Abstract
Background
Otosclerosis is a primary osteodystrophy of the otic capsule that causes stapedo-vestibular ankylosis. Its diagnosis is suspected on the basis of clinical and audiometric elements, basically in the presence of conductive hearing loss with a normal eardrum. The CT-scan is an essential examination for the preoperative evaluation of otosclerosis. The aim of our study was to evaluate the use of CT-scanning in predicting the functional outcome of otosclerosis surgery by correlating postoperative audiometric results and preoperative CT findings.
Methods
We conducted a retrospective study at the ENT Department in association with the Medical Imaging Department of our hospital, over a period of 8 years, from January 2014 to December 2022 and involving 90 patients (104 ears).
Results
The average age of our patients was 40 years with extremes ranging from 22 to 61 years. We noted a sex ratio of 0.38. The preoperative CT-scan showed signs of otosclerosis in 87% of the cases and infra-radiological forms in 13% of the cases. Veillon stage II was the most frequent radiological stage encountered with a percentage of 48%. A good audiometric evolution, defined by a closure of postoperative Air Bone Gap (ABG ≤ 20 dB) and by an improvement of Bone Conduction (BC gain ≥ 0), was recorded in 86 cases (82.7%) for ABG and in 84 cases (80.8%) for BC gain. Scanographic predictive factors of poor postoperative outcome for ABG and BC gain were: advanced stages (Veillon stage III and IV), endosteal effraction, and round window involvement. According to multivariate analysis, only the extent of otosclerotic foci was directly and independently associated with the postoperative audiometric outcome.
Conclusion
The CT-scan is an essential examination in the preoperative evaluation of otosclerosis. It allows a positive diagnosis to be made and evaluate the extension of otosclerosis. Moreover, thanks to the analysis of the extent of the otosclerosis foci, mainly by the Veillon classification, the CT-scan allows to predict the postoperative audiometric prognosis.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Otosclerosis is a primary osteodystrophy of the peri-labyrinthine bone responsible for progressive blockage of the stapedial plate in the oval window, resulting in vestibulo-stapedial ankylosis [1].
In most cases, the diagnosis of otosclerosis is based on clinical and audiometric findings in the presence of conductive hearing loss with a normal eardrum, and is confirmed by middle ear surgery [2].
Computed tomography (CT) is the radiological examination of choice for preoperative evaluation of otosclerosis. It confirms the diagnosis in cases of doubt and determines the preoperative stage of the disease by studying the extent of the otosclerosis focus.
Several factors can influence the outcome of functional stapedial surgery. It is therefore essential to study these prognostic factors and to inform patients about the objectives, modalities, and predicted risks of this surgery.
The aims of this study were to determine the value of CT-scans in predicting functional results of otosclerosis surgery and to investigate the association between stage (or radiological appearance) and postoperative audiometric results.
Materials and methods
This is a retrospective study conducted at the ENT Department in association with the Medical Imaging Department of our hospital, over a period of 8 years, from January 2014 to December 2022 and covering 90 patients (104 ears).
We included in this study patients with unilateral or bilateral otosclerosis operated on and confirmed intraoperatively, having a preoperative CT-scan of the temporal bone, a preoperative and postoperative audiometric assessment performed between 6 weeks and 1 year.
The positive diagnosis of otosclerosis on imaging was based on the visualisation of labyrinthine hypodensity and the detection of a plate with a thickness greater than or equal to 0.7 mm. The presence or absence of an endosteal effraction, the existence of involvement of the round window, and the Veillon scanographic stage were specified. The scan report also specified the existence of an anatomical variant, such as procidence of the facial nerve, narrowness of the oval window according to the Ukkola–Pons method, a short BDE, and the persistence of a stapedial artery.
The following parameters were studied according to the recommendations of the American Academy of Otolaryngology-Head and Neck Surgery "AAO-HNS" [3] with rounding of the mean to the nearest whole number.
-
Mean air conduction threshold (AC).
-
Mean bone conduction threshold (BC).
-
Postoperative ABG (ABG) (postoperative AC–postoperative BC).
-
BC gain (Preoperative BC–postoperative BC).
The functional success criteria considered in the study were
-
A postoperative ABG at one year ABG ≤ 20 dB.
-
A mean postoperative BC gain ≥ 0.
We investigated the influence of preoperative prognostic factors on postoperative functional outcome. These factors were identified by preoperative imaging and were: The radiological stage according to the Veillon classification, which distinguishes infra-radiological forms (Stage 0), localized forms (Stages I and II) and extensive forms (Stages III and IV), endosteal invasion, and involvement of the round window.
The Chi-square test was used to determine whether there was an association between two qualitative variables. If the Chi-square test was not significant or not valid, Fisher’s exact test was used. For the multivariate study, binary logistic regression was used to determine the independent factors and the odds ratio.
