Abstract
Purpose
Evaluating whether changes in gut microbiota induced by a bifidobacterial strain may have an effect on the hepatic vascular function in portal hypertensive cirrhotic rats.
Methods
Bile duct ligation (BDL) was performed in rats. A subgroup of animals received B. pseudocatenulatum CECT7765 (109 cfu/daily ig.) for 1 week prior to laparotomy. Hemodynamic, biochemical and inflammatory markers were evaluated. Ileal microbiota composition was identified. Statistical analysis was performed.
Results
Sham-operated (n = 6), BDL (n = 6) and BDL treated with bifidobacteria (n = 8) rats were included. B. pseudocatenulatum CECT7765 significantly decreased proteobacteria (p = 0.001) and increased Bacteroidetes (p = 0.001) relative abundance. The bifidobacteria decreased the Firmicutes/Bacteroidetes ratio in the BDL model (p = 0.03). BDL with bifidobacteria vs BDL rats showed: significantly reduced portal vein area, portal flow, congestion index, alkaline phosphatase and total bilirubin, significantly increased serum cytokines and nitric oxide levels, gene expression levels of bile acids receptor FXR and endothelial nitric oxide synthase. Quantitative changes in the Clostridiales and Bacteroidales orders were independently associated with variations in portal vein area and portal flow, while changes in the Proteobacteria phylum were independently associated with congestion. Variations in all liver function markers significantly correlated with total OTUs mainly in the Firmicutes, but only changes in the Clostridiales were independently associated with alkaline phosphatase in the ANCOVA analysis.
Conclusion
Hemodynamic alterations and liver dysfunction induced by BDL in rats are partially restored after oral administration of B. pseudocatenulatum CECT7765. Results provide a proof-of-concept for the beneficial effect of this bifidobacterial strain in reducing complications derived from portal hypertension in cirrhosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cirrhosis is an advanced liver disease resulting from a chronic liver injury, characterized by generalized progressive vasodilatation, related to portal hypertension, mainly due to increased intrahepatic resistance [1]. Patients with decompensated liver cirrhosis have a poor prognosis [2] and an increased mortality, most often attributed to direct complications resulting from the loss of liver function, portal hypertension and the development of hepatocellular carcinoma.
Patients with cirrhosis and portal hypertension may develop hyperdynamic circulatory syndrome due to splanchnic arterial vasodilation [3]. These patients are at higher risk of developing esophageal varices. The use of prophylactic antibiotics in the setting of acute variceal bleeding is standard practice because it is known to decrease the rate of bacterial infection, risk of early rebleeding, and mortality [4, 5].
There is emerging evidence that the gut microbiome plays an important role in the progression of the complications of cirrhosis such as hepatic encephalopathy and others [6,7,8]. Studies have found a gut microbiota dysbiosis in patients with cirrhosis. Intestinal bacterial overgrowth (IBO) has been associated with advanced liver dysfunction [9,10,11] and may predispose patients to bacterial translocation. In fact, spontaneous bacterial peritonitis is more likely to develop in patients with IBO [9, 12].
Portal hypertension management could benefit from chronic manipulation of the gut microbiota [13,14,15]. B. pseudocatenulatum CECT7765 has previously shown to help in improving gut barrier integrity and reducing bacterial antigen translocation in experimental cirrhosis [16], and its capacity to repolarize cirrhotic patients’ macrophages towards an anti-inflammatory M2 phenotype [17]. The aim of the present study was to evaluate whether changes in gut microbiota composition induced by this bifidobacterial strain have an effect on the vascular function in a bile duct ligated rat model of liver damage.
Animals and methods
Study design
Study flowchart is represented in Supplementary Fig. 1. Male Sprague–Dawley rats [18] (Harlan, Barcelona, Spain) weighing 100–150 g were included in this study. Rats were individually caged at a constant room temperature of 21 °C and exposed to a 12:12 light/dark cycle. The animals were fed standard rodent chow along the study protocol. After 1 week for quarantine, animals were subjected to bile duct ligation (BDL) surgery. Briefly, rats were anesthetized with ketamine and xylazine. After midline laparotomy, we ligated the common bile duct at two different levels with 5-0 silk sutures, and sectioned the duct between the ligatures. Abdominal wall was closed with 5-0 silk sutures. A subgroup of animals acted as controls and was sham-operated.
After surgeries, animals started then a 4-week protocol to develop experimental cirrhosis. In week 3, animals intragastrically received B. pseudocatenulatum CECT7765 (109 cfu daily) or placebo (vehicle). In week 4, ultrasound Doppler images were performed to all sham or BDL animals. Laparotomies were performed under anesthesia with ketamine and xylazine after the ultrasound measurements. Animals remained fasting the night before laparotomies. The skin was sterilized with iodine and a short incision in the abdominal wall was performed. Blood (2 mL) from the vena cava were inoculated under aseptic conditions in sterile, rubber-sealed Vacutainer SST II tubes (BD Diagnostics, Belgium) that were never exposed to free air. The liver was perfused in situ with HBSS without Ca2+ and Mg2+ at 37 °C. This was followed by perfusion with HBSS containing 100 mM CaCl2 solution at the same perfusion rate. The liver was then removed and rinsed with HBSS. Liver biopsy specimens, 10–15 mm in size, were collected and conserved in RNA later (Sigma-Aldrich, Madrid, Spain). Intestinal content from the ileum (10 cm) proximal to the ileocecal valve were collected in a sterile cryotube, and the corresponding intestinal wall was washed with warm saline three times to minimize bacterial attachment [19] and stored in RNA later (Sigma). Animals were then euthanized by overdose of anesthesia.
