Abstract
Aims
Compound 21 (C21), selective AT2 receptor agonist, has cardioprotective effects in experimental models of hypertension and myocardial infarction. The aims of the study was to evaluate the effect of C21, losartan, or both in Zucker diabetic fatty (ZDF) rats (type 2 diabetes) on (1) the prevention of myocardial hypertrophy; (2) myocardial expression of phosphatase and tensin homolog (PTEN), a target gene of miR-30a-3p, involved in myocardial remodelling.
Methods
Experiments were performed in ZDF (n = 33) and in control Lean (8) rats. From the 6th to the 20th week of age, we administered C21 (0.3 mg/kg/day) to 8 ZDF rats. 8 ZDF rats were treated with losartan (10 mg/kg/day), 8 rats underwent combination treatment, C21+ losartan, and 9 ZDF rats were left untreated. Blood glucose and blood pressure were measured every 4 weeks. At the end of the study the hearts were removed, the apex was cut for the quantification of PTEN mRNA and miR-30a-3p expression (realtime-PCR). Myocardial hypertrophy was evaluated by histomorphometric analysis, and nitrotyrosine expression (as marker of oxidative stress) by immunohistochemistry.
Results
ZDF rats had higher blood glucose (p < 0.0001) with respect to control Lean rats, while blood pressure did not change. Both parameters were not modified by C21 treatment, while losartan and losartan + C21 reduced blood pressure in ZDF rats (p < 0.05). miR-30a-3p expression was increased in ZDF rats (p < 0.01) and PTEN mRNA expression was decreased (p < 0.05). ZDF rats developed myocardial hypertrophy (p < 0.01) and increased oxidative stress (p < 0.01), both were prevented by C21 or losartan, or combination treatment. C21 or losartan normalized the expression of miR-30a-3p and PTEN.
Conclusions
Activation of AT2 receptors or AT1 receptor blockade prevents the development of myocardial hypertrophy in ZDF rats. This occurs through the modulation of the miR-30a-3p/PTEN interaction.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
An “epidemic” of type 2 diabetes is presently ongoing on a worldwide basis [1, 2]. Cardiovascular complications remain a major cause of morbility and mortality in diabetic patients [3, 4]. Diabetic cardiomyopathy is characterized by functional and structural modifications caused by glyco-metabolic disorders, which eventually causes oxidative stress, mitochondrial dysfunction, inflammation, fibrosis and hypertrophy. The activation of the renin-angiotensin system plays a central role in the development and progression of diabetic cardiomyopathy [5, 6], and drugs acting on the renin angiotensin system (RAS), by inhibiting the angiotensin converting enzyme or by blocking the angiotensin type 1 (AT1) receptors, are treatments of choice for the cardiovascular complications of diabetes [7]. Two membrane G-protein coupled receptors, AT1 and AT2 receptors, primarily mediate the activity of angiotensin II, the main effector of the RAS. The pharmacological effects of the blockade of the AT1 receptors, as occurs with AT1 receptor blockers, are well-known [8]. AT1 receptor blockers by increasing the circulating levels of angiotensin II could end up by stimulating the AT2 receptors, which are generally considered capable to counteract AT1 receptor mediated effects [9,10,11,12,13].
Compound 21 (C21), a highly selective AT2 receptor agonist [14], directly stimulates AT2 receptors, allowing to investigate the AT2 receptor mediated effects. Cardiomyocytes, myocardial fibroblasts and endothelial cells express AT2 receptors, and the AT2 receptor-mediated effects in the cardiovascular system are complex [15]. C21 administration improves cardiac function in rat with myocardial infarction [12], reduces myocardial fibrosis in experimental model of cyclosporine nephropathy [16], prevents vascular stiffness in an experimental model of N-nitro-l-arginine-methyl ester-induced hypertension [17] and reduces myocardial and vascular fibrosis in stroke-prone spontaneously hypertensive rats [18].
MicroRNAs (miRNAs) are small, non-coding RNAs, which negatively control gene expression [19,20,21]. Each miRNA controls the expression of several genes, which may have different effects, displaying the complexity of this regulatory system. Increasing evidence indicate that specific miRNAs are involved in myocardial remodelling, modulating fibrosis [22, 23] and/or hypertrophy [22,23,24,25].
Among them, members of miR-30 family, which contains five components (miR-30a, miR-30b, miR-30c, miR-30d, miR-30e), showing different actions depending on their modulation and on target genes [26], are involved in myocardial fibrosis in high renin hypertension [22], in angiotensin II-induced myocardial hypertrophy [27], and in pressure-overload hypertrophy [27, 28].
