Abstract
Growth/differentiation factor−15 (Gdf-15) is a member of the transforming growth factor-β (Tgf-β) superfamily and has been shown to be a potent neurotrophic factor for midbrain dopaminergic (DAergic) neurons both in vitro and in vivo. Gdf-15 has also been shown to be involved in inflammatory processes. The aim of this study was to identify the role of endogenous Gdf-15 in the MPTP (1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine) mouse model of Parkinson’s disease (PD) by comparing Gdf-15 +/+ and Gdf-15 −/− mice. At 4 days and 14 days post-MPTP administration, both Gdf-15 +/+ and Gdf-15 −/− mice showed a similar decline in DAergic neuron numbers and in striatal dopamine (DA) levels. This was followed by a comparable restorative phase at 90 days and 120 days, indicating that the absence of Gdf-15 does not affect the susceptibility or the recovery capacity of the nigrostriatal system after MPTP administration. The MPTP-induced microglial and astrocytic response was not significantly altered between the two genotypes. However, pro-inflammatory and anti-inflammatory cytokine profiling revealed the differential expression of markers in Gdf-15 +/+ and Gdf-15 −/− mice after MPTP administration. Thus, the MPTP mouse model fails to uncover a major role of endogenous Gdf-15 in the protection of MPTP-lesioned nigrostriatal DAergic neurons, in contrast to its capacity to protect the 6-hydroxydopamine-intoxicated nigrostriatal system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is an age-related neurodegenerative disorder affecting more than 7 million people worldwide (Antony et al. 2013). Pathological hallmarks include degeneration of dopaminergic (DAergic) neurons in the substantia nigra (SN), loss of projecting fibers, and a subsequent depletion of the neurotransmitter dopamine (DA) in the caudate putamen (CPu; Hirsch et al. 1988), with current treatment strategies only providing symptomatic relief to PD patients.
The use of neurotoxin-induced animal models has been crucial for elucidating the pathophysiology of PD and for developing therapeutic approaches aimed at alleviating the motor symptoms (Schober 2004; Bové and Perier 2012; Simms et al. 2015). Of these, the classical neurotoxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) is widely used to elicit degeneration of the DAergic nigrostriatal system (Heikkila et al. 1984; Beal 2001; Przedborski and Vila 2003) and to study accompanying neuropathological and neurochemical changes (Schmidt and Ferger 2001). Losses of DAergic neurons following MPTP administration are accompanied by neuroinflammatory responses consisting primarily of activated microglia and reactive astrocytes and of an increase in levels of pro-inflammatory cytokines (Nagatsu et al. 2000; Vila et al. 2001; Barcia 2013).
During the past few decades, several neurotrophic factors have been tested with regard to their neuroprotective and neurorestorative properties in animal models of PD (Aron and Klein 2011; Weissmiller and Wu 2012; Hegarty et al. 2014). Growth/differentiation factor-15 (Gdf-15) is a member of the transforming growth factor-β (Tgf-β) superfamily and was identified by its role as an autocrine regulator of macrophage activation (Bootcov et al. 1997). It has broad anti-inflammatory and immunosuppressive properties, as recently described for models of atherosclerosis and rheumatoid arthritis (Breit et al. 2011; Unsicker et al. 2013). It is ubiquitously expressed in the rat and mouse central nervous systems, with the choroid plexus being the site of highest expression (Strelau et al. 2000a, 2000b). Gdf-15 has been shown to be a survival-promoting factor for central and peripheral neurons (Subramaniam et al. 2003; Strelau et al. 2009) and a potent neurotrophic factor for midbrain DAergic neurons both in vitro and in vivo (Strelau et al. 2000b). Gdf-15 promotes the survival of cultured DAergic neurons with an efficacy exceeding that of glial cell-line derived neurotrophic factor (Gdnf). In vivo, unilateral injection of Gdf-15 into the medial forebrain bundle and into the left ventricle, just before a 6-hydroxydopamine (6-OHDA) injection, significantly reduces DAergic neuron loss and abrogates pathological rotational motor behavior (Strelau et al. 2000a, 2000b). However, the effects of Gdf-15 in the MPTP mouse model of PD have so far not been investigated.
Our aim in this study has been to examine whether endogenous Gdf-15 is required to maintain the integrity and recovery of the nigrostriatal system after MPTP administration, and to determine possible alterations in the inflammatory responses, if any. We show here that MPTP-lesioned Gdf-15 +/+ and Gdf-15 −/− mice exhibit a concomitant decrease in the number of DAergic neurons and striatal DA levels, followed by a recovery phase, indicating that the lack of Gdf-15 alters neither the vulnerability nor the recovery of the nigrostriatal system after MPTP administration. Moreover, Gdf-15-deficient mice fail to reveal differences in the numbers of microglial cells and astrocytes in the two genotypes but clearly provide evidence for differential cytokine expression.
Materials and Methods
Animals
All animal work was performed in strict compliance with the German Federal Animal Welfare Law and after approval of the Official Animal Welfare Officer of the Centre for Experimental Models and Transgenic Services (CEMT) at the University of Freiburg. The Gdf-15lacZ/lacZ mouse colony was established via embryo-transfer from Heidelberg, Germany (Strelau et al. 2009). The animals were housed at 22 ± 2° C under a 12-h light/dark cycle with free access to food and water.
Generation of MPTP-lesioned mice
The preparation, handling, storage, and disposal of the neurotoxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridin (MPTP) was carried out in accordance with the published guidelines (Przedborski et al. 2001). Biohazard safety precautions and decontamination (with 1% sodium hypochlorite) were followed after contact with the MPTP-injected mice or the neurotoxin itself. Animal procedures were conducted in accordance with local ethical guidelines and have been approved by the Animal Experimentation Committee of the University of Freiburg (G-11/77). Sixty-three adult male Gdf-15 +/+ and Gdf-15 −/− mice, aged 10–12 weeks, were intraperitoneally injected with 20 mg/kg of the neurotoxin MPTP hydrochloride (Sigma-Aldrich) in 0.2 ml PBS (phosphate-buffered saline), once a day, for three consecutive days as previously described (Schober et al. 2007). Mice were killed after 2, 4, 14, 90, and 120 days. Sixty-one adult male Gdf-15 +/+ and Gdf-15 −/− mice were injected with PBS only (vehicle) and served as the control group.
Tissue processing
Mice were sacrificed by cervical dislocation at 4, 14, 90, and 120 days. Brains were removed from the skull, and a cut was made at the level of Bregma 0 (Paxinos and Franklin 2012). The CPu was dissected out (Bregma 1.32-0) and used for high performance liquid chromatography-electrochemical detection (HPLC-ED). The remaining brain comprising the SN was fixed in 4% paraformaldehyde (PFA; Merck, Germany) overnight at 4° C and transferred into a 15% sucrose solution followed by a 30% sucrose solution (overnight, 4° C, each). The cryo-protected brains were embedded in Tissue Tek (Leica, Germany), snap-frozen in liquid nitrogen (−196° C), and stored at −80° C. Brains were cut with a cryostat (Leica, Germany) at a thickness of 30 μm. Serial sections were collected on super-frost slides (Thermo Scientific, USA) and stored at −80° C until further processing.
