Abstract
This study contains 2 arms: (1) the ASIR-V technique combined with low-tube-voltage in lower limb deep vein thrombosis (DVT) diagnosis was investigated; and (2) CT venography and ultrasound results in DVT diagnosis were compared. For arm 1, 90 patients suspected of DVT were randomly divided into 3 groups (30/group): groups A and B were scanned under 100-kV with pre-set ASIR-V weights of 30% and 50% respectively; group C were scanned under 70-kV with a 50% weight. For arm 2, 75 patients were divided into 3 groups (25/group), each group was CT scanned as in arm 1 and then all subjects were examined by ultrasound. Groups A, B and C had 16, 14 and 17 patients diagnosed with DVTs, respectively. There was no significant difference in subjective ratings of image quality among all groups. The 70-kV protocol remarkably increased venous attenuation value while all groups had similar DVT attenuation value. Higher noise was observed in group C, the CNR however, was actually augmented due to elevated venous attenuations. More importantly, group C had significantly lower CTDIvol and DLP values. In conclusion, the 70-kV protocol is superior to the 100 kV protocols, which was supported by findings from the second arm study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Deep vein thrombosis (DVT), the formation of blood thrombi in the deep veins, remains a common and serious clinical condition worldwide. It often manifests as DVT in the lower extremity, but may also occur in veins of other body parts, e.g., in cerebral sinus, arms, retina, etc1,2. DVT in the lower extremity can progress to involve the proximal veins, leading to pulmonary embolism3,4,5, a life-threatening condition with a mortality rate of 2–3%6. DVT can effectively be treated with anticoagulants, thrombolytic agents or embolectomy1,7,8, underscoring the importance of early and accurate diagnosis of DVT.
As DVT is often asymptomatic and its clinical features are unspecific, to date, diagnosis of DVT relies on imaging technologies, such as ultrasound and computed tomography (CT) venography9. It has been shown that CT venography is superior to ultrasound in the detection of DVT in calf veins, and in identification of pelvic or abdominal thrombi9,10,11. Currently, radiation exposure still remains a serious concern in CT scanning12,13. A variety of techniques beyond the traditional reconstruction method of filtered back projection (FBP) have evolved, such as hybrid iterative reconstruction, model-based iterative reconstruction (MBIR) and adaptive statistical iterative reconstruction (ASIR). The use of advanced reconstruction techniques allows for low-dose protocols, since they yield higher quality imaging data when compared to FBP14,15,16,17. Recently, a new generation of ASIR technique, namely ASIR-V, has emerged and been compared with other analytical reconstruction methods, e.g., FBP, MBIR and ASIR18,19,20,21. The effects of low-tube-voltage in conjunction with ASIR-V in CT venography for DVT has not been investigated. This study was therefore conducted to compare the impacts of 70 kV and 100 kV combined with ASIR-V technique in CT venography of lower limb DVT.
Materials and Methods
Patients
The protocol of this prospective study was reviewed and approved by the Research Ethics Committee of Weihai Municipal Hospital. This study was conducted in accordance with the guidelines of biomedical research involving humans established by the Ministry of Health of the People’s Republic of China. Informed written consent to participating in this study was obtained from all subjects. This study contained 2 arms, the first was to examine the effect of different CT protocols. For this purpose, 90 patients suspected of DVT were recruited. The second was to compare the CT venography and ultrasound results in detection of DVTs, and additional 75 patients were enrolled. All patients enrolled did not have severe liver, kidney or cardiovascular disease. Those who were allergic to iodine contrast media or with a body mass index ≥30 were excluded.
