Abstract
Background
Deficiency of complement factor H-related plasma proteins and complement factor H autoantibody-positive hemolytic uremic syndrome (DEAP-HUS), which is characterized by the deficiency of complement-factor H-related (CFHR) plasma proteins and the subsequent formation of autoantibodies against complement factor H (CFH), has been reported to have an adverse outcome in one third of patients. Therapy options include prompt removal of antibodies by plasma exchange and immunosuppressive therapy. Recently, restoration of complement control using the monoclonal antibody eculizumab has been shown to be effective as first- and as second-line therapy in cases of therapy resistance or severe side effects of the applied therapy.
Diagnosis/treatment
Here, we report a 6-year-old girl with DEAP-HUS and first-line therapy with eculizumab under immunosuppressive therapy with glucocorticoids and mycophenolate mofetil (MMF). This therapy led to a prompt and sustained clinical recovery, to a stable reduction of complement activation, and to a rapid decline in autoantibody titer. A second increase in the autoantibody titer was successfully treated with methylprednisolone and the child remained in remission. After 8.3 months of sustained complement control and 4.5 months of stable antibody suppression, eculizumab was successfully discontinued without any sign of relapse.
Conclusions
To our knowledge, this is the first reported case of a child with DEAP-HUS treated with the combination of eculizumab and immunosuppression as first-line therapy avoiding any HUS- or therapy-related complications and resulting in prompt clinical recovery. Importantly, clinical remission is maintained after discontinuation of eculizumab under stable immunosuppression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The atypical hemolytic uremic syndrome (aHUS) is a rare, but life-threatening disease and is defined by microangiopathic hemolytic anemia, acute renal failure, and thrombocytopenia. aHUS is caused by dysregulation of the alternative complement pathway owing to mutations in complement inhibitory or activating factors [1, 2]. Among the subtypes of aHUS, deficiency of complement factor H-related plasma proteins and complement factor H autoantibody-positive hemolytic uremic syndrome (DEAP-HUS) accounts for around 10% of cases and has gained particular attention because of its autoimmune character. It displays the unique combination of a genetic mutation resulting in the absence of CFHR1 and CFHR3 proteins in plasma and the presence of subsequently acquired autoantibodies to the C-terminus of CFH [3, 4].
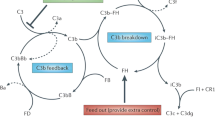
Treatment options include prompt removal or reduction of the antibodies by therapeutic plasma exchange (TPE) with consecutive immunosuppressive therapy (IS), and re-establishing proper complement control by blocking C5 with the monoclonal antibody eculizumab, which has been shown to be effective in other forms of aHUS [1, 5–7].
In recent years, a large cohort of Indian DEAP-HUS patients was treated with TPE and IS, but with a substantial proportion of adverse outcomes [8, 9]. Given the experiences in other types of aHUS, the use of eculizumab also in DEAP-HUS appears promising, but data are limited to a very small number of patients, most of them receiving eculizumab as second-line therapy [10–16]. Data on withdrawal of eculizumab, as proposed in the latest consensus recommendations on aHUS and in a recent meeting report of a KDIGO conference [1, 5], are extremely scarce [11, 14–16].
Here, we report a case of a 6-year-old girl with DEAP-HUS and a favorable clinical course under first-line eculizumab and glucocorticoids as induction therapy, followed by glucocorticoids and mycophenolate mofetil (MMF) as maintenance therapy. After continuous antibody reduction was achieved, eculizumab was successfully withdrawn.
