Abstract
Objective
The present study examined the objective and patient-reported measures of physical impairments, sensory disturbance, and functional ability between cancer patients with and without chemotherapy-induced peripheral neuropathy (CIPN) symptoms.
Methods
Forty-one cancer survivors exposed to neurotoxic chemotherapies were conveniently recruited and completed a single cross-sectional assessment of patient-reported outcomes (VAS for pain intensity and ABC scale) and objective assessments (SWM test, TUG test, 5xSTS test, Romberg test with eyes open and eyes closed, 6MWT, and FAB scale).
Results
Cancer patients who had undergone chemotherapy with CIPN symptoms did significantly worse in the SWM test, TUG test, 5xSTS test, Romberg test with eyes closed, 6MWT, FAB scale, and ABC scale (p < 0.05) when compared with cancer survivors without CIPN symptoms.
Conclusion
Cancer survivors with CIPN symptoms have lower physical performance, sensory perception, and functional ability, which may increase the risk of falling and disability. These findings further emphasize the need for effective rehabilitation and interventions to treat CIPN symptoms and related physical impairment and functional deficits.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The chemotherapy-induced peripheral neuropathy (CIPN) is the most frequently disabling side effect of neurotoxic chemotherapy agents [1]. The previous systematic review and meta-analysis study showed that the prevalence rate of CIPN symptoms ranges from 19 to 85%, which was highest in the first month after chemotherapy (68.1%), still persisted after 3 months (60.0%), and fell to half at 6 months or more (30.0%) [2]. Chemotherapy agents, especially taxane and platinum compounds, are associated with a high prevalence of CIPN symptoms, ranging from 71 to 83% [3, 4]. Several studies have indicated many clinical risk factors associated with CIPN including the specific drug, dose, schedule, and therapy duration [5,6,7]. CIPN symptoms can precipitate the premature cessation of chemotherapy, which may increase the risks of morbidity and mortality [8, 9].
Falls are associated with the morbidity and mortality rate in patients with cancer [10, 11]. One previous systematic review suggested that patients with cancer are at higher risk of falls than the general population [12]. Moreover, cancer patients who receive neurotoxic chemotherapy are at greater risk of fall than those who are not [13]. A previous study showed that patients with CIPN symptoms have a higher risk of falling three times or more [14], as evidenced by increased mean Time Up and Go (TUG) scores and decreased gait performance (gait speed and step length) [15]. Patients with persistent CIPN symptoms have been identified as experiencing greater functional limitations, greater disability, increased risk of falling, and increased of health care utilization [16]. Moreover, many studies have reported that the functional ability of cancer survivors who receive neurotoxic chemotherapy agents decreases, such as a decrease in the 6-min walk test (6MWT) distance [17], worse short physical performance battery scores [16], lower Fullerton Advanced Balance (FAB) scales, and increased TUG times [18].
Cancer patients with CIPN symptoms usually present sensory impairments (reduction of sensation and perception of joint position) as early symptoms [19, 20]. The Semmes–Weinstein monofilaments (SWM) test is a screening tool for identifying sensory impairment (tactile dysfunction) and is commonly used to detect sensory impairment in a variety of patients, including patients with CIPN symptoms, diabetes, and leprosy [21,22,23]. Although motor impairments such as lower limb muscle weakness, cramp, and foot drop are uncommon in patients with CIPN, previous studies found that such individuals with CIPN symptoms with motor impairments are at increased risk of falls [24]. The five-time sit to stand (5xSTS) test is a valid and reliable measurement tool commonly used to assess lower-extremity strength and balance [25, 26]. Moreover, Winter-stone et al. indicated a high severity of CIPN symptoms associated with increased time to complete the 5xSTS test [16].
