Abstract
Purpose
The choice of distal fusion level in adolescent idiopathic scoliosis (AIS) patients with major thoracolumbar or lumbar (TL/L) curves (Lenke type 3C, 5C, or 6C) remains debatable. One of the most controversial issues involves stopping the distal fusion at L3, which might result in an increased risk of decompensation but save more mobile spinal segments. The purpose of this study was to evaluate and compare the clinical and radiological outcomes of corrective surgery for AIS with major TL/L curves according to the distal fusion level.
Methods
229 AIS patients with Lenke type 3C, 5C, or 6C curves that underwent corrective surgery were included. Patients were grouped according to distal fusion level, either L3 (group A) or L4 (group B), and followed up for over 2 years. Group A was further divided into lower end vertebra (LEV) and last touching vertebra (LTV). The SRS-22 score was used to assess clinical outcomes. All radiological parameters were assessed pre- and postoperatively by standing anteroposterior whole-spine radiographs. Clinical and radiological parameters were compared between the groups.
Results
Postoperative decompensation was found in 4.6 % (9/197) of group A patients and 9.3 % (3/32) of group B patients. This difference was not statistically significant (P = 0.258). No difference was found in the clinical and radiological parameters between the two groups either pre- or postoperatively. Subgroup analysis showed that the scoliosis correction rate and postoperative apical vertebral translation were lower in cases with an LEV ≤ L4 or LTV = L5 when the fusion stopped at L3 distally. The adjacent disc wedge angle was aggravated postoperatively in these cases, although this did not reach statistical significance.
Conclusions
There is no difference in the radiological and clinical outcomes in AIS according to the distal fusion level. Major TL/L curve correction in AIS may be sufficient distally at L3 in cases with an LEV ≥ L3 and LTV ≥ L4. However, stopping fusion at L3 requires caution in LEV ≤ L4 or LTV = L5 patients, as this correction rate might be suboptimal and causes a possible progression of the adjacent disc wedge angle.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The selection of distal fusion level in adolescent idiopathic scoliosis (AIS) patients with large thoracolumbar/lumbar (TL/L) curves has previously been addressed [1–3]. Saving the lumbar mobile segments during scoliosis surgery might preserve lumbar function and reduce the risk of back pain, although this hypothesis lacks definitive evidence [4, 5]. However, the risk of decompensation or unsatisfactory correction may theoretically be increased by shortening the distal fusion level.
Following the introduction of powerful instrumentation systems, several groups have attempted to reduce the distal fusion level in idiopathic scoliosis with major TL/L curves [2, 3, 6]. Traction X-ray has been used to reduce the distal fusion level in cases with Lenke 3C or 6C curves [6]. Another study reported no benefit to extending the fusion beyond the lower end vertebra [3]. There has been no definitive conclusion concerning the distal fusion level in AIS with major TL/L curves. The sufficiency of stopping the distal fusion at L3 remains debatable.
The aim of this study was to investigate the clinical and radiological benefits of extending distal fusion to L4 in the correction of AIS with major TL/L.
Materials and methods
This study included 229 patients who underwent corrective surgery for AIS with major TL/L curves (Lenke type 3C, 5C, or 6C) between January 2006 and December 2011 at our hospital. Patients with other types of scoliosis, such as neuromuscular scoliosis or syndrome-related scoliosis, were excluded. Demographic data, including sex, age, height, weight, and body mass index (BMI), were obtained from the electronic medical records. Radiological data were obtained from whole-spine anteroposterior (AP) and lateral radiographs using the picture archiving communication system at our institution. Plain radiographs were obtained with the patients in an upright, standing position in both views and with arms folded forward in lateral views. Whole-spine AP radiographs were preoperatively obtained in the prone and active bending positions. Pre- and postoperative SRS-22 scores were used to assess clinical outcomes.
All patients underwent posterior surgery using the rod derotation method with pedicle screw fixations by single surgeon (C.S.L.) [7]. The patients were divided by the distal fusion level, L3 (group A) and L4 (group B). Group A was divided into two subgroups by lower end vertebra (LEV) and last touching vertebra (LTV). Patients were regularly followed up at 1, 6, and 12 months post-surgery and annually thereafter. This study was approved by the Institutional Review Board of our institution, which waived the requirement for informed consent due to the retrospective nature of the analysis.
