Abstract
Purpose
Among Chinese breast cancer survivors, treatment decision-making is different than that in western countries. Among Chinese women, family often plays an important role during the treatment period, and Chinese-specific cultural factors have negative influences on their psychological conditions. The aim of the present study was to explore the treatment decision making, family influences, and cultural influences of Chinese breast cancer survivors.
Methods
This study used an expressive writing method to explore the experiences of breast cancer survivors who were diagnosed with stage 0 to III cancer. Participants were instructed to write 30 min per week over a period of 3 weeks. All writings were analyzed using a qualitative method.
Results
Three themes were identified: treatment decision making, family influences, and cultural influences. Treatment decision-making included the subthemes of preference for mastectomy, passive involvement, and active involvement. Family influences included the subthemes of financial burden, family expectations, and family support. Cultural influences included the subthemes of fatalism, barriers to expressing emotions, and stigma related to cancer.
Conclusions
Information on breast cancer treatment and survivorship should be provided to patients through multiple methods to improve their knowledge of breast cancer. Family support should be maintained to ensure patients’ confidence and courage during the treatment period. Necessary and appropriate psychological interventions that consider cultural influences should be administered.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Breast cancer is the most common cancer among women worldwide. In China, an estimated 268,600 new breast cancer cases and 69,500 cancer deaths occurred in 2015, accounting for 15.1% of all new cancer cases and 6.9% of all cancer deaths [1, 2]. The epidemiology of Chinese breast cancer is different from that in western countries. While the median age at diagnosis is 64 years in the USA, it is 48–50 years in China [3]. A survey suggested that nearly two-thirds of patients with breast cancer in China are diagnosed with advanced disease. In contrast, in the USA, 60% of women are diagnosed at stages I and II, 33% re-diagnosed at stage III, and only 5% are diagnosed at stage IV [3]. Therefore, compared with breast cancer in Western countries, breast cancer in China is characterized by a younger age and more advanced disease at diagnosis.
Facing this health burden, the control of breast cancer in China is more focused on treatments, while the psychosocial support needs of patients are given little attention by the physicians and the healthcare providers.
When confronted with a breast cancer diagnosis, Chinese women tend to feel fearful, stressed, and even emotionally overwhelmed [4]. Breast cancer survivors also still experience negative life changes, including fear of recurrence, experience of symptoms, poor body image, altered sexuality and intimacy, and financial burden [5]. Psychological problems may occur in the periods of both diagnosis and long-term survival. Some women may seek psychosocial support from family, but few seek support from professional psychological counseling providers. Chinese cultural philosophies, which are completely different from western cultural foundations, shape individual perceptions of disease. Influenced by traditional culture, Chinese people are not willing to talk about their feelings and thoughts in public, especially regarding cancer-related issues [6]. Therefore, there are barriers to self-expression that have negative impacts on their psychological conditions.
Expressive writing is a psychological intervention that can allow people to disclose their thoughts and beliefs that are not openly discussed and therefore helps them overcome communication barriers [7]. To date, there have been two qualitative studies using an expressive writing approach to research Chinese American breast cancer survivors [8, 9]. Lu’s research focused on the beliefs and thoughts of breast cancer survivors. She found that the participants feared death when diagnosed and tended to undergo surgery immediately. She also found that the participants preferred to have a mastectomy for safety, which then had impacts on their body image [8]. Warmoth’s study focused on cultural issues and challenges related to immigrant status [9]. Our study in mainland China was conducted in a similar Chinese cultural context but different medical and social environments from these two previous studies, and it focused more on treatment decision making, family influences, and cultural influences, yielding some similar but unique results.
Methods
Participants
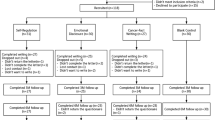
Forty-four Chinese breast cancer survivors were recruited from Weifang People’s Hospital for the expressive writing study. The inclusion criteria were as follows: (1) a stage 0 to stage III breast cancer diagnosis, (2) within 1 year from the time of diagnosis, and (3) ability to write and speak in Chinese. The detailed demographic characteristics are listed in Table 1.
