Abstract
The magnitude of cataract pathology is indeed significant as it is the principal cause of blindness worldwide. Also, the prominence of this concept escalates with the current aging population. The burden of the disease is more tangible in developing countries than developed ones. Regarding this concern, there is a gap in classifying the pathogenesis of the ultraviolet (UV) radiation-induced cataracts and explaining the possible cellular and subcellular pathways. In this review, we aim to revisit the effect of UV radiation on cataracts categorizing the cellular pathways involved. This may help for better pharmaceutical treatment alternatives and their wide-reaching availability. Also, in the last section, we provide an overview of the protecting agents utilized as UV shields. Further studies are required to enlighten new treatment modalities for UV radiation-induced pathologies in human lens.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cataracts are the leading cause of blindness in the world [1,2,3]. For the most people, the detrimental effects of solar ultraviolet (UV) radiation on the human eye are intangible as it has been more popular for skin complications [4]. Nevertheless, the UV radiation is a cumulative omnipresent hazard for every individual [5]. It was more than a hundred years ago when Widmark showed that UV radiation ruins the lens [6]. In contrast to UV’s late discovery, human history has been acquainted with the phenomenon of cataracts. The earliest documented case of cataracts goes back to centuries ago, circa 2460 B.C. [7]. Then, it was during 600 B.C. when cataracts were further described in texts and surgical approaches were established [8]. A detailed history of cataracts can be found in a study by Rucker [9]. After centuries, scientific research shed light on the exact risk factors and the extent of their association with cataracts. In the literature, there has been a considerable focus on UVB, yet the probable effects of UVA are less investigated. In this review, we aim to gather the recent evidence behind the association of UV radiation and the cataracts, and cellular pathways responsible for this association. We categorized the probable pathways in six groups, namely (a) oxidative stress, (b) phototoxicity, (c) crystallin proteins, (d) tryptophan, and (e) apoptosis. Generally, oxidative stress is recognized as the fundamental mechanism igniting the apoptotic precursors, aging pathways, and enhancing protein aggregations [10]. On the other hand, crystallins and tryptophan-related pathways are identified as natural protective entities. The detailed exploration of these mechanisms may obviously be supportive for further pharmaceutical, environmental, and public health research. Literature gaps and suggestions for future research are further discussed in the conclusion section.
The UV radiation
The UV radiation is a high-energy electromagnetic field with a broad range of wavelengths starting from 400 to 10 nm [11]. UVs with less than 200 nm wavelength have an ionizing effect when passing through the atmosphere; thus, they never reach the ground and are absorbed by atmospheric oxygen fluctuating in concentration in the ozone layer [12, 13]. There are different sorts of classification with regard to different UV properties from which the UVA, UVB, and UVC classifications are the most widely used ones in medical applications [14]. Table 1 shows wavelengths of these three types of UV radiation. With respect to this classification, it is not likely for UVC (wavelengths between 280 and 100 nm) to pass through the ozone layer [17]. Despite this fact, in a category of occupations such as arc welding and food sterilization, there is a large amount of UVC exposure and it is necessary for the workers to protect themselves sufficiently against UVC exposure. Nevertheless, UVA and UVB are primarily responsible for medical harms and pathologies [18] and are of the main focus in this study. Figure 1 demonstrates the percentage of the UV transmittance through the atmosphere [17]. Generally, UV transmittance depends on several environmental factors, namely clouds, aerosols, and surface reflectivity [19]. As shown in Fig. 1, a considerable amount of UVB attenuates through the atmosphere by the effect of the clouds. Yet, according to studies [20,21,22], UVB is the chief culprit for cataracts affliction. According to several studies [23,24,25], UVs of less than 240 nm (UVC) are completely absorbed by cornea. Also, it has been reported that UV radiation up to 295 nm of wavelength, including all UVC band, is fully absorbed by the cornea inducing acute photokeratitis and causing serious damage to the cornea [26]. In addition, Dixon et al. reported that as it is being completely absorbed, it does increase the risk of cataracts [27]. Furthermore, the human lens can absorb UVs of less than 370 nm (UVA and UVB). UVB is absorbed both by cornea and the lens, approximately 70% and 30% respectively.
The lens and cataracts
A cataract, the leading cause of blindness worldwide, is a condition in which the human lens becomes colored occluding the clear vision [28]. This process is mostly encouraged by accumulative sun exposure during aging and other risk factors including but not limited to smoking, diabetes, and alcohol [29, 30]. Cataracts may account for almost half of the blindness round the world, being the most appalling in African and developing countries, yet more benign in developed ones [3]. Still, its trend is expected to be rising even in developed countries including the USA as the population ages [31, 32]. But globally, those in low- or middle-income conditions are more affected. Cataracts have been thought to afflict more than half of the people at the age of 80 or higher [33]. In many countries, surgical services are inadequate, and cataracts remain the leading cause of blindness [32]. Since the present-day treatment of cataracts is still limited to surgery, high health expenditures have been allocated to confront this ailment [34]. In developing countries, the present burden is as yet later diagnosis, insufficient surgical facilities, or unaffordable costs of surgery, which results in visional sequels [35].
There are various proteins in human lens absorbing the UV radiation and protecting the eye from probable photo-induced damage [36]. These low molecular–weighted proteins are classified into tryptophan and non-tryptophan florescent compounds. Several studies have modeled the molecular effects and optical properties of these proteins [37,38,39,40]. This gradual and continuous filtering of UV radiation leads to clouding of the lens and blurred vision [41]. From a clinical point of view, there are mainly three types of non-congenital cataracts (i.e., nuclear, cortical, and posterior subcapsular) from which the nuclear type, the most common one, is more associated with aging [42]. Among these, there is abundant evidence showing that cortical cataracts are more associated with UV radiation and sun exposure [15]. This association might be in part due to the differential lens UV transmittance pattern of human lens. Pajer et al. have demonstrated that the anterior cortex of the lens is mainly responsible for low transmittance rate of UV and especially the substantial loss of transmittance of UVC [43].
Cataracts might be produced experimentally with UV lasers for research purposes. Ample research has been conducted to propose a new way of treatment, novel pharmaceutical approaches, and preventive techniques to fight the consequences following the cataracts [44,45,46]. However, practical progress has not been adequately made with respect to its prevention. Presently, the UV-filtering (sun)glasses and lenses are the only ubiquitous and mostly known preventive practice [47]. Also, several external factors, including contact lenses, caffeine eye drops, zinc, vitamin E, and topical use of antioxidants, are proposed to protect the eye from UV-induced damage. Caffeine eye drops decrease the activation of caspase-3, so it has been reported to be a protective agent against cataracts [48]. Two other protective factors against UV exposure are zinc and vitamin E which both act through calcium-mediated mitochondrial apoptotic pathway to protect epithelial cells of the lens [49]. Kador et al. showed that topical antioxidant applications can protect the lens against UV-induced damage [50].
In aphakic eyes, the risk of retinal damage increases excessively [51]. Consequently, intraocular lenses (IOLs) absorbing UV radiation could protect the retina. A spectrographic check of UV transmittance by standard IOLs and UV absorbing IOLs has shown that the UV absorbing IOLs block all radiations below 400 nm [52, 53]. If diagnosed at earlier grades, symptoms may alleviate with filtering glasses and lenses blocking the UV radiation [54, 55]. In the last section, we will provide a review of the protecting agents and protective molecular pathways.
Crystallins are the prominent absorbers of UVB [56, 57]. It has been shown that the absorption of protein fractions increases by aging. Post-translational modifications enhanced by the aging process are a main cause of this phenomenon [58,59,60]. Alternatively, the modified crystallins and non-UV filter metabolites absorb the main portion of UVA [58, 61]. This is responsible for different protein aggregation pathways in UVA compared to UVB. Nevertheless, the beginning of both pathologies is roughly the same as seen in oxidative stress induced by phototoxicity [52]. Cellular mechanisms and pathogenesis of cataract are further discussed in detail in the next section of this study.