Arm 1: CT venography
ASIR-V still uses FBP data sets as building blocks for image reconstruction and is blended with FBP in 10% increments. A higher percentage of ASIR (weight 60–70%) results in degradation of image quality18,22. Therefore, a weight of 50% was chosen as the maximum ASIR-V blending percentage in this study. For the first arm of study, 90 patients were randomly divided into 3 groups (30 subjects/group): patients in groups A and B were scanned by GE Revolution CT under a tube voltage of 100 kV with pre-set ASIR-V weights of 30% and 50% respectively, and a noise index of 10 (the tube current was automated between 0–400 mAs). Patients in group C (with a pre-set ASIR-V weight of 50%) were scanned with the same parameters as those in groups A and B, but with a tube voltage of 70 kV and an automated tube current between 0–500 mAs. The contrast medium, lopromide, was injected (1.5 ml/kg) at the speed of 3.5 ml/s in the right antecubital vein followed by the injection of 60 ml saline. Three minutes post the administration of saline, CTV was performed from pelvis to feet following routine clinical practice (a gantry rotation time of 0.35 seconds with a pitch of 0.992). Images were reconstructed using a section thickness of 5.0 mm without overlap.
Arm 1: Image post-processing and reconstruction
Image post-processing and reconstruction were accomplished on the GE ADW4.6 workstation using maximum intensity projection, multi-planar reformation and volume rendering techniques.
Arm 1: Quantitative image analysis
Objective image analysis was done by measuring the attenuation (in HU) in the inferior vena cava, iliac vein, femoral vein, and popliteal vein at the L4 vertebral body, the inferior margin of the sacroiliac joint, the greater trochanter of the femur, and the medial epicondyle of the femur, respectively. A small round region of interest (ROI) was set at the center of the vein lumen for such measurement. To quantify the attenuation differences between the vein and the surrounding tissue, the attenuation of psoas, iliopsoas, iliacus and semimembranosus muscles was also measured. The image noise was determined as the standard deviation of the attenuation in the muscles. Contrast-to-noise ratio (CNR) was calculated using the formula: (the attenuation value of the vein - the attenuation value of the adjacent muscle)/noise. Similarly, the attenuation value of DVT was measured by placing a small oval ROI in the DVT. If multiple DVTs were detected, the largest was selected for measurement.
Arm 1: Qualitative image analysis
Qualitative image analysis was performed independently in a blinded manner by 2 radiologists who had over 5 years of experience in CT venography interpretation. Images were evaluated for graininess, streak artifact and vessel enhancement. Overall image quality was rated using a 4-point scale as described elsewhere17, with 4 being the highest score, indicating an excellent diagnostic value, and 1 the lowest score, indicating that the image is uninterpretable.
Arm 1: Analysis of radiation dose
The volume CT dose index (CTDIvol) and dose length product (DLP) automatically recorded by the CT scanner after each scanning were used for the analysis of radiation dose.
Arm 2: Comparison of diagnostic results between CT venography and ultrasound scanning
In this arm of study, 75 patients were randomly divided into 3 groups (25/group): patients in group 1 were scanned using the 100-kV with 30% weight protocol; group 2 using 100-kV with 50% weight and group 3 using 70-kV with 50% weight as described above. Additionally all patients were also examined with ultrasound. Compression and pulsed wave Doppler ultrasound were performed by 2 technologists with over 10-year experience using the iU22 ultrasound system from Philips (Amsterdam, Netherland) with a 5–12 MHz transducer. Compression was performed at 2-cm intervals from the inguinal ligament to the ankle.
Statistical analysis
Data normality was determined by the Shapiro-Wilk test. All continuous data were expressed as mean ± standard deviation, and analyzed by one-way ANOVA with Fisher’s least significant difference post hoc test. Categorical data were tested with the Chi-square test. Inter-rater agreement between the 2 radiologists was determined by Cohen’s kappa test. Interpretation of the Cohen’s kappa coefficient K value was as follows: K > 0.75, good agreement; 0.4 < K < 0.7, moderate agreement; and K < 0.4, slight agreement. All statistical analyses were performed using the SPSS 20.0 software and a p-value of <0.05 was considered as statistically significant.
Results
Arm 1: Patients
Demographics and basic characteristics of all patients are shown in Table 1. There were no significant differences in age, gender ratio, weight, height or BMI among all groups of patients. Groups A, B and C had 16, 14 and 17 patients diagnosed with DVT by CT venography, respectively (The diagnosis of DVT was made after clots were identified in CT images, see Fig. 1).
