Abstract
Purpose
Arterial hypotension is a major adverse effect of general anesthesia. Patients with pre-existing autonomic dysfunction are at greater risk of hypotension. This study was performed to examine whether objective measurement of the pupillary light reflex is predictive of intraoperative hypotension.
Methods
We studied 79 patients who underwent scheduled surgery under general anesthesia. Patients with severe cardiovascular disease or receiving antihypertensive agents were excluded. The light reflex was measured preoperatively using a portable infrared pupillometer, and the hemodynamic parameters were obtained from the anesthesia records. The patients were divided into two groups according to the development of hypotension: the hypotension and normotension groups. Multivariate logistic regression analysis was performed to determine the pupil parameters predictive of hypotension.
Results
Patients in the hypotension group were older and had a greater pupil size or constriction velocity than those in the normotension group. Logistic regression analysis showed that post-induction hypotension was significantly associated with maximum pupil size or constriction velocity after adjustment for age and other clinical variables. Latency of the light reflex and the percent reduction of pupil size were not associated with hypotension. Age was a relatively strong predictor of hypotension; other confounding factors were not associated with hypotension.
Conclusion
Measurement of maximum pupil size is useful to identify patients at risk for intraoperative hypotension. The influence of age must be considered during measurement of the pupil response.
Clinical trial number
UMIN000023729
Registry URL
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Arterial hypotension is a frequent adverse effect of general anesthesia and is associated with perioperative morbidity [1, 2]. A substantial fraction of intraoperative hypotension in non-cardiac surgery occurs prior to surgical incision [3]. Intraoperative hypotension is also associated with a prolonged hospital stay and high mortality [4, 5]. The predictors of hypotension include age, a higher American Society of Anesthesiologists (ASA) physical status, the use of propofol, the dose of fentanyl, and performance of emergency surgery [6, 7]. Patients with pre-existing autonomic dysfunction are also at greater risk of hypotension during general anesthesia [8]. Preoperative heart rate variability is reportedly useful for predicting hypotension during general anesthesia [9].
Pupil size or the pupillary light reflex is determined by the interaction between sympathetic and parasympathetic nerves; the iris dilator muscle is doubly dominated by sympathetic and parasympathetic nerves, whereas the iris sphincter muscle is subjected only to parasympathetic control [10, 11]. A previous study demonstrated that age was associated with a smaller pupil diameter [12, 13]. Another previous report showed an association between heart rate variability and light reflex [14]. Pupillary evaluation in the clinical setting is usually performed subjectively using a penlight; however, this is a visual determination that lacks quantitativeness.
In the current study, we used a portable infrared pupillometer to objectively measure the pupillary light reflex [15]. We hypothesized that preoperative screening of the pupillary light reflex is useful for evaluation of autonomic function. We, therefore, investigated whether the pupillary response can function as a predictive factor of hypotension after induction of general anesthesia.
Methods
This clinical trial was approved by the Ethical Committee for Clinical Studies of the Kyushu University School of Medicine and was prospectively registered at UMIN Clinical Trial Registry (UMIN000023729). Written informed consent was obtained from all study subjects. Eighty patients who underwent scheduled surgery under general anesthesia were enrolled. One patient was excluded because of an unpleasant feeling during measurement of the light reflex. Patients with brain infarction, cataract, glaucoma, other eye diseases, ischemic heart disease, heart failure, an ASA physical status of > 2, autonomic disorder, or thyroid disease were excluded. Patients undergoing emergency surgery or who were receiving calcium channel blockers, angiotensin receptor blockers, or beta blockers were also excluded.
Pupillary measurements
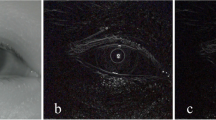
Ambient lightning and noise were well controlled after the patients’ arrival. After 10 min of resting time, pupillary measurements were performed in the operating room using an quantitative pupillometer (NPi-100; NeurOptics Inc., Irvine, CA, USA). This FDA approved handheld pupillometer can capture pupil movement and measure light reflection noninvasively via an infrared camera. This device was used for evaluating neurological outcome after cardiac arrest [16], intracranial hypertension [17], and clinical severity of subarachnoid hemorrhages [18]. The light reflex was acquired using a flash of visible white light of 800-ms duration [19]. The pupillometer calculates the maximum (initial) pupil size, minimum pupil size (after light stimulation), percent reduction of pupil size, latency, and constriction velocity.
