Abstract
Purpose
Activated CDC42-associated kinase-1 (ACK1/TNK2) and epigenetic regulators of the histone deacetylase (HDAC) family regulate the proliferation and survival of leukemic cells. 18 HDACs fall into four classes (I–IV). We tested the impact of clinically relevant histone deacetylase inhibitors (HDACi) on ACK1 and if such drugs combine favorably with the therapeutically used ACK1 inhibitor Dasatinib.
Methods
We applied the broad-range HDACi Panobinostat/LBH589 and the class I HDAC-specific inhibitor Entinostat/MS-275 to various acute and chronic myeloid leukemia cells (AML/CML). We also used the replicative stress inducer Hydroxyurea (HU), a standard drug for leukemic patients, and the apoptosis inducer Staurosporine (STS). To assess cytotoxic effects of HDACi, we measured cell cycle profiles and DNA fragmentation by flow cytometry. Western blot was employed to analyze protein expression and phosphorylation.
Results
LBH589 and MS-275 induce proteolysis of ACK1 in CML and AML cells. Panobinostat more strongly induces apoptosis than Entinostat, and this correlates with a significantly pronounced loss of ACK1. STS and HU also propel the degradation of ACK1 in leukemic cells. Moreover, the caspase inhibitor z-VAD-FMK reduces ACK1 degradation in the presence of HDACi. Concomitant with the attenuation of ACK1, we noticed decreased phosphorylation of STAT3. Direct inhibition of ACK1 with Dasatinib also suppresses STAT3 phosphorylation. Furthermore, Dasatinib and HDACi combinations are effective against CML cells.
Conclusion
HDACs sustain the ACK1-STAT3 signaling node and leukemic cell growth. Consistent with their different effects on ACK1 stability or auto-phosphorylation, Dasatinib and HDACi combinations produce beneficial antileukemic effects.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The non-receptor tyrosine kinase (TK) ACK1 critically regulates the growth and development of solid tumors (Mahajan and Mahajan 2015). Increasing evidence suggests that ACK1 also controls leukemic cell fate (Maxson et al. 2013, 2016; Nonami et al. 2015). For example, in chronic neutrophilic leukemia and atypical BCR-ABL1-negative CML, activating mutations in the receptor for colony-stimulating factor-3 induce signaling involving ACK1 (Maxson et al. 2013). Furthermore, NRAS and ACK1 are often dysregulated in human cancers, and the selective RAS antagonist GNF-7 inhibits NRAS-dependent AML and acute lymphoblastic leukemia cell growth through a combined inhibition of ACK1 and other kinases (Nonami et al. 2015). Moreover, ACK1 point mutations leading to oncogenic alterations occur in patients with AML and chronic myelomonocytic leukemia. Cells with such mutations are sensitive to Dasatinib and other ACK1 inhibitors (XMD8-87/XMD16-5) (Maxson et al. 2016). Dasatinib is useful for patients suffering from BCR-ABL-positive CML and other malignancies (Mace et al. 2015). It is known that Dasatinib also inhibits ACK1 in prostate and breast cancer cells (Liu et al. 2010; Mahajan et al. 2014), and in CML clones (Shah et al. 2016).
HDACi are epigenetic drugs that target the acetylation/deacetylation balance of histones and non-histone proteins (Afifi et al. 2015; Ma et al. 2016; Müller and Krämer 2010; Seto and Yoshida 2014). The HDACi Panobinostat (LBH589), Depsipeptide (FK228), Vorinostat (SAHA), and Belinostat (PXD101) are approved drugs against cutaneous and peripheral T-cell lymphoma, and the FDA permits LBH589 for the treatment of multiple myeloma (Afifi et al. 2015; Ma et al. 2016). As for other chemotherapies, HDACi give optimal benefits in combinatory schedules. Optimal application schemes as well as markers showing the therapeutic efficacy of HDACi need to be established (Graham et al. 2009; Müller and Krämer 2010).
ACK1 has a large number of cancer-relevant downstream targets (Mahajan and Mahajan 2015; Maxson et al. 2013, 2016; Nonami et al. 2015). Recent evidence suggests that ACK1 also promotes the phosphorylation of signal transducer and activator of transcription-1 (STAT1) (Fujimoto et al. 2011), but it is unknown if the related molecule STAT3 is also controlled by ACK1. Given that STAT3 is an important regulator of tumorigenesis (Yu et al. 2014), it could be therapeutically relevant to address a putative ACK1-STAT3 signaling node, e.g., with HDACi and/or Dasatinib. As HDACi accelerate the proteasomal degradation of certain proteins (Krämer et al. 2013) and as ACK1 undergoes lysosomal and proteasomal degradation (Buchwald et al. 2010, 2013; Knauer et al. 2015), we hypothesized that such drugs attenuate ACK1 levels.
