Abstract
Purpose
The aim of this study is to analyze the efficacy of a new modified pharyngoplasty technique with barbed sutures: barbed suspension pharyngoplasty (BSP).
Methods
We enrolled patients affected by obstructive sleep apnea–hypopnea syndrome (OSAHS), having the main site of obstruction at the palatal and lateral pharyngeal walls, who refused or failed to tolerate CPAP therapy and underwent non-resective pharyngoplasty with barbed sutures between January 2014 and October 2017. Two surgical techniques with barbed sutures were used: barbed reposition pharyngoplasty (BRP) and BSP; the main characteristics of the latter are a double passage of the needle, each side, through the soft palate.
Results
Forty-two patients met the study inclusion criteria and were included in the analysis. Twenty-two patients underwent BRP and 20 BSP. Patients treated with both BRP and BSP achieved significant improvement in polysomnographic parameters: AHI, ODI, t90%, and daily sleepiness tested by the ESS questionnaire (p < 0.001). There were no significant differences between groups considering gender, age, or severity of OSAHS (p > 0.05). Outcomes were also comparable (p = 0.10) in the two groups; patients who underwent BSP had successful treatment in 100% of cases, compared to 86% with BRP, with a cure rate of 40% vs. 18%.
Conclusions
BSP is a novel surgical technique that is effective in treating oropharyngeal collapse and can be tailored for patients with high collapsibility of the soft palate who might benefit from the palatal stiffness given by multiple passages of the suture inside it.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea–hypopnea syndrome (OSAHS) is a common health problem affecting a large number of individuals. The overall prevalence ranges from 9 to 38% with an Apnea–Hypopnea Index (AHI) more than 5, being higher in men [1]. Several degrees and patterns of collapse of the upper airway during sleep have been described in patients affected by OSAHS. In our study, attention is mainly focused on soft palatal collapse which is considered the most common site causing OSAHS and snoring [2, 3].
As outlined by NICE guidelines, CPAP remains the treatment of choice for moderate–severe OSAHS, although the compliance rate can be poor. In selected patients, who are not compliant to CPAP therapy, and whose main site of obstruction, evaluated during drug-induced sleep endoscopy, is palatal or lateral pharyngeal wall (LPW) collapse, surgical management with pharyngoplasty techniques can be offered. The main aim of this type of surgery is to improve upper airway dimensions by reducing soft-tissue collapsibility with the goal to be curative, or at least to improve compliance to CPAP therapy [4].
The recent evolutions regarding techniques of pharyngoplasty aimed to obtain the expansion and stabilization of the pharyngeal airspace through the conservative treatment of LPW collapse rather than through ablation of excess pharyngeal soft tissue [5].
The role of LPW collapse in the pathogenesis of OSAHS has been demonstrated by Schwab et al. [6]. LPW collapse should be noted and documented, as it plays a significant role in the pathogenesis of OSAHS. The first surgical technique aimed at stabilizing the lateral wall was lateral pharyngoplasty, described by Cahali in 2003; this procedure was not widely used, as it involves a marked modification of the lateral wall with sectioning of the superior pharyngeal constrictor muscle and a significant risk of important complications, including postoperative dysphagia [7, 8].
On the other hand, expansion sphincter pharyngoplasty (ESP), described by Pang and Woodson in 2007, had greater agreement. It originated from the technique of sphincter pharyngoplasty, described for the correction of palatal incompetence with the medial rotation of the palatal pharyngeal muscle, restricting the velopharyngeal isthmus [8, 9]. This technique was improved by Sorrenti by giving tension on the lateral wall and fixing the palatopharyngeal muscle to the palatine musculature, close to the pterygoid hamulus, allowing advancement of the soft palate more effectively and less invasively than the previous techniques of lateral pharyngoplasty [5].
