Abstract
Introduction
Posterior fusion of traumatic odontoid fractures by C1 lateral mass and C2 isthmic screws (modified Harms–Goel technique) is a viable alternative to transarticular screw fixation due to its universal applicability. This retrospective study reports on a series of 127 patients.
Material and methods
Our clinical database was screened for patients with fractures of the upper cervical spine incorporating a C2 fracture, operated on between 2007 and 2015. Patients were included if fused by internal fixation via C1 lateral mass screws, C2 isthmic screws in freehand technique under lateral fluoroscopy. Screw placement was controlled postoperatively by computed tomography and rated using the Gertzbein & Robbins classification. Surgery-related complications, consecutive treatment, revision surgeries and duration of surgeries were registered.
Results
In total, 127 patients were identified with altogether 572 screws. Correct screw positions of grade A and B according to Gertzbein & Robbins were achieved in a total of 539 (94.2%) screws (grade A: 453 (79.2%); grade B: 86 (15%)), grade C screw malpositions noted in 21 (3.7%), grade D in 10 (1.7%) and grade E in 2 (0.3%) screws. Vertebral artery canal breaches occurred in 29 screws (5.1%), with vertebral artery occlusion in 4 patients. Coiling of injured vertebral artery had to be performed in one patient. None of these patients suffered clinically apparent cerebrovascular complications. Revision surgery was performed in 8 patients (6%).
Conclusion
Posterior fixation of atlantoaxial fractures by C1 lateral mass and C2 isthmic screws with fluoroscopy without navigation is a safe and feasible method but not free of risk of vertebral artery injuries.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Atlantoaxial instability is a frequent finding in spine care units. Underlying pathologies for this condition are versatile like trauma, rheumatoid arthritis, neoplasms or spinal deformities. Nevertheless, the most common cause is traumatic odontoid fractures of the elderly alone or in combination with C1 fractures. The best treatment of these fractures is a highly discussed matter of debate [1, 2]. There is an increasing evidence favoring surgical over conservative treatment for odontoid fractures in the elderly [3, 4]. Surgical treatment of unstable fractures consists of C1–C2 fixation by implantation of an internal fixation construct. Anterior odontoid screw fixation as a motion-preserving technique is less suitable, if not contraindicated in elderly patients [5, 6]. So posterior transarticular screw fixation was the mainstay of C1–C2 fixation techniques [7, 8], but various techniques have been described since [9, 10]. The well-known technique by Goel [11, 12] with modifications by Harms [13] of C1 lateral mass and C2 isthmic screws is an alternative to transarticular screw fixation. The advantage of this technique over the transarticular screw technique is its universal applicability in all types of odontoid fractures, irrespective of the fracture line, underlying fracture dislocation or comminution and a reduced risk of vascular complications due to lesion of the vertebral artery [14,15,16,17]. Even though this risk can be reduced with the latter technique under fluoroscopic guidance, the risk is not completely avoidable [18]. Various studies tried to improve the safety of this procedure. Image-guided navigation techniques have evolved and showed promising results [19,20,21,22,23]. Nevertheless, up to now freehand screw implantation under fluoroscopic guidance represents the clinical gold standard.
The results of the first 35 patients of our series operated on in this technique have been reported previously [24]. This study is a continuation of this series of patients with upper cervical spine instabilities including C2 fractures and gives account of the results as an update to the previously reported data.
Material and methods
The clinical database of our neurosurgical department was screened retrospectively for patients treated surgically for upper cervical spine instabilities including C2 fractures of any type by posterior C1–C2 (-C3) fixation using a screw-rod construct between 2007 and 2015. Postoperative imaging of the construct by computed tomography had to be available to evaluate screw positioning.
Demographic data of the patients were recorded as well as the type of odontoid fracture according to Anderson & D’Alonso and the type of accompanying injuries of the upper cervical spine.
All surgeries were performed by experienced spine surgeons under fluoroscopic control in lateral projection using an open midline posterior approach. No spinal navigation was used.
