Abstract
Lead acetate (PbAC) toxicity can occur by either ingestion or inhalation from contaminated surfaces or from the environment. Nigella sativa is a natural product with immense pharmacological properties, which include antioxidant, antibacterial, and antianemia properties. It has been showed to counter the effect of PbAC-induced hematological and biochemical changes in short-term studies. This study hypothesized that the N. sativa (NS) administration will ameliorate the deleterious effects of chronic PbAC toxicity in rats. A total of 75 Sprague Dawley rats were divided into three groups of 25 rats, and each group was further sub-divided into five groups of five rats each. Group 1 rats (negative control) were given distilled water, group 2 (positive control; PC) were given 10 mg/kg of lead acetate (PbAC) daily, and groups 3 (T1), 4 (T2), and 5 (T3) were each given 10 mg/kg of PbAC followed by graded concentrations of powdered seeds of NS; 100, 150, and 200 mg/kg, respectively. Five rats in each group were euthanized at 30, 60, and 90 days for collection of whole blood and selected organs. Whole blood was collected after euthanized via cardio puncture and used to evaluate the complete blood profile, while plasma was used for biochemical analysis. Tissue samples of the liver and kidney were fixed with 10% buffered formalin, processed, and stained with H&E and periodic acid–Schiff (PAS) for the liver. Aggression and fear were increased in the PbAC-exposed group and absent in the T3 group. There was a lower (p < 0.05) red blood cell count (RBC), packed cell volume (PCV), mean corpuscular hemoglobin concentration (MCHC), and lymphocyte count in the PC and T1 groups only. Biochemical analysis revealed elevated (p < 0.05) liver enzyme and creatinine levels in the PC and T1 groups on day 90 for AST and day 30 for ALT and creatinine. The level of alkaline phosphatase (ALP) was higher (p < 0.05) in the PC at 30 and 60 days of sampling. Other parameters, such as WBCs, prothrombin, urea, and cholesterol, were not significant in all groups. Histopathological lesions in the liver and kidneys were more severe in the PC and T1 groups, while the T2 and T3 groups showed mild lesions resulting from N. sativa administration. There was a decrease (p < 0.05) in the total PAS-stained area signifying glycogen depletion in the PC, T1, and T2 groups at 60 days and a higher distribution of the PAS-stained areas (p < 0.05) in the T3 group. At 90 days, the PC group had a lower (p < 0.05) distribution of PAS-stained areas in comparison to the other groups. The results showed the therapeutic potential of N. sativa extract in modulating both hematological and biochemical alterations induced by chronic lead acetate administration in rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lead (Pb) is a common contaminant of the environment and water bodies found in paints, leaded gasoline, dust and soil in gold mining areas, as well as a result of improper industrial waste disposal. Following exposure to Pb, it binds to the blood, soft tissues, and bones, thus remaining in these tissues for a long time. Lead is particularly deadly to young children, resulting in non-regenerative anemia, nervous signs, and development of nutritional deficiencies (Assi et al. 2016a). Adults are mostly exposed at work and show clinical signs of microcytic anemia and nervous symptoms (Papanikolaou et al. 2005). Experimental toxicity studies in laboratory animals have shown various disruptions and alterations in the animal’s physiological function. In one study, acute toxicity of lead acetate (PbAC) administered in rats (10 or 100 mg) caused elevation of alanine aminotransferase enzyme (ALT) after 12 and 24 h, respectively (Bharali 2013). In another study, administration of graded doses of PbAC to rats for 30 days showed reduction in total protein, albumin, globulin, total bilirubin, RBC counts, WBC counts, hemoglobin (Hb), and PCV, while increasing the levels of ALT, aspartate aminotransferase (AST), alkaline phosphatase (ALP), urea, and creatinine (Dalia 2010). Other researchers have found similar findings following chronic administration of PbAC to rats for periods lasting 14–24 weeks (Allouche et al. 2009; Allouche et al. 2011; Ibrahim et al. 2012).
