Abstract
Purpose
Spinopelvic sagittal alignment is crucial for assessing balance and determining treatment efficacy in patients with adult spinal deformity (ASD). Only a limited number of reports have addressed spinopelvic parameters and lumbosacral transitional vertebrae (LSTV). Our primary objective was to study spinopelvic sagittal parameter changes in patients with LSTV. A secondary objective was to investigate clinical symptoms and quality of life (QOL) in patients with LSTV.
Methods
In this study, we investigated 371 participants who had undergone medical check-ups for the spine. LSTV was evaluated using Castellvi’s classification, and patients were divided into LSTV+ (type II-IV, L5 vertebra articulated or fused with the sacrum) and LSTV- groups. After propensity score matching for demographic data, we analyzed spinopelvic parameters, sacroiliac joint degeneration, clinical symptoms, and QOL for these two participant groups. Oswestry Disability Index (ODI) scores and EQ-5D (EuroQol 5 dimensions) indices were compared between the two groups.
Results
Forty-four patients each were analyzed in the LSTV + and LSTV- groups. The LSTV + group had significantly greater pelvic incidence (52.1 ± 11.2 vs. 47.8 ± 10.0 degrees, P = 0.031) and shorter pelvic thickness (10.2 ± 0.9 vs. 10.7 ± 0.8 cm, P = 0.018) compared to the LSTV- group. The “Sitting” domain of ODI (1.1 ± 0.9 vs. 0.6 ± 0.7, P = 0.011) and “Pain/Discomfort” domain of EQ-5D (2.0 ± 0.8 vs. 1.6 ± 0.7, P = 0.005) were larger in the LSTV + group.
Conclusion
There was a robust association between LSTV and pelvic sagittal parameters. Clinical symptoms also differed between the two groups in some domains. Surgeons should be aware of the relationship between LSTV assessment, radiographic parameters and clinical symptoms.
Level of evidence
3.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The complementary and compensatory chain of skeletal and vertebral alignments stretching from the head to the lower extremities are recognized as an essential mechanism for standing and normal life activities and are associated with quality-of-life (QOL) in patients with adult spinal deformity (ASD) [1, 2]. Spinopelvic alignment observed on spinal sagittal plane radiographs has been reported in several studies to be associated with surgical outcomes, including QOL in patients with ASD [3, 4]. Of these spinopelvic sagittal alignments, the pelvic parameters reflect patient-specific pelvic morphology and are crucial in assessing the compensatory status of changes in the spinal column above the pelvis, including lumbar lordosis (LL) [5, 6].
On the other hand, the anatomy of the lumbosacral transition region and the pelvis has many individual variations [7,8,9]. Lumbosacral transitional vertebrae (LSTV) are found in 6–30% of the population, and this anatomic variance alters the mechanical loading of the lumbopelvic junction that is known to be associated with clinical symptoms, including low back pain, and disc degeneration progression [10, 11]. However, despite the relatively high prevalence of LSTV, there is limited and under-reported research on radiographic spinopelvic sagittal alignment parameters in patients with LSTV. We hypothesize that the anatomical features that form the basis of radiological outcomes in the treatment of patients with LSTV are not being analyzed and used to treat and manage ASD.
The aim of this study was to investigate the general impact of LSTV on spinopelvic sagittal alignment and its clinical outcomes. We focused on the anatomic variations in the lumbosacral transition region and hypothesized that patients presenting with a type of LSTV where the L5 vertebra and sacrum are articulated or fused have characteristic pelvic sagittal parameters that differ from those without LSTV and have degenerative changes in the adjacent sacroiliac joints and worsening clinical symptoms. We believed that clarifying the relationship between the anatomical variations of the lumbosacral transition region, the spinopelvic sagittal alignment parameters, and the clinical symptoms would be beneficial in understanding the etiology of the symptoms of ASD patients with LSTV and planning a surgical strategy for the treatment of patients with ASD.
