSCs are more widely studied because of their high multipotency; we have shown evidence of MSC transplantation efficacy in clinical trials of patients with SCI [33, 36]. However, we acknowledged that the therapeutic effect of pure MSCs is insufficient, despite its known safety.
Based on the evidence of the safety and therapeutic potential of MSCs, we investigated a more powerful method to enhance their therapeutic effect on SCI. We developed Wnt3a-secreting human mesenchymal stem cells (hMSCs) by transfecting the Wnt3a gene into hMSCs, and evaluated their therapeutic effectiveness using a rat model of SCI.
Materials and methods
Animal preparation
A total of 50 female Sprague–Dawley rats (Orient Bio, Seongnam, Korea) weighing 250–300 g at the time of injury were used. Before injury, all the rats were housed as groups of three per cage under simulated daylight conditions with alternating 12-h light–dark cycles, with food and water provided ad libitum. The animal experiments were approved by the Institutional Animal Care and Use Committee of the Asan Institute for Life Sciences, Seoul, Republic of Korea.
Each rat was anesthetized with 2% isoflurane. Next, the vertebral column was exposed between T7 and T8, and a total laminectomy was performed at T7 without incision of the dura. A moderate spinal cord injury was induced by a 250-kdyn force using an Infinite Horizon (IH) impactor (Precision System and Instrumentation, Fairfax, VA, USA). After the procedure, the contusion site was washed with normal saline, and the skin was closed. Each rat was administered a subcutaneous injection of cefazolin (10 mg/kg) as a prophylactic antibiotic. For pain management, each animal was administered a subcutaneous injection of ketoprofen (5 mg/kg) once daily for 3 days. After the injury, all the rats were housed individually in the same pre-injury environment. Their bladders were emptied manually thrice a day until spontaneous control of urination returned.
The rats were divided into five groups: (1) 15 μl phosphate-buffered saline (PBS) injection only group (sham group, n = 10); [39] Wnt3a protein injection group (Wnt3a protein group, n = 10); (3) hMSC transplantation group (MSC group, n = 10); (4) hMSC transfected with pLenti vector transplantation group (pLenti-MSC group, n = 10); (5) hMSC transfected with pLenti+Wnt3a vector transplantation group (Wnt3a-MSC group, n = 10).
Cell preparation
The cells were prepared as reported previously [23, 54]. In this study, MSCs derived from human umbilical cord blood were multiplied and cultivated in alpha modification Eagle medium (a-MEM; HyClone, Logan, WY, USA) at 37°C and 5% CO2.
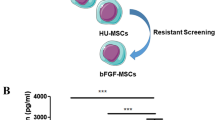
For the production of Wnt3a-secreting hMSCs, pLenti-Wnt3a-GFP vector, made by combining the pLenti-viral vector with the mouse Wnt3a gene, was transfected into MSCs at a rate of 3:1 by colonizing for 36 h. The prepared cells were identified by GFP expression observed using confocal microscopy (Carl Zeiss Meditec, Jena, Germany) after cultivation in media mixed with 2.5 μl/ml puromycin for an additional 48 h. Enzyme-linked immunosorbent assay (ELISA; Immunodiagnostic Systems Holdings, Boldon, UK) was performed for the quantitative analysis of Wnt3a expression from 5 × 105 selected Wnt3a-secreting hMSCs 24 h after culture selection.
The procedure for preparation of MSCs with the control viral vector was similar to that of Wnt3a-secreting hMSCs, except that pLenti vectors without the Wnt3a gene domain were transfected. In the preparation of the Wnt3a protein, 300 pg of the recombinant mouse Wnt3a protein (R&D Systems, Minneapolis, MN, USA) were dissolved in 15 μl of PBS. Later, the Wnt3a protein solution was injected at the rate of 1 μl/min.
Cell transplantation
One week after SCI, all rats were anesthetized using the same method, and the injured site of the spinal cord was re-exposed. The cells were delivered at a rate of 1 μl/min using a 25-μl Hamilton syringe (Hamilton Company, Reno, NV, USA) with a 33-gauge micro-needle, which was inserted into the center of the contusion site at a rate of 1 mm/min at a 1-mm depth from the dorsal dura without a dura opening. The injected number of cells in each group for transplantation was 1 × 106 cells/15 μl. In the Wnt3a protein group, 300 pg/15 μl Wnt3a protein solution was delivered at the rate of 1 μl/min. After injection, the needle was left for 3 min and was then withdrawn at a rate of 1 mm/min to avoid regurgitation of the injected materials. The surgical site was then re-closed.
Behavioral tests
After the preparation of the rat SCI models we assessed the neurological functions of each rat according to the Basso–Beattie–Bresnahan (BBB) locomotor rating scale and the ladder rung test [6, 30]. The behavioral tests were performed on the 1st, 2nd, and 3rd day after injury, and then weekly for 8 weeks. Before the BBB test, each rat was allowed to adapt to the open field (90 cm × 90 cm, 10 cm wall height). Once the rat had demonstrated acclimatization by walking continuously in the open field, the locomotor performance was recorded with a video camera for 10 min. From the video, an examiner blinded to the group-identification information used the video to quantitatively assess the locomotor performance of each rat according to the BBB scale.
