Abstract
Objective
The incidence of scrotal migration of a ventriculoperitoneal shunt (VPS) catheter is rare and may lead to life-threatening visceral complications. Management requires prompt removal of the migrated portion of the shunt and closure of the scrotal sac. We report an interesting case of a young child who presented with asymptomatic unilateral swelling of his scrotum secondary to a migrated VPS catheter. A repeat X-ray prior to his surgery to remove the migrated catheter showed that the entire length of the distal VPS catheter was back in the peritoneal cavity. In view of this unusual phenomenon, the case is discussed in corroboration with published literature.
Methods and results
A systematic search of publications in the English language is performed in PubMed and Google Scholar. Our findings show that there are 49 reported cases (including our patient) of scrotal migration of shunt catheters in patients less than 18 years old. There is only 1 other case of spontaneous resolution of shunt catheter from the scrotum. Favoured management of choice is repositioning the distal shunt catheter back into the peritoneal cavity and herniotomy in the same setting, if possible. Overall, the literature suggests this is a shunt-related complication that has a good prognosis if intervention is timely.
Conclusion
Scrotal migration of a VPS catheter is a rare but potentially life-threatening complication in children. Our case report highlights the role of updated preoperative imaging and the need for consistent long-term shunt surveillance in children.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neonatal hydrocephalus is an extremely common condition managed by paediatric neurosurgeons. To date, the ventriculoperitoneal shunt (VPS) is the most established method of cerebrospinal fluid (CSF) diversion for lifesaving measures [1]. Nonetheless, the VPS remains imperfect, and implant-related morbidities are still prevalent worldwide [1, 2]. One such example is the migration of the distal end of the VPS catheter into the scrotum—a rare complication that has been infrequently described in the literature at the time of this writing [3, 4]. At the time of this writing, there is a paucity of literature describing the spontaneous regression of a migrated VPS catheter from the scrotum back into the peritoneal cavity. We present a case of a child who initially presented with scrotal migration of his VPS catheter and subsequently had spontaneous regression of the catheter back into his peritoneum. Given the infrequency of this phenomenon, this unique case is discussed in corroboration with current literature and management strategies.
Historical background
In 1983, Croffort and Balsam reported the first case series of 4 children presenting with migration of the distal VPS tip through the patent process vaginalis (PV) [5]. Of note, this is the period in neurosurgery whereby VPS is replacing ventriculoatrial shunt as the procedure of choice owing to its comparatively lower complication and revision rates for CSF diversion in children [5]. Although significant progress has been made in implant biomaterials and perioperative sterility practices, shunt complications are still major public health challenges [1, 6, 7]. In children, scrotal migration of the distal end of the VPS catheter is a rare complication that has been limited to case reports and small series in the literature [3,4,5, 8, 9]. Management usually involves prompt removal of the distal catheter from the scrotal sac to avoid serious sequelae such as scrotal oedema, acute scrotum, scrotal perforation, incarcerated hernia, shunt extrusion, and CSF leak from scrotum [3, 10,11,12]. To identify articles pertinent to our topic of interest, a systematic search of publications in the English language according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines is performed [13]. Patients aged 18 years old and above are excluded from the review, as we are primarily interested in the condition’s incidence in children.
Diagnosis and management
The PV is a blind-ended evagination of the abdominal wall that develops during fetal life and typically undergoes obliteration in early life [10]. Persistence of PV is associated with a spectrum of pathologies, including congenital indirect inguinal hernias, communicating hydroceles, funicular and encysted hydroceles, canal of Nuck cysts, and acquired undescended testis [10]. A patent PV is reported to be more prevalent in premature infants [14]. Broadly speaking, asymptomatic scrotal swelling in young males is not uncommon, and the physiological obliteration of a male PPV is typically completed by 2 years old [10]. However, patent PVs have been reported to be present in up to 40% of males between 2 and 16 years old [10]. Most of the time, scrotal swelling in young children is likely secondary to a hydrocoele caused by a collection of fluid within a patent PV. Regardless, the discovery of an onset of scrotal swelling warrants early medical evaluation for diagnosis to guide the next step of treatment.
Separately, several theories exist with regard to the mechanism of scrotal migration in VPS. The most accepted theory is that VPS implantation results in an increase in intra-abdominal pressure, resulting in the prolonged patency of the PV [3]. In addition, the smaller size of a young child’s peritoneal cavity compared to adults has been postulated to be a risk factor for VPS migration into a patent PV. For a male patient with a VPS in situ, the presence of a patent PV predisposes him to the herniation of a distal VPS catheter into the scrotum, especially within the first year of insertion. One of the salient concerns is that the skin sac (also known as the dartos fascia) overlying the scrotum is thin [3, 15] and hence, it has the theoretical risk of perforation if there is pressure from prolonged implant contact, excess CSF accumulation, or both. Under such circumstances, concurrent surgical repositioning of the VPS and obliteration of the patent PV are recommended to prevent further complications and malfunctioning of the shunt [3, 10].
