Abstract
Purpose
We hypothesized that lower body microvessels are particularly challenged during exposure to gravity and hypergravity leading to failure of resistance vessels to withstand excessive transmural pressure during hypergravitation and gravitation-dependent microvascular blood pooling.
Methods
Using a short-arm human centrifuge (SAHC), 12 subjects were exposed to +1Gz, +2Gz and +1Gz, all at foot level, for 4 min each. Laser Doppler imaging and near-infrared spectroscopy were used to measure skin perfusion and tissue haemoglobin concentrations, respectively.
Results
Pretibial skin perfusion decreased by 19 % during +1Gz and remained at this level during +2Gz. In the dilated area, skin perfusion increased by 24 and 35 % during +1Gz and +2Gz, respectively. In the upper arm, oxygenated haemoglobin (Hb) decreased, while deoxy Hb increased with little change in total Hb. In the calf muscle, O2Hb and deoxy Hb increased, resulting in total Hb increase by 7.5 ± 1.4 and 26.6 ± 2.6 µmol/L at +1Gz and +2Gz, respectively. The dynamics of Hb increase suggests a fast and a slow component.
Conclusion
Despite transmural pressures well beyond the upper myogenic control limit, intact lower body resistance vessels withstand these pressures up to +2Gz, suggesting that myogenic control may contribute only little to increased vascular resistance. The fast component of increasing total Hb indicates microvascular blood pooling contributing to soft tissue capacitance. Future research will have to address possible alterations of these acute adaptations to gravity after deconditioning by exposure to micro-g.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Humans are generally well adapted to the upright posture which started approximately 4.5 million years ago (Tattersall and Matternes 1992). Yet, orthostatic cardiovascular dysfunction occurs in a number of disease conditions (Groothuis et al. 2010, 2011a, b; Verheyden et al. 2008) in patients after prolonged confinement to bed rest (Wieser et al. 2014) and in astronauts after prolonged exposure to microgravity (Fritsch-Yelle et al. 1994, 1996) and is not uncommon even in healthy individuals (Fu et al. 2012; Ganzeboom et al. 2003; Serletis et al. 2006).
The focus of previous studies concerning cardiovascular deconditioning after bed rest or exposure to microgravity has been primarily directed at studying changes in blood volume (Maillet et al. 1996; Millet et al. 2001), a putative reduction of the baroreceptor reflex sensitivity (Adami et al. 2013; Robertson et al. 1994; Shoemaker et al. 2003), and the activity of sympathetic efferent fibres to peripheral, mostly muscle, blood vessels (Kamiya et al. 1999, 2000; Shoemaker et al. 1999). Also, an increase in venous and soft tissue capacitance has been associated with orthostatic intolerance after bed rest (Arbeille et al. 2008, 2012; Capri et al. 2004; Kerbeci et al. 2007). However, the sum of the observed alterations does not seem to suffice to explain the marked orthostatic intolerance after exposure to micro-g or head-down bed rest (HDBR). Only few studies have focused on the possibility of altered resistance vessel reactivity to sympathetic or other vasoactive stimuli. In these studies, the α-adrenergic receptor-mediated constriction of cutaneous resistance vessels seems to be maintained after HDBR (Kamiya et al. 2004), while flow-induced vasodilation of the radial and femoral artery was increased (Bonnin et al. 2001; van Duijnhoven et al. 2010).
A different challenge to the cardiovascular system occurs in jet fighter pilots, who are exposed to transient periods of hypergravity, which may exceed the counter-regulatory capacity of the cardiovascular system. This may result in a fall of central arterial blood pressure, compromising cerebral perfusion (Siitonen et al. 2003) to an extent, such that blur of vision and loss of consciousness occur (Sevilla and Gardner 2005). Repetitive exposure to hypergravity, as in the case of fighter pilots, during simulated air combat manoeuvres or centrifuge exposition, seems to stimulate adaptive responses, which enhance the tolerance of the cardiovascular system during gravitational stress (Convertino 1998; Lalande and Buick 2009; Newman and Callister 2008; Newman et al. 1998). To date, this adaptation is attributed to an increased baroreceptor reflex sensitivity (Newman et al. 1998). Whether an increased vasoconstrictor capacity of lower body microvasculature may contribute to this increased tolerance to hypergravity has not been investigated.
