Abstract
Introduction
Evidence of whether to use hemiarthroplasty (HA) or total hip arthroplasty for displaced femoral neck fractures (FNF) is still widely debated, especially when taking ambulatory status, age, and patient cognitive status into account. The current study aims to report the rates of dislocations, revisions and other complications for primary cemented HA in patients with displaced FNF.
Materials and methods
Single-center retrospective follow-up study of an unselected historic cohort. 743 consecutive hips (551 W and 192 M) at mean (SD) age of 83.6 (8.4) years received primary cemented HA for displaced FNF by posterolateral surgical approach between January 2012 and December 2019. Patient files and radiographs were evaluated for dislocations, revisions, and other complications until death or end of the follow-up period, and the educational level of the surgeon was noted.
Results
During a mean (SD) follow-up period of 2.7 (2.2) years, there were 6.1% (n = 45) dislocations, in which 82% (first dislocation) appeared within the first 30 postoperative days, and 51% (n = 23) of the dislocations requiring subsequent surgery. At the time of the last available follow-up, 57% (n = 421) of the patients were dead. A non-dislocation related revision was needed in 3.4% (n = 25) of the patients [in which infection accounted for 40% (n = 10) and traumatic periprosthetic fracture for 32% (n = 8)]. Thirty-day mortality was 9.2% and 1-year mortality 25.8%. There were no differences in patient's age, gender, or educational level of the surgeon between the dislocation and the no dislocation groups. Patients aged < 70 years presented with a higher dislocation rate (p < 0.001) than the patients aged > 70 years.
Conclusion
Primary HA presents a safe and robust approach with acceptable complication rates in a genuine unselected cohort of displaced FNF, particularly for patients aged > 70.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Hip fractures are common and constitute a sizeable burden for the existing and future health care system, particularly with the increasing life expectancy [24]. By 2050, it is globally projected that more than 6 million hip fractures will be accounted for annually [4]. Femoral neck fractures (FNF) represent approximately 50% of all hip fractures. In cases of displaced FNF (classified as Garden type III or IV [11]) and when femoral head preservation is not applicable, it is generally appreciated that treatment should involve joint arthroplasty [9, 10]. Evidence of whether to apply primary HA or THA for displaced FNF is still widely debated, especially when taking ambulatory status, age, life expectancy, and patient cognitive status into account [1, 23].
Patients suffering a displaced FNF are generally considered frail with high hospital demands, decreasing mobility and function as well as an increased risk for complications, e.g. dislocations and revisions [22, 28]. The risk of performing secondary surgery in this patient group is a concern for both patients and surgeons and in the event of a complication, many patients may not have the capacity to withstand a subsequent procedure [23]. Therefore, it is important to continuously evaluate the existing evidence and local treatment regimens to provide the optimal treatment for displaced FNF.
At our institution, hemiarthroplasty (HA) bipolar CPT stem was introduced in 1997 as the primary treatment for all displaced FNFs in patients aged > 70 years, reasoned by less complex surgery, expected low dislocation rate, and lower initial costs than that of total hip arthroplasty (THA), enabling sufficient fast-track surgery within 24 h [14]. The current study aims to report the rates of dislocations, revisions, and other complications for primary HA used as the treatment for displaced FNF in an unselected consecutive series of patients during an 8-year period.
Materials and methods
The study design was a single-center retrospective follow-up study of an unselected historic cohort receiving standard treatment with primary cemented HA for radiologically confirmed displaced femoral neck fractures (Garden type III or IV) between January 2012 and December 2019 at Aarhus University Hospital, Denmark. Exclusion criteria were secondary HA (e.g., due to failed internal osteosynthesis), HA due to malignant cancer or metastasis, and foreign status (unable to follow-up). We identified 816 HA procedures during the study period. 73 patients were excluded according to the exclusion criteria, leaving 743 hips (17 bilateral hips, performed in separate procedures) for final evaluation.