To date, there have only been a few studies investigating the physical impairments and functional limitations in cancer patients with and without CIPN symptoms. Therefore, the purpose of this study was to investigate the objective and patient-reported measures of physical impairments, sensory disturbance, and functional limitation between cancer patients with and without CIPN symptom. The hypothesis of this study was that there are differences in physical impairments and functional limitations between cancer patients with and without CIPN symptoms. Such information would provide oncology teams’ information for use in screening patients for referral to rehabilitation teams.
Materials and methods
Participants
Forty-one cancer patients who received a complete first course of chemotherapy treatment were conveniently recruited. Participants were recruited from Chulabhorn hospital in Bangkok, Thailand. Individuals were included if they were 20–70 years of age, had an ECOG score ≤ 2, had completed the first course of chemotherapy treatment (4 to 12 cycles) in the past 30 days before participation with no targeted therapy and radiotherapy before, and were able to read and understand the Thai language. Exclusion criteria were bone metastasis, brain metastasis, bleeding precaution, nerve compression syndrome, current, or past history of underlying diseases that affect neurological deficits (i.e., diabetes mellitus, HIV, alcoholism, SLE, GBS, inherited disorder, or vitamin deficiency). Additionally, our classification of patients with or without CIPN symptoms was based on the CTCAE version 5.0 score, which was obtained during the screening procedure. All subjects were provided information about the study and signed an informed consent form prior to their participation. The study was approved by the Human Research Ethics Committee of Chulabhorn Research Institute (028/2560).
Measures and procedures
Demographics and cancer status
All outcomes used for this analysis were obtained from baseline data collected before patients were allocated to the CIPN or non-CIPN groups. Participants were asked to report age, gender, type of cancer, and pain score using the 100-mm visual analogue scale (VAS). Chemotherapy agents, cumulative dose, and duration of receiving chemotherapy drugs were obtained from medical records. The CTCAE sensory version 5.0 was used to assess the severity of CIPN [27]. The CTCAE grade is a 5-point Likert scale; a grade of 2 is associated with impairment of activities associated with normal daily life, which may relate to falling [28]. Therefore, in this study, the CTCAE score was used to classify patients with CIPN symptoms (≥ 2 score) and without CIPN symptoms (< 2 score).
Semmes–Weinstein monofilaments (SWM) test
The sensory assessment was tested using Semmes–Weinstein monofilaments (SWM) (Monofilament, Berlin Pharmaceutical Industry, Bangkok, Thailand). The SWMs are used to determine light touch sensation in various populations [21,22,23]. In this study, the SWM testing was performed with monofilament 5.07 (10 g) applied to the surface of the skin in an up-down fashion on both feet of the subject. The assessment was conducted in a quiet setting and subjects were instructed to close their eyes during the test. First, the monofilament was applied to the subject’s forearm and they were asked about the feeling and location of the test to ensure the subject’s understanding. All subjects were tested at four points in both feet three times including the plantar surface of the hallux, and the first, third, and fifth metatarsal heads in each foot. The monofilament was applied to the skin for approximately 1.5 s in each area. Subjects were asked to name the exact location where a monofilament was detected. If subjects perceived the test location correctly 2 out of 3 times, the subject’s sensory score was noted as intact.
Timed Up and Go (TUG) test
The Timed Up and Go (TUG) test was used to determine functional mobility and the ability to maintain balance while walking. The TUG was measured using a standard chair (seat height 43 cm) and the subject’s usual walking aid. The subject was asked to get up from the chair, walk 3 m to a line of colored tape on the floor, turn around and return to the chair, and sit back down. The stopwatch was started when the subject’s buttocks lifted from the seat, and the timing was completed when the buttocks retouched the chair.
Five-time sit to stand (5xSTS) test
The five-time sit to stand (5xSTS) test was used to measure functional ability and lower limb muscle strength. Participants were asked to stand up from a standard chair (seat height: 43 cm) as quickly as possible for five times without any hand support. The time to finish 5xSTS was recorded as an outcome measure.
