Abstract
The proper function of the skeletal muscle is essential for the survival of most animals. Thus, efficient and rapid repair of muscular damage following injury is crucial. In recent years, satellite cells have emerged as key players of muscle repair, capable of undergoing extensive proliferation after injury, fusing into myotubes and restoring muscle function. Furthermore, it has been shown that Ca2+/calmodulin-dependent generation of nitric oxide (NO) is an important regulator of muscle repair. Here, we demonstrate the functional expression of transient receptor potential, subfamily A1 (TRPA1) channel in human primary myoblasts. Stimulation of these cells with well-known TRPA1 ligands led to robust intracellular Ca2+ rises which could be inhibited by specific TRPA1 antagonists. Moreover, we show that TRPA1 activation enhances important aspects of skeletal muscle repair such as cell migration and myoblast fusion in vitro. Interestingly, TRPA1 levels and inducible Ca2+ transients decline with ongoing myoblast differentiation. We suggest that TRPA1 might serve as a physiological mediator for inflammatory signals and appears to have a functional role in promoting myoblast migration, fusion, and potentially also in activating satellite cells in humans.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Skeletal muscle is essential for mobility and therefore for survival of most animals. It is capable of restoring functionality after injuries and also of responding to exercise with hypertrophy. Key elements ensuring these abilities are satellite cells (SCs), which are mononuclear progenitor cells residing in a quiescent state between the basement membrane and the sarcolemma of muscle fibers [36, 42]. Upon traumatic or disease-induced muscle injury, satellite cells are activated, reenter the cell cycle, and proliferate as myoblasts, which are crucial for muscle repair [36, 56]. Activation, proliferation, and differentiation of satellite cells are precisely regulated processes, whose exact modulation is still not fully understood. Different stimuli can initiate and influence muscle repair, comprising cellular stretch, several cytokines and growth factors as well as other inflammatory mediators such as nitric oxide (NO) which has emerged as a key regulator of skeletal muscle repair [18, 22, 23, 51, 60, 62, 67]. Intracellular Ca2+ elevations activate nitric oxide synthases (NOS), which, in turn, stimulates matrix metallopeptidase 2 (MMP-2) via generation of NO, causing the liberation of ECM-bound hepatocyte growth factor (HGF) [19, 62, 67]. HGF potently induces activation of quiescent satellite cells and further promotes proliferation and migration of activated SCs [2, 57, 60]. In addition, the inflammatory response following muscle injury [49] also plays a major role in the activation of satellite cells. Rigamonti et al. could demonstrate that NO originating from invading macrophages is essential for muscle repair, further emphasizing the importance of NO [53]. As the precise signaling mechanisms orchestrating the process of muscle repair, especially in response to inflammatory stimuli, are still not fully clarified, we aimed at finding other chemoreceptors involved in adult myogenesis. Therefore, we focused on members of the transient receptor potential (TRP) channel family as some members are known to be involved in inflammatory processes throughout the body. We found strong expression of the cation channel TRPA1, which is widely expressed in a variety of neuronal and non-neuronal cell types. It is activated by noxious cold [6, 30, 64], a great number of chemical irritants [40, 43, 45] and also by peptides and compounds usually associated with inflammation such as prostaglandins, other phospholipid derivatives, reactive oxygen species, and nitric oxide [8, 59, 63]. Moreover, mechanosensitivity has been demonstrated for TRPA1, thus making it a highly versatile receptor [12, 35, 65]. In this study, we show that TRPA1 is not only present in human primary myoblasts but also downregulated in the course of differentiation. Stimulation with known TRPA1 agonists (thymol, allyl isothiocyanate, nitric oxide) led to a strong Ca2+ influx in human myoblasts, which was diminished in later stages of differentiation. In addition, we demonstrate important physiological effects of TRPA1 activation on cell migration and fusion, thereby giving evidence for a potential role of TRPA1 in the repair of skeletal muscle injury. Finally, we were also able to in part elucidate the signaling pathway following TRPA1 activation with MMP-2 upregulation and subsequent putative liberation of HGF. We conclude that TRPA1 is potentially involved in adult myogenesis which may boost migration and fusion during muscle repair in a self-promoting manner and is downregulated during differentiation when excessive migration is not further required. As TRPA1 can be targeted with pharmaceutical modulators, this study might lead to novel treatments for muscle injury or muscle-related disease.
Material and methods
Muscle satellite cell culture and differentiation
Primary human myoblast cultures were donated from the Muscle Tissue Culture Collection, Friedrich-Baur-Institut Munich. Myoblasts were maintained at 37 °C and 6 % CO2 in a humidified incubator. To induce differentiation, skeletal muscle growth medium (Promocell, Heidelberg, Germany) was completely removed (cells were briefly washed with phosphate-buffered saline (PBS)) and replaced by skeletal muscle differentiation medium (Promocell). Differentiation medium was replaced every 2–3 days till the experiments were carried out.
Gene expression analysis
RNA isolation was performed on freshly harvested cells (3 × 106) by using RNeasy Kit (QIAGEN, Hilden, Germany). Subsequently, RNA was DNAase treated, transcribed in cDNA, amplified with TRPA1 primers (fw: CCGCTTACAGCCCTCAACG; rv: AGCTCTAAATCCATAAGCCAACC) (Eurofins MWG Operon, Ebersberg, Germany) and analyzed with Mastercycler® ep realplex (Epperdorf, Hamburg, Germany). Tata box binding protein (fw: TCCAGCGCAAGGGTTTCTGGT; rv: GGCCAAGCCCTGAGCGTAAGG) amount was used as a normalization control [58]. We used the PCR efficiency-corrected ΔΔCT method [50] to quantify target gene expression.
Immunohistochemistry and Western blotting
To perform immunofluorescent stainings of cultured myoblasts, cells were plated on 20-mm2 glass cover slips and allowed to grow over night. Cells were fixed in 4 % ice-cold paraformaldehyde (PFA) and permeabilized with 0.1 % PBS/Triton X. Unspecific binding sites were blocked with 1 % fish gelatine in PBS with 0.05 % Tween 20 (PBST) for 1 h at room temperature (RT). Incubation with primary antibodies for TRPA1 (ANKTM1 C-19; 1:50; Santa Cruz, Dallas, TX, USA) or Pax7 (1:50; Santa Cruz) was performed over night at 4 °C. After washing with PBS, cells were incubated with secondary antibodies (Alexa Fluor; Life Technologies, Carlsbad, CA, USA) for 45 min at room temperature, washed again, and mounted using ProLong® Gold Antifade (Life Technologies). Fluorescent images were acquired with a laser scanning confocal microscope (Zeiss LSM 510 Meta; Zeiss AG, Oberkochen, Germany).
