Abstract
Objective
X-linked myopathy with excessive autophagy (XMEA) linked to the VMA21 gene leads to autophagy failure with progressive vacuolation and atrophy of skeletal muscles. Current knowledge of this rare disease is limited. Our objective was to define the clinical, radiological, and natural history of XMEA.
Methods
We conducted a retrospective study collecting clinical, genetic, muscle imaging, and biopsy data of XMEA patients followed in France and reviewed the literature for additional cases.
Results
Eighteen males had genetically confirmed XMEA in France, carrying four different VMA21 variants. Mean age at disease onset was 9.4 ± 9.9 (range 1–40) years. In 14/18 patients (77.8%), onset occurred during childhood (< 15 years); however in four patients, the disease started in adulthood. Patients had anterior and medial compartment thigh muscle weakness, distal contractures (56.3%), elevated CK levels (1287.9 ± 757.8 U/l) and autophagic vacuoles with sarcolemmal features on muscle histopathology. Muscle MRI (n = 10) showed a characteristic pattern of lower limb muscle involvement. In 11 patients, outcome measures were available for an average follow-up period of 10.6 ± 9.8 years and six of them show disease progression. Mean change of functional outcomes was 0.5 ± 1.2 points for Brooke and 2.2 ± 2.5 points for Vignos score, 7/16 patients (43.8%) needed a walking aid and 3/16 (18.8%) were wheelchair-bound (median age of 40 years old, range 39–48). The variant c.164-7 T > G was associated with a later onset of symptoms. Respiratory insufficiency was common (57.1%) but cardiac involvement rare (12.5%).
Interpretation
XMEA has variable age of onset, but a characteristic clinical, histopathological, and muscle imaging presentation, guiding the diagnosis. Although slowly, motor disability progresses with time, and relevant genotype–phenotype correlations will help design future clinical trials.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
X-linked myopathy with excessive autophagy (XMEA) (OMIM 310440) is a monogenic disorder characterized by a progressive vacuolation and atrophy of skeletal muscles. XMEA is caused by pathogenic variants in the VMA21 gene at Xq28, resulting in a reduced expression of the vacuolar ATPase assembly factor 21 (VMA21) protein, a key proton pump for endo-lysosomal acidification, with consequent impairment of lysosomal function leading to autophagy failure [1]. From a pathological point of view, this leads to the accumulation of cytoplasmic vacuoles in muscle cells, described by Sugie et al. as autophagic vacuoles with sarcolemmal features (AVSF) [2].
First reported by Kalimo et al. in 1988 [3], the disease was initially described as a childhood-onset, slowly progressive, proximal-predominant myopathy, sparing cardiac and respiratory muscles. Individual case reports and small patient series have been published since. Nevertheless, a comprehensive description of a large series of patients with XMEA is lacking and the natural history of the disease is mostly unknown. Finally, although potential treatment strategies in myopathies with AVSF already exist, such as targeting autophagy through the overexpression of Vps15 + PIK3C3 [4], no current disease-modifying therapy is available for XMEA.
In this multicentric retrospective study, we describe the clinical, electrophysiological, histopathological, and muscle MRI features as well as the progression of the disease in 18 patients with genetically confirmed XMEA followed in France, the largest cohort reported so far. In addition, the literature was carefully revisited to include an additional eight genetically confirmed XMEA patients for a pooled analysis.
Patients and methods
Data from the French patient series originated from the electronic clinical records of Pitié-Salpêtrière Hospital in Paris and seven other neuromuscular reference centers in France (Angers, Bordeaux, Lyon, Marseille, Nantes, Rennes, Strasbourg) (n = 18).
The following data were collected: “first progressive symptom” as the first progressive motor deficit, leading the patient (or parents) to request a medical advice; age at onset; neonatal or infantile manifestations before the first progressive symptom; age at first examination; neurological examination (including Medical Research Council scale, MRC); functional data (Brooke and Vignos scores), need for a walking aid or loss of ambulation; electroneuromyography (ENMG) findings; initial creatine kinase (CK) level (normal < 200 U/l); and histopathological data from muscle biopsies. Cardiac and respiratory examinations were also reviewed. Respiratory insufficiency was considered moderate if vital capacity (VC) was 50–79% of the populations’ theorical value and severe if it was less than 50%.