Pathogenesis: oxidative stress, phototoxicity, proteins denature, and apoptosis
Oxidative stress
Oxidative stress is known to be one of the central initiating elements which trigger cellular aging pathways and apoptotic cascades [10]. The imbalance between oxidative agents and antioxidants favors this phenomenon. The production of reactive oxygen species (ROS) and oxygen singlet after UV exposure is a known fact, yet the extent of this photodamage is of scientific value [62]. In young lens, glutathione and pyruvate are two natural protective mechanisms against oxidative stress induced by UV [63,64,65]. Further, the increased expression of numerous protective genes, including but not limited to superoxide dismutase, catalase, and glutathione peroxidase, supports a defense against intracellular oxidative stress [66,67,68]. However, according to a study by Bova et al., as the lens ages, the efficacy of this natural filter declines with a rate of 12% per decade [69]. Accumulated ROS gives rise to crystallin and tryptophan denatures which are explained later in this section. Also, an increased activity of xanthine oxidase has been shown to be associated with the increased oxidative stress in senile patients with cataracts [70]. Aside from these pathways, a mitochondrial induced oxidative stress suggests an increase in ROS driven out from UV-exposed respiratory chain leading to phospholipid hyperperoxidase which, in turn, enhances lipid peroxidation and cellular membrane damage in lens epithelial cells [71,72,73]. Also, Wu et al. showed that damaged gap junctions within the cell membrane induced by oxidative stress helps impair inter-cellular antioxidant communication [74]. Besides, It has been described that dysregulation of Na+/K+ ATPase activity caused by oxidative stress deteriorates osmoregulatory function in the cell [75]. In respect to genetic mechanisms responsible for oxidative stress in lens, the possible types of DNA damage and the effects of miRNAs are of considerable importance [76,77,78]. In this regard, Wu et al. proposed regulated miRNA target genes via binding to 3’ UTR and the TATA box regions of oxidative stress genes as a cause of this occurrence [79]. A year later, Wang et al. demonstrated an association between miRNA dysregulations and H2O2 oxidative stress to explain pathogenesis of age-related cataract [80]. Also, Zhu et al. showed that leucine-rich repeat in G protein-couple receptor 4 decreases cellular tolerance to oxidative stress in mice lens augmenting cataract [81]. In addition, Nrf2-Keap1 has been known as a chief defense mechanism against oxidative stress [82]. Nrf2 is one of the nuclear transcriptional proteins which transcribe many antioxidant genes including glutathione-S-transferase, glutathione reductase, and thioredoxin reductase. Keap1 supports Nrf2 to maintain a reasonable level within the cell. Dysregulation in this system induces oxidative stress, which favors cataract [83]. Figure 2 summarizes the main pathways of oxidative stress relating it to other pathogeneses.
Phototoxicity
Vola et al. reported phototoxicity on lens and retina by UV radiation between 392 and 400 nm. During the first decade of life, radiations in this wavelength interval are not absorbed by the human cornea. Progressively, cumulative effect of near-UV on the lens follows fluorescent chromophore formations, reduced lens proteins synthesis, increased insoluble proteins, and lens pigmentation [53]. In 1982, a study by Lerman demonstrated photosensitized damage to the lens and retina with psoralen plus UV radiation (320–400 nm) (PUVA) in experimental animals and reported cataracts in patients undergoing PUVA therapy [84]. An et al. revealed that even though there were no significant differences in the retinal structures comparing UVB-treated mice and the control group, the expression of apoptotic marker proteins, such as Bax, cytochrome c, and p21, decreased in the UVB-treated mice retinas [44, 85]. They argue that cone photoreceptors may be more susceptible to the low-energy UVB light than the other cell types in the retina; thus, low-energy UVB irradiation does not affect the retinal structure, yet it considerably alters cellular protein expression leading to apoptosis and decreased cell survival [85, 86]. Figure 3 shows the schematic view of pathogenesis in UV-induced cataract.
Crystallin proteins
Through a series of transparent tissues, light is transmitted to reach the retina. Despite the fact that the vitreous is not much optically active, cornea and lens play a vital role in filtering the UV radiation. For a young eye, the cornea filters out all radiations with wavelengths less than 295 nm, yet the lens is responsible for absorbing both UVA and UVB [87]. The most abundant component of human lens is composed of a family of proteins called crystallins which cannot be repaired or fixed in case of any damage [88, 89]. α-Crystallins make up about 40% of eye lens proteins. Aside from its role in preventing the formation of aggregates which scatters the light, it plays an important role in sustaining the refractive index of the lens [89]. α-Crystallins are composed of αA and αB components [90]. Investigations on these subunits have shown that A subunit is more susceptible to UVA in contrast to B subunit; thus, the B subunit lingers in its function and keeps a protective role [90]. On the other hand, the B subunit is susceptible to high temperatures leaving the A subunit as the guardian of the lens in hot conditions [91].
In 2004, Fujii et al. investigated the effect of gamma and UVC radiation on the activity of crystallins. They showed that both radiations may affect these proteins. As stated in their research, it is noteworthy that the amount of gamma radiation needed for these effects is far more than the amount one may be exposed to in daily life. However, the situation is different for UVC. The observed effect is seen at lower levels of UVC with which people are actually exposed to on a daily basis [92]. In addition, it has been shown that mutation R116C can regulate α-crystallin capacity to resist stress-induced apoptosis [93]. Besides, it has been revealed that factors other than UV alone can impress the process of aggregation. For instance, hypericin, which is used mostly as an herbal treatment of depression, can make α-crystallins more susceptible to UV light and even incidental visible light [94].
The next key crystallins are the γD-crystallins in the nucleus of the lens. Photooxidation of γ-crystallins is thought to be the major cause in age-related and congenital cataracts which involves misfolding of the proteins and aggregates formations. Moran et al. suggested UVB irradiation as a cause of amorphous amyloid fibers aggregates which leads to cataracts [95]. To date, it has been proven that a wide variety of mutations in γ-crystallin gene make individuals susceptible to cataracts. In this regard, it has been reported that a mutant human γD-crystallin may cause congenital nuclear cataract in afflicted individuals [96]. There have been extensive bio-molecular investigations, mostly in vitro, in order to find out the mechanisms involved in the process of cataracts. In 2013, an in vitro investigation of Schafheimer et al. showed that tryptophan (Trp) clusters protect γ-crystallins by absorbing the energy of UVB light. They further hypothesized that aromatic subunits may absorb light energy protecting from free radicals production. In a further study, they have also found that tyrosine/cysteine clusters sensitize γD-crystallins to UV-induced aggregations [97, 98]. In a study on molecular dynamics simulations carried out in 2013, Xia et al. demonstrated that transformation of Trp to kynurenine (Kyn) under UV exposure affects the stability of γD-crystallins. Besides, they showed that Kyn draws extra water and other polar side chains owing to its additional amino and carbonyl groups on the damaged Trp side chains. Consequently, it breaks through the integrity of the adjacent dry center regions formed by two Greek key motifs in each domain. Large instabilities in the Tyr-Trp-Tyr sandwich-like hydrophobic clusters caused by the damaged Trp residues, in turn, break key hydrogen bonds bridging two b-strands in the Greek key motifs at the “tyrosine corner” [99]. Roskamp et al. investigated different pathways of γS-crystallin aggregations and suggested UVA exposure as the main cause of deamination and oxidation which subsequently leads to protein aggregations. They also proposed that there might be factors other than UV exposure involved in the process of crystallin aggregation. It was observed that wild-type γS-crystallins necessitate a low pH environment to form amyloid fibrils in body temperature [100].
