Abstract
Objective
Laparoscopic liver resection (LLR) for Hepatocellular Carcinoma (HCC) is one of the most important indications for the minimally invasive approach. Our study aims to analyze the experience of the Italian Group of Minimally Invasive Liver Surgery with laparoscopic surgical treatment of HCC, with a focus on tumor location and how it affects morbidity and mortality.
Methods
38 centers participated in this study; 372 cases of LLR for HCC were prospectively enrolled. Patients were divided into two groups according to the HCC nodule location. Group 1 favorable location and group 2 unfavorable location. Perioperative outcomes were compared between the two groups before and after a propensity score match (PS) 1:1.
Results
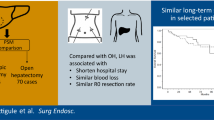
Before PS in group 2 surgical time was longer; conversion rate was higher; postoperative transfusion and comprehensive complication index were also higher. PS was performed with a cohort of 298 patients (from 18 centers), with 66 and 232 patients with HCC in unfavorable and favorable locations, respectively. After PS matching, 62 patients from group 1 and group 2 each were compared. Operative and postoperative course were similar in patients with HCC in favorable and unfavorable LLR locations. Surgical margins were found to be identical before and after PS.
Conclusions
These results show that LLR in patients with HCC can be safely performed in all segments because of the extensive experience of all surgeons from multiple centers in performing traditional open liver surgery as well as laparoscopic surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Hepatocellular carcinoma (HCC) is the fifth most common primary cancer and the second and sixth most common cause of cancer-related deaths worldwide in males and females, respectively [1]. Surgical resection is a potential curative treatment for patients with HCC [2]. Minimally invasive approaches for liver resection have considerably improved since the First International Consensus Conference on Laparoscopic Liver Resection (LLR) (Louisville 2008) [3]. Laparoscopic segments and minor LLRs should be a standard practice. In 2014 in Morioka, it was concluded that major LLR is still in exploratory or learning phase and has undefined risks [4]. LLR for patients with HCC has confirmed the theoretical benefits of the laparoscopic approach, such as reduced parietal and hepatic injury, preserved collateral venous circulation, and decreased rates of postoperative liver failure and ascites. Here, we aim to analyze the experience of the Italian Group of Minimally Invasive Liver Surgery (IGoMILS) with laparoscopic surgical treatment of HCC, with a focus on tumor location and how it affects morbidity and mortality.
Methods
Since November 2014, all cases of LLR have been prospectively registered. All Italian centers had the opportunity to participate in this project. We analyzed all cases of HCC resection registered from November 2014 to August 31, 2016. Thirty-eight centers participated in this study; 372 cases of LLR for HCC were enrolled. Patient characteristics and surgical and perioperative data, including duration of surgery, estimated blood loss, length of postoperative hospital stay, types of complications, and other variables, were obtained from the database.
HCC nodule location was defined as a favorable location in case of anterolateral segments 2, 3, 4b, 5, and 6 and as an unfavorable location in case of posterior superior Couinaud segments 1, 4a, 7, and 8. Major hepatectomy was defined as resection of three or more Couinaud segments. Portal hypertension was defined as portal venous pressure of > 10 mmHg, presence of portosystemic collateral vessels, or the presence of esophageal varices.
Patients were divided into two groups on the basis of HCC nodule location. Group 1 (favorable location) included patients with HCC nodule on laparoscopic segments and group 2 (unfavorable location) included patients with HCC nodule on non-laparoscopic segments. Postoperative complications were defined according to the comprehensive complication index (CCI) [5]. Patients in group 1 were matched at a ratio of 1:1 with patients who had undergone resection in group 2. The matching was achieved on the basis of propensity scores (PSs), including the following eight covariables: sex, age, body mass index (BMI), Model for End-Stage Liver Disease (MELD), Child-Pugh Score (Child), previous cholecystectomy, type of liver parenchyma, nodule diameter. Written informed consent was obtained from all patients in accordance with the Declaration of Helsinki, and this study was approved by the institutional review board.