Arm 1: Quantitative image analysis
The mean attenuation values of all measured veins in groups A, B and C were 113.23 ± 11.98 HU, 119.16 ± 12.89 HU and 157.90 ± 21.78, respectively, of which, no significant difference was observed between groups A and B. However, group C had a markedly higher mean attenuation value than groups A and B (both p < 0.001, Table 2). Representative images from groups B and C demonstrating the venous enhancement are shown in Fig. 2 (venous enhancement was stronger at all slice levels under 70 kV). There was no significant difference in the average noise between groups A and B. In contrast, group C had higher average noise compared with groups A and B (Table 2). Nevertheless, the average CNR in group C was significantly higher than those in groups A and B (Table 2). Similar results were observed in all measured segmental veins, i.e., in inferior vena cava, iliac vein, femoral vein and popliteal vein (Table 2). The mean attenuation values of DVT in groups A, B and C were 65.71 ± 3.63 HU, 65.53 ± 3.65 HU and 66.43 ± 3.45 HU, respectively. There were no significant differences in mean attenuation values of DVT among the 3 groups.
Venous enhancement under 70 kV and 100 kV. Representative images under 70 kV: inferior vena cava (2a) right iliac vein (2b) right femoral vein (2c) and right popliteal vein (2d). Representative images under 100 kV: inferior vena cava (2e) right iliac vein (2f) right femoral vein (2g) and right popliteal vein (2h). Venous enhancement (arrows) was stronger at all levels under low-tube-voltage.
Arm 1: Subjective image analysis
The Cohen’s kappa test showed that the rating of images between the 2 radiologists was in good agreement with a K = 0.78. In a 4-point scale analysis, the overall image scores in groups A, B and C were 3.20 ± 0.52, 3.19 ± 0.50 and 3.34 ± 0.58, respectively, which are not significantly different (Table 3). Scores of pelvic and thigh regions among the 3 groups were similar (Table 3). However, the score of the leg was significantly higher in group C compared with those in groups A and B (both p < 0.05, Table 3).
Arm 1: Radiation dose
Radiation dose data are shown in Table 4. The CTDIvol (in mGy) and DLP (in mGy.cm) values in group B were markedly lower compared with group A. The CTDIvol value in group C was 1.76 ± 0.13, which is significantly lower than 4.22 ± 0.50 of group A (p < 0.001) and 3.45 ± 0.30 of group B (p < 0.001). The DLP value in group C was 235.07 ± 42.41, also significantly lower than those in groups A and B (Table 4).
Arm 2: Ultrasound and CT venography results comparison
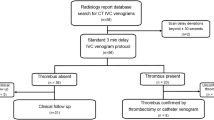
There were no differences in age, gender ratio, weight, height or BMI among the 3 groups in this arm of study (data not shown). The results from the 3 CT protocols are: 100-kV with 30% weights, 100-kV with 50% weight and 70-kV with 50% weight discovered 12, 12 and 14 patients with DVTs, respectively. Ultrasound identified 13 patients with DVTs in each of the 100-kV groups but 1 in each group was ruled out by CT scanning. In the 70-kV group 14 patients were diagnosed as having DVTs by ultrasound with 1 ruled out and 1 ruled in by CT scanning.
Discussion
In the present study, using ASIR-V technique, we compared the effects of a 70 kV protocol and the 100 kV protocol in CT venography of lower limb DVT, and observed that: (1) lower tube voltage significantly increased the attenuation value of the vein but not the DVT’s, facilitating DVT diagnosis; (2) although lower tube voltage increased the image noise, the CNR was actually augmented due to the elevated venous attenuation value; (3) the subjective rating of image quality was not significantly different among all groups; and (4) use of lower tube voltage significantly reduced radiation dose.