Western blot analysis was carried out with myoblasts in different differentiation stages. Myoblasts were harvested 2, 1, and 0 days prior to differentiation or after cultivation for 1, 2, or 7 days in differentiation medium, followed by a membrane preparation via ultracentrifugation. Protein amount was determined using Protein Quantification Assay (Machery-Nagel, Düren, Germany). Equivalent amounts of protein were electrophoresed and transferred to a nitrocellulose membrane. Blocking of unspecific binding sites was achieved by incubation with 3 % “Eiweiß Shake” (Layenberger, Rodenbach, Germany) in PBST overnight at 4 °C. Membranes were incubated with primary antibody TRPA1 (ANKTM1 C-4; 1:200; Santa Cruz) or PMCA4b (1:200; Santa Cruz) overnight at 4 °C, washed, incubated with appropriate secondary antibody (dilution 1:10,000) for 1 h at room temperature, and washed again before detection reagent ECL Prime (GE Healthcare, Little Chalfont, UK) was applied. Chemoluminescence was detected with Fusion SL (Vilber Lourmat Deutschland GmbH, Eberhardzell, Germany). To ensure equal gel loading, ponceau or PMCA4b stainings were carried out. Densitometric analysis of protein bands was performed with ImageJ software (http://rsbweb.nih.gov/ij/).
Calcium imaging and patch clamp
In brief, myoblasts were grown for 24 h on glass cover slides. Prior to Ca2+ imaging measurements, cells were loaded with Fura 2-AM (Life Technologies) for 1 h, washed, and equilibrated in Ringer’s solution for 5 min. Ca2+ imaging setup included a monochromator (TILL Photonics, Munich, Germany), Axiovert 200 inverted microscope (Zeiss AG) with an attached high speed CCD camera (TILL Photonics) and TillVision software (TILL Photonics). To exclude mechanically induced responses, cells were constantly superfused with Ringer’s solution followed by the desired application protocol. Substances were diluted in Ringer’s solution and applied to the investigated cells via a custom-made, air pressure-controlled application system with magnetic high-precision valves. Changes in intracellular Ca2+ concentration (measured as changes in relative fluorescence) were considered a response when they exceeded baseline Ca2+ levels more than 2-fold of standard deviation. Response amplitudes are always depicted as the maximal Ca2+ signal intensity relative to basal signal intensity.
For patch clamp recordings, cells were treated as stated above skipping Fura 2-AM loading.
Patch pipettes were pulled from borosilicate glass capillaries (1.17 × 1.50 × 100 mm, Science Products, Hofheim, Germany) and were fire polished to 3–5 MΩ tip resistance using a horizontal puller (Zeitz Instruments, Martinsried, Germany). We used an Axiovert 35 inverted microscope (Zeiss AG) and an EPC 7 amplifier (HEKA, Lambrecht, Germany). Capacity and series resistance was adjusted manually. Data were acquired using PULSE software (HEKA) (for detailed description of patch clamp procedure, see [39]). Holding potential for voltage-clamp recordings were individually adjusted according to each cells resting membrane potential.
Migration assays
Cells were grown for at least 24 h prior to experiments. After detachment, cells were admixed with liquid collagen solution (consisting of PureCol Collagen (Advanced BioMatrixCell, San Diego, CA, USA), minimal essential medium (Sigma-Aldrich, St. Louis, MO, USA), and sodium bicarbonate (Sigma-Aldrich)) and added with 200 μM thymol. Cell/collagen mixture was filled into measurement chambers and placed in a humidified incubator for 30 min at 37 °C. After polymerization, collagen matrix was covered with Ringer solution and the chamber sealed with wax. Measurement chambers were then placed under a microscope in a 37 °C incubation compartment. Pictures were taken every 76 s for 5 h. Time lapse videos were produced and the last 4 h analyzed with homemade software (for detailed description, see [7]). The first hours was excluded as the cells had to recover from experimental procedure. The duration of each analyzed time period was 15 min.
Fusion index assays
Cells were cultured for 24 h after seeding. Growth medium was replaced by differentiation medium (Promocell) containing 0, 20, or 200 μM of thymol. Medium was changed every 1–2 days. After 7 days of differentiation, cells were fixed and stained with 0.1 % crystal violet. Fusion index was determined by dividing the number of nuclei present in myotubes (myotube = cell with three or more nuclei) by the number of all nuclei in the visual field. For each experiment, fusion indices of six different visual fields were determined, and the mean was calculated.
Statistics
Statistical significance between two groups was calculated by either Student’s t tests or the Mann–Whitney U test, test according to distribution of data. Comparison of multiple groups was accomplished by using a one-way analysis of variance or Kruskal–Wallis one-way analysis of variance with post hoc test as appropriate. N numbers correspond to the number of individual experiments performed. For all statistical tests, a confidence interval of p < 0.05 or less was accepted for statistical significance. All results are presented with ± SEM.
Results
TRPA1 is expressed in human primary myoblasts
The repair of a damaged muscle requires the formation of multinucleated myofibers. To achieve this, myoblasts have to multiply, migrate, and fuse to adjacent cells. In vitro analysis of myogenesis can be accomplished by switching growth medium (GM) to differentiation medium (DM), thereby triggering the differentiation of myoblasts to fusion-competent myocytes followed by the formation of small myotubes (Fig. 1a). In PCR experiments, we detected a strong expression of TRPA1 in undifferentiated human myoblasts. To analyze potential changes of TRPA1 expression levels in the course of differentiation, we cultivated human primary myoblasts and induced differentiation by applying DM. TRPA1 amounts were determined by qPCR at defined time points: 2 and 1 days before, directly prior to, and after 1, 2, and 7 days subsequent to applying DM. All results were normalized to expression of TATA box binding protein (TBP) as it is considered to be stably expressed during myogenesis [58]. Relative to undifferentiated cells, TRPA1 expression significantly declined during the progressing differentiation to nearly one third of its original value after 7 days (Fig. 1b). To clarify if the reduction of TRPA1 mRNA also affected protein amounts, Western blot analyses were performed after the same differentiation periods as stated above. The drop in protein amount was even more prominent with a reduction to about 1/10th of initial protein levels after 1 day and almost no detectable protein (1.08 ± 0.76 %) after 7 days (Fig. 1c, d, e). Moreover, we noticed an increase in TRPA1 levels after cultivation for 2 days. Immunofluorescence stainings of undifferentiated myoblasts showed a strong localization of TRPA1 protein around the cell nucleus (probably ER) and often in clusters in the cell’s pseudopodia plasma membranes (Fig. 2a). All in all, we conclude that TRPA1 appears to be expressed in early phases of myoblast differentiation and is reduced with progressing differentiation.