We addressed these questions. We analyzed whether HDACi modulated ACK1 and we additionally investigated whether combinations of HDACi and Dasatinib were effective against leukemic cells (Liu et al. 2010; Mahajan et al. 2014). We reveal that HDACi induce a z-VAD-FMK-sensitive destruction of ACK1, an ensuing reduction of p-STAT3, and that Dasatinib/HDACi combination schedules efficiently kill leukemic cells.
Materials and methods
Cell lines
K562 (human chronic myeloid leukemia, CML), HEL, and MV4-11 (human acute myeloid leukemia, AML) cells were purchased from the German Collection of Microorganisms and Cell Cultures (DSMZ, Braunschweig, Germany). The identity of the cell lines was verified by DNA fingerprint (Hennig et al. 2015). Cells were grown in RPMI-1640 medium supplemented with l-glutamine, 10 % fetal bovine serum and 1 % penicillin/streptomycin, at 37 °C in a 5 % CO2 atmosphere.
Drugs and chemicals
MS-275, LBH589, z-VAD-FMK, and Staurosporine were purchased from Selleckchem. Lactacystin and Hydroxyurea were obtained from Sigma-Aldrich. Dasatinib was provided by Santa Cruz Biotechnology.
Western Blot
Cells were seeded into 60-mm dishes at a density of 2 × 105 cells/mL. After 24 h, cells were exposed to drugs for 24–48 h. z-VAD-FMK was applied 1 h before HDACi treatment and Lactacystin 6 h before harvesting the cells. Cell pellets were lysed with 80–150 µL NETN lysis buffer containing protease and phosphatase inhibitors. Protein concentrations of these whole cell extracts were determined by Bradford assay. Cell lysis, SDS-PAGE, and Western blot are described (Buchwald et al. 2013). Fluorescence-coupled secondary antibodies (goat-anti-mouse/rabbit 800 CW, LI-COR) were used to detect protein expression with an infrared imager (Odyssey®, LI-COR). Densitometric evaluations were performed with Image Studio Lite 4.0. Antibodies for Western blot analyses were obtained from Abcam: α-Tubulin, ab176560; BD Pharmingen™: cleaved PARP1 (D214); Cell Signaling Technology: cleaved Caspase-3 (D175), #9661; Enzo Life Sciences: HSP90 (AC88), ADI-SPA-830-F; Merck Millipore: p-ACK1 (Y284), 09-142; acetyl-Histone H3, 06-599; Santa Cruz Biotechnology: ACK1, sc-28336; β-Actin, sc-47778; STAT3, sc-482; pY705-STAT3, sc-7993-R; Sigma-Aldrich: Ubiquitin, U5379.
Flow cytometry
Apoptosis was measured by cell cycle analysis of propidium iodide-stained cells. These were seeded on 12-well plates at a density of 2 × 105 cells/mL. After 24 h adaption, cells were stimulated with drugs for 24–48 h. Cells were transferred into flow cytometry tubes and centrifuged at 317×g for 5 min. The cell pellet was once washed with PBS. After another centrifugation step, cells were resuspended in 100 µL cold PBS. Subsequently, 1 mL ice cold ethanol (80 %) was added to the cell suspension while vortexing. Samples were fixed for at least 1 h at −20 °C. After the fixation step, cells were centrifuged at 751×g for 5 min. The cell pellet was resuspended in a mixture of 333 µL PBS and 1 µL RNase (stock solution 10 mg/mL) and incubated for 1 h at room temperature. Following steps were performed in the dark. Cellular DNA was stained by adding 164 µL propidium iodide (stock solution 50 µg/mL) to each sample. Samples were kept on ice and directly measured on a FACSCanto II flow cytometer (BD-Biosciences). Cell cycle distribution including subG1 fractions (dead cell population) was evaluated with the FACSDiva software 7.0 (BD-Biosciences).
Statistical analyses
We used one-way ANOVA (Bonferroni multiple comparisons test) and unpaired two-tailed t-test to assess the significance of control cells with stimulated cells. Analyses were performed with the GraphPad Prism 6 software.
