Abstract
Purpose
To evaluate the subjective and objective qualities of computed tomography (CT) venography images at 80 kVp using model-based iterative reconstruction (MBIR) and to compare these with those of filtered back projection (FBP) and adaptive statistical iterative reconstruction (ASIR) using the same CT data sets.
Materials and methods
Forty-four patients (mean age: 56.1 ± 18.1) who underwent 80 kVp CT venography (CTV) for the evaluation of deep vein thrombosis (DVT) during 4 months were enrolled in this retrospective study. The same raw data were reconstructed using FBP, ASIR, and MBIR. Objective and subjective image analysis were performed at the inferior vena cava (IVC), femoral vein, and popliteal vein.
Results
The mean CNR of MBIR was significantly greater than those of FBP and ASIR and images reconstructed using MBIR had significantly lower objective image noise (p < .001). Subjective image quality and confidence of detecting DVT by MBIR group were significantly greater than those of FBP and ASIR (p < .005), and MBIR had the lowest score for subjective image noise (p < .001).
Conclusion
CTV at 80 kVp with MBIR was superior to FBP and ASIR regarding subjective and objective image qualities.
Key Points
• MBIR provides superior image quality compared with FBP and ASIR
• CTV at 80kVp with MBIR improves diagnostic confidence in diagnosing DVT
• CTV at 80kVp with MBIR presents better image quality with low radiation
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Venous thromboembolism (VTE) refers to pathological thrombosis of the venous system and embolism to the pulmonary arteries. Deep vein thrombosis (DVT) of the lower extremities is the most common type of VTE [1]. Pulmonary embolism (PE) is the most fatal complication of DVT with fatality rates ranging from 7 % to 11 % according to prospective cohort studies, and other complications include post-thrombotic syndrome and pulmonary hypertension [1, 2]. Therefore, early diagnosis and proper management of DVT are important to prevent complications.
Computed tomography (CT) venography has high accuracy for diagnosing DVT of the lower extremities, which is similar to that of Doppler ultrasound (US) [3–6]. CT venography (CTV) can also evaluate DVT in the pelvic veins, which would be difficult to diagnose on Doppler US, and detect other pathologies, such as, malignancies. However, radiation exposure and the use of iodinated contrast media are disadvantages of CTV [5, 7, 8]. Because of these issues, the value of combining CTV with CT pulmonary angiography (CTPA) remains controversial [5, 9] and CTPA is not routinely included in our institution for detecting DVT.
According to the previous literature, risk for thrombosis is higher in oral contraceptives users and postmenopausal women with hormone replacement therapy [3, 10], and CTV can be used as an accurate diagnostic tool. Furthermore, CTV is currently used to evaluate varicose veins in the lower extremities, which are one of the most common diseases of adults between the second and sixth decades [11, 12]. In these situations, CT exams for diagnosis and follow-up lead to a high dose of radiation exposure, which could be harmful, especially for young women of childbearing age [5, 13]. Therefore, dose reduction techniques should be considered in CTV.
Recently, lower tube voltages have been applied to reduce radiation dose during CT acquisition, and other methods, such as tube current modulation and the usages of noise reduction filters and a higher pitch, have also been shown to be effective [14, 15].
However, lower tube voltages, such as 80 kVp, have not been widely applied to CTV, because of increased image noise and reduced image quality of the standard filtered back-projection (FBP) algorithm at low dose [14, 16, 17]. Furthermore, in patients with high BMI, image quality tends to be poorer due to increased image noise [18, 19]. Therefore, the low tube voltage technique may not be appropriate in these patients.
Recently, new iterative reconstruction (IR) methods, such as, adaptive statistical iterative reconstruction (ASiR, GE Healthcare, Waukesha, WI, USA), and model-based iterative reconstruction (Veo, GE Healthcare, Waukesha, WI, USA) have been introduced, and studies on low dose chest, abdominal, and cardiac CT using IR methods have reported improved image quality and reduced image noise as compared with FBP [16, 17, 20–28].
Therefore, the purpose of this study was to evaluate objective and subjective image qualities and image noise of CTV at 80 kVp with model-based iterative reconstruction (MBIR), and to compare these with those of FBP and adaptive statistical iterative reconstruction (ASIR).