Downregulation of TRPA1 mRNA and protein amount during differentiation. a Images depicting cultured human primary myoblasts derived from adult donors in different differentiation stages. Undifferentiated cells (0 days) grow unordered and evenly distributed. During later stages of differentiation, myoblasts clearly align to each other and form multinucleated myotubes after 2 days; scale bar = 40 μm. b Downregulation of TRPA1 mRNA in the course of differentiation relative to undifferentiated cells (0 days). TRPA1 expression is stable prior to differentiation and significantly declines with proceeding differentiation to 43.1 ± 4.2, 37.9 ± 3.5, and 34.7 ± 3 % after 1, 2, and 7 days, respectively; n = 8. c Downregulation of TRPA1 protein amount during differentiation relative to undifferentiated cells (0 days). On day 2 and 1 before differentiation, TRPA1 protein amount appears to increase, although this is not significant. A significant reduction in the TPRA1 protein level to 10.25 ± 0.61 % is observable 1 day after differentiation. The amount further decreases to 7.1 ± 2.5 % after 2 days and is almost not detectable (1.08 ± 0.76 %) after 7 days; n = 4. P values were calculated using one-way ANOVA; ***p ≤ 0.001. d–e Exemplary Western blot of a myoblast membrane protein preparation showing TRPA1 protein bands. Undifferentiated myoblasts exhibit a strong signal prior to differentiation, which rapidly declines with ongoing differentiation. f–g Equal band loading was confirmed by PCMA4b staining (prior differentiation) and ponceau staining after differentiation
Immunostaining of TRPA1 in cultured cells. a Confocal image depicting an exemplary immunostaining of TRPA1 and Pax7 in undifferentiated myoblasts. TRPA1 is predominantly localized in regions surrounding cell nuclei and in punctate clusters on pseudopodia. Pax7 staining serves as control to ensure myogenic identity; scale bar = 20 μm. b Confocal image showing untransfected HEK cells stained with α-TRPA1 antibody. No staining is observable. c Confocal image showing an immunostaining of TRPA1-transfected HEK cells with an α-TRPA1 antibody. A strong TRPA1 staining is apparent in several cells; scale bar = 50 μm
TRPA1 activation increases intracellular Ca2+ in human myoblasts
To prove the functionality of TRPA1 in human myoblasts, we performed Ca2+ imaging experiments. In initial measurements, allyl isothiocyanate (AITC) was used as a well-known activator of TRPA1 [6, 29]. Application of AITC (200 μM) to undifferentiated human myoblasts resulted in a strong Ca2+ increase in the majority of the cells. Ca2+ responses could be inhibited by coapplying 20 μM of the specific TRPA1 antagonist HC-030031 [17] and rescued after washout of HC-030031 (Fig. 3a, b, c). As AITC had severe side effects on cell viability upon long-term exposure (6 h), we replaced AITC by the TRPA1 ligand thymol [33]. Thymol application (200 μM) elicited strong Ca2+ responses in undifferentiated human myoblasts, which were abolished by coapplication of 20 μM HC-030031 (Fig. 3d, e, f). To ensure that these responses were caused by TRPA1 activation, we additionally performed the same experiments with the highly specific and potent TRPA1 inhibitor A 967079 [13] (Fig. 3g, h, i). To exclude any potential desensitization effects, we also tested repeated thymol applications without the use of a pharmacological antagonist and saw no effect on the responses (Fig. 3j). Moreover, removal of extracellular Ca2+ completely abrogated thymol-evoked Ca2+ increases (Fig. 3k), clearly demonstrating the necessity of extracellular Ca2+.
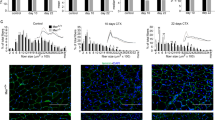
Stimulation of undifferentiated myoblasts with AITC, thymol, or SNAP (NO) causes TRPA1 activation. a Exemplary Ca2+ imaging trace of undifferentiated myoblasts stimulated with AITC (200 μM) for 20 s with or without coapplication of TRPA1 antagonist HC-030031 (20 μM). AITC induces a strong increase of intracellular Ca2+ which is abrogated under the influence of HC-030031. b–c Bar charts depicting averaged intracellular Ca2+ responses and percentage of responsive cells triggered by AITC (n = 7) compared to thymol (n = 38). No significant differences are observable although AITC tends to cause stronger Ca2+ influxes. d Exemplary Ca2+ imaging trace of undifferentiated myoblasts stimulated with thymol (200 μM) for 20 s with or without coapplication of TRPA1 antagonist HC-030031 (20 μM). AITC induces a strong increase of intracellular Ca2+ which is abrogated under the influence of HC-030031. e–f Bar charts depicting averaged intracellular Ca2+ responses and percentage of responsive cells triggered by thymol, which both are significantly reduced by coadministration with HC-030031; n = 38. g Exemplary Ca2+ imaging trace undifferentiated myoblasts stimulated with thymol (200 μM) in the absence and presence of A-967079 (1 μM). As seen before, under the influence of HC-030031, Ca2+ influx is completely diminished. h–i Bar charts showing averaged intracellular Ca2+ responses and number of thymol-responsive with or without addition of A-967079 (1 μM). A-967079 caused a significant reduction of the Ca2+ influx as well as the number of responding cells; n = 24. j Exemplary Ca2+ imaging trace from undifferentiated myoblasts stimulated with thymol (200 μM) three repetitive times. No obvious desensitization is detectable. k Exemplary Ca2+ imaging trace from undifferentiated myoblasts stimulated with thymol (200 μM) in the absence and presence of extracellular Ca2+ with the former completely abolishing all Ca2+ responses. l Exemplary whole-cell voltage-clamp recording (holding potential = −20 mV) of an undifferentiated myoblast. Administration of thymol (200 μM) causes a prominent inward current which is completely inhibited upon coadministration of thymol (200 μM) with the TRPA1 antagonist HC-030031 (20 μM). m Bar chart showing highly significant inhibition of thymol-induced increase in conductance in undifferentiated myoblasts. Holding potential was adjusted to each individual cells’ resting membrane potential, recorded prior to the voltage-clamp recording. n thymol = 33, n thymol + HC = 6, n 2.thymol = 4. o Exemplary Ca2+ imaging trace of undifferentiated myoblasts stimulated with SNAP (200 μM) with or without coapplication of HC-030031 (20 μM). SNAP-induced response is inhibited in the presence of HC-030031. p–q Bar charts depicting averaged intracellular Ca2+ responses from SNAP-responsive myoblasts that were completely inhibited by coadministration with HC-030031, as well as the amount of SNAP-sensitive cells observed during these experiments; n = 8. Significance levels were calculated using one-way ANOVA, Kruskal–Wallis test or Mann–Whitney U test: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
To characterize these thymol-evoked responses in more detail, whole-cell patch clamp experiments were carried out. The holding potentials were adjusted to the resting membrane potential of each individual cell, ranging from −35 to −5 mV (mean −11.89 mV). Cells were stimulated with thymol (200 μM) followed by coapplication with HC-030031 (20 μM) and finally thymol again. In the presence of TRPA1 inhibitor HC-030031, thymol-evoked increase of the conductance was completely abolished and showed full recovery after washout, indicating that it is exclusively mediated by TRPA1 (Fig. 3l, m).