Romberg test
The body’s sense of positioning (proprioception) was measured by using the Romberg test, which is a part of the standard neurological assessment. A positive result of the Romberg test indicates the presence of a neurological disease. Participants were instructed to remain still with both feet together and cross their arms for a period of 30 s. The researcher asked the participants to perform the test twice (open eyes and closed eyes). The test was initiated when the participants assumed the correct position and stopped when they moved their feet, lost the positioning of their upper limbs, or opened their eyes. The duration for which the subjects could maintain balance was defined as the balance time (in seconds).
6-min walk test (6MWT)
The 6-min walk test (6MWT) was performed according to international guidelines. Participants were instructed to walk at their own pace while attempting to cover the greatest distance possible. Standardized encouragement was provided every minute by telling the patients either “You are doing well” or “Keep up the good work” and informing them of the remaining time. The tests were supervised by qualified staff that walked behind the participant. Participants were permitted to stop (if required) during the test but were also instructed to resume walking once able. The 6MWT was registered in meters and patients were allowed to use their walking aids during the tests.
Fullerton advanced balance scale (FAB)
The Fullerton advanced balance scale (FAB) was used to test the functional balance state of individuals. The FAB scale is a balance scale with a 5-point ordinal scale (0–4) for each item and a maximum score of 40 points (higher values indicate better performance). The FAB scale consists of 10 items: balancing with the feet together and eyes closed, forward reach, turn 360 degrees, stepping up, onto and over a 6-inch bench, tandem walk, standing on one leg, standing on foam with eyes closed, two-footed jump, walking with head turns, and postural reaction.
Activities-Specific Balance Confidence scale (ABC scale)
The Activities-Specific Balance Confidence scale (ABC scale) is used to measure the balance confidence of a patient during performing various activities. The ABC scale is a 16-item self-report questionnaire, which is rated on a scale ranging from 0–100 (0 denotes no confidence and 100 denotes complete confidence).
Statistical analysis
Participants’ characteristics, type of cancer, cumulative dose of chemotherapy drugs, and pain score, and a number of CIPN and non-CIPN cases were described by means or proportions. The independent t test for continuous data and the chi-square test for non-continuous data were used to determine baseline group differences. The relationships between the cumulative doses of chemotherapy drugs and the severity of CIPN symptoms (CTCAE score in sensory and motor) were examined using the Pearson correlation coefficients. The Shapiro–Wilk test was performed to check the distribution of data; the results indicated non-normal distribution. Therefore, the physical impairment and functional ability data between CIPN and non-CIPN groups were analyzed by the Mann–Whitney U test. All statistical analyses were conducted using SPSS statistical software, version 23.0 (SPSS Inc., Chicago, IL, USA). Statistical significance was accepted for values of p < 0.05.
Results
A total of 41 cancer patients participated in the study (Fig. 1). Table 1 presents the characteristics of the participants. The sample population comprised mainly middle-aged females. Their average BMI was in the normal range. The majority of participants (56%) had breast cancer. Of the participants, 46% received 6 cycles of chemotherapy drugs (3 weeks between cycles). Only paclitaxel was given to 56.1% of the participants, while 43.9% received both paclitaxel and carboplatin. According to the CTCAE sensory score, 13 participants were classified as belonging to the CIPN group and 28 participants to the non-CIPN group. There were no significant differences in any of the characteristics of the participants between two groups, except for CTCAE sensory, CTCAE motor, and pain score using VAS. All of the patients in this study were able to walk without assistance or mobility aids.
To investigate the effect of gender and type of cancer, we compared the results from 41 to 37 patients (excluding 4 participants who were men and lung cancer patients). No alteration of the finding was found between the two sets of data. Therefore, the results from the 41 participants (including the 4 participants who were men and lung cancer patients) are given below.
For the association between cumulative doses of chemotherapy drugs and the severity of CIPN symptoms (CTCAE score in sensory and motor), there was no significant relationship between the cumulative doses and severity of CIPN symptoms (r = 0.09, p = 0.57 for CTCAE score in sensory and r = 0.25, p = 0.11 for CTCAE score in motor). In this study, some participants in the non-CIPN group had more cumulative doses of the chemotherapy drugs than those in the CIPN group. In Table 1, the average cumulative doses of chemotherapy drugs in the non-CIPN group were higher than in the CIPN group. However, no significant difference was found (p = 0.87).