Materials and methods
Patient selection and population
This retrospective study was approved by our institutional review board, which waived the requirement to obtain an informed consent. From November 2013 to February 2014, 48 patients who visited our vascular centre underwent CTV at 80 kVp due to clinical suspicion of DVT. Patients with suspicion of PE underwent combined CTPA and CTV, and they were not enrolled in this study. Patients who underwent arthroplasty of both knees (n = 1), with chronic DVT of both popliteal veins (n = 1), and who underwent repeated CT exams during the period (n = 2) were excluded. Finally, 44 patients were enrolled in the present study (24 men, 20 women; mean age, 56.1 ± 18.1 years). Height (mean, 1.64 ± 0.09 m) and body weight (BW; mean, 67.20 ± 14.77 kg) of the patients were also recorded and body mass index (BMI; mean, 25.03 ± 4.56 kg/m2) was calculated.
CT scanning technique
All 44 patients underwent imaging with a 64-detector CT (Discovery 750 HD, GE Healthcare, Waukesha, WI, USA) with the following parameters: tube voltage, 80 kVp; automatic tube current modulation (ATCM); section thickness, 2.5 mm; slice interval, 2.5 mm; gantry rotation time, 0.6 seconds; and pitch, 0.984. CTV was performed in the supine position from the 12th thoracic vertebra to toes in a craniocaudal direction using a single breath-hold. For contrast enhancement, all patients received 2 mL/kg BW (maximum, 120 mL) of nonionic iodinated contrast medium (Optiray 320 mg/mL; Mallinckrodt Pharmaceuticals, Dublin, Ireland) at a flow rate of 3 mL/s, and followed this with a 25 mL of 0.9 % saline solution at the same flow rate. CTV scans were initiated at 4 minutes after commencing the IV injection of contrast media. ATCM (AutomA, GE Healthcare, Waukesha, WI, USA) was used at a noise index (NI) level of 21, as determined by a pilot study performed at our institution that compared two groups (NI, 24 [20] and NI, 21) of 20 patients. The specific noise index was chosen by two subspecialty radiologists with consensus.
Image reconstruction
Raw data were reconstructed in the axial plane using a 2.5 mm slice thickness with traditional FBP as the reference standard. A blending factor of 60 % was used for ASIR, as this provides acceptable image quality according to previous studies [29, 30] and our experience with the use of ASIR for diverse indications. Images were also reconstructed with MBIR (Veo 2.0), which is a pure IR technique, and mean reconstruction time for MBIR was 120.8 ± 17.0 minutes. All images were anonymized.
Analysis of image quality and image noise
Images were loaded onto a picture archiving and communication system (PACS) workstation (Marosis, Infinitt, Seoul, Korea), and image analysis was performed using axial images and a window level of 40 Hounsfield units (HU) and a window width of 400 HU. Two readers (one radiologist with 2 years and another with 17 years of experience in vascular imaging) independently reviewed CTV images for quality and noise.
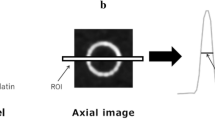
For objective analysis, vascular enhancement was quantitatively evaluated using attenuation values of the following; inferior vena cava (IVC) at the level of the left renal vein, right femoral vein at the level of the femoral head, and right popliteal vein at the level of the knee joint. When a patient had DVT of a right side vein, measurements were performed on the contralateral left side vein. Mean attenuation values for each vein were measured using a region of interest (ROI). The two readers independently placed a circular ROI on the vein to be measured to include more than two thirds of the vessel diameter and vascular enhancements were measured in HU with standard deviations (image noise) in the same slices using identical ROIs on FBP, ASIR, and MBIR image series. The readers also measured the contrast-to-noise ratio (CNR) of each vein, by placing a 90-110 mm2 circular ROI in homogeneous subcutaneous fat at the mid level of the medial thigh and in adductor muscle. CNRs were calculated by using, CNR = (VHU – MHU) / FSD (where VHU and MHU are the attenuation values of each vein and adductor muscle, and FSD is the noise of subcutaneous fat) [31]. The mean values obtained by the two readers were calculated (Fig. 1).