The ladder rung test was performed on a 1.2-m runway. A total of 80 rungs (bars) of 0.5-cm diameter were separated by 1.5 cm. The number of adequate steps for every ten steps on the bars was calculated, and the evaluation was repeated three times. The behavioral test scores for all the groups were analyzed by one-way ANOVA followed by a post-hoc Tukey–Kramer multiple comparison test. All statistical analyses were performed using SPSS 12.0.1 (SPSS, Chicago, IL, USA). Results with p values < 0.05 were considered statistically significant.
Immunofluorescence
For the immunofluorescence analysis, the rats were sacrificed and perfused with PBS and 4% paraformaldehyde (PFA; Sigma Aldrich, St. Louis, MO, USA) at 7 weeks after transplantation (8 weeks after SCI). A 20-mm length of the spinal cord centered on the lesion site was extracted and fixed with 4% PFA for 6 h, followed by incubation with 30% sucrose in PBS overnight. Serial longitudinal spinal cord sections with 10-μm thickness were obtained every 50 μm with a cryotome (Microm, Waldorf, Germany) and mounted on poly-L-lysine-coated Superfrost Plus slides (Matsunami, Osaka, Japan). The sections were washed three times with Tris-buffered saline (TBS) and then blocked with TBS containing 5% bovine serum albumin and 0.1% Triton X-100 for 1 h at room temperature. The sections were incubated overnight with the primary antibody at 4 °C, washed three times with TBS, and then incubated with the fluorescent-conjugated secondary antibody (1:1,000; Invitrogen, Carlsbad, CA, USA). Primary monoclonal antibodies against choline acetyltransferase (ChAT, 1:200; Abcam, Cambridge, UK), growth-associated protein 43 (GAP43, 1:200; Abcam), and microtubule-associated protein 2 (MAP2, 1:200; Abcam) were used. Sections were observed under a fluorescence microscope (Carl Zeiss Meditec, Jena, Germany).
Reverse transcription polymerase chain reaction (RT-PCR)
Injury epicenters (0.5 cm in size) harvested 8 weeks after SCI were extracted. For RNA isolation, 1 ml TRIzol® reagent (Invitrogen) was added per 100 mg of spinal cord specimen, homogenized with a pestle and mortar in liquid nitrogen, and washed with 1 ml diethylpyrocarbonate-treated water (Invitrogen). The homogenized samples were incubated for 5 min at room temperature, and 200 μl of chloroform (Sigma Aldrich) was added per 1 ml of TRIzol® reagent. The samples were vigorously hand-shaken for 15 s, incubated for 3 min, and divided, following centrifugation at 12,000 g for 10 min at 4 °C. The aqueous phase was transferred to a fresh tube (1.5 ml), and 500 μl of isopropyl alcohol (Sigma Aldrich) was added per 1 ml of TRIzol® reagent. The samples were incubated at room temperature for 10 min and centrifuged at 12,000 g for 10 min at 4 °C. The RNA was washed by centrifugation at 7,500 g for 5 min at 4 °C after supernatant removal, and 1 ml of 75% ethanol was added per 1 ml of TRIzol® reagent. The RNA pellet was briefly dried and dissolved in RNase-free water and incubated for 10 min at 60 °C. The cDNA mixture was incubated at 65 °C for 5 min, placed on ice for 1 min, and then incubated at 50 °C for 50 min in the following cDNA synthesis mixture: 2 μl 10× reverse transcriptase (RT) buffer, 4 μl 25 mM MgCl2, 2 μl 0.1 M DTT, 1 μl RNase OUT™ (40 U/μl; Invitrogen), and 1 μl Superscript™ III RT (200 U/μl; Invitrogen). The mixture was placed at 85 °C for 5 min, chilled on ice, and then briefly centrifuged. Following the addition of 1 μl of RNase H, the sample was incubated for 20 min at 37 °C. For the PCR mixture, sense and antisense primers (Table 1), template DNA, and distilled water were used. PCR was performed under the following conditions: 10 min at 95 °C, followed by 30 cycles of 50 s at 95 °C, 50s at 60 °C, and 50s at 75 °C. The products were loaded and run on 1.5% agarose gels and bands were developed using a UV transilluminator, and then photographed. A template dilution cDNA condition, which showed the same density of the β-actin “housekeeping” gene as the internal control, was chosen per group. Subsequently, the densitometric measurement of markers such as ChAT, GAP43, and MAP2 in the selected condition of the template cDNA dilution was analyzed. As the template condition of all the groups had the same signal intensity as that of the internal control, relative signal intensities in the markers of each group could be quantified and plotted as relative density levels (RDL) using the Image J program.
