Abstract
It is well known that sepsis and inflammation reduce male fertility. Within the testis, toll-like receptor 3 (TLR3) is constitutively expressed and recognizes double-stranded RNA (dsRNA) from viruses, degraded bacteria, damaged tissues and necrotic cells. To characterize the potential role of TLR3 in response to testicular infections, its expression and downstream signaling were investigated upon challenge with lipopolysaccharides (LPS) in two mouse strains that differ in their immuno-competence regarding T cell-regulated immunity. Thereto, Balb/c and Foxn1nu mice were randomized into six interventional groups treated with either i.v. application of saline or LPS followed by 20 min, 5 h 30 min and 18 h of observation and two sham-treated control groups. LPS administration induced a significant stress response; the amplification was manifested for TLR3 and interleukin 6 (IL6) mRNA in the impaired testis 5 h 30 min after LPS injection. TLR3 immunostaining revealed that TLR3 was primarily localized in spermatocytes. The TLR3 expression displayed different temporal dynamics between both mouse strains. However, immunofluorescence staining indicated only punctual interferon regulatory factor 3 (IRF3) expression upon LPS treatment along with minor alterations in interferon β (IFNβ) mRNA expression. Induction of acute inflammation was closely followed by a significant shift of the Bax/Bcl2 ratio to pro-apoptotic signaling accompanied by augmented TUNEL-positive cells 18 h after LPS injection with again differing patterns in both mouse strains. In conclusion, this study shows the involvement of TLR3 in response to LPS-induced testicular inflammation in immuno-competent and -incompetent mice, yet lacking transmission into its signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sepsis is a systemic inflammatory state caused by the immune system’s response to serious infection. While it is well known that serious illness and inflammation reduce male fertility, the inflammatory pathways are not well understood. In this regard, lipopolysaccharides (LPS) were shown to compromise testicular function at multiple levels in vivo, notably transient testicular dysfunction accompanied by apoptosis of testicular germ cells (Kajihara et al. 2006).
Pathophysiologic mechanisms of sepsis are highly complex as there can be infectious and sterile triggers (Akira et al. 2006). It is known that either microbial components from infectious agents can initiate innate response through interaction with toll-like-receptors (TLRs) (Ward 2012), or in the case of sterile infection, endogenous factors such as nucleic acid, histones and heat shock proteins (Chen and Nunez 2010). During innate immune response, TLR3 plays an important role. It recognizes double-stranded RNA (dsRNA) from viruses, degraded bacteria, damaged tissues and necrotic cells (Alexopoulou et al. 2001). Moreover, TLR3 serves as an endogenous sensor of tissue necrosis independent of viral activation (Cavassani et al. 2008) and is able to trigger apoptosis (Glavan and Pavelic 2014). Presumably dsRNA induce apoptosis through a complex associating TLR3 to caspase-8 (Estornes et al. 2012).
The mammalian testis is an immuno-privileged organ with regard to its ability to tolerate both, allo- and auto-antigens (Fijak et al. 2011; Head and Billingham 1985). Particularly, Sertoli cells and testicular macrophages are decisive in maintaining the immuno-privileged status of the testis (Head et al. 1983). Still, abundant expressions of TLR1-TLR9 mRNAs have been reported in rat testis (Bhushan et al. 2008; Palladino et al. 2007). Focusing on the mouse testis, expressions of TLR2-TLR6 have been described in Sertoli cells, which also can be activated by their agonists and initiate testicular innate immune response (Riccioli et al. 2006; Starace et al. 2008; Wu et al. 2008). Besides Sertoli cells, constitutive TLR3 gene expression was detected in murine primary isolated Leydig cells (C57BL/6) (Shang et al. 2011) and primary isolated germ cells (C57BL/6) (Wang et al. 2012). Also in these testicular cells, TLR3 can be activated by a synthetic double-stranded RNA analogue (Shang et al. 2011; Wang et al. 2012).
Understanding of the molecular components of stress leading to apoptosis during infection-induced damage is an essential step towards the development of novel therapeutic strategies to control testicular injury during sepsis. Therefore, in the present study, the role of TLR3 in testicular stress response is evaluated during LPS-induced sepsis in two mouse strains that differ in their immuno-competence. The Balb/c strain disposes of an intact innate and acquired immune response, making it suitable for immunological research while the athymic Foxn1nu strain possesses a dysfunctional rudimentary thymus due to spontaneous deletion in the FOXN1 gene, consequently lacking T cell-mediated immunity. Yet, the cytotoxic cell-mediated response, initiated by natural killer (NK) and cytotoxic T lymphocytes (CTL), is central to eliminating virally infected and transformed cells by the immune system (Barry and Bleackley 2002). Given that TLR3 is also involved in viral defense via recognition of double-stranded RNA (dsRNA) (Alexopoulou et al. 2001), we aim at investigating whether this immuno-regulative deficit exerts a direct effect on testicular damage upon LPS challenge. Therefore, both mouse strains were subjected to systemic LPS as an important structural component of the outer membrane of gram-negative bacteria (Raetz and Whitfield 2002), which is one of the best studied immuno-stimulatory components of bacteria and reliably induces severe systemic inflammation and sepsis (Beutler and Rietschel 2003).
