Abstract
Purpose
In the current investigation, the effects of the mTOR inhibitors, Rapa and Torin1 on the TGF-β2-induced conjunctival fibrogenesis were studied.
Study design
Experimental research.
Methods
2D and 3D cultures of HconF were subjected to the following analyses; (1) planar proliferation evaluated by TEER (2D), (2) Seahorse metabolic analyses (2D), (3) subepithelial proliferation evaluated by the 3D spheroids’ size and hardness, and (4) the mRNA expression of ECM proteins and their regulators (2D and 3D).
Result
Rapa or Torin1 both significantly increased planar proliferation in the non-TGF-β2-treated 2D HconF cells, but in the TGF-β2-treated cells, this proliferation was inhibited by Rapa and enhanced by Torin1. Although Rapa or Torin1 did not affect cellular metabolism in the non-TGF-β2-treated HconF cells, mTOR inhibitors significantly decreased and increased the mitochondrial respiration and the glycolytic capacity, respectively, under conditions of TGF-β2-induced fibrogenesis. Subepithelial proliferation, as evidenced by the hardness of the 3D spheroids, was markedly down-regulated by both Rapa and Torin1 independent of TGF-β2. The mRNA expressions of several ECM molecules and their regulators fluctuated in the cases of 2D vs 3D and TGF-β2 untreated vs treated cultures.
Conclusion
The present findings indicate that mTOR inhibitors have the ability to increase and to reduce planar and subepithelial proliferation in HconF cells, depending on the inhibitor being used.
Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
An antifungal metabolite, Rapa initially discovered from Streptomyces hygroscopicus, was subsequently identified as being a potent suppressor of a serine/threonine kinase, S6K1 [1,2,3] as well as functioning as a pivotal inducer of PI3 kinase (PI3K) signaling axis [4], thereby inducing immunosuppression and anti-proliferation in mammalian cells [5]. At the same time, TOR was also discovered within yeast cells in addition to animal cells [6, 7]. This involves the binding of Rapa with the FK506-binding protein (FKBP12). Rapa forms a gain-of-function complexes, mTOR complex (mTORC) and various biochemical and genetic analyses have revealed that there are two functionally distinct complexes related to mTOR, that is mTORC1 and mTORC2 [6, 8]. It is known that the S6 kinase 1 (S6K1) is the best characterized substrate for mTORC1 [9]. Functionally Rapa can inhibit only mTORC1 but in case of a long-term exposure to Rapa, mTORC2 could be also inhibited in some cells by newly produced mTOR proteins [6]. In terms of the physiological roles of mTORC1 regulation, mTORC1 was identified as a signal processor in response to various biological signals related to growth, nutrition, energy production and consumption and oxygen levels to regulate energy metabolism and autophagy by regulating nucleotide, proteins and lipids synthesis [5]. Pathologically, improperly regulated mTORC1 signaling has been frequently observed in malignant tumors, several genetic disorders and age-related diseases [10]. However, although the physiological and pathological roles of the mTORC2 have not been well characterized in contrast to mTORC1, mTORC2 has been identified as being involved in the activation of Akt and SGK1–related cell survival mechanisms by regulating the actin-cytoskeleton organization [6].
TGF-β has been identified as a pivotal inducer of fibrogenesis [11,12,13,14], through the stimulation of downstream signaling mechanisms [15,16,17], such as Smad related and unrelated signaling pathways [18, 19]. Such TGF-β induced fibrogenesis is pivotally involved in nearly all wound healing related phenomena including subconjunctival fibrogenesis [20]. Regarding TGF-β isoforms, it has been reported that TGF-β1, TGF-β2, and TGF-β3 have been identified, and among these, TGF-β2 was predominantly located within corneal tissues [21], conjunctival fibroblasts [22] vitreous, aqueous humor, and tears [23, 24]. In fact, it was reported that significantly high concentrations of TGF-β2 are present in the AH of patients with glaucoma as compared to non-glaucoma subjects [25].
To maintain healthy barrier functions in human conjunctiva, subconjunctival fibrosis that occurs in response to conjunctival wound healing needs to be appropriately controlled [26,27,28,29,30,31,32,33,34]. It has been shown that among the non-Smad signaling pathways, the PI3K-Akt-mTOR axis function as an important role in TGF-β-evoked fibrogenesis [35, 36]. In fact, several recent transcriptomics studies have demonstrated that mTOR, fibrogenesis and TGF-β are cooperatively involved in the molecular pathogenesis of vascular alterations such as inherited retinopathies (IRDs) [37, 38], brain arteriovenous malformation (bAVM) and cerebral cavernous malformations (CCM) [39,40,41]. Therefore, we rationally speculated that pharmacological suppressors of the PI3K-Akt-mTOR pathway represents a promising strategy for preventing TGF-β-induced conjunctival fibrogenesis without the requirement for the full inactivation of TGF-β signaling. In fact, Sun et al. [42] and Huang et al. [43] demonstrated that PI3K/Akt signaling is involved in the migration, differentiation, and ECM synthesis of HconF, and that the PI3K/Akt pathway in subconjunctival fibrosis of conjunctival fibroblast was activated by TGF-β1 [44] and TGF-β2 [45]. Furthermore, fibrogenesis in human conjunctival epithelial (HCjE) cells is induced by prolonged exposure to TGF-β1 and/or TGF-β2 [46] and Rapa inhibited proliferation and differentiation of human corneal myofibroblasts [47].
In addition, since, among the various TGF-β-induced conjunctival wound-healing responses [48, 49], there are two different issues, namely, (1) superficial re-epithelialization and wound contraction, and (2) subconjunctival fibrous scar formation [50]. Appropriate in vitro models that replicate these two different conjunctival fibrosis processes are needed. For this purpose, we have established in vitro models mimicking planar fibrosis and subconjunctival fibrosis of human conjunctiva utilizing 2D and 3D cell culture methods using HconF that had been treated with TGF-β2 as the representative TGF-β isoform [51,52,53]. Here, to obtain insights into this issue, we studied the effects of the mTORC1 inhibitor, Rapa and the mTORC1 and 2 inhibitor, Torin1, on 2D and 3D HconF cell cultures that had been treated and untreated with TGF-β2.
Patients and methods
Human conjunctival fibroblasts (HconF)
All experiments using human-derived cells were conducted in compliance with the tenets of the Declaration of Helsinki but the internal review board of Sapporo Medical University has ruled that approval was not required for the study because of use of commercially available HconF cells (ScienCell Research laboratories, CA USA).
Preparations of 2D and 3D cultured HconF
2D and 3D of cultured HconF were performed for 6 days as described in our previous studies [51, 54,55,56]. In brief, HconF cells were planar 2D cultured in the Fibroblast Medium (ScienCell Research laboratories, CA USA). For further 3D spheroid culture, 2D HconF cells were washed with phosphate buffered saline (PBS), detached by treatment with 0.25% Trypsin/EDTA, re-suspended in a medium supplemented with 0.25% methylcellulose (Methocel A4M) at a level of approximately 20,000 HconF cells in 28 μL, and each well was subjected to hanging drop culture plates (# HDP1385, Sigma-Aldrich, St Louis, MO, USA) (Day 0). On each subsequent day until Day 6, half of the medium (14 μL) was exchanged with fresh medium. During Days 1 through 6, TGF-β2 (5 ng/ml) and/or mTOR inhibitors, Rapa or Torin1 (100 nM) were administered to the 2D or 3D cultured Hcon F cells based on these chemical dosages reported in previous studies [51, 57,58,59].