Our experiments aimed to ascertain whether in Zucker diabetic fatty rats, a well-known experimental model of type 2 diabetes [29, 30], C21 administration had cardioprotective effects and to investigate the potential role of miR-30a-3p in myocardial remodelling.
Methods
Experimental protocol
Animal husbandry handled in conformity with the Institutional Guidelines in compliance with National laws and policies (D.L.n. 116, Gazzetta Ufficiale della Repubblica Italiana, suppl.40, Feb.18, 1992) and experiments were performed in accordance with the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication No. 85-23, revised 1996).
Conscious male Zucker Diabetic Fatty rats and control lean (5–6 week old, Charles River, Calco, Italy) were individually housed in a temperature-controlled room (22 °C) with a 12:12 light–dark cycle and allowed to accustom with the experimental procedures. Animals had free access to high protein diet (Formulab Diet 5008) and tap water [31].
At 5–6 weeks of age, before the onset of hyperglycemia in ZDF rats, and once a month, body weight (BW, g) and blood glucose (mg/dl, OneTouch Ultra system, LifeScan Inc, Milpitas CA, USA) were measured. C21 (0.3 mg/kg/day, intraperitoneal injection; n = 8; Vicore Pharma. Sweden) or losartan (Los, 10 mg/kg/day, in drinking water; n = 8) or combination treatment C21 + losartan (n = 8) were administered to ZDF rats for 15 weeks. A group of ZDF rats (n = 9) and control Lean (n = 8) were maintained without any treatment. At the end of the experimental protocol the rats were euthanized with an overdose of anesthesia (sodium pentobarbital). Systolic blood pressure (SBP, mmHg) was measured monthly according to the tail cuff method (average of 6 recordings. BP Recorder, Ugo Basile Instruments, Italy) by an investigator who was unaware of the specific treatments [31].
After the sacrifice, the hearts were immediately excised and weighted. The apex of the heart was cutted, frozen in liquid nitrogen and stored at − 80 °C until miRNA and total RNA extraction. The heart, sectioned into three transverse slices from the apex to the base, was fixed with 10% formalin, embedded in paraffin and used for light microscopic examination and morphometric analysis of myocardial hypertrophy and nitrotyrosine expression by immunohistochemistry.
Histological analysis and morphometric evaluation of myocardial hypertrophy
For all rats the transversal cardiac sections (4 µm) were deparaffinized, rehydrated, and stained with hematoxylin–eosin (H&E). Changes in cardiac morphology were assessed by light microscopic analysis of sections for each group studied. A computerized digital camera (Olympus Camedia 5050, Olympus Inc., Tokyo, Japan) was used to capture 5 Mp (24 bit color depth) 10 images (× 400 magnification) of left ventricular myocardium, including ventricular septum (stored as JPG files), and analyzed for morphometric evaluation of myocardial hypertrophy with a computerized imaging software (ImageJ, NIH, Bethesda, Maryland). Myocardial hypertrophy was evaluated in 100 cardiomyocytes transversally sectioned and expressed as the ratio between nuclear area and cell area.
Immunohistochemical evaluation of myocardial nitrotyrosine expression
Immunohistochemical evaluation was performed on consecutive sections (3 µm) of formalin fixed, paraffin embedded cardiac tissue. Sections were deparaffinized in xylene and rehydrated through graded alcohol series. Endogenous peroxidase activity was blocked by 3% hydrogen peroxide. The sections were treated by boiling in citrate buffer (0.01 mol/l, pH 6) in microwave (750 W), and incubated over night at 4 °C with primary antibody anti Nitrotyrosine (1:150, anti-rabbit polyclonal antibody, ab42789, Abcam Cambridge, UK). The reaction was amplified with LSAB2 + System-HRP (Dako, CA, USA). A positive immunoreaction was identified after incubation with DAB (Dako, Glostrup, Danimarca) counterstaining with Mayer haematoxylin. Negative controls were obtained omitting the primary antibody. Sections were analyzed using a Leica microscope (Leitz Camera). Two independent pathologists, blinded to the treatment, observed the immunostaining with a Leica microscope (Leitz Camera) and, subsequently, for each rat, 5-Mp (24-bit colour depth) images (× 400 magnification) were captured by a computerized digital camera (Olympus Camedia 5050, Olympus). Immunostaining was quantified by a pathologist, using a computerized imaging software (ImageJ, NIH), in automated fashion in 20 fields, randomly selected from each section. Nitrotyrosine immunostaining was expressed as percentage (ratio between immunostaining area and total area).
