Abstract
Cholesterol is an essential component in the structure and function of cell membranes and has been associated with the major pathological signatures of Alzheimer’s disease (AD). To maintain brain cholesterol homeostasis, it is converted into 24(S)-hydroxycholesterol (24OHC) which can be driven through the blood–brain barrier. Several studies have already described a decrease in 24OHC and an increase of 27(S)-hydroxycholesterol (27OHC) in AD, as a reflection of disease burden, the loss of metabolically active neurons and the degree of structural atrophy. It is also well known that peripheral cholesterol is altered in AD patients. However, there are no data regarding effects of AD treatment in this cholesterol pathway. Since a study from our group indicated a significant increase in membrane phospholipid metabolism by donepezil, the aim of this study was to evaluate the effect of short- and long-term donepezil treatment on cholesterol and metabolites 24OHC and 27OHC in plasma of AD patients and in healthy volunteers. At baseline, we found a decrease of 24OHC (p = 0.003) in AD patients. Cholesterol levels increased with donepezil treatment (p = 0.04) but no differences were observed regarding 24OHC and 27OHC. However, these results confirm and extend previous studies demonstrating disturbed cholesterol turnover in Alzheimer’s disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Altered lipid metabolism is believed to be a key event to central nervous system (CNS) injuries [1, 2]. In fact, phospholipid bilayer and associated lipids provide not only a permeability barrier but also a structured environment that is essential for the proper functioning of membrane-bound proteins [3]. One of the most important regulators of lipid organization is cholesterol. Its structure allows filling interstitial spaces between hydrophobic fatty acid chains of phospholipids [3].
Alterations in membrane metabolism has been extensively described in Alzheimer’s disease (AD) mostly those caused by decrease in phospholipase A2 (PLA2) activity, the main enzymes accountable for membrane phospholipids metabolism [4,5,6]. Furthermore, disturbances in cholesterol metabolism have been associated with the major pathological signatures of AD, i.e. extracellular deposition of Aβ in senile plaques, intracellular accumulation of hyperphosphorylated aggregated Tau in neurofibrillary tangles and degeneration of neurons and their synapses [7, 8].
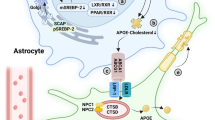
The major pool of cholesterol in the central nervous system (CNS) is in myelin although neurons and glial cells also contain cholesterol. Brain cells synthesize all cholesterol found in CNS, since the blood–brain barrier (BBB) hinders entry of cholesterol synthesized in the periphery [9]. To maintain brain cholesterol homeostasis, it is converted into a more polar metabolite, the 24(S)-hydroxycholesterol (24OHC) which can be driven through the BBB [10,11,12,13]. 24OHC is an endogenous regulator of the nuclear receptor Liver X Receptor (LXR) potentially regulating the cholesterol and fatty acid synthesis pathways in the brain. In the adult brain almost all the neuronal requirements of cholesterol are supplied by cholesterol transported by ApoE-containing lipoproteins released from astrocytes. Via LXR, 24OHC regulates the expression, synthesis and secretion of ApoE [14] and the expression of the sterol transporters ATP-binding cassette A1, G1 and G4, involved in the transporter of cholesterol from glia to ApoE particle [15]. Therefore, 24OHC participates in both cholesterol efflux pathways. Plasma levels are kept constant by liver clearance of 24OHC converted into bile acids or further conjugated for final elimination. Thus, all 24OHC present in blood plasma arises from CNS, reflecting the brain cholesterol catabolism [15].
In the periphery, the major cholesterol metabolite is 27-hydroxycholesterol (27OHC), representing an important mechanism for the daily elimination of cholesterol from the body. It is also able to cross the BBB [9, 16].
It is worth stressing the importance of ApoE in lipid homeostasis: it regulates cholesterol, triglyceride and phospholipid transport and metabolism [17]. APOE gene has three common alleles ε2, ε3 and ε4 and gives rise to three main structural isoforms protein that differ in their effectiveness: ApoE2, ApoE3 and ApoE4. 65–80% of AD patients carry at least one of ε4 [18]. The presence of this allele leads to a less effective protein highlighting 24OHC role in cholesterol efflux [19,20,21].