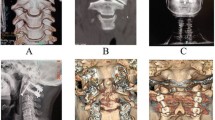
Screw positioning was assessed on postoperative computed tomography scans and rated using the Gertzbein & Robbins classification scale as the most frequently cited classification in the literature to ensure good comparability of study data. This scale defines a grade A screw placement as 0 mm extraosseous position (example in Fig. 1), grade B as ≤ 2 mm extraosseous position, grade C as ≤ 4 mm extraosseous position (example in Fig. 2), grade D as ≤ 6 mm extraosseous position and grade E as > 6 mm extraosseous position (example in Fig. 3). All malpositioned screws with contact to the vertebral artery canal and all cases of resulting vascular complications were recorded. Consecutive surgical revisions or endovascular treatments due to screw malpositioning were registered.
Results
In total, 127 patients were identified, 49 males and 78 females. Median age was 78 ± 17.6 years (range 7 to 99 years). Ninety-two patients (72%) had Anderson & D’Alonso type 2 fractures, nine (7%) type 3 and 7 (6%) atypical odontoid fractures. Nineteen (15%) patients had combined fractures of C1 and C2 (type 2 plus Jefferson fracture in two cases, type 3 with unilateral hangman’s fracture in 7 cases and atypical combined fractures in 10 cases) (Table 1).
Altogether 572 screws were inserted. In total, 253 screws were implanted in C1, 243 in C2 and 76 in C3. In 9 cases, the construct was extended beyond C3 due to the type of injury. Screw accuracy was only rated for the vertebrae C1 through C3.
A correct screw positioning on postoperative computed tomography scans according to Gertzbein & Robbins grades A and B was achieved in 94.2% (453/79.2% grade A; 86/15.0% grade B), and 21 screws (3.7%) were rated grade C, 10 screws (1.7%) grade D and two grade E positions (0.3%) (Table 2).
Good accuracy (G&R grades A and B) for C1 lateral mass screws was achieved in 94.0%, for C2 isthmic screws in 95.4% and for C3 lateral mass screws in 90.8% (Table 3).
In total, 15 (45%) of the malpositioned screws were located in C1. Here the majority of screws (11 of 15/73%) were placed too medially, thus breaching the medial wall of the C1 lateral mass. Three screws were placed too laterally, compromising the vertebral artery canal. One of these and five of the medialized screws were also placed too cranially with contact to the atlantooccipital joint.
In total, 11 misplaced screws were located in C2. All directions of misplacement were seen. A relevant compromise of the C3 nerve root was seen in two cases. In one case, both C2 screws broke out of the isthmus postoperatively due to a lateralized placement.
Seven screws were misplaced in level C3. These were placed too laterally or reached the vertebral artery canal anteriorly with the tip of the screw without compromising it.
No new neurologic deficit or radicular pain was seen due to the screw misplacements.
Breaching of the vertebral artery canal was seen in 29 screws (5.1%; 15 in C1; 14 in C2) in 25 patients (19.7%). An actual vertebral artery lesion on the consequently performed computed tomography angiography was seen in four patients (3.0%), three in C1 and one in C2. One of these patients needed endovascular coiling of the injured and not completely obliterated artery (0.7% of patients). After occlusion of the artery, the misplaced C1 screw was revised due to contact with the internal carotid artery (Fig. 4). There were no ischemic cerebral strokes or other clinically apparent vascular complications due to the vertebral artery injuries in these patients.
The revision rate overall was 7.0% (9 patients). Five patients were revised due to the misplacement of screws in C1 (≈ 4%). Three patients were revised due to screw misplacement in C2 (≈ 2%). One patient (≈ 1%) had to be revised due to insufficient repositioning of the fragmented bone and persisting CSF fistula from a traumatic dural tear.
Mean OR time of the 83 patients who received C1–C2 fixation only was 100 ± 32 min (range 37–210).
