Abstract
Previous studies suggest an inhibitory top-down control of the amygdala by the prefrontal cortex (PFC). Both brain regions play a role in the modulation of prepulse modification (PPM) of the acoustic startle response by a pre-stimulus. Repetitive transcranial magnetic stimulation (rTMS) can modulate the activity of the PFC and might thus affect PPM. This study tested the effect of inhibitory rTMS on PPM accounting for a genetic variant of the dopamine transporter gene (DAT1). Healthy participants (N = 102) were stimulated with continuous theta burst stimulation (cTBS, an intense form of inhibitory rTMS) or sham treatment over the right PFC. Afterwards, during continuous presentation of a background white noise a louder noise burst was presented either alone (control startle) or preceded by a prepulse. Participants were genotyped for a DAT1 variable number tandem repeat (VNTR) polymorphism. Two succeeding sessions of cTBS over the right PFC (2 × 600 stimuli with a time lag of 15 min) attenuated averaged prepulse inhibition (PPI) in participants with a high resting motor threshold. An attenuation of PPI induced by prepulses with great distances to the pulse (480, 2000 ms) was observed following active cTBS in participants that were homozygous carriers of the 10-repeat-allele of the DAT1 genotype and had a high resting motor threshold. Our results confirm the importance of the prefrontal cortex for the modulation of PPM. The effects were observed in participants with a high resting motor threshold only, probably because they received a higher dose of cTBS. The effects in homozygous carriers of the DAT1 10-repeat allele confirm the relevance of dopamine for PPM. Conducting an exploratory study we decided against the use of a correction for multiple testing.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Previous studies suggest an inhibitory top-down control of emotions: Since they argue for a key role of the amygdala in emotion processing, it is hypothesized that overshooting emotions and mental disorders are the result of an insufficient inhibition of the amygdala by the prefrontal cortex (PFC) [1–3]. A promising marker of (pathological) changes within the cerebral network processing emotions and especially anxiety is the acoustic startle response [4].
The acoustic startle response is a reflex response to an alarming stimulus such as a sudden clicking sound. In humans, eyelid closure (blinking) is triggered, which can be detected by electromyography of the orbicularis oculi muscle [5]. By presenting a pre-stimulus 30–500 ms before the presentation of the stimulus, the startle response is usually attenuated (prepulse inhibition, PPI) [6–8]. PPI is considered a measure of the ability of individuals to inhibit external or internal stimuli [9] and to filter information [10]. Neuroanatomical regions involved in the modulation of PPI are amongst others localized within the amygdala, the nucleus accumbens, the hippocampus and the PFC [11, 12]. PPI has been shown to be reduced in schizophrenia [13], obsessive compulsive disorder [14], and panic disorder [15]. A larger interval between prepulse and pulse may lead to facilitation instead of inhibition of the startle response (generic term prepulse modification, PPM [16]). Few studies address the genetic underpinnings of PPM: Gajewska et al. (2013) showed a significant effect of caffeine on PPM depending on gender and the adenosine 2A receptor gene (ADORA2A) 1976T/C (rs5751876) polymorphism, a well-documented genetic risk factor in the development of anxiety disorders [16].
Just like PPM, repetitive transcranial magnetic stimulation (rTMS) has been investigated in different psychiatric disorders. Potential therapeutic effects of rTMS have amongst others been studied in depression, schizophrenia, obsessive compulsive disorders and panic disorder [17]. Repetitive Transcranial Magnetic Stimulation (rTMS) modulates cortical activity non-invasively and focally [18]. The PFC that plays a crucial role in the modulation of PPM [11] is the main target region of rTMS in psychiatric disorders [17]. Speer et al. [19] showed normalization of PFC hypoactivation in depression by the use of rTMS. Antidepressant effects were mostly achieved with either activating rTMS over the left or inhibitory rTMS over the right prefrontal cortex [20]. Huang et al. published a protocol for theta burst stimulation (TBS) as a more intense form of rTMS with extended after-effects [21]. Intermittent theta burst stimulation (iTBS) aims, such as high frequency rTMS, at activation of the stimulated regions, while continuous theta burst stimulation (cTBS) is, similar to low frequency rTMS, applied to inhibit brain activity [21]. However, some studies question this approach, e.g. a study by Hamada et al. [22]. By stimulating the primary motor cortex, they elicited the “expected” response of inhibition after cTBS and excitation after iTBS in only one quarter of participants. Almost half of the participants responded as anticipated to one but not the other stimulation technique. Beyond that, participants showed opposite reactions, for example excitation following cTBS [22].
Stimulation of the motor cortex induces a series of descending waves of corticospinal activity. The earliest wave is called D-wave, since it is assumed to be caused by direct activation of the axons of fast pyramidal tract neurones. The later waves, called I-waves, come presumably from indirect, trans-synaptic activation of pyramidal tract neurones and can be subdivided into early and late I-waves [23, 24]. The results of Hamada et al. [22] indicate that the interindividual variability of responses to TBS can partially be explained by the recruitment of late I-waves: Participants with a poor recruitment have responses that are opposite to those originally described by Huang et al. [21]. Unfortunately, a direct observation of responses is only possible for the motor cortex and not for the PFC. However, it seems likely that responses to stimulation of the PFC are as well variable between individuals which makes it important to study possible factors accounting for this variance.
To avoid side effects of too intense stimulation (e.g. epileptic seizures), in most studies and also in the present study rTMS intensity is varied depending on the individual resting motor threshold (RMT) [25]. The RMT is considered a marker of trans-synaptic excitability of cortico-spinal neurons [26]. The RMT is defined as the minimum TMS intensity that is capable to evoke a muscle contraction in the contralateral abductor pollicis brevis in at least 50% of trials starting with relaxed muscles [27, 28]. Since stimulation intensity is varied depending on RMT, participants with a higher RMT receive a more intense stimulation. If the excitability of the prefrontal cortex was exactly the same as the excitability of the primary motor cortex in every participant, this would result in comparable effects in all participants. However, the excitability of the prefrontal cortex cannot be determined and it is unknown, if it even correlates with the excitability of the motor cortex. Some indirect evidence for such a correlation comes from a study by Stokes et al. (2013) who found a correlation of RMT and phosphene threshold (lowest stimulation dose that leads to the perception of phosphenes after stimulation of the visual cortex) [25]. However, Stokes et al. (2013) emphasize the importance of scalp-cortex distance measured by structural MRI for the individual RMT which was not available in the study described here [25]. In contrast to Stokes et al. (2013), other studies did not find a correlation between RMT and phosphene threshold (e.g. [29]). If some people display significant deviations regarding the excitability of different brain areas, this may result in a too low stimulation in a subset of participants with low RMT, but high threshold for the excitation of the prefrontal cortex. Therefore, we decided to take RMT into account as a factor possibly influencing the results in this study.
