Abstract
Objectives
To investigate whether there was an optimal interim size reduction (iΔSPD) cutoff value that could discriminate diffuse large B cell lymphoma (DLBCL) patients with poor prognosis.
Methods
This retrospective study enrolled 265 newly diagnosed DLBCL patients with baseline and interim (after 3 cycles) contrast-enhanced computed tomographic scan (CECT) available. Two radiologists evaluated CECT images and selected target lesions according to the Lugano Response Criteria. Lymph nodes greater than 15 mm in longest diameter (LDi) and extra-nodal lesions with LDi greater than 10 mm could be chosen as target lesions and used to calculate iΔSPD. A software tool, X-Tile, was used to calculate the optimal iΔSPD cutoff value to differentiate patients with good vs. poor prognosis. Receiver operating characteristic curve analysis, Cox regression analysis, and Kaplan–Meier analyses were further used to validate the optimal cutoff value.
Results
The optimal cutoff value of iΔSPD calculated by X-tile was 80%. Compared with 50% and 100%, 80% cutoff value had the intermediate sensitivity and specificity (57.75% and 86.69% for overall survival (OS), 48.98% and 92.22% for progression-free survival (PFS), respectively), but the maximal Youden index (0.4744 for OS, 0.4120 for PFS, respectively) and areas under the curve (0.737 [0.680, 0.789] for OS). Cox regression analysis also revealed that iΔSPD < 80% could independently predict an inferior OS and PFS (both p < 0.001) while neither iΔSPD < 50% nor iΔSPD = 100% could.
Conclusions
iΔSPD with the cutoff value 80% is an independent predictor of PFS and OS for patients with DLBCL. Results suggest that treatment should be modified for patients with iΔSPD < 80%.
Key Points
• The aim of interim response assessment is to identify patients whose disease has not responded to or has progressed on induction therapy.
• A cutoff value of 80% in size reduction (ΔSPD) is an independent predictor of PFS and OS for DLBCL patients and is better than 50%.
• In DLBCL patients with interim ΔSPD < 80%, a change to a more efficient therapy should be considered.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Diffuse large B cell lymphoma (DLBCL) is the most common lymphoid malignancy in adults, accounting for approximately 32.5% of non-Hodgkin lymphomas diagnosed annually [1]. In spite of the inspiring achievements in the treatment of DLBCL since adding rituximab (R) to CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone) [2], about 30% of patients experience disease relapse or refractory to induction therapy. Thus, it is crucial to seek an efficient method that could early identify high-risk DLBCL patients who may benefit from a prompt therapy change.
Interim response assessment is performed to identify patients whose disease has not responded to or has progressed on induction therapy. The Lugano Response Criteria has been widely used for interim response assessment for DLBCL [3]. Based on it, patients with interim reduction percentage of the sum of the products of the greatest perpendicular diameters for multiple lesions (iΔSPD) between baseline and interim contrast-enhanced (CE) computed tomographic (CT) scan less than 50% are regarded as non-sensitive to induction therapy and may benefit from a prompt therapy change. However, the prognosis of patients with iΔSPD ≥ 50% was not always promising either. Actually, there is no consensus on the criteria for early therapy change during interim response assessment yet, which led us to investigate whether there was an iΔSPD cutoff value that could discriminate DLBCL patients with poor prognosis. To the best of our knowledge, no data has been published until now.
Materials and methods
Ethics
The study was approved by the Ethics Committee of the First Affiliated Hospital of Nanjing Medical University. Informed consent and permissions were obtained from all the subjects involved in this study at the time of first DLBCL admission.
Patients
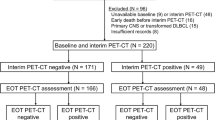
Two hundred and sixty-five subjects with newly diagnosed DLBCL between August 2009 and November 2017 from the First Affiliated Hospital of Nanjing Medical University were enrolled in this single-center retrospective study if both baseline and interim CECT scans were performed and no malignancy other than DLBCL was present at the time of examination. Patients diagnosed with high-grade B cell lymphoma, primary mediastinal large B cell lymphoma, and primary central nervous system lymphoma were excluded. All patients were treated with R-CHOP.
Data collection
Baseline clinical characteristics and laboratorial data including age, gender, serum lactate dehydrogenase (LDH) level, Ann Arbor stage, extra-nodal site involvement, Eastern Cooperative Oncology Group (ECOG) score, B symptoms, the Hans classification of germinal center B cell–like (GCB) or non-GCB, and Ki-67 of the immunohistochemistry were collected from medical records and hospital-based laboratory service.