Discussion
We report on a large series of posterior C1–C2 fixations by C1 lateral mass and C2 isthmic screws in traumatic atlantoaxial instability. Studies reporting accuracy and complications of this technique have already been published, but with rather small patient cohorts including parts of our cohort [5, 17, 24,25,26,27,28]. The results of this series are well in line with previously demonstrated data [29] and might improve the body of evidence on this topic as well as improve comparability of the various techniques for atlantoaxial fusion.
In our study, we found a high accuracy of freehand screw placement for C1 lateral mass and C2 isthmic screws (94.2% accuracy according to Gertzbein & Robbins grades A and B). Injuries of the vertebral artery were rare but still posed a relevant complication. Nevertheless, no patient suffered from clinically apparent or relevant stroke or vertebral artery hemorrhage. However, endovascular treatment of a vertebral artery lesion and revision surgery due to vascular reasons was necessary in one patient only.
Transarticular fixation of the C1–C2 complex for treatment of instability was introduced by Magerl in 1978. This technique bears a risk of vertebral artery lesions which is reported to be as high as 4.1% [16]. As the Magerl technique is challenging and not universally applicable to certain fracture types, alternatives were looked for. One alternative is the modified Harms and Goel technique: a C1 lateral mass—C2 isthmic screw construct. A meta-analysis comparing both techniques could show a significantly reduced risk of neurovascular complications for the modified Goel–Harms technique of 2.0% versus 4.1% for vertebral artery lesion [30].
Most misplaced screws in C1 in our study were implanted too medially. This may be due to the apprehension of injuring the vertebral artery on the one hand and unintended slippage of the drill on the slightly convex C1 lateral mass with a tendency to slip medially since a slight convergence angle of 10° for lateral mass screw placement is aimed for during screw placement. The fact of four respective lesions in our cohort shows that the risk of laceration of the vertebral artery is not to be underestimated. To avoid lesioning of the vertebral artery meticulous preparation and visualization and maintenance of the entry point during drilling in the C1 lateral mass is essential.
The fact of a lower accuracy of C3 lateral mass screws (90.8%) than C2 isthmic screws (95.4) may be surprising. This might be an overrepresentation of misplaced screws due to the significantly lower amount of C3 screws, 76 versus 243. But also establishing the correct trajectory in the C2 isthmus is easier, especially in the medio-lateral orientation than in C3 where the necessary diverging screw trajectory can pose a problem during screw placement.
Various studies report on the results of posterior stabilization of the atlantoaxial complex using different image-guided navigation techniques [21,22,23, 31,32,33,34,35]. Reported screw accuracies, as far as mentioned, range from 90.5% (for C1 lateral mass screws) [34] to 92.4% [21] and 97.9% [35] to 98.5% [31] and 100% [22, 23] which are in the range of or better than our results. However, the reported mean OR times of these series were up to three times as long with mean durations of 130 [33], 161.7 [31], 165 [35], 177.8 [34], 188.7 [23], 225 [22] and 306 min [32] compared to our series with a mean length of surgery of only 100 min without the use of navigation. Also in these studies patient numbers are rather small, so larger volume studies are warranted.
The majority of patients treated for odontoid fractures or other instabilities of the atlantoaxial complex are geriatric patients. In our series the mean age was 78 years. This patient collective is known to be prone to an increased perioperative morbidity and mortality. The risk of perioperative complications, especially surgical site infections, but also the need of blood transfusions, the length of hospital stay and the rate of medical complications such as pneumonia increases exponentially with increasing lengths of surgery and increasing age [36]. Shorter OR times and minimization of intraoperative blood loss may therefore play a crucial role in reducing the rate of perioperative complications and improving clinical outcome and should therefore be aimed for. Undoubtedly, spinal navigation can enhance accuracy and safety of screw placement, but these benefits must be weighed against the risk of longer OR times and its related complications. Whether navigation can substantially improve accuracy and safety and abate the risk of revision surgeries and surgery-related complications and consecutively improve clinical outcome and whether these advantages outweigh the disadvantages related to substantially longer OR times needs to be proven in future prospective randomized trials. Right now the use of a spinal navigation seems to significantly prolong the duration of surgery without improving clinical outcome compared to freehand surgery. However, we need to keep in mind that navigation for this procedure is still in its infancy which will hopefully improve with time.