Radiological assessment
The scoliosis angle was assessed by the Cobb’s angles of the major TL/L curves pre- and postoperatively. The coronal plane trunk shift was defined as the distance between the C7 plumb line and the central sacral vertical line. Coronal plane decompensation was defined as a trunk shift over 20 mm. The shoulder height difference was defined as the difference between the horizontal lines passing both tips of the acromion. The apical vertebral translation (AVT) was defined as the distance between the central sacral vertical line and the center of the apical vertebrae. The apical vertebral rotation (AVR) was defined by Pedriolle’s method [8]. The pelvic obliquity was defined as the angle between the line linking the highest point of both iliac crests and the horizontal line. The LIV+1 tilt was defined as the slanted angle of the upper endplate of the vertebra just inferior to the lowest instrumented vertebra (LIV). In addition, bone maturity was assessed by the degree of ossification in iliac crest (Risser sign) [9]. Thoracic kyphosis was assessed by the angle between upper endplate of T1 and lower endplate of T12. Lumbar lordosis was assessed by the angle between upper endplate of L1 and S1. Postoperative radiological parameters were measured at most recent follow-up. Radiological parameters were measured by the orthopedic surgeon (J.H.C.) who had 5-year experience as a spine surgeon, and did not relate with the subjects of this study. All radiological measurements are summarized in Fig. 1.
Statistical analysis
Demographic data were compared between the two groups using the Student’s t test or the Chi square test. Pre- and postoperative radiological parameters between groups were compared using the Student’s t test. Chi square test was used to compare the frequency of postoperative decompensation. SRS-22 scores were compared pre- and postoperatively between both groups. Postoperative changes in clinical and radiological parameters were compared using a paired t test. Statistical analyses were performed using the Statistical Package for Social Sciences (version 21.0, SPSS Inc., Chicago, IL) with P values <0.05 considered statistically significant.
Results
Demographic data and curve types
Of the 229 patients in our current series, 31 were male and 198 were female. The mean age was 15.6 ± 4.0 years. The mean height of the patients was 159.6 ± 7.5 cm, and the mean weight was 50.5 ± 9.8 kg. The mean BMI of the patients was 19.8 ± 2.9 kg/m2. The mean follow-up period was 44.9 ± 14.8 months. The distribution of specific Lenke types is depicted in Fig. 2. There was no significant difference between group A and group B with respect to the demographic data or curve types (Table 1). The most frequently selected upper instrumented vertebra was T4 (107 cases, 46.7 %), followed by T5 (55 cases, 24.0 %), T3 (20 cases, 8.7 %), and T9 (13 cases, 5.7 %). The distribution of upper instrumented vertebra was similar between both the groups (P = 0.131).
Radiological outcomes
The mean scoliosis angle of the major curves was 57.5 ± 11.6°. The mean angle decreased to 42.3 ± 12.4° in the prone position, 29.0 ± 14.2° in the bending position, and 13.6 ± 8.7° postoperatively (P < 0.001). The mean correction rate after surgery was 76.8 ± 14.9 %. The preoperative trunk shift, shoulder height difference, and apical vertebral translation were 6.6 ± 15.5 , 7.9 ± 10.8, and 43.2 ± 13.4 mm, respectively. Thoracic kyphosis improved from 25.4 to 28.8° postoperatively (P < 0.001). However, lumbar lordosis did not show any difference. Postoperative changes in these radiological parameters are described in Table 2.
Preoperative radiological parameters were compared between our two study groups (Table 3). In group B, more immaturity was shown; however, this was not statistically significant (P = 0.160). Although the scoliotic curve was more severe in group B, this was not statistically significant (P = 0.064). The trunk shift, shoulder height difference, thoracic kyphosis, lumbar lordosis and apical vertebral translation did not differ between the two groups preoperatively. However, the proportion of LEV ≤ L4 or LTV = L5 cases was significantly higher in group B.
Postoperative decompensation was found in 12 cases. The frequency of decompensation was lower in group A (4.6 %, 9/197) than in group B (9.3 %, 3/32), although this difference was not statistically significant (P = 0.258). Revision surgery was not performed in either study group until the final follow-up. Radiological parameters did not differ postoperatively except the number of fusion level (Table 4). Figure 3 depicts a case of fusion to L3, and Fig. 4 illustrates a case of fusion to L4.
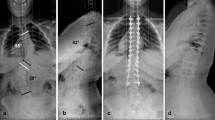
a, b Preoperative radiographs of a 12-year-old female patient diagnosed with Lenke type 3CN idiopathic scoliosis and a 63° thoracolumbar curve. c, d Postoperative (4 years) radiograph demonstrating maintenance of the coronal balance and shoulder balance of this patient following distal fusion to L3. (TK thoracic kyphosis; LL lumbar lordosis)
a, b Preoperative radiographs of a 12-year-old female patient diagnosed with Lenke type 3CN idiopathic scoliosis with a 60° thoracolumbar curve. c, d Postoperative (3 years) radiograph demonstrating maintenance of the coronal balance and shoulder balance of the patient following distal fusion to L4. (TK thoracic kyphosis; LL lumbar lordosis)
Subgroup analysis by LEV for the group A patients is summarized in Table 5. The correction rate of scoliotic curves was lower when LEV ≤ L4 (73.3 vs. 78.8 %). The trunk shift, decompensation, and LIV + 1 tilt were not different postoperatively. However, the degrees of AVT decreased less in the patients with LEV ≤ L4 postoperatively (34.3 vs. 59.8 %). Although the adjacent disc wedge angle was different between our two study groups, this difference was not statistically significant (P = 0.053).