Furthermore, in all patients, lower limb or whole-body muscle MRI had been performed as part of the routine diagnostic process. T1-weighted (T1W) and short-tau inversion recovery (STIR) sequences were analyzed and scored by the same radiologist (IA), with experience in muscle imaging. Images were scored using the Mercuri muscle MRI staging [5] as follows: 1. normal appearance; 2. early moth-eaten appearance, with scattered small areas of increased signal or with numerous discrete areas of increased signal with beginning confluence, comprising less than 30% of the volume of the individual muscle (mild involvement); 3. late moth-eaten appearance, with numerous discrete areas of increased signal with beginning confluence, comprising 30–60% of the volume of the individual muscle (moderate involvement); 4. an end-stage, washed-out or fuzzy appearance due to confluent areas of increased signal, with muscle replaced by increased density connective tissue and fat and only a rim of fascia and neurovascular structures distinguishable (severe involvement).
VMA21 (NM_001017980.4) gene variants were analyzed through Sanger sequencing or a dedicated next generation sequencing (NGS) gene panel. Each variant was classified following the American College of Medical Genetics (ACMG) classification [6].
For all but two patients (patients 12 and 18, lost to follow-up), follow-up data were collected and reviewed, focusing on the appearance of new symptoms and the variation of functional scores.
A review of the literature was performed using the PubMed tool to explore the Medline database and identify all reports of XMEA patients. The keywords “XMEA” and “X-linked myopathy with excessive autophagy” and the filter “human” identified 12 case reports and/or series accounting for 38 XMEA patients [3, 7,8,9,10,11,12,13,14,15,16,17], among whom 15 had a genetic confirmation [9,10,11,12, 14,15,16,17]. Seven of these genetically confirmed XMEA patients from the literature review were already part of our French series [8, 12, 17]; therefore, eight genetically confirmed XMEA patients from the literature were finally added, for a total of 26 patients to run a pooled analysis.
In accordance with French legislation, the study was registered with and is accessible to the French data protection authority (CNIL, Commission Nationale de l’Informatique et des Libertés).
Statistical analysis
Data analysis was performed using GraphPad Prism 10.0.3. Mean and median values, standard deviation (SD), range of quantitative variables, and absolute or relative frequencies of categorical variables were reported. Association was studied through the Mann–Whitney test (continuous dependent variables) and the Fisher’s exact test (categorical dependent variables). Kaplan–Meier curves and log-rank test were used to estimate the probability of needing a walking aid. Statistical significance was established at p ≤ 0.05.
Results
Clinical features at onset
Eighteen male patients from 13 different families were included in the French series (Table 1). Fourteen patients (77.8%) had an onset of the first symptom during childhood or adolescence (age < 15 years), with a mean age of 5 ± 2.6 years, while four (22.2%) had an onset during adulthood (≥ 15 years), with a mean age of 25.3 ± 10.4 years. Of the four latter, one patient had a very late onset of symptoms (40 years).
A symmetrical, proximal-predominant lower limb muscle weakness was the first progressive symptom in all patients, with psoas and quadriceps muscles being most frequently weak at the first examination. MRC scores for limb muscle weakness at first examination are shown in Fig. 1. Distal limb contractures were frequent (56.3%), scapula alata was present in four patients (22.2%), and no facial weakness or ptosis was observed (Table 1). Functional outcomes at first examination showed a median Brooke score of 1 (range 1–3) and a median Vignos score of 2 (range 1–6), and all patients were ambulatory without the need of walking aids. No patient showed respiratory insufficiency or cardiac disease at onset.
