Abstract
Increased activity of the sympathetic system is an important feature contributing to the pathogenesis and progression of chronic heart failure. While the mechanisms and consequences of enhanced norepinephrine release from sympathetic nerves have been intensely studied, the role of the adrenal gland in the development of cardiac hypertrophy and progression of heart failure is less well known. Thus, the aim of the present study was to determine the effect of chronic cardiac pressure overload in mice on adrenal medulla structure and function. Cardiac hypertrophy was induced in wild-type mice by transverse aortic constriction (TAC) for 8 weeks. After TAC, the degree of cardiac hypertrophy correlated significantly with adrenal weight and adrenal catecholamine storage. In the medulla, TAC caused an increase in chromaffin cell size but did not result in chromaffin cell proliferation. Ablation of chromaffin α2C-adrenoceptors did not affect adrenal weight or epinephrine synthesis. However, unilateral denervation of the adrenal gland completely prevented adrenal hypertrophy and increased catecholamine synthesis. Transcriptome analysis of microdissected adrenal medulla identified 483 up- and 231 downregulated, well-annotated genes after TAC. Among these genes, G protein-coupled receptor kinases 2 (Grk2) and 6 and phenylethanolamine N-methyltransferase (Pnmt) were significantly upregulated by TAC. In vitro, acetylcholine-induced Pnmt and Grk2 expression as well as enhanced epinephrine content was prevented by inhibition of nicotinic acetylcholine receptors and Ca2+/calmodulin-dependent signaling. Thus, activation of preganglionic sympathetic nerves innervating the adrenal medulla plays an essential role in inducing adrenal hypertrophy, enhanced catecholamine synthesis and induction of Grk2 expression after cardiac pressure overload.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Overactivity of the sympathetic nervous system is a prominent characteristic of chronic heart diseases. Elevated sympathetic tone represents an essential compensatory mechanism to maintain cardiac output by increasing heart rate, cardiac contractility and peripheral vascular resistance [4, 8, 40]. As a long-term consequence, increased catecholamine levels facilitate the progression of cardiac hypertrophy and fibrosis [5]. Moreover, the incidence of arrhythmias and sudden cardiac death is increased [25–27]. In cardiac myocytes, chronic sympathetic stimulation results in depletion of sarcoplasmic calcium stores leading to impaired myocardial contractility [41]. In addition, chronically enhanced norepinephrine levels are associated with a worsened prognosis of chronic heart failure patients [10], thus providing an explanation for the beneficial therapeutic effects of β-blockers [9, 12, 31]. But also activation of myocyte α1-adrenoceptors [15] as well as other factors worsens the development of chronic heart disease [23, 34, 39].
The level of circulating norepinephrine linearly correlates with adverse outcome of patients with chronic heart failure [10]. While plasma epinephrine concentrations may be normal during initial stages of heart failure, patients with cardiac cachexia showed elevated epinephrine plasma levels [1]. The contribution of adrenal catecholamines to the progression of heart failure has also been documented in experimental models. Mice lacking α2C-adrenoceptors which control epinephrine secretion via an autocrine feedback loop in adrenal chromaffin cells show rapid deterioration of cardiac function and raised mortality after transverse aortic constriction [6, 7, 16]. Adrenal gland hypertrophy and increased plasma epinephrine levels have been discovered in rats after experimental myocardial infarction and in mice overexpressing the sarcoplasmic reticulum calcium-binding protein calsequestrin [28]. Interestingly, upregulation of the G protein-coupled receptor kinase 2 (Grk2) in the adrenal medulla was demonstrated to desensitize inhibitory feedback α2C-receptors, thus allowing higher levels of adrenal epinephrine secretion and progression of heart failure [28, 29, 33].
Thus the aim of the present study was to determine the mechanisms of adrenal hypertrophy and increased epinephrine secretion in mice in response to the development of cardiac hypertrophy. Here, we demonstrate that preganglionic cholinergic nerves innervating the adrenal gland are essential to mediate adrenal hypertrophy, upregulation of Grk2 and increased epinephrine synthesis during cardiac pressure overload. Increased expression of Grk2 and Pnmt expression as well as epinephrine synthesis was induced by acetylcholine via a nicotinic receptor—Ca2+/calmodulin-dependent pathway.
Methods
Transverse aortic constriction and unilateral adrenal denervation
Cardiac pressure overload was induced in 8- to 12-week-old male mice (C57BL/6J) [16]. For surgery, mice were anesthetized with isoflurane (2 vol% in O2) and placed on a heating pad (37°C). After thoracotomy, the aortic arch was constricted to the width of a 27-G canula using a 6.0 nylon suture. All experiments were performed 8 weeks following TAC. Only one series of experiments was terminated 1 week after TAC (Fig. S2). To investigate the impact of sympathetic innervation of the adrenal gland, the left splanchnic nerve was transected at the left side within 48 h after aortic constriction. All experiments were approved by the responsible animal care committee of the University of Freiburg, Germany. The investigation conforms to the Guide for the Care and Use of Laboratory Animals (Institute of Laboratory Animal Resources, 1996).