Results
HDACi decrease ACK1 levels and the phosphorylation of STAT3
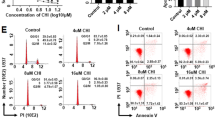
MS-275 is a class I HDAC-specific inhibitor that only blocks HDAC1, 2, 3, and LBH589 can inactivate all 11 zinc-dependent HDACs (Fig. 1a) (Bradner et al. 2010). We treated K562 CML cells with 5 µM MS-275 or 100 nM LBH589 for 48 h and analyzed lysates from these cells by Western blot. We chose these concentrations of HDACi because they induced roughly equal levels of histone hyperacetylation (Fig. 1b), which is a marker for HDAC inhibition (Göttlicher 2004). We found that both MS-275 and LBH589 significantly reduced the levels of ACK1. Moreover, we noted that LBH589 was more potent than MS-275 against ACK1 (Fig. 1b, c).
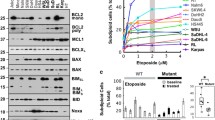
HDACi-reduced ACK1 levels in CML cells correlate with apoptosis. a Chemical structure of HDACi and their activity against HDACs. b K562 cells were treated with 5 µM MS-275, 100 nM LBH589 and/or 10 µM Lactacystin for 48 h. Lysates were analyzed by Western Blot for ACK1, pY705-STAT3, STAT3, acetyl-Histone H3 (ac-H3) and poly-Ubiquitin; β-Actin, loading control. c Densitometric evaluation of ACK1 band intensity normalized to β-Actin; n = 2 ± SD; one-way ANOVA (Bonferroni’s multiple comparisons test); **P ≤ 0.01, ****P ≤ 0.0001. d K562 cells were treated with HDACi as indicated for 48 h; Ctrl, untreated. PI-stained cells were subjected to flow cytometry. Shown is a representative cell cycle distribution. e Quantification of cell cycle distribution of K562 cells treated as stated; n = 3 ± SD. f Extracts of K562 cells were analyzed for cleaved PARP1 and cleaved Caspase-3; α-Tubulin, loading control; cl., cleaved
As ACK1 promotes the phosphorylation of STAT1 (Fujimoto et al. 2011), we suspected that ACK1 also controls STAT3. Figure 1b shows that the attenuation of ACK1 correlates with decreased phosphorylation of STAT3 at Y705. Total STAT3 levels though remained constant (Fig. 1b).
Since HDACi can promote proteasomal degradation of TKs (Buchwald et al. 2010; Knauer et al. 2015), we hypothesized that HDACi accelerate a proteasome-dependent turnover of ACK1. Consequently, we applied HDACi with the highly selective proteasomal inhibitor Lactacystin (Corey and Li 1999). While Lactacystin potently induced the accumulation of poly-ubiquitinylated protein species, it failed to rescue ACK1 in HDACi-treated K562 cells (Fig. 1b, c). Hence, HDACi unlikely accelerate the proteasomal degradation of ACK1 in leukemic cells.
These data suggest that HDACi induce a decline of ACK1 and p-STAT3.
Decreased expression of ACK1 correlates with apoptosis
When we investigated the cell cycle profiles of K562 cells that had been treated with MS-275 and LBH589 for 48 h, we found that MS-275 mainly stalled cells in the G1 phase and that LBH589 depleted cells in G1 (Fig. 1d). About 10 % of cells had fragmented genomic DNA in response to MS-275 (subG1 cells with DNA content <2 N) and LBH589 increased the subG1 population up to 35 % (Fig. 1e).
Immunoblotting for the pro-apoptotic conversion of Caspase-3 and its target PARP1 in MS-275- and LBH589-treated K562 cells demonstrated the occurrence of both processes (Fig. 1f). At first glance, these results for MS-275 contradict data shown in Fig. 1e. However, it appears logical that the manifestation of cell death within the cell population by flow cytometry lags behind the activation of the pro-apoptotic caspase cascade.
To corroborate these results, we analyzed leukemic cells that are more sensitive to MS-275 than K562 cells. In response to 5 µM MS-275, 32 % of MV4-11 AML cells and 25 % of HEL AML cells showed DNA fragmentation (Fig. 2a–c) and cleaved forms of Caspase-3 and PARP1 (Fig. 2b–d). LBH589 induced similar effects in MV4-11 cells (30 % dead cells; Fig. 2a). Compared to K562 cells (about 10 % of cell death) (Fig. 1e), ACK1 protein levels dropped more strongly in HEL and MV4-11 cells when they were treated with MS-275 (Fig. 2b–d). These data suggest that cytotoxic effects, and not the variable spectrum of HDACs that are blocked by MS-275 and LBH589 (Fig. 1a), are responsible for the reduction of ACK1 in HDACi-treated cells.