Evidence about the combination of rTMS and PPI is sparse: To the best knowledge of the authors, no studies on the effects of rTMS over the prefrontal cortex on PPI in humans have been published so far. Wang et al. [30] found an impaired PPI in a rat model of posttraumatic stress disorder that could be prevented by high-frequency (excitatory) rTMS treatment.
In contrast to the effects of rTMS, the effects of psychiatric medication on PPI have been studied in humans. An attenuation of PPI by dopamine agonists is reversible by administration of dopamine antagonists in rodents and humans [31, 32]. Still, evidence for a crucial role of the dopaminergic system in PPI comes also from other studies: PPI was inversely correlated with the blink rate as a physiological marker of the dopamine tone in healthy men [33]. The neurotransmitter dopamine plays an important role in disorders displaying altered PPI [12] such as schizophrenia [34], obsessive compulsive disorder [35] and panic disorder [36]. Dopamine transporter knockout mice display reduced PPI [37].
The dopamine transporter is a membrane protein that binds dopamine and clears it from synapses after release into the extracellular space. The 3′ untranslated region variable number tandem repeat (VNTR) is a polymorphism in the dopamine transporter gene (DAT1; SLC6A3). The VNTR element is repeated between 3 and 13 times, but 9 to 10 repeats are most common [38]. The functional role of this polymorphism is not yet fully understood and results of studies have been contradictory. The majority of studies point to an association of the 9-repeat-allele with increased dopamine transporter activity in healthy participants [39] which would imply a faster clearing of dopamine from synapses (dopamine reuptake). However, heterogeneous results of studies may be caused by a more complex influence of the DAT1 genotype on dopamine transporter activity that possibly varies between brain regions, age groups and clinical pictures [39].
Homozygosity for the 10-repeat-allele has been linked to decreased thickness of the right lateral prefrontal cortex in children and adolescents with ADHD [40], lower connectivity between striatal and lateral prefrontal regions in healthy adults [41] and lower activity in the lateral prefrontal cortex during reward delivery [42]. This genotype has furthermore been implied in worse performance in several cognitive tasks, e.g. regarding working memory [43], selective attention [44] and increased sensitivity to distracting stimuli [45]. In summary, previous evidence suggests a reduction of prefrontal cortex function and top-down-control in homozygous carriers of the 10-repeat-allele leading to the hypothesis of less PPI in 10-repeat-allele homozygotes in the present study. The possibly decreased dopamine transporter activity in homozygous carriers of the 10-repeat allele points to the same direction, since the intake of dopamine agonists and a high dopamine tone have been associated with less PPI.
In the present study, applying a gene–environment (GxE) interaction approach the main and interactive effects of cTBS and DAT1 receptor gene variation on PPM in healthy participants were investigated. The aim of the study was to gain insights into the complex interaction of different factors on PPI. Given the alterations of PPI in many psychiatric disorders, a better understanding of PPI helps with the understanding of common pathomechanisms in these disorders. Insights in the mode of action of cTBS may allow for the development of more effective and specific therapeutic brain stimulation techniques.
The following hypotheses were tested. (1) CTBS over the right prefronal cortex attenuates PPI and promotes prepulse facilitation. (2) Effects of cTBS are more pronounced in participants with a higher RMT, since they received a stronger stimulation. (3) Homozygous carriers of the DAT1 10-repeat-allele display attenuated PPI and enhanced prepulse facilitation compared to carriers of the 9-repeat-allele. (4) The interaction of cTBS intervention, genotype and RMT results in an especially strong reduction of PPI and promotion of prepulse facilitation in homozygous carriers of the 10-repeat-allele with a high RMT following brain stimulation.
Materials and methods
Sample
A sample of 102 healthy participants was recruited at the Department of Psychiatry and Psychotherapy, University of Muenster, Germany, between 2011 and 2013. They had to be between 18 and 50 years of age. Exclusion criteria were current or previous diagnosis of DSM-IV axis-I disorders ruled out by the Mini-International Neuropsychiatric Interview (M.I.N.I. [46]), severe somatic disorders, high caffeine consumption (with more than three cups of coffee/tea per day [47]), alcohol consumption of more than 140 g per week, daily smoking of more than 10 cigarettes [48], illegal drug consumption, daily intake of any medication (except for hormonal contraception or thyroid hormonal substitution therapy), pregnancy, breastfeeding, history of seizures, tinnitus, history of major head trauma or of migraine, hearing loss and contraindications regarding transcranial magnetic stimulation (e.g. ferromagnetic implants). Participants were asked to abstain from caffeine and nicotine on the day of the experiment [47, 48].
The procedure was approved by the ethics committee of the medical faculty of the University of Muenster, Germany. All procedures performed were in accordance with the declaration of Helsinki. Written informed consent was obtained from all participants.
Procedure
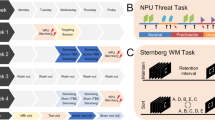
The study was conducted with a single-blind, sham-controlled and between subject design. Figure 1 gives an overview of the course of the study. After a screening interview prior to the study day, the experiment was conducted in the afternoon (duration 3.75 h). Exclusion criteria were assessed by interview and physical examination. Blood samples were collected immediately after physical examination. Self-report questionnaires measuring anxiety sensitivity, state and trait anxiety were completed, results of which are reported by [49]. Electrode position F4 (right dorsolateral prefrontal cortex, DLPFC) according to the international 10–20 system for electrode positioning [50, 51] was determined as the site of cTBS stimulation. Afterwards, cTBS was conducted (approximately 60 min after the beginning of the investigation). Subsequently, the acoustic startle response paradigms were performed. Before the prepulse modification paradigm, another acoustic startle response paradigm (duration: approximately 1 h) was run (results are reported by [49]).
Genotyping
Genomic DNA was extracted from blood samples (15 ml EDTA blood) according to the standard protocols. Genotyping of the DAT1 variable number tandem repeat (VNTR) polymorphism was performed by polymerase chain reaction (PCR) and subsequent gel electrophoresis as published previously [52].