CT images obtained at the level of the inferior vena cava (a–c), femoral vein (d–f), and popliteal vein (g–i) for objective analysis. Contrast-to-noise ratio (CNR) was higher for MBIR (c, f, and i) than for FBP (a, d, and g) or ASIR (b, e, and h). Image noise (SD) was lower for MBIR than FBP or ASIR. However, vascular enhancements (Mean) were not different between the three reconstruction techniques. *FBP, filtered back-projection; ASIR, adaptive statistical iterative reconstruction; MBIR, model-based iterative reconstruction
For subjective assessments, four images of each reconstructed series (IVC at the level of the left renal vein, right common iliac vein at the level of L5 vertebra, right femoral vein at the level of the femoral head, and right popliteal vein at the level of the knee joint) were saved as DICOM files and stored in image folders in random order (performed using Microsoft Office Excel 2007; Microsoft, Redmond, WA, USA). The readers subjectively evaluated image sets independently using a PACS workstation and recorded findings using a previously described template [32–35] and a 3 to 5 point scale for the following attributes: image quality, image noise, and confidence of detecting DVT (Table 1). Mean values of individual folders were subjected to statistical analysis (Fig. 2). Objective and subjective evaluations were performed at least 4 weeks apart.
CT images obtained at the level of the inferior vena cava (a–c), common iliac vein (d–f), femoral vein (g–i), and popliteal vein (j–l) reconstructed by FBP (a, d, g, and j), ASIR (b, e, h, and k), and MBIR (c, f, i, and l) for subjective analysis. Image quality score was higher in the MBIR group (c, 4; f, 5; i, 5; l, 5; mean, 4.25) than in the FBP (a, 2; d, 3; g, 3; j, 3; mean, 2.75) or ASIR groups (b, 3; e, 3; h, 4; k, 4; mean, 3.50), and the confidence of detecting deep vein thrombosis (DVT) score was greater for MBIR (5; 5; 5; 5; mean, 5.00) than for FBP (2; 4; 3; 2; mean, 2.75) or ASIR (4; 5; 5; 4; mean, 4.50). Furthermore, image noise was lower for MBIR (1; 1; 1; 1; mean, 1.00) than in the FBP (3; 2; 2; 2; mean, 2.25) or ASIR groups (2; 1; 1; 1; mean, 1.25). *FBP, filtered back-projection; ASIR, adaptive statistical iterative reconstruction; MBIR, model-based iterative reconstruction
Evaluation of radiation dose
Dose-length product (DLP) was used as a CT radiation dose descriptor and was provided by the imaging system.
Statistical analysis
The data were analyzed using dedicated statistical software (SPSS version 18; SPSS, Chicago, IL, USA). Objective and subjective image data obtained using the three reconstruction algorithms were compared using repeated measures ANOVA. A P < .050 was considered statistically significant. To determine the inter-observer reliabilities of objective and subjective assessments, intraclass correlation coefficients (ICCs) were used, and an ICC was defined by 0.00-0.20 as poor, 0.21-0.40 as fair, 0.41-0.60 as moderate, 0.61-0.80 as good, and 0.81-1.00 as excellent. Pearson's correlation analysis was performed to compare BMI with CNR among the three reconstruction techniques.
Results
Of the 44 patients, eight had DVT (18.2 %, five men and three women; mean age, 57.0 ± 23.2 years). The distribution of thrombi was as follows: common iliac vein in two patients, femoral vein in two, from common iliac vein to popliteal vein in two, and from femoral vein to popliteal vein in two (Fig. 3). All images reconstructed by MBIR were acceptable for the diagnosis of DVT.