The results of the subgroup analysis by LTV for group A were similar to the results for LEV (Table 6). Postoperative AVT changes were lower in LTV ≤ L5 cases (33.7 vs. 54.8 %). The LIV + 1 tilt differed pre- and postoperatively in both the groups (P < 0.001). However, the trunk shift and decompensation did not differ between our study groups.
Clinical outcomes
SRS-22 scores did not change between the pre- and postoperative periods (3.58 vs. 3.56, P = 0.956). However, function/activity domain scores significantly decreased between the pre- and postoperative periods (4.02 vs. 3.54, P = 0.036). The pain and mental health scores also decreased between the pre- and postoperative periods (3.97 vs. 3.75 and 3.65 vs. 3.62, respectively), although these differences were not statistically significant (P = 0.110 and P = 0.953, respectively). The self-image domain score significantly increased between the pre- and postoperative periods (2.87 vs. 3.35, P = 0.037). The satisfaction score also increased between the pre- and postoperative periods (3.03 vs. 3.53), although this difference was not statistically significant (P = 0.099).
The preoperative and final follow-up SRS-22 domain scores for groups A and B are presented in Table 7. No differences were found between the pre- and postoperative periods.
Discussion
The selection of the distal fusion level in AIS patients has been widely discussed. For Lenke type 1 curves in single thoracic idiopathic scoliosis, a neutral vertebra is important for selecting the distal fusion level [10]. Proper selection of the distal fusion level is important for preventing a distal adding-on phenomenon in single thoracic idiopathic scoliosis [11, 12]. However, selection of the distal fusion level in major TL/L curves is associated with the preservation of lumbar motion.
Cotrel-Dubousset instrumentation has been used to preserve distal motion segments in AIS patients [13]. However, distal fusion to L4 has been recommended even in cases that did not meet the specific requirements for this procedure [13]. Although Lenke classification can be used to systematically determine the fusion levels [14], fusion level selection varies widely among surgeons [15]. A favorable outcome was reported previously when the preoperative L3 crossed the mid-sacral line with a rotation of less than grade II in bending radiographs [1]. However, that study was limited by a small sample size, an arbitrary definition of unfavorable outcomes, and a lack of clinical outcomes. Another previous study also found no difference between distal fusion to L3 or L4 in terms of the subsequent quality of life of AIS patients [2]. However, that study included a heterogeneous group of curves (Lenke type 1A, 1C, 2C, and 4C). Although lumbar mobility and health-related quality of life were also reported as moderately correlated with the distal fusion level, the study in question was limited by its small sample size [16]. Our present study had the advantage of analyzing a much larger cohort of patients.
In our present analyses, there were no differences observed in the clinical and radiological outcomes between groups A and B at final follow-up, with the exception of LEV and LTV. A trend towards extending the fusion to L4 in cases where the LEV ≤ L4 or LTV = L5 was observed. In LEV ≤ L4 or LTV = L5 cases also, the degree of correction was lower when the fusion stopped at L3. In addition, the subjacent disc wedge angle was slightly higher in these patients, although this difference was not statistically significant. This observation might be indicative of early disc degeneration or an adding-on phenomenon. However, coronal decompensation and trunk shift did not differ by LEV or LTV. In cases of LEV ≥ L3 and LTV ≥ L4, fusion to L3 was sufficient. Based on our present findings, fusion to L3 might be cautiously considered in cases where a suboptimal correction rate is acceptable.
In our current study patients treated at an earlier stage, distal fusion to L4 was primarily performed. However, in many cases, distal fusion was stopped at L3 due to the numerous benefits of this approach. First, sacral slanting, which can stop distal fusion at L3, has been frequently observed in patients with AIS [17]. A trunk shift might be aggravated by extending the fusion to L4 [17]. Second, lumbosacral transitional vertebrae (LSTV) have been observed in one-eighth of AIS patients [18]. Due to the fusion of L5-S1 in LSTV, saving one lumbar segment is of critical importance. Third, early disc degeneration at the L5-S1 level is related to larger lumbar curves [18] indicating that the preservation of further disc levels is more important than previously thought.