Induction and maintenance of anesthesia
None of the patients were premedicated. Each patient’s electrocardiograph, pulse rate, blood pressure, respiratory rate, and oxygen saturation were constantly monitored from the time of their arrival in the operating room. The pupillary reactivity was measured, and an intravenous catheter was inserted. Ringer’s acetate solution was initially infused at a rate of 10 ml/kg/h. No patient was given epidural anesthesia. General anesthesia was induced with propofol (1.5 mg/kg) and fentanyl (1.0 µg/kg). Remifentanil was administered continuously at 0.3 μg/kg/min until tracheal intubation. Rocuronium (0.6 mg/kg) was administered to facilitate tracheal intubation. No cases of difficult intubation were encountered. Anesthesia was maintained with desflurane (5.0% in oxygen and air) and remifentanil at a rate of 0.1 μg/kg/min. The consumption of remifentanil and rocuronium was calculated using the patient’s ideal body weight. Bispectral index monitoring (BIS)—algorithm version 4.0—was undertaken to determine the depth of anesthesia. Noninvasive blood pressure was measured at least every 2 min. Hypotension was defined by a > 30% decrease in mean arterial pressure (MAP) from baseline or an MAP of < 60 mmHg from the start of anesthetic induction until 15 min after tracheal intubation. Hypotensive episodes were promptly treated with ephedrine administration and rapid infusion of hydroxyethyl starch.
Data collection
Basic patient data (age, sex, height, weight, pre-existing diseases, and current medications) were obtained from the hospital records. The blood pressure and BIS score were recorded every minute and downloaded by digital file from the anesthesia records. The MAP reading immediately after 10 min of resting time was defined as the baseline MAP. BIS values after intubation were defined as the average of 10 measurements obtained each minute during the 6–15-min period after intubation (omitting the first 5 min to account for the induction).
Statistical analysis
A t test was used to compare two groups after assessment of data normality by the Shapiro–Wilk test. The Chi square test was used to examine the association between two categorical variables.
Two multivariate logistic regression analysis models were developed to determine pupil parameters associated with hypotension during the post-induction period. Age was included as a variable in Model 1 because previous studies have suggested a strong association between pupil size and age [12, 13]. The following variables were selected for Model 2 as factors potentially affecting hypotension: age, sex, body mass index (BMI), diabetes, baseline MAP, and ASA physical status. The variance inflation factor was used to check for multicollinearity. No collinearity was present in Model 1 or 2. Odds ratios are presented with their 95% confidence intervals. For continuous variables, the odds ratio is considered the per-unit increase of the respective variable.
Sample size calculation
Significance level of alpha and beta were set at 0.05 and 0.1. On the basis of previous study of light reflex and autonomic function [11], we assumed that the sample size required for detecting the deference of maximum constriction velocity between hypotension group and normotension group was 22, and for detecting the deference of resting pupil size was 30.
When the percentage of hypotensive group was set to 60% based on the general anesthesia record of a previous 100 cases in our hospital, the minimum number of cases required to construct Model 1 of logistic regression analysis was assumed to be 50 [20]. Considering 20% dropout rate, a total sample size of 63 patients was required.
Results
Seventy-nine patients completed the study according to the study protocol. The patients’ demographics and characteristics are shown in Table 1.
The patients were divided into two groups according to whether they developed hypotension (n = 44) or remained normotensive (n = 35). The patients’ characteristics and pupil response parameters according to the presence or absence of hypotension are shown in Table 2. As expected, patients in the hypotension group were significantly older than patients in the normotension group. Anesthetic depths for the hypotension and normotension groups were comparable, and the correlation ratio for the BIS score and the development of hypotension was very low (η2 = 0.015). There was a negative correlation between pupil size and age; predicted pupil size is equal to 4.61–0.016 × age (R2 = 0.13, p = 0.001). Among the pupil response parameters, the maximum pupil size and the constriction velocity were smaller in the hypotension group than normotension group. Latency and the percent reduction of pupil size were comparable between the two groups.