The primary objective of the present study was to determine the changes in the radiological spinopelvic sagittal parameters of patients with LSTV. Additionally, a secondary objective was to investigate the degenerative changes in the sacroiliac joints, the clinical symptoms, and QOL in patients with LSTV.
Materials and methods
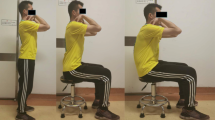
In this study, we focused on the anatomic variations in the lumbosacral transition region and hypothesized that patients presenting with a type of LSTV where the L5 vertebra and sacrum are articulated or fused have characteristic pelvic sagittal parameters that differ from those without LSTV and have degenerative changes in the adjacent sacroiliac joints with worsening clinical symptoms. We included 371 participants in this study who had undergone spinal check-ups at a single institution. The participants in this study were individuals who opted for a spinal radiographic examination as part of their health check-up. Participants with a history of treatment for spinal disorders, a history of spinal surgery, or those with a subnormal number of vertebrae, i.e., other than 12 thoracic or 5 lumbar vertebrae, were excluded from the study. Participants underwent full-body radiographs with a “hands-on-cheek” posture. Clinical symptoms and QOL measurements were recorded using a questionnaire. This study was approved by the local Institutional Review Board (IRB Approval Number 2022-012 [0478]). Informed consent was waived because of the retrospective nature of the study and the analysis used anonymous clinical data.
Anatomical evaluation of the lumbosacral transition region
The lumbosacral transition region in frontal radiographs was evaluated using Castellvi’s classification [12] with participants showing either no anatomical abnormality (where the observed anatomy does not fit Castellvi’s classification) or displaying Castellvi’s type I anatomy being classified as belonging to the LSTV- group (Fig. 1). Participants presenting with Castellvi type II, III, and IV anatomies, displaying either an articulation between the L5 transverse process and ala of the sacrum or a bony union of the L5 posterior component with the sacrum, were classified as belonging to the LSTV + group. After these two groups were adjusted for age, height, and body weight using propensity score matching, the spinopelvic sagittal radiographic parameters, sacroiliac joint degeneration, clinical symptoms, and QOL scores of their participants were compared and analyzed.
Evaluation of radiographic parameters and sacroiliac joint degeneration
Radiographic parameters were evaluated using sagittal whole-body radiographs acquired with a scanning X-ray imaging system (EOS Imaging, Paris, France) and included thoracic kyphosis (TK: T1–12), lumbar lordosis (LL), pelvic incidence (PI), pelvic tilt (PT), sagittal pelvic thickness (SPT: distance between the center of the sacral endplate and the femoral heads), sagittal vertical axis (SVA), sacrofemoral angle (SFA: reflex angle between the center of the sacral endplate and the center of the femoral heads and the distal femoral axis), and knee flexion (KF: angle between the femoral axis and the tibial axis) (Fig. 2). Sacroiliac joint degeneration (SID) was also evaluated using the New York (NY) classification [13] to assess frontal radiographs. Participants with an NY classification grade 2 or higher assessment were categorized as SID+. To investigate interobserver error in the classification of LSTV and SID, radiographic image classification was repeated independently by two surgeons with 15 and 5 years of clinical experience: disagreements in the grading were resolved by mutual consultation. The kappa coefficient was calculated to test the interobserver reliability of the measurements.
Assessment of clinical symptoms and quality of life measurements
Clinical symptoms were assessed using the Oswestry disability index (ODI), and the ODI score was calculated by dividing the sum of the scores obtained for the 9 items by the full score, excluding the “sexual activity” item that had a significantly low response rate. QOL was also assessed using the European QOL 5 Dimensions 5 Levels (EQ-5D-5 L) questionnaire; the Japanese version of the EQ-5D index was calculated. [14]. Sub-items within the ODI and the EQ-5D indices were also compared between the two groups.