Physical impairment and functional performance
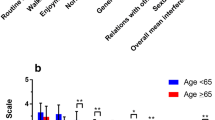
Table 2 summarizes the results of the monofilaments test, Timed Up and Go test, 5-time sit to stand test, Romberg test, 6-min walk test, Fullerton advanced balance scale, and Activities-Specific Balance Confidence Scale in the CIPN and non-CIPN groups.
The Mann–Whitney U test revealed there was a significant difference in the SWM test, TUG test, 5xSTS test, Romberg test with eyes closed, 6MWT, FAB scale, and ABC scale between CIPN and non-CIPN groups (p < 0.05). No significant difference was found in the Romberg test with eyes open.
Discussion
The present study demonstrated the physical impairments, sensory disturbance, and functional ability between cancer patients with and without CIPN symptoms. The Mann–Whitney U test was used to evaluate the differences in the SWM test, TUG test, 5xSTS test, Romberg test, 6MWT, FAB scale, and ABC scale between CIPN and non-CIPN groups. The findings of this study showed that cancer patients with CIPN symptoms had a significantly more physical impairment, sensory disturbance, and functional limitation, which may partly lead to a fall in patients with CIPN symptoms.
Our results indicated the monofilaments score in the CIPN group was significantly lower than those in the non-CIPN group. The SWM test is the most common tool used to evaluate the sensory disturbance in patients with diabetes mellitus and determine changes in light touch sensation in patients with CIPN symptoms [21, 22, 29, 30]. The results of the present study are in line with the findings of previous studies showing that cancer survivors with CIPN symptoms have significantly lower monofilaments scores when compared with cancer survivors without CIPN symptoms [21]. Possible causes of sensory change are the accumulation of neurotoxic chemotherapy drugs in the dorsal root ganglia (DRG) and its ability to pass through the blood-nerve barriers, which leads to sensory neuron damage and alterations of sensory perception regarding touch, pinpricks, and vibrations [31]. Moreover, the CIPN group was significantly weaker in their lower extremities using the 5xSTS test, which was used to assess lower limb muscle strength [32]. Our results are consistent with Winter-Stone et al.’s (2017) study, showing women with CIPN symptoms performed significantly worse on the 5xSTS test when compared with women without CIPN symptoms [16]. To our knowledge, taxane-based chemotherapy agents may induce sensory and motor neuropathy according to which nerve fibers are affected [4]. Lower-extremity motor neuron impairment can cause muscle weakness and is associated with reducing lower-extremity physical function [33]. The findings of this study lend further support to the notion that cancer patients with CIPN symptoms may be at increased risk of falling and disability.
This study found that the CIPN group had significantly less functional capacity, as assessed by 6MWT, when compared to the non-CIPN group. These results are similar to those of McCrary et al. (2019), which showed that increased CIPN symptom severity was significantly associated with decreased 6MWT distance in cancer patients [17]. However, the 6MWT distance of patients with CIPN symptoms in this study was greater than our study (416.4 m and 295.5 m). One possible explanation for this finding is the difference in the gender proportions between the two studies. McCrary et al.’s (2019) study was near equal between male (40%) and female (60%) subjects but in our study most participants were female (92.3%). The literature suggests that gender might be associated with 6MWT distance [17]. Unsurprisingly, males have greater muscle strength and are taller than females and are associated with a longer stride. This is one possible reason resulting in the greater 6MWT distance in males when compared with females.