Thus, despite the indispensible contribution of resistance vessels to the maintenance of blood pressure during gravitational challenges, detailed knowledge about altered microvascular responsiveness after cardiovascular deconditioning and possible limits of their ability to withstand the unphysiologically high transmural pressures during exposure to hypergravity is lacking. The aim of this study, therefore, was to comprehensively characterize the acute microvascular responses to gravity and hypergravity induced by a short-arm human centrifuge (SAHC) in healthy young human subjects. The focus was on lower body microvessels which are particularly challenged by markedly increased transmural pressures on both the arterial and venous branches of the vasculature. Arterial resistance vessels are known to respond to this increased pressure load by vasoconstriction mediated by a combination of local myogenic and systemic sympathetic mechanisms. However, the upper pressure limit of myogenic perfusion control is limited to about 160 mmHg (Bullivant 1978; Strandgaard et al. 1974) and the pressures induced by hypergravity well exceed this upper limit (Watenpaugh et al. 2004). We, therefore, hypothesized that constriction of lower body resistance vessels would suffice to maintain or even decrease skin perfusion during exposure to normal gravity, but would fail to withstand the high transmural pressures during hypergravitation, resulting in an increase of skin perfusion. To test this hypothesis, we measured the pretibial skin perfusion by laser Doppler imaging and combined this with iontophoretic drug application to appreciate the difference between intact resistance vessels actively responding to the orthostatic challenge with paralysed vessels which would distend passively due to increased transmural pressure.
Lower body veins serve as capacitance vessels and are responsible for the blood pooling during orthostatic challenge. However, previous studies also identified increased fluid accumulation in soft tissue as a risk factor for orthostatic intolerance (Arbeille et al. 2008). We hypothesized that this soft tissue capacitance is at least partly due to blood pooling in venous microvessels, which would be obvious from increased tissue haemoglobin concentration. This was quantified by measuring changes in muscle haemoglobin concentration using near-infrared spectroscopy (NIRS).
Methods
In performing this experiment, 12 civilian volunteers (7 females, 5 males) without a history of cardiovascular or metabolic disease were recruited. Written informed consent was obtained from all subjects before participating in this study. The study procedures were approved by the Ethics Committee of the Medical Council North Rhine and all experiments were performed in accordance with the Declaration of Helsinki. The age of the subjects ranged between 21 and 36 years (mean ± standard deviation 28.4 ± 3.9). The mean height was 176 ± 6 cm and mean weight was 72 ± 7 kg.
Subjects were screened by an independent physician who was not involved in the study. Screening comprised resting ECG, Schellong test, blood test and cycle ergometry as well as a medical questionnaire/examination to determine whether medical reasons, such as arrhythmia, syncope or other orthostatic abnormalities precluded participation in the study. Tests and exclusion criteria followed the guidelines of the German Aerospace Agency as applied for determination of aviation fitness required for private pilots. All subjects were cleared for centrifuge testing.
Experiments were performed at the facilities of the German Aerospace Center (Deutsches Zentrum für Luft- und Raumfahrt, DLR) in Cologne, Germany. Prior to the experiments, a final health examination was undertaken by an independent physician to ensure that no subject was showing any evidence of disease.
Haemodynamic monitoring
Non-invasive continuous cardiovascular monitoring and data storage were performed during the entirety of the experiment using a Portapres monitor via Beatscope software (BMI-TNO, Amsterdam, The Netherlands). The recorded parameters (sampling rate 2000 Hz) included heart rate (HR) by electrocardiogram (ECG), blood pressure (systolic (SBP), diastolic (DBP) and mean (MAP) by finger plethysmography and at 5 min intervals by an automatically inflated upper arm oscillometric pressure cuff to adjust the output from the plethysmographic measurements. The hand carrying the plethysmographic finger cuff was fixed in a sling at the assumed plane of orthostatic indifference at the base of the heart (Watenpaugh et al. 2004). Stroke volume (SV) was assessed by thoracic impedance technology (NICO100C, Biopac Systems, Goleta, CA, USA). From these parameters, cardiac output (CO) and total peripheral resistance (TPR) were derived at beat to beat frequency.
Near-infrared spectroscopy (NIRS)
Microvascular blood pooling was determined in the right gastrocnemius muscle by near-infrared spectroscopy (NIRO 200, Hamamatsu Instruments, Hamamatsu, Japan). To this end, a pair of optodes (emitter and detector) was fixed to the lateral head of the gastrocnemius muscle by a black rubber scaffold which ensured a constant distance of 4 cm between both optodes by means of a double-sided adhesive disc. The differential path length factor was set at 4.5, resulting in an assumed path length of 18 cm. The concentration changes of oxygenated (O2Hb) and deoxygenated haemoglobin (deoxyHb) as well as regional oxygen saturation (rSO2) were continuously recorded at a sampling rate of 1 Hz. Changes in total haemoglobin concentration were calculated (O2Hb + deoxyHb) off-line. A second pair of optodes was placed on the distal biceps muscle, close to the plane of orthostatic indifference and served as control.