Measurement of left ventricular contractile function
A 1.4F pressure–volume catheter (Millar Instruments, Houston, TX, USA) was inserted into the right carotic artery and left ventricle (anesthesia with 2 vol% isoflurane) [3, 16]. Chart v5.4 software (AD Instruments, Castle Hill, Australia) was used for data analysis. Two-dimensional guided M-mode and Doppler echocardiography using a Vivid 7 Dimension echocardiograph (GE Healthcare, Munich, Germany) equipped with a 14-MHz transducer were used to determine left ventricular ejection fraction and blood flow across the aortic stenosis.
Histology
Hearts were fixed in 4% paraformaldehyde in phosphate-buffered saline (PBS) and were embedded in paraffine [17]. Sections were stained with hematoxylin–eosin, Sirius red or wheat germ agglutinin (WGA, Alexa Fluor 488 conjugate, Invitrogen, Karlsruhe, Germany) [17]. Nuclei of WGA-stained sections were counterstained with propidium iodide. All adrenal weights given in this study refer to single adrenal glands. Adrenal tissues were fixed in paraformaldehyde solution for hematoxylin–eosin and WGA staining or frozen in liquid nitrogen for Ki67 staining. For Ki67 staining, cryosections were fixed with 4% paraformaldehyde in PBS, permeabilized with 0.1% Triton X-100 and blocked with 3% bovine serum albumin and 3% normal goat serum. Following incubation with the Ki67 antibody (rabbit monoclonal 1:1,000, 4°C, overnight; ThermoScientific, Waltham, MA, USA), Alexa Fluor® 488 secondary antibody (goat anti-rabbit; Invitrogen, Karlsruhe, Germany) was used. Cell nuclei were counterstained with DAPI (Sigma-Aldrich, Munich, Germany), and histological analysis was performed using AxioVision Rel.4.5 software (Carl Zeiss AG, Heidenheim, Germany).
Catecholamine determination
For measuring the catecholamine content, an isocratic HPLC with electrochemical detection was used consisting of an HPLC pump (UltiMate® 3000 Quaternary Analytical, Dionex), an autosampler (WISP 717plus, Waters, Eschborn) and an amperometric detector (Antec Intro, Antec-Leyden) [16, 17]. Data were registered and analyzed using Chromeleon 6 software (Dionex, Sunnyvale, CA, USA). Catecholamines were separated on a Prontosil 120-3-C18 AQ column (3 μm; 120 × 2 mm; Bischoff chromatography, Leonberg, Germany) [16, 17].
Microdissection and microarray analysis
Adrenal glands were frozen in liquid nitrogen. 12 μm cryosections were dehydrated in xylene. Adrenal medullary tissue was isolated by microdissection with a MicroChisel (Eppendorf, Hamburg, Germany) using a Leica AM6000 inverted microscope (Leica Microsystems, Wetzlar, Germany). Dissected tissue was aspirated in xylene, and RNA was isolated with the RNeasy Micro-Kit (Qiagen, Hilden, Germany). RNA expression was determined with a Murine Genome Chip 430 2.0 (Affymetrix, Santa Clara, CA, USA) and analyzed with ArrayAssist 5.0 software (Stratagene, Amsterdam, The Netherlands) [17]. Microarray data have been deposited in NCBI’s Gene Expression Omnibus (accession number GSE21829).
For determination of cardiac gene expression, RNA was isolated and analyzed as described previously [16, 17].
Adrenal medulla in vitro culture
Adrenal glands were prepared, collected in Locke’s buffer on ice, and the cortex was removed. The adrenal medulla was incubated at 37°C and 7.5% CO2 for 24 h using incubation medium (M199 Medium Earle (Biochrom AG, Berlin, Germany), 1% bovine serum albumin, 10% fetal calf serum, 100 U/mL penicillin/streptomycin). Samples were incubated with 200 μmol/L acetylcholine, 100 μmol/L hexamethonium, 1 μmol/L calmidazolium or 10 μmol/L KN-62 (Sigma-Aldrich, Munich, Germany). After 24 h, RNA of the adrenal medulla was isolated using the RNeasy Micro-Kit (Qiagen, Hilden, Germany), reverse transcribed (QuantiTect Rev. Transcription Kit, Qiagen, Hilden, Germany) and quantitative real-time PCR was performed as described previously [17] (Table 1).
Statistical analysis
Unpaired two-tailed Students t test or two-way ANOVA followed by Bonferroni post-hoc tests were performed for statistical analysis using GraphPad Prism software. A p value of <0.05 was considered statistically significant. Data are expressed as mean ± SEM.
Results
Adrenal hypertrophy in response to chronic cardiac pressure overload
After 8 weeks of TAC, mice developed significant cardiac and adrenal hypertrophy (Fig. 1a–g). Cardiac ventricle weight/tibia length ratios were increased from 6.7 ± 0.14 to 10.7 ± 0.50 mg/mm. 24% of the TAC-operated mice developed heart failure as indicated by severe lung edema. The hypertrophic response of the ventricle was accompanied by a 40% increase of the adrenal weight:tibia length ratios compared to levels observed in sham-operated mice (Fig. 1a, b). Adrenal weight showed a significant linear correlation with cardiac weight (Fig. 1c). This correlation was similar when the parameters were corrected for tibia length (Fig. S1), while the correlation coefficients for the individual sham-operated and TAC groups did not reach statistical significance (sham p = 0.244; TAC p = 0.54). After 8 weeks of TAC, the adrenal content of epinephrine and norepinephrine was increased as compared with sham-operated mice (Fig. 1h, i). Further experiments revealed that the concordant increase of adrenal weight and ventricle weight was already present after 1 week of TAC (Fig. S2), indicating a fast onset of the hypertrophic response in both tissues.