miRNA and total RNA extraction and real-time PCR
The miRNAs and total RNA were extracted from rat heart using Mirvana kit (Ambion, Applied Biosystems, Foster City, CA), according to the manufacturer’s protocol. TaqMan microRNA assays (Applied Biosystems) that include miRNA-specific RT primers and TaqMan probes were used to quantify the expression of mature miRNAs. In brief, reverse transcriptase reactions (TaqMan MicroRNA Reverse Transcription Kit, Foster City, CA) containing 1 ng of small RNA, 3 μl stem–loop RT primer, 1.5 μl RT buffer, 0.15 μl dNTP mix, 1 μl MultiScribe reverse, and 0.19 μl RNase inhibitor were performed. The 15 μl reactions were incubated for 30 min at 16 °C, 30 min at 42 °C, and 5 min at 85 °C. The miR-30a-3p and U87 (Applied Biosystems) were evaluated by real-time PCR using the ABI PRISM 7900 Sequence Detection System (Applied Biosystems). The 15 μl PCR included 2 μl reverse transcription product, 10 μl of 2× TaqMan Universal PCR Master Mix and the specific 20× TaqMan MicroRNA Assay. The reactions were incubated at 95 °C for 10 min, followed by 40 cycles of 95 °C for 15 s and 60 °C for 60 s. All reactions were performed in duplicate. Expression levels were normalized to U87 expression, used as reference, following the 2− ΔΔCt formula, as previously described [23].
The mRNA expression of Phosphatase and Tensin homologue (PTEN) and GAPDH, used as reference gene, was evaluated by quantitative real-time PCR using the TaqMan Realtime ABI Prism 7900 HT Sequence Detection System (Applied Biosystems). PTEN mRNA and GAPDH expression was evaluated using the Assay-on-Demand Gene Expression Product (Applied Biosystem), following the manufacturer’s instructions, as previously described [32]. Values are reported as PTEN/GAPDH mRNA ratio and expressed in arbitrary units.
Bioinformatic analysis
TargetScan v.7.2 (http://www.targetscan.org/), miRDB (http://www.mirdb.org), Mirwalk 3.0 (http://mirwalk.umm.uni-heidelberg.de/) and Tarbase v.7.0 (http://diana.imis.athena-innovation.gr) software were used to investigate miR-30a-3p targets.
Statistical analysis
Data are presented as means ± standard error of the mean (SEM). Differences among the groups of rats (control Lean rats, ZDF rats, ZDF rats + C21, ZDF rats + losartan, ZDF rats + C21 + losartan) for blood glucose, systolic blood pressure, body weight, heart/body weight, myocardial hypertrophy, nitrotyrosine expression, miR-30a-3p expression, and PTEN mRNA expression were assessed with the use of analysis of variance (ANOVA) followed by the Fisher’s protected least-significant test for post-hoc comparisons. Differences between means were considered significant at p < 0.05.
Results
Effects of Compound 21 and losartan on blood glucose, systolic blood pressure, myocardial hypertrophy and nitrotyrosine expression
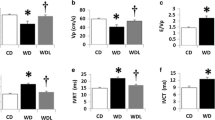
At the end of the experimental period blood glucose levels were significantly higher in diabetic rats (Table 1) and were not modified by Compound 21 or losartan treatment (Table 1). Blood pressure was similar in control Lean and ZDF rats, and was not significantly modified by C21 treatment (Table 1), while losartan treatment, alone or in combination with C21 caused a detectable reduction (Table 1). Body weight and heart/body weight ratio were not significantly modified in ZDF rats and in ZDF rats treated or not with C21 or losartan or losartan + C21 combination with respect to control Lean rats (Table 1).
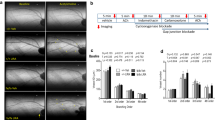
At the end of the experimental period ZDF rats developed myocardial hypertrophy (Fig. 1a, b), while administration of C21 or losartan or losartan + C21 combination prevented the onset of myocardial hypertrophy in ZDF rats. In our experimental model, the presence of myocardial hypertrophy was evaluated by histomorphometric techniques, which are more sensitive than the heart/body weight ratio to evaluate the initial changes in cardiomyocytes that characterize hypertrophy.