In compliance with the Danish hip fracture reference program, primary HA or THA is the standard treatment in Denmark in patients aged > 70 years and in younger patients where the fracture cannot be acceptably reduced for osteosynthesis [6]. Using this age as cut-off, a dislocation sub-analysis was performed for patients aged above and below 70 years. Our business intelligence system was searched for the surgical procedure code for insertion of distal cemented hemiarthroplasty component (KNFB12). Retrospective analysis of patient records and radiology were retrieved in October 2020 from the electronic medical report and the radiology program Impax v. 6.5 allowing for retrieval of data of complications encountered from four out of five hospitals with acute orthopedic intake in the Central Denmark Region. All patient files were crosschecked for dislocations, revisions, and other complications until death or end of the follow-up period, and the educational level (residents and specialists) of the surgeon was noted. Pulmonary embolism and deep vein thrombosis were considered to be in relation to HA surgery when occurring within 3 months after the operation.
The surgical procedure was performed by supervised residents in 55% of cases (n = 406) and by an orthopedic specialist in 45% of cases (n = 337). All patients were operated with the posterolateral approach and completed with capsule repair and resuturing of the external rotators in all cases. All patients received cemented (Palacos bone cement, Haereus Medical GmbH, Wehrheim, Germany) bipolar CPT stem (Zimmer Biomet, Warsaw, Indiana, USA), with a head size (range 22–28 mm) and corresponding shell according to the anatomical size of the extracted femoral head. All patients received a single dose of either dicloxacillin or cefuroxime as intravenous antibiotic prophylaxis before surgery. Tranexamic acid according to weight (10 mg/kg) was used preoperative if preferred. Full weight bearing was initiated as soon as possible after surgery. Postoperative radiographs were taken on the first day after index surgery.
Statistical analysis
The dislocation rate was the primary endpoint. Secondary endpoints included revision rates, mortality (30 days and 1 year), postoperative deep vein thrombosis and pulmonary embolism, associations between dislocation rate and patient age, and the influence of the educational level of the surgeon. A two-sample t test with equal variances was used to test for age differences between the dislocation and non-dislocation groups. The distribution of dislocations related to the educational level of the surgeon and patient gender was tested using a Chi-squared test. Statistical tests were performed using Stata (v. 14.1, StataCorp LLC, College Station, TX, USA).
Ethics
The study was approved by the Danish Patient Safety Authority (registration number 31-1521-407).
Results
Mean (range) follow-up time was 2.7 (0–8.4) years, and mean (range) age at the time of surgery was 82.6 (53.4–103.5) years. Gender distribution; female 74% (n = 551), male 26% (n = 192) hips. At the time of the last available follow-up, 57% (n = 421) of the patients were dead. 30-day mortality was 9.2% (n = 43) and 1-year mortality 25.8% (n = 192). No iatrogenic fracture was found on the primary postoperative X-ray.
Dislocations
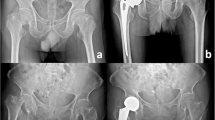
6.1% (n = 45) of the hips had an event of dislocation with a mean (SD) time to first dislocation of 18 (17) days. Dislocation demographics are presented in Table 1. The mean (range) number of dislocations was 2 (1–5). 49% (n = 22) of the hips in the dislocation group were solely treated with closed reduction(s). In the remaining 51% (n = 23) of the hips in the dislocation group, subsequent surgery was needed either with open reduction with/without component replacement (n = 4), conversion to THA due to recurrent dislocation (n = 14), Girdlestone procedure (n = 2) or fractured after closed reduction require conversion to THA (n = 1). In two cases, we found complication with deep infection and performed revision to THA (Fig. 1). 82% (n = 37) of the dislocations (first dislocation) occurred within the first 30 postoperative days. No differences in patient's age, gender, or educational level of the surgeon were found between the dislocation and no dislocation group (Table 1).
6.8% (n = 50) of the hips were aged < 70 years when receiving HA. Of these, 16% (n = 8) dislocated at least once during the follow-up period, which were higher (p < 0.001) than the dislocation rate of 5.3% (n = 37) in the patient group aged > 70 years.