Increased weight and catecholamine content of adrenal glands following transverse aortic constriction (TAC). Cardiac ventricle weight/tibia length ratio (a) or adrenal weight/tibia length ratio (b) of wild-type C57BL/6 mice 8 weeks after TAC or sham operation (n = 10–19 per group). c Correlation of adrenal weight to ventricle weight in sham (open squares) and TAC (filled squares) operated mice (r 2 = 0.3190; p = 0.0006). d–g Hematoxylin–eosin staining of mid-ventricular cardiac (d, e, scale bars 1 mm) or adrenal gland (f, g, insert, scale bars 500 μm) and adrenal medulla (f, g, large picture, scale bars 100 μm) sections following sham and TAC surgery. h, i Adrenal epinephrine (h) and norepinephrine (i) content as determined by HPLC (n = 6–12 per group; *p < 0.05, ***p < 0.001 TAC vs. sham)
Effect of ablation of adrenal α2C-adrenoceptor expression
Previous studies have demonstrated that α2C-adrenoceptors are important feedback regulators of catecholamine secretion from the adrenal gland [6, 7, 16, 28]. Genetic ablation of α2C-receptor expression led to increased circulating epinephrine levels and accelerated progression of cardiac hypertrophy [7]. Thus, we sought to determine whether loss of α2C-adrenoceptors affected adrenal weight and catecholamine storage. When compared with wild-type mice, α2C-deficient mice did not show differences in adrenal, heart or body weight and did not store higher amounts of epinephrine in the adrenal gland (Table 2). This finding indicates that increased catecholamine release due to loss or desensitization of α2-adrenoceptors per se does not lead to adrenal hypertrophy.
Cardiac function and morphology after unilateral adrenal denervation
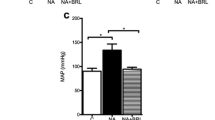
Thus, we investigated whether circulating factors or sympathetic innervation of the adrenal gland were responsible for adrenal hypertrophy after cardiac pressure overload. To distinguish between these two possibilities, preganglionic nerves innervating the adrenal gland were unilaterally transected in sham- and TAC-operated mice. 8 weeks of TAC resulted in impaired cardiac function as evidenced by a reduction in left ventricular ejection fraction (EF) and fractional shortening (FS) (EF −43.8%, FS −59.7% vs. sham, p < 0.05; Fig. 2a–c). Heart rate and systolic blood pressure in the ascending aorta were increased after TAC compared to controls (+56.4 and +42.9%, respectively vs. sham, p < 0.05; Fig. 2d, e). Unilateral adrenal denervation within the first 48 h after transverse aortic constriction had no effect on cardiovascular parameters, both under basal conditions and following TAC compared with the corresponding control groups (Fig. 2).
Alterations in left ventricular contractile function after transverse aortic constriction and unilateral adrenal denervation. a–c Representative 2D-guided M-mode echocardiography from parasternal short axis view (a), left ventricular ejection fraction (b) and fractional shortening (c) in sham- or TAC-operated mice with or without unilateral adrenal denervation. d, e Heart rate and systolic aortic pressure as determined by direct catheterization during isoflurane anesthesia (n = 4–12, *p < 0.05, **p < 0.01, ***p < 0.001 TAC vs. sham)
After 8 weeks of pressure overload, cardiac myocyte cross-sectional area and interstitial fibrosis were significantly increased compared to controls (+62.9 and +752%, respectively vs. sham, p < 0.05; Fig. 3a–d). Similarly, cardiac atrial natriuretic peptide and periostin mRNA expression were increased after TAC (Fig. 3e, f). Again, unilateral adrenal gland denervation had no effect on these parameters as compared with the corresponding control groups (Fig. 3a–f).
Cardiac hypertrophy and fibrosis following TAC and unilateral adrenal denervation. a, b Cardiac myocyte cross-sectional area as determined by wheat germ agglutinin staining of mid-ventricular cardiac sections (a, scale bars 50 μm). c, d Left ventricular interstitial fibrosis detected by Sirius red staining of mid-ventricular cardiac sections (c, scale bars 100 μm). e, f Cardiac mRNA expression of atrial natriuretic peptide (Nppa, e) and periostin (Postn, f) (n = 4–7; *p < 0.05, **p < 0.01, ***p < 0.001 TAC vs. sham)
Adrenal morphology and epinephrine secretion after unilateral adrenal denervation
After 8 weeks of TAC, unilateral denervation within 48 h after transverse aortic constriction completely prevented the increase in adrenal gland weight after pressure overload (Fig. 4a, b). Both adrenal medulla and cortex contributed to the enlargement of the adrenal gland after TAC (Fig. 4c, d). Both adrenal compartments were unchanged after TAC and unilateral denervation, indicating an essential role of sympathetic innervation for adrenal gland hypertrophy. After TAC the cross-sectional area of chromaffin cells in the adrenal medulla was significantly increased (Fig. 4e). The cellular hypertrophy was in addition reflected by a reduced density of nuclei in the adrenal medulla (Fig. S3), while the number of chromaffin cells which were positive for the proliferation marker Ki67 did not differ between sham and TAC specimens (Fig. 4f).
