Abstract
Exposure of an organism to chronic social isolation (CSIS) has been shown to have an important role in depression. Fluoxetine (Flx) is a first-line treatment for depression; however, its downstream mechanisms of action beyond serotonergic signaling remain ill-defined. We investigated the effect of 3 weeks of Flx (15 mg/kg/day) treatment on behavioral changes and protein expression/activity of the GSH-dependent defense system, including reduced glutathione (GSH), glutathione peroxidase (GPx), glutathione reductase (GLR), and glutathione S-transferase (GST), as well as catalase (CAT), in the hippocampus of rats exposed to 6 weeks of CSIS. The subcellular distributions of nuclear factor-κB (NF-κB), as well as, cytosolic IL-1β and IL-6 protein expression, were also determined. CSIS induced depressive- and anxiety-like behaviors, evidenced by a decrease in sucrose preference and an increase in the number of buried marbles. Moreover, CSIS compromised redox homeostasis, targeting enzymes such as GPx, CAT, GST, and caused NF-κB nuclear translocation with a concomitant increase in IL-6 protein expression, without an effect on IL-1β. Flx treatment reversed CSIS-induced depressive- and anxiety-like behaviors, modulated GSH-dependent defense by increasing GLR and GST activity, and suppressed NF-κB activation and cytosolic IL-6 protein expression in socially isolated rats. The present study suggests that changes in the GSH-dependent defense system, NF-κB activation and increased IL-6 protein expression may have a role in social isolation-induced changes in a rat model of depression and anxiety, and contributes to our understanding of the mechanisms that underlie the antidepressant and anti-inflammatory activity of Flx in socially isolated rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Exposure of an organism to various chronic stressors may result in oxidative stress that leads to the activation of intracellular signaling pathways involved in psychiatric disorders [1]. Particularly interesting are those stressors with a psychosocial component, whereby chronic psychosocial stress in adulthood modulates brain structure and function, and may result in cognitive deficits and an increased risk of psychiatric disorders [2,3,4]. During chronic stress, overproduction of reactive oxygen/nitrogen species (ROS/RNS) triggers redox dysregulation, leading to oxidative/nitrosative damage to brain structures [5]. Hence, impaired glutathione (GSH) regulation, or compromised activity of enzymes involved in the GSH-dependent defense system, such as glutathione peroxidase (GPx), and glutathione reductase (GLR) as well as glutathione S-transferase (GST), may contribute to the pathophysiology of depression [6]. In addition, catalase (CAT) plays an important role in protection from oxidative stress [7]. Moreover, oxidative stress may be related to inflammation [8], as inflammatory, oxidative and nitrosative stress pathways are key features of depression and anxious behavior [1]. Also, changes of these factors show strong overlaps between depression and related disorders, such as schizophrenia, which include depressive mood episodes [9]. Interleukin-6 (IL-6) and interleukin-1β (IL-1β) are inflammatory cytokines that have been reported to be elevated in the serum or plasma of depressed patients [10, 11]. An important mediator of the inflammatory response is nuclear factor-κB (NF-κB), which is activated by oxidative and nitrosative stress and in turn activates the production of cytokines involved in inflammatory responses [12]. NF-κB-dependent inflammation has been demonstrated to contribute to anxiety-like behavior in rats following sub-chronic oxidative stress [13].
Fluoxetine (Flx) is an antidepressant that belongs to the class of selective serotonin reuptake inhibitors (SSRI) that are the first therapeutic choice for the treatment of depression [14]. In addition to an elevation in serotonin, secondary long-term downstream effects of Flx, such as neurogenesis [15], neuronal plasticity [16] and the attenuation of hypothalamic–pituitary–adrenocortical (HPA) axis reactivity [17], may also be involved in the alleviation of depressive symptoms. Previous studies have shown that Flx has neuroprotective activity against depressive-like behavior in rats exposed to restraint stress, in which its antidepressant properties have been attributed to its potent antioxidant [18] and anti-inflammatory effects [19]. However, the exact molecular mechanisms that underlie the antidepressive effect of Flx with regard to the suppression of oxidative stress and anti-inflammatory effect remain unclear.
The aim of this study was to examine the effects of 3 weeks of Flx treatment (15 mg/kg/day) on behavioral changes of socially isolated rats and on the GSH-dependent defense system as well as CAT. We also explored the effects of Flx on the cytosolic/nuclear distribution of NF-κB and cytosolic IL-1β and IL-6 protein expression. These parameters were assessed in the hippocampus of rats exposed to 6 weeks of social isolation, which is an animal model for depression. We used chronic social isolation (CSIS), a mild psychosocial stress that has been shown to evoke a variety of neurochemical and neuroendocrine changes in rats similar to those observed in people with psychiatric disorders, including depression [20] and schizophrenia [21]. Recently, we demonstrated that 3 weeks of CSIS was able to diminish interest in rewarding stimuli, evidenced by reduced preference for sucrose solution and compromised superoxide dismutases (SODs) activity, resulting in ROS defense inefficiency [22, 23]. This is in line with the notion that repeated antidepressant treatments can antagonize stress-induced anhedonia [24, 25]. The question of how chronic antidepressant treatment induced reversal of psychosocial stress-induced oxidative stress may coincide with the normalization of behavioral changes has not yet been fully addressed. We postulated that CSIS-induced depressive- and anxiety-like behaviors may be associated with altered GSH-dependent antioxidative defense system and increased proinflammatory cytokines, which may be reversed by Flx. Understanding the role of proinflammatory cytokines in the pathophysiology of depression may also help to identify characteristics of treatment-resistant depression. The hippocampus was chosen as it is a brain structure responsible for the regulation of the HPA stress response and undergoes structural and physiological alterations following chronic stress exposure.
Experimental procedures
Animals
Adult male Wistar rats (2.5 months old) were housed under standard conditions in groups of four per cage in a temperature 20 ± 2 °C, humidity 55 ± 10% with access to water and food (commercial rat pellets) ad libitum. All animals were maintained under a 12 h light/dark cycle (lights on 0700–1900 h). All experimental procedures were carried out in accordance with the Ethical Committee for the Use of Laboratory Animals of the Institute of Nuclear Sciences “Vinča”, which follows the guidelines of the registered “Serbian Society for the Use of Animals in Research and Education”, license 323-07-01893/2015-05.
Preparation of fluoxetine-hydrochloride solution
Flunisan tablets (containing 20 mg of fluoxetine-hydrochloride) were purchased from Hemofarm AD Vršac, with the reference standard obtained from the same company. To prepare the fluoxetine-hydrochloride (hereafter referred to as Flx) solution for treatment, Flunisan tablets were crushed and dissolved in distilled, sterile water with the aid of ultrasound, and filtered through Whatman No. 42 filter paper. Maximal fluoxetine solubility in water is reported to be 50 mg/ml (http://www.drugbank.ca/drugs/DB00472). The concentration of the Flx solution was determined using ultra performance liquid chromatography (UPLC) analysis [26]. The actual concentration of Flx in our solution was 4.2 mg/ml, accompanied with an unknown concentration of the tablet’s excipients. This Flx concentration, together with rats’ weights, determined once a week, was used to calculate volume of drug solution (1.0–1.5 ml) which should be administered to each animal to achieve the target dose. We treated the animals with 15 mg/kg/day of Flx solution intraperitoneally (i.p.) for a period of 3 weeks, which resulted in a mean (±SEM) serum concentration of 280 ± 29 ng/ml in Flx-treated controls and 230 ± 6 ng/ml in Flx-treated CSIS animals, as measured 24 h after the last treatment [27]; these serum Flx levels are similar to those reported in human patients treated with therapeutically effective doses of 20–80 mg/day Prozac (100–700 ng/ml) [28]. There was no significant difference between Flx-treated controls and Flx-treated CSIS animals which is in agreement with the findings of Czéh et al. [29].
