Abstract
Background and purpose
We reported previously that hydrogen gas (H2) reduced hepatic ischemia and reperfusion injury (IRI) after prolonged cold storage (CS) of livers retrieved from heart-beating donors. The present study was designed to assess whether H2 reduced hepatic IRI during donation of a cardiac death (DCD) graft with subsequent CS.
Methods
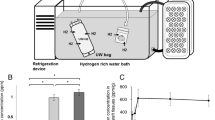
Rat livers were harvested after 30-min cardiac arrest and stored for 4 h in University of Wisconsin solution. The graft was reperfused with oxygenated buffer, with or without H2 (H2 or NT groups, respectively), at 37° for 90 min on isolated perfused rat liver apparatus.
Results
In the NT group, liver enzyme leakage, apoptosis, necrosis, energy depletion, redox status, impaired microcirculation, and bile production were indicative of severe IRI, whereas in the H2 group these impairments were significantly suppressed. The phosphorylation of cytoplasmic MKK4 and JNK were enhanced in the NT group and suppressed in the H2 group. NFkB-p65 and c-Fos in the nucleus were unexpectedly unchanged by IRI regardless of H2 treatment, indicating the absence of inflammation in this model.
Conclusion
H2 was observed to ameliorate IRI in the DCD liver by maintaining microcirculation, mitochondrial functions, and redox status, as well as suppressing the cytoplasmic MKK4–JNK-mediated cellular death pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Critical donor shortage has prompted the safe implementation of extended-criteria donor (ECD) grafts, including DCDs. Although simple cold storage in University of Wisconsin (UW) solution has contributed to the development of liver and kidney transplantation [1], a gold standard for the use of DCD liver has not yet been established because of the associated severe IRI, which leads to primary non-function, biliary complications, and eventual graft loss [1, 2]. A retrospective analysis of DCD liver transplantation showed that primary non-function (PNF) and bile duct complications were uncommon when there were few risk factors [3]. A recent encouraging report demonstrated that the outcome of DCD livers subjected to normothermic machine perfusion (NMP) was better than that of donation after brain death (DBD) with NMP, when donors and recipients were appropriately selected [4].
DCD graft injury after transplantation progresses in three phases, namely, warm ischemia, subsequent cold preservation (low temperature and hypoxia), and reperfusion (rewarming and reoxygenation). Unlike the standard criteria donor (SCD) liver, refrigeration under energy deficiency leads to the accumulation of sodium and calcium ions, resulting in reperfusion injury [5]. Furthermore, warm IRI caused mainly by reactive oxygen species (ROS) results in the production of inflammatory cytokines, tissue injury and microcirculatory disturbance [6, 7]. However, if the cold preservation time is within certain limits, it will not enhance injury significantly [6, 7]. Based on these factors, if the degree of impairment in each phase can be suppressed, then the IRI of DCD liver could be suppressed. Accordingly, we chose the safe limit for warm ischemia in the DCD liver graft as 30 min [3] and sought the shortest clinically applicable cold preservation time. We then looked for ways to reduce IRI by starting treatment at the initiation of reperfusion.
We focused on the medical gas H2 to assess its ability to reduce IRI in DCD liver grafts. Ohsawa et al. reported that hydrogen gas acts as a therapeutic antioxidant, and could play significant roles in radical scavenging and anti-inflammation [8]. Some authors have reported that H2 reduces reperfusion injury in the brain [8], lung [9], heart [10], intestine [11], kidney [12] and liver [13, 14]. We felt that these factors could be potentially applicable to the amelioration of IRI in DCD liver grafts.
In hepatic IRI, signaling molecules such as c-jun N-terminal kinase (JNK) are activated by inflammatory cytokines and various stressors including oxidative stress [15, 16]. Furthermore, prolonged JNK activation promotes the mitochondrial release of cytochrome c, cleavage of caspase 3, and then apoptosis [17], as well as necrosis caused by impaired mitochondrial energy production [16]. Although the protective effect of H2 against hepatic cold IRI in an isolated perfused rat liver (IPRL) has been reported [18], the precise molecular mechanisms remain unclear. The aims of this study were to investigate whether H2 ameliorates reperfusion injury of the DCD graft, and to elucidate the mechanism of its protection.