Results
The age group most affected in our study was between 30 and 50 years. The average age of our patients was 40 years with extremes ranging from 22 to 61 years. The sex ratio was 0.38. The dominant functional sign, reported by all our patients, was hearing loss.
Pure-tone audiometry showed conductive hearing loss in 83 ears (80%) and mixed hearing loss in 21 ears (20%). The stapedial reflex was absent in all ears tested. The tympanogram was normal type A in 97 ears.
CT-scans, performed preoperatively in all our patients, showed signs of otosclerosis in 87% of cases and infra-radiological forms in 13% of cases. Veillon stage II was the radiological stage most frequently encountered, with a percentage of 48% (Table 1) (Figs. 1, 2).
A Stage III otosclerosis: CT-scan of the left temporal bone in axial section, showing a prestapedial hypodensity in contact with the outer wall of the cochlea (yellow star) and surrounding the recess of the oval window (red arrow). B Stage IVa focal otosclerosis: CT-scan of the left temporal bone in axial section showing a single hypodensity in front of the cochlea (red arrow) associated with a prespace hypodensity with cochlear contact (blue star). C Stage IVa continuous otosclerosis: CT-scan of the right temporal bone in axial section showing a peri cochlear hypodense arciform focus (blue arrow) with an internal premeatic location (red arrow)
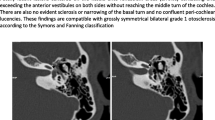
Involvement of the round window was found in 7 ears (6.7%). Endosteal effraction was found in 8 ears (7.7%) (Fig. 3).
Otosclerosis with involvement of the round window: CT-scan of the right temporal bone in axial section (a and b) showing hypodensity on the lateral side (white arrow) and circumferential hypodensities on the medial and lateral margins (Hexagon). Note the presence of an endosteal effraction (red arrow). 3’: Otosclerosis with obliterative involvement of the round window. Axial CT-scan section of the left temporal bone with evidence of hypodensity completely filling the round window (blue arrow). Endosteal effraction is associated
In the study of peroperative difficulties: Facial nerve procidence was found in 18 ears and was associated with dehiscence in 5 cases. No cases of persistent stapedial artery or short descending branch of the incus were reported. A narrow oval window was diagnosed in 6 operated ears. Procidence of the jugular gulf was present in 10 ears.
In the study of differential diagnoses: No cases of tympanosclerosis, ossicular fixation, Minor's syndrome, or dilatation of the posterior vestibular aqueduct were noted. There was one case of osteogenesis imperfecta associated with bilateral otosclerosis.
Surgery was bilateral in 16% of cases and unilateral in 84%. The surgical technique most commonly used was calibrated platinotomy, which was performed in 86 of the 104 ears operated on. The piston was made of Teflon in all our patients, with a diameter of 0.6 mm in 88 cases and a length of 4.5 mm in 80 cases.
A platinum fracture leading to hemiplatinectomy was observed in 12 cases. A floating plate, which was successfully removed, was noted in two cases.
Intraoperative procidence of the facial nerve was observed in 16 cases, of which only 8 were identified on the CT-scan. Dehiscence of the facial nerve canal was noted in two patients. In our study, a narrow oval window intraoperatively was noted in 6 of the 104 ears operated (in 5.7% of cases), of which only 2 were noted on the radiological report.
The majority of our patients progressed well, with a 74% subjective improvement in hearing. The main immediate postoperative complication was the onset of vertigo in 22.1% of cases.
Postoperative pure-tone audiometry was performed in all patients included in this study and postoperative ABG and BC gain were the main measures used to assess functional success in our patients.
Good audiometric progression, defined by ABG closure (ABG ≤ 20 dB) and BC improvement (BC gain ≥ 0), was recorded in 86 cases (82.7%) for ABG and in 84 cases (80.8%) for BC gain.
Postoperative failure due to both ABG opening and deterioration in BC was noted in 11 operated ears, i.e., 10.6% of cases.
According to the univariate analysis, the localized forms of otosclerosis corresponding to Veillon stages I and II (68.3%) were associated with a better rate of postoperative ABG closure and improvement in postoperative BC compared with the extensive forms represented by stages III and IV (18.3% of cases) with P < 0.001 in both cases (Tables 2 and 3).
Multivariate analysis (Tables 4, 5, 8) showed that this was indeed an independent factor with a significant and direct influence on the postoperative audiometric result. Extensive involvement of the otosclerosis (Stages III and IV) multiplies the risk of having an open ABG (ABG > 20) by 9.03 [2.16–37.21] and the risk of having a deterioration in postoperative BC (gain in BC < 0) by 11.91 [2.8–49.6].
Patients with subradiological stages (Stage 0, normal CT) were not significantly associated with better postoperative audiometric results compared with those with positive CT (Tables 2 and 3).