Revisions
3.4% (n = 25) experienced a hip-related revision due to a non-dislocation complication (Fig. 1).
Other complications
Three patients (0.4%) died during surgery. 4 patients (0.5%) experienced postoperative deep vein thrombosis and 7 patients (0.9%) pulmonary embolism within the first 3 months after surgery.
Discussion
In this consecutive single cohort study of 743 unselected FNF treated with primary cemented HA, we report a dislocation rate of 6.1% (n = 45) during a mean follow-up period of 2.7 years. Of those, 49% (n = 22) were solely treated with closed reduction(s), and of the remaining 51% (n = 23) subsequent surgery was needed. Patients aged < 70 years presented with a higher dislocation rate than the patients aged > 70 years.
HA dislocation rate
Our dislocation rate findings are comparable to a similar retrospective study of 602 consecutive cemented HA hips performed by both supervised residents and orthopedic specialists applying the posterolateral approach (dislocation rate 5.6%) [19]. However, other posterolateral approach cemented HA studies of unselected cohorts report higher dislocation rates; 10% in 101 HA hips (mean age 83.3, mean follow-up 25.4 months) [2], and 10.7% in 373 HA hips (mean age 84, follow-up range 6 months to 7 years) [21]. In turn, one systematic review (411 HA hips), and one multi-center randomized trial comparing THA with HA (723 HA hips), demonstrate dislocation rates as low as 2.4–3% [1, 3]. Notably, Bhandari et al. excluded patients with dementia and only allowed experienced surgeons to participate, while the results from Burgers et al. represent the fit elderly population, and none of these two studies reports or discuss the implication of the surgical approach. As our findings represent a genuine unselected cohort, irrespective of comorbidities and surgeon skill level, and only apply to the posterolateral surgical approach, a direct comparison to these two latter studies seems unequal. At our institution, we apply the posterolateral approach for HA surgery given its advantages of providing a good surgical field overview and simple femur preparation and instrumentation. Furthermore, it is the standard approach used by our hip surgeons performing primary THA and used in approximately 96% of primary THAs in Denmark [5]. The essential limitations of the approach remain an obligate injury of the posterior soft tissue in the hip. For HA surgery, the anterolateral approach has been associated with a lower risk of dislocation in comparison to the posterolateral approach (3% vs 8.5%) [8]. A recent systematic review concluded that the posterolateral approach may be associated with more dislocations in comparison to the direct lateral approach, but presented with less walking problems and lower tendency to abductor insufficiency [27]. Prudently, these differences in dislocation rates across the surgical approaches may be reasoned by the differences in soft tissue damage and thus the stability of the hip. Although the literature might indicate otherwise, the ideal surgical approach remains an interesting and ongoing matter of dispute, and to a wide extent continues to rely on local tradition and surgeon preferences.
The patients < 70 years in our study displayed a higher dislocation rate (16%) in comparison to the patient group aged > 70 years (5.3%), which may be explained by a lower physical activity level and/or higher grade of comorbidities in the patients aged > 70 years [13]. Although this difference was significant, there may be a risk of overestimating this complication due to the low number of patients aged < 70.
Mortality, infections, periprosthetic fractures, and educational level of the surgeon
Our mortality rates are within the recommendations from the Danish National Guideline for Hip Fracture Treatment aiming for 30-day mortality below 10% after hip fractures in general [5]. Notably, our mortality rates are consistent with a comparable Danish cohort treating displaced FNF with primary dual-mobility THA [26] and parallels the Danish Multidisciplinary Hip Fracture Registry of all types of hip fractures, reporting 30-day mortality rates in the range of 10–12% [15].
We found no iatrogenic fractures on the primary postoperative X-ray, traumatic periprosthetic fracture in 1.1% (n = 8) and revision due to infection in 1.6% (n = 12) of all operated hips. While several studies fail to report infection rates, our rate of traumatic periprosthetic fracture is considerably lower than reported otherwise [1]. For uncemented HA, a hazard risk ratio of 5.1 on reoperation due to periprosthetic fracture has been reported in comparison to cemented HA [16]. This may partly explain our low traumatic periprosthetic fracture rates as exclusively cemented stems were applied.