Continuous theta burst stimulation (cTBS)
CTBS was applied with a figure-eight coil (MCF-B65, 75 mm outer diameter) by a MagVenture MagPro X100 with Option (MagVenture, Farum, Denmark). Continuous Theta Burst Stimulation (cTBS) consisted of 200 theta-bursts (5 Hz) and was continuously repeated every 200 ms for 39 s (600 pulses per session [21]). It was applied twice at 80% of the resting motor threshold within 15 min to achieve a sufficient duration of stimulation effects [53, 54]. Nyffeler et al. [53, 54] could prove that a twofold application of theta burst stimulation with a 15-min interval in between results in long-lasting effects up to several hours. Their decision to choose such an interval was based on a pre-experiment and on animal studies showing that long-term potentiation can be achieved rather with a rest period between stimulation sessions than by massed delivery [55]. During verum cTBS, the coil was held tangentially to the scalp with a 45° angle to the medial sagittal line of the skull and the handle pointing backwards. For sham stimulation, it was rotated by 90°, so the stimulation face was not in contact with the scalp [56].
Resting motor threshold (RMT)
To take into account individual differences in cortical excitability, the participants’ RMT was determined. RMT and stimulation intensity (which was always 80% of RMT) are indicated as percentages of maximum power of the stimulation device. Devices differ in their maximum power. Therefore, the percentages from this study cannot be compared to other samples investigated with a different stimulation device.
Individual RMT was determined visually by observing the reaction of the fingers of the left hand to single TMS pulses over the right primary motor cortex (‘observation of movement’ method; [57, 58]). This way of determination is easy and reliable [58, 59].
Prepulse modification paradigm (PPM)
The prepulse modification paradigm used here and the recordings of the acoustic startle response including skin preparation and electromyography recording procedures have already been described elsewhere [16, 60]. Participants were seated on a comfortable chair in a dimly lit room. They were asked to keep their gaze steady by looking at a little white fixation cross presented on a computer screen approximately one meter in front of them, to stay awake with eyes open and to sit still.
During continuous presentation of a background white noise (60 dB), a 95 dB 50 ms noise burst was presented either alone (control startle) or preceded by a prepulse (70 dB, 20 ms, instantaneous rise time) at 60, 120, 240, 480 or 2000 ms. Two additional conditions were presentation of the prepulse alone and a blank trial without acoustic stimuli exceeding the background noise. There were eight presentations per condition adding up to a total of 64 trials and a total time of about 20 min. The time between the onset of the prepulse and the onset of the startle stimulus is referred to as stimulus onset asynchrony (SOA). The percent difference between the magnitude of the startle modified by a preceding prepulse and the pulse alone trials is referred to as prepulse modification (PPM) (100 − [100 × startle magnitude of prepulse trials/magnitude of control startle trials]; [61]). A positive result of this calculation indicated an inhibition of the startle response by the prepulse (prepulse inhibition, PPI), while a negative result indicated a facilitation of the startle response by the prepulse (prepulse facilitation, PPF). The paradigm started with a 1-minute habituation phase, during which the background noise was presented alone to allow familiarization of participants with the sound. Duration of inter-trial-intervals was randomized. They lasted between 7 and 15 s.
Pre-processing of data
BrainVision Analyzer 2 (Brain Products GmbH) was used for preprocessing of electromyography data. The signals were rectified, filtered (low cut-off 28 Hz; high cut off 499 Hz; notch 50 Hz), and smoothed (time constant of 50 ms). Startle magnitude was calculated as the difference between the highest peak 21–200 ms after and the average during 50 ms before startle probe presentation. Pulse alone trials were checked for zero trials. All trials with startle stimuli were checked for artefacts. Artefacts were defined as trials in which the usual pattern of baseline and startle response could not be observed (e.g. because of excessive movement or spontaneous eye-blinks). These trials were excluded from the analysis. Startle trials with no detectable responses (<5 µV) were scored as zero. Reasons to exclude participants from analyses were too many zero trials (more than 3 standard deviations above mean number of zero trials) in the control startle trials, less than two valid startle responses in the control startle trials, too many artefacts (more than 3 standard deviations above mean number of artefacts) in all 56 trials including startle stimuli or a PPF of more than 200% during SOA trials of 60, 120, 240 or 480 ms (to prevent outlier effects) [16].
Statistical data analysis
Statistical analyses were calculated with IBM SPSS Statistics 22. To detect possible baseline differences between groups, χ 2 tests were conducted including the factors theta burst stimulation (TBS) intervention group (verum vs. sham), gender (female vs. male), DAT1 genotype (carriers of a 9-repeat allele (+9) vs. homozygous carriers of the 10-repeat-allele (10/10)) and resting motor threshold (RMT) median split (high RMT vs. low RMT according to median split). One-way analyses of variance (ANOVAs) were conducted for RMT and age with TBS intervention group, gender and genotype as between-subject factors.
The effects of blinding regarding TBS intervention were analysed using binomial tests (test proportion: 0.5) for the subjectively perceived TBS condition (verum vs. sham) in each TBS intervention group separately.
Main and interactive effects of TBS intervention group, gender, genotype and RMT median split on startle alone trials were tested by univariate ANOVA.
Analysis of prepulse modification (PPM) was conducted by mixed-design ANOVA with TBS intervention group, genotype and RMT median split as between subject factors and SOAs (prepulses at 60, 120, 240, 480 or 2000 ms) as a within-subject factor. The analysis was repeated after replacing the factor RMT median split by the factor gender, because of a slightly unequal distribution of RMT across genders (see sample characteristics). Greenhouse-Geisser correction was used if appropriate. The main and interaction effects were further explored by post hoc ANOVAs and t tests. Pearson’s correlations between RMT and PPM following SOAs 60, 120, 240, 480 and 2000 were obtained separately for four groups (actively stimulated homozygous carriers of the 10-repeat-allele, sham stimulated homozygous carriers of the 10-repeat-allele, actively stimulated carriers of the 9-repeat-allele, sham-stimulated carriers of the 9-repeat-allele). Alpha level was set to p < 0.05.
Since this study is to our knowledge the first to investigate the influence of brain stimulation on prepulse modification in humans, we decided not to apply a correction for multiple testing to minimize the risk of missing effects that might be the origin of further research (typ II error). Our decision is in accordance with the criteria for the application of a correction for multiple testing recommended by Armstrong (2014) [62].