In fact several studies have already described a decrease in 24OHC and an increase of 27OHC in AD [22] in serum [23, 24] and CSF [25, 26], as a reflection of disease burden, the loss of metabolically active neurons and the degree of structural atrophy [23, 25, 27,28,29,30,31,32,33,34]. Findings from cell culture and animal studies suggest that 27OHC is associated with increased levels of APP as well as β-secretase (BACE1), the enzyme that cleaves APP to yield Aβ. On the other hand, 24OHC is associated with increased levels of sAPPα, suggesting that 24OHC facilitates the processing of APP by non-amyloidogenic pathway [35,36,37,38].
Donepezil hydrochloride, a selective acetylcholinesterase inhibitor (AChEi), is one of the widely used drugs in AD treatment [39,40,41]. These drugs delay the progression of brain atrophy, indicating a disease-modifying effect by attenuating neuronal death and a neuroprotective role and seem to affect cholesterol levels [42].
Since study from our group shows a significant effect of donepezil on PLA2 activity, increasing membrane phospholipid metabolism [4], the aim of this study was to evaluate if short- and long-term donepezil treatment also affects lipid metabolism in a broader way by assessing cholesterol and metabolites 24OHC and 27OHC in plasma of AD patients and in healthy volunteers. Moreover, we investigated a possible role for APOE genotypes on cholesterol metabolism.
Materials and methods
The sample comprised 30 patients with mild or moderate AD and 33 physically and cognitively healthy elderly controls. This open-label study was conducted at the Institute of Psychiatry, University of Sao Paulo, Brazil and participants were middle-income, community-dwelling individuals from the hospital catchment area. Local Ethical Committee approved this study, and all subjects signed a written informed consent prior to inclusion in the study. The diagnosis of probable AD was made according to the NINCDS–ADRDA diagnostic criteria [43]. Cognitive assessments were made with the Cambridge Cognitive Test (CAMCOG) [44] and the Mini-Mental State Examination (MMSE) [45] (Table 1). Table 2 shows the genotype frequencies of ApoE. In the last 6 months prior to enrolment in the study, patients and the control group did not use AChEi or other drugs (e.g. neuroleptics, antidiabetic, lithium, antidepressants and anticonvulsants). After the completion of baseline assessments, all patients were started on donepezil treatment (5 mg/day). Doses were administered orally and increased to 10 mg/day after 1 month. Patients were monitored monthly, the MMSE was evaluated after 3 and 6 months, and CAMCOG was evaluated 6 months after donepezil treatment.
Sample collection
Blood samples were collected, in the morning after 8-h fasting, using Vacutainer tubes containing EDTA (Vacutainer, Becton Dickinson). Samples were centrifuged at 20 °C and 1400g for 10 min. Plasma was obtained, frozen and stored at −80 °C until analysis.
Plasma cholesterol concentrations were measured using commercially available enzymatic–colorimetric methods (Labtest Diagnostica, Brazil).
Measurements of oxysterols (24-hydroxycholesterol and 27-hydroxycholesterol) were performed according to Dzeletovic et al. [46]. Following is a brief description of the method.
Sample preparation
To plasma (1 mL) was added a mixture of deuterium-labelled internal standards followed by an alkaline hydrolysis with potassium hydroxide (0.4 M). After 2 h of incubation, the pH was adjusted to 7 with phosphoric acid. Extraction was performed with the addition of 20 mL of chloroform and 6 mL of 0.9 M NaCl followed by vigorous shaking. The organic phase was evaporated using a rotary evaporator at room temperature. The residue was resuspended with 1 mL of toluene. The next step was a solid-phase extraction using a silica cartridge (Supelclean LC-Si SPE tube) and isopropanol as eluent solution. The collected isopropanol was evaporated and the residue was treated with pyridine:trimethysilyl trifluoroacetamide (1:1, v/v) at 60 °C for 30 min.
Analysis by gas chromatography–mass spectrometry
The samples (1 μL) were injected in split mode into a gas chromatograph (GC) coupled to a mass spectrometer (MS) (Shimadzu GCMS-QP2010 Plus) equipped with the GCMS solution software version 2.5. The separation was performed with a Restek capillary column (30 m × 0.25 mm, 0.25 μm phase thickness). The oven temperature program was as follows: 240 °C for 7 min, 5 °C/min to 290 °C. Helium was used as carrier gas. The gas chromatograph was operated in constant flow mode with the flow rate set to 44.1 cm/s. The mass spectrometer was operated in single ion monitoring and the electron ionization energy was 70 eV. The ion source and interface temperature was 300 °C. [46].
