Abstract
Introduction
The optimal lower-limb alignment after unicompartmental knee arthroplasty (UKA) remains controversial. This study aimed to investigate the optimal lower-limb alignment for functional improvement in the early post-UKA period. We hypothesized that a small change (Δ) in the arithmetic hip-knee-ankle (aHKA) angle during surgery would result in better postoperative knee function.
Materials and methods
This single-centered, retrospective study analyzed 91 patients (91 knees) who underwent UKA from April 2021 and December 2022. Preoperative and postoperative standing whole-leg radiographs were used to evaluate the mechanical HKA angle and aHKA angle. The aHKA angle was calculated from the medial proximal tibial angle (MPTA) and lateral distal femoral angle (LDFA). We defined restored aHKA angle as a postoperative aHKA angle within ± 3° of the preoperative aHKA angle. Functional improvement was evaluated using the preoperative and one-year postoperative Knee Society Scoring 2011 (KSS 2011). A multivariate regression analysis was performed to investigate the optimal lower-limb alignment for functional improvement.
Result
Postoperative restored aHKA angle (p = 0.020) was the only significant factor for improved KSS 2011 scores. Postoperative restored aHKA angle was obtained in 64 patients (70%). ΔMPTA (p < 0.001) and ΔLDFA (p = 0.037) were significant factors associated with a postoperative restored aHKA angle.
Conclusions
UKA restores the native knee, including resurfacing constitutional alignment and medial collateral ligament tension. Minimal change in the aHKA angle during UKA improves the functional outcomes of the knee during the early postoperative period, consistent with the minimally invasive surgical concept of UKA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Unicompartmental knee arthroplasty (UKA) is an established treatment for patients with unicompartmental knee osteoarthritis (OA) [1,2,3,4]. The clinical outcomes of UKA have improved with advances in prostheses and instrumentation [1], a better understanding of knee kinematics [2], and strict patient selection [3, 4]. In recent years, UKA indications have expanded, and more patients have been selected for this procedure owing to reports of good clinical outcomes in patients with obesity, as well as young and highly active patients [5,6,7,8,9].
UKA is minimally invasive and preserves the cruciate ligaments and lateral femorotibial compartment, allowing for earlier functional recovery than total knee arthroplasty [10,11,12]. However, the optimal alignment for knee arthroplasty remains controversial. Mechanical alignment is the traditional and most popular method with a neutral hip-knee-ankle (HKA) angle [13]. However, in recent years, there has been a paradigm shift to kinematic alignment in total knee arthroplasty, with native articular surface orientation and restoration of the physiological soft tissue knee balance [14]. Therefore, some have attempted to adopt this alignment method for UKA [15]. The arithmetic HKA (aHKA) angle is calculated from the preoperative medial proximal tibial angle (MPTA) and lateral distal femoral angle (LDFA) and is often set as a target value for postoperative alignment [16]. UKA restores the native knee, including resurfacing constitutional alignment and medial collateral ligament tension [17,18,19].
Minimal changes in the joint line (preoperative to postoperative restoration) may contribute to postoperative knee joint function, but no studies have explored this. Therefore, this study investigated the optimal lower-limb alignment for functional improvement in the early post-UKA period. We hypothesized that a small change in the aHKA angle during surgery would result in better postoperative knee function.
Methods
Patient selection
This case series has an evidence level of 4. Consecutive patients who underwent cemented fixed-bearing UKA (Unicompartmental Persona® partial knee and Zimmer Uni®; Zimmer Biomet, Warsaw, IN, USA) for knee OA with a varus deformity were included between April 2021 and December 2022. All of the surgeries were performed by two experienced surgeons at a single center. The surgical indication for medial UKA was symptomatic isolated anteromedial compartment OA with a correctable varus deformity of < 10° and a flexion contracture of < 10° [20]. Patients who underwent bilateral UKA or had a history of neuromuscular disease, postoperative complications (infection, periprosthetic fracture), medical complications (e.g., stroke) and significantly decreased levels of activities of daily living or symptomatic contralateral knee or ipsilateral hip OA were excluded.