HPLC-ED analysis
At the appropriate time-points, the CPu was dissected out (Bregma 1.32-0) and transferred to ice-cold 0.2 M perchloric acid. Dissected brain regions were homogenized in 0.2 M perchloric acid by using the Precellys 24 tissue homogenizer (Peqlab, Germany). HPLC-ED was performed as previously described (Schneider et al. 2011). Homogenates were centrifuged at 20,000g for 5 min at 4° C and were filtered through 0.2-μm filters. DA concentrations were measured by using an HPLC pump (UltiMate 3000 Quaternary Analytical, Dionex), an autosampler (WISP 717plus, Waters, Germany), and an amperometric detector (Antec Intro, AntecLeyden, Netherlands). The isocratic mobile phase consisted of sodium acetate (90 mM), citric acid monohydrate (60 mM), ethylenediaminetetraacetic acid (2 mM), 1-octanesulfonic acid (3 mM), and 8% methanol and was adjusted to pH 5.3. DA was separated on a Prontosil 120-3-C18 AQ column (3 μm, 120 × 2 mm; Bischoff chromatography, Germany) by using a fixed flow rate of 300 μl/min. Data were registered and analysed by using Chromeleon 6 software (Dionex).
RNA isolation and quantitative reverse transcription plus polymerase chain reaction
Mice were killed by cervical dislocation at the designated time-points. The CPu was dissected out at the level of Bregma 1.32-0. For isolation of the SN, a paramedian cut was made to exclude the ventral tegmental area (VTA) from the analyses, and the SN (including pars compacta and pars reticularis) were trimmed. Both the SN and the CPu were transferred to RNA later (Ambion, Germany). The tissues were then homogenized in peqGOLD TriFast (Peqlab, Germany) by using the Precellys 24 tissue homogenizer (Peqlab, Germany). RNA was extracted by using a modification of the phenol-chloroform extraction procedure with bromo-chloro-propane instead of chloroform (Chey et al. 2011). The extracted RNA was purified on columns (RNA Clean & Concentrator-25, Zymo Research, Germany). RNA purity and concentration were determined by using the NanoDrop 2000 (Thermo Scientific, Germany).
RNA was reverse-transcribed to cDNA with RevertAid H Minus Reverse Transcriptase (Thermo Scientific, Germany). Quantitative reverse transcription plus polymerase chain reaction (qRT-PCR) analysis was performed with the MyiQ (Bio-Rad, USA) and SYBR Green PCR Mastermix (Life Technologies, Germany). Primer sequences are listed in Table 1. Results were analyzed with Bio-Rad iQ5 Optical System Software and the comparative CT method (Livak and Schmittgen 2001). Data are expressed as 2-ΔΔCT for the experimental gene of interest, normalized to the housekeeping gene Gapdh (D-glyceraldehyde-3-phosphate dehydrogenase), and presented as the fold-change relative to control.
Immunohistochemistry
For 3,3’-diaminobenzidine (DAB)-based immunohistochemistry, sections were washed three times for 5 min each with PBS, followed by heat-based antigen retrieval in citrate buffer, pH 6.0 for 10 s at 600 W in a commercial microwave. The sections were then allowed to cool for 15–20 min and washed three times with PBS. This was followed by blocking endogenous peroxidase activity with 3% H2O2 in 100% methanol for 15 min in the dark. The sections were then washed three times with PBS and blocked with 1% bovine serum albumin (10% normal goat serum in the case of ionised calcium-binding adapter molecule 1 [Iba1]) and 1% Triton X-100 in PBS for 2 h at room temperature. This was followed by incubation with sheep anti-Th (tyrosine hydroxylase; 1:500; polyclonal, AB1542, Millipore, Germany) or rabbit anti-Iba1 (1:500; polyclonal, 019–19741, Wako, Japan) or mouse anti-Gfap (glial fibrillary acidic protein; 1:1000; MAB3402, Millipore, Germany) primary antibodies overnight at 4° C. On the next day, sections were washed three times with PBS, followed by an incubation with either biotinylated rabbit anti-sheep (1:200; Vector Laboratories, USA) or biotinylated goat anti-rabbit (1:500; Dianova, Germany) secondary antibodies for 2 h at room temperature. The secondary antibody step was followed by incubation with an avidin-biotin-peroxidase-conjugated complex (Vectastain ABC kit, Vector Laboratories, USA) for 2 h at room temperature. DAB (DAB Substrate Kit, Vector Laboratories, USA) was used as a chromogen for visualization, with a developing time of 5 min. Sections were then counter-stained with 0.5% cresyl violet acetate solution for 1–2 min, dehydrated in graded alcohols followed by incubation in Rotihistol (Roth, Germany), and finally mounted in Entellan (Merck, Germany). For fluorescent staining, donkey anti-sheep Alexa-594 and goat anti-mouse Alexa-488 secondary antibodies (1:500; Cell Signaling Technology, Germany) were added in PBS to the sections for 1 h at room temperature. Sections were then washed three times in PBS followed by a 5-min incubation with DAPI (4′,6-diamidino-2′-phenylindole dihydrochloride; 1:1000, Roche, Germany), washed again three times in PBS followed by a wash in distilled water, mounted with Fluoromount G (SouthernBiotech, USA), and sealed with clear nail polish.
Stereological analysis
Assessment of the number of Th-ir (immunoreactive) neurons or the Iba1-ir microglia was made according to the optical fractionator principle by using StereoInvestigator software (Version 8.23, MBF Bioscience, Germany). Unilateral counting was performed blind for treatment by using an oil immersion 63× objective (AxioImager M1, Zeiss), with a counting frame of 50 μm × 50 μm and a grid size of 100 μm × 120 μm. The optical disector was 11 μm thick, with 2-μm guard zones at the top and bottom of the section. Estimated numbers correspond to cell numbers in one hemisphere.
Statistical analysis
All statistical analyses were performed by using SPSS (IBM, version 22) and plotted by using GraphPad Prism (version 6.0; GraphPad Software). Data are expressed as means ± SEM. In all analyses, the null hypothesis was rejected at the 0.05 level. A two-way analysis of variance (ANOVA) with repeated measures followed by a Tukey’s post-hoc test was performed for Th-ir and Iba1-ir (total and activated) cell numbers. Striatal DA levels were analyzed with a two-way ANOVA with repeated measures followed by a Dunnett’s post-hoc test, with the Gdf-15 +/+ PBS group set to 100%. Cytokine expression profiling via qRT-PCR was analyzed by using a one-way ANOVA followed by a Tukey’s post-hoc test, with the respective PBS groups at each time-point serving as controls.
Results
Gdf-15 +/+ and Gdf-15 −/− mice exhibit similar DAergic neuron numbers and striatal DA levels following MPTP administration
Previous studies from our group have indicated that exogenous Gdf-15 application protects midbrain DAergic neurons from 6-OHDA-induced death (Strelau et al. 2000b). The present study addresses the role of endogenous Gdf-15 in an alternate PD lesion model by using the neurotoxin MPTP (Schober 2004). Both Gdf-15 +/+ and Gdf-15 −/− mice were injected with the neurotoxin MPTP and analyzed over a period of 120 days. Figure 1a-d’’’ illustrates the distribution of Th-ir DAergic neurons after vehicle (PBS) or MPTP administration in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days post-injection. Quantification of Th-ir neurons in the SN indicates a decrease in neuron numbers in both genotypes at 4 days and 14 days post-MPTP administration (not significant). This was followed by a subsequent increase in neuron numbers in the MPTP-treated groups at the later time-points (90 days and 120 days), in both genotypes, indicating a similar recovery at both times (Fig. 1e).