Case report
A 6-year-old girl with no past medical history presented in reduced clinical conditions with vomiting and fever accompanied by petechiae. HUS was confirmed by the evidence of acute kidney failure (serum creatinine: 1.99 mg/dl [<0.9 mg/dl]), hemolytic anemia (hemoglobin: 5.1 g/dl [11.5–15 g/dl]), lactate dehydrogenase (LDH): 1,764 U/l (120–300 U/l), haptoglobin: <0.2 g/l (0.3–2 g/l), and thrombocytopenia (platelets: 97 × 103/μl [150–530 × 103/μl]) with no evidence of extra-renal manifestations. Diagnostic work-up revealed normal ADAMTS13 protease activity, negative vasculitis (ANAs, ANCAs) and microbiological screening (Shiga toxin-producing E. coli, Streptococcus pneumoniae). C3 was reduced to 0.72 g/l (0.9–1.8 g/l). The initial therapy consisted of the transfusion of packed red blood cells owing to symptomatic ongoing hemolytic anemia as well as blood pressure control, and diuretic therapy. Seven days after admission, we received the result of a significant activation of the terminal complement complex (sC5b-9: 2,047 ng/ml [<320 ng/ml]); thus, aHUS was diagnosed and we instantly started therapy with eculizumab administered weekly for 4 weeks and thereafter biweekly. The day after, we were informed about the presence of CFH autoantibodies (plasma titer 666 AU/ml [<60 AU/ml]) and a homozygous CFHR1/3 deletion in line with the diagnosis of DEAP-HUS. The additional analyses of the genes encoding CFI, C3, CD46, CFB, THBD, MMACHC, and DGKE yielded unremarkable results. We therefore started the patient on a pulsed methylprednisolone regimen (500 mg/m2 body surface area (BSA)/day on three consecutive days, followed by gradual prednisolone tapering, starting with 40 mg/m2BSA/day) and therapy with MMF (1,100 mg/m2BSA/day). The patient responded promptly with rapid normalization of LDH, platelets, and serum creatinine, and was discharged after 16 days (Fig. 1a). Meningococcal A, B, C, W, Y vaccination was performed before eculizumab and the girl was put on additional penicillin prophylaxis.
a Short-term clinical course. The induction therapy consisting of eculizumab, glucocorticoids, and mycophenolate mofetil resulted in the prompt normalization of lactate dehydrogenase (LDH), platelets, and serum creatinine. Conversion factors for SI units: serum creatinine in mg/dl to μmol/l, ×88.4. b Long-term clinical course. Stable complement and antibody control were achieved under immunosuppressive maintenance therapy, allowing the successful discontinuation of eculizumab
Four months later, a remarkable increase in CFH autoantibody titer without any clinical or hematological evidence for a relapse of DEAP-HUS was noted during the monthly follow-up. We applied another pulsed methyl-prednisolone course (500 mg/m2 BSA/day on three consecutive days) and CFH autoantibody titer promptly decreased and remained remained in stable reduction during the further follow-up period of 15.7 months to date (Fig. 1b). Eculizumab was withdrawn 8.3 months after initiation of the therapy (4.5 months after the second rise in antibodies). MMF has been continued as maintenance therapy with a stable exposure to mycophenolic acid (MPA-AUC 0–12 h: 77 mg*h/l at months 3 and 15 respectively). Glucocorticoids were gradually tapered to 4 mg/m2BSA/day to date. Parents have been taught to perform daily urinary dipstick controls and to immediately report any potential sign of relapse (i.e., the onset of hematuria), as recommended [11, 14].
Discussion
We report a case of DEAP-HUS with a favorable outcome applying eculizumab with glucocorticoid pulse therapy in the acute phase followed by glucocorticoids and MMF as maintenance therapy to suppress antibody production in the long-term. Furthermore, owing to constantly reduced antibody titers and sustained effective complement inhibition (normal C3, C3d, and sC5b-9), eculizumab could be withdrawn in the maintenance phase.
Of note, this therapy scheme was recommended in the latest consensus recommendations of aHUS and in a recent meeting report of a KDIGO conference on aHUS [1, 5]. However, to date, no reports on using this therapeutic scheme have been published. The prompt restoration of complement control and the reduction of CFH autoantibody titer resulted in a favorable clinical course with complete renal recovery avoiding renal replacement therapy (RRT), achieving prompt normalization of hematological parameters, short hospitalization and an absence of any treatment-related complications. In addition, the consequent IS resulted in stable antibody control, facilitating the withdrawal of eculizumab.