Logistic regression analysis of the pupil response parameters was conducted to estimate the risk of hypotension (Table 3). The univariate analysis showed that hypotension was associated with the maximum pupil size or constriction velocity. After adjustment for age (Model 1) and other clinical variables potentially affecting hypotension (Model 2), these associations were slightly attenuated but remained statistically significant. Similarly, latency and the percent reduction of pupil size were not associated with hypotension after adjustment for confounding factors. The odds ratios (95% confidence intervals) of each confounding factor in the analysis of maximum pupil diameter using Model 2 were as follows: age (1.06 [1.00–1.13], p = 0.035), male sex (0.53 [0.16–1.66], p = 0.273), BMI (1.06 [0.91–1.25], p = 0.466), diabetes (0.94 [0.20–4.65]), p = 0.934), baseline MAP (0.98 [0.94–1.02], p = 0.3205), and ASA physical status of 2 (vs. 1: 1.12 [0.21–6.29], p = 0.896).
Discussion
The current study was performed to evaluate the pupil response parameters affecting hypotension after induction of general anesthesia. The factors significantly associated with hypotension were the maximum pupil size and constriction velocity, whereas the percent reduction of pupil size and latency were not predictors of hypotension.
At first glance, a decrease in constriction velocity seems to suggest a parasympathetic disorder because miosis is regulated only by parasympathetic nerves [10]. The mean constriction velocity during the pupillary light reflex is calculated by dividing the pupil constriction distance by the constriction time. The pupil constriction distance can be calculated from the maximum pupil diameter and percent reduction of pupil size. In the present study, we demonstrated an association between hypotension and constriction velocity. However, this is more likely to be a secondary change due to the decrease in maximum pupil size because the reduction rate of the pupil size was not associated with hypotension. This is also suggested from the finding that latency, an indicator of parasympathetic activity, has no effect on post-induction hypotension [11]. In contrast, mydriasis is regulated by the interaction between sympathetic and parasympathetic nerves [10]. The association between decreased pupil size and hypotension suggests that a selective deficit of sympathetic nerve function plays an important role in the development of hypotension. In this context, measurement of the pupil dilation response after the light reflex is likely to be a good predictor of hypotension. However, it is relatively difficult to obtain stable measurement values of the pupil dilation response because of blinking. Actually, we could not measure the pupil dilation velocity in about 30% of the patients in this study. Therefore, we did not add the pupil dilation velocity as a predictive factor for hypotension.
Some previous studies have demonstrated an association between autonomic dysfunction and intraoperative hypotension [8]. Patients with a sympathetic deficit are likely to exhibit failure to compensate for anesthetic-induced vasodilation. Measurement of the light reflex is easier and less time-consuming than measurement of heart rate variability or measurement of cardiovascular responses to the Valsalva maneuver or head-up tilt [9, 21]. Measurement of the light reflex is a routine procedure performed by the attending anesthesiologist. Prediction of hypotension after anesthetic induction using the maximum pupil diameter seems to be clinically useful because the magnitude of the pupil diameter is easy to judge intuitively even without using a portable infrared pupillometer. However, we must be aware that the pupil diameter is influenced by age.
Autonomic functions are influenced by the sleep–wake cycle and circadian rhythm [22, 23]. Pupil diameter is also affected by time-of-day under constant light condition [24, 25]. However, we assumed that the diurnal variation of autonomic activity did not have a significant effect on our result because all pupil measurements were performed around 8 a.m. in the current study. Diurnal variation should be taken into consideration on pupil measurement.
Age was a strong predictor of hypotension after our logistic regression analysis. Senile miosis reportedly results from organic iris damage, sympathetic deficit, and defective central inhibition [26]. Other confounding factors, including sex, BMI, ASA physical status, diabetes, and baseline blood pressure, were not associated with hypotension. There was a small difference between Models 1 and 2 in the logistic regression analysis, suggesting that we should mainly consider only the influence of age in measurement of the pupillary response.