Results
Sample characteristics
The participation of two of initially 102 recruited participants was discontinued due to pain and contractions of face muscles in one case and due to discomfort while watching anxiety relevant pictures (as part of the second experiment reported by [49]) in the other case. In one participant, analysis of prepulse modification (PPM) was impossible due to technical issues during recording. Three participants showed too many zero trials in the control startles (mean zero trials 0.96, SD: 1.67; see “Materials and methods”) and two of those also displayed less than two valid startle responses. Two participants revealed too many artefacts (> 8; mean artefact responses per participant: 2.36, SD 2.35; see “Materials and methods”) and six had a PPF of more than 200% in SOAs 60 to 480 (one of them had already been excluded for having too many zero trials). Therefore, in total 13 participants were excluded from further analyses. Seven more participants had to be excluded, because it was impossible to assign them to one of the genotype groups. Three of them displayed an atypical DAT1 VNTR length (N = 2: 11-repeat-allele; N = 1: 8-repeat allele) and in four of them either collection of the blood sample or extraction of the DNA had failed. In the remaining sample (N = 82), 50 participants were homozygous carriers of the 10-repeat-allele (10/10) and 32 were carriers of at least one 9-repeat-allele (9+).
The sample was almost equally distributed regarding gender across theta burst stimulation (TBS) intervention groups (χ 2 1 < 0.001, p = 0.991), regarding genotype across TBS intervention groups (χ 2 1 = 0.076, p = 0.782), regarding resting motor threshold (RMT) median split across TBS intervention groups (χ 2 1 = 2.46, p = 0.117), regarding gender (χ² 1 = 0.31, p = 0.580) across genotype and regarding RMT median split (χ²1 = 2.07, p = 0.150) across genotype. The distribution of gender across RMT median split was not equal (high vs. low; χ²1 = 5.06, p = 0.024), because there were more females in the low and more males in the high RMT group. One-way ANOVAs of age and RMT revealed no differences between intervention groups, gender or genotype (see Table 1). However, there was—matching the result of the χ 2-test—a significantly lower RMT in female participants.
Effectiveness of blinding
In the sham group, 30 participants thought they had been sham-stimulated while 10 assumed to have received active cTBS. 31 participants in the verum group believed they had been stimulated actively, while 11 assumed that they received sham stimulation. Participants’ estimates differed significantly from chance for both intervention groups (binomial test; sham group: p = 0.002, verum group: p = 0.003).
Control startle responses
There were no significant main effects or interactions of the factors TBS intervention group, gender, genotype or RMT median split on the control startle responses (all F ≤ 2.97, p ≥ 0.09).
Prepulse modification (PPM)
ANOVA revealed a significant main effect of SOAs (F(3,256) = 52.63, p < 0.001). Startle response was inhibited significantly stronger by prepulses at 60 and 120 ms than by prepulses at 240 and 480 ms. There were no significant differences in the extent of inhibition between 60 and 120 and neither between 240 and 480 ms. Prepulses at 2000 ms before startle let on average to a facilitation of startle response (see Fig. 2).
Impact of cTBS on PPM
There was a significance between subject interaction of TBS intervention group and RMT median split (F(1,74) = 5.67, p = 0.020). To clarify the sources of this interaction effect, we calculated a mean score of all SOAs and conducted a univariate ANOVA with the factors TBS intervention group and RMT median split which yielded a significant effect (F(1,78) = 6.05, p = 0.016). Post hoc t tests for RMT median split groups separately revealed a significant difference between TBS intervention groups in participants with a high RMT (on the level of the median or higher) only. In these participants, the mean inhibition over all SOAs and trials was significantly stronger in the sham group compared to the verum group (see Table 2; Fig. 3). Within the group with a low RMT (below the median), no difference between sham and verum group occurred for the mean of all SOAs and trials (see Table 2; Fig. 3). While the values in Table 2 suggest differential effects across SOAs between the groups, there was no significant three-way interaction TBS intervention group*RMT median split*SOAs.
Prepulse modification by SOAs 60 to 2000 after cTBS or sham stimulation for participants with a low resting motor threshold and for participants with a high resting motor threshold, respectively. cTBS continuous theta burst stimulation, low RMT resting motor threshold below the median, high RMT resting motor threshold on the level of the median or above, SOA stimulus onset asynchrony; *p < 0.05; error bars represent standard errors of the mean
Impact of cTBS on PPM depending on DAT1 genotype
There was a significant four-way-interaction TBS intervention group*RMT median split*DAT1 genotype* SOAs (F(3,256) = 5.40, p = 0.001). Post hoc ANOVAs for DAT1 genotype groups separately revealed a significant between subject interaction of TBS intervention group and RMT median split (F(1,46) = 4.55, p = 0.038) as well a three-way interaction TBS intervention groups*RMT median split*SOAs in homozygous carriers of the 10-repeat-allele only (F(4,184) = 6.12, p < 0.001). Aside from the main effect of SOAs, no main or interaction effects were observed in carriers of a 9-repeat-allele. Within homozygous carriers of the 10-repeat-allele, post hoc ANOVAs revealed a significant interaction of TBS intervention groups and SOAs in participants with a high RMT (F(4,112) = 2.91, p = 0.025) as well as in those with a low RMT (F(4,72) = 4.91, p = 0.001). T tests for SOAs 60, 120, 240, 480 and 2000 were, therefore, conducted separately for both groups. Regarding SOA 480, there was a significantly stronger prepulse inhibition in the sham group compared to the active cTBS group within homozygous carriers of the 10-repeat-allele with a high RMT (t(28) = 2.87, p = 0.008) (see Fig. 4). In homozygous carriers of the 10-repeat allele with a low RMT, there was a significant difference between sham and verum group in response to SOA 2000 (t(18) = 4.37, p < 0.001). Only the sham group displayed prepulse facilitation, while the verum group reacted with prepulse inhibition to SOA 2000 (see Fig. 4).
a Prepulse modification by SOA 480 after cTBS or sham stimulation in homozygous carriers of the 10-repeat-allele (10/10) and carriers of the 9-repeat-allele (9+) of the DAT1 VNTR. b Prepulse modification by SOA 2000 after cTBS or sham stimulation in homozygous carriers of the 10-repeat-allele (10/10) and carriers of the 9-repeat-allele (9+) of the DAT1 VNTR. cTBS continuous theta burst stimulation, DAT1 VNTR variable number repeat polymorphism of the dopamine transporter gene, low RMT resting motor threshold below the median, high RMT resting motor threshold on the level of the median or above, SOA stimulus onset asynchrony; *p < 0.05; **p < 0.01; ***p < 0.001; error bars represent standard errors of the mean
Within verum stimulated homozygous carriers of the 10-repeat-allele, a significant difference between the low RMT group and the high RMT group was found. SOAs 480 and 2000 caused prepulse inhibition in the group with a low RMT. In the group with a high RMT, a significantly minor prepulse inhibition following SOA 480 (t(23) = 2.95, p = 0.007) and prepulse facilitation following SOA 2000 were observed (t(23) = 3.19, p = 0.004; see Fig. 4).