Nigella sativa seeds and leaves have been commonly used to alleviate ailments for centuries. Its seeds and oil have been proved to have low toxicity and exhibited good anti-inflammatory, analgesic, anticarcinogenic, antidiabetic, antiulcer, antimicrobial, and antiparasitic activities (Ali and Blunden 2003; Gali-Muhtasib et al. 2006). Animal studies have shown the protective effects of N. sativa against several toxic compounds, such as isoproterenol, tramadol, carbon tetrachloride, cisplatin, and sodium valproate. The protective effect of N. sativa in these studies was attributed to the regulation of oxidative enzyme levels, hepatic enzyme activities, renal function markers, and blood lipid profiles (Hala 2011; Awadalla 2012; Murugesan et al. 2012; Krishnan and Muthukrishnan 2012; Elkhateeb et al. 2015). In another study, N. sativa seeds were shown to ameliorate the biochemical imbalances and tissue damage associated with PbAC toxicity in rats (Farrag et al. 2007). However, the study lasted for only 6 weeks and did not reflect the true picture associated with chronic PbAC toxicity. Currently, there is a paucity of information on the effects of powdered seeds of N. sativa administration in chronic PbAC toxicity in rats. Thus, in this study, we investigated the effect of PbAC toxicity for 90 days and how concurrent administration of graded doses of NS counteracted these effects in the blood, serum, and tissues.
Materials and methods
Preparation of N. sativa seed suspension and lead acetate solution
Black seeds (N. sativa) were purchased from a local market in Serdang, Selangor, Malaysia, certified, c leaned, and prepared into powder form as described earlier (Assi et al. 2017a). Lead acetate (Oxford Lab. Co., India) was also prepared at a concentration of 10 mg/kg body weight in distilled water as previously described (Assi et al. 2017a).
Animal management, grouping, and clinical observation
In this study, 75 male Sprague Dawley rats aged 8–10 weeks and 250–300 g were used. The rats were acclimatized for 2 weeks before the commencement of the experiment. They were fed standard pellet commercial rat chow (Gold Coin, Malaysia), and clean water was provided ad libitum. Before the experimentation, the rats were grouped into five groups of 15 animals each as shown in Table 1.
Clinical monitoring of the rats was done every day. However, important observations, such as aggression, fear, and reduced appetite, were summarized at the each of each sampling period and presented in percentages based on the number of rats showing such signs within a group.
Sample collection for hematology, biochemistry, and histopathology
Following anesthesia at stipulated periods (30, 60, and 90 days), whole blood was collected intracardially from five animals per group and stored in EDTA-laced tubes (Weisbroth et al. 2013). Plasma was obtained following centrifugation of the blood at 2500 rpm for 10 min (Hettich, Germany). Tissue samples of the liver and kidneys were collected and fixed in 10% neutral buffered formalin.
Evaluation of hematological and biochemical parameters
Whole blood was used for estimation of hematological parameters using an Automatic Cell Counter (CELL-DYN 3700, Roche, USA). Biochemical parameters for the serum obtained from whole blood were evaluated with an automated chemistry analyzer (Siemens, USA) as described earlier (Assi et al. 2017b).
Histopathology
Formalin-fixed tissues were processed routinely before embedding in paraffin wax. Tissue blocks were then sectioned at a thickness of 5–6 μm and stained with hematoxylin and eosin for histopathological examination of lesions with light microscopy. Photomicrographs of tissue microscopic focal fields were captured using Mioticam® camera. Histopathological lesion scoring was done as described earlier, using a scale of 0–3 for lesion severity (Othman et al. 2016). Six microscopic focal fields were examined per slide using 400× magnification, and the lesion scores equated as 0–3.
The periodic acid–Schiff (PAS) staining was performed on the sectioned slides. Briefly, the slides were inserted in a container of 0.5% periodic acid for 5 min, followed by three wash cycles using distilled water. The slides were placed into a solution of Schiff’s reagent for 15 min, then washed in 0.55% metabisulfite twice for 1 min each, followed by washing in running tap water for 10 min for bluing. Acidified Harris hematoxylin was used to counterstain the slides for 30 s followed by washing the slides in water. The sections were dehydrated in 95–100% alcohol then xylene before mounting with coverslips and viewing using light microscopy. The presence of rose pink or magenta coloration within the hepatocytes was used as an indication of glycogen deposition or presence of polysaccharides.