The study was approved by the Animal Research Committee of Universidad Miguel Hernandez (Alicante, Spain).
B. pseudocatenulatum CECT7765 culture conditions
The strain B. pseudocatenulatum CECT7765 was obtained from the Spanish Type Culture Collection (CECT). The strain was grown in MRS broth (Scharlau, Barcelona, Spain) supplemented with 0.05% (w/v) cysteine (MRS-C Sigma, St. Louis, MO, USA) and incubated at 37 °C for 22 h (at stationary growth phase) under anaerobic conditions (AnaeroGen, Oxoid, Basingstoke, UK). Cells were harvested by centrifugation (6.000×g for 15 min), washed twice in phosphate-buffered saline (PBS, 130 mM sodium chloride, 10 mM sodium phosphate, pH 7.4) and re-suspended in 10% skimmed milk for oral administration to rats. Aliquots of these suspensions were frozen in liquid nitrogen and stored at − 80 °C until used. The number of live cells was determined by colony-forming unit (CFU) counting on MRS-C agar (Biomerieux) after 48-h incubation at 37 °C. For the strains tested, more than 90% cells were alive upon thawing and no significant differences were found during storage time (2 months). One fresh aliquot was thawed for every new experiment to avoid variability in the viability of cultures.
Microbiota composition analyses
gDNA from intestinal content from the ileum was extracted using a Fast DNA Stool Mini Kit (Qiagen) according to the manufacturer’s instructions with minor variations. 180–220 mg aliquots of intestinal content were placed in sterile tubes filled with glass beads and 1 mL of Inhibitex buffer (Qiagen). Samples were homogenized in a beadbeater for two successive rounds for 1 min with intermittent cooling on ice. Samples were then heated to 95 °C for 10 min and DNA extraction was carried out according to the manufacturer’s standard protocol. Samples were amplified in triplicate via PCR using primers (S-D-Bact-0563-a-S-15/S-D-Bact-0907-b-A-20) that target the V4–V5 variable regions of the 16S rDNA [20]. Triplicate reactions consisted of final concentrations of Buffer HF (1×), dNTPs (0.11 µM), primers (0.29 µM each) and Taq Phusion High Fidelity (0.007 U/µL) in final volumes of 35 µL. Cycling conditions consisted of 98 °C for 3 min, followed by 25 cycles of 95 °C for 20 s, 55 °C for 20 s, and 72 °C for 20 s, followed by a final extension step of 72 °C for 5 min. Each sample was tagged with a barcode to allow multiplexing during the sequencing process. Triplicate sample amplicons were combined and purified using the Illustra GFX PCR DNA and Gel Band Purification Kit (GE Healthcare) according to the manufacturer’s instructions and combined in equimolar concentrations before carrying out sequencing on a MiSeq instrument (Illumina).
Bioinformatic processing of data was carried out using the software Mothur [21] following the MiSeq standard operating procedure in Mothur for analyzing paired-end Illumina reads [22]. Forward and reverse Illumina reads were joined into contigs, poor-quality reads were removed, and barcodes and primers were removed. Sequences were aligned using the Mothur-provided SILVA-based bacterial reference alignment [23]. Chimeras were then removed using the Mothur implementation of UCHIME algorithm [24]. A distance matrix was created using the processed sequences and then sequences were clustered into operational taxonomic units (OTUs) at 97% identity. OTUs were classified using the Mothur-formatted version of the RDP training set (v.9) [25]. Samples were subsampled to the lowest number of sequences among samples and alpha diversity richness estimators and diversity indices (observed OTUs, Chao 1, Shannon’s diversity index, Simpson’s diversity index) were calculated. A phylogenetic tree was generated using Mothur’s implementation of the software program Clearcut using a relaxed neighbor joining algorithm [26].
Bifidobacteria were also quantified using 16S rRNA gene-specific primers for this genus [27, 28] by qPCR using LightCyclerH 480 SYBR Green I Master (Roche, USA) with an ABI PRISM 7000- PCR sequence detection system (Applied Biosystems, UK), as described previously [29].
Ultrasound imaging and analysis
All animals were anesthetized using isoflurane (1.5–2.5% in oxygen, titrated to maintain stable heart rate, respiration rate, and body temperature). The upper abdomen was shaved and depilatory cream applied below the xiphoid process. Animals were positioned supine on a heated platform [Vevo 2100 Imaging Station (integrated rail system); Visualsonics, Toronto, Canada]. Body temperature was monitored continuously, via a rectal probe, and maintained at 37 °C throughout the experiment using the heated table and when necessary, a supplemental heat lamp. The height of the transducer was set to apply minimal pressure to the abdomen while still allowing adequate views of the abdominal vessels of interest. Once the transducer was positioned, the x–y knobs of the platform were used to move the transducer small increments in the cranial and caudal directions to display the major abdominal vessels significant to this study: abdominal aorta, inferior vena cava, and portal vein (PV) in the same view [30]. Ultrasound recordings from individual rats during chronic studies were collected at the same time each day and feeding schedule remained consistent throughout the studies.