In comparison, β-crystallins are identical to γ-crystallins in structure and play an important role in the maintenance of lens refractive index. Unlike γ-crystallins, β-crystallins have various forms of homomers and heteromers and become easily denaturized both thermally and chemically [101]. Domain substitution and N- and C-terminal extensions account for their oligomerization. This undergoes various modifications as the organism ages [102]. In 2012, Xu et al., in an in vitro investigation, showed that A2V mutations are linked with congenital cataracts by impairing tetramer formation and increasing βB2-crystallin aggregation [103].
Tryptophan proteins
The human eye protects itself against harmful effects of UV light through its UV filter compounds [104]. These proteins have extremely weak photosensitizing properties despite their high absorbance of UV light; thus, they can dissipate the energy from UV to heat and vibration efficiently [105]. The main compounds with such properties are derived from the amino acid Trp via the Kyn pathway. These compounds include Kyn, 3-hydroxykynurenine (3OHKyn) and 3-hydroxykynurenine-O-beta-d-glucoside (3OHKG) and reside in the central part of the human lens—i.e., its nucleus [105]. These compounds are abundant in human lens and have plentiful concentrations until the middle age, after which they decrease in concentration and become involved in chemical reactions, which renders them ineffective and rather harmful in the process of cataractogenesis. It has been shown that these molecules in their free forms can exert their protective effects against UV lights, but when bound to the proteins of the lens (which consists of highest protein concentration in the body with 35% of its wet mass being proteins), they have harmful effects such as production of reactive oxygen species [40, 104]. The process of protein binding of Trp derivatives starts with spontaneous deamination of these compounds to form alpha1-beta unsaturated carbonyls [105]. These carbonyls in turn bind to various residues on lens proteins and glutathione (e.g., cysteine, lysine and histidine residues). Binding to these proteins, Trp derivatives become far better photosensitizers compared to their free counterparts and cause deleterious effects such as cross-linking of lens proteins, conformational changes in these proteins, and oxidative stress in the lens environment. These effects in turn cause alterations in the properties of lens proteins and make them less soluble and more prone to precipitation in the lens [105]. The oxidative stress caused by photosensitization of protein-bound Trp derivatives also increases oxidation of lens proteins and combined with decreased anti-oxidant effectiveness in the aging process, which makes the lens more prone to oxidative damage from UV [104, 106]. Other pathways can also cause oxidation of Trp derivatives, one of which is increasing concentrations of Cu(II) and Fe(III). These elements can decrease the amount of free Trp derivatives through UV-independent redox reactions [105].
The non-enzymatic degradation of Trp due to type I and II photosensitivity reactions is another pathway of oxidative Trp degradation. In these reactions, Trp degrades to compounds such as Trp and oxindolealanine. These reactions happen in the presence of UV light and substances such as riboflavin and advanced glycation end-products (AGEs) [104, 107]. This causes decreased levels of lens protective filters and contributes to cataractogenesis caused by UV in the aged population. AGEs play a key role in cataractogenesis of diabetic and old individuals [108, 109]. A study by Linetsky et al. has revealed the production of AGEs via the ascorbate photooxidation by protein-bound kynurenines induced by UVA [110]. It has also been shown that through aging and UV exposure, the concentration of riboflavin bound Trp increases, which can cause protein aggregation in the lens and contribute to cataractogenesis [111].
Apoptosis
Post-UV exposure apoptosis is a natural protective mechanism directed to remove damaged cells and prevent neoplastic changes; however, it may lead to several complications [112]. It is believed that human lens epithelial cell (HLEC) apoptosis is an initiating element in cataract development [113]. UVB-induced cataract initiates with damages to HLECs triggering apoptosis [71, 114]. In general, UVB-induced apoptosis is regulated by a number of molecular processes which target mitochondria initiating the cell death pathway. Besides, caspase activities may be initiated by the released cytochrome c (Cyt c) from mitochondria [115]. Herein, we discuss and review the studied molecular pathways.
Bax/Bcl-2
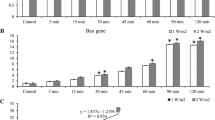
It has been well characterized that apoptosis is regulated by imbalance between bcl-2 and Bax as a pro-apoptotic factor [116]. Ji et al. proved that UVB-induced apoptosis in HLECs leads to lens opacification and cataract. According to the study, the apoptosis occurs by the promoted expression of pro-apoptotic Bax gene and an inhibited expression of anti-apoptotic Bcl-2 gene at both transcript and protein levels. Notably, the ratio of Bax/Bcl-2 displayed a high positive correlation with the proportion of apoptotic HLECs [71].
Caspase-3
It is believed that caspase-3 plays an important role in the execution of apoptosis [117, 118]. Also, the role of caspase-3 activity in HLECs has been noted in the formation of cataracts [118, 119]. After exposure to UV light, the activated caspase-3 is significantly increased in the cell which favors apoptosis [114, 119]. Kim and Koh exposed cultured HLEC lines to UV light and showed an increased expression of NOXA gene and caspase-3 without any increase in the expression of p53. This may suggest that UV-induced apoptosis is caused by a p53-independent pathway in human lens cells [114].
JNK cascade
Ultraviolet-B-induced c-Jun N-terminal kinase (JNK) activation preceded DNA fragmentation in lens [120]. Phosphorylation and activation of JNK are reported to occur prior to caspase-3 cleavage. Long et al. reported JNK activation as an early event in UVB-induced apoptosis which occurs within 30 min subsequent to UVB irradiation. Later, activation of caspase-3 occurs after 1 h and peaks 6 h after UV exposure [113].
MAPK cascade
Evidence suggests that MAPKs are critical in regulating lens apoptosis and cataractogenesis [113, 121]. The intracellular activation of MAPK cascade is a mechanism by which UV radiation mediates cellular responses. Bomser concluded that protein kinase C (PKC) and phosphatidylinositol 3-kinase (PI3-K) activities are not required for UVR-induced MAPK activation; thus, this is not a receptor-mediated event [121].
CALML3
Overexpression of calmodulin-like 3 (CALML3) reverses the effects of UVB irradiation on apoptosis in human lens by decreasing the expression of caspase-3 and Bax and increasing the expression of Bcl-2. In fact, silencing CALML3 had similar effects on UVB irradiation and inhibited the activation of JNK1/2 and ERK1/2 pathways [120].
CRTAC1
Recently, novel mechanisms have been taken into consideration regarding the role of Cartilage acidic protein 1 (CRTAC1). Ji et al. studied the role of CRTAC1 gene in UVB-induced apoptosis in lens and revealed the inhibitory effect of CRTAC1 on oxidative stress and inflammatory response. This is accomplished by inactivating the calcium-signaling, p38, and JNK1/2 signal pathways. This, eventually, reduces UVB-induced apoptosis in HLECs, representing it as a novel target for cataract treatment [122].
Protecting agents
Along many degenerative diseases and abnormalities caused by DNA damage response (DDR) systems, various methods have been introduced in order to reduce the harmful effect of UV on the lens [123]. Various clinical in vitro and in vivo studies have been conducted examining the effect of various agents and their relative outcome. A noteworthy merit of these studies has been the use of diabetic models to evaluate the effect of protective agents [124]. Another merit of these studies is ROS and their corrosive effect on the lens. ROS are able to induce the DDR cascade leading to the activation and cross linking of DNA damage sensors, which in part activates transducers of DNA damage [125]. The two most efficient mediators discussed in these articles are ATM/CHK2 and ATR/CHK1 pathways [126]. These molecular structures activate downstream effector molecules such as p53 and are able to activate complementary systems of cellular stress, such as the VHL/HIF-alpha pathway. This pathway plays a critical role in the appearance of the dusky lens, typically evidenced in cataract. This pathway has also been the focus of various studies, including those exposing the lens to anti-VGEF agents [127]. The convergence of the DNA repair machinery and the angiogenesis cascade has led some researchers to use anti-ROS agents, as a therapy and prevention for UV-induced cataract. They argue that a single blow to the cellular genome and intracellular structures causes the avalanche of signaling which results in cataract [128]. Various agents have been used and the first results have remained rather controversial, as no definitive agent has been proposed, while the ones showing any significant effect have limited availability in clinical contexts [129].