Propensity score matching
PS matching was performed on the cohort to adjust any difference in average outcomes for segment location selection bias. PS matching was performed by considering all significant variables between the two groups in the preliminary analysis. PSs were generated by logistic regression and relied on the following covariables: sex, age, BMI, MELD, Child, previous cholecystectomy, type of liver parenchyma, and nodule diameter. After estimation of PSs, a regular 1:1 nearest-neighbor matching process was performed. A small caliper (0⋅1) was specified to improve balance.
Statistical analysis
A 1:1 PS matching was performed between group 1 and group 2 to minimize selection bias in the baseline characteristics between the two groups of patients. A logistic regression model was used to estimate PS for a patient who underwent LLR for an anterolateral nodule to match with a patient who underwent LLR for a posterolateral nodule.
All variables were compared using the χ2 or Fisher’s exact test for categorical data, the Mann–Whitney U-test for non-normally distributed continuous data, and the Student’s t-test for normally distributed continuous variables. All data are expressed as mean ± standard deviation or median and range. A p value of < 0.05 was considered as statistically significant. Statistical analyses were performed using the SPSS Statistics version 21.0 (IBM SPSS).
Results
A total of 378 patients who underwent LLR for HCC were enrolled from 38 Italian centers. Group 1 comprised 306 patients; group 2 comprised 66 patients. In the first group, nodules were in segment II in 49 cases, in segment III in 69 cases, in segment IVb in 33 cases, in segment V in 62 cases, and in segment VI in 93 cases. In group 2, nodules were in segment: I in 3 cases, IVa in 16 cases, VII in 28 cases, and in VIII in 19 cases.
Before matching the two groups, no differences were observed regarding sex, age, BMI, clamping time, number of nodules, Edmondson grade, vascular infiltration, Classification of Malignant Tumours (TNM), previous cholecystectomy, alphafetoprotein, portal hypertension, nodule diameter, surgical margin, estimated blood loss, intraoperative transfusion, and the length of hospital stay. On the other hand, there were more Child B in the laparoscopic group (21 vs. 0; p = 0.008), and the MELD score was higher in group 1 (8 vs. 7; p = 0.021). Surgical time was longer in group 2 (180 min vs. 240 min, p < 0.001); conversion rate was higher in group 2 (5% vs. 18%; p < 0.001). Postoperative transfusion and CCI were also greater in group 2 (p = 0.027; p < 0.001). Results are further provided in Table 1.
Portal hypertension was observed in 109 patients, of whom 93 (85.3%) were in group 1 and 16 (14.7%) in group 2.
PS was performed with a cohort of 298 patients (from 18 centers), with 66 and 232 patients with HCC in unfavorable and favorable locations, respectively. After PS matching, 62 patients from group 1 and group 2 each were compared (Fig. 1). Surgical findings such as nodule diameter (p = 0.677), margin resection (p = 0.283), surgical time (p = 0.438), type of resection (p = 0.063), estimated blood loss (p = 0.966), and intraoperative transfusion (p = 0.499) were similar between the two groups. The rate of conversion to open surgery (p = 0.041) was higher in the unfavorable group. Postoperative morbidity was similar for postoperative transfusion (p = 0.143), CCI (p = 0.061) and the length of hospital stay (p = 0.112). All results after matching are provided in Table 2. We analyzed the contributions of 38 centers to control potential bias. Eighteen centers enrolled 66 and 232 patients with HCC in unfavorable and favorable (74.3% of group 1) locations, respectively. Only patients from these 18 centers were considered for PS.
