Abstract
A 7-year-old Holstein-Friesian dairy cow that was culled because of traumatic motor dysfunction due to accidental falling down showed a variety of gross postmortem findings, such as fracture of the caudal vertebra, massive hemorrhage in the pelvic cavity, edematous swelling of the right sciatic nerve, and brown discoloration of the masseter muscle, tongue, cardiac muscle, diaphragmatic muscle, liver, adrenal cortex, and intestinal wall. Histopathologically, the discolored and some other internal organs/tissues exhibited varying degrees of intracellular deposition of lipofuscin granules. A small number of eosinophilic proteinaceous granules, along with lipofuscin granules, were found in the smooth muscle fibers of the intestinal muscular layer. The diaphragmatic muscle showed a lesion of autophagic vacuolar myopathy, representing frequent occurrence of autophagic vacuoles that contained amorphous materials, lipofuscin granules, and eosinophilic proteinaceous droplets. It is presumable that the pathogenetic mechanism of this systemic lipofuscinosis had a close relationship with ischemia due to anemic condition caused by pelvic hemorrhage. This bovine case was considered a newly identified variant of systemic lipofuscinosis associated with an autophagic vacuolar lesion in the diaphragmatic muscle.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Dark pigmentation due to deposition of lipofuscin granules (LGs) occurs in muscle tissues of domestic animals, including cardiac, skeletal, or smooth muscle of the bovine species (Bradley and Duffell 1982; Jolly 1995; McGavin 1995; Myers et al. 2012; Ohfuji 2015; Valentine 2017). It has been acknowledged that the autophagy system is required for basal muscle fiber homeostasis in skeletal muscle (Nishino 2010; Sandri 2010). Autophagic vacuoles (AVs) are known to be a frequent feature in a group of muscle disorders referred to as autophagic vacuolar myopathies (AVM) in humans, including Pompe disease, Danon disease, and X-linked myopathy with excessive autophagy (Sugie et al. 2005; Nishino 2003; Nishino 2006; Malicdan et al. 2008; Grumati and Bonaldo 2012). Recent studies by using molecular genetic techniques have revealed that a heterozygous CLN3 mutation is associated with juvenile onset neuronal ceroid-lipofuscinosis and AVM in humans (Licchetta et al. 2015; Taschner et al. 2015; Radke et al. 2018). Lesions of AVM have scarcely been described in domestic animals including the bovine species. The present report describes the histopathological findings in a bovine case of systemic lipofuscinosis associated with a vacuolar lesion similar to that of AVM in the diaphragmatic muscle.
Case description
A 7-year-old Holstein-Friesian dairy cow that had been raised in a local dairy farm fell down accidentally in a cow barn. Immediately thereafter, the animal showed clinical signs of motor dysfunction, such as difficulty in rising, inability to rise, and ultimately sternal recumbency. There were no clinical signs indicative of those seen in the central nervous system (CNS) disorder, such as loss of consciousness, convulsion, and abnormal behavior. Because of poor prognosis determined by the referring veterinarian, the owner decided to cull the cow. The animal was slaughtered at a public abattoir 5 days after the onset of clinical sign. After postmortem inspection, tissue samples for histopathological examination were taken from various internal visceral organs and tissues, including the liver, spleen, kidney, heart, lung, adrenal gland, small intestine, tongue, masseter muscle, diaphragmatic muscle, semimembranosus muscle, semitendinosus muscle, and medulla oblongata. These samples were fixed in 10% neutral buffered formalin for 72 h, processed by routine methods, and embedded in paraffin wax. Four-μm-thick sections were cut and stained with hematoxylin and eosin (HE). Selected sections were stained with periodic acid-Schiff (PAS), Masson’s trichrome, luxol fast blue (LFB)-HE, phosphotungstic acid-hematoxylin (PTAH), Prussian blue, and Sudan black B. Selected unstained paraffin-embedded sections were examined with fluorescence microscopy under ultraviolet light.
Results
On postmortem inspection, the present cow exhibited fracture of the caudal vertebra, extensive hemorrhage in the pelvic cavity, and edematous swelling of the right sciatic nerve. In addition, brown discoloration of the masseter muscle, tongue, cardiac muscle, diaphragmatic muscle, liver, adrenal cortex, and wall of the small intestine was noted. Other internal visceral organs and tissues were generally unremarkable.
