Abstract
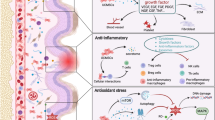
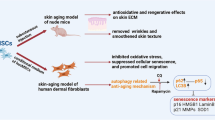
Skin is the largest organ in the body and the first defense to resist various diseases and external stimuli that easily cause infection and inflammation. Aseptic inflammation, barrier damage, and foreign aid pressure induce the destruction and damage to the skin microenvironment. Subsequently, it destroys the skin’s physiological function, leading to the maintenance and circulation of steady-state imbalance and aggravating the process of skin disorders. Our study evaluated the therapeutic potential of the secretome of human umbilical cord mesenchymal stem cells (UC-CM) for dermatological diseases in adult human skin cells, ex vivo skin tissue, and a 3D skin model. Our data suggested several advantages of UC-CM due to (1) their low cytotoxicity and sensitization properties; (2) their anti-inflammatory capacity for treating inflammatory chronic cutaneous diseases; (3) their enhanced capacity of the skin barrier for treating abnormal barrier metabolism; and (4) their positive impact on restoring skin homeostasis due to effective regulation ability of skin physiological function including cell apoptosis, detoxification, and anti-aging. We thus envisage that the possibility of harnessing the therapeutic potential of UC-CM might benefit patients suffering from inflammatory skin disorders such as atopic dermatitis, acne, and psoriasis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The human skin is the largest and most complex organ that serves as a physical barrier and protects the body from being invaded (Lephart 2016). Its dysfunction leads to the development of many skin diseases, especially inflammatory skin diseases (Spergel et al. 1998; Montero-Vilchez et al. 2021). Inflammatory skin diseases, such as atopic dermatitis (AD) (Shin et al. 2020; Leshem et al. 2020; Wallach and Taïeb 2014) and psoriasis (Ring et al. 2012; Eichenfield et al. 2014), reduce the quality of life, which is a major public concern (Spergel et al. 1998). A better clinical quality scheme is still challenging for the clinical management of some skin disorders, especially for patients who have debilitating systemic autoimmune and inflammatory skin conditions and are non-responsive to regular therapies. Mesenchymal stem cell (MSC)-based therapies can be used for treating skin diseases, as they provide new cells for epidermal homeostasis and repairing injured tissue (Wong et al. 2015; Kim et al. 2017; Guo et al. 2020). However, some disadvantages limit their application, including low implantation efficiency, unexpected differentiation risk, risk of tumor formation, short half-life, difficulties in quality control, and high storage requirements (Shin et al. 2020; Park et al. 2018; Bhang et al. 2014). MSCs provide a tissue-specific microenvironment through paracrine signaling for regulating inflammation and regeneration (Kim et al. 2017). According to some studies, the secretome from MSC (MSC-Sec) exhibits the same characteristics as MSC and might replace live cell application (Caplan 2007) to provide an opportunity to treat skin disease.
MSC-Sec, also known as a conditioned medium, contains a large number of bioactive molecules secreted by MSCs, such as proteins, microRNA, growth factors, antioxidants, proteasomes, and exosomes (Damayanti et al. 2021). These factors facilitate communication between cells to help skin regeneration (Le Blanc et al. 2003; Tang et al. 2004; Damayanti et al. 2021). MSC-Sec therapy has key advantages over MSC-based applications of resolved safety profiles of tumorigenicity and emboli formation. It is also more practical for clinical applications since it is convenient and suitable for skin application scenarios. Based on their accessibility, umbilical cord-derived MSCs (UCMSCs), with higher proliferation capacity, immunomodulatory activity, plasticity, and self-renewal capacity, are the second leading source used in clinical studies (Xiang et al. 2020; Cruz-Barrera et al. 2020). Comprehensive preclinical research results have shown that the mechanism of UC-CM (secretome from UCMSCs) in skin application (Montero-Vilchez et al. 2021) includes rapid wound closure (Li et al. 2017), improved proliferation and migration of various dermal cells (Li et al. 2017), protection from UV radiation by a reduction in ROS formation (Liu et al. 2013), regulation of polarized macrophages (Zhang et al. 2020b), and inhibition of inflammation and fibrosis (Xiang et al. 2020; Zhang et al. 2020b). However, most of these studies focused on wound healing and rejuvenation, while lesser attention was paid to the progress in the treatment of inflammatory skin diseases. However, two clinical trials confirmed the potential of MSC-Sec in treating inflammatory skin diseases with positive results of improvements in skin barrier function in AD patients (Kim et al. 2020) and a decrease in psoriatic plaques in psoriasis scalp patients (Seetharaman et al. 2019).
The skin is critical for ensuring homeostasis, and the loss of the integrity of the skin occurs in several inflammatory skin diseases, particularly in AD (Alwan and Di Meglio 2021). Several preclinical and clinical studies have found that UC-CM helps to maintain tissue homeostasis by repairing the skin and providing immunity against inflammatory skin diseases (Robert et al. 2019; Fernández-Gallego et al. 2021; Mackenzie 1969; Liu et al. 2019). Despite the therapeutic success of UC-CM in clinical studies, the potential targets and mechanisms of action in maintaining skin homeostasis by regulating cell function and eliminating dysfunctional cells remain unknown. Thus, for inflammatory skin diseases, a better clinical quality scheme is required before more detailed scientific studies can validate its safety and effectiveness.
In this study, we determined the role of UC-CM in maintaining the integrity of the barrier, inhibiting inflammation, and regulating the skin microenvironment, which shapes cell functions, such as cell detoxification and ECM secretion. To support our hypothesis, we established UV-induced human skin cells and ex vivo skin tissue or sodium dodecyl sulfate (SLS)-induced 3D skin model and found that UC-CM is involved in many aspects of skin physiology, which has implications in inflammatory skin disease management.
Materials and methods
Isolation, culture, identification of human UCMSC, and UC-CM preparation
Human umbilical cords were harvested after obtaining written informed consent with ethic approval. UCMSC isolation was performed in the Current Good Manufacturing Practice (cGMP)-accredited laboratory and cultured in mesenchymal stem cells basic medium (MSC-BM, Beijing Yocon Biology Co., Ltd, China) supplemented with a serum-free replacement. In the fifth passage, UCMSCs (P5) were starved for 24 h and recultured for 48 h, then UC-CM were harvested for identity test. Subsequently, UC-CM was subjected to sequential centrifugation at 800 g for 5 min and 2000 g for 10 min to remove larger particles and cell debris and stored at −20 °C for further analyses.
UCMSCs were analyzed using flow cytometry to examine the expression of cell surface markers for UCMSC characterization (Alhasan et al. 2016). The MSCs were labeled with mouse anti-human FITC-CD73 (Biolegend, USA), PE-CD90 (Biolegend, USA), PE-CD34 (Biolegend, USA), APC-HLA-DR (Biolegend, USA), PE-CD45 (Biolegend, USA), PE-CD105-PE (Biolegend, USA), and FITC-CD44 (Biolegend, USA). The flow cytometry data analysis software (Flowing Software, v2.5.1, www.flowingsoftware.com) was used to plot the results. In addition, Alizarin red staining was used for osteogenic identification, Oil red O staining for adipogenic differentiation, and Alcian blue and safranin O staining for chondrogenic differentiation.
Cell culture and UV irradiation
Unless indicated otherwise, cell lines were cultured in the following media: HaCaT and HUVEC were grown in DMEM (Invitrogen, USA) supplemented with 10% FBS (Invitrogen, USA), and HSF cells in DMEM supplemented with 15% FBS. All cell lines were purchased from ATCC and grown at 37 °C, 5% CO2 in a humidified atmosphere. For some experiments, cells were subjected to UVB irradiation at 70 mJ/cm2 by a UV lighter (Waldmann, Schwenningen, Germany) when > 90% confluency was achieved (Kim et al. 2009).