Statistical methods
All values are expressed as means ± standard deviation. The Mann-Whitney U test was used to determine significant differences between the two groups for continuous variables and ordered variables. Fisher’s exact test was used for univariate analysis including categorical variables. The result of the kappa coefficient measures of reliability were classified as very good (0.61–0.8) or reached near-perfect agreement (0.81-1.0) according to the criteria previously reported [15]. Statistical significance was set at P < 0.05. The IBM SPSS Statistics version 23.0 software (IBM Corp., Armonk, NY) was used for statistical analyses.
Results
Of the 371 participants, three showed a lack of data and 31 had abnormal vertebral counts (e.g., four or six lumbar vertebrae), and were excluded from the study. Of the remaining 337 cases, 46 (13.6%) were classified as Castellvi type II, III, or IV and were assigned to the LSTV + group. After adjusting for age, height, and body weight by propensity score matching, the LSTV + and the LSTV- groups with 44 patients each were analyzed. A flow chart of the analysis is shown in Fig. 3. There was no demographic difference between the two groups, and SID was found in 9 (20.5%) cases in the LSTV- group and 17 (38.6%) in the LSTV + group (P = 0.101). Demographic data comparing the LSTV- and LSTV + groups are shown in Table 1. The interobserver reliability of the radiographic classification was 0.818 and 0.649 for LSTV + indicating Castellvi type II, III, and IV and for SID indicating NY classification grade 2 or higher, respectively (Table 2).
A comparison of radiographic parameters between the LSTV- and LSTV + groups showed that PI was 47.8 ± 10.0 and 52.1 ± 11.2 (degrees, P = 0.031), and SPT was 10.7 ± 0.8 and 10.2 ± 0.9 (cm, P = 0.018), respectively. There were no significant differences in other vertebro-pelvic sagittal parameters (Table 3).
In the comparison of clinical symptoms and QOL measurements, there were no significant differences between the two groups in the ODI and EQ-5D indices. A comparison of the domains of each questionnaire showed that the LSTV − and LSTV + groups were 0.6 ± 0.7 and 1.1 ± 0.9 (P = 0.011) for the domain of 5 “Sitting” on the ODI, and 1.6 ± 0.7 and 2.0 ± 0.8 (P = 0.005) for the domain of “Pain/Discomfort” on the EQ-5D, respectively (Table 4).
Discussion
The present study showed that adults with LSTV have a specific anatomical and radiographic pelvic profile and present with a worsening of the “Sitting” domain of the ODI and the “Pain/Discomfort” domain of the EQ-5D questionnaires. This is the first study to detail the relationship between LSTV, radiographic spinopelvic sagittal alignment, and clinical symptoms in an adult cohort.
The radiographic profile of the spinopelvic sagittal plane morphology is an important factor in determining the treatment strategy pertaining to spine surgery for ASD that is aimed at restoring a harmonious spinopelvic alignment in the sagittal plane [3, 4]. There are many variations in human pelvic anatomy and pelvic sagittal parameters are specific to each person. It has been reported that pelvic radiographic sagittal parameters are associated with the progression of lumbar degeneration [7,8,9]. Haffer et al. [16] investigated the relationship between the number of abnormalities of lumbar vertebrae and pelvic sagittal parameters, and reported that patients with four or six lumbar vertebrae had a greater PI in both groups, compared to a control group with five lumbar vertebrae. Although only patients with five vertebrae were included in our present analysis, the PI for the LSTV + group tended to be greater than that in the LSTV- group. SPT is an anatomical and functional parameter known to correlate with PI [17, 18]. Jean [18] observed that this parameter, along with a ratio involving the length of the upper plate of S1, reflects the lever arm of action of spinopelvic muscles and ligaments and describing the ability of a subject to compensate a sagittal imbalance. Based on the results of this study, simultaneous evaluation of LSTV would be necessary during SPT measurement. Although the change of the PI between the two groups, the magnitude of change is very small, and the clinical relevance of changes in the PI with LSTV might be negligible. On the other hand, these result suggests that patients with LSTV have a different pelvic anatomy, at least radiographically, including the sacral endplate that is a landmark in determining the PI value, and is not simply a location for various measurement points involved in determining the parameters. Hsieh et al. [19] showed that patients with LSTV have lower L5/S disc height that is independent of degeneration. This, combined with the present study where the PI was greater in patients with LSTV, suggests that a greater restoration of lumbar lordosis at cranial levels to the LSTV level is warranted, commensurate with the greater PI in surgical treatment for ASD. Aihara et al. [11] demonstrated that the iliolumbar ligaments at the level above the transitional vertebrae were thinner and weaker than those without LSTV. Several studies have shown that the proximal adjacent levels to a transitional vertebra were more degenerative than that of the lumbosacral transitional region [20, 21]. These findings suggest that patients with LSTV have different functional lumbosacral boundaries and load distributions. Based on these findings, a surgical strategy that does not extend the lower end of fixation to the sacral pelvis, such as a floating fixation, may be clinically applicable more in cases with LSTV than in cases without LSTV. We believe that evaluation of the LSTV is essential in determining a surgical strategy for corrective fixation of ASD involving the lumbosacral region.