CECT imaging technique
Whole body CECT inclusive of the neck, thorax, and abdomen/pelvis was performed using a 64-row multidetector CT scanner (Sensation 64; Siemens). Intravenous non-ionic iodinated contrast (ioversol, 320 mgI/mL, HengRui Medicine Ltd.) was administered via the antecubital vein by a double-cylinder high-pressure syringe at a flow rate of 2.5–3.0 mL/s. A total of 80–120 mL of contrast agent was injected, followed by 40 mL of normal saline at a flow rate of 3.0 mL/s. Each patient was scanned using the same parameters: 120 kV voltage, 180 mAs current, pitch of 0.8, 256 × 256 matrix, and slice thickness of 5 mm. Arterial-phase thoracic CT was done in deep inhalation with a delay of 35 s, followed by portal-phase abdominal CT with a delay of 65–70 s scanning from the top of the liver to the thighs. Ultimately, scanning from the bottom of the skull to the supraclavicular region with a delay of 90 s was done. A baseline whole body CECT was performed within 28 days before the start of treatment. An interim whole body CECT was performed after 3 courses of chemotherapy.
CECT imaging analysis
Two radiologists with more than 10 years of experience who were unaware of clinical findings and outcomes evaluated all CT images independently on a picture archiving and communication system (PACS; Medvis), and recorded the number, size, and location of nodal and extra-nodal lesions. Then the two radiologists selected target lesions strictly according to the Lugano Response Criteria [3] together. Any discrepancies in interpretation between two radiologists were resolved by consensus. Lymph nodes greater than 15 mm in longest diameter (LDi) and extra-nodal lesions with LDi greater than 10 mm could be considered measurable lesions and used to calculate SPD. At most six of the largest target nodes, nodal masses or other lymphomatous lesions that are measurable in LDi and shortest diameter were selected from disparate body regions representative of the patient’s overall disease burden and mediastinal and retroperitoneal disease sites were included, if involved. Measurable extra-nodal diseases such as hepatic nodules were included in the six target lesions. All the remaining lesions were considered non-measured lesions.
Statistical analyses
Cutoff value was determined by use of X-tile [4], a software tool that can divide tumors into subgroups based on the expression level of clinical parameters. By inputting the survival time, survival status, and expression level of the clinical parameters studied, the software can automatically give the optimal cutoff value. Receiver operating characteristic (ROC) curve analysis and Cox proportional hazards regression analysis were further used to validate the optimal cutoff value. Statistical analyses were performed using the SPSS software for Windows (version, 24.0) and MedCalc for Windows, version 15.2.2.0 (MedCalc Software). Progression-free survival (PFS) was defined as interval from diagnosis to first progression or relapse, and overall survival (OS) was defined as interval from diagnosis to death or last follow-up. Survival curves were constructed by the Kaplan–Meier method, and log-rank test was used to test for significant differences. To address the multiple comparisons, a Bonferroni correction was applied. ROC curve analysis and the corresponding areas under the curve (AUCs) were used to assess the predictive accuracy of the cutoff values. Prognostic significances of three iΔSPD cutoff values (50%, 80%, and 100%) and clinical variables (age, gender, International Prognostic Index (IPI) score, LDH level, Ann Arbor stage, extra-nodal sites, ECOG score, B symptoms, the Hans classification, and Ki-67) were assessed by univariate and multivariate Cox proportional hazards regression analysis. The results were evaluated in 95% confidence interval and at a significance level of two-sided p < 0.05.
Results
Patients’ characteristics
Clinical characteristics of the 265 patients were outlined in Table 1. The median age at diagnosis was 58 years (range, 18–88 years), and 111 (41.9%) of them were more than 60 years old. One hundred and thirty-nine patients (52.5%) were male; 100 (37.7%) had an IPI score ≥ 3; 112 (42.3%) had elevated LDH; 179 (67.5%) were at stage III or IV according to the Ann Arbor classification; 78 (29.4%) had more than one extra-nodal sites of involvement; 50 (18.9%) had an ECOG score ≥ 2; 100 (37.7%) had B symptoms. One hundred and seventy-two patients (64.9%) were non-GCB type according to the Hans classification and 10 (3.8%) were unavailable. Ki-67 ≥ 80% were observed in 115 (43.4%) patients and 24 (9.1%) were unavailable.