Effect of C21 and losartan administration on myocardial hypertrophy in ZDF rats. a Representative images of histological transverse sections (stained with EE) and related microscopic fields that show left ventricular hypertrophy with related enlarged cardiomyocyte nuclei (EE, 40×) in ZDF rats as compared to control Lean, ZDF + C21, ZDF + losartan and ZDF + C21 + losartan treated rats. C21, losartan and co-administration of C21 plus losartan prevented the development of myocardial hypertrophy in ZDF rats. b Quantification of myocardial hypertrophy in the different groups of rats. Data are means ± SEM. *p < 0.01 vs. other groups
Nitrotyrosine expression, marker of oxidative stress, in myocardial tissue was increased in ZDF rats, but not in ZDF rats treated with C21 or losartan or losartan + C21 combination (Fig. 2a, b), indicating that both AT1 receptor blockade and AT2 receptor stimulation, alone or in combination, counteract myocardial oxidative stress in diabetic rats.
Effects of C21 and losartan treatment on myocardial nitrotyrosine expression in ZDF rats. a Representative immunohistochemistry photomicrographs of nitrotyrosine expression in control Lean, ZDF, ZDF + C21, ZDF + losartan, and ZDF + C21 + losartan treated rats (original magnification 40×). Immunostaining (cytoplasmic brownish staining) shows a significant increase in nitrotyrosine expression in ZDF rats as compared to control Lean, while C21 or losartan or C21 + losartan treatments caused a reduction of nitrotyrosine expression as compared to ZDF rats. b Quantification of myocardial nitrotyrosine expression in the different groups of rats. Data are means ± SEM. *p < 0.01 vs. Lean rats, #p < 0.01 vs. ZDF rats, §p < 0.05 vs. ZDF rats
Effects of C21 and losartan on myocardial miR-30a-3p and PTEN mRNA expression
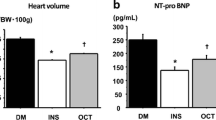
Myocardial miR-30a-3p expression, evaluated by real-time PCR, was increased in ZDF rats with respect to control Lean rats, while in ZDF rats treated with C21 or losartan or losartan + C21, myocardial miR-30a-3p was similar to control Lean rats (Fig. 3).
Effects of C21 and losartan administration on myocardial miR-30a-3p and PTEN mRNA expression in ZDF rats. a Myocardial miR-30a-3p expression was significantly up-regulated in ZDF rats with respect to control Lean rats. C21 or losartan treatment, alone or in combination, prevented the increase of myocardial miR-30a-3p expression in ZDF rats. Data are mean ± SEM. *p < 0.01 vs. control Lean rats, §p < 0.05 vs. ZDF rats. b Myocardial PTEN mRNA expression was significantly down-regulated in ZDF rats with respect to control Lean rats. C21 or losartan treatment, alone or in combination, caused an increase of myocardial PTEN expression in ZDF rats. Data are mean ± SEM. *p < 0.05 vs. Lean rats, §p < 0.01 vs. ZDF rats
Real-time PCR experiments demonstrated that myocardial PTEN mRNA expression, target of miR-30a-3p [33], was decreased in ZDF rats with respect to control Lean rats. This effect was blocked by C21 or losartan treatment, alone or in combination, in ZDF rats (Fig. 3).
Discussion
The results of this study demonstrate that C21 administration prevented the onset of myocardial hypertrophy in diabetic rats. Activation of AT2 receptors in ZDF rats, by C21 administration, is as effective as the blockade of AT1 receptors (losartan treatment) in the prevention of myocardial hypertrophy. Since the single treatment with C21 or losartan is able to prevent the development of hypertrophy in our experimental model, it is not surprising that combination therapy, which showed additive effects in other experimental setting, as in reducing albuminuria in diabetic nephropathy [31], or in reducing interstitial myocardial collagen content in stroke prone spontaneously hypertensive rats [18], did not have additive effect in the prevention of myocardial hypertrophy in Zucker diabetic rats. In addition, these data demonstrate that miR-30a-3p expression increased in the hearts of Zucker diabetic rats, while the expression of PTEN, a phosphatase involved in the myocardial hypertrophy through PI3K-AKT pathway and molecular target of miR-30a-3p [33], showed a reduction.