Lack of growth/differentiation factor-15 (Gdf-15) does not affect dopaminergic (DAergic) neuron numbers or striatal dopamine (DA) levels following 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) administration. a–d’’’ Representative images of the substantia nigra (SN) of Gdf-15 +/+ and Gdf-15 −/− mice demonstrating the distribution of tyrosine-hydroxylase-immunoreactive (Th-ir) neurons at 4, 14, 90, and 120 days (d) after phosphate-buffered saline (PBS) or MPTP injections. Bar 100 μm. e Graph showing the quantification of Th-ir neurons in Gdf-15 +/+ and in Gdf-15 −/− mice at 4, 14, 90, and 120 days after either PBS or MPTP injection (n = 4). f Striatal DA levels in Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days after PBS or MPTP administration (n = 4). Data presented as means ± SEM. **P ≤ 0.01, ****P < 0.0001
As seen in Fig. 1f, MPTP administration caused a sharp decrease in striatal DA levels in both Gdf-15 +/+ and Gdf-15 −/− mice at 4 days and 14 days, followed by a recovery phase at 90 days, with return to baseline levels (as compared with the PBS controls) at 120 days, post-MPTP administration. A two-way ANOVA with repeated measures was performed to examine the effects of treatment and time on the striatal DA levels between the two genotypes. A statistically significant interaction was seen between the effect of the genotypes (F [1, 45] = 31.750, P < 0.0001), the treatments (F [1, 45] = 207.423, P <0.0001), and the time-points (F [3, 45] = 10.262, P <0.0001) on the levels. Furthermore, a strong time-based interaction effect was noted between the genotypes (F [3, 45] = 7.664, P < 0.0001) and between the treatments (F [3, 45] = 8.198, P < 0.0001). A Dunnett’s post-hoc test showed a significant increase in striatal DA levels at 90 days (97.44 ± 37.69, P <0.0001) and 120 days (90.68 ± 13.32, P =0.001) as compared with 4 days (71.47 ± 32.28). However, no significant differences were detected between the genotypes.
Effect of MPTP administration on nigrostriatal glia
MPTP-induced neurodegeneration of DAergic neurons is accompanied by a neuroinflammatory response consisting of a strong glial reaction, namely increased microglial activation and reactive astrogliosis (Hirsch et al. 2005; McGeer and McGeer 2008). Figure 2a-d’’’ shows the distribution of Iba1-ir microglia in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days after PBS or MPTP administration. Activated microglia were distinguished from resting microglia based on their intense staining for Iba-1, their amoeboid shape, and their retracted processes (Fig. 2e’, f’). The numbers of Iba1-ir total and activated microglia in the SN were quantified stereologically. Figure 2e depicts the estimated numbers of total microglia in both Gdf-15 +/+ and Gdf-15 −/− mice after PBS or MPTP treatment at the various time-points. A two-way ANOVA with repeated measures was performed to examine the effects of treatment and time on the total Iba1-ir microglia numbers between the two genotypes. No statistically significant interaction was observed between the groups analyzed. Out of the total microglia, the activated microglia fraction was also estimated stereologically. As seen in Fig. 2f, the numbers of Iba1-ir activated microglia were increased in both Gdf-15 +/+ and Gdf-15 −/− mice at 4 days after MPTP administration and showed a gradual decrease with the progression of time. A two-way ANOVA with repeated measures was performed to examine the effects of treatment and time on the Iba1-ir activated microglia numbers between the two genotypes. A statistically significant interaction was noted between the effect of treatment on activated microglia numbers (F [1, 32] = 14.570, P = 0.001. A statistically significant time-based effect was also seen on activated microglia numbers (F [3, 32] = 8.223, P = 0.001). A Tukey’s post-hoc test showed a significant reduction in the number of Iba1-ir activated microglia at 14 days (696.89 ± 427.07, P = 0.009), 90 days (645.23 ± 308.67, P = 0.004), and 120 days (489.53 ± 189.29, P <0.0001), as compared with the numbers at 4 days (1297.15 ± 812.01). This suggests that, although a time-dependent decrease occurs in the microglial response, activated microglial cells are still present long after the toxin has been cleared from the system.
Microglial distribution and quantification in the substantia nigra (SN) of Gdf-15 +/+ and Gdf-15 −/− mice after MPTP lesion. a–d’’’ Representative images showing the distribution of ionised calcium-binding adapter molecule 1 (Iba1)-ir microglia in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days after PBS or MPTP administration. The dashed line in a delineates the substantia nigra pars compacta (SNpc) and the substantia nigra pars reticularis (SNpr). e Estimated numbers of Iba1-ir total microglia in the SN of Gdf-15 +/+ and Gdf-15 −/− mice after PBS or MPTP treatment at 4, 14, 90, and 120 days. f Estimated numbers of Iba1-ir activated microglia in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days after PBS or MPTP treatment (n = 4). e’, f’ Morphological differences between resting (e’) and activated (f’) microglia. Data are presented as means ± SEM. **P ≤ 0.01, ****P < 0.0001. SN; . Bar 100 μm (a–d’’’), 20 μm (e’, f’)
We next compared the astroglial response between Gdf-15 +/+ and Gdf-15 −/− mice after MPTP administration. Figure 3a-d’’’ shows the distribution of Gfap-ir astrocytes (green) and Th-ir DAergic neurons (red) in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days post-PBS or -MPTP administration. At 4 days post-MPTP lesion, both Gdf-15 +/+ and Gdf-15 −/− mice exhibited an increased astroglial reaction in the SN, with the presence of reactive astrocytes (inset, Fig. 3a’), as compared with normal astrocytes (inset in Fig. 3a’’). Astrocytic reaction was reduced at the later time-points. This indicated that, in comparison with Gdf-15 +/+ mice, Gdf-15 −/− mice do not show an altered astrocytic reaction post-MPTP lesion.
