Abstract
Purpose
Our aim was to study the anatomy of the left and right main adrenal veins (LAV and RAV) and to identify their anatomical variations in order to see the practical application of these findings to adrenal venous sampling (AVS).
Methods
Our work is based on dissection of 80 adrenal glands from fresh corpses in the forensic medicine department. We studied the number, the drainage, the direction and the level of termination of the main adrenal veins.
Results
The average length of the LAV was 21 mm. It ended in 100% of cases at the upper edge of the left renal vein with a mean connection angle of 70° and after an anastomosis with the lower phrenic vein in 36 cases(90%). The average length of the RAV was 9 mm. It ended in 100% of cases at the level of the retro hepatic inferior vena cava (IVC) mainly on its posterior face in 21 cases (53%) and on its right lateral border in 18 cases (45%). The mean angle of the RAV in relation to the vertical axis of the IVC was 40°, with extremes ranging from 15° to 90°.
Conclusions
AVS seems to be easier on the left than on the right side because of the greater length of the adrenal vein (21 mm vs. 9 mm) and a greater angle of connection (70° with the left renal vein vs. 40° with the IVC), which explains the lower success rate of cannulation and the more frequent occurrence of blood sample contamination on the right side.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary aldosteronism (PA) is caused by an excessive and abnormal overproduction of aldosterone from the cortex of one or both adrenal glands [5]. Its current prevalence is estimated to be around 5–13% in the general hypertensive population making this etiology the most frequent cause of secondary hypertension [7, 10]. PA is caused by bilateral adrenal hyperplasia which requires medical treatment with mineralocorticoid receptor antagonists (MRA) or by an aldosterone producing adenoma which is a potentially surgically curable condition [9]. Patients with PA have a two to five times increased risk of myocardial infarction, coronary heart disease, heart failure and atrial fibrillation compared to matched patients with essential hypertension [20]. In the long-term, PA causes fibrosis and remodeling in critical organs which leads to increased risk of cardiovascular, renal and cerebrovascular morbidity and mortality [3, 17, 24]. For this reason, an early diagnosis and specific treatment are important to revert target organ damage and prevent cardiovascular events. Once the diagnosis of PA has been confirmed, subtype classification is of fundamental importance to distinguish between unilateral and bilateral PA. According to the Endocrine Society Guideline, a subtype diagnosis is based on adrenal CT scanning and adrenal venous sampling (AVS) [9].
AVS remains an expensive procedure, available only in expert tertiary centers and technically challenging [15], especially in terms of successfully cannulating the right adrenal vein. In a review of the literature including 47 studies, the success rate for cannulating the right adrenal veins in 384 patients was 74% [25]. The complication rate associated with AVS is 2.5% or lower at centers with experienced radiologists, mainly represented by adrenal hemorrhage [6, 12].
Knowledge of the drainage of the main adrenal veins and their anatomical variations is a key factor in significantly improving sampling success and limiting the risk of bleeding.
The objective of our cadaveric anatomical research was to study the anatomy of the left and right adrenal principal veins and their anatomical variations in order to extrapolate these anatomical findings when performing an AVS.
Materials and methods
Our work is a prospective study based on the anatomical dissection of fresh donated bodies in the autopsy room of the legal and forensic medicine department at a Teaching Hospital between August 2014 and December 2016 after approval of the hospital’s research ethics committee.
We included all specimens of adult subjects dead in the previous 24 h in different circumstances (trauma, drowning, and sudden death). The donated bodies with history of retro peritoneal or adrenal surgery and whose death occurred after an abdominal trauma where the lesions of organs and hemorrhagic suffusions could interfere with the identification of anatomical elements, were not included. Out of 53 dissected cadavers, 40 donated bodies were retained on the basis of inclusion, non-inclusion and exclusion criteria. The mean age of the subjects included in this study was 37.8 years. The extremes of age were 19 and 78 years. Of the 40 subjects studied, 28 were male (70%) and 12 were female (30%). The sex ratio of the study population was 2.3.
All the measurements were carried out in situ in the same way on both sides. The lengths and diameters were measured in millimeters using a Vernier caliper. The donated bodies were placed in the supine position with their arms lying alongside. A rubber block was placed under the scapular points to allow better exposure of the retro-peritoneal region.
A mento-pubic incision was made. Intra-abdominal organs were left in place and the vessels were left filled with blood to get closer to the dissection conditions in the living. We didn’t use any injection or coloring method.