Activation of AT2 receptors, using C21 administration, or the blockade of AT1 receptors with losartan, alone or in combination, were effective in the prevention of myocardial hypertrophy in diabetic rats. The cardioprotective effects of AT2 receptor stimulation occurred in the absence of blood glucose or blood pressure modifications, which are the main factors promoting cardiomyopathy in diabetes. The antihypertrophic effect of C21 was similar to that observed with losartan treatment, which also caused a reduction in blood pressure. In fact, as expected, even if in our experimental conditions blood pressure did not increase in diabetic rats at 20 weeks of age, losartan treatment, alone or in combination with C21, caused a reduction in blood pressure, which might play a role in mediating the cardioprotective effects of AT1 blockade.
Activation of the renin-angiotensin system plays a role in diabetic cardiomyopathy [5, 6] and drugs acting on the renin angiotensin system, as ACE inhibitors or AT1 receptors blockers, are the main tools to counteract this diabetic complication. Hyperglycemia causes an increase of oxidative stress leading to a direct cardiomyocyte damage [34]. In our experimental conditions, nitrotyrosine expression, a marker of oxidative stress, was increased in the cardiomyocytes of Zucker diabetic rats when compared to control Lean rats. Both C21 and losartan treatment prevented the increase of oxidative stress in myocardial tissue in Zucker diabetic rats. Since no treatment was planned to correct hyperglycemia in the original design of the protocol, the increased expression of nitrotyrosine and the development of myocardial hypertrophy are reasonably sustained by hyperglycemia, i.e. by metabolic factors, while we can rule out a systemic hemodynamic effect, as blood pressure was not modified in ZDF rats in our experimental conditions. Experimental data showed that AT2 receptor stimulation, alone or in combination with AT1 receptor blockade, has positive effects in case of metabolic disorders [35]. In some conditions the activation of AT2 receptors may exceed the effect of the blockade of AT1 receptors. In high-fat/high fructose fed rats, a model of diet-induced insulin resistance, both AT2 receptor stimulation with C21/M24 and AT1 receptor blockade with losartan restored normal adipocyte size distribution and reduced high fat/high fructose diet-induced insulin resistance [36]. Interestingly, AT2 receptor stimulation, but not AT1 receptor blockade, showed a tendency to reduce fasting triglyceride levels in high fat/high fructose fed rats, while caused a significant reduction of triglycerides in control diet fed rats [36]. In line with these data, we can hypothesize that in our study the cardioprotective effects of the AT2 receptor stimulation, alone or in combination with AT1 receptor blockade, may be due at least in part to a better control of the lipid profile, as we have previously shown in the same experimental model of diabetes [31].
In type 2 diabetic mice it has also been demonstrated that AT2 receptor stimulation reduced serum TNF-α and increased adiponectin levels [37]. AT2 receptor stimulation was also able to ameliorate streptozotocin-induced diabetes by protecting pancreatic islets via antioxidative mechanisms [38].
miRNAs, non coding RNAs with an important role in the regulation of gene expression, are involved in the development of diabetic complications [39, 40]. In the present study, in the hearts of diabetic rats we have observed an increased expression of miR-30a-3p, member of miR-30 family, which is involved in neoplastic proliferation, invasiveness and metastasis [41], myocardial remodelling [22] and apoptosis [41, 42]. In ZDF rats treated with C21 or losartan, which did not develop myocardial hypertrophy, miR-30a-3p expression did not increase, suggesting a role of miR-30a-3p in myocardial hypertrophy in diabetic rats. In the heart of diabetic rats, we have evaluated PTEN mRNA expression, a phosphatase involved in PI3K-AKT signalling [43]. PTEN is a molecular target of miR-30a-3p [33], and acts as negative regulator of the PI3K system. A link between the activation of AT2 receptors and PI3K signalling or NO/cyclic guanosine monophosphate (cGMP) pathway has been previously described and implicated in cardiovascular protective effects in hypertension [44, 45]. In obesity PI3K signalling pathway was shown to modulate Ca2+ handling and vasoconstriction in mesenteric arteries from obese Zucker rats [46]. Even if an in-depth investigation of PI3K/AKT or NO/cGMP signalling pathways exceeds the purpose of this study, our results, by demonstrating a normalization of myocardial PTEN and nitrotyrosine expression, support the role of these pathways in the cardioprotective effects of both AT2 receptor stimulation and AT1 receptor blockade in Zucker diabetes rats. In the hearts of ZDF rats PTEN mRNA expression was decreased with respect to control Lean rats, while C21 or losartan treatment prevented the decrease of PTEN expression, suggesting that the anti-hypertrophic effect caused by C21 or losartan treatment might be mediated also by the modulation of miR-30a-3p/PTEN interaction. Taken together, these data demonstrate that AT2 receptor stimulation prevented the development of myocardial hypertrophy in diabetic rats and the similarities with the effects observed in diabetic rats treated with losartan allows to hypothesize that this cardioprotective action is equivalent to that obtained by AT1 receptor blockers, which represent at the moment the drugs of choice to treat diabetic cardiomyopathy. Consequently, the results of this study suggest that activation of AT2 receptors by modulation of miR-30a-3p/PTEN and the reduction of oxidative stress could represent a therapeutic strategy to counteract the development of myocardial hypertrophy in the presence of diabetes.