All vessel diameter measurements were made by the same ultrasonographer, using image frames from periods of cardiac systole and during exhalation obtained with a Vevo Imaging system (Visualsonic). Cine loops of the images were viewed on a desktop station using Vevo LAB 1.7.1 software (Visualsonic). Both vertical and horizontal diameters (vessel height and vessel width) of vessel cross-sections were measured and then averaged to obtain final values from each time point.
Liver and metabolic function biochemical markers
Serum levels of alkaline phosphatase (ALP), alanine transferase (ALT), urea, albumin (ALB), total protein (TP), glucose, cholesterol, total bile acids (TBA) and total bilirubin were determined in 200 µL of total blood using an automatic liquid biochemistry analyzer (Skyla Vb1, CVM practice, Navarra, Spain).
Tissue lysates and gene expression analysis
Total cellular RNA was isolated from 20 to 30 mg of liver disrupted by sonication. Oligonucleotides for selected genes were designed according to the Roche software. Quantitative real-time PCR (qRT-PCR) was performed in an IQ5 Real-Time PCR (BioRad, Hercules, CA, USA). B2-microglobulin was used as housekeeping gene in all gene expression analyses. Assays were made in triplicate and results normalized according to the expression level of the reference gene. Results were expressed using the ∆∆CT method for quantitation. Genes determined were cyclooxygenase (COX)-2 (forward 5′-CAGCCATGCAGCAAATCCTT-3′; reverse 5′-AAGTGGTAACCGCTCAGGTG-3′); farnesoid X-activated receptor (FXR) (forward 5′-CCACGACCAAGCTATGCAG-3′; reverse 5′-TCTCTGTTTGCTGTATGAGTCCA-3′) ; endothelial nitric oxide synthase (eNOS) (forward 5′-TCCTCAGGCTTGGGTCTTGT-3′; reverse 5′-ATCCTGTGTTGTTGGGCTGG-3′); inducible nitric oxide synthase (iNOS) (forward 5′-CAGCGCTGATGGAAATGTCG-3′; reverse 5′-ATTGTGGCTCGGGTGGATTT-3′); collagen 1 alpha 1 (Col1a1) (forward 5′-TGCTAAAGGTGCCAATGGTG-3′; reverse 5′-GGGACCTTGTACACCACGTT-3′); metallopeptidase inhibitor 1(TIMP1) (forward 5′-CGCTAGAGCAGATACCACGA-3′; reverse 5′-AGCGTCCGAATCCTTTGAGCA-3′) and transforming growth factor, beta 1 (Tgfb1) (forward 5′-GCTGAACCAAGGAGACGGAA-3′; reverse 5′-CCACGTAGTAGACGATGGGC-3′).
ELISAs
Enzyme-linked immunosorbent assays (ELISA) from R&D Systems (Minneapolis, MN, USA) were performed in serum samples according to the manufacturers’ instructions, for determining quantitative levels of TNF-α, IL-6 and total nitric oxide. All samples were tested in duplicate and read in a Sunrise Microplate Reader (Tecan, Mannedorf, Switzerland). Lower limits of detection of all cytokine assays were between 10 and 20 pg/mL. Standard curves were generated for each plate, and the average zero standard optical densities were subtracted from the rest of standards, controls, and samples to obtain a corrected concentration for all cytokines.
Statistical analysis
For indirect management of the plots was carried out an analysis of multidimensional non-metric scaling, NMDS (non-metric multidimensional scaling distance) that uses the matrix of dissimilarity between plots. We clustered separately the three different groups of rats. The first axis (NMDS1) separated treatment with Bifidobacteria CECT7765 from the other groups. The second axis (NMDS2) separated control from cirrhotic rats with BDL. This analysis was performed with phyloseq package of R (version 3.2.2).
The diversity índices of intestinal microbiota, the relative abundance of OTUs, biochemistry values and hemodynamic parameters were compared between three treatment groups by Kruskall–Wallis test. Mann–Whitney U test was used for paired comparisons between treatment groups with the Bonferroni correction for multiple comparisons. An ANCOVA analysis was performed to study the variability components of hemodynamic and liver function variables according to treatment group and relative abundance of OTUs. Significant level was 0.05. Statistical analyses were performed with SPSS (version 22.0).
Results
A total of 25 rats were initially included in the study. Mortality rate in BDL groups was 26.3% (5 out of 19 animals). The five deaths occur prior to bifidobacterial administration. None of the sham-operated rats (n = 6) died before laparotomies. BDL rats were randomly distributed to receive (n = 8) or not (n = 6) B. pseudocatenulatum CECT7765 for 1 week previous to laparotomy. Fibrotic liver damage was confirmed in BDL rats by measuring gene expression levels of profibrogenic markers (Supplementary Fig. 2).
Gut microbiota analysis and sample clustering
We first evaluated the composition of the microbiota community in sham-operated rats, BDL rats and BDL rats treated with B. pseudocatenulatum CECT7765 (Fig. 1). The BDL protocol decreased total mean OTUs of main phyla compared with sham-operated animals, whereas the bifidobacterial treatment in BDL rats significantly increased total mean OTUs of these phyla compared with the other two groups (Fig. 1a). When relative abundance is considered, the BDL treatment increased Firmicutes, Proteobacteria and Actinobacteria phyla while decreased Bacteroidetes phylum compared with sham-operated animals. Differences in Actinobacteria (p = 0.02) and Bacteroidetes (p = 0.01) reached statistical significance. Bifidobacteria treatment significantly increased bacteroidetes (p = 0.01) and reduced Proteobacteria phyla (p < 0.001) compared to BDL-untreated animals (Fig. 1b). Figure 1c shows the main differences in total median OTUs at genus level between bifidobacteria-treated BDL and sham-operated control rats, and Fig. 1d shows the main differences between B. pseudocatenulatum CECT7765 treated vs non-treated BDL rats. Table 1 shows the statistically significant differences in the amount of identified genus between the three groups of rats.
