Abstract
Background
Closed reduction and spica cast is still the preferred treatment option for children presenting with developmental dysplasia of the hip (DDH) after the age of 6 months. This study aims to investigate the outcomes of patients with DDH treated by closed reduction and dynamic cast immobilization.
Methods
In total, 159 patients (mean age 15.6 ± 4.2 months; 172 hips) were treated with a dynamic cast immobilization for 3 months, followed by an abduction brace until a stable concentric reduction was achieved. Radiological examination was performed at each follow-up visit to assess reduction, redislocation rate and presence of avascular necrosis (AVN) of the femoral epiphysis. Final radiographic results were evaluated with the Severin classification.
Results
The redislocation rate was 4.1% (7/172); the overall AVN rate was 14.5% (grade II: 16 hips; grade III: 5 hips; grade IV: 3 hips). At last follow-up visit, the mean age of patients was 61.6 ± 21.3 months (range 30.8–141), and the mean acetabular index was 22.6° ± 5.6°; 67.3% of the hips had Severin type I radiographic criteria, 8.5% had type II, 23.6% had type III, and 0.6% had type IV.
Conclusions
Dynamic cast is an alternative to spica cast immobilization in DDH patients undergoing closed reduction. It has similar redislocation and AVN rates compared to standard spica cast immobilization, as reported by previous studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The aim of treatment for DDH is to obtain a stable and concentric reduction in the hip as early as possible and to maintain it during growth to acquire a normal hip at the time of skeletal maturity. At present, closed reduction (CR) and spica cast immobilization under general anesthesia are the gold standard of treatment for children older than 6 months of age and for those in whom the Pavlik harness has failed to provide a good reduction [1,2,3].
Although a variety of cast methods have been used to immobilize the hip [4,5,6,7], a spica cast with the patient in the “human position” is the most frequently used technique in clinical practice. Hips are placed in 90°–100°s of flexion and 45°–65° of abduction to achieve stable reduction without increasing the risk of redislocation or AVN. In particular, the reported rates of redislocation and AVN following spica cast immobilization in DDH patients undergoing closed reduction ranged from 1.7 to 17.4% [8,9,10] and from 0 to 67% [11,12,13], respectively.
At present, a casting technique called “dynamic cast immobilization” (DCI) is widely used in China [14, 15], including at our Institution. The DCI casting technique places the hips in abduction and flexion but does not immobilize the trunk because the lower extremities are fixed in abduction only through a connecting bar. The system allows the femoral epiphysis to move in flexion and extension within the acetabulum.
The purpose of this study is to describe the DCI technique of cast immobilization in DDH patients older than 6 months of age and to evaluate the radiographic outcome. In particular, the redislocation rate, the AVN rate as per the Kalamchi and McEwen criteria [16] and the final radiographic outcome as per the Severin radiographic criteria [17] were assessed.
Materials and methods
Following the approval of the Ethical Committee of Guangzhou Women and Children’s Medical Center (No. 2015020904), the records of 273 consecutive patients (328 hips) aged 6–24 months who were diagnosed with DDH and who were managed at our Institution by closed reduction and DCI technique during the period 2007–2014 were retrospectively reviewed.
Patients older than 24 months of age at the time of index procedure, patients with failed initial reduction, patients initially managed at a different institution, patients with missing or insufficient clinical and radiographic data and/or patients with less than 2 years follow-up were excluded from the analysis. In particular, patients with failed initial reduction were excluded as they underwent open reduction and spica cast immobilization.
A total of 159 patients (135 girls, 24 boys; 172 hips) met the inclusion criteria. All patients underwent regular clinical and radiographic follow-up. The mean age at the time of closed reduction and DCI immobilization was 15.6 ± 4.2 months (range 6–24). The mean follow-up time was 44.8 ± 20.3 months (range 24–128).
Dynamic cast immobilization technique
Prior to closed reduction, all patients underwent vertical skin traction of the lower extremities for 2–3 weeks. After 2 weeks of traction, patients undergo anterior–posterior pelvis radiograph. If the hip dislocation improved, closed reduction is performed. If no improvement, traction is continued for one additional week prior to closed reduction.