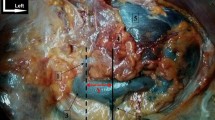
To access the right adrenal gland, we started by releasing the liver with a section of the right triangular ligament which was followed to the level of the origin of the supra-hepatic veins. Dislocation of the liver allowed progressive release of the adrenal compartment from its attachment to the posterior surface of the caudate lobe of the liver, exposing the right adrenal gland (Fig. 1a).
Dissection of the right and left adrenal glands a Detachment from the posterior surface of the right liver to the right edge of the inferior vena cava (IVC) to allow access to the right adrenal gland, 1: Right adrenal gland, 2: Right kidney, 3: Right liver, 4: IVC, 5: Diaphragm. b Opening of the posterior parietal peritoneum and Gerota fascia (red arrows) to allow access to the left adrenal gland, 1: Left adrenal gland, 2: Left kidney, 3: Pancreas, 4: Spleen, 5: Left colonic angle
To access the left adrenal gland, we took off the left colon starting from the left colic angle to the sigmoid colon. We then incised the suspensory ligaments of the spleen which was mobilized upwards with the tail of the pancreas thus exposing the left adrenal gland (Fig. 1b).
For each side, the measurements performed were:
-
The length of the main adrenal vein.
-
The width of the main adrenal vein.
-
We studied the number of adrenal veins.
-
We studied the drainage of the main adrenal vein as well as its level of termination.
-
We measured the distance between the level of termination of the left main adrenal vein and the level of termination of the gonadal vein in the left renal vein: Y Distance.
Results
Left adrenal vein
Biometrics
The average length of the left adrenal vein was 21 mm ranging from 10 to 32 mm.
The mean width of the left adrenal vein was 5 mm ranging from 2 to 7 mm (Fig. 2).
Drainage and anatomical variants
The left adrenal vein ended in 100% of cases at the upper edge of the left renal vein:
-
After an anastomosis with the lower phrenic vein in 36 cases (90%) (Fig. 3).
-
Without anastomosis with the lower phrenic vein in four cases (10%).
The left adrenal vein ended at the upper edge of the left renal vein, either :
-
At the same level as the termination of the left gonadal vein in 14 cases (35%).
-
Medial to the termination of the left gonadal vein in 26 cases (65%). In this case, the left adrenal vein was medial to the left gonadal vein by an average of 8 mm with extremes ranging from 2 to 20 mm (Fig. 4).
The number of left adrenal veins was variable :
-
In 22 cases (55%), a unique central adrenal vein was found.
-
In 12 cases (30%), a major central adrenal vein with several small veins was found.
-
In six cases (15%), two major central adrenal veins were found.
Direction
The direction of the left adrenal vein was :
-
oblique from top to bottom and from outside to inside in 19 cases (47.5%).
-
almost vertical in 21 cases (52.5%).
The mean angle of the left adrenal vein in relation to the horizontal axis of the left renal vein (Fig. 5) was 70° towards the kidney, ranging from 35° to 90°. In 75% of cases, this angle was between 70° and 90°.
Right adrenal vein
Biometrics
The average length of the right adrenal vein was 9 mm ranging from 4 to 20 mm.
The mean width of the right adrenal vein was 4 mm ranging from 2 to 5 mm (Fig. 6).
Drainage and anatomical variants
The right adrenal vein ended in 100% of cases at the level of the retro hepatic inferior vena cava (IVC) :
-
At its right lateral border in 18 cases (45%).
-
On its posterior face in 21 cases (52.5%).
-
On its anterior face via a common trunk with an accessory right hepatic vein in one case (2.5%) (Fig. 7).
The number of right adrenal veins was variable :
-
In 26 cases (65%), a single central adrenal vein was found (Fig. 8).
-
In 11 cases (27.5%) a major central adrenal vein with several small veins was found.
-
In three cases (7.5%), two major central adrenal veins were found (Fig. 9).
Direction
The direction of the right adrenal vein was :
-
oblique upwards and outwards in 38 cases (95%).
-
horizontal in 2 cases (5%).
The mean angle of the right adrenal vein in relation to the vertical axis of the IVC was 40° towards IVC, ranging from 15° to 90°. In 65% of cases this angle was between 30° and 50° (Fig. 10).