References
Hu FB (2011) Globalization of diabetes. The role of diet, lifestyle, and genes. Diabetes Care 34:1249–1257. https://doi.org/10.2337/dc11-0442
Zimmet PZ, Magliano DJ, Herman WH, Shaw JE (2014) Diabetes: a 21st century challenge. Lancet Diabetes Endocrinol 2:56–64. https://doi.org/10.1016/S2213-8587(13)70112-8
UKPDS Group (1998) Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 317:703–713
Lorber D (2014) Importance of cardiovascular disease risk management in patients with type 2 diabetes mellitus. Diabetes Metab Syndr Obes 7:169–183. https://doi.org/10.2147/DMSO.S61438
Jia G, Whaley-Connell A, Sowers JR (2018) Diabetic cardiomyopathy: a hyperglycaemia and insulin-resistance-induced heart disease. Diabetologia 61:21–28. https://doi.org/10.1007/s00125-017-4390-4
Dhalla NS, Liu X, Panagia V, Takeda N (1998) Subcellular remodeling and heart dysfunction in chronic diabetes. Cardiovasc Res 40:239–247
Mancia G, Fagard R, Narkiewicz K et al (2013) 2013 ESH/ESC guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 31:1281–1357. https://doi.org/10.1097/01.hjh.0000431740.32696.cc
Borghi C, SIIA Task Force, Rossi F, SIF Task Force (2015) Role of the renin-angiotensin-aldosterone system and its pharmacological inhibitors in cardiovascular diseases: complex and critical issues. High Blood Press Cardiovasc Prev 22:429–444. https://doi.org/10.1007/s40292-015-0120-5
McCarthy CA, Widdop RE, Denton KM, Jones ES (2013) Update on the angiotensin AT2 receptor. Curr Hypertens Rep 15:25–30. https://doi.org/10.1007/s11906-012-0321-4
Ali Q, Wu Y, Hussain T (2013) Chronic AT2 receptor activation increases renal ACE2 activity, attenuates AT1 receptor function and blood pressure in obese Zucker rats. Kidney Int 84:931–939. https://doi.org/10.1038/ki.2013.193
Rompe F, Artuc M, Hallberg A et al (2010) Direct angiotensin II type 2 receptor stimulation acts anti-inflammatory through epoxyeicosatrienoic acid and inhibition of nuclear factor kappaB. Hypertension 55:924–931. https://doi.org/10.1161/HYPERTENSIONAHA.109.147843
Kaschina E, Grzesiak A, Li J et al (2008) Angiotensin II type 2 receptor stimulation: a novel option of therapeutic interference with the renin-angiotensin system in myocardial infarction? Circulation 118:2523–2532. https://doi.org/10.1161/CIRCULATIONAHA.108.784868
Lauer D, Slavic S, Sommerfeld M et al (2014) Angiotensin type 2 receptor stimulation ameliorates left ventricular fibrosis and dysfunction via regulation of tissue inhibitor of matrix metalloproteinase 1/matrix metalloproteinase 9 axis and transforming growth factor β1 in the rat heart. Hypertension 63:e60–e67. https://doi.org/10.1161/HYPERTENSIONAHA.113.02522
Unger T, Dahlöf B (2010) Compound 21, the first orally active, selective agonist of the angiotensin type 2 receptor (AT2): implications for AT2 receptor research and therapeutic potential. J Renin Angiotensin Aldosterone Syst 11:75–77. https://doi.org/10.1177/1470320309347792
Kaschina E, Namsolleck P, Unger T (2017) AT2 receptors in cardiovascular and renal diseases. Pharmacol Res 125:39–47. https://doi.org/10.1016/j.phrs.2017.07.008
Castoldi G, di Gioia CR, Carletti R et al (2016) Angiotensin type-2 (AT-2)-receptor activation reduces renal fibrosis in cyclosporine nephropathy: evidence for blood-pressure independent effect. Biosci Rep 36:e00403. https://doi.org/10.1042/BSR20160278
Paulis L, Becker ST, Lucht K et al (2012) Direct angiotensin II type 2 receptor stimulation in Nω-nitro-L-arginine-methyl ester-induced hypertension. The effect on pulse wave velocity and aortic remodeling. Hypertension 59:485–492. https://doi.org/10.1161/HYPERTENSIONAHA.111.185496