HDACi-reduced ACK1 levels in AML cells correlate with apoptosis. a MV4-11 cells were treated with 5 µM MS-275 or 100 nM LBH589 for 24 h. Cell death was measured by cell cycle analysis after propidium iodide staining. The subG1 population represents the apoptotic fraction; n = 3 ± SD; one-way ANOVA (Bonferroni’s multiple comparisons test); ****P ≤ 0.0001. b MV4-11 cell lysates were analyzed by Western Blot for ACK1 and cleavage of PARP1/Caspase-3. HDACi stimulation evokes the advent of a cleavage product of ACK1 (100 kDa); α-Tubulin, loading control; cl., cleaved. c SubG1 population of HEL cells treated with 2-5 µM MS-275 or 48 h; n = 3 ± SD; one-way ANOVA (Bonferroni’s multiple comparisons test); **P ≤ 0.01, ****P ≤ 0.0001. d Lysates of HEL cells were analyzed for ACK1 and cleaved Caspase-3. The ACK1 cleavage product can be observed in HDACi-treated extracts; α-Tubulin, loading control; cl., cleaved. e SubG1 population of HEL cells treated with 1 mM HU for 24 h; n = 3 ± SD; unpaired two-tailed t-test; **P = 0.0058. f Extracts of HEL cells were analyzed for ACK1 and its cleavage product; α-Tubulin, loading control
Due to these results, we aimed to delineate further if HDAC inhibition or cytotoxic stress was a requirement to regulate ACK1 negatively. We treated HEL cells with HU, a ribonucleotide reductase inhibitor, which causes replicative stress by a depletion of dNTPs (Stauber et al. 2012). This cell system was chosen based on preliminary experiments that showed its high sensitivity to HU. We noticed that HU induced a subG1 fraction of 32 % (Fig. 2e) and decreased ACK1 levels (Fig. 2f).
Hence, a degradation of ACK1 correlates with the induction of cell death and therefore appears druggable with various agents.
Caspase activation reduces ACK1 protein levels
A common feature of drugs that evoke a degradation of ACK1 is the induction of caspases, which are the main executers of apoptosis (Mukhopadhyay et al. 2014). To analyze whether caspase activity is also crucial for the HDACi-induced demise in ACK1, we blocked these enzymes with z-VAD-FMK. This cell-permeable caspase inhibitor restricted the cleavage of Caspase-3 and PARP1 in LBH589-treated K562 cells (Fig. 3b). Immunoblot analyses further showed that z-VAD-FMK reduced the HDACi-evoked decrease in ACK1 and phosphorylated STAT3 (Fig. 3a).
Pro-apoptotic caspase activation reduces ACK1 levels. a K562 cells were treated with 100 nM LBH589 and/or 50 µM z-VAD-FMK for 48 h. Lysates were analyzed for ACK1, pY705-STAT3, and STAT3. By adding z-VAD-FMK, ACK1 is partially rescued in LBH589-treated cells. b Cleaved PARP1 and cleaved Caspase-3 were also detected by Western Blot. α-Tubulin, loading control; cl., cleaved. c Chemical structure of Staurosporine. d Flow cytometry profiles of K562 cells treated with 1–10 µM STS for 24–48 h; Ctrl, untreated. e SubG1 population of K562 cells treated as indicated; n = 3 ± SD; one-way ANOVA (Bonferroni’s multiple comparisons test); *P ≤ 0.05, **P ≤ 0.01, ***P ≤ 0.001. f Extracts of K562 cells were analyzed for ACK1 levels; HSP90, loading control
Next, we used the bacterial kinase inhibitor STS, which is a potent inducer of caspases (Fig. 3c) (Omura et al. 1977). STS causes a significant time- and dose-dependent increase in the subG1 population of K562 cells (Fig. 3d, e). This cytotoxicity tied in with significantly decreased ACK1 levels (Fig. 3f).
These results show that caspase activation leads to a reduction of ACK1.
Dasatinib inhibits the phosphorylation of ACK1 and STAT3 and blocks cell cycle progression
HDACi reduce ACK1 and p-STAT3 (Fig. 1b). To assess the biological relevance of this finding, we treated K562 cells with Dasatinib (Fig. 4a), a clinically relevant inhibitor of ACK1 (Liu et al. 2010; Mahajan et al. 2014; Shah et al. 2016). While 5 nM Dasatinib was sufficient to halt K562 cells in the G1 phase, even 100 nM Dasatinib did not induce cell death after 24 h (Fig. 4b, c).