Discussion
The present study reports the results of a prospective multicentric study of LLR for patients with HCC before and after PS matching. Operative and postoperative course were similar in patients with HCC in favorable and unfavorable LLR locations. Pre-matching analysis revealed some differences between LLR for patients with HCC in favorable and unfavorable locations. Preoperative differences were observed in the MELD score and Child score. Surgical time was greater in HCC in group 2 (p = 0.001). Conversion rate was higher in group 2 (p = 0.001), particularly for oncological radicality, biliary stasis, and anesthesia-related concerns. postoperative transfusion and CCI (p = 0.001) were higher in group 2. These results suggest that LLR for patients with HCC in unfavorable locations is more complicated than that in favorable locations. Careful PS matching did not confirm the previous differences between the groups. Preoperative, surgical, and postoperative characteristics were similar between the groups (Table 2). Surgical time (p = 0.438) and morbidity (p = 0.061) were also similar between the groups. Surgical margins were found to be similar after the first analysis (p = 0.347) and PS matching (p = 0.283). These data support the use of PS matching, which contradicts the current thinking that laparoscopy does not provide an oncologically adequate margin for the unfavorable locations. This is an imperative finding with respect to LLR of HCC. The Louisville consensus conference [3] and Morioka [4] recommended the resection of anterior segments only and referring the resection of lesions in the posterior segments to specialized centers. The Southampton Guidelines (2017) confirmed the previous statement and recommended that patients with HCC or cirrhotic liver should be referred to specialized centers [6].
We also want to acknowledge the participation of the 38 centers in this study, of which 18 have reported at least one patient in the group of patients with HCC in unfavorable locations (Table 3). The prevalence of LLR in many Italian centers is growing; many of them use laparoscopy in cases of HCC in unfavorable locations and have obtained good outcomes.
Furthermore, in our series, 29 patients were classified as Child B. Tumor localization of this subgroup of patients was in the laparoscopic segments (segment 2 in two cases, segment 3 in 11 cases, segment 4b in three cases, segment 5 in five cases, and segment 6 in eight cases). Only one patient underwent a major hepatectomy; others were treated with minor resections. Moreover, 109 patients had portal hypertension with 16 cases in group 2 and 93 in group 1. The results are in parallel with those of the abovementioned Child B.
The LLR ‘‘success’’ was first based on the concept appropriate patient, with appropriate disease treated at the appropriate center. Nevertheless, many studies on LLR for patients with HCC are available. Most of these studies compare open surgery with laparoscopic approach with respect to minor resections, major resections, and cases of HCC in unfavorable locations. The minimal invasive approach has contributed to expand the indication for LLR for patients with HCC without increasing the incidence of perioperative morbidity [7]. Moreover, many studies have compared the results of LLR with those of open liver resection for HCC without finding differences or better yet improving short-term outcomes [8, 9]. Techniques for laparoscopic approaches for lesions in the deep segments of the liver were originally described by Gayet [10]. LLR has been reported as feasible for all liver segments with acceptable morbidity [11, 12]. In this way, other studies confirmed the possibility of expanding the use of LLR for HCC in unfavorable locations. Recent improvements in surgical techniques and accumulated experience allow surgeons to perform resection of HCC in segments 7 and 8 [13, 14] as well as the right anterior sectionectomy [15] or the right posterior sectionectomy [16]. Besides, major resection such as right hepatectomy has been reported to be safe in selected patients and represents a viable alternative to the traditional approach [17,18,19].
Some previous limitations for LLR indication seem to have been overpassed recently. Patient age [20] and tumor size [21] are no longer the limitations for LLR in patients with HCC [22, 23]. More recently, cirrhosis has been proposed as an extended indication for LLR in patients with HCC [24, 25].
The present results are from an Italian multicentric study comparing LLR before and after the implementation of PS matching in patients with HCC localized in favorable or unfavorable locations. The inclusion of a large number of hepatectomies in both groups permitted a high degree of PS matching. Concerning the number of patients with HCC localized in the unfavorable locations, we observed a good balance between all enlistment centers. These results show that LLR in patients with HCC can be safely performed in all segments because of the extensive experience of all surgeons from multiple centers in performing traditional open liver surgery as well as laparoscopic surgery.