Cytotoxicity assay
HaCaT, HUVEC, and HSF cells were seeded into 96-well microplates (100 μL/well) at a density of 1 × 104 cells/well for 24 h. According to the manufacturer’s instructions, UC-CM was treated for another 48 h and tested using cell counting Kit-8 (Beyotime, China). The absorbance of the experimental group was recorded using molecular devices (Thermo, USA) at a 450-nm wavelength and reported as cell relative growth rate (RGR%) [(average optical density of test materials-Blank)/(average negative control-Blank) × 100%] to evaluate the cytotoxicity grade according to the 5-level (0–4) definition (see the notation under Table 1) of ISO-10993–5 (Cao et al. 2009).
Skin irritation test of multiple applications
The New Zealand white rabbits purchased from Shanghai Songjiang Chedun experimental animal breeding farm Co., Ltd (Shanghai, China) were used in this experiment, and the dorsal skin of each rabbit was divided into four regions for 0.5-mL applications of UC-CM and PBS, respectively, twice a day for 14 days for irritation test. The test regions’ irritation scores were obtained by assessing the extent of erythema and edema based on the criteria reported previously (Paolino et al. 2002). Average irritation scores = (erythema reaction scores + dropsy reaction scores) / amount of animals.
Morphology and inflammatory factors testing of EpiKutis inflammatory model
EpiKutis® (3D epidermal skin model) was purchased from Guangdong Biocell Biotechnology Co., Ltd and treated as mentioned in Table 1. EpiKutis was transferred to a 6-well plate with 0.9-mL TA culture solution (Gibco, USA), and 25 μL 0.2% SLS (Sigma, L6026, Germany) working solution was added to the surface of negative control (NC). In the sample group, 12.5 μL 0.4% SLS and 12.5 μL 100% UC-CM were added to the model surface. The model medium directly replaced the blank control (BC). After treatment, all the models were incubated at 37 °C, 5% CO2 for 24 h, and the model culture solution was collected and stored in –80 °C refrigerator until ELISA analysis. IL-1α (IL-1α ELISA kit, Abcam, British), TNF-α (TNF-α ELISA kit, Abcam, USA), and PGE2 (PGE2 ELISA kit, Abcam, USA) analyses were carried out according to the manufacturer’s instructions. Then, the remaining liquid inside and outside the models was cleaned, fixed by 4% paraformaldehyde, and sliced for H&E staining. The skin tissues were observed and documented using a microscope.
Immunofluorescence staining of EpiKutis
After SLS was treated, EpiKutis® (Guangdong Biocell Biotechnology Co., Ltd, China) was ring-cut and fixed with 4% paraformaldehyde for 24 h for further use. The sample was blocked for 1 h, stained with primary antibody (LOR antibody, Abcam, USA; FLG antibody, Abcam, USA), at 4 °C overnight, and followed with FITC-conjugated secondary antibody (Goat anti-rabbit IgG, Abcam, USA; Goat anti-mouse IgG, Abcam, USA) for 1 h at room temperature. Cell nuclei were stained with Hoechst 33342 (Invitrogen, Paisley, UK), observed, and documented under the fluorescence microscope (Leica; DM2500, Germany).
Reverse transcription-quantitative (real-time) polymerase chain reaction (RT-qPCR)
According to the manufacturer’s instructions, the total RNA from the cells was isolated using an RNApure Tissue kit (CWBIO, Beijing, China), and first-strand cDNA was synthesized using a ReverTra Ace-α® kit (Toyobo, Osaka, Japan). Primers were designed using DNAman software (Lynnon Biosoft, San Ramon, USA) as follows: human collagen I (Col I) sense, 5′-5′-GAG AGC ATG ACC GAT GGA TT and anti-sense, 5′-CCT TCT TGA GGT TGC CAG TC; human MMP-1 sense, 5′-TGG ACC TGG AGG AAA TCT TG and anti-sense, 5′-GGT ACA TCA AAG CCC CGA TA; human β-actin sense, 5′-CTTCC TGGGCATGGAGTC and anti-sense, 5′-GCCGATCCACACGGAGTA. RT-qPCR was performed using Ultra SYBR Mixture (CWBIO, Beijing, China) on a QuantStudio3 PCR detection system (Thermo Fisher Scientific, USA), and the transcriptional levels of target genes were quantified using the 2−ΔΔCt method (Livak and Schmittgen 2001) and expressed as the means ± SD from triplicate experiments.
Enzyme-linked immunosorbent assay (ELISA)
HaCaT or HSF cells were exposed to UVB as described above, cleaned with PBS, and cultured with or without UC-CM for 48 h. The culture was collected and measured by human IL-1 alpha ELISA Kit (BOSTER, Wuhan, China), human TNF-α ELISA Kit (BOSTER, Wuhan, China), human Col I ELISA kit (Cusabio Biotech Co., Ltd, Wuhan, China), and human MMP-1 ELISA kit (Cusabio Biotech Co., Ltd, Wuhan, China) according to the manufacturer’s instructions at a 450-nm wavelength.
Western blotting
Cells were exposed to UVB, re-cultured for 24 h, and all cells and lysed were collected using T-PER Tissue Protein Extraction Reagent (Thermo Fisher Scientific, Rockford, IL). Proteins were quantified using a BCA Protein Assay Kit (Beyotime, China), and equal amounts of proteins were loaded onto 10% gradient SDS-PAGE. After membrane transfer, blots were blocked with 5% nonfat milk in PBS for 1 h at 37 °C, and incubated with mouse anti-human FLG or anti-β-tubulin I IgG1 (Sigma, USA) overnight at 4 °C, washed, and stained with respective HRP-conjugated secondary antibodies for 1 h at room temperature. Subsequently, signals were detected using a Chemi Doc XRS+ system (Bio-Rad, Hercules, CA).
Cellular senescence detection
Natural passage aging and UVB-treated HSFs were used to detect senescence. HSF cells were continuously cultured for 5, 15, and 30 generations. The P5 generation HSF cells were treated with UVB as described above. HSF cells cultured in 6-well plates were fixed and stained with senescence cells histochemical staining Kit (Sigma, USA) at 37 °C overnight and identified using light microscopy (OLYMPUS, Japan).
Intracellular ROS generation
ROS production was quantified using flow cytometry as previously described (Leoncini et al. 1991; Maresca et al. 2010). Briefly, cells were subjected to UVB as described previously and cultured for 12 h with or without UC-CM at different concentrations and detected using a DCFH-DA kit (Beyotime, China). Briefly, cells were incubated with DCFH-DA (1 mM) at 37 °C in the dark for 30 min, washed thrice immediately, and resuspended in PBS. Intracellular ROS production was measured using a flow cytometer (BD FACSCelesta, USA).
Ex vivo skin culture, UVA/UVB exposure, and Masson staining
Ex vivo skin was obtained from Guangdong Biocell Biotechnology Co., Ltd (Guangzhou, China). The freshly obtained skin tissue was immersed in 75% alcohol, washed for 30 s, and subsequently washed with PBS. The skin tissue was cut into small disks and placed into the culture mold, with the epidermis facing up and the dermis facing down. The culture mold was then transferred into a 6-well plate containing an isolated skin tissue culture medium (FSK4, Gibco, USA) and incubated at 37 °C with 5% CO2. After 24-h incubation, isolated skin tissues were subjected to UVA 30 J/cm2 and UVB 50 mJ/cm2 for 4 days. After each irradiation, the culture medium of the negative control group was changed, and the sample group was replaced with the corresponding working fluid and added UC-CM (2 μL) on the tissue surface. After 4 days of continuous irradiation, the skin tissue in vitro was cultured for 3 days, stained using Masson staining, and observed under a microscope. Micrographs were processed using Image-ProⓇPlus Image processing software to analyze the collagen fibers.
Statistical analysis
All experiments were performed in triplicates. The results were reported as the average value standard deviation unless otherwise stated. Data were statistically analyzed using the Prism 5 software program and compared using Student’s t-test. Data with p < 0.05 was considered statistically significant.