Radiation exposure from medical imaging has increased significantly in the past several decades, and remains the largest source of average annual radiation exposure that is under our direct control23. It has been shown that medical radiation exposure is associated with the subsequent risk of cancer for both pediatric and adult patients13,24, necessitating better managing for dose reduction in medical imaging25. A number of strategies including modulation of tube voltage have been explored in CT scanning25. Lower extremity DVT is a serious medical condition that can result in death or major disability due to pulmonary embolism or post-thrombotic syndrome, requiring early and accurate diagnosis for prompt and effective intervention. CT venography is the key diagnostic modality for DVT9. Using the ASIR-V technique combined with low-tube-voltage, we showed that low voltage dramatically reduced the radiation dose (by 40–50%, Table 4). Thus, transformation of the low-voltage protocol into clinical application would be of great benefit for patients.
Tube voltage has a direct influence on radiation dose. McNitt-Gray estimates that if all other technical parameters are held constant, an increase of voltage from 120 kV to 140 kV on a CT/scanner will result in an increase of radiation dose by 37.5% for the head phantom and 39% for the body phantom26. Shen et al. summarized studies published from January 2011 to November 2015 that aimed to reduce radiation dose using low-tube-voltage, and discovered that low-tube-voltage was a powerful tool to reduce radiation dose, although most of the reviewed studies were conducted with CT angiography27. For example, Wang et al. showed a marked reduction in radiation dose with an 80 kV protocol compared with 100 kV and 120 kV settings in coronary CT angiography28, and similar results were reported in pulmonary CT angiography29. However, few studies have investigated the effects of low-tube-voltage in lower extremity CT venography. Cho et al. revealed that 100 kV reduced contrast medium, but not irradiation dose compared with a 120-kV setting30. In contrast, other studies have shown that low-tube-voltage significantly reduces radiation dose in lower extremity CT venography17,31, which align with our findings.
In addition to reducing radiation dose, another advantage for low-tube-voltage is that it improves vascular enhancement. In this study, the 70 kV protocol dramatically increased venous attenuation values while the attenuation values for DVT among different protocols were similar, making it easier for radiologists to recognize DVT, which facilitates the diagnosis. We compared the diagnostic results from ultrasound scanning with those of venography in another arm of study. While each CT protocol ruled out a positive case from ultrasound examinations, the 70 kV protocol additionally identified an ultrasound-determined negative case to be positive. These results are in agreement with reports in the literature, i.e., CT venography is superior to ultrasound in the detection of lower extremity DVTs9. The 70 kV protocol corrected a false negative case in ultrasound scanning, likely a result of low voltage leading to increased difference between venous and DVT attenuation values which facilitates DVT diagnosis. Taken together, the low-voltage protocol improves DVT diagnosis, which however needs to be further validated in a large series. Previous studies of CT venography for lower limb DVT also show that low-tube-voltage increases venous enhancement17,30,31. Reduction of tube voltage leads to an increase in tube current. Hence, in this study, all protocols were set with an automated tube current, which has been shown to reduce image noise32. It has been shown that voltage reduction increases image noise17,30,31 and indeed we found group C had significantly higher noise than groups A and B at all measured segmental veins. Nevertheless, the contrast-to-noise ratio in group C was markedly elevated due to enhanced venous attenuation. Furthermore, subjective rating of images from all groups by 2 experienced radiologists did not differ significantly, indicating that 70 kV combined with the ASIR-V technique does not compromise image quality. In view of the results in radiation reduction, image quality and diagnostic accuracy, we concluded that the 70 kV protocol is superior to 100 kV protocols in the detection of lower extremity DVTs.
MBIR is superior to ASIR with regard to reduction of radiation dose and image noise. However, image reconstruction by MBIR takes about 1 h/case, substantially limiting its clinical application33. As a new generation of ASIR, ASIR-V, according to the developer, reduces radiation dose up to 82%, improves low-contrast detectability up to 135% and reduces image noise up to 84% relative to FBP (http://www3.gehealthcare.co.uk/~/media/downloads/uk/product/computed-tomography/general/ct%20-%20revolution%20evo%20asir-v%20white%20paper.pdf). A distinctive feature of ASIR-V is that it significantly reduces radiation dose, therefore a higher blending percentage of ASIR-V will result in lower radiation dose, which explains the differences between radiation doses seen between groups A and B. To our knowledge, our study is the first to investigate the effects of the ASIR-V technique in CT venography of lower extremity DVT. Our data show that ASIR-V in combination with 70 kV reduces radiation dose while maintaining image quality and enhancing the diagnostic value, suggesting this technique might be useful for the evaluation of lower extremity DVT in clinical practice.