Direct comparison of the genotype groups revealed a significant difference within participants from the verum group with a low RMT: They displayed prepulse facilitation following SOA 2000, if they were carriers of a 9-repeat-allele, but prepulse inhibition, if they were homozygous carriers of the 10-repeat-allele (t(21) = 2.21, p = 0.038) (see Fig. 4).
No other main or interaction effects of TBS intervention group, RMT median split and genotype on SOAs were observed.
Effects of gender
There were no main or interaction effects including the factor gender (all F ≤ 0.71, p ≥ 0.559).
Correlations
In homozygous carriers of the 10-repeat-allele who had been stimulated with active cTBS, there was a significant negative correlation between PPM following SOA 480 and RMT (r(23) = −0.568, p = 0.003) as well as between PPM following SOA 2000 and RMT (r(23) = −0.443, p = 0.027). There were no significant correlations of PPM and RMT in homozygous carriers of the 10-repeat-allele who had been sham stimulated. There were no significant correlations of PPM and RMT in carriers of the 9-repeat allele. PPM following SOAs 60, 120 and 240 and RMT were correlated in none of the groups.
Discussion
In the present study, we investigated the impact of continuous theta burst stimulation (cTBS) as an innovative, intense form of inhibitory brain stimulation on prepulse modification (PPM). PPM is altered in a number of psychiatric disorders [12]. Since PPM is known to be influenced by the brain dopamine system, the influence of a variable number tandem repeat (VNTR) polymorphism in the dopamine receptor (DAT1) gene was investigated. Participants’ resting motor threshold (RMT) was included as an additional factor.
Mean PPM was significantly lower (higher remaining startle response following prepulses) due to less inhibition and more facilitation in the active cTBS group compared to the sham group in participants with a high RMT (on the level of or above the median). DAT1 genotypes did not differ regarding PPM. However, the DAT1 genotype modulated the interaction of RMT and cTBS stimulation group on PPM by prepulses with long distances to the pulse (480 and 2000 ms). None of the investigated parameters had an effect on the control startle response, confirming that differences between groups were caused by modulation of PPM and not of startle response.
The significantly higher remaining mean startle response after prepulses in actively cTBS stimulated participants is in line with our first hypothesis. However, the effect was limited to those with a high RMT. We assume that an inhibition of prefrontal cortex function by cTBS interferes with prepulse inhibition and makes prepulse facilitation more likely. Our results confirm that the prefrontal cortex plays an important role in the modulation of PPM and thereby in the pre-attentive filtering of information (sensorimotor gating) [63]. It suits the results of a previous animal study by Wang et al. [30] who successfully worked against impaired prepulse inhibition with high-frequency rTMS, the effect of which is opposed to the effect of cTBS. Another way to influence PPM that should be considered by future studies might be stimulation of the medial prefrontal cortex. Rats selectively bred for deficient prepulse inhibition displayed reduced neuronal activity in the medial prefrontal cortex [64]. A hypoactivation or lesion of the medial prefrontal cortex and attenuation of prepulse inhibition were also associated with each other in a number of other animal studies (for review see [11]).
Our results suggest an influence of brain stimulation on sensorimotor gating. Since sensorimotor gating is altered in different psychiatric disorders, our results support the idea of brain stimulation as a potential therapeutic option in various psychiatric disorders by influencing common psychopathological patterns.
In line with our second hypothesis, the stimulation effect was present only in participants with a high RMT. These participants received a higher dose of cTBS, since this dose was determined individually for every participant depending on his or her RMT. Possibly, the dose that participants with a low RMT received was not sufficient to influence prepulse inhibition. Future studies will nevertheless have to rely on RMT for the determination of stimulation intensity to allow for a safe stimulation. Possibly, the determination of RMT by the “observation of movement” method was not exact enough, leading to an underestimation of RMT in some participants that then received a lower stimulation intensity than the intensity that would have been suitable for them. Future studies should consider using other methods to determine RMT, e.g. by measuring electromyographic response that is more objective, because it does not depend on the observer [59]. In addition, if MRI is available, the scalp-cortex distance that may differ between primary motor cortex and target region should be taken into account for the determination of stimulation intensity [25]. In any case, future studies should include RMT as a factor to find out, if it influences the results in terms of a stronger effect (or effects only) in participants that are stimulated more intensely.
In contrast to our third hypothesis, there was no significant difference regarding PPM between DAT1 genotypes. However, in accordance with our fourth hypothesis, DAT1 genotype modulated the interaction of RMT and cTBS stimulation group on PPM: Homozygous carriers of the 10-repeat-allele with a high RMT displayed less inhibition after active cTBS following SOAs with long latencies (SOA 480 and 2000). The observed negative correlations of PPM following SOAs 480 and 2000 with RMT in actively stimulated homozygous carriers of the 10-repeat-allele suggest a dose-dependent effect of cTBS: The stronger the stimulation, the smaller was the extent of startle inhibition provoked by these prepulses. Homozygous carriers of the 10-repeat-allele have been characterized by alterations of prefrontal cortex function under certain circumstances [40–42] and worse performance in cognitive tasks [43–45]. Therefore, their prefrontal cortex may be especially prone to an additional loss of function after inhibitory stimulation in terms of a smaller reserve capacity. Only the prepulses 480 and 2000 may be affected, because longer intervals between pulse and prepulse tend to evoke facilitation instead of inhibition anyway [16], a trend that was apparently reinforced by the stimulation.
In addition, we observed a significant difference regarding SOA 2000 between verum and sham group in participants with a low RMT and two DAT1 10-repeat-alleles due to inhibition in the verum and facilitation in the sham group. In this regard, homozygous carriers of the 10-repeat-allele differed also significantly from carriers of the 9-repeat-allele who displayed prepulse facilitation in the low RMT group following verum stimulation. These results are hard to interpret. Since they were related to SOA 2000 only and group sizes in the post hoc analyses were small, this may also be a random effect. A speculative explanation would be that the effect of cTBS goes into reverse in homozygous carriers of the 10-repeat-allele with a low RMT and promotes prepulse inhibition instead of facilitation. A recent study by Hamada et al. [22] demonstrated that the response of individuals to TBS is highly variable. CTBS can have inhibitory or facilitatory effects on the excitability of the stimulated area. Differences in RMT and in genotype might influence the individual probability to react with inhibition or facilitation to a certain stimulation technique. However, Hamada et al. [22] found no influence of thresholds (like RMT) on TBS effects. Future studies should investigate the genetic influences on response to TBS also for the motor cortex.