Western blotting
Injury epicenters 0.5-cm in size, harvested 8 weeks after SCI, were lysed by homogenization in 300 μl lysis buffer containing 20 mM Tris pH 7.4, 50 mM NaCl2, 1% Triton X-100, and protease inhibitor (Intron, Seoul, Korea). The debris was cleared by centrifugation, and the supernatants were aliquoted and stored at −80 °C. The samples were assayed for their protein concentration using the bicinchoninic acid assay (Thermo Scientific, Rockford, IL, USA). After heating at 100 °C for 5 min in 5× sample buffer, equal amounts of denatured protein (30 μg) were separated by sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) on 10% gels and transferred onto polyvinylidene difluoride membranes at 20 V for 7 min with an iBlot® gel transfer device (Invitrogen). After incubating for 1 h at room temperature with blocking solution (0.4% Tween-20 and 5% dry milk in PBS), membranes were incubated overnight with primary antibodies against ChAT (1:500; Abcam), GAP43 (1:500; Abcam), or MAP2 (1:200; Abcam); an antibody against β-actin (1:10,000; Sigma Aldrich) was used as a control for equal loading. After washing with 0.1% Tween-20/TBS, the blots were incubated with horseradish peroxidase-conjugated secondary antibodies (Sigma Aldrich) and developed with enhanced chemiluminescence reagents (Pierce Biotechnology, Rockford, IL, USA). The blots were then scanned after exposure to X-rays. Subsequent analysis involved the densitometric measurements of the mean black levels and intensities of each band using the Image J program, as with RT-PCR.
Results
Cell selection for transplantation and gene expression
Before the in vivo testing, we used fluorescent microscopy to confirm the selection of cells to be transplanted after 48-h cultivation; the expression of GFP distinguished the hMSCs successfully transfected with the pLenti-Wnt3a-GFP vector from the non-transfected hMSCs (Fig. 1). The cells selected for transplantation were also quantitatively evaluated for the expression of the Wnt3a gene by ELISA of expressed Wnt3a proteins in cultivated media after additional 24-h cultivation. The media of the Wnt3a-secreting hMSCs showed significantly higher expression of Wnt3a proteins (3.66 pg/ml) than other media such as the normal, hMSC, and hMSC with pLenti vector media.
Confirmation of Wnt3a expression through GFP gene expression by confocal microscopy. The expression of GFP distinguished the successful transfection of the pLenti-Wnt3a-GFP vector into hMSCs from non-transfected hMSCs. Three types of cells in Wnt3a-conditioned media could be observed through the microscope: a MSC only group, b MSC with pLenti viral vector, c MSC with pLenti-Wnt3a-GFP vector. The Wnt3a-positive cells were strongly detected by GFP expression induced in the presence of the pLenti-Wnt3a-GFP viral vector (magnification, 200×). GFP green fluorescent protein, hMSC human mesenchymal stem cell
Behavioral tests—BBB test and ladder rung test
Seven weeks after the transplantation (8 weeks after SCI), rats in the Wnt3a-MSC group obtained an average BBB score of 15.8 ± 1.72, which was significantly higher (p < 0.05) than that in the sham (9.16 ± 0.4), Wnt3a protein (11.5 ± 0.84), MSC (13.5 ± 0.55), and pLenti-MSC (13.3 ± 0.52) groups (Fig. 2). In the ladder rung test, the average score of rats in the Wnt3a-MSC group (76.7 ± 22.5) was significantly higher (p < 0.05) than that of rats in the sham (5 ± 5.46), Wnt3a protein (45 ± 13.8), MSC (61.7 ± 7.52), and pLenti- MSC (51.7 ± 13.3) groups (Fig. 3).
BBB locomotor function test. In the BBB test, locomotor function in the Wnt3a-MSC group improved significantly more than it did in the sham, Wnt3a protein, MSC, and pLenti-MSC groups. The scores at 8 weeks after SCI (7 weeks after cell transplantation) showed statistically significant improvements in the Wnt3a-MSC group (*p < 0.05). BBB Basso-Beattie-Bresnahan, MSC mesenchymal stem cell, SCI spinal cord injury
Immunofluorescence
The expression of markers was analyzed in just the proximal part of the injury epicenter in which the cells were injected. Immunofluorescent staining was performed using three monoclonal antibodies. The expression of ChAT, a motor neuronal marker, was higher in all groups compared with that in the sham group, with the Wnt3a-MSC group showing the highest expression of ChAT (Fig. 4). The expression of GAP43, an axonal regeneration marker, was higher in the Wnt3a protein, MSC, pLenti-MSC, and Wnt3a-MSC groups than in the sham group, with the Wnt3a-MSC group showing the highest expression level (Fig. 5). The expression of MAP2, another axonal regeneration marker, showed a similar pattern of expression; its expression was lower in the sham group compared with the other groups, and was highest in the Wnt3a-MSC group (Fig. 6).