Clinical presentation of VMA21-linked XMEA patients. A.1) Heatmap showing the detailed MRC muscle power scale score results of muscle testing in 13 patients. Gray squares indicate that data were unavailable. A.2) Summary of clinical muscle involvement in XMEA, with a predominant hip flexion (psoas), knee extension (quadriceps) and hip adduction (adductor muscles) motor weakness, milder deltoid and triceps muscle weakness in the upper limbs as well as distal lower limb involvement
Regarding psychomotor development, one patient had language delay and one patient had mild intellectual disability, although no intellectual quotient tests were performed. MRI imaging for the second patient did not reveal cortical brain atrophy or white matter abnormalities.
The mother of the siblings P1, P2, and P3 as well as the one of P13 and the one of P16, three probable (although unconfirmed) female carriers of VMA21 variants, were explored by experts in neuromuscular disorders (MS, ESC and TS), showing no signs nor symptoms of the disease. However, no other test was performed (CK levels or muscle MRI).
Disease progression.
Data at last examination were available for 16/18 patients (mean age of 36.1 ± 17 years); the median Brooke score was 3 (mean 2.8 ± 2.3, range 1–6) and the median Vignos score at last examination was 6 (mean 4.7 ± 2.6, range 1–9).
In 11/18 patients, two Brooke and Vignos scores were available at different time points (with a mean elapsed time between measurements of 10.6 ± 9.8 years): mean change was 0.5 ± 1.2 points for the Brooke score and 2.2 ± 2.5 points for the Vignos score. In 5/11 patients these scores were stable, although in two cases follow-up was less than 2 years.
Regarding ambulation, seven (43.8%) patients needed a walking aid at a median disease duration of 15 years (range 2–29) and three (18.8%) patients were wheelchair-bound at a median disease duration of 37 years (range 35–47) (and a median age of 40 years old, range 39–48).
Respiratory insufficiency was reported in 8/14 patients (57.1%) at a median age of 31.5 years old (range 15–45) and occurred at a median of 9 years (range 5–28) after onset of the disease. Four patients needed non-invasive ventilation (NIV) by the last examination. Pulmonary function tests were available in 4/8 patients with respiratory insufficiency, showing a restrictive pattern. Three of these patients had moderate restrictive respiratory insufficiency (VC theoretical value = 70% at 15 years old, 64% at 24 years old, and 70% at 35 years old, respectively) and one patient had a severe restrictive respiratory insufficiency (VC theoretical value = 22% at 52 years old), the latter requiring NIV since asymptomatic respiratory acidosis was diagnosed on routine arterial blood gases.
Only two patients developed cardiac disease: patient 7 developed a type 1 atrioventricular block and right bundle branch block at 37 years old requiring a pacemaker implantation at 43 years old after an episode of syncope. Patient 17 developed a hypertrophic cardiomyopathy at the age of 63 years in the context of arterial hypertension.
Muscle MRI.
Ten patients had undergone a lower limb or whole-body muscle MRI, with a mean age at muscle MRI of 28.8 ± 11.2 years and a mean disease duration of 19.5 ± 12.1 years (Fig. 2). The muscle MRI findings of VMA21 patients can be described as follows:
-
A predominant muscle degeneration of the anterior and medial compartment of the thigh, with relative sparing of rectus femoris, tensor fasciae latae, adductor longus, and gracilis muscles (as in patients 2, 8, 10, and 11).
-
Earlier involvement of biceps femoris brevis (as in patients 2, 8, and 9) compared to the rest of the proximal lower limb posterior muscles.
-
Earlier involvement of soleus and both gastrocnemius medialis and lateralis in the distal compartment with relative sparing of tibialis anterior muscle (as in patients 1, 5, and 6)
Heatmap representation of the lower limb muscle MRI Mercuri score for fat degeneration in VMA21-linked XMEA patients. The heatmap color represents the Mercuri score, ranging from light green (low) to dark green (high). Gray squares indicate that data were unavailable. Rows are labeled with muscle names, and columns are labeled with patient identifiers. Row annotations (left side) indicate the “Age at onset of symptom” (color gradient from red to blue), “Time since disease onset” (light to dark blue), “Vignos Scale” (palette from green to red), and “Gene variant” (cyan, red, pink). Muscles are divided in different regions (gluteal region, thigh, leg) and hierarchical clustering is applied to both rows and columns based on the Manhattan distance using the Ward.D2 clustering method. The heatmap was generated using R programming language, version 4.3.0, using the Complex Heatmap library to generate the heatmap and handle clustering and annotations, with the help of Frederic Fer
This common MRI muscle involvement can be observed in Fig. 3. As expected, patients with an earlier onset of symptoms and longer disease duration before muscle MRI had more severe muscle involvement on MRI. Similarly, patients with a higher Vignos score showed more severe muscle involvement on imaging.