Materials and methods
Chemicals and reagents
Chemicals and reagents were purchased from Wako Pure Chemical Co. Ltd (Osaka, Japan) and antibodies were purchased from Cell Signaling Technology Japan (Tokyo, Japan) unless otherwise noted.
Animals
All experiments were conducted with the approval of the Institutional Guide of Hokkaido University in accordance with the Care and Use of Laboratory Animals. Male Sprague–Dawley rats (6–7 weeks old, 220–260 g) were purchased from Sankyo Labo Service Corporation, Inc (Tokyo, Japan), and used for the experiments after being raised for 5–7 days in our animal facility. The feed and other laboratory conditions were as described previously [19].
Operation
Animals were operated on without being fasted and were anesthetized by isoflurane inhalation. Cardiopulmonary arrest (CPA) was initiated by phrenotomy. After 30 min of CPA, the portal vein was cannulated with a 16-G catheter (NIPRO, Osaka, Japan). The liver was flushed via the portal vein with 50 ml saline (room temperature) containing 1000 IU of sodium heparin (Mochida pharmaceutical CO., LTD, Tokyo, Japan) and with 10 ml of ice-chilled UW solution thereafter. The bile duct was cannulated with a PE-10 catheter (Intramedic, Clay Adams, NJ, USA) and the liver was removed.
Experimental protocol
In the control group, the liver without CPA and cold storage was reperfused immediately after procurement on IPRL apparatus (CT group; n = 6). The cold preservation group was sub-divided into two groups. After CPA and subsequent cold preservation in UW solution for 4 h, livers were reperfused as an IPRL without hydrogen gas supplementation [no treatment (NT) group; n = 6] or with hydrogen gas treatment (H2 group; n = 6).
Isolated perfused rat liver (IPRL)
Conditions of the IPRL were set in accordance with techniques described previously [20] with slight modifications [18]. Briefly, livers were perfused with 300 ml of Krebs–Henseleit bicarbonate buffer (KHB), supplemented with glucose and sodium taurocholate, at 37° and a constant pressure of 12 cmH2O in a recirculating system. In the H2 group, H2-saturated KHB in a sealed glass bottle was connected before the portal cannula, and mixed in the perfusion circuit at a flow rate of 4% versus total flow. We measured portal vein pressure (PVP; cmH2O), portal vein resistance [PVR; cmH2O/(ml/min/g)], bile production during 90 min of perfusion (µl/g liver), and the oxygen consumption rate (OCR) [18].
Sample collection
At the end of perfusion, the livers were weighed and stored at − 80° until use, or fixed in 10% buffered formalin and embedded in paraffin. For adenosine triphosphate (ATP) and glutathione measurements, they were snap-frozen. The effluent (KHB) was collected just after anesthesia and then 30 and 90 min after perfusion to examine activities of aspartate aminotransferase (AST), alanine aminotransferase (ALT), and lactate dehydrogenase (LDH). They were measured with a Hitachi 7020 automatic biochemical analyzer (Hitachi, Tokyo, Japan), and liver injury was expressed as the enzyme leakage at the end of reperfusion: enzyme leakage (IU/g) = (activity R90) [IU/l] × perfusate volume [l]/liver weight [g] [18].
Histology and apoptosis
The paraffin-embedded sections were stained with hematoxylin and eosin and by the terminal deoxynucleotidyl transferase (TUNEL) method. Liver injury was assessed by a single pathologist in a blind manner. The apoptotic index was calculated by the number of TUNEL-positive cells divided by the total cell number [18].
ATP assay
Tissue ATP was measured by the HPLC-UV method [19]. Data were expressed as micromoles per gram wet weight.
Redox status of glutathione
Tissue extract with 5% sulfosalicylic acid and reduced glutathione (GSH) quenched from the extract was applied to the NADPH-GR-DTNB-based oxidized glutathione (GSSG) recycling assay [19]. The amounts of (GSH + GSSG) and GSH are expressed as micromoles GSH equivalent per g liver. The amount of GSSG is expressed as micromoles per g liver. The redox status of glutathione was measured by the molar ratio of GSH and GSSG (GSH/GSSG).