References
Tovey, C. & Wyatt, S. Diagnosis, investigation, and management of deep vein thrombosis. BMJ. 326, 1180–1184 (2003).
Kesieme, E., Kesieme, C., Jebbin, N., Irekpita, E. & Dongo, A. Deep vein thrombosis: a clinical review. J Blood Med. 2, 59–69 (2011).
Di Nisio, M., van Es, N. & Büller, H. R. Deep vein thrombosis and pulmonary embolism. Lancet. 388, 3060–3073 (2016).
Goldhaber, S. Z. & Bounameaux, H. Pulmonary embolism and deep vein thrombosis. Lancet. 379, 1835–1846 (2012).
Kearon, C. Natural history of venous thromboembolism. Circulation 107(23 Suppl 1), I22–130 (2003).
Jiménez, D. et al. Trends in the management and outcomes of acute pulmonary embolism: analysis from the RIETE registry. J Am Coll Cardiol. 67, 162 (2016).
Kearon, C. & Akl, E. A. Duration of anticoagulant therapy for deep vein thrombosis and pulmonary embolism. Blood. 123, 1794–1801 (2014).
Scarvelis, D. & Wells, P. S. Diagnosis and treatment of deep-vein thrombosis. CMAJ. 175, 1087–1092 (2006).
Karande, G. Y. et al. Advanced imaging in acute and chronic deep vein thrombosis. Cardiovasc Diagn Ther. 6, 493–507 (2016).
Loud, P. A., Katz, D. S., Bruce, D. A., Klippenstein, D. L. & Grossman, Z. D. Deep venous thrombosis with suspected pulmonary embolism: detection with combined CT venography and pulmonary angiography. Radiology. 219, 498–502 (2001).
Moll, S. Use of combined CT venography and CT pulmonary arteriography. J Thromb Haemost. 1, 637–639 (2003).
Brenner, D. J. & Hall, E. J. Computed tomography-an increasing source of radiation exposure. N Engl J Med. 357, 2277–2284 (2007).
Pearce, M. S. et al. Radiation exposure from CT scans in childhood and subsequent risk of leukemia and brain tumors: a retrospective cohort study. Lancet. 380, 499–505 (2012).
Sulaiman, N. et al. Comparison of low-dose coronary artery calcium scoring using low tube current technique and hybrid iterative reconstruction vs. filtered back projection. Clin Imaging. 43, 19–23 (2017).
Kim, J. H. et al. Comparison of the image qualities of filtered back-projection, adaptive statistical iterative reconstruction, and model-based iterative reconstruction for CT venography at 80 kV. Eur Radiol. 26, 2055–2063 (2016).
Nakamoto, A. et al. Diagnostic performance of reduced-dose CT with a hybrid iterative reconstruction algorithm for the detection of hypervascular liver lesions: a phantom study. Eur Radiol. 27, 2995–3003 (2017).
Oda, S. et al. Evaluation of deep vein thrombosis with reduced radiation and contrast material dose at computed tomography venography: clinical application of a combined iterative reconstruction and low-tube-voltage technique. Circ J. 76, 2614–2622 (2012).
Kwon, H. et al. The adaptive statistical iterative reconstruction-V technique for radiation dose reduction in abdominal CT: comparison with the adaptive statistical iterative reconstruction technique. Br J Radiol. 88, 20150463 (2015).
Lim, K. et al. Initial phantom study comparing image quality in computed tomography using adaptive statistical iterative reconstruction and new adaptive statistical iterative reconstruction v. J Comput Assist Tomogr. 39, 443–448 (2015).