APOE genotyping
DNA was extracted from peripheral blood by salting out [47]. Two single nucleotide polymorphisms (SNPs) (rs7412 and rs429358) were evaluated to determine the APOE genotype as previously described [48]. Amplification reactions were performed using real-time polymerase chain reaction (PCR) SNP genotyping systems (TaqMan Assays; Life Technologies, Carlsbad, CA, USA), as follows: TaqMan PCR Mastermix 1×/μL, TaqMan SNP genotyping assay 1×/μL, 10 ng/μL genomic DNA and ultrapure water to make up a volume of 7 μL were mixed in each well of an optical plate. Allelic discrimination was evaluated in a 7500 real-time PCR system (Life Technologies) comparing fluorescence levels before and after amplification (45 cycles of 15 s at 95 °C and 1 min at 60 °C).
Statistical analysis
Baseline comparison of sociodemographic characteristics of patients and controls were assessed with Fisher’s exact test for categorical variables and with Student’s t test for numerical ones. Longitudinal analysis of patients was carried out with a linear mixed-effect model (24OHC, 27OHC, cholesterol, APOE, MMSE and CAMCOG). Pairwise comparison of means by time was corrected using sequential Bonferroni method. Normality assumptions were checked inspecting the QQ plots. All statistical analyses were performed with the SPSS (Statistical Package for Social Sciences, for Windows, v. 14, Chicago, IL) and significance level was p < 0.05.
Results
At baseline, we found a decrease of plasma 24OHC (p = 0.003) in probable AD patients. No differences were observed regarding 27OHC and cholesterol levels at baseline comparing to controls. After 3 months with 10-mg donepezil treatment we did not find any change in cholesterol or 24OHC, which remained lower than controls but 27OHC levels presented a slight increase (p = 0.023). After 6 months of treatment we found a discrete increment in cholesterol levels (198.66 ± 54.49 mg/dL) (p = 0.04), but no change in 24OHC. 27OHC restored the baseline levels (Table 3; Fig. 1).
The presence of an ApoE4 allele did not show an association with cholesterol (p = 0.051), 24OHC (p = 0.262) or 27OHC (p = 0.167). Education years and cognitive assessments (MMSE and CAMCOG) also show no association with the metabolites. In our samples there were no differences between probable AD and controls regarding the presence of APOE4 allele.
After 6 months on donepezil, 46% of the patients remained cognitively stable or slightly improved on CAMCOG (mean improvement 7.1 ± 3.5 points), while the remaining patients deteriorated (4.7 ± 3.2). These results did not show any association with the metabolite levels.
Discussion and conclusions
In the present sample, we found reduced plasma levels of 24OHC in probable AD patients, whereas no differences were found regarding 27OHC and total cholesterol levels when compared to controls.
Decreased 24OHC levels in AD were reported in several studies [49,50,51,52,53]. In fact, considerable evidences suggest a relationship between the degree of brain atrophy and the cholesterol metabolite 24OHC in plasma level of AD patients and in other neurodegenerative diseases [28, 54]. Famer and colleagues [36] addressed in vitro the effects of 24OHC on the activity of α- and β-secretases, the two key enzymes involved in APP metabolism. They found the α-secretase activity and the relative protein values of extracellular sAPPα and total sAPP were significantly increased, whereas the β-secretase activity was reduced by 24OHC, demonstrating that this oxysterol tends toward APP α-cleavage [36].
However, others studies report that plasma levels of 24OHC in AD patients were not significantly different or increased comparing to control [34, 55, 56]. Some authors suggest that demyelination may cause a transient increase in the flux of 24OHC from the brain to the blood. Conversely, a destruction of neurons in combination with a loss of myelin occurring during a long period would be expected to result in decreased circulating levels of 24OHC at a later stage of the disease [57]. Thus, we assume that at least part of the contradictory findings regarding 24OHC levels in probable AD may be explained by sample heterogeneity regarding the different stages of the disease.
Regarding 27OHC, some authors have reported that this oxysterol increases levels of Aβ and p-tau and induces endoplasmic reticulum stress, a cellular response that is implicated in AD [58]. Based on this, it is expected to find a decrease in plasma 27OHC and an increase in AD patients’ brain. In fact, brain levels of 27OHC were described to be increased in several areas of autopsied AD brains [57]. Likewise, Kolsch and colleagues [30] found significantly reduced 27OHC in plasma of patients with dementing disorders compared to non-demented subjects [17]. Despite all, our study found no differences in 27OHC plasma levels between AD patients and controls.