Lipid peroxidation
Hepatic oxidative damage at the end of perfusion was assessed by the total amounts of malondialdehyde (MDA) and 4-hydroxy-2-nonenal (4-HNE) using an LPO586 kit (Oxis International, Foster City, CA) in accordance with the manufacturer’s instructions [19]. Microsomal fraction was obtained from the 10% (%w/v) homogenate containing butylated hydroxytoluene (0.05%). The summation of MDA and 4-HNE contents were calculated and expressed as the nmol 4-HNE equivalent per mg of wet tissue weight [19].
Cell death and inflammatory signals
The stress-associated cell death pathway was assessed by western blot analysis as described previously (15). Frozen tissue (50 mg) was homogenized in ice-chilled lysis buffer containing EDTA-2Na, NaF, sodium orthovanadate, Nonidet P-40, and a protease inhibitor cocktail (Sigma-Aldrich, St. Louis, MO). After the serial centrifugations at 1000×g for 10 min, and the resulting supernatant at 15,000×g for 10 min, they were stored at − 80 °C. Protein concentration was measured using a BCA Protein Assay Kit (Thermo Scientific, Rockford, IL).
After solubilization and denaturing, 40 mg of protein was applied to Any-kD precast gel (Bio-Rad). Standard SDS polyacrylamide gel electrophoresis (SDS-PAGE) and immunoblots were performed. The dilutions of primary antibodies were 1:1000 (pan-MKK4, phsopho-MKK4, pan-JNK, phospho-JNK, Caspase3, GAPDH), and that of horseradish peroxidase-conjugated anti-rabbit IgG secondary antibody was 1:5000. Protein bands were detected by a chemiluminescent detector Chem Doc XRS® (Bio-Rad) using a chemiluminescence reagent, West Dura (Thermo Scientific). The band density of GAPDH was determined as a loading control, and the ratio of phosphorylated vs. total (pan) or that of cleaved vs. intact were calculated.
Statistical analyses
Values are expressed as the means (n = 6). The Student’s t test or one-way ANOVA was used for evaluating statistical significance. A p value of < 0.05 was considered significant. Statistical analyses were performed using Stat View 5.0 for Windows (SAS Institute Inc., Cary, NC). *p < 0.05 (NT vs. H2), †p < 0.05 (vs. CT).
Results
Liver damage
In the CT group, the liver histology at the end of perfusion appeared to be almost normal. In the NT group, nuclear condensation and severe necrosis were observed, whereas in the H2 group these changes were attenuated in Fig. 1a. Apoptosis at the end of perfusion was minimal in the CT group, whereas it was significantly augmented in the NT group, and significantly suppressed in the H2 group (Fig. 1b, c).
Tissue damage after 90 min of reperfusion. Hematoxylin and eosin staining (×20 magnifications) revealed minimal changes in the control (CT) group. Severe vacuolization, pericentral necrosis, and nuclear condensation were observed in the no treatment (NT) group, but these changes were suppressed in the hydrogen gas (H2) group (a). Few TUNEL-positive cells were observed in the CT group. These cells were increased in NT group, but were significantly suppressed in the H2 group (b). The apoptotic index was significantly suppressed in the H2 group (c) (p < 0.01) [n = 6, means; *p < 0.05 (NT vs. H2, Student’s t test), †p < 0.05 (vs. CT, Student’s t test)]
In the CT group, accumulation of ALT and LDH in the perfusate during 90 min of reperfusion was 0.13 ± 0.05 and 0.08 ± 0.04 (IU/g liver), respectively. In the NT group, the ALT and LDH leakage were significantly augmented to 1.47 ± 0.61 and 4.01 ± 2.44 (IU/g liver), respectively, whereas they were significantly suppressed to 0.83 ± 0.24 and 1.25 ± 0.75 (IU/g liver) in the H2 group, respectively (Fig. 2a, b). AST activity showed a similar trend, but did not reach significance (p = 0.08) (Fig. 2c).
The hepatic enzyme leakage after 90 min of reperfusion was minimally changed in the CT group. H2 reduced the alanine aminotransferase (ALT) (a, p < 0.05), lactate dehydrogenase (LDH) (b, p < 0.05) and aspartate aminotransferase (AST) (c, p = 0.08) activities [n = 6, means; *p < 0.05 (NT vs. H2, Student’s t test), †p < 0.05 (vs. CT, Student’s t test)]
Hepatic microcirculation
After 30 min of equilibration perfusion, the graft was perfused at constant pressure (12 cmH2O). In the CT group, portal vein resistance (PVR) was lowest throughout perfusion. In the NT group, it was highest throughout perfusion, whereas augmentation of PVR was significantly suppressed in the H2 group (Fig. 3a).