All patients were Japanese. Furthermore, all provided informed consent before participation, and the local institutional review board for clinical research (No. 2020–204) approved this retrospective study, which was performed following the Declaration of Helsinki.
Radiological and clinical evaluations
Radiological parameters were routinely evaluated in all patients using whole-leg anteroposterior (AP) standing radiographs and AP and lateral knee radiographs preoperatively and one year postoperatively. The HKA angle, MPTA, and LDFA were measured using whole-leg radiographs (Fig. 1). The HKA angle was the angle between the mechanical axis of the femur and tibia. The MPTA was the angle between the mechanical axis of the tibia and the tibial joint line. LDFA was the angle between the mechanical axis of the femur and the femoral joint line. Following a previous study, the LDFA was subtracted from the MPTA to calculate the aHKA angle [20, 21]. Component alignments were evaluated as the coronal femoral component angle (c-FCA), coronal tibial component angle (c-TCA), sagittal femoral component angle (s-FCA), and sagittal tibial component angle (s-TCA) using postoperative AP and lateral knee radiographs, following a previous study [21] (Fig. 2). All patients were routinely evaluated for patient-reported outcome measures (PROMs) using the Knee Society Scoring 2011 (KSS 2011) preoperatively and one year postoperatively.
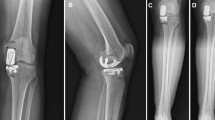
Radiographic measurements of component alignment. c-FCA and c-TCA are measured on anteroposterior knee radiographs and s-FCA and s-TCA on ateral knee radiographs. c-FCA, coronal femoral component angle; c-TCA, coronal tibial component angle; s-FCA, sagittal femoral component angle; s-TCA, sagittal tibial component angle
Data analyses
Continuous variables are presented as means ± standard deviations. A multivariate regression analysis was performed to investigate the optimal lower limb alignment for functional improvement (i.e., postoperative – preoperative KSS 2011 score). Lower limb alignment was defined based on the following reference values and included in a multivariable model:
-
1)
Preoperative “moderate” or “severe” varus mechanical HKA (mHKA) angle deformity [22]: “moderate”: 0°< mHKA angle < 10°; “severe”: mHKA angle > 10°.
-
2)
Postoperative “neutral” or “varus” mHKA angle alignment [15]: “varus”: mHKA angle > 3°; “neutral”: 0°< mHKA angle < 3°.
-
3)
Preoperative or postoperative aHKA phenotype [20, 23]: “varus”: aHKA angle <–2°; “neutral”: − 2°< aHKA angle < 2°; “valgus”: aHKA angle > 2°.
-
4)
Postoperative “pre-arthritic/kinematic” alignment or “outlier” [16]: “pre-arthritic/kinematic” alignment: the postoperative mHKA angle was within ± 3° of the preoperative aHKA angle.
-
4)
Postoperative “pre-arthritic/kinematic” alignment or “outlier” [16]: “pre-arthritic/kinematic” alignment: the postoperative mHKA angle was within ± 3° of the preoperative aHKA angle.
-
5)
Postoperative “restored” aHKA angle or “non-restored”: “restored” aHKA angle: the postoperative aHKA angle was within ± 3° of the preoperative aHKA angle.
The patients were also divided into two groups based on whether the aHKA angle was restored. Then, the KSS 2011 scores and radiological parameters were compared between the subgroups. Differences in the KSS 2011 (total and subscale scores) were evaluated if they exceeded the previously reported minimal clinically important difference value of 10 points [24, 25]. Radiological parameters were compared using either the t-test or the Wilcoxon signed-rank test, as appropriate, based on the Shapiro–Wilk test results. Statistical significance was set at p < 0.05. Variables with p-values of < 0.1 were included in a multivariable model to identify the independent factors for a postoperative restored aHKA angle. A multivariate logistic regression analysis was performed using the stepwise variable entry method. Statistical analyses were performed using JMP statistical analysis software (version 15.0; SAS Institute, Cary, NC, USA). To evaluate intra- and inter-observer reproducibility in the study group, measurements were performed twice by one examiner (YK) and once by another examiner (JA). The intra- and inter-class correlation coefficients were good (0.86 to 0.91 and 0.80 to 0.88, respectively) for all measurements.