Many studies have shown that changes in membrane cholesterol levels influence APP processing [59]. Cholesterol in the brain is mainly located in neuronal cell membranes and myelin sheets. This lipid is essential for cell membrane structure and function, particularly in lipid rafts, specialized membrane microdomains where the last step in Aβ production [60] occurs. On the periphery, elevated cholesterol has been proposed to be a risk factor to developing AD by animal models and in vitro studies [61, 62]. However, in human studies, the results of cholesterol levels are controversial, both on the periphery and in the brain [63]. In our study, cholesterol levels at baseline were no different in plasma of probable AD patients as compared to controls.
APOE*4 allele was found to be associated with lowest levels of 24OHC, according to the hypothesis of an earlier faster and more intensive degenerative process in ε4 and the positive effect of ε4 allele on AD markers [64]. Despite this, the presence of an APOE4 allele did not show an association with cholesterol and oxysterol plasma levels in this study.
Regarding treatment with donepezil, we did not find an effect of 3- and 6-month treatment on 24OHC plasma levels. With respect to 27OHC, we observed a slight increase with 3 months of treatment, but this increment was not maintained during the 6 months of donepezil treatment. Numerous studies have revealed that AChEI could regulate cholesterol level through activating the LXR pathway [65]. LXRs act as a dominant supervisor in cholesterol metabolism including synthesis, uptake and trafficking. In studies with NPC mice, donepezil delayed the loss of cerebellar Purkinje cells and improved motor function via regulating the cholesterol-related homeostasis. These data suggest that donepezil reduced the cholesterol accumulation via inhibition of cholesterol synthesis through upregulation of the LXR pathway in NPC mice [66]. Contrasting, in our study we observed a significant increase in cholesterol levels as a result of donepezil treatment. Nonetheless, this increment of total cholesterol levels should not be overemphasized, as the mean values remained within the normal range (<200 mg/dL). It is, however, of interest that Adunsky and colleagues [67], in a cross-sectional study, found increased plasma cholesterol in AD patients using donepezil compared with AD patients who did not.
More studies are necessary in this field to confirm the effect of donepezil on cholesterol and metabolites. A relevant factor, to be taken into account, is the small size of our sample, follow-up length and the lack of lumbar punctures. Despite this, it is a valuable sample, since patients were free of AChEi treatment and solely one variable was introduced in the follow-up: donepezil treatment. However, these results confirm and extend previous studies demonstrating disturbed cholesterol turnover in Alzheimer’s disease.
References
Adibhatla RM, Hatcher JF (2008) Altered lipid metabolism in brain injury and disorders. Subcell Biochem 49:241–268
Adibhatla RM, Hatcher JF, Dempsey RJ (2006) Lipids and lipidomics in brain injury and diseases. AAPS J 8:314–321
Maxfield FR, Tabas I (2005) Role of cholesterol and lipid organization in disease. Nature 438:612–621
Talib LL, Hototian SR, Joaquim HP, Forlenza OV, Gattaz WF (2015) Increased iPLA2 activity and levels of phosphorylated GSK3B in platelets are associated with donepezil treatment in Alzheimer’s disease patients. Eur Arch Psychiatry Clin Neurosci 265:701–706
Schaeffer EL, Forlenza OV, Gattaz WF (2009) Phospholipase A2 activation as a therapeutic approach for cognitive enhancement in early-stage Alzheimer disease. Psychopharmacology 202:37–51
Gattaz WF, Levy R, Cairns NJ, Förstl H, Braus DF, Maras A (1996) Relevance of metabolism of membrane phospholipids for Alzheimer dementia. Fortschr Neurol Psychiatr 64:8–12
Vance JE (2012) Dysregulation of cholesterol balance in the brain: contribution to neurodegenerative diseases. Dis Model Mech 5:746–755