The PAS-stained areas were estimated used ImageJ software as previously described by Rangan and Tesch (2007). Briefly, the images were opened with the ImageJ software and converted to grayscale. The image threshold is then set from an image montage and adjusted while viewing the histogram in order to ensure a precise selection of the stained areas. Once the threshold is set, the image is converted to binary (black and white), and the stained areas (mm2) were determined and recorded as mean ± S.E. by using the analyze option.
Statistical analysis
Data obtained from hematology, biochemistry, and histopathology scores were summarized as mean ± SE and analyzed with the aid of GraphPad Prism 6.0 software using two-way analysis of variance (ANOVA) with Bonferroni’s multiple comparison test. Comparison between histopathological scores was done using Kruskal–Wallis (non-parametric) test with Dunn’s multiple comparison. Statistical significance was set at p < 0.05.
Results
Clinical observations
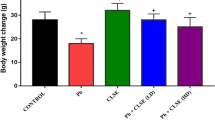
The mortality rate at 30 days was 7% (n = 15) in the PC, T1, and T2 groups, while none was observed in the T3 group. At 60 days, mortality was 10% (n = 10) in the PC group only, while no mortality was recorded in all groups at 90 days of sampling. The main clinical observations, such as aggression, fear, and loss of appetite, were observed to be higher in the PC and T1 groups at 30 days of sampling, while the T2 had a lower percentage and the T3 had none. At 60 days, aggression and fear were higher in the PC group, while reduced appetite was comparable and higher in both PC and T1 groups. Similarly, at 90 days, the PC group had higher values of all observations followed by the T1, while the T2 had a lower percentage (Table 2).
Hematology findings
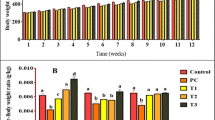
The total red blood cell (RBC) count was lower (p < 0.05) in the positive control (PC) group on days 30, 60, and 90 of sampling with no changes in all treatment groups at all time periods. There was no significant change in hemoglobin concentration in the entire days of sampling. The PCV was lower (p < 0.05) in the PC group on days 30 and 60, while no changes were observed at 90 days. There was no difference in the MCV values of all groups on days 30 and 60, while at 90 days, both PC and treatment groups had lower MCV values when compared to the control group. The MCHC value was lower in the PC and T1 groups at day 30 of sampling. However, on day 60, both the PC and treatment groups had a lower MCHC value than the control, while no changes were observed at 90 days of sampling. There was no significant change in prothrombin concentration on entire days of sampling (Fig. 1).
Graphs showing hematological changes in rats exposed to PbAc and treatment groups. a RBC count, b hemoglobin concentration, c packed cell volume, d mean corpuscular volume, e mean corpuscular hemoglobin concentration, and f prothrombin concentration. a,b,cBars with different superscript letters indicate statistical significance at p < 0.05
There was no significant change in total white blood cell, monocytes, and eosinophil counts in all groups in entire days of sampling. However, the lymphocyte count was lower (p < 0.05) in the T1 group on day 30 with no changes on subsequent sampling periods. Similarly, neutrophil count was higher in the PC group on day 30 without any changes on days 60 and 90. The thrombocyte count was comparable in all groups on days 30 and 90, while in the T3 group, it was lower (p < 0.05) on day 60 (Fig. 2).
Biochemical findings
The level of AST activity was unchanged in all groups on days 30 and 60 of sampling. On day 90, AST activity was elevated in the PC and T1 groups when compared to the control group. On the other hand, ALT activity was elevated in the PC and T1 groups on day 30 of sampling, while no changes were observed on days 60 and 90. Similarly, ALP activity was higher (p < 0.05) in the PC group on days 30 and 60, with no changes on day 90. The concentration of creatinine was higher (p < 0.05) in the PC and T1 groups on day 30 of sampling with no changes seen on days 60 and 90. There were no significant changes in cholesterol and urea concentration in the entire days of sampling (Fig. 3).