Immunofluorescent staining of ChAT showed greater staining in the Wnt3a-MSC group than in sham, Wnt3a protein, MSC, and pLenti-MSC groups (magnification, 200×). The extracted spinal cord section of the Wnt3a-MSC showed the region used for immunofluorescent staining, which were located just above the injured lesion (yellow box). R rostral, C caudal, ChAT choline acetyltransferase, MSC mesenchymal stem cell
Immunofluorescent staining of GAP43 showed greater staining in the Wnt3a-MSC group than in sham, Wnt3a protein, MSC, and pLenti-MSC groups (magnification, 200×). The extracted spinal cord section of the Wnt3a-MSC showed the region used for immunofluorescent staining, which were located just above the injured lesion (yellow box). R rostral, C caudal, ChAT choline acetyltransferase, MSC mesenchymal stem cell
Immunofluorescent staining of MAP2 showed greater staining in the Wnt3a-MSC group than in sham, Wnt3a protein, MSC, and pLenti-MSC groups (magnification, 200×). The extracted spinal cord section of the Wnt3a-MSC showed the region used for immunofluorescent staining, which were located just above the injured lesion (yellow box). R rostral, C caudal, ChAT choline acetyltransferase, MSC mesenchymal stem cell
RT-PCR and Western blot
For RT-PCR, the relative detection levels were determined by assessing and comparing the band densities between groups. The relative expression levels of ChAT, GAP43, and MAP2, the three markers of neural regeneration, were higher in the MSC, pLenti-MSC, and Wnt3a-MSC groups than in the other groups. However, the Wnt3a-MSC group showed a significantly higher expression than other groups (p < 0.05, Fig. 7).
RT-PCR analysis. RT-PCR analysis was evaluated after extraction of the spinal cord 0.5-cm in size including the injury epicenter 8 weeks after SCI (a). The band densities were converted into RDL values, and the Wnt3a-MSC group showed significantly higher values for ChAT (b), GAP43 (c), and MAP2 (d) (*p < 0.05). RDL relative density level, SCI spinal cord injury, RT-PCR reverse transcriptase polymerase chain reaction, MSC mesenchymal stem cell
Similarly, the results of the Western blot showed highest relative density levels (RDLs) of all the markers (except MAP2) in the Wnt3a-MSC group, compared with the other groups (p < 0.05, Fig. 8). The RDL of MAP2 in the Wnt3a-MSC group was not significantly different from the MSC and pLenti-MSC group RDLs, but it was higher than that in the sham and Wnt3a protein groups (Fig. 8d).
Western blotting analysis in the extracted spinal cord 0.5-cm in size including the injury epicenter 8 weeks after SCI (a). Band densities were converted into RDL values, and the Wnt3a-MSC group showed significantly higher values for ChAT (b) and GAP43 (c) (*p < 0.05). However, the statistical significance of MAP2 levels in the Wnt3a-MSC group appeared only when compared to the sham or Wnt3a protein groups (d) (*p < 0.05). SCI spinal cord injury, RDL relative density level, MSC mesenchymal stem cell
Discussion
There are two strategic approaches of stem cell therapy for SCI. One of them is neural stem/progenitor cell transplantation, which is expected to promote functional recovery by playing a role in anti-inflammatory mechanisms, replacement of damaged neurons, secretion of neurotrophic molecules such as neurotrophin, and improvement of the spinal conductivity [10, 17, 46]. Another is transplantation of MSCs, which is considered to improve axonal regeneration through several mechanisms, such as secreting bioactive molecules like growth factors and cytokines, providing structural support, suppressing inflammation, decreasing glial scar, and reducing apoptosis [14, 26, 50]. Although some animal studies have established neural stem/progenitor cell transplantation as a technique, its application in a clinical trial has still not been investigated. Clinical trials of pure MSCs, by comparison, have demonstrated neurological functional recovery in SCI patients [12, 33, 36]. However, the insufficient therapeutic effects of pure MSCs present a challenging problem at present.
Unlike the inhibitory effects of endogenously induced Wnt1 and Wnt5a signaling in axonal regeneration leading to limited functional recovery after SCI [28, 31], the canonical Wnt3a signaling pathway, which was described in our previous study, promotes spinal cord neural precursor development and stimulates axonal regeneration [38, 45]. Moreover, improved functional recovery has been shown in animal SCI models after injection of Wnt3a molecules alone, Wnt3a-secreting fibroblasts, or Wnt3a-secreting fibroblasts with alginate scaffolds [37, 45, 53]. Based on the safety and positive findings of improved neurological recovery by hMSC transplantation in clinical trials, on the effect of exogenous Wnt3a-secreting fibroblasts in a rat SCI model [33, 36, 45], we designed Wnt3a-secreting hMSCs to investigate their enhanced therapeutic effect in SCI animal model. The results of this study show that this combination of therapeutic agents might be applicable in SCI treatment.
Locomotor functional improvement following cell transplantation was confirmed by the BBB and ladder rung tests. In both the behavioral tests, the Wnt3a-MSC group showed significantly greater improvements than other groups 7 weeks after transplantation. Eight weeks after injury (7 weeks after transplantation), the scores appeared to plateau, and the evaluation at this time may be representative of the final motor recovery and appropriate for assessing therapeutic effects. Interestingly, the Wnt3a-MSC group showed a steep increase over 7 weeks in the ladder rung test scores, whereas the BBB scores showed similar patterns as observed in our previous study on the transplantation of Wnt3a-secreting fibroblasts in SCI rats, in that the scores increased continuously for 6 weeks and then appeared to plateau [37].