A previous study showed that patients with diabetes have a greater risk of hypotension and require more vasopressors than patients without diabetes [8]. However, the present study showed no association between diabetes and hypotension. A significant positive correlation has been reported between hypertension and diabetes [27, 28]. We might have eliminated patients with diabetes because we excluded patients receiving calcium channel blockers, angiotensin receptor blockers, and beta blockers.
The present study had some limitations. First, we measured the light reflex in the operating room to ensure that the ambient brightness was as constant as possible. Although there was a resting time before measurement of the pupil response parameters, sympathetic tone may have affected the measured values. Second, iris damage such as hyalinization or sclerotic change may also have affected the maximum pupil size, but we did not evaluate organic lesions before surgery. Third, although a substantial fraction of intraoperative hypotension in non-cardiac surgery occurs prior to surgical incision, there are few papers which directly investigated the relationship between post-induction hypotension and postoperative outcomes. The influence of pupil measurement on postoperative outcome is unclear. Fourth, we used multiple anesthetics in the study period. It is difficult to elucidate which drug is responsible for the hypotension associated with the pupil diameter. Finally, the sample size of this study was relatively small. Further studies are need to confirm our results.
In conclusion, we demonstrated an association between pupil size and general anesthesia-induced hypotension. The influence of age must be considered during measurement of the pupil response.
References
van Waes JA, van Klei WA, Wijeysundera DN, van Wolfswinkel L, Lindsay TF, Beattie WS. Association between intraoperative hypotension and myocardial injury after vascular surgery. Anesthesiology. 2016;124:35–44.
Bijker JB, Persoon S, Peelen LM, Moons KG, Kalkman CJ, Kappelle LJ, van Klei WA. Intraoperative hypotension and perioperative ischemic stroke after general surgery: a nested case–control study. Anesthesiology. 2012;116:658–64.
Maheshwari K, Turan A, Mao G, Yang D, Niazi AK, Agarwal D, Sessler DI, Kurz A. The association of hypotension during non-cardiac surgery, before and after skin incision, with postoperative acute kidney injury: a retrospective cohort analysis. Anaesthesia. 2018;73:1223–8.
Tassoudis V, Vretzakis G, Petsiti A, Stamatiou G, Bouzia K, Melekos M, Tzovaras G. Impact of intraoperative hypotension on hospital stay in major abdominal surgery. J Anesth. 2011;25:492–9.
Monk TG, Bronsert MR, Henderson WG, Mangione MP, Sum-Ping ST, Bentt DR, Nguyen JD, Richman JS, Meguid RA, Hammermeister KE. Association between intraoperative hypotension and hypertension and 30-day postoperative mortality in noncardiac surgery. Anesthesiology. 2015;123:307–19.
Reich DL, Hossain S, Krol M, Baez B, Patel P, Bernstein A, Bodian CA. Predictors of hypotension after induction of general anesthesia. Anesth Analg. 2005;101:622–8.
Südfeld S, Brechnitz S, Wagner JY, Reese PC, Pinnschmidt HO, Reuter DA, Saugel B. Post-induction hypotension and early intraoperative hypotension associated with general anaesthesia. Br J Anaesth. 2017;119:57–64.
Burgos LG, Ebert TJ, Asiddao C, Turner LA, Pattison CZ, Wang-Cheng R, Kampine JP. Increased intraoperative cardiovascular morbidity in diabetics with autonomic neuropathy. Anesthesiology. 1989;70:591–7.
Bein B, Hanss R, Scholz J, Tonner PH. Pre-operative measurement of heart rate variability and incidence of hypotension. Acta Anaesthesiol Scand. 2006;50:1170–1.
Loewenfeld IE, Lowenstein O. The Pupil: Anatomy, Physiology, and Clinical Applications. Oxford: Butterworth Heinemann; 1999.
Muppidi S, Adams-Huet B, Tajzoy E, Scribner M, Blazek P, Spaeth EB, Frohman E, Davis S, Vernino S. Dynamic pupillometry as an autonomic testing tool. Clin Auton Res. 2013;23:297–303.