Laser Doppler imaging and iontophoresis
Pretibial skin perfusion approximately 25 cm proximal to the ankle was measured by laser Doppler imaging (Periscan PIM3, Perimed, Uppsala, Sweden). The observation area was shaved and defatted with alcoholic disinfectant. The scanner was mounted to the centrifuge platform to ensure optimal stability. The scanned area was 10.3 ± 0.1 cm long and 1.9 ± 0.1 cm wide. The average duration of a complete scan was 12.7 ± 0.7 s, resulting in a temporal resolution of 4.9 ± 0.3 scans per min. In the centre of the area, an iontophoresis chamber was fixed with a double-sided adhesive disc and filled with 1 % solution of freshly dissolved sodium nitroprusside (Nipruss, Schwarz Pharma, Monheim, Germany). An adhesive reference electrode was placed about 20 cm distally to the chamber. Iontophoresis with 100 µA was started 20 min prior to centrifugation and continued throughout the duration of the protocol. For data analysis, three regions of interest (ROI) were defined: one within the iontophoresis chamber and one each at the distal and proximal ends of the scanned area. No differences between the proximal and distal control areas were detected and the values were averaged. Since centrifugation induced a distal movement of the legs, the three ROIs were moved simultaneously such that the central ROI always covered the whole iontophoretic chamber area. Mean laser Doppler flux from each of the ROIs was averaged over the last four to five scans (about 1 min) during each experimental phase.
Short-arm human centrifuge
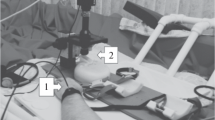
The short-arm human centrifuge (SAHC-TN-007-VE, QinetiQ Company, Antwerp, Belgium) can generate acceleration forces from +0.1Gz to +5Gz, where Gz represents the artificial gravitational force acting on the test subject along the selected body axis. It has a maximum swing radius of 2.82 m and a maximum angular velocity of 40 RPM. The maximal G-acceleration rate is 0.25 G/s. For our protocol, the test subjects assumed a supine position while undergoing acceleration, such that the resulting vector of gravitational force was along the longitudinal z-axis, or from head to foot. Ambient temperature in the SAHC testing chamber was maintained at 23–25 °C. To prevent convective cooling, transparent air flow shields were placed on either side of the centrifuge table and additionally covered with transparent polymer foil fixed to the shields with adhesive tape. Thus, subjects were fully encased and protected from air flow due to centrifugation. The head of the subjects was placed within a light tight chamber to eliminate external visual stimuli. This chamber was equipped with a light source and infrared camera, and subjects were equipped with a microphone headset, allowing for continuous communication with the independent physician. Additionally a “panic button” was made readily accessible to each subject.
The independent physician monitored the subjects’ condition by camera view of their faces, continuous display of haemodynamic variables and by direct verbal communication. Centrifugation runs were immediately terminated on the decision of this physician based on request by the subjects, facial sweating or haemodynamic instability.
Each subject was placed in the SAHC with the heels against the foot plate, securely restrained via safety harness and then instrumented with all monitoring and measuring devices. Subjects were instructed to relax their leg muscles throughout the baseline and centrifugation periods so as not to interfere with the NIRS measurements. After the final uplink and safety check was completed by the command team before leaving the centrifuge area, an “all clear” signal was given and the subjects verbalized their readiness, the experiment could begin.
Experimental protocol
The protocol started with 20 min at +0Gz for stabilization. Then the SAHC was accelerated by +1Gz, +2Gz and +1Gz, all at the subject’s foot level for 4 min each and then decelerated to 0Gz. The shifts between Gz phases lasted about 10 s.
Data analyses and statistics
Data were averaged over the last 30 s of each acceleration phase unless stated otherwise. Statistical analyses were performed with SigmaStat (Systat Software, Inc., San Jose, CA). Data are presented as mean ± standard error. Data were tested for normality prior to statistical comparisons by Kolmogorov–Smirnov test and analysed by one-way repeated measures ANOVA followed by Holm–Sidak post hoc test. p < 0.05 was considered to be statistically significant.
Results
Haemodynamics
The effects of gravitation on macro-haemodynamic parameters are listed in Table 1. Heart rate increased significantly only at +2Gz. Arterial pressure was maintained at or above baseline throughout the protocol. Stroke volume and cardiac output decreased with increasing acceleration. A significant increase in total peripheral resistance was observed only during the +2Gz phase.