Immunocytochemistry
The 2D cultured HconF cells fixed with 4% paraformaldehyde were successively treated with the 1st antibodies; an anti-human S6 ribosomal protein (5G10) rabbit mAb (#2217, Cell Signaling Technology, Danvers MA, USA), phosphor-S6 ribosomal protein (Ser235/236) antibody (#2211, Cell Signaling Technology, Danvers MA, USA), an Akt antibody (#9272, Cell Signaling Technology, Danvers MA, USA) and phosphor-Akt (Ser473) (#9271, Cell Signaling Technology, Danvers MA, USA) (1:200 dilutions), and a mixture of 1:1000 dilutions of a goat anti-rabbit IgG (488 nm), DAPI and phalloidin. After mounting in ProLong Gold Antifade Mountant with a cover glass, immunofluorescent labeling images were obtained by means of a Nikon A1 confocal microscope using a × 20 air objective with a resolution of 1024 × 1024 pixels as described in our previous studies [55, 60].
Trans-epithelial electrical resistance (TEER) and cellular metabolic analyses
To evaluate planar proliferation and cellular metabolic functions of the 2D HconF cells prepared as above, TEER and seahorse metabolic analyses were performed essentially as described in detail in our recent studies [52, 53, 61,62,63]. In brief, in the absence and presence of Rapa or Torin1 (100 nM), HconF monolayers that had been treated with TGF-β2 (5 ng/ml) and untreated HconF monolayers were placed in each well of the TEER plate (0.4 μm pore size and 12 mm diameter; Corning Transwell, Sigma-Aldrich) and were cultured as above. On Day 6, the TEER values were measured using an electrical resistance system (KANTO CHEMICAL CO. INC., Tokyo, Japan). Alternatively, for the bio-cellular function of the 2D HconF cell, their oxygen consumption rate (OCR) and the extracellular acidification (ECAR) of 2D HconF cells were evaluated by a Seahorse XFe96 Bioanalyzer (Agilent Technologies). Briefly, 20 × 103 2D HconF cells were placed in wells of a 96-well assay plate as follows: (1) non-treated control (NT), (2) treated with TGF-β2, (3) treated with Rapa or Torin1 (100 nM) and (4) treated with TGF-β2 and Rapa or Torin1 (100 nM). After replacing the culture medium with Seahorse XF DMEM assay medium (pH 7.4, Agilent Technologies, #103575–100) supplemented with 5.5 mM glucose, 2.0 mM glutamine, and 1.0 mM sodium pyruvate, the basal OCR and ECAR values were determined using a Seahorse XFe96 Bioanalyzer and thereafter, the samples were further analyzed after supplementation with 2.0 μM oligomycin, 5.0 μM carbonyl cyanide p-trifluoromethoxyphenylhydrazone (FCCP), 1.0 μM rotenone and antimycin A, and 10 mM 2-deoxyglucose (2-DG). The OCR and ECAR values were normalized to the amount of protein per well.
Physical aspects analyses of 3D HconF spheroids
As physical aspects of the 3D HconF spheroids, their mean sizes and hardness were evaluated essentially as described in our previous studies [54, 56]. In brief, the mean sizes of the 3D spheroids were measured using an inverted microscope (Nikon ECLIPSE TS2; Tokyo, Japan). Alternatively, for the stiffness measurement, a single living 3D spheroid was placed on a 3-mm × 3-mm plate and compressed until a 50% deformation was achieved for 20 s using a micro-compressor (MicroSquisher, CellScale, Waterloo, ON, Canada). The force required (μN) was determined, and force/displacement (μN/μm) was calculated.
Other analytical methods
As described in previous reports [55, 60], total RNA extracted from 2D or 3D HconF cells using an RNeasy mini kit (Qiagen, Valencia, CA, USA) was then subjected to reverse transcription using the SuperScript IV kit (Invitrogen) as per manufacturer’s instructions. Each respective gene expression was quantified by real-time PCR with the Universal Taqman Master mix using a StepOnePlus machine (Applied Biosystems/Thermo Fisher Scientific) using specific primers and probes (supplementary Table 1). cDNA quantities were normalized to the expression of 36B4 (Rplp0) and are shown as fold-change relative to the control.
As experimental data, the arithmetic mean ± the standard error of the mean (SEM) was used in conjugation with statistical analyses essentially as described in our previous reports [55, 60]. A significant difference of less than 0.05 between experimental groups by ANOVA followed by a Tukey’s multiple comparison test was defined to be statistically significant.
Results
Effects of mTOR inhibitors on 2D planar proliferation of HconF cells
By utilizing the 3D cell culture method as well as conventional 2D planar cultures, we recently succeeded in producing suitable in vitro models that mimic the TGF-β2-related fibrogenesis on the superficial epithelial plane as well as under epithelial spatial space, respectively [51]. Using these models, here, we studied the roles of mTOR signaling in fibrogenesis of human conjunctiva. To first confirm the key downstream target reactions of mTORC1, the inhibition of the phosphorylation of S6 (p-S6) by Rapa and Torin1, and mTORC2, an inhibition of phosphorylation of Akt (p-Akt) by Torin1, but not Rapa, immunocytochemistry was performed using 2D cultured HconF cells. As shown in Fig. 1, both Rapa and Torin1 significantly inhibited p-S6 or p-S6 and p-Akt, respectively [64]. The inhibitory effects of mTORC1 by Rapa and mTORC 1 and 2 by Torin1 on the TGF-β2-induced planar proliferation was evaluated by TEER measurements of 2D HconF monolayers (Fig. 2). The results indicated that a significantly increased TEER values was observed upon exposure of the cultures to TGF-β2. Similarly, a monotreatment of both Rapa and Torin1 also induced a significant elevation in the TEER values. Interestingly, such increased effects in the TEER values by Rapa or Torin1 were lesser or higher compared with TGF-β2, but both effects were additionally enhanced by the presence of TGF-β2.
Representative confocal microscopy images of the immunolabeling of S6, p-S6, Akt and p-Akt of the 2D HconF cells. 2D HconF cells treated or untreated with 100 nM Rapa (Rapa) or Torin1 for 6 days were each immunostained for S6, p-S6, Akt and p-Akt (green) without or with phalloidin (red) and DAPI (blue) in duplicate using fresh preparations (n = 5). Scale bar; 100 μm
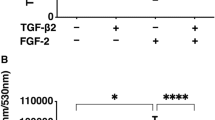
TEER of the 2D HconF monolayers in the absence and presence of TGF-β2 and /or mTOR inhibitors. TEER measurements (Ωcm2) of the TGF-β2 (5 ng/ml) treated or untreated 2D monolayers of HconF cells were performed in the absence or presence of 100 nM Rapa (Rapa) or Torin1 for 6 days in triplicate using fresh preparations (total n = 9), and those values were plotted. **P < 0.01, ***P < 0.005, ****P < 0.001
Effects of mTOR inhibitors on intracellular metabolism of 2D HconF cells
The modulations of mTOR signaling by treatment with Rapa or Torin1 of the TGF-β2 untreated or treated 2D cultured HconF cells on intracellular metabolism were evaluated by using an XFe96 Extracellular Flux Analyzer (Fig. 3). Treatment with TGF-β2 alone tended to induce metabolism toward energetic, but the changes did not reach statistical significance in the present study. Rapa or Torin1 also did not significantly alter key metabolic parameters, including basal OCR, ATP-linked respiration, maximal mitochondrial respiration, basal EACR, glycolytic capacity, and glycolytic reserve in the TGF-β2 untreated cells. However, interestingly, the mitochondrial respiratory indices and glycolytic functions of the TGF-β2 treated cells were significantly suppressed and enhanced, respectively by Rapa or Torin1. These findings suggest that Rapa or Torin1 has an ability to shift cellular metabolism from oxidative phosphorylation to glycolysis in HconF cells in the TGF-β2 treated cells.