Rehman A, Leibowitz A, Yamamoto N, Rautureau Y, Paradis P, Schiffrin EL (2012) Angiotensin type 2 receptor agonist compound 21 reduces vascular injury and myocardial fibrosis in stroke-prone spontaneously hypertensive rats. Hypertension 59:291–299. https://doi.org/10.1161/HYPERTENSIONAHA.111.180158
Bartel DP (2004) MicroRNAs: genomics, biogenesis, mechanism, and function. Cell 116:281–297
Huntzinger E, Izaurralde E (2011) Gene silencing by microRNAs: contributions of translational repression and mRNA decay. Nat Rev Genet 12:99–110. https://doi.org/10.1038/nrg2936
Guo H, Ingolia NT, Weissman JS, Bartel DP (2010) Mammalian microRNAs predominantly act to decrease target mRNA levels. Nature 466:835–840. https://doi.org/10.1038/nature09267
Duisters RF, Tijsen AJ, Schroen B et al (2009) miR-133 and miR-30 regulate connective tissue growth factor: implications for a role of microRNAs in myocardial matrix remodeling. Circ Res 104:170–178. https://doi.org/10.1161/CIRCRESAHA.108.182535
Castoldi G, Di Gioia CR, Bombardi C et al (2012) MiR-133a regulates collagen 1A1: potential role of miR-133a in myocardial fibrosis in angiotensin II-dependent hypertension. J Cell Physiol 227:850–856. https://doi.org/10.1002/jcp.22939
Guan X, Wang L, Liu Z et al (2016) miR-106a promotes cardiac hypertrophy by targeting mitofusin 2. J Mol Cell Cardiol 99:207–217. https://doi.org/10.1016/j.yjmcc.2016.08.016
Zheng D, Ma J, Yu Y et al (2015) Silencing of miR-195 reduces diabetic cardiomyopathy in C57BL/6 mice. Diabetologia 58:1949–1958. https://doi.org/10.1007/s00125-015-3622-8
Yang SJ, Yang SY, Wang DD et al (2017) The miR-30 family: versatile players in breast cancer. Tumor Biol 39:1–13. https://doi.org/10.1177/1010428317692204
Pan W, Zhong Y, Cheng C et al (2013) MiR-30-regulated autophagy mediates angiotensin II-induced myocardial hypertrophy. PLoS One 8:e53950. https://doi.org/10.1371/journal.pone.0053950
Yin X, Peng C, Ning W et al (2013) miR-30a downregulation aggravates pressure overload-induced cardiomyocyte hypertrophy. Mol Cell Biochem 379:1–6. https://doi.org/10.1007/s11010-012-1552-z
Peterson RG, Shaw WN, Neel MA, Little LA, Eichberg J (1990) Zucker diabetic fatty rat as a model for non-insulin dependent diabetes mellitus. ILAR J 32:16–19. https://doi.org/10.1093/ilar.32.3.16
King AJ (2012) The use of animal models in diabetes research. Br J Pharmacol 166:877–894. https://doi.org/10.1111/j.1476-5381.2012.01911.x
Castoldi G, di Gioia CR, Bombardi C et al (2014) Prevention of diabetic nephropathy by compound 21, selective agonist of angiotensin type 2 receptors, in Zucker diabetic fatty rats. Am J Physiol Renal Physiol 307:F1123–F1131. https://doi.org/10.1152/ajprenal.00247.2014
Castoldi G, di Gioia CR, Giollo F et al (2016) Different regulation of miR-29a-3p in glomeruli and tubules in an experimental model of angiotensin II-dependent hypertension: potential role in renal fibrosis. Clin Exp Pharmacol Physiol 43:335–342. https://doi.org/10.1111/1440-1681.12532
Karginov FV, Hannon GJ (2013) Remodeling of Ago2-mRNA interactions upon cellular stress reflects miRNA complementarity and correlates with altered translation rates. Genes Develop 27:1624–1632. https://doi.org/10.1101/gad.215939.113
Tate M, Grieve DJ, Ritchie RH (2017) Are targeted therapies for diabetic cardiomyopathy on the horizon? Clin Sci 131:897–915. https://doi.org/10.1042/CS20160491