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61(2):69–90
Roayaie S, Jibara G, Tabrizian P, Park JW, Yang J, Yan L, Schwartz M, Han G, Izzo F, Chen M, Blanc JF, Johnson P, Kudo M, Roberts LR, Sherman M (2015) The role of hepatic resection in the treatment of hepatocellular cancer. Hepatology 62(2):440–451
Buell JF, Cherqui D, Geller DA, O’Rourke N, Iannitti D, Dagher I, Koffron AJ, Thomas M, Gayet B, Han HS, Wakabayashi G, Belli G, Kaneko H, Ker CG, Scatton O, Laurent A, Abdalla EK, Chaudhury P, Dutson E, Gamblin C, D’Angelica M, Nagorney D, Testa G, Labow D, Manas D, Poon RT, Nelson H, Martin R, Clary B, Pinson WC, Martinie J, Vauthey JN, Goldstein R, Roayaie S, Barlet D, Espat J, Abecassis M, Rees M, Fong Y, McMasters KM, Broelsch C, Busuttil R, Belghiti J, Strasberg S, Chari RS, World Consensus Conference on Laparoscopic Surgery (2009) The international position on laparoscopic liver surgery: The Louisville Statement, 2008. Ann Surg 250:825–830
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, OʼRourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schön MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Slankamenac K, Graf R, Barkun J, Puhan MA, Clavien PA l (2013) The comprehensive complication index: a novel continuous scale to measure surgical morbidity. Ann Surg Jul 258(1):1–7. https://doi.org/10.1097/SLA.0b013e318296c732
Abu Hilal M, Aldrighetti L, Dagher I, Edwin B, Troisi RI, Alikhanov R, Aroori S, Belli G, Besselink M, Briceno J, Gayet B, D’Hondt M, Lesurtel M, Menon K, Lodge P, Rotellar F, Santoyo J, Scatton O, Soubrane O, Sutcliffe R, Van Dam R, White S, Halls MC, Cipriani F, Van der Poel M, Ciria R, Barkhatov L, Gomez-Luque Y, Ocana-Garcia S, Cook A, Buell J, Clavien PA, Dervenis C, Fusai G, Geller D, Lang H, Primrose J, Taylor M, Van Gulik T, Wakabayashi G, Asbun H, Cherqui D (2017) The southampton consensus guidelines for laparoscopic liver surgery: from indication to implementation. Ann Surg. https://doi.org/10.1097/SLA.0000000000002524
Gruttadauria S, Tropea A, Pagano D, Guarini A, Liotta R, Ling T, Tuzzolino F, Luca A, Vizzini G, Gridelli B (2016) Mini-invasive approach contributes to expand the indication for liver resection for hepatocellular carcinoma without increasing the incidence of posthepatectomy liver failure and other perioperative complications: a single-center analysis. J Laparoendosc Adv Surg Tech A 26(6):439–446. https://doi.org/10.1089/lap.2016.0134
Sposito C, Battiston C, Facciorusso A, Mazzola M, Muscarà C, Scotti M, Romito R, Mariani L, Mazzaferro V (2016) Propensity score analysis of outcomes following laparoscopic or open liver resection for hepatocellular carcinoma. Br J Surg 103(7):871–880. https://doi.org/10.1002/bjs.10137
Cheung TT, Dai WC, Tsang SH, Chan AC, Chok KS, Chan SC, Lo CM (2016) Pure laparoscopic hepatectomy versus open hepatectomy for hepatocellular carcinoma in 110 patients with liver cirrhosis: a propensity analysis at a single center. Ann Surg 264(4):612–620. https://doi.org/10.1097/SLA.0000000000001848
Gumbs AA, Gayet B (2008) Video: the lateral laparoscopic approach to lesions in the posterior segments. J Gastrointest Surg 12(7):1154. https://doi.org/10.1007/s11605-007-0455-x