Immunofluorescence was used for the visual analysis of axonal regeneration, and RT-PCR was used for the quantitative analysis of proteins expressed through the RNA from the extracted spinal cord tissue. Similarly, Western blotting was used for the quantitative analysis of expressed proteins from the tissue using electrophoresis. Among the markers studied, ChAT, a motor neuronal marker, is located at the neurotransmitter-secreting axon terminal, and GAP43 and MAP2 are known as representative markers of axonal regeneration. Therefore, these markers were used to determine whether increased behavioral test scores were affected by axonal regeneration rather than neuroprotective effects. In this study, the Wnt3a-MSC group had significantly higher quantitative expression of all markers compared with other groups in the biomolecular study (p < 0.05, Figs. 7 and 8) as well as higher qualitative expression in the immunofluorescence study (Figs. 4, 5, and 6). However, in the western blot, the three hMSC transplantation groups (i.e., MSC, pLenti-MSC, and Wnt3a-MSC) were distinguished by high ChAT and GAP43 expression levels, but not MAP2 expression. We assumed these results were due to the nature of each marker. For instance, MAP2 is a microtubule-associated protein in the cytoskeleton and is located mainly at dendrites and dendritic spines [32], while GAP43 is mainly located at the growth cone membrane of regenerative axons [19, 39]. As the Wnt3a protein helps to strengthen axonal growth cones [11], GAP43 expression in the Wnt3a-MSC group might be more prominent than in the MSC and pLenti-MSC groups. It may be the case that the expression of MAP2 was influenced not only by the presence of Wnt3a but also by the effects of MSCs. The overall findings of this study suggest that the axonal regenerative effects of Wnt3a-secreting hMSCs, evident from behavioral and biomolecular tests, were enhanced compared with those following Wnt3a protein injection or pure hMSC transplantation. In this respect, Wnt3a-secreting hMSC transplantation could provide synergistic effects. In the present study, we did not evaluate the survival of grafted cells, which is a limitation of this study. However, grafted cells are not likely to survive for longer than 1 month, as per our previous study [51] and based on the knowledge that the Wnt3a molecule does not function in increasing cell survival. In this regard, the images, which represent the cells harvested and stained at 7 weeks after transplantation, might not include the grafted cells. Although the survival of grafted cells was temporary, they could provide sufficient stimuli to enhance axonal regeneration through the injured cord [20].
In this study, the lentiviral vector was a useful tool for gene transfer in the transfection of the mouse Wnt3a gene, as reported elsewhere [18, 52]. The lentivirus is a single-stranded RNA virus that can be infected into both dividing and non-dividing cells, and can integrate stably into the host genome to provide sustained expression in the target cell [4, 55]. The virus is also widely used for various applications such as gene overexpression, gene knockdown, gene modification of stem cells, and rat genetic transformation [4, 16, 42, 48, 49]. Moreover, various clinical trials using lentivirus-mediated gene therapy have been introduced [8, 15, 29, 47]. Therefore, Wnt3a-secreting hMSCs could be applicable to clinical trials for SCI patients, though it would be essential to determine the optimal cell dosage for clinical trials. In the author’s previous experiences of human studies [33, 36], 8 × 106 autologous MSCs were injected into the intramedullary space and 4 × 107 cells in the subdural space for each injection of a multiple application protocol, while 1.6 × 107 autologous MSCs were injected into the intramedullary area and 3.2 × 107 cells in the subdural space in a single application protocol. Thus, this evidence can be used to guide the determination of cell dosage. However, the potential amount of Wnt3a protein secreted from the cells should be evaluated with respect to safety issues including oncogenesis.
Conclusions
We created Wnt3a-secreting hMSCs to enhance the efficacy of axonal regeneration based on the safety of pure MSCs confirmed through clinical trials of SCI treatment. This study suggests that these cells can increase axonal regeneration and promote recovery of motor function in a rat SCI model.
BBB, Basso-Beattie-Bresnahan; ChAT, choline acetyltransferase; CNS, central nervous system; GAP43, growth associated protein 43; GSK-3, glycogen synthase kinase 3; hMSC, human mesenchymal stem cell; MAP2, microtubule-associated protein 2; PBS, Phosphate-buffered Saline; PFA, paraformaldehyde; RDL, relative density levels; RT, reverse transcriptase; RT-PCR, reverse transcription polymerase chain reaction; SCI, spinal cord injury; TBS, Tris-buffered saline.