The mitochondrial and glycolytic aspects of 2D HconF cells in the absence and presence of TGF-β2 and/or mTOR inhibitors. A real-time metabolic function analysis by a XFe96 Extracellular Flux Analyzer of the TGF-β2 (5 ng/ml) treated or untreated 2D monolayers of HconF cells were performed in the absence or presence of 100 nM Rapa (Rapa) or Torin1 for 6 days in fresh preparations (n = 8). Panel a; plot of OCR values, Panel b; plot of ECAR values, Panel c; key parameters of mitochondrial functions, Panel d; key parameters of glycolytic functions. Both OCR and ECAR values were normalized by the protein amount per well. Basal OCR; (the OCR at baseline) – (OCR with R/A), ATP-linked respiration; (the OCR at the baseline) – (the OCR with Oligo), Maximal respiration; (the OCR with FCCP) – (the OCR with R/A), Basal ECAR; (ECAR at the baseline) – (ECAR with 2DG), Glycolytic capacity; (ECAR with Oligo) – (ECAR with 2DG), Glycolytic reserve; (ECAR with Oligo) – (ECAR at baseline). OCR; oxygen consumption rate, ECAR; extracellular acidification rate, Oligo; oligomycin, FCCP; carbonyl cyanide p-trifluoromethoxyphenylhydrazone (FCCP), R/A; otenone/antimycin A, 2DG; 2-deoxyglucose. *P < 0.05
Effects of mTOR inhibitors on the size and hardness of 3D HconF spheroids
Next, to examine the influences of Rapa or Torin1 on TGF-β2-related fibrogenesis that occurred under epithelial spatial space, as their parameters, the spheroids’ size and hardness were determined. Figure 4 demonstrated that down-sizing and less stiffened effects were observed for both Rapa or Torin1 and these effects were independent of TGF-β2. These results indicate that the inhibition of mTOR by Rapa or Torin1 significantly suppressed the TGF-β2-related and unrelated myofibroblast-induced changes in the subepithelial spatial direction but not in the planar direction although both drugs substantially influenced the cellular metabolic states, as described above.
The physical aspects of 3D HconF spheroids in the absence and presence of TGF-β2 and/or mTOR inhibitors. The mean sizes (μm) (A) and stiffness (μN/μm) (B), the force (μN) required to produce their 50% deformity for 20 s, of the TGF-β2 (5 ng/ml) treated or untreated 3D HconF spheroids were measured in the absence or presence of 100 nM Rapa (Rapa) or Torin1 for 6 days in triplicate using fresh preparations (total n = 16), and those values were plotted. *P < 0.05, ****P < 0.001
Effects of mTOR inhibitors on the expression of ECM proteins and their modulators on 2D and 3D HconF cells
To obtain further insights into the underlaid responsible molecular mechanisms for the above observed characteristic effects by mTOR inhibitors, Rapa or Torin1, the gene expressions of collagen1 (COL1), COL4, COL6, fibronectin (FN) and α smooth muscle actin (αSMA) were evaluated, and the following results were obtained (Fig. 5); (1) a Rapa monotreatment induced a marked down-regulation of COL1 (3D) and COL6 (2D and 3D), (2) a Torin1 monotreatment resulted in the down-regulated COL1 (3D), COL6 (2D) and FN (3D) or the up-regulation of COL4 (3D), and (3) TGF-β2 significantly up-regulated all except for COL6 in 2D HconF cells, or FN in the 3D HconF spheroids and these effects were substantially inhibited by Rapa or Torin1. In terms of the mRNA expression of TIMPs and MMPs (Fig. 6), although the TGF-β2 monotreatment significantly up-regulated TIMP2 and 3, and MMP2, or down-regulated TIMP1 and 4 (2D) or up-regulated of MMP2 (3D), mTOR inhibitors induced 1) marked down-regulations of TIMP3 and 4 (2D) or substantial down-regulations of TIMP1, 2 and 4, and MMP14 (3D). In addition, Rapa or Torin1 inhibited the TGF-β-2-induced effects of TIMP1 and 3 (2D and 3D) and TIMP4 (3D), or TIMP2 and 3 and MMP14 (2D) and TIMP1 and TIMP4 (3D), respectively.
The mRNA expression of ECM molecules of 2D and 3D cultured HconF cells in the absence and presence of TGF-β2 and /or mTOR inhibitors. qPCR analysis of COL1, COL4, COL6, FN, and aSMA of the TGF-β2 (5 ng/ml) treated or untreated 2D and 3D HconF cells was performed in the absence or presence of 100 nM Rapa (Rapa) or Torin1 for 6 days in duplicate 3 different confluent 6-well dishes (2D) or 15 freshly prepared 3D spheroids (3D), and those values were plotted. *P < 0.05, **P < 0.01, ***P < 0.005
The mRNA expression of TIMPs and MMPs of 2D and 3D cultured HconF cells in the absence and presence of TGF-β2 and/or mTOR inhibitors. qPCR analysis of TIMP1-4 (A) and MMP2, 9 and 14 (B) of the TGF-β2 (5 ng/ml) treated or untreated 2D and 3D HconF cells was performed in the absence or presence of 100 nM Rapa (Rapa) or Torin1 for 6 days in duplicate 3 different confluent 6-well dishes (2D) or 15 freshly prepared 3D spheroids (3D), and those values were plotted. *P < 0.05, **P < 0.01, ***P < 0.005
Taken together, we concluded that the mTOR inhibitors, Rapa or Torin1 have the potential for altering the expression of ECM metabolism related molecules, thereby inducing characteristic effects on the TGF-β2-related and unrelated fibrogenesis in the planar and subepithelial spatial directions, as described above.