The pathology of LSTV and its clinical manifestations have been discussed in previous studes, with the “Bertolotti syndrome” reported to occur mainly in young patients with low back pain [10, 22, 23]. Earlier reports using the LSTV classification have reported that Castellvi types II, III, and IV, in which the fifth lumbar vertebra is in contact with the sacrum, have a high rate of lumbar degeneration and symptoms [8, 24]. In the present study, there was no difference between the two groups in ODI scores and EQ-5D indices, but there was a worsening in the “Sitting” domain of ODI and “Pain/Discomfort” domain of EQ-5D in the LSTV + group comprised of Castellvi types II, III, and IV. Avimadje et al. [23] reported the effects of intra-articular steroid injections in patients with an enlarged L5 transverse process articulating with the sacrum or iliac crest. Several studies using bone scintigraphy have demonstrated inflammation of transverse-sacral articulation in symptomatic LSTV [25, 26]. Anatomic variations in the lumbosacral transition region alter the mechanical loading on the superior intervertebral discs and surrounding joints, including the sacroiliac joints [9,10,11]. We hypothesized that adult patients with LSTV would have decreased mobility between the fifth lumbar vertebra and sacrum [10], and increased mechanical stress on the sacroiliac joints [9], resulting in increased degeneration of the sacroiliac joints adjacent to the lumbosacral transition region compared to those without LSTV. However, the results of this study showed no statistical difference in the progression of degeneration of sacroiliac joints between the two groups. This result may be related to the relatively low interobserver reliability of SID classification determinations and lack of statistical power in this study. Future studies, including evaluation with CT, MRI, and bone scintigraphy, are needed to clarify the relationship between LSTV, sacroiliac joint degeneration, and clinical symptoms [26, 27].
This study has several limitations. First, this study used Castellvi’s classification for LSTV that is inherently a classification of congenital anatomical features and may be inappropriate for adults, where age-related changes cannot be excluded. Also, the method used to evaluate LSTV on frontal radiographs may have overestimated the original anatomical features of the patient, and this may explain the relatively high prevalence of LSTV in the present study compared to previous reports using computed tomography to diagnose LSTV [16]. Understanding these limitations underscores the need for future studies utilizing other modalities that can provide a more detailed structural assessment of LSTV. Furthermore, anatomical variations in the thoracolumbar transition and lumbosacral transition areas, other than LSTV, were not included as variables in this study. This limitation may result in overlooking potential anatomical variations and their impact on spinal alignment. Another limitation is the lack of detailed data on the etiology of the clinical symptoms presented in this study. Data on the association of clinical symptoms with local treatments, such as sacroiliac joint injection and orthotics, are needed to clarify this issue [23]. Although the findings that patients with LSTV showed statistically significant changes in the ODI and EQ-5D indices, whether these changes are clinically relevant remains unclear. Despite these limitations, the present study showed that adults with LSTV tended to have specific clinical symptoms and functional impairments.