Coronal multiplanar reconstruction images with FBP (a), ASIR (b), and MBIR (c) methods. Intraluminal filling defect was detected in left femoral vein, which was diagnosed as deep vein thrombosis. On axial image at this level, image qualities in both objective and subjective analysis were higher in MBIR than in FBP or ASIR. *FBP, filtered back-projection; ASIR, adaptive statistical iterative reconstruction; MBIR, model-based iterative reconstruction
The mean CNR of MBIR was significantly higher than those of FBP and ASIR at the IVC, femoral vein, and popliteal vein (p < .001), and MBIR images had significantly lower objective image noise (p < .001). However, mean vascular enhancement by MBIR was not significantly different from those obtained by FBP or ASIR (p = .928 at the IVC, p = .170 at the femoral vein, and p = .900 at the popliteal vein) (Table 2). In addition, subjective image qualities (p < .001 for reader 1, R1 and p = .031 for reader 2, R2) and confidence of detecting DVT (p = .033 for R1 and p < .001 for R2) for MBIR were significantly higher than for FBP or ASIR. However, MBIR had the lowest level of subjective image noise (p < .001 for R1 and R2) (Table 3).
The inter-observer reliability of MBIR was excellent by objective analysis (ICC for vascular enhancement of 0.988 and for image noise of 0.962) and good to excellent by subjective assessment (ICC for image quality 0.751, for image noise 0.828, and for confidence of detecting DVT of 0.629).
Mean DLP of 80 kVp CTV was 364.31 ± 61.20 mGy cm, and this was 10 %-70 % lower than the values reported by previous studies [33, 36–39].
There was no significant correlation between BMI and image quality in FBP (r = -0.195, p = 0.205 at the IVC; r = -0.040, p = 0.796 at the femoral vein; and r = 0.074, p = 0.635 at the popliteal vein), ASIR (r = -0.213, p = 0.165 at the IVC; r = -0.225, p = 0.872 at the femoral vein; and r = 0.610, p = 0.696 at the popliteal vein), and MBIR (r = -0.199, p = 0.195 at the IVC; r = -0.033, p = 0.831 at the femoral vein; and r = 0.062, p = 0.691 at the popliteal vein) (Fig. 4).
Scatter plots of image noise (CNR) against body mass index show no correlation at the level of the inferior vena cava (a–c), femoral vein (d–f), and popliteal vein (g–i) with FBP (a, d, and g), ASIR (b, e, and h), and MBIR (c, f, and i). * IVC, inferior vena cava; FV, femoral vein; PopV, popliteal vein. ** FBP, filtered back-projection; ASIR, adaptive statistical iterative reconstruction; MBIR, model-based iterative reconstruction
Discussion
In this retrospective study of 80 kVp CTV with MBIR, image quality was found to be significantly increased and image noise was significantly reduced as compared with 80 kVp CTV with FBP or ASIR. However, no significant difference was found between the vascular enhancements achieved by the three reconstruction techniques. Previous studies reported that CTV at 80 kVp reduced radiation dose and improved image quality [9, 11, 38, 39]. However, application of their results to Westerners was uncertain because of increased image noise and decreased image quality in obese and heavy patients [9, 18, 19, 38, 39]. The present results demonstrate that the low tube voltage CTV with MBIR can reduce these problems.
In the present study, there was no significant correlation between BMI and CNR in all three reconstruction techniques. That could be probably due to small-sized patients that were enrolled in this study (BMI; mean, 25.03 ± 4.56 kg/m2). If many obese patients were included in our study, image quality would be decreased when BMI increased, as consistent with previous studies [18, 19].
Reduced tube voltage has the advantage of improved vascular enhancement with radiation dose reduction [36, 39]. At CTV, previously reported mean venous attenuation range with various concentrations and amounts of contrast media was 91 to 115 HU [40–43] and mean DVT clot attenuation was 51 HU or greater [40, 44]. The present study with 80 kVp CTV showed greater venous attenuation than previous reports (mean, 153.9 HU with FBP; 153.8 HU with ASIR; and 153.4 HU with MBIR), and these results were similar to those reported in the literature [9]. Furthermore, mean DLP of this study was 364.31 ± 61.20 mGy cm, and this was 10 %-70 % lower than the values reported by previous articles [33, 36–39].