Discussion
Rapa, an immunomodulator approved by the FDA, efficiently binds to the FK506 binding protein (FKBP12), and the Rapa-FKBP12 complex allosterically inhibits mTOR signaling, thereby possibly modulating both innate and adaptive immune responses by regulating the functions of antigen-presenting cells [65] as well as autophagy, thus having a pivotal role in immunity and inflammation [66]. In the ophthalmic field, interest has been shown in the suppression of mTOR signaling as a possible method for treatment of ocular surface-related diseases. In fact, previous studies have shown that the significant up-regulations of several cytokines and Akt3 in the lacrimal gland (LG) of a mouse model of Sjögren’s syndrome (SS) were significantly inhibited by 12-week Rapa treatment [67,68,69,70]. Thus, these observations suggest that upon topical administration of Rapa, a potent anti-inflammatory effect within the LG could be expected by reducing autoimmune inflammation in the LG, increasing tear secretion, and restoring the ocular surface homeostasis in an SS mouse model. Trujillo-Vargas et al. recently reported that, in addition that significant decreases in inflammatory markers in the LG, conjunctival goblet cell density and area were substantially increased by daily instillation of eyedrops containing Rapa for 3 months in aged mice [71]. Based upon their findings, they suggested that the use of eyedrops containing Rapa may be a potential therapeutic strategy for suppressing the unfavorable age-related phenomena within the ocular surface including tear-producing tissues. It was also reported that the increased expression of mTOR signaling proteins in experimental allergic conjunctivitis (EAC) was effectively reduced by Rapa treatment, thus suggesting that Rapa has a role in the attenuation of allergic conjunctivitis [72].
In addition to the above-described effects of Rapa that are related to immunity and inflammation, Rapa also appears to have the ability to modulate several other mechanisms including cellular growth and proliferation, protein synthesis, and autophagy through mTORC1. It was shown that upon substantially stimulated mTORC1 signaling, aberrant apoptosis as well as cell proliferation seemed to occur in pterygium since their resting epithelial cells exhibit aberrant apoptosis and cell proliferation. This suggests that mTORC1 could provide a potential therapy for the treatment of pterygium [58]. As an additional therapeutic possibility within the ophthalmic field, Igarashi et al. recently reported that mTOR inhibitors, Rapa and Torin1, significantly inhibited TGF-β1-induced fibrotic changes in an in vitro model for postoperative subconjunctival scarring using HconF cells [59]. They also reported that topical administration of an mTOR inhibitor in a rabbit model of trabeculectomy effectively suppressed deposition of COLs in rabbit eyes after trabeculectomy. Based on these findings, they suggested that the use of mTOR inhibitors may be a novel treatment strategy to reduce the fibrotic response in HconF resulting in improvement of bleb survival (rates) after filtration surgery [59]. In our recent study, we compared the effects of three major TGF-b isoforms, TGF-β1, TGF-β2 and TGF-β3, on conjunctival fibrogenesis using our established in vitro 2D and 3D culture models [73]. Our results showed that all three isoforms induced fibrogenetic effects but that the efficacies of the isoforms were quite different. That is, the effects of TGF-β1 and TGF-β3 on 2D HconF planar cell proliferation assessed by TEER and cellular metabolic functions assessed by a Seahorse bioanalyzer and on physical properties of 3D HconF cells were significantly different and the effects of TGF-β2 were the average effects of both isoforms, suggesting the rationale to use TGF-β2 as a representative TGF-β isoform in the current study. Our present study to examine the effects of mTOR inhibitors demonstrated that Rapa and Torin1 on TGF-β2 induced conjunctival fibrogenesis by using recently established in vitro models using 2D and 3D cultures of HconF cells in the presence of TGF-β2 replicating planar and subepithelial fibrogenesis, respectively. The results indicated that (1) Rapa or Torin1 significantly increased planar proliferation of TGF-β2-untreated 2D HconF cells, but this was inhibited or enhanced, respectively, in TGF-β2-treated cells, (2) mono-treatment of Rapa or Torin1 did not affect cellular metabolism, but both drugs induced a significant energy shift from oxidative phosphorylation to glycolysis in TGF-β2-treated HconF cells, (3) subepithelial proliferation, as evidenced by the 3D spheroid’s stiffness, was markedly decreased by both Rapa and Torin1 independent of TGF-β2 and (4) the gene expression of ECM metabolism-related molecules fluctuated among the conditions for both the 2D and 3D TGF-β2-untreated or TGF-β2-treated cultures. Differences between gene expression profiles of ECM proteins and their modulators in 2D and 3D cell cultures have been observed in other cells including human orbital fibroblasts [54], human trabecular meshwork cells [74] and others due to the differences of cell-to-cell interactions, 2D; side by side, vs 3D; cell can interact on everywhere around another cell, as suggested by previous study [75].
The mechanism by which mTOR inhibition can suppress mitochondrial function and enhance glycolytic capacity only under the condition of TGF-β2-induced fibrogenesis in HconF cells is still speculative. However, given that mTORC1 has been reported to be involved in mitochondrial biosynthesis in several types of cells [76, 77], the explanation that mTOR inhibition induced a compensatory shift in cellular metabolism to glycolysis from oxidative phosphorylation in response to metabolic demand by TGF-β2 is reasonable. Therefore, investigating whether these metabolic responses are also observed in other cells and the effects of mTOR inhibition on different time courses of fibrogenesis are our next research projects.
Taken together, we conclude that these mTOR inhibitors may increase and reduce planar proliferation and subepithelial proliferation of HconF cells, respectively. However, as study limitations in the current investigation, the following issues should be taken into consideration. Firstly, as revealed by Seahorse metabolic measurements, Rapa and Torin1 significantly modulated both mitochondrial and glycolytic functions, especially in the presence of TGF-β2, although the underlying molecular mechanisms have not yet been elucidated. Secondly, we simply used 2D planar cultures and 3D spheroid cultures as models of conjunctival superficial and subconjunctival scarring. However, previous studies demonstrated that culture conditions could significantly influence the cell phenotype and the maintenance of specific cell populations [78], and, in fact, gene expression levels were reported to be altered in conjunctiva among ex vivo, primary conjunctiva and cultured conjunctival cell lines (Tong et al. 2009) [79]. In addition, our currently used method for evaluating the barrier functions of 2D cultured HconF cells involves estimating conjunctival superficial re-epithelialization and wound contraction. However, several previous studies have suggested that commercially available HconF cells may have characteristics that are different from those of primary cultured human conjunctival cells or cell lines derived from them. For example, benzalkonium chloride (BAC) was reported to cause shrinkage and plate detachment in primary cultured human conjunctival fibroblasts [80] and a low dose of BAC (10−4%) was reported to cause cell lysis in a human conjunctival cell line [81], whereas in our recent study, no morphological changes or changes in TEER were detected in HconF 2D-cultured cells that were exposed to BAC [61]. In fact, KRT24 is expressed in the human conjunctiva [82, 83] but not in HconF cells [84]. Therefore, investigation of additional types of conjunctival cells will be required to confirm that our current results could be clinically relevant. Thirdly, it is well known that TGF-β induces conjunctival fibrogenesis [85, 86], and we therefore used a representative TGF-β isoform, TGF-2, among various factors. However, in several previous studies, other TGF-β isoforms, TGF-β1 and TGF-β3 [42, 43, 46, 87,88,89,90], and nerve growth factor (NGF) [91,92,93] were also identified as possible pivotal fibrogenetic inducing factors in the conjunctiva. Fourthly, it has been shown that various types of crosslinking can occur between PI3K/Akt, the Smad, and the non-Smad MAPK and RhoA/Rho-kinase signaling pathways in ocular fibrotic disorders [94]. Therefore, for a better understanding new results related to the effects of mTOR inhibitors on fibrogenetic changes of 2D and 3D cultures of HconF cells, additional investigations will be required to elucidate the currently unidentified issues related to our current observations among several complex signaling networks of mTOR, other TGF-β isoforms such as TGF-β1, TGF-β3 and others, and NGF as well as the use of additional animal models with conjunctival fibrosis.