Near-infrared spectroscopy (NIRS)
In the control area in the biceps, centrifugation induced a gravitation-dependent increase in deoxygenated Hb (deoxy Hb) concentration, mirrored by a similar decrease in the concentration of oxygenated Hb (O2Hb) (Fig. 1). Total Hb (tHb) concentration was only minimally affected, while regional oxygen saturation (rSO2) decreased according to the gravitational stimulus. After return to +0Gz, all values returned to baseline. In the gastrocnemius, O2Hb only increased slightly at +2Gz. Deoxy Hb increased moderately at +1Gz by 7.4 ± 1.0 µM and more pronounced to 23.4 ± 1.7 µM at +2Gz. After return to +1Gz, deoxy Hb decreased only slightly to 18.9 ± 1.4 µM but returned to baseline after 5 min of rest at +0Gz. Accordingly, tHb increased by 7.5 ± 1.4 µM at +1Gz, further to 26.6 µM at +2Gz and decreased only moderately after return to +1Gz to 18.8 ± 1.8 µM. Gastrocnemius rSO2 decreased only minimally at +1Gz, but markedly at +2Gz and remained low after return to +1Gz.
The results of the NIRS measurements are presented. a Biceps muscle deoxygenated haemoglobin concentration is (deoxy Hb) in blue and oxygenated haemoglobin (O2Hb) concentration in red. b The same as in a for gastrocnemius muscle. c Total haemoglobin (tHb) concentration for gatrocnemius and biceps muscles. d Regional oxygen saturation (rSO2) for gastrocnemius and biceps muscles. All data are mean ± SE. *p < 0.05 versus initial +0Gz, # p < 0.05 versus first +1Gz, $ p < 0.05 versus +2Gz
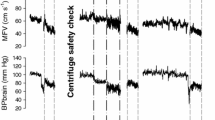
To analyse the dynamics of muscle microvascular blood pooling, tHb concentration changes were normalized to peak value at the end of the +2Gz phase and averaged in 30 s intervals (Fig. 2, upper panel). After onset of +1Gz, a rapid accumulation of tHb in muscle tissue within the first 30 s was obvious. This was followed by a slow incremental increase, which does not reach a steady state until the end of the 4 min centrifugation phase. After acceleration to +2Gz, a steady but more pronounced increase of tHb can be observed, which again does not reach a steady state within the 4 min time interval. Reduction of acceleration from +2Gz to +1Gz induces a quick drop in muscle tHb, which plateaus at more than twice the value of the initial +1Gz phase. After return to +0Gz, tHb quickly drops to near baseline values.
Time course of total haemoglobin accumulation in the gastrocnemius muscle during the whole centrifugation protocol. Upper panel the tHb concentration was normalized to the individual maxima at the end of the +2Gz phase and determined in 30 s intervals. The three experimental phases with +1Gz, +2Gz and again +1Gz are represented by the shaded areas; mean ± SE. Lower panel bi-exponential fits (solid lines) were applied to the mean normalised tHb values during +1Gz (grey) and +2Gz (black). The fast component of tHb increase is represented by short dashed lines and the slow component by long dashed lines. The resulting maximum relative tHb concentration is given above each line. R 2 = 0.9995 for +1Gz and 0.9997 for +2Gz
To estimate the time course of tHb increase beyond the 4 min observation period, curves assuming a bi-exponential rise to maximum were fitted to the data (Fig. 2, lower panel) (Uhlig and von Bethmann 1997). This two-component model was chosen to reflect both the fast initial and the slower delayed increase in tHb and provided R > 0.999 for both +1Gz and +2Gz. Interestingly, the maximum relative tHb concentration estimated for +1Gz of 0.70 coincided with the plateau values measured after reduction from +2Gz to +1Gz of also 0.70.
Skin perfusion by laser Doppler imaging and iontophoresis
Iontophoresis of sodium nitroprusside induced a 4.4-fold increase in skin perfusion from 38 ± 2 to 168 ± 11 perfusion units (PU), while perfusion in the untreated control areas remained essentially unchanged (Fig. 3). Application of +1Gz increased perfusion in the dilated area further to 208 ± 14 PU. In contrast, control area perfusion decreased by 19 % from 58 ± 5 to 47 ± 3 PU. Acceleration to +2Gz further increased perfusion in the dilated area to 226 ± 16 PU, while no further change occurred in the control areas. Return to +1Gz reduced perfusion in the dilated area to the level of the initial +1Gz phase, while again no change occurred in the control areas. After termination of +Gz acceleration, all perfusion values essentially returned to the initial +0Gz levels.