Procedure
Ethical approval was obtained from the Research Ethics Committee of Weifang Medical University (No. 2014--317), and written informed consent was obtained from all the participants. The first author contacted all participants in the hospital to talk about their cancer experience. After the author gained their trust, the participants were given three sealed envelopes and asked to complete three essays in the next 3 weeks. The envelopes were labeled “week 1,” “week 2,” and “week 3” and contained writing instructions for the corresponding week. The participants were asked to open each envelope only at the scheduled writing time and to write continuously for up to 30 min (a standard time limit for expressive writing methodology) each week in Chinese at home. They were asked to write about their deepest thoughts and feelings regarding their cancer diagnosis and treatment (week 1), their most stressful experiences related to cancer and treatment (week 2), and their positive experiences related to breast cancer (week 3). This writing task aimed to facilitate emotional disclosure, effective coping, and benefit finding to make the participants aware of their stress and personal goals and to help them regulate their thoughts and emotions related to their cancer experiences. They wrote a minimum of one page and a maximum of three pages.
The participants were asked to write in a private place to avoid disturbance. They sent their essays back to the hospital by mail or brought them back when they had treatment or follow-up. The participants were compensated with gifts for completing the three writing essays.
Data analysis
A phenomenological research method was employed in the data analysis phase that involved collecting and reading the written data, dividing the data into parts, organizing and interpreting the data from a disciplinary perspective, and synthesizing and summarizing the data for communication to the scholarly community [10]. The detailed procedure was as follows: (1) The authors transcribed the participants’ essays into word documents. (2) The authors read all the essays to understand the overall meaning of the essays. (3) The authors reviewed all the transcripts, identifying meaningful units that represented meanings relevant to the study. (4) Meaningful units expressed in everyday language were examined, probed, and translated into disciplinary language. (5) Line-by-line content analysis was conducted to synthesize the relevant content to identify themes and subthemes. Any divergences were discussed between the authors, and a consensus was reached. As the authors conducted rereadings and discussions, they added new subthemes and themes and deleted preidentified themes as necessary. The five phases were repeated until all researchers agreed on the themes and subthemes extracted from the transcript.
Results
Themes, subthemes and, participants frequency are listed in Table 2.
Treatment decision-making
Preference for mastectomy
When faced with a breast cancer diagnosis, some participants thought that mastectomy was an appropriate method to save their lives.
ID 6: The doctor asked me to decide on the surgery plan as soon as possible. Under the pressure of sadness, my brain was running quickly; I made a total mastectomy decision. At that moment, I thought nothing was more important than life. As long as it would save my life, any kind of sacrifice was worth it.
Even some participants who were candidates for breast-conserving surgery were still preferred to have a radical mastectomy. They considered radical mastectomy to be safer, as they thought mastectomy could remove all the cancer cells. Because of their lack of medical knowledge, some participants believed that there was no need to worry after a total mastectomy.
ID 9: The doctor asked me to choose the surgical method. Without hesitation, I chose a radical mastectomy because it would remove all the bad cells, leaving healthy cells.
ID15: After the radical mastectomy was done, I had no worries anymore.
Passive involvement
Because of the lack of knowledge and experience in cancer treatment, some participants felt very fearful and stressed and did not know what to do when faced with the diagnosis. These participants, especially those who were older or of lower educational levels, tended to take passive roles in treatment decision-making and delegated decision-making to their doctors or family.
ID20: After the surgery, my family gradually told me about the disease. I was very scared of surgery, and I totally didn’t want to have surgery. My husband made the decision that I had to undergo surgery.
ID26: The diagnosis of cancer scared me and made me completely out of my mind; my family members made a decision to have a radical mastectomy. When it came to my senses, the surgery was already done.
Active involvement
A very small proportion of participants took active roles in treatment decision-making. By seeking relevant information, they learned that breast cancer was not an incurable disease and that they could achieve long-term survival with standard treatment. By developing a rational and clear understanding of the disease, they were able to make the appropriate decisions by themselves.
ID19: The doctor said I had stage II invasive breast cancer with lymph node metastasis. I was 59 and did not care about my appearance and fertility as young women did. After discussing it with my husband and daughter, I made the decision to have a mastectomy.
ID7: At the beginning of the diagnosis, I knew nothing about breast cancer. I learned a lot about it from the website and the brochure provided by the hospital. I knew that breast cancer was not incurable, and I believed the disease was like a serious cold that would take more time to heal.
Family influences
Financial burden
In China, the diagnosis of cancer is not only an individual event but also a family crisis. It is a family crisis mainly because of the financial burden during the treatment period. Many participants perceived financial distress to be a result of cancer treatment. Surgery, chemotherapy, radiotherapy, and targeted therapy could cost a large amount of money, and some participants, especially those without medical insurance, could not afford them.
ID2: The several periods of chemotherapy cost a lot. Our family’s income is very limited, and now, our family is in a “financial crisis.”