Discussion
AVS is an invasive procedure that aims to identify lateralized aldosterone secretion along a gradient between the right and left adrenal venous effluents [6]. It involves the introduction of catheters through the femoral vein to measure aldosterone and cortisol concentrations in the right and IVC and adrenal veins either simultaneously or sequentially [18]. According to the majority of authors, it is useful to precede it by an adrenal CT scan to identify the anatomical landmarks which will allow easier catheterization, especially of the right adrenal vein [6, 12]. Indeed, the exact anatomy of the adrenal veins is identified in 76% of cases by high resolution adrenal CT scan [14]. AVS remains a complex procedure with failure rates of 10–20% [14, 18, 19].
The failures are mainly related the difficulty of catheterizing the right adrenal vein for several reasons:
1/ The right adrenal vein which drains into the IVC is short. In our study we found study that the mean length of the right adrenal vein was 9 mm with extremes ranging from 4 to 20 mm whereas in other cadaveric and radiological studies the mean length of the right adrenal vein varied from 4 to 7 mm with extremes ranging from 1 to 15 mm [8, 14, 22]. When the right adrenal vein is catheterized, its short length makes it difficult for the catheter to be stable and blood collection becomes difficult, particularly due to respiratory movements and because of the compression of the IVC secondary to the patient lying down during the procedure [6, 12, 26].
2/ The right adrenal vein which drains into the right posterior wall of the IVC which makes the passage of the catheter from IVC to the right adrenal vein difficult requiring an even more difficult rotational movement in cases where the vein drains into the left posterior quadrant reported in 3 to 23% of cases [6, 12,13,14, 26]. In our study we found that the right adrenal vein ended up at the right lateral border of the IVC in 45%, posteriorly in 52.5% and anteriorly in 2.5% of cases. Ending in the anterior face of the IVC may be responsible for additional difficulty in recognizing the adrenal vein and for the rotation of the catheter.
3/ The acute angle caudally of the right adrenal vein in relation to the vertical axis of the IVC explains the difficulties in catheterizing the right vein in comparison with the left vein, whose angle in relation to the horizontal axis of the left renal vein is more open. This angulation causes the tip of the catheter to jam against the wall of the vein which will prevent the catheter from progressing and hinder the collection of blood samples [14, 26]. The angle of the right adrenal vein abutment to the vertical axis of the IVC was measured by Matsuura et al. on a radiological study and ranged from 30° to 136° with a mean of 73° [14]. Most of the patients had a value between 50° and 90° [14]. In our study the mean angulation was 40° with extremes ranging from 15° to 90° and in the majority of cases the value was between 30° and 50°.
4/ The right adrenal vein can sometimes be difficult to differentiate from an accessory hepatic vein. In our study there was a case of a right adrenal vein which terminated at the anterior wall of the IVC via a common trunk with an accessory hepatic vein. This variant has been reported by several authors with a frequency that varies from 8 to 10% depending on the series [14, 16, 22]. The common trunk often terminates in the anterior wall of the retrohepatic IVC more rarely in the right lateral border [14]. In this variant, the catheter tip must be advanced selectively into the right adrenal vein, as holding the catheter in the common trunk will result in a contaminated sample of blood from the accessory hepatic vein, which will distort the results [6, 13, 14]. The other risk is the erroneous advancement of the catheter in the accessory hepatic vein [6]. Other unusual anastomoses of the right adrenal vein with intercostal veins or the phrenic vein as well as direct drainage into the right renal vein may be accompanied by additional difficulty in AVS, especially in identifying the adrenal vein [6, 13, 14].
In contrast to the difficult catheterization of the right adrenal vein, catheterization of the left vein is relatively simpler with success rates of over 90% [6, 13, 14]. This is because the left adrenal vein drains into the left renal vein, is longer and therefore more easily accessible.
In our study its length was 21 mm on average with extremes ranging from 10 to 32 mm. In other cadaveric and radiological studies the length varied from 10 to 40 mm [8, 11, 22]. This relatively long length helps to stabilise the catheter and makes sampling easier. The mean angle of the left adrenal vein to the horizontal axis of the left renal vein in our study was 73° with extremes ranging from 35° to 90°. In 75% of cases, it was between 70° and 90°. This angle has not been measured in any study, but the left adrenal vein has been described as parallel to the left edge of the spine, suggesting that the angle is close to 90° [13]. This relatively open angle makes it easier for the catheter to pass through and prevents the tip of the catheter from getting stuck against the wall of the vein.
Although left adrenal vein catheterization is described as relatively easy, there are situations and anatomical variations that can make the procedure more complex [13].