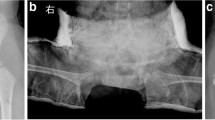
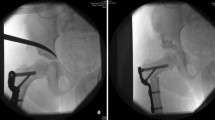
Closed reduction was performed under general anesthesia, and adductor tenotomy was performed if the adductor tightness was considered as a factor preventing reduction. Arthrography was performed in all patients to assess the most stable reduction by evaluating the hip joint at different flexion and abduction angles. The most stable reduction was maintained while placing the patient on a cast table. Cotton cast padding was then wound around the lower limbs, from the proximal thigh to the malleoli, with the knee flexed at 80°–90°. Additional padding was placed over the anterior superior iliac spine, the greater trochanter, the lateral and medial epicondyle of the femur, and the lateral and medial malleoli to protect all bony prominences. A polyester resin synthetic long leg cast was then applied to both lower extremities, with the knees flexed at 80°–90° and subsequently fixed in abduction through a connecting bar. The system allowed the femoral head to move in full flexion and partial extension within the acetabulum as the trunk was not included (Fig. 1).
After the DCI immobilization was completed, an antero-posterior (AP) radiograph of the pelvis was obtained to confirm reduction. In patients with clinically unstable reduction, magnetic resonance imaging was performed to confirm concentric reduction in the hip.
Overall, the DCI cast was kept in place for 12 weeks, and it was changed once after 6 weeks under general anesthesia. After DCI cast removal, a removable dynamic abduction brace was prescribed for 3–4 months of full-time use. After this period, the brace was switched to nighttime use for 3 additional months.
Follow-up and radiographic evaluation
All patients were followed for at least 2 years (range 2–10) after DCI cast removal, and AP pelvis radiographs in neutral and frog position of the hips were obtained at each follow-up visit. AP and frog position radiographs were assessed to evaluate the presence or absence of reduction (redislocation) and AVN of the femoral epiphysis. In particular, AVN of the femoral epiphysis was graded according to the criteria of Kalamchi and MacEwen [16]. Because type I AVN is considered a transient ischemia of the femoral head, which can recover completely [17, 18], we grouped type 1 AVN with the normal hip category.
At the final follow-up, acetabular index (AI) and Center–Edge–Angle (CEA) were assessed, radiographic results were classified according to the Severin criteria, and hips were graded from I to VI [17].
Statistical analysis
Data were expressed as frequencies and percentages, with means and standard deviations as appropriate. Statistical analysis was carried out using Student’s t test, and statistical significance was established at p < 0.05.
Results
A total of 159 patients (135 girls, 24 boys) and 172 hips (60 right, 86 left, 13 bilateral) met the inclusion criteria. The mean age at the time of closed reduction and DCI immobilization was 15.6 ± 4.2 months (range 6–24) (Fig. 2). Overall, 154 out of 159 patients (96.8%) had adductor tenotomy at the time of closed reduction. The mean follow-up was 44.8 ± 20.3 months (range 24–128). Overall, 66 hips (38.3%) were graded as Tönnis grade II dislocation, 98 (57%) as Tönnis grade III dislocation and 8 (4.7%) as Tönnis grade IV dislocation.
Redislocation rate
The overall redislocation rate after initial concentric reduction was 4.1% (7/172); all 7 patients had adductor tenotomy at the time of the initial closed reduction. The mean age of this patients group was 17.9 ± 4.5 months (range 11.5–24), and it did not differ significantly from the age of patients with stable reduction (15.6 ± 4.2 months; range 6–22.5; p > 0.05). All 7 of these hips were Tönnis grade III dislocations.
Of these 7 patients, 3 were lost to follow-up 1 year after index procedure, and 4 did undergo open reduction (Pemberton’s osteotomy and proximal femoral shortening osteotomy, 3 cases; Salter’s osteotomy and proximal femoral shortening osteotomy, 1 case).
AVN rate
The overall AVN rate of the femoral epiphysis was 14.5%. Sixteen hips (9.7%) had grade II AVN, 5 hips (3%) had grade III AVN, and 3 hips (1.8%) had grade IV AVN. No AVN was observed on the contralateral hip (Table 1).