Among non-resective pharyngoplasty, barbed reposition pharyngoplasty (BRP) and the Roman blind techniques (RBT) have recently been described in the literature. These procedures allow surgeons to achieve widening and stiffening of the naso-pharyngeal inlet without any tissue sacrifice using a bidirectional-barbed suture that is inserted through the fibro-muscular tissues of the soft palate and posterior tonsillar pillars, and tightened around three steady holds: the posterior nasal spine and the two pterygoid hamulii lateral to the pterygomandibuar raphe [10, 11].
The aim of the study is to analyze the efficacy of a new modified non-resective pharyngoplasty technique with the objective to give more tension and displace the soft palate anteriorly and lateralize the lateral pharyngeal wall.
Methods
Study design and population
An observational retrospective study was carried analyzing the records of 42 consecutive patients with OSAHS who refused or failed to tolerate CPAP and underwent non-resective pharyngoplasty with barbed sutures between January 2014 and October 2017 at our Institution.
Surgical planning
Preoperative assessment included polysomnography (PSG), endoscopic evaluation, sleep history assessment including the Epworth sleepiness scale (ESS) [12, 13] and drug-induced sleep endoscopy (DISE) evaluated using the NOHL classification [14].
Inclusion criteria were as follows: diagnosis of mild-to-severe OSAHS (AHI ≥ 5) with body mass index (BMI) ≤ 35, having the main site of obstruction at the oropharyngeal level, as palatal either LPW collapse, according to NOHL classification [14], who failure to tolerate or comply with CPAP or a mandibular advancement device (MAD) and who were treated with non-resective pharyngoplasty with barbed sutures. We excluded patients with hypopharyngeal or laryngeal complete collapse, or significant craniofacial anomalies affecting the airway, severe comorbidities, contraindications for surgery, and those with incomplete clinical data. All patients underwent a PSG at least six months postoperatively.
Surgical procedures
All patients underwent non-resective antero-lateral pharyngoplasty with barbed sutures (Stratafix™ Spiral PDO 2.0 SH, 26 mm, 1/2 Circle Taper Point, SXPD2B414, Ethicon), whose aim was to displace anteriorly and stiffen the soft palate to increase the retrovelar space and to reduce its collapsibility, as it is the main site of obstruction in this selected cohort of patients.
The entire cohort was divided into two groups: group A with 22 patients treated between 2014 and 2016 and group B with 20 patients treated in 2017. The first 22 patients (group A) underwent a BRP (BRP) according to Vicini et al. [10], while for the last 20 patients (group B), we introduced some surgical steps to increase palatal tension given by the cicatricial fibrosis and to augment the antero-lateral suspension forces to the soft palate (Fig. 1), calling this barbed suspension pharyngoplasty (BSP).
The surgical technique of the BSP (Fig. 2a, b) encompasses these surgical steps:
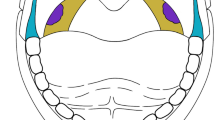
Surgical drawings illustrating the planning of suture route on the right side in BSP (a, b), symmetric procedures are performed on the left side. a, posterior nasal spine; b, upper part of tonsillectomy bed; c, palatopharyngeal muscle; d, right pterygomandibular raphe; e, base of the uvula; f, left pterygomandibular raphe; blue lines represent the pterygomandibular raphes
-
1.
Oropharyngeal exposure is achieved by a Boyle–Davis mouth gag (Fig. 3a), and a mucosectomy of tonsillar bed is performed; if tonsils are present, a bilateral tonsillectomy is done. It is mandatory to spare the palatoglossus and palatophayngeous muscles and the mucosal layer covering both pillars [10];
-
2.
Using bidirectional barbed sutures PDO 2.0, the first stitch is from the midline, at the level of the posterior nasal spine (a) antero-laterally towards the upper part of tonsillectomy bed (b), usually in two passages re-introducing the needle close to point of exit (Fig. 2a);
-
3.
Multiple stitches (from 2 to 4 passages) are placed around the upper portion of palatopharyngeal muscle (c), anchoring it to the anterior pillar (Fig. 2a);
-
4.