Martins IJ, Berger T, Sharman MJ, Verdile G, Fuller SJ, Martins RN (2009) Cholesterol metabolism and transport in the pathogenesis of Alzheimer’s disease. J Neurochem 111:1275–1308
Vance JE, Hayashi H, Karten B (2005) Cholesterol homeostasis in neurons and glial cells. Semin Cell Dev Biol 2:193–212
Björkhem I, Lütjohann D, Diczfalusy U, Ståhle L, Ahlborg G, Wahren J (1998) Cholesterol homeostasis in human brain: turnover of 24S-hydroxycholesterol and evidence for a cerebral origin of most of this oxysterol in the circulation. J Lipid Res 8:1594–1600
Lund EG, Guileyardo JM, Russell DW (1999) cDNA cloning of cholesterol 24-hydroxylase, a mediator of cholesterol homeostasis in the brain. Proc Natl Acad Sci USA 13:7238–7243
Tedde A, Rotondi M, Cellini E et al (2006) Lack of association between the CYP46 gene polymorphism and Italian late-onset sporadic Alzheimer’s disease. Neurobiol Aging 5:773-e1
Garcia AN, Muniz MT, e Silva HRS, da Silva HA, Athayde-Junior L (2009) Cyp46 polymorphisms in Alzheimer’s disease: a review. J Mol Neurosci 3:342–345
Abildayeva K, Jansen PJ, Hirsch-Reinshagen VW Bloks, Bakker AH, Ramaekers J, de Ventre FC, Groen AK, Wellington CL, Kuipers F, Mulder M (2006) 24(S)-hydroxycholesterol participates in a liver X receptor-controlled pathway in astrocytes that regulates apolipoprotein E-mediated cholesterol efflux. J Biol Chem 281:12799–12808
Leoni V, Caccia C (2011) Oxysterols as biomarkers in neurodegenerative diseases. Chem Phys Lipids 164:515–524
Gosselet F, Saint-Pol J, Fenart L (2014) Effects of oxysterols on the blood-barrier: implications for Alzheimer’s disease. Biochem Biophys Res Commun 446:687–691
Mahley RW (2016) Central nervous system lipoproteins: ApoE and regulation of cholesterol metabolism. Arterioscler Thromb Vasc Biol 36:1305–1315
Solfrizzi V, Panza F, D’Introno A et al (2002) Lipoprotein(a), apolipoprotein E genotype, and risk of Alzheimer’s disease. J Neurol Neurosurg Psychiatry 72:732–736
Bu G (2009) Apolipoprotein E and its receptors in Alzheimer’s disease, pathways, pathogenesis and therapy. Nat Rev Neurosci 10:333–344
Posse-de-Chaves E, Narayanaswami V (2008) Apolipoprotein E and cholesterol in aging and disease in the brain. Future Lipidol 3:505–530
Bjorkhem I, Leoni V, Meaney S (2010) Genetic connections between neurological disorders and cholesterol metabolism. J Lipid Res 51:2489–2503
Koudinov AR, Koudinova NV (2001) Essential role for cholesterol in synaptic plasticity and neuronal degeneration. FASEB J 15:1858–1860
Teunissen CE, Lütjohann D, von-Bergmann K et al (2003) Combination of serum markers related to several mechanisms in Alzheimer’s disease. Neurobiol Aging 24:893–902
Popp J, Lewczuk P, Kölsch H et al (2012) Cholesterol metabolism is associated with soluble amyloid precursor protein production in Alzheimer’s disease. J Neurochem 123:310–316
Besga A, Cedazo-Minguez A, Kåreholt I et al (2012) Differences in brain cholesterol metabolism and insulin in two subgroups of patients with different CSF biomarkers but similar white matter lesions suggest different pathogenic mechanisms. Neurosci Lett 510:121–126
Popp J, Meichsner S, Kölsch H et al (2013) Cerebral and extracerebral cholesterol metabolism and CSF markers of Alzheimer’s Disease. Biochem Pharmacol 86:32–42
Bretillon L, Lutjohann D, Stahle L et al (2000) Plasma levels of 24S-hydroxycholesterol reflect the balance between cerebral production and hepatic metabolism and are inversely related to body surface. J Lipid Res 41:840–845
Bretillon L, Siden Å, Wahlund LO et al (2000) Plasma levels of 24S-hydroxycholesterol in patients with neurological diseases. Neurosci Lett 293:87–90
Karrenbauer VD, Leoni V, Lim ET et al (2006) Plasma cerebrosterol and magnetic resonance imaging measures in multiple sclerosis. Clin Neurol Neurosurg 108:456–460
Kölsch H, Heun R, Kerksiek A, Bergmann KV, Maier W, Lutjohann D (2004) Altered levels of plasma 24S- and 27-hydroxycholesterol in demented patients. Neurosci Lett 368:303–308