Change history
26 August 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00417-024-06617-4
References
Chung J, Kuo CJ, Crabtree GR, Blenis J (1992) Rapamycin-FKBP specifically blocks growth-dependent activation of and signaling by the 70 kd S6 protein kinases. Cell 69:1227–1236. https://doi.org/10.1016/0092-8674(92)90643-q
Kuo CJ, Chung J, Fiorentino DF, Flanagan WM, Blenis J, Crabtree GR (1992) Rapamycin selectively inhibits interleukin-2 activation of p70 S6 kinase. Nature 358:70–73. https://doi.org/10.1038/358070a0
Price DJ, Grove JR, Calvo V, Avruch J, Bierer BE (1992) Rapamycin-induced inhibition of the 70-kilodalton S6 protein kinase. Science (New York, NY) 257:973–977. https://doi.org/10.1126/science.1380182
Chung J, Grammer TC, Lemon KP, Kazlauskas A, Blenis J (1994) PDGF- and insulin-dependent pp70S6k activation mediated by phosphatidylinositol-3-OH kinase. Nature 370:71–75. https://doi.org/10.1038/370071a0
Li J, Kim SG, Blenis J (2014) Rapamycin: one drug, many effects. Cell Metab 19:373–379. https://doi.org/10.1016/j.cmet.2014.01.001
Laplante M, Sabatini DM (2012) mTOR signaling in growth control and disease. Cell 149:274–293. https://doi.org/10.1016/j.cell.2012.03.017
Loewith R, Hall MN (2011) Target of rapamycin (TOR) in nutrient signaling and growth control. Genetics 189:1177–1201. https://doi.org/10.1534/genetics.111.133363
Cornu M, Albert V, Hall MN (2013) mTOR in aging, metabolism, and cancer. Curr Opin Genet Dev 23:53–62. https://doi.org/10.1016/j.gde.2012.12.005
Ma XM, Blenis J (2009) Molecular mechanisms of mTOR-mediated translational control. Nat Rev Mol Cell Biol 10:307–318. https://doi.org/10.1038/nrm2672
Johnson SC, Rabinovitch PS, Kaeberlein M (2013) mTOR is a key modulator of ageing and age-related disease. Nature 493:338–345. https://doi.org/10.1038/nature11861
Finnson KW, McLean S, Di Guglielmo GM, Philip A (2013) Dynamics of transforming growth factor beta signaling in wound healing and scarring. Adv Wound Care 2:195–214. https://doi.org/10.1089/wound.2013.0429
Phan SH (2002) The myofibroblast in pulmonary fibrosis. Chest 122:286s–289s. https://doi.org/10.1378/chest.122.6_suppl.286s
Vaughan MB, Howard EW, Tomasek JJ (2000) Transforming growth factor-beta1 promotes the morphological and functional differentiation of the myofibroblast. Exp Cell Res 257:180–189. https://doi.org/10.1006/excr.2000.4869
White ES, Lazar MH, Thannickal VJ (2003) Pathogenetic mechanisms in usual interstitial pneumonia/idiopathic pulmonary fibrosis. J Pathol 201:343–354. https://doi.org/10.1002/path.1446
Kalluri R, Weinberg RA (2009) The basics of epithelial-mesenchymal transition. J Clin Investig 119:1420–1428. https://doi.org/10.1172/jci39104
Moustakas A, Heldin CH (2007) Signaling networks guiding epithelial-mesenchymal transitions during embryogenesis and cancer progression. Cancer Sci 98:1512–1520. https://doi.org/10.1111/j.1349-7006.2007.00550.x
Xu J, Lamouille S, Derynck R (2009) TGF-beta-induced epithelial to mesenchymal transition. Cell Res 19:156–172. https://doi.org/10.1038/cr.2009.5
Derynck R, Zhang YE (2003) Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 425:577–584. https://doi.org/10.1038/nature02006
Moustakas A, Heldin CH (2005) Non-Smad TGF-beta signals. J Cell Sci 118:3573–3584. https://doi.org/10.1242/jcs.02554
Bolaños-Jiménez R, Navas A, López-Lizárraga EP, de Ribot FM, Peña A, Graue-Hernández EO, Garfias Y (2015) Ocular surface as barrier of innate immunity. Open Ophthalmol J 9:49–55. https://doi.org/10.2174/1874364101509010049
Nishida K, Sotozono C, Adachi W, Yamamoto S, Yokoi N, Kinoshita S (1995) Transforming growth factor-beta 1, -beta 2 and -beta 3 mRNA expression in human cornea. Curr Eye Res 14:235–241. https://doi.org/10.3109/02713689509033520
Cordeiro MF, Gay JA, Khaw PT (1999) Human anti-transforming growth factor-beta2 antibody: a new glaucoma anti-scarring agent. Invest Ophthalmol Vis Sci 40:2225–2234
Jampel HD, Roche N, Stark WJ, Roberts AB (1990) Transforming growth factor-beta in human aqueous humor. Curr Eye Res 9:963–969. https://doi.org/10.3109/02713689009069932
Kokawa N, Sotozono C, Nishida K, Kinoshita S (1996) High total TGF-beta 2 levels in normal human tears. Curr Eye Res 15:341–343. https://doi.org/10.3109/02713689609007630
Tripathi RC, Li J, Chan WF, Tripathi BJ (1994) Aqueous humor in glaucomatous eyes contains an increased level of TGF-beta 2. Exp Eye Res 59:723–727. https://doi.org/10.1006/exer.1994.1158
Khaw PT, Migdal CS (1996) Current techniques in wound healing modulation in glaucoma surgery. Curr Opin Ophthalmol 7:24–33. https://doi.org/10.1097/00055735-199604000-00005
Chiou AG, Florakis GJ, Kazim M (1998) Management of conjunctival cicatrizing diseases and severe ocular surface dysfunction. Surv Ophthalmol 43:19–46. https://doi.org/10.1016/s0039-6257(98)00005-8
Chui J, Di Girolamo N, Wakefield D, Coroneo MT (2008) The pathogenesis of pterygium: current concepts and their therapeutic implications. Ocul Surf 6:24–43. https://doi.org/10.1016/s1542-0124(12)70103-9
Dale SB, Saban DR (2015) Linking immune responses with fibrosis in allergic eye disease. Curr Opin Allergy Clin Immunol 15:467–475. https://doi.org/10.1097/aci.0000000000000197
Munir SZ, Aylward J (2017) A review of ocular graft-versus-host disease. Optom Vis Sci 94:545–555. https://doi.org/10.1097/opx.0000000000001071
Broadway DC, Chang LP (2001) Trabeculectomy, risk factors for failure and the preoperative state of the conjunctiva. J Glaucoma 10:237–249. https://doi.org/10.1097/00061198-200106000-00017
Schlunck G, Meyer-ter-Vehn T, Klink T, Grehn F (2016) Conjunctival fibrosis following filtering glaucoma surgery. Exp Eye Res 142:76–82. https://doi.org/10.1016/j.exer.2015.03.021
Hinz B (2016) Myofibroblasts. Exp Eye Res 142:56–70. https://doi.org/10.1016/j.exer.2015.07.009