References
Akiyama Y, Radtke C, Kocsis JD (2002) Remyelination of the rat spinal cord by transplantation of identified bone marrow stromal cells. J Neurosci 22:6623–6630
Arbeit JM, Hilaris BS, Brennan MF (1987) Wound complications in the multimodality treatment of extremity and superficial truncal sarcomas. J Clin Oncol 5:480–488
Arevalo JC, Chao MV (2005) Axonal growth: where neurotrophins meet Wnts. Curr Opin Cell Biol 17:112–115
Barde I, Verp S, Offner S, Trono D (2011) Lentiviral vector mediated transgenesis. Curr Protoc Mouse Biol 1:169–184
Barry FP, Murphy JM (2004) Mesenchymal stem cells: clinical applications and biological characterization. Int J Biochem Cell Biol 36:568–584
Basso DM, Beattie MS, Bresnahan JC (1995) A sensitive and reliable locomotor rating scale for open field testing in rats. J Neurotrauma 12:1–21
Blesch A, Tuszynski MH (2002) Spontaneous and neurotrophin-induced axonal plasticity after spinal cord injury. Prog Brain Res 137:415–423
Cavazzana-Calvo M, Payen E, Negre O, Wang G, Hehir K, Fusil F, Down J, Denaro M, Brady T, Westerman K, Cavallesco R, Gillet-Legrand B, Caccavelli L, Sgarra R, Maouche-Chretien L, Bernaudin F, Girot R, Dorazio R, Mulder GJ, Polack A, Bank A, Soulier J, Larghero J, Kabbara N, Dalle B, Gourmel B, Socie G, Chretien S, Cartier N, Aubourg P, Fischer A, Cornetta K, Galacteros F, Beuzard Y, Gluckman E, Bushman F, Hacein-Bey-Abina S, Leboulch P (2010) Transfusion independence and HMGA2 activation after gene therapy of human beta-thalassaemia. Nature 467:318–322
Chao MV (2003) Neurotrophins and their receptors: a convergence point for many signalling pathways. Nat Rev Neurosci 4:299–309
Cheng Z, Zhu W, Cao K, Wu F, Li J, Wang G, Li H, Lu M, Ren Y, He X (2016) Anti-Inflammatory mechanism of neural stem cell transplantation in spinal cord injury. Int J Mol Sci 17
Ciani L, Salinas PC (2005) WNTs in the vertebrate nervous system: from patterning to neuronal connectivity. Nat Rev Neurosci 6:351–362
Cizkova D, Rosocha J, Vanicky I, Jergova S, Cizek M (2006) Transplants of human mesenchymal stem cells improve functional recovery after spinal cord injury in the rat. Cell Mol Neurobiol 26:1167–1180
Dasari VR, Spomar DG, Cady C, Gujrati M, Rao JS, Dinh DH (2007) Mesenchymal stem cells from rat bone marrow downregulate caspase-3-mediated apoptotic pathway after spinal cord injury in rats. Neurochem Res 32:2080–2093
De Miguel MP, Fuentes-Julian S, Blazquez-Martinez A, Pascual CY, Aller MA, Arias J, Arnalich-Montiel F (2012) Immunosuppressive properties of mesenchymal stem cells: advances and applications. Curr Mol Med 12:574–591
De Ravin SS, Wu X, Moir S, Anaya-O’Brien S, Kwatemaa N, Littel P, Theobald N, Choi U, Su L, Marquesen M, Hilligoss D, Lee J, Buckner CM, Zarember KA, O’Connor G, McVicar D, Kuhns D, Throm RE, Zhou S, Notarangelo LD, Hanson IC, Cowan MJ, Kang E, Hadigan C, Meagher M, Gray JT, Sorrentino BP, Malech HL (2016) Lentiviral hematopoietic stem cell gene therapy for X-linked severe combined immunodeficiency. Sci Transl Med 8:335ra357
Diaz RM, Bateman A, Emiliusen L, Fielding A, Trono D, Russell SJ, Vile RG (2000) A lentiviral vector expressing a fusogenic glycoprotein for cancer gene therapy. Gene Ther 7:1656–1663
Einstein O, Ben-Hur T (2008) The changing face of neural stem cell therapy in neurologic diseases. Arch Neurol 65:452–456
Fuerer C, Nusse R (2010) Lentiviral vectors to probe and manipulate the Wnt signaling pathway. PLoS One 5:e9370
Goslin K, Schreyer DJ, Skene JH, Banker G (1990) Changes in the distribution of GAP-43 during the development of neuronal polarity. J Neurosci 10:588–602
Himes BT, Neuhuber B, Coleman C, Kushner R, Swanger SA, Kopen GC, Wagner J, Shumsky JS, Fischer I (2006) Recovery of function following grafting of human bone marrow-derived stromal cells into the injured spinal cord. Neurorehabil Neural Repair 20:278–296
Hirabayashi Y, Itoh Y, Tabata H, Nakajima K, Akiyama T, Masuyama N, Gotoh Y (2004) The Wnt/beta-catenin pathway directs neuronal differentiation of cortical neural precursor cells. Development 131:2791–2801
Huelsken J, Behrens J (2002) The Wnt signalling pathway. J Cell Sci 115(Pt 21):3977–3978
Im J, Kim H, Kim S, Jho EH (2007) Wnt/beta-catenin signaling regulates expression of PRDC, an antagonist of the BMP-4 signaling pathway. Biochem Biophys Res Commun 354:296–301
Keirstead HS, Nistor G, Bernal G, Totoiu M, Cloutier F, Sharp K, Steward O (2005) Human embryonic stem cell-derived oligodendrocyte progenitor cell transplants remyelinate and restore locomotion after spinal cord injury. J Neurosci 25:4694–4705