Pretibial skin perfusion measured as laser Doppler flux (LDF) in arbitrary perfusion units (PU) at untreated control areas and skin areas where resistance vessels were dilated by iontophoretic application of Na nitroprusside. To better appreciate the changes in control areas, a break was introduced in the y-axis with different scalings for control areas and dilated areas. All data are mean ± SE. *p < 0.05 versus initial +0Gz, # p < 0.05 versus first +1Gz, $ p < 0.05 versus +2Gz
Discussion
The major results of this study, which investigated the microvascular responses to gravity and hypergravity using an SAHC were that: (1) constriction of resistance vessels in response to gravity can help withstand the high transmural pressures not only at +1Gz, but also at +2Gz for 4 min, and thus contributes to the maintenance of mean arterial pressure during exposure to moderate hypergravity; (2) microvascular blood pooling seems to contribute to soft tissue capacitance during orthostatic challenge and can be quantified with NIRS measurement of total tissue haemoglobin concentration.
Numerous previous studies have elucidated the haemodynamic responses to gravity and, fewer, to hypergravity. It is well understood that gravitational forces along the body axis lead to venous blood pooling in the lower body which reduces cardiac preload and thus stroke volume. Baroreceptor reflex activity counteracts the resulting decrease in arterial pressure by increasing heart rate and total peripheral resistance to maintain arterial pressure. The haemodynamic responses correspond to the well-known physiology of cardiovascular adaptation to gravity and were much more pronounced after the shift from +1Gz to +2Gz as compared to the changes from 0Gz to +1Gz. Namely, heart rate increased only slightly by 5 bpm during +1Gz, but was much more pronounced by a further 23 bpm after acceleration from +1Gz to +2Gz. This moderate sympathetic activation is certainly due to the use of the SAHC where the respective G+ levels were achieved at foot level and gravitational forces were much lower at more proximal body parts. Accordingly, the heart rate increased considerably more during exposure to +1Gz on a long-arm centrifuge or during tilt table testing as compared to SAHC (Watenpaugh et al. 2004). Non-linear dynamics of gravitation-dependent haemodynamic changes similar to those given in Table 1 have also been reported for long-arm centrifuges (Bonjour et al. 2011).
The focus of this study, however, was on microvascular responses, namely in the lower body, in which blood vessels are exposed to dramatically increased transmural pressures as a result of the effect of gravity on the intravascular blood volume. It has been suggested that resistance vessels would respond by vasoconstriction through the combined effects of two mechanisms: local myogenic response to increased transmural pressure (Groothuis et al. 2011b) and a systemic α-adrenergic receptor-mediated constriction due to baroreceptor reflex-induced sympathetic activation (Shoemaker et al. 1999). Such constriction should result in parallel decrease of perfusion, because the arterial to venous pressure gradient is only minimally affected by gravity. Accordingly, during +1Gz, we detected a decrease of pretibial skin perfusion by 19 %, indicating substantial resistance vessel constriction. This is considerably less than the almost 40 % decrease observed by Watenpaugh et al. (2004) under similar conditions. Whether a different technique of measuring skin perfusion, laser Doppler flux versus laser Doppler imaging, or a different centrifugation protocol suffices to explain this discrepancy remains unclear.
Increasing the acceleration to +2Gz induced no further change in skin perfusion, indicating that resistance vessels were able to maintain their diameters against the increased transmural pressure, but did not constrict further despite that both constrictive stimuli, that is transmural pressure and sympathetic activation, as evident from the increase in heart rate, increased markedly. However, at +2Gz, with a mean arterial pressure of 100 mmHg at heart level, the local arterial pressure at the pretibial skin well exceeded 200 mmHg (Watenpaugh et al. 2004) and was thus above the upper limit of myogenic autoregulation, beyond which even renal or cerebral perfusion increases with pressure (Bullivant 1978; Strandgaard et al. 1974). Either myogenic control contributes only little to the maintenance of vessel tone in skin or increased sympathetic vasoconstriction was able to maintain flow resistance beyond this autoregulatory pressure range.
To better appreciate the ability of resistance vessels to withstand increasing transmural pressure, skin perfusion was also measured in areas treated with iontophoretic application of the potent vasodilator sodium nitroprusside. As expected, the gravitational-induced rise of transmural pressure in resistance vessels increased skin perfusion by 24 % at +1Gz and by an additional 9 % at +2Gz versus +1Gz, indicating passive distension of vessels. The striking difference between these relative increases during identical increments of transmural pressure may be explained by the nonlinear pressure–diameter relationship of dilated resistance vessels. (Cornelissen et al. 2000). The expected diameter increases correspond well to the observed increases in skin perfusion.