Selection of the optimal iΔSPD cutoff value
The follow-up results of all 265 patients enrolled in the study were at the end of Nov. 2018 with a median follow-up of 47 months (range, 18 − 111 months). Ninety-eight (37.0%) patients progressed or relapsed and 71 (26.8%) died. In the whole cohort, the estimated 3- and 5-year PFS were 65.2% ± 2.9% and 59.9% ± 3.4%, respectively. The estimated 3- and 5-year OS were 75.2% ± 2.7% and 71.8% ± 3.0%, respectively.
According to the analysis by X-tile, the cutoff value of iΔSPD that yielded the highest difference in OS was 80%. The prognostic values of three cutoff values (100%, 80%, and 50%) were compared using the ROC curves. AUCs of 100%, 80%, and 50% cutoff values were 0.667 [0.606, 0.723] (p < 0.001), 0.737 [0.680, 0.789] (p < 0.001), and 0.641 [0.580, 0.699] (p < 0.001), respectively, when OS was considered the entire follow-up period (Fig. 1).
Sensitivity, specificity, Youden’s index, positive predictive value (PPV), and negative predictive value (NPV) were also used to compare the prognostic values of three cutoffs (Table S1). PPV and NPV of 80% cutoff value were 78.69% and 75.49% for PFS, but 67.21% and 85.29% for OS, respectively. For PFS, the 100% cutoff value had the maximal sensitivity (82.65%), but the minimal specificity (50.90%) and the intermediate Youden index (0.3355). Fifty percent cutoff value had the maximal specificity (95.21%), but the minimal sensitivity and Youden index (23.50% and 0.1871, respectively). Although the sensitivity and specificity of the 80% cutoff value were intermediate (48.98% and 92.22, respectively), the Youden index (0.4120) was maximal. For OS, which was in line with the result for PFS, the sensitivity and specificity of the 80% cutoff were intermediate (57.75% and 86.69%, respectively) while the Youden index (0.4744) was maximal.
Univariate Cox regression analysis showed that all baseline clinical characteristics except gender were significantly associated with PFS, and all baseline clinical characteristics except gender and number of extra-nodal sites were significantly associated with OS. However, in multivariate Cox regression analysis, only advanced stage and iΔSPD < 80% remained significantly associated with PFS (HR 3.215, 95% CI 1.515–6.825, p = 0.002; HR 4.137, 95% CI 2.321–7.374, p < 0.001; respectively) and OS (HR 4.993, 95% CI 1.759–14.172, p = 0.003; HR 4.988, 95% CI 2.486–10.006, p < 0.001; respectively). Non-GCB type remained significantly associated with OS (HR 2.316, 95% CI 1.136–4.724, p = 0.021) but not with PFS. Notably, iΔSPD < 50% and iΔSPD = 100% were not significant for both PFS and OS anymore (Table 2).
Combining the results of ROC curve analysis and Cox regression analysis, we selected 80% as the optimal cutoff value to compute for further analysis.
Survival analysis of the whole cohort
The whole cohort was divided into 4 groups according to three iΔSPD cutoff values: iΔSPD = 100% group (102 (38.5%)), 80% ≤ iΔSPD < 100% group (102 (38.5%)), 50% ≤ iΔSPD < 80% group (30 (11.3%)), and iΔSPD < 50% group (31 (11.7%)). The iΔSPD = 100% group had significantly superior PFS than the 80% ≤ iΔSPD < 100% group (Bonferroni-corrected p = 0.027), while no statistical significance (Bonferroni-corrected p = 0.21) for OS was observed between them. There were no statistical differences for PFS and OS between the 50% ≤ iΔSPD < 80% group and iΔSPD < 50% groups Bonferroni-corrected (p = 0.741, Bonferroni-corrected p = 0.267, respectively). The 50% ≤ iΔSPD < 80% group had significantly inferior PFS and OS than the 80% ≤ iΔSPD < 100% group (both Bonferroni-corrected p < 0.001) (Fig. 2a, b).