A suspension stitch is made by passing the needle into the pterygomandibular raphe (d) and applying traction without needing to make knots (Fig. 2a);
-
5.
Further stitches are made in the palatal muscles through the base of the uvula (e) to the contralateral pterygomandibular raphe (f) and going back through the midline to the ipsilateral pterygomandibular raphe (g, d), and finally cutting the suture (h) (Figs. 2b, 3b, 4 and Supplementary Video).
A simultaneous multilevel procedure was chosen if nasal obstruction was significant, also performing turbinoplasty and/or septoplasty.
Outcome evaluation
Surgical success was evaluated at least 6 months after surgery, performing PSG and repeating the ESS questionnaire [12]. Criteria for evaluation of outcomes, in agreement with Montevecchi et al. [15], are reported in Table 1.
Statistical analysis
Categorical variables were described as absolute and relative frequencies; standard descriptive statistics were used expressing medians, first and third quartiles of quantitative variables. The Shapiro–Wilk normality test was applied and the Wilcoxon signed-rank test for matched samples was chosen to compare pre- and posttreatment values of variables of interest. Groups’ comparison analysis was performed by Fisher’s exact test, Chi-square test, or Mann–Whitney test, as appropriate.
GraphPad Prism Version 6.0 (San Diego, CA, USA) and IBM SPSS Statistics version 24.0 were used for statistical analysis and graph drawing. For all tests, a two-tailed p value < 0.05 was considered significant.
Results
Patients and treatments
Forty-two patients met the study inclusion criteria and were included in the analysis. The median age was 54 years and the cohort was composed of 38 men (90%) and 4 women (10%). Eight patients (19%) were affected by mild OSAHS, 19 (45%) by moderate and 15 (35%) by severe OSAHS. Twenty-two (52%) patients underwent BRP and 20 (48%) BSP. Given the presence of nasal obstruction, a multilevel surgical procedure with nasal surgery was chosen for 35 patients (84%) by performing turbinoplasty in 12 (29%) and both septoplasty and turbinoplasty in 23 cases (55%). Categorical data and summary statistics are reported in Table 2.
Postoperative course
The median hospital stay was 2 days (range 1–4 days); complications related to the surgical procedures encompassed one case of hemorrhage from tonsillar bed on 11th postoperative day managed by medical therapy, two cases of temporary velopharyngeal insufficiency, spontaneously solved before the discharge, and five cases of minimal partial thread extrusion (four cases among BRP group and one case among BSP one), treated by its cutting at outpatient clinic.
Improvement in polysomnographic parameters
Non-resective pharyngoplasty with barbed sutures (BRP or BSP) in a uni-level or multilevel setting led to significant improvement of all polysomnographic parameters and of the daily sleepiness as assessed by the ESS questionnaire (p < 0.001). In particular, the surgical procedure achieved a significant reduction of AHI (p < 0.001), Oxygen Desaturation Index (ODI) (p < 0.001), and t90% (p < 0.001), as shown in Table 3. Successful treatment was achieved in 39 patients (93%) with a cure rate of 29%, while three patients (7%) experienced treatment failure. Among the two groups, there were no significant differences regarding gender, age, severity of OSAHS, or multilevel surgery (p > 0.05). Outcomes were also comparable (p = 0.10). Patients who underwent BSP had successful treatment in 100% of cases with a cure rate of 40%.
Discussion
Since the introduction of non-resective pharyngoplasty techniques, as expansion sphincter pharyngoplasty or a decrease in surgical complications and improvement of success has been observed [8, 16].
In our experience, treatment of oropharyngeal and palatal collapse with non-resective barbed pharyngoplasty (BRP or BSP) is effective, with significant improvement of objective parameters such as AHI and ODI (p < 0.001) and with significant reduction of daily sleepiness evaluated by the ESS questionnaire (p < 0.001).