Gut microbiota composition in study groups. a Total mean OTUs of main phyla in the three groups of study. b Relative abundance of main phyla in the three groups of study. c Main differences in total median OTUs at genus level between bifidobacteria-treated BDL and sham-operated control rats. d Main differences in total median OTUs at genus level between B. pseudocatenulatum CECT7765 treated vs non-treated BDL rats. *p = 0.01 between sham-operated and BDL rats; $p ≤ 0.01 between BDL and BDL administered with B. pseudocatenulatum CECT7765. BDL bile duct ligation, OTUs operational taxonomic units
Figure 2a shows the Chao1, Shannon and Simpson scores for microbial diversity. Median Shannon (p = 0.002) and Simpson (p = 0.002) scores were significantly different between sham-operated rats and BDL rats. Median values for all scores in BDL rats treated with bifidobacteria showed partial restoration of the microbial diversity modified by BDL treatment, although this trend was not statistically significant compared with BDL animals. The NMDS analysis of the three different groups of animals is represented in Fig. 2b. The analysis clustered BDL rats treated with the bifidobacterial strain separately from the rest of groups, as determined by the first axis (NMDS1). On the other hand, BDL surgery in rats was not clustered separately from sham-operated rats, as distributed by second axis (NMDS2).
Gut microbiota diversity in study groups. a Alpha diversity scores in all study groups. b Two-dimensional non-metric multidimensional scaling (NMDS) plot of three study groups by taxonomic composition. NDMS1 axis was set to determine distances between animals by B. pseudocatenulatum CECT7765 administration, and NMDS2 axis to determine distances by BDL surgery
The Firmicutes/Bacteroidetes ratio was significantly increased in BDL animals compared with sham-operated rats (1.20 vs 3.18, p = 0.003). The administration of the bifidobacterial strain significantly decreased this ratio (2.21, p = 0.03) compared with BDL rats not receiving B. pseudocatenulatum CECT7765.
Hemodynamic, biochemical and inflammatory parameters in studied animals
When the experimental groups were compared, cirrhosis induction by BDL significantly worsened hemodynamics parameters, as evaluated by ultrasound Doppler imaging, showing an increased portal vein area and portal flow leading to a significantly increased congestion index. The oral administration of the Bifidobacterium strain to BDL rats significantly reduced the portal vein area and the portal flow, resulting in a significantly decreased congestion index (Table 2).
Biochemical markers of liver and metabolic function were analyzed in blood of all included animals between experimental groups and are represented in Table 3. As expected, a significantly reduced liver function is observed in BDL vs sham-operated rats. The administration of B. pseudocatenulatum CECT7765 to BDL rats significantly improved total bilirubin and alkaline phosphatase levels. B. pseudocatenulatum CECT7765 was not able to recover hepatocyte capacity to produce ALT after the induced liver damage. The actual improvement in the rest of parameters did not reach statistical significance. No significant changes in glucose and cholesterol levels were observed in BDL rats after bifidobacterial administration. Bile acids levels were significantly increased in BDL rats compared to controls. The administration of B. pseudocatenulatum CECT7765 did not show a significant reduction in serum bile acid levels.
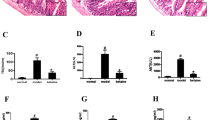
Regarding systemic inflammatory mediators, serum levels of TNF-α, IL-6 and nitric oxide were significantly increased in BDL compared to sham-operated rats. The bifidobacterial administration to BDL rats significantly reduced all three variables (Fig. 3).
Liver gene expression levels of FXR and eNOS were significantly reduced in BDL vs sham-operated rats, while iNOS and COX-2 were significantly upregulated. The administration of B. pseudocatenulatum CECT7765 significantly increased FXR and eNOS gene expression levels in the liver of studied animals, while iNOS and COX-2 were reduced, although this reduction did not reach statistical significance (Fig. 4).
Gene expression levels of FXR, eNOS, iNOS and COX-2 in the livers of animals in different study groups. FXR farnesoid X receptor, eNOS endothelial nitric oxide synthase, iNOS inducible nitric oxide synthase, COX-2 cyclo-oxygenase 2. *p ≤ 0.01 compared with sham-operated group: $p ≤ 0.01 compared with BDL rats
Correlation between changes in gut microbiota induced by B. pseudocatenulatum CECT7765 and hemodynamic and liver function parameters in BDL rats.
The congestion index correlated with the total OTUs of Lactobacillus (r = 0.800; p = 0.01) and Proteobacteria (r = 0.725; p = 0.03) when comparing sham-operated vs BDL rats. When BDL rats were compared according to the administration of B. pseudocatenulatum CECT7765, OTUS from several firmicutes like Allobaculum, Lactococcus and the Erysipelotrichaceae family and Proteobacteria phylum inversely correlated with the congestion index. Supplementary Table 1 shows all significant correlations between different hemodynamic parameters and total OTUS of genus in animals comparing BDL vs sham-operated rats and BDL rats treated or not with the bifidobacterial strain.