Results
In total, 109 consecutive patients (118 knees) who underwent UKA for knee OA were evaluated for inclusion. However, 28 patients were excluded for bilateral UKA (n = 9 patients; 18 knees), a history of neuromuscular disease (n = 2; 2 knees), postoperative complications (infection, periprosthetic fracture) (n = 3; 3 knees), medical complications (e.g., stroke) and significantly decreased levels of activities of daily living (n = 2; 2knees), and symptomatic contralateral knee OA or ipsilateral hip OA (n = 2; 2knees). Finally, 91 patients (91 knees) were enrolled in this study (Fig. 3).
Tables 1 and 2a present the demographic and radiographic parameters of the entire cohort. The mHKA angle improved from 8.0° ± 3.6° preoperatively to 5.0° ± 2.9° postoperatively, and no patient had a valgus alignment postoperatively. The KSS 2011 scores also improved, from 70.6 ± 22.3 preoperatively to 136.2 ± 26.3 postoperatively (p < 0.0001, Table 2b). Table 3 presents the multivariate analysis results regarding preoperative to postoperative improvements in the KSS 2011 scores. Postoperative restored aHKA angle (p = 0.020) was the only significant factor for improved KSS 2011 scores. Postoperative restored aHKA angle was obtained in 64 patients (70%). Table 4a details the radiographic parameter and KSS 2011 score subgroup analyses between the postoperative restored and non-restored aHKA angle groups. The preoperative varus deformity (i.e., a large mHKA angle) in the non-restored aHKA angle group was severe. Patients with a restored aHKA angle had significantly higher total scores (p = 0.032), and the difference was greater than that of the minimal clinically important difference. Finally, the multivariate analysis showed that ΔMPTA and ΔLDFA were significant factors associated with a postoperative restored aHKA angle (Table 4b).
Discussion
This study demonstrates that a small change in the aHKA angle during UKA improved functional outcomes in the early postoperative period. The aHKA angle predicts the constitutional knee joint geometry considering the LDFA and MPTA, and this parameter is not affected by joint space narrowing or tibio-femoral subluxation [23]. Based on the UKA concept, it is clinically important that the aHKA angle is restored from preoperative to postoperative. This study is the first to confirm that this restoration is a significant factor for favorable knee function in the early postoperative period.
Nonetheless, optimal alignment after UKA remains controversial. Until recently, neutral mechanical alignment has been the gold standard for UKA [13, 26], but new evidence emphasizes the importance of avoiding postoperative valgus alignment in mHKA [2]and that slight varus alignment (postoperative varus < 7°) is acceptable [21, 27]. We found no cases of postoperative valgus alignment of the mHKA, nor was postoperative varus alignment a significant factor in the multivariate analysis. The pre-arthritic/kinematic alignment reported by Plancher et al. [16] was also not a significant factor for PROM improvement in this study. Their study cohort had a mean follow-up of 10 years, and our cohort aimed for slight varus alignment, which may explain the differing results. Although the optimal alignment after UKA remains controversial, we demonstrate that restoring the aHKA angle allows for significant PROM improvements in the early postoperative period, consistent with the surgical concept of UKA.
The ΔMPTA was smaller in patients with a restored aHKA angle. Previous studies have suggested that restoring native tibial alignment may improve clinical outcomes [21, 28]. In contrast to previous reports, this study focused on the aHKA angle, a parameter that considers the geometry of the femoral articular surface. The cases in which the aHKA angle was not restored were tibial vara knees with a small preoperative MPTA [29]. In this case, the postoperative MPTA is similar; thus, the large ΔMPTA in these cases indicates insufficient thickness of the proximal tibial resection. In the case of UKA with spacer block technique, insufficient tibial proximal resection thickness also caused insufficient femoral resection thickness (i.e., a small ΔLDFA) due to re-tensioning of the medial collateral ligament. The multivariate analysis showed that the significant factors related to a restored aHKA angle were ΔMPTA and ΔLDFA. As previously reported, the restored aHKA angle, a significant factor for improved KSS 2011 scores, was not achieved by restoring the tibial side only, suggesting that paying close attention to the femoral side is also necessary.