The use of barbed sutures in pharyngeal surgery is described in many techniques such as Roman blinds pharyngoplasty [11], barbed reposition pharyngoplasty [10], and barbed expansion pharyngoplasty [17]. This type of suture seems to reduce invasiveness and operating times without the need of making knots inside the oral cavity and oropharynx [16].
Our results using the BRP succeeded in getting comparable results obtained by other authors [15] in terms of cure rate (18% vs. 20.7%, respectively) and failures (14% vs. 27%, respectively), confirming the good reproducibility and efficacy of this technique. In addition, complications of our procedures were similar to other studies (bleeding events < 5%, partial thread extrusion 11%) [15, 17]
In BSP technique, suture passage directly from the posterior nasal spine towards the tonsillar fossa seems to increase the anterior displacement of the soft palate, as shown in Fig. 1, by the sum of the main vector forces (p + r) applied to the soft palate and lateral pharyngeal wall. This suggests that the technique will be especially useful if soft palate collapse is observed during preoperative DISE.
In our opinion, the multiple passages through the soft palate, used in the BSP technique, reinforce the stiffness of the palate that can be attributed to the cicatricial fibrosis, thereby reducing its collapsibility, which is one of the main causes of obstructive apnea in these patients [14]. By introducing the BSP, although statistical significance was not reached, we saw a trend of increasing cure rate vs. BRP (40% vs. 18%) with no treatment failures.
Our preliminary and encouraging data about this novel surgical technique should be confirmed in wider, as well as multicentric and randomized series of patients. The small sample size should be considered one of the main limits of our study, whereas the lacking of randomization has been overcome by the temporal criteria selection, so being the two groups comparable.
Conclusion
Although CPAP therapy remains the gold standard for treatment of patients affected by moderate–severe OSAHS, in our experience, BSP is a safe and effective surgical technique, with a high success rate, to correct lateral pharyngeal wall and palatal collapse in patients refusing or not tolerating CPAP.
References
Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC, Hamilton GS, Dharmage SC (2017) Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 34:70–81. https://doi.org/10.1016/j.smrv.2016.07.002
Eichler C, Sommer JU, Stuck BA, Hormann K, Maurer JT (2013) Does drug-induced sleep endoscopy change the treatment concept of patients with snoring and obstructive sleep apnea? Sleep Breath 17(1):63–68. https://doi.org/10.1007/s11325-012-0647-9
Vroegop AV, Vanderveken OM, Boudewyns AN, Scholman J, Saldien V, Wouters K, Braem MJ, Van de Heyning PH, Hamans E (2014) Drug-induced sleep endoscopy in sleep-disordered breathing: report on 1249 cases. Laryngoscope 124(3):797–802. https://doi.org/10.1002/lary.24479
Sethukumar P, Kotecha B (2018) Tailoring surgical interventions to treat obstructive sleep apnoea: one size does not fit all. Breathe (Sheff) 14(3):e84–e93. https://doi.org/10.1183/20734735.020118
Sorrenti G, Piccin O (2013) Functional expansion pharyngoplasty in the treatment of obstructive sleep apnea. Laryngoscope 123(11):2905–2908. https://doi.org/10.1002/lary.23911
Schwab RJ, Pack AI, Gupta KB, Metzger LJ, Oh E, Getsy JE, Hoffman EA, Gefter WB (1996) Upper airway and soft tissue structural changes induced by CPAP in normal subjects. Am J Respir Crit Care Med 154(4 Pt 1):1106–1116. https://doi.org/10.1164/ajrccm.154.4.8887615
Cahali MB (2003) Lateral pharyngoplasty: a new treatment for obstructive sleep apnea hypopnea syndrome. Laryngoscope 113(11):1961–1968
Pang KP, Woodson BT (2007) Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck Surg 137(1):110–114. https://doi.org/10.1016/j.otohns.2007.03.014