The results of this study indicate that cancer patients with CIPN symptoms have significantly less balance ability and postural control according to the TUG test, Romberg test with eyes closed, and FAB scale. Our results are similar to a previous study that determines balance and postural control in cancer patients [18]. Wampler et al. (2007) study showed that breast cancer patients had worse balance and postural control based on TUG time and FAB score when compared with healthy women’s control (TUG: 6.69 ± 0.994 and 5.85 ± 0.86; p < 0.008, and FAB: 33.90 ± 3.46 and 36.48 ± 2.13; p < 0.02) [18]. The postural control components, which include the interaction between the musculoskeletal and sensorimotor integration systems, are associated with the ability to control balance [34]. A previous study suggested that FAB and TUG were related to many components of postural control including the musculoskeletal, muscle synergies, sensory system, sensory organization, postural orientation, reactive balance system, and proactive balance system [18, 34, 35]. Moreover, Einarsson et al. found that patients who had neurotoxic side effects from chemotherapy agents might have reduced sensorimotor adaptation and poor balance performance [36]. In addition, cancer patients with CIPN symptoms who had positive Romberg signs with the eyes closed, an indication of problems in sensory ataxia, were found to be significantly associated with an increased risk of falling [37]. To our knowledge, chemotherapy agents can have toxic effects on the sensory and motor fibers, leading to sensory ataxia and balance problems [14, 16]. Therefore, sensory ataxia or low balance ability may contribute to the risk of falls among cancer patients.
In addition, we found that the balance confidence score using the ABC scale in the CIPN group was significantly less than the non-CIPN group. Previous studies suggested that patients with CIPN symptoms might experience reduced sensation and proprioception in their lower extremities and this leads to an increased risk of fall [14, 16]. Moreover, a recent study suggested that patients who have a high risk of falls might develop a fear of falling which restricts their mobility [38]. The results of Huang et al.’s (2016) study found that the individual’s self-reported balance confidence using the ABC scale was strongly associated with TUG. Balance confidence is a strong predictor of perceived mobility limitations during daily activities in older cancer survivors [39]. Thus, thorough screening or monitoring of the balance confidence of patients who received neurotoxic chemotherapy and have CIPN symptoms may facilitate effective strategies for fall prevention.
Based on our findings, CIPN symptoms should be screened earlier in the clinical pathway and used as potential information for referral to rehabilitation teams. We suggest that rehabilitation or physical therapy programs for improving physical and functional abilities should be provided to the cancer patients who receive neurotoxic agents, especially those with CIPN symptoms [40, 41]. Also, oncologists planning to use neurotoxic agents should perform pre-treatment functional assessments and repeat these at intervals during and after treatment to prevent and reduce physical impairment and functional limitation, which improve patient health and survivorship care plans.
A strength of the present study is the use of several objective measurements for assessing physical impairments, sensory disturbance, and functional abilities. However, there are a number of methodological limitations that are noteworthy. First, the sample size was relatively small (n = 41), increasing the likelihood of a type II error. Future studies with a larger sample size are required to confirm the present study findings. Second, cancer patients in this study had normal BMI, had no underlying diseases that affect neurological deficits (i.e., diabetes mellitus, HIV, alcoholism, SLE, GBS, inherited disorder, or vitamin deficiency), and were recruited by convenience sampling without controlling the nutritional status, body habitus, and treatment toxicity, which limits the external validity. Thus, generalization of the findings from our study to patients with other diseases, in which also a proportion are overweight and obese, should be made with caution. Third, the group sizes in this study were unequal, which diminishes statistical power. Therefore, equal group size is recommended for future study. Fourth, this study only assessed the sensory disturbance using the Semmes–Weinstein monofilament test, which might not cover the sensory function. Future study should examine other sensory testing such as temperature, vibration, and reflex examinations in cancer patients with and without CIPN symptoms. Finally, because this study design is cross-sectional, it is impossible to determine the nature of the change in CIPN symptoms during chemotherapy treatment. Only the relationship between exposure and outcome was investigated. As a result, future studies should examine the pre-treatment assessments of function and inquire about falls to establish the sequence of events after receiving chemotherapy. More research with a prospective study design is needed to confirm our findings.
