Abstract
Elevated von Willebrand factor (vWF):Antigen plasma levels have been observed in conjunction with cardiovascular diseases or vasculitis. The association of Kawasaki disease, a vascular inflammatory disease and vWF:Antigen, vWF:Collagen binding activity, and vWF multimers is unknown. We therefore investigated vWF parameters in 28 patients with acute Kawasaki disease in association with disease activity and coronary artery lesions. VWF:Antigen and vWF:Collagen binding activity were assessed via enzyme-linked immunoassay. The ratio of both (vWF:Collagen binding activity and VWF:Antigen) was calculated and vWF multimeric structure analysis performed. We analyzed the association between vWF parameters and our clinical data focusing on coronary artery outcome. VWF:Antigen and vWF:Collagen binding activity levels were significantly higher in the acute than in the disease’s convalescence phase, and correlated positively with CRP levels. Neither variable was associated with coronary artery lesions. The vWF:Collagen binding activity/vWF:Antigen ratio, however, was significantly decreased in patients with a coronary artery lesion (z-score > 2; N = 10; mean ratio 0.96 vs. 0.64; p = 0.031) and even more so in those with a coronary artery aneurysm (z-score > 2.5; N = 8; mean ratio 0.94 vs. 0.55; p = 0.02). In a sub-analysis, those patients with a very low ratio in the acute phase presented a persistent coronary artery aneurysm at their 1-year follow-up.
Conclusion: This study suggests that comprehensive analysis of vWF parameters may help to both monitor KD inflammation and facilitate the identification of those patients carrying an increased risk for coronary artery lesion.
What is Known: • Von Willebrand factor (VWF)-parameters represent surrogate markers for vascular inflammation. • Kawasaki disease is a generalized vasculitis in children, which can be complicated by coronary artery lesions. | |
What is New: • In those Kawasaki disease patients with coronary artery lesions, the vWF:CB/vWF:Ag ratio was significantly decreased. • VWF parameters may help to identify patients at risk for coronary artery lesions. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Kawasaki disease (KD) entails generalized vasculitis in children who clinically present with fever, cervical lymphadenopathy, and polymorphous exanthema: red eyes (conjunctivitis), lips, palms, and feet soles. Because of its impact on the coronary arteries, KD is characterized by substantial morbidity and mortality, and is thus the most common cause for acquired heart disease in the USA and Japan today [1, 22]. Its overall occurrence varies substantially throughout the world and among different ethnicities. KD’s highest reported annual incidence is in Japan [239 in 100,000] [16]. Its incidence in Germany is much lower [7.2 in 100,000] [9]. Although its etiology is unknown, different signaling pathways inducing inflammation, e.g., interleukin (IL)-1, IL-6, and tumor necrosis factor α (TNFα) are known to be involved in its pathogenesis [5, 15, 20]. This immune activation during KD’s acute phase is associated with endothelial cell damage observed in small-to-medium-sized arteries [12]. The endothelium activation evident in cardiovascular diseases and vasculitis is associated with an increased von Willebrand factor (vWF) release [2, 11]. vWF, a large multimeric glycoprotein essential for primary hemostasis, is stored in the vascular endothelium and platelets.. In vitro analyses indicate that some inflammatory cytokines may stimulate this release, and others may inhibit the cleavage of ultra-large vWF multimers suggesting a potential linkage between inflammation and thrombosis [2]. KD is an acute vascular inflammatory disease involving worsening thrombocytosis during its course [15].
We assessed the impact of Kawasaki disease on circulating vWF:Antigen (vWF:Ag) as well as on vWF activity measured as vWF:Collagen binding activity (vWF:CB), the ratio of vWF:CB and vWF:Ag, and structural changes in vWF multimers as a surrogate marker for disease activity and coronary artery lesion.
Material and methods
Patients
Kawasaki disease patients were recruited from a nation-wide active surveillance study through the hospital-based German Pediatric Surveillance Unit (ESPED), including 5 patients from our institution (the Department of Pediatric Cardiology, University of Freiburg). These patients underwent clinical follow-up for one year and serial vWF-parameter analyses. As previously described, reporting physicians were sent a standardized questionnaire for clinical details [9]. As part of this study, reporting physicians were also invited to send citrated blood for vWF analyses. Study approval was provided by the Ethics Committee of the University of Freiburg, in accordance with the Declaration of Helsinki ethical standards. Due to data protection regulations, only those patients were included to this study whose parents had provided written informed consent.