Kumagai G, Tsoulfas P, Toh S, McNiece I, Bramlett HM, Dietrich WD (2013) Genetically modified mesenchymal stem cells (MSCs) promote axonal regeneration and prevent hypersensitivity after spinal cord injury. Exp Neurol 248:369–380
Le Blanc K, Ringden O (2006) Mesenchymal stem cells: properties and role in clinical bone marrow transplantation. Curr Opin Immunol 18:586–591
Lee HJ, Kim KS, Park IH, Kim SU (2007) Human neural stem cells over-expressing VEGF provide neuroprotection, angiogenesis and functional recovery in mouse stroke model. PLoS One 2:e156
Liu Y, Wang X, Lu CC, Kerman R, Steward O, Xu XM, Zou Y (2008) Repulsive Wnt signaling inhibits axon regeneration after CNS injury. J Neurosci 28:8376–8382
Mansilla-Soto J, Riviere I, Boulad F, Sadelain M (2016) Cell and gene therapy for the beta-thalassemias: advances and prospects. Hum Gene Ther 27:295–304
Metz GA, Whishaw IQ (2009) The ladder rung walking task: a scoring system and its practical application. J Vis Exp 28:e1204. doi:10.3791/1204
Miyashita T, Koda M, Kitajo K, Yamazaki M, Takahashi K, Kikuchi A, Yamashita T (2009) Wnt-Ryk signaling mediates axon growth inhibition and limits functional recovery after spinal cord injury. J Neurotrauma 26:955–964
Oestreicher AB, De Graan PN, Gispen WH, Verhaagen J, Schrama LH (1997) B-50, the growth associated protein-43: modulation of cell morphology and communication in the nervous system. Prog Neurobiol 53:627–686
Oh SK, Choi KH, Yoo JY, Kim DY, Kim SJ, Jeon SR (2016) A phase III clinical trial showing limited efficacy of autologous mesenchymal stem cell therapy for spinal cord injury. Neurosurgery 78:436–447
Ohta M, Suzuki Y, Noda T, Ejiri Y, Dezawa M, Kataoka K, Chou H, Ishikawa N, Matsumoto N, Iwashita Y, Mizuta E, Kuno S, Ide C (2004) Bone marrow stromal cells infused into the cerebrospinal fluid promote functional recovery of the injured rat spinal cord with reduced cavity formation. Exp Neurol 187:266–278
Osaka M, Honmou O, Murakami T, Nonaka T, Houkin K, Hamada H, Kocsis JD (2010) Intravenous administration of mesenchymal stem cells derived from bone marrow after contusive spinal cord injury improves functional outcome. Brain Res 1343:226–235
Park JH, Kim DY, Sung IY, Choi GH, Jeon MH, Kim KK, Jeon SR (2012) Long-term results of spinal cord injury therapy using mesenchymal stem cells derived from bone marrow in humans. Neurosurgery 70:1238–1247
Park JH, Min J, Baek SR, Kim SW, Kwon IK, Jeon SR (2013) Enhanced neuroregenerative effects by scaffold for the treatment of a rat spinal cord injury with Wnt3a-secreting fibroblasts. Acta Neurochir (Wien) 155:809–816
Parr BA, Shea MJ, Vassileva G, McMahon AP (1993) Mouse Wnt genes exhibit discrete domains of expression in the early embryonic CNS and limb buds. Development 119:247–261
Pertz OC, Wang Y, Yang F, Wang W, Gay LJ, Gristenko MA, Clauss TR, Anderson DJ, Liu T, Auberry KJ, Camp DG 2nd, Smith RD, Klemke RL (2008) Spatial mapping of the neurite and soma proteomes reveals a functional Cdc42/Rac regulatory network. Proc Natl Acad Sci U S A 105:1931–1936
Rubinfeld B, Albert I, Porfiri E, Fiol C, Munemitsu S, Polakis P (1996) Binding of GSK3beta to the APC-beta-catenin complex and regulation of complex assembly. Science 272:1023–1026
Sakai D, Mochida J, Yamamoto Y, Nomura T, Okuma M, Nishimura K, Nakai T, Ando K, Hotta T (2003) Transplantation of mesenchymal stem cells embedded in Atelocollagen gel to the intervertebral disc: a potential therapeutic model for disc degeneration. Biomaterials 24:3531–3541
Salmon P, Trono D (2002) Lentiviral vectors for the gene therapy of lympho-hematological disorders. Curr Top Microbiol Immunol 261:211–227
Samdani AF, Paul C, Betz RR, Fischer I, Neuhuber B (2009) Transplantation of human marrow stromal cells and mono-nuclear bone marrow cells into the injured spinal cord: a comparative study. Spine (Phila Pa 1976) 34:2605–2612
Sondell M, Lundborg G, Kanje M (1999) Vascular endothelial growth factor has neurotrophic activity and stimulates axonal outgrowth, enhancing cell survival and Schwann cell proliferation in the peripheral nervous system. J Neurosci 19:5731–5740
Suh HI, Min J, Choi KH, Kim SW, Kim KS, Jeon SR (2011) Axonal regeneration effects of Wnt3a-secreting fibroblast transplantation in spinal cord-injured rats. Acta Neurochir (Wien) 153:1003–1010