Paulis L, Foulquier S, Namsolleck P, Recarti C, Steckelings UM, Unger T (2016) Combined angiotensin receptor modulation in the management of cardio-metabolic disorders. Drugs 76:1–12. https://doi.org/10.1007/s40265-015-0509-4
Shum M, Pinard S, Guimond MO et al (2013) Angiotensin II type 2 receptor promotes adipocyte differentiation and restores adipocyte size in high-fat/high-fructose diet-induced insulin resistance in rats. Am J Physiol Endocrinol Metab 304(2):E197–E210. https://doi.org/10.1152/ajpendo.00149.2012
Ohshima K, Mogi M, Jing F et al (2012) Direct angiotensin II type 2 receptor stimulation ameliorates insulin resistance in type 2 diabetes mice with PPARγ activation. PLoS One 7(11):e48387. https://doi.org/10.1371/journal.pone.0048387
Shao C, Yu L, Gao L (2014) Activation of angiotensin type 2 receptors partially ameliorates streptozotocin-induced diabetes in male rats by islet protection. Endocrinology 155(3):793–804. https://doi.org/10.1210/en.2013-1601
Guo R, Nair S (2017) Role of microRNA in diabetic cardiomyopathy: from mechanism to intervention. BBA Mol Basis Dis 1863:2070–2077. https://doi.org/10.1016/j.bbadis.2017.03.013
Kato M, Natarajan R (2015) MicroRNAs in diabetic nephropathy: functions, biomarkers, and therapeutic targets. Ann N Y Acad Sci 1353:72–88. https://doi.org/10.1111/nyas.12758
Wang W, Lin H, Zhou L et al (2014) MicroRNA-30a-3p inhibits tumor proliferation, invasiveness and metastasis and is downregulated in hepatocellular carcinoma. EJSO 40:1586–1594. https://doi.org/10.1016/j.ejso.2013.11.008
Li W, Dai H, Ou Q, Zuo GQ, Liu CA (2016) Overexpression of microRNA-30a-5p inhibits liver cancer cell proliferation and induces apoptosis by targeting MTDH/PTEN/AKT pathway. Tumor Biol 37:5885–5895. https://doi.org/10.1007/s13277-015-4456-1
Oudit GY, Penninger JM (2009) Cardiac regulation by phosphoinositide 3-kinases and PTEN. Cardiovasc Res 82:250–260. https://doi.org/10.1093/cvr/cvp014
Gao S, Park BM, Cha SA, Park WH, Park BH, Kim SH (2013) Angiotensin AT2 receptor agonist stimulates high stretch induced- ANP secretion via PI3K/NO/sGC/PKG/pathway. Peptides 47:36–44. https://doi.org/10.1016/j.peptides.2013.06.008
Savoia C, Ebrahimian T, He Y, Gratton JP, Schiffrin EL, Touyz RM (2006) Angiotensin II/AT2 receptor-induced vasodilation in stroke-prone spontaneously hypertensive rats involves nitric oxide and cGMP-dependent protein kinase. J Hypertens 24(12):2417–2422. https://doi.org/10.1097/01.hjh.0000251902.85675.7e
Sánchez A, Contreras C, Climent B et al (2018) Impaired Ca2+ handling in resistance arteries from genetically obese Zucker rats: Role of the PI3K, ERK1/2 and PKC signaling pathways. Biochem Pharmacol 152:114–128. https://doi.org/10.1016/j.bcp.2018.03.020
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Animal studies were in conformity with the Institutional Guidelines in compliance with National laws and policies (D.L.n. 116, Gazzetta Ufficiale della Repubblica Italiana, suppl.40, Feb.18, 1992) and experiments were performed in accordance with the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication No. 85-23, revised 1996).
Informed Consent
For this type of study (experimental study on animal model) it is not required.
Additional information
Managed by Massimo Porta.
Rights and permissions
About this article
Cite this article
Castoldi, G., di Gioia, C.R.T., Roma, F. et al. Activation of angiotensin type 2 (AT2) receptors prevents myocardial hypertrophy in Zucker diabetic fatty rats. Acta Diabetol 56, 97–104 (2019). https://doi.org/10.1007/s00592-018-1220-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-018-1220-1