The present results that dose-reduced CTV with MBIR shows significant improvements in image quality and image noise over FBP and ASIR are consistent with previous reports. Yasaka et al. [14] evaluated ultralow-dose abdominopelvic CT images reconstructed using MBIR and ASIR, and reported that MBIR improved image noise and streak artefacts significantly, and that it achieved radiation dose reductions without compromising image quality. Ichikawa et al. [16] suggested that MBIR has better image quality and lower image noise than ASIR for the detection of enlarged mediastinal lymph nodes and lower lung attenuation (bulla, emphysema, or cyst) on low-dose chest CT. Singh et al. [45] reported 50 mAs abdominal CT with MBIR provides acceptable image quality and diagnostic confidence, but that CT with FBP or ASIR does not.
FBP has remained the standard CT image reconstruction technique for decades. It is based on several assumptions that simplify CT geometry to accomplish rapid reconstruction. However, it suffers from relatively high levels of image noise and streaky artefacts, especially when low dose CT acquisition is used [16, 17, 23].
ASIR is a currently used hybrid IR algorithm. It models photons and electronic noise statistically and compares the data obtained with FBP until the algorithm converges [14, 24, 25]. Using this method, technicians can blend ASIR with FBP images to obtain final images [27]. It reduces image noise without compromising image quality, and 25-40 % dose reductions have been reported for this algorithm [20, 46–49].
The recently developed MBIR technique is a pure IR and does not involve blending with FBP data. It relies on a more complex, accurate IR algorithm than ASIR [14, 16], and in addition to using the statistical model used in ASIR, MBIR also predicts more complex models that included the modelling of system optics (size of the focal x-ray spot, shape and size of image voxels, and the size of the active detector) [21, 24]. In other words, MBIR is not based on FBP, and it is used to develop a synthesized projection model using knowledge of three main key models in the IR algorithm: the forward model (system optics model and all geometry-related effects), the noise model, and the image model. Therefore, it provides considerably reduced noise as well as much improved spatial resolution [50].
Several studies have reported significant dose reductions for low dose CT with MBIR of up to 80 % for various parts of the body [14, 16, 20, 22, 23, 51]. However, MBIR has also been suggested to have some limitations. Firstly, the MBIR algorithm requires greater computational capacity, and thus, reconstruction times are longer even when the most modern processors are used [21–23]. It takes one second to obtain a reconstructed image with MBIR, whereas FBP and ASIR can reconstruct 15 and ten images, respectively, in the same time [23]. For instance, mean reconstruction time for MBIR was 120.8 ± 17.0 minutes in this study. For this reason, CT with MBIR may be limited in emergency conditions [52, 53]. Secondly, MBIR images tend to have a unique, blotchy, pixilated texture, whereas FBP and ASIR images do not. The exact reasons for this are unknown [14, 23]. Xu et al. [54] suggested that statistical reconstruction might reduce diagnostic ability due to radiologists’ familiarity with FBP. However, in the present study, all images obtained using MBIR were acceptable in terms of detecting DVT.
The present study has several limitations. First, it was conducted using a retrospective design on a relatively small number of patients. A large prospective study is required to further assess the use of low dose CTV conducted using MBIR in DVT. Second, the diagnostic accuracies of the reconstruction techniques were not compared. However, all images reconstructed using MBIR were diagnostically acceptable, and confidence of detecting DVT with MBIR was significantly greater than with FBP or ASIR by subjective assessment. Third, due to the unique appearance of MBIR images, it was not possible to blind radiologists to the technique used during subjective analysis. Nevertheless, all image sets were randomly ordered and times between objective and subjective evaluations were more than 4 weeks to avoid adaptation. Finally, present results may not be applied to CT data performed from other vendors, because MBIR is vendor-specific.
In conclusion, CTV at 80 kVp using the MBIR algorithm provided acceptable image quality for the evaluation of DVT, and was found to be superior to FBP and ASIR in terms of objective and subjective image qualities.