Results
Characterization and identification of UCMSC
MSC activity affects the active secretome in a conditioned medium (UC-CM). Therefore, we first characterized the characteristic molecule markers of UCMSC and verified its differentiation ability in vitro by detecting adipogenic, osteogenic, and chondrogenic differentiation ability. Immunophenotypes of MSC showed a high expression of CD73 (99.8%), CD90 (100%), CD105 (98.4%), and CD44 (97.6%) and a low expression of CD45 (0.097%), CD34 (0.94%), and HLA-DR (0.015%) (Fig. 1a–b″). In addition, the positive results of Oil red O, Alizarin red S, Alcian blue, and safranin O staining proved the multi-lineage differentiation potential of UCMSC (Fig. 1c–f). Thus, this indicated that UCMSC used to produce UC-CM had good activity and characterization.
Characterization of UCMSCs and safety evaluation of UC-CM. a–b″ UCMSCs were positive for CD73, CD90, CD105, and CD44, and negative for CD45, CD34, and HLA-DR, as shown by flow cytometry analysis. The multi-lineage differentiation of UCMSCs into c adipocytes (Oil red O staining, upper left, scale bar: 50 μm), d osteoblasts (Alizarin red S staining, upper right, scale bar: 300 μm), e and f chondrocytes (safranin O staining, lower left and Alcian blue staining, lower right, scale bar: 100 μm). g Detection of cytotoxicity of UC-CM. HaCaT, HSF, and HUVEC cells were treated with or without UC-CM for 48 h. The proliferation of all cells was detected using the CCK8 test, and the relative growth rate (RGR%) was calculated. *vs. corresponding NC, p < 0.05. h, h′, h″, h‴ Skin irritation test of multiple applications. Photographs of multiple skin irritation tests in New Zealand rabbits at day 14. Control = PBS, CM = 100% UC-CM, n = 4
Detection of cytotoxicity and skin irritation of UC-CM
A cytotoxicity assay and multiple skin irritation tests at cell or animal levels were conducted to evaluate the safety of UC-CM in skin application. The cytotoxicity of UC-CM after 48-h cell treatment is presented in Table 2 and Fig. 1g. All experimental groups showed no (toxicity grade-0) or low cytotoxicity (toxicity grade = 1) for three cell types (HaCaT\HSF\HUVEC). The concentration of UC-CM under 50% could promote cell proliferation compared with negative control (NC), while at 70% or 100%, it could decrease cell proliferation in HaCaT and HSF cells, except HUVEC cells.
The results of the skin irritation test for multiple applications of UC-CM (14 days) in New Zealand rabbits are presented in Table 3 and Fig. 1h–h‴, indicating no irritation to normal skins after continuous applications for 14 days compared with NC. In brief, the current experiment corroborated the low cytotoxicity and no-irritation of UC-CM to skin local applications, and thus the concentration of UC-CM at 50 or 100 percent was used in the subsequent experiments.
Therapeutic potential of UC-CM by anti-inflammatory effect and improving skin barrier function in the 3D dermal model
A 3D dermal model (EpiKutis®) exposed to 0.2% SLS treatment which can enhance oxidative stress and increase the release of inflammatory factors, such as interleukin (IL)-1α, prostaglandin E2 (PGE2), destroys the skin barrier and leads to the occurrence of skin inflammatory reaction was used to determine the therapeutic potential of UC-CM in the skin. Firstly, the effect of UC-CM on the tissue morphology and viability of the 3D skin model was examined. There was no significant difference in the tissue viability of the 3D skin model when treated with UC-CM compared with the NC group (Fig. 2a). Simultaneously, H&E staining was performed on the model after culture to evaluate UC-CM’s ability to repair barrier damage. As reported, 0.2% SLS resulted in visible tissue damage, with the stratum granulosum being no longer distinguishable from the stratum spinosum in EpiDerm cultures (Gibbs et al. 2002). In the 3D dermal model, compared with the BC group, the NC group had indistinguishable granular layer and spinous layer, loose and thickened cuticle (marked by yellow arrow), decreased number of living cell layers (marked by green arrow), and vacuoles appeared (black circle), indicating an effective SLS stimulation condition (Fig. 2b–b″). Compared with the NC group, even though the number of viable cell layers did not improve, the tissue morphology improved by fewer vacuoles and thinner cuticles after UC-CM administration.
Tissue viability, morphology, and inflammatory factor of 3D EpiKutis® model. Viability (a) and histological examination (b, b′, b″) analysis of EpiKutis model. i: Stratum corneum; ii: granular layer; iii: spinous layer; iv: basal layer. Yellow arrow: cuticle; green arrow: living cell layer; black circle: vacuoles. Scale bar: 50 μm. BC, black control; NC, SLS treatment; CM, SLS + UC-CM treatment. ELISA for IL-1α (c), TNF-α (d), and PGE2 (e). **vs BC, p < 0.01, ***p < 0.001; #vs NC, p < 0.05, ##p < 0.01; ns, not significant
Meanwhile, three important inflammatory factors were detected in the 3D skin model. The IL-1 and tumor necrosis factor (TNF) families of cytokines play important roles in immune regulation and inflammatory processes (Barksby et al. 2007; Hänel et al. 2013). PGE2 is a major inflammatory mediator involved in skin disorders (Heard 2020). As shown in Fig. 2c–e, the content of IL-1α, TNF-α, and PGE2 in the NC group significantly increased (p < 0.01) compared with the BC group. Interestingly, the content of IL-1α and TNF-α significantly decreased compared with the NC group, while the PGE2 content did not change significantly after UC-CM treatment in the 3D skin model. The content changes of two skin barrier proteins, filaggrin (FLG) and loricrin (LOR), in the 3D skin model by immunofluorescence staining were compared to directly evaluate the role of UC-CM in repairing damaged skin barrier function. Dysregulation of FLG and LOR leads to epidermal barrier defects, resulting in skin fragility and sensitivity (Bigliardi et al. 2016; Odou et al. 2001). LOR and FLG were detectable with a strong signal in the BC group (Fig. 3a and d) but undetectable in the NC group (Fig. 3b and e). It is worth noting that a positive signal of FLG (Fig. 3c and g, p < 0.001) and a negative result of LOR (Fig. 3f and h, ns) were found in the CM group compared with the NC group. The data suggested that IL-1α, TNF-α, and FLG play an important role in anti-inflammatory and barrier repair by using UC-CM.
Barrier protein expression of 3D EpiKutis® model and verification of UV-irradiated HaCaT cell. a–f Image of immunofluorescence staining of FLG and LOR and relative IOD analysis of FLG (g) and LOR (h). Scale bar: 20 μm; BC, black control; NC, SLS treatment; CM, SLS + UC-CM treatment. i–j ELISA for IL-1 and TNF-α in HaCaT cell. k Western blotting for HaCaT. Con, control, *vs BC, p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001; #vs NC, p < 0.05, ##p < 0.01, ###p < 0.001; ns, not significant
UC-CM abrogated the skin microenvironment disorder due to UV radiation by enhanced detoxification ability
Excessive exposure to UV can damage various biological molecules, induce inflammatory responses, and increase the oxidative stress level, contributing to the skin microenvironment imbalance. Firstly, UVB-irradiated HaCaT cells were used to confirm the results obtained in the 3D model. Cells showed a 147% (p < 0.0001) higher IL-1 and 165% (p < 0.0001) higher TNF-α than non-irradiated cells (Fig. 3i and j). Treatment with 50% or 100% UC-CM led to a 22% (p < 0.05) and 28% (p < 0.01) decrease in IL-1 level and a 29% (p < 0.01) and 43% (p < 0.001) decrease in TNF-α, respectively, compared to the UV group. A decreased level of FLG was observed at protein level detecting by western blotting in the UV cell models associated with a slightly increased expression of FLG after UC-CM treatment (Fig. 3k).