Dopamine is an important neurotransmitter within the primary motor cortex [65]. Therefore, one could have expected that the DAT1 genotype groups would differ in their cortical excitability. However, there was no difference in RMT. This result matches the results of Meintzschel and Ziemann [66] who reported neither the dopamine agonist Cabergoline nor the dopamine antagonist Haloperidol to influence RMT. Future studies should, therefore, consider the importance of other neurotransmitter systems for RMT.
The present study has some limitations: Blinding was not successful, since correct guesses of intervention differed significantly from chance in both the active cTBS and the sham group. Some actively stimulated participants complained about unpleasant sensations at the site of stimulation or twitching of facial muscles which was not the case in sham-stimulated participants who had of course also been informed about these possible effects. This may explain our result. Although other studies achieved successful blinding using the same method [67], placebo effects cannot be ruled out. However, intentional processes seem not to have an important role in influencing startle response [68, 69] and thereby in its modification by prepulses. That is why we do not assume placebo effects to have had a crucial impact on our results.
The PPM paradigm was started approximately 1 h after cTBS stimulation which may have resulted in weaker stimulation effects compared to a performance of the paradigm directly after stimulation. However, two succeeding sessions of cTBS, as were applied in this study, have been shown to be capable to alter brain activity for up to several hours [53, 54].
While for this study a between subjects study design was chosen, amongst other reasons because of the potentially long lasting effects of cTBS and the noticeable differences between verum and sham stimulation, a within-subject design (verum and sham stimulation of each participant in randomized order) would have enlarged statistical power and reduced the impact of inter-individual differences on the results.
Another important limitation regards RMT. Differences between participants with a low and those with a high RMT may have partly been caused by cortical excitability and not exclusively by the stimulation dose. Although the comparison with the sham group allows for the conclusion that cortical excitability was not the main factor influencing PPM in this study, it may have modulated the stimulation effect. Additional parameters that were not measured in this study (e.g. intracortical inhibition, intracortical facilitation, cortical silent period [70]) would have allowed for a more exact determination of cortical excitability than RMT alone. Besides, RMT was only determined once in the beginning of the study. Even though changes in RMT by stimulation of another target region have to our knowledge never been described, we cannot exclude that RMT was changed by stimulation. At least, after stimulation of the primary motor cortex a change in excitability of the contralateral motor cortex has been observed [71].
Reduced PPI has been described in relatives of patients with schizophrenia [72]. Since participants in our study were not asked, if they had first-degree relatives with a psychiatric disorder, this has to be taken into account as another limitation.
Summarizing our results, two succeeding sessions of cTBS over the right dorsolateral prefrontal cortex were capable of attenuating prepulse inhibition and promoting prepulse facilitation, though only in participants that presented with a high RMT and, therefore, received a higher dose of cTBS. An attenuation of prepulse inhibition by prepulses with long distances to the pulse (480, 2000 ms) was observed in homozygous carriers of the 10-repeat-allele of the DAT1 VNTR with a high RMT only.
References
Hariri AR, Mattay VS, Tessitore A, Fera F, Weinberger DR (2003) Neocortical modulation of the amygdala response to fearful stimuli. Biol Psychiatry 53:494–501
Etkin A, Wager TD (2007) Functional neuroimaging of anxiety: a meta-analysis of emotional processing in PTSD, social anxiety disorder, and specific phobia. Am J Psychiatry 164:1476–1488
Eden AS, Schreiber J, Anwander A, Keuper K, Laeger I, Zwanzger P, Zwitserlood P et al (2015) Emotion regulation and trait anxiety are predicted by the microstructure of fibers between amygdala and prefrontal cortex. J Neurosci 35:6020–6027
Davis M, Walker DL, Lee Y (1997) Amygdala and bed nucleus of the stria terminalis: differential roles in fear and anxiety measured with the acoustic startle reflex. Philos Trans R Soc Lond B Biol Sci 352:1675–1687
Berg K, Balaban MT (2008) Startle elicitation: stimulus parameters, recording techniques, and quantification. In: Dawson ME, Schell AM, Bohmelt AH (ed) Startle modification: implications for neuroscience, cognitive science, and clinical science, 2nd edn. Cambridge University Press, Cambridge, pp 21–50
Graham FK, Putnam LE, Leavitt LA (1975) Lead-stimulation effects of human cardiac orienting and blink reflexes. J Exp Psychol Hum Percept Perform 104:175–182
Hoffman HS, Ison JR (1980) Reflex modification in the domain of startle: I. Some empirical findings and their implications for how the nervous system processes sensory input. Psychol Rev 87:175–189
Ison JR, Hoffman HS (1983) Reflex modification in the domain of startle: II. The anomalous history of a robust and ubiquitous phenomenon. Psychol Bull 94:3–17
Ludewig S (2003) Die Panikstörung: kognitive Theorien und der akustische Schreckreflex. Schweizer Archiv für Neurologie und Psychiatrie 154:440–444
Braff DL, Geyer MA, Swerdlow NR (2001) Human studies of prepulse inhibition of startle: normal subjects, patient groups, and pharmacological studies. Psychopharmacology (Berl) 156:234–258
Swerdlow NR, Weber M, Qu Y, Light GA, Braff DL (2008) Realistic expectations of prepulse inhibition in translational models for schizophrenia research. Psychopharmacology (Berl) 199:331–388.
Kohl S, Heekeren K, Klosterkotter J, Kuhn J (2013) Prepulse inhibition in psychiatric disorders—apart from schizophrenia. J Psychiatr Res 47:445–452
Meincke U, Mörth D, Voß T, Thelen B, Geyer MA, Gouzoulis–Mayfrank E (2004) Prepulse inhibition of the acoustically evoked startle reflex in patients with an acute schizophrenic psychosis—a longitudinal study. Eur Arch Psychiatry Clin Neurosci 254:415–421
Ahmari SE, Risbrough VB, Geyer MA, Simpson HB (2012) Impaired sensorimotor gating in unmedicated adults with obsessive-compulsive disorder. Neuropsychopharmacology 37:1216–1223
Ludewig S, Geyer MA, Ramseier M, Vollenweider FX, Rechsteiner E, Cattapan-Ludewig K (2005) Information-processing deficits and cognitive dysfunction in panic disorder. J Psychiatry Neurosci 30:37–43
Gajewska A, Blumenthal TD, Winter B, Herrmann MJ, Conzelmann A, Muhlberger A, Warrings B et al (2013) Effects of ADORA2A gene variation and caffeine on prepulse inhibition: a multi-level risk model of anxiety. Prog Neuropsychopharmacol Biol Psychiatry 40:115–121
Lefaucheur JP, Andre-Obadia N, Antal A, Ayache SS, Baeken C, Benninger DH, Cantello RM et al (2014) Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clin Neurophysiol 125:2150–2206
Wassermann EM, Zimmermann T (2012) Transcranial magnetic brain stimulation: therapeutic promises and scientific gaps. Pharmacol Ther 133:98–107
Speer AM, Kimbrell TA, Wassermann EM, D Repella J, Willis MW, Herscovitch P, Post RM (2000) Opposite effects of high and low frequency rTMS on regional brain activity in depressed patients. Biol Psychiatry 48:1133–1141
Garcia-Toro M, Salva J, Daumal J, Andres J, Romera M, Lafau O, Echevarria M et al (2006) High (20-Hz) and low (1-Hz) frequency transcranial magnetic stimulation as adjuvant treatment in medication-resistant depression. Psychiatry Res 146:53–57
Huang YZ, Edwards MJ, Rounis E, Bhatia KP, Rothwell JC (2005) Theta burst stimulation of the human motor cortex. Neuron 45:201–206
Hamada M, Murase N, Hasan A, Balaratnam M, Rothwell JC (2013) The role of interneuron networks in driving human motor cortical plasticity. Cereb Cortex 23:1593–1605
Di Lazzaro V, Rothwell JC (2014) Corticospinal activity evoked and modulated by non-invasive stimulation of the intact human motor cortex. J Physiol (Lond) 592:4115–4128.