Goodenberger, M. H. et al. Computed tomography image quality evaluation of a new iterative reconstruction algorithm in the abdomen (adaptive statistical iterative reconstruction-V) a comparison with model-based iterative reconstruction, adaptive statistical iterative reconstruction, and filtered back projection reconstructions. J Comput Assist Tomogr., https://doi.org/10.1097/RCT.0000000000000666 (2017).
Gatti, M. et al. Adaptive statistical iterative reconstruction-V versus adaptive statistical iterative reconstruction: impact on dose reduction and image quality in body computed tomography. J Comput Assist Tomogr. 42, 191–196 (2018).
Geyer, L. L. et al. State of the art: iterative CT reconstruction techniques. Radiology. 276, 339–357 (2015).
Mettler, F. A. Jr. et al. Radiologic and nuclear medicine studies in the United States and worldwide: frequency, radiation dose, and comparison with other radiation sources 1950–2007. Radiology. 253, 520–531 (2009).
Smith-Bindman, R. et al. Radiation dose associated with common computed tomography examinations and the associated lifetime attributable risk of cancer. Arch Intern Med. 169, 2078–2086 (2009).
Hricak, H. et al. Managing radiation use in medical imaging: a multifaceted challenge. Radiology. 258, 889–905 (2011).
McNitt-Gray, M. F. AAPM/RSNA physics tutorial for residents: topics in CT. Radiation dose in CT. Radiographics. 22, 1541–1553 (2002).
Shen, Y. et al. Did low-tube-voltage CT combined with low contrast media burden protocols accomplish the goal of “double low” for patients? An overview of applications in vessels and abdominal parenchymal organs over the past 5 years. Int J Clin Pract. 70(Suppl 9B), B5–B15 (2016).
Wang, D. et al. Image quality and dose performance of 80 kV low dose scan protocol in high-pitch spiral coronary CT angiography: feasibility study. Int J Cardiovasc Imaging. 28, 415–423 (2012).
Szucs-Farkas, Z. et al. Diagnostic accuracy of computed tomography pulmonary angiography with reduced radiation and contrast material dose: a prospective randomized clinical trial. Invest Radiol. 49, 201–208 (2014).
Cho, E. S. et al. CT venography for deep vein thrombosis using a low-tube-voltage (100 kVp) setting could increase venous enhancement and reduce the amount of administered iodine. Korean J Radiol. 14, 183–193 (2013).
Oda, S. et al. Indirect computed tomography venography with a low-tube-voltage technique: reduction in the radiation and contrast material dose–a prospective randomized study. J Comput Assist Tomogr. 35, 631–636 (2011).
Schindera, S. T. et al. Effect of automatic tube current modulation on radiation dose and image quality for low-tube-voltage multidetector row CT angiography: phantom study. Acad Radiol. 16, 997–1002 (2009).
Ning, P., Zhu, S., Shi, D., Guo, Y. & Sun, M. X-ray dose reduction in abdominal computed tomography using advanced iterative reconstruction algorithms. Plos One. 9, e92568 (2014).
Acknowledgements
We sincerely thank Dr. Qiuwang Zhang and Mr. Anthony Cannavicci from the Keenan Research Center for Biomedical Sciences at the Li Ka Shing Knowledge Institute, St. Michael’s Hospital, University of Toronto for help in English editing.
Author information
Authors and Affiliations
Contributions
D.C., J.Z., Q.G. and M.X. recruited patients, performed C.T. scanning and analyzed the data; D.C. searched the literature and wrote the manuscript; W.Q. and X.L. collected and analyzed the data; X.W. participated in C.T. procedure and data collection. P.W. conceived the concept, designed the study, critically revised and finally approved the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, D., Zhou, J., Wang, P. et al. Low-tube-voltage combined with adaptive statistical iterative reconstruction-V technique in CT venography of lower limb deep vein thrombosis. Sci Rep 8, 11174 (2018). https://doi.org/10.1038/s41598-018-29519-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-29519-y
- Springer Nature Limited
This article is cited by
-
Imaging Modalities for Detecting Deep Venous Thrombosis After Bariatric Surgery
Current Surgery Reports (2018)