Abstract
Purpose
Interosseous tuberosities have been described in adults on the radial and ulnar sides. However, their presence at birth and their development during growth is still unknown. The objective of this work is to establish the age of onset of this tuberosity among a cohort of children aged 1-year-old or older.
Methods
All anterior–posterior and lateral radiographs performed in our hospital during a consecutive period of 6 months were retrospectively analyzed. Exclusion criteria were: presence of a fracture, a tumor, an age higher than 16 years, radiograph not performed strictly from the front with supination or from the side. On the anterior–posterior radiograph, the presence of the following structures was sought: radial interosseous tuberosity and determination of its length and width; the appearance of the epiphyseal nucleus of the radial head, of the bicipital tuberosity, and of the distal epiphysis. On the lateral views, the presence of the following structures was sought: ulnar interosseous tuberosity and determination of its length and width; the appearance of the olecranon epiphyseal nucleus, and the distal epiphysis.
Results
Over the review period, anterior–posterior and lateral radiographs were performed on 368 consecutive children. Finally, 179 patients were included in the radiographic analysis. The radial and ulnar interosseous tuberosities and bicipital tuberosity were present in all cases, from 1-year-old. Only the distal radial epiphysis began to appear at the age of one year, the others ossifying progressively during growth.
Conclusion
Tuberositas interossea ulnarii and radii exists, are present from 1-year-old and continue to develop during growth.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The anatomy of the ulna and radius have been represented for a long time with tuberosities on their interosseous sides [9, 10, 14, 17]. Nevertheless, true interosseous tuberosities have been described recently [11, 12]. They correspond to cortical thickenings that may play a role in forearm stability and fingers mobility, especially the thumb.
On each of the interosseous tuberosities is found the biomechanically active part of the interosseous membrane: the central band [4, 13, 15, 16]. On the radial interosseous tuberosity, most of the extrinsic muscles for the thumb (flexor pollicis longus and extensor pollicis brevis) are also found [11]. The abductor pollicis longus is attached to the upper third of the lateral side of the ulnar interosseous tuberosity and on the upper two-thirds of the radial interosseous tuberosity [11, 12]. On the lateral side of the ulnar interosseous tuberosity, the extensor pollicis longus as well as the extensor indicis are inserted, and the flexor digitorum profundus muscle is on the medial side [12]. Nevertheless, the age of appearance and ossification of this structure, as well as its development during growth, are unknown.
The objective is to describe a radiographic cohort of pediatric patients of varying ages to estimate the age of onset of these interosseous tuberosities, as well as describe their evolution. The hypothesis is that these structures could ossify during growth in response to traction phenomena at the time when the child begins to acquire a certain level of digital mobility, grip or forearm prono-supination.
Materials and methods
The study was registered with the Commission Nationale de l’Informatique et des Libertés (CNIL—no. 2227470 version 0). The review of the data was conducted in accordance with the ethical standards of the 1964 Declaration of Helsinki and the reference methodology MR-003.
Cases identification
The hospital's database was analyzed for the period between January 1, 2021 and June 30, 2022. All anterior–posterior and lateral radiographs taken over this period were retrospectively analyzed using the image archiving and communication system (PACS, Carestream Vue Pacs, version 12.1, Carestream Health, Rochester, New York, USA). Inclusion criteria were: absence of a fracture or a tumor, and age higher than 16 years. Exclusion criteria were: radiograph not made strictly from the front with supination position or the side.
Study protocol and data collection
Two observers blinded to each other were included in the analysis of the radiographs (one resident and one senior, both orthopedic surgeons). All the measurements were carried out according to the same protocol defined before the study, on a computer. The observers could zoom and manage the contrasts to obtain the most precise measurements possible.
The ulna was analyzed on the lateral radiographs and the radius on the supinated anterior–posterior radiograph. They used the same methodology previously described on the radiograph to analyze the presence of an interosseous tuberosity [11, 12]. They looked for diaphyseal cortical thickening on the interosseous side of the bone studied: if thickening was identified, the tuberosity was considered present. The beginning of the tuberosity was considered to be at the level of the start of cortical thickening, and its end at the moment when the cortical width decreased until it reached a constant value.