Definitions
Kawasaki disease
Complete cases were defined as those with persistent fever for ≥ 5 days (or fever that resolved in < 5 days in response to IVIG treatment) and ≥ 4 of the principal clinical criteria such as (1) changes in extremities; [1] polymorphous exanthema; [16] bilateral conjunctival inflammation without exudate; [9] changes in the lips and oral cavity; and [15] cervical lymphadenopathy. Incomplete cases included those with fever presenting fewer than four clinical features but entailing the detection of a coronary artery lesion. The z-score equation proposed by Dallaire et al. [4] was used. This model was reported in a Caucasian pediatric population (Canada) and provides normative data for the left circumflex branch. According to the calculated z-score, we subdivided coronary artery lesions into coronary artery aneurysm (z-score > 2.5) and coronary artery ectasia (z-score between > 2 ≤ 2.5). Refractory KD cases were defined as those patients with persistent fever for longer than 36 h after IVIG treatment who therefore underwent a second course of intravenous immunoglobulin (IVIG).
Laboratory methods
Citrated blood was sent via 24-h shipping from the referring hospital to the University of Freiburg at room temperature. Plasma was prepared from citrated blood via centrifugation and stored at − 80 °C for further analyses.
VWF:Ag and vWF:CB were determined according to standard protocols (Siemens Healthcare Diagnostics, Eschborn, Germany): Collagen type I (Nycomed Pharma, Unterschleissheim, Germany) was immobilized on a microtiter plate and collagen binding activity (vWF:CB) in plasma was determined photometrically by ELISA (Enzyme-linked immunoassay) technique.
Ratios of vWF:CB to vWF:Ag (vWF:CB/vWF:Ag) were calculated. They reflect the biological activity of the available vWF with regard to the binding to collagen. VWF:CB measures the binding of vWF to collagen and therefore, this assay detects preferentially vWF’s high molecular weight multimers.
In addition, we analyzed the vWF structure using multimeric structure analysis: vWF multimers were separated on SDS-agarose low resolution gels (1.0% agarose) and high resolution gels (2.2% agarose) and blotted on a PVDF (polyvinylidene difluoride) membrane. vWF was detected using appropriate primary and secondary antibodies (DAKO, Hamburg, Germany) and chemiluminescence.
Statistical analysis
The descriptive statistics are presented as mean and standard deviation (SD). A p value of 0.05 was considered significant throughout our analyses. The impact of the patients’ sex, age, and day of illness when blood was collected on vWF parameters was assessed by linear models. The Pearson correlation coefficient was used to evaluate the correlation between vWF parameters and standard inflammatory markers. To test whether vWF parameters differ between KD patients in two different groups, Welch’s t test (vWF:Ag, vWF:CB, and vWF:CB/vWF:Ag ratio) and Fisher’s exact test (multimer analysis) were used.
Results
After excluding 10 citrated blood samples from 10 patients (see Fig. 1), 38 blood samples from 28 KD patients (21 male) remained for further analyses. Patient baseline characteristics and laboratory values are provided in Table 1. The patients’ ages ranged from 2 months to 15 years. Ten children presented with a coronary artery lesion during the acute phase of disease. Eight children were classified as having a coronary artery aneurysm (z-score range 2.59–16) and two as coronary artery ectasia.