Histopathological findings
The histopathological lesion scores of the liver and kidney are presented in Table 3. At day 30 of sampling, tubular degeneration (TD) in the kidneys was higher (p < 0.05) in the PC group than in the T1 group. T2 and T3 groups had TD comparable with the control group. Hepatocyte vacuolation (HV), Kupffer cell proliferation (KCP), and pyknotic hepatocytes (PH) were higher in the PC and T1 groups at 30 days of experiment.
At 60 days of sampling, TD and HV were higher (p < 0.05) in PC and T1 groups, while KCP and PH were higher in PC group alone.
At day 90 of sampling, TD and HV were comparable and low (p < 0.05) in all PbAC exposed and treated groups. However, KCP was higher (p < 0.05) in the PC and T1 groups, while PH was comparable and higher (p < 0.05) in PC, T1, and T2 groups (Figs. 4 and 5).
Photomicrograph of the kidneys of rats at day 30 of sample collection. a1 NC showing mild vacuolation of the renal tubular cells, b1 PC showing moderate vacuolation of the renal tubular cells, c1 T1 showing mild vacuolation of the renal tubular cells, d1 T2, and e1 T3 not having obvious vacuolation of the renal tubular cells (arrows); 60 days of sample collection. a2 NC, b2 PC showing moderate vacuolation of the renal tubular cells, c2 T1 showing mild vacuolation of the renal tubular cells, d2 T2, and e2 T3 not having obvious vacuolation of the renal tubular cells; 90 days of sample collection. a3 NC, b3 PC, c3 T1, d3 T2, and e3 T3; note mild and occasional vacuolation of the renal tubular cells in B3 and C3, H&E 200×
Photomicrograph of the liver of rats at 30 days of sample collection. a1 NC showing mild vacuolation of the hepatocytes, b1 PC showing moderate vacuolation of the hepatocytes (yellow arrows) and pyknotic hepatocytes cells (black arrow), c1 T1 showing moderate vacuolation of hepatocytes (yellow arrow) and mild hepatocyte pyknosis (black arrow), d1 T2 and e1 T3 showing mild hepatocyte vacuolation (yellow arrow) and pyknotic hepatocytes (black arrow); 60 days of sample collection. a2 NC showing occasional mild vacuolation of the hepatocytes (yellow arrow), b2 PC showing an area of leucocytic infiltration (black arrow), moderate vacuolation of the hepatocytes (yellow arrow), and pyknotic hepatocytes (blue arrow). c2 T1 showing moderate vacuolation of hepatocytes. d2 T2 and e2 T3 showing mild hepatocyte vacuolation (yellow arrow) and nuclear pyknosis (black arrow); 90 days of sample collection. a3 NC showing apparently normal liver tissue with a congested central vein, b3 PC, c3 T1, d3 T2, and e3 T3 showing pyknotic hepatocytes (black arrow) and numerous active Kupffer cells (green arrows), H&E 200×
Periodic acid–Schiff staining
The mean ± SE of PAS-stained areas in the liver of the various groups is shown in Table 4. The PAS-stained section of the liver at 30 days showed uneven magenta staining of mucopolysaccharides within the hepatocytes of all groups examined. However, there was no difference (p > 0.05) in the distribution of PAS-positive areas in all the groups (Fig. 6). At day 60 post-treatment, the PC, T1, and T2 groups had lower distribution of PAS-positive areas in comparison to the control, which is an indicative of glycogen depletion within the hepatocytes. However, the T3 group showed a diffuse and higher (p < 0.05) distribution of PAS-positive areas in the liver (Fig. 6). After 90 days of treatment, the distribution of PAS-positive areas was comparable in the control and all the treatment groups. However, the PC group showed a lower (p < 0.05) distribution of PAS-stained areas in comparison to the control and treatment groups, indicative of mild glycogen depletion in the hepatocytes of this group (Fig. 6).