Materials and methods
Animals
Male Balb/c (OlaHsd) and athymic nude-Foxn1nu mice (Harlan), 3–5 weeks old, were kept in approved plastic cages, with water and food ad libitum and were housed in rooms equipped with a 12-h light cycle. All procedures involving animals were approved by the Animal Care and Use Committee of the state of Hesse in Germany (V54-19 c 20/15-FK/1037). Surgery and animal care were performed in accordance with the “Guide for the care and use of laboratory animals” (National Institutes of Health, volume 25, no. 28, revised 1996), EU Directive 86/609 EEC and German Protection of Animals Act.
Interventional groups and surgical procedure
Balb/c and Foxn1nu mice were randomized into six interventional groups (n = 8): three control groups with i.v. application of saline followed by 20 min, 5 h 30 min and 18 h of observation (designated as NaCl 20 min, NaCl 5 h 30 min and NaCl 18 h, respectively) as well as three groups with i.v. application of LPS followed by 20 min, 5 h 30 min and 18 h of observation (designated as LPS 20 min, LPS 5 h 30 min and LPS 18 h, respectively). Mice were anesthetized with an isoflurane-/O2 mixture (0.5 l O2/min and 2 vol% isofluran) in an induction box. Hereafter, 100 μl sterile saline versus 100 μl LPS solution (E. coli, serotype 0111:B4, L2630, Sigma Aldrich) at a dosage of 10 mg/kg body weight dissolved in 100 μl sterile saline was administered intravenously retrobulbary. Upon completion of the respective observation periods, animals were sacrificed and both testes of each animal were carefully removed. One was fixed in 4% paraformaldehyde overnight, the other was stored at − 80 °C until further processing. One testicle was consistently used for all qRT-PCR analyses and the contra-lateral testicle for immunofluorescence staining immunohistochemical staining, and TUNEL assay. Furthermore, one sham group of each mouse strain without any treatment (n = 6) was used as additional control.
Quantitative real-time polymerase chain reaction (qRT-PCR)
Total RNA was isolated from homogenized testis samples (interventional groups n = 8, sham groups n = 6) using peqGOLD TriFast™ (VWR), according to the manufacturer’s protocol. Next, cDNA was synthesized using a cDNA Synthesis Kit (5x Reaction Mix, no. R1362, Thermo Scientific). Gene expression profiles were assessed by qRT-PCR using a Peltier Thermo Cycler 200 IQ5 Multicolour RT-PCR-Detection System (Bio-Rad). Briefly, after a denaturation phase at 94 °C, followed by an annealing phase between 50 and 60 °C, a synthesis step at 74 °C was performed. Specificity was established by adding a melting curve analysis. Primer sequences are listed in Table 1. Relative changes in mRNA expression were calculated by normalizing the values to their corresponding β-actin expression using the 2-dCt method (Livak and Schmittgen 2001).
Immunofluorescence staining
Paraformaldehyde-fixed (4%) and paraffin-embedded testicles were sectioned at 5 μm of thickness. Sections (n = 4 per group) were deparaffinized overnight in xylene. The sections were rehydrated; antigens were retrieved in TEG buffer (10 mMTris, 0.5 mM EGTA, pH 9) and aldehyde groups were quenched in 50 mM NH4Cl in PBS. The sections were incubated overnight at 4 °C with primary antibodies directed against TLR3 (rabbit anti-mouse ab62566, Abcam, dilution 1:200) or interferon regulatory factor 3 (IRF3) (rabbit anti-mouse PA5–20086, Thermo Fisher Scientific, dilution 1:200). The following day, the sections were rinsed and incubated for 30 min at room temperature with secondary donkey anti-rabbit-649 antibody (DyLight™, no. 406406, BioLegend, dilution 1:400) and Hoechst (no. 33342, Invitrogen, 2 μg/mL), followed by mounting of coverslips using glycergel mounting medium (Dako/Agilent C0563) + 2.5 w/v% antifade (1,4-Diazabicyclo[2.2.2]octane (DABCO)). Imaging was performed using a Nikon EclipseTi-E system equipped with a × 40 air objective, a Perfect Focus 3 system and a Zyla sCMOS5.5 Megapixel camera (Andor) controlled by NIS Elements software from Nikon. The fluorescence illumination system was Cool LED-pE-300 white. Fluorescence filter sets were standard DAPI and Cy5. For imaging, 4 × 4 images were acquired and stitched using the NIS software. For each antibody stain and mouse strain exposure, time and light intensity were adjusted according to the brightest condition and the settings were kept constant for the acquisition of the remainder slides as Foxn1nu mice exhibited a slightly higher constitutive expression of TLR3 (Supplemental Fig. 1a, equal exposure). A positive and negative staining control for TLR3 specific expression was performed on sections from a murine kidney (C57BL/6 mice) 24 h after ischemia and reperfusion injury (Supplemental Fig. 1b) as previously published (Paulus et al. 2014). Image analysis was performed with Fiji Image J software (Schindelin et al. 2012).
Immunohistochemical staining
Immunohistochemistry was performed on paraffin-embedded sequential testicle sections at 5 μm of thickness in order to localize TLR3 expression within the testis (n = 2 per interventional group and control groups). For specific staining, slides were incubated with a primary germ cell-specific antigen antibody (TRA98) (rat anti-mouse ab82527, Abcam, dilution 1:100) and anti-TLR3 antibody (rabbit anti-mouse ab62566, Abcam, dilution 1:20) overnight at 4 °C. For signal development, slides were incubated with the respective horseradish peroxidase-conjugated secondary rabbit anti-rat (P0162, Dako, dilution 1:200) or goat anti-rabbit (P448, Dako, dilution 1:200) antibodies for 1 h at room temperature followed by DAB incubation and counterstaining with Mayer’s hematoxylin. Sections were examined with a Leica DMR microscope equipped with a Leica DFC320 camera. Images were transferred by a Leica TFC Twain 6.1.0 program and processed using Adobe Photoshop 8.0.