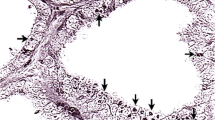
Histopathologically, this cow exhibited a pigmented condition of systemic lipofuscinosis. Although to varying degrees, deposition of LGs was found in a wide variety of otherwise normal cells, including the hepatocytes, renal tubular epithelial cells, cardiac muscle fibers, cardiac Purkinje fibers, adrenocortical cells, striated muscle fibers (the masseter muscle, tongue, diaphragmatic muscle, semimembranosus muscle, and semitendinosus muscle), and smooth muscle fibers in the muscular layer of small intestine (Fig. 1). In the medulla oblongata nuclei, LGs were deposited within neurons and glial cells that exhibited no significant increase in number. LGs stained yellowish brown with HE and Masson’s trichrome, positively with PAS, dark blue with LFB-HE, pale blue with PTAH, negatively with Prussian blue, and black with Sudan black B (Fig. 2, inset). LGs showed yellow-orange autofluorescence emission with fluorescence microscopy.
Along with LGs, a small number of eosinophilic proteinaceous granules (EPGs) were found in the smooth muscle fibers of the intestinal muscular layer (Fig. 2). These EPGs were scattered randomly in the smooth muscle fibers. In addition, the diaphragmatic muscle often had clear sarcoplasmic vacuoles (< 30 μm in diameter) that were consistent with AVs. In many instances, these AVs were situated at the deeper or central portion of each muscle fiber, occurring singly per muscle fiber. Some AVs contained amorphous materials together with varying amounts of LGs (Fig. 3). Eosinophilic proteinaceous droplets (EPDs) that exhibited a hyaline appearance and were up to 10 μm in diameter were rarely found within the AVs (Fig. 4). Although both EPGs and EPDs stained negatively with PAS, LFB-HE, Prussian blue, and Sudan black B, they stained blue with PTAH and orange-red with Masson’s trichrome. No autofluorescence emission was recognized in EPGs and EPDs with fluorescence microscopy.
Changes in other internal visceral organs included a mild infiltration of lymphocytes and siderophages in the interlobular connective tissue of the liver and prominent splenic hemosiderosis.
Discussion
On the basis of the histochemical findings and fluorescent characteristics, the intracellular pigment granules recognized in a wide variety of internal visceral organs and tissues of the present cow were identical to LGs. This pigmented condition, diagnosed as systemic lipofuscinosis, was different from an inherited neurodegenerative disorder of bovine ceroid-lipofuscinosis in as much as it lacked neurological clinical signs, such as dementia, blindness, and ataxia. Bovine ceroid-lipofuscinosis, a disorder characterized by lysosomal storage of a fluorescent lipopigment within a variety of cells, is histopathologically associated with elective necrosis/loss of neurons and astrocytosis throughout the CNS (Jolly et al. 1992; Jubb and Huxtable 1993; Jolly and Walkley 1997; Hafner et al. 2005; Houweling et al. 2006). These neural lesions were absent in the medulla oblongata of the present cow. Although the precise risk factor for the development of this systemic lipofuscinois could not be determined, it should be noted that the animal had anemia due to massive hemorrhage involving the pelvic cavity. Therefore, there is the likelihood that the ischemic insult associated with anemic condition had a close relationship with the pathogenesis of such a variant of lipofuscinosis. Indeed, previous studies have verified sufficient evidence that ischemia is pathogenetically associated with accumulation of LGs in various organs and tissues, including cardiac muscle fibers of young rabbits with acute myocardial infarction (Tatariunas 1991), black esophagus with ischemic necrosis of the mucosa, submucosa, and muscularis propria in humans (Altenburger et al. 2011), and brain or spiral ganglion following global brain ischemia in experimental animals (Lukan et al. 2000; Ohtaki et al. 2012). Some authors thought that the incidence of LGs is related to the peroxidative membrane damage due to ischemia (Lukan et al. 2000).
As is the case with the present cow, intracellular accumulations of proteins on HE-stained sections usually exhibit a hyaline (homogenous, eosinophilic, and translucent) appearance (Miller and Zachary 2017) or likewise appear as rounded, eosinophilic droplets (Kumar et al. 2015). Both the LGs and EPGs (or EPDs) were present within the same muscle fibers in this cow, suggesting that these morphologically different types of intrasarcoplasmic deposits might have been metabolically related to each other. This possibility may be substantiated, in part, by the previous studies which have revealed that lipofuscin consists of a variety of chemical composition, including lipids, proteins, dolichols, carbohydrates, and metals (Jolly et al. 1995; MacLachlan and Cullen 1995; Miller and Zachary 2017).
The diaphragmatic muscle of the present cow noticeably exhibited a vacuolar lesion similar to that seen in AVM in humans. This vacuolar lesion, characterized by intrasarcoplasmic occurrence of many AVs, was differentiated from that reported previously in a genetic/metabolic disorder of generalized glycogenosis in cattle (Howell et al. 1981; Zlotowski et al. 2006; Cítek et al. 2007) on the basis of the absence of PAS-positive substances in the sarcoplasmic AVs. In addition, the presence of LGs and EPDs within the AVs excluded the likelihood of another type of vacuolation (hydropic degeneration) that is known as a less common, non-specific feature of myopathies (Hulland 1993; Berridge et al. 2018).