Other studies have suggested that initial molecules of the DDR machinery should be the main target of therapy and prevention. In a study by Zhao et al., it is reported that if the DNA repair machinery is sufficiently activated, or in some instances deactivated, it is possible to completely reverse the effects of ROS and aging, via directing cells to conservative genome repair pathways [130]. The MRN complex, RPA, and the 9-1-1 molecules have been of special interest in this regard [131, 132]. The in vitro and in vivo studies conducted had no follow-up clinical trials.
Most studies conducted on human subjects have used more invasive methods as protection strategies against cataract. Some scholars have proposed the use of intraocular lenses to reduce the harmful effects of the UV light. The trials pertaining to these methods have shown a significantly favorable clinical outcome, as rates of sever cataract have dropped and patients have gained functions such as sleep and dexterity [133]. Regardless of their benefits, these methods have not been without disadvantages, as no case selection has been proposed so far. In addition, the methods themselves are extremely invasive compared to the previously mentioned strategies which aim to reach optimal prevention using supplementary medication [134].
List of studies examining the effectiveness of some recently used agents in UV protection is mentioned in Table 2.
Conclusion
Due to the unquestionable significance of cataracts, in this review, we aimed to revisit the role of ultraviolet radiation in cataracts and to review the cellular pathways behind this ailment. Unlike age as a principal risk factor, ultraviolet radiation exposure can be modified and prevented. In the case of affliction, surgery has been the sole treatment alleviating the disease; however, in accordance with pathogenesis of cataract, more focus on its prevention and novel treatment modalities is expected in the future research. A cost-effective treatment strategy would be indeed indispensable, especially for developing countries as they face grave adversity of outnumbered blindness. The advent of pharmaceutical agents will help avoid considerable expenditure on surgical approaches. Also, new surgical methods and techniques might be clinically and economically facilitative. Further studies are required to enlighten a more detailed picture of signaling pathways in cataractogenesis. In addition, a preventive and curative approach on these pathways will offer original strategies fighting the onerous burden of disease. This review was written to bridge the gap for a detailed classification of ultraviolet effects on cataracts.
References
Bourne RR, Jonas JB, Flaxman SR, Keeffe J, Leasher J, Naidoo K, Parodi MB, Pesudovs K, Price H, White RA, Wong TY, Resnikoff S, Taylor HR, Vision Loss Expert Group of the Global Burden of Disease S (2014) Prevalence and causes of vision loss in high-income countries and in Eastern and Central Europe: 1990-2010. Br J Ophthalmol 98(5):629–638. https://doi.org/10.1136/bjophthalmol-2013-304033
Bourne RRA, Jonas JB, Bron AM, Cicinelli MV, Das A, Flaxman SR, Friedman DS, Keeffe JE, Kempen JH, Leasher J, Limburg H, Naidoo K, Pesudovs K, Peto T, Saadine J, Silvester AJ, Tahhan N, Taylor HR, Varma R, Wong TY, Resnikoff S, Vision Loss Expert Group of the Global Burden of Disease S (2018) Prevalence and causes of vision loss in high-income countries and in Eastern and Central Europe in 2015: magnitude, temporal trends and projections. Br J Ophthalmol 102(5):575–585. https://doi.org/10.1136/bjophthalmol-2017-311258
Khairallah M, Kahloun R, Bourne R, Limburg H, Flaxman SR, Jonas JB, Keeffe J, Leasher J, Naidoo K, Pesudovs K, Price H, White RA, Wong TY, Resnikoff S, Taylor HR, Vision Loss Expert Group of the Global Burden of Disease S (2015) Number of people blind or visually impaired by cataract worldwide and in world regions, 1990 to 2010. Invest Ophthalmol Vis Sci 56(11):6762–6769. https://doi.org/10.1167/iovs.15-17201
Young AR (2006) Acute effects of UVR on human eyes and skin. Prog Biophys Mol Biol 92(1):80–85. https://doi.org/10.1016/J.PBIOMOLBIO.2006.02.005
Abraham AG, Cox C, West S (2010) The differential effect of ultraviolet light exposure on cataract rate across regions of the lens. Invest Ophthalmol Vis Sci 51(8):3919–3923. https://doi.org/10.1167/iovs.09-4557
Widmark J (1891) Ueber die Durchlässigkeit der Augenmedien für ultraviolette Strahlen. Beitr z Ophthalmologie Stockholm:460–502
Davis G (2016) The evolution of cataract surgery. Mo Med 113(1):58–62
Grzybowski A, Ascaso FJ (2014) Sushruta in 600 BC introduced extraocular expulsion of lens material. Acta Ophthalmol 92(2):194–197
Rucker CW (1965) Cataract: a historical perspective. Investig Ophthalmol 4:377–383
Truscott RJ (2005) Age-related nuclear cataract—oxidation is the key. Exp Eye Res 80(5):709–725. https://doi.org/10.1016/j.exer.2004.12.007
Shanmugam P, Ahn Y (2007) Reference solar irradiance spectra and consequences of their disparities in remote sensing of the ocean colour. Ann Geophys 6:1235–1252. https://doi.org/10.5194/angeo-25-1235-2007
Cutchis P (1974) Stratospheric ozone depletion and solar ultraviolet radiation on Earth. Science 184(4132):13–19. https://doi.org/10.1126/science.184.4132.13
Smith RC, Prezelin BB, Baker KS, Bidigare RR, Boucher NP, Coley T, Karentz D, MacIntyre S, Matlick HA, Menzies D et al (1992) Ozone depletion: ultraviolet radiation and phytoplankton biology in Antarctic waters. Science 255(5047):952–959
ISO 21348 Definitions of solar irradiance spectral categories. SpaceWx. https://www.spacewx.com/pdf/SET_21348_2004.pdf. Accessed 20 Feb 2019
McCarty CA, Taylor HR (2002) A review of the epidemiologic evidence linking ultraviolet radiation and cataracts. Dev Ophthalmol 35:21–31
WHO Programme for the Prevention of Blindness & World Health Organization, Office of Global and Integrated Environmental Health (1994) The effects of solar UV radiation on the eye: report of an informal consultation, Geneva, 30 August - 3 September 1993 World Health Organization http://wwwwhoint/iris/handle/10665/62584 Accessed 20 Feb 2019
Giese AC (2012) Living with our sun’s ultraviolet rays. Springer Science & Business Media, Berlin
Diffey BL (1991) Solar ultraviolet radiation effects on biological systems. Phys Med Biol 36(3):299–328
Bais AF, McKenzie RL, Bernhard G, Aucamp PJ, Ilyas M, Madronich S, Tourpali K (2015) Ozone depletion and climate change: impacts on UV radiation. Photochem Photobiol Sci 14(1):19–52. https://doi.org/10.1039/c4pp90032d
Dillon J (1995) UV-B as a pro-aging and pro-cataract factor. Doc Ophthalmol 88(3–4):339–344