Conclusions
We evaluated radiological whole-body sagittal parameters, sacroiliac joint degeneration, clinical symptoms, and QOL scores in patients with LSTV using Castellvi’s classification in adult spinal checkup subjects. For radiographical parameters, PI was significantly greater in the LSTV + group. The prevalence of SID with an NY classification grade of 2 or higher, the ODI score and EQ-5D index did not differ between the two groups, but the “Sitting” domain of ODI and “Pain/Discomfort” domain of EQ-5D were larger in the LSTV + group than in the LSTV - group. When evaluating the clinical presentation and radiologic alignment of patients with ASD, surgeons should be aware of the association with LSTV.
Data availability
Data will be made available on request.
References
Barrey C, Roussouly P, Perrin G, Le Huec JC (2011) Sagittal balance disorders in severe degenerative spine. Can we identify the compensatory mechanisms? Eur Spine J 20 Suppl 5:626–633. https://doi.org/10.1007/s00586-011-1930-3
Ouchida J, Nakashima H, Kanemura T et al (2023) The age-specific normative values of standing whole-body sagittal alignment parameters in healthy adults: based on international multicenter data. Eur Spine J 32:562–570. https://doi.org/10.1007/s00586-022-07445-y
Takemoto M, Boissière L, Vital JM et al (2017) Are sagittal spinopelvic radiographic parameters significantly associated with quality of life of adult spinal deformity patients? Multivariate linear regression analyses for pre-operative and short-term post-operative health-related quality of life. Eur Spine J 26:2176–2186. https://doi.org/10.1007/s00586-016-4872-y
Ames CP, Smith JS, Scheer JK et al (2012) Impact of spinopelvic alignment on decision making in deformity surgery in adults: a review. J Neurosurg Spine 16:547–564. https://doi.org/10.3171/2012.2.SPINE11320
Legaye J, Duval-Beaupère G, Hecquet J, Marty C (1998) Pelvic incidence: a fundamental pelvic parameter for three-dimensional regulation of spinal sagittal curves. Eur Spine J 7:99–103. https://doi.org/10.1007/s005860050038
Le Huec JC, Aunoble S, Philippe L, Nicolas P (2011) Pelvic parameters: origin and significance. Eur Spine J 20 Suppl 5:564–571. https://doi.org/10.1007/s00586-011-1940-1
Strube P, Pumberger M, Sonnow L et al (2018) Association between lumbar spinal degeneration and anatomic pelvic parameters. Clin Spine Surg 31:263–267. https://doi.org/10.1097/BSD.0000000000000660
Hanhivaara J, Määttä JH, Niinimäki J, Nevalainen MT (2020) Lumbosacral transitional vertebrae are associated with lumbar degeneration: retrospective evaluation of 3855 consecutive abdominal CT scans. Eur Radiol 30:3409–3416. https://doi.org/10.1007/s00330-020-06691-2
Mahato NK (2010) Morphological traits in sacra associated with complete and partial lumbarization of first sacral segment. Spine J 10:910–915. https://doi.org/10.1016/j.spinee.2010.07.392
Luoma K, Vehmas T, Raininko R, Luukkonen R, Riihimäki H (2004) Lumbosacral transitional vertebra: relation to disc degeneration and low back pain. Spine 29:200–205. https://doi.org/10.1097/01.BRS.0000107223.02346.A8
Aihara T, Takahashi K, Ogasawara A et al (2005) Intervertebral disc degeneration associated with lumbosacral transitional vertebrae: a clinical and anatomical study. J Bone Joint Surg Br 87:687–691. https://doi.org/10.1302/0301-620X.87B5.15727
Castellvi AE, Goldstein LA, Chan DP (1984) Lumbosacral transitional vertebrae and their relationship with lumbar extradural defects. Spine 9:493–495. https://doi.org/10.1097/00007632-198407000-00014
van der Linden S, Valkenburg HA, Cats A (1984) Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum 27:361–368. https://doi.org/10.1002/art.1780270401