a Kaplan–Meier analyses of progression-free survival according to three iΔSPD cutoff values: (a) p value between the iΔSPD = 100% group and the 80% ≤ iΔSPD < 100% group; (b) p value between the 80% ≤ iΔSPD < 100% group and the 50% ≤ iΔSPD < 80% group; (c) p value between the 50% ≤ iΔSPD < 80% group and the iΔSPD < 50% group. b Kaplan–Meier analyses of overall survival according to three iΔSPD cutoff values: (a) p value between the iΔSPD = 100% group and the 80% ≤ iΔSPD < 100% group; (b) p value between the 80% ≤ iΔSPD < 100% group and the 50% ≤ iΔSPD < 80% group; (c) p value between the 50% ≤ iΔSPD < 80% group and the iΔSPD < 50% group. Log-rank p values are indicated. p values have been adjusted after Bonferroni’s correction
According to the optimal iΔSPD cutoff value 80%, 204 (77.0%) patients were iΔSPD ≥ 80% and 61 (23.0%) were iΔSPD < 80%. Not only did PFS estimation differ between patients with iΔSPD ≥ 80% and iΔSPD < 80% (hazard ratio (HR) 4.137, 95% confidence interval (CI) 2.321–7.374, p < 0.001), but also worse OS was observed in patients with iΔSPD < 80% than in those with iΔSPD ≥ 80% (HR 4.988, 95% CI 2.486–10.006, p < 0.001); the 3- and 5-year PFS were 78.4% ± 2.9% and 72.4% ± 3.6% in patients with iΔSPD ≥ 80% vs. 19.7% ± 5.3% and 15.7% ± 5.5% in patients with iΔSPD < 80%, respectively. The 3- and 5-year OS were also higher for patients with iΔSPD ≥ 80% than for those with iΔSPD < 80%, with 87.4% ± 2.4% and 83.8% ± 2.9% vs. 34.4% ± 6.3% and 31.8% ± 6.4% (Fig. 3a, b).
Discussion
Interim response assessment is performed to identify patients who can benefit from a prompt therapy change. However, there is no consensus on the criteria for early therapy change during interim response assessment yet. Although end-of-treatment assessment is more accurate with PET-CT than CECT for patients with DLBCL [5, 6], different from the Hodgkin lymphoma, the predictive value of interim positron emission tomography/CT (iPET/CT) in DLBCL remains a matter of significant debate [7,8,9,10,11,12,13,14,15,16]. Some studies have revealed that interim positron emission tomography/computed tomography (iPET/CT) has encouraging prognostic value [7,8,9,10], while some studies hold the opposite opinion [11,12,13,14,15]. And the optimal timing for iPET/CT scanning still needs to be further studied [17,18,19,20]. Besides, iPET/CT scans are associated with an increased false positive rate and some patients turn out to achieve a favorable long-term outcome despite a positive iPET/CT. In a prospective study that investigated the role of iPET/CT in DLBCL patients (after 4 cycles of R-CHOP), only 5 of 37 (13.5%) patients with a positive iPET/CT had a positive biopsy result; PFS outcome in patients who were iPET/CT-positive and biopsy-negative was similar to that in patients with a negative iPET/CT [21]. Therefore, NCCN guidelines still have reservations for patients with a positive iPET/CT, and iPET/CT imaging is not yet recommended to be used to guide changes in therapy at present. If treatment modifications are considered based on iPET/CT results, a repeat biopsy of residual masses should be strongly considered to confirm PET positivity prior to additional therapy. In addition, PET/CT is expensive and technically challenging and is not standardized for clinical use in developing countries. Thus, we tried to investigate whether there was an iΔSPD cutoff value that could discriminate patients with DLBCL who may benefit from an early therapy change just using interim CECT. Actually, this is the first time to date to find out an optimal iΔSPD cutoff value for patients with DLBCL in interim response assessment.
In our study, we found that according to the analysis by X-tile, the cutoff value of iΔSPD that yielded the highest difference in OS was 80%. Then, we compared the prognostic value of it with 50% and 100% through ROC curve analysis and Cox regression analysis. Eighty percent cutoff value showed the maximal AUC and Youden index. For PFS, the sensitivity, specificity, PPV, and NPV of 80% cutoff value were 48.98%, 92.22%, 78.69%, and 75.49%, respectively; for OS, these were 57.75%, 86.69%, 67.21%, and 85.29%, respectively. Burggraaff et al [22] performed a systematic review and meta-analysis from 18 studies comprising 2255 DLBCL patients treated with first-line immunochemotherapy regimens and showed NPV, PPV, sensitivity, and specificity of iPET/CT for progression of 64–95%, 20–74%, 33–87%, and 49–94%, respectively, which was in line with our results. This means our approach using interim CECT on the basis of 80% cutoff value is comparable, at least not inferior to iPET/CT. Cox regression analysis also revealed that the iΔSPD < 80% cutoff value could independently predict an inferior PFS and OS while neither iΔSPD < 50% nor iΔSPD = 100% could. Given its superiority, we selected 80% as the optimal cutoff value to identify patients with DLBCL who need a prompt therapy change.