Rogers CS, Chan LM, Sims YS, Byrd KD, Hinton DL, Twining SS (2004) The effects of sub-solar levels of UV-A and UV-B on rabbit corneal and lens epithelial cells. Exp Eye Res 78(5):1007–1014. https://doi.org/10.1016/j.exer.2003.12.011
Shoji E (1997) DNA damage and the mechanism following UV-B irradiation in lens epithelial cells. J Jpn Ophthalmol Soc 101(1):40–45
Artigas C, Navea A, Lopez-Murcia MM, Felipe A, Desco C, Artigas JM (2014) Spectral transmission of the pig lens: effect of ultraviolet A+B radiation. J Fr Ophtalmol 37(10):773–779. https://doi.org/10.1016/j.jfo.2014.06.006
Kinsey VE (1948) Spectral transmission of the eye to ultraviolet radiations. Arch Ophthal 39(4):508–513
Sherashov SG (1970) Spectral sensitivity of the cornea to ultraviolet radiation. Biofizika 15(3):543–544
Cullen AP (2002) Photokeratitis and other phototoxic effects on the cornea and conjunctiva. Int J Toxicol 21(6):455–464. https://doi.org/10.1080/10915810290169882
Dixon AJ, Dixon BF (2004) Ultraviolet radiation from welding and possible risk of skin and ocular malignancy. Med J Aust 181(3):155–157
Brown NA (1993) The morphology of cataract and visual performance. Eye (Lond) 7(1):63–67. https://doi.org/10.1038/eye.1993.14
The Italian- American Cataract Study Group (1991) Risk factors for age-related cortical, nuclear, and posterior subcapsular cataracts. Am J Epidemiol 133(6):541–553
Leske MC, Chylack LT Jr, Wu SY (1991) The lens opacities case-control study: risk factors for cataract. Arch Ophthalmol 109(2):244–251. https://doi.org/10.1001/archopht.1991.01080020090051
Pascolini D, Mariotti SP (2012) Global estimates of visual impairment: 2010. Br J Ophthalmol 96(5):614–618. https://doi.org/10.1136/bjophthalmol-2011-300539
Brian G, Taylor H (2001) Cataract blindness: challenges for the 21st century. Bull World Health Organ 79(3):249–256
Javitt JC, Wang F, West SK (1996) Blindness due to cataract: epidemiology and prevention. Annu Rev Public Health 17(1):159–177
Chader GJ, Taylor A (2013) Preface: the aging eye: normal changes, age-related diseases, and sight-saving approaches. Invest Ophthalmol Vis Sci 54(14):ORSF1–ORSF4. https://doi.org/10.1167/iovs.13-12993
Khanna R, Pujari S, Sangwan V (2011) Cataract surgery in developing countries. Curr Opin Ophthalmol 22(1):10–14. https://doi.org/10.1097/ICU.0b013e3283414f50
Balogh TS, Velasco MV, Pedriali CA, Kaneko TM, Baby AR (2011) Ultraviolet radiation protection: current available resources in photoprotection. An Bras Dermatol 86(4):732–742
Kurzel RB, Wolbarsht M, Yamanashi BS, Staton GW, Borkman RF (1973) Tryptophan excited states and cataracts in the human lens. Nature 241(5385):132–133
Gakamsky A, Duncan RR, Howarth NM, Dhillon B, Buttenschon KK, Daly DJ, Gakamsky D (2017) Tryptophan and non-tryptophan fluorescence of the eye lens proteins provides diagnostics of cataract at the molecular level. Sci Rep 7:40375. https://doi.org/10.1038/srep40375
Gakamsky DM, Dhillon B, Babraj J, Shelton M, Smith SD (2011) Exploring the possibility of early cataract diagnostics based on tryptophan fluorescence. J R Soc Interface 8(64):1616–1621. https://doi.org/10.1098/rsif.2010.0608
Mizdrak J, Hains PG, Truscott RJW, Jamie JF, Davies MJ (2008) Tryptophan-derived ultraviolet filter compounds covalently bound to lens proteins are photosensitizers of oxidative damage. Free Radic Biol Med 44(6):1108–1119. https://doi.org/10.1016/j.freeradbiomed.2007.12.003
Taylor LM, Andrew Aquilina J, Jamie JF, Truscott RJ (2002) UV filter instability: consequences for the human lens. Exp Eye Res 75(2):165–175
Chylack LT, Wolfe JK, Singer DM, Leske MC, Bullimore MA, Bailey IL, Friend J, McCarthy D, Wu S-Y, Group LSoCS (1993) The lens opacities classification system III. Arch Ophthalmol 111:1506–1506
Pajer V, Tiboldi A, Bae N, Li K, Kang SU, Hopp B, Kolozsvari L, Lubec G, Nogradi A (2013) The molecular background of the differential UV absorbance of the human lens in the 240-400 nm range. Photochem Photobiol 89(4):856–863. https://doi.org/10.1111/php.12063
Babizhayev MA, Yegorov YE (2014) Biomarkers of oxidative stress and cataract. Novel drug delivery therapeutic strategies targeting telomere reduction and the expression of telomerase activity in the lens epithelial cells with N-acetylcarnosine lubricant eye drops: anti-cataract which helps to prevent and treat cataracts in the eyes of dogs and other animals. Curr Drug Deliv 11(1):24–61
Thrimawithana TR, Rupenthal ID, Rasch SS, Lim JC, Morton JD, Bunt CR (2018) Drug delivery to the lens for the management of cataracts. Adv Drug Deliv Rev. https://doi.org/10.1016/j.addr.2018.03.009
Nguyen SL (2017) Compositions for the treatment of cataracts. U.S. Patent 2017/0027961 A1 Feb 2017
Chen JL, Chen A (2017) Older eyes, cataracts, Lasik and laser eye surgery. Astronomy for Older Eyes. Springer, In, pp 37–54. https://doi.org/10.1007/978-3-319-52413-9_4
Talebizadeh N, Yu Z, Kronschlager M, Soderberg P (2014) Time evolution of active caspase-3 labelling after in vivo exposure to UVR-300 nm. Acta Ophthalmol 92(8):769–773. https://doi.org/10.1111/aos.12407
Ayala MN, Soderberg PG (2004) Vitamin E can protect against ultraviolet radiation-induced cataract in albino rats. Ophthalmic Res 36(5):264–269. https://doi.org/10.1159/000081206
Kador PF, Guo C, Kawada H, Randazzo J, Blessing K (2014) Topical nutraceutical Optixcare EH ameliorates experimental ocular oxidative stress in rats. J Ocul Pharmacol Ther 30(7):593–602. https://doi.org/10.1089/jop.2014.0016
Kleinmann G, Hoffman P, Schechtman E, Pollack A (2002) Microscope-induced retinal phototoxicity in cataract surgery of short duration. Ophthalmology 109(2):334–338
Aldana BZ (2011) Phototoxicity: ultraviolet radiation and cataracts. Arch Soc Esp Oftalmol 86(9):306–306. https://doi.org/10.1016/j.oftal.2011.06.013
Vola J, Petrakian J, Mardrus R (1988) Phototoxicity of ultraviolet rays on crystalline lens and retina. Study of the optic transmission of implants with or without anti-UV treatment. J Francais D’ophtalmologie 11(3):277–283
Sliney DH (1995) UV radiation ocular exposure dosimetry. J Photochem Photobiol B 31(1–2):69–77
Taylor HR, West SK, Rosenthal FS, Munoz B, Newland HS, Abbey H, Emmett EA (1988) Effect of ultraviolet radiation on cataract formation. N Engl J Med 319(22):1429–1433. https://doi.org/10.1056/NEJM198812013192201
Cetinel S, Semenchenko V, Cho JY, Sharaf MG, Damji KF, Unsworth LD, Montemagno C (2017) UV-B induced fibrillization of crystallin protein mixtures. PLoS One 12(5):e0177991. https://doi.org/10.1371/journal.pone.0177991
Lofgren S (2017) Solar ultraviolet radiation cataract. Exp Eye Res 156:112–116. https://doi.org/10.1016/j.exer.2016.05.026