Flow chart of the blood samples. A single asterisk denotes citrated blood was clotted; reliable analysis was not possible. Double asterisks denote loss of follow-up: We received a pseudonymized blood sample, but neither the standardized questionnaire providing clinical details to verify the KD diagnosis nor the parents’ informed consent. Triple asterisks denote withdrawn: Kawasaki disease was ruled out after a different diagnosis was made after we had received this blood sample
Age and sex revealed no influence on any of the vWF parameters (data not shown). Blood samples for vWF-parameter analysis were taken from 23 patients during the illness’ acute phase (i.e., within 21 days after the first day of fever) and from 5 patients in the convalescence phase (28–58 days after the first day of fever). No association between the time-point of blood withdrawal and vWF parameters was detected in the disease’s acute phase (see Fig. 2). However, comparing vWF-values from KD’s acute phase with those from its convalescence phase, we observed mean vWF:Ag levels (2.03 vs. 1.06; p = 0.0082) and mean vWF:CB levels (1.75 vs. 1.09; p = 0.0198) that were significantly higher in the disease’s acute phase. IVIG treatment appeared to have no significant influence on vWF parameters (data not shown).
Von Willebrand factor parameters and time-points of blood sampling (acute phase of disease). Linear regression analysis ( y = β0 + β1x + ϵ) of von Willebrand factor:antigen, von Willebrand factor:collagen binding activity, and von Willebrand factor:collagen binding activity/von Willebrand factor:antigen ratio in association with the time-point of day of illness when blood samples were drawn. No significant association was found. Since multimers were pathologic in only 5 cases, no meaningful statistical statement is possible
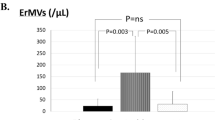
Concerning the coronary-artery-lesion outcome, the absolute vWF:Ag and vWF:CB levels from the disease’s acute phase revealed no significant differences either between patients with or without a coronary artery lesion or with or without a coronary artery aneurysm (see Table 2 and Fig. 3a, b). The vWF:CB/vWF:Ag ratio, however, was significantly lower in those patients with coronary artery involvement (coronary artery lesion: mean 0.96 vs. 0.64; p = 0.03; coronary artery aneurysm: mean ratio 0.94 vs. 0.55; p = 0.02).
a Von Willebrand factor parameters in Kawasaki disease patients with and without coronary artery lesion (N = 10). Von Willebrand factor:collagen binding activity/von Willebrand factor:antigen was significantly lower in all patients presenting coronary artery lesion (mean 0.96 vs. 0.64; p = 0.03). b Von willebrand factor parameters in Kawasaki disease patients with and without coronary artery aneurysm (N = 8) in the acute phase of the disease. Von Willebrand factor:collagen binding activity/von Willebrand factor:antigen ratio was significantly lower in patients presenting coronary artery aneurysm (mean 0.94 vs. 0.55; p = 0.02)
Serial vWF analyses were possible in the 5 patients from the University of Freiburg. Three had a coronary artery aneurysm in the acute disease phase, which persisted in two patients until their follow-up at one year. Although no statistical analysis is possible, in two patients with persistent coronary artery aneurysm, not only were their vWF:CB/vWF:Ag ratios the lowest of all investigated patients during the acute phase but their multimeric structure analyses were also pathological, i.e., high molecular weight multimers were absent.
The association between VWF parameters collected during the disease’s acute stage and routine laboratory values were analyzed according to the Pearson coefficient. CRP levels correlated positively with vWF:Ag and vWF:CB (0.30 and 0.36, respectively), a higher platelet count correlated positively with a higher vWF:Ag (0.36), and a lower vWF:CB/vWF:Ag ratio correlated with a higher leucocyte count (− 0.38).
Discussion
The aforementioned results constitute a comprehensive analysis of vWF parameters in children with Kawasaki disease and provide evidence of their impact on the clinical course with particular focus on coronary artery lesions. vWF:Ag and vWF:CB were elevated in the acute phase of the disease, and revealed a moderate correlation with routine inflammatory markers. Although neither vWF:Ag nor vWF:CB alone were associated with coronary artery lesions, the vWF:CB/vWF:Ag ratio was significantly decreased in KD patients with coronary artery lesions.