Characteristic lower limb muscle MRI involvement in VMA21-linked XMEA patients. T1-weighted MRI sequences of three patients with pathogenic variants in the VMA21 gene at differing stages of muscle fat transformation. Muscles with yellow arrows had marked fat replacement; muscles with yellow stars were completely or partially spared. Patient 8 (P8: aged 12 years at onset of symptoms; 24 years old and Vignos 6 at MRI) shows general end-stage muscle involvement with relative sparing of rectus femoris and tibialis anterior muscles. Patient 2 (P2: aged 5 years at onset of symptoms; 23 years old and Vignos 5 at MRI) shows the described VMA21-linked XMEA muscle MRI phenotype with predominant vastus medius, intermedius and lateralis, and adductor magnus muscle involvement and sparing of rectus femoris, sartorious, gracilis, and adductor longus muscles in the thigh. In the distal lower limb, we observed soleus, gastrocnemius medialis, and lateralis muscle involvement with preserved tibialis anterior muscles. Finally, patient 11 (P11: aged 25 years at onset of symptoms; 44 years old and Vignos 6 at MRI) shows similar muscle involvement on MRI to that of patient P2, with early vastus medius, intermedius and lateralis, and adductor magnus muscle fat transformation in the thigh as well as gastrocnemius medialis and lateralis muscle involvement in the distal lower limb. AL adductor longus, AM adductor magnus, BF biceps femoris, Gmax gluteus maximus, GM gastrocnemius medialis, Gmed gluteus medius, GL gastrocnemius lateralis, Gr gracilis, RF rectus femoris, S Soleus, Sa sartorious, SM semimembranosus, TA tibialis anterior, VI vastus intermedius, VL vastus lateralis, VM vastus medialis
Other paraclinical findings
The mean CK value at the first examination was 1287.9 ± 757.8 U/l (range = 380–2900); therefore, no patient had normal CK levels at the first examination. When available (n = 6), patients’ ENMG examinations showed the typical features of a myopathic process without signs of neuropathic involvement and myotonic discharges were found in two patients (33.3%).
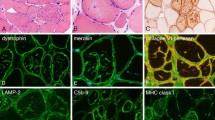
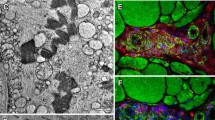
Muscle biopsy was performed in 15 patients and disclosed a myopathic process with muscle fiber splitting and numerous cytoplasmic rimmed vacuoles expressing dystrophin and other sarcolemmal proteins on immunostaining, indicating ongoing autophagy. Only one patient showed signs of necrosis/regeneration. In 4/6 (66.7%) biopsies where a reaction for complement deposit was performed, a deposition of C5b-9 at the muscle fiber surface membrane and in the cytoplasmic rimmed vacuoles was observed. Immunostaining for TDP43, a DNA-binding protein whose aggregates have been described in other myopathies with rimmed vacuoles, and p62, a protein involved in the autophagy pathway, was performed in four muscle biopsies, confirming p62 aggregates (1/4), TDP43 inclusions (1/4) or both (2/4).
Phenotype–genotype correlations.
Regarding VMA21 gene variants, most patients carried splicing variants (17/18, 94.4%): nine patients from six different families carried the c.163 + 4A > G variant, seven patients from five different families carried the c.164-7 T > G variant and one recently reported patient who is also part of the French series carried the splicing variant c.164-20 T > A [17]. Only one patient carried a missense variant (c.272G > C, p.Gly91Ala). The probable effects of these mutations are summarized in Table 2.