Hains PG, Truscott RJ (2007) Post-translational modifications in the nuclear region of young, aged, and cataract human lenses. J Proteome Res 6(10):3935–3943. https://doi.org/10.1021/pr070138h
Wilmarth P, Tanner S, Dasari S, Nagalla S, Riviere M, Bafna V, Pevzner P, David L (2006) Age-related changes in human crystallins determined from comparative analysis of post-translational modifications in young and aged lens: does deamidation contribute to crystallin insolubility? J Proteome Res 5(10):2554–2566. https://doi.org/10.1021/pr050473a
Miesbauer LR, Zhou X, Yang Z, Sun Y, Smith D, Smith J (1994) Post-translational modifications of water-soluble human lens crystallins from young adults. J Biol Chem 269(17):12494–12502
Weinreb O, Dovrat A, Dunia I, Benedetti EL, Bloemendal H (2001) UV-A-related alterations of young and adult lens water-insoluble alpha-crystallin, plasma membranous and cytoskeletal proteins. Eur J Biochem 268(3):536–543
Varma SD, Chand D, Sharma YR, Kuck JF Jr, Richards RD (1984) Oxidative stress on lens and cataract formation: role of light and oxygen. Curr Eye Res 3(1):35–57
Lu Q, Hao M, Wu W, Zhang N, Isaac AT, Yin J, Zhu X, Du L, Yin X (2018) Antidiabetic cataract effects of GbE, rutin and quercetin are mediated by the inhibition of oxidative stress and polyol pathway. Acta Biochim Pol 65(1):35–41. https://doi.org/10.18388/abp.2016_1387
Kaur J, Kukreja S, Kaur A, Malhotra N, Kaur R (2012) The oxidative stress in cataract patients. J Clin Diagn Res 6(10):1629–1632. https://doi.org/10.7860/JCDR/2012/4856.2626
Spector A, Wang GM, Wang RR, Garner WH, Moll H (1993) The prevention of cataract caused by oxidative stress in cultured rat lenses. I. H2O2 and photochemically induced cataract. Curr Eye Res 12(2):163–179
Zhang Y, Zhang L, Sun D, Li Z, Wang L, Liu P (2011) Genetic polymorphisms of superoxide dismutases, catalase, and glutathione peroxidase in age-related cataract. Mol Vis 17:2325
Cejková J, Stipek S, Crkovska J, Ardan T (2000) Changes of superoxide dismutase, catalase and glutathione peroxidase in the corneal epithelium after UVB rays. Histochemical and biochemical study. Histol Histopathol 15(4):1043–1050. https://doi.org/10.14670/HH-15.1043
Fecondo JV, Augusteyn RC (1983) Superoxide dismutase, catalase and glutathione peroxidase in the human cataractous lens. Exp Eye Res 36(1):15–23
Bova LM, Sweeney MH, Jamie JF, Truscott RJ (2001) Major changes in human ocular UV protection with age. Invest Ophthalmol Vis Sci 42(1):200–205
Miric DJ, Kisic BB, Zoric LD, Mitic RV, Miric BM, Dragojevic IM (2013) Xanthine oxidase and lens oxidative stress markers in diabetic and senile cataract patients. J Diabetes Complicat 27(2):171–176. https://doi.org/10.1016/j.jdiacomp.2012.09.005
Ji Y, Cai L, Zheng T, Ye H, Rong X, Rao J, Lu Y (2015) The mechanism of UVB irradiation induced-apoptosis in cataract. Mol Cell Biochem 401(1–2):87–95. https://doi.org/10.1007/s11010-014-2294-x
Babizhayev MA (2011) Mitochondria induce oxidative stress, generation of reactive oxygen species and redox state unbalance of the eye lens leading to human cataract formation: disruption of redox lens organization by phospholipid hydroperoxides as a common basis for cataract disease. Cell Biochem Funct 29(3):183–206. https://doi.org/10.1002/cbf.1737
Bantseev V, Youn HY (2006) Mitochondrial “movement” and lens optics following oxidative stress from UV-B irradiation: cultured bovine lenses and human retinal pigment epithelial cells (ARPE-19) as examples. Ann N Y Acad Sci 1091:17–33. https://doi.org/10.1196/annals.1378.051
Wu D, Zhao J, Wu D, Zhang J (2011) Ultraviolet A exposure induces reversible disruption of gap junction intercellular communication in lens epithelial cells. Int J Mol Med 28(2):239–245. https://doi.org/10.3892/ijmm.2011.665
Chan AW, Ho YS, Chung SK, Chung SS (2008) Synergistic effect of osmotic and oxidative stress in slow-developing cataract formation. Exp Eye Res 87(5):454–461. https://doi.org/10.1016/j.exer.2008.08.001
Mesa R, Bassnett S (2013) UV-B-induced DNA damage and repair in the mouse lens. Invest Ophthalmol Vis Sci 54(10):6789–6797. https://doi.org/10.1167/iovs.13-12644
Osnes-Ringen O, Azqueta AO, Moe MC, Zetterstrom C, Roger M, Nicolaissen B, Collins AR (2013) DNA damage in lens epithelium of cataract patients in vivo and ex vivo. Acta Ophthalmol 91(7):652–656. https://doi.org/10.1111/j.1755-3768.2012.02500.x
Yu X, Zheng H, Chan MT, Wu WKK (2017) MicroRNAs: new players in cataract. Am J Transl Res 9(9):3896–3903
Wu C, Liu Z, Ma L, Pei C, Qin L, Gao N, Li J, Yin Y (2017) MiRNAs regulate oxidative stress related genes via binding to the 3' UTR and TATA-box regions: a new hypothesis for cataract pathogenesis. BMC Ophthalmol 17(1):142–142. https://doi.org/10.1186/s12886-017-0537-9
Wang S, Guo C, Yu M, Ning X, Yan B, Zhao J, Yang A, Yan H (2018) Identification of H2O2 induced oxidative stress associated microRNAs in HLE-B3 cells and their clinical relevance to the progression of age-related nuclear cataract. BMC Ophthalmol 18(1):93–93. https://doi.org/10.1186/s12886-018-0766-6
Zhu J, Hou Q, Dong XD, Wang Z, Chen X, Zheng D, Zhou L, He C, Liu M, Tu L, Qu J (2015) Targeted deletion of the murine Lgr4 gene decreases lens epithelial cell resistance to oxidative stress and induces age-related cataract formation. PLoS One 10(3):e0119599. https://doi.org/10.1371/journal.pone.0119599
Motohashi H, Yamamoto M (2004) Nrf2–Keap1 defines a physiologically important stress response mechanism. Trends Mol Med 10(11):549–557. https://doi.org/10.1016/j.molmed.2004.09.003
Liu XF, Hao JL, Xie T, Malik TH, Lu CB, Liu C, Shu C, Lu CW, Zhou DD (2017) Nrf2 as a target for prevention of age-related and diabetic cataracts by against oxidative stress. Aging Cell 16(5):934–942. https://doi.org/10.1111/acel.12645
Lerman S (1982) Ocular phototoxicity and psoralen plus ultraviolet radiation (320–400 nm) therapy: an experimental and clinical evaluation. J Natl Cancer Inst 69(1):287–302
An MJ, Kim CH, Nam GY, Kim DH, Rhee S, Cho SJ, Kim JW (2018) Transcriptome analysis for UVB-induced phototoxicity in mouse retina. Environ Toxicol 33(1):52–62. https://doi.org/10.1002/tox.22494
Bhuyan DK, Bhuyan KC (1994) Assessment of oxidative stress to eye in animal model for cataract. Methods Enzymol 233:630–639
Bassnett S, Shi Y, Vrensen GFJM (2011) Biological glass: structural determinants of eye lens transparency. Philos Trans R Soc B Biol Sci 366(1568):1250–1264. https://doi.org/10.1098/rstb.2010.0302
Andley UP (2007) Crystallins in the eye: function and pathology. Prog Retin Eye Res 26:78–98. https://doi.org/10.1016/J.PRETEYERES.2006.10.003
Horwitz J, Bova MP, Ding L-L, Haley DA, Stewart PL (1999) Lens α-crystallin: function and structure. Eye 13:403. https://doi.org/10.1038/eye.1999.114