Astrocytic response in the substantia nigra (SN) of Gdf-15 +/+ and Gdf-15 −/− mice following MPTP administration. a–d’’’ Representative images illustrating the distribution of glial fibrillary acidic protein (Gfap)-ir astrocytes (green) and tyrosine-hydroxylase (Th)-ir DAergic neurons (red) in the SN of Gdf-15 +/+ and Gdf-15 −/− mice at 4, 14, 90, and 120 days after PBS or MPTP administration (dashed line in a demarcates SNpc and SNpr). A reactive astrocyte (inset in a’) is characterised by its difference in morphology as compared with that of a normal astrocyte (inset in a’’). Bar 100 μm (insets 10 μm)
Cytokine expression profile in Gdf-15 +/+ and Gdf-15 −/− mice after MPTP administration
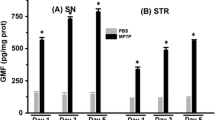
Regulation of both pro-inflammatory and anti-inflammatory cytokines is observed post-MPTP administration in animal models of PD (Nagatsu et al. 2000; Grünblatt et al. 2000; Sawada et al. 2006). Figure 4 shows the mRNA expression pattern of Gdf-15, iNos, Tnf-α, and Il-6 in the CPu and SN of Gdf-15 +/+ and Gdf-15 −/− mice at 2, 4, 14, 90, and 120 days after MPTP administration. An increase occurred in Gdf-15 mRNA expression in the CPu of Gdf-15 +/+ mice at 2 days (8.721 ± 2.13) followed by a decrease at 4 days and 14 days and a subsequent increase at 90 days (7.90 ± 2.77), which was significantly different from the levels at 4 days (P = 0.0148). Gdf-15 mRNA levels returned to basal levels at 120 days post-MPTP administration (Fig. 4a). In the SN, a slight increase was seen in Gdf-15 mRNA expression in the Gdf-15 +/+ mice at 2 days, which significantly increased at 90 days (19.03 ± 2.04, P <0.0001) as compared with all other time-points (Fig. 4b). As seen in Fig. 4c, the expression of iNos in the CPu was comparable in both genotypes at all time-points, except at 90 days, when a significant increase occurred in the expression in the Gdf-15 +/+ mice (4.724 ± 1.026) as compared with the Gdf-15 −/− mice (1.193 ± 0.29). This increase in iNos mRNA expression at 90 days was also significantly different from the expression at all other time-points in the Gdf-15 +/+ mice (P = 0.0004). A similar expression pattern was seen in the SN, with a significant increase in iNos mRNA expression at 90 days in the Gdf-15 +/+ mice (24.40 ± 6.27) as compared with the Gdf-15 −/− mice (0.812 ± 0.216); this was also significantly different from all other time-points (P = 0.0047; Fig. 4d). As depicted in Fig. 4e, Tnf-α mRNA levels were also significantly higher in the CPu of Gdf-15 +/+ mice (16.93 ± 5.58) as compared with Gdf-15 −/− mice (1.55 ± 0.60) at 90 days post-MPTP administration. Moreover, the increase at 90 days was also significantly different from the values at all other time-points as shown by a one-way ANOVA (P = 0.0014). The SN showed a similar expression pattern, with elevated Tnf-α mRNA levels at 90 days in Gdf-15 +/+ mice (27.81 ± 7.67) as compared with Gdf-15 −/− mice (0.89 ± 0.21); these were also significantly different from all other time-points (P <0.0001; Fig. 4f). Il-6 mRNA expression was significantly increased in the CPu of Gdf-15 +/+ mice (9.37 ± 2.52) as compared with Gdf-15 −/− mice (0.51 ± 0.26) at 90 days post-MPTP administration; this was also significantly higher as compared with all other time-points (P = 0.0007; Fig. 4g). The SN exhibited a similar trend, with an increase in Gdf-15 +/+ mice (10.23 ± 3.48) as compared with Gdf-15 −/− mice (0.54 ± 0.81) at 90 days post-MPTP administration; this was also significantly higher compared with all other time-points (P = 0.0002; Fig. 4h).
Expression pattern of pro-inflammatory cytokines in the nigrostriatal system of Gdf-15 +/+ and Gdf-15 −/− mice after MPTP lesion. mRNA expression pattern of Gdf-15, iNos (inducible form of nitric oxide synthase), Tnf-α (tumor necrosis factor-α), and Il-6 (interleukin-6) in the caudate putamen (CPu) and substantia nigra (SN) of Gdf-15 +/+ and Gdf-15 −/− mice at 2, 4, 14, 90, and 120 days post-MPTP administration (for an explanation of gene names, see Table 1). a Gdf-15 mRNA levels were significantly increased in the CPu of Gdf-15 +/+ mice at 90 days as compared with 4 days (P = 0.0148). b SN shows an increase at 90 days in the Gdf-15 mRNA level, which was significantly different from the other time-points (P < 0.0001). c iNos expression was significantly increased in the CPu of Gdf-15 +/+ mice at 90 days and was also significantly different from the levels at all other time-points (P = 0.0004). d iNos mRNA expression was also elevated in the SN of Gdf-15 +/+ mice at 90 days and was significantly different from all other time-points (P = 0.0047). e Tnf-α mRNA levels at 90 days were higher in the CPu of Gdf-15 +/+ mice. This increase was significantly different from the expression levels at all time-points (P = 0.0014). f Tnf-α levels in the SN were also significantly higher in the Gdf-15 +/+ mice at 90 days compared to all time-points (P < 0.0001). g Il-6 mRNA levels were significantly increased in the CPu of Gdf-15 +/+ mice at 90 days as compared with Gdf-15 −/− mice and were significantly different from the levels at all other time-points (P = 0.0007). h SN shows an increase in Il-6 level in the Gdf-15 +/+ mice as compared with Gdf-15 −/− mice at 90 days. This level was also significantly higher as compared with all time-points (P = 0.0002). Data are expressed as means ± SEM. A one-way ANOVA with a Tukey’s post-hoc test was used for all analyses. n = 3, *P ≤ 0.05, **P ≤ 0.01, ***P < 0.001, #compared with expression in respective genotype at all time-points. n.d = not detectable, CPu; Striatum, SN; Substantia nigra
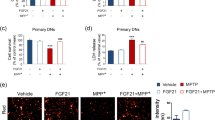
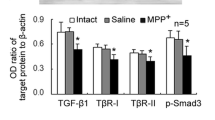
Alternative activation of microglia is associated with expression of genes involved in anti-inflammatory effects such as tissue repair, extracellular matrix remodeling, and resolution of inflammation (Tang and Le 2015; Haas et al. 2016). Hence, the mRNA expression of alternative or anti-inflammatory markers, namely Tgfβ-1, Arg1, Fizz-1, and Ym1 was also assessed in the CPu and SN of Gdf-15 +/+ and Gdf-15 −/− mice at 2, 4, 14, 90, and 120 days post-MPTP administration (Fig. 5). Interestingly, the Tgfβ-1 mRNA level showed a significant increase in the CPu at 4 days in Gdf-15 −/− mice (17.60 ± 3.64) as compared with Gdf-15 +/+ mice (0.94 ± 0.15); this was significantly higher as compared with all other time-points. In addition, at 90 days post-MPTP, the Gdf-15 +/+ mice showed increased Tgfβ-1 expression (13.90 ± 3.99) as compared with the Gdf-15 −/− mice (2.49 ± 0.63), as tested by a one-way ANOVA with a Tukey’s post-hoc test (P <0.0001; Fig. 5a). The SN showed an increase in mRNA levels in the Gdf-15 −/− mice at 4 days (5.28 ± 1.05), with Gdf-15 +/+ mice exhibiting increased Tgfβ-1 expression (150.7 ± 25.49) as compared with the Gdf-15 −/− mice at 90 days (0.77 ± 0.20, P <0.0001; Fig. 5b). As seen in Fig. 5c, Arg1 mRNA was also increased at 90 days in the CPu of Gdf-15 +/+ mice (6.29 ± 1.53 in Gdf-15 +/+ mice versus 1.18 ± 0.36 in Gdf-15 −/− mice) and in the SN (22.23 ± 6.27 in Gdf-15 +/+ mice versus 0.59 ± 1.14 in Gdf-15 −/− mice). Moreover, this increase at 90 days in the Gdf-15 +/+ mice was significantly different from all other time-points (CPu, P = 0.0004; SN, P = 0.0001; Fig. 5c, d). Fizz-1 mRNA was also increased at 90 days in the CPu and in the SN of Gdf-15 +/+ mice as compared with Gdf-15 −/− mice. Furthermore, this increase at 90 days in the Gdf-15 +/+ mice was significantly different from all other time-points (CPu, P = 0.0024; SN, P <0.0001; Fig. 5e, f). As seen in Fig. 5g, Ym1 mRNA expression was increased (not significantly) in the CPu of Gdf-15 +/+ mice at 90 days. In the SN, a significant increase occurred in the mRNA expression levels of Ym1 at 90 days in Gdf-15 +/+ mice (46.79 ± 17.42) as compared with Gdf-15 −/− mice (1.50 ± 0.94), with a significant difference at 90 days in Gdf-15 +/+ mice as compared with all other time-points (P = 0.0019; Fig. 5h).