ID4: Since I have had the disease, the economic status of my family has been lower than ever. The costs of surgery were near 30,000 RMB, and with chemotherapy, the costs could be 50,000–60,000 RMB. There was endocrine therapy for 5 years afterwards, and I didn’t know the exact costs of the whole treatment. Considering the two children’s schooling costs, there was indeed financial pressure.
Family expectations
Some women were determined to survive the sickness for reasons other than their personal intentions. In addition, they believed they had a responsibility to survive, not just for themselves but for their families. These beliefs were often tied to obligations of maintaining family harmony and preventing additional distress and burden for other family members. Some women tried their best to meet family expectations to undergo treatment and try to recover despite their reluctance to endure painful and distressing treatments.
ID11: When diagnosed with such a disease, I just wanted to let myself go. But sometimes, I would think, if I were gone, how my parents could accept this horrible news? How sad they will be when they take part in my funeral. My mother had cardiovascular disease for many years, how could she bear this?
ID14: Sometimes I fell sleep crying, worrying about, how sad my husband, children, parents and siblings would be if I could not overcome the illness. If I were gone, it would be tragic to leave them in this world. I should stay alive for them.
Family support
The participants used different adjustment methods to reduce their suffering during cancer treatment. Family support was an important theme in the essay content. In most situations, the survivors wanted to seek familial emotional support. Family involvement also influenced the women’s decisions about which treatment procedure to pursue. Family beliefs seemed to be a strong determinant of whether the participants underwent a treatment.
ID17: Without the support of my family, I could not make it. The familial support makes me believe there's still hope in life. And I have to be strong and not let my husband and children worry.
ID15: As the saying goes, misfortune tests the sincerity of friends. In the face of the cruel reality, my husband always accompanied me, showed forbearance with me, cared for me and loved me.
Cultural influences
Fatalism
Chinese people seem to have strong beliefs in external control, which means fatalism played an important role in the participants’ perceptions of cancer treatment. In China, cancer is thought to be due to immoral behavior by the individual or an ancestor and that cancer is the result of karma or bad luck. Many of the participants exhibited passive cognitive appraisals of cancer through their fatalistic beliefs about the consequences. These fatalistic beliefs made them think that they were unable to change the final outcome of the illness. They were tempted to keep the disease a secret from others to avoid being associated with bad luck or adversity.
ID8: After I became ill, my beliefs about the world collapsed. Since everything is settled and fated at the time we were born, I would rather believe in ghosts and gods. I must have been too arrogant before, so the gods punished me.
ID9: God controls human life and decides whether people live or die. All is God's arrangement, and all is fated.
Barriers to expressing emotions
It was somewhat difficult for the participants to express their true emotions and feelings because they did not want to burden their family members.
ID1: Although I felt very anxious and stressed, I had to behave as if nothing wrong had happened. Unless I was too weak to work, I pretended to be happy as a normal person. I didn’t tell my mother about the diagnosis because I was worried that she could not accept the truth. I didn’t tell my son about the diagnosis because I didn’t want him to worry about it. I didn’t tell my husband about the diagnosis because I didn’t want to burden him. Sometimes, I felt like I was wearing a mask to live.
Stigma related to cancer
In Chinese culture, acting normal is a routine in interpersonal relationships. This behavior may also be interpreted as one domain of the attributes of “saving face”. In the Chinese context, acting normal may be interpreted as a strategy to maintain the integrity of social interactions and avoid stigma. Chinese culture values emotional suppression as a way to avoid disturbing the harmonious equilibrium of interpersonal relationships. This value of emotional suppression set barriers to the participants’ ability to express emotions and led to their refusal to communicate with others.
ID24: I have changed a lot because of the sickness. I used to love to communicate with my friends, but now I do not like to meet them due to not wanting them to know about my disease.
ID30: With hair loss, I was becoming very afraid of startled looks from strangers. People were dodging me as if I was the god of the plague. Without others’ understanding, I felt lonely and could not tell anybody else.
Beliefs in traditional Chinese medicine
Some participants especially with older age believed the traditional Chinese medicine (TCM). And these people would prefer to seek for the TCM when they were attacked by a specific disease, as they thought the TCM were an effective treatment with little side-effects.
ID2: Through what learn about the breast cancer, I believe that western medicine cures the symptoms, while Chinese medicine cures the root.