Microcirculation and liver function. Portal vein resistance (PVR) was the lowest in the CT group and highest in NT group, while the elevation was significantly suppressed in the H2 group (a) (p < 0.05). The oxygen consumption rate (OCR) (b) (p < 0.05), adenosine triphosphate (ATP) content (c) (p < 0.01), and bile production (d) (p < 0.01) were lowest in the NT group, but the decrease was significantly suppressed in the H2 group [n = 6, means; *p < 0.05 (NT vs. H2, Student’s t test), †p < 0.05 (vs. CT, Student’s t test)]
Mitochondrial respiration
Mitochondrial respiratory function was evaluated by the oxygen consumption rate (OCR). By 90 min after perfusion, it was highest in the CT group (1.31 ± 0.15 µmol O2/min/g liver). It fell to 0.86 ± 0.21 (µmol O2/min/g liver) in the NT group, whereas the decrease was significantly suppressed in the H2 group, at 1.20 ± 0.25 µmol O2/min/g liver (Fig. 3b). The ATP content at the end of perfusion was highest in the CT group (0.30 ± 0.05 µmol/g liver). It was significantly lower in the NT group (0.13 ± 0.03 µmol/g liver), but the decrease was significantly suppressed in the H2 group (0.24 ± 0.08 µmol/g liver; Fig. 3c).
Bile production
Integrated hepatic function was assessed by bile production during 90 min of perfusion. Bile production was highest in the CT group (124 ± 13 µl/g liver). It was significantly lower in the NT group (30 ± 14 µl/g liver), but the decrease was significantly suppressed in the H2 group (52 ± 7 µl/g liver; Fig. 3d).
Redox status and lipid peroxidation
The molecular ratio of reduced and oxidized glutathione (GSH/GSSG) was 40 ± 21 in the CT group. This was significantly reduced in the NT group (19 ± 6), but the decrease was significantly suppressed in the H2 group (35 ± 13; Fig. 4a). The sum of MDA and 4-HNE at the end of the perfusion did not differ significantly among the groups (Fig. 4b).
Redox status and lipid peroxidation at the end of 90 min of reperfusion. The reduced glutathione (GSH)/oxidized glutathione (GSSG) ratio decreased in the NT group, but this decrease was suppressed in the H2 group (a) (p < 0.05). Lipid peroxidation (LPO) assessed by MDA + 4-HNE did not change significantly among the groups (b) [n = 6, means; *p < 0.05 (NT vs. H2, Student’s t test)]
Cell death and inflammatory signals
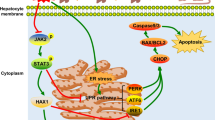
Acute stress responses were evaluated by western blot of the cytoplasmic MKK4–JNK pathway. The NT group had significantly higher values than both the CT group and the H2 group (Fig. 5a, b). Caspase 3, a downstream constituent of the MKK4–JNK pathway, was increased in the NT group, but was inhibited significantly in the H2 group (Fig. 5c).
The mitogen-activated protein kinase 4 (MKK4)–c-jun N-terminal kinase (JNK) cell death signal pathway. Cytosolic protein in the liver at the end of reperfusion was applied to the western blot (top) and the relative band intensity (bottom) was calculated. The phosphorylation of MKK4 (a) (p < 0.001) and JNK (b) (p < 0.01) and the cleavage of caspase 3 (c) (p < 0.05) were highest in the NT group, but were significantly suppressed in the H2 group [n = 6, means; *p < 0.05 (NT vs. H2, Student’s t test), †p < 0.05 (vs. CT, Student’s t test)]
Discussion
We demonstrated the efficacy of H2 in DCD grafts with CS, evidenced by the maintenance of microcirculation, mitochondrial function, and suppressed cellular death. Although the precise mechanism of H2-mediated protection is still not fully understood, the MKK4–JNK pathway was shown to be a therapeutic target.