Involvement of the round window and endosteal effraction significantly influenced postoperative audiometric results (Tables 6 and 7). Indeed, they were associated with higher rates of postoperative BC impairment and ABG non-closure. However, on multivariate analysis, these two factors could not be considered independent predictors of postoperative failure. Preoperative and postoperative audiograms were compared for all our patients (Fig. 4).
Discussion
In our study, localized forms of otosclerosis (stages I and II) were associated with better postoperative ABG closure and greater postoperative BC improvement than extensive forms (stages III and IV), with a statistically significant relationship (P < 0.001). Logistic regression identified this factor as an independent factor, significantly influencing both:
-
Postoperative ABG with an adjusted odds ratio (OR) of 9.032, 95% confidence interval (CI): [2.16–37.21].
-
The gain in BC with an adjusted odds ratio (OR) of 11.91, 95% confidence interval (CI): [2.8–49.6].
Conversely, patients with subradiological stages (Stage 0, normal CT) were not significantly associated with better postoperative outcomes compared with those with positive CT (Stages I, II, III, and IV).
This association remains controversial in the literature. Indeed, Halily [4] in a recent study of 108 cases published in 2022 demonstrated that the opening of the ABG and deterioration in BC were significantly associated with advanced forms of the disease (Stages III and IV). Karakus [5], in a study published in 2021 involving 37 cases, demonstrated an association between the degree of extent of otosclerosis foci and postoperative audiometric results. Patients with localized stages of otosclerosis had better postoperative ABG closure, whereas BC gain was not influenced by this factor. Sbaihi [6], in a recent study of 54 ears operated on, also confirmed that localized involvement was associated with a better rate of ABG closure and improvement in BC gain. Conversely, the association between the extent of otosclerosis foci and postoperative functional outcome was not statistically significant for the two parameters studied according to the literature [7, 8]. For infra-radiological forms, Karakus [5] showed that Veillon stage 0 was associated with better ABG closure rates (P = 0.002). However, BC gain was not influenced by this factor. Marx [9] found that patients with infra-radiological otosclerosis (Veillon stage 0) had better results in terms of ABG closure (P = 0.02) than those with a positive CT-scan. However, he found no significant difference in the mean postoperative BC threshold between the two groups. Vartiainen [10], in his study of 43 patients, found no significant difference in BC gain between patients with infra-radiological forms and those with a positive CT-scan. This may be explained by the fact that in some cases, the infra-radiological forms correspond to the final and most advanced histopathological stage of the disease [11, 12]. However, this stage remains undetectable on the CT-scan, as it is difficult to differentiate them from the normal otic capsule. It is for this reason that some authors have studied the value of measuring bone density on CT, particularly in the fissula ante fenestram, which showed reduced values compared with those in the otic capsule, which is taken as a reference [13]. According to Grayeli [14], a density in the fissula ante fenestram < 2022 HU was correlated with a hearing loss in AC and BC. Therefore, it seems to be recommended to measure the Hounsfield Units of typical otosclerosis points on the CT-scan to improve its capacity to evaluate cochlear endosteal involvement.
With regard to the factor "Involvement of the round window", our study did not allow it to be retained as an independent factor influencing postoperative audiometric results. This was explained by some authors by the fact that damage of the round window is rarely isolated. It is often associated with more advanced stages of the disease. Shin [15] found 14 cases of round window involvement in his study; 8 of these 14 ears presented with extensive involvement, which in turn were associated with a poor postoperative audiometric result. In our case series, 7 cases of round window involvement were diagnosed and all were associated with advanced stages (III or IV) of Veillon. Schuknecht [11] in a series of 118 ears with clinical otosclerosis did not find a statistically significant relationship between the involvement of the round window, which was present in 9 cases (7%), and the threshold values of the postoperative BC. This involvement was associated with other otosclerosis foci in the otic capsule in all 9 cases. Paradoxically, Mansour [16], in a study of 930 ears in which a round window was involved in 121 cases (13%), found a statistically significant association between involvement of the RW and alteration of postoperative BC and the opening of the ABG. He showed that as the grade of involvement of the round window increases, the postoperative results become less satisfactory, with average audiometric results in the case of a circumferential focus (Mansour stage III) and a high postoperative failure rate in the case of complete obliteration (Mansour stage IV), sometimes leading to surgery being contraindicated [17].
We also showed that the group with an endosteal effraction had greater BC degradation and higher postoperative ABG values. This difference was statistically significant according to univariate analysis (P < 0.05). However, logistic regression did not identify this factor as an independent factor impacting postoperative audiometric prognosis. This subject remains controversial in the literature: Shin [15] highlighted 14 cases of endosteal effraction among the 437 ears studied. He showed a statistically significant difference in ABG and BC gain between the group with and without endocystectomy. Our findings are in line with those published by Sbaihi [6] who found a statistically significant correlation on univariate analysis between endosteal effraction and deterioration of postoperative audiometric thresholds for ABG and BC gain without being able to define this factor as an independent factor of poor postoperative outcome based on logistic regression.