The detoxification ability of the skin to deal with external pressure is reflected in its ability to eliminate stress responses, such as inhibition of cell apoptosis and ROS generation (Li et al. 2019). Thus, the detoxification ability of UC-CM at the cell level using UVB-irradiated HaCaT and HSF was discussed. Too little proliferation might yield thinner skin and loss of protection. As we found that UC-CM could improve cell proliferation (Fig. 1g), the study focused on its positive effects on decreasing cell apoptosis. The results showed that 50% and 100% UC-CM were able to protect the cells from UV-induced apoptosis (Fig. 4a–b‴) with average percentage of apoptosis 2.59% (p < 0.0001) and 1.01% (p < 0.0001) in HaCaT cells (Fig. 4c) or 9.74% (p < 0.0001) and 2.92% (p < 0.0001) in HSF cells (Fig. 4d) compared with the sole UV treated group (7.48% in HaCaTs or 16.68% in HSFs). Furthermore, our data indicated that 50% or 100% UC-CM was able to inhibit ROS production with relative mean fluorescence intensity of 2.80 (p < 0.01) and 1.24 (p < 0.001) in HaCaTs (Fig. 5a and c) or 1.42 (p < 0.01) and 1.2 (p < 0.01) in HSFs (Fig. 5b and d) compared with the UV group, and reduce the oxidative toxicity caused by the increase of free radical production source.
Effects of UC-CM on cell function by reducing ROS generation. Reactive oxygen species (ROS) intracellular level reduction and relative analysis in HaCaT cells (a, c) and HSF cells (b, d). Data are representative of three separate experiments. *vs control, p < 0.05, ***p < 0.001; ##vs UV, p < 0.01, ###p < 0.001
UC-CM protect HSFs from oxidative stress and contribute to maintaining skin homeostasis
Oxidative stress produces inflammatory factors and senescent cells that destroy the microenvironment, finally accelerating extracellular matrix (ECM) disassembly, providing pressure for the healthy maintenance of the skin (Koentges et al. 2019; Xiong et al. 2016; Bao et al. 2020). ECM, mainly secreted by skin fibroblasts, plays a crucial role in maintaining skin elasticity, improving the skin microenvironment, and strengthening the epidermal barrier. ECM’s ability for secretion and senescent cell deletion were evaluated in HSF cells. As one of the most important ECM components, collagen participates in cell physiological function. mRNA levels of col-I and mmp-1, two important contents of ECM responsible for collagen synthesis and decomposition, were evaluated using RT-qPCR. Our experiment indicated that UV irradiation significantly decreased the col-I expression and increased mmp-1 expression (Fig. 6a and b). This phenomenon was reversed by UC-CM protection followed by upregulation of col-I and downregulation of mmp-1 at the mRNA level, consistent at the protein level using ELISA assay (Fig. 6c and d). The above results were further confirmed by the Masson staining of collagen fibers in UV-irradiated ex vivo skin tissue. As shown in Fig. 6e–e″ and f, the collagen fiber content in the NC group significantly decreased compared with the BC group, whereas it significantly increased in the CM group compared with the NC group. Thus, suggesting that UC-CM could protect skin from ultraviolet damage, adjust ECM composition, and strengthen skin defense.
Effects of UC-CM on ECM secretion. Quantitative RT-PCR for col I (a) and mmp-1 (b) and ELISA test for Col I (c) and MMP-1 (d). mRNA and protein levels of collagen I (Col I) and matrix metalloproteinase (MMP-1) with or without UC-CM treatment in UV-induced HSF cells were detected by RT-qPCR and ELISA. The relative transcriptional levels of target genes were quantified using the 2−ΔΔCt method. The values shown are the means ± SD from triplicate experiments. Image of Masson staining in skin tissue (e, e′, e″) and relative statistical results (f). BC, black control; NC, SLS treatment; CM, SLS + UC-CM treatment; *vs corresponding control, p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001; #vs corresponding UV, p < 0.05, ###p < 0.001, ####p < 0.0001
The activity of SA-β-gal in natural passage HSF cells and UV-irradiated HSF cells with or without UC-CM treatment was evaluated. In young HSF culture, all groups’ senescent HSF cell ratio was low. In the intermediate (P15) and senescent (P30) group, the senescent HSF cell ratio was lower than in the control group (p < 0.05 in P15; p < 0.01 in P30) after UC-CM treatment (Fig. 7a–c″ and d). Protection by 50% UC-CM decreased senescent ratio in UV-irradiated HSF cells (p < 0.05) than the UV group, while HSF cells exhibited similar trends to 100% UC-CM protection group (p < 0.05, Fig. 7e–e‴ and f).
Effects of UC-CM on cell function by reducing senescent cells. a–c″ Morphology and SA-β-Gal expression of young (P5), intermediate (P15), and senescent (P30) HSF cells with or without UC-CM treatment, scale bar: 30 μm. e, e′, e″, e‴ Morphology and SA-β-Gal expression in HSF under UV irradiation after UC-CM treatment, scale bar: 50 μm. d, f Analysis of cellular senescence. *vs corresponding control, p < 0.05,**p < 0.01, ***p < 0.001; #vs UV, p < 0.05; ns, not significant
Discussion
MSC-Sec is considered to be a therapeutic agent because of its promising clinical features in skin disorders (Kim et al. 2020; Seetharaman et al. 2019). However, the mechanism by which they treat inflammatory skin disorders is still unclear. Defects in the development of the skin barrier occur in skin diseases, including AD and psoriasis (Elias et al. 2008; Hänel et al. 2013). As the main barrier in contact with the external environment, the intact skin barrier is crucial for the maintenance of tissue homeostasis (Akdis 2021). Inflammatory skin disease is associated with an imbalance in the internal environment of the skin, including biochemical defects, imbalance in immune responses, and abnormalities of the cytokine system (Farzanfar et al. 2018; Kim et al. 2020). Extrinsic damage, such as that caused by UVR, increases ROS formation; damages DNA, lipids, and proteins; destroys the extracellular matrix (ECM); and promotes cell apoptosis and cell aging, which accelerates inflammatory damage (Lephart 2016). Overall, skin homeostasis is a series of pathological events that occurs during crosstalk between cells and the microenvironment of the skin, and its imbalance initiates cell dysfunction, which leads to the occurrence and development of dermatological diseases. In this study, we addressed the therapeutic potential of the UC-CM for dermatological diseases using ex-vivo skin tissue and a 3D skin model to determine its ability to maintain skin homeostasis.
First, the secretome of UCMSC through the conditioned medium was obtained, and its safety was evaluated by performing cytotoxicity and skin irradiation tests with continuous applications for 14 days at the cell and animal levels. Our results suggested that UC-CM could improve cell proliferation in HaCaT, HSF, and HUVEC cells under 50% concentration, as excessive concentration might change the composition of the basic culture medium when cultured. One hundred percent concentration of UC-CM application was found to be safe using New Zealand rabbits by conducting continuous multiple skin irritation experiments.
The SLS pre-treatment is a highly reproducible and effective procedure for barrier disruption (Döge et al. 2017). Additionally, SLS can cause the cells to release a large quantity of the inflammatory factor IL-1α, a cytokine that is often used as an early marker for skin irritation (Gibbs et al. 2002; Müller-Decker et al. 1998; Welzel et al. 1996). We selected SLS irritation in EpiKutis® to mimic the skin environment with intensified inflammation and barrier disruption. The cultured tissues were evaluated by performing histomorphometry and determining tissue activity. We found that, although UC-CM did not improve tissue activity, the tissue morphology improved in the CM group. Basal cell vacuolization, which is the most prominent feature, was one of the primary morphological changes in interface dermatitis (Joshi 2013). After UC-CM treatment, a reducing vacuolar in living cells was found compared to the BC group. The stratum corneum (SC) in the epidermis acts in homeostatic control and blocks the formation of ROS (Rocha and Bagatin 2018). Exogenous stimulation promotes epidermal hyperplasia and mediates inflammation in human skin cells (Zhao et al. 2021). Compared to the SC of the BC group, the SC of the CM group was loose and thickened but was better than that of the NC group. To determine whether SC improvement occurred, we further examined the changes in two important proteins, including the filament-forming FLG and the structural protein LOR, which are responsible for the formation of a physically stronger barrier in SC.