Tomasek JJ, Gabbiani G, Hinz B, Chaponnier C, Brown RA (2002) Myofibroblasts and mechano-regulation of connective tissue remodelling. Nat Rev Mol Cell Biol 3:349–363. https://doi.org/10.1038/nrm809
Bakin AV, Tomlinson AK, Bhowmick NA, Moses HL, Arteaga CL (2000) Phosphatidylinositol 3-kinase function is required for transforming growth factor beta-mediated epithelial to mesenchymal transition and cell migration. J Biol Chem 275:36803–36810. https://doi.org/10.1074/jbc.M005912200
Lamouille S, Derynck R (2007) Cell size and invasion in TGF-beta-induced epithelial to mesenchymal transition is regulated by activation of the mTOR pathway. J Cell Biol 178:437–451. https://doi.org/10.1083/jcb.200611146
Donato L, Alibrandi S, Scimone C, Rinaldi C, Dascola A, Calamuneri A, D’Angelo R, Sidoti A (2022) The impact of modifier genes on cone-rod dystrophy heterogeneity: an explorative familial pilot study and a hypothesis on neurotransmission impairment. PLoS One 17:e0278857. https://doi.org/10.1371/journal.pone.0278857
Donato L, Scimone C, Alibrandi S, Scalinci SZ, Rinaldi C, D'Angelo R, Sidoti A (2022) Epitranscriptome analysis of oxidative stressed retinal epithelial cells depicted a possible RNA editing landscape of retinal degeneration. Antioxidants (Basel, Switzerland) 11(10). https://doi.org/10.3390/antiox11101967
Scimone C, Donato L, Marino S, Alafaci C, D’Angelo R, Sidoti A (2019) Vis-à-vis: a focus on genetic features of cerebral cavernous malformations and brain arteriovenous malformations pathogenesis. Neurol Sci : Off J Ital Neurol Soc Ital Soc Clin Neurophysiol 40:243–251. https://doi.org/10.1007/s10072-018-3674-x
Scimone C, Donato L, Alafaci C, Granata F, Rinaldi C, Longo M, D’Angelo R, Sidoti A (2020) High-throughput sequencing to detect novel likely gene-disrupting variants in pathogenesis of sporadic brain arteriovenous malformations. Front Genet 11:146. https://doi.org/10.3389/fgene.2020.00146
Rinaldi C, Bramanti P, Famà A, Scimone C, Donato L, Antognelli C, Alafaci C, Tomasello F, D’Angelo R, Sidoti A (2015) Glyoxalase I A111E, paraoxonase 1 Q192R and L55M polymorphisms in Italian patients with sporadic cerebral cavernous malformations: a pilot study. J Biol Regul Homeost Agents 29:493–500
Sun L, Dong Y, Zhao J, Yin Y, Zheng Y (2016) The CLC-2 chloride channel modulates ECM synthesis, differentiation, and migration of human conjunctival fibroblasts via the PI3K/Akt signaling pathway. Int J Mol Sci 17(6):910. https://doi.org/10.3390/ijms17060910
Huang L, Ye Q, Lan C, Wang X, Zhu Y (2022) AZD6738 inhibits fibrotic response of conjunctival fibroblasts by regulating checkpoint kinase 1/P53 and PI3K/AKT pathways. Front Pharmacol 13:990401. https://doi.org/10.3389/fphar.2022.990401
Hwang YH, Jung SA, Lyu J, Kim YY, Lee JH (2019) Transforming growth factor-β1-induced human subconjunctival fibrosis is mediated by MicroRNA 143/145 expression. Invest Ophthalmol Vis Sci 60:2064–2071. https://doi.org/10.1167/iovs.19-26797
Jung SA, Lee HK, Yoon JS, Kim SJ, Kim CY, Song H, Hwang KC, Lee JB, Lee JH (2007) Upregulation of TGF-beta-induced tissue transglutaminase expression by PI3K-Akt pathway activation in human subconjunctival fibroblasts. Invest Ophthalmol Vis Sci 48:1952–1958. https://doi.org/10.1167/iovs.06-1164
Rajić J, Dinić S, Uskoković A, Arambašić Jovanović J, Tolić A, Đorđević M, Đorđević M, Poznanović G, Mihailović M, Inic-Kanada A, Barisani-Asenbauer T, Grdović N, Vidaković M (2020) DNA methylation of miR-200 clusters promotes epithelial to mesenchymal transition in human conjunctival epithelial cells. Exp Eye Res 197:108047. https://doi.org/10.1016/j.exer.2020.108047
Milani BY, Milani FY, Park DW, Namavari A, Shah J, Amirjamshidi H, Ying H, Djalilian AR (2013) Rapamycin inhibits the production of myofibroblasts and reduces corneal scarring after photorefractive keratectomy. Invest Ophthalmol Vis Sci 54:7424–7430. https://doi.org/10.1167/iovs.13-12674
Cordeiro MF, Chang L, Lim KS, Daniels JT, Pleass RD, Siriwardena D, Khaw PT (2000) Modulating conjunctival wound healing. Eye (Lond) 14(Pt 3B):536–547. https://doi.org/10.1038/eye.2000.141
Saika S, Yamanaka O, Okada Y, Tanaka S, Miyamoto T, Sumioka T, Kitano A, Shirai K, Ikeda K (2009) TGF beta in fibroproliferative diseases in the eye. Front Biosci (Schol Ed) 1:376–390. https://doi.org/10.2741/s32
Cordeiro MF, Occleston NL, Khaw PT (1997) New concepts: manipulation of the wound-healing response. Dev Ophthalmol 28:242–260. https://doi.org/10.1159/000060701
Oouchi Y, Watanabe M, Ida Y, Ohguro H, Hikage F (2021) Rosiglitasone and ROCK inhibitors modulate fibrogenetic changes in TGF-β2 treated human conjunctival fibroblasts (HconF) in different manners. Int J Mol Sci 22(14):7335. https://doi.org/10.3390/ijms22147335
Tsugeno Y, Furuhashi M, Sato T, Watanabe M, Umetsu A, Suzuki S, Ida Y, Hikage F, Ohguro H (2022) FGF-2 enhances fibrogenetic changes in TGF-β2 treated human conjunctival fibroblasts. Sci Rep 12:16006. https://doi.org/10.1038/s41598-022-20036-7
Tsugeno Y, Sato T, Watanabe M, Higashide M, Furuhashi M, Umetsu A, Suzuki S, Ida Y, Hikage F, Ohguro H (2022) All trans-retinoic acids facilitate the remodeling of 2D and 3D cultured human conjunctival fibroblasts. Bioengineering (Basel, Switzerland) 9(9):463. https://doi.org/10.3390/bioengineering9090463
Hikage F, Atkins S, Kahana A, Smith TJ, Chun TH (2019) HIF2A-LOX pathway promotes fibrotic tissue remodeling in thyroid-associated orbitopathy. Endocrinology 160:20–35. https://doi.org/10.1210/en.2018-00272
Itoh K, Hikage F, Ida Y, Ohguro H (2020) Prostaglandin F2α agonists negatively modulate the size of 3D organoids from primary human orbital fibroblasts. Invest Ophthalmol Vis Sci 61:13. https://doi.org/10.1167/iovs.61.6.13
Ota C, Ida Y, Ohguro H, Hikage F (2020) ROCK inhibitors beneficially alter the spatial configuration of TGFβ2-treated 3D organoids from a human trabecular meshwork (HTM). Sci Rep 10:20292. https://doi.org/10.1038/s41598-020-77302-9