NIRS measurement of haemoglobin concentration has been used previously during tilt table testing to determine the pressure–volume relationship of calf muscle microvasculature (Binzoni et al. 2000). For a reference control area, a second probe was placed on the distal aspect of the biceps muscle that is roughly at the hydrostatic indifference level and should thus not be exposed to local pressure changes during acceleration. The observed alterations, decrease in total haemoglobin and O2Hb concentration while deoxy Hb concentration increase, are best explained by increased oxygen extraction due to a reduction of perfusion via sympathetic vasoconstriction of skeletal muscle resistance vessels. In contrast, the gastrocnemius muscle total Hb concentration increased markedly by 7.5 and 26.6 µmol/L at, respectively, +1 and +2Gz, thereby reflecting microvascular blood pooling. Obviously, the bulk of blood pooling occurs in large veins and the microvascular increase of haemoglobin concentration by 26.6 µmol/L at +2Gz equalizes to only 11.4 ml of blood pooling within a volume of 1 L muscle tissue when assuming a mean blood haemoglobin concentration of 15 g/100 mL (Binzoni et al. 2000). Nevertheless, by combining NIRS with the conventional plethysmographic techniques, which reflect total blood pooling, differential effects of interventions such as longtime bed rest or exposure to micro-g on large vein versus microvascular blood pooling might be identified in future studies. The differential changes in deoxy Hb, O2Hb and rSO2 are consistent with the notion that microvascular blood pooling occurs mostly in venules.
A surprising observation was the marked difference between total Hb concentration at +1Gz before and after exposure to +2Gz. The individual courses of haemoglobin concentration changes (not shown) indicated that a steady state was not be reached within the 4 min observation period. Therefore, the dynamics of total Hb concentration changes was analysed at 30 s intervals using normalized Hb values. Total Hb concentrations were still rising at the end of the +1Gz and +2Gz exposure periods of 4 min, but had reached a plateau at about 2 min after deceleration from +2Gz to +1Gz (Fig. 3, upper panel). Since the shapes of these and the individual continuously recorded curves suggest the presence of a fast and a slow filling compartment, a bi-exponential fit was applied to the data. This is analogous to the well-established technique of venous occlusion plethysmography where the fast component represents limb volume increase by venous filling and the slow component volume increase by transvascular fluid filtration. Although the extrapolations from these curves should be interpreted with care, because they are based on only nine data points obtained within 4 min, the fast component of haemoglobin concentration increase in muscle tissue is easily explained by venous filling. The origin of the slow component is less clear. A possible explanation might be a slow increase in muscle microvascular haemoglobin concentration resulting from increased capillary fluid filtration, which would tend to increase blood haemoglobin concentration at the venular end of capillaries. At low venular blood flow velocity due to the combined effects of precapillary vasoconstriction and venular pressure-induced distension, blood in the venules would be slowly replaced by capillary outflow with higher haemoglobin concentration. Indeed, the haemoconcentration of venous blood from the foot has been reported as a response to gravitational pressure increase (Moyses et al. 1987). Simultaneous measurement of limb volume by plethysmography and muscle haemoglobin concentration by NIRS might allow further insights into these events.
In conclusion, lower body resistance vessel smooth muscle tone increased during exposure to gravity and, contrary to our hypothesis, withstood the high transmural pressures even during hypergravitation of +2Gz. As expected, microvascular blood pooling in calf muscle was found to be biphasic with a fast component due to venular filling and a slow component, possibly reflecting either capillary recruitment or enhanced fluid filtration and pooling of blood with higher haemoglobin concentration. We propose that assessment of putative alterations of these acute microvascular adaptations to gravity by long-term exposure to microgravity or its analogue, head-down tilt bed rest, might allow for new insights into the mechanisms of orthostatic dysfunction of astronauts undertaking prolonged spaceflights.