This study had several limitations. First, the KSS 2011 score was only investigated in the early postoperative period. Most studies performed postoperative functional evaluations after at least two years of follow-up. However, UKA is advantageous over total knee arthroplasty because it is less invasive and has faster functional recovery. Therefore, early postoperative recovery evaluations are important after UKA. Second, this study was a retrospective analysis of cemented fixed-bearing UKA only. Similar results may not be observed with different types of prostheses. Therefore, prospective studies using multiple types of prostheses (including cementless and mobile-bearing UKA) should be conducted. Third, functional outcomes were evaluated using only KSS 2011. KSS 2011 is one of the most commonly used PROMs that has been validated as responsive and reliable [30]. Further studies using other PROMs such as Oxford Knee Score and Knee Injury and Osteoarthritis Outcome Score should be considered [31].
Conclusions
A small change in the aHKA angle during UKA improves the functional outcomes of the knee during the early postoperative period.
Data availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
Code Availability
Not applicable.
References
Gill JR, Vermuyten L, Wastnedge E, Nicolai P (2021) The effect of component alignment on clinical outcomes in fixed bearing unicompartmental knee arthroplasty. Knee 29:126–133
Hernigou P, Deschamps G (2004) Alignment influences wear in the knee after medial unicompartmental arthroplasty. Clin Orthop Relat Res 161–165
Kozinn SC, Scott R (1989) Unicondylar knee arthroplasty. J Bone Joint Surg Am 71:145–150
Thornhill TS (1986) Unicompartmental knee arthroplasty. Clin Orthop Relat Res 205:121
Affatato S, Caputo D, Bordini B (2019) Does the body mass index influence the long-term survival of unicompartmental knee prostheses? A retrospective multi-centre study. Int Orthop 43:1365–1370
Greco NJ, Lombardi AV Jr, Price AJ et al (2018) Medial Mobile-Bearing Unicompartmental knee arthroplasty in young patients aged Less Than or Equal to 50 years. J Arthroplasty 33:2435–2439
Berend KR, Lombardi AV Jr, Morris MJ et al (2011) Does preoperative patellofemoral joint state affect medial unicompartmental arthroplasty survival? Orthopedics 34:e494–e496
Crawford DA, Adams JB, Lombardi AV Jr, Berend KR (2019) Activity level does not affect survivorship of Unicondylar Knee Arthroplasty at 5-Year Minimum Follow-Up. J Arthroplasty 34:1364–1368
Pandit H, Jenkins C, Gill HS et al (2011) Unnecessary contraindications for mobile-bearing unicompartmental knee replacement. J Bone Joint Surg Br 93:622–628
Friesenbichler B, Item-Glatthorn JF, Wellauer V et al (2018) Short-term functional advantages after medial unicompartmental versus total knee arthroplasty. Knee 25:638–643
Liddle AD, Pandit H, Judge A, Murray DW (2015) Patient-reported outcomes after total and unicompartmental knee arthroplasty: a study of 14,076 matched patients from the National Joint Registry for England and Wales. Bone Joint J 97–B:793–801
Pongcharoen B, Liengwattanakol P, Boontanapibul K (2023) Comparison of Functional Recovery between Unicompartmental and total knee arthroplasty: a Randomized Controlled Trial. J Bone Joint Surg Am 105:191–201
Whiteside LA (2005) Making your next unicompartmental knee arthroplasty last: three keys to success. J Arthroplasty 20:2–3
Pandit H, Spiegelberg B, Clavé A et al (2016) Aetiology of lateral progression of arthritis following Oxford medial unicompartmental knee replacement: a case-control study. Musculoskelet Surg 100:97–102
Rivière C, Sivaloganathan S, Villet L et al (2022) Kinematic alignment of medial UKA is safe: a systematic review. Knee Surg Sports Traumatol Arthrosc 30:1082–1094
Plancher KD, Brite JE, Briggs KK, Petterson SC (2022) Pre-Arthritic/Kinematic alignment in fixed-bearing medial unicompartmental knee arthroplasty results in return to activity at Mean 10-Year follow-up. J Bone Joint Surg Am 104:1081–1089