Tashiro S, Nishimura S, Iwai H, Sugai K, Zhang L, Shinozaki M, Iwanami A, Toyama Y, Liu M, Okano H, Nakamura M (2016) Functional recovery from neural stem/progenitor cell transplantation combined with treadmill training in mice with chronic spinal cord injury. Sci Rep 6:30898
Touzot F, Hacein-Bey-Abina S, Fischer A, Cavazzana M (2014) Gene therapy for inherited immunodeficiency. Expert Opin Biol Ther 14:789–798
Van Damme A, Thorrez L, Ma L, Vandenburgh H, Eyckmans J, Dell’Accio F, De Bari C, Luyten F, Lillicrap D, Collen D, VandenDriessche T, Chuah MK (2006) Efficient lentiviral transduction and improved engraftment of human bone marrow mesenchymal cells. Stem Cells 24:896–907
Woods NB, Mikkola H, Nilsson E, Olsson K, Trono D, Karlsson S (2001) Lentiviral-mediated gene transfer into haematopoietic stem cells. J Intern Med 249:339–343
Xue F, Wu EJ, Zhang PX, Li-Ya A, Kou YH, Yin XF, Han N (2015) Biodegradable chitin conduit tubulation combined with bone marrow mesenchymal stem cell transplantation for treatment of spinal cord injury by reducing glial scar and cavity formation. Neural Regen Res 10:104–111
Yang KH, Kim E-S, Min JK, Roh S-W, Rhim S-C, Jeon SR (2007) Therapeutic effect and optimal injection time by human mesenchymal stem cell at spinal cord injury of rat. J Korean Neurotraumatol Soc 3:99–102
Yang XT, Bi YY, Chen ET, Feng DF (2014) Overexpression of Wnt3a facilitates the proliferation and neural differentiation of neural stem cells in vitro and after transplantation into an injured rat retina. J Neurosci Res 92:148–161
Yin ZS, Zu B, Chang J, Zhang H (2008) Repair effect of Wnt3a protein on the contused adult rat spinal cord. Neurol Res 30:480–486
Yun S, Rim Y, Jho EH (2007) Induced expression of the transcription of tropomodulin 1 by Wnt5a and characterization of the tropomodulin 1 promoter. Biochem Biophys Res Commun 363:727–732
Zufferey R, Dull T, Mandel RJ, Bukovsky A, Quiroz D, Naldini L, Trono D (1998) Self-inactivating lentivirus vector for safe and efficient in vivo gene delivery. J Virol 72:9873–9880
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The Asan Medical Center provided financial support in the form of the Asan Life Science Institute Grant (13–176). The sponsor played no role in the design or conduct of this research.
Conflict of interest
None
Ethical approval
This study was reviewed and approved by the Institutional Animal Care and Use Committee (IACUC) of the Asan Institute for Life Sciences, Asan Medical Center (2014-12-031). The committee abides by the Institute of Laboratory Animal Resources guide.
Additional information
Comments
This is an interesting study, providing robust evidence that transplantation of Wnt3a-secreting human mesenchymal stem cells (hMSCs) improves functional recovery after spinal cord injury (SCI) in an experimental rodent model. To proceed to the application of Wnt3a-secreting hMSCs in clinical trials, fundamental data, not yet available, will be necessary, however. Among others, the safety profile should be verified through long-term follow-up of injected animals. The optimal cell number for injection and the efficiency in terms of number of injections should also be determined. Nonetheless, the strategy is promising and further studies are warranted on the basis of the results presented in this article.
Alfredo Conti,
Messina, Italy
Clinical trials have proven some axonal regenerative effect of human mesenchymal stem cells in patients with spinal cord injury. However, with rather insufficient therapeutic effects. Based on findings in a rat spinal cord injury model of improved axonal regeneration by transplantation of human mesenchymal stem cells transfected with exogenous Wnt3a secreting fibroblasts, the authors designed a protocol involving the combination of continuous Wnt3a secretion and human mesenchymal stem cell transplantation. The results of this animal study showed that combination of these therapeutic agents may serve as an experimental basis for future SCI treatment. It has been confirmed again that Wnt3a signaling promotes spinal cord neural precursor development and stimulates axonal regeneration.
Tamas Peter Doczi
Pecs, Hungary
Dong Kwang Seo and Jeong Hoon Kim contributed equally to this work.
Rights and permissions
About this article
Cite this article
Seo, D.K., Kim, J.H., Min, J. et al. Enhanced axonal regeneration by transplanted Wnt3a-secreting human mesenchymal stem cells in a rat model of spinal cord injury. Acta Neurochir 159, 947–957 (2017). https://doi.org/10.1007/s00701-017-3097-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3097-0