Alternative marker expression profile in the nigrostriatal system of Gdf-15 +/+ and Gdf-15 −/− mice post-MPTP lesion. mRNA expression pattern of Tgfβ-1, Arg1, Fizz-1, and Ym1 in the CPu and SN of Gdf-15 +/+ and Gdf-15 −/− mice at 2, 4, 14, 90, and 120 days post-MPTP administration (for an explanation of gene names, see Table 1). a Tgfb-1 mRNA levels show a significant increase in the CPu of Gdf-15 −/− mice at 4 days; this was significantly higher compared with all time-points. At 90 days, Gdf-15 +/+ mice showed increased Tgfb-1 levels as compared with those in Gdf-15 −/− mice (P < 0.0001). b Tgfb-1 levels in the SN were also higher in the Gdf-15 −/− mice at 4 days (not significant). Furthermore, Gdf-15 +/+ mice showed an increase in expression at 90 days compared with Gdf-15 −/− mice (P < 0.0001). c, d Arg1 mRNA was also increased between the two genotypes at 90 days in the CPu and in the SN. Moreover, this increase at 90 days in the Gdf-15 +/+ mice was significantly different from all other time-points (CPu, P = 0.0004; SN, P = 0.0001). e, f Fizz-1 mRNA expression was elevated at 90 days in the CPu and in the SN of Gdf-15 +/+ as compared with Gdf-15 −/− mice. This increase at 90 days was significantly different from all other time-points (CPu, P = 0.0024; SN, P < 0.0001). g Ym1 mRNA expression was increased in the CPu of Gdf-15 +/+ mice at 90 days (not significant). h In the SN, a significant increase was seen in Ym1 levels at 90 days in Gdf-15 +/+ mice as compared with Gdf-15 −/− mice, with a significant difference at 90 days in Gdf-15 +/+ mice ccompared with all other time-points (P = 0.0019). Data are expressed as means ± SEM. A one-way ANOVA with a Tukey’s post-hoc test was used for all analyses. n = 3, *P ≤0.05, **P ≤ 0.01, ***P < 0.001, #compared with expression in the respective genotype at all time-points
Together, these data indicate that cytokine expression (both pro-inflammatory and anti-inflammatory) is not only increased immediately after MPTP administration, but also months after toxin administration, suggesting that MPTP administration causes a long-term regulation of the nigrostriatal cytokine network.
Discussion
Exogenous application of Gdf-15 has been shown to protect midbrain DAergic neurons from 6-OHDA-induced neurotoxicity and the associated pathological rotational behavior (Strelau et al. 2000b). In contrast to the drastic permanent lesion exerted by 6-OHDA, the MPTP lesion is transient, allowing recovery of the system after several months (Beal 2001; Schober 2004; Bové and Perier 2012). The recovery phase has also been shown to be dependent on neurotrophic support, for example, on the presence of the Gdnf ligand and receptor system (Kowsky et al. 2007; Kells et al. 2010).
An involvement of endogenous Gdf-15 in the MPTP nigrostriatal lesion response has so far not been described. In our study, we have shown that in spite of a decrease in the number of Th-ir neurons in the SN of Gdf-15 −/− mice at 4 days and 14 days post-MPTP administration, this difference is not significantly different as compared with the Gdf-15 +/+ mice. A subsequent increase took place in Th-ir neuronal cell bodies in the SN at 90 days and 120 days post-lesion, demonstrating that a disappearance of the Th phenotype had occurred rather than neuron death (Peterson and Nutt 2008). However, the lack of Gdf-15 did not affect the neuron numbers. Moreover, MPTP administration led to an approximately 50% decrease in striatal DA levels in both Gdf-15 +/+ and Gdf-15 −/− mice at 4 days and 14 days, followed by a recovery phase at 90 days. The DA levels returned to baseline at 120 days post-MPTP administration. At all time-points assessed, Gdf-15 −/− mice (both PBS and MPTP treated) had slightly higher DA levels than Gdf-15 +/+ mice. Thus, the reappearance of Th-ir in both the DAergic neuron cell bodies and their axonal fibers in the CPu were not affected by the lack of Gdf-15 after MPTP administration. In the light of a previous study, in which we have shown the significant potential of endogenous Gdf-15 to ameliorate the deleterious consequences of a 6-OHDA-mediated nigrostriatal lesion (Machado et al. 2015), the present results come as a surprise. The discrepancy between the two studies can perhaps be explained by the more rigorous destruction of the nigrostriatal system by 6-OHDA as compared with MPTP (Sarre et al. 2004), leaving an avenue for a more significant improvement by endogenous Gdf-15. Fibroblast growth factor-2 (Fgf-2) is another growth factor that has shown potential in ameliorating the destructive actions of MPTP in nigrostriatal lesions, when applied exogenously (Otto and Unsicker 1990, 1993, 1994). Similar to Gdf-15, an analysis of the effects of MPTP in Fgf-2 −/− mice failed to reveal a curative potential of endogenous Fgf-2 (Zechel et al. 2006).
The role of Gdf-15 in inflammatory processes was revealed when it was shown to down-regulate macrophage activation in response to secreted pro-inflammatory cytokines (Bootcov et al. 1997; Fairlie et al. 1999). Recent studies have underlined its importance in inflammatory processes, such as in models of atherosclerosis, and as a biomarker for patients with suspected cardiac events (de Jager et al. 2011; Kempf et al. 2011; Schaub et al. 2012; Rossaint et al. 2013). MPTP administration is known to induce a glial reaction in humans and in animal models of PD (Langston et al. 1999; Teismann et al. 2003; Barcia et al. 2012). In our study, the total number of microglia in the SN of both Gdf-15 +/+ and Gdf-15 −/− mice remained constant at all time-points after MPTP administration, with the Gdf-15 −/− mice showing lower numbers at 90 days and 120 days (not significant). Although the numbers of activated microglia gradually decreased in both genotypes, the presence of scattered activated microglia at 120 days post-MPTP administration indicates that inflammatory processes were still ongoing long after the toxin had been metabolized and cleared from the system. The activated microglial response precedes the reactive astrocytic response and is strongest before the peak of DAergic neuron death (Kohutnicka et al. 1998; Liberatore et al. 1999). The glial response, however, is secondary to neuronal death as demonstrated by the blocking of MPP+ uptake into DAergic neurons, an action that not only prevents neuron death, but also Gfap up-regulation (O’Callaghan et al. 1990; Przedborski et al. 2000). Based on histological observations, the Gfap-ir astrocytic response in Gdf-15 −/− mice did not significantly differ from that in Gdf-15 +/+ mice after MPTP administration.