Ettorre GM, Levi Sandri GB, Santoro R, Vennarecci G, Lepiane P, Colasanti M, Felli E, de Werra E, Colace L, D’Offizi G, Montalbano M, Visco U, Maritti M, Antonini M, Santoro E (2015) Laparoscopic liver resection for hepatocellular carcinoma in cirrhotic patients: single center experience of 90 cases. Hepatobiliary Surg Nutr 4(5):320–324. https://doi.org/10.3978/j.issn.2304-3881.2015.06.13
Ishizawa T, Gumbs AA, Kokudo N, Gayet B (2012) Laparoscopic segmentectomy of the liver: from segment I to VIII. Ann Surg 256(6):959–964. https://doi.org/10.1097/SLA.0b013e31825ffed3
Guro H, Cho JY, Han HS, Yoon YS, Choi Y, Jang JS, Kwon SU, Kim S, Choi JK (2017) Laparoscopic liver resection of hepatocellular carcinoma located in segments 7 or 8. Surg Endosc. https://doi.org/10.1007/s00464-017-5756-x
Jang JY, Han HS, Yoon YS, Cho JY, Choi Y, Lee W, Shin HK, Choi HL (2017) Three-dimensional laparoscopic anatomical segment 8 liver resection with glissonian approach. Ann Surg Oncol 24(6):1606–1609. https://doi.org/10.1245/s10434-017-5778-6
Kirchner VA, Kim KH, Kim SH, Lee SK (2017) Pure laparoscopic right anterior sectionectomy for hepatocellular carcinoma with great vascular exposure. Surg Endosc 31(8):3349–3350. https://doi.org/10.1007/s00464-016-5349-0
Tarantino G, Magistri P, Serra V, Berardi G, Assirati G, Ballarin R, Di Benedetto F (2017) Laparoscopic liver resection of right posterior segments for hepatocellular carcinoma on cirrhosis. J Laparoendosc Adv Surg Tech A 27(6):559–563. https://doi.org/10.1089/lap.2016.0506
Levi Sandri GB, Colasanti M, Santoro R, Ettorre GM (2015) Laparoscopic right hepatectomy for hepatocellular carcinoma in cirrhotic patient. Hepatobiliary Surg Nutr 4(6):436–438. https://doi.org/10.3978/j.issn.2304-3881.2015.07.01
Krüger JA, Fonseca GM, Coelho FF, Jeismann V, Herman P (2017) Laparoscopic right hepatectomy for cirrhotic patients: Takasaki’s Hilar control and caudal approach. Ann Surg Oncol 24(2):558–559. https://doi.org/10.1245/s10434-016-5288-y
Yoon YI, Kim KH, Kang SH, Kim WJ, Shin MH, Lee SK, Jung DH, Park GC, Ahn CS, Moon DB, Ha TY, Song GW, Hwang S, Lee SG (2017) Pure laparoscopic versus open right hepatectomy for hepatocellular carcinoma in patients with cirrhosis: a propensity score matched analysis. Ann Surg 265(5):856–863. https://doi.org/10.1097/SLA.0000000000002072
Amato B, Aprea G, De Rosa D, Milone M, di Domenico L, Amato M, Compagna R, Santoro M, Johnson LB, Sanguinetti A, Polistena A, Avenia N (2017) Laparoscopic hepatectomy for HCC in elderly patients: risks and feasibility. Aging Clin Exp Res Feb 29(Suppl 1):179–183. https://doi.org/10.1007/s40520-016-0675-6
Gil E, Kwon CHD, Kim JM, Choi GS, Heo JS, Cho W, Gwak MS, Gwak GY, Joh JW (2017) Laparoscopic liver resection of hepatocellular carcinoma with a tumor size larger than 5 cm: review of 45 cases in a tertiary institution. J Laparoendosc Adv Surg Tech A. https://doi.org/10.1089/lap.2016.0575
Levi Sandri GB, de Werra E, Mascianà G, Colasanti M, Lepiane P, Vennarecci G, D’Andrea V, Ettorre GM (2016) Laparoscopic and robotic approach for hepatocellular carcinoma-state of the art. Hepatobiliary Surg Nutr Dec 5(6):478–484. https://doi.org/10.21037/hbsn.2016.05.05
Levi Sandri GB, Spoletini G, Vennarecci G, Francone E, Abu Hilal M, Ettore GM (2018) Laparoscopic liver resection for large HCC: short- and long-term outcomes in relation to tumor size. Surg Endosc. https://doi.org/10.1007/s00464-018-6225-x