When comparing the two most frequent variants (c.163 + 4A > G and c.164-7 T > G), patients carrying the c.164-7 T > G had a later age at onset of symptoms (median 6, range 5–40 years vs median 3, range 1–18 years respectively; p = 0.03). Concerning disease progression, no patient carrying the c.164-7 T > G lost ambulation during follow-up; however, the log-rank test was non-significant, possibly due to low sample size. When available, the Brooke and Vignos scores seemed to progress more steeply for patients with the c.163 + 4A > G variant compared to those with the c.164-7 T > G (Fig. 4). Finally, patients with the c.164-7 T > G variant also had less muscle fat transformation on muscle MRI (Fig. 2). This was particularly the case for patient 11, who underwent the MRI 19 years after the onset of symptoms (Fig. 3).
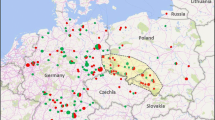
Genetics in VMA21-linked XMEA patients and distinct progression curves of motor function with time. A.1) Median age at onset of symptoms was significantly different between patients carrying the two most common variants (p = 0.03). A.2) No patient carrying the c.164-7 T > G variant lost ambulation (Kaplan–Meier curve) however the Log-Rank test was non-significant when compared to patients carrying the c.163 + 4A > G (p = 0.182); in turn, three patients carrying the c.163 + 4A > G variant lost ambulation at 35, 37, and 42 years of disease duration, respectively, as reflected in the Kaplan–Meier curve. Scatter plots showing A.3) Brooke and A.4) Vignos scores and their progression with time; B) pathogenic variants in the VMA21 gene are frequently localized in intron 2, in the splicing regions flacking exons 2 and 3. Colored variants are those found in the French series
Literature review and pooled analysis
Thirty-eight XMEA patients from the literature were reviewed and the summarized data are presented in Supplementary material.
Globally, genetically confirmed (n = 26) vs unconfirmed patients (n = 23) were similar, with an almost identical age at onset of symptoms (10.2 ± 12.8 vs 10.9 ± 7.4 years) and a predominantly proximal lower limb girdle weakness. Muscle biopsies of genetically confirmed vs unconfirmed patients also showed similar myopathic abnormalities with AVSF, bearing in mind that histopathology has been the standard for XMEA diagnosis in the past.
We then proceeded to run a pooled analysis of the 18 patients from the French series and the eight additional genetically confirmed VMA21 patients from the literature, for a total of 26 patients (Table 1). The pooled analysis confirmed the clinical and paraclinical findings from the French series described above, with an anterior compartment proximal lower limb weakness, frequent distal contractures (43.5% since some patients had both finger flexor and ankle contractures), moderate elevations of CK levels (1440.7 ± 977.4 U/l), and a muscle biopsy showing in all available cases (n = 22) a myopathic pattern with AVSF. Details are shown in Table 1.
Mean age at onset of symptoms was 10.2 ± 12.8 years (range 1–55). We could again define two subgroups of patients: a larger one (20/26, 77%) comprising patients with an onset during childhood or adolescence (< 15 years), with a mean age at onset of 4.5 ± 2.6 years, and a smaller one (6/26, 23%) comprising patients with an adulthood onset (≥ 15 years), with a mean age at onset of 29.2 ± 15.2 years. In the latter subgroup, an additional patient with a very late onset of the disease (55 years) had been reported by Crockett et al [10].
In terms of disease progression in the pooled analysis, eight patients (30.8%) needed a walking aid at a median of 15 years (range 2–29) after disease onset, and four (15.4%) were wheelchair-bound at a median of 36 years (range 19–47) after disease onset. Only one additional patient with respiratory insufficiency and no patients with cardiac involvement were reported in the literature.