In addition, two things based on the current study could support stopping distal fusion at L3. First, extending the fusion to L4 can cause decompensation because of fewer mobile levels to compensate. Second, whatever the LIV is, clinical outcomes are not affected.
There are a number of controversial issues that have made the decision-making process more complex in AIS. Selective thoracic fusion (STF) may be considered in Lenke type 3C curves and can save additional lumbar segments. Several studies have reported good radiological outcomes from STF in properly selected cases [19–21]. In addition, the direct vertebral rotation (DVR) method may minimize the distal fusion level, as it corrects rotational deformity more frequently than the rod derotation method [22]. However, we do not have experience with the DVR method in our own clinical settings. Furthermore, it remains unclear whether saving more lumbar segments leads to decreased back pain or increased functional activity [4, 5]. In a previous cadaveric study, intradiscal pressure was reported to be higher in the caudal adjacent disc level [23]. Furthermore, the degree of back pain was reported to be higher in patients with a fusion to L4 compared with a control group [24]. Hence, reduction of the distal fusion level should be attempted whenever possible. However, it was reported that proximal junctional angle increased if the location of LIV was above or equal to L3 after posterior selective TL/L curve fusion [25]. This demands caution to select distal fusion level.
This study had several limitations, mainly due to its retrospective nature. First, the sample size of the AIS patients fused to L4 was smaller than patients fused to L3. This was due to our preference of stopping the distal fusion at L3. Second, the selection criteria we used for the distal fusion level were not standardized. However, preoperative clinical and radiological parameters did not differ between our two study groups except LEV and LTV. Third, our follow-up period was relatively short, which might explain the lack of differences we observed between the two groups.
The strengths of our present study include its relatively large sample size and its focus on AIS patients with major TL/L curves. The clinical and radiological outcomes were similar regardless of the distal fusion level in our current AIS patient cohort. However, the correction rate was often suboptimal in cases of LEV ≤ L4 or LTV = L5 and the fusion was stopped distally at L3 in these patients.
In conclusion, stopping the distal fusion at L3 might be a good option for saving mobile lumbar segments in cases of idiopathic scoliosis with major TL/L curves where the LEV ≥ L3 and LTV ≥ L4. It is also a possible option in cases where the LEV ≤ L4 or LTV = L5. However, caution is required in selecting the distal fusion level in such cases, as the correction rate might be suboptimal, and there can be progression of the distal disc wedge angle. Further comparative, long-term follow-up studies are required to establish definitive guidelines for the selection of the distal fusion level when treating AIS.
References
Kim SS, Lim DJ, Kim JH, Kim JW, Um KS, Ahn SH, Suk SI (2014) Determination of the distal fusion level in the management of thoracolumbar and lumbar adolescent idiopathic scoliosis using pedicle screw instrumentation. Asian Spine J 8:804–812
Ding R, Liang J, Qiu G, Shen J, Li Z (2014) Evaluation of quality of life in adolescent idiopathic scoliosis with different distal fusion level: a comparison of L3 versus L4. J Spinal Disord Tech 27:E155–E161
Sun Z, Qiu G, Zhao Y, Wang Y, Zhang J, Shen J (2014) Lowest instrumented vertebrae selection for selective posterior fusion of moderate thoracolumbar/lumbar idiopathic scoliosis: lower-end vertebra or lower-end vertebra +1? Eur Spine J 23:1251–1257
Danielsson AJ, Romberg K, Nachemson AL (2006) Spinal range of motion, muscle endurance, and back pain and function at least 20 years after fusion or brace treatment for adolescent idiopathic scoliosis: a case-control study. Spine (Phila Pa 1976) 31:275–283
Danielsson AJ, Nachemson AL (2003) Back pain and function 23 years after fusion for adolescent idiopathic scoliosis: a case-control study-part II. Spine (Phila Pa 1976) 28:E373–E383
Hamzaoglu A, Ozturk C, Enercan M, Alanay A (2013) Traction X-ray under general anesthesia helps to save motion segment in treatment of Lenke type 3C and 6C curves. Spine J 13:845–852