Among genus modified by the administration of B. pseudocatenulatum CECT7765 in BDL rats, Table 4 shows the genus which total OTUs variations are independently associated with hemodynamic changes, according to the ANCOVA analysis. Quantitative changes in the Clostridiales and Bacteroidales classes were independently associated with variations in portal vein area and portal flow. In the case of congestion, only changes in the Proteobacteria phylum caused by the administered bifidobacterial strain remained significant and independent.
Variations in all liver function biochemical markers between BDL and sham-operated rats, and between BDL rats according to the administration of B. pseudocatenulatum CECT7765, significantly correlated with total OTUs changes in the Clostridiales class. All correlations are described in Supplementary Table 2. However, only quantitative changes in the Clostridiales class were independently associated with variations in ALP levels in the ANCOVA analysis (Table 5). Regarding metabolic biochemical markers, only variations in total bile acids correlated with total OTUs changes in Clostridiales, Lactobacillales and γ-Proteobacteria classes in the ANCOVA analysis (Table 6). All significant bivariate correlations between quantitative changes in different genus and total bile acids are shown in Supplementary Table 3.
Discussion
In the present study, we show that hemodynamic alterations and liver dysfunction in induced cirrhotic rats by bile duct ligation are partially restored after oral administration of B. pseudocatenulatum CECT7765. The increased gene expression levels of FXR and eNOS in the liver of BDL rats treated with the bifidobacterial strains suggests a beneficial effect on these parameters through modulation of bile acids metabolism and endothelial dysfunction. Results presented herein provide a proof-of-concept to design further studies on the effects of the bifidobacterial strain in reducing the complications derived from portal hypertension in cirrhosis.
Cirrhosis is the common end-stage liver histologic distortion for several hepatic diseases, characterized by generalized progressive systemic vasodilatation, related to portal hypertension. This fact in turn alters intestinal motility inducing intestinal bacterial overgrowth [31, 32], one of the proposed mechanisms of bacterial translocation in cirrhosis [33, 34]. Translocation of gut-derived bacterial products to the mesenteric lymph nodes and systemic circulation triggers the activation of immune effectors in the mucosal and mesenteric lymphoid tissues increasing the synthesis and vascular release of nitric oxide [34,35,36]. Indeed, TNF-α is known to be involved in the pathogenesis of the hyperdynamic circulatory syndrome in portal hypertension [37, 38], in impairing liver function and in contributing to hemostatic failure [39]. Thus, reducing bacterial translocation to decrease the excessive oxidative stress and/or the increased vasodilator factors is an interesting approach to improve the general vascular dysfunction in portal hypertension. In this context, B. pseudocatenulatum CECT7765 has shown to reduce gut permeability and bacterial translocation episodes into MLNs of mice with CCl4-induced cirrhosis [16]. However, the impact of this intervention on gut microbiota content and, of utmost relevance, on liver vascular function remained to be elucidated.
In our model, changes in the clostridiales and bacteroidales were independently associated with hemodynamic variations in portal flow and portal vein area, which in turn, may explain the amelioration in the congestion index of BDL rats receiving the bifidobacterial strain. These results can be interpreted considering that only variations in certain classes are enough to show an effect on hemodynamics while other clusters are not involved, or show a residual effect, in liver function. Previous studies using VSL#3 have shown results in this same line. Gupta et al. demonstrated its significant beneficial effect of when added to propranolol, increasing the hepatic venous pressure gradient (HVPG) response rate compared to propranolol alone from 31 to 58%, in a large double-blind, placebo-controlled study [13]. In a recent study in cirrhotic patients, the oral administration of VSL#3 resulted in reductions of the HVPG, cardiac index and heart rate, and in increases of the systemic vascular resistance and mean arterial pressure [40].
Additional evidences support the relationship between gut microbiota changes and hemodynamic alterations. The increase in the Firmicutes/Bacteroidetes ratio, a well-established marker of gut dysbiosis in numerous pathologies [41], is increased in spontaneously hypertensive rats, and in a small group of humans with essential hypertension [42]. Also, the administration of magnesium acetate (200 mmol/L in drinking water) to hypertensive rats decreases the gut dysbiosis, measured by the ratio Firmicutes/Bacteroidetes, preventing the development of hypertension and heart failure [43]. In our study, we observe an increment in the Firmicutes/Bacteroidetes ratio in BDL animals and, interestingly, a decrease after administration of B. pseudocatenulatum CECT7765. Along with the inverse correlation observed between congestion index and the total OTUs of allobaculum, these results support a vascular benefit of the intervention through gut microbiota modification in BDL animals. In fact, species such as allobaculum produce short-chain fatty acid (SCFA) [44], to which both epithelial cells and neutrophils have specific receptors [45], and that induce nuclear factor kappa (NFκ)-B blockade [46]. Its depletion in BDL rats may favor inflammation, mucosal damage or colonocyte starvation [47, 48].
Our second aim was to evaluate the relationship between gut microbiota modification and biochemical liver function. The possibility of reducing liver inflammation and ameliorating functional markers has been reported in ob/ob mice [49] and in nonalcoholic steatohepatitis-related cirrhotics using VSL#3 [50]. The B. pseudocatenulatum CECT7765-induced increment in the Clostridiales class was independently associated with a significant reduction in ALP levels. This enzyme, as well as gamma glutamyl transferase, is typically increased in cholestasis, reflecting the biliary damage [51]. This would suggest that the bifidobacterial strain, through induction of gut microbiota composition changes, is able to reduce the cholestatic damage in BDL rats.