References
Merli G (2005) Diagnostic assessment of deep vein thrombosis and pulmonary embolism. Am J Med 118:3S–12S
Stein PD, Kayali F, Olson RE (2004) Estimated case fatality rate of pulmonary embolism, 1979 to 1998. Am J Cardiol 93:1197–1199
Kyrle PA, Eichinger S (2005) Deep vein thrombosis. Lancet 365:1163–1174
Byun SS, Kim JH, Kim YJ, Jeon YS, Park CH, Kim WH (2008) Evaluation of deep vein thrombosis with multidetector row CT after orthopedic arthroplasty: a prospective study for comparison with Doppler sonography. Korean J Radiol 9:59–66
Kanne JP, Lalani TA (2004) Role of computed tomography and magnetic resonance imaging for deep venous thrombosis and pulmonary embolism. Circulation 109:I15–I21
Goodman LR, Stein PD, Matta F et al (2007) CT venography and compression sonography are diagnostically equivalent: data from PIOPED II. AJR Am J Roentgenol 189:1071–1076
Rhee KH, Iyer RS, Cha S et al (2007) Benefit of CT venography for the diagnosis of thromboembolic disease. Clin Imaging 31:253–258
Peterson DA, Kazerooni EA, Wakefield TW et al (2001) Computed tomographic venography is specific but not sensitive for diagnosis of acute lower-extremity deep venous thrombosis in patients with suspected pulmonary embolus. J Vasc Surg 34:798–804
Nakaura T, Awai K, Oda S et al (2011) A low-kilovolt (peak) high-tube current technique improves venous enhancement and reduces the radiation dose at indirect multidetector-row CT venography: initial experience. J Comput Assist Tomogr 35:141–147
Rosendaal FR, Van Hylckama VA, Tanis BC, Helmerhorst FM (2003) Estrogens, progestogens and thrombosis. J Thromb Haemost 1:1371–1380
Cho ES, Kim JH, Kim S et al (2012) Computed tomographic venography for varicose veins of the lower extremities: prospective comparison of 80-kVp and conventional 120-kVp protocols. J Comput Assist Tomogr 36:583–590
Golledge J, Quigley FG (2003) Pathogenesis of varicose veins. Eur J Vasc Endovasc Surg 25:319–324
Rademaker J, Griesshaber V, Hidajat N, Oestmann JW, Felix R (2001) Combined CT pulmonary angiography and venography for diagnosis of pulmonary embolism and deep vein thrombosis: radiation dose. J Thorac Imaging 16:297–299
Yasaka K, Katsura M, Akahane M, Sato J, Matsuda I, Ohtomo K (2013) Model-based iterative reconstruction for reduction of radiation dose in abdominopelvic CT: comparison to adaptive statistical iterative reconstruction. SpringerPlus 2:209
Kalra MK, Maher MM, Toth TL et al (2004) Strategies for CT radiation dose optimization. Radiology 230:619–628
Ichikawa Y, Kitagawa K, Nagasawa N, Murashima S, Sakuma H (2013) CT of the chest with model-based, fully iterative reconstruction: comparison with adaptive statistical iterative reconstruction. BMC Med Imaging 13:27
Nelson RC, Feuerlein S, Boll DT (2011) New iterative reconstruction techniques for cardiovascular computed tomography: how do they work, and what are the advantages and disadvantages? J Cardiovasc Comput Tomogr 5:286–292
Tatsugami F, Husmann L, Herzog BA et al (2009) Evaluation of a body mass index-adapted protocol for low-dose 64-MDCT coronary angiography with prospective ECG triggering. AJR Am J Roentgenol 192:635–638
Irie T, Inoue H (2005) Individual modulation of the tube current-seconds to achieve similar levels of image noise in contrast-enhanced abdominal CT. AJR Am J Roentgenol 184:1514–1518
Pickhardt PJ, Lubner MG, Kim DH et al (2012) Abdominal CT with model-based iterative reconstruction (MBIR): initial results of a prospective trial comparing ultralow-dose with standard-dose imaging. AJR Am J Roentgenol 199:1266–1274
Deak Z, Grimm JM, Treitl M et al (2013) Filtered back projection, adaptive statistical iterative reconstruction, and a model-based iterative reconstruction in abdominal CT: an experimental clinical study. Radiology 266:197–206
Vardhanabhuti V, Loader RJ, Mitchell GR, Riordan RD, Roobottom CA (2013) Image quality assessment of standard- and low-dose chest CT using filtered back projection, adaptive statistical iterative reconstruction, and novel model-based iterative reconstruction algorithms. AJR Am J Roentgenol 200:545–552