Discussion
Qualitative research methods have provided insight into the thoughts and beliefs of Chinese breast cancer survivors. Qualitative findings have provided details on survivors’ psychological conditions during decision-making and treatment periods. In 2003, Lam conducted the first qualitative study that described how Chinese women made sense of their breast cancer experiences [4]. These women reported that the ever-changing interruptions imposed by breast cancer disrupted their previous assumptions about life and ultimately forced them to reorganize and redefine their personal meanings. In addition, Lee found that it was rare for Chinese American breast cancer survivors to openly talk about their illnesses to other family members [6]. The present qualitative study using an expressive writing approach was the first attempt to explore the experiences of the cancer decision-making and treatment periods among mainland Chinese breast cancer survivors.
Our findings suggest that Chinese breast cancer patients often prefer mastectomy over breast-conserving surgery, even if breast-conserving surgery is an option. This finding is similar to that of another finding on Chinese American breast survivors [8, 11]. Lam found that people chose mastectomy because of survival expectations rather than physical appearance, which may account for the Chinese survivors’ choices [12]. Because of patients’ perceptions and the medical environment in China, mastectomies are actually highly prevalent, while breast-conserving surgery is rare. A multicenter retrospective study showed that the rate of mastectomy was 88.12%, while the breast conservation rate was only 11.88% in China [13]. In our study, twelve participants (27.3%) preferred to take a passive role in decision-making, as they were fearful and stressed and did not know which treatment to choose. These participants tended to rely on physicians or families to make treatment decisions. Three reasons likely explain these participants’ desires for passive involvement. The first is lack of knowledge about professional cancer treatment [14]. The second is respect for doctors as authorities whose judgments should not be questioned [15]. The third is that family influences rather than personal choices dominated their decision making [16]. In contrast, only 3 participants (6.8%) chose to take an active role in decision-making. It is supposed that those who took actives roles in decision-making had higher educational levels and a better ability to seek information. This finding is in accordance with Kwok’s study, which indicated that among Chinese Australian women with breast cancer, decision makers were active in and capable of information seeking [14].
Most of the participants thought their breast cancer diagnoses had negative impacts on their families, mainly because of financial burden. Financial burden can be classified into two categories. The first category is an objective lack of money, and the other category is the subjective pressure from financial burden [17]. These two kinds of financial burden were observed in our study. According to a multicenter survey in China, the overall average expenditure for breast cancer and treatment was US$8450; however, the mean previous year household income was US$8722 [18]. Thus, breast cancer is a financial burden to some breast cancer survivors in China. Being unable to fulfill family responsibilities is also a source of distress for breast cancer survivors [19]. As nurturers and caregivers of the family, rather than dependents, survivors feel obliged to take care of their children and their parents [20, 21]. Their primary worry is about who will take care of their families instead of them. They care more about their families than about themselves, especially when they have dependent children [20]. Through familial expectations and support, the participants could eventually accept their disease and cooperate with the treatment prescribed by their doctors. Our study indicated that family played an important role in participants’ emotional adjustment to breast cancer and provided them with strong psychological support during treatment. A similar result was found in a study by Peggy, which indicated that family beliefs significantly influenced patients’ psychological reactions and coping patterns [22]. Levkovich et al. also emphasized the importance of family support when coping with breast cancer [23].
Fatalism is the belief that the outcomes of events are governed by external forces, including luck, fate, and destiny, and that nothing can be done to change the eventual outcomes [24]. Our study found that participants with fatalistic beliefs tended to passively accept their diagnoses and were unwilling to take action to become involved in their disease treatment. Fatalistic beliefs involve negative attitudes towards treatment and result in poor treatment decision-making [25, 26]. In line with Lu’s report [19], our research also indicated that breast cancer survivors seldom disclose their feelings to avoid placing emotional burdens on their family members. Eastern culture values emotional control, emotional restraint, and emotional suppression to achieve interpersonal harmony [27]. Therefore, for Chinese people, it is unusual to talk about cancer-related issues in public, and it is difficult for Chinese cancer patients to disclose their true thoughts. Expressive writing is a private intervention which facilitates emotional expression without damaging harmony with others and may be especially suitable for Chinese [28]. The participants in our study experienced cancer-related stigma, which is consistent with previous studies [6, 19]. People with feelings of stigma perceive that they are rejected by others [29]. Nyblade et al. identified three reasons that may cause feelings of stigma, including fear of transmission, personal factors causing cancer, and cancer being incurable [30].