Suk SI, Kim JH, Kim SS, Lim DJ (2012) Pedicle screw instrumentation in adolescent idiopathic scoliosis (AIS). Eur Spine J 21:13–22
Pedrille R, Vidal J (1985) Thoracic idiopathic scoliosis curve evolution and progress. Spine (Phila Pa 1976) 10:785–791
Risser JC (1958) The Iliac apophysis; an invaluable sign in the management of scoliosis. Clin Orthop 11:111–119
Suk SI, Lee SM, Chung ER, Kim JH, Kim WJ, Sohn HM (2003) Determination of distal fusion level with segmental pedicle screw fixation in single thoracic idiopathic scoliosis. Spine (Phila Pa 1976) 28:484–491
Lakhal W, Loret JE, de Bodman C, Fournier J, Bergerault F, de Courtivron B, Bonnard C (2014) The progression of lumbar curves in adolescent Lenke 1 scoliosis and the distal adding-on phenomenon. Orthop Traumatol Surg Res 100:S249–S254
Matsumoto M, Watanabe K, Hosogane N, Kawakami N, Tsuji T, Uno K, Suzuki T, Ito M, Yanagida H, Yamaguchi T, Minami S, Akazawa T (2013) Postoperative distal adding-on and related factors in Lenke type 1A curve. Spine (Phila Pa 1976) 38:737–744
Lenke LG, Bridwell KH, Baldus C, Blanke K, Schoenecker PL (1993) Ability of Cotrel-Dubousset instrumentation to preserve distal lumbar motion segments in adolescent idiopathic scoliosis. J Spinal Disord 6:339–350
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 83:1169–1181
Lenke LG, Betz RR, Haher TR, Lapp MA, Merola AA, Harms J, Shufflebarger HL (2001) Multisurgeon assessment of surgical decision-making in adolescent idiopathic scoliosis: curve classification, operative approach, and fusion levels. Spine (Phila Pa 1976) 26:2347–2353
Sanchez-Raya J, Bago J, Pellise F, Cuxart A, Villanueva C (2012) Does the lower instrumented vertebra have an effect on lumbar mobility, subjective perception of trunk flexibility, and quality of life in patients with idiopathic scoliosis treated by spinal fusion? J Spinal Disord Tech 25:437–442
Lee CS, Ha JK, Kim DG, Kim H, Hwang CJ, Lee DH, Cho JH (2015) The clinical importance of sacral slanting in patients with adolescent idiopathic scoliosis undergoing surgery. Spine J 15:834–840
Lee CS, Ha JK, Kim DG, Hwang CJ, Lee DH, Cho JH (2015) The clinical importance of lumbosacral transitional vertebra in patients with adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 40:E964–E970
Behensky H, Cole AA, Freeman BJ, Grevitt MP, Mehdian HS, Webb JK (2007) Fixed lumbar apical vertebral rotation predicts spinal decompensation in Lenke type 3C adolescent idiopathic scoliosis after selective posterior thoracic correction and fusion. Eur Spine J 16:1570–1578
Chang MS, Bridwell KH, Lenke LG, Cho W, Baldus C, Auerbach JD, Crawford CH 3rd, O’Shaughnessy BA (2010) Predicting the outcome of selective thoracic fusion in false double major lumbar “C” cases with five- to twenty-four-year follow-up. Spine (Phila Pa 1976) 35:2128–2133
Takahashi J, Newton PO, Ugrinow VL, Bastrom TP (2011) Selective thoracic fusion in adolescent idiopathic scoliosis: factors influencing the selection of the optimal lowest instrumented vertebra. Spine (Phila Pa 1976) 36:1131–1141
Lee SM, Suk SI, Chung ER (2004) Direct vertebral rotation: a new technique of three-dimensional deformity correction with segmental pedicle screw fixation in adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 29:343–349
Auerbach JD, Lonner BS, Errico TJ, Freeman A, Goerke D, Beaubien BP (2012) Quantification of intradiscal pressures below thoracolumbar spinal fusion constructs: is there evidence to support “saving a level”? Spine (Phila Pa 1976) 37:359–366
Bartie BJ, Lonstein JE, Winter RB (2009) Long-term follow-up of adolescent idiopathic scoliosis patients who had Harrington instrumentation and fusion to the lower lumbar vertebrae: is low back pain a problem? Spine (Phila Pa 1976) 34:E873–E878
Sun Z, Qiu G, Zhao Y, Guo S, Wang Y, Zhang J, Shen J (2015) Risk factors of proximal junctional angle increase after selective posterior thoracolumbar/lumbar fusion in patients with adolescent idiopathic scoliosis. Eur Spine J 24:290–297
Acknowledgments
This study was not supported by any kind of funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declared that there was no potential conflict of interest.
Rights and permissions
About this article
Cite this article
Lee, C.S., Ha, JK., Hwang, C.J. et al. Is it enough to stop distal fusion at L3 in adolescent idiopathic scoliosis with major thoracolumbar/lumbar curves?. Eur Spine J 25, 3256–3264 (2016). https://doi.org/10.1007/s00586-015-4373-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4373-4