Suppa A, Huang Y, Funke K, Ridding M, Cheeran B, Di Lazzaro V, Ziemann U et al (2016) Ten years of theta burst stimulation in humans: established knowledge, unknowns and prospects. Brain stimulation 9:323–335
Stokes MG, Barker AT, Dervinis M, Verbruggen F, Maizey L, Adams RC, Chambers CD (2013) Biophysical determinants of transcranial magnetic stimulation: effects of excitability and depth of targeted area. J Neurophysiol 109:437–44
Brigo F, Storti M, Benedetti MD, Rossini F, Nardone R, Tezzon F, Fiaschi A et al (2012) Resting motor threshold in idiopathic generalized epilepsies: a systematic review with meta-analysis. Epilepsy Res 101:3–13
Rossini PM, Barker A, Berardelli A, Caramia M, Caruso G, Cracco R, Dimitrijević M et al (1994) Non-invasive electrical and magnetic stimulation of the brain, spinal cord and roots: basic principles and procedures for routine clinical application. Report of an IFCN committee. Electroencephalogr Clin Neurophysiol 91:79–92
Herbsman T, Forster L, Molnar C, Dougherty R, Christie D, Koola J, Ramsey D et al (2009) Motor threshold in transcranial magnetic stimulation: the impact of white matter fiber orientation and skull-to-cortex distance. Hum Brain Mapp 30:2044–2055
Gerwig M, Kastrup O, Meyer B, Niehaus L (2003) Evaluation of cortical excitability by motor and phosphene thresholds in transcranial magnetic stimulation. J Neurol Sci 215:75–78
Wang HN, Bai YH, Chen YC, Zhang RG, Wang HH, Zhang YH, Gan JL et al (2015) Repetitive transcranial magnetic stimulation ameliorates anxiety-like behavior and impaired sensorimotor gating in a rat model of post-traumatic stress disorder. PMC Biophys 10:e0117189
Abduljawad KA, Langley RW, Bradshaw CM, Szabadi E (1999) Effects of bromocriptine and haloperidol on prepulse inhibition: comparison of the acoustic startle eyeblink response and the N1/P2 auditory-evoked response in man. J Psychopharmacol 13:3–9
Andersen MP, Pouzet B (2001) Effects of acute versus chronic treatment with typical or atypical antipsychotics on d-amphetamine-induced sensorimotor gating deficits in rats. Psychopharmacology (Berl) 156:291–304
Swerdlow NR, Wasserman LC, Talledo JA, Casas R, Bruins P, Stephany NL (2003) Prestimulus modification of the startle reflex: relationship to personality and physiological markers of dopamine function. Biol Psychol 62:17–26
Pratt J (2015) Schizophrenia in the 21st century: new insights and translation into improved therapies. J Psychopharmacol 29:83–84
Pauls DL, Abramovitch A, Rauch SL, Geller DA (2014) Obsessive-compulsive disorder: an integrative genetic and neurobiological perspective. Nat Rev Neurosci 15:410–424
Maron E, Nutt DJ, Kuikka J, Tiihonen J (2010) Dopamine transporter binding in females with panic disorder may vary with clinical status. J Psychiatr Res 44:56–59
Fox MA, Panessiti MG, Hall FS, Uhl GR, Murphy DL (2013) An evaluation of the serotonin system and perseverative, compulsive, stereotypical, and hyperactive behaviors in dopamine transporter (DAT) knockout mice. Psychopharmacology (Berl) 227:685–695
Bannon MJ, Michelhaugh SK, Wang J, Sacchetti P (2001) The human dopamine transporter gene: gene organization, transcriptional regulation, and potential involvement in neuropsychiatric disorders. Eur Neuropsychopharmacol 11:449–455
Faraone SV, Spencer TJ, Madras BK, Zhang-James Y, Biederman J (2014) Functional effects of dopamine transporter gene genotypes on in vivo dopamine transporter functioning: a meta-analysis. Mol Psychiatry 19:880–889
Fernandez-Jaen A, Lopez-Martin S, Albert J, Fernandez-Mayoralas DM, Fernandez-Perrone AL, de La Pena MJ, Calleja-Perez B et al (2015) Cortical thickness differences in the prefrontal cortex in children and adolescents with ADHD in relation to dopamine transporter (DAT1) genotype. Psychiatry Res 233:409–417
Gordon EM, Devaney JM, Bean S, Vaidya CJ (2015) Resting-state striato-frontal functional connectivity is sensitive to DAT1 genotype and predicts executive function. Cereb Cortex 25:336–345
Dreher JC, Kohn P, Kolachana B, Weinberger DR, Berman KF (2009) Variation in dopamine genes influences responsivity of the human reward system. Proc Natl Acad Sci USA 106:617–622. doi:10.1073/pnas.0805517106
Brehmer Y, Westerberg H, Bellander M, Furth D, Karlsson S, Backman L (2009) Working memory plasticity modulated by dopamine transporter genotype. Neurosci Lett 467:117–120
Caldu X, Vendrell P, Bartres-Faz D, Clemente I, Bargallo N, Jurado MA, Serra-Grabulosa JM et al (2007) Impact of the COMT Val108/158 Met and DAT genotypes on prefrontal function in healthy subjects. Neuroimage 37:1437–1444
Newman DP, Cummins TD, Tong JH, Johnson BP, Pickering H, Fanning P, Wagner J et al (2014) Dopamine transporter genotype is associated with a lateralized resistance to distraction during attention selection. J Neurosci 34:15743–15750
Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E, Hergueta T et al (1998) The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59(Suppl 20):22–33 (quiz 34–57)
Andrews SE, Blumenthal TD, Flaten MA (1998) Effects of caffeine and caffeine-associated stimuli on the human startle eyeblink reflex. Pharmacol Biochem Behav 59:39–44
Duncan E, Madonick S, Chakravorty S, Parwani A, Szilagyi S, Efferen T, Gonzenbach S et al (2001) Effects of smoking on acoustic startle and prepulse inhibition in humans. Psychopharmacology (Berl) 156:266–272
Vennewald N, Winter B, Limburg K, Diemer J, Notzon S, Fohrbeck I, Arolt V et al (2016) Emotional processing and rTMS: does inhibitory theta burst stimulation affect the human startle reflex?. J Neural Transm (Vienna) 123:1121–1131