Dasatinib blocks ACK1 phosphorylation and stalls cells in the G1 phase. a Chemical structure of Dasatinib. b Flow cytometry profiles of K562 cells treated with 5–100 nM Dasatinib for 24 h; Ctrl, untreated. c Distribution of the cell cycle phases of K562 cells treated as stated; n = 3 ± SD. d Lysates of K562 cells were analyzed by Western Blot for ACK1, pY284-ACK1, pY705-STAT3, and STAT3; β-Actin, loading control
Analysis of ACK1 and STAT3 signaling by Western blot revealed that already 5 nM Dasatinib abrogated the activating phosphorylation of ACK1 at Y284 and the phosphorylation of STAT3 at Y705 (Fig. 4d). Such data suggest that an inhibition of ACK1 decreases the phosphorylation of STAT3 irrespective of cell death (Fig. 1b). Consistent with the finding that pro-apoptotic processes are involved in the reduction of ACK1 (Figs. 2, 3), total ACK1 levels were only marginally reduced and STAT3 remained stable in the presence of 100 nM Dasatinib (Fig. 4d).
We conclude that Dasatinib blocks the phosphorylation of STAT3 through the inhibition of the catalytic activity of ACK1 and irrespective of cytotoxicity.
Dasatinib and HDACi combine favorably against K562 cells
Having found that HDACi and Dasatinib inactivated ACK1 either by degradation or by the inhibition of its phosphorylation, we speculated that combinations of these drugs would generate beneficial antileukemic effects.
We exposed K562 cells to 1.5–5 µM MS-275, 30–100 nM LBH589, and a fixed dose of Dasatinib. Western blot analyses showed that Dasatinib abrogated ACK1 phosphorylation and slightly increased the HDACi-induced attenuation of ACK1 (Fig. 5a).
Favorable effect of Dasatinib and MS-275 against CML cells. a K562 cells were treated with 1.5–5 µM MS-275, 30–100 nM LBH589, and/or 50 nM Dasatinib for 24 h. Western Blot analyses show levels of ACK1 and pY284-ACK1; β-Actin, loading control. b Flow cytometry profiles of K562 cells treated as indicated for 24–48 h. c SubG1 population of K562 cells treated as stated; n = 3 ± SD; one-way ANOVA (Bonferroni’s multiple comparisons test); *P ≤ 0.05, ***P ≤ 0.001, ****P ≤ 0.0001
Flow cytometry disclosed that the combined application of Dasatinib with 1.5–5 µM MS-275 and 30 nM LBH589 increased the portion of subG1 cells after 24–48 h (Fig. 5b, c). The already very strong pro-apoptotic effect of 100 nM LBH589 was not augmented further in this assay (Fig. 5b, c).
These data demonstrate that HDACi/Dasatinib combinations can produce additive to synergistic antileukemic effects, particularly at lower doses of HDACi.
Discussion
HDACi, HU, and STS attenuate the expression of ACK1 in AML and CML cells. Furthermore, HDACi combine favorably with Dasatinib against notoriously chemoresistant K562 cells (BCR/ABL-positive/p53-null) (Boschelli et al. 2010). We additionally demonstrate that the caspase inhibitor z-VAD-FMK partially rescues ACK1 in HDACi-treated cells. Likewise, the extent of caspase activation by HDACi, HU, and STS in various cell types correlates with the processing of ACK1 and with the occurrence of a smaller ACK1 fragment; such fragments are typical signs of proteolytic cleavage. Inspection of the ACK1 sequence with ExPASy unfortunately gave no hints for typical caspase cleavage sites. This discrepancy might be explained by uncommon cleavage site(s) or by alternative protease(s) acting downstream of caspases. Examples for such enzymes may include mitochondrial proteases (Mukhopadhyay et al. 2014), and HDACi-activated z-VAD-FMK-sensitive cathepsins (Cheriyath et al. 2011; Rozman-Pungercar et al. 2003). Further studies are underway to answer which of the plethora of protease(s) cleave(s) ACK1 in response to HDACi.