Boettner F, Springer B, Windhager R, Waldstein W (2020) The tibial spine sign does not indicate cartilage damage in the central area of the distal lateral femoral condyle. Knee Surg Sports Traumatol Arthrosc 28:2592–2597
Nam D, Khamaisy S, Gladnick BP et al (2013) Is tibiofemoral subluxation correctable in unicompartmental knee arthroplasty? J Arthroplasty 28:1575–1579
Liu C, Ge J, Sun X et al (2023) Coronal tibiofemoral subluxation under valgus stress force radiography is useful for evaluating postoperative coronal tibiofemoral subluxation in mobile-bearing UKA. Arch Orthop Trauma Surg 143:4349–4361
de Brauw TN, Bayoumi GV, Ruderman T LV, et al (2023) Knees with anteromedial osteoarthritis show a substantial phenotypic variation prior and following medial unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-023-07603-9
Micicoi L, Machado A, Ernat J et al (2023) Restoration of preoperative tibial alignment improves functional results after medial unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 31:5171–5179
Oh S-M, Bin S-I, Kim J-Y et al (2019) Impact of preoperative varus deformity on postoperative mechanical alignment and long-term results of mechanical aligned total knee arthroplasty. Orthop Traumatol Surg Res 105:1061–1066
MacDessi SJ, Griffiths-Jones W, Harris IA et al (2021) Coronal plane alignment of the knee (CPAK) classification. Bone Joint J 103–B:329–337
Nishitani K, Yamamoto Y, Furu M et al (2019) The minimum clinically important difference for the Japanese version of the new knee society score (2011KSS) after total knee arthroplasty. J Orthop Sci 24:1053–1057
Sebastia-Forcada E, Ruiz-Lozano M, Perez-Aznar A et al (2024) Functional Outcome Change over 10 years after primary total knee arthroplasty. A prospective longitudinal cohort study. J Arthroplasty 39:374–378
Walker T, Heinemann P, Bruckner T et al (2017) The influence of different sets of surgical instrumentation in Oxford UKA on bearing size and component position. Arch Orthop Trauma Surg 137:895–902
Ridgeway SR, McAuley JP, Ammeen DJ, Engh GA (2002) The effect of alignment of the knee on the outcome of unicompartmental knee replacement. J Bone Joint Surg Br 84:351–355
Baur J, Zwicky L, Hirschmann MT et al (2015) Metal backed fixed-bearing unicondylar knee arthroplasties using minimal invasive surgery: a promising outcome analysis of 132 cases. BMC Musculoskelet Disord 16:177
Park DY, Park K-H, Jin YJ et al (2023) Fixed-bearing unicompartmental knee arthroplasty in Tibia Vara Knees results in Joint Surface Malalignment and Varus Joint Line Obliquity, but does not affect functional outcomes at Greater Than 5 years Follow-Up. J Arthroplasty. https://doi.org/10.1016/j.arth.2023.09.024
Taniguchi N, Matsuda S, Kawaguchi T et al (2015) The KSS 2011 reflects symptoms, physical activities, and radiographic grades in a Japanese population. Clin Orthop Relat Res 473:70–75
Deng W, Shao H, Zhou Y et al (2022) Reliability and validity of commonly used patient-reported outcome measures (PROMs) after medial unicompartmental knee arthroplasty. Orthop Traumatol Surg Res 108:103096
Acknowledgements
We thank Hidetoshi Tsushima and Junki Adachi (Department of Orthopaedic Surgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan) for data collection and their invaluable advice for this study.
Funding
No funds, grants, or other support was received..
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Yasuhiko Kokubu, Shinya Kawahara, Yukio Akasaki, Satoshi Hamai, and Taishi Sato. The first draft of the manuscript was written by Yasuhiko Kokubu and Shinya Kawahara. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the local Institutional Review Board (No. 2020–204).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
All authors have reviewed and confirmed the whole manuscript.
Conflicts of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kokubu, Y., Kawahara, S., Hamai, S. et al. Small change in the arithmetic hip-knee-ankle angle during unicompartmental knee arthroplasty improves early postoperative functional outcomes. Arch Orthop Trauma Surg 144, 2297–2304 (2024). https://doi.org/10.1007/s00402-024-05309-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-024-05309-2