Study design
At the onset of experiment, the animals were randomly divided into control rats, housed in groups of four animals per cage, and rats that underwent chronic social isolation (CSIS) stress for 6 weeks. CSIS rats were housed individually and deprived of any visual or tactile contacts with other animals, but had normal auditory and olfactory experiences, according to the model of Garzón and Del Río [30]. After 3 weeks, Flx was administered i.p. at a dose of 15 mg/kg/day. Flx treatment was administered to controls and the CSIS group (Cont + Flx and CSIS + Flx, n = 9 rats in each group) during the last 3 weeks of social isolation in CSIS animals. Both vehicle groups received daily i.p. injections of physiological saline (0.9% NaCl) (Cont + Veh and CSIS + Veh, n = 9 rats in each group) under conditions matching those of the Flx-treated groups (Fig. 1). Behavioral studies, such as sucrose preference and marble burying tests were carried out between 1200 and 1600 h.
Behavioral testing
Sucrose preference test
The relative preference for a sucrose solution versus water provides a simple measure to assess anhedonia, a common characteristic of depression [31]. Animals were individually placed in separate plastic cages and presented simultaneously with two preweighed bottles (±0.1 g) containing 0% (tap water) or 2% sucrose solution for 3 days, with fluid intake monitored for 1 h. Rats were not deprived of food or water to avoid any stress related to these procedures. To eliminate potential side preferences, the position of bottles was alternated across days. The sucrose preference (SP) test was calculated using the formula SP = [consumed sucrose solution/total liquid consumed (sucrose solution + water)] × 100. The SP test was conducted prior to the start (baseline) and at the end of the third and sixth week of the experiment. Attenuated sucrose intake in this test is hypothesized to model anhedonia by reflecting impaired sensitivity to rewards.
Marble burying test
The marble burying (MB) test was used to measure anxiety-like behavior [32]. Each animal was individually placed in a separate plastic cage with a 2-cm-thick layer of bedding (aspen shavings). Briefly, six glass marbles (2.5 cm in diameter) were placed along a side wall of each cage, and the behavior of rats was observed during a 30-min test period. After 30 min, the animals were removed from the cages and the number of buried marbles (with at least two-thirds of the surface covered with bedding) was assessed. The MB test was performed prior to the start (baseline) and at the end of the third and sixth week of the experiment. MB behavior reflects an active effort in rodents to hide unfamiliar objects in bedding and may indicate anxiety-like behavior [32].
Preparation of nuclear/cytosolic fractions from the rat hippocampus
Animals were deeply anesthetized with ketamine/xylazine (100/5 mg/kg i.p.), transcardially perfused with physiological saline and then killed by guillotine decapitation. The whole brain was immediately removed and the hippocampus was dissected on ice. To obtain cellular fractions, hippocampi were homogenized at 4 °C using 20 strokes of a Potter–Elvehjem glass homogenizer with a Teflon pestle in cold homogenization buffer containing 0.25 M sucrose, 10 mM Tris/HCl (pH 7.4) containing a protease inhibitor cocktail tablet (complete tablets, Mini, EASY pack, Roche). The samples were centrifuged at 1000×g at 4 °C for 10 min to obtain the pellet of nuclei [23]. The obtained supernatant (S1) was further centrifuged at 15,000×g at 4 °C for 25 min and the resulting supernatant (S2) was further centrifuged at 100.000×g at 4 °C for 60 min to obtain the cytosolic fraction which were stored at −70 °C until experimental work. The protein concentration was measured by the method of Lowry et al. [33] using purified bovine serum albumin as a standard.
Biochemical assays
GSH was determined from freshly prepared cytosol fraction according to Ellman’s method and modified by Hissin and Hilf [34]. The activity of cytosolic GPx was assayed at 340 nm, using a Ransel kit (Randox Laboratories, Crumlin, UK). The activity of cytosolic GLR was assayed according the method of Carlberg and Mannervik [35]. GPx and GLR activities were calculated using molar extinction coefficients of nicotinamide adenine dinucleotide phosphate (NADPH) (6.2 mM−1cm−1) and were expressed as mU/mg of proteins, where 1 U is the amount of GPx or GLR necessary for conversion of 1 µmol of NADPH into NADP+ in one minute, per mg of proteins in sample. Cytosolic GST activity was assessed at 340 nm, using 1-chloro-2,4-dinitrobenzene (CDNB) as a substrate, as described by Habig et al. [36]. GST activity was expressed as mU/mg of proteins by measuring the rate of GSH-CDNB conjugate formation using extinction coefficient of 9.6 mM−1cm−1 for CDNB. Cytosolic CAT activity was measured using the method of [37], in which a decrease in absorbance at 240 nm was measured, CAT activity was expressed as the amount of CAT that decomposes 1 µmol of H2O2 per minute per milligram of protein (U/mg), using an extinction coefficient of 43.6 M−1cm−1.
Western blot analysis of GPx, GLR, CAT, NF-κB, IL-6 and IL-1β
The hippocampal cytosolic and nuclear protein fractions were separated on an SDS–polyacrylamide gel and transferred to a polyvinylidene difluoride membrane using Mini Trans-blot apparatus (Bio-Rad). Immunodetection was performed with specific primary antibodies against GLR (SC-32886, Santa Cruz Biotechnology, Inc), GPx (SC-30147, Santa Cruz, Biotechnology, Inc), NF-κB (SC-372, Santa Cruz, CA, USA), CAT (PA5-29183, Thermoscientific), IL-6 (ab6672, Abcam) and IL-1β (AB1832P, Millipore) followed by 1 h for GPx, NF-κB, IL-6 and IL-1β, and 2 h for GLR and CAT incubation with anti-rabbit HRP-conjugated secondary antibodies (A-5316, Sigma) and goat anti-rabbit HRP-conjugated secondary antibodies (SC-2004, Santa Cruz Biotechnology, Inc), respectively. To confirm a consistent protein loading, β-actin (SC-1616-R, Santa Cruz, CA, USA) was used, followed by anti-rabbit HRP-labeled secondary antibody (SC-2004, Santa Cruz Biotechnology, Inc). Antigen–antibody complexes were visualized by chemiluminescence using Immobilon western chemiluminescent HRP substrate (Millipore Corporation, Billerica, MA 01821 USA), evaluated using a Chemidoc-MP System (Bio-Rad) and analyzed with Image Lab 5.0 software (BioRad). Western blot results are expressed as protein/β-actin ratio. We evaluated statistically significant percent difference between each band of treated samples compared to controls (relative quantification); thus they are consequently presented as percentages of their corresponding controls, taken as 100%. We used Pierce Prestained protein Molecular Weight Marker (Thermo Scientific, USA) as a calibration standard for protein molecular mass.
Statistical analysis
Two-way repeated measures analysis of variance (ANOVA) [the factors were drug treatment (levels: vehicle and Flx), stress (levels: control and CSIS)] and the time as repeated measure [levels: baseline (week 0), and at week 3 and 6] followed by a Duncan’s post hoc test for sucrose preference and marble burying test were used (STATISTICA Release 7) (n = 9 animals per each group). Biochemical parameters were analyzed by a two-way ANOVA [the factors were drug treatment (levels: vehicle and Flx) and stress (levels: controls and CSIS)]. Duncan’s post hoc test was used to evaluate differences between groups. For biochemical parameters, hippocampal samples from each group (n = 9) were pooled in 3 × 3. Statistical significance was set at p < 0.05. The data are presented as mean ± SEM derived from n = 5–7 independent measurements per each group.
Results
Flx reversed depressive- and anxiety-like behaviors induced by CSIS in rats
The results of the sucrose preference test are shown in Fig. 2a. A two-way repeated measures ANOVA revealed significant main effects of CSIS (F 1.32 = 16.78, p < 0.001) and time (F 2.64 = 4.66, p < 0.05). Post hoc tests revealed a significant decrease in preference for sucrose in the CSIS + Veh group at the end of 3 (* p < 0.05) and 6 weeks (** p < 0.01) compared to baseline. The CSIS + Flx group, prior to treatment with Flx, also showed a significant decrease in sucrose preference at the end of 3 weeks compared to baseline (* p < 0.05). The CSIS + Flx group showed a significant increase in sucrose preference (^ p < 0.05) at the end of 6 weeks, compared to the 3-week time point. A significant increase in sucrose preference in CSIS + Flx compared to CSIS + Veh rats at the end of 6 weeks (++ p < 0.01) was noted while no significant change was seen in Flx-treated controls or vehicle-treated rats. Results indicate that CSIS resulted in a reduction of sucrose preference that was time dependent, suggesting that 6 weeks of CSIS induced anhedonic-like behavior; furthermore, 3 weeks of Flx treatment (15 mg/kg/day) reversed this reduction in socially isolated rats, as seen at the 6 weeks time point.