Shuman WP, Green DE, Busey JM et al (2013) Model-based iterative reconstruction versus adaptive statistical iterative reconstruction and filtered back projection in liver 64-MDCT: focal lesion detection, lesion conspicuity, and image noise. AJR Am J Roentgenol 200:1071–1076
Smith EA, Dillman JR, Goodsitt MM, Christodoulou EG, Keshavarzi N, Strouse PJ (2014) Model-based iterative reconstruction: effect on patient radiation dose and image quality in pediatric body CT. Radiology 270:526–534
Brady SL, Moore BM, Yee BS, Kaufman RA (2014) Pediatric CT: implementation of ASIR for substantial radiation dose reduction while maintaining pre-ASIR image noise. Radiology 270:223–231
Gay F, Pavia Y, Pierrat N, Lasalle S, Neuenschwander S, Brisse HJ (2014) Dose reduction with adaptive statistical iterative reconstruction for paediatric CT: phantom study and clinical experience on chest and abdomen CT. Eur Radiol 24:102–111
Jensen K, Martinsen AC, Tingberg A, Aalokken TM, Fosse E (2014) Comparing five different iterative reconstruction algorithms for computed tomography in an ROC study. Eur Radiol 24:2989–3002
Herin E, Gardavaud F, Chiaradia M et al (2015) Use of Model-Based Iterative Reconstruction (MBIR) in reduced-dose CT for routine follow-up of patients with malignant lymphoma: dose savings, image quality and phantom study. Eur Radiol 25:2362–2370
Kulkarni NM, Uppot RN, Eisner BH, Sahani DV (2012) Radiation dose reduction at multidetector CT with adaptive statistical iterative reconstruction for evaluation of urolithiasis: how low can we go? Radiology 265:158–166
Leipsic J, Labounty TM, Heilbron B et al (2010) Adaptive statistical iterative reconstruction: assessment of image noise and image quality in coronary CT angiography. AJR Am J Roentgenol 195:649–654
Kulkarni NM, Sahani DV, Desai GS, Kalva SP (2012) Indirect computed tomography venography of the lower extremities using single-source dual-energy computed tomography: advantage of low-kiloelectron volt monochromatic images. J Vasc Interv Radiol 23:879–886
Schueller-Weidekamm C, Schaefer-Prokop CM, Weber M, Herold CJ, Prokop M (2006) CT angiography of pulmonary arteries to detect pulmonary embolism: improvement of vascular enhancement with low kilovoltage settings. Radiology 241:899–907
Park CK, Choo KS, Jeon UB et al (2013) Image quality and radiation dose of 128-slice dual-source CT venography using low kilovoltage combined with high-pitch scanning and automatic tube current modulation. Int J Cardiovasc Imaging 29:47–51
Volders D, Bols A, Haspeslagh M, Coenegrachts K (2013) Model-based iterative reconstruction and adaptive statistical iterative reconstruction techniques in abdominal CT: comparison of image quality in the detection of colorectal liver metastases. Radiology 269:469–474
Matsuoka S, Hunsaker AR, Gill RR et al (2009) Vascular enhancement and image quality of MDCT pulmonary angiography in 400 cases: comparison of standard and low kilovoltage settings. AJR Am J Roentgenol 192:1651–1656
Cho ES, Chung JJ, Kim S, Kim JH, Yu JS, Yoon CS (2013) CT venography for deep vein thrombosis using a low tube voltage (100 kVp) setting could increase venous enhancement and reduce the amount of administered iodine. Korean J Radiol 14:183–193
Fujikawa A, Matsuoka S, Kuramochi K et al (2011) Vascular enhancement and image quality of CT venography: comparison of standard and low kilovoltage settings. AJR Am J Roentgenol 197:838–843
Oda S, Utsunomiya D, Funama Y et al (2012) Evaluation of deep vein thrombosis with reduced radiation and contrast material dose at computed tomography venography: clinical application of a combined iterative reconstruction and low-tube-voltage technique. Circ J 76:2614–2622