SIAH ubiquitin ligases accelerate the proteasomal turnover of ACK1 (Buchwald et al. 2013), but we found no evidence that HDACi accelerate this process. This finding does rather not result from strong pro-apoptotic effects of Lactacystin/HDACi combinations, as these are hardly more cytotoxic than HDACi for K562 cells (data not shown). While others also found that one should carefully examine whether HDACi propel an accelerated proteasomal degradation of oncoproteins (Newbold et al. 2013), we cannot exclude that HDACi promote the proteasomal turnover of ACK1 in other cell systems. Another possibility, a loss of ACK1 mRNA expression in response to HDACi appears unlikely, as HDACi increase ACK1 mRNA levels in leukemic cells (Starkova et al. 2007).
ACK1 phosphorylates STAT1 in hepatocellular carcinoma cells (Fujimoto et al. 2011). We demonstrate that an inactivation of ACK1 by HDACi and Dasatinib attenuates the phosphorylation of STAT3, which shares high homology with STAT1 (Wieczorek et al. 2012). In contrast to its phosphorylation, STAT3 levels are stable in response to such treatments. Consistent with this observation, HDACi do not reduce STAT3 in HDACi-treated, apoptotic acute promyelocytic leukemia cells (Licht et al. 2014). The option that HDACi reduce STAT3 phosphorylation through increased acetylation is not likely, since most studies noted that acetylation regulates the phosphorylation of STAT3 positively (Wieczorek et al. 2012). Whether or not the five other members of the STAT family are targets of ACK1, and if this has an impact on cancer cells, remains unclear.
STAT3 is an important regulator of tumor growth and development (Yu et al. 2014) and STAT3 can promote the resistance of primary and permanent CML cells to the BCR/ABL-inhibitor Imatinib (Wang et al. 2016). Therefore, the inactivation of p-ACK1 and p-STAT3 by Dasatinib/HDACi combinations might be therapeutically useful. The finding that Dasatinib combines favorably with LBH589 and PXD101 against thyroid cancer cells (Chan et al. 2013) supports to test Dasatinib/HDACi regimen further. As ACK1 is an important factor for the migration and metastasis of cells (Ahmad et al. 2012; Mahajan and Mahajan 2015), the HDACi-induced attenuation of ACK1 might as well contribute to the known anti-metastatic effect of HDACi, see e.g., (Göttlicher et al. 2001). It is also tempting to speculate that the suppression of androgen receptor (AR) signaling by HDACi (Stempin et al. 2013; Trtkova et al. 2010) involves their negative effect on ACK1, which activates AR by direct phosphorylation (Karaca et al. 2015; Liu et al. 2010; Mahajan et al. 2012). Therefore, we expect that the data presented here have significant relevance for additional systems.
References
Afifi S, Michael A, Azimi M, Rodriguez M, Lendvai N, Landgren O (2015) Role of histone deacetylase inhibitors in relapsed refractory multiple myeloma: a focus on vorinostat and panobinostat. Pharmacotherapy 35:1173–1188. doi:10.1002/phar.1671
Ahmad M et al (2012) Understanding histone deacetylases in the cancer development and treatment: an epigenetic perspective of cancer chemotherapy. DNA Cell Biol 31(Suppl 1):S62–S71. doi:10.1089/dna.2011.1575
Boschelli F, Arndt K, Gambacorti-Passerini C (2010) Bosutinib: a review of preclinical studies in chronic myelogenous leukaemia. Eur J Cancer 46:1781–1789. doi:10.1016/j.ejca.2010.02.032
Bradner JE et al (2010) Chemical genetic strategy identifies histone deacetylase 1 (HDAC1) and HDAC2 as therapeutic targets in sickle cell disease. Proc Natl Acad Sci USA 107:12617–12622. doi:10.1073/pnas.1006774107
Buchwald M, Pietschmann K, Müller JP, Böhmer FD, Heinzel T, Krämer OH (2010) Ubiquitin conjugase UBCH8 targets active FMS-like tyrosine kinase 3 for proteasomal degradation. Leukemia 24:1412–1421. doi:10.1038/leu.2010.114