Section of the liver of rats in different treatment groups showing PAS-positive areas indicating presence of mucopolysaccharide within the hepatocytes. There is no difference in the distribution of PAS-positive areas in all groups at 30 days. Note lower distribution of PAS-positive areas in the PC, T1, and T2 at 60 days; the PC group showed lower PAS-stained areas than the other groups, PAS stain 400×
Discussion
Lead acetate has been shown to induce neurological dysfunction in lab animals. Some of these dysfunctions include cognitive impairment, aggression, slower acquisition, and visual discrimination (Driscoll and Stegner 1976). However, the dose and duration of PbAC exposure and age at which the animals were exposed significantly affected these dysfunctions. For example, the administration of 0.5% PbAC to older mice (330 and 660 days old) increased aggression when compared with administration to younger mice (65 and 120 days) (Burright et al. 1983; Engellenner et al. 1986). In this study, we observed increased aggression and fear in animals exposed to PbAC, while those treated with low-dose powdered seeds of N. sativa had lower incidence of these signs. Interestingly, rats treated with 200 mg/kg of N. sativa did not show signs of aggression and fear during all sampling periods, thus suggesting that the powdered seeds of N. sativa prevented the manifestations of these signs.
In this study, PbAC induced decrease in RBCs and PCV counts in the PC group on 30 and 60 days of treatment, and these effects were reversed by N. sativa seed powder administration in treated animals. This shows that N. sativa seeds can prevent anemia induced by PbAC. Similarly, decrease in lymphocytes and increase in neutrophil counts in the PC and T1 groups were observed, both of which were reversed by N. sativa seed powder administration in the treatment groups. These results supported the earlier toxicity studies showing the negative effects of PbAC on the hemogram of laboratory animals (Dalia 2010; Ibrahim et al. 2012), adding to the therapeutic effects of N. sativa in improving the hemogram as previously described (Ali and Blunden 2003; Gali-Muhtasib et al. 2006).
Another pertinent finding observed in this study was the elevated levels of ALT and ALP in the PC group at 30 and 60 days of sampling and increased AST at 90 days of sampling. ALT and AST are two important enzymes that signify liver function in animals. An increased level of these enzymes indicates possible hepatocellular damage or injury. Increased levels of these enzymes have been previously reported following PbAC toxicity in rats (Allouche et al. 2011; Ibrahim et al. 2012; Bharali 2013). In these studies, elevated levels of AST, ALT, and ALP were observed following acute and chronic PbAC administration to rats. Furthermore, we also observed that powdered seeds of N. sativa acted as a hepatoprotective agent since it regulates the levels of ALT, AST, and ALP in treated rats. Similarly, based on our histopathological findings, the PbAC-exposed group had a higher distribution of hepatocyte degeneration and necrosis, which was responsible for the increased enzyme levels observed. On the other hand, the treated groups had lower distribution of these pathological lesions, suggesting a hepatoprotective effect of the seed extract against PbAC-induced liver damage. In our previous report, we showed evidence of decreased GSH and SOD enzyme levels in rats exposed to PbAC. We also showed increased levels indicative of antioxidant capacity in rats treated with powdered seeds of N. sativa especially at 200 mg/kg body weight (Assi et al. 2016b). Presence of PbAC in the hepatocytes has been reported to induce necrosis, degeneration, and fatty change in a dose-dependent manner (Mudipalli 2007). In this study, the use of PAS stain in the liver sections revealed the presence of glycogen depletion in the PC, T1, and T2 groups, especially at 60 days of sampling. Glycogen depletion has been shown to be one of the toxic effects of LA in the liver. In a study by Hegazy and Fouad (2014), mild and moderate glycogen depletions were observed in rats administered 0.13% lead acetate after 4 and 8 weeks, respectively. Although there are no studies on the effect of N. sativa administration on LA-induced glycogen depletion in the liver, a related study by Al-Rouby and Gawish (2013) showed unaltered glycogen deposits in the liver of rats treated with N. sativa oil following exposure to sodium valproate. Based on this limited information, it can be deduced that N. sativa seeds prevent damage to hepatocytes which thus prevents depletion of their glycogen stores. N. sativa has been shown to restore deficits in oxidative enzyme levels, such as GSH and SOD in the cell following exposure to oxidant compounds, such as PbAC, which often results in lower concentration of these enzymes (Salem 2005). In a study by Farrag et al. (2007), rats exposed to PbAC for 6 weeks were observed to have elevated levels of AST, which was ameliorated by administration of N. sativa seeds. However, the study was only able to show the sub-chronic effects of N. sativa treatment on PbAC induced toxicity, while our study evaluated the sub-chronic and chronic effects altogether. Furthermore, we observed that both ALP and ALT were not elevated in all groups at 90 days, while AST was higher in the PC and T1 groups only. This may be attributed to increased excretion of lead in the bile and intestines with less retention in the liver, hence resulting in less hepatocyte necrosis as the time of exposure was prolonged. Since the dose of PbAC reported to cause inhibition of CYP450 and cytochrome b5 in the liver and kidney was 50 mg/kg, there may be minimal to low inhibition of these enzymes in rats in this study (Mudipalli 2007).