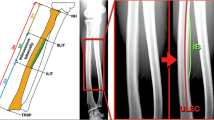
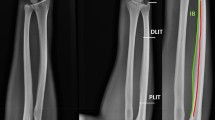
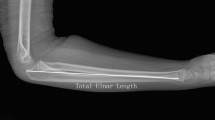
The following measurements were made on the anterior–posterior radiographs: length of the radial interosseous tuberosity (RTL), as well as the cortical width proximally (RT1), at its level (RT2), and distally (RT3). Then, the presence of the following structures was sought: appearance of the epiphyseal nucleus of the radial head, the bicipital tuberosity, and the distal epiphysis. On the lateral radiographs, the following measurements were made: length of the ulnar interosseous tuberosity (UTL), as well as the cortical width proximally (UT1), at its level (UT2), and distally (UT3). Then, the presence of the following structures was sought: the appearance of the epiphyseal nucleus of the olecranon and the distal epiphysis. Finally, the total length of the radius and ulna was measured between the two growth plates. The radiographic measurement protocol is shown in Fig. 1.
Protocol for identification and measurement of interosseous tuberosity. Identification of the radial (a) and ulnar (b) interosseous tuberosity at the level of the interosseous cortical thickening. Protocol for measuring the length of the radial interosseous tuberosity (RTL), as well as the width proximally (RT1), at its level (RT2), and distally (RT3) (c). Then identification of the ossification of the radial head, bicipital tuberosity, and distal radial epiphysis (c). Protocol for measuring the length of the ulnar interosseous tuberosity (UTL), as well as the width proximally (UT1), at its level (UT2), and distally (UT3) (d). Then identification of the ossification of the olecranon and the distal ulnar epiphysis (d)
For all radiographic measurements performed the inter-observer reproducibility was determined for the first 50 patients of the radiological series. The intra-observer reproducibility was determined with the senior observer, having performed his second series of measurements on the same patients with a delay of two months, blinded to his first results.
Statistical analysis
The Wilcoxon–Mann Whitney for unpaired data was used to analyze the association between the different variables. The alpha risk was set to 0.05. The intra-class correlation coefficient (ICC) was used to evaluate the intra-rater and inter-rater agreements in radiological measurements. An ICC value below 0.4 was considered as a poor agreement, between 0.4 and 0.75 as a good agreement, and above 0.75 as an excellent agreement. Statistical analysis was performed using software developed by Sorbonne University (R software, INSERM UMR S1136).
Results
Finally, 179 patients were included in the radiological study: 80 girls and 99 boys. The patient selection process is reported in Fig. 2. The distribution of girls and boys by age group is reported in Table 1.
Sequential development of tuberosities and ossifications of epiphyseal nuclei (Fig. 3)
On anterior–posterior radiographs, the radial interosseous tuberosity was identified from the age of one year in all cases. Ossification of the distal radial epiphyseal nucleus was present in the majority of 1-year-old subjects, and in all 2-year-old subjects. Ossification of the radial head began at the age of three years, in all girls at the age of five years, and six years for boys. In all cases, both observers were always in agreement on the identification of the presence/appearance of the radial interosseous tuberosity, the epiphyseal ossification nuclei of the radial head, the bicipital tuberosity, and the distal epiphysis. The results for the radius are shown in Fig. 4. On lateral radiographs, the ulnar interosseous tuberosity was always present from 1-year-old. Ossification of the olecranon began at the age of seven years in girls and eight years in boys. Ossification of the distal ulnar epiphysis occurred from the age of four years in girls and five years in boys. In all cases, the two observers always agreed on the identification of the presence/appearance of the ulnar interosseous tuberosity, the epiphyseal ossification nuclei of the olecranon and the distal epiphysis. The results for the ulna are shown in Fig. 5.
Evolution of interosseous tuberosities length during growth
The length of the radial and ulnar interosseous tuberosities increases during growth, as does the total bone length. The radial interosseous tuberosity represents between 25 and 34% of the total bone length depending on age. The ulnar interosseous tuberosity represents between 29 and 36% of the total bone length depending on the age. The results are shown in Fig. 6.
Evolution of interosseous tuberosities width during growth (Table 2)
The radial and ulnar interosseous tuberosities are significantly thicker than the proximally and distally located cortices at all ages analyzed, starting at 1-year-old. The radial interosseous tuberosity averaged 2 ± 0.3 mm at 1-year-old, and thickened to an average of 6.9 ± 1.1 mm at 15 years old. The ulnar interosseous tuberosity averaged 2 ± 0.3 mm at 1-year-old, and thickened to an average of 6.2 ± 1.2 mm at 15 years old.
Reproducibility of the different radiological measurements
Inter- and intra-observer reproducibility was excellent for all radiological measurements of bone length or cortical width. The results are summarized in Table 3.
Discussion
The main finding of this study is the existence of radial and ulnar interosseous tuberosities from 1-year-old, regardless of gender. In the same way, as in adults, children from the age of 1-year-old showed a significant thickening of the cortex at this level. The growth of the different interosseous tuberosities was linear in length and width throughout growth.