The role of vWF in generalized inflammatory states and during vascular inflammation has been investigated [19]. Few studies that measured only absolute vWF:Ag levels have also addressed the impact of vWF-Antigen on Kawasaki disease. In summary [8, 14, 17] and in line with our results, vWF:Ag levels were elevated in the disease’s acute phase, supporting the hypothesis that increased vWF:Ag values reflect an acute phase reaction. However, the vWF:Ag value does not seem to be specific either for Kawasaki disease itself or coronary artery lesions. In this study, we identified the vWF:CB/vWF:Ag ratio as being significantly decreased in KD patients with coronary artery lesion. Furthermore, our follow-up analysis in a small subset of patients suggests that those with a very low vWF:CB/vWF:Ag ratio during the acute phase of the disease exhibited persisting coronary artery aneurysms one year after the start of the disease. This finding may provide a possible pathogenetic explanation and may be of diagnostic value.
Different mediators of inflammation known to be pivotal in the inflammatory reaction of KD, e.g., TNFα, stimulate the release of vWF:Ag, especially ultra-large vWF multimers (UL-VWF) [2]. UL-vWF strings support the interaction between platelets and vascular endothelium. This could be a link explanatory to antiplatelet medication in Kawasaki disease, a field still requiring clarification [21]. UL-vWF strings also support leucocyte adhesion and extravasation into the inflamed vessel [18]. Bernard et al. showed that under the high-shear blood flow condition like that in our arteries, leucocytes tethered and rolled not directly on the endothelial layer but on an ideal matrix of platelets adhering to UL-vWF on activated endothelial cells [3]. This mechanism may support leucocyte accumulation in the inflamed vascular lesion such as in the coronary artery lesions in Kawasaki disease. The lower vWF:CB/vWF:Ag ratio in Kawasaki disease patients with coronary artery aneurysm could be attributable to increased attachment of activated vWF to inflamed coronary arteries’ endothelium and subsequently enhanced cleaving of the vWF, leading to the loss of high molecular weight multimers.
These findings imply that patients with a lower vWF:CBA/vWF:Ag ratio may have a higher risk to develop coronary artery aneurysm, suggesting an intensified follow-up and therapy strategy. Those Kawasaki disease patients who are unresponsive to IVIG treatment carry a higher risk for developing coronary artery aneurysms. Several predictors for IVIG resistance have been identified [10, 13]. But there is no definitive risk score by which to clinically classify or predict IVIG resistance, especially in Caucasians [6, 10]. As only five of our study patients were refractive to IVIG treatment, no conclusive statistical statement on this issue is possible. VWF parameters did not differ from patients pre- vs. post-IVIG treatment, a finding that Linn et al. already interpreted as a persistent inflammation at the coronary-arteries level. This might be an argument to supplement first-line therapy with prolonged corticosteroid treatment, as is increasingly discussed [23]. In addition, vWF-blocking antibodies may provide a causal therapeutic option in Kawasaki disease. In a murine model of vasculitis, vWF-blocking antibodies were shown to attenuate neutrophil recruitment [7].
Strengths and limitations
This study investigated the impact of KD on multiple vWF parameters. In this context, we were able to clinically assess a considerable amount of data including specific information on coronary arteries and biochemical parameters. Patients were identified prospectively all over Germany. Nevertheless, the statistical power of this study is limited by its small sample size comprising 28 Kawasaki disease patients with serial vWF analysis in 5 patients only. It cannot be ruled out that with a larger sample size, further significant associations could be found. Although the KD patients were recruited for a prospective surveillance study, clinical characteristics were collected retrospectively via a standardized questionnaire. Therefore, our data quality depends on the reporting physicians’ data input. Regarding the citrated blood samples, we had not required an exact time-point when blood was collected, resulting in various blood sample time-points, both during the disease’s acute phase and during its later course.
Conclusion
Current results support vWF’s role as an inflammatory marker, as demonstrated by the positive correlation with standard acute phase parameters. Moreover, the vWF:CB/vWF:Ag ratio was significantly lower in KD patients with coronary artery lesions (and even lower in those with coronary artery aneurisms). These findings may be diagnostically valuable and help us better understand the pathogenesis of coronary artery lesions. They may also have an impact on setting a therapeutic target. Therefore, further analyses should be conducted prospectively in a larger study population.
Abbreviations
- AHA:
-
American Heart Association
- ALAT:
-
Alanine aminotransferase
- ASAT:
-
Aspartate aminotransferase
- CRP:
-
C-reactive protein
- ELISA:
-
Enzyme-linked immunoassay
- ESPED:
-
German Pediatric Surveillance Unit
- ESR:
-
Erythrocyte sedimentation rate
- Gamma GT:
-
Gamma-glutamyltransferase
- IVIG :
-
Intravenous immunoglobulin
- KD:
-
Kawasaki disease
- PVDF:
-
Polyvinylidene difluoride
- SD:
-
Standard deviation
- TNFα:
-
Tumor necrosis factor α
- vWF:
-
von Willebrand factor
- vWF:Ag:
-
von Willebrand factor: antigen
- vWF:CB:
-
von Willebrand factor: collagen binding
References
Ayusawa M, Sonobe T, Uemura S, Ogawa S, Nakamura Y, Kiyosawa N, Ishii M, Harada K, Kawasaki Disease Research Committee (2005) Revision of diagnostic guidelines for Kawasaki disease (the 5th revised edition). Pediatrics international : official journal of the Japan Pediatric Society 47(2):232–234
Bernardo A, Ball C, Nolasco L, Moake JF, Dong JF (2004) Effects of inflammatory cytokines on the release and cleavage of the endothelial cell-derived ultralarge von Willebrand factor multimers under flow. Blood. 104(1):100–106
Bernardo A, Ball C, Nolasco L, Choi H, Moake JL, Dong JF (2005) Platelets adhered to endothelial cell-bound ultra-large von Willebrand factor strings support leukocyte tethering and rolling under high shear stress. JTH. 3(3):562–570
Dallaire F, Dahdah N (2011) New equations and a critical appraisal of coronary artery Z scores in healthy children. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography 24(1):60–74
Dietz SM, van Stijn D, Burgner D, Levin M, Kuipers IM, Hutten BA, Kuijpers TW (2017) Dissecting Kawasaki disease: a state-of-the-art review. Eur J Pediatr 176(8):995–1009
Fabi M, Andreozzi L, Corinaldesi E, Bodnar T, Lami F, Cicero C, Tchana B, Landini C, Sprocati M, Bigucci B, Balsamo C, Sogno Valin P, di Fazzio G, Iughetti L, Valletta E, Marchetti F, Donti A, Lanari M (2019) Inability of Asian risk scoring systems to predict intravenous immunoglobulin resistance and coronary lesions in Kawasaki disease in an Italian cohort. Eur J Pediatr 178(3):315–322
Hillgruber C, Steingraber AK, Poppelmann B, Denis CV, Ware J, Vestweber D et al (2014) Blocking von Willebrand factor for treatment of cutaneous inflammation. The Journal of investigative dermatology 134(1):77–86
Irazuzta JE, Elbl F, Rees AR (1990) Factor VIII related antigen (von Willebrand’s factor) in Kawasaki disease. Clin Pediatr 29(6):347–348
Jakob A, Whelan J, Kordecki M, Berner R, Stiller B, Arnold R, von Kries R, Neumann E, Roubinis N, Robert M, Grohmann J, Höhn R, Hufnagel M (2016) Kawasaki disease in Germany: a prospective, population-based study adjusted for underreporting. Pediatr Infect Dis J 35(2):129–134
Jakob A, von Kries R, Horstmann J, Hufnagel M, Stiller B, Berner R, Schachinger E, Meyer K, Obermeier V (2018) Failure to predict high-risk Kawasaki disease patients in a population-based study cohort in Germany. Pediatr Infect Dis J 37(9):850–855
Lenting PJ, Casari C, Christophe OD, Denis CV (2012) von Willebrand factor: the old, the new and the unknown. JTH 10(12):2428–2437
Leung DY, Cotran RS, Kurt-Jones E, Burns JC, Newburger JW, Pober JS (1989) Endothelial cell activation and high interleukin-1 secretion in the pathogenesis of acute Kawasaki disease. Lancet (London, England) 2(8675):1298–1302
Li X, Chen Y, Tang Y, Ding Y, Xu Q, Sun L, Qian W, Qian G, Qin L, Lv H (2018) Predictors of intravenous immunoglobulin-resistant Kawasaki disease in children: a meta-analysis of 4442 cases. Eur J Pediatr 177(8):1279–1292
Lin MT, Tsao LY, Cheng ML, Chang YJ, Chiu HY, Chen HN, Kuo SF, Chiou SJ (2005) Absence of hypercoagulability in acute Kawasaki disease. Pediatrics international : official journal of the Japan Pediatric Society. 47(2):126–131
McCrindle BW, Rowley AH, Newburger JW, Burns JC, Bolger AF, Gewitz M, Baker AL, Jackson MA, Takahashi M, Shah PB, Kobayashi T, Wu MH, Saji TT, Pahl E, American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young; Council on Cardiovascular and Stroke Nursing; Council on Cardiovascular Surgery and Anesthesia; and Council on Epidemiology and Prevention (2017) Diagnosis, treatment, and long-term management of Kawasaki Disease: a scientific statement for health professionals from the American Heart Association. Circulation. 135(17):e927–e999
Nakamura Y, Yashiro M, Uehara R, Sadakane A, Tsuboi S, Aoyama Y, Kotani K, Tsogzolbaatar EO, Yanagawa H (2012) Epidemiologic features of Kawasaki disease in Japan: results of the 2009-2010 nationwide survey. J Epidemiol 22(3):216–221
Nash MC, Shah V, Dillon MJ (1995) Soluble cell adhesion molecules and von Willebrand factor in children with Kawasaki disease. Clin Exp Immunol 101(1):13–17
Petri B, Broermann A, Li H, Khandoga AG, Zarbock A, Krombach F, Goerge T, Schneider SW, Jones C, Nieswandt B, Wild MK, Vestweber D (2010) von Willebrand factor promotes leukocyte extravasation. Blood. 116(22):4712–4719
Pottinger BE, Read RC, Paleolog EM, Higgins PG, Pearson JD (1989) von Willebrand factor is an acute phase reactant in man. Thromb Res 53(4):387–394
Ritz N (2017) Kawasaki disease: what the paediatrician needs to know. Eur J Pediatr 176(8):1011
Tanoshima R, Hashimoto R, Suzuki T, Ishiguro A, Kobayashi T (2019) Effectiveness of antiplatelet therapy for Kawasaki disease: a systematic review. Eur J Pediatr 178(6):947–955
Taubert KA, Shulman ST (1999) Kawasaki disease. Am Fam Physician 59(11):3093–3102 3107-3098
Wardle AJ, Connolly GM, Seager MJ, Tulloh RM (2017) Corticosteroids for the treatment of Kawasaki disease in children. The Cochrane database of systematic reviews 1:Cd011188
Funding
André Jakob received funding for this work by a grant from the German Heart Foundation.
Author information
Authors and Affiliations
Contributions
André Jakob: Conceived and designed the study, contributed to statistical analyses and data interpretation, drafted the manuscript and approved the final manuscript as submitted.
Eva Schachinger: Responsible for data collection, contributed to statistical analysis and study design, as well as approved the final manuscript as submitted.
Simon Klau: Conducted the statistical analysis, contributed to drafting the manuscript and approved the final manuscript as submitted.
Anja Lehner, Sarah Ulrich and Brigitte Stiller: Contributed to data interpretation, served on the adjudicating committee and approved the final manuscript as submitted.
Barbara Zieger: Contributed to the study design, data interpretation and statistical analysis. She is responsible for the VWF analyses and contributed to drafting the manuscript; she has approved the final manuscript as submitted.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Approval for our study had been provided by the Ethics Committee of the University of Freiburg, in accordance with Declaration of Helsinki ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Communicated by Peter de Winter
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Clinical Trial Registration: German clinical trial registration, DRKS00010071 http://apps.who.int/trialsearch/Trial2.aspx?TrialID=DRKS00010071
Rights and permissions
About this article
Cite this article
Jakob, A., Schachinger, E., Klau, S. et al. Von Willebrand factor parameters as potential biomarkers for disease activity and coronary artery lesion in patients with Kawasaki disease. Eur J Pediatr 179, 377–384 (2020). https://doi.org/10.1007/s00431-019-03513-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-019-03513-6