Together with histological findings from post-mortem samples, the evidence of an accompanying cytokine response, both in patients and in animal models, has led to important advancements in the field of PD research (Barcia et al. 2004; Teismann and Schulz 2004). Cytokine release by glial cells is part of the network of repair processes in the context of degenerative events. However, long-term exposure of DAergic neurons to cytokines released by glia leads to deleterious effects and progressive neurodegeneration (Hirsch et al. 2005). In our study, MPTP administration led to an up-regulation of Gdf-15 in both the CPu and the SN of Gdf-15 +/+ mice at 2 days post-lesion, followed by a significant further increase at 90 days. The expression profiles of pro-inflammatory cytokines such as iNos, Tnf-α, and Il-6 were also evaluated in Gdf-15 −/− mice as compared with Gdf-15 +/+ mice. Microglial interferon-γ (Ifn-γ) and astrocytic Tnf-α are both strong inducers of iNos expression (Barcia et al. 2012), which leads to nitric oxide production and subsequent DNA damage and neurotoxicity (Knott 2000). Neither iNos nor Tnf-α mRNA levels showed marked differences in expression in the Gdf-15 −/− mice as compared with Gdf-15 +/+ mice. Ifn-γ and Tnf-α also induce Il-6 production in both neurons and glia (Gadient and Otten 1997; Scheller et al. 2011). In the MPTP model, Il-6 has been shown to be neuroprotective, with increased sensitivity of Il-6 −/− mice to MPTP-induced DAergic neurodegeneration (Bolin et al. 2002, 2005). Moreover, Il-6 −/− mice exhibit impaired microgliosis after MPTP lesion, underscoring the importance of Il-6 in the microglial responses (Cardenas and Bolin 2003). Transgenic mice overexpressing Gdf-15 have lower Il-6 levels and a reduced inflammatory response (Kim et al. 2013). Post MPTP administration, however, Il-6 mRNA expression was not differentially regulated in Gdf-15 −/− mice. Interestingly, Tgfβ-1 mRNA expression was increased in the CPu and the SN of Gdf-15 −/− mice at 4 days post-lesion. Physiologically, Tgf-β1 expression is rapidly elevated in response to injury, with glial cells being the primary source (Finch et al. 1993). Endogenous Tgf-β1 has been shown to suppress inflammation and reactive microgliosis as is evident from studies of Tgf-β1 −/− mice (Brionne et al. 2003; Makwana et al. 2007). A recent investigation has shown that murine dendritic cells treated with various concentrations of recombinant human GDF-15 exhibit increased secretion of Tgf-β1 into the culture supernatant (Zhou et al. 2013). Nevertheless, the putative interdependent regulation of Tgf-β1 and Gdf-15 needs validation. Microglial alternative activation markers such as Arg1, Fizz-1, and Ym1 showed mRNA regulation at 90 days post-MPTP in the Gdf-15 +/+ mice. The relevance of this increase at 90 days is still unclear, since Gdf-15 −/− mice do not show abnormalities in the number of Th-ir neurons, in striatal DA levels or recovery, or in microglia numbers after MPTP administration as compared with Gdf-15 +/+ mice. The actual protein expression for the markers of interest should be validated by immunohistochemistry to check their protein expression and to identify the cells responsible for the putative regulation.
In summary, lack of Gdf-15 does not alter the vulnerability of the nigrostriatal DAergic system to MPTP-lesion-induced neurodegeneration. Moreover, glial responses are not altered in the Gdf-15 −/− mice post-MPTP lesion. The cytokine profile is differentially regulated in Gdf-15 +/+ as compared with Gdf-15 −/− mice, especially at 90 days post-lesion; this, however, should be corroborated at the protein level.
References
Antony PMA, Diederich NJ, Krüger R, Balling R (2013) The hallmarks of Parkinson’s disease. FEBS J 280:5981–5993. doi:10.1111/febs.12335
Aron L, Klein R (2011) Repairing the parkinsonian brain with neurotrophic factors. Trends Neurosci 34:88–100. doi:10.1016/j.tins.2010.11.001
Barcia C (2013) Glial-mediated inflammation underlying parkinsonism. Scientifica 2013:357805. doi:10.1155/2013/357805
Barcia C, Sánchez Bahillo A, Fernández-Villalba E, Bautista V, Poza Y Poza M, Fernández-Barreiro A, Hirsch EC, Herrero MT (2004) Evidence of active microglia in substantia nigra pars compacta of parkinsonian monkeys 1 year after MPTP exposure. Glia 46:402–409. doi:10.1002/glia.20015
Barcia C, Ros CM, Annese V, Gómez A, Ros-Bernal F, Aguado-Llera D, Martínez-Pagán ME, de Pablos V, Fernandez-Villalba E, Herrero MT (2012) IFN-γ signaling, with the synergistic contribution of TNF-α, mediates cell specific microglial and astroglial activation in experimental models of Parkinson’s disease. Cell Death Dis 3:e379. doi:10.1038/cddis.2012.123
Beal MF (2001) Experimental models of Parkinson’s disease. Nat Rev Neurosci 2:325–334. doi:10.1038/35072550
Bolin LM, Strycharska-Orczyk I, Murray R, Langston JW, Di Monte D (2002) Increased vulnerability of dopaminergic neurons in MPTP-lesioned interleukin-6 deficient mice. J Neurochem 83:167–175. doi:10.1046/j.1471-4159.2002.01131.x
Bolin LM, Zhaung A, Strychkarska-Orczyk I, Nelson E, Huang I, Malit M, Nguyen Q (2005) Differential inflammatory activation of IL-6 (−/−) astrocytes. Cytokine 30:47–55. doi:10.1016/j.cyto.2004.11.007
Bootcov MR, Bauskin AR, Valenzuela SM, Moore AG, Bansal M, He XY, Zhang HP, Donnellan M, Mahler S, Pryor K, Walsh BJ, Nicholson RC, Fairlie WD, Por SB, Robbins JM, Breit SN (1997) MIC-1, a novel macrophage inhibitory cytokine, is a divergent member of the TGF-beta superfamily. Proc Natl Acad Sci U S A 94:11514–11519. doi:10.1073/pnas.94.21.11514
Bové J, Perier C (2012) Neurotoxin-based models of Parkinson’s disease. Neuroscience 211:51–76. doi:10.1016/j.neuroscience.2011.10.057
Breit SN, Johnen H, Cook AD, Tsai VW, Mohammad MG, Kuffner T, Zhang HP, Marquis CP, Jiang L, Lockwood G, Lee-Ng M, Husaini Y, Wu L, Hamilton JA, Brown DA (2011) The TGF-β superfamily cytokine, MIC-1/GDF15: a pleotrophic cytokine with roles in inflammation, cancer and metabolism. Growth Factors 29:187–195. doi:10.3109/08977194.2011.607137
Brionne TC, Tesseur I, Masliah E, Wyss-Coray T (2003) Loss of TGF-beta 1 leads to increased neuronal cell death and microgliosis in mouse brain. Neuron 40:1133–1145. doi:10.1016/S0896-6273(03)00766-9
Cardenas H, Bolin LM (2003) Compromised reactive microgliosis in MPTP-lesioned IL-6 KO mice. Brain Res 985:89–97. doi:10.1016/S0006-8993(03)03172-X