H2 ameliorated hepatic reperfusion injury after warm ischemia in mice [13] and pigs [21]. H2 administration during reperfusion reduced hepatic reperfusion injury after prolonged CS in heart-beating rat donors [18]. In the DCD liver, minimal change was observed at the end of CS and/or machine perfusion, but the injury became apparent during reperfusion [22, 23]. Accordingly, we tested whether post-reperfusion treatment by H2 suppressed IRI in DCD grafts with CS. The H2 concentration in the perfusion circuit is calculated as 29.3 µM theoretically, and 11.5 µM in reality [18]. Moreover, the possible amount of H2 leaked from the perfusion circuit is sufficiently below the explosion hazard concentration of 4.7% in air [8].
In this study, the GSH/GSSG ratio was decreased in the NT group, but was augmented in the H2 group, leading to minimization of the IRI. GSH is converted to GSSG through its function as a co-factor for antioxidant enzymes [19]. GSSG, on binding with the protein thiol, reduces free GSH levels gradually, thereby reducing the availability of GSH, antioxidant enzyme activity, and increasing oxidative stress [24, 25]. Mitochondrial function is maintained in hepatic warm ischemia, and reperfusion with NAPDH and ATP is maintained, with both the GSH and GSH/GSSG recovering early after reperfusion, suppressing subsequent impairment [19]. In this study, GSH/GSSG and ATP recovered quickly, supporting the suppression of tissue injury.
Lipid peroxidation (LPO) products, assessed by the summation of MDA and 4-HNE, did not differ significantly among the groups. This is controversial because H2 is recognized as a radical scavenger [8, 18]. Lipid hydroperoxides, the initial products of LPO, are produced even under hypoxia, whereas MDA and 4-HNE are produced by a cleavage of hydroperoxides in an oxygen-dependent manner. Therefore, lower values of MDA and 4-HNE do not necessarily mean the absence of lipid peroxidation, especially under conditions of low inconsistent oxygen delivery [19]. A possible explanation for the discrepancy is that H2 administration suppressed the ROS-mediated initiation of LPO. Concomitantly, H2 increased oxygen delivery, thereby possibly accelerating cleavage of lipid hydroperoxide. Conversely, in the NT group, the production efficiency of MDA and 4-HNE decreased with the reduced oxygen supply. These results indicate that the main effect of H2 lies in the improvement of microcirculation rather than in radical scavenging.
The energy state (Fig. 3c) and oxygen consumption rate (Fig. 3b) suggested protection of mitochondrial function. Mitochondrial aerobic metabolism promotes an increase in the production of ROS [26]. In this study, H2 treatment resulted in high GSH/GSSG (Fig. 4a), a constant LPO level (Fig. 4b), and augmented bile productivity (Fig. 3d). Therefore, it cannot be assumed that rising OCR means enhancement of oxidative damage. From these data, hydrogen gas was observed to protect mitochondrial function and breaking the vicious cycle of mitochondrial dysfunction and oxidative stress. Since bile duct complications are an important issue in liver transplantation using DCD grafts, the effect of H2 treatment on bile duct injury should be evaluated by a liver transplantation model with arterial reconstruction in future studies.
Mitochondria-dependent apoptosis in hepatic IRI [15] and transplantation [27] are promoted in part by JNK, which was also shown to amplify ROS generation after translocation to mitochondria [28]. Moreover, the inhibition of JNK reduced cardiac IRI [29] and improved outcome after hepatic cold preservation and transplantation [30]. In the present study, cytosolic phospho-JNK and phospho-MKK4 were much lower in the H2 group than in the NT group (Fig. 5a, b), as were apoptosis and cleavage of caspase 3 (Figs. 1b, 5c). To our knowledge, this is the first report to demonstrate the involvement of MKK4–JNK axis as a target cascade of H2 treatment. Since MKK4 and JNK rapidly translocate to mitochondria upon oxidative stress and enhance oxidative stress thereafter [29, 31], determining whether H2 works on the mitochondrial MKK4–JNK pathway is important. However, we could not evaluate MKK4–JNK in mitochondria, due to the difficulty in the isolation of mitochondria in severely damaged tissue. Biological responses in mitochondria are now under investigation.