In this study, the kidney function was not severely affected by PbAC toxicity, since elevated levels of creatinine were only observed at 30 days of sampling in both PC and T1 groups. Other studies using PbAC at graded doses also observed similar or more severe increases in kidney enzymes, such as creatinine and urea (Farrag et al. 2007; Dalia 2010; Elkhateeb et al. 2015). Exposure to high levels of lead has been shown to induce acute and chronic nephropathy characterized by increased renal biochemical parameters. This has been attributed to the development of degenerative changes in the renal tubules and presence of nuclear inclusion bodies containing lead complexes (Rastogi 2008). In this study, treatment of rats with 150 and 200 mg/kg of powdered seeds of N. sativa prevented the increase in creatinine in blood on day 30 of PbAC toxicity, suggesting a possible nephro-protective effect by the seed extract of N. sativa. The nephro-protective effect of N. sativa has been previously reported following PbAC, gentamycin, and tramadol nephron-toxicities (Farrag et al. 2007; Yaman and Balikci 2010; Saleem et al. 2012; Elkhateeb et al. 2015). In these studies, N. sativa was shown to ameliorate nephro-toxicity induced by these compounds due to a restoration of the imbalance of oxidative enzyme levels.
Furthermore, in this study, PbAC induced histopathological lesions in both the kidney and liver. The lesions observed appeared more severe in the PC and T1 groups and mild in the treated groups, indicating that treatment with powdered seeds of N. sativa reduced and eventually reversed these injuries at 150 and 200 mg/kg. PbAC has been previously shown to induce increased vacuolation in the liver of rats 24 h after administration of 100 mg/kg (Bharali 2013) of PbAC. In other related studies, PbAC has also been shown to induce severe damages to the kidney and liver after 4–6 weeks of administration (Farrag et al. 2007; Dalia 2010). In the study by Farrag et al. (2007), administration of N. sativa to the PbAC-intoxicated rats improved the histopathological lesions in the kidney and liver. This finding substantiates with our current results since we observed a restoration of normal enzyme levels and tissue morphology in both the kidney and liver after 90 days of PbAC and N. sativa seed powder administration, especially 200 mg/kg N. sativa. Similarly, our recent study on the prophylactic activity of N. sativa showed promising results against PbAc-induced toxicity by preventing the development of hemato-biochemical and histopathological alterations in rats (Assi et al. 2017b).
Conclusion
To conclude, this study showed that chronic PbAC administration to rats induced hematological, biochemical, and histopathological changes. The concurrent administration of powdered seeds of N. sativa at 150 and 200 mg/kg was able to reverse the alterations induced by PbAC in sub-chronic and chronic conditions.