A possible mechanism explored herein may involve, on one hand, the bile acids receptor FXR. In cirrhosis, low bile acids levels are associated with increased inflammation and fibrosis, and may account for gut-derived bacterial translocation [52,53,54]. The partial gut microbiota restoration induced by the bifidobacteria may reduce these negative events during disease and slow down its progression. Supporting these results, gene expression levels of FXR at short-term in the liver of BDL mice are significantly decreased compared to sham-operated animals [55], and the lack of FXR in mice induces an enhanced renal removal of bile acids in mice [56]. On the second hand, gene expression levels of eNOS are significantly increased in the liver of BDL rats treated with the bifidobacterial strain. Reduced intrahepatic eNOS activity is a major contributor of endothelial dysfunction leading to portal hypertension [57]. The significant reduction of serum inflammatory cytokines levels in BDL rats after administration of the bifidobacteria would also support its role in improving endothelial dysfunction, which is aggravated by inflammation [58].
Including the present study, a considerable amount of evidence has been collected by now regarding the beneficial effect of B. pseudocatenulatum CECT7765 on experimental liver damage. The bifidobacterial strain has been described to reduce gut permeability, bacterial translocation and inflammation [16, 59], and we offer now results supporting its effect on improving hemodynamic and liver function markers. Moreover, the use of the bifidobacterial strain has shown to drive in vitro a transition in macrophages from ascitic fluid of patients with cirrhosis towards an anti-inflammatory profile without reducing their phagocytic capacity [17]. Although partially evaluated in all these studies with positive results, a specifically designed study on safety would be required before evaluating the use of this promising bifidobacterial strain in human clinical studies.
In summary, we provide evidence that oral intervention with B. pseudocatenulatum CECT7765 in BDL rats promotes the improvement of hemodynamic and liver function parameters associated with the modification of the gut microbiota content in portal hypertensive cirrhotic rats. The observed effect of the bifidobacterial strain on liver FXR and eNOS expression as a possible mechanism for inducing such beneficial effects will require further studies.
References
Bosch J, Pizcueta P, Feu F, Fernandez M, Garcia-Pagan JC (1992) Pathophysiology of portal hypertension. Gastroenterol Clin N Am 21:1–14
Bataller R, Brenner DA (2005) Liver fibrosis. J Clin Invest 115:209–218
Colombato LA, Albillos A, Groszmann RJ (1992) Temporal relationship of peripheral vasodilatation, plasma volume expansion and the hyperdynamic circulatory state in portal-hypertensive rats. Hepatology 15:323–328
Fernandez J, Ruiz del Arbol L, Gomez C, Durandez R, Serradilla R, Guarner C et al (2006) Norfloxacin vs ceftriaxone in the prophylaxis of infections in patients with advanced cirrhosis and hemorrhage. Gastroenterology 131:1049–1056 (quiz 1285)
Rimola A, Garcia-Tsao G, Navasa M, Piddock LJ, Planas R, Bernard B et al (2000) Diagnosis, treatment and prophylaxis of spontaneous bacterial peritonitis: a consensus document. Int Ascites Club J Hepatol 32:142–153
Bajaj JS, Ridlon JM, Hylemon PB, Thacker LR, Heuman DM, Smith S et al (2012) Linkage of gut microbiome with cognition in hepatic encephalopathy. Am J Physiol Gastrointest Liver Physiol 302:G168-175
Bajaj JS, Hylemon PB, Ridlon JM, Heuman DM, Daita K, White MB et al (2012) Colonic mucosal microbiome differs from stool microbiome in cirrhosis and hepatic encephalopathy and is linked to cognition and inflammation. Am J Physiol Gastrointest Liver Physiol 303:G675-685
Chen Y, Yang F, Lu H, Wang B, Chen Y, Lei D et al (2011) Characterization of fecal microbial communities in patients with liver cirrhosis. Hepatology 54:562–572
Morencos FC, de las Heras Castano G, Martin Ramos L, Lopez Arias MJ, Ledesma F, Pons Romero F (1995) Small bowel bacterial overgrowth in patients with alcoholic cirrhosis. Digest Dis Sci 40:1252–1256
Pande C, Kumar A, Sarin SK (2009) Small-intestinal bacterial overgrowth in cirrhosis is related to the severity of liver disease. Aliment Pharmacol Ther 29:1273–1281
Bauer TM, Steinbruckner B, Brinkmann FE, Ditzen AK, Schwacha H, Aponte JJ et al (2001) Small intestinal bacterial overgrowth in patients with cirrhosis: prevalence and relation with spontaneous bacterial peritonitis. Am J Gastroenterol 96:2962–2967
Chang CS, Chen GH, Lien HC, Yeh HZ (1998) Small intestine dysmotility and bacterial overgrowth in cirrhotic patients with spontaneous bacterial peritonitis. Hepatology 28:1187–1190