Matsumura T, Fujimoto T, Futakuchi A, Takihara Y, Watanabe-Kitamura F, Takahashi E, Inoue-Mochita M, Tanihara H, Inoue T (2020) TGF-β-induced activation of conjunctival fibroblasts is modulated by FGF-2 and substratum stiffness. PLoS One 15:e0242626. https://doi.org/10.1371/journal.pone.0242626
Liu Y, Xu H, An M (2017) mTORC1 regulates apoptosis and cell proliferation in pterygium via targeting autophagy and FGFR3. Sci Rep 7:7339. https://doi.org/10.1038/s41598-017-07844-y
Igarashi N, Honjo M, Aihara M (2021) Effects of mammalian target of rapamycin inhibitors on fibrosis after trabeculectomy. Exp Eye Res 203:108421. https://doi.org/10.1016/j.exer.2020.108421
Ida Y, Hikage F, Itoh K, Ida H, Ohguro H (2020) Prostaglandin F2α agonist-induced suppression of 3T3-L1 cell adipogenesis affects spatial formation of extra-cellular matrix. Sci Rep 10:7958. https://doi.org/10.1038/s41598-020-64674-1
Tsugeno Y, Sato T, Watanabe M, Furuhashi M, Umetsu A, Ida Y, Hikage F, Ohguro H (2022) Benzalkonium chloride, even at low concentrations, deteriorates intracellular metabolic capacity in human conjunctival fibroblasts. Biomedicines 10(9):2315. https://doi.org/10.3390/biomedicines10092315
Sato T, Chang HC, Bayeva M, Shapiro JS, Ramos-Alonso L, Kouzu H, Jiang X, Liu T, Yar S, Sawicki KT, Chen C, Martínez-Pastor MT, Stumpo DJ, Schumacker PT, Blackshear PJ, Ben-Sahra I, Puig S, Ardehali H (2018) mRNA-binding protein tristetraprolin is essential for cardiac response to iron deficiency by regulating mitochondrial function. Proc Natl Acad Sci U S A 115:E6291-e6300. https://doi.org/10.1073/pnas.1804701115
Sato T, Ichise N, Kobayashi T, Fusagawa H, Yamazaki H, Kudo T, Tohse N (2022) Enhanced glucose metabolism through activation of HIF-1α covers the energy demand in a rat embryonic heart primordium after heartbeat initiation. Sci Rep 12:74. https://doi.org/10.1038/s41598-021-03832-5
Hua H, Kong Q, Zhang H, Wang J, Luo T, Jiang Y (2019) Targeting mTOR for cancer therapy. J Hematol Oncol 12:71. https://doi.org/10.1186/s13045-019-0754-1
Saric A, Hipolito VE, Kay JG, Canton J, Antonescu CN, Botelho RJ (2016) mTOR controls lysosome tubulation and antigen presentation in macrophages and dendritic cells. Mol Biol Cell 27:321–333. https://doi.org/10.1091/mbc.E15-05-0272
Benjamin D, Colombi M, Moroni C, Hall MN (2011) Rapamycin passes the torch: a new generation of mTOR inhibitors. Nat Rev Drug Discovery 10:868–880. https://doi.org/10.1038/nrd3531
Li X, Wu K, Edman M, Schenke-Layland K, MacVeigh-Aloni M, Janga SR, Schulz B, Hamm-Alvarez SF (2010) Increased expression of cathepsins and obesity-induced proinflammatory cytokines in lacrimal glands of male NOD mouse. Invest Ophthalmol Vis Sci 51:5019–5029. https://doi.org/10.1167/iovs.09-4523
Lessard CJ, Li H, Adrianto I, Ice JA, Rasmussen A, Grundahl KM, Kelly JA, Dozmorov MG, Miceli-Richard C, Bowman S, Lester S, Eriksson P, Eloranta ML, Brun JG, Gøransson LG, Harboe E, Guthridge JM, Kaufman KM, Kvarnström M, Jazebi H, Cunninghame Graham DS, Grandits ME, Nazmul-Hossain AN, Patel K, Adler AJ, Maier-Moore JS, Farris AD, Brennan MT, Lessard JA, Chodosh J, Gopalakrishnan R, Hefner KS, Houston GD, Huang AJ, Hughes PJ, Lewis DM, Radfar L, Rohrer MD, Stone DU, Wren JD, Vyse TJ, Gaffney PM, James JA, Omdal R, Wahren-Herlenius M, Illei GG, Witte T, Jonsson R, Rischmueller M, Rönnblom L, Nordmark G, Ng WF, Mariette X, Anaya JM, Rhodus NL, Segal BM, Scofield RH, Montgomery CG, Harley JB, Sivils KL (2013) Variants at multiple loci implicated in both innate and adaptive immune responses are associated with Sjögren’s syndrome. Nat Genet 45:1284–1292. https://doi.org/10.1038/ng.2792
Nocturne G, Mariette X (2013) Advances in understanding the pathogenesis of primary Sjögren’s syndrome. Nat Rev Rheumatol 9:544–556. https://doi.org/10.1038/nrrheum.2013.110
Shah M, Edman MC, Reddy Janga S, Yarber F, Meng Z, Klinngam W, Bushman J, Ma T, Liu S, Louie S, Mehta A, Ding C, MacKay JA, Hamm-Alvarez SF (2017) Rapamycin eye drops suppress lacrimal gland inflammation in a murine model of Sjögren’s Syndrome. Invest Ophthalmol Vis Sci 58:372–385. https://doi.org/10.1167/iovs.16-19159
Trujillo-Vargas CM, Kutlehria S, Hernandez H, de Souza RG, Lee A, Yu Z, Pflugfelder SC, Singh M, de Paiva CS (2020) Rapamycin eyedrops increased CD4(+)Foxp3(+) cells and prevented goblet cell loss in the aged ocular surface. Int J Mol Sci 21(23):8890. https://doi.org/10.3390/ijms21238890
Shin S, Lee JH, Lee HJ, Chang SY, Chung SH (2018) Rapamycin attenuates Th2-driven experimental allergic conjunctivitis. Clin Immunol (Orlando, Fla) 190:1–10. https://doi.org/10.1016/j.clim.2018.02.004
Watanabe M, Tsugeno Y, Sato T, Umetsu A, Nishikiori N, Furuhashi M, Ohguro H (2023) TGF-β isoforms affect the planar and subepithelial fibrogenesis of human conjunctival fibroblasts in different manners. Biomedicines 11(7):2005. https://doi.org/10.3390/biomedicines11072005
Watanabe M, Ida Y, Ohguro H, Ota C, Hikage F (2021) Establishment of appropriate glaucoma models using dexamethasone or TGFβ2 treated three-dimension (3D) cultured human trabecular meshwork (HTM) cells. Sci Rep 11:19369. https://doi.org/10.1038/s41598-021-98766-3
Ryu NE, Lee SH, Park H (2019) Spheroid culture system methods and applications for mesenchymal stem cells. Cells 8(12):1620. https://doi.org/10.3390/cells8121620
de la Cruz López KG, Toledo Guzmán ME, Sánchez EO, García Carrancá A (2019) mTORC1 as a regulator of mitochondrial functions and a therapeutic target in cancer. Front Oncol 9:1373. https://doi.org/10.3389/fonc.2019.01373
Wang L, Xu X, Jiang C, Ma G, Huang Y, Zhang H, Lai Y, Wang M, Ahmed T, Lin R, Guo W, Luo Z, Li W, Zhang M, Ward C, Qian M, Liu B, Esteban MA, Qin B (2020) mTORC1-PGC1 axis regulates mitochondrial remodeling during reprogramming. Febs J 287:108–121. https://doi.org/10.1111/febs.15024