Buchwald M, Pietschmann K, Brand P, Gunther A, Mahajan NP, Heinzel T, Krämer OH (2013) SIAH ubiquitin ligases target the nonreceptor tyrosine kinase ACK1 for ubiquitinylation and proteasomal degradation. Oncogene 32:4913–4920. doi:10.1038/onc.2012.515
Chan D et al (2013) Belinostat and panobinostat (HDACI): in vitro and in vivo studies in thyroid cancer. J Cancer Res Clin Oncol 139:1507–1514. doi:10.1007/s00432-013-1465-6
Cheriyath V, Kuhns MA, Kalaycio ME, Borden EC (2011) Potentiation of apoptosis by histone deacetylase inhibitors and doxorubicin combination: cytoplasmic cathepsin B as a mediator of apoptosis in multiple myeloma. Br J Cancer 104:957–967. doi:10.1038/bjc.2011.42
Corey EJ, Li WD (1999) Total synthesis and biological activity of lactacystin, omuralide and analogs. Chem Pharm Bull 47:1–10
Fujimoto Y et al (2011) A single nucleotide polymorphism in activated Cdc42 associated tyrosine kinase 1 influences the interferon therapy in hepatitis C patients. J Hepatol 54:629–639. doi:10.1016/j.jhep.2010.07.021
Göttlicher M (2004) Valproic acid: an old drug newly discovered as inhibitor of histone deacetylases. Ann Hematol 83(Suppl 1):S91–S92. doi:10.1007/s00277-004-0850-2
Göttlicher M et al (2001) Valproic acid defines a novel class of HDAC inhibitors inducing differentiation of transformed cells. EMBO J 20:6969–6978
Graham JS, Kaye SB, Brown R (2009) The promises and pitfalls of epigenetic therapies in solid tumours. Eur J Cancer 45:1129–1136. doi:10.1016/j.ejca.2009.01.003
Hennig D et al (2015) Antagonism between granulocytic maturation and deacetylase inhibitor-induced apoptosis in acute promyelocytic leukaemia cells. Br J Cancer 112:329–337. doi:10.1038/bjc.2014.589
Karaca M, Liu Y, Zhang Z, De Silva D, Parker JS, Earp HS, Whang YE (2015) Mutation of androgen receptor N-terminal phosphorylation site Tyr-267 leads to inhibition of nuclear translocation and DNA binding. PLoS ONE 10:e0126270. doi:10.1371/journal.pone.0126270
Knauer SK, Mahendrarajah N, Roos WP, Krämer OH (2015) The inducible E3 ubiquitin ligases SIAH1 and SIAH2 perform critical roles in breast and prostate cancers. Cytokine Growth Factor Rev 26:405–413. doi:10.1016/j.cytogfr.2015.04.002
Krämer OH, Stauber RH, Bug G, Hartkamp J, Knauer SK (2013) SIAH proteins: critical roles in leukemogenesis. Leukemia 27:792–802. doi:10.1038/leu.2012.284
Licht V et al (2014) Caspase-3 and caspase-6 cleave STAT1 in leukemic cells. Oncotarget 5:2305–2317
Liu Y, Karaca M, Zhang Z, Gioeli D, Earp HS, Whang YE (2010) Dasatinib inhibits site-specific tyrosine phosphorylation of androgen receptor by Ack1 and Src kinases. Oncogene 29:3208–3216. doi:10.1038/onc.2010.103
Ma N, Luo Y, Wang Y, Liao C, Ye WC, Jiang S (2016) Selective histone deacetylase inhibitors with anticancer activity. Curr Top Med Chem 16:415–426
Mace ML, Dahl J, Jabbour EJ (2015) Which tyrosine-kinase inhibitor to use first in chronic phase chronic myelogenous leukemia? Expert Opin Pharmacother 16:999–1007. doi:10.1517/14656566.2015.1031107
Mahajan K, Mahajan NP (2015) ACK1/TNK2 tyrosine kinase: molecular signaling and evolving role in cancers. Oncogene 34:4162–4167. doi:10.1038/onc.2014.350
Mahajan K et al (2012) Ack1-mediated androgen receptor phosphorylation modulates radiation resistance in castration-resistant prostate cancer. J Biol Chem 287:22112–22122. doi:10.1074/jbc.M112.357384
Mahajan K, Lawrence HR, Lawrence NJ, Mahajan NP (2014) ACK1 tyrosine kinase interacts with histone demethylase KDM3A to regulate the mammary tumor oncogene HOXA1. J Biol Chem 289:28179–28191. doi:10.1074/jbc.M114.584425
Maxson JE et al (2013) Oncogenic CSF3R mutations in chronic neutrophilic leukemia and atypical CML. N Engl J Med 368:1781–1790. doi:10.1056/NEJMoa1214514
Maxson JE et al (2016) Identification and characterization of tyrosine kinase nonreceptor 2 mutations in leukemia through integration of kinase inhibitor screening and genomic analysis. Cancer Res 76:127–138. doi:10.1158/0008-5472.CAN-15-0817