References
Adami A, Pizzinelli P, Bringard A, Capelli C, Malacarne M, Lucini D, Simunic B, Pisot R, Ferretti G (2013) Cardiovascular re-adjustments and baroreflex response during clinical reambulation procedure at the end of 35-day bed rest in humans. Appl Physiol Nutr Metab 38:673–680
Arbeille P, Kerbeci P, Mattar L, Shoemaker JK, Hughson RL (2008) WISE-2005: tibial and gastrocnemius vein and calf tissue response to LBNP after a 60-day bed rest with and without countermeasures. J Appl Physiol (1985) 104:938–943
Arbeille P, Shoemaker K, Kerbeci P, Schneider S, Hargens A, Hughson R (2012) Aortic, cerebral and lower limb arterial and venous response to orthostatic stress after a 60-day bedrest. Eur J Appl Physiol 112:277–284
Binzoni T, Quaresima V, Ferrari M, Hiltbrand E, Cerretelli P (2000) Human calf microvascular compliance measured by near-infrared spectroscopy. J Appl Physiol (1985) 88:369–372
Bonjour J, Bringard A, Antonutto G, Capelli C, Linnarsson D, Pendergast DR, Ferretti G (2011) Effects of acceleration in the Gz axis on human cardiopulmonary responses to exercise. Eur J Appl Physiol 111:2907–2917
Bonnin P, Ben DA, Benessiano J, Maillet A, le Pavy TA, Levy BI (2001) Enhanced flow-dependent vasodilatation after bed rest, a possible mechanism for orthostatic intolerance in humans. Eur J Appl Physiol 85:420–426
Bullivant M (1978) Autoregulation of plasma flow in the isolated perfused rat kidney. J Physiol 280:141–153
Capri A, Kerbeci P, Pascaud L, Arbeille P (2004) Assessment of the calf vein cross section change during stand-test after a 90 day bed rest by echography. J Gravit Physiol 11:83–84
Convertino VA (1998) High sustained +Gz acceleration: physiological adaptation to high-G tolerance. J Gravit Physiol 5:51–54
Cornelissen AJ, Dankelman J, VanBavel E, Stassen HG, Spaan JA (2000) Myogenic reactivity and resistance distribution in the coronary arterial tree: a model study. Am J Physiol Heart Circ Physiol 278:H1490–H1499
Fritsch-Yelle JM, Charles JB, Jones MM, Beightol LA, Eckberg DL (1994) Spaceflight alters autonomic regulation of arterial pressure in humans. J Appl Physiol (1985) 77:1776–1783
Fritsch-Yelle JM, Whitson PA, Bondar RL, Brown TE (1996) Subnormal norepinephrine release relates to presyncope in astronauts after spaceflight. J Appl Physiol (1985) 81:2134–2141
Fu Q, Verheyden B, Wieling W, Levine BD (2012) Cardiac output and sympathetic vasoconstrictor responses during upright tilt to presyncope in healthy humans. J Physiol 590:1839–1848
Ganzeboom KS, Colman N, Reitsma JB, Shen WK, Wieling W (2003) Prevalence and triggers of syncope in medical students. Am J Cardiol 91(1006–8):A8
Groothuis JT, Rongen GA, Geurts AC, Smits P, Hopman MT (2010) Effect of different sympathetic stimuli-autonomic dysreflexia and head-up tilt-on leg vascular resistance in spinal cord injury. Arch Phys Med Rehabil 91:1930–1935
Groothuis JT, Esselink RA, Seeger JP, van Aalst MJ, Hopman MT, Bloem BR (2011a) Lower vascular tone and larger plasma volume in Parkinson’s disease with orthostatic hypotension. J Appl Physiol (1985) 111:443–448
Groothuis JT, Thijssen DH, Lenders JW, Deinum J, Hopman MT (2011b) Leg vasoconstriction during head-up tilt in patients with autonomic failure is not abolished. J Appl Physiol (1985) 110:416–422
Kamiya A, Michikami D, Fu Q, Iwase S, Mano T (1999) Sympathetic vasoconstriction and orthostatic intolerance after simulated microgravity. J Gravit Physiol 6:101–102
Kamiya A, Iwase S, Sugiyama Y, Mano T, Sudoh M (2000) Vasomotor sympathetic nerve activity in men during bed rest and on orthostasis after bed rest. Aviat Space Environ Med 71:142–149
Kamiya A, Michikami D, Iwase S, Hayano J, Kawada T, Sugimachi M, Sunagawa K (2004) Alpha-adrenergic vascular responsiveness to sympathetic nerve activity is intact after head-down bed rest in humans. Am J Physiol Regul Integr Comp Physiol 286:R151–R157
Kerbeci P, Shoemaker K, Hughson R, Roncin A, Arbeille P (2007) Tibial and gastrocnemian vein response to LBNP after a 60 day bedrest with and without counter-measures (WISE study). J Gravit Physiol 14:57–58