TUNEL assay
TUNEL-staining was performed according to the manufacturer’s protocol (ApopTag® Peroxidase In Situ Apoptosis Detection Kit, S7100, Milipore). Counterstaining was carried out with hematoxylin. Analysis of the slides was performed in a blinded fashion. At × 200 total magnification, all tubules of one testicle cross-section were analyzed by counting the total number of tubules as well as the total number of tubules with at least one TUNEL-positive nucleus. Results are presented as percentage (positive tubules/all tubules × 100) (n = 4–5 per interventional group, n = 2–3 for control groups). In order to evaluate the distribution of TUNEL-positive cells, the density in each TUNEL-positive tubule was evaluated by counting the number of TUNEL positive cells within each affected tubule (with at least one TUNEL-positive nucleus). Ten randomly chosen positive tubules per cross-section were analyzed and an average value was calculated for each cross-section of one animal (n = 4–5 per interventional group, n = 2–3 for control groups). Sections were examined with a Leica DM750 microscope equipped with a Leica ICC50 HD camera. Images were analyzed using Leica Application Suite EZ, Version 3.0.0.
Statistical analysis
Statistical analysis was performed applying GraphPadPrism® 5.02 software (GraphPad Software, La Jolla, CA, USA). The distribution of variables was tested for normality using the Kolmogorov-Smirnov test. Accordingly, statistical significance was calculated using either one-way ANOVA followed by Tukey’s multiple comparison test or Kruskal-Wallis test followed by Dunn’s posthoc test, where applicable. Significance of correlations was determined by Pearson’s test including all investigated groups. p values ≤ 0.05 were considered as statistically significant. In the figures, horizontal lines within the boxes represent the medians, boxes represent the interquartile range. Whiskers above and below the box indicate the 1.5 IQR. The individual points that are plotted beyond the whiskers represent outliers, which were included in the statistical analysis.
Results
Differing body and testicular weights between Balb/c and Foxn1nu mouse strains but unaltered constitutive IL6 and TLR3 mRNA expression
Balb/c mice mean body weight was insignificantly lower than the body weight of the Foxn1nu mice (18.98 g ± 0.71 vs. 20.35 g ± 0.48) (Fig. 1a). In contrast, the testicle weight of Balb/c mice displayed a significantly higher mean weight than those of Foxn1nu mice (67.79 mg ± 3.74 vs. 43.37 mg ± 1.64) (Fig. 1a′). Neither the constitutive testicular expression of IL6 nor TLR3 mRNA displayed significant differences between the mouse strains (ns) (Fig. 1b, b′).
Constitutional levels. To analyze relevant baseline levels of both mouse strains Balb/c and Fonxn1nu (n = 6 per group), we determined the average body (a) and testicular weight (a′). Furthermore, the basal IL6 and TLR3 mRNA expression relative to β-actin was analyzed in testicular tissue homogenates of sham animals (b, b′). ***p < 0.001
Increased inflammatory response in testicular tissue upon LPS challenge
First, we examined the IL6 gene expression, a typical marker of inflammatory response after systemic LPS injection (Fig. 2a, a′, a″). We detected a significant increase in testicular IL6 mRNA expression in both mouse strains 5 h 30 min after LPS injection in comparison to the corresponding saline-treated mice (p < 0.001) and the 20 min LPS-treated mice (p < 0.001). This marked increase was abolished 18 h after LPS injection (Fig. 2a, a′). Comparing both mouse strains, Balb/c mice displayed a significantly higher IL6 mRNA expression level than Foxn1nu mice at 5 h 30 min (p < 0.001) (Fig. 2a″).
Increased inflammatory response and TLR3 mRNA expression in testicular tissue upon LPS injection. To analyze IL6 (a–a″), TLR3 mRNA expression (b–b″) as well as TLR4 (d–d′) after LPS injection, we performed qRT-PCR analyses of their mRNA expression relative to β-actin in testicular homogenates (n = 8 per group). Corresponding correlations (Pearson’s test) (c–c′). *Significant difference between LPS and saline-treated mice at one point in time; ƒ, significant difference in the time course within LPS or saline-treated mice; x, significant difference between Balb/c and Foxn1nu mice. *p < 0.05, ***/xxx/ƒƒƒ p < 0.001
Systemic LPS increased testicular TLR3 but not TLR4 mRNA expression in both mouse strains
In both mouse strains, TLR3 mRNA expression displayed a similar trajectory as IL6 mRNA including a significant increase at 5 h 30 min after LPS injection in comparison to the corresponding saline-treated mice (p < 0.001) and 20 min LPS-treated mice (p < 0.001) (Fig. 2b, b′). While no significant difference between mouse strains with regard to their TLR3 mRNA expression levels could be detected (ns) (Fig. 2b″), we observed a positive correlation between testicular IL6 and TLR3 mRNA expression in Balb/c (Pearson r = 0.742; p < 0.001), as well as in Foxn1nu (Pearson r = 0.743; p < 0.001) mice potentially indicating a linkage between TLR3 and inflammatory signaling (Fig. 2c, c′). Furthermore, we analyzed TLR4 mRNA expression, as the receptor recognizes LPS and binding of LPS to TLR4 is well known to result in a pro-inflammatory response (Poltorak et al. 1998; Qureshi et al. 1999). However, in contrast to TLR3, TLR4 mRNA expression did not increase upon LPS treatment. TLR4 mRNA remained unaltered in Balb/c mice but decreased transiently 5 h 30 min after LPS exposure in Foxn1nu mice (Fig. 2d, d′).