Influence of unilateral adrenal denervation on adrenal hypertrophy following chronic cardiac pressure overload. a, b Adrenal weight/tibia length ratio and histology after transverse aortic constriction and unilateral adrenal denervation (b, hematoxylin–eosin staining, scale bars 500 μm). c, d Morphometric analysis of adrenal medulla (c) and cortex (d) cross-sectional areas. e Wheat germ agglutinin staining and morphometry of adrenal medullary sections to determine chromaffin cell size (scale bars 20 μm). f Ki67 and DAPI staining of the adrenal medulla (scale bars 20 μm) (n = 3–15, *p < 0.05, **p < 0.01, ***p < 0.001 TAC vs. sham)
To measure the impact of TAC and unilateral denervation on epinephrine secretion, 24 h urine was collected. 8 weeks after TAC-operation, the epinephrine content was 2.5-fold higher than after sham-operation. Unilateral denervation did not affect the amount of secreted epinephrine, but no further raise in epinephrine secretion was observed after TAC (Fig. S4).
Transcriptome analysis of the adrenal medulla after cardiac pressure overload
In order to identify which changes in gene expression accompany the development of adrenal hypertrophy, the adrenal medulla from sham- and TAC-operated mice was microdissected, and mRNA was subjected to microarray expression analysis. After TAC, expression of 714 well annotated and 108 probe sets of hypothetical genes was changed more than 1.5-fold in the adrenal medulla (Fig. 5a; Suppl. Table 1). Among the well-annotated genes, 483 genes were increased and 231 genes were decreased in their expression levels. Pathway analysis revealed that adrenal medullary MAPK signaling, notch signaling, focal adhesion and actin cytoskeleton pathways were significantly affected by cardiac pressure overload (Suppl. Table 1). Among the adrenergic target genes, the G protein-coupled receptor kinases 2 and 6 (Grk2, Grk6) and the phenylethanolamine N-methyltransferase (Pnmt) were significantly upregulated after TAC (Fig. 5b, c). Increased expression of Grk2, Grk6 and Pnmt after TAC was validated by quantitative real-time PCR in independently microdissected medullary specimens (Fig. 5c). Unilateral denervation prevented the increased expression of Grk2 and Pnmt which was induced by cardiac pressure overload (Fig. 5d, e). In addition, the β4-subunit of the nicotinic acetylcholine receptor (Chrnb4) was increased in its mRNA expression after TAC to 2.04-fold of control (Suppl. Table 1).
Microarray analysis of gene expression in the adrenal medulla after chronic cardiac pressure overload. a Adrenal medulla was isolated by microdissection of cryostat sections using a piezo-driven microneedle (a, insert). Microarray analysis of total adrenal medulla mRNA from sham- versus TAC-operated wild-type C57BL/6 mice revealed 714 well-annotated genes which were differentially expressed (red, >1.5-fold, p < 0.05). b Expression of adrenergic target genes in adrenal medulla (n = 3 sham, 3 TAC samples). Red color depicts higher expression than mean of control; green indicates lower expression. c Expression of G protein-coupled receptor kinases 2 (Grk2) and 6 (Grk6) and phenylethanolamine N-methyltransferase (Pnmt) derived from microarray analysis in the adrenal medulla of sham- or TAC-operated mice (n = 3 per group). d, e Expression of Grk2 and Pnmt in microdissected adrenal medulla as measured by qPCR (n = 4–6; *p < 0.05, **p < 0.01 TAC vs. sham)
In vitro regulation of gene expression and adrenal epinephrine content
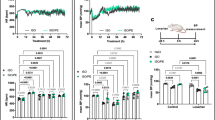
In order to confirm that preganglionic cholinergic innervation is essential for gene expression of Pnmt, Grk2 and Grk6, mRNA expression of these genes was measured after in vitro stimulation of adrenal medulla biopsies with acetylcholine (Fig. 6a). Similar to the in vivo situation, in vitro incubation with acetylcholine increased Pnmt mRNA expression to 2.3-fold and Grk2 mRNA expression to 1.6-fold of unstimulated control (Fig. 6a, b; p < 0.05). Hexamethonium, an inhibitor of nicotinic acetylcholine receptors, prevented the acetylcholine-induced rise in Pnmt and Grk2 expression (Fig. 6a, b). Similarly, acetylcholine-induced Pnmt and Grk2 expression could be inhibited by the calmodulin inhibitor calmidazolium and the CaM kinase II inhibitor KN-62 (Fig. 6a, b). No alterations in Grk6 mRNA expression were observed under the various conditions (Fig. 6c).
Regulation of Pnmt, Grk2 and GRK6 expression in adrenal medulla in vitro. a–c Pnmt, Grk2 and Grk6 mRNA levels in adrenal medulla after 24-h incubation in vitro. Medulla specimens were stimulated with 200 μmol/L acetylcholine in the absence or presence of the nicotinic acetylcholine receptor antagonist hexamethonium (100 μmol/L), calmidazolium (1 μmol/L, calmodulin antagonist) or KN-62 (10 μmol/L, CaM kinase II inhibitor) (n = 4–6; *p < 0.05, ***p < 0.001 acetylcholine vs. unstimulated). d Model of the effect of preganglionic cholinergic nerves on adrenal chromaffin structure and function after chronic cardiac pressure overload. For details, see “Discussion”
Concordant with the induction of Pnmt mRNA expression, adrenal epinephrine content was elevated after in vitro stimulation with acetylcholine (Fig. S5a). This effect was also prevented by application of hexamethonium, calmidazolium or KN-62. These results underpin the relevance of this pathway for the regulation of epinephrine synthesis in the adrenal medulla. However, pretreatment with acetylcholine did not affect the amount of epinephrine released into media upon acute acetylcholine stimulation (Fig. S5b). Furthermore, incorporation of [14C]phenylalanine and cell size were not altered by 24 h of acetylcholine stimulation (Fig. S5c, d).