Next, we examined the effect of UC-CM on the release of pro-inflammatory factors. Skin resident cells produce cytokines resulting in a complex network of signaling molecules that affect the quality of the skin barrier (Hänel et al. 2013). Based on the SLS stimulation of EpiKutis®, UC-CM was found to mainly inhibit IL-1 α and TNF-α, but not PGE2 expression, in the SLS-induced 3D skin model in our study. The difference between the three cytokines is that TNF-α and IL-1α affect immune system-based inflammation processes, especially as an innate immune response, while PGE2 is a major factor in all types of skin inflammation (Ahuja et al. 2008; Gholijani et al. 2017; Agard et al. 2013). We speculated that UC-CM might promote skin immunity and affect the skin barrier through different regulatory pathways. This regulatory function makes IL-1α and TNF-α have synergistic effects, which is different from the effects of PGE2. Previous studies have shown that IL-α and TNF-α have a strong synergistic effect on the expression of CXCL8 and b-defensin 2 (BD2) in psoriatic skin (Guilloteau et al. 2010). Some studies have also shown that PGE2 helps to mobilize skin dendritic cells (DCs) to drain lymph nodes (dLNs) in an IL-1-independent manner in skin infection (Krmeská et al. 2022). DC migration is necessary for initiating adaptive immunity, indicating that PGE2 also participates in adaptive immunity. Additionally, IL-1α and TNF-α are strong pro-inflammatory cytokines (Jin et al. 2021), and a decrease in their expression has positive therapeutic effects on recovering FLG involved in the formation of the skin barrier (Hänel et al. 2013). Specifically, TNF-α is expressed abnormally in psoriasis patients (Portugal-Cohen et al. 2012; Pasparakis 2012), and targeting it in psoriasis patients significantly reduces the disease symptoms (Pasparakis 2012). IL-1α leads to hyperkeratosis (O'Shaughnessy et al. 2010), and consistent with this concept, we found that an improvement in tissue morphology by thinner cuticles after UC-CM treatment might be due to a decrease in IL-1α levels (Fig. 2b″). The above-mentioned results support the therapeutic potential of UC-CM in the treatment of inflammatory skin diseases.
Disruption of the epidermal barrier is an important trigger in abnormal cutaneous inflammation (Zhang et al. 2020a). Pro-inflammatory cytokines can alter the expression of proteins involved in skin barrier function (Furue 2020); for example, TNF-α inhibits the expression of the FLG and LOR mRNAs in calcium differentiated keratinocytes (Kim et al. 2011). In many studies, FLG and LOR were found to be the main indicators of barrier function improvement and had a synergistic effect. For example, Elaeagnus L gum polysaccharides (EAP) inhibited the production of several information mediators and increased FLG and LOR (Wang et al. 2021). The extracts of Terminalia chebula (TC), a deciduous tree, can increase the skin barrier establishment by upregulating the expression of the LOR and FLG mRNA and protein levels (Swindell et al. 2020). Our results suggested that UC-CM could increase the level of the barrier protein FLG without affecting the LOR expression, but both decreased in the NC group. LOR promotes the maturation of corneocytes and is an essential effector of cornification in the uppermost layer of stratum granulosum, (Ishitsuka and Roop 2021) while the primary function of FLG is to maintain corneocyte humidity. FLG participates in epidermal differentiation and contributes to the structural and functional integrity of the horny layer (Rocha and Bagatin 2018) and strongly influences the balance of the internal environment of the skin (Cabanillas and Novak 2016). During differentiation of the granular layer, FLG undergoes degradation that leads to the formation of the natural moisturizing factor (NMF), which is crucial for the maintenance of a healthy SC (Rocha and Bagatin 2018; Celleno 2018). On the other hand, the degradation products of FLG facilitate skin hydration and an acidic environment, which are crucial for the optimal activity of enzymes involved in skin inflammation, lipid synthesis, and desquamation (Kim and Lim 2021). Abnormalities in the integrity of the skin barrier are mainly associated with reduced FLG production in AD (Scharschmidt et al. 2009; Kawasaki et al. 2012). We speculated that UC-CM might have medical value in the treatment of AD.
In the above-mentioned study, we found that UC-CM treatment can significantly reduce the expression of TNF-α in skin inflammation. While according to the report, TNF-α induces epidermal cell death and apoptosis (Zhao et al. 2021). Therefore, we hypothesized that UC-CM might enhance the defense function of the skin by improving the skin microenvironment. Subsequently, the therapeutic potential of UC-CM for dermatological diseases was evaluated based on cell functions, such as ECM secretion and cell detoxification. An increase in inflammatory factors was shown in UV-irradiated cell models, and FLG expression in HaCaT cells agreed with the 3D model. As reported, proteases, ROS, and pro-inflammatory cytokines induce tissue breakdown and impair physiological healing of the skin (Fisher 2005). New and old cells alternate to promote skin cell renewal via cell proliferation (Nguyen and Aragona 2021) and take rapid actions to recover cell functions, such as the reduction of reactive oxygen species (ROS) and removal of aging cells (Pignolo et al. 2020). In another study, we found that UC-CM can protect HaCaT and HSF cells from UV radiation by reducing ROS generation and cell apoptosis. On the other hand, we found activated SA-β-gal in both natural passage cultured old HSF cells and UVB-radiated young HSF cells, while UC-CM protection could significantly reduce the number of senescent cells. Our results suggested that UC-CM could effectively regulate and positively affect the restoration of skin homeostasis and enhance the anti-oxidation and anti-apoptosis ability of the skin to effectively resist endogenous damage.
UC-CM includes numerous cytokines (Ratajczak et al. 2012; Deng et al. 2018), which remodel the extracellular matrix in injured organs (Ratajczak et al. 2012). Collagen fiber is an important part of ECM. It is tough and plays an important role in maintaining skin tissue morphology and function (Shmulevich and Krizhanovsky 2021). The breakdown of collagen and the increase in MMP-1 are the key features of the pathology of various inflammatory skin diseases (Chung et al. 2001). According to our results, IL-1α increased in the UV-induced cell models. IL-1 triggers the production of MMPs (Kalinski 2012), which can degrade collagen. Thus, we determined the expression of the Col-I and MMP-1 mRNA and protein levels. A positive regulation function of col-I and negative regulation of mmp-1 was found at the mRNA and protein level in our study, indicating the function of UC-CM in adjusting the components of ECM. Similar results were also obtained in the human adipose-derived mesenchymal stem cell-conditioned medium-treated UVB-induced human skin cells (Li et al. 2019).
A complex skin environment network affects the homeostasis, metabolism, and barrier function of the skin leading to the occurrence and development of dermatological diseases (Lephart 2016; Shmulevich and Krizhanovsky 2021; Ovadya et al. 2018). The most important aspect of our study was the examination of the role of UC-CM in regulating immune response, skin barrier, and cell function. Considering that this is the first study on the role of UC-CM in maintaining skin homeostasis, some doubts need to be addressed. For example, which aspect of UC-CM plays a key role in the above-mentioned functions. Cytokine balance is essential for efficient barrier formation, and the management of cytokine expression and activity is important for controlling and ameliorating the development of skin diseases (Vizoso et al. 2017). The balance between anti-inflammatory cytokines (such as tumor necrosis factor β1 (Zagoura et al. 2012), IL-13, and neurotrophin-3 (Bermudez et al. 2016)) and pro-inflammatory cytokines (such as IL1β (Zagoura et al. 2012), IL6 (Cantinieaux et al. 2013; See et al. 2011), IL8 (Mirabella et al. 2011; Lee et al. 2011), and IL9 (Lee et al. 2011)) in UC-CM might determine the final effect. However, the UC-CM can provide exosomes (Exo). UC-Exo is produced and released by UCMSC and plays key immunomodulatory roles in the pathogenesis of various inflammatory skin diseases (Kim et al. 2019), such as psoriasis (Cheung et al. 2016; Jiang et al. 2019), AD (Kim et al. 2019), and systemic lupus erythematosus (SLE) (Kim et al. 2019). To summarize, the different regulatory abilities of UC-CM to perform immune regulation and mediate functional differences in barrier proteins need to be highlighted in greater detail.