Martínez-Osorio H, Calonge M, Corell A, Reinoso R, López A, Fernández I, San José EG, Diebold Y (2009) Characterization and short-term culture of cells recovered from human conjunctival epithelium by minimally invasive means. Mol Vis 15:2185–2195
Tong L, Diebold Y, Calonge M, Gao J, Stern ME, Beuerman RW (2009) Comparison of gene expression profiles of conjunctival cell lines with primary cultured conjunctival epithelial cells and human conjunctival tissue. Gene Expr 14:265–278. https://doi.org/10.3727/105221609788681231
Kim EJ, Kim YH, Kang SH, Lee KW, Park YJ (2013) In vitro effects of preservative-free and preserved prostaglandin analogs on primary cultured human conjunctival fibroblast cells. Korean J Ophthalmol 27:446–453. https://doi.org/10.3341/kjo.2013.27.6.446
De Saint JM, Brignole F, Bringuier AF, Bauchet A, Feldmann G, Baudouin C (1999) Effects of benzalkonium chloride on growth and survival of Chang conjunctival cells. Invest Ophthalmol Vis Sci 40:619–630
Ehrlich F, Laggner M, Langbein L, Burger P, Pollreisz A, Tschachler E, Eckhart L (2019) Comparative genomics suggests loss of keratin K24 in three evolutionary lineages of mammals. Sci Rep 9:10924. https://doi.org/10.1038/s41598-019-47422-y
Ligocki AJ, Fury W, Gutierrez C, Adler C, Yang T, Ni M, Bai Y, Wei Y, Lehmann GL, Romano C (2021) Molecular characteristics and spatial distribution of adult human corneal cell subtypes. Sci Rep 11:16323. https://doi.org/10.1038/s41598-021-94933-8
Shibata N, Ishida H, Kiyokawa E, Singh DP, Sasaki H, Kubo E (2020) Relative gene expression analysis of human pterygium tissues and UV radiation-evoked gene expression patterns in corneal and conjunctival cells. Exp Eye Res 199:108194. https://doi.org/10.1016/j.exer.2020.108194
Leight JL, Wozniak MA, Chen S, Lynch ML, Chen CS (2012) Matrix rigidity regulates a switch between TGF-β1-induced apoptosis and epithelial-mesenchymal transition. Mol Biol Cell 23:781–791. https://doi.org/10.1091/mbc.E11-06-0537
Matsumura T, Fujimoto T, Iraha S, Futakuchi A, Takihara Y, Watanabe-Kitamura F, Takahashi E, Inoue-Mochita M, Tanihara H, Inoue T (2021) Correction: TGF-β-induced activation of conjunctival fibroblasts is modulated by FGF-2 and substratum stiffness. PLoS One 16:e0251615. https://doi.org/10.1371/journal.pone.0251615
Khaw PT, Bouremel Y, Brocchini S, Henein C (2020) The control of conjunctival fibrosis as a paradigm for the prevention of ocular fibrosis-related blindness. “Fibrosis has many friends.” Eye (Lond) 34:2163–2174. https://doi.org/10.1038/s41433-020-1031-9
Meyer-Ter-Vehn T, Grehn F, Schlunck G (2008) Localization of TGF-beta type II receptor and ED-A fibronectin in normal conjunctiva and failed filtering blebs. Mol Vis 14:136–141
Li DQ, Lee SB, Tseng SC (1999) Differential expression and regulation of TGF-beta1, TGF-beta2, TGF-beta3, TGF-betaRI, TGF-betaRII and TGF-betaRIII in cultured human corneal, limbal, and conjunctival fibroblasts. Curr Eye Res 19:154–161. https://doi.org/10.1076/ceyr.19.2.154.5321
Sun L, Cui R, Meng H, Liu X, Liu X, Lu Y, Liu K, Jia L, Zheng Y (2021) Gene suppression of the chloride channel 2 suppressed TGF-β1-induced proliferation, collagen synthesis, and collagen gel contraction mediated by conjunctival fibroblasts. Ophthalmic Res 64:775–784. https://doi.org/10.1159/000507632
Lambiase A, Bonini S, Micera A, Rama P, Bonini S, Aloe L (1998) Expression of nerve growth factor receptors on the ocular surface in healthy subjects and during manifestation of inflammatory diseases. Invest Ophthalmol Vis Sci 39:1272–1275
Micera A, Puxeddu I, Lambiase A, Antonelli A, Bonini S, Bonini S, Aloe L, Pe’er J, Levi-Schaffer F (2005) The pro-fibrogenic effect of nerve growth factor on conjunctival fibroblasts is mediated by transforming growth factor-beta. Clin Exp Allergy : J British Soc Allergy Clin Immunol 35:650–656. https://doi.org/10.1111/j.1365-2222.2005.02241.x
Micera A, Puxeddu I, Balzamino BO, Bonini S, Levi-Schaffer F (2012) Chronic nerve growth factor exposure increases apoptosis in a model of in vitro induced conjunctival myofibroblasts. PLoS One 7:e47316. https://doi.org/10.1371/journal.pone.0047316
Mallone F, Costi R, Marenco M, Plateroti R, Minni A, Attanasio G, Artico M, Lambiase A (2021) Understanding drivers of ocular fibrosis: current and future therapeutic perspectives. Int J Mol Sci 22(21):11748. https://doi.org/10.3390/ijms222111748
Acknowledgements
This study is partly supported by the special support-grant provided by Sapporo Medical University.
Author information
Authors and Affiliations
Contributions
Y.T. conducted the experiments, data analysis and figures and table preparation. T.S. conducted the experiments, data analysis and figures and table preparation. M.W. conducted the experiments, data analysis and figures and table preparation. M.H. conducted experiments and data analysis. A.U. conducted experiments and data analysis. M.F. analyzed data and reviewed manuscript. H.O. conducted experimental design, data analysis and manuscript preparation.
Corresponding authors
Ethics declarations
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards approved by the institutional review board (IRB registration number 282–8, Sapporo Medical University Hospital, Japan,) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised due to a retrospective Open Access cancellation order.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Watanabe, M., Tsugeno, Y., Sato, T. et al. Inhibition of mTOR differently modulates planar and subepithelial fibrogenesis in human conjunctival fibroblasts. Graefes Arch Clin Exp Ophthalmol (2024). https://doi.org/10.1007/s00417-024-06481-2
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00417-024-06481-2