Gupta N, Kumar A, Sharma P, Garg V, Sharma BC, Sarin SK (2013) Effects of the adjunctive probiotic VSL#3 on portal haemodynamics in patients with cirrhosis and large varices: a randomized trial. Liver Int 33:1148–1157
Rahimi RS, Rockey DC (2012) Complications of cirrhosis. Curr Opin Gastroenterol 28:223–229
Wiest R, Chen F, Cadelina G, Groszmann RJ, Garcia-Tsao G (2003) Effect of Lactobacillus-fermented diets on bacterial translocation and intestinal flora in experimental prehepatic portal hypertension. Dig Dis Sci 48:1136–1141
Moratalla A, Gomez-Hurtado I, Santacruz A, Moya A, Peiro G, Zapater P et al (2014) Protective effect of Bifidobacterium pseudocatenulatum CECT7765 against induced bacterial antigen translocation in experimental cirrhosis. Liver Int 34:850–858
Moratalla A, Caparros E, Juanola O, Portune K, Puig-Kroger A, Estrada-Capetillo L et al (2016) Bifidobacterium pseudocatenulatum CECT7765 induces an M2 anti-inflammatory transition in macrophages from patients with cirrhosis. J Hepatol 64:135–145
Kountouras J, Billing BH, Scheuer PJ (1984) Prolonged bile duct obstruction: a new experimental model for cirrhosis in the rat. Br J Exp Pathol 65:305–311
Wu MJ, Chen M, Sang S, Hou LL, Tian ML, Li K et al (2017) Protective effects of hydrogen rich water on the intestinal ischemia/reperfusion injury due to intestinal intussusception in a rat model. Med Gas Res 7:101–106
Claesson MJ, Wang Q, O’Sullivan O, Greene-Diniz R, Cole JR, Ross RP et al (2010) Comparison of two next-generation sequencing technologies for resolving highly complex microbiota composition using tandem variable 16S rRNA gene regions. Nucleic Acids Res 38:e200
Schloss PD, Westcott SL, Ryabin T, Hall JR, Hartmann M, Hollister EB et al (2009) Introducing mothur: open-source, platform-independent, community-supported software for describing and comparing microbial communities. Appl Environ Microbiol 75:7537–7541
Kozich JJ, Westcott SL, Baxter NT, Highlander SK, Schloss PD (2013) Development of a dual-index sequencing strategy and curation pipeline for analyzing amplicon sequence data on the MiSeq Illumina sequencing platform. Appl Environ Microbiol 79:5112–5120
Pruesse E, Quast C, Knittel K, Fuchs BM, Ludwig W, Peplies J et al (2007) SILVA: a comprehensive online resource for quality checked and aligned ribosomal RNA sequence data compatible with ARB. Nucleic Acids Res 35:7188–7196
Edgar RC, Haas BJ, Clemente JC, Quince C, Knight R (2011) UCHIME improves sensitivity and speed of chimera detection. Bioinformatics 27:2194–2200
Cole JR, Wang Q, Fish JA, Chai B, McGarrell DM, Sun Y et al (2014) Ribosomal database project: data and tools for high throughput rRNA analysis. Nucleic Acids Res 42:D633–642
Evans J, Sheneman L, Foster J (2006) Relaxed neighbor joining: a fast distance-based phylogenetic tree construction method. J Mol Evol 62:785–792
Matsuki T, Watanabe K, Fujimoto J, Miyamoto Y, Takada T, Matsumoto K et al (2002) Development of 16S rRNA-gene-targeted group-specific primers for the detection and identification of predominant bacteria in human feces. Appl Environ Microbiol 68:5445–5451
Matsuki T, Watanabe K, Fujimoto J, Takada T, Tanaka R (2004) Use of 16S rRNA gene-targeted group-specific primers for real-time PCR analysis of predominant bacteria in human feces. Appl Environ Microbiol 70:7220–7228
Santacruz A, Collado MC, Garcia-Valdes L, Segura MT, Martin-Lagos JA, Anjos T et al (2010) Gut microbiota composition is associated with body weight, weight gain and biochemical parameters in pregnant women. Br J Nutr 104:83–92
Seitz BM, Krieger-Burke T, Fink GD, Watts SW (2016) Serial measurements of splanchnic vein diameters in rats using high-frequency ultrasound. Front Pharmacol 7:116
Guarner C, Runyon BA, Young S, Heck M, Sheikh MY (1997) Intestinal bacterial overgrowth and bacterial translocation in cirrhotic rats with ascites. J Hepatol 26:1372–1378
Guarner C, Soriano G (2005) Bacterial translocation and its consequences in patients with cirrhosis. Eur J Gastroenterol Hepatol 17:27–31
Berg RD (1992) Bacterial translocation from the gastrointestinal tract. J Med 23:217–244
Wiest R, Garcia-Tsao G (2005) Bacterial translocation (BT) in cirrhosis. Hepatology 41:422–433
Wiest R, Groszmann RJ (2002) The paradox of nitric oxide in cirrhosis and portal hypertension: too much, not enough. Hepatology 35:478–491
Theodorakis NG, Wang YN, Skill NJ, Metz MA, Cahill PA, Redmond EM et al (2003) The role of nitric oxide synthase isoforms in extrahepatic portal hypertension: studies in gene-knockout mice. Gastroenterology 124:1500–1508
Quigley EM (1996) Gastrointestinal dysfunction in liver disease and portal hypertension. Gut-liver interactions revisited. Dig Dis Sci 41:557–561
Lopez-Talavera JC, Merrill WW, Groszmann RJ (1995) Tumor necrosis factor alpha: a major contributor to the hyperdynamic circulation in prehepatic portal-hypertensive rats. Gastroenterology 108:761–767