Limitations
The current study has several limitations. First, our participants were mainly from Weifang, a third-tier city in China. Therefore, our sample could not represent patients from large cities. Second, our participants were from one hospital; a sample of participants from multiple hospitals should be used in the future. Third, the content of the essays included the patients’ subjective experiences but did not include the patients’ objective physiological indicators. Thus, a specific scale should be used to assess the factors related to the themes listed in this paper. Fourth, the instructions for the expressive writing were not tailored to the treatment decision-making theme. Therefore, the information that participants provided in relation to this theme was incomplete, and some participants did not mention details concerning their treatment decision-making. For a qualitative study, it is common to conduct interviews with specific questions to participants. However, in the expressive writing, the instructions for the writing content are somewhat general.
Clinical implications
Treatment decision-making is mainly dependent on relevant information available to patients. According to a recent study, Chinese breast cancer survivors’ knowledge of breast cancer was still very poor and survivors lacked appropriate access to cancer treatment information [31]. Thus, doctors and medical institutions should pay more attention to the education of patients through brochures, lectures, the internet, etc. We should let the patients know that breast cancer is curable through standard treatment and alleviate their fears. In the past, we have usually focused our attention on treatment. However, in addition to treatment, psychological care is also crucial. When patients are in good psychological condition, they better comply with doctors’ treatments. Therefore, we must attach importance to addressing patients’ negative psychological conditions and provide appropriate psychological interventions that consider family and cultural influences.
Conclusions
This article has highlighted the specific barriers common to Chinese women in mainland China in making decisions about breast cancer treatment. These unique family and cultural traditions must be considered when tailoring information about breast cancer treatment options to these women. In particular, beliefs in traditional Chinese medicine is a new finding not previously identified in other research and demonstrates the usefulness of expressive writing in clarifying beliefs Chinese women are uncomfortable expressing in other formats.
References
Chen W, Zheng R, Baade PD, Zhang S, Zeng H, Bray F, Jemal A, Yu XQ, He J (2016) Cancer statistics in China, 2015. CA cancer j clin 66:115–132
Zuo TT, Zheng RS, Zeng HM, Zhang SW, Chen WQ (2017) Female breast cancer incidence and mortality in China, 2013. Thorac cancer 8:214–218
Fan L, Strasser-Weippl K, Li JJ, St Louis J, Finkelstein DM, Yu KD, Chen WQ, Shao ZM, Goss PE (2014) Breast cancer in China Lancet Oncol 15:e279–e289
Lam WW, Fielding R (2003) The evolving experience of illness for Chinese women with breast cancer: a qualitative study. Psycho-oncology 12:127–140
Cheng H, Sit JWH, KKF C (2016) Negative and positive life changes following treatment completion: Chinese breast cancer survivors’ perspectives Supportive care in cancer:official journal of the Multinational Association. Support Care Cancer 24:791–798
Lee S, Chen L, Ma GX, Fang CY, Oh Y, Scully L (2013) Challenges and needs of Chinese and Korean American breast cancer survivors: in-depth interviews. N Am j med sci 6:1–8
Lu Q, Zheng D, Young L, Kagawa-Singer M, Loh A (2012) A pilot study of expressive writing intervention among Chinese-speaking breast cancer survivors Health psychology : official journal of the Division of Health Psychology. American Psychological Association 31:548–551
Lu Q, Yeung NC, You J, Dai J (2016) Using expressive writing to explore thoughts and beliefs about cancer and treatment among Chinese American immigrant breast cancer survivors. Psycho-oncology 25:1371–1374
Warmoth K, Cheung B, You J, NCY Y, Lu Q (2017) Exploring the social needs and challenges of Chinese American immigrant breast cancer survivors: a qualitative study using an expressive writing approach. Int j behav med 24:827–835
Giorgi A (1997) The theory, practice, and evaluation of the phenomenological method as a qualitative research procedure 28: 235
Killoran M, Moyer A (2006) Surgical treatment preferences in Chinese-American women with early-stage breast cancer. Psycho-oncology 15:969–984
Lam WW, Fielding R, Ho EY, Chan M, Or A (2005) Surgeon’s recommendation, perceived operative efficacy and age dictate treatment choice by Chinese women facing breast cancer surgery. Psycho-oncology 14:585–593