H2 reduced vascular resistance in hypertensive rats [32] and in porcine DCD lungs [33]. In this study, the H2-mediated reduction of PVR was evident within 15 min, but increased with perfusion time, with detritus on the in-line filter, regardless of H2 treatment and was not observed in the CS model. In fact, the liver weight was decreased in the DCD model after perfusion without affecting the water and non-water contents. Therefore, it is speculated that constant flow perfusion efficiently washes out embolization factors; however, re-entry of small particles that could pass the in-line filter may cause a gradual increase of PVR. These results imply that H2 reduced PVR, independent of the washout and/or organ swelling factors.
The blood levels of inflammatory cytokines, such as IL-1beta and TNF alpha, were elevated within 3 h of reperfusion [34], and maintained high expression thereafter [35]. Since H2 treatment suppressed TNF alpha and HMGB1 levels in a sepsis model [36], we evaluated pro-inflammatory transcription factors, including NF kappa B (p65 subunit) and AP-1 (c-Fos), in the nuclear fraction. These factors did not differ significantly among the groups [37]. Moreover, phosphorylation of cytoplasmic c-Fos, c-Jun, ASK1, p38 MAPK, Erk1/2, p90RSK, PI3k, PDK1, Akt, mTOR, and cPLA2 did not change significantly with H2 treatment (data not shown). The absence of inflammation in this model could be explained by the absence of leukocytes, the approximately 30-times dilution by perfusate (vs. circulating volume in vivo), and the end-point of 90 min. These results imply that extracorporeal acellular perfusion may become a useful tool to condition the DCD graft without enhancing the inflammatory cascade.
In conclusion, post-reperfusion treatment by H2 gas for a DCD liver graft with cold preservation suppressed reperfusion injury, primarily by maintaining hepatic microcirculation and also by protecting mitochondria. Thus, H2 treatment contributed to liver protection by the maintaining redox status as well as inhibiting the MKK4–JNK pathway.
Abbreviations
- ATP:
-
Adenosine triphosphate
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- CPA:
-
Cardiopulmonary arrest
- DCD:
-
Donation after cardiac death
- DBD:
-
Donation after brain death
- ECD:
-
Expanded criteria donor
- GSSG:
-
Oxidized glutathione
- GSH:
-
Reduced glutathione
- HPFs:
-
High power fields
- H2 :
-
Hydrogen gas
- 4-HNE:
-
4-Hydroxy-2-nonenal
- IRI:
-
Ischemia and reperfusion injury
- IPRL:
-
Isolated perfused rat liver
- JNK:
-
c-jun N-terminal kinase
- KHB:
-
Krebs–Henseleit bicarbonate buffer
- LDH:
-
Lactate dehydrogenase
- LPO:
-
Lipid peroxidation
- MDA:
-
Malondialdehyde
- MKK4:
-
Mitogen-activated protein kinase 4
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate
- NMP:
-
Normothermic machine perfusion
- OCR:
-
Oxygen consumption rate
- PNF:
-
Primary non-function
- PVP:
-
Portal vein pressure
- PVR:
-
Portal vein resistance
- ROS:
-
Reactive oxygen species
- SCD:
-
Standard criteria donor
- SDS-PAGE:
-
SDS polyacrylamide gel electrophoresis
- TUNEL:
-
Terminal deoxynucleotidyl transferase
References
Foley DP, Fernandez LA, Leverson G, Chin LT, Krieger N, Cooper JT, et al. Donation after cardiac death: the University of Wisconsin experience with liver transplantation. Ann Surg. 2005;242:724–31.
Karp SJ, Johnson S, Evenson A, Curry MP, Manning D, Malik R, et al. Minimising cold ischaemic time is essential in cardiac death donor-associated liver transplantation. HPB (Oxford). 2011;13:411–6.
Schlegel A, Kalisvaart M, Scalera I, Laing RW, Mergental H, Mirza DF, et al. The UK DCD risk score: a new proposal to define futility in donation-after-circulatory-death liver transplantation. J Hepatol. 2018;68:456–64.
Nasralla D, Coussios CC, Mergental H, Akhtar MZ, Butler AJ, Ceresa CDL, et al. A randomized trial of normothermic preservation in liver transplantation. Nature. 2018;557:50–6.