Based on the available literature, several issues of the case are relevant and deserve further discussion. In a large cohort of Indian children with DEAP-HUS (n = 139), induction treatment with TPE plus corticosteroids and iv cyclophosphamide or rituximab was effective in inducing remission and led to a rapid removal of CFH autoantibodies. However, adverse outcomes [stage 4–5 chronic kidney disease (CKD) or death] were reported in 30% of patients [8]. In addition, TPE procedure itself was reported with serious catheter-related complications in one third of children with aHUS [17]. As our patient had a mild form of DEAP-HUS (stable general conditions, renal dysfunction without the need for renal RRT, no extra-renal manifestations), we opted for eculizumab as first-line therapy. This was feasible as eculizumab was available in our center within 24 h and could thus be started as soon as the diagnosis of aHUS was confirmed. Choosing this therapeutic strategy, we were able to avoid TPE with its related side effects, including central venous catheter-related complications, and the use a more intensified IS. However, in patients with a more severe disease course presenting with end-stage renal disease and/or extrarenal manifestations, prompt TPE combined with eculizumab at the end of each session, in addition to a more aggressive IS regimen (including cyclophosphamide and repeated doses of rituximab), may be indicated to obtain full remission and stable antibody control.
To date, there are very few reported pediatric cases of treatment with eculizumab in DEAP-HUS, as summarized in Table 1 [10–14]: Noone et al. have reported 2 children with DEAP-HUS, 1 with a plasma therapy-dependent course and the other 1 with an allergic reaction to fresh frozen plasma. In both cases, the initiation of eculizumab resulted in a complete remission of disease activity [10]. Chiodini et al. described a case of DEAP-HUS in which eculizumab (without IS) was initiated after an unsatisfactory response to plasma treatment and was effective not only in the recovery of renal but also of extrarenal manifestations [12]. Another child was effectively treated with plasma infusions and eculizumab, even before DEAP-HUS was confirmed [13]. A study on the discontinuation of eculizumab in aHUS included 3 children with CHFR1/3 deletion and CHF autoantibodies who recovered under eculizumab. However, no data were given on maintenance IS [11, 14]. In addition to these pediatric cases, 3 adult DEAP-HUS patients have been reported to have been successfully treated with eculizumab [15, 16, 18], in 1 case after an unsatisfactory response to TPE [18] and in 2 cases as first-line therapy (with reported co-IS comprising TPE and rituximab in 1 of them) [15, 16]. Outcome in these relatively few cases was excellent compared with previous studies with adverse outcomes (CKD stages 4–5 and/or death) in around 30% of patients [8, 19, 20].
There is compelling evidence that high antibody titers at follow-up are associated with an increased risk for relapse [9], even in clinically asymptomatic patients, and that therapy should therefore be guided by antibody-monitoring [1, 5]. Of note, comparison of the autoantibody titer to other studies (determined in different laboratories) and concluding the severity of disease courses from particular titer levels is still hampered, as different, laboratory-specific standards are applied in the analysis of the CFH autoantibody titer [5, 21]. Accordingly, the need for a consensus assay using a standard arbitrary unit scale based on a titration curve from a common positive anti-serum has been recently addressed by three European complement laboratories after comparing different ELISA methods [22].
For our patient, the longitudinal, monthly monitoring of the titer course using the same laboratory enabled the early detection of a significantly increased antibody titer (3,071 AU/ml). A second methylprednisolone pulse therapy was thus applied, even before any hematological sign of relapse and the girl remained in remission. This case underlines the importance of antibody monitoring to guide therapy and as the best available early detection method of a relapse, especially in the first months when patients are most susceptible to relapse.