Conclusions
The present study revealed that cancer survivors who have undergone chemotherapy with CIPN symptoms have lower physical performance, sensory perception, and functional ability when compared with cancer survivors without CIPN symptoms. In addition, these results indicate that patients with CIPN symptoms may be at increased risk of falling and disability. For cancer patients with CIPN symptoms, customizing rehabilitation program to prevent and reduce physical impairment and functional limitation could improve patient health and survivorship care plans.
Availability of data and material
The data that support the findings of this study are available on request from the corresponding author (Pooriput). The data are not publicly available due to ethical restrictions.
Code availability
Not applicable.
References
Iżycki D, Niezgoda A, Kaźmierczak M, Nowak-Markwitz E (2016) Chemotherapy-induced peripheral neuropathy - epidemiology and pathogenesis. Ginekol Pol 87:293–299
Seretny M, Currie GL, Sena ES, Ramnarine S, Grant R, MacLeod MR, Colvin LA, Fallon M (2014) Incidence, prevalence, and predictors of chemotherapy-induced peripheral neuropathy: a systematic review and meta-analysis. Pain® 155:2461–2470
Molassiotis A, Cheng HL, Leung KT, Li YC, Wong KH, Au JSK, Sundar R, Chan A, Ng TR, Suen LKP, Chan CW, Yorke J, Lopez V (2019) Risk factors for chemotherapy-induced peripheral neuropathy in patients receiving taxane- and platinum-based chemotherapy. Brain Behav 9:e01312
Rivera E, Cianfrocca M (2015) Overview of neuropathy associated with taxanes for the treatment of metastatic breast cancer. Cancer Chemother Pharmacol 75:659–670
Chaudhry V, Rowinsky EK, Sartorius SE, Donehower RC, Cornblath DR (1994) Peripheral neuropathy from taxol and cisplatin combination chemotherapy: clinical and electrophysiological studies. Ann Neurol 35:304–311
Chaudhry V, Chaudhry M, Crawford TO, Simmons-O’Brien E, Griffin JW (2003) Toxic neuropathy in patients with pre-existing neuropathy. Neurology 60:337–340
Goel S, Goldberg GL, Kuo DY, Muggia F, Arezzo J, Mani S (2008) Novel neurosensory testing in cancer patients treated with the epothilone B analog, ixabepilone. Ann Oncol 19:2048–2052
Cavaletti G, Frigeni B, Lanzani F, Mattavelli L, Susani E, Alberti P, Cortinovis D, Bidoli P (2010) Chemotherapy-induced peripheral neurotoxicity assessment: a critical revision of the currently available tools. Eur J Cancer 46:479–494
Loprinzi CL, Lacchetti C, Bleeker J, Cavaletti G, Chauhan C, Hertz DL, Kelley MR, Lavino A, Lustberg MB, Paice JA, Schneider BP, Lavoie Smith EM, Smith ML, Smith TJ, Wagner-Johnston N, Hershman DL (2020) Prevention and management of chemotherapy-induced peripheral neuropathy in survivors of adult cancers: ASCO guideline update. J Clin Oncol 38:3325–3348
Tinetti ME, Williams CS (1997) Falls, injuries due to falls, and the risk of admission to a nursing home. N Engl J Med 337:1279–1284
(2006) Fatalities and injuries from falls among older adults--United States, 1993–2003 and 2001–2005. MMWR Morb Mortal Wkly Rep 55:1221–1224
Wildes TM, Dua P, Fowler SA, Miller JP, Carpenter CR, Avidan MS, Stark S (2015) Systematic review of falls in older adults with cancer. J Geriatr Oncol 6:70–83
Ward PR, Wong MD, Moore R, Naeim A (2014) Fall-related injuries in elderly cancer patients treated with neurotoxic chemotherapy: a retrospective cohort study. J Geriatr Oncol 5:57–64
Kolb NA, Smith AG, Singleton JR, Beck SL, Stoddard GJ, Brown S, Mooney K (2016) The association of chemotherapy-induced peripheral neuropathy symptoms and the risk of falling. JAMA Neurol 73:860–866