AI and CEA
At last follow-up visit, the mean AI was 22.6° ± 5.6° (range 10–37.2), and the mean CEA was 20.5 ± 8.4 (range 2.2–41).
Severin criteria
Severin criteria were assessed in all hips without redislocation (165/172). At last follow-up visit, 67.3% of hips (111/165) were graded as Severin type I, 8.5% (14/165) as type II, 23.6% (39/165) as type III and 0.6% (1/165) as type IV (Tables 2, 3) (Fig. 3).
Complications
Of the 159 patients treated with the above-mentioned technique, 76 patients (47.8%) developed skin breaks secondary to skin traction. The skin healed in all patients by the time of cast change (6 weeks after index procedure); no skin infections were recorded.
During cast treatment, 25 patients (15.7%) had skin breaks, and 3 of them developed more severe skin infections that required debridement and antibiotic treatment. All patients recovered within 4 weeks after the cast removal.
Discussion
The purpose of this study was to evaluate the radiographic outcome in DDH patients undergoing closed reduction and the DCI technique. Our results show that the reported technique is not contraindicated for the treatment of DDH patients aged 6–24 months who require closed reduction and cast immobilization. In particular, the DCI technique has similar redislocation (4.1% in our series) and AVN rates (14.5% in our series) compared to spica cast immobilization, as reported by other investigators [13, 19, 20] (Tables 4, 5). Moreover, our results highlight a similar Severin grade distribution compared to previous studies.
The reported rate of Severin grade I and II hips following closed reduction and spica cast immobilization ranges from 62 to 93.6% [15, 19, 21,22,23,24,25,26,27] (Table 3). Kaneko et al. [21] reviewed 67 patients with DDH (75 hips) treated by closed reduction and spica cast immobilization. They reported that 82.7% of the hips were rated as Severin grade I or II and 7.3% as Severin grade III. In a similar work, Aksoy et al. [22] reported a series of 200 hips undergoing closed reduction and spica cast immobilization for DDH. They found that 76% of hips were rated as Severin grade I or II. We found similar results as in our series; 75.8% of the hips treated with the reported technique were rated as Severin grade I or II at the last follow-up visit (Tables 2, 3).
AVN is still the main concern following the treatment of DDH by closed reduction and cast immobilization. The reported rate of AVN ranges from 0 to 67% [11, 12, 20, 28,29,30,31,32,33,34,35,36]. The AVN rates reported by different authors are listed in Table 4, and only three studies included a large number of cases. In the studies of Herold et al. (450 hips) [28], Gregosiewicz et al. (1211 hips) [29] and Kruczynski et al. (823 hips) [30], the reported incidences of AVN were 12, 21, and 14%, respectively, and the mean AVN rate of these studies was 17%. This is similar to the 14.5% incidence of AVN found in our series of 172 hips. There are still controversies regarding the risk factors for AVN. Gregosiewicz et al. [29] showed that age less than 6 months, severe acetabular dysplasia, use of an abduction apparatus and frog-leg position after reduction are risk factors associated with AVN following closed reduction and cast immobilization. However, Brougham et al. [31] found no significant correlation of the AVN rate with gender, side, age at reduction, duration of traction, degree of abduction in traction, adductor tenotomy or the use of a previous abduction device. Furthermore, Sibiński et al. [32] reported that the degree of dislocation and age at the onset of treatment were the risk factors for AVN, but the presence of the ossific nucleus, use of traction, use of an abduction apparatus and lateralization were not. Although we did not directly compare the AVN rate between our cast method (dynamic frog position) with spica cast in this study, the AVN rate was comparable to those reported in most previous studies [13, 19, 20, 28,29,30] (Tables 1, 4).