In conclusion, our study highlighted the cosmetic or therapeutic applications of UC-CM on skin barrier dysfunction and abnormal skin homeostasis using ex vivo skin tissue, a 3D skin model, and human cells. We studied the biological effects of UC-CM on anti-inflammatory and skin barrier repair ability and also showed the importance of safety profiles. We found that cell function, which contributes to skin homeostasis, improved in UV-induced adult human skin cells after UC-CM treatment. We reported that the features of UC-CM in maintaining skin homeostasis might serve as an effective therapeutic strategy with a low risk of side effects. Thus, this therapeutic technique can overcome the limitations of inflammatory skin treatment in use.
References
Agard M, Asakrah S, Morici LA (2013) PGE(2) suppression of innate immunity during mucosal bacterial infection. Front Cell Infect Microbiol 3:45
Ahuja M, Dhake AS, Sharma SK, Majumdar DK (2008) Topical ocular delivery of NSAIDs. AAPS J 10:229–241
Akdis CA (2021) Does the epithelial barrier hypothesis explain the increase in allergy, autoimmunity and other chronic conditions? Nat Rev Immunol 21:739–751
Alhasan L, Qi A, Rezk AR, Yeo LY, Chan PP (2016) Assessment of the potential of a high frequency acoustomicrofluidic nebulization platform for inhaled stem cell therapy. Integr Biol 8:12–20
Alwan W, Di Meglio P (2021) Guardians of the barrier: microbiota engage AHR in keratinocytes to mantain skin homeostasis. Cell Host Microbe 29:1213–1216
Bao J, Chen Z, Xu L, Xiong Y (2020) Rapamycin protects chondrocytes against IL-18-induced apoptosis and ameliorates rat osteoarthritis. Aging 12:5152–5167
Barksby HE, Lea SR, Preshaw PM, Taylor JJ (2007) The expanding family of interleukin-1 cytokines and their role in destructive inflammatory disorders. Clin Exp Immunol 149:217–225
Bermudez MA, Sendon-Lago J, Seoane S, Eiro N, Gonzalez F, Saa J, Vizoso F, Perez-Fernandez R (2016) Anti-inflammatory effect of conditioned medium from human uterine cervical stem cells in uveitis. Exp Eye Res 149:84–92
Bhang SH, Lee S, Shin JY, Lee TJ, Jang HK, Kim BS (2014) Efficacious and clinically relevant conditioned medium of human adipose-derived stem cells for therapeutic angiogenesis. Mol Ther 22:862–872
Bigliardi PL, Dancik Y, Neumann C, Bigliardi-Qi M (2016) Opioids and skin homeostasis, regeneration and aging - what’s the evidence? Exp Dermatol 25:586–591
Cabanillas B, Novak N (2016) Atopic dermatitis and filaggrin. Curr Opin Immunol 42:1–8
Cantinieaux D, Quertainmont R, Blacher S, Rossi L, Wanet T, Noël A, Brook G, Schoenen J, Franzen R (2013) Conditioned medium from bone marrow-derived mesenchymal stem cells improves recovery after spinal cord injury in rats: an original strategy to avoid cell transplantation. PLoS ONE 8:e69515
Cao BM, Tingfei XI, Zheng YD, Yang LF, Zheng Q (2009) Cupric ion release and cytotoxicity for Yuangong Cu-IUDs and the release behavior of indomethacin for medicated 220 Cu-IUD. Chin Sci Bull 54:3160–3166
Caplan AI (2007) Adult mesenchymal stem cells for tissue engineering versus regenerative medicine. J Cell Physiol 213:341–347
Celleno L (2018) Topical urea in skincare: a review. Dermatol Ther 31:e12690
Cheung KL, Jarrett R, Subramaniam S, Salimi M, Gutowska-Owsiak D, Chen YL, Hardman C, Xue L, Cerundolo V, Ogg G (2016) Psoriatic T cells recognize neolipid antigens generated by mast cell phospholipase delivered by exosomes and presented by CD1a. J Exp Med 213:2399–2412
Chung JH, Seo JY, Choi HR, Lee MK, Youn CS, Rhie G, Cho KH, Kim KH, Park KC, Eun HC (2001) Modulation of skin collagen metabolism in aged and photoaged human skin in vivo. J Invest Dermatol 117:1218–1224
Cruz-Barrera M, Flórez-Zapata N, Lemus-Diaz N, Medina C, Galindo CC, González-Acero LX, Correa L, Camacho B, Gruber J, Salguero G (2020) Integrated analysis of transcriptome and secretome from umbilical cord mesenchymal stromal cells reveal new mechanisms for the modulation of inflammation and immune activation. Front Immunol 11:575488
Damayanti RH, Rusdiana T, Wathoni N (2021) Mesenchymal stem cell secretome for dermatology application: a review. Clin Cosmet Investig Dermatol 14:1401–1412
Deng H, Sun C, Sun Y, Li H, Yang L, Wu D, Gao Q, Jiang X (2018) Lipid, protein, and microRNA composition within mesenchymal stem cell-derived exosomes. Cell Reprogram 20:178–186
Döge N, Avetisyan A, Hadam S, Pfannes EKB, Rancan F, Blume-Peytavi U, Vogt A (2017) Assessment of skin barrier function and biochemical changes of ex vivo human skin in response to physical and chemical barrier disruption. Eur J Pharm Biopharm 116:138–148
Eichenfield LF, Tom WL, Chamlin SL, Feldman SR, Hanifin JM, Simpson EL, Berger TG, Bergman JN, Cohen DE, Cooper KD, Cordoro KM, Davis DM, Krol A, Margolis DJ, Paller AS, Schwarzenberger K, Silverman RA, Williams HC, Elmets CA, Block J, Harrod CG, Smith Begolka W, Sidbury R (2014) Guidelines of care for the management of atopic dermatitis: section 1. Diagnosis and assessment of atopic dermatitis. J Am Acad Dermatol 71:116–132
Elias PM, Hatano Y, Williams ML (2008) Basis for the barrier abnormality in atopic dermatitis: outside-inside-outside pathogenic mechanisms. J Allergy Clin Immunol 121:1337–1343
Farzanfar D, Dowlati Y, French LE, Lowes MA, Alavi A (2018) Inflammation: a contributor to depressive comorbidity in inflammatory skin disease. Skin Pharmacol Physiol 31:246–251
Fernández-Gallego N, Sánchez-Madrid F, Cibrian D (2021) Role of AHR ligands in skin homeostasis and cutaneous inflammation. Cells 10:3176
Fisher GJ (2005) The pathophysiology of photoaging of the skin. Cutis 75:5–8 (discussion 8–9)
Furue M (2020) Regulation of filaggrin, loricrin, and involucrin by IL-4, IL-13, IL-17A, IL-22, AHR, and NRF2: pathogenic implications in atopic dermatitis. Int J Mol Sci 21:5382
Gholijani N, Ataollahi MR, Samiei A, Aflaki E, Shenavandeh S, Kamali-Sarvestani E (2017) An elevated pro-inflammatory cytokines profile in Behcet’s disease: a multiplex analysis. Immunol Lett 186:46–51
Gibbs S, Vietsch H, Meier U, Ponec M (2002) Effect of skin barrier competence on SLS and water-induced IL-1alpha expression. Exp Dermatol 11:217–223
Guilloteau K, Paris I, Pedretti N, Boniface K, Juchaux F, Huguier V, Guillet G, Bernard FX, Lecron JC, Morel F (2010) Skin inflammation induced by the synergistic action of IL-17A, IL-22, oncostatin M, IL-1{alpha}, and TNF-{alpha} recapitulates some features of psoriasis. J Immunol 184:5263–5270
Guo S, Wang T, Zhang S, Chen P, Cao Z, Lian W, Guo J, Kang Y (2020) Adipose-derived stem cell-conditioned medium protects fibroblasts at different senescent degrees from UVB irradiation damages. Mol Cell Biochem 463:67–78
Hänel KH, Cornelissen C, Lüscher B, Baron JM (2013) Cytokines and the skin barrier. Int J Mol Sci 14:6720–6745