Discussion
This study presents by far the largest series of XMEA patients to date, depicting the full landscape of clinical findings, muscle involvement on MRI, natural history of the disease and relevant genotype–phenotype correlations. While XMEA has been so far considered a childhood-onset myopathy, we show that an adult onset is relatively frequent (almost a quarter of patients). Therefore, it is important to consider XMEA in the differential diagnosis of adult-onset vacuolar myopathies and limb girdle muscular dystrophies (LGMD). Despite this variable age at onset, the first symptom was almost systematically a proximal lower limb weakness involving the anterior and medial compartment of the thighs. Half of the patients presented with distal limb contractures, particularly in the Achilles tendons. All patients were male and three females, parents of VMA21 patients, had a normal neuromuscular examination. No symptomatic female patient with VMA21 gene variants has been described to date, contrary to other X-linked myopathies like female carriers of Duchenne muscular dystrophy/Becker muscular dystrophy (DMD/BMD) [18].
Importantly, we show that the motor function, especially Vignos score of lower limbs, can deteriorate with time in more than half of patients, leading to walking difficulties. Although the rate of disease progression may vary between carriers of the two most frequent VMA21 variants (c.163 + 4A > G and c.164-7 T > G), patients in both groups can progress with time. Therefore, all patients with XMEA need to be monitored from a neuromuscular point of view. Also, we identified that respiratory insufficiency is more frequent than previously reported, being present in more than half of the patients during follow-up, sometimes requiring non-invasive ventilation, and should be monitored as well.
Given that V-ATPases are implicated in lysosomal function and autophagy, a process which is crucial in all cell types, extra skeletal muscle involvement could be expected in XMEA as in other autophagic vacuolar myopathies, such as Pompe or Danon disease [19, 20]. On the contrary, multiorgan involvement does not seem to be frequent if present at all. Only two patients had cardiac manifestations (hypertrophic cardiomyopathy and an atrioventricular block) and in the first case it was in the context of hypertension. In terms of central nervous system involvement, mild psychomotor delay was reported in two patients, although we lack a systematic cognitive assessment. Therefore, the restricted skeletal muscle involvement in XMEA could be the result of specific skeletal muscle-related altered lysosomal functions, such as sarcolemma repair, and/or differently expressed VMA21 isoforms, like the VMA21-120 isoform, which is predominantly expressed in skeletal muscle, as has been recently described [21].
Regarding the ancillary investigations, XMEA does not show specific findings in ENMG studies aside from classic myopathic features with sometimes spontaneous activity such as myotonic discharges, as already described in other autophagic vacuolar myopathies [22]. Fortunately, muscle biopsy oriented the diagnosis in all patients from both the French series and case reports from the literature, showing hallmark findings (autophagic vacuoles with sarcolemmal feature or AVSF) of XMEA. Not surprisingly, in all cases there was a positive reaction for sarcolemmal components on the membrane of rimmed vacuoles and sometimes, but not systematically as we have shown, complement C5b-9 deposit within vacuoles and p62 and TDP43 aggregates. It is worth mentioning that XMEA patients with or without a genetic confirmation, had a similar age at onset of symptoms and a similar clinical phenotype, which a priori supports the notion that several of these patients without a genetic analysis most likely do carry VMA21 pathogenic variants. However, it is also possible that in some of these patients, the disease is not linked to the VMA21 gene, as others and ourselves have failed to identify VMA21 mutations in some individuals with AVSF [23]. Therefore, the histopathological findings of AVSF are not 100% specific to VMA21 gene variants and other genes implicated in sarcolemmal membrane homeostasis and lysosomal function should consequently be explored in VMA21-negative XMEA patients.
Muscle MRI is an important tool in the differential diagnosis and follow-up of patients with myopathies, however reports of muscle imaging in XMEA are scarce [12]. We showed that VMA21-linked XMEA patients have consistent findings on muscle MRI which can help guide the genetic diagnosis: a predominant muscle degeneration of the anterior and medial compartment of the thigh, with relative sparing of the rectus femoris, tensor fasciae latae, adductor longus and gracilis muscles, early involvement of biceps femoris brevis in the posterior compartment of the thigh, and a more posterior than anterior compartment muscle involvement in the leg (Fig. 3). This pattern of muscle involvement on muscle MRI is somewhat different from that of BMD, a more frequent X-linked myopathy with anterior and medial compartment of the thigh motor deficit, where the semimembranosus and biceps femoris longus are more severely damaged than in XMEA [24]. In BMD, mean fat fraction calculated using the Dixon technique and T2 measurements have already been shown to be an excellent marker of disease severity, correlating with disability [25]. In line with this, we also observed that patients with more severe muscle involvement on MRI had longer disease duration before muscle MRI and higher (more severe) lower limb motor function Vignos score. Thus, muscle MRI should also be explored as a surrogate outcome measure of disease progression in XMEA patients.