Thalheimer U, Triantos CK, Samonakis DN, Patch D, Burroughs AK (2005) Infection, coagulation, and variceal bleeding in cirrhosis. Gut 54:556–563
Rincon D, Vaquero J, Hernando A, Galindo E, Ripoll C, Puerto M et al (2014) Oral probiotic VSL#3 attenuates the circulatory disturbances of patients with cirrhosis and ascites. Liver Int 34:1504–1512
Everard A, Cani PD (2013) Diabetes, obesity and gut microbiota. Best Pract Res Clin Gastroenterol 27:73–83
Yang T, Santisteban MM, Rodriguez V, Li E, Ahmari N, Carvajal JM et al (2015) Gut dysbiosis is linked to hypertension. Hypertension 65:1331–1340
Marques FZ, Nelson E, Chu PY, Horlock D, Fiedler A, Ziemann M et al (2017) High-fiber diet and acetate supplementation change the gut microbiota and prevent the development of hypertension and heart failure in hypertensive mice. Circulation 135:964–977
Zhang X, Zhao Y, Xu J, Xue Z, Zhang M, Pang X et al (2015) Modulation of gut microbiota by berberine and metformin during the treatment of high-fat diet-induced obesity in rats. Sci Rep 5:14405
Sina C, Gavrilova O, Forster M, Till A, Derer S, Hildebrand F et al (2009) G protein-coupled receptor 43 is essential for neutrophil recruitment during intestinal inflammation. J Immunol 183:7514–7522
Kumar A, Wu H, Collier-Hyams LS, Kwon YM, Hanson JM, Neish AS (2009) The bacterial fermentation product butyrate influences epithelial signaling via reactive oxygen species-mediated changes in cullin-1 neddylation. J Immunol 182:538–546
Maslowski KM, Vieira AT, Ng A, Kranich J, Sierro F, Yu D et al (2009) Regulation of inflammatory responses by gut microbiota and chemoattractant receptor GPR43. Nature 461:1282–1286
De Filippo C, Cavalieri D, Di Paola M, Ramazzotti M, Poullet JB, Massart S et al (2010) Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. Proc Natl Acad Sci USA 107:14691–14696
Li Z, Yang S, Lin H, Huang J, Watkins PA, Moser AB et al (2003) Probiotics and antibodies to TNF inhibit inflammatory activity and improve nonalcoholic fatty liver disease. Hepatology 37:343–350
Loguercio C, Federico A, Tuccillo C, Terracciano F, D’Auria MV, De Simone C et al (2005) Beneficial effects of a probiotic VSL#3 on parameters of liver dysfunction in chronic liver diseases. J Clin Gastroenterol 39:540–543
Giannini EG, Testa R, Savarino V (2005) Liver enzyme alteration: a guide for clinicians. CMAJ 172:367–379
Inagaki T, Moschetta A, Lee YK, Peng L, Zhao G, Downes M et al (2006) Regulation of antibacterial defense in the small intestine by the nuclear bile acid receptor. Proc Natl Acad Sci USA 103:3920–3925
Verbeke L, Farre R, Verbinnen B, Covens K, Vanuytsel T, Verhaegen J et al (2015) The FXR agonist obeticholic acid prevents gut barrier dysfunction and bacterial translocation in cholestatic rats. Am J Pathol 185:409–419
Lorenzo-Zuniga V, Bartoli R, Planas R, Hofmann AF, Vinado B, Hagey LR et al (2003) Oral bile acids reduce bacterial overgrowth, bacterial translocation, and endotoxemia in cirrhotic rats. Hepatology 37:551–557
Park YJ, Qatanani M, Chua SS, LaRey JL, Johnson SA, Watanabe M et al (2008) Loss of orphan receptor small heterodimer partner sensitizes mice to liver injury from obstructive cholestasis. Hepatology 47:1578–1586
Marschall HU, Wagner M, Bodin K, Zollner G, Fickert P, Gumhold J et al (2006) Fxr(−/−) mice adapt to biliary obstruction by enhanced phase I detoxification and renal elimination of bile acids. J Lipid Res 47:582–592
Thabut D, Massard J, Gangloff A, Carbonell N, Francoz C, Nguyen-Khac E et al (2007) Model for end-stage liver disease score and systemic inflammatory response are major prognostic factors in patients with cirrhosis and acute functional renal failure. Hepatology 46:1872–1882
Vairappan B (2015) Endothelial dysfunction in cirrhosis: Role of inflammation and oxidative stress. World J Hepatol 7:443–459
Moratalla A, Gomez-Hurtado I, Moya-Perez A, Zapater P, Peiro G, Gonzalez-Navajas JM et al (2016) Bifidobacterium pseudocatenulatum CECT7765 promotes a TLR2-dependent anti-inflammatory response in intestinal lymphocytes from mice with cirrhosis. Eur J Nutr 55:197–206
Funding
This work has been partially funded by Grants PI16/0967 from Instituto de Salud Carlos III, Madrid, Spain, PROMETEO/2016/001 from Generalitat Valenciana, Valencia, Spain, by FEDER funds and by the European Union’s Seventh Framework Program under the grant agreement no 613979 (MyNewGut).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gómez-Hurtado, I., Zapater, P., Portune, K. et al. Improved hemodynamic and liver function in portal hypertensive cirrhotic rats after administration of B. pseudocatenulatum CECT 7765. Eur J Nutr 58, 1647–1658 (2019). https://doi.org/10.1007/s00394-018-1709-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-018-1709-y