TLR3 expression is constitutively expressed within spermatocytes of both mouse strains and induced upon LPS treatment
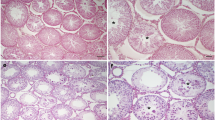
Consistent with the TLR3 mRNA expression analysis, constitutive (Fig. 3a–d″′) and induced (Fig. 4a–h″) TLR3 expression upon LPS treatment was explored in testicular tissue sections. To further localize TLR3 expression, we performed immunohistochemical investigations using a TLR3 and a specific germ cell marker (TRA98) antibody on sequential sections. As a result, sickle-shaped TLR3 expression was observed within the tubules and more precisely within spermatocytes in both mouse strains (Fig. 3a–d″′). In order to analyze TLR3 expression and distribution in comparison to LPS challenge, we performed immunofluorescence analyses. Representative pictures are shown in Fig. 4. As a result, Balb/c mice exhibited a relatively low and only focal TLR3 expression within the tubules in saline-treated mice and upon LPS treatment after 5 h 30 min. However, we detected a marked increase in expression 18 h after LPS treatment (Fig. 4a–d″). In contrast, Foxn1nu mice exhibited a higher constitutive expression of TLR3 equally within the tubules but there seemed to occur an acute decreased expression 5 h 30 min after LPS treatment reflected by only focal TLR3 expression. Yet, after 18 h of LPS exposure, the TLR3 expression regained similar intensity as observed in the control group (Fig. 4e–h″). Thus, in Foxn1nu mice, an increased expression of TLR3 after LPS administration, as observed in Balb/c mice, could not be detected. However, in both mouse strains, we found tubules with very intensive TLR3 expression, as well as with low and focal TLR3 expression. This corresponds to the observations made in the previous immunohistochemical microscopy (Fig. 3a–d″′).
Immunohistochemical localization of TLR3. To localize TLR3 expression, we performed immunohistochemical staining using a TLR3 and a specific germ cell (TRA98) antibody on sequential testicular tissue sections (n = 2 per group). Representative juxtaposed micrographs of Balb/c (a–b″′) as well as Foxn1nu (c–d″′) mice 18 h after injection of NaCl are displayed. TLR3 (vertical ←), spermatocytes (horizontal ←), Sertoli cells (black asterisk), spermatogonia (white asterisk)
Systemic LPS increased TLR3 protein expression. To analyze TLR3 expression upon LPS administration, we performed immunofluorescence staining of TLR3 in testicular tissue sections (n = 4 per group). Representative juxtaposed micrographs of Balb/c (a–d″) as well as Foxn1nu mice (e–h″) with LPS or saline treatment are displayed for each point of observation
Systemic LPS induced TLR3 expression in testicular mouse tissue but not its downstream pathway
To test whether TLR3 upregulation correlates with initiation of the subsequent signaling pathway, we examined IRF3 by immunohistochemistry and IFNβ as readout gene via qRT-PCR analyses (Fig. 5). IRF3 expression could not be detected 5 h 30 min after LPS administration (pictures not shown); however, 18 h after LPS injection, a weak punctual expression was observed within tubules in both Balb/c and Foxn1nu mice (Fig. 5a–d′). Regarding IFNβ, an elevated expression in Balb/c mice was seen but none in Foxn1nu mice (Fig. 5e, e″), which is in line with increased IRF expression in Balb/c mice (Fig. 5c–c″). In summary, only marginal activation of the subsequent signaling pathway can be assumed.