Supported by previous HA studies [8, 19], we found no association between the educational level of the surgeon and dislocation rates. As standard practice at our institution, we perform no selection between supervised residents and orthopedic specialists conducting the surgery, and the surgery is often conducted by surgeons from several different orthopedic subspecialties performing on-call duties. Although our practice present acceptable complication rates paralleling the existing literature, pure involvement of experienced surgeons conducting the HA surgery or more structured education of residents, might result in fewer complications [7].
HA vs THA for FNF
In comparison to THA, HA is a faster, less invasive procedure with lower initial costs and has also been associated with lower dislocation rates [3, 14, 20]. However, a recent retrospective study of a comparable patient cohort (n = 966 displaced FNF) treated with an anti-dislocation THA dual-mobility cup and primarily by experienced hip surgeons, demonstrated a dislocation rate of only 4.7%. In addition, 0.8% had intraprosthetic dislocation requiring open reduction and liner replacement [26]. Evaluated by the risk of revision, Harris Hip Score and Quality of Life (Short Form 36), a recent review concluded that THA appears to be superior to HA, especially in patients < 80 years and with a life expectancy > 4 years [18].
In total, 3.6% (n = 27 hips) were converted to a THA in our follow-up period. It has recently been demonstrated that converting a HA to THA has poorer outcome than primary THA evaluated by adverse outcomes and costs [12]. In our cohort, 0.5% hips (n = 4) in the non-dislocation group were converted to THA due to radiological visible acetabular erosion and persistent hip pain, which is lower than reported by Schmitz et al. demonstrating acetabulum wear and a pain conversion rate of 5.6%, although only reported for patients aged under 75 [25]. As patients with FNF are considered frail and the mean age of the patients included in our study is rather high, there is a judicious risk of underestimating this complication [17].
Limitations
The retrospective design may result in a risk of underestimating the complications, as some complications may have encountered outside the four hospitals in the Central Denmark Region and, therefore, not registered. However, given the rather high age and the general frailty of patients with FNF, only a few patients are expected to move outside the Central Denmark Region. Moreover, no control group was included for comparison with a different treatment modality, e.g. THA, and the design did not allow for the registration of patient-reported outcome measures (pain, functional outcome, or quality of life), excluding qualitative assessment of the inserted HA nor any assessment of postoperative walking capabilities. Also, we were not able to evaluate the influence of patient cognitive status and patient specified demographics (e.g. body mass index, osteoporosis status, ASA-classification, etc.) as this was inconsistently described in the electronic medical report. Lastly, diagnosis of pulmonary embolism and deep vein thrombosis were only crosschecked for in the patient files, which introduces an obligate risk of underestimating these complications.
Conclusion
In summary, this study adds further to the evidence of treating displaced FNF. Primary HA presents a safe and robust treatment option, particularly for patients aged > 70, with acceptable complication rates in a normal clinical practice set-up, allowing for supervised residents to perform the surgery without increasing the dislocation risk. Our study promotes further curious discussion to the continuous debate regarding the optimal treatment for FNF, and to the definition of an exact optimal cut-off in which clinical situations HA is superior to THA, and vice versa. As our study population represents a genuine unselected cohort, our findings may readily be extrapolated, but we encourage future high-quality prospective studies conducting strict, thorough, and individual preoperative patient assessments when evaluating various treatment arms for the heterogeneous group of patients with displaced FNF rather than local preferences and traditions [23].