It is acknowledged that lysosomes play an important role in the autophagic pathway by digesting their contents (Lieberman et al. 2012) and that some fragments of cell components digested by lysosomal enzymes persist within AVs as lipofuscin (Grune et al. 2001; Miller and Zachary 2017). Furthermore, autophagy activation is critical for protein breakdown in skeletal muscle (Sandri 2010), and proteins are known to be major targets of oxidative modification (Grune et al. 2001). The balance between the protein damage and clearance of damaged proteins is disturbed under stress conditions, which may lead to a malfunctioning of proteostasis and an accumulating mass of oxidized proteins, finally resulting in the accumulation of highly cross-linked materials such as lipofuscin (Höhn and Grune 2013). Therefore, it is probable that in the diaphragmatic muscle of the present cow, the microscopically visible retention of EPDs within AVs as well as the identification of pigmented AVs may imply incomplete degradation of proteins and lipids (Sulzer et al. 2008), suggesting an impairment or block of autophagic flux (Sandri 2010; Lieberman et al. 2012). Although autophagy has been invoked as a mechanism of cell loss in degenerative diseases of muscle (Kumar et al. 2015), this cow’s diaphragmatic muscle exhibited no significant changes other than intrasarcoplasmic deposition of LGs, as in many other muscle tissues. Therefore, it remains to be accounted for why excessive development of AVs was restricted to this respiratory muscle.
In conclusion, this bovine case was considered a newly identified variant of systemic lipofuscinosis associated with an autophagic vacuolar lesion in the diaphragmatic muscle. Further research by using more specific methodologies, such as ultrastructural investigations and molecular genetic techniques, would be warranted for more accurate understanding of the pathophysiological mechanism for eliciting this condition in the bovine species.
References
Altenburger DL, Wagner AS, Li S et al (2011) A case of black esophagus with histopathologic description and characterization. Arch Pathol Lab Med 135:797–798
Berridge BR, Bolon B, Herman E (2018) Skeletal muscle system. In: Walling M, Haschek WM, Rousseaux CG (eds) Fundamentals of toxicologic psthology, 3rd edn. Academic Press, London, pp 196–212
Bradley R, Duffell SJ (1982) The pathology of the skeletal and cardiac muscles of cattle with xanthosis. J Comp Pathol 92:85–97
Cítek J, Rehout V, Vecerek L et al (2007) Genotyping glycogen storage disease type II and type V in cattle reared in the Czech Republic. J Vet Med A Physiol Pathol Clin Med 54:257–259
Grumati P, Bonaldo P (2012) Autophagy in skeletal muscle homeostasis and in muscular dystrophies. Cells 1:325–345
Grune T, Shringarpure T, Sitte N et al (2001) Age-related changes in protein oxidation and proteolysis in mammalian cells. J Gerontol A Biol Sci Med Sci 56:B459–B467
Hafner S, Flynn TE, Harmon BG et al (2005) Neuronal ceroid-lipofuscinosis in a Holstein steer. J Vet Diagn Investig 17:194–197
Höhn A, Grune T (2013) Lipofuscin: formation, effects and role of macroautophagy. Redox Biol 1:140–144
Houweling PJ, Cavanagh JA, Palmer DN, Frugier T, Mitchell NL, Windsor PA, Raadsma HW, Tammen I (2006) Neuronal ceroid lipofuscinosis in Devon cattle is caused by a single base duplication (c.662dupG) in the bovine CLN5 gene. Biochimica et Biophysica Acta 1762:890–897
Howell JM, Dorling PR, Cook RD (1981) Infantile and late onset of generalized glycogenosis typeIIin cattle. J Pathol 134:267–277
Hulland TJ (1993) Muscle and tendon. In: Jubb KVF, Kennedy PC, Palmer N (eds) Pathology of domestic animals, 4th edn. Academic Press, San Diego, pp 183–265
Jolly RD, Walkley SU (1997) Lysosomal storage diseases of animals: an essay in comparative pathology. Vet Pathol 34:527–548
Jolly RD, Gibson AJ, Healy PJ, Slack PM, Birtles MJ (1992) Bovine ceroid- lipofuscinosis: pathology of blindness. N Z Vet J 40:107–111