The DCI casting technique places the hips in abduction and flexion but does not immobilize the trunk, allowing the femoral epiphysis to move in flexion and extension within the acetabulum. The technique requires clinicians to check the hip under fluoroscopic control for the most stable reduction by assessing the hip joint at different flexion and abduction angles. The most stable reduction is maintained while performing the DCI. The reported technique is significantly different from previously reported frog position cast immobilization, as the trunk is not included, and both hips are free to move in flexion and extension, thus avoiding continuous compression stress on the femoral head. Li et al. [37] evaluated the effect of dynamic hip immobilization on chondrocyte and blood perfusion in the femoral head in 152 rabbits immobilized in three different positions, i.e., “human position,” “frog-leg position” and “dynamic leg” position. They found that “dynamic leg” immobilization caused relatively less chondrocyte apoptosis and disturbance to the femoral head perfusion than other forms of immobilization, and they hypothesized that it could be useful for reducing AVN following closed treatment of DDH. Other advantages are that patients seem more comfortable and that caregivers can take care of the casted children more easily.
Redislocation is another concern in patients undergoing closed reduction and cast immobilization. In our series, 7/172 hips (4.1%) redislocated during cast treatment and required open reduction. The redislocation rate found in our series is similar to those reported in previous studies, with redislocation rates between 0.7 and 3.8% [8,9,10, 35, 38,39,40] (Table 5).
It should be noted that there are some limitations in the present study. First, this is a retrospective study. Second, although all patients underwent DCI, we did not compare it to spica cast immobilization. As it, it is still hard to definitively say which method is better to cast DDH patients. However, our study shows that the DCI technique is not inferior to spica cast immobilization when compared to previously published studies. Third, the overall number of patients treated by DCI is limited. However, the present series is the largest to date assessing the outcome of DDH patients managed by DCI.
In conclusion, a low rate of redislocation and good radiographic results can be achieved by means of closed reduction and the DCI technique in DDH patients treated between 6 and 24 months of age. Moreover, the reported technique does not significantly increase the rate of AVN of the femoral epiphysis in this patient population when compared with the AVN rates reported in previous studies. Overall, patients are more comfortable, and caregivers can take care of the casted children more easily.
References
Cooper AP, Doddabasappa SN, Mulpuri K (2014) Evidence-based management of developmental dysplasia of the hip. Orthop Clin N Am 45(3):341–354. https://doi.org/10.1016/j.ocl.2014.03.005
Kotlarsky P, Haber R, Bialik V, Eidelman M (2015) Developmental dysplasia of the hip: What has changed in the last 20 years? World J Orthop 6(11):886–901. https://doi.org/10.5312/wjo.v6.i11.886
Noordin S, Umer M, Hafeez K, Nawaz H (2010) Developmental dysplasia of the hip. Orthop Rev 2(2):e19. https://doi.org/10.4081/or.2010.e19
Tennant SJ, Eastwood DM, Calder P, Hashemi-Nejad A, Catterall A (2016) A protocol for the use of closed reduction in children with developmental dysplasia of the hip incorporating open psoas and adductor releases and a short-leg cast: mid-term outcomes in 113 hips. Bone Jt J 98-b(11):1548–1553. https://doi.org/10.1302/0301-620x.98b11.36606
Leeprakobboon D, Kaewpornsawan K, Eamsobhana P (2014) Four-point molding: a new cast molding technique for closed reduction treatment of developmental dysplasia of the hip. J Med Assoc Thail 97(Suppl 9):S29–S33