TLR3 signaling pathway was only marginally induced by systemic LPS administration. To analyze the TLR3 signaling pathway in response to LPS, we performed immunofluorescence staining of IRF3 in testicular tissue sections (n = 4 per group). Representative juxtaposed micrographs of Balb/c as well as Foxn1nu mice with LPS or saline treatment are displayed (a–d″). Background subtracted. qRT-PCR analyses of IFNβ mRNA relative to β-actin in testicular tissue homogenates (n = 8 per group) (e, e′). ƒ, significant difference in the time course within LPS or saline treated mice. ƒ p < 0.05
Systemic LPS treatment favored apoptosis in testicular tissue
Bax (Bcl2-associated X protein) represents a pro-apoptotic, whereas Bcl2 (B cell lymphoma 2), an anti-apoptotic key molecule, however, both acting together as regulators of cell apoptosis (Adams and Cory 1998). Therefore, we measured Bax and Bcl2 mRNA expression and calculated the Bax/Bcl2 ratio in testes homogenates of both mouse strains treated with LPS and corresponding controls. The Bax/Bcl2 mRNA ratio marginally increased 5 h 30 min after LPS injection in Balb/c mice and hereafter decreased significantly 18 h after LPS injection (p < 0.05) (Fig. 6a). In contrast, in Foxn1nu mice, an increase occurred temporarily delayed, lacking any alteration at 5 h 30 min but showing a significant increase in LPS-treated mice 18 h after LPS treatment in comparison to the corresponding saline-treated mice (p < 0.01) as well as to LPS-treated mice after 5 h 30 min (p < 0.01) (Fig. 6a′). This also resulted in a clear difference when comparing both mouse strains upon LPS injection: After 18 h, Foxn1nu mice displayed a significantly higher testicular Bax/Bcl2 mRNA ratio than Balb/c mice (p < 0.01) (Fig. 6a″), indicating enhanced apoptotic signaling. Consequently, we morphologically quantified apoptosis by TUNEL-staining (Fig. 6b–b″′, c–d″″). Animals that received LPS exhibited no altered apoptosis rates compared to saline-treated mice at 5 h 30 min (ns). In contrast, after 18 h, LPS-treated mice of both strains demonstrated a significantly increased apoptosis rate in testes in comparison to the corresponding saline-treated mice (p < 0.001) as well as to LPS-treated mice after 5 h 30 min (Balb/c, p < 0.01; Foxn1nu, p < 0.001). Notably, the density of TUNEL positive cells within TUNEL positive tubules (with at least one TUNEL positive nucleus) was strikingly different between both mouse strains 18 h after LPS injection (p < 0.001) (Fig. 6b″′). In this respect, Foxn1nu mice displayed a significantly higher density of TUNEL positive cells in affected tubules, whereas in Balb/c mice, the distribution of apoptotic cells appeared less dense (Fig. 6c″″, d″″).
Increased apoptosis within testicular tissue upon LPS injection. To provide an insight into apoptotic processes within testicular tissue, we performed qRT-PCR analyses of Bax and Bcl2 mRNA relative to β-actin and calculated their ratio (n = 8 per group) (a–a″). Further investigations encompassed TUNEL staining: TUNEL positive tubules (b–b″) as well as the TUNEL density (b″′) in affected tubules have been evaluated. Representative juxtaposed micrographs of Balb/c as well as Foxn1nu mice with LPS or saline treatment are displayed for each point of observation (n = 4–5 per interventional group, n = 2–3 for sham groups) (c–d″″). *Significant difference between LPS and saline-treated mice at one point in time; ƒ, significant difference in the time course within LPS or saline treated mice. x, significant difference between Balb/c and Foxn1nu mice. ƒ p < 0.05, **/xx/ƒƒ p < 0.01, ***/ƒƒƒ p < 0.001
Discussion
Growing evidence suggests that TLRs exert a prominent role in the response to infectious events. In the present study, we focused on the role of TLR3 as a potential mediator of testicular injury during sepsis, which initially has been characterized for its response to double-stranded RNA (Alexopoulou et al. 2001) and subsequently for its response to endogenous nucleic acids from necrotic cells (Baiersdorfer et al. 2010; Brentano et al. 2005; Kariko et al. 2004).
First, we characterized basal testicular TLR3 and pro-inflammatory IL6 mRNA in both employed Balb/c and Foxn1nu mouse strains regarding their anatomic preconditions and base line expression. Even though the body weight of both strains was almost equal, the mean testicular weight of Balb/c mice was significantly higher than in Foxn1nu mice. However, the constitutive expression of IL6 or TLR3 mRNA in the testis homogenates was virtually equal.
As expected, IL6 displayed a significant peak after 5 h 30 min after LPS injection and decreased to nearly basal level 18 h after LPS injection. This is in accordance with previous findings in rats where IL6 mRNA levels equally reached a maximum expression 6 h after LPS stimulation (O’Bryan et al. 2005; Winnall et al. 2011). This response was also reproducible in vitro, given that cultured mouse Sertoli cells (Riccioli et al. 1995) as well as rat Sertoli cells (Stephan et al. 1997) produced a marked IL6 production upon LPS stimulation. Also, LPS stimulation of cultured Leydig cells demonstrated a strong induction of major pro-inflammatory cytokines such as IL6 mRNA (Boockfor et al. 1994; Shang et al. 2011). Thus, the latter findings indicate that the applied LPS-treatment effectively provoked sepsis in our mouse model.
In comparison to other TLRs, TLR3 mRNA is frequently higher and moreover expressed in nearly all primary isolated rat testicular cell types (Bhushan et al. 2008). Bacterial LPS generally exerts its effects through the TLR4 receptor complex (Poltorak et al. 1998; Qureshi et al. 1999), resulting in a pro-inflammatory state characterized by the expression of TLR-response genes such as IL6. In this regard, recent studies revealed that Sertoli cells express TLR4 mRNA and protein in mouse and rat testis (Bhushan et al. 2008; Riccioli et al. 2006; Wu et al. 2008). Besides, Leydig cells, testicular macrophages (Winnall et al. 2011) as well as spermatocytes (Bhushan et al. 2008) seem to express TLR4 at basal levels in rat testis. Surprisingly, in an earlier study, testicular TLR4 was not acutely inducible by LPS (Winnall et al. 2011). Comparably, an increase in TLR4 mRNA upon LPS treatment did not become apparent in this present study neither, although the typical response gene IL6 was increased in testis homogenates in both mouse strains. These findings suggest that TLR4 mRNA expression may not be involved in testicular immune response, although known to function in LPS-TLR4 signaling during the innate immune response to LPS.