Chey S, Claus C, Liebert UG (2011) Improved method for simultaneous isolation of proteins and nucleic acids. Anal Biochem 411:164–166. doi:10.1016/j.ab.2010.11.020
De Jager SCA, Bermúdez B, Bot I, Koenen RR, Bot M, Kavelaars A, de Waard V, Heijnen CJ, Muriana FJ, Weber C, van Berkel TJ, Kuiper J, Lee SJ, Abia R, Biessen EA (2011) Growth differentiation factor 15 deficiency protects against atherosclerosis by attenuating CCR2-mediated macrophage chemotaxis. J Exp Med 208:217–225. doi:10.1084/jem.20100370
Fairlie WD, Moore AG, Bauskin AR, Russell PK, Zhang HP, Breit SN (1999) MIC-1 is a novel TGF-beta superfamily cytokine associated with macrophage activation. J Leukoc Biol 65:2–5
Finch CE, Laping NJ, Morgan TE, Nichols NR, Pasinetti GM (1993) TGF-beta 1 is an organizer of responses to neurodegeneration. J Cell Biochem 53:314–322. doi:10.1002/jcb.240530408
Gadient RA, Otten UH (1997) Interleukin-6 (IL-6)—a molecule with both beneficial and destructive potentials. Prog Neurobiol 52:379–390. doi:10.1016/S0301-0082(97)00021-X
Grünblatt E, Mandel S, Youdim MB (2000) MPTP and 6-hydroxydopamine-induced neurodegeneration as models for Parkinson’s disease: neuroprotective strategies. J Neurol 247 (Suppl 2):II95–II102. doi:10.1007/PL00022909
Haas SJ-P, Zhou X, Machado V, Wree A, Krieglstein K, Spittau B (2016) Expression of Tgfβ1 and inflammatory markers in the 6-hydroxydopamine mouse model of Parkinson’s disease. Front Mol Neurosci 9:7. doi:10.3389/fnmol.2016.00007
Hegarty SV, O’Keeffe GW, Sullivan AM (2014) Neurotrophic factors: from neurodevelopmental regulators to novel therapies for Parkinson’s disease. Neural Regen Res 9:1708–1711. doi:10.4103/1673-5374.143410
Heikkila RE, Hess A, Duvoisin RC (1984) Dopaminergic neurotoxicity of 1-methyl-4-phenyl-1, 2, 5, 6-tetrahydropyridine in mice. Science 224:1451–1453. doi:10.1126/science.6610213
Hirsch E, Graybiel AM, Agid YA (1988) Melanized dopaminergic neurons are differentially susceptible to degeneration in Parkinson’s disease. Nature 334:345–348. doi:10.1038/334345a0
Hirsch EC, Hunot S, Hartmann A (2005) Neuroinflammatory processes in Parkinson’s disease. Parkinsonism Relat Disord 11:S9–S15. doi:10.1016/j.parkreldis.2004.10.013
Kells AP, Eberling J, Su X, Pivirotto P, Bringas J, Hadaczek P, Narrow WC, Bowers WJ, Federoff HJ, Forsayeth J, Bankiewicz KS (2010) Regeneration of the MPTP-lesioned dopaminergic system after convection-enhanced delivery of AAV2-GDNF. J Neurosci 30:9567–9577. doi:10.1523/JNEUROSCI.0942-10.2010
Kempf T, Zarbock A, Widera C, Butz S, Stadtmann A, Rossaint J, Bolomini-Vittori M, Korf-Klingebiel M, Napp LC, Hansen B, Kanwischer A, Bavendiek U, Beutel G, Hapke M, Sauer MG, Laudanna C, Hogg N, Vestweber D, Wollert KC (2011) GDF-15 is an inhibitor of leukocyte integrin activation required for survival after myocardial infarction in mice. Nat Med 17:581–588. doi:10.1038/nm.2354
Kim JM, Kosak JP, Kim JK, Kissling GM, Germolec DR, Zeldin DC, Bradbury JA, Baek SJ, Eling TE (2013) NAG-1/GDF15 transgenic mouse has less white adipose tissue and a reduced inflammatory response. Mediators Inflamm 2013:641851. doi:10.1155/2013/641851
Knott C (2000) Inflammatory regulators in Parkinson’s disease: iNOS, lipocortin-1, and cyclooxygenases-1 and −2. Mol Cell Neurosci 16:724–739. doi:10.1006/mcne.2000.0914
Kohutnicka M, Lewandowska E, Kurkowska-Jastrzebska I, Członkowski A, Członkowska A (1998) Microglial and astrocytic involvement in a murine model of Parkinson’s disease induced by 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP). Immunopharmacology 39:167–180. doi:10.1016/S0162-3109(98)00022-8
Kowsky S, Pöppelmeyer C, Kramer ER, Falkenburger BH, Kruse A, Klein R, Schulz JB (2007) RET signaling does not modulate MPTP toxicity but is required for regeneration of dopaminergic axon terminals. Proc Natl Acad Sci 104:20049–20054. doi:10.1073/pnas.0706177104
Langston JW, Forno LS, Tetrud J, Reeves AG, Kaplan JA, Karluk D (1999) Evidence of active nerve cell degeneration in the substantia nigra of humans years after 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine exposure. Ann Neurol 46:598–605. doi:10.1002/1531-8249(199910)46:4<598::AID-ANA7>3.0.CO;2-F
Liberatore GT, Jackson-Lewis V, Vukosavic S, Mandir AS, Vila M, McAuliffe WG, Dawson VL, Dawson TM, Przedborski S (1999) Inducible nitric oxide synthase stimulates dopaminergic neurodegeneration in the MPTP model of Parkinson disease. Nat Med 5:1403–1409. doi:10.1038/70978
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−Delta Delta C(T)) method. Methods San Diego Calif 25:402–408. doi:10.1006/meth.2001.1262
Machado V, Haas SJ, von Bohlen und Halbach O, Wree A, Krieglstein K, Unsicker K, Spittau B (2015) Growth/differentiation factor-15 deficiency compromises dopaminergic neuron survival and microglial response in the 6-hydroxydopamine mouse model of Parkinson’s disease. Neurobiol Dis 88:1-15. doi:10.1016/j.nbd.2015.12.016
Makwana M, Jones LL, Cuthill D, Heuer H, Bohatschek M, Hristova M, Friedrichsen S, Ormsby I, Bueringer D, Koppius A, Bauer K, Doetschman T, Raivich G (2007) Endogenous transforming growth factor beta 1 suppresses inflammation and promotes survival in adult CNS. J Neurosci 27:11201–11213. doi:10.1523/JNEUROSCI.2255-07.2007
McGeer PL, McGeer EG (2008) Glial reactions in Parkinson’s disease. Mov Disord 23:474–483. doi:10.1002/mds.21751
Nagatsu T, Mogi M, Ichinose H, Togari A (2000) Cytokines in Parkinson’s disease. J Neural Transm Suppl 58:143-151. doi:10.1007/978-3-7091-6284-2_12
O’Callaghan JP, Miller DB, Reinhard JF (1990) Characterization of the origins of astrocyte response to injury using the dopaminergic neurotoxicant, 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine. Brain Res 521:73–80. doi:10.1016/0006-8993(90)91526-M
Otto D, Unsicker K (1990) Basic FGF reverses chemical and morphological deficits in the nigrostriatal system of MPTP-treated mice. J Neurosci 10:1912–1921
Otto D, Unsicker K (1993) FGF-2 modulates dopamine and dopamine-related striatal transmitter systems in the intact and MPTP-lesioned mouse. Eur J Neurosci 5:927–932. doi:10.1111/j.1460-9568.1993.tb00943.x
Otto D, Unsicker K (1994) FGF-2 in the MPTP model of Parkinson’s disease: effects on astroglial cells. Glia 11:47–56. doi:10.1002/glia.440110107
Paxinos G, Franklin K (2012) Paxinos and Franklin’s the mouse brain in stereotaxic coordinates, 4th edn. Academic Press, Amsterdam