Discussion
The main finding of the present study is that chronic cardiac pressure overload in mice induces adrenal medulla hypertrophy, increased epinephrine synthesis and induction of Grk2 via a nicotinic acetylcholine receptor-dependent pathway in chromaffin cells.
Adrenal hypertrophy has been observed in several animal models of cardiac dysfunction or stress. Induction of heart failure by experimental myocardial infarction in rats or by transgenic cardiac expression of calsequestrin in mice resulted in hypertrophy of the adrenal gland [28]. Adrenal hypertrophy has also been shown in several stress models in rodents, e.g. chronic immobilization [18], normobaric hypoxia [42] and exposure to a hyperbaric environment [19]. Similar to the observation in the present study, hyperbaric conditions led to increased size of both adrenal cortex and medulla [19]. Adrenocortical hypertrophy has been shown to be reversible and is likely to be a stress response [22]. This may be explained at least partly by the observation that heart failure causes not only an activation of the sympathetic nervous system, but also an enhanced activity of the renin–angiotensin–aldosterone system [21, 24, 30, 32, 35]. Elevated levels of epinephrine and norepinephrine and also cortisol and aldosterone have been described for patients with cardiac cachexia [2]. There are strong interactions between the adrenal medulla and the cortex. In isolated adrenal glands with intact splanchnic nerves, activation of the splanchnic nerve as well as perfusion with epinephrine caused release of cortisol and aldosterone [13]. After incubation with epinephrine, increased steroidogenesis and enhanced levels of P450-mRNAs were observed. Interactions have also been described vice versa: venous blood from the adrenal cortex goes to the adrenal medulla by an intra-adrenal portal vascular system. This causes extremely high glucocorticoid concentrations in the adrenal medulla inducing PNMT expression. Suppression of glucocorticoid production is described to determine a decrease of epinephrine level [46]. The PNMT promoter region contains a glucocorticoid response element, where the activated glucocorticoid receptor can bind and induce PNMT expression [47]. Mice lacking the glucocorticoid receptor do not show a central adrenal medulla and are not able to produce epinephrine [11]. These interactions show that an isolated hypertrophy of one compartment is unlikely. Further studies are required to clarify the involved pathways and the relevance for the pathophysiology of cardiac hypertrophy and heart failure.
The underlying mechanisms of adrenal hypertrophy were dissected in an elegant series of recent studies demonstrating that cardiac failure led to upregulation of the G protein-coupled receptor kinase 2 (Grk2) in adrenal chromaffin cells [28, 29, 33]. In the heart, increased Grk2 levels contribute significantly to β-adrenoceptor desensitization and left ventricular dysfunction [36]. In the adrenal medulla, Grk2 potentially downregulates and desensitizes α2C-adrenoceptors, which play an essential role as inhibitory feedback regulators of adrenal catecholamine secretion (Fig. 6b) [6, 28]. Genetic deletion of the α2C-receptor gene in mice led to increased circulating epinephrine levels and facilitated the development of heart failure after cardiac pressure overload [6, 7, 16].
Here, we demonstrate that loss of α2C-receptor expression per se was not sufficient to induce adrenal hypertrophy or increased catecholamine storage. Thus, in addition to α2C-adrenoceptors, Grk2 may have additional targets which contribute to adrenal hypertrophy and enhanced catecholamine secretion during heart failure. Indeed, a number of G protein-coupled receptors were found to be dysregulated in the adrenal medulla after cardiac pressure overload, and the transcriptome analysis performed in the present study may help to identify these additional pathways engaged by Grk2 in chromaffin cell hypertrophy. The central role of Grk2 was proposed in a recent study by selective ablation of Grk2 expression in chromaffin cells by using a Pnmt-driven Cre recombinase mouse line [29]. Loss of Grk2 in the adrenal medulla resulted in reduced adrenal gland weight; it prevented α2-receptor downregulation and functional desensitization and caused improvement of circulating catecholamine levels and cardiac function after experimental myocardial infarction [29]. However, Grk2 deletion did not completely prevent adrenal hypertrophy after infarction indicating that additional pathways beside Grk2 may contribute to adrenal dysfunction in this situation [29].
In order to distinguish between circulating versus neuronal factors activating adrenal hypertrophy and catecholamine synthesis, adrenal glands were unilaterally denervated from the preganglionic cholinergic nerves. Previous studies in dogs have demonstrated that bilateral adrenal denervation greatly reduced cardiac remodeling and dysfunction after cardiac pressure overload [43]. In order to avoid potential problems with adrenal cortical function after bilateral adrenal denervation, the present study was not designed to further document the effects of adrenal medulla catecholamines on cardiac remodeling. However, we chose the unilateral adrenal denervation to determine the effect of cardiac pressure overload on one adrenal with intact sympathetic innervation and one adrenal with disrupted innervation in the same animal. Interestingly, unilateral adrenal denervation prevented adrenal hypertrophy, Grk2 upregulation and increased expression of Pnmt and associated catecholamine storage.