In adults, the mean length of the radial interosseous tuberosity was estimated to be 93.9 ± 15.8 mm, corresponding to 37% of the total radial length [11]. On the ulnar side, the average length of the interosseous tuberosity in adults was estimated to be 107 ± 5 mm [12]. These lengths in adults are slightly greater than those estimated in this series among the 15–16-year-old group. This is also the case for the ratio of tuberosity length to total radial and ulnar bone length, estimated to be approximately 37% and 40%, respectively [11, 12]. Finally, the average width of these interosseous tuberosities in the upper 15–16-year-old group was 6.9 ± 1.1 mm versus 7.6 ± 1.8 mm in adults on the radial side, and 6.2 ± 1.2 mm versus 6.9 ± 1 mm in adults on the ulnar side [11, 12]. This difference could be explained by the possible residual growth between the 16 years-old in this series, and 18 years old corresponding to the inclusion criterion of the study of adult subjects [12].
Cadaveric studies in adults have confirmed that these bony reliefs were indeed tuberosities on which the central band of the interosseous membrane [1, 2, 4,5,6] was inserted, as well as the main muscles destined for the thumb and fingers: flexor pollicis longus, abductor pollicis longus and extensor pollicis brevis for the radial interosseous tuberosity; and flexor digitorum profundus, extensor pollicis longus and extensor indicis for the ulnar interosseous tuberosity [11, 12]. The presence of a cortical thickening forming a relief is never a coincidence and is often secondary to the traction forces it absorbs [8, 11, 12]. The early appearance of these interosseous tuberosities could be explained by the fact that finger mobility is acquired very early. Indeed, a fetal ultrasound study found that all fetuses show total finger flexion and extension as early as 16 weeks of amenorrhea [7]. Numerous archaic reflexes present from birth involve finger mobility such as grasping and could maintain these forces applied to these structures. This is the hypothesis that can be put forward to explain the existence of these structures on radiographs taken as early as one year of life.
During fetal life, no tuberosity or epiphysis is visible [18]. The average age of appearance of the other structures analyzed in this series for boys and girls confirms the previous series (Table 4) [17]. However, only one discrepancy in results was found concerning the estimated appearance of the radial bicipital tuberosity. In their 1938 anatomical report, von Lanz and Wachsmuth estimated the age of onset of the radial bicipital tuberosity to be between 10 and 12 years, with no gender difference [17]. However, Eberhard performed bicipital tuberosity transpositions in children as young as 6 years of age in cases of obstetrical brachial plexus injury [3]. This suggests that the apparition of the bony tuberosity may be earlier than the estimate of von Lanz and Wachsmuth [17]. In the present series, the bicipital tuberosity was always visible, starting at the youngest age of 1–2 years. As an example, these structures are well illustrated in the four cases reported in Fig. 3. The early appearance of these tuberosities could be explained in the same way as for the interosseous tuberosities. Fetal elbow mobilities during growth and then at the newborn stage could explain the earlier appearance of these structures than previously thought. Indeed, during fetal life and the first months after birth, reflex muscle tension is predominant in the flexion of the upper limb [18]. Nevertheless, these are assumptions because the present study can only prove the presence of this tuberosity from the age of one year. Exploratory ultrasound in children under one year of age and/or newborns could help answer this question.
However, this study has several limitations. The first is its retrospective nature. Indeed, such a prospective analysis protocol is not ethical if carried out in healthy children, because it is irradiating. In addition, unlike other studies performed in adults, it is not possible to perform cadaveric studies in children, especially in the youngest age group [11, 12]. Other possibilities of radiological examinations, such as MRI, could have been considered. However, few examinations are carried out specifically on the forearms, most often for tumoral reasons, which prevents any retrospective analysis of this type of examination. Completing this radiological assessment of these bony structures with an ultrasound examination in young children could be of interest to investigate whether these interosseous tuberosities also have a thickening of their periosteum like their cortices. A specific study of the periosteum in children of each of these age groups could be very interesting and would deepen the knowledge of these structures. Another limitation is the measurement of the actual thickness of the interosseous tuberosities. It would have been preferable to measure the exact thickness by 3D CT scan, which was not possible for reasons of radiation dose in children and adolescents. Finally, it was impossible to know whether newborns have these structures from birth because no usable radiographs were taken before the age of at least one year. Further work remains to be done to confirm these results.