Conclusion
Posterior fusion of atlantoaxial instabilities by C1 lateral mass and C2 isthmic screws is a safe and feasible treatment option. The risks of screw misplacement and vascular lesions are rare but not to be underestimated. In our opinion the freehand technique still has its place in times of neuronavigation due to its universal applicability and significantly shorter OR times for posterior C1–C2 fixation. Future studies comparing freehand C1–C2 posterior fixation with navigated screw placement with regard to morbidity and mortality and clinical outcome are needed.
References
Denaro V, Papalia R, Di Martino A, Denaro L, Maffulli N (2011) The best surgical treatment for type II fractures of the dens is still controversial. Clin Orthop Relat Res 469(3):742–750. https://doi.org/10.1007/s11999-010-1677-x
Harrop JS (2013) Type II odontoid fractures: what to do? World Neurosurg 80(3–4):313–314. https://doi.org/10.1016/j.wneu.2012.04.011
Chapman J, Smith JS, Kopjar B, Vaccaro AR, Arnold P, Shaffrey CI, Fehlings MG (2013) The AOSpine North America geriatric odontoid fracture mortality study: a retrospective review of mortality outcomes for operative versus nonoperative treatment of 322 patients with long-term follow-up. Spine 38(13):1098–1104. https://doi.org/10.1097/BRS.0b013e318286f0cf
Vaccaro AR, Kepler CK, Kopjar B, Chapman J, Shaffrey C, Arnold P, Gokaslan Z, Brodke D, France J, Dekutoski M, Sasso R, Yoon ST, Bono C, Harrop J, Fehlings MG (2013) Functional and quality-of-life outcomes in geriatric patients with type-II dens fracture. J Bone Joint Surg Am 95(8):729–735. https://doi.org/10.2106/JBJS.K.01636
Ryang YM, Torok E, Janssen I, Reinke A, Buchmann N, Gempt J, Ringel F, Meyer B (2016) Early morbidity and mortality in 50 very elderly patients after posterior atlantoaxial fusion for traumatic odontoid fractures. World Neurosurg 87:381–391. https://doi.org/10.1016/j.wneu.2015.12.026
Kaesmacher J, Schweizer C, Valentinitsch A, Baum T, Rienmuller A, Meyer B, Kirschke JS, Ryang YM (2017) Osteoporosis Is the most important risk factor for odontoid fractures in the elderly. J Bone Miner Res 32(7):1582–1588. https://doi.org/10.1002/jbmr.3120
Jeanneret B, Magerl F (1992) Primary posterior fusion C1/2 in odontoid fractures: indications, technique, and results of transarticular screw fixation. J Spinal Disord 5(4):464–475
Magerl F, Seemann P-S (1987) Stable posterior fusion of the atlas and axis by transarticular screw fixation. In: Cervical spine I. Springer, pp 322–327
Huang DG, Hao DJ, He BR, Wu QN, Liu TJ, Wang XD, Guo H, Fang XY (2015) Posterior atlantoaxial fixation: a review of all techniques. Spine J 15(10):2271–2281. https://doi.org/10.1016/j.spinee.2015.07.008
Steltzlen C, Lazennec JY, Catonne Y, Rousseau MA (2013) Unstable odontoid fracture: surgical strategy in a 22-case series, and literature review. Orthop Traumatol Surg Res 99(5):615–623. https://doi.org/10.1016/j.otsr.2013.02.007
Goel A, Laheri V (1994) Plate and screw fixation for atlanto-axial subluxation. Acta Neurochir (Wien) 129(1–2):47–53
Goel A, Desai KI, Muzumdar DP (2002) Atlantoaxial fixation using plate and screw method: a report of 160 treated patients. Neurosurgery 51(6):1351–1356