Typically, the left adrenal vein anastomoses with the inferior phrenic vein and ends in the superior border of the left renal vein via a common trunk [2, 4, 11].
In our study this anastomosis was absent in six cases and the left adrenal vein and the left inferior phrenic vein terminated separately in the left renal vein in 15% of cases. In the literature, this anastomosis is relatively constant, with cases of separate termination of the two veins not exceeding 1% [1, 21]. This notion is important because the tip of the catheter must be placed selectively in the left adrenal vein, neither in the common trunk nor in the left inferior phrenic vein, in order to avoid contamination of the sample by blood from the phrenic vein [6]. Distinguishing the adrenal vein from the inferior phrenic vein on the venogram is usually possible because the adrenal vein is more lateral and is non-valvular [6]. Other unusual anastomoses of the left adrenal vein with lumbar, hemi-azygos or even genital veins may be seen and may be accompanied by additional difficulty in AVS, especially in identifying the adrenal vein [6, 13, 14].
Anatomical variants such as a direct connection of the left adrenal vein to the left lateral border of the IVC have only been reported twice in the literature [23]. This variant was not recorded in our series.
A left renal vein anomaly of the type of periaortic renal vein has been reported with a mean frequency of 5.7%, ranging from 0.2 to 30%. This variant is defined by the presence of two veins on each side of the aorta [6, 8, 13, 14].
Daunt has shown that in the case of a periaortic renal vein, the left adrenal vein drains into the retro aortic vein which is below the 4 cm pre-aortic vein (usually at the level of L3), and catheterization should be performed via this retro aortic vein [6]. In contrast to Daunt, Sebe et al. [22] reported that drainage was always into the preaortic vein and in this case catheterization was performed via the latter.
All these variants and possibilities of anastomosis of the adrenal vein with the neighbouring veins can increase the risk of complications, which remain rare at less than 2.5% [6, 12]. The main complication of AVS is intra and peri-glandular haematoma [6, 12, 26]. Other complications reported in the literature are vein perforation, thrombosis, adrenal ischaemia with risk of adrenal insufficiency and hypertensive crises [6, 12, 26].
Our study has few limitations :
-
The injection and corrosion methods were not used. Injection-corrosion specimens are very fragile, and in most cases fragile tissues such as adrenal veins are damaged, making analysis impossible.
-
The limited number of donated bodies studied. However, in most of the series that have studied adrenal anatomy in cadavers, the number of subjects has not exceeded 40. This anatomical study has clinical application in interventional radiology. As future development perspectives, this project could be enriched by other anatomical-radiological work, based on cadaveric dissection data, on high resolution CT or MRI venography images and on large prospective intraoperative laparoscopic studies.
Conclusion
The results of our work show that the left main adrenal vein has a relatively modal anatomy but there are variations. The most important one being direct drainage into the left renal vein without anastomosis with the lower phrenic vein. As described in previous studies published in the literature, the right adrenal vein has a length that is short with an acute angle of abutment with the inferior vena cava and its identification can be confusing when it achieves anatomical variations in its termination, especially with accessory hepatic veins that may form a common stem with the right adrenal vein.
All these findings help to explain the relative simplicity of catheterization of the left adrenal vein, in contrast to the greater difficulty of catheterization of the right adrenal vein.
Data availability
Data is available on demand.