Urine epinephrine levels indicate that the remaining innervated adrenal gland functionally replaces the denervation of one adrenal in sham-operated animals, but fails to elevate epinephrine levels further in response to cardiac pressure overload.
In vitro experiments confirmed the central role of acetylcholine released from preganglionic sympathetic nerves for the induction of Pnmt and Grk2 via a nicotinic acetylcholine—Ca2+/calmodulin dependent pathway. The relevance of the Pnmt regulation is supported by experiments showing that epinephrine content of the adrenal gland is modulated by this pathway in vitro. The anticipated hypertrophic effect elicited by induction of Grk2 expression was not observed after in vitro stimulation with acetylcholine. Maybe the onset of the hypertrophic effect is too slow to be detectable after 24 h, but at least in vivo only 1 week of cardiac pressure overload induced adrenal hypertrophy. This discrepancy may suggest the implication of additional hypertrophic pathways.
The main class of nicotinic receptors in chromaffin cells consists of α3- and β4-subunits [37]. Their effect is to increase the permeability of sodium, potassium and calcium ions upon activation by acetylcholine. Expression of α3β4-nicotinic receptors has been shown to increase after chronic stimulation with agonists [37]. In the present study, mRNA levels of the β4-nicotinic receptor subunit in chromaffin cells were twofold elevated after TAC as compared with sham-operated mice. Thus, a positive feedback loop activated by acetylcholine may facilitate further intracellular signaling events in chromaffin cells.
Activation of nicotinic receptors is able to modulate the expression of genes within minutes [20]. The regulation of Pnmt expression by calcium has been shown in bovine chromaffin cell culture after stimulation with angiotensin II [38]. Pnmt expression was increased after treatment with calcium ionophores and could be inhibited by nifedipine. This suggested a dependency on calcium. Enhanced Pnmt expression by angiotensin II stimulation could be inhibited by calmidazolium. Calmidazolium was also used in our study and was able to inhibit enhanced Pnmt expression following acetylcholine stimulation. Our findings are consistent with several reports, demonstrating an involvement of nicotinic receptors in vivo and in vitro in Pnmt regulation [14, 44, 45]. Antagonists of nicotinic receptors prevented an increase of Pnmt expression in bovine chromaffin cell culture [14].
In conclusion, the present study demonstrates that activation of preganglionic sympathetic nerves innervating the adrenal medulla plays an essential role in induction of adrenal hypertrophy, enhanced catecholamine synthesis and induction of Grk2 expression, which is thought to desensitize feedback control of catecholamine release in chromaffin cells. Future studies are required to unravel the precise molecular mechanisms of adrenal medulla hypertrophy and the interplay between nicotinic receptors, Grk2 and α2C-adrenoceptors in chromaffin cells. Uncovering the role of these target proteins in the adrenal medulla may not only lead to novel therapeutic strategies to halt progression of heart failure but also to prevent adverse adrenal effects of chronic stress.
References
Anker SD, Chua TP, Ponikowski P, Harrington D, Swan JW, Kox WJ, Poole-Wilson PA, Coats AJ (1997) Hormonal changes and catabolic/anabolic imbalance in chronic heart failure and their importance for cardiac cachexia. Circulation 96(2):526–534
Anker SD, Steinborn W, Strassburg S (2004) Cardiac cachexia. Ann Med 36(7):518–529. doi:10.1080/07853890410017467
Beetz N, Harrison MD, Brede M, Zong X, Urbanski MJ, Sietmann A, Kaufling J, Barrot M, Seeliger MW, Vieira-Coelho MA, Hamet P, Gaudet D, Seda O, Tremblay J, Kotchen TA, Kaldunski M, Nusing R, Szabo B, Jacob HJ, Cowley AW Jr, Biel M, Stoll M, Lohse MJ, Broeckel U, Hein L (2009) Phosducin influences sympathetic activity and prevents stress-induced hypertension in humans and mice. J Clin Invest 119(12):3597–3612. doi:10.1172/JCI38433
Braunwald E (2008) Biomarkers in heart failure. N Engl J Med 358(20):2148–2159. doi:10.1056/NEJMra0800239
Braunwald E, Bristow MR (2000) Congestive heart failure: fifty years of progress. Circulation 102(20 Suppl 4):IV14–IV23
Brede M, Nagy G, Philipp M, Sorensen JB, Lohse MJ, Hein L (2003) Differential control of adrenal and sympathetic catecholamine release by alpha 2-adrenoceptor subtypes. Mol Endocrinol 17(8):1640–1646. doi:10.1210/me.2003-0035