Prognosis and outcomes
Overall, the incidence of scrotal shunt migration in the paediatric age group remains uncommon, with varying estimates up to approximately 3.7% [3, 11, 16, 17]. Our literature review combines selected cases from a recent systematic review by Hauser et al. and subsequent case reports to date [3, 8, 11, 18] (Table 1). At this juncture, we want to highlight that there are limitations to our literature review as the patient numbers are modest and, therefore, our findings are, at best, descriptive. Based on our results, there are 49 reported cases (including our patient) of scrotal migration of shunt catheters in patients less than 18 years old. We included a case report of a 2-month-old infant whereby this complication developed very early post-operatively and spontaneously resolved [18]. Pertinent differences between this case and ours include the age (2 months old versus 24 months old) and the time interval between VPS insertion and scrotal migration of its catheter (5 days versus 18 months). This is significant as the patent PV is theoretically obliterated by 2 years old [10]—thereby reducing the risks of this particular VPS complication. Of interest, the incidence of right-sided scrotal migration of VPS catheters is also higher (76.9%). Despite its potentially worrisome sequelae, scrotal shunt migration has a good prognosis when timely surgical intervention is initiated. Recommendations are for hernia repair in addition to repositioning the migrated shunt catheter [3]. Figure 1 is a pictorial representation of our literature review.
A Pie chart illustrating breakdown of total number of published cases based on patients aged less than 2 years old versus those who are older. Based on the literature review, the main risk factor for scrotal migration of VPS catheter is the presence of a patent PV. Overall, management of these patients are similar—which is removal of the catheter from the scrotal sac and PPV closure. B Pie chart illustrating that majority of cases reports that the right scrotum is more frequent in cases of VPS catheter migration
Exemplary case description
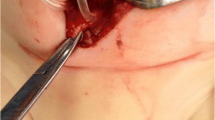
A 2-year-old male with a background of prematurity, non-immune foetal hydrops, and congenital hydrocephalus had a VPS insertion at 6 weeks old. He was otherwise progressing well with regard to his developmental milestones. During an outpatient review for VPS surveillance, his parents mentioned that the patient had asymptomatic, bilateral scrotal swelling. A referral to the paediatric surgery team was initiated. A follow-up groin ultrasound confirmed the diagnosis of bilateral hydroceles. There was no sonographic evidence of hernia incarceration, vascular anomaly, or other suspicious masses. A decision was made for an interval herniotomy when the child was older. However, the patient presented with increased painless, swelling of his right scrotum, especially noticeable when he was crying. There were no symptoms of VPS malfunction. Clinical examination noted a palpable, coiled tubular structure within his right scrotum. An abdominal X-ray reported loops of shunt tubing within the right scrotum, likely herniating through the right inguinal canal. Overall, the impression was that of scrotal migration of the patient’s distal VPS catheter likely through a patent PV (Fig. 2). In view of this finding, the patient was counselled for early surgical intervention to re-place the shunt tubing back into the peritoneal cavity and definitive closure of bilateral PPVs. Owing to an ongoing viral illness, the surgery was listed at 2 weeks from the time of diagnosis. During his elective admission, repeat X-rays were ordered by the neurosurgical team to re-assess the position of the tip of the distal shunt catheter. These demonstrated that no segment of the shunt catheter was visualised in the right scrotum (Fig. 2). Put together, it was likely that the previously migrated catheter in the scrotum had spontaneously been reduced back into the peritoneal cavity. The patient went on to have bilateral herniotomies. Intraoperative findings confirmed both hernia sacs were empty and that the right sac had intussuscepted into the adjacent hydrocele sac. He was discharged home uneventfully on the same day after his surgery (Fig. 3).
A Repeat antero-posterior X-ray of patient’s abdomen in supine position performed just prior to planned surgery. The VPS is intact and no segment of the catheter is seen herniating into the scrotum (white arrow). B Lateral X-ray shows that the tip of the VPS catheter is projected over the left abdomen within the peritoneal cavity (white arrow). No pneumoperioneum is radiologically evident
In the case of our patient, we postulate that the spontaneous regression of the shunt loop from his scrotum back into his peritoneum was likely from a combination of increased intra-abdominal pressure from his preoperative viral upper respiratory tract symptoms causing increased abdominal pressures. Furthermore, this phenomenon illustrated in our patient concurs with the theory that VPS catheter movement within the peritoneum is congruent with increased abdominal pressures. Nevertheless, we are cognizant that our hypothesis requires validation in a real-time setting to be proven. We were fortunate that the child did not have any visceral complications. At the same time, we acknowledge the value of updated imaging to re-evaluate the patient.
Conclusions
We therein report a case of a previously migrated shunt catheter in the scrotum that spontaneously regressed back into the peritoneal cavity more than 1 year after the VPS was inserted. This case contributes to the limited body of literature on this unique complication. Our findings reiterate the need for consistent long-term shunt surveillance in growing children.
Availability of data and materials
All data generated or analysed during this study are included in this published article.