Based on the results of this study and the most frequently encountered radiological errors encountered, we propose the following reading grid in order to optimize the interpretation of CT scans of the temporal bone performed in cases of clinical suspicion otosclerosis (Table 8).
Conclusion
A CT-scan is an essential examination in cases of otosclerosis. It allows a positive diagnosis to be made, evaluate the extension of the otosclerosis and difficulties in surgery to be predicted. In addition, by analysing the extent of otosclerosis foci, principally using the Veillon classification, CT can predict the postoperative audiometric prognosis.
References
Purohit B, Hermans R, Op de Beeck K (2014) Imaging in otosclerosis: a pictorial review. Insights Imaging 5(2):245–252
Thomassin JM, Collin M, Bailhache A, Dessi P, Rodriguez F, Varoquaux A (2010) Otospongiose. EMC - Oto-Rhino-Laryngol 5(2):1–15
Committee on Hearing and Equilibrium (1995) Committee on hearing and equilibrium guidelines for the evaluation of results of treatment of conductive hearing loss∗. Otolaryngol Neck Surg 113(3):186–187
Halily S, Abdulhakeem B, Oukessou Y, Rouadi S, Abada R, Roubal M et al (2022) CT scan findings impact on hearing thresholds in otosclerosis: A study of 108 patients. Ann Med Surg 77:103716
Karakus M, Colak M, Ozcan K, Ikinciogullari A, Ensari S, Dere H (2021) Postoperative audiometric results of patients with otosclerosis in relation with high-resolution computed tomography and intraoperative macroscopic findings. J Coll Phys Surg Pak 31(08):969–974
Sbaihi S, Kharrat G, Lagha M, Sammoud S, Bouzaidi K (2022) Facteurs scannographiques influençant les résultats audiométriques post opératoires dans l’otospongiose. J Tun ORL 47(3):1–7
Kanzaki S, Kanzaki J, Ogawa K (2021) Surgical treatment of otosclerosis using a unique stapes prosthesis without a hook. Acta Otolaryngol (Stockh) 141(1):10–13
Maaloul I, Souissi B, Achour I, Kharrat I, Haddar S, Mahfoudh KB et al (2018) Corrélation audiométrie-radiologie dans l’otospongiose. J Tun Orl 13:5
Marx M, Lagleyre S, Escudé B, Demeslay J, Elhadi T, Deguine O et al (2011) Correlations between CT scan findings and hearing thresholds in otosclerosis. Acta Otolaryngol (Stockh) 131(4):351–357
Vartiainen E, Saari T (1993) Value of computed tomography (CT) in the diagnosis of cochlear otosclerosis. Clin Otolaryngol Allied Sci 18(6):462–464
Schuknecht HF, Barber W (1985) Histologic variants in otosclerosis. Laryngoscope 95(11):1307–1317
Quesnel AM, Ishai R, McKenna MJ (2018) Otosclerosis: temporal bone pathology. Otolaryngol Clin North Am 51(2):291–303
Tringali S, Pouget JF, Bertholon P, Dubreuil C, Martin C (2007) Value of temporal bone density measurements in otosclerosis patients with normal-appearing computed tomographic scan. Ann Otol Rhinol Laryngol 116(3):195–198
Grayeli AB, Yrieix CS, Imauchi Y, Cyna-gorse F, Ferrary E, Sterkers O (2004) Temporal bone density measurements using CT in otosclerosis. Acta Otolaryngol (Stockh) 124(10):1136–1140
Shin YJ, Fraysse B, Deguine O, Cognard C, Charlet JP, Sévely A (2001) Sensorineural hearing loss and otosclerosis: a clinical and radiologic survey of 437 cases. Acta Otolaryngol (Stockh) 121(2):200–204
Mansour S, Nicolas K, Ahmad HH (2011) Round window otosclerosis: radiologic classification and clinical correlations. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol. 32(3):384–392
Veillon F, Stierle JL, Dussaix J, Ramos-Taboada L, Riehm S (2006) Imagerie de l’otospongiose : confrontation clinique et imagerie. J Radiol 87(11 Part 2):1756–1764
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
This is a retrospective study which does not pose any ethical problem.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bouatay, R., Benelhaj, C., Saad, J. et al. Interest of computer tomography in the study of prognostic factors of otosclerosis. Eur Arch Otorhinolaryngol 281, 4113–4119 (2024). https://doi.org/10.1007/s00405-024-08585-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-024-08585-1