Brede M, Wiesmann F, Jahns R, Hadamek K, Arnolt C, Neubauer S, Lohse MJ, Hein L (2002) Feedback inhibition of catecholamine release by two different alpha2-adrenoceptor subtypes prevents progression of heart failure. Circulation 106(19):2491–2496
Ceconi C, Curello S, Ferrari R (1998) Catecholamines: the cardiovascular and neuroendocrine system. Eur Heart J 19(Suppl F):F2–F6
CIBIS-II Investigators and Committees (1999) The Cardiac Insufficiency Bisoprolol Study II (CIBIS-II): a randomised trial. Lancet 353(9146):9–13. doi:S0140673698111819
Cohn JN, Levine TB, Olivari MT, Garberg V, Lura D, Francis GS, Simon AB, Rector T (1984) Plasma norepinephrine as a guide to prognosis in patients with chronic congestive heart failure. N Engl J Med 311(13):819–823
Cole TJ, Blendy JA, Monaghan AP, Krieglstein K, Schmid W, Aguzzi A, Fantuzzi G, Hummler E, Unsicker K, Schutz G (1995) Targeted disruption of the glucocorticoid receptor gene blocks adrenergic chromaffin cell development and severely retards lung maturation. Genes Dev 9(13):1608–1621
(1999) Effect of metoprolol CR/XL in chronic heart failure: Metoprolol CR/XL Randomised Intervention Trial in Congestive Heart Failure (MERIT-HF). Lancet 353(9169):2001–2007. doi:S0140673699044402
Ehrhart-Bornstein M, Bornstein SR, Gonzalez-Hernandez J, Holst JJ, Waterman MR, Scherbaum WA (1995) Sympathoadrenal regulation of adrenocortical steroidogenesis. Endocr Res 21(1–2):13–24
Evinger MJ, Ernsberger P, Regunathan S, Joh TH, Reis DJ (1994) A single transmitter regulates gene expression through two separate mechanisms: cholinergic regulation of phenylethanolamine N-methyltransferase mRNA via nicotinic and muscarinic pathways. J Neurosci 14(4):2106–2116
Frey UH, Lieb W, Erdmann J, Savidou D, Heusch G, Leineweber K, Jakob H, Hense HW, Lowel H, Brockmeyer NH, Schunkert H, Siffert W (2008) Characterization of the GNAQ promoter and association of increased Gq expression with cardiac hypertrophy in humans. Eur Heart J 29(7):888–897. doi:10.1093/eurheartj/ehm618
Gilsbach R, Brede M, Beetz N, Moura E, Muthig V, Gerstner C, Barreto F, Neubauer S, Vieira-Coelho MA, Hein L (2007) Heterozygous alpha 2C-adrenoceptor-deficient mice develop heart failure after transverse aortic constriction. Cardiovasc Res 75(4):728–737. doi:10.1016/j.cardiores.2007.05.017
Gilsbach R, Schneider J, Lother A, Schickinger S, Leemhuis J, Hein L (2010) Sympathetic alpha(2)-adrenoceptors prevent cardiac hypertrophy and fibrosis in mice at baseline but not after chronic pressure overload. Cardiovasc Res 86(3):432–442. doi:10.1093/cvr/cvq014
Gomez F, Lahmame A, de Kloet ER, Armario A (1996) Hypothalamic-pituitary-adrenal response to chronic stress in five inbred rat strains: differential responses are mainly located at the adrenocortical level. Neuroendocrinology 63(4):327–337
Gosney JR (1985) Adrenal corticomedullary hyperplasia in hypobaric hypoxia. J Pathol 146(1):59–64. doi:10.1002/path.1711460107
Greenberg ME, Ziff EB, Greene LA (1986) Stimulation of neuronal acetylcholine receptors induces rapid gene transcription. Science 234(4772):80–83
Grippo AJ, Johnson AK (2009) Stress, depression and cardiovascular dysregulation: a review of neurobiological mechanisms and the integration of research from preclinical disease models. Stress 12(1):1–21. doi:10.1080/10253890802046281
Harvey PW, Sutcliffe C Adrenocortical hypertrophy: establishing cause and toxicological significance. J Appl Toxicol 30(7):617–626. doi:10.1002/jat.1569
Haworth RS, Cuello F, Avkiran M (2011) Regulation by phosphodiesterase isoforms of protein kinase A-mediated attenuation of myocardial protein kinase D activation. Basic Res Cardiol 106(1):51–63. doi:10.1007/s00395-010-0116-1
Johnson AK, Grippo AJ (2006) Sadness and broken hearts: neurohumoral mechanisms and co-morbidity of ischemic heart disease and psychological depression. J Physiol Pharmacol 57(Suppl 11):5–29
Kaye DM, Lefkovits J, Jennings GL, Bergin P, Broughton A, Esler MD (1995) Adverse consequences of high sympathetic nervous activity in the failing human heart. J Am Coll Cardiol 26(5):1257–1263. doi:10.1016/0735-1097(95)00332-0
Keating MT, Sanguinetti MC (2001) Molecular and cellular mechanisms of cardiac arrhythmias. Cell 104(4):569–580. doi:S0092-8674(01)00243-4
Leineweber K, Heusch G, Schulz R (2007) Regulation and role of the presynaptic and myocardial Na+/H+ exchanger NHE1: effects on the sympathetic nervous system in heart failure. Cardiovasc Drug Rev 25(2):123–131. doi:10.1111/j.1527-3466.2007.00010.x
Lymperopoulos A, Rengo G, Funakoshi H, Eckhart AD, Koch WJ (2007) Adrenal GRK2 upregulation mediates sympathetic overdrive in heart failure. Nat Med 13(3):315–323. doi:10.1038/nm1553