An endogenous substance with an important role in inflammation and repair of skeletal muscle is nitric oxide (NO), which is thought to be a key signaling molecule in the activation and proliferation of satellite cells/myoblasts [18, 19, 53, 61]. Additionally, NO was reported to directly activate hTRPA1 recombinantly expressed in HEK cells [59]. Nitric oxide was administered by using S-Nitroso-N-acetyl-DL-penicillamine (SNAP) which spontaneously releases NO into the surrounding medium. Like thymol, SNAP application (200 μM) caused a strong Ca2+ influx which could be abrogated by coadministration of HC-030031 (Fig. 3o, p, q). In conclusion, these results prove the functionality of TRPA1 in human myoblasts and its responsiveness to several ligands.
Ca2+ responses decline during differentiation
We then investigated if the observed downregulation of TRPA1 also affected the thymol-induced Ca2+ increases. Therefore, we performed Ca2+ imaging experiments with human myoblasts 1 or 2 days before (−1 and −2 days), on the day of (day 0) and 1, 2, and 7 days after differentiation. No significant alterations in the amplitude of the thymol-induced Ca2+ increases could be observed until day 1 after differentiation. However, at the second day of differentiation, we detected a significant reduction of the response amplitude of about 50 % which did not further change after 7 days of differentiation (Fig. 4a). In contrast, the number of responsive cells remained, except for an insignificant increase during the first 2 days, unaltered until 2 days past differentiation, and significantly decreased to nearly one third after 7 days (Fig. 4b). These imaging results are in agreement with and therefore substantiate our qPCR and Western blot results, clearly demonstrating that TRPA1 protein decline also affects TRPA1-mediated signaling in human myoblasts.
Reduction of thymol-induced Ca2+ signals with ongoing myoblast differentiation. a Bar chart depicting thymol-evoked Ca2+ rises of myoblasts at different differentiation stages. A significant reduction (from 50.19 ± 11.35 % (day 0) to 15.67 ± 3.11 % (day 2)) of thymol-induced responses is present at day 2 after differentiation onset. A further decrease is not observable after 7 days. b Bar chart illustrating the number of thymol-responsive myoblasts, which remains unaltered for the first 5 days (−2 till 2) and significantly declines to 18.64 ± 4.97 % after 7 days of differentiation; n = 6–19. Significance levels were calculated using one-way ANOVA: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
TRPA1 activation enhances migration activity
As the migration of myoblasts is a crucial step in the beginning of muscle repair [20], we investigated the impact of TRPA1 stimulation on the migration activity of human myoblasts. Cells were embedded in a 3D collagen layer to provide an environment more similar to an in vivo situation than in classical migration experiments. Time-lapse microscopy was performed for 5 h, and the migration paths of 30 individual cells per experiment and condition were tracked for 4 h after a 1-h lag phase, during which myoblasts had to recover from assay preparation. Analysis of tracked migration paths revealed migration speed and migration activity. On average, nearly 80 % of untreated human myoblasts exhibited a migration activity which was significantly increased by about 10 % upon thymol stimulation (Fig. 5a, c). In addition, migration speed was also elevated about one third (Fig. 5b, d). To test if the observed thymol-induced effects on myoblast migration are TRPA1-mediated, we repeated the performed experiment as stated before; however, this time it was conducted in the presence of the TRPA1 antagonist HC-030031 (20 μM). Coadministration of thymol and HC-030031 significantly decreased migration activity and speed within the first 4 h following the initial 1-h lag phase (Fig. 5e, f, g, h). We therefore conclude that TRPA1 activation is indeed able to enhance myoblast migration.
TRPA1-mediated enhancement of myoblast migration. a–b Diagrams are representing the averaged values of the myoblasts migration behavior for the entire duration of the experiments in the presence or absence of thymol (200 μM). Depicted are the percentage of actively migrating cells and migration speed. c–d Bar charts represent the mean migration rate/speed throughout the whole time of the experiment (summed values of migration rate/speed at each time point divided by the number of measurement time points). The bars clearly show that thymol application causes a significant increase in myoblast migration activity and speed from 75.85 ± 1.46 to 82.61 ± 1.73 % (8.42 ± 2.46 % increase) and from 25.91 ± 1.15 to 33.16 ± 1.54 μm/s (27.98 ± 6.75 %), respectively; n = 10. e–f Diagrams are depicting the averaged values of the myoblast migration behavior for the entire duration of the experiments in the presence of thymol (200 μM) and with or without coapplication of HC-030031 (20 μM). Inhibiting effects of HC-030031 on migration behavior are significant in the early phase and attenuate over time. g–h Bar charts showing a significant decrease of migration activity and cell speed caused by HC-030031; n = 5. Significance levels were calculated using Student’s t test or Mann–Whitney U test: *p ≤ 0.05, ***p ≤ 0.001
TRPA1 activation elevates myoblast fusion rate
Another important aspect of muscle repair is the ability of myotubes to fuse and build syncytia that can later fuse with adjacent fibers [1, 27]. Cultured human myoblasts are able to fuse and form syncytia after placing them in a differentiation medium. To investigate a putative role of TRPA1 in myoblast fusion, we performed fusion assays during which myoblasts were differentiated for 7 days. Addition of 20 μM thymol to the DM significantly increased the fusion rate by almost 2-fold, and it could be further increased to ~2.5-fold after addition of 200 μM thymol (Fig. 6a). Again, coadministration of HC-030031 or A-967079 significantly decreased the effect of thymol on myoblast fusion, reaching levels equal to those observed under control conditions (Fig. 6b). Thus, TRPA1 activation potently promotes myoblast fusion.