According to the aHUS international consensus recommendation of 2016, the withdrawal of eculizumab should be considered in stable remission and CFH autoantibody titers constantly below 1,000 AU/ml in addition to ongoing maintenance IS therapy [1]. To date, discontinuation has been reported in 5 of the 10 DEAP-HUS patients treated with eculizumab (Table 1): Ardissino et al. reported 3 children with DEAP-HUS and the discontinuation of eculizumab, 2 of whom experienced a relapse (duration of therapy less than 1 month in both cases) that promptly resolved after re-initiation of treatment [11, 14]. It is important to note that in none of these cases are data of an antibody-depleting maintenance therapy parallel to or after withdrawal of eculizumab given, although this significantly reduces the risk of relapse [1]. The four other reported children with a favorable outcome under eculizumab have not yet been withdrawn from eculizumab [10, 12, 13]. There are a further 2 reports on adult DEAP-HUS with successful discontinuation of eculizumab [15, 16]: in 1 case, a combination of eculizumab plus glucocorticoids and rituximab resulted in stable remission, which allowed the successful withdrawal of eculizumab [15]; in the other case, no distinct data on co-IS are provided [16]. Although the experience of withdrawal of eculizumab is limited, it seems essential to underline the need for stable remission and antibody reduction before considering discontinuation. In our case, a withdrawal of eculizumab before the second rise of antibodies may have resulted in an early relapse. This case thus nicely confirms the reported risk of antibody re-rise, particularly in the first months [5, 20]. Notably, the reported patients experiencing relapse after eculizumab withdrawal were also treated with eculizumab for less than 1 month, whereas those with successful discontinuation were treated for a longer period and using co-IS in most cases. Therefore, it appears most reasonable to continue eculizumab therapy for at least 6–12 months of HUS remission with stably decreased CFH autoantibody titer before considering withdrawal.
In summary, to the best of our knowledge, our patient is the first pediatric patient in whom eculizumab has been withdrawn under continuous IS, providing stable, low antibody titers and a significant reduction in complement activation.
Distinct data on duration, dosing, and form of maintenance therapy following eculizumab are limited so far. We successfully applied methylprednisolone pulses as induction therapy and in antibody re-rise, and later slowly tapered oral prednisolone. MMF was administered with a stable MPA-AUC0–12 of 77 mg*h/l. However, we cannot exclude the possibility that a less intensive IS might also be effective. Therefore, further studies on this issue are required. In any case, we feel that control of MPA exposure is extremely important, as was previously shown in other conditions [23].
In summary, our study confirms that eculizumab is safe and effective in the treatment of DEAP-HUS. In addition, we showed for the first time that the discontinuation of eculizumab under antibody-depleting maintenance therapy and thorough antibody monitoring can be considered for DEAP-HUS patients in stable remission, as was proposed in the latest aHUS consensus recommendations and a KDIGO meeting report [1, 5].
Abbreviations
- ADAMTS13:
-
A disintegrin and metalloproteinase with thrombospondin-1 motifs (13th member of the family)
- aHUS:
-
Atypical hemolytic uremic syndrome
- ANAs:
-
Anti-nuclear antibodies
- ANCAs:
-
Anti-neutrophil cytoplasmic antibodies
- AUC:
-
Area under the curve
- BSA:
-
Body surface area
- CFH/CFI/CFB:
-
Complement factor H/I/B
- CFHR:
-
Complement factor H-related
- CKD:
-
Chronic kidney disease
- DEAP-HUS:
-