Keren Y, Sadia S, Eidelman M (2011) The use of the lotus position during spica cast application for the treatment of developmental dysplasia of the hip: a technical note. Orthopedics 34(9):708–709. https://doi.org/10.3928/01477447-20110714-12
Fettweis E (1990) Treatment of congenital dislocation of the hip in a squatting position, Fettweis method. Acta Orthop Belgica 56(1):155–165
Yamada N, Maeda S, Fujii G, Kita A, Funayama K, Kokubun S (2003) Closed reduction of developmental dislocation of the hip by prolonged traction. J Bone Jt Surg Br 85(8):1173–1177
Pospischill R, Weninger J, Ganger R, Altenhuber J, Grill F (2012) Does open reduction of the developmental dislocated hip increase the risk of osteonecrosis? Clin Orthop Relat Res 470(1):250–260. https://doi.org/10.1007/s11999-011-1929-4
Sankar WN, Gornitzky AL, Clarke NM, Herrera-Soto JA, Kelley SP, Matheney T, Mulpuri K, Schaeffer EK, Upasani VV, Williams N, Price CT (2016) Closed reduction for developmental dysplasia of the hip: early-term results from a prospective, multicenter cohort. J Pediatr Orthop. https://doi.org/10.1097/bpo.0000000000000895
Crego CH Jr, Schwartzmann JR (1948) Follow-up study of the early treatment of congenital dislocation of the hip. J Bone Jt Surg Am 30a(2):428–442
Esteve R (1960) Congenital dislocation of the hip: a review and assessment of results of treatment with special reference to frame reduction as compared with manipulative reduction. J Bone Jt Surg Br 42-b:253–263
Tiderius C, Jaramillo D, Connolly S, Griffey M, Rodriguez DP, Kasser JR, Millis MB, Zurakowski D, Kim YJ (2009) Post-closed reduction perfusion magnetic resonance imaging as a predictor of avascular necrosis in developmental hip dysplasia: a preliminary report. J Pediatr Orthop 29(1):14–20. https://doi.org/10.1097/BPO.0b013e3181926c40
Bao Q, Bao S (1996) Long-term investigation of closed reduction of congenital hip dislocation in children with modified frog-leg cast. Zhonghua wai ke za zhi [Chinese journal of surgery] 34(4):212–214
Cai Z, Li L, Zhang L, Ji S, Zhao Q (2017) Dynamic long leg casting fixation for treating 12- to 18-month-old infants with developmental dysplasia of the hip. J Int Med Res 45(1):272–281. https://doi.org/10.1177/0300060516675110
Kalamchi A, MacEwen GD (1980) Avascular necrosis following treatment of congenital dislocation of the hip. J Bone Jt Surg Am 62(6):876–888
Severin E (1941) Contribution to the knowledge of congenital dislocation of the hip joint: late results of closed reduction and arthrographic studies of recent cases. Acta Chir Scand 84(Suppl 63):53–54
Gage JR, Winter RB (1972) Avascular necrosis of the capital femoral epiphysis as a complication of closed reduction of congenital dislocation of the hip: a critical review of twenty years’ experience at Gillette Children’s Hospital. J Bone Jt Surg Am 54(2):373–388
Terjesen T, Halvorsen V (2007) Long-term results after closed reduction of latedetected hip dislocation: 60 patients followed up to skeletal maturity. Acta Orthop 78(2):236–246. https://doi.org/10.1080/17453670710013744
Murray T, Cooperman DR, Thompson GH, Ballock T (2007) Closed reduction for treatment of development dysplasia of the hip in children. Am J Orthop (Belle Mead, NJ) 36(2):82–84
Kaneko H, Kitoh H, Mishima K, Matsushita M, Ishiguro N (2013) Long-term outcome of gradual reduction using overhead traction for developmental dysplasia of the hip over 6 months of age. J Pediatr Orthop 33(6):628–634. https://doi.org/10.1097/BPO.0b013e31829b2d8b
Aksoy MC, Ozkoc G, Alanay A, Yazici M, Ozdemir N, Surat A (2002) Treatment of developmental dysplasia of the hip before walking: results of closed reduction and immobilization in hip spica cast. Turk J Pediatr 44(2):122–127
Rampal V, Sabourin M, Erdeneshoo E, Koureas G, Seringe R, Wicart P (2008) Closed reduction with traction for developmental dysplasia of the hip in children aged between one and five years. J Bone Jt Surg Br 90(7):858–863. https://doi.org/10.1302/0301-620x.90b7.20041