Heard CM (2020) An ex vivo skin model to probe modulation of local cutaneous arachidonic acid inflammation pathway. J Biol Methods 7:e138
Ishitsuka Y, Roop DR (2021) The epidermis: redox governor of health and diseases. Antioxidants 11:47
Jiang M, Fang H, Shao S, Dang E, Zhang J, Qiao P, Yang A, Wang G (2019) Keratinocyte exosomes activate neutrophils and enhance skin inflammation in psoriasis. FASEB J 33:13241–13253
Jin Q, Teng F, Cheng Z (2021) Association between common polymorphisms in IL-1 and TNFα and risk of peri-implant disease: a meta-analysis. PLoS ONE 16:e0258138
Joshi R (2013) Interface dermatitis. Indian J Dermatol Venereol Leprol 79:349–359
Kalinski P (2012) Regulation of immune responses by prostaglandin E2. J Immunol 188:21–28
Kawasaki H, Nagao K, Kubo A, Hata T, Shimizu A, Mizuno H, Yamada T, Amagai M (2012) Altered stratum corneum barrier and enhanced percutaneous immune responses in filaggrin-null micee. J Allergy Clin Immunol 129:1538–1546
Kim BE, Howell MD, Guttman-Yassky E, Gilleaudeau PM, Cardinale IR, Boguniewicz M, Krueger JG, Leung DY (2011) TNF-α downregulates filaggrin and loricrin through c-Jun N-terminal kinase: role for TNF-α antagonists to improve skin barrier. J Invest Dermatol 131:1272–1279
Kim J, Bin BH, Choi EJ, Lee HG, Lee TR, Cho EG (2019) Staphylococcus aureus-derived extracellular vesicles induce monocyte recruitment by activating human dermal microvascular endothelial cells in vitro. Clin Exp Allergy 49:68–81
Kim KH, Blasco-Morente G, Cuende N, Arias-Santiago S (2017) Mesenchymal stromal cells: properties and role in management of cutaneous diseases. J Eur Acad Dermatol Venereol 31:414–423
Kim WS, Park BS, Park SH, Kim HK, Sung JH (2009) Antiwrinkle effect of adipose-derived stem cell: activation of dermal fibroblast by secretory factors. J Dermatol Sci 53:96–102
Kim Y, Lim KM (2021) Skin barrier dysfunction and filaggrin. Arch Pharm Res 44:36–48
Kim YJ, Ahn HJ, Lee SH, Lee MH, Kang KS (2020) Effects of conditioned media from human umbilical cord blood-derived mesenchymal stem cells in the skin immune response. Biomed Pharmacother 131:110789
Koentges C, Cimolai MC, Pfeil K, Wolf D, Marchini T, Tarkhnishvili A, Hoffmann MM, Odening KE, Diehl P, von Zur MC, Alvarez S, Bode C, Zirlik A, Bugger H (2019) Impaired SIRT3 activity mediates cardiac dysfunction in endotoxemia by calpain-dependent disruption of ATP synthesis. J Mol Cell Cardiol 133:138–147
Krmeská V, Aggio JB, Nylén S, Wowk PF, Rothfuchs AG (2022) Cyclooxygenase-derived prostaglandin E(2) drives IL-1-independent Mycobacterium bovis Bacille Calmette-Guérin-triggered skin dendritic cell migration to draining lymph node. J Immunol 208:2549–2557
Le Blanc K, Tammik C, Rosendahl K, Zetterberg E, Ringden O (2003) HLA expression and immunologic properties of differentiated and undifferentiated mesenchymal stem cells. Exp Hematol 31:890–896
Lee MJ, Kim J, Lee KI, Shin JM, Chae JI, Chung HM (2011) Enhancement of wound healing by secretory factors of endothelial precursor cells derived from human embryonic stem cells. Cytotherapy 13:165–178
Leoncini G, Maresca M, Colao C (1991) Oxidative metabolism of human platelets. Biochem Int 25:647–655
Lephart ED (2016) Skin aging and oxidative stress: equol’s anti-aging effects via biochemical and molecular mechanisms. Ageing Res Rev 31:36–54
Leshem YA, Wong A, McClanahan D, Simpson EL (2020) The effects of common over-the-counter moisturizers on skin barrier function: a randomized, observer-blind, within-patient, controlled study. Dermatitis 31:309–315
Li L, Ngo HTT, Hwang E, Wei X, Liu Y, Liu J, Yi TH (2019) Conditioned medium from human adipose-derived mesenchymal stem cell culture prevents UVB-induced skin aging in human keratinocytes and dermal fibroblasts. Int J Mol Sci 21:49
Li M, Luan F, Zhao Y, Hao H, Liu J, Dong L, Fu X, Han W (2017) Mesenchymal stem cell-conditioned medium accelerates wound healing with fewer scars. Int Wound J 14:64–73
Liu N, Matsumura H, Kato T, Ichinose S, Takada A, Namiki T, Asakawa K, Morinaga H, Mohri Y, De Arcangelis A, Geroges-Labouesse E, Nanba D, Nishimura EK (2019) Stem cell competition orchestrates skin homeostasis and ageing. Nature 568:344–350
Liu Q, Luo Z, He S, Peng X, Xiong S, Wang Y, Zhong X, Zhou X, Eisenberg CA, Gao BZ (2013) Conditioned serum-free medium from umbilical cord mesenchymal stem cells has anti-photoaging properties. Biotechnol Lett 35:1707–1714
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408
Mackenzie JC (1969) Ordered structure of the stratum corneum of mammalian skin. Nature 222:881–882
Maresca M, Colao C, Leoncini G (2010) Generation of hydrogen peroxide in resting and activated platelets. Cell Biochem Funct 10:79–85
Mirabella T, Cilli M, Carlone S, Cancedda R, Gentili C (2011) Amniotic liquid derived stem cells as reservoir of secreted angiogenic factors capable of stimulating neo-arteriogenesis in an ischemic model. Biomaterials 32:3689–3699
Montero-Vilchez T, Sierra-Sánchez Á, Sanchez-Diaz M, Quiñones-Vico MI, Sanabria-de-la-Torre R, Martinez-Lopez A, Arias-Santiago S (2021) Mesenchymal stromal cell-conditioned medium for skin diseases: a systematic review. Front Cell Dev Biol 9:654210
Müller-Decker K, Heinzelmann T, Fürstenberger G, Kecskes A, Lehmann WD, Marks F (1998) Arachidonic acid metabolism in primary irritant dermatitis produced by patch testing of human skin with surfactants. Toxicol Appl Pharmacol 153:59–67
Nguyen TM, Aragona M (2021) Regulation of tissue architecture and stem cell dynamics to sustain homeostasis and repair in the skin epidermis. Semin Cell Dev Biol 21:00243–00253
O’Shaughnessy RF, Choudhary I, Harper JI (2010) Interleukin-1 alpha blockade prevents hyperkeratosis in an in vitro model of lamellar ichthyosis. Hum Mol Genet 19:2594–2605
Odou P, Azar R, Luyckx M, Brunet C, Dine T (2001) A hypothesis for endogenous opioid peptides in uraemic pruritus: role of enkephalin. Nephrol Dial Transplant 16:1953–1954
Ovadya Y, Landsberger T, Leins H, Vadai E, Gal H, Biran A, Yosef R, Sagiv A, Agrawal A, Shapira A, Windheim J, Tsoory M, Schirmbeck R, Amit I, Geiger H, Krizhanovsky V (2018) Impaired immune surveillance accelerates accumulation of senescent cells and aging. Nat Commun 9:5435
Paolino D, Ventura CA, Fresta M, Puglisi G, Nistico S (2002) Lecithin microemulsions for the topical administration of ketoprofen: percutaneous adsorption through human skin and in vivo human skin tolerability. Int J Pharm 244:21–31
Park SR, Kim JW, Jun HS, Roh JY, Lee HY, Hong IS (2018) Stem cell secretome and its effect on cellular mechanisms relevant to wound healing. Mol Ther 26:606–617
Pasparakis M (2012) Role of NF-κB in epithelial biology. Immunol Rev 246:346–358