Deficiency of complement factor H-related plasma proteins and complement factor H autoantibody-positive hemolytic uremic syndrome
- DGKE:
-
Diacylglycerol kinase epsilon
- IS:
-
Immunosuppression
- LDH:
-
Lactate dehydrogenase
- MMACHC:
-
Methylmalonic aciduria and homocystinuria type C protein
- MMF:
-
Mycophenolate mofetil
- MPA:
-
Mycophenolic acid
- PI:
-
Plasma infusions
- RRT:
-
Renal replacement therapy
- sC5b-9:
-
Soluble C5b-9
- THBD:
-
Thrombomodulin
- TPE:
-
Therapeutic plasma exchange
References
Loirat C, Fakhouri F, Ariceta G, Besbas N, Bitzan M, Bjerre A, Coppo R, Emma F, Johnson S, Karpman D, Landau D, Langman CB, Lapeyraque AL, Licht C, Nester C, Pecoraro C, Riedl M, van de Kar NC, Van de Walle J, Vivarelli M, Frémeaux-Bacchi V, HUS International (2016) An international consensus approach to the management of atypical hemolytic uremic syndrome in children. Pediatr Nephrol 31:15–39
Kavanagh D, Goodship T (2010) Genetics and complement in atypical HUS. Pediatr Nephrol 25:2431–2442
Zipfel PF, Mache C, Müller D, Licht C, Wigger M, Skerka C, European DEAP-HUS Study Group (2010) DEAP-HUS: deficiency of CFHR plasma proteins and autoantibody-positive form of hemolytic uremic syndrome. Pediatr Nephrol 25:2009–2019
Józsi M, Licht C, Strobel S, Zipfel SL, Richter H, Heinen S, Zipfel PF, Skerka C (2008) Factor H autoantibodies in atypical hemolytic uremic syndrome correlate with CFHR1/CFHR3 deficiency. Blood 111:1512–1514
Goodship TH, Cook HT, Fakhouri F, Fervenza FC, Frémeaux-Bacchi V, Kavanagh D, Nester CM, Noris M, Pickering MC, Rodríguez de Córdoba S, Roumenina LT, Sethi S, Smith RJ, Participants C (2016) Atypical hemolytic uremic syndrome and C3 glomerulopathy: conclusions from a “Kidney Disease: Improving Global Outcomes” (KDIGO) Controversies Conference. Kidney Int. doi:10.1016/j.kint.2016.10.005
Legendre CM, Licht C, Muus P, Greenbaum LA, Babu S, Bedrosian C, Bingham C, Cohen DJ, Delmas Y, Douglas K, Eitner F, Feldkamp T, Fouque D, Furman RR, Gaber O, Herthelius M, Hourmant M, Karpman D, Lebranchu Y, Mariat C, Menne J, Moulin B, Nürnberger J, Ogawa M, Remuzzi G, Richard T, Sberro-Soussan R, Severino B, Sheerin NS, Trivelli A, Zimmerhackl LB, Goodship T, Loirat C (2013) Terminal complement inhibitor eculizumab in atypical hemolytic-uremic syndrome. N Engl J Med 368:2169–2181
Greenbaum LA, Fila M, Ardissino G, Al-Akash SI, Evans J, Henning P, Lieberman KV, Maringhini S, Pape L, Rees L, van de Kar NC, Vande Walle J, Ogawa M, Bedrosian CL, Licht C (2016) Eculizumab is a safe and effective treatment in pediatric patients with atypical hemolytic uremic syndrome. Kidney Int 89:701–711
Sinha A, Gulati A, Saini S, Blanc C, Gupta A, Gurjar BS, Saini H, Kotresh ST, Ali U, Bhatia D, Ohri A, Kumar M, Agarwal I, Gulati S, Anand K, Vijayakumar M, Sinha R, Sethi S, Salmona M, George A, Bal V, Singh G, Dinda AK, Hari P, Rath S, Dragon-Durey MA, Bagga A, Indian HUS Registry (2014) Prompt plasma exchanges and immunosuppressive treatment improves the outcomes of anti-factor H autoantibody-associated hemolytic uremic syndrome in children. Kidney Int 85:1151–1160
Khandelwal P, Gupta A, Sinha A, Saini S, Hari P, Dragon Durey MA, Bagga A (2015) Effect of plasma exchange and immunosuppressive medications on antibody titers and outcome in anti-complement factor H antibody-associated hemolytic uremic syndrome. Pediatr Nephrol 30:451–457
Noone D, Waters A, Pluthero FG, Geary DF, Kirschfink M, Zipfel PF, Licht C (2014) Successful treatment of DEAP-HUS with eculizumab. Pediatr Nephrol 29:841–851
Ardissino G, Testa S, Possenti I, Tel F, Paglialonga F, Salardi S, Tedeschi S, Belingheri M, Cugno M (2014) Discontinuation of eculizumab maintenance treatment for atypical hemolytic uremic syndrome: a report of 10 cases. Am J Kidney Dis 64:633–637