References
Ali BH, Blunden G (2003) Pharmacological and toxicological properties of Nigella sativa. Phytother Res 17(4):299–305. https://doi.org/10.1002/ptr.1309
Allouche L, Hamadouche M, Touabti A, Khennouf S (2011) Effect of long-term exposure to low or moderate lead concentrations on growth, lipid profile and liver function in albino rats. Adv Biol Res 5(6):339–347
Allouche L, Hamadouche M, Touabti A (2009) Chronic effects of low lead levels on sperm quality, gonadotropins and testosterone in albino rats. Exp Toxicol Pathol 61(5):503–510. https://doi.org/10.1016/j.etp.2008.12.003
Al-Rouby NM, Gawish SM (2013) Histological study on the possible protective effect of nigella sativa oil on experimentally induced hepatotoxicity in albino rats treated with sodium valproate. Glo Adv Res J of Med Med Sci 2(4):090–099
Assi MA, Hezmee MNM, Abba Y, Rajion MA, Wahid H, Yusof MSM (2017a) Assessment of therapeutic effects of Nigella sativa against chronic lead acetate-induced reproductive dysfunction in male Sprague-Dawley rats. Comp Clin Path 26(1):87–97. https://doi.org/10.1007/s00580-016-2349-3
Assi MA, Hezmee MNM, Abba Y, Sabri MY, Haron AW, Baiee FH, Rajion MA (2017b) Effect of Nigella sativa pre-treatment on sub-chronic lead acetate induced hematological and biochemical alterations. J Comput Theor Nanosci 14(6):2752–2758. https://doi.org/10.1166/jctn.2017.6565
Assi MA, Noor MHM, Bachek NF, Ahmad H, Haron AW, Yusoff MSM, Rajion MA (2016a) The various effects of Nigella sativa on multiple body systems in human and animals, pp 1–19
Assi MA, Hezmee MNM, Haron AW, Sabri MYM, Rajion MA (2016b) The detrimental effects of lead on human and animal health. Veterinary world 9(6):660–671. https://doi.org/10.14202/vetworld.2016.660-671
Awadalla EA (2012) Ameliorative effect of the crude oil of the Nigella sativa on oxidative stress induced in rat testes by cisplatin treatment. Biomedicine & Preventive Nutrition 2(4):265–268. https://doi.org/10.1016/j.bionut.2012.08.005
Bharali MR (2013) Effect of acute lead acetate exposure on liver of mice. Journal of Global Biosciences 2:121–125
Burright RG, Engellenner WJ, Donovick PJ (1983) Lead exposure and agonistic behavior of adult mice of two ages. Physiol Behav 30(2):285–288. https://doi.org/10.1016/0031-9384(83)90020-3
Dalia M (2010) Effect of using pectin on lead toxicity. J Am Sci 6:541–554
Driscoll JW, Stegner SE (1976) Behavioral effects of chronic lead ingestion on laboratory rats. Pharmacol Biochem Behav 4(4):411–417. https://doi.org/10.1016/0091-3057(76)90057-5
Elkhateeb A, El Khishin I, Megahed O, Mazen F (2015) Effect of Nigella sativa Linn oil on tramadol-induced hepato- and nephrotoxicity in adult male albino rats. Toxicol Rep 2:512–519. https://doi.org/10.1016/j.toxrep.2015.03.002
Engellenner WJ, Burright RG, Donovick PJ (1986) Lead, age and aggression in male mice. Physiol Behav 36(5):823–828. https://doi.org/10.1016/0031-9384(86)90437-3
Farrag ARH, Mahdy KA, Abdel Rahman GH, Osfor MM (2007) Protective effect of Nigella sativa seeds against lead-induced hepatorenal damage in male rats. Departments of Pathology, Department of Medical Biochemistry. Pak J Biol Sci 10(17):2809–2816
Gali-Muhtasib H, El-Najjar N, Schneider-Stock R (2006) The medicinal potential of black seed (Nigella sativa) and its components. Advances in Phytomedicine 2:133–153. https://doi.org/10.1016/S1572-557X(05)02008-8
Hala MA (2011) Protective effect of Nigella sativa, linseed and celery oils against testicular toxicity induced by sodium valproate in male rats. J Am Sci 7(5):687–693
Hegazy AM, Fouad UA (2014) Evaluation of lead hepatotoxicity; histological, histochemical and ultrastructural study. Forensic Medicine and Anatomy Research 2(03):70–79. https://doi.org/10.4236/fmar.2014.23013