In conclusion, iΔSPD with the cutoff value 80% is an independent predictor of PFS and OS for patients with DLBCL. Treatment modification is recommended for patients with iΔSPD < 80% at interim response assessment. However, whether such modification will improve survival should be proven in further prospective, multicenter studies.
Abbreviations
- AUCs:
-
Areas under the curve
- CECT:
-
Contrast-enhanced computed tomography
- CHOP:
-
Cyclophosphamide, doxorubicin, vincristine, and prednisone
- DLBCL:
-
Diffuse large B cell lymphoma
- ECOG:
-
Eastern Cooperative Oncology Group
- GCB:
-
Germinal center B cell–like
- iΔSPD:
-
Interim reduction percentage of the sum of the products of the greatest perpendicular diameters for multiple lesions
- iPET/CT:
-
Interim positron emission tomography/computed tomography
- IPI:
-
International Prognostic Index
- LDH:
-
Lactate dehydrogenase
- LDi:
-
Longest diameter
- NCCN:
-
National Comprehensive Cancer Network
- OS:
-
Overall survival
- PACS:
-
Picture archiving and communication system
- PFS:
-
Progression-free survival
- R:
-
Rituximab
- ROC:
-
Receiver operating characteristics
References
Al-Hamadani M, Habermann TM, Cerhan JR, Macon WR, Maurer MJ, Go RS (2015) Non-Hodgkin lymphoma subtype distribution, geodemographic patterns, and survival in the US: a longitudinal analysis of the National Cancer Data Base from 1998 to 2011. Am J Hematol 90:790–795. https://doi.org/10.1002/ajh.24086
Habermann TM, Weller EA, Morrison VA et al (2006) Rituximab-CHOP versus CHOP alone or with maintenance rituximab in older patients with diffuse large B-cell lymphoma. J Clin Oncol 24:3121–3127. https://doi.org/10.1200/JCO.2005.05.1003
Cheson BD, Fisher RI, Barrington SF et al (2014) Recommendations for initial evaluation, staging, and response assessment of Hodgkin and non-Hodgkin lymphoma: the Lugano classification. J Clin Oncol 32:3059–3068. https://doi.org/10.1200/JCO.2013.54.8800
Camp RL, Dolled-Filhart M, Rimm DL (2004) X-tile: a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clin Cancer Res 10:7252–7259. https://doi.org/10.1158/1078-0432.CCR-04-0713
Cheson BD, Pfistner B, Juweid ME et al (2007) Revised response criteria for malignant lymphoma. J Clin Oncol 25:579–586. https://doi.org/10.1200/JCO.2006.09.2403
Juweid ME, Wiseman GA, Vose JM et al (2005) Response assessment of aggressive non-Hodgkin’s lymphoma by integrated International Workshop Criteria (IWC) and fluorine-18-fluorodeoxyglucose positron emission tomography. J Clin Oncol 23:4652–4661. https://doi.org/10.1200/JCO.2005.01.891
Mamot C, Klingbiel D, Hitz F et al (2015) Final results of a prospective evaluation of the predictive value of interim positron emission tomography in patients with diffuse large B-cell lymphoma treated with R-CHOP-14 (SAKK 38/07). J Clin Oncol 33:2523–2529. https://doi.org/10.1200/JCO.2014.58.9846
Safar V, Dupuis J, Itti E et al (2012) Interim [18F]fluorodeoxyglucose positron emission tomography scan in diffuse large B-cell lymphoma treated with anthracycline-based chemotherapy plus rituximab. J Clin Oncol 30:184–190. https://doi.org/10.1200/JCO.2011.38.2648
Mikhaeel NG, Timothy AR, Hain SF, O'Doherty MJ (2000) 18-FDG-PET for the assessment of residual masses on CT following treatment of lymphomas. Ann Oncol 11(Suppl 1):147–150
Chow A, Phillips M, Siew T et al (2013) Prognostic nomogram for diffuse large B-cell lymphoma incorporating the International Prognostic Index with interim-positron emission tomography findings. Intern Med J 43:932–939. https://doi.org/10.1111/imj.12194
Pregno P, Chiappella A, Bellò M et al (2012) Interim 18-FDG-PET/CT failed to predict the outcome in diffuse large B-cell lymphoma patients treated at the diagnosis with rituximab-CHOP. Blood 119:2066–2073. https://doi.org/10.1182/blood-2011-06-359943