Tredger JM. Ischaemia–reperfusion injury of the liver: treatment in theory and in practice. Biofactors. 1998;8:161–4.
Ikeda T, Yanaga K, Kishikawa K, Kakizoe S, Shimada M, Sugimachi K. Ischemic injury in liver transplantation: difference in injury sites between warm and cold ischemia in rats. Hepatology. 1992;16:454–61.
Monbaliu D, Crabbe T, Roskams T, Fevery J, Verwaest C, Pirenne J. Livers from non-heart-beating donors tolerate short periods of warm ischemia. Transplantation. 2005;79:1226–30.
Ohsawa I, Ishikawa M, Takahashi K, Watanabe M, Nishimaki K, Yamagata K, et al. Hydrogen acts as a therapeutic antioxidant by selectively reducing cytotoxic oxygen radicals. Nat Med. 2007;13:688–94.
Kawamura T, Wakabayashi N, Shigemura N, Huang CS, Masutani K, Tanaka Y, et al. Hydrogen gas reduces hyperoxic lung injury via the Nrf2 pathway in vivo. Am J Physiol Lung Cell Mol Physiol. 2013;304:L646–L656.
Sun Q, Kang Z, Cai J, Liu W, Liu Y, Zhang JH, et al. Hydrogen-rich saline protects myocardium against ischemia/reperfusion injury in rats. Exp Biol Med (Maywood). 2009;234:1212–9.
Zheng X, Mao Y, Cai J, Li Y, Liu W, Sun P, et al. Hydrogen-rich saline protects against intestinal ischemia/reperfusion injury in rats. Free Radic Res. 2009;43:478–84.
Abe T, Li XK, Yazawa K, Hatayama N, Xie L, Sato B, et al. Hydrogen-rich University of Wisconsin solution attenuates renal cold ischemia–reperfusion injury. Transplantation. 2012;94:14–21.
Fukuda K, Asoh S, Ishikawa M, Yamamoto Y, Ohsawa I, Ohta S. Inhalation of hydrogen gas suppresses hepatic injury caused by ischemia/reperfusion through reducing oxidative stress. Biochem Biophys Res Commun. 2007;361:670–4.
Liu Q, Shen WF, Sun HY, Fan DF, Nakao A, Cai JM, et al. Hydrogen-rich saline protects against liver injury in rats with obstructive jaundice. Liver Int. 2010;30:958–68.
Uehara T, Bennett B, Sakata ST, Satoh Y, Bilter GK, Westwick JK, et al. JNK mediates hepatic ischemia reperfusion injury. J Hepatol. 2005;42:850–9.
King LA, Toledo AH, Rivera-Chavez FA, Toledo-Pereyra LH. Role of p38 and JNK in liver ischemia and reperfusion. J Hepatobiliary Pancreat Surg. 2009;16:763–70.
Kamata H, Honda S, Maeda S, Chang L, Hirata H, Karin M. Reactive oxygen species promote TNFalpha-induced death and sustained JNK activation by inhibiting MAP kinase phosphatases. Cell. 2005;120:649–61.
Shimada S, Wakayama K, Fukai M, Shimamura T, Ishikawa T, Fukumori D, et al. Hydrogen gas ameliorates hepatic reperfusion injury after prolonged cold preservation in isolated perfused rat liver. Artif Organs. 2016;40(12):1128–1136. https://doi.org/10.1111/aor.12710.
Fukai M, Hayashi T, Yokota R, Shimamura T, Suzuki T, Taniguchi M, et al. Lipid peroxidation during ischemia depends on ischemia time in warm ischemia and reperfusion of rat liver. Free Radic Biol Med. 2005;38:1372–81.
Bessems M, t Hart NA, Tolba R, Doorschodt BM, Leuvenink HG, Ploeg RJ, et al. The isolated perfused rat liver: standardization of a time-honoured model. Lab Anim. 2006;40:236–46.
Matsuno N, Watanabe R, Kimura M, Iwata S, Fujiyama M, Kono S, et al. Beneficial effects of hydrogen gas on porcine liver reperfusion injury with use of total vascular exclusion and active venous bypass. Transplant Proc. 2014;46:1104–6.
Nassar A, Liu Q, Farias K, Buccini L, Baldwin W, Bennett A, et al. Impact of temperature on porcine liver machine perfusion from donors after cardiac death. Artif Organs. 2016;40:999–1008.