te Group Eq. 5D-5L index value calculator for MAC.:https:. http://euroqol.org/wp-content/uploads/2018/02/EQ-5D-5L_Crosswalk_Index_Value_Calculator_MAC.xls
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174. https://doi.org/10.2307/2529310
Haffer H, Becker L, Putzier M et al (2021) Changes of fixed anatomical spinopelvic parameter in patients with lumbosacral transitional vertebrae: a matched pair analysis. Diagnostics (Basel) 11:59. https://doi.org/10.3390/diagnostics11010059
Hasegawa K, Hatsushikano S, Le Huec JC et al (2022) Pelvic thickness, sex, ethnicity, and age affect pelvic incidence in healthy volunteers of multi-ethnic alignment normative study (MEANS) database. Eur Spine J 31:1421–1430. https://doi.org/10.1007/s00586-022-07134-w
Jean L (2013) The sagittal pelvic thickness: a determining parameter for the regulation of the sagittal spinopelvic balance. International Scholarly Research Notices 2013
Hsieh CY, Vanderford JD, Moreau SR, Prong T (2000) Lumbosacral transitional segments: classification, prevalence, and effect on disk height. J Manipulative Physiol Ther 23:483–489. https://doi.org/10.1067/mmt.2000.108817
Vergauwen S, Parizel PM, van Breusegem L et al (1997) Distribution and incidence of degenerative spine changes in patients with a lumbo-sacral transitional vertebra. Eur Spine J 6:168–172. https://doi.org/10.1007/BF01301431
Konin GP, Walz DM (2010) Lumbosacral transitional vertebrae: classification, imaging findings, and clinical relevance. AJNR Am J Neuroradiol 31:1778–1786. https://doi.org/10.3174/ajnr.A2036
Quinlan JF, Duke D, Eustace S (2006) Bertolotti’s syndrome. A cause of back pain in young people. J Bone Joint Surg Br 88:1183–1186. https://doi.org/10.1302/0301-620X.88B9.17211
Avimadje M, Goupille P, Jeannou J, Gouthière C, Valat JP (1999) Can an anomalous lumbo-sacral or lumbo-iliac articulation cause low back pain? A retrospective study of 12 cases. Rev Rhum Engl Ed 66:35–39
Tang M, Yang XF, Yang SW et al (2014) Lumbosacral transitional vertebra in a population-based study of 5860 individuals: prevalence and relationship to low back pain. Eur J Radiol 83:1679–1682. https://doi.org/10.1016/j.ejrad.2014.05.036
Connolly LP, d’Hemecourt PA, Connolly SA et al (2003) Skeletal scintigraphy of young patients with low-back pain and a lumbosacral transitional vertebra. J Nucl Med 44:909–914
Pekindil G, Sarikaya A, Pekindil Y, Gültekin A, Kokino S (2004) Lumbosacral transitional vertebral articulation: evaluation by planar and SPECT bone scintigraphy. Nucl Med Commun 25:29–37. https://doi.org/10.1097/00006231-200401000-00005
Hanhivaara J, Määttä JH, Karppinen J, Niinimäki J, Nevalainen MT (2022) The association of lumbosacral transitional vertebrae with low back pain and lumbar degenerative findings in MRI: a large cohort study. Spine 47:153–162. https://doi.org/10.1097/BRS.0000000000004244
Funding
No funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Author information
Authors and Affiliations
Contributions
J.O. and H.N. designed the study. J.O. carried out the data collection and analysis. J.O. and H.N. wrote the manuscript. T.K., M.T., S.I., N.S., H.T., K.M., H.O., K.O., and S.I. supervised the entire study and reviewed the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the local Institutional Review Board. Informed consent was waived because of the retrospective nature of the study and the analysis used anonymous clinical data.
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ouchida, J., Nakashima, H., Kanemura, T. et al. Analysis of spinopelvic parameters in adult patients with lumbosacral transitional vertebrae. Eur Spine J 33, 2952–2959 (2024). https://doi.org/10.1007/s00586-024-08378-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-024-08378-4