Harms J, Melcher RP (2001) Posterior C1–C2 fusion with polyaxial screw and rod fixation. Spine 26(22):2467–2471
Madawi A, Solanki G, Casey AT, Crockard HA (1997) Variation of the groove in the axis vertebra for the vertebral artery. Implications for instrumentation. J Bone Joint Surg Br 79(5):820–823
Madawi AA, Casey AT, Solanki GA, Tuite G, Veres R, Crockard HA (1997) Radiological and anatomical evaluation of the atlantoaxial transarticular screw fixation technique. J Neurosurg 86(6):961–968. https://doi.org/10.3171/jns.1997.86.6.0961
Wright NM, Lauryssen C (1998) Vertebral artery injury in C1–2 transarticular screw fixation: results of a survey of the AANS/CNS section on disorders of the spine and peripheral nerves. J Neurosurg 88(4):634–640
Gautschi OP, Payer M, Corniola MV, Smoll NR, Schaller K, Tessitore E (2014) Clinically relevant complications related to posterior atlanto-axial fixation in atlanto-axial instability and their management. Clin Neurol Neurosurg 123:131–135. https://doi.org/10.1016/j.clineuro.2014.05.020
Akinduro OO, Baum GR, Howard BM, Pradilla G, Grossberg JA, Rodts GE Jr, Ahmad FU (2016) Neurological outcomes following iatrogenic vascular injury during posterior atlanto-axial instrumentation. Clin Neurol Neurosurg 150:110–116. https://doi.org/10.1016/j.clineuro.2016.08.012
Kraus M, dem Berge S, Perl M, Krischak G, Weckbach S (2014) Accuracy of screw placement and radiation dose in navigated dorsal instrumentation of the cervical spine: a prospective cohort study. Int J Med Robot 10(2):223–229. https://doi.org/10.1002/rcs.1555
Scheufler KM, Franke J, Eckardt A, Dohmen H (2011) Accuracy of image-guided pedicle screw placement using intraoperative computed tomography-based navigation with automated referencing, part I: cervicothoracic spine. Neurosurgery 69(4):782–795. https://doi.org/10.1227/NEU.0b013e318222ae16
Hecht N, Kamphuis M, Czabanka M, Hamm B, Konig S, Woitzik J, Synowitz M, Vajkoczy P (2016) Accuracy and workflow of navigated spinal instrumentation with the mobile AIRO((R)) CT scanner. Eur Spine J 25(3):716–723. https://doi.org/10.1007/s00586-015-3814-4
Kantelhardt SR, Keric N, Giese A (2012) Management of C2 fractures using Iso-C(3D) guidance: a single institution's experience. Acta Neurochir (Wien) 154(10):1781–1787. https://doi.org/10.1007/s00701-012-1443-9
Smith JD, Jack MM, Harn NR, Bertsch JR, Arnold PM (2016) Screw placement accuracy and outcomes following O-Arm-Navigated atlantoaxial fusion: a feasibility study. Global Spine J 6(4):344–349. https://doi.org/10.1055/s-0035-1563723
Ringel F, Reinke A, Stuer C, Meyer B, Stoffel M (2012) Posterior C1–2 fusion with C1 lateral mass and C2 isthmic screws: accuracy of screw position, alignment and patient outcome. Acta Neurochir (Wien) 154(2):305–312. https://doi.org/10.1007/s00701-011-1224-x
Payer M, Luzi M, Tessitore E (2009) Posterior atlanto-axial fixation with polyaxial C1 lateral mass screws and C2 pars screws. Acta Neurochir (Wien) 151(3):223–229. https://doi.org/10.1007/s00701-009-0198-4
Tessitore E, Bartoli A, Schaller K, Payer M (2011) Accuracy of freehand fluoroscopy-guided placement of C1 lateral mass and C2 isthmic screws in atlanto-axial instability. Acta Neurochir (Wien) 153(7):1417–1425. https://doi.org/10.1007/s00701-011-1039-9