References
Anson BJ, Cauldwell EW, Pick JW et al (1948) The anatomy of the Pararenal System of veins, with comments on the renal arteries. J Urol 60:714–737
Avisse C, Marcus C, Patey M et al (2000) Surgical anatomy and embryology of the adrenal glands. Surg Clin North Am 80:403–415
Catena C, Colussi GL, Nadalini E et al (2008) Cardiovascular outcomes in patients with primary aldosteronism after treatment. Arch Intern Med 168:80–85
Cesmebasi A, Du Plessis M, Iannatuono M et al (2014) A review of the anatomy and clinical significance of adrenal veins: the anatomy and clinical significance of AV. Clin Anat 27:1253–1263
Conn JW (1955) Primary aldosteronism. J Lab Clin Med 45:661–664
Daunt N (2005) Adrenal vein sampling: how to make it quick, Easy, and successful. Radiographics 25:S143–S158
Douma S, Petidis K, Doumas M et al (2008) Prevalence of primary hyperaldosteronism in resistant hypertension: a retrospective observational study. Lancet 371:1921–1926
El-Sherief MA (1982) Adrenal vein catheterization: anatomic considerations. Acta Radiol Diagn (Stockh) 23:345–360
Funder JW, Carey RM, Mantero F et al (2016) The management of primary aldosteronism: case detection, diagnosis, and treatment: an endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab 101:1889–1916
Hannemann A, Wallaschofski H (2012) Prevalence of primary aldosteronism in patient’s cohorts and in population-based studies - a review of the current literature. Horm Metab Res 44:157–162
Hureau J, Hidden G, Minh ATT (1979) Vascularisation Des glandes surrénales. Anat Clin 2:127–146. https://doi.org/10.1007/BF01654426
Kahn SL, Angle JF (2010) Adrenal vein sampling. Tech Vasc Interv Radiol 13:110–125
Kahn PC, Lester V, Nickrocz MD (1970) Selective adrenal angiography. Cesk Radiol 24:4–7
Matsuura T, Takase K, Ota H et al (2008) Radiologic anatomy of the right adrenal vein: preliminary experience with MDCT. AJR Am J Roentgenol 191:402–408
Monticone S, Viola A, Rossato D et al (2015) Adrenal vein sampling in primary aldosteronism: towards a standardised protocol. Lancet Diabetes Endocrinol 3:296–303
Nakamura S, Tsuzuki T (1981) Surgical anatomy of the hepatic veins and the inferior vena cava. Surg Gynecol Obstet 152:43–50
Rossi GP, Bernini G, Desideri G et al (2006) Renal damage in primary aldosteronism: results of the PAPY study. Hypertension 48:232–238
Rossi GP, Auchus RJ, Brown M et al (2014) An Expert Consensus Statement on Use of adrenal vein sampling for the subtyping of primary Aldosteronism. Hypertension 63:151–160
Sarlon-Bartoli G, Michel N, Taieb D et al (2011) Adrenal venous sampling is crucial before an adrenalectomy whatever the adrenal-nodule size on computed tomography. J Hypertens 29:1196–1202
Savard S, Amar L, Plouin PF et al (2013) Cardiovascular complications associated with primary aldosteronism: a controlled cross-sectional study. Hypertension 62:331–336
Scholten A, Cisco RM, Vriens MR et al (2013) Variant adrenal venous anatomy in 546 laparoscopic adrenalectomies. JAMA Surg 148:378
Sèbe P, Peyromaure M, Raynaud A et al (2002) Anatomical variations in the drainage of the principal adrenal veins: the results of 88 venograms. Surg Radiol Anat 24:222–225
Stack SP, Rösch J, Cook DM et al (2001) Anomalous left adrenal venous drainage directly into the Inferior Vena Cava. J Vasc Interv Radiol 12:385–387
Stowasser M (2001) New perspectives on the role of aldosterone excess in cardiovascular disease. Clin Exp Pharmacol Physiol 28:783–791
Young WF, Klee GG (1988) Primary aldosteronism. Diagnostic evaluation. Endocrinol Metab Clin North Am 17:367–395
Young WF, Stanson AW (2009) What are the keys to successful adrenal venous sampling (AVS) in patients with primary aldosteronism? Clin Endocrinol (Oxf) 70:14–17
Acknowledgements
The authors would like to express their sincere gratitude to those who have donated their bodies to science so that anatomical research can be carried out. The results of such research have the potential to increase human knowledge, which in turn can improve patient care. Therefore, these donors and their families deserve our highest gratitude.
Funding
No funding was received.
Author information
Authors and Affiliations
Contributions
A. Saadi: Protocol development; Data collection or management; Data analysis; Manuscript writing MA. Bedoui : Data collection or management; Data analysis; Manuscript writing S. Mokadem : Manuscript editing S. Zaghbib : Manuscript editing H. Boussaffa : Manuscript editing M. Bellali : Manuscript editing H. Ayed: Manuscript editing A. Bouzouita: Manuscript editing A. Derouiche: Manuscript editing M. Allouche: Manuscript editing M. Chakroun : Manuscript editing R. Ben Slama : Manuscript editing.
Corresponding author
Ethics declarations
Ethical approval
The approval of the current study has been granted by the medical committee of research ethics of Charles Nicolle Hospital. A copy of the approval is available for review by the Editor-in-Chief of this journal on request. Reference number is not available.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Saadi, A., Bedoui, M., Mokadem, S. et al. Anatomy and anatomical variations of adrenal veins and its application to adrenal venous sampling. Surg Radiol Anat 46, 543–550 (2024). https://doi.org/10.1007/s00276-024-03331-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-024-03331-y