References
Low SYY, Kestle JRW, Walker ML, Seow WT (2023) Cerebrospinal fluid shunt malfunctions: a reflective review. Childs Nerv Syst. https://doi.org/10.1007/s00381-023-06070-4. (Epub ahead of print. PMID: 37462810)
Lim JX, Han HP, Foo YW, Chan YH, Ng LP, Low DCY, Seow WT, Low SYY (2023) Paediatric ventriculoperitoneal shunt failures: 12-year experience from a Singapore children’s hospital. Childs Nerv Syst. https://doi.org/10.1007/s00381-023-06007-x. (Epub ahead of print. PMID: 37284980)
Hauser T, Auer C, Ludwiczek J, Senker W, Rauch PR, Kargl S, Gruber A (2021) Treatment options for scrotal migration of ventriculoperitoneal shunts: case illustration and systematic review of 48 cases. Oper Neurosurg 21:87–93
Nejat F (2018) Scrotal complications of ventriculoperitoneal shunt. Asian J Neurosurg 13:197
Crofford MJ, Balsam D (1983) Scrotal migration of ventriculoperitoneal shunts. AJR Am J Roentgenol 141:369–371
Kraemer MR, Sandoval-Garcia C, Bragg T, Iskandar BJ (2017) Shunt-dependent hydrocephalus: management style among members of the American Society of Pediatric Neurosurgeons. J Neurosurg Pediatr 20:216–224
Stein SC, Guo W (2008) Have we made progress in preventing shunt failure? A critical analysis. J Neurosurg Pediatr 1:40–47
Chanchlani R, Sharma PK, Gunasekaran V, Kasundra A (2023) Scrotal migration of peritoneal end of ventriculoperitoneal shunt in an infant - a rare entity. J Neurosci Rural Pract 14:365–367
Kita D, Hayashi Y, Kinoshita M, Ohama K, Hamada J (2010) Scrotal migration of the peritoneal catheter of a ventriculoperitoneal shunt in a 5-year-old male. Case report. Neurol Med Chir (Tokyo) 50:1122–1125
Brainwood M, Beirne G, Fenech M (2020) Persistence of the processus vaginalis and its related disorders. Australas J Ultrasound Med 23:22–29
Topp G, Entezami P, Ambati S, Szewczyk B, Adamo MA (2023) Cerebrospinal fluid leakage from scrotum secondary to ventriculoperitoneal shunt migration. Asian J Neurosurg 18:333–335
Rehm A, Bannister CM, Victoratos G (1997) Scrotal perforation by a ventriculoperitoneal shunt. Br J Neurosurg 11:443–444
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62:e1–e34
Acer-Demir T, Ekenci BY, Özer D, Turanoğlu MA, Haberal KC, Bilgin EB, Hiçsönmez A (2018) Natural history and conservative treatment outcomes for hydroceles: a retrospective review of one center’s experience. Urology 112:155–160
Jacob S (2008) Chapter 4 - Abdomen. In: Jacob S (ed) Human Anatomy. Churchill Livingstone, pp 71–123
Oktem IS, Akdemir H, Koç K, Menkü A, Tucer B, Selçuklu A, Turan C (1998) Migration of abdominal catheter of ventriculoperitoneal shunt into the scrotum. Acta Neurochir (Wien) 140:167–170
Bawa M, Garge S, Garg R, Narasimha Rao KL (2017) Scrotal migration of tubing: an unusual complication after ventriculo-peritoneal shunt. Asian J Neurosurg 12:738–740
Alkhudari A, Galal M, Wagley Z, Sabbah BN, Houdane A, Aljabr A (2022) A case of spontaneous resolution of a scrotal ventriculoperitoneal shunt migration. Radiol Case Rep 17:3620–3623
Funding
We report no funding, financial support, or industrial affiliations received for the writing of this article.
Author information
Authors and Affiliations
Contributions
All authors have read and approved the manuscript. Conceptualization: YW and SYYL. Data curation: YC, LPN and SYYL. Formal analysis: YC and SYYL. Investigation: YW, LPN, SYYL. Methodology: SYYL. Project administration: YW, YC and LPN. Resources: SYYL. Validation: SYYL. Writing – original draft: YW, SYYL. Writing – review & editing: SYYL.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethics approval is provided by the hospital ethics review board (reference: SingHealth CIRB 2020/2416). The participants and/or their legal guardians signed a written consent for this study.
Consent for publication
The consent to publish has been included as part of the study consent.
Conflict of interest
The authors declare no competing interests.
Disclaimer
The authors certify that this manuscript is a unique submission and is not being considered for publication, in part or in full, with any other source in any medium. All authors made substantial contributions to the manuscript and approved its final version.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, Y., Chen, Y., Ng, L.P. et al. Spontaneous regression of migrated ventriculoperitoneal shunt catheter from scrotum to peritoneum: a case-based review. Childs Nerv Syst 40, 19–25 (2024). https://doi.org/10.1007/s00381-023-06192-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-023-06192-9