Conclusion
The radial and ulnar interosseous tuberosities are visible as early as 1-year-old. Their early appearance could be explained by the traction of the fingers and thumb during fetal life and the first months of life. Further studies should be performed to complement this work and investigate the presence of these tuberosities between birth and 1-year-old, particularly using ultrasound.
Data availability
Upon justified request, the data can be deposited in a data repository.
References
Adams JE (2017) Forearm instability: anatomy, biomechanics, and treatment options. J Hand Surg 42:47–52
Chandler JW, Stabile KJ, Pfaeffle HJ, Li ZM, Woo SL, Tomaino MM (2003) Anatomic parameters for planning of interosseous ligament reconstruction using computer-assisted techniques. J Hand Surg Am 28:111–116
Eberhard D (1997) Transposition of the bicipital tuberosity for treatment of fixed supination contracture in obstetric brachial plexus lesions. J Hand Surg Br 22(2):261–263
Farr LD, Werner FW, McGrattan ML, Zwerling SR, Harley BJ (2015) Anatomy and biomechanics of the forearm interosseous membrane. J Hand Surg 40:1145–1151
Green JB, Zelouf DS (2009) Forearm instability. J Hand Surg 34:953–961
Hotchkiss RN, An KN, Sowa DT, Basta S, Weiland AJ (1989) An anatomic and mechanical study of the interosseous membrane of the forearm: pathomechanics of proximal migration of the radius. J Hand Surg 14:256–326
Katz K, Mashiach R, Meizner I (2007) Normal range of fetal finger movements. J Pediatr Orthop B 16(4):252–255
Markolf KL, Lamey D, Yang S, Meals R, Hotchkiss R (1998) Radioulnar load-sharing in the forearm. A study in cadavera. J Bone Jt Surg Am 80:879–888
Miller-Keane (2003) Encyclopedia and dictionary of medicine, nursing, and allied health, 7th edn. Saunders, Elsevier, Philadelphia
Netter FH (2006) Atlas of human anatomy. Saunders/Elsevier, Philadelphia
Rougereau G, Valteau B, Creze M, Soubeyrand M (2021) The interosseous tuberosity of radius: a descriptive radiological and cadaveric anatomical study. Surg Radiol Anat 43(5):727–734
Rougereau G, Langlais T, Valteau B, Creze M, Soubeyrand M (2021) The ulnar interosseous tuberosity exists: a radiological and descriptive cadaveric study. Surg Radiol Anat 43(10):1609–1617
Rougereau G, Marty-Diloy T, Vigan M, Vialle R, Soubeyrand M, Langlais T (2022) Biomechanical assessment of the central band of the interosseous membrane using shear wave elastography: reliability and reproducibility. J Hand Surg Eur 11:17531934221114300
Rouvière H (1976) Précis d’anatomie et de dissections. Masson, Paris
Soubeyrand M, Oberlin C, Dumontier C, Belkheyar Z, Lafont C, Degeorges R (2006) Ligamentoplasty of the forearm interosseous membrane using the semitendinosus tendon: anatomical study and surgical procedure. Surg Radiol Anat 28:300–307
Soubeyrand M, Wassermann V, Hirsch C, Oberlin C, Gagey O, Dumontier C (2011) The middle radioulnar joint and triarticular forearm complex. J Hand Surg Eur 36:447–454
Von Lanz T, Wachsmuth W (1938) Praktische anatomie. Julius Springer, Berlin
Wiśniewski M, Baumgart M, Grzonkowska M, Siedlecki Z, Piec M, Szpinda M, Pawlak-Osińska K (2019) Quantitative anatomy of the primary ossification center of the radial shaft in human fetuses. Surg Radiol Anat 41(8):901–909
Funding
None.
Author information
Authors and Affiliations
Contributions
NM: data collection, data analysis. TL: data analysis, manuscript validation. MS: project development, manuscript validation. RV: project development, manuscript validation. MC: radiological assessment protocol validation, manuscript validation. GR: data collection, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
RV is occasional consultant for Nuvasive, Eos imaging and Stryker, outside the scope of this work. Other authors do not have competing interests.
Ethical approval
The study was registered with the Commission Nationale de l’Informatique et des Libertés (CNIL—no. 2227470 version 0). The review of the data was conducted in accordance with the ethical standards of the 1964 Declaration of Helsinki and the reference methodology MR-003.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mainard, N., Langlais, T., Soubeyrand, M. et al. The interosseous tuberosities of the forearm exist from 1-year-old: a pediatric radiological study describing the ages of appearance of the different forearm reliefs. Surg Radiol Anat 45, 593–602 (2023). https://doi.org/10.1007/s00276-023-03119-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-023-03119-6