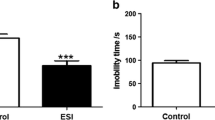
Sucrose preference (a) and number of buried marbles (b) in controls (Cont) and chronic social isolation (CSIS) rats at baseline and after 3 and 6 weeks treated either with vehicle (Veh. 0.9% NaCl), or fluoxetine (Flx, 15 mg/kg/day). Results are expressed as mean ± SEM. n = 9 rats in each group. Significant differences between groups obtained from two-way repeated measures ANOVA followed by Duncan’s post hoc test are indicated as follows: a sucrose preference (* p < 0.05 CSIS + Veh (3 weeks) vs. CSIS + Veh (baseline): ** p < 0.01 CSIS + Veh (6 weeks) vs. CSIS + Veh (baseline); ^ p < 0.05 CSIS + Flx (6 weeks) vs. CSIS + Veh (3 weeks); ++ p < 0.01 CSIS + Flx (6 weeks) vs. CSIS + Veh (6 weeks); b number of buried marbles (*** p < 0.001 CSIS + Veh (3 weeks) vs. CSIS + Veh (baseline); * p < 0.05 CSIS + Veh (6 weeks) vs. CSIS + Veh (baseline); ^^^ p < 0.05 CSIS + Flx (6 weeks) vs. CSIS + Flx (3 weeks); + p < 0.05 CSIS + Flx (6 weeks) vs. CSIS + Veh (6 weeks)
To examine CSIS-induced anxiety in rats, the marble burying test was used (Fig. 2b). A two-way repeated measures ANOVA revealed significant main effects of CSIS (F 1.32 = 41.13, p < 0.001) and time (F 2.64 = 15.94, p < 0.001), as well as a significant CSIS × time interaction (F 2.64 = 17.83, p < 0.001), drug treatment × time interaction (F 2.64 = 6.34, p < 0.01), and CSIS × drug treatment × time interaction (F 2.64 = 3.95, p < 0.05). Post hoc tests demonstrated no change in the number of buried marbles in vehicle-groups (Cont + Veh, Cont + Flx). An increased number of buried marbles in the vehicle-treated CSIS group after 3 and 6 weeks compared to baseline values (*** p < 0.001 and * p < 0.05, respectively) was found. Prior to treatment, the CSIS–Flx group showed an increase in marble burying test at the end of 3 weeks compared to baseline (*** p < 0.01). Moreover, post hoc tests revealed a significant decrease in the number of buried marbles in the CSIS + Flx group (6 weeks), as compared to the 3-week time point (^^^ p < 0.001) and to CSIS + Veh rats at the 6-week time point (+ p < 0.05). Results suggest that 6 weeks of CSIS produced anxiety-like behaviors as assessed by an increased number of buried marbles, and chronic Flx treatment (15 mg/kg/day) reversed this effect in socially isolated rats.
Hippocampal GSH content and activity of GPx, GLR, GST and CAT
To determine whether CSIS-induced behavioral changes are associated with alterations in the GSH-dependent defense system, we measured GSH content and GPx, GLR, GST, and CAT activity in cytosolic fractions of rat hippocampus (Fig. 3a–e). A two-way ANOVA revealed a significant main effect of Flx treatment (F 1.20 = 7.73, p < 0.05) on cytosolic GSH. Post hoc analyses showed a significant increase in GSH content in the CSIS + Flx group as compared to CSIS alone (^ p < 0.05). In comparison to vehicle-treated controls, CSIS rats showed a trend toward a decrease in GSH that was not statistically significant (p > 0.05) (Fig. 3a).
GSH level (nmol/mg protein) (a), GPx activity (mU/mg protein) (b), GLR activity (mU/mg protein) (c), GST activity (mU/mg protein) (d) and CAT activity (U/mg protein) (e) in the cytosolic fraction of the hippocampus in control (Cont) and chronic social isolation (CSIS) rats treated either with vehicle (0.9% NaCl) or Flx (15 mg/kg/day). Results are expressed as mean ± SEM, n = 6 independent measurements in each group. Significant differences between groups obtained from two-way ANOVA analyses followed by post hoc Duncan test are indicated as follows: a GSH content (^ p < 0.05 CSIS + Flx vs. CSIS + Veh); b GPx activity (** p < 0.01 and *** p < 0.001 all experimental treated groups vs. Cont + Veh; ^ p < 0.05 CSIS + Flx vs. CSIS + Veh; # p < 0.05 Flx-treated CSIS vs. Flx-treated controls); c GLR activity (** p < 0.01 and *** p < 0.001 Flx-treated groups (Cont and CSIS) vs. Cont + Veh; ^ p < 0.05 CSIS + Flx vs. CSIS + Veh); d GST activity (*** p < 0.001 CSIS + Veh vs. Cont + Veh; ^^^ p < 0.001 CSIS + Flx vs. CSIS + Veh); e CAT activity (*** p < 0.001 Flx-treated groups (Cont and CSIS) vs. Cont + Veh; # p < 0.05 Flx-treated CSIS vs. Flx-treated controls
The activity of GPx in cytosolic fractions of rat hippocampus is shown in Fig. 3b. A two-way ANOVA revealed a significant main effect of Flx treatment (F 1.20 = 47.81, p < 0.001) and a significant CSIS × Flx treatment interaction (F 1.20 = 14.50, p < 0.01) on hippocampal cytosolic GPx activity. A significant increase was observed in the vehicle-treated CSIS (** p < 0.01) and Flx-treated (controls and CSIS) groups (*** p < 0.001) as compared to vehicle-treated control animals. Post hoc tests showed a significant increase in GPx activity in the Flx-treated CSIS group compared to vehicle-treated CSIS rats (^ p < 0.05), but decreased compared to Flx-treated controls (# p < 0.05).
The activity of GLR in cytosolic fractions of rat hippocampus is shown in Fig. 3c. A two-way ANOVA revealed a significant main effect of Flx treatment (F 1.20 = 12.20, p < 0.01) on hippocampal cytosolic GLR activity. Post hoc tests showed a significant increase in GLR activity in Flx-treated controls (* p < 0.05) and the Flx-treated CSIS (** p < 0.01) group, as compared to vehicle-treated controls. Flx-treated CSIS animals showed a significant increase in GLR activity compared to the vehicle-treated CSIS group (^ p < 0.05).
The activity of GST in cytosolic fractions of rat hippocampus is shown in Fig. 3d. A two-way ANOVA revealed significant main effects of CSIS (F 1.20 = 9.07, p < 0.001) and Flx treatment (F 1.20 = 10.11, p < 0.001), and a significant CSIS × Flx treatment interaction (F 1.20 = 10.28, p < 0.001) on cytosolic GST activity. Post hoc tests showed a significant decrease in GST activity in vehicle-treated CSIS rats compared to vehicle-treated controls (*** p < 0.001). Also, a significant increase in GST activity in the Flx-treated CSIS group compared to vehicle-treated CSIS animals was observed (^^^ p < 0.001).
The activity of CAT in cytosolic fractions of rat hippocampus is shown in Fig. 3e. A two-way ANOVA revealed significant main effects of CSIS (F 1.20 = 28.41, p < 0.001) and Flx (F 1.20 = 20.99, p < 0.001), and a significant CSIS × Flx treatment interaction (F 1.20 = 4.66, p < 0.05) on cytosolic CAT activity. Post hoc tests showed significantly reduced CAT activity following CSIS relative to vehicle controls (*** p < 0.001), as well as in both Flx-treated groups (control or CSIS) in comparison to vehicle-treated controls (*** p < 0.001). Moreover, a significant decrease in CAT activity in the Flx-treated CSIS group compared to Flx-treated controls (# p < 0.05) was found.