On the other hand, TLR3 mRNA expression, opposed to TLR4, was significantly inducible upon LPS injection in both mouse strains. Interestingly, the TLR3 expression displayed a similar trajectory as IL6 mRNA including a significant increase at 5 h 30 min. Accordingly, we observed a positive correlation between IL6 and TLR3 mRNA in Balb/c, as well as in Foxn1nu mice, thus possibly indicating a linkage between TLR3 and inflammatory signaling. However, as we analyzed whole testis homogenates not only cells of the seminiferous tubules but also immune cells such as macrophages within the interstitium are depicted in the results, too.
Next to the TLR3 gene expression analyses, we also histomorphologically examined TLR3 expression and regulation upon LPS treatment, which differed between both mouse strains. Balb/c mice exhibited a relatively low and only focal constitutive TLR3 expression within the tubules but marked increase in expression 18 h after LPS treatment. In contrast, Foxn1nu mice exhibited a higher constitutive expression of TLR3 equally within the tubules, but an acute decreased expression 5 h 30 min occurred after LPS treatment, which returned to base line 18 h after LPS treatment. Thus, in Foxn1nu mice, an increased expression of TLR3 after LPS administration, as observed in Balb/c mice, was not detected. However, localization of the TLR3 expression did not alter and was observed within the tubules and more precisely within spermatocytes in both mouse strains. It is characteristic in all sections with enhanced TLR3 expression, whether in Balb/c or Foxn1nu mice, that some tubules express TLR3 very intensively, whereas there is low and only focal TLR3 expression detectable in others. Hence, the TLR3 expression seems to be dependent on the spermatogenic stage. Even though expression of TLR3 has also been described in primary isolated murine Sertoli cells (Shang et al. 2011; Wu et al. 2008) and Leydig cells (Shang et al. 2011) besides primary isolated murine germ cells (Wang et al. 2012), altered cell biochemical and morphological characteristics during in vitro culture have to be considered (Sofikitis et al. 2005). Thus, comparison of in vivo findings with in vitro culture experiments remains difficult.
Referring to the TLR3 signaling pathway, TLR3 is known to induce antiviral responses by inducing IFNβ and IFNα through IRF3 activation (Akira and Takeda 2004). However, despite high expectations in view of the amplified TLR3 mRNA expression upon LPS treatment, our results uncovered only marginal further activation of its signaling pathway. Analyses concerning this matter showed only very weak immunohistochemical signals of IRF3 along with aptly very low and hardly altering IFNβ mRNA expression in response to LPS. Nevertheless, these findings may be comprehensible as IFNα/β induction depends on the level of the transcription factors IRF3 and IRF7 through a positive feedback mechanism (Taniguchi and Takaoka 2001).
LPS was shown to compromise testicular function at multiple levels in vivo, notably transient testicular dysfunction accompanied by apoptosis of testicular germ cells in mice (Kajihara et al. 2006). Besides, TLR3 is known to trigger apoptosis (Glavan and Pavelic 2014). Herein, the Bcl2 family is thought to regulate apoptosis by formation of hetero- and homodimers in the mitochondrial membrane and the prevailing outcome depends on the ratio of protector (Bcl2) to the promoter (Bax) of apoptosis (Adams and Cory 1998). In the present study, the inflammation generated in response to bacterial LPS also triggered the apoptotic pathway manifested by changes in the Bax/Bcl2 mRNA ratio and TUNEL staining. In Balb/c mice, the Bax/Bcl2 mRNA ratio marginally increased 5 h 30 min after LPS injection and decreased significantly 18 h after LPS injection. In contrast, Foxn1nu mice displayed a temporarily delayed increase lacking any alteration at 5 h 30 min but showing a significant increase in LPS-treated mice after 18 h. In this regard, Metukuri et al. (Metukuri et al. 2010) analyzed immunoblots of anti-apoptotic Bcl2/pro-apoptotic Bax in testicular whole-cell lysates from saline and LPS- (5 mg LPS/kg bw) injected rats. They showed that LPS treatment caused a significant decrease in Bcl2/Bax ratio as early as 12 up to 72 h post LPS treatment compared to saline-treated control rats (Metukuri et al. 2010). This is in line with our results as protein expression would be expected to be delayed in relationship to mRNA expression.
Furthermore, we morphologically validated a potential pro-apoptotic effect as indicated by an altered Bax/Bcl2 ratio via TUNEL staining. Apoptosis is considered to be the underlying mechanism of germ–cell death during normal spermatogenesis in various mammals (Sinha Hikim and Swerdloff 1999). Accordingly, in sham groups and saline-treated groups, scattered TUNEL-positive cells were detected. Yet, after 18 h, LPS-treated mice of both mouse strains demonstrated significantly increased apoptosis rates in comparison to the corresponding saline-treated mice. Notably, the density of TUNEL positive cells within TUNEL positive tubules (with at least one TUNEL positive nucleus) was strikingly different between both mouse strains 18 h after LPS injection. In this respect, Foxn1nu mice displayed a significantly higher density in affected tubules, whereas the distribution of apoptotic cells appeared more scattered in Balb/c mice.
Hence, the temporal displacement and difference in the severity of damage between both mouse strains suggest a regulatory role for the adaptive immune response as to testicular injury in LPS challenge. Herein, to a lower extent, LPS per se than the subsequent LPS-associated immuno-regulation may cause the arising damage.