Cipriani F, Fantini C, Ratti F, Lauro R, Tranchart H, Halls M, Scuderi V, Barkhatov L, Edwin B, Troisi RI, Dagher I, Reggiani P, Belli G, Aldrighetti L, Abu Hilal M (2017) Laparoscopic liver resections for hepatocellular carcinoma. Can we extend the surgical indication in cirrhotic patients? Surg Endosc. https://doi.org/10.1007/s00464-017-5711-x
Cheung TT, Lo CM (2015) Laparoscopic liver resection for hepatocellular carcinoma in patients with cirrhosis. Hepatobiliary Surg Nutr 4(6):406–410. https://doi.org/10.3978/j.issn.2304-3881.2015.06.12
Acknowledgements
Collaborators of the I Go MILS Group on HCC: Adelmo Antonucci, (Policlinico di Monza, Monza); Giulio Belli, (Ospedale SM Loreto Nuovo, Napoli); Stefano Berti, (Ospedale Civile S. Andrea, La Spezia); Ugo Boggi, (AOU Pisana, Pisa); Pasquale Bonsignore, (IRCCS-ISMETT, Palermo); Alberto Brolese, (Ospedale S. Chiara, Trento); Fulvio Calise, (Ospedale Pinetagrande, Castel Volturno); Graziano Ceccarelli, (Ospedale San Donato, Arezzo); Michele Colledan, (AO Papa Giovanni XXIII, Bergamo); Andrea Coratti, (AOU Careggi, Firenze); Fabio Ferla, (ASST Grande Ospedale Metropolitano Niguarda, Milan); Antonio Floridi, (AO Ospedale Maggiore, Crema); Antonio Frena, (Ospedale Centrale, Bolzano); Antonio Giuliani, (AO R. N. Cardarelli, Napoli); Felice Giuliante, (Policlinico Gemelli, Rome); Gian Luca Grazi, (Istituto Nazionale Tumori Regina Elena, Roma); Enrico Gringeri, (University of Padua, Padova); Guido Griseri, (Ospedale San Paolo, Savona); Maurizio Iaria, (Parma University Hospital, Parma); Elio Jovine, (Ospedale Maggiore, Bologna); Magistri Paolo, (University of Modena and Reggio Emilia); Pietro Maida, (Ospedale Villa Betania, Napoli); Pietro Mezzatesta, (Casa di Cura La Maddalena, Palermo); Nadia Russolillo, (Ospedale Mauriziano Umberto I, Torino); Giuseppe Navarra, (AOU Policlinico G. Martino, Messina); Amilcare Parisi, (AO Santa Maria di Terni, Terni); Antonio Daniele Pinna, (Policlinico Sant’Orsola Malpighi, Bologna); Francesca Ratti, (IRCCS San Raffaele Hospital, Milano); Giorgio Ettore Rossi, (Policlinico di Milano, Milano); Andrea Ruzzenente, (University of Verona, Verona); Roberto Santambrogio, (AO San Paolo, Milano); Andrea Scotti, (San Camillo Hospital, Rome); Giovanni Sgroi, (AO Treviglio-Caravaggio, Treviglio); Abdallah Slim, (AO Desio e Vimercate, Vimercate); Guido Torzilli, (Istituto Clinico Humanitas, Rozzano); Leonardo Vincenti, (AOU Consorziale Policlinico, Bari); Matteo Virdis, (University of Milan, Milano) and Fausto Zamboni, (Ospedale Brotzu, Cagliari).
Author information
Authors and Affiliations
Consortia
Corresponding authors
Ethics declarations
Disclosure
Giovanni Battista Levi Sandri Giuseppe Maria Ettorre, Luca Aldrighetti, Umberto Cillo, Raffaele Dalla Valle, Alfredo Guglielmi, Vincenzo Mazzaferro, Alessandro Ferrero, Fabrizio Di Benedetto, Salvatore Gruttadauria, Luciano De Carlis, and Giovanni Vennarecci have no conflicts of interest or financial ties to disclose.
Additional information
Collaborators of the I Go MILS Group on HCC are listed in “Acknowledgments” section.
Rights and permissions
About this article
Cite this article
Levi Sandri, G.B., Ettorre, G.M., Aldrighetti, L. et al. Laparoscopic liver resection of hepatocellular carcinoma located in unfavorable segments: a propensity score-matched analysis from the I Go MILS (Italian Group of Minimally Invasive Liver Surgery) Registry. Surg Endosc 33, 1451–1458 (2019). https://doi.org/10.1007/s00464-018-6426-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6426-3