Jolly RD, Douglas BV, Davey PM, Roiri JE (1995) Lipofuscin in bovine muscle and brain: a model for studying age pigment. Gerontol 41(Suppl 2):283–293
Jubb KVF, Huxtable CR (1993) The nervous system. In: Jubb KVF, Kennedy PC, Palmer N (eds) Pathology of domestic animals, 4th edn. Academic Press, San Diego, pp 267–439
Kumar V, Abbas AK, Aster JC (2015) Cellular responses to stress and toxic insults: adaptation, injury, and death. In: Robbins and Cotran pathologic basis of disease, 9th edn. Elsevier. Saunders, Philadelphia, pp 31–68
Licchetta L, Bisulli F, Fietz M, Valentino ML, Morbin M, Mostacci B, Oliver KL, Berkovic SF, Tinuper P (2015) A novel mutation af Cln3 associated with delayed-classic juvenile ceroid lipofuscinois and autophagic vacuolar myopathy. Eur J Med Genet 58:540–544
Lieberman AP, Puertollano R, Raben N, Slaugenhaupt S, Walkley SU, Ballabio A (2012) Autophagy in lysosomal storage disorders. Autophagy 8:719–730
Lukan N, Fercakova A, Jalc P (2000) Morphology of lipofuscin in the rat spiral ganglion after ischemia. Biologia 55:695–699
MacLachlan NJ, Cullen JM (1995) Liver, biliary system, and exocrine pancreas. In: Carlton WW, McGavin MD (eds) Thomson’s special veterinary pathology, 2nd edn. Mosby, St. Louis, pp 81–115
Malicdan MC, Noguchi S, Nonaka I, Saftig P, Nishino I (2008) Lysosomal myopathies: an excessive build-up in autophagosomes is too much to handle. Neuromuscul Disord 18:521–529
McGavin MD (1995) Muscle. In: Carlton WW, McGavin MD (eds) Thomson’s special veterinary pathology, 2nd edn. Mosby, St. Louis, pp 393–422
Miller MA, Zachary JF (2017) Mechanisms and morphology of cellular injury. In: Pathologic basis of veterinary disease, 6th edn. Elsevier, St. Louis, pp 1–43
Myers K, McGavin D, Zachary JF (2012) Chronic cell injury and cell adaptation. In: Zachary JF, McGavin D (eds) Pathologic basis of veterinary disease, 5th edn. Elsevier, St. Louis, pp 26–48
Nishino I (2003) Autophagic vacuolar myopathies. Curr Neurol Neurosci Rep 3:64–69
Nishino I (2006) Autophagic vacuolar myopathy. Semin Pediatr Neurol 13:90–95
Ohfuji S (2015) Bovine generalized lipofuscinosis and sarcoplasmic inclusions: histopathological and histochemical features in three cases. Comp Clin Pathol 24:1237–1244
Ohtaki H, Ohara K, Song D, Miyamoto K, Tsumuraya T, Yofu S, Dohi K, Tanabe S, Sasaki S, Uchida S, Matsunaga M, Shioda S (2012) Accumulation of autofluorescent storage material in brain is accelerated by ischemia in chloride channel 3 gene-deficient mice. J Neurosci Res 90:2163–2172
Radke J, Koll R, Gill E, Wiese L, Schulz A, Kohlschütter A, Schuelke M, Hagel C, Stenzel W, Goebel HH (2018) Autophagic vacuolar myopathy is a common feature of CLN3 disease. Ann Clin Transl Neurol 5:1385–1393
Sandri M (2010) Autophagy in skeletal muscle. FEBS Lett 584:1411–1416
Sugie K, Noguchi S, Kozuka Y (2005) Autophagic vacuoles with sarcolemmal features delineate Danon disease and related myopathies. J Neuropathol Exp Neurol 64:513–522
Sulzer D, Mosharov E, Talloczy Z, Zucca FA, Simon JD, Zecca L (2008) Neuronal pigmented autophagic vacuoles: lipofuscin, neuromelanin, and ceroid as macroautophagic responses during aging and disease. J Neurochem 106:24–36
Taschner PE, Cortese A, Tucci A (2015) Novel CLN3 mutation causing autophagic vacuolar myopathy. Neurol 84:632
Tatariunas AB (1991) Accumulation of lipofuscin granules in acute myocardial infarct as a model of cell aging. Biull Eksp Biol Med 111:443–446
Valentine BA (2017) Skeletal muscle. In: Pathologic basis of veterinary disease, 6th edn. Elsevier, St. Louis, pp 908–953
Zlotowski P, Gimeno EJ, Diaz A (2006) Lectin-histochemistry: glycogenosis in cattle. Vet Res Commun 30:369–377
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ohfuji, S. Systemic lipofuscinosis associated with a lesion of autophagic vacuolar myopathy in the diaphragmatic muscle of a cow. Comp Clin Pathol 28, 705–709 (2019). https://doi.org/10.1007/s00580-019-02951-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00580-019-02951-w