Carnevale ME, Balaban CL, Guibert EE, Bottai H, Rodriguez JV. Hypothermic machine perfusion versus cold storage in the rescuing of livers from non-heart-beating donor rats. Artif Organs. 2013;37:985–91.
Imai H, Nakagawa Y. Biological significance of phospholipid hydroperoxide glutathione peroxidase (PHGPx, GPx4) in mammalian cells. Free Radic Biol Med. 2003;34:145–69.
Kobayashi H, Nonami T, Kurokawa T, Kitahara S, Harada A, Nakao A, et al. Changes in the glutathione redox system during ischemia and reperfusion in rat liver. Scand J Gastroenterol. 1992;27:711–6.
Schild L, Reinheckel T, Wiswedel I, Augustin W. Short-term impairment of energy production in isolated rat liver mitochondria by hypoxia/reoxygenation: involvement of oxidative protein modification. Biochem J. 1997;328(Pt 1):205–10.
Bradham CA, Stachlewitz RF, Gao W, Qian T, Jayadev S, Jenkins G, et al. Reperfusion after liver transplantation in rats differentially activates the mitogen-activated protein kinases. Hepatology. 1997;25:1128–35.
Chambers JW, LoGrasso PV. Mitochondrial c-Jun N-terminal kinase (JNK) signaling initiates physiological changes resulting in amplification of reactive oxygen species generation. J Biol Chem. 2011;286:16052–62.
Chambers JW, Pachori A, Howard S, Iqbal S, LoGrasso PV. Inhibition of JNK mitochondrial localization and signaling is protective against ischemia/reperfusion injury in rats. J Biol Chem. 2013;288:4000–11.
Uehara T, Xi Peng X, Bennett B, Satoh Y, Friedman G, Currin R, et al. c-Jun N-terminal kinase mediates hepatic injury after rat liver transplantation. Transplantation. 2004;78:324–32.
Hanawa N, Shinohara M, Saberi B, Gaarde WA, Han D, Kaplowitz N. Role of JNK translocation to mitochondria leading to inhibition of mitochondria bioenergetics in acetaminophen-induced liver injury. J Biol Chem. 2008;283:13565–77.
Zheng H, Yu YS. Chronic hydrogen-rich saline treatment attenuates vascular dysfunction in spontaneous hypertensive rats. Biochem Pharmacol. 2012;83:1269–77.
Haam S, Lee S, Paik HC, Park MS, Song JH, Lim BJ, et al. The effects of hydrogen gas inhalation during ex vivo lung perfusion on donor lungs obtained after cardiac death. Eur J Cardiothorac Surg. 2015;48:542–7.
Shimada S, Fukai M, Wakayama K, Ishikawa T, Kobayashi N, Kimura T, et al. Hydrogen sulfide augments survival signals in warm ischemia and reperfusion of the mouse liver. Surg Today. 2015;45:892–903.
Nakamitsu A, Hiyama E, Imamura Y, Matsuura Y, Yokoyama T. Kupffer cell function in ischemic and nonischemic livers after hepatic partial ischemia/reperfusion. Surg Today. 2001;31:140–8.
Zheng Y, Zhu D. Molecular hydrogen therapy ameliorates organ damage induced by sepsis. Oxidative Med Cell Longev. 2016;2016:5806057.
Zwacka RM, Zhang Y, Zhou W, Halldorson J, Engelhardt JF. Ischemia/reperfusion injury in the liver of BALB/c mice activates AP-1 and nuclear factor kappaB independently of IkappaB degradation. Hepatology. 1998;28:1022–30.
Acknowledgements
We thank Mr. Masatoshi Horigome for the animal care, Ms. Sayaka Miyoshi for technical assistance, and the staff of the Department of Gastroenterological Surgery I, Hokkaido University Graduate School of Medicine, for their kind cooperation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Ishikawa, T., Shimada, S., Fukai, M. et al. Post-reperfusion hydrogen gas treatment ameliorates ischemia reperfusion injury in rat livers from donors after cardiac death: a preliminary study. Surg Today 48, 1081–1088 (2018). https://doi.org/10.1007/s00595-018-1693-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-018-1693-0