Jasper HH (1958) The ten twenty electrode system of the international federation. Electroencephalogr Clin Neurophysiol 10:371–375
Herwig U, Satrapi P, Schonfeldt-Lecuona C (2003) Using the international 10–20 EEG system for positioning of transcranial magnetic stimulation. Brain Topogr 16:95–99
Hunnerkopf R, Strobel A, Gutknecht L, Brocke B, Lesch KP (2007) Interaction between BDNF Val66Met and dopamine transporter gene variation influences anxiety-related traits. Neuropsychopharmacology 32:2552–2560
Nyffeler T, Wurtz P, Luscher HR, Hess CW, Senn W, Pflugshaupt T, von Wartburg R et al (2006) Extending lifetime of plastic changes in the human brain. Eur J Neurosci 24:2961–2966
Nyffeler T, Cazzoli D, Hess CW, Muri RM (2009) One session of repeated parietal theta burst stimulation trains induces long-lasting improvement of visual neglect. Stroke 40:2791–2796
Abraham WC, Logan B, Greenwood JM, Dragunow M (2002) Induction and experience-dependent consolidation of stable long-term potentiation lasting months in the hippocampus. J Neurosci 22:9626–9634
Lisanby SH, Gutman D, Luber B, Schroeder C, Sackeim HA (2001) Sham TMS: intracerebral measurement of the induced electrical field and the induction of motor-evoked potentials. Biol Psychiatry 49:460–463
Pridmore S, Fernandes Filho JA, Nahas Z, Liberatos C, George MS (1998) Motor threshold in transcranial magnetic stimulation: a comparison of a neurophysiological method and a visualization of movement method. J ECT 14:25–27
Varnava A, Stokes MG, Chambers CD (2011) Reliability of the ‘observation of movement’ method for determining motor threshold using transcranial magnetic stimulation. J Neurosci Methods 201:327–332
Rossi S, Hallett M, Rossini PM, Pascual-Leone A, Safety of TMS Consensus Group (2009) Safety, ethical considerations, and application guidelines for the use of transcranial magnetic stimulation in clinical practice and research. Clin Neurophysiol 120:2008–2039
Domschke K, Gajewska A, Winter B, Herrmann MJ, Warrings B, Mühlberger A, Wosnitza K et al (2012) ADORA2A gene variation, caffeine, and emotional processing: a multi-level interaction on startle reflex. Neuropsychopharmacology 37:759–769
Blumenthal TD, Cuthbert BN, Filion DL, Hackley S, Lipp OV, van Boxtel A (2005) Committee report: guidelines for human startle eyeblink electromyographic studies. Psychophysiology 42:1–15
Armstrong RA (2014) When to use the Bonferroni correction. Ophthalmic Physiol Optics 34:502–508
Geyer MA (2006) The family of sensorimotor gating disorders: comorbidities or diagnostic overlaps? Neurotox Res 10:211–220
Alam M, Angelov S, Stemmler M, von Wrangel C, Krauss JK, Schwabe K (2015) Neuronal activity of the prefrontal cortex is reduced in rats selectively bred for deficient sensorimotor gating. Prog Neuropsychopharmacol Biol Psychiatry 56:174–184
Hosp JA, Luft AR (2013) Dopaminergic meso-cortical projections to M1: role in motor learning and motor cortex plasticity. Front Neurol 4:145
Meintzschel F, Ziemann U (2006) Modification of practice-dependent plasticity in human motor cortex by neuromodulators. Cereb Cortex 16:1106–1115
Notzon S, Deppermann S, Fallgatter A, Diemer J, Kroczek A, Domschke K, Zwanzger P et al (2015) Psychophysiological effects of an iTBS modulated virtual reality challenge including participants with spider phobia. Biol Psychol 112:66–76
Grillon C, Baas J (2003) A review of the modulation of the startle reflex by affective states and its application in psychiatry. Clin Neurophysiol 114:1557–1579
Grillon C (2008) Models and mechanisms of anxiety: evidence from startle studies. Psychopharmacology (Berl) 199:421–437.
Lefaucheur J (2005) Motor cortex dysfunction revealed by cortical excitability studies in Parkinson’s disease: influence of antiparkinsonian treatment and cortical stimulation. Clin Neurophysiol 116:244–253
Suppa A, Ortu E, Zafar N, Deriu F, Paulus W, Berardelli A, Rothwell JC (2008) Theta burst stimulation induces after-effects on contralateral primary motor cortex excitability in humans. J Physiol 586:4489–4500
Cadenhead KS, Swerdlow NR, Shafer KM, Diaz M, Braff DL (2000) Modulation of the startle response and startle laterality in relatives of schizophrenic patients and in subjects with schizotypal personality disorder: evidence of inhibitory deficits. Am J Psychiatry 157:1660–1668
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
The study has been approved by the ethics committee of the medical faculty of the University of Muenster, Germany, and has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All participants gave their informed consent prior to their inclusion in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This work was supported by the fund “Innovative Medical Research” of the University of Muenster Medical School (project ZW 211105), and the SFB-TRR58, project C02 (Deutsche Forschungsgemeinschaft, DFG).
Additional information
S. Notzon and N. Vennewald contributed equally to this work and should therefore both be considered first authors.
Rights and permissions
About this article
Cite this article
Notzon, S., Vennewald, N., Gajewska, A. et al. Is prepulse modification altered by continuous theta burst stimulation? DAT1 genotype and motor threshold interact on prepulse modification following brain stimulation. Eur Arch Psychiatry Clin Neurosci 267, 767–779 (2017). https://doi.org/10.1007/s00406-017-0786-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-017-0786-x