Weinreb O, van Boekel MA, Dovrat A, Bloemendal H (2000) Effect of UV-A light on the chaperone-like properties of young and old lens alpha-crystallin. Invest Ophthalmol Vis Sci 41(1):191–198
van Boekel MA, Hoogakker SE, Harding JJ, de Jong WW (1996) The influence of some post-translational modifications on the chaperone-like activity of alpha-crystallin. Ophthalmic Res 28(Suppl 1):32–38. https://doi.org/10.1159/000267940
Fujii N, Uchida H, Saito T (2004) The damaging effect of UV-C irradiation on lens alpha-crystallin. Mol Vis 10:814–820
Andley UP, Patel HC, Xi JH (2002) The R116C mutation in alpha A-crystallin diminishes its protective ability against stress-induced lens epithelial cell apoptosis. J Biol Chem 277(12):10178–10186. https://doi.org/10.1074/jbc.M109211200
Ehrenshaft M, Roberts JE, Mason RP (2013) Hypericin-mediated photooxidative damage of alpha-crystallin in human lens epithelial cells. Free Radic Biol Med 60:347–354. https://doi.org/10.1016/j.freeradbiomed.2013.02.023
Moran SD, Zhang TO, Decatur SM, Zanni MT (2013) Amyloid fiber formation in human gammaD-crystallin induced by UV-B photodamage. Biochemistry 52(36):6169–6181. https://doi.org/10.1021/bi4008353
Ji F, Jung J, Koharudin LM, Gronenborn AM (2013) The human W42R gammaD-crystallin mutant structure provides a link between congenital and age-related cataracts. J Biol Chem 288(1):99–109. https://doi.org/10.1074/jbc.M112.416354
Schafheimer N, King J (2013) Tryptophan cluster protects human gammaD-crystallin from ultraviolet radiation-induced photoaggregation in vitro. Photochem Photobiol 89(5):1106–1115. https://doi.org/10.1111/php.12096
Schafheimer N, Wang Z, Schey K, King J (2014) Tyrosine/cysteine cluster sensitizing human gammaD-crystallin to ultraviolet radiation-induced photoaggregation in vitro. Biochemistry 53(6):979–990. https://doi.org/10.1021/bi401397g
Xia Z, Yang Z, Huynh T, King JA, Zhou R (2013) UV-radiation induced disruption of dry-cavities in human gammaD-crystallin results in decreased stability and faster unfolding. Sci Rep 3:1560–1560. https://doi.org/10.1038/srep01560
Roskamp KW, Montelongo DM, Anorma CD, Bandak DN, Chua JA, Malecha KT, Martin RW (2017) Multiple aggregation pathways in human gammaS-crystallin and its aggregation-prone G18V variant. Invest Ophthalmol Vis Sci 58(4):2397–2405. https://doi.org/10.1167/iovs.16-20621
Serebryany E, King JA (2014) The betagamma-crystallins: native state stability and pathways to aggregation. Prog Biophys Mol Biol 115(1):32–41. https://doi.org/10.1016/j.pbiomolbio.2014.05.002
Sergeev YV, Hejtmancik JF, Wingfield PT (2004) Energetics of domain–domain interactions and entropy driven association of β-crystallins. Biochemistry 43(2):415–424. https://doi.org/10.1021/bi034617f
Xu J, Wang S, Zhao W-J, Xi Y-B, Yan Y-B, Yao K (2012) The congenital cataract-linked A2V mutation impairs tetramer formation and promotes aggregation of βB2-crystallin. PLoS One 7(12):e51200. https://doi.org/10.1371/journal.pone.0051200
Avila F, Friguet B, Silva E (2015) Photosensitizing activity of endogenous eye lens chromophores: an attempt to unravel their contributions to photo-aging and cataract disease. Photochem Photobiol 91(4):767–779. https://doi.org/10.1111/php.12443
Tweeddale HJ, Hawkins CL, Janmie JF, Truscott RJW, Davies MJ (2016) Cross-linking of lens crystallin proteins induced by tryptophan metabolites and metal ions: implications for cataract development. Free Radic Res 50(10):1116–1130. https://doi.org/10.1080/10715762.2016.1210802
Kurzel RB, Wolbarsht M, Yamanashi BS, Staton GW, Borkman RF (1973) Tryptophan excited states and cataracts in the human lens 20. Nature 241(5385):132–133. https://doi.org/10.1038/241132a0
De La Rochette A, Birlouez-Aragon I, Silva E, Morlière P (2003) Advanced glycation endproducts as UVA photosensitizers of tryptophan and ascorbic acid: consequences for the lens. Biochim Biophys Acta Gen Subj 1621(3):235–241. https://doi.org/10.1016/S0304-4165(03)00072-2
Stitt AW (2001) Advanced glycation: an important pathological event in diabetic and age related ocular disease. Br J Ophthalmol 85(6):746–753. https://doi.org/10.1136/bjo.85.6.746
Katta AV, Suryakar A, Katkam R, Shaikh K, Ghodake SR (2009) Glycation of lens crystalline protein in the pathogenesis of various forms of cataract
Linetsky M, Raghavan CT, Johar K, Fan X, Monnier VM, Vasavada AR, Nagaraj RH (2014) UVA light-excited kynurenines oxidize ascorbate and modify lens proteins through the formation of advanced glycation end products: implications for human lens aging and cataract formation. J Biol Chem 289(24):17111–17123. https://doi.org/10.1074/jbc.M114.554410
Mancini M, Edwards AM, Becker MI (2000) Reactivity of monoclonal antibodies against a tryptophan-riboflavin adduct toward irradiated and non-irradiated bovine-eye-lens protein fractions: an indicator of in vivo visible-light-mediated phototransformations. J Photochem Photobiol B Biol 55(1):9–15. https://doi.org/10.1016/S1011-1344(00)00014-2
Ibuki Y, Goto R (2002) Antiapoptotic effects induced by different wavelengths of ultraviolet light. Photochem Photobiol 75(5):495–502
Long AC, Colitz CM, Bomser JA (2004) Apoptotic and necrotic mechanisms of stress-induced human lens epithelial cell death. Exp Biol Med 229(10):1072–1080
Kim S-T, Koh J-W (2011) Mechanisms of apoptosis on human lens epithelium after ultraviolet light exposure. Korean J Ophthalmol 25(3):196–201. https://doi.org/10.3341/kjo.2011.25.3.196
Ricci J-E, Gottlieb RA, Green DR (2003) Caspase-mediated loss of mitochondrial function and generation of reactive oxygen species during apoptosis. J Cell Biol 160(1):65–75. https://doi.org/10.1083/jcb.200208089
Siddiqui WA, Ahad A, Ahsan H (2015) The mystery of BCL2 family: Bcl-2 proteins and apoptosis: an update. Arch Toxicol 89(3):289–317. https://doi.org/10.1007/s00204-014-1448-7
Roy S (2000) Caspases at the heart of the apoptotic cell death pathway. Chem Res Toxicol 13(10):961–962
Andersson M, Honarvar A, Sjöstrand J, Peterson A, Karlsson J-O (2003) Decreased caspase-3 activity in human lens epithelium from posterior subcapsular cataracts. Exp Eye Res 76(2):175–182
Yao H, Tang X, Shao X, Feng L, Wu N, Yao K (2007) Parthenolide protects human lens epithelial cells from oxidative stress-induced apoptosis via inhibition of activation of caspase-3 and caspase-9. Cell Res 17(6):565. https://doi.org/10.1038/cr.2007.6
Jia Y, Qin Q, Fang CP, Shen W, Sun TT, Huang YL, Li WJ, Deng AM (2018) UVB induces apoptosis via downregulation of CALML3-dependent JNK1/2 and ERK1/2 pathways in cataract. Int J Mol Med 41(5):3041–3050. https://doi.org/10.3892/ijmm.2018.3478