References
Bhandari M, Einhorn TA, Guyatt G et al (2019) Total hip arthroplasty or hemiarthroplasty for hip fracture. N Engl J Med 381(23):2199–2208. https://doi.org/10.1056/NEJMoa1906190
Boukebous B, Boutroux P, Zahi R, Azmy C, Guillon P (2018) Comparison of dual mobility total hip arthroplasty and bipolar arthroplasty for femoral neck fractures: a retrospective case-control study of 199 hips. Orthop Traumatol Surg Res 104(3):369–375. https://doi.org/10.1016/j.otsr.2018.01.006
Burgers PT, Van Geene AR, Van den Bekerom MP et al (2012) Total hip arthroplasty versus hemiarthroplasty for displaced femoral neck fractures in the healthy elderly: a meta-analysis and systematic review of randomized trials. Int Orthop 36(8):1549–1560. https://doi.org/10.1007/s00264-012-1569-7
Dhanwal DK, Dennison EM, Harvey NC, Cooper C (2011) Epidemiology of hip fracture: worldwide geographic variation. Indian J Orthop 45(1):15–22. https://doi.org/10.4103/0019-5413.73656
DHRR (2016) Danish hip replacement registry—annual report. http://danskhoftealloplastikregister.dk/wp-content/uploads/2015/11/DHR-%C3%A5rsrapport-2016.pdf. Accessed 8 June 2021
DOS (2008) Danish Orthopaedic Society. Reference programme for patients with hip fractures. https://www.ortopaedi.dk/fileadmin/Guidelines/Referenceprogrammer/Referenceprogram_for_patienter_med_hoftebrud2008.pdf. Accessed 8 June 2021
Ekman E, Nurmi H, Reito A, Paloneva J (2019) Complications following 250 cemented modular hip hemiarthroplasties. Scand J Surg 108(4):321–328. https://doi.org/10.1177/1457496918812226
Enocson A, Tidermark J, Tornkvist H, Lapidus LJ (2008) Dislocation of hemiarthroplasty after femoral neck fracture: better outcome after the anterolateral approach in a prospective cohort study on 739 consecutive hips. Acta Orthop 79(2):211–217. https://doi.org/10.1080/17453670710014996
Frihagen F, Nordsletten L, Madsen JE (2007) Hemiarthroplasty or internal fixation for intracapsular displaced femoral neck fractures: randomised controlled trial. BMJ 335(7632):1251–1254. https://doi.org/10.1136/bmj.39399.456551.25
Gao H, Liu Z, Xing D, Gong M (2012) Which is the best alternative for displaced femoral neck fractures in the elderly? A meta-analysis. Clin Orthop Relat Res 470(6):1782–1791. https://doi.org/10.1007/s11999-012-2250-6
Garden RS (1961) Low-angle fixation in fractures of the femoral neck. J Bone Joint Surg 43(4):647–663
Hernandez NM, Fruth KM, Larson DR, Kremers HM, Sierra RJ (2019) Conversion of hemiarthroplasty to THA carries an increased risk of reoperation compared with primary and revision THA. Clin Orthop Relat Res 477(6):1392–1399. https://doi.org/10.1097/CORR.0000000000000702
Jobory A, Karrholm J, Hansson S, Akesson K, Rogmark C (2021) Dislocation of hemiarthroplasty after hip fracture is common and the risk is increased with posterior approach: result from a national cohort of 25,678 individuals in the Swedish hip arthroplasty register. Acta Orthop 92(4):413–418. https://doi.org/10.1080/17453674.2021.1906517
Keating JF, Grant A, Masson M, Scott NW, Forbes JF (2005) Displaced intracapsular hip fractures in fit, older people: a randomised comparison of reduction and fixation, bipolar hemiarthroplasty and total hip arthroplasty. Health Technol Assess 9(41):1–65. https://doi.org/10.3310/hta9410
Kristensen PK, Rock ND, Christensen HC, Pedersen AB (2020) The Danish multidisciplinary hip fracture registry 13-year results from a population-based cohort of hip fracture patients. Clin Epidemiol 12:9–21. https://doi.org/10.2147/CLEP.S231578