Guillon M, Dumbleton K, Theodoratos P, Gobbe M, Wooley CB, Moody K. The effects of age, refractive status, and luminance on pupil size. Optom Vis Sci. 2016;93:1093–100.
Borthne A, Davanger M. Mydriatics and age. Acta Ophthalmol. 1971;49:380–7.
Okutucu S, Civelekler M, Aparci M, Sabanoglu C, Dikmetas O, Aksoy H, Yetis Sayin B, Oto A. Computerized dynamic pupillometry indices mirrors the heart rate variability parameters. Eur Rev Med Pharmacol Sci. 2016;20:2099–105.
Boev AN, Fountas KN, Karampelas I, Boev C, Machinis TG, Feltes C, Okosun I, Dimopoulos V, Troup C. Quantitative pupillometry: normative data in healthy pediatric volunteers. J Neurosurg. 2005;103:496–500.
Oddo M, Sandroni C, Citerio G, Miroz JP, Horn J, Rundgren M, Cariou A, Payen JF, Storm C, Stammet P, Taccone FS. Quantitative versus standard pupillary light reflex for early prognostication in comatose cardiac arrest patients: an international prospective multicenter double-blinded study. Intensive Care Med. 2018;44:2102–11.
Jahns FP, Miroz JP, Messerer M, Daniel RT, Taccone FS, Eckert P, Oddo M. Quantitative pupillometry for the monitoring of intracranial hypertension in patients with severe traumatic brain injury. Crit Care. 2019;23:155.
Natzeder S, Mack DJ, Maissen G, Strässle C, Keller E, Muroi C. Portable infrared pupillometer in patients with subarachnoid hemorrhage: prognostic value and circadian rhythm of the Neurological Pupil Index (NPi). J Neurosurg Anesthesiol. 2018. https://doi.org/10.1097/ANA.0000000000000553.
Rollins MD, Feiner JR, Lee JM, Shah S, Larson M. Pupillary effects of high-dose opioid quantified with infrared pupillometry. Anesthesiology. 2014;121:1037–44.
Peduzzi P, Concato J, Kemper E, Holford TR, Feinstein AR. A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol. 1996;49:1373–9.
Ewing DJ, Martyn CN, Young RJ, Clarke BF. The value of cardiovascular autonomic function tests: 10 years experience in diabetes. Diabetes Care. 1985;8:491–8.
Hermida RC, Ayala DE, Fernández JR, Mojón A, Alonso I, Calvo C. Modeling the circadian variability of ambulatorily monitored blood pressure by multiple-component analysis. Chronobiol Int. 2002;19:461–81.
Vandewalle G, Middleton B, Rajaratnam SM, Stone BM, Thorleifsdottir B, Arendt J, Dijk DJ. Robust circadian rhythm in heart rate and its variability: influence of exogenous melatonin and photoperiod. J Sleep Res. 2007;16:148–55.
Lavie P. Ultradian rhythms in alertness—a pupillometric study. Biol Psychol. 1979;9:49–62.
Daguet I, Bouhassira D, Gronfier C. Baseline pupil diameter is not a reliable biomarker of subjective sleepiness. Front Neurol. 2019;10:108.
Loewenfeld IE. Pupillary changes related to age. Baltimore: Williams and Wilkins; 1979.
Iimura O. Insulin resistance and hypertension in Japanese. Hypertens Res. 1996;19(Suppl 1):S1–8.
Henry P, Thomas F, Benetos A, Guize L. Impaired fasting glucose, blood pressure and cardiovascular disease mortality. Hypertension. 2002;40:458–63.
Acknowledgements
We thank Angela Morben, DVM, ELS, from Edanz Group (www.edanzediting.com/ac), for editing a draft of this manuscript.
Funding
Support was provided solely from departmental sources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Miyazaki, R., Sumie, M., Kandabashi, T. et al. Resting pupil size is a predictor of hypotension after induction of general anesthesia. J Anesth 33, 594–599 (2019). https://doi.org/10.1007/s00540-019-02672-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-019-02672-y