Woodson BT, Wooten MR (1994) Manometric and endoscopic localization of airway obstruction after uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg 111(1):38–43. https://doi.org/10.1177/019459989411100109
Vicini C, Hendawy E, Campanini A, Eesa M, Bahgat A, AlGhamdi S, Meccariello G, DeVito A, Montevecchi F, Mantovani M (2015) Barbed reposition pharyngoplasty (BRP) for OSAHS: a feasibility, safety, efficacy and teachability pilot study. "We are on the giant's shoulders". Eur Arch Otorhinolaryngol 272(10):3065–3070. https://doi.org/10.1007/s00405-015-3628-3
Mantovani M, Minetti A, Torretta S, Pincherle A, Tassone G, Pignataro L (2012) The velo-uvulo-pharyngeal lift or "roman blinds" technique for treatment of snoring: a preliminary report. Acta Otorhinolaryngol Ital 32(1):48–53
Vignatelli L, Plazzi G, Barbato A, Ferini-Strambi L, Manni R, Pompei F, D'Alessandro R, Ginsen (2003) Italian version of the Epworth sleepiness scale: external validity. Neurol Sci 23(6):295–300. https://doi.org/10.1007/s100720300004
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Vicini C, De Vito A, Benazzo M, Frassineti S, Campanini A, Frasconi P, Mira E (2012) The nose oropharynx hypopharynx and larynx (NOHL) classification: a new system of diagnostic standardized examination for OSAHS patients. Eur Arch Otorhinolaryngol 269(4):1297–1300. https://doi.org/10.1007/s00405-012-1965-z
Montevecchi F, Meccariello G, Firinu E, Rashwan MS, Arigliani M, De Benedetto M, Palumbo A, Bahgat Y, Bahgat A, Lugo Saldana R, Marzetti A, Pignataro L, Mantovani M, Rinaldi V, Carrasco M, Freire F, Delgado I, Salamanca F, Bianchi A, Onerci M, Agostini P, Romano L, Benazzo M, Baptista P, Salzano F, Dallan I, Nuzzo S, Vicini C (2017) Prospective multicentre study on barbed reposition pharyngoplasty standing alone or as a part of multilevel surgery for sleep apnoea. Clin Otolaryngol. https://doi.org/10.1111/coa.13001
Rashwan MS, Montevecchi F, Cammaroto G, Badr El Deen M, Iskander N, El Hennawi D, El Tabbakh M, Meccariello G, Gobbi R, Stomeo F, Vicini C (2017) Evolution of soft palate surgery techniques for obstructive sleep apnea patients: a comparative study for single-level palatal surgeries. Clin Otolaryngol. https://doi.org/10.1111/coa.13027
Pianta L, Bertazzoni G, Morello R, Perotti P, Nicolai P (2018) Barbed expansion sphincter pharyngoplasty for the treatment of oropharyngeal collapse in obstructive sleep apnoea syndrome: a retrospective study on 17 patients. Clin Otolaryngol 43(2):696–700. https://doi.org/10.1111/coa.13008
Funding
None of the authors have any commercial interest in the subject of this study or received any financial or material support for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research did not involve any animal models; the research involved human participants in accordance with the ethical standards of the institutional and/or national research committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards; and informed consent was obtained from all individual participants included in the study. Ethical review and approval was not required for this study in accordance with the national and institutional requirements (Ethics committee IRCCS Ospedale Policlinico San Martino, Genoa). However, all patients preoperatively signed a consent form for disclosure of privacy in managing personal data for scientific purposes.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary file1 (MOV 37446 kb)
Rights and permissions
About this article
Cite this article
Barbieri, M., Missale, F., Incandela, F. et al. Barbed suspension pharyngoplasty for treatment of lateral pharyngeal wall and palatal collapse in patients affected by OSAHS. Eur Arch Otorhinolaryngol 276, 1829–1835 (2019). https://doi.org/10.1007/s00405-019-05426-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-019-05426-4