González-Barca E, Canales M, Cortés M et al (2013) Predictive value of interim 18F-FDG-PET/CT for event-free survival in patients with diffuse large B-cell lymphoma homogenously treated in a phase II trial with six cycles of R-CHOP-14 plus pegfilgrastim as first-line treatment. Nucl Med Commun 34:946–952. https://doi.org/10.1097/MNM.0b013e328363c695
Yoo C, Lee DH, Kim JE et al (2011) Limited role of interim PET/CT in patients with diffuse large B-cell lymphoma treated with R-CHOP. Ann Hematol 90:797–802. https://doi.org/10.1007/s00277-010-1135-6
Cashen AF, Dehdashti F, Luo J et al (2011) 18F-FDG PET/CT for early response assessment in diffuse large B-cell lymphoma: poor predictive value of international harmonization project interpretation. J Nucl Med 52:386–392. https://doi.org/10.2967/jnumed.110.082586
Micallef IN, Maurer MJ, Wiseman GA et al (2011) Epratuzumab with rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone chemotherapy in patients with previously untreated diffuse large B-cell lymphoma. Blood 118:4053–4061. https://doi.org/10.1182/blood-2011-02-336990
Dupuis J, Itti E, Rahmouni A et al (2009) Response assessment after an inductive CHOP or CHOP-like regimen with or without rituximab in 103 patients with diffuse large B-cell lymphoma: integrating 18fluorodeoxyglucose positron emission tomography to the International Workshop Criteria. Ann Oncol 20:503–507. https://doi.org/10.1093/annonc/mdn671
Kitajima K, Okada M, Kashiwagi T et al (2019) Early evaluation of tumor response to 90Y-ibritumomab radioimmunotherapy in relapsed/refractory B cell non-Hodgkin lymphoma: what is the optimal timing for FDG-PET/CT? Eur Radiol 29:3935–3944. https://doi.org/10.1007/s00330-019-06134-7
Kasamon YL, Wahl RL (2008) FDG PET and risk-adapted therapy in Hodgkin’s and non-Hodgkin’s lymphoma. Curr Opin Oncol 20:206–219. https://doi.org/10.1097/CCO.0b013e3282f5123d
Casasnovas RO, Meignan M, Berriolo-Riedinger A et al (2011) SUVmax reduction improves early prognosis value of interim positron emission tomography scans in diffuse large B-cell lymphoma. Blood 118:37–43. https://doi.org/10.1182/blood-2010-12-327767
Zhang X, Fan W, Xia Z-J et al (2015) Use of subsequent PET/CT in diffuse large B-cell lymphoma patients in complete remission following primary therapy. Chin J Cancer 34:70–78. https://doi.org/10.5732/cjc.014.10124
Moskowitz CH, Schoder H, Teruya-Feldstein J et al (2010) Risk-adapted dose-dense immunochemotherapy determined by interim FDG-PET in advanced-stage diffuse large B-cell lymphoma. J Clin Oncol 28:1896–1903. https://doi.org/10.1200/JCO.2009.26.5942
Burggraaff CN, De Jong A, Hoekstra OS et al (2019) Predictive value of interim positron emission tomography in diffuse large B-cell lymphoma: a systematic review and meta-analysis. Eur J Nucl Med Mol Imaging 46:65–79. https://doi.org/10.1007/s00259-018-4103-3
Acknowledgments
The authors thank the participating patients, their families, and staff at the study site. We sincerely thank Professor Jun-Chen Dai, a qualified statistician in Nanjing Medical University, for his contribution to statistical analysis in this study.
Funding
This study was supported by the National Natural Science Foundation of China (81470328, 81600130, 81770166, 81720108002), Jiangsu Province’s Medical Elite Programme (ZDRCA2016022), Project of National Key Clinical Specialty, Jiangsu Provincial Special Program of Medical Science (BE2017751), and National Science and Technology Major Project (2018ZX09734007).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Wei Xu.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• Retrospective
• Diagnostic or prognostic study
• Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 52.6 kb)
Rights and permissions
About this article
Cite this article
Wei, YC., Ding, CY., Liang, JH. et al. Interim response in diffuse large B cell lymphoma on CT: what is the optimal size reduction (ΔSPD) for predicting outcome?. Eur Radiol 30, 3094–3100 (2020). https://doi.org/10.1007/s00330-019-06552-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06552-7