Ibrahim NM, Eweis EA, El-Beltagi HS, Abdel-Mobdy YE (2012) Effect of lead acetate toxicity on experimental male albino rat. Asian Pac J Trop Biomed 2(1):41–46. https://doi.org/10.1016/S2221-1691(11)60187-1
Kocyigit Y, Atamer Y, Uysal E (2009) The effect of dietary supplementation of Nigella sativa L. on serum lipid profile in rats. Saudi Med J 30(7):893–896
Krishnan N, Muthukrishnan S (2012) Effect of Nigella sativa seed extract on carbon tetrachloride-induced hepatotoxicity in rats. Acute Med 2(4):107–113. https://doi.org/10.1016/j.jacme.2012.09.001
Mudipalli A (2007) Lead hepatotoxicity & potential health effects. Indian J Med Res 126(6):518
Murugesan M, Ragunath M, Prabu T, Nadanasabapathi S, Sakthivel M, Manju V (2012) Protective role of black cumin (Nigella sativa) on isoproterenol induced myocardial infarction in rats. Int J Pharmacol Clin Sci 1:45–53
Mustafa HN, Hussein AM (2016) Does allicin combined with vitamin B-complex have superior potentials than alpha-tocopherol alone in ameliorating lead acetate-induced Purkinje cell alterations in rats? An immunohistochemical and ultrastructural study. Folia Morphol (Warsz) 75(1):76–86. https://doi.org/10.5603/FM.a2015.0076
Othman AM, Abba Y, Jesse FFA, Ilyasu YM, Saharee AA, Haron AW, Zamri-Saad M, Lila MAM (2016) Reproductive pathological changes associated with experimental subchronic Corynebacterium pseudotuberculosis infection in nonpregnant boer does. J Pathog 2016:1–7. https://doi.org/10.1155/2016/4624509
Papanikolaou NC, Hatzidaki EG, Belivanis S, Tzanakakis GN, Tsatsakis AM (2005) Lead toxicity update. A brief review. Med Sci Monit 11(10):RA329–RA336
Rangan GK, Tesch GH (2007) Quantification of renal pathology by image analysis (methods in renal research). Nephrology 12(6):553–558. https://doi.org/10.1111/j.1440-1797.2007.00855.x
Rastogi SK (2008) Renal effects of environmental and occupational lead exposure. Indian Journal of Occupational and Environmental Medicine 12(3):103–106. https://doi.org/10.4103/0019-5278.44689
Saleem U, Ahmad B, Rehman K, Mahmood S, Alam M, Erum A (2012) Nephro-protective effect of vitamin C and Nigella sativa oil on gentamicin associated nephrotoxicity in rabbits. Pak J Pharm Sci 25(4):727–730
Salem ML (2005) Immunomodulatory and therapeutic properties of the Nigella sativa L. seed. Int Immunopharmacol 5(13):1749–1770. https://doi.org/10.1016/j.intimp.2005.06.008
Weisbroth SH, Flatt RE, Kraus AL (2013) The biology of the laboratory rabbit. Academic Press
Yaman İ, Balikci E (2010) Protective effects of Nigella sativa against gentamicin-induced nephrotoxicity in rats. Exp Toxicol Pathol 62(2):183–190. https://doi.org/10.1016/j.etp.2009.03.006
Author information
Authors and Affiliations
Contributions
All authors contributed equally to this work.
Corresponding author
Ethics declarations
Ethical statement
The animal experimental protocol used in this study was approved by the Institutional Animal Care and Use Committee (IACUC) with reference number UPM/IACUC/AUP-R047/2015, in accordance with the standard guidelines on usage and care of laboratory animals. The animals were humanely handled and euthanized at stipulated dates (30, 60, and 90 days) during the experimental period, using CO2 asphyxiation method after anesthesia procedure with ketamine + xylazine (50 mg/kg + 10 mg/kg body weight).
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Assi, M.A., Abba, Y., Abdulkhaleq, L.A. et al. Effect of powdered seed of Nigella sativa administration on sub-chronic and chronic lead acetate induced hemato-biochemical and histopathological changes in Sprague Dawley rats. Comp Clin Pathol 27, 705–716 (2018). https://doi.org/10.1007/s00580-018-2655-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00580-018-2655-z