Peterson AL, Nutt JG (2008) Treatment of Parkinson’s disease with trophic factors. Neurother J Am Soc Exp Neurother 5:270–280. doi:10.1016/j.nurt.2008.02.003
Przedborski S, Jackson-Lewis V, Djaldetti R, Liberatore G, Vila M, Vukosavic S, Almer G (2000) The parkinsonian toxin MPTP: action and mechanism. Restor Neurol Neurosci 16:135–142
Przedborski S, Jackson-Lewis V, Naini AB, Jakowec M, Petzinger G, Miller R, Akram M (2001) The parkinsonian toxin 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine (MPTP): a technical review of its utility and safety. J Neurochem 76:1265–1274. doi:10.1046/j.1471-4159.2001.00183.x
Przedborski S, Vila M (2003) The 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine mouse model: a tool to explore the pathogenesis of Parkinson’s disease. Ann N Y Acad Sci 991:189–198. doi:10.1111/j.1749-6632.2003.tb07476.x
Rossaint J, Vestweber D, Zarbock A (2013) GDF-15 prevents platelet integrin activation and thrombus formation. J Thromb Haemost 11:335–344. doi:10.1111/jth.12100
Sarre S, Yuan H, Jonkers N, Van Hemelrijck A, Ebinger G, Michotte Y (2004) In vivo characterization of somatodendritic dopamine release in the substantia nigra of 6-hydroxydopamine-lesioned rats: effect of an MFB lesion on nigral cell bodies. J Neurochem 90:29–39. doi:10.1111/j.1471-4159.2004.02471.x
Sawada M, Imamura K, Nagatsu T (2006) Role of cytokines in inflammatory process in Parkinson’s disease. J Neural Transm Suppl 70:373-381. doi:10.1007/978-3-211-45295-0_57
Schaub N, Reichlin T, Twerenbold R, Reiter M, Steuer S, Bassetti S, Stelzig C, Wolf C, Winkler K, Haaf P, Meissner J, Drexler B, Mueller C (2012) Growth differentiation factor-15 in the early diagnosis and risk stratification of patients with acute chest pain. Clin Chem 58:441–449. doi:10.1373/clinchem.2011.173310
Scheller J, Chalaris A, Schmidt-Arras D, Rose-John S (2011) The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochim Biophys Acta 1813:878–888. doi:10.1016/j.bbamcr.2011.01.034
Schmidt N, Ferger B (2001) Neurochemical findings in the MPTP model of Parkinson’s disease. J Neural Transm 108:1263–1282. doi:10.1007/s007020100004
Schneider J, Lother A, Hein L, Gilsbach R (2011) Chronic cardiac pressure overload induces adrenal medulla hypertrophy and increased catecholamine synthesis. Basic Res Cardiol 106:591–602. doi:10.1007/s00395-011-0166-z
Schober A (2004) Classic toxin-induced animal models of Parkinson’s disease: 6-OHDA and MPTP. Cell Tissue Res 318:215–224. doi:10.1007/s00441-004-0938-y
Schober A, Peterziel H, von Bartheld CS, Simon H, Krieglstein K, Unsicker K (2007) GDNF applied to the MPTP-lesioned nigrostriatal system requires TGF-β for its neuroprotective action. Neurobiol Dis 25:378–391. doi:10.1016/j.nbd.2006.10.005
Simms SL, Huettner DP, Kortagere S (2015) In vivo characterization of a novel dopamine D3 receptor agonist to treat motor symptoms of Parkinson’s disease. Neuropharmacology 100:106–115. doi:10.1016/j.neuropharm.2015.04.004
Strelau J, Böttner M, Lingor P, Suter-Crazzolara C, Galter D, Jaszai J, Sullivan A, Schober A, Krieglstein K, Unsicker K (2000a) GDF-15/MIC-1 a novel member of the TGF-beta superfamily. J Neural Transm Suppl 60:273-276. doi:10.1007/978-3-7091-6301-6_18
Strelau J, Sullivan A, Böttner M, Lingor P, Falkenstein E, Suter-Crazzolara C, Galter D, Jaszai J, Krieglstein K, Unsicker K (2000b) Growth/differentiation factor-15/macrophage inhibitory cytokine-1 is a novel trophic factor for midbrain dopaminergic neurons in vivo. J Neurosci 20:8597–8603
Strelau J, Strzelczyk A, Rusu P, Bendner G, Wiese S, Diella F, Altick AL, von Bartheld CS, Klein R, Sendtner M, Unsicker K (2009) Progressive postnatal motoneuron loss in mice lacking GDF-15. J Neurosci 29:13640–13648. doi:10.1523/JNEUROSCI.1133-09.2009
Subramaniam S, Strelau J, Unsicker K (2003) Growth differentiation factor-15 prevents low potassium-induced cell death of cerebellar granule neurons by differential regulation of Akt and ERK pathways. J Biol Chem 278:8904–8912. doi:10.1074/jbc.M210037200
Tang Y, Le W (2015) Differential roles of M1 and M2 microglia in neurodegenerative diseases. Mol Neurobiol. doi:10.1007/s12035-014-9070-5
Teismann P, Schulz JB (2004) Cellular pathology of Parkinson’s disease: astrocytes, microglia and inflammation. Cell Tissue Res 318:149–161. doi:10.1007/s00441-004-0944-0
Teismann P, Tieu K, Cohen O, Choi DK, Wu DC, Marks D, Vila M, Jackson-Lewis V, Przedborski S (2003) Pathogenic role of glial cells in Parkinson’s disease. Mov Disord 18:121–129. doi:10.1002/mds.10332
Unsicker K, Spittau B, Krieglstein K (2013) The multiple facets of the TGF-β family cytokine growth/differentiation factor-15/macrophage inhibitory cytokine-1. Cytokine Growth Factor Rev 24:373–384. doi:10.1016/j.cytogfr.2013.05.003
Vila M, Jackson-Lewis V, Guégan C, Wu DC, Teismann P, Choi DK, Tieu K, Przedborski S (2001) The role of glial cells in Parkinson’s disease. Curr Opin Neurol 14:483–489. doi:10.1097/00019052-200108000-00009
Weissmiller AM, Wu C (2012) Current advances in using neurotrophic factors to treat neurodegenerative disorders. Transl Neurodegener 1:14. doi:10.1186/2047-9158-1-14
Zechel S, Jarosik J, Kiprianova I, Schober A, Unsicker K, von Bohlen und Halbach O (2006) FGF-2 deficiency does not alter vulnerability of the dopaminergic nigrostriatal system towards MPTP intoxication in mice. Eur J Neurosci 23:1671–1675. doi:10.1111/j.1460-9568.2006.04700.x
Zhou Z, Li W, Song Y, Wang L, Zhang K, Yang J, Zhang W, Su H, Zhang Y (2013) Growth differentiation factor-15 suppresses maturation and function of dendritic cells and inhibits tumor-specific immune response. PLoS One 8:e78618. doi:10.1371/journal.pone.0078618
Acknowledgments
We are grateful to Günter Frank for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors state that they have no conflict of interest.
Additional information
This study was supported in part by the Excellence Initiative of the German Research Foundation (GSC-4, Spemann Graduate School) and by grants from the German Research Foundation (DFG).
Rights and permissions
About this article
Cite this article
Machado, V., Gilsbach, R., Das, R. et al. Gdf-15 deficiency does not alter vulnerability of nigrostriatal dopaminergic system in MPTP-intoxicated mice. Cell Tissue Res 365, 209–223 (2016). https://doi.org/10.1007/s00441-016-2406-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-016-2406-x