Kristensen TB, Dybvik E, Kristoffersen M et al (2020) Cemented or uncemented hemiarthroplasty for femoral neck fracture? Data from the Norwegian hip fracture register. Clin Orthop Relat Res 478(1):90–100. https://doi.org/10.1097/CORR.0000000000000826
Leonardsson O, Karrholm J, Akesson K, Garellick G, Rogmark C (2012) Higher risk of reoperation for bipolar and uncemented hemiarthroplasty. Acta Orthop 83(5):459–466. https://doi.org/10.3109/17453674.2012.727076
Lewis DP, Waever D, Thorninger R, Donnelly WJ (2019) Hemiarthroplasty vs total hip arthroplasty for the management of displaced neck of femur fractures: a systematic review and meta-analysis. J Arthroplasty 34(8):1837–1843. https://doi.org/10.1016/j.arth.2019.03.070
Madanat R, Makinen TJ, Ovaska MT, Soiva M, Vahlberg T, Haapala J (2012) Dislocation of hip hemiarthroplasty following posterolateral surgical approach: a nested case-control study. Int Orthop 36(5):935–940. https://doi.org/10.1007/s00264-011-1353-0
Migliorini F, Trivellas A, Driessen A et al (2020) Hemiarthroplasty versus total arthroplasty for displaced femoral neck fractures in the elderly: meta-analysis of randomized clinical trials. Arch Orthop Trauma Surg 140(11):1695–1704. https://doi.org/10.1007/s00402-020-03409-3
Mukka S, Lindqvist J, Peyda S et al (2015) Dislocation of bipolar hip hemiarthroplasty through a postero-lateral approach for femoral neck fractures: a cohort study. Int Orthop 39(7):1277–1282. https://doi.org/10.1007/s00264-014-2642-1
NICE (2011) NICE—National Institute for Health and Care Excellence—Clinical guideline, Hip fracture: management. https://www.nice.org.uk/guidance/cg124. Accessed 8 June 2021
Rogmark C, Leonardsson O (2016) Hip arthroplasty for the treatment of displaced fractures of the femoral neck in elderly patients. Bone Joint J 98(3):291–297. https://doi.org/10.1302/0301-620X.98B3.36515
Rosengren BE, Bjork J, Cooper C, Abrahamsen B (2017) Recent hip fracture trends in Sweden and Denmark with age-period-cohort effects. Osteoporos Int 28(1):139–149. https://doi.org/10.1007/s00198-016-3768-3
Schmitz PP, van Susante JLC, Somford MP (2019) Low conversion rates toward total hip arthroplasty after hemiarthroplasty in patients under 75 years of age. Eur J Orthop Surg Traumatol 29(8):1687–1691. https://doi.org/10.1007/s00590-019-02498-0
Tabori-Jensen S, Hansen TB, Stilling M (2019) Low dislocation rate of Saturne((R))/Avantage((R)) dual-mobility THA after displaced femoral neck fracture: a cohort study of 966 hips with a minimum 1.6-year follow-up. Arch Orthop Trauma Surg 139(5):605–612. https://doi.org/10.1007/s00402-018-3093-8
Tol M, van Beers L, Willigenburg NW et al (2021) Posterolateral or direct lateral approach for hemiarthroplasty after femoral neck fractures: a systematic review. Hip Int 31(2):154–165. https://doi.org/10.1177/1120700020931766
Vasu BK, Ramamurthi KP, Rajan S, George M (2018) Geriatric patients with hip fracture: frailty and other risk factors affecting the outcome. Anesth Essays Res 12(2):546–551. https://doi.org/10.4103/aer.AER_61_18
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
The study was approved by the Danish Patient Safety Authority (registration number 31–1521-407).
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bue, M., Jakobsen, S.S., Barckman, J. et al. Dislocation rate, revisions and other complications of primary cemented hemiarthroplasty for displaced femoral neck fractures: a single-center cohort study of 743 unselected hips with a mean 2.7-year follow-up. Arch Orthop Trauma Surg 142, 3797–3802 (2022). https://doi.org/10.1007/s00402-021-04252-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04252-w