Finally, this study contributes to the knowledge of TLR3 expression and signaling in testicular damage during bacterial LPS induced acute inflammation in immuno-competent or -incompetent mice. Interception with innate immune system receptors like TLR3 appears a promising strategy for the moderation of the inflammatory response secondary to LPS. Although TLR3 upregulation upon LPS injection is not followed by enhancement of the corresponding signaling pathway, TLR3 may exert its effects through distinct signal transduction, which still remains to be investigated.
References
Adams JM, Cory S (1998) The Bcl-2 protein family: arbiters of cell survival. Science 281:1322–1326
Akira S, Takeda K (2004) Toll-like receptor signalling. Nat Rev Immunol 4:499–511
Akira S, Uematsu S, Takeuchi O (2006) Pathogen recognition and innate immunity. Cell 124:783–801
Alexopoulou L, Holt AC, Medzhitov R, Flavell RA (2001) Recognition of double-stranded RNA and activation of NF-kappaB by toll-like receptor 3. Nature 413:732–738
Baiersdorfer M, Schwarz M, Seehafer K, Lehmann C, Heit A, Wagner H, Kirschning CJ, Koch-Brandt C (2010) Toll-like receptor 3 mediates expression of clusterin/apolipoprotein J in vascular smooth muscle cells stimulated with RNA released from necrotic cells. Exp Cell Res 316:3489–3500
Barry M, Bleackley RC (2002) Cytotoxic T lymphocytes: all roads lead to death. Nat Rev Immunol 2:401–409
Beutler B, Rietschel ET (2003) Innate immune sensing and its roots: the story of endotoxin. Nat Rev Immunol 3:169–176
Bhushan S, Tchatalbachev S, Klug J, Fijak M, Pineau C, Chakraborty T, Meinhardt A (2008) Uropathogenic Escherichia coli block MyD88-dependent and activate MyD88-independent signaling pathways in rat testicular cells. J Immunol 180:5537–5547
Boockfor FR, Wang D, Lin T, Nagpal ML, Spangelo BL (1994) Interleukin-6 secretion from rat Leydig cells in culture. Endocrinology 134:2150–2155
Brentano F, Schorr O, Gay RE, Gay S, Kyburz D (2005) RNA released from necrotic synovial fluid cells activates rheumatoid arthritis synovial fibroblasts via toll-like receptor 3. Arthritis Rheum 52:2656–2665
Cavassani KA, Ishii M, Wen H, Schaller MA, Lincoln PM, Lukacs NW, Hogaboam CM, Kunkel SL (2008) TLR3 is an endogenous sensor of tissue necrosis during acute inflammatory events. J Exp Med 205:2609–2621
Chen GY, Nunez G (2010) Sterile inflammation: sensing and reacting to damage. Nat Rev Immunol 10:826–837
Estornes Y, Toscano F, Virard F, Jacquemin G, Pierrot A, Vanbervliet B, Bonnin M, Lalaoui N, Mercier-Gouy P, Pacheco Y, Salaun B, Renno T, Micheau O, Lebecque S (2012) dsRNA induces apoptosis through an atypical death complex associating TLR3 to caspase-8. Cell Death Differ 19:1482–1494
Fijak M, Bhushan S, Meinhardt A (2011) Immunoprivileged sites: the testis. Methods Mol Biol 677:459–470
Glavan TM, Pavelic J (2014) The exploitation of toll-like receptor 3 signaling in cancer therapy. Curr Pharm Des 20:6555–6564
Head JR, Billingham RE (1985) Immune privilege in the testis. II. Evaluation of potential local factors. Transplantation 40:269–275
Head JR, Neaves WB, Billingham RE (1983) Immune privilege in the testis. I. Basic parameters of allograft survival. Transplantation 36:423–431
Kajihara T, Okagaki R, Ishihara O (2006) LPS-induced transient testicular dysfunction accompanied by apoptosis of testicular germ cells in mice. Med Mol Morphol 39:203–208
Kariko K, Ni H, Capodici J, Lamphier M, Weissman D (2004) mRNA is an endogenous ligand for toll-like receptor 3. J Biol Chem 279:12542–12550
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408
Metukuri MR, Reddy CM, Reddy PR, Reddanna P (2010) Bacterial LPS-mediated acute inflammation-induced spermatogenic failure in rats: role of stress response proteins and mitochondrial dysfunction. Inflammation 33:235–243
O'Bryan MK, Gerdprasert O, Nikolic-Paterson DJ, Meinhardt A, Muir JA, Foulds LM, Phillips DJ, de Kretser DM, Hedger MP (2005) Cytokine profiles in the testes of rats treated with lipopolysaccharide reveal localized suppression of inflammatory responses. Am J Physiol Regul Integr Comp Physiol 288:R1744–R1755
Palladino MA, Johnson TA, Gupta R, Chapman JL, Ojha P (2007) Members of the toll-like receptor family of innate immunity pattern-recognition receptors are abundant in the male rat reproductive tract. Biol Reprod 76:958–964
Paulus P, Rupprecht K, Baer P, Obermuller N, Penzkofer D, Reissig C, Scheller B, Holfeld J, Zacharowski K, Dimmeler S, Schlammes J, Urbschat A (2014) The early activation of toll-like receptor (TLR)-3 initiates kidney injury after ischemia and reperfusion. PLoS One 9:e94366