Finally, pathogenic variants in the VMA21 gene commonly affect splicing and are located in intron 2 in the case of the most common variants (c.163 + 4A > G and c.164-7 T > G). Importantly, the c.164-7 T > G variant was associated with a later onset of symptoms when compared to patients carrying the c.163 + 4A > G variant. Furthermore, no patient with this variant were wheelchair-bound and both patients with the c.164-7 T > G who underwent an MRI were among the three least affected XMEA patients in our study. Interestingly, another VMA21 variant, c.164 - 6 T > G, located only one nucleotide away from the c.164 - 7 T > G variant, causes a severe congenital autophagic vacuolar myopathy (CAVM) with respiratory failure [26]. This very striking phenotype disparity can be at least partially explained by the fact that the c.164-6 T > G variant leads to greater reductions of both VMA21 transcript and protein than the c.164-7 T > G variant, likely due to a more severe impact on splicing failure [21]. We speculate by analogy that the difference in onset of disease and progression between the carriers of the c.163 + 4A > G and c.164-7 T > G variant observed in our study might be due to difference in residual protein expression; however, other alternatives like a differential expression of other genes, or even epigenetic factors modulating transcriptional or translational regulators, could also influence the observed differences in onset of the disease.
In conclusion, XMEA linked to VMA21 gene variants can have a variable age of onset, but a highly characteristic clinical, histopathological, and muscle imaging presentation, helping to guide the molecular diagnosis. Although slowly, motor disability progresses with time and respiratory involvement is more common than previously thought. A better understanding of the natural history of the disease and of specific genotype–phenotype correlations and the potential of muscle MRI as a biomarker of the disease are important considerations for clinical trial readiness in XMEA.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Ramachandran N, Munteanu I, Wang P et al (2013) VMA21 deficiency prevents vacuolar ATPase assembly and causes autophagic vacuolar myopathy. Acta Neuropathol 125(3):439–457
Sugie K, Noguchi S, Kozuka Y et al (2005) Autophagic vacuoles with sarcolemmal features delineate danon disease and related myopathies. J Neuropathol Exp Neurol 64(6):513–522
Kalimo H, Savontaus M-L, Lang H et al (1988) X-Linked myopathy with excessive autophagy: a new hereditary muscle disease. Ann Neurol 23(3):258–265
Nemazanyy I, Blaauw B, Paolini C et al (2013) Defects of Vps15 in skeletal muscles lead to autophagic vacuolar myopathy and lysosomal disease. EMBO Mol Med 5(6):870–890
Mercuri E, Pichiecchio A, Allsop J et al (2007) Muscle MRI in inherited neuromuscular disorders: past present, and future. J Magn Reson Imag 440:433–440
Richards S, Aziz N, Bale S et al (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of medical genetics and genomics and the association for molecular pathology. Genet Med 17(5):405–424
Villanova M, Louboutin JP, Chateau D et al (1995) X-linked vacuolated myopathy: complement membrane attack complex on surface membrane of injured muscle fibers. Ann Neurol 37(5):637–645
Chabrol B, Figarella-Branger D, Coquet M et al (2001) X-linked myopathy with excessive autophagy: a clinicopathological study of five new families. Neuromuscul Disord 11(4):376–388
Kurashige T, Takahashi T, Yamazaki Y et al (2013) Elevated urinary β2 microglobulin in the first identified Japanese family afflicted by X-linked myopathy with excessive autophagy. Neuromuscul Disord 23(11):911–916
Crockett CD, Ruggieri A, Gujrati M et al (2014) Late adult-onset of X-linked myopathy with excessive autophagy. Muscle Nerve 50(1):138–144