Marshall TF, Zipp GP, Battaglia F, Moss R, Bryan S (2017) Chemotherapy-induced-peripheral neuropathy, gait and fall risk in older adults following cancer treatment. J Cancer Res Pract 4:134–138
Winters-Stone KM, Horak F, Jacobs PG, Trubowitz P, Dieckmann NF, Stoyles S, Faithfull S (2017) Falls, functioning, and disability among women with persistent symptoms of chemotherapy-induced peripheral neuropathy. J Clin Oncol 35:2604–2612
McCrary JM, Goldstein D, Wyld D, Henderson R, Lewis CR, Park SB (2019) Mobility in survivors with chemotherapy-induced peripheral neuropathy and utility of the 6-min walk test. J Cancer Surviv 13:495–502
Wampler MA, Topp KS, Miaskowski C, Byl NN, Rugo HS, Hamel K (2007) Quantitative and clinical description of postural instability in women with breast cancer treated with taxane chemotherapy. Arch Phys Med Rehabil 88:1002–1008
Stubblefield MD, Burstein HJ, Burton AW, Custodio CM, Deng GE, Ho M, Junck L, Morris GS, Paice JA, Tummala S, Von Roenn JH (2009) NCCN task force report: management of neuropathy in cancer. J Natl Compr Canc Netw 7(Suppl 5):S1–S26; quiz S27-28
Wickham R (2007) Chemotherapy-induced peripheral neuropathy: a review and implications for oncology nursing practice. Clin J Oncol Nurs 11:361–376
da Silva Simão DA, Teixeira AL, Souza RS, de Paula Lima ED (2014) Evaluation of the Semmes-Weinstein filaments and a questionnaire to assess chemotherapy-induced peripheral neuropathy. Support Care Cancer 22:2767–2773
Dros J, Wewerinke A, Bindels PJ, van Weert HC (2009) Accuracy of monofilament testing to diagnose peripheral neuropathy: a systematic review. Ann Fam Med 7:555–558
Saranjit W, Penvadee P, Onjuta C, Kamonpan L, Pacharee I, Suteeraporn C (2015) Comparison between different methods of monofilament test in multibacillary leprosy. J Med Assoc Thai 98:1124–1132
Gewandter JS, Fan L, Magnuson A, Mustian K, Peppone L, Heckler C, Hopkins J, Tejani M, Morrow GR, Mohile SG (2013) Falls and functional impairments in cancer survivors with chemotherapy-induced peripheral neuropathy (CIPN): a University of Rochester CCOP study. Support Care Cancer 21:2059–2066
Goldberg A, Chavis M, Watkins J, Wilson T (2012) The five-times-sit-to-stand test: validity, reliability and detectable change in older females. Aging Clin Exp Res 24:339–344
Griffith KA, Couture DJ, Zhu S, Pandya N, Johantgen ME, Cavaletti G, Davenport JM, Tanguay LJ, Choflet A, Milliron T, Glass E, Gambill N, Renn CL, Dorsey SG (2014) Evaluation of chemotherapy-induced peripheral neuropathy using current perception threshold and clinical evaluations. Support Care Cancer 22:1161–1169
US Department of Health Human Services (2017) Common terminology criteria for adverse events (CTCAE) version 5.0. Retrieved from https://ctep.cancer.gov/protocolDevelopment/electronic_applications/docs/CTCAE_v5_Quick_Reference_8.5x11.pdf
Komatsu H, Yagasaki K, Komatsu Y, Yamauchi H, Yamauchi T, Shimokawa T, Doorenbos AZ (2019) Falls and functional impairments in breast cancer patients with chemotherapy-induced peripheral neuropathy. Asia Pac J Oncol Nurs 6:253
Miaskowski C, Mastick J, Paul SM, Topp K, Smoot B, Abrams G, Chen LM, Kober KM, Conley YP, Chesney M, Bolla K, Mausisa G, Mazor M, Wong M, Schumacher M, Levine JD (2017) Chemotherapy-induced neuropathy in cancer survivors. J Pain Symptom Manage 54:204-218.e202