Leoni V, Mariotti C, Nanetti L et al (2011) Whole body cholesterol metabolism is impaired in Huntington’s disease. Neurosci Lett 494:245–249
Qureischie H, Heun R, Lutjohann D et al (2008) CETP polymorphisms influence cholesterol metabolism but not Alzheimer’s disease risk. Brain Res 1232:1–6
Solomon A, Leoni V, Kivipelto M et al (2009) Plasma levels of 24S-hydroxycholesterol reflect brain volumes in patients without objective cognitive impairment but not in those with Alzheimer’s disease. Neurosci Lett 462:89–93
Zuliani G, Donnorso MP, Bosi C et al (2011) Plasma 24S-hydroxycholesterol levels in elderly subjects with late onset Alzheimer’s disease or vascular dementia: a case control study. BMC Neurol 11:121
Prasanthi JR, Huls A, Thomasson S, Thompson A, Schommer E, Ghribi O (2009) Differential effects of 24-hydroxycholesterol and 27-hydroxycholesterol on beta-amyloid precursor protein levels and processing in human neuroblastoma SH-SY5Y cells. Mol Neurodegener 6:4–7
Famer D, Meaney S, Mousavi M, Nordberg A, Bjorkem I, Crisby M (2007) Regulation of alpha- and beta-secretase activity by oxysterols: cerebrosterol stimulates processing of APP via the alpha-secretase pathway. Biochem Biophys Res Commun 359:46–50
Dasari B, Prasanthi JR, Marwarha G, Singh BB, Ghribi O (2010) The oxysterol 27-hydroxycholesterol increases β-amyloid and oxidative stress in retinal pigment epithelial cells. BMC Ophthalmol 13:10–22
Prasanthi JR, Larson T, Schommer J, Ghribi O (2011) Silencing GADD153/CHOP gene expression protects against Alzheimer’s disease-like pathology induced by 27-hydroxycholesterol in rabbit hippocampus. PLoS One 6:2640
Leyhe T, Hoffmann N, Stransky E, Laske C (2009) Increase of SCF plasma concentration during donepezil treatment of patients with early Alzheimer’s disease. Int J Neuropsychopharmacol 12:1319–1326
Shen H, Kihara T, Hongo H et al (2010) Neuroprotection by donepezil against glutamate excitotoxicity involves stimulation of alpha7 nicotinic receptors and internalization of NMDA receptors. Br J Pharmacol 161:127–139
Noh MY, Koh SH, Kim SM, Maurice T, Ku SK, Kim SH (2013) Neuroprotective effects of donepezil against Aβ42-induced neuronal toxicity are mediated through not only enhancing PP2A activity but also regulating GSK-3β and nAChRs activity. J Neurochem 127:562–574
Cacabelos R (2007) Donepezil in Alzheimer’s disease: from conventional trials to pharmacogenetics. Neuropsychiatr Dis Treat 3:303–333
McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM (1984) Clinical diagnosis of Alzheimer’s disease: report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology 34:939–944
Roth M, Tym E, Mountjoy CQ et al (1986) CAMDEX: a standardized Instrument for the diagnosis of mental disorders in the elderly with special reference to early detection of dementia. Br J Psychiatry 149:698–709
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”—a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Dzeletovic S, Breuer O, Lund E, Diczfalusy U (1995) Determination of cholesterol oxidation products in human plasma by isotope dilution-mass spectrometry. Anal Biochem 22:573–580
Laitinen J, Samarut J, Holtta E (1994) A nontoxic and versatile protein salting-out method for isolation of DNA. Biotechniques 17:316–322
Forlenza OV, Diniz BS, Talib LL et al (2010) Clinical and biological predictors of Alzheimer’s disease in patients with amnestic mild cognitive impairment. Rev Bras Psiquiatr 32:216–222
Burkard I, von Eckardstein A, Waeber A, Vollenweider P, Rentsch KM (2007) Lipoprotein distribution and biological variation of 24S- and 27-hydroxycholesterol in healthy volunteers. Atherosclerosis 194:71–78
Babiker A, Diczfalusy U (1998) Transport of side-chain oxidized oxysterols in the human circulation. Biochim Biophys Acta 1392:333–339
Frears ER, Stephens DJ, Walters CE, Davies H, Austen BM (1999) The role of cholesterol in the biosynthesis of beta-amyloid. NeuroReport 10:1699–1705