Poltorak A, He X, Smirnova I, Liu MY, Van Huffel C, Du X, Birdwell D, Alejos E, Silva M, Galanos C, Freudenberg M, Ricciardi-Castagnoli P, Layton B, Beutler B (1998) Defective LPS signaling in C3H/HeJ and C57BL/10ScCr mice: mutations in Tlr4 gene. Science 282:2085–2088
Qureshi ST, Lariviere L, Leveque G, Clermont S, Moore KJ, Gros P, Malo D (1999) Endotoxin-tolerant mice have mutations in toll-like receptor 4 (Tlr4). J Exp Med 189:615–625
Raetz CR, Whitfield C (2002) Lipopolysaccharide endotoxins. Annu Rev Biochem 71:635–700
Riccioli A, Filippini A, De Cesaris P, Barbacci E, Stefanini M, Starace G, Ziparo E (1995) Inflammatory mediators increase surface expression of integrin ligands, adhesion to lymphocytes, and secretion of interleukin 6 in mouse Sertoli cells. Proc Natl Acad Sci U S A 92:5808–5812
Riccioli A, Starace D, Galli R, Fuso A, Scarpa S, Palombi F, De Cesaris P, Ziparo E, Filippini A (2006) Sertoli cells initiate testicular innate immune responses through TLR activation. J Immunol 177:7122–7130
Schindelin J, Arganda-Carreras I, Frise E, Kaynig V, Longair M, Pietzsch T, Preibisch S, Rueden C, Saalfeld S, Schmid B, Tinevez JY, White DJ, Hartenstein V, Eliceiri K, Tomancak P, Cardona A (2012) Fiji: an open-source platform for biological-image analysis. Nat Methods 9:676–682
Shang T, Zhang X, Wang T, Sun B, Deng T, Han D (2011) Toll-like receptor-initiated testicular innate immune responses in mouse Leydig cells. Endocrinology 152:2827–2836
Sinha Hikim AP, Swerdloff RS (1999) Hormonal and genetic control of germ cell apoptosis in the testis. Rev Reprod 4:38–47
Sofikitis N, Pappas E, Kawatani A, Baltogiannis D, Loutradis D, Kanakas N, Giannakis D, Dimitriadis F, Tsoukanelis K, Georgiou I, Makrydimas G, Mio Y, Tarlatzis V, Melekos M, Miyagawa I (2005) Efforts to create an artificial testis: culture systems of male germ cells under biochemical conditions resembling the seminiferous tubular biochemical environment. Hum Reprod Update 11:229–259
Starace D, Galli R, Paone A, De Cesaris P, Filippini A, Ziparo E, Riccioli A (2008) Toll-like receptor 3 activation induces antiviral immune responses in mouse sertoli cells. Biol Reprod 79:766–775
Stephan JP, Syed V, Jegou B (1997) Regulation of Sertoli cell IL-1 and IL-6 production in vitro. Mol Cell Endocrinol 134:109–118
Taniguchi T, Takaoka A (2001) A weak signal for strong responses: interferon-alpha/beta revisited. Nat Rev Mol Cell Biol 2:378–386
Wang T, Zhang X, Chen Q, Deng T, Zhang Y, Li N, Shang T, Chen Y, Han D (2012) Toll-like receptor 3-initiated antiviral responses in mouse male germ cells in vitro. Biol Reprod 86:106
Ward PA (2012) New approaches to the study of sepsis. EMBO Mol Med 4:1234–1243
Winnall WR, Muir JA, Hedger MP (2011) Differential responses of epithelial Sertoli cells of the rat testis to Toll-like receptor 2 and 4 ligands: implications for studies of testicular inflammation using bacterial lipopolysaccharides. Innate Immun 17:123–136
Wu H, Wang H, Xiong W, Chen S, Tang H, Han D (2008) Expression patterns and functions of toll-like receptors in mouse sertoli cells. Endocrinology 149:4402–4412
Acknowledgements
We especially thank Ecatarina Oplesch, Michael Dreher and Hanne Sidelmann for their technical support.
Funding
This study was funded by a junior researchers grant by the Goethe University Frankfurt (Fokus Programme, Förderlinie A) to AU.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures involving animals were approved by the Animal Care and Use Committee of the state of Hesse in Germany (V54-19 c 20/15-FK/1037). Surgery and animal care was performed in accordance with the “Guide for the care and use of laboratory animals” (National Institutes of Health, volume 25, no. 28, revised 1996), EU Directive 86/609 EEC and German Protection of Animals Act.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplemental Fig. 1
Applying the same settings for both mouse strains Foxn1nu mice exhibited a higher constitutive immuno-histochemical expression of TLR3 (images from three animals 18 h following NaCl injection) (a - b”). Positive and negative staining control for TLR3 in order to prove the specificity of TLR3 expression using sections from a murine (C57BL/6) kidney 24 h after ischemia and reperfusion injury (IR) and a control kidney (c, c’). (PNG 453 kb)
Rights and permissions
About this article
Cite this article
Nejsum, L.N., Piec, A., Fijak, M. et al. Systemic LPS induces toll-like receptor 3 (TLR3) expression and apoptosis in testicular mouse tissue. Cell Tissue Res 378, 143–154 (2019). https://doi.org/10.1007/s00441-019-03022-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-019-03022-w