Lalande S, Buick F (2009) Physiologic +Gz tolerance responses over successive +Gz exposures in simulated air combat maneuvers. Aviat Space Environ Med 80:1032–1038
Maillet A, Fagette S, Allevard AM, Pavy-Le TA, Guell A, Gharib C, Gauquelin G (1996) Cardiovascular and hormonal response during a 4-week head-down tilt with and without exercise and LBNP countermeasures. J Gravit Physiol 3:37–48
Millet C, Custaud MA, Maillet A, Allevard AM, Duvareille M, Gauquelin-Koch G, Gharib C, Fortrat JO (2001) Endocrine responses to 7 days of head-down bed rest and orthostatic tests in men and women. Clin Physiol 21:172–183
Moyses C, Cederholm-Williams SA, Michel CC (1987) Haemoconcentration and accumulation of white cells in the feet during venous stasis. Int J Microcirc Clin Exp 5:311–320
Newman DG, Callister R (2008) Cardiovascular training effects in fighter pilots induced by occupational high G exposure. Aviat Space Environ Med 79:774–778
Newman DG, White SW, Callister R (1998) Evidence of baroreflex adaptation to repetitive +Gz in fighter pilots. Aviat Space Environ Med 69:446–451
Robertson D, Convertino VA, Vernikos J (1994) The sympathetic nervous system and the physiologic consequences of spaceflight: a hypothesis. Am J Med Sci 308:126–132
Serletis A, Rose S, Sheldon AG, Sheldon RS (2006) Vasovagal syncope in medical students and their first-degree relatives. Eur Heart J 27:1965–1970
Sevilla NL, Gardner JW (2005) G-induced loss of consciousness: case-control study of 78 G-Locs in the F-15, F-16, and A-10. Aviat Space Environ Med 76:370–374
Shoemaker JK, Hogeman CS, Sinoway LI (1999) Contributions of MSNA and stroke volume to orthostatic intolerance following bed rest. Am J Physiol 277:R1084–R1090
Shoemaker JK, Hogeman CS, Sinoway LI (2003) Sympathetic responses to Valsalva’s manoeuvre following bed rest. Can J Appl Physiol 28:342–355
Siitonen SL, Kauppinen T, Leino TK, Vanninen E, Kuronen P, Lansimies E (2003) Cerebral blood flow during acceleration in flight measured with SPECT. Aviat Space Environ Med 74:201–206
Strandgaard S, MacKenzie ET, Sengupta D, Rowan JO, Lassen NA, Harper AM (1974) Upper limit of autoregulation of cerebral blood flow in the baboon. Circ Res 34:435–440
Tattersall I, Matternes JH (1992) The Cambridge encyclopedia of human evolution. Cambridge University Press, New York
Uhlig S, von Bethmann AN (1997) Determination of vascular compliance, interstitial compliance, and capillary filtration coefficient in rat isolated perfused lungs. J Pharmacol Toxicol Methods 37:119–127
van Duijnhoven NT, Thijssen DH, Green DJ, Felsenberg D, Belavy DL, Hopman MT (2010) Resistive exercise versus resistive vibration exercise to counteract vascular adaptations to bed rest. J Appl Physiol (1985) 108:28–33
Verheyden B, Ector H, Aubert AE, Reybrouck T (2008) Tilt training increases the vasoconstrictor reserve in patients with neurally mediated syncope evoked by head-up tilt testing. Eur Heart J 29:1523–1530
Watenpaugh DE, Breit GA, Buckley TM, Ballard RE, Murthy G, Hargens AR (2004) Human cutaneous vascular responses to whole-body tilting, Gz centrifugation, and LBNP. J Appl Physiol (1985) 96:2153–2160
Wieser M, Gisler S, Sarabadani A, Ruest RM, Buetler L, Vallery H, Klamroth-Marganska V, Hund-Georgiadis M, Felder M, Schoenberger JL, Gutknecht C, Riener R (2014) Cardiovascular control and stabilization via inclination and mobilization during bed rest. Med Biol Eng Comput 52:53–64
Acknowledgments
The study was sponsored by a Grant (50WB1123) from Bundesministerium für Wirtschaft und Technologie via Deutsches Zentrum für Luft- und Raumfahrt (German Aerospace Center).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Additional information
Communicated by Massimo Pagani.
Rights and permissions
About this article
Cite this article
Habazettl, H., Stahn, A., Nitsche, A. et al. Microvascular responses to (hyper-)gravitational stress by short-arm human centrifuge: arteriolar vasoconstriction and venous pooling. Eur J Appl Physiol 116, 57–65 (2016). https://doi.org/10.1007/s00421-015-3241-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-015-3241-6