Zhang BL, Sivasubramaniam PG, Zhang Q, Wang J, Zhang B, Gao JD, Tang ZH, Chen GJ, Xie XM, Wang Z, Yang HJ, He JJ, Li H, Li JY, Fan JH, Wang X, Qiao YL (2015) Trends in radical surgical treatment methods for breast malignancies in China: a multicenter 10-year retrospective study. Oncologist 20:1036–1043
Kwok C, Koo FK (2017) Participation in treatment decision-making among Chinese-Australian women with breast cancer Supportive care in cancer: official journal of the Multinational Association. Support Care Cancer 25:957–963
Bennett K, Smith DH, Irwin H (1999) Preferences for participation in medical decisions in China Health Communication 11: 261-284
Wong-Kim E, Sun A, Merighi JR, Chow EA (2005) Understanding quality-of-life issues in Chinese women with breast cancer: a qualitative investigation. Cancer Control 12(Suppl 2):6–12
Carrera PM, Kantarjian HM, Blinder VS (2018) The financial burden and distress of patients with cancer: understanding and stepping-up action on the financial toxicity of cancer treatment. CA cancer j clin 68:153–165
Liao XZ, Shi JF, Liu JS, Huang HY, Guo LW, Zhu XY, Xiao HF, Wang L, Bai YN, Liu GX, Mao AY, Ren JS, Sun XJ, Mai L, Liu YQ, Song BB, Gong JY, Zhou JY, Du LB, Zhou Q, Cao R, Zhu L, Ren Y, Lou PA, Lan L, Sun XH, Qi X, Wang YZ, Zhang K, He J, Dai M (2018) Medical and non-medical expenditure for breast cancer diagnosis and treatment in China: a multicenter cross-sectional study. Asia Pac J Clin Oncol 14:167–178
Lu Q, Wong CC, Gallagher MW, Tou RY, Young L, Loh A (2017) Expressive writing among Chinese American breast cancer survivors: a randomized controlled trial Health psychology : official journal of the Division of Health Psychology. American Psychological Association 36:370–379
Kim S, Ko YH, Jun EY (2012) The impact of breast cancer on mother-child relationships in Korea. Psycho-oncology 21:640–646
Tam Ashing K, Padilla G, Tejero J, Kagawa-Singer M (2003) Understanding the breast cancer experience of Asian American women. Psycho-oncology 12:38–58
Simpson P (2005) Hong Kong families and breast cancer: beliefs and adaptation strategies. Psycho-oncology 14:671–683
Levkovich I, Cohen M, Karkabi K (2019) The Experience of fatigue in breast cancer patients 1-12 month post-chemotherapy: a qualitative study. Behav Med 45:7–18
Straughan PT, Seow A (1998) Fatalism reconceptualized: a concept to predict health screening behavior Journal of Gender. Culture and Health 3:85–100
Powe BD, Finnie R (2003) Cancer fatalism: the state of the science. Cancer Nurs 26:454–465 quiz 466-457
Shields CG, Morrow GR, Griggs J, Mallinger J, Roscoe J, Wade JL, Dakhil SR, Fitch TR (2004) Decision-making role preferences of patients receiving adjuvant cancer treatment: a university of Rochester cancer center community clinical oncology program. Support Cancer Ther 1:119–126
Wei M, Su JC, Carrera S, Lin SP, Yi F (2013) Suppression and interpersonal harmony: a cross-cultural comparison between Chinese and European Americans. J Couns Psychol 60:625–633
Lu Q, Gallagher MW, Loh A, Young L (2018) Expressive writing intervention improves quality of life among Chinese-American breast cancer survivors: a randomized controlled trial. Ann Behav Med 52:952–962
Else-Quest NM, LoConte NK, Schiller JH, Hyde JS (2009) Perceived stigma, self-blame, and adjustment among lung, breast and prostate cancer patients. Psychol Health 24:949–964
Nyblade L, Stockton M, Travasso S, Krishnan S (2017) A qualitative exploration of cervical and breast cancer stigma in Karnataka, India. BMC Womens Health 17:58
Zhang L, Gao J, Lin D, Xie L, Wang T, Zou L (2019) Personal factors influencing breast cancer patients’ perception of breast conservation surgery in west China. Ann Transl Med 7:313
Funding
This research is supported by the Shandong Education Department (J17RA137), Science and Technology Development Plan of Weifang (2015WS009, 2018YX003), Health and Family Planning Commission of Shandong Province (2017WS852), and Natural Science Foundation of Shandong Province ( ZR2016GM05).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures in studies involving human participants were conducted in accordance with the ethical standards of the Southern Adelaide Clinical Human Research Ethics Committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical
standards.
Statement of informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, L., Geng, X., Ji, L. et al. Treatment decision-making, family influences, and cultural influences of Chinese breast cancer survivors: a qualitative study using an expressive writing method. Support Care Cancer 28, 3259–3266 (2020). https://doi.org/10.1007/s00520-019-05161-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-05161-w