Oda S, Utsunomiya D, Awai K et al (2011) Indirect computed tomography venography with a low-tube-voltage technique: reduction in the radiation and contrast material dose--a prospective randomized study. J Comput Assist Tomogr 35:631–636
Cham MD, Yankelevitz DF, Shaham D et al (2000) Deep venous thrombosis: detection by using indirect CT venography. The Pulmonary Angiography-Indirect CT Venography Cooperative Group. Radiology 216:744–751
Bruce D, Loud PA, Klippenstein DL, Grossman ZD, Katz DS (2001) Combined CT venography and pulmonary angiography: how much venous enhancement is routinely obtained? AJR Am J Roentgenol 176:1281–1285
Begemann PG, Bonacker M, Kemper J et al (2003) Evaluation of the deep venous system in patients with suspected pulmonary embolism with multi-detector CT: a prospective study in comparison to Doppler sonography. J Comput Assist Tomogr 27:399–409
Yankelevitz DF, Gamsu G, Shah A et al (2000) Optimization of combined CT pulmonary angiography with lower extremity CT venography. AJR Am J Roentgenol 174:67–69
Baldt MM, Zontsich T, Stumpflen A et al (1996) Deep venous thrombosis of the lower extremity: efficacy of spiral CT venography compared with conventional venography in diagnosis. Radiology 200:423–428
Singh S, Kalra MK, Do S et al (2012) Comparison of hybrid and pure iterative reconstruction techniques with conventional filtered back projection: dose reduction potential in the abdomen. J Comput Assist Tomogr 36:347–353
Sagara Y, Hara AK, Pavlicek W, Silva AC, Paden RG, Wu Q (2010) Abdominal CT: comparison of low-dose CT with adaptive statistical iterative reconstruction and routine-dose CT with filtered back projection in 53 patients. AJR Am J Roentgenol 195:713–719
Prakash P, Kalra MK, Kambadakone AK et al (2010) Reducing abdominal CT radiation dose with adaptive statistical iterative reconstruction technique. Investig Radiol 45:202–210
Kambadakone AR, Chaudhary NA, Desai GS, Nguyen DD, Kulkarni NM, Sahani DV (2011) Low-dose MDCT and CT enterography of patients with Crohn disease: feasibility of adaptive statistical iterative reconstruction. AJR Am J Roentgenol 196:W743–W752
Mitsumori LM, Shuman WP, Busey JM, Kolokythas O, Koprowicz KM (2012) Adaptive statistical iterative reconstruction versus filtered back projection in the same patient: 64 channel liver CT image quality and patient radiation dose. Eur Radiol 22:138–143
Hsieh J, Nett B, Yu Z, Sauer K, Thibault J-B, Bouman CA (2013) Recent advances in CT image reconstruction. Curr Radiol Rep 1:39–51
Mieville FA, Gudinchet F, Brunelle F, Bochud FO, Verdun FR (2013) Iterative reconstruction methods in two different MDCT scanners: physical metrics and 4-alternative forced-choice detectability experiments--a phantom approach. Phys Med 29:99–110
Willemink MJ, Schilham AM, Leiner T, Mali WP, de Jong PA, Budde RP (2013) Iterative reconstruction does not substantially delay CT imaging in an emergency setting. Insights Imaging 4:391–397
Yamada Y, Jinzaki M, Tanami Y et al (2012) Model-based iterative reconstruction technique for ultralow-dose computed tomography of the lung: a pilot study. Investig Radiol 47:482–489
Xu J, Mahesh M, Tsui BM (2009) Is iterative reconstruction ready for MDCT? J Am Coll Radiol 6:274–276
Acknowledgements
The scientific guarantor of this publication is Ki Seok Choo. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. This study was supported by Research Institute for Convergence of Biomedical Science and Technology (30-2014-013), Pusan National University Yangsan Hospital. Institutional Review Board approval was obtained. Written informed consent was waived by the Institutional Review Board.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, J.H., Choo, K.S., Moon, T.Y. et al. Comparison of the image qualities of filtered back-projection, adaptive statistical iterative reconstruction, and model-based iterative reconstruction for CT venography at 80 kVp. Eur Radiol 26, 2055–2063 (2016). https://doi.org/10.1007/s00330-015-4060-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-015-4060-1