Kitoh H, Kitakoji T, Katoh M, Ishiguro N (2006) Prediction of acetabular development after closed reduction by overhead traction in developmental dysplasia of the hip. J Orthop Sci 11(5):473–477. https://doi.org/10.1007/s00776-006-1049-2
Gogus MT, Aksoy MC, Atay OA, Acaroglu RE, Surat A (1997) Treatment of congenital dislocation of the hip. Results of closed reduction and immobilization in the hip spica cast. Turk J Pediatr 39(4):499–503
Sibinski M, Murnaghan C, Synder M (2006) The value of preliminary overhead traction in the closed management of DDH. Int Orthop 30(4):268–271. https://doi.org/10.1007/s00264-006-0080-4
Shin CH, Yoo WJ, Park MS, Kim JH, Choi IH, Cho TJ (2016) Acetabular remodeling and role of osteotomy after closed reduction of developmental dysplasia of the hip. J Bone Jt Surg Am 98(11):952–957. https://doi.org/10.2106/jbjs.15.00992
Herold HZ (1980) Avascular necrosis of the femoral head in congenital dislocation of the hip. Isr J Med Sci 16(4):295–300
Gregosiewicz A, Wosko I (1988) Risk factors of avascular necrosis in the treatment of congenital dislocation of the hip. J Pediatr Orthop 8(1):17–19
Kruczynski J (1996) Avascular necrosis of the proximal femur in developmental dislocation of the hip. Incidence, risk factors, sequelae and MR imaging for diagnosis and prognosis. Acta Orthop Scand Suppl 268:1–48
Brougham DI, Broughton NS, Cole WG, Menelaus MB (1990) Avascular necrosis following closed reduction of congenital dislocation of the hip: review of influencing factors and long-term follow-up. J Bone Jt Surg Br 72(4):557–562
Sibinski M, Synder M, Domzalski M, Grzegorzewski A (2004) Risk factors for avascular necrosis after closed hip reduction in developmental dysplasia of the hip. Ortop Traumatol Rehabil 6(1):60–66
Burgos J, Gonzalez-Herranz P, Ocete G, Rapariz JM (1995) Secondary avascular necrosis after treatment for congenital dislocation of the hip. J Pediatr Orthop B 4(2):188–193
Schur MD, Lee C, Arkader A, Catalano A, Choi PD (2016) Risk factors for avascular necrosis after closed reduction for developmental dysplasia of the hip. J Child Orthop 10(3):185–192. https://doi.org/10.1007/s11832-016-0743-7
Barakat AS, Zein AB, Arafa AS, Azab MA, Reda W, Hegazy MM, Al Barbary HM, Kaddah MA (2017) Closed reduction with or without adductor tenotomy for developmental dysplasia of the hip presenting at walking age. Curr Orthop Pract 28(2):195–199. https://doi.org/10.1097/bco.0000000000000478
Sucato DJ, De La Rocha A, Lau K, Ramo BA (2017) Overhead Bryant’s traction does not improve the success of closed reduction or limit AVN in developmental dysplasia of the hip. J Pediatr Orthop 37(2):e108–e113. https://doi.org/10.1097/bpo.0000000000000747
Li LY, Zhang LJ, Jia JY, Zhao Q, Wang EB, Li QW (2013) Does dynamic immobilization reduce chondrocyte apoptosis and disturbance to the femoral head perfusion? Int J Clin Exp Pathol 6(2):212–223
Bhaskar A, Desai H, Jain G (2016) Risk factors for early redislocation after primary treatment of developmental dysplasia of the hip: Is there a protective influence of the ossific nucleus? Indian J Orthop 50(5):479–485. https://doi.org/10.4103/0019-5413.189610
Kim NH, Park BM, Lee HM (1990) Congenital dislocation of the hip: a long-term follow-up in Korea. Yonsei Med J 31(2):134–143. https://doi.org/10.3349/ymj.1990.31.2.134
Quinn RH, Renshaw TS, DeLuca PA (1994) Preliminary traction in the treatment of developmental dislocation of the hip. J Pediatr Orthop 14(5):636–642
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Informed consent
No patients were involved. This is a retrospective study of patient’s data, and an IRB approval was obtained.
Rights and permissions
About this article
Cite this article
Li, Y., Zhou, Q., Liu, Y. et al. Closed reduction and dynamic cast immobilization in patients with developmental dysplasia of the hip between 6 and 24 months of age. Eur J Orthop Surg Traumatol 29, 51–57 (2019). https://doi.org/10.1007/s00590-018-2289-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-018-2289-5