Yamanaka K, Saito Y, Yamamori T, Urano Y, Noguchi N (2011) 24(S)-hydroxycholesterol induces neuronal cell death through necroptosis, a form of programmed necrosis. J Biol Chem 286:24666–24673
Blennow K, de Leon MJ, Zetterberg H (2006) Alzheimer disease. Lancet 368:387–403
Papassotiropoulos A, Lütjohann D, Bagli M et al (2000) Plasma 24S-hydroxycholesterol, a peripheral indicator of neuronal degeneration and potential state marker for Alzheimer’s disease. NeuroReport 11:1959–1962
Juliano L, Monticolo R, Straface G et al (2010) Vitamin E and enzymatic/oxidative stress-driven oxysterols in amnestic mild cognitive impairment subtypes and Alzheimer’s disease. J Alzheimers Dis 21:1383–1392
Lütjohann D, Papassotiropoulos A, Björkhem I et al (2000) Plasma 24S-hydroxycholesterol (cerebrosterol) is increased in Alzheimer and vascular demented patients. J Lipid Res 41:195–198
Heverin M, Bogdanovic N, Lütjohann D et al (2004) Changes in the levels of cerebral and extracerebral sterols in the brain of patients with Alzheimer’s disease. J Lipid Res 45:186–193
Marwarha G, Dasari B, Prabhakara JP, Schommer J, Ghribi O (2010) β-Amyloid regulates leptin expression and tau phosphorylation through the mTORC1 signaling pathway. J Neurochem 115:373–384
Lim WLF, Martins IJ, Martins RN (2014) The involvement of lipids in Alzheimer’s disease. J Genet Genom 41:261–271
Cheng H, Vetrivel KS, Gong P, Parent A, Thinakaran G (2007) Mechanisms of disease: new therapeutic strategies for Alzheimer’s disease—targeting amyloid precursor protein processing in lipid rafts. Nat Clin Pract Neurol 7:374–382
Pappolla MA, Bryant-Thomas T, Herbert D et al (2003) Mild hypercholesterolemia is an early risk factor for the development of Alzheimer amyloid pathology. Neurology 61:199–205
Solomon A, Kivipelto M, Wolozon B, Zhou J, Whitmer RA (2009) Midlife serum cholesterol and increased risk of Alzheimer’s and vascular dementia three decades later. Dement Geriatr Cogn Disord 28:75–80
Wood WG, Li L, Muller WE, Eckert GP (2014) Cholesterol as a causative factor in Alzheimer’s disease: a debatable hypothesis. J Neurochem 129:559–572
Leoni V, Caccia C (2013) 24S-hydroxycholesterol in plasma: a marker of cholesterol turnover in neurodegenerative diseases. Biochimie 95:595–612
Hong C, Tontonoz P (2014) Liver X receptors in lipid metabolism: opportunities for drug discovery. Nat Rev Drug Discov 6:433–444
Seo Y, Shin Y, Kim HS et al (2014) Donepezil enhances Purkinje cell survival and alleviates motor dysfunction by inhibiting cholesterol synthesis in a murine model of Niemann Pick disease type C. J Neuropathol Exp Neurol 73:234–243
Adunsky A, Chesnin V, Ravona R, Harats D, Davidson M (2004) Plasma lipid levels in Alzheimer’s disease patients treated by Donepezil hydrochloride: a cross-sectional study. Arch Gerontol Geriatr 38:61–68
Acknowledgements
The authors wish to gratefully acknowledge the contribution of Associação Beneficente Alzira Denise Hertzog da Silva (ABADHS) and NAPNA (Núcleo de Apoio à Pesquisa em Neurociências Aplicada—USP).
Author information
Authors and Affiliations
Contributions
Authors LLT and WFG designed the study. Author OVF performed patient recruitment and neuropsychiatry and clinical evaluation. Authors HPGJ, ACC and LLT managed the literature searches, wrote the first draft of the manuscript and undertook the statistical analysis. Authors VNS and ACC wrote the protocol and performed the laboratory analyses. All authors contributed to and have approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Rights and permissions
About this article
Cite this article
Costa, A.C., Joaquim, H.P.G., Nunes, V.S. et al. Donepezil effects on cholesterol and oxysterol plasma levels of Alzheimer’s disease patients. Eur Arch Psychiatry Clin Neurosci 268, 501–507 (2018). https://doi.org/10.1007/s00406-017-0838-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-017-0838-2