Western blot analysis of GPx, GLR, CAT, NF-κBp65, IL-1β and IL-6
To examine the possible molecular mechanisms underlying the CSIS-induced behavioral changes, we evaluated cytosolic protein levels of GPx, GLR and CAT, as well as the cytosolic/nuclear distribution of NF-κB p65 in rat hippocampus (Figs. 4a–c, 5a). A two-way ANOVA revealed a significant main effect of CSIS (F 1.23 = 16.65, p < 0.001), Flx (F 1.23 = 10.10, p < 0.01) and a significant Flx treatment × CSIS interaction (F 1.23 = 15.45, p < 0.001) on cytosolic GPx protein expression. Post hoc analysis showed a significant increase in GPx protein levels in the vehicle-treated CSIS group as compared to vehicle-treated controls (*** p < 0.001) (Fig. 4a). A significant decrease in cytosolic GPx protein level in the Flx-treated CSIS group as compared to the vehicle-treated CSIS group was observed (^^^ p < 0.001).
Protein levels of GPx (a), GLR (b) and CAT (c) in the hippocampus of controls (Cont) and chronic social isolation (CSIS) rats treated either with vehicle (0.9% NaCl), or Flx (15 mg/kg/day). Results are expressed as mean ± SEM, n = 5–7 independent measurements in each group. Significant differences between groups obtained from two-way ANOVA analyses followed by post hoc Duncan test are indicated as follows: a GPx protein expression (*** p < 0.001 CSIS + Veh vs. Cont + Veh; ^^^ p < 0.001 CSIS + Flx vs. CSIS + Veh); b GLR protein expression (* p < 0.01 and *** p < 0.001 Cont + Flx or CSIS + Flx vs. Cont + Veh; ^^^ p < 0.001 CSIS + Flx vs. CSIS + Veh; ## p < 0.01 CSIS + Flx vs. Con + Flx); c CAT protein expression (*** p < 0.001 CSIS +Veh vs. Cont + Veh; ^^^ p < 0.001 CSIS + Flx vs. CSIS + Veh; # p < 0.01 CSIS + Flx vs. Con + Flx)
Protein levels of NF-κBp65 (a), IL-6 (b) and IL-1β (c) in the hippocampus of controls (Cont) and chronic social isolation (CSIS) rats treated either with vehicle (0.9% NaCl), or Flx (15 mg/kg/day). Results are expressed as mean ± SEM, n = 5–7 independent measurements in each group. Significant differences between groups obtained from two-way ANOVA analyses followed by post hoc Duncan test are indicated as follows: a NF-κBp65 cytosolic/nuclear protein expression (** p < 0.001 CSIS + Veh vs. Cont + Veh; ^^ p < 0.01, ^ p < 0.05 CSIS + Flx vs. CSIS + Veh); b IL-6 (** p < 0.001 CSIS + Veh vs. Cont + Veh; ^^ p < 0.01 CSIS + Flx vs. CSIS + Veh); c IL-1β (no significant effects were observed)
With regard to GLR protein levels, a two-way ANOVA revealed significant main effects of CSIS (F 1.17 = 12.96, p < 0.05) and Flx treatment (F 1.17 = 32.11, p < 0.001) on GLR protein expression. Post hoc tests showed significant increase of GLR levels in Flx-treated rats (vehicle or CSIS) in comparison to vehicle-treated controls (* p < 0.05, *** p < 0.001) (Fig. 4b). However, no statistically significant difference between vehicle-treated CSIS rats and vehicle-treated controls (p > 0.05) was observed. Moreover, a significant increase in GLR protein levels was observed in the CSIS + Flx group compared to Flx-treated controls (## p < 0.01) and the vehicle-treated CSIS group (^^^ p < 0.001).
A two-way ANOVA revealed a significant main effect of Flx treatment (F 1.20 = 9.42, p < 0.01) and a significant Flx treatment × CSIS interaction (F 1.20 = 23.90, p < 0.001) on CAT protein expression. A significant decrease in cytosolic CAT protein levels was found in vehicle-treated CSIS animals (*** p < 0.001) as compared to vehicle-treated rats. The Flx-treated CSIS group showed a significant increase in CAT levels as compared to the vehicle-treated CSIS group (^^^ p < 0.01) and Flx-treated controls (# p < 0.05) (Fig. 4c).
NF-κB activation and its nuclear translocation were examined by monitoring NF-κB p65 localization in cytosolic and nuclear fractions in the rat hippocampus (Fig. 5a). A two-way ANOVA showed significant main effects of CSIS (F 1.23 = 7.31, p < 0.05) and Flx treatment (F 1.23 = 5.07, p < 0.05) on NF-κB protein expression in the cytosolic fraction of the hippocampus. A significant decrease in the vehicle-treated CSIS group compared to vehicle-treated rats (** p < 0.01) and an increase in the Flx-treated CSIS group compared to vehicle-treated CSIS (^^ p < 0.01) were observed. In the nuclear fraction, a two-way ANOVA revealed a significant main effect of CSIS (F 1.21 = 5.578, p < 0.05) and a significant Flx treatment × CSIS interaction (F 1.21 = 6.209, p < 0.05) on NF-κB protein levels (Fig. 5a). Post hoc tests showed a significant increase of NF-κB levels in vehicle-treated CSIS group as compared to vehicle-treated rats (** p < 0.01). Furthermore, significant decrease in Flx-treated CSIS group as compared to vehicle-treated CSIS group (^ p < 0.05) was revealed.
To determine whether CSIS stress may lead to an inflammatory response, the protein expression of proinflammatory cytokines such as IL-1β and IL-6 was determined. A two-way ANOVA revealed a significant main effect of Flx (F 1.20 = 6.56, p < 0.05) and a significant Flx treatment × CSIS interaction (F 1.20 = 7.60, p < 0.05) on cytosolic IL-6 protein levels. Post hoc tests showed a significant increase in cytosolic IL-6 levels in the vehicle-treated CSIS group as compared to vehicle-treated rats (** p < 0.01) (Fig. 5b). Furthermore, significant decrease in the Flx-treated CSIS group as compared to vehicle-treated CSIS group (^^ p < 0.01) was revealed. With regard to cytosolic IL-1β protein levels, a two-way ANOVA did not reveal significant main effects of CSIS stress (F 1.19 = 0.72, p = 0.41) or Flx (F 1.19 = 0.34, p = 0.57), or a Flx treatment × CSIS interaction (F 1.19 = 1.66, p = 0.21) (Fig. 5c).
Discussion
The most common stressors reported as risk factors for psychiatric disorders, such as depression, are of a social nature in humans [38] and social animals [39]. Our results suggest that 6 weeks of CSIS during adulthood in male Wistar rats may be deleterious, as rats exposed to CSIS showed a reduced sucrose preference, indicative of an impaired sensitivity to reward and anhedonia, one of the basic symptoms of depression [31, 40]. We recently reported that CSIS induced an increase in immobility and decrease in time spent swimming and climbing in the forced swim test [23], in which prolonged immobility time represents a “behavioral despair” and may reflect depressed mood and/or behavioral helplessness [41]. We also observed anxiety-like behaviors in socially isolated rats in the marble burying test. Moreover, CSIS rats showed enhanced anxiety-like behavior in open field [42] and elevated plus maze testing [25], characterized by an avoidance of the central zone in the open field test and a general decrease in locomotion (total number of arm entries) in the elevated plus maze, both indicative of anxiogenic behavior relevant for mood disorders and schizophrenia (psychiatric disorders). Furthermore, socially isolated rats have been shown to spend less time in the light compartment of the light–dark box, again indicative of anxiety-like behavior [43]. CSIS-induced anhedonia and anxiety have been identified as a correlate of depression [44], and previous studies have suggested that the reversal of depressive- and anxiety-like behaviors may be associated with the antioxidant activity of drugs. In our study, chronic treatment with Flx reversed depressive- and anxiety-like behaviors in CSIS rats, assessed by an increase in SP, indicative of an antidepressant-like effect, and a decrease in the number of buried marbles, indicative of an anxiolytic-like effect. These results are consistent with previous studies of the antidepressant effect of Flx and other SSRIs. For example, SSRIs, including Flx, have been shown to reduce immobility and stimulate swimming in the forced swim test [41]. Nevertheless, the underlying molecular mechanisms of chronic CSIS-induced depressive- and anxiety-like behaviors remain unclear. Given that the brain is particularly vulnerable to free radical damage, compromised brain GSH content may be associated with stress-induced behavioral depression [45]. GSH plays an important role in cellular defense against oxidative stress by scavenging ROS and serves as a cofactor for GPx and GST [46]. In our study, GSH content following CSIS showed a tendency toward a reduction but without statistical significance. Given that GPx, GLR and GST provide protection from oxidative stress at the expense of GSH, alternation in these enzyme activities may also result in GSH content changes [46]. Hence, the (unchanged) GSH content following CSIS may be a result of synergistic effects of altered activities of GSH-dependent enzymes (Fig. 6). Even though the activity of GPx was increased, suggesting depletion of GSH because of its elevated consumption used for reduction of H2O2 and yielding glutathione disulfide (GSSG), it was accompanied by unchanged GLR activity, the main enzyme that recycles GSSG to GSH using the reduced NADPH [47]. Moreover, CSIS decreased GST activity, implying reduced consumption of GSH as a substrate in its conjugation reactions. Increased GPx activity following CSIS suggests the induction of antioxidant defense mechanisms while unchanged GLR activity in CSIS rats may result from an NADPH deficiency [48] or increased H2O2 concentration [49]. A decrease in GST activity following CSIS stress is in agreement with the data obtained from clinical trials [6]. Also, chronic restraint stress decreases mRNA expression levels of the most prevalent GST form in hippocampus of mice [50]. Since GSTs are not only involved in the metabolism of xenobiotics, but also in the removal of oxidized products such as peroxidized lipids and oxidized proteins, they play an important role in cellular protection against oxidative stress. Therefore, a reduction in GST activity may signify a diminished ability of cells to remove toxins and free radicals, implying an enhanced cellular susceptibility to CSIS-induced oxidative damage. This may result in the accumulation of undesirable oxidized products, causing the morphological changes observed in hippocampus in major depression [51]. Besides major depression, morphological changes (white matter changes, reduced volumes) in the hippocampus are also recognized in schizophrenia, since hippocampus has an important part in pathopsychology state of this psychiatric disorder [52, 53].
High concentrations of superoxide anions are able to decrease the activity of CAT, a hydrogen peroxide-metabolizing enzyme, by oxidizing the heme group in the active site. In this study, we found decreased CAT activity following CSIS stress. Furthermore, a reduction in activity of CAT may have been associated with a large amount of H2O2 available to react with transition metals and generate hydroxyl radicals (the most harmful radical) [54], which could further promote NF-κB signaling. Our findings may also relate to previous data demonstrating changes in CAT levels during the course of depression in humans [55]. High levels of ROS, which can compromise redox balance, may arise from mitochondrial electron transport chain and increased superoxide production in the mitochondria [47], xanthine oxidase [56], microglial NADPH oxidase activation [57] or glutamate concentration increases [58]. Based on these results, we may assume that CSIS stress compromises redox homeostasis in the rat hippocampus. Our findings confirm a previous study that reported depressive-like behavior was associated with decreased CAT and GLR activities in a mouse model of major depression, and repeated administration of Flx for 14 days at a dose of 10 mg/kg/day significantly reversed stress-induced depressive-like behavior and oxidative damage [59].
Chronic Flx treatment increased GPx and GLR activity in control rats, suggesting that it possesses antioxidant effects in the absence of oxidative stress. The simultaneous upregulation of GPx and GLR activity in Flx-treated CSIS rats compared to the CSIS group suggests an efficient defense against CSIS-induced oxidative stress. Moreover, the ability of Flx to provide neuroprotection against oxidative stress is at least partially mediated by the suppression of microglial NADPH oxidase activation and nitric oxide synthase, causing a decrease in ROS and RNS production [60]. Recent studies have revealed that Flx modulates genes related to redox pathways, stimulating the expression of the transcriptional nuclear factor E2-related factor 2 (Nrf2) and Nrf2 antioxidant response elements in a mouse model of anxiety/depression [61]. Interestingly, Flx treatment did not reverse the CSIS-induced decrease of CAT activity. In fact, Flx treatment decreased CAT activity in controls. A “cumulative” effect of CSIS and Flx may cause decreased CAT activity, likely via mitochondrial ROS generation. Furthermore, Curti et al. [62] reported that Flx per se interacts with the lipid bilayer of the inner membrane in isolated rat brain mitochondria, and affects electron transport and F 1 F 0-ATPase activity, thereby inhibiting oxidative phosphorylation in rat brain. Moreover, antidepressants are known to be highly membrane soluble and able to affect biological events associated with the membrane [63]. As the decreased CAT activity did not correspond to increased protein expression under CSIS, this may indicate the lack of an effective CAT response. The discrepancy between protein expression and activity of CAT may be indicative of the underlying oxidative stress.
Nonetheless, GSH levels in Flx-treated CSIS rats were increased as compared to CSIS alone, in parallel with an increase in GLR activity. Moreover, increased GST activity in Flx-treated CSIS animals compared to CSIS alone is likely a defensive response against the presence of the drug and its metabolites. In line with this, Zafir et al. [64] demonstrated that 3 weeks of Flx treatment (20 mg/kg/day) in a restraint-induced depression-like rat model re-established the functionality of CAT, GST, GLR activities and GSH levels in the brain following disruption caused by restraint stress. Moreover, restoring the affected GSH pathways with Flx treatment may relate to neuroprotection, as the antioxidative effects of Flx [64] are thought to be mediated by increases in serotonin levels [65].
In the present study, we found increased levels of NF-κB in the nuclear fraction of the hippocampus of CSIS rats, accompanied by increased IL-6 protein levels, indicative of enhanced neuroinflammation. We focused on the proinflammatory cytokine IL-1β and IL-6 in our study because of previous studies indicating increased serum IL-1β and IL-6 concentrations in depressed patients [66, 67] and clinically anxious individuals [68], as well as in animal models of depression [69]. Moreover, in the most recent study performed on humans, correlation was made between selective increase of IL-6 in cerebrospinal liquid during endotoxin-induced systemic inflammation and a severity of the accompanying mood impairment, indicating a potential key role of IL-6 in the onset of mood disorders and thereby depression [70]. In accordance with this study, we did not detect differences in IL-1β protein levels between experimental groups, suggesting no specific chronic treatment or CSIS effects on this level. Therefore, we speculate that changes in GSH-dependent redox status enabled NF-κB translocation into the nucleus, possibly leading to transcriptional activation of the IL-6 receptor, thus increasing IL-6 expression. Moreover, oxidative stress facilitates the activation of NF-κB, reported to promote inflammation including IL-6 in anxiety disorder [68]. It is also possible that proinflammatory cytokines in the periphery may provoke neuroinflammation [70, 71] to primarily affect the hippocampus [72], but this mechanism remains to be determined. Hence, cytokines present in the brain following stress may come from the periphery, brain endothelial cells and epithelial cells of the choroids plexus and ventricles, as well as glia and neurons of the hippocampus, hypothalamus and amygdala [73, 74]. Moreover, increased levels of IL-1β and IL-6 have been observed in the hippocampus and blood of rats exposed to chronic mild stress [75, 76], as well as in the plasma and cerebrospinal fluid of depressed patients, whereby IL-6 has been recently proposed to play a crucial role [70, 77]. Chourbaji et al. [78] demonstrated that IL-6 knockout mice (IL-6(−/−) showed resistance to stress-induced helplessness, suggesting that it plays a role in the molecular mechanisms mediating depressive-like behavior, as external stressors increase IL-6 in wild-type hippocampi and a lack of IL-6 confers resistance to depression-like behavior. Previous studies have demonstrated that depressive-like behavior following CSIS is associated with activated NF-κB and peripheral and central inflammation [71]. Treatment with Flx significantly reduces the activity of the transcription factor NF-κB, decreasing its nuclear protein levels. NF-κB is shown to be functionally related to activity of NMDA receptors [79] which are known to be inhibited by antidepressants, including direct inhibition by Flx [80]. These NF-κB changes could also be accompanied with the controlled expression of IL-6. Moreover, fluvoxamine, an SSRI, has been shown to inhibit IL-6 secretion in stimulated microglial cell culture [81]. Inhibition of IL-6 in the amygdala and hippocampus also significantly reduced immobility time in the forced swim test [82], and reduced circulating levels of IL-6 in response to SSRIs have been observed in in vivo studies [83]. Liu et al. [19] demonstrated that Flx promotes a decrease in production of IL-6 by reducing the transcription levels of mRNA for IL-6. In our study, a decrease in IL-6 protein levels in CSIS rats may be explained by a suppression of NF-κB activation following Flx treatment [84]. The immunomodulatory feature of antidepressants was also shown in the study with bupropion, the antidepressant with different mechanism of action, where it showed its effectiveness in lowering the levels of proinflammatory cytokines as well as in increasing the level of anti-inflammatory cytokine interleukin-10 [85, 86]. The same results regarding negative immunomodulatory effect were reported for Flx with hypothesis of molecular mechanism that is PKA pathway-activation mediated [87]. In addition, NF-κB is known to be regulated by mGlu5 receptors [88] which have an important role in the regulation of emotionality [89].
In summary, our data reveal that 6 weeks of CSIS in adult male Wistar rats caused depressive- and anxiety-like behaviors, as indicated by a decrease in sucrose preference test and an increase in the number of buried marbles. Furthermore, we have identified a signaling cascade in which CSIS compromised redox homeostasis in the hippocampus, targeting enzymes such as GPx, CAT and GST, as well as provoking oxidative stress. The latter may promote NF-κB-dependent inflammation via increased IL-6. All of these changes may contribute to depressive and anxiety-like behaviors. Altogether, our findings support a link between hippocampal oxidative stress, an inflammatory response, and a social isolation-induced depression- and anxiety-like rat model. In good agreement with this, 3 weeks of Flx treatment (15 mg/kg/day) produced significant antidepressant- and anxiolytic-like effects, coinciding with the modulation of the GSH-dependent defense system associated with suppression of NF-κB activation, the major upstream mechanism regulating oxidative and nitrosative pathways, and cytosolic IL-6 protein expression in the hippocampus of socially isolated rats, causing a protective effect against oxidative stress and neuroinflammation. These results may be relevant to understanding the neurobiological effects of psychosocial stress in humans and may contribute to our understanding of the mechanisms that underlie the antidepressant and anti-inflammatory activity of Flx in socially isolated rats.
References
Maes M, Galecki P, Chang YS, Berk M (2011) A review on the oxidative and nitrosative stress (O&NS) pathways in major depression and their possible contribution to the (neuro)degenerative processes in that illness. Prog Neuropsychopharmacol Biol Psychiatry 35:676–692. doi:10.1016/j.pnpbp.2010.05.004
de Kloet ER, Joëls M, Holsboer F (2005) Stress and the brain: from adaptation to disease. Nat Rev Neurosci 6:463–475. doi:10.1038/nrn1683
Lupien SJ, McEwen BS, Gunnar MR, Heim C (2009) Effects of stress throughout the lifespan on the brain, behaviour and cognition. Nat Rev Neurosci 10:434–445. doi:10.1038/nrn2639
Filipović D, Todorović N, Bernardi RE, Gass P (2017) Oxidative and nitrosative stress pathways in the brain of socially isolated adult male rats demonstrating depressive- and anxiety-like symptoms. Brain Struct Funct 222:1–20. doi:10.1007/s00429-016-1218-9
Chen H-JC, Spiers JG, Sernia C, Lavidis NA (2015) Response of the nitrergic system to activation of the neuroendocrine stress axis. Front Neurosci 9:3. doi:10.3389/fnins.2015.00003
Gawryluk JW, Wang J-F, Andreazza AC et al (2011) Prefrontal cortex glutathione S-transferase levels in patients with bipolar disorder, major depression and schizophrenia. Int J Neuropsychopharmacol 14:1069–1074. doi:10.1017/S1461145711000617
Halliwell B (2011) Free radicals and antioxidants—quo vadis? Trends Pharmacol Sci 32:125–130. doi:10.1016/j.tips.2010.12.002
Hovatta I, Juhila J, Donner J (2010) Oxidative stress in anxiety and comorbid disorders. Neurosci Res 68:261–275. doi:10.1016/j.neures.2010.08.007
Anderson G, Maes M (2013) Schizophrenia: linking prenatal infection to cytokines, the tryptophan catabolite (TRYCAT) pathway, NMDA receptor hypofunction, neurodevelopment and neuroprogression. Prog Neuro-Psychopharmacol Biol Psychiatry 42:5–19. doi:10.1016/j.pnpbp.2012.06.014
Maes M, Bosmans E, De Jongh R et al (1997) Increased serum Il-6 and Il-1 receptor antagonist concentrations in major depression and treatment resistant depression. Cytokine 9:853–858. doi:10.1006/cyto.1997.0238
Loftis JM, Huckans M, Morasco BJ (2010) Neuroimmune mechanisms of cytokine-induced depression: current theories and novel treatment strategies. Neurobiol Dis 37:519–533. doi:10.1016/j.nbd.2009.11.015
Gordon S, Martinez FO (2010) Alternative activation of macrophages: mechanism and functions. Immunity 32:593–604. doi:10.1016/j.immuni.2010.05.007
Salim S, Asghar M, Taneja M et al (2011) Potential contribution of oxidative stress and inflammation to anxiety and hypertension. Brain Res 1404:63–71. doi:10.1016/j.brainres.2011.06.024
Wilde MI, Benfield P (1998) Fluoxetine. A pharmacoeconomic review of its use in depression. Pharmacoeconomics 13:543–561. doi:10.2165/00019053-199813050-00007
Santarelli L, Saxe M, Gross C et al (2003) Requirement of hippocampal neurogenesis for the behavioral effects of antidepressants. Science 301:805–809. doi:10.1126/science.1083328
Vaidya VA, Duman RS (2001) Depresssion–emerging insights from neurobiology. Br Med Bull 57:61–79
Holsboer F (2001) Stress, hypercortisolism and corticosteroid receptors in depression: implications for therapy. J Affect Disord 62:77–91. doi:10.1016/S0165-0327(00)00352-9
Zafir A, Banu N (2007) Antioxidant potential of fluoxetine in comparison to Curcuma longa in restraint-stressed rats. Eur J Pharmacol 572:23–31. doi:10.1016/j.ejphar.2007.05.062
Liu D, Wang Z, Liu S et al (2011) Anti-inflammatory effects of fluoxetine in lipopolysaccharide(LPS)-stimulated microglial cells. Neuropharmacology 61:592–599. doi:10.1016/j.neuropharm.2011.04.033
Heinrich LM, Gullone E (2006) The clinical significance of loneliness: a literature review. Clin Psychol Rev 26:695–718. doi:10.1016/j.cpr.2006.04.002
Möller M, Du Preez JL, Viljoen FP et al (2013) Social isolation rearing induces mitochondrial, immunological, neurochemical and behavioural deficits in rats, and is reversed by clozapine or N-acetyl cysteine. Brain Behav Immun 30:156–167. doi:10.1016/j.bbi.2012.12.011
Filipović D, Zlatković J, Inta D et al (2011) Chronic isolation stress predisposes the frontal cortex but not the hippocampus to the potentially detrimental release of cytochrome c from mitochondria and the activation of caspase-3. J Neurosci Res 89:1461–1470. doi:10.1002/jnr.22687
Zlatković J, Todorović N, Bošković M et al (2014) Different susceptibility of prefrontal cortex and hippocampus to oxidative stress following chronic social isolation stress. Mol Cell Biochem 393:43–57. doi:10.1007/s11010-014-2045-z
Zurita A, Murúa S, Molina V (1996) An endogenous opiate mechanism seems to be involved in stress-induced anhedonia. Eur J Pharmacol 299:1–7. doi:10.1016/0014-2999(95)00754-7
Djordjevic J, Djordjevic A, Adzic M et al (2015) Alterations in the Nrf2-Keap1 signaling pathway and its downstream target genes in rat brain under stress. Brain Res 1602:20–31. doi:10.1016/j.brainres.2015.01.010
Kovacevic I, Pokrajac M, Miljkovic B et al (2006) Comparison of liquid chromatography with fluorescence detection to liquid chromatography-mass spectrometry for the determination of fluoxetine and norfluoxetine in human plasma. J Chromatogr B Analyt Technol Biomed Life Sci 830:372–376. doi:10.1016/j.jchromb.2005.11.034
Zlatković J, Todorović N, Tomanović N et al (2014) Chronic administration of fluoxetine or clozapine induces oxidative stress in rat liver: a histopathological study. Eur J Pharm Sci 59:20–30. doi:10.1016/j.ejps.2014.04.010
Dulawa SC, Holick KA, Gundersen B, Hen R (2004) Effects of chronic fluoxetine in animal models of anxiety and depression. Neuropsychopharmacology 29:1321–1330. doi:10.1038/sj.npp.1300433
Czéh B, Müller-Keuker JIH, Rygula R et al (2007) Chronic social stress inhibits cell proliferation in the adult medial prefrontal cortex: hemispheric asymmetry and reversal by fluoxetine treatment. Neuropsychopharmacology 32:1490–1503. doi:10.1038/sj.npp.1301275
Garzón J, Del Río J (1981) Hyperactivity induced in rats by long-term isolation: further studies on a new animal model for the detection of antidepressants. Eur J Pharmacol 74:287–294
Willner P, Muscat R, Papp M (1992) Chronic mild stress-induced anhedonia: a realistic animal model of depression. Neurosci Biobehav Rev 16:525–534. doi:10.1016/S0149-7634(05)80194-0
Ho Y-J, Eichendorff J, Schwarting RKW (2002) Individual response profiles of male Wistar rats in animal models for anxiety and depression. Behav Brain Res 136:1–12
Lowry OH, Rosenbrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the folin phenol reagent. J Biol Chem 193:265–275
Hissin PJ, Hilf R (1976) A fluorometric method for determination of oxidized and reduced glutathione in tissues. Anal Biochem 74:214–226
Carlberg I, Mannervik B (1985) [59] Glutathione reductase. Methods Enzymol 113:484–490. doi:10.1016/S0076-6879(85)13062-4
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249:7130–7139
Greenwald RA (1985) CRC handbook of methods for oxygen radical research. CRC Press, New York
House JS (2001) Social isolation kills, but how and why? Psychosom Med 63:273–274. doi:10.1097/00006842-200103000-00011
Fuchs E (2005) Social stress in tree shrews as an animal model of depression: an example of a behavioral model of a CNS disorder. CNS Spectr 10:182–190
Vollmayr B, Bachteler D, Vengeliene V et al (2004) Rats with congenital learned helplessness respond less to sucrose but show no deficits in activity or learning. Behav Brain Res 150:217–221. doi:10.1016/S0166-4328(03)00259-6
Cryan JF, Valentino RJ, Lucki I (2005) Assessing substrates underlying the behavioral effects of antidepressants using the modified rat forced swimming test. Neurosci Biobehav Rev 29:547–569. doi:10.1016/j.neubiorev.2005.03.008
Djordjevic J, Djordjevic A, Adzic M, Radojcic MB (2012) Effects of chronic social isolation on wistar rat behavior and brain plasticity markers. Neuropsychobiology 66:112–119. doi:10.1159/000338605
Carrier N, Kabbaj M (2012) Testosterone and imipramine have antidepressant effects in socially isolated male but not female rats. Horm Behav 61:678–685. doi:10.1016/j.yhbeh.2012.03.001
Sandi C, Richter-Levin G (2009) From high anxiety trait to depression: a neurocognitive hypothesis. Trends Neurosci 32:312–320. doi:10.1016/j.tins.2009.02.004
Dean O, Bush AI, Berk M et al (2009) Glutathione depletion in the brain disrupts short-term spatial memory in the Y-maze in rats and mice. Behav Brain Res 198:258–262. doi:10.1016/j.bbr.2008.11.017
Dringen R (2000) Metabolism and functions of glutathione in brain. Prog Neurobiol 62:649–671. doi:10.1016/S0301-0082(99)00060-X
Andreyev AY, Kushnareva YE, Starkov AA (2005) Mitochondrial metabolism of reactive oxygen species. Biochemistry 70:200–214. doi:10.1016/j.mito.2013.01.008
Singh R, Lemire J, Mailloux RJ, Appanna VD (2008) A novel strategy involved in [corrected] anti-oxidative defense: the conversion of NADH into NADPH by a metabolic network. PLoS One 3:e2682. doi:10.1371/journal.pone.0002682
Gutierrez-Correa J, Stoppani AO (1997) Inactivation of yeast glutathione reductase by Fenton systems: effect of metal chelators, catecholamines and thiol compounds. Free Radic Res 27:543–555
Ejchel-Cohen TF, Wood GE, Wang J-F et al (2006) Chronic restraint stress decreases the expression of glutathione S-transferase pi2 in the mouse hippocampus. Brain Res 1090:156–162. doi:10.1016/j.brainres.2006.03.062
Shah PJ, Ebmeier KP, Glabus MF, Goodwin GM (1998) Cortical grey matter reductions associated with treatment-resistant chronic unipolar depression. Controlled magnetic resonance imaging study. Br J Psychiatry 172:527–532. doi:10.1192/bjp.172.6.527
Heckers S, Heinsen H, Geiger B, Beckmann H (1991) Hippocampal neuron number in schizophrenia. A stereological study. Arch Gen Psychiatry 48:1002–1008. doi:10.1001/archpsyc.1991.01810350042006
Wright IC, Rabe-Hesketh S, Woodruff PWR et al (2000) Meta-analysis of regional brain volumes in Schizophrenia. Am J Psychiatry 157:16–25. doi:10.1176/ajp.157.1.16
Meister A, Anderson ME (1983) Glutathione. Annu Rev Biochem 52:711–760. doi:10.1146/annurev.bi.52.070183.003431
Galecki P, Szemraj J, Zboralski K et al (2009) Relation between functional polymorphism of catalase gene (−262C > T) and recurrent depressive disorder. Neuro Endocrinol Lett 30:357–362
Abramov AY, Scorziello A, Duchen MR (2007) Three distinct mechanisms generate oxygen free radicals in neurons and contribute to cell death during anoxia and reoxygenation. J Neurosci 27:1129–1138
Schiavone S, Sorce S, Dubois-Dauphin M et al (2009) Involvement of NOX2 in the development of behavioral and pathologic alterations in isolated rats. Biol Psychiatry 66:384–392. doi:10.1016/j.biopsych.2009.04.033
Lee AL, Ogle WO, Sapolsky RM (2002) Stress and depression: possible links to neuron death in the hippocampus. Bipolar Disord 4:117–128. doi:10.1034/j.1399-5618.2002.01144.x
Moretti M, Colla A, de Oliveira Balen G et al (2012) Ascorbic acid treatment, similarly to fluoxetine, reverses depressive-like behavior and brain oxidative damage induced by chronic unpredictable stress. J Psychiatr Res 46:331–340. doi:10.1016/j.jpsychires.2011.11.009
Chung ES, Chung YC, Bok E et al (2010) Fluoxetine prevents LPS-induced degeneration of nigral dopaminergic neurons by inhibiting microglia-mediated oxidative stress. Brain Res 1363:143–150. doi:10.1016/j.brainres.2010.09.049
Mendez-David I, Tritschler L, El Ali Z et al (2015) Nrf2-signaling and BDNF: a new target for the antidepressant-like activity of chronic fluoxetine treatment in a mouse model of anxiety/depression. Neurosci Lett 597:121–126. doi:10.1016/j.neulet.2015.04.036
Curti C, Mingatto FE, Polizello AC et al (1999) Fluoxetine interacts with the lipid bilayer of the inner membrane in isolated rat brain mitochondria, inhibiting electron transport and F1F0-ATPase activity. Mol Cell Biochem 199:103–109. doi:10.1023/A:1006912010550
Seeman P (1977) Anti-schizophrenic drugs–membrane receptor sites of action. Biochem Pharmacol 26:1741–1748. doi:10.1016/0006-2952(77)90340-9
Zafir A, Ara A, Banu N (2009) Invivo antioxidant status: a putative target of antidepressant action. Prog Neuropsychopharmacol Biol Psychiatry 33:220–228. doi:10.1016/j.pnpbp.2008.11.010
Huether G, Schuff-Werner P (1996) Platelet serotonin acts as a locally releasable antioxidant. Adv Exp Med Biol 398:299–306
Bob P, Raboch J, Maes M et al (2010) Depression, traumatic stress and interleukin-6. J Affect Disord 120:231–234. doi:10.1016/j.jad.2009.03.017
Diniz BS, Teixeira AL, Talib L et al (2010) Interleukin-1beta serum levels is increased in antidepressant-free elderly depressed patients. Am J Geriatr Psychiatry 18:172–176. doi:10.1097/JGP.0b013e3181c2947f
O’Donovan A, Hughes BM, Slavich GM et al (2010) Clinical anxiety, cortisol and interleukin-6: evidence for specificity in emotion-biology relationships. Brain Behav Immun 24:1074–1077. doi:10.1016/j.bbi.2010.03.003
Leonard B, Maes M (2012) Mechanistic explanations how cell-mediated immune activation, inflammation and oxidative and nitrosative stress pathways and their sequels and concomitants play a role in the pathophysiology of unipolar depression. Neurosci Biobehav Rev 36:764–785. doi:10.1016/j.neubiorev.2011.12.005
Engler H, Brendt P, Wischermann J et al (2017) Selective increase of cerebrospinal fluid IL-6 during experimental systemic inflammation in humans: association with depressive symptoms. Mol Psychiatry. doi:10.1038/mp.2016.264
Kubera M, Obuchowicz E, Goehler L et al (2011) In animal models, psychosocial stress-induced (neuro)inflammation, apoptosis and reduced neurogenesis are associated to the onset of depression. Prog Neuro-Psychopharmacology Biol Psychiatry 35:744–759. doi:10.1016/j.pnpbp.2010.08.026
Monje ML, Toda H, Palmer TD (2003) Inflammatory blockade restores adult hippocampal neurogenesis. Science 302:1760–1765. doi:10.1126/science.1088417
Munhoz CD, García-Bueno B, Madrigal JLM et al (2008) Stress-induced neuroinflammation: mechanisms and new pharmacological targets. Brazilian J Med Biol Res 41:1037–1046. doi:10.1590/S0100-879X2008001200001
McCusker RH, Kelley KW (2013) Immune-neural connections: how the immune system’s response to infectious agents influences behavior. J Exp Biol 216:84–98. doi:10.1242/jeb.073411
Tagliari B, Tagliari AP, Schmitz F et al (2011) Chronic variable stress alters inflammatory and cholinergic parameters in hippocampus of rats. Neurochem Res 36:487–493. doi:10.1007/s11064-010-0367-0
You Z, Luo C, Zhang W et al (2011) Pro- and anti-inflammatory cytokines expression in rat’s brain and spleen exposed to chronic mild stress: involvement in depression. Behav Brain Res 225:135–141. doi:10.1016/j.bbr.2011.07.006
Fonseka TM, McIntyre RS, Soczynska JK, Kennedy SH (2015) Novel investigational drugs targeting IL-6 signaling for the treatment of depression. Expert Opin Investig Drugs 24:459–475. doi:10.1517/13543784.2014.998334
Chourbaji S, Urani A, Inta I et al (2006) IL-6 knockout mice exhibit resistance to stress-induced development of depression-like behaviors. Neurobiol Dis 23:587–594. doi:10.1016/j.nbd.2006.05.001
Lipsky RH, Xu K, Zhu D et al (2001) Nuclear factor kappaB is a critical determinant in N-methyl-D-aspartate receptor-mediated neuroprotection. J Neurochem 78:254–264. doi:10.1046/j.1471-4159.2001.00386.x
Szasz BK, Mike A, Karoly R et al (2007) Direct inhibitory effect of fluoxetine on N-methyl-D-aspartate receptors in the central nervous system. Biol Psychiatry 62:1303–1309. doi:10.1016/j.biopsych.2007.04.014
Hashioka S, Klegeris A, Monji A et al (2007) Antidepressants inhibit interferon-gamma-induced microglial production of IL-6 and nitric oxide. Exp Neurol 206:33–42. doi:10.1016/j.expneurol.2007.03.022
Wu T-H, Lin C-H (2008) IL-6 mediated alterations on immobile behavior of rats in the forced swim test via ERK1/2 activation in specific brain regions. Behav Brain Res 193:183–191. doi:10.1016/j.bbr.2008.05.009
Hannestad J, DellaGioia N, Bloch M (2011) The effect of antidepressant medication treatment on serum levels of inflammatory cytokines: a meta-analysis. Neuropsychopharmacology 36:2452–2459. doi:10.1038/npp.2011.132
Lim C-M, Kim S-W, Park J-Y et al (2009) Fluoxetine affords robust neuroprotection in the postischemic brain via its anti-inflammatory effect. J Neurosci Res 87:1037–1045. doi:10.1002/jnr.21899
Englisch S, Inta D, Esser A, Zink M (2010) Bupropion for depression in Schizophrenia. Clin Neuropharmacol 33:257–259. doi:10.1097/WNF.0b013e3181f5a5f9
Brustolim D, Ribeiro-dos-Santos R, Kast RE et al (2006) A new chapter opens in anti-inflammatory treatments: the antidepressant bupropion lowers production of tumor necrosis factor-alpha and interferon-gamma in mice. Int Immunopharmacol 6:903–907. doi:10.1016/j.intimp.2005.12.007
Maes M, Kenis G, Kubera M et al (2005) The negative immunoregulatory effects of fluoxetine in relation to the cAMP-dependent PKA pathway. Int Immunopharmacol 5:609–618. doi:10.1016/j.intimp.2004.11.008
Riordan KJO, Huang I, Pizzi M et al (2006) Regulation of nuclear factor B in the hippocampus by group I metabotropic glutamate receptors. New York 26:4870–4879. doi:10.1523/JNEUROSCI.4527-05.2006
Inta D, Vogt MA, Pfeiffer N et al (2013) Dichotomy in the anxiolytic versus antidepressant effect of C-terminal truncation of the GluN2A subunit of NMDA receptors. Behav Brain Res 247:227–231. doi:10.1016/j.bbr.2013.03.036
Acknowledgements
This work was supported by the Grant of Ministry of Education, Science and Technological Development of the Republic of Serbia (173044) to I.P., A.S. and D.F, and Grant from the Deutsche Forschungsgemeinschaft (SFB636-TP3) to P.G. We gratefully thank the staff from Faculty of Medicine, University of Belgrade, for using Chemidoc-MP System (Bio-Rad).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interests.
Rights and permissions
About this article
Cite this article
Perić, I., Stanisavljević, A., Gass, P. et al. Fluoxetine reverses behavior changes in socially isolated rats: role of the hippocampal GSH-dependent defense system and proinflammatory cytokines. Eur Arch Psychiatry Clin Neurosci 267, 737–749 (2017). https://doi.org/10.1007/s00406-017-0807-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-017-0807-9