Ruggieri A, Ramachandran N, Wang P et al (2015) Non-coding VMA21 deletions cause X-linked myopathy with excessive autophagy. Neuromuscul Disord 25(3):207–211
Mercier S, Magot A, Caillon F et al (2015) Muscle magnetic resonance imaging abnormalities in X-linked myopathy with excessive autophagy. Muscle Nerve 52(4):673–680
Rao S, Chandra S, Narayanappa G (2019) X-linked myopathy with excessive autophagy; a case report. Neurol India 67(5):1344
Cotta A, Carvalho E, da Cunha-Junior AL et al (2020) Clinical, imaging, morphologic, and molecular features of X-linked VMA21-related myopathy in two unrelated Brazilian families. J Neurol Sci 415:116977
Alon T, Sadeh M, Lev D, Dabby R (2021) X-linked myopathy with excessive autophagy: first report of an Israeli family presenting with late onset lower limb girdle weakness. Neuromuscul Disord 31(9):854–858
Yang J, Chen D, Feng L et al (2022) X-linked myopathy with excessive autophagy due to a mutation in VMA21 gene: the first case in China. Neurol Sci 43(3):2137–2139
Pegat A, Streichenberger N, Lacoste N et al (2022) Novel intronic mutation in VMA21 causing severe phenotype of X-linked myopathy with excessive autophagy—case report. Genes (Basel) 13(12):2245
Ishizaki M, Kobayashi M, Adachi K et al (2018) Female dystrophinopathy: review of current literature. Neuromuscul Disord 28(7):572–581
Kishnani PS, Hwu WL, Mandel H et al (2006) A retrospective, multinational, multicenter study on the natural history of infantile-onset Pompe disease. J Pediatr 148(5):671-676.e2
Sugie K, Yamamoto A, Murayama K et al (2002) Clinicopathological features of genetically confirmed Danon disease. Neurology 58(12):1773–1778
Cocchiararo I, Cattaneo O, Rajendran J et al (2023) Identification of a muscle-specific isoform of VMA21 as a potent actor in X-linked myopathy with excessive autophagy pathogenesis. Hum Mol Genet 26(3):312–318
Hobson-Webb LD, DeArmey S, Kishnani PS (2011) The clinical and electrodiagnostic characteristics of Pompe disease with post-enzyme replacement therapy findings. Clin Neurophysiol 122(11):2312–2317
Dowling JJ, Moore SA, Kalimo H, Minassian BA (2015) X-linked myopathy with excessive autophagy: a failure of self-eating. Acta Neuropathol 129(3):383–390
Tasca G, Iannaccone E, Monforte M et al (2012) Muscle MRI in becker muscular dystrophy. Neuromuscul Disord 22(SUPPL. 2):S100–S106
Fischer D, Hafner P, Rubino D et al (2016) The 6-minute walk test, motor function measure and quantitative thigh muscle MRI in Becker muscular dystrophy: a cross-sectional study. Neuromuscul Disord 26(7):414–422
Munteanu I, Ramachandran N, Ruggieri A et al (2015) Congenital autophagic vacuolar myopathy is allelic to X-linked myopathy with excessive autophagy. Neurology 84(16):1714–1716
Acknowledgements
The authors would like to thank Frédéric Fer for assistance with developing the R code to generate a heatmap of the MRI muscle involvement.
The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors. MS is supported by a clinician scientist INSERM position (CIHU INSERM).
Funding
The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors. MS is supported by a clinician scientist INSERM position (CIHU INSERM).
Author information
Authors and Affiliations
Contributions
Concept and design: GFE, AB, TS. Acquisition and analysis of data: GFE, GA, MS, IAB, FD, GS, FC, SM, YP, AM, AP, ESC, BC, SG, MK, VB, TE. Drafting of the manuscript and figures: GFE, GA, MS, AB, CM, TS.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflict of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fernández-Eulate, G., Alfieri, G., Spinazzi, M. et al. Phenotype variability and natural history of X-linked myopathy with excessive autophagy. J Neurol 271, 4008–4018 (2024). https://doi.org/10.1007/s00415-024-12298-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-024-12298-0