Lymperopoulos A, Rengo G, Gao E, Ebert SN, Dorn GW 2nd, Koch WJ (2010) Reduction of sympathetic activity via adrenal-targeted GRK2 gene deletion attenuates heart failure progression and improves cardiac function after myocardial infarction. J Biol Chem 285(21):16378–16386. doi:10.1074/jbc.M109.077859
Nicholls DP, Onuoha GN, McDowell G, Elborn JS, Riley MS, Nugent AM, Steele IC, Shaw C, Buchanan KD (1996) Neuroendocrine changes in chronic cardiac failure. Basic Res Cardiol 91(Suppl 1):13–20
Packer M, Bristow MR, Cohn JN, Colucci WS, Fowler MB, Gilbert EM, Shusterman NH (1996) The effect of carvedilol on morbidity and mortality in patients with chronic heart failure. U.S. Carvedilol Heart Failure Study Group. N Engl J Med 334(21):1349–1355
Pool PE (1998) Neurohormonal activation in the treatment of congestive heart failure: basis for new treatments? Cardiology 90(1):1–7. doi:crd90001
Rengo G, Leosco D, Zincarelli C, Marchese M, Corbi G, Liccardo D, Filippelli A, Ferrara N, Lisanti MP, Koch WJ, Lymperopoulos A (2010) Adrenal GRK2 lowering is an underlying mechanism for the beneficial sympathetic effects of exercise training in heart failure. Am J Physiol Heart Circ Physiol 298(6):H2032–H2038. doi:10.1152/ajpheart.00702.2009
Richter W, Xie M, Scheitrum C, Krall J, Movsesian MA, Conti M (2011) Conserved expression and functions of PDE4 in rodent and human heart. Basic Res Cardiol 106(2):249–262. doi:10.1007/s00395-010-0138-8
Riegger AJ (1991) Role of neuroendocrine mechanisms in the pathogenesis of heart failure. Basic Res Cardiol 86(Suppl 3):125–131
Rockman HA, Koch WJ, Lefkowitz RJ (2002) Seven-transmembrane-spanning receptors and heart function. Nature 415(6868):206–212. doi:10.1038/415206a
Sala F, Nistri A, Criado M (2008) Nicotinic acetylcholine receptors of adrenal chromaffin cells. Acta Physiol 192(2):203–212. doi:10.1111/j.1748-1716.2007.01804.x
Stachowiak MK, Jiang HK, Poisner AM, Tuominen RK, Hong JS (1990) Short and long term regulation of catecholamine biosynthetic enzymes by angiotensin in cultured adrenal medullary cells. Molecular mechanisms and nature of second messenger systems. J Biol Chem 265(8):4694–4702
Takahama H, Asanuma H, Sanada S, Fujita M, Sasaki H, Wakeno M, Kim J, Asakura M, Takashima S, Minamino T, Komamura K, Sugimachi M, Kitakaze M (2010) A histamine H receptor blocker ameliorates development of heart failure in dogs independently of beta-adrenergic receptor blockade. Basic Res Cardiol 105(6):787–794. doi:10.1007/s00395-010-0119-y
Watson AM, Hood SG, May CN (2006) Mechanisms of sympathetic activation in heart failure. Clin Exp Pharmacol Physiol 33(12):1269–1274. doi:10.1111/j.1440-1681.2006.04523.x
Wehrens XH, Marks AR (2003) Altered function and regulation of cardiac ryanodine receptors in cardiac disease. Trends Biochem Sci 28(12):671–678. doi:S096800040300255X
Wolman M, Cervos-Navarro J, Sampaolo S, Cardesa A (1993) Pathological changes in organs of rats chronically exposed to hypoxia. Development of pulmonary lipidosis. Histol Histopathol 8(2):247–255
Womble JR, Larson DF, Copeland JG, Brown BR, Haddox MK, Russell DH (1980) Adrenal medulla denervation prevents stress-induced epinephrine plasma elevation and cardiac hypertrophy. Life Sci 27(24):2417–2420
Wong DL, Bildstein CL, Siddall B, Lesage A, Yoo YS (1993) Neural regulation of phenylethanolamine N-methyltransferase in vivo: transcriptional and translational changes. Brain Res Mol Brain Res 18(1–2):107–114
Wong DL, Ebert SN, Morita K (1998) Neural control of phenylethanolamine-N-methyltransferase via cholinergic activation of Egr-I. Adv Pharmacol 42:77–81
Wurtman RJ (2002) Stress and the adrenocortical control of epinephrine synthesis. Metabolism 51(6 Suppl 1):11–14. doi:ameta0510s11
Yamamoto KR (1985) Steroid receptor regulated transcription of specific genes and gene networks. Annu Rev Genet 19:209–252. doi:10.1146/annurev.ge.19.120185.001233
Acknowledgments
This study was supported by the Deutsche Forschungsgemeinschaft (DFG He 2073/3-1). We thank the EMBL GeneCore (Heidelberg, Germany) staff, especially Vladimir Benes and Tomi Ivacevic, for performing the Affymetrix microarray experiments.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Schneider, J., Lother, A., Hein, L. et al. Chronic cardiac pressure overload induces adrenal medulla hypertrophy and increased catecholamine synthesis. Basic Res Cardiol 106, 591–602 (2011). https://doi.org/10.1007/s00395-011-0166-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00395-011-0166-z