Mukhopadhyay S, Panda PK, Sinha N, Das DN, Bhutia SK (2014) Autophagy and apoptosis: Where do they meet? Apoptosis Int J Program Cell Death 19:555–566. doi:10.1007/s10495-014-0967-2
Müller S, Krämer OH (2010) Inhibitors of HDACs—Effective drugs against cancer? Curr Cancer Drug Targets 10:210–228
Newbold A et al (2013) Molecular and biologic analysis of histone deacetylase inhibitors with diverse specificities. Mol Cancer Ther 12:2709–2721. doi:10.1158/1535-7163.MCT-13-0626
Nonami A et al (2015) Identification of novel therapeutic targets in acute leukemias with NRAS mutations using a pharmacologic approach. Blood 125:3133–3143. doi:10.1182/blood-2014-12-615906
Omura S, Iwai Y, Hirano A, Nakagawa A, Awaya J, Tsuchya H, Takahashi Y, Masuma R (1977) A new alkaloid AM-2282 OF Streptomyces origin. Taxonomy, fermentation, isolation and preliminary characterization. J Antibiot (Tokyo) 30(4):275–282
Rozman-Pungercar J et al (2003) Inhibition of papain-like cysteine proteases and legumain by caspase-specific inhibitors: when reaction mechanism is more important than specificity. Cell Death Differ 10:881–888. doi:10.1038/sj.cdd.4401247
Seto E, Yoshida M (2014) Erasers of histone acetylation: the histone deacetylase enzymes. Cold Spring Harbor Perspect Biol 6:a018713. doi:10.1101/cshperspect.a018713
Shah NP et al (2016) Dasatinib in imatinib-resistant or -intolerant chronic-phase, chronic myeloid leukemia patients: 7-year follow-up of study CA180-034. Am J Hematol. doi:10.1002/ajh.24423
Starkova J et al (2007) The identification of (ETV6)/RUNX1-regulated genes in lymphopoiesis using histone deacetylase inhibitors in ETV6/RUNX1-positive lymphoid leukemic cells. Clin Cancer Res Off J Am Assoc Cancer Res 13:1726–1735. doi:10.1158/1078-0432.CCR-06-2569
Stauber RH et al (2012) A combination of a ribonucleotide reductase inhibitor and histone deacetylase inhibitors downregulates EGFR and triggers BIM-dependent apoptosis in head and neck cancer. Oncotarget 3:31–43
Stempin S, Andres S, Scheer MB, Rode A, Nau H, Seidel A, Lampen A (2013) Valproic acid and its derivatives enhanced estrogenic activity but not androgenic activity in a structure dependent manner. Reprod Toxicol 42:49–57. doi:10.1016/j.reprotox.2013.07.019
Trtkova K, Paskova L, Matijescukova N, Kolar Z (2010) Formation of AR-SMRT binding in prostate cancer cells treated with natural histone deacetylase inhibitor. Cancer Biomark Sect A Dis Markers 7:79–90. doi:10.3233/CBM-2010-0150
Wang H et al (2016) Overexpression of RPS27a contributes to enhanced chemoresistance of CML cells to imatinib by the transactivated STAT3. Oncotarget. doi:10.18632/oncotarget.7888
Wieczorek M, Ginter T, Brand P, Heinzel T, Krämer OH (2012) Acetylation modulates the STAT signaling code. Cytokine Growth Factor Rev 23:293–305. doi:10.1016/j.cytogfr.2012.06.005
Yu H, Lee H, Herrmann A, Buettner R, Jove R (2014) Revisiting STAT3 signalling in cancer: new and unexpected biological functions. Nat Rev Cancer 14:736–746. doi:10.1038/nrc3818
Acknowledgments
We thank Christina Brachetti for excellent technical support. This study was mainly supported by grants to OHK from the Wilhelm Sander-Stiftung (#2010.078) and additionally by grants to OHK from the Deutsche Krebshilfe (#110909/#110125), the Deutsche Forschungsgemeinschaft (#KR2291/4-1/5-1), and intramural funding from the NMFZ Mainz and the University Medical Center Mainz.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Mahendrarajah, N., Paulus, R. & Krämer, O.H. Histone deacetylase inhibitors induce proteolysis of activated CDC42-associated kinase-1 in leukemic cells. J Cancer Res Clin Oncol 142, 2263–2273 (2016). https://doi.org/10.1007/s00432-016-2229-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-016-2229-x