Bomser JA (2002) Selective induction of mitogen-activated protein kinases in human lens epithelial cells by ultraviolet radiation. J Biochem Mol Toxicol 16(1):33–40
Ji Y, Rong X, Li D, Cai L, Rao J, Lu Y (2016) Inhibition of cartilage acidic protein 1 reduces ultraviolet B irradiation induced-apoptosis through P38 mitogen-activated protein kinase and Jun amino-terminal kinase pathways. Cell Physiol Biochem 39(6):2275–2286. https://doi.org/10.1159/000447920
Huang L-L, Hess JL, Bunce G (1990) DNA damage, repair, and replication in selenite-induced cataract in rat lens. Curr Eye Res 9(11):1041–1050
Pollreisz A, Schmidt-Erfurth U (2010) Diabetic cataract—pathogenesis, epidemiology and treatment. J Ophthalmol 2010:608751. https://doi.org/10.1155/2010/608751
Babizhayev MA, Yegorov YE (2016) Reactive oxygen species and the aging eye: specific role of metabolically active mitochondria in maintaining lens function and in the initiation of the oxidation-induced maturity onset cataract—a novel platform of mitochondria-targeted antioxidants with broad therapeutic potential for redox regulation and detoxification of oxidants in eye diseases. Am J Ther 23(1):e98–e117. https://doi.org/10.1097/MJT.0b013e3181ea31ff
Wang Y, Zhang J, Wu J, Guan H (2017) Expression of DNA repair genes in lens cortex of age-related cortical cataract. Exp Mol Pathol 102(2):219–223. https://doi.org/10.1016/j.yexmp.2017.02.006
Falcão MS, Freitas-Costa P, Beato JN, Pinheiro-Costa J, Rocha-Sousa A, Carneiro Â, Brandão EM, Falcão-Reis F (2017) Safety and effectiveness of cataract surgery with simultaneous intravitreal anti-VEGF in patients with previously treated exudative age-related macular degeneration. Acta medica portuguesa 30(2):127–133. https://doi.org/10.20344/amp.7850
Thiagarajan R, Manikandan R (2013) Antioxidants and cataract. Free Radic Res 47(5):337–345. https://doi.org/10.3109/10715762.2013.777155
Gritz DC, Srinivasan M, Smith SD, Kim U, Lietman TM, Wilkins JH, Priyadharshini B, John RK, Aravind S, Prajna NV (2006) The Antioxidants in Prevention of Cataracts Study: effects of antioxidant supplements on cataract progression in South India. Br J Ophthalmol 90(7):847–851. https://doi.org/10.1136/bjo.2005.088104
Zhao W, Zhao W, Zhao J, Wang D, Li J (2015) Screening of potential target genes for cataract by analyzing mRNA expression profile of mouse Hsf4-null lens. BMC Ophthalmol 15(1):76. https://doi.org/10.1186/s12886-015-0066-3
Valverde GL, Martin EG, Povés JML, Llorens VP, Júlvez LEP (2016) Study of association between pre-senile cataracts and the polymorphisms rs2228000 in XPC and rs1042522 in p53 in Spanish population. PLoS One 11(6):e0156317. https://doi.org/10.1371/journal.pone.0156317
Lim PX, Patel DR, Poisson KE, Basuita M, Tsai C, Lyndaker AM, Hwang B-J, Lu A-L, Weiss RS (2015) Genome protection by the 9-1-1 complex subunit HUS1 requires clamp formation, DNA contacts, and ATR signaling-independent effector functions. J Biol Chem 290(24):14826–14840. https://doi.org/10.1074/jbc.M114.630640
Ayaki M, Negishi K, Tsubota K (2014) Rejuvenation effects of cataract surgery with ultraviolet blocking intra-ocular lens on circadian rhythm and gait speed. Rejuvenation Res 17(4):359–365. https://doi.org/10.1089/rej.2014.1550
Augustin A (2014) Reliable UV-light protection in intraocular lenses--scientific rationale and quality requirements. Klinische Monatsblatter fur Augenheilkunde 231(9):901–908. https://doi.org/10.1055/s-0034-1368566
Abdel-Ghaffar A, Ghanem HM, Ahmed EK, Hassanin OA, Mohamed RG (2018) Ursodeoxycholic acid suppresses the formation of fructose/streptozotocin-induced diabetic cataract in rats. Fundam Clin Pharmacol 32(6):627–640. https://doi.org/10.1111/fcp.12385
Lodovici M, Caldini S, Morbidelli L, Akpan V, Ziche M, Dolara P (2009) Protective effect of 4-coumaric acid from UVB ray damage in the rabbit eye. Toxicology 255(1–2):1–5. https://doi.org/10.1016/j.tox.2008.09.011
Avetisov S, Polunin G, Sheremet N, Makarov I, Fedorov A, Karpova O, Muranov K, Dizhevskaia A, Soustov L, Chelnokov E (2008) Chaperon-like anticataract agents, the antiaggregants of lens crystallin. Communication 4. Study of the effect of a mixture of di-and tetrapeptides on a prolonged rat model of UV-induced cataract. Vestnik oftalmologii 124(2):12–16135
Mayer U, Müller Y, Blüthner K (2001) Vitamins C and E protect cultures of bovine lens epithelium from the damaging effects of blue light (430 nm) and UVA light (300-400 nm). Klinische Monatsblatter fur Augenheilkunde 218(2):116–120. https://doi.org/10.1055/s-2001-12255
Danielczyk K, Dziegiel P (2009) The expression of MT1 melatonin receptor and Ki-67 antigen in melanoma malignum. Anticancer Res 29(10):3887–3895
Varma SD, Hegde KR, Kovtun S (2008) UV-B-induced damage to the lens in vitro: prevention by caffeine. J Ocul Pharmacol Ther 24(5):439–444. https://doi.org/10.1089/jop.2008.0035
Hegde KR, Kovtun S, Varma SD (2007) Induction of ultraviolet cataracts in vitro: prevention by pyruvate. J Ocul Pharmacol Ther 23(5):492–502. https://doi.org/10.1089/jop.2007.0038
Liao J-H, Lin I-L, Huang K-F, Kuo P-T, Wu S-H, Wu T-H (2014) Carnosine ameliorates lens protein turbidity formations by inhibiting calpain proteolysis and ultraviolet C-induced degradation. J Agric Food Chem 62(25):5932–5938. https://doi.org/10.1021/jf5017708
Hu C-C, Liao J-H, Hsu K-Y, Lin IL, Tsai M-H, Wu W-H, Wei T-T, Huang Y-S, Chiu S-J, Chen H-Y, Wu S-H, Wu T-H (2011) Role of pirenoxine in the effects of catalin on in vitro ultraviolet-induced lens protein turbidity and selenite-induced cataractogenesis in vivo. Mol Vis 17:1862–1870
Attanasio F, Cataldo S, Fisichella S, Nicoletti S, Nicoletti VG, Pignataro B, Savarino A, Rizzarelli E (2009) Protective effects of L-and D-carnosine on α-crystallin amyloid fibril formation: implications for cataract disease. Biochemistry 48(27):6522–6531. https://doi.org/10.1021/bi900343n
Kronschlager M, Galichanin K, Ekstrom J, Lou MF, Soderberg PG (2012) Protective effect of the thioltransferase gene on in vivo UVR-300 nm-induced cataract. Invest Ophthalmol Vis Sci 53(1):248–252. https://doi.org/10.1167/iovs.11-8504
Liu L, Yu R, Shi Y, Dai Y, Zeng Z, Guo X, Ji Q, Wang G, Zhong J (2014) Transduced protein transduction domain linked HSP27 protected LECs against UVB radiation-induced damage. Exp Eye Res 120:36–42. https://doi.org/10.1016/j.exer.2013.12.016
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kamari, F., Hallaj, S., Dorosti, F. et al. Phototoxicity of environmental radiations in human lens: revisiting the pathogenesis of UV-induced cataract. Graefes Arch Clin Exp Ophthalmol 257, 2065–2077 (2019). https://doi.org/10.1007/s00417-019-04390-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04390-3