Molassiotis A, Cheng HL, Lopez V, Au JSK, Chan A, Bandla A, Leung KT, Li YC, Wong KH, Suen LKP, Chan CW, Yorke J, Farrell C, Sundar R (2019) Are we mis-estimating chemotherapy-induced peripheral neuropathy? Analysis of assessment methodologies from a prospective, multinational, longitudinal cohort study of patients receiving neurotoxic chemotherapy. BMC Cancer 19:132
Velasco R, Bruna J (2015) Taxane-induced peripheral neurotoxicity. Toxics 3:152–169
Guralnik JM, Simonsick EM, Ferrucci L, Glynn RJ, Berkman LF, Blazer DG, Scherr PA, Wallace RB (1994) A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 49:M85-94
van Schie CH (2008) Neuropathy: mobility and quality of life. Diabetes Metab Res Rev 24(Suppl 1):S45-51
Shumway-Cook A, Woollacott MH (2007) Motor control: translating research into clinical practice. Lippincott Williams & Wilkins
Schlenstedt C, Brombacher S, Hartwigsen G, Weisser B, Möller B, Deuschl G (2015) Comparing the Fullerton Advanced Balance Scale with the Mini-BESTest and Berg Balance Scale to assess postural control in patients with Parkinson disease. Arch Phys Med Rehabil 96:218–225
Einarsson E-J, Patel M, Petersen H, Wiebe T, Fransson P-A, Magnusson M, Moëll C (2016) Decreased postural control in adult survivors of childhood cancer treated with chemotherapy. Sci Rep 6:36784
Argyriou AA, Bruna J, Anastopoulou GG, Velasco R, Litsardopoulos P, Kalofonos HP (2020) Assessing risk factors of falls in cancer patients with chemotherapy-induced peripheral neurotoxicity. Support Care Cancer 28:1991–1995
Kang GE, Najafi B (2020) Sensor-based daily physical activity: towards prediction of the level of concern about falling in peripheral neuropathy. Sensors 20:505
Huang MH, Righter A, Shilling T (2016) Self-reported balance confidence relates to perceived mobility limitations in older cancer survivors. Rehabilitation Oncology 34:64–71
Kleckner IR, Park SB, Streckmann F, Wiskemann J, Hardy S, Mohile N (2021) Clinical and practical recommendations in the use of exercise, physical therapy, and occupational therapy for chemotherapy-induced peripheral neuropathy. Diagnosis, Management and Emerging Strategies for Chemotherapy-Induced Neuropathy. Springer, pp 243–252
Brayall P, Donlon E, Doyle L, Leiby R, Violette K (2018) Physical therapy–based interventions improve balance, function, symptoms, and quality of life in patients with chemotherapy-induced peripheral neuropathy: a systematic review. Rehabil Oncol 36:161–166
Acknowledgements
The authors would like to thank Mr. Pasanut Panuraksirikul for his help with the data collection.
Author information
Authors and Affiliations
Contributions
The authors have contributed in the following ways: N. R. provided the concept/research design, data collection, and manuscript writing. C. S. and N. P. provided the concept/research design and data collection. P. W. contributed to the concept/research design, data analysis, and manuscript writing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the Human Research Ethics Committee of Chulabhorn Research Institute (028/2560). All included patients provided signed informed consents prior to participation in the study.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
All of the authors read the final version of the paper and approved its submission for publication.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rattanakrong, N., Promma, N., Saraboon, C. et al. Physical impairments, sensory disturbance, and functional ability in a cancer patient with and without chemotherapy-induced peripheral neuropathy symptoms. Support Care Cancer 30, 5055–5062 (2022). https://doi.org/10.1007/s00520-022-06927-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-022-06927-5