Nitising A, Jetjumnong C, Tisavipat N, Nantaaree S (2011) Posterior C1–C2 fusion using C1 lateral mass and C2 pars screw with rod fixation: techniques and outcomes. J Med Assoc Thai 94(7):794–800
Bourdillon P, Perrin G, Lucas F, Debarge R, Barrey C (2014) C1–C2 stabilization by Harms arthrodesis: indications, technique, complications and outcomes in a prospective 26-case series. Orthop Traumatol Surg Res 100(2):221–227. https://doi.org/10.1016/j.otsr.2013.09.019
Elliott RE, Tanweer O, Boah A, Morsi A, Ma T, Smith ML, Frempong-Boadu A (2014) Atlantoaxial fusion with screw-rod constructs: meta-analysis and review of literature. World Neurosurg 81(2):411–421. https://doi.org/10.1016/j.wneu.2012.03.013
Elliott RE, Tanweer O, Boah A, Morsi A, Ma T, Frempong-Boadu A, Smith ML (2014) Outcome comparison of atlantoaxial fusion with transarticular screws and screw-rod constructs: meta-analysis and review of literature. J Spinal Disord Tech 27(1):11–28. https://doi.org/10.1097/BSD.0b013e318277da19
Costa F, Ortolina A, Attuati L, Cardia A, Tomei M, Riva M, Balzarini L, Fornari M (2015) Management of C1–2 traumatic fractures using an intraoperative 3D imaging-based navigation system. Journal of neurosurgery Spine 22(2):128–133. https://doi.org/10.3171/2014.10.SPINE14122
Jeon SW, Jeong JH, Choi GH, Moon SM, Hwang HS, Choi SK (2012) Clinical outcome of posterior fixation of the C1 lateral mass and C2 pedicle by polyaxial screw and rod. Clin Neurol Neurosurg 114(6):539–544. https://doi.org/10.1016/j.clineuro.2011.11.001
Yang YL, Zhou DS, He JL (2013) Comparison of isocentric C-arm 3-dimensional navigation and conventional fluoroscopy for C1 lateral mass and C2 pedicle screw placement for atlantoaxial instability. J Spinal Disord Tech 26(3):127–134. https://doi.org/10.1097/BSD.0b013e31823d36b6
Bredow J, Oppermann J, Kraus B, Schiller P, Schiffer G, Sobottke R, Eysel P, Koy T (2015) The accuracy of 3D fluoroscopy-navigated screw insertion in the upper and subaxial cervical spine. Eur Spine J 24(12):2967–2976. https://doi.org/10.1007/s00586-015-3974-2
Czabanka M, Haemmerli J, Hecht N, Foehre B, Arden K, Liebig T, Woitzik J, Vajkoczy P (2017) Spinal navigation for posterior instrumentation of C1–2 instability using a mobile intraoperative CT scanner. J Neurosurg Spine 27(3):268–275. https://doi.org/10.3171/2017.1.SPINE16859
Akins PT, Harris J, Alvarez JL, Chen Y, Paxton EW, Bernbeck J, Guppy KH (2015) Risk factors associated with 30-day readmissions after instrumented spine surgery in 14,939 patients: 30-day readmissions after instrumented spine surgery. Spine (Phila Pa 1976) 40(13):1022–1032. https://doi.org/10.1097/BRS.0000000000000916
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors state that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Buchmann, N., Schweizer, C., Kirschke, J.S. et al. C1–C2 posterior screw fixation in atlantoaxial fractures revisited: technical update based on 127 cases. Eur Spine J 29, 1036–1042 (2020). https://doi.org/10.1007/s00586-019-06244-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06244-2