Diamante Chiodini B, Davin JC, Corazza F, Khaldi K, Dahan K, Ismaili K, Adams B (2014) Eculizumab in anti-factor h antibodies associated with atypical hemolytic uremic syndrome. Pediatrics 133:e1764–e1768
Hisano M, Ashida A, Nakano E, Suehiro M, Yoshida Y, Matsumoto M, Miyata T, Fujimura Y, Hattori M (2015) Autoimmune-type atypical hemolytic uremic syndrome treated with eculizumab as first-line therapy. Pediatr Int 57:313–317
Ardissino G, Possenti I, Tel F, Testa S, Salardi S, Ladisa V (2015) Discontinuation of eculizumab treatment in atypical hemolytic uremic syndrome: an update. Am J Kidney Dis 66:172–173
Fakhouri F, Delmas Y, Provot F, Barbet C, Karras A, Makdassi R, Courivaud C, Rifard K, Servais A, Allard C, Besson V, Cousin M, Châtelet V, Goujon JM, Coindre JP, Laurent G, Loirat C, Frémeaux-Bacchi V (2014) Insights from the use in clinical practice of eculizumab in adult patients with atypical hemolytic uremic syndrome affecting the native kidneys: an analysis of 19 cases. Am J Kidney Dis 63:40–48
Fakhouri F, Fila M, Provôt F, Delmas Y, Barbet C, Châtelet V, Rafat C, Cailliez M, Hogan J, Servais A, Karras A, Makdassi R, Louillet F, Coindre JP, Rondeau E, Loirat C, Frémeaux-Bacchi V (2017) Pathogenic variants in complement genes and risk of atypical hemolytic uremic syndrome relapse after eculizumab discontinuation. Clin J Am Soc Nephrol 12:50–59
Johnson S, Stojanovic J, Ariceta G, Bitzan M, Besbas N, Frieling M, Karpman D, Landau D, Langman C, Licht C, Pecoraro C, Riedl M, Siomou E, van de Kar N, Walle JV, Loirat C, Taylor CM (2014) An audit analysis of a guideline for the investigation and initial therapy of diarrhea negative (atypical) hemolytic uremic syndrome. Pediatr Nephrol 29:1967–1978
Green H, Harari E, Davidovits M, Blickstein D, Grossman A, Gafter U, Gafter-Gvili A (2014) Atypical HUS due to factor H antibodies in an adult patient successfully treated with eculizumab. Ren Fail 36:1119–1121
Hofer J, Janecke AR, Zimmerhackl LB, Riedl M, Rosales A, Giner T, Cortina G, Haindl CJ, Petzelberger B, Pawlik M, Jeller V, Vester U, Gadner B, van Husen M, Moritz ML, Würzner R, Jungraithmayr T, German-Austrian HUS Study Group (2013) Complement factor H-related protein 1 deficiency and factor H antibodies in pediatric patients with atypical hemolytic uremic syndrome. Clin J Am Soc Nephrol 8:407–415
Dragon-Durey MA, Sethi SK, Bagga A, Blanc C, Blouin J, Ranchin B, André JL, Takagi N, Cheong HI, Hari P, Le Quintrec M, Niaudet P, Loirat C, Fridman WH, Frémeaux-Bacchi V (2010) Clinical features of anti-factor H autoantibody-associated hemolytic uremic syndrome. J Am Soc Nephrol 21:2180–2187
Licht C, Noone D (2014) Treatment of DEAP-HUS—seeking the best strategy. Pediatr Nephrol 29:941–942
Watson R, Lindner S, Bordereau P, Hunze EM, Tak F, Ngo S, Zipfel PF, Skerka C, Dragon-Durey MA, Marchbank KJ (2014) Standardisation of the factor H autoantibody assay. Immunobiology 219:9–16
Weber LT (2015) Therapeutic drug monitoring in pediatric renal transplantation. Pediatr Nephrol 30:253–265
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Support/funding
There was no financial support or funding for this study
Conflicts of interest
AH and BBB received fees for invited lectures from Alexion. MK received fees for invited lectures and advisory board meetings from Alexion and for lectures from Euro Diagnostica. PFZ received lecture fees from Alexion. LTW is a member of the Scientific Advisory Board of Alexion. RE and SH declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Hackl, A., Ehren, R., Kirschfink, M. et al. Successful discontinuation of eculizumab under immunosuppressive therapy in DEAP-HUS. Pediatr Nephrol 32, 1081–1087 (2017). https://doi.org/10.1007/s00467-017-3612-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-017-3612-9