Pignolo RJ, Passos JF, Khosla S, Tchkonia T, Kirkland JL(2020)Reducing senescent cell burden in aging and disease. Trends Mol Med 26:630–638
Portugal-Cohen M, Horev L, Ruffer C, Schlippe G, Voss W, Ma’or Z, Oron M, Soroka Y, Frušić-Zlotkin M, Milner Y, Kohen R (2012) Non-invasive skin biomarkers quantification of psoriasis and atopic dermatitis: cytokines, antioxidants and psoriatic skin auto-fluorescence. Biomed Pharmacother 66:293–299
Ratajczak MZ, Kucia M, Jadczyk T, Greco NJ, Wojakowski W, Tendera M, Ratajczak J (2012) Pivotal role of paracrine effects in stem cell therapies in regenerative medicine: can we translate stem cell-secreted paracrine factors and microvesicles into better therapeutic strategies? Leukemia 26:1166–1173
Ring J, Alomar A, Bieber T, Deleuran M, Fink-Wagner A, Gelmetti C, Gieler U, Lipozencic J, Luger T, Oranje AP, Schafer T, Schwennesen T, Seidenari S, Simon D, Stander S, Stingl G, Szalai S, Szepietowski JC, Taieb A, Werfel T, Wollenberg A, Darsow U, European Dermatology Forum, European Academy of Dermatology and Venereology, European Task Force on Atopic Dermatitis, European Federation of Allergy, European Society of Pediatric Dermatology, Global Allergy and Asthma European Network (2012) Guidelines for treatment of atopic eczema (atopic dermatitis) Part II. J Eur Acad Dermatol Venereol 26:1176–1193
Robert AW, Azevedo Gomes F, Rode MP, Marques da Silva M, Veleirinho MBDR, Maraschin M, Hayashi L, Wosgrau Calloni G, Stimamiglio MA (2019) The skin regeneration potential of a pro-angiogenic secretome from human skin-derived multipotent stromal cells. J Tissue Eng 10:2041731419833391
Rocha MA, Bagatin E (2018) Skin barrier and microbiome in acne. Arch Dermatol Res 310:181–185
Scharschmidt TC, Man MQ, Hatano Y, Crumrine D, Gunathilake R, Sundberg JP, Silva KA, Mauro TM, Hupe M, Cho S, Wu Y, Celli A, Schmuth M, Feingold KR, Elias PM (2009) Filaggrin deficiency confers a paracellular barrier abnormality that reduces inflammatory thresholds to irritants and haptens. J Allergy Clin Immunol 124:496–506
See F, Seki T, Psaltis PJ, Sondermeijer HP, Gronthos S, Zannettino AC, Govaert KM, Schuster MD, Kurlansky PA, Kelly DJ, Krum H, Itescu S (2011) Therapeutic effects of human STRO-3-selected mesenchymal precursor cells and their soluble factors in experimental myocardial ischemia. J Cell Mol Med 15:2117–2129
Seetharaman R, Mahmood A, Kshatriya P, Patel D, Srivastava A (2019) Mesenchymal stem cell conditioned media ameliorate psoriasis vulgaris: a case study. Case Rep Dermatol Med 2019:8309103
Shin KO, Ha DH, Kim JO, Crumrine DA, Meyer JM, Wakefield JS, Lee Y, Kim B, Kim S, Kim HK, Lee J, Kwon HH, Park GH, Lee JH, Lim J, Park S, Elias PM, Park K, Yi YW, Cho BS (2020) Exosomes from human adipose tissue-derived mesenchymal stem cells promote epidermal barrier repair by inducing de novo synthesis of ceramides in atopic dermatitis. Cells 9:680
Shmulevich R, Krizhanovsky V (2021) Cell senescence, DNA damage, and metabolism. Antioxid Redox Signal 34:324–334
Spergel JM, Mizoguchi E, Brewer JP, Martin TR, Bhan AK, Geha RS (1998) Epicutaneous sensitization with protein antigen induces localized allergic dermatitis and hyperresponsiveness to methacholine after single exposure to aerosolized antigen in mice. J Clin Invest 101:1614–1622
Swindell WR, Bojanowski K, Chaudhuri RK (2020) A standardized Terminalia chebula fruit extract alters the expression of genes associated with skin architecture and barrier formation. Eur J Dermatol 30:469–492
Tang YL, Zhao Q, Zhang YC, Cheng L, Liu M, Shi J, Yang YZ, Pan C, Ge J, Phillips MI (2004) Autologous mesenchymal stem cell transplantation induce VEGF and neovascularization in ischemic myocardium. Regul Pept 117:3–10
Vizoso FJ, Eiro N, Cid S, Schneider J, Perez-Fernandez R (2017) Mesenchymal stem cell secretome: toward cell-free therapeutic strategies in regenerative medicine. Int J Mol Sci 18:1852
Wallach D, Taïeb A (2014) Atopic dermatitis/atopic eczema. Chem Immunol Allergy 100:81–96
Wang B, Tai M, Zhang K, Chen H, Gan X, Che B, Abudukelimu N, Wang G, Xin X, Lin L, Han P, Peng Y, Du Z, Aker Aisa H (2021) Elaeagnus L gum polysaccharides alleviate the impairment of barrier function in the dry skin model mice. J Cosmet Dermatol 20:647–656
Welzel J, Wilhelm KP, Wolff HH (1996) Skin permeability barrier and occlusion: no delay of repair in irritated human skin. Contact Dermatitis 35:163–168
Wong SP, Rowley JE, Redpath AN, Tilman JD, Fellous TG, Johnson JR (2015) Pericytes, mesenchymal stem cells and their contributions to tissue repair. Pharmacol Ther 151:107–120
Xiang E, Han B, Zhang Q, Rao W, Wang Z, Chang C, Zhang Y, Tu C, Li C, Wu D (2020) Human umbilical cord-derived mesenchymal stem cells prevent the progression of early diabetic nephropathy through inhibiting inflammation and fibrosis. Stem Cell Res Ther 11:336
Xiong Y, Wang M, Zhao J, Han Y, Jia L (2016) Sirtuin 3: a Janus face in cancer (Review). Int J Oncol 49:2227–2235
Zagoura DS, Roubelakis MG, Bitsika V, Trohatou O, Pappa KI, Kapelouzou A, Antsaklis A, Anagnou NP (2012) Therapeutic potential of a distinct population of human amniotic fluid mesenchymal stem cells and their secreted molecules in mice with acute hepatic failure. Gut 61:894–906
Zhang J, Wu J, Sun M, Zhang S, Huang J, Man M, Hu L (2020a) Phospholipase C epsilon mediates cytokine cascade induced by acute disruption of epidermal permeability barrier in mice. Biochem Biophys Rep 24:100869
Zhang S, Chen L, Zhang G, Zhang B (2020b) Umbilical cord-matrix stem cells induce the functional restoration of vascular endothelial cells and enhance skin wound healing in diabetic mice via the polarized macrophages. Stem Cell Res Ther 11:39
Zhao Y, Chen Y, Li X, Sun Y, Shao Y, Zhang Y, Liu Z (2021) RIPK1 regulates cell function and death mediated by UVB radiation and TNF-α. Mol Immunol 135:304–311
Funding
This research was funded by China National Key R&D Program during the 14th Five-year Plan Period (Grant No. 2021YFA1101500).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval and informed consent
Human umbilical cords were harvested with written informed consent from the donor through the Yantai Yuhuangding Hospital with ethical approval ([2021]003). All procedures performed involving human participants in experiments were carried out per ethical standards of the institutional and/or national research committee and the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, X., Wang, Q., Yin, P. et al. Secretome of human umbilical cord mesenchymal stem cell maintains skin homeostasis by regulating multiple skin physiological function. Cell Tissue Res 391, 111–125 (2023). https://doi.org/10.1007/s00441-022-03697-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-022-03697-8