TRPA1 activation increases myoblast fusion of undifferentiated myoblasts. a Bar chart depicting averaged fusion indices of myoblast differentiated for 7 days. Thymol dose-dependently elevates fusion rate of differentiated myoblasts; n = 10. b Bar chart presenting the averaged fusion indices in the absence and presence of thymol, with pharmacological TRPA1 inhibitors HC-030031 (20 μM) and A-967079 (1 μM), and the inhibitors alone. Coapplication of thymol (200 μM) and HC-030031/A-967079 completely inhibited the thymol-induced increase in myoblast fusion. HC-030031 and A-967079 both did not significantly reduce the fusion rate below the control levels; n = 8. Significance levels were calculated using one-way ANOVA: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
Signaling events downstream of TRPA1 activation
A well-described pathway of satellite cell activation and muscle repair comprises the activation of matrix metalloproteinase-2 (MMP-2) [62, 67]. We therefore investigated if TRPA1 stimulation affects MMP-2 protein levels or its activation state. Hence, we treated undifferentiated myoblasts with 200 μM thymol or SNAP for 24 h and subsequently used Western blotting to analyze MMP-2 levels. MMP-2 is produced as a pro form which is eventually cleaved to produce the active form [23, 41, 47]. In undifferentiated myoblasts, thymol application significantly increased both proMMP-2 and active MMP-2. Mean amounts of proMMP-2 and active MMP-2 were elevated by 98.3 ± 26.58 and 69.5 ± 25.6 %, respectively (Fig. 7). In contrast, SNAP application did not cause any significant changes in active MMP-2 amounts but in proMMP-2 abundance (72 ± 54.67 %).
TRPA1 agonists thymol and SNAP (NO) increase MMP-2 protein abundance in undifferentiated myoblasts. a Bar chart indicating significantly increased levels of inactive proMMP-2 protein upon stimulation of undifferentiated myoblasts with thymol (200 μM) or SNAP (200 μM) for 24 h. b Bar chart depicting a significant increase in active MMP-2 protein upon stimulation with thymol (200 μM) for 24 h, whereas SNAP-induced changes are not significant. c Exemplary Western blot showing proMMP-2 (72 kDa) and active MMP-2 (62 kDa) protein bands for different conditions; n = 6. Significance levels were calculated using Kolmogorov–Smirnov test or Mann–Whitney U test: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001
In summary, our results demonstrate that TRPA1 in human myoblast can be activated by different ligands and that TRPA1 stimulation causes enhanced migration and fusion. Furthermore, we can show that MMP-2 activation is likely involved in TRPA1-mediated signaling. Interestingly, expression of TRPA1 is precisely downregulated during the course of differentiation thereby also decreasing TRPA1 signaling capabilities in later stages of differentiation.
Discussion
The process of muscle repair and its regulation is achieved by a complex interplay of different proteins and cell types. The importance of satellite cells has been shown in different studies, and their activity appears to be crucial for muscle repair [36, 56, 66]. Although, understanding of major signaling pathways has been achieved in recent years, the detailed regulation of all mechanisms that are necessary for muscle repair such as migration, proliferation, and fusion is still not fully understood.
In this study, we present TRPA1 as a novel component which is potentially able to influence skeletal muscle repair by modulating migration and fusion activity of myoblasts and which is putatively involved in satellite cell activation. TRPA1 is strongly expressed in undifferentiated myoblasts on an mRNA and protein level. However, whereas the mRNA amount is also relatively stable 2 days before the differentiation was initiated, the protein amount appears to be rising up to the day of differentiation. However, the difference is not statistically significant. After differentiation, both RNA and protein levels significantly decline. The considerable drop of TRPA1 protein, while mRNA is reduced to lower extent, may point to a targeted degradation of the protein after initiation of differentiation or to high TRPA1 turnover rates. This regulation indicates a role of TRPA1 for undifferentiated myoblasts and early myocytes whereas it appears to be not important or even detrimental in later stages of differentiation. It has been demonstrated that a transient Ca2+ increase is crucial for the initiation of differentiation [4, 14, 52] and several transcription factors are activated in a Ca2+-dependent manner [11, 44]. However, constantly elevated Ca2+ levels due to sustained TRPA1 activation could disturb efficient intracellular signaling. Therefore, downregulation of the channel might be required for normal differentiation.
Application of the TRPA1 agonist thymol [33] elicited strong Ca2+ influxes in myoblasts. In agreement with our expression data, the amplitude of the Ca2+ responses as well as the number of responding cells significantly decreased with ongoing differentiation. At day 7 after differentiation, TRPA1 was not detectable by Western blot, and accordingly, thymol stimulation only evoked minor responses in fewer cells, most likely due to residual amounts of TRPA1. Furthermore, we used the NO donor SNAP which could as well evoke strong Ca2+ responses in human myoblasts. However, it is possible that SNAP may not only act on TRPA1 via NO release but is likely to have effects on TRPA1 on its own as it has been shown by Eberhardt et al. in murine DRG neurons [16].
NO is of special interest as it has already been demonstrated as a versatile signaling molecule [31, 38] and most importantly as a key regulator of skeletal muscle repair and inflammation [18, 19, 61, 67]. NO can cause activation of MMP-2, which releases HGF from the extracellular matrix subsequently leading to activation and increasing migration of satellite cells via binding of HGF to the HGFR [2, 57, 60]. Ca2+ increases caused by thymol and SNAP could be diminished by coapplying different specific TRPA1 antagonists, clearly demonstrating TRPA1 dependency. In addition, our patch clamp experiments revealed that the thymol-evoked increase of the conductance was exclusively mediated via TRPA1. Tatsumi et al. stated that in the murine model, a Ca2+/calmodulin complex is important for satellite cell activation mediated by subsequent NOS and MMP-2 activity [62]. In accordance, we were able to verify an increase of proMMP-2 and active MMP-2 following TRPA1 activation by thymol and subsequent Ca2+ influx which would induce Ca2+/calmodulin formation. A physiological effect of TRPA1 signaling has been demonstrated by our migration assays in which stimulation of TRPA1 by thymol significantly increased myoblast migration whereas application of HC-030031 significantly inhibited thymol-induced promotion of myoblast migration. In addition to the aforementioned NO/MMP-2 pathway, myoblast migration can also be mediated by Ca2+-induced calpain activity [34, 37] which might also be directly caused by TRPA1-dependent Ca2+ influx. Furthermore, TRPA1 activation did not only increase migration but also fusion rates of human myoblasts in a dose-dependent manner. It has been demonstrated before that Ca2+ is highly important to initiate cell fusion and that fusion is preceded by Ca2+ transients [14, 15, 24]. These transients act via Ca2+-dependent calcineurin, which, in turn, activates NFAT family of transcription factors regulating gene transcription to coordinate proliferation, survival, and differentiation in myoblasts and many other cell types [25]. Thus, Ca2+ influx mediated by TRPA1 might also be sufficient to trigger cell fusion events or to support the rise of intracellular Ca2+ mediated by other pathways. Another possible reason for elevated fusion rates may be provided by the increased migration activity. Augmentation of migration leads to a higher frequency of cell–cell contacts and thereby to an improved myocyte fusion [5, 21, 26, 28, 32].
In summary, TRPA1 might fulfill several potential functions in quiescent SCs and activated SCs/myoblasts. Muscle injury is always accompanied by local inflammation and the invasion of inflammatory cells which is essential for the repair process [41, 53]. TRPA1 is able to detect several different inflammatory cues such as ROS, RNS, cyclopentenone prostaglandins, other fatty acid derivatives or acidification of the extracellular milieu [8–10, 46, 48, 54]. Thus, TRPA1 might have two main functions in muscle repair. First, it might be involved in the activation of quiescent SCs, as opening of TRPA1 leads to a strong Ca2+ influx, resulting in the formation of Ca2+/calmodulin complexes, which then could initiate the activation of quiescent satellite cells via the aforementioned NO/MMP-2/HGF pathway. A probable second function of TRPA1 in already activated human myoblasts might be the detection of sustained levels of different inflammatory cues during the repair process. As TRPA1 activation significantly increases myoblast migration and fusion, this continued TRPA1 activation could boost these cellular functions and thus potentially the whole muscle repair process.
In regard to our results obtained by using SNAP, we already stated that all effects caused by SNAP might not be solely attributed to NO as a discrete molecule but may be caused by SNAP itself. However, if we assume that NO is responsible for TRPA1 activation, it could be readily present as it directly freed by damaged or torn muscle fibers [3, 55]. Moreover, TRPA1 activation by NO might trigger increased NO generation as stated above, resulting in elevated TRPA1 activity and thereby constituting a self-promoting feedback mechanism.
Either way, the downregulation of TRPA1 and a subsequent decrease of the migration-promoting signaling may pose as a regulatory mechanism for a precise boost of migration and fusion activity at earlier stages of muscle repair and a shutdown of this pathway when it is no longer beneficial or even detrimental, namely in later stages of the repair.
In summary, our results clearly demonstrate a major role of TRPA1 in human myoblast migration and fusion in culture and furthermore suggest a putative role in SC activation.
References
Abmayr SM, Pavlath GK (2012) Myoblast fusion: lessons from flies and mice. Development 139:641–56. doi:10.1242/dev.068353
Allen RE, Sheehan SM, Taylor RG, Kendall TL, Rice GM (1995) Hepatocyte growth factor activates quiescent skeletal muscle satellite cells in vitro. J Cell Physiol 165:307–12. doi:10.1002/jcp.1041650211
Anderson JE (2000) A role for nitric oxide in muscle repair: nitric oxide-mediated activation of muscle satellite cells. Mol Biol Cell 11:1859–74
Arnaudeau S, Holzer N, Bader CR, Bernheim L (2006) Calcium sources used by post-natal human myoblasts during initial differentiation. 445:435–445.
Bae G-U, Gaio U, Yang Y-J, Lee H-J, Kang J-S, Krauss RS (2008) Regulation of myoblast motility and fusion by the CXCR4-associated sialomucin, CD164. J Biol Chem 283:8301–9. doi:10.1074/jbc.M706730200
Bandell M, Story GM, Hwang SW, Viswanath V, Eid SR, Petrus MJ, Earley TJ, Patapoutian A (2004) Noxious cold ion channel TRPA1 is activated by pungent compounds and bradykinin. Neuron 41:849–57
Bastian P, Lang K, Niggemann B, Zaenker KS, Entschladen F (2005) Myosin regulation in the migration of tumor cells and leukocytes within a three-dimensional collagen matrix. Cell Mol Life Sci 62:65–76. doi:10.1007/s00018-004-4391-6
Bautista DM, Pellegrino M, Tsunozaki M (2012) TRPA1: a gatekeeper for inflammation. Annu Rev Physiol 75:181–200. doi:10.1146/annurev-physiol-030212-183811
Bessac BF, Jordt S-E (2008) Breathtaking TRP channels: TRPA1 and TRPV1 in airway chemosensation and reflex control. Physiology (Bethesda) 23:360–70. doi:10.1152/physiol.00026.2008
Bessac BF, Sivula M, von Hehn CA, Escalera J, Cohn L, Jordt S-E (2008) TRPA1 is a major oxidant sensor in murine airway sensory neurons. J Clin Invest 118:1899–1910. doi:10.1172/JCI34192
Black BL, Olson EN (1998) Transcriptional control of muscle development by myocyte enhancer factor-2 (MEF2) proteins. Annu Rev Cell Dev Biol 14:167–96. doi:10.1146/annurev.cellbio.14.1.167
Brierley SM, Castro J, Harrington AM, Hughes PA, Page AJ, Rychkov GY, Blackshaw LA (2011) TRPA1 contributes to specific mechanically activated currents and sensory neuron mechanical hypersensitivity. J Physiol 589:3575–93. doi:10.1113/jphysiol.2011.206789
Chen J, Joshi SK, DiDomenico S, Perner RJ, Mikusa JP, Gauvin DM, Segreti JA, Han P, Zhang X-F et al (2011) Selective blockade of TRPA1 channel attenuates pathological pain without altering noxious cold sensation or body temperature regulation. Pain 152:1165–72. doi:10.1016/j.pain.2011.01.049
Constantin B, Cognard C, Raymond G (1996) Myoblast fusion requires cytosolic calcium elevation but not activation of voltage-dependent calcium channels. Cell Calcium 19:365–74
David JD, See WM, Higginbotham CA (1981) Fusion of chick embryo skeletal myoblasts: role of calcium influx preceding membrane union. Dev Biol 82:297–307
Eberhardt M, Dux M, Namer B, Miljkovic J, Cordasic N, Will C, Kichko TI, de la Roche J, Fischer M et al (2014) H2S and NO cooperatively regulate vascular tone by activating a neuroendocrine HNO–TRPA1–CGRP signalling pathway. Nat Commun 5:4381
Eid SR, Crown ED, Moore EL, Liang HA, Choong K-C, Dima S, Henze DA, Kane SA, Urban MO (2008) HC-030031, a TRPA1 selective antagonist, attenuates inflammatory- and neuropathy-induced mechanical hypersensitivity. Mol Pain 4:48. doi:10.1186/1744-8069-4-48
Filippin LI, Cuevas MJ, Lima E, Marroni NP, Gonzalez-Gallego J, Xavier RM (2011) Nitric oxide regulates the repair of injured skeletal muscle. Nitric Oxide Biol Chem 24:43–9. doi:10.1016/j.niox.2010.11.003
Filippin LI, Moreira AJ, Marroni NP, Xavier RM (2009) Nitric oxide and repair of skeletal muscle injury. Nitric Oxide Biol Chem 21:157–63. doi:10.1016/j.niox.2009.08.002
Griffin CA, Apponi LH, Long KK, Pavlath GK (2010) Chemokine expression and control of muscle cell migration during myogenesis. J Cell Sci 123:3052–60. doi:10.1242/jcs.066241
Griffin CA, Kafadar KA, Pavlath GK (2009) MOR23 promotes muscle regeneration and regulates cell adhesion and migration. Dev Cell 7:649–61. doi:10.1016/j.devcel.2009.09.004
Hannon K, Kudla AJ, McAvoy MJ, Clase KL, Olwin BB (1996) Differentially expressed fibroblast growth factors regulate skeletal muscle development through autocrine and paracrine mechanisms. J Cell Biol 132:1151–9
Hara M, Tabata K, Suzuki T, Do M-KQ, Mizunoya W, Nakamura M, Nishimura S, Tabata S, Ikeuchi Y et al (2012) Calcium influx through a possible coupling of cation channels impacts skeletal muscle satellite cell activation in response to mechanical stretch. Am J Physiol Cell Physiol 302:C1741–50. doi:10.1152/ajpcell.00068.2012
Hindi SM, Tajrishi MM, Kumar A (2013) Signaling mechanisms in mammalian myoblast fusion. Sci Signal 6:re2. doi:10.1126/scisignal.2003832
Horsley V, Friday BB, Matteson S, Kegley KM, Gephart J, Pavlath GK (2001) Regulation of the growth of multinucleated muscle cells by an NFATC2-dependent pathway. J Cell Biol 153:329–38
Horsley V, Jansen KM, Mills ST, Pavlath GK (2003) IL-4 acts as a myoblast recruitment factor during mammalian muscle growth. Cell 113:483–94
Horsley V, Pavlath GK (2004) Forming a multinucleated cell: molecules that regulate myoblast fusion. Cells Tissues Organs 176:67–78. doi:10.1159/000075028
Jansen KM, Pavlath GK (2006) Mannose receptor regulates myoblast motility and muscle growth. J Cell Biol 174:403–413
Jordt S-E, Bautista DM, Chuang H-H, McKemy DD, Zygmunt PM, Högestätt ED, Meng ID, Julius D (2004) Mustard oils and cannabinoids excite sensory nerve fibres through the TRP channel ANKTM1. Nature 427:260–5. doi:10.1038/nature02282
Karashima Y, Talavera K, Everaerts W, Janssens A, Kwan KY, Vennekens R, Nilius B, Voets T (2009) TRPA1 acts as a cold sensor in vitro and in vivo. Proc Natl Acad Sci U S A 106:1273–8. doi:10.1073/pnas.0808487106
Kolluru GK, Shen X, Kevil CG (2013) A tale of two gases: NO and H2S, foes or friends for life? Redox Biol 1:313–318. doi:10.1016/j.redox.2013.05.001
Lafreniere JF, Mills P, Bouchentouf M, Tremblay JP (2006) Interleukin-4 improves the migration of human myogenic precursor cells in vitro and in vivo. Exp Cell Res 312:1127–41. doi:10.1016/j.yexcr.2006.01.002
Lee SP, Buber MT, Yang Q, Cerne R, Cortés RY, Sprous DG, Bryant RW (2008) Thymol and related alkyl phenols activate the hTRPA1 channel. Br J Pharmacol 153:1739–49. doi:10.1038/bjp.2008.85
Leloup L, Mazères G, Daury L, Cottin P, Brustis J-J (2006) Involvement of calpains in growth factor-mediated migration. Int J Biochem Cell Biol 38:2049–63. doi:10.1016/j.biocel.2006.04.012
Lennertz RC, Kossyreva EA, Smith AK, Stucky CL (2012) TRPA1 mediates mechanical sensitization in nociceptors during inflammation. PLoS One 7:e43597. doi:10.1371/journal.pone.0043597
Lepper C, Partridge TA, Fan C-M (2011) An absolute requirement for Pax7-positive satellite cells in acute injury-induced skeletal muscle regeneration. Development 138:3639–46. doi:10.1242/dev.067595
Louis M, Zanou N, Van Schoor M, Gailly P (2008) TRPC1 regulates skeletal myoblast migration and differentiation. J Cell Sci 121:3951–9. doi:10.1242/jcs.037218
Lowenstein CJ, Dinerman JL, Snyder SH (1994) Nitric oxide: a physiologic messenger. Ann Intern Med 120:227–37
Lübbert M, Kyereme J, Schöbel N, Beltrán L, Wetzel CH, Hatt H (2013) Transient receptor potential channels encode volatile chemicals sensed by rat trigeminal ganglion neurons. PLoS One 8:e77998. doi:10.1371/journal.pone.0077998
Macpherson LJ, Dubin AE, Evans MJ, Marr F, Schultz PG, Cravatt BF, Patapoutian A (2007) Noxious compounds activate TRPA1 ion channels through covalent modification of cysteines. Nature 445:541–5. doi:10.1038/nature05544
Mann CJ, Perdiguero E, Kharraz Y, Aguilar S, Pessina P, Serrano AL, Muñoz-Cánoves P (2011) Aberrant repair and fibrosis development in skeletal muscle. Skelet Muscle 1:21. doi:10.1186/2044-5040-1-21
Mauro A (1961) Satellite cell of skeletal muscle fibers. J Biophys Biochem Cytol 9:493–5
McNamara CR, Mandel-Brehm J, Bautista DM, Siemens J, Deranian KL, Zhao M, Hayward NJ, Chong JA, Julius D et al (2007) TRPA1 mediates formalin-induced pain. Proc Natl Acad Sci U S A 104:13525–30. doi:10.1073/pnas.0705924104
Molkentin JD, Olson EN (1996) Combinatorial control of muscle development by basic helix-loop-helix and MADS-box transcription factors. Proc Natl Acad Sci U S A 93:9366–9373
Nilius B, Appendino G, Owsianik G (2012) The transient receptor potential channel TRPA1: from gene to pathophysiology. Pflugers Arch 464:425–58. doi:10.1007/s00424-012-1158-z
Nilius B, Prenen J, Owsianik G (2011) Irritating channels: the case of TRPA1. J Physiol 589:1543–9. doi:10.1113/jphysiol.2010.200717
Nishida Y, Miyamori H, Thompson EW, Takino T, Endo Y, Sato H (2008) Activation of matrix metalloproteinase-2 (MMP-2) by membrane type 1 matrix metalloproteinase through an artificial receptor for proMMP-2 generates active MMP-2. Cancer Res 68:9096–104. doi:10.1158/0008-5472.CAN-08-2522
Okajima F (2013) Regulation of inflammation by extracellular acidification and proton-sensing GPCRs. Cell Signal 25:2263–2271. doi:10.1016/j.cellsig.2013.07.022
Paulsen G, Crameri R, Benestad HB, Fjeld JG, Mørkrid L, Hallén J, Raastad T (2010) Time course of leukocyte accumulation in human muscle after eccentric exercise. Med Sci Sports Exerc 42:75–85. doi:10.1249/MSS.0b013e3181ac7adb
Pfaffl MW (2001) A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res 29:e45
Philippou A, Halapas A, Maridaki M, Koutsilieris M (2007) Type I insulin-like growth factor receptor signaling in skeletal muscle regeneration and hypertrophy. J Musculoskelet Nueronal Interact 7:208–18
Przybylski RJ, Szigeti V, Davidheiser S, Kirby AC (1994) Calcium regulation of skeletal myogenesis. II. Extracellular and cell surface effects. Cell Calcium 15:132–42
Rigamonti E, Touvier T, Clementi E, Manfredi AA, Brunelli S, Rovere-Querini P (2013) Requirement of inducible nitric oxide synthase for skeletal muscle regeneration after acute damage. J Immunol 190:1767–77. doi:10.4049/jimmunol.1202903
Roche J, Eberhardt MJ, Klinger AB, Stanslowsky N, Wegner F, Koppert W, Reeh PW, Lampert A, Fischer MJM et al (2013) The molecular basis for species-specific activation of human TRPA1 protein by protons involves poorly conserved residues within transmembrane domains 5 and 6. J Biol Chem 288:20280–20292. doi:10.1074/jbc.M113.479337
Rubinstein I, Abassi Z, Coleman R, Milman F, Winaver J, Better OS (1998) Involvement of nitric oxide system in experimental muscle crush injury. J Clin Invest 101:1325–33. doi:10.1172/JCI810
Sambasivan R, Yao R, Kissenpfennig A, Van Wittenberghe L, Paldi A, Gayraud-Morel B, Guenou H, Malissen B, Tajbakhsh S et al (2011) Pax7-expressing satellite cells are indispensable for adult skeletal muscle regeneration. Development 138:3647–56. doi:10.1242/dev.067587
Sheehan SM, Tatsumi R, Temm-Grove CJ, Allen RE (2000) HGF is an autocrine growth factor for skeletal muscle satellite cells in vitro. Muscle Nerve 23:239–45
Stern-Straeter J, Bonaterra GA, Hörmann K, Kinscherf R, Goessler UR (2009) Identification of valid reference genes during the differentiation of human myoblasts. BMC Mol Biol 10:66. doi:10.1186/1471-2199-10-66
Takahashi N, Mizuno Y, Kozai D, Yamamoto S, Kiyonaka S, Shibata T, Uchida K, Mori Y (2008) Molecular characterization of TRPA1 channel activation by cysteine-reactive inflammatory mediators. Channels 2:287–98
Tatsumi R, Anderson JE, Nevoret CJ, Halevy O, Allen RE (1998) HGF/SF is present in normal adult skeletal muscle and is capable of activating satellite cells. Dev Biol 194:114–28. doi:10.1006/dbio.1997.8803
Tatsumi R, Liu X, Pulido A, Morales M, Sakata T, Dial S, Hattori A, Ikeuchi Y, Allen RE (2006) Satellite cell activation in stretched skeletal muscle and the role of nitric oxide and hepatocyte growth factor. Am J Physiol Cell Physiol 290:C1487–94. doi:10.1152/ajpcell.00513.2005
Tatsumi R, Wuollet AL, Tabata K, Nishimura S, Tabata S, Mizunoya W, Ikeuchi Y, Allen RE (2009) A role for calcium-calmodulin in regulating nitric oxide production during skeletal muscle satellite cell activation. Am J Physiol Cell Physiol 296:C922–9. doi:10.1152/ajpcell.00471.2008
Taylor-Clark TE, Undem BJ, Macglashan DW, Ghatta S, Carr MJ, McAlexander MA (2008) Prostaglandin-induced activation of nociceptive neurons via direct interaction with transient receptor potential A1 (TRPA1). Mol Pharmacol 73:274–81. doi:10.1124/mol.107.040832
Vay L, Gu C, McNaughton PA (2012) The thermo-TRP ion channel family: properties and therapeutic implications. Br J Pharmacol 165:787–801. doi:10.1111/j.1476-5381.2011.01601.x
Vilceanu D, Stucky CL (2010) TRPA1 mediates mechanical currents in the plasma membrane of mouse sensory neurons. PLoS One 5:e12177. doi:10.1371/journal.pone.0012177
Wang YX, Rudnicki MA (2011) Satellite cells, the engines of muscle repair. Nat Rev Mol Cell Biol 5:1–7. doi:10.1038/nrm3265
Yamada M, Sankoda Y, Tatsumi R, Mizunoya W, Ikeuchi Y, Sunagawa K, Allen RE (2008) Matrix metalloproteinase-2 mediates stretch-induced activation of skeletal muscle satellite cells in a nitric oxide-dependent manner. Int J Biochem Cell Biol 40:2183–91. doi:10.1016/j.biocel.2008.02.017
Acknowledgments
We thank S. Pyschny and Uta Müller for technical assistance and S. Kurtenbach and M. Lübbert for comments on the manuscript. We also thank F. Entschladen and the Institute for Immunology (Witten/Herdecke) for their support with the migration assays. We thank the Muscle Tissue Culture Collection MTCC for providing human myoblast cultures. The Muscle Tissue Culture Collection is part of the German network on muscular dystrophies (MD-NET) and the German network for mitochondrial disorders (mito-NET, project D2, 01GM1113A) funded by the German ministry of education and research (BMBF, Bonn, Germany). The Muscle Tissue Culture Collection is a partner of EuroBioBank (www.eurobiobank.org) and TREAT-NMD (www.treat-nmd.eu). We also thank the Sonderforschungsbereich 642 for their financial support.
Author contributions
Experiment design: MO, HH. Performed the experiments: MO, SO, MB, BK. Analyzed the data: MO, MB. Wrote the paper: MO, SO, HH.
Ethical standards
All experiments comply with the current laws of the Federal Republic of Germany.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Osterloh, M., Böhm, M., Kalbe, B. et al. Identification and functional characterization of TRPA1 in human myoblasts. Pflugers Arch - Eur J Physiol 468, 